Abstract
Background: There are several new strategies proposed to improve the outcome of patients with ST-elevation myocardial infarction (STEMI). One approach is the resurgent use of facilitated percutaneous coronary interventions (PCI). Until recently, deciding whether immediate PCI after combined treatment (facilitated PCI) is more appropriate than delayed PCI (short time) has not been investigated. The aim of this study, therefore, was to investigate the outcomes in patients initially successfully treated pharmacologically and immediate PCI < 2 hr, and in patients initially successfully treated with pharmacological therapy and with delayed PCI (12–72 h).
Methods: 451 reperfused STEMI patients, aged 18 to 75 years, class I–II Killip, with an acceptable echocardiographic window and admitted within 12 hs of the onset of symptoms were randomized into two groups. All patients had to have successful reperfusion, to receive the combination of a standard tirofiban infusion or abciximab plus half dose rtPA. Thereafter, patients were sub-grouped as follows:group 1 (immediate PCI) patients had PCI within 2 h; and group 2 (delayed PCI) patients in which PCI was performed after 12 hs and within 72 hs.
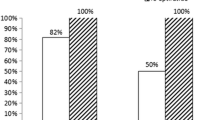
Results: The 225 reperfused (immediate-PCI) and 226 reperfused (delayed-PCI) patients (time from randomization to PCI 165 ± 37 min in immediate PCI versus 45.1 ± 20.2 h in delayed PCI group) showed similar results in ejection fraction, CK release and patency of the IRA. In addition, the delayed PCI group showed a significant reduction in ischemic events, restenosis and bleedings (P = 0.005, 0.01, 0.01 respectively) and significant reduced angiographic evidence of thrombus formation in the infarction-related artery (IRA) (p = 0.001).
Conclusion: Our data suggest the safety and possible use of delayed facilitated PCI in patients with STEMI, and that delayed PCI in patients treated with combined lytic and IIb/IIIa inhibitors appears to be as effective and possibly superior (reduced ischemic events and repeat PCI) as immediate PCI. The patients in this study were successfully reperfused, with TIMI-3 flow and our data may not apply to patients with TIMI 0–2 flow. This strategy could allow transferring the reperfused patients and performing PCI after hours < 72 hours and not immediately, thereby reducing the number of urgent PCI and costs, obtaining similar results, but mostly causing less discomfort to the patient. Our results had to be interpreted with caution, because current guidelines do not recommend the combined therapy, but suggest further studies.
Abbreviated abstract
The study was aimed to investigate the outcomes in patients initially successfully treated pharmacologically and immediate PCI < 2 h, and in patients initially successfully treated with pharmacological therapy and delayed PCI (12–72 h). All patients had to have successful reperfusion, to receive the combination of a standard abciximab or tirofiban infusion plus half dose rtPA. Similar results were observed in both groups. Delayed PCI group showed a significant lower incidence in restenosis (0.01), minor bleedings (0.005), ischemic events (0.01) and a reduced angiographic evidence of thrombus formation in IRA (0.001). Our data suggest the safety and possible use of delayed facilitated PCI in patients with STEMI. Our results had to be interpreted with caution, because current guidelines do not recommend the combined therapy, but suggest further studies.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Topol EJ. Current status and future prospects for acute myocardial infarction therapy. Circulation 2003;108 (suppl III): III-6-III-13.
Weaver WD, Simes RJ, Betrin A, et al. Comparison of primary angioplasty and intravenous thrombolityc therapy for acute myocardial infarction:a quantitative overview. JAMA 1997;278:2093–2098.
Keeley EC, Boura JA, Grines CL. Primary angioplasty versus intravenous thrombolytic therapy for acute myocardial infarction:a quantitative overview of 23 randomized trials. Lancet 2003;361:13–20.
Widimsky P, Budesinsky T, Vorac D, et al. Long distance transport for primary angioplasty vs immediate thrombolysis in acute myocardial infarction: final results of the randomized national multicentre trial-PRAGUE-2. Eur Heart J 2003;24:94–104.
Grines CL, Westerhausen DR, Grines LL, et al. A randomized trial of transfer for primary angioplasty versuson-site thrombolysis in high risk myocardial infarction:the Air Primary Angioplasty in Myocardial Infarction study. J Am Coll Cardiol 2002;39:1713–1719. (ARIRPAMI).
Andersen HR, Nielsen TT, Rasmussen K, et al. for the DANAMI-2 investigators. A comparison of coronary angioplasty with fibrinolytic therapy in acute myocardial infarction. N Engl J Med 2003;349:733–742.
Bonnefoy E, Lapostolle F, Leizorovicz A, et al. on behalf of the Comparison of Angioplasty and prehospital thrombolysis in acute myocardial infarction (CAPTIM) study group. Primary angioplasty versus prehospital fibrinolysis in acute myocardial infarction:a randomised study. Lancet 2002;360:825–829.
Scheller B, Hennen B, Hammer B, et al. And SIAM III Study Group. Beneficial effects of immediate stenting after thrombolysis in acute myocardial infarction J Am Coll Cardiol 2003;42:634–641.
Ross AM, Coyne KS, Reiner JS, et al. A randomized trial comparing primary angioplasty with a strategy of short-acting thrombolysis and immediate planned rescue angioplasty in acute myocardial infarction: the PACT trial. J Am Coll Cardiol 1999;34.1954–1962.
Gibson CM. A union in reperfusion: the concept of facilitated percutaneous coronary intervention. J Am Coll Cardiol 2000;36;1497–1451.
Schweiger MJ, Cannon CP, Murphy SA, et al. and the TIMI 10B and TIMI 14 Investigators. Early coronary intervention following pharmacologic therapy for acute myocardial infarction (the combined TIMI 10B-TIMI14 experience). Am J Cardiol 2001:88:831–836.
Antman EM, Giugliano RP, Gibson CM, et al. for the Thrombolysis in Myocardial Infarction (TIMI) 14 Investigators. Abciximab facilitates the rate and the extent of thrombolysis: results of the thrombolysis in myocardial infarction (TIMI) 14 trial. Circulation 1999;99:2720–2732.
Hermann HC, Moliterno DJ, Ohman EM, et al. Facilitation of early percutaneous coronary intervention after reteplase with or without abciximab in acute myocardial infarction:Results from the SPEED (GUSTO-4 Pilot)trial. J Am Coll Cardiol 2000;36:1489–1496.
Di Pasquale P, Cannizzaro S, Giambanco F, et al. Immediate versus delayed facilitated percutaneous coronary intervention: a pilot study. J Cardiovasc Pharmacol 2005:46(1):83–88.
Cura FA, Roffi M, Pasca N, et al. ST-segment resolution 60 minutes after combination treatment of abciximab with reteplase or reteplase alone for acute myocardial infarction (30-day mortality results from the resolution of ST-segment after reperfusion therapy substudy). Am J Cardiol 2004 1;94(7):859–863.
Dong J, Ndrepepa G, Schmitt C, Mehilli J, et al. A.Early Resolution of ST-Segment Elevation Correlates with Myocardial Salvage Assessed by Tc-99m Sestamibi Scintigraphy in Patients With Acute Myocardial Infarction After Mechanical or Thrombolytic Reperfusion Therapy. Circulation 2002;105:2946.
Schröder R. Prognostic. Impact of Early ST-Segment Resolution in Acute ST-Elevation Myocardial Infarction. Circulation 2004;110:e506–e510.
Core JM, Sloan M, Price T, et al. Intracerebral hemmorrhage, cerebral infarction, and subdural hematoma after acute myocardial infarction and thrombolytic therapy in the Thrombolysis in Myocardial Infarction Study:Thrombolysis in Myocardial Infarction, phase II, pilot and clinical trial. Circulation 1991;83:448–459.
TIMI Study Group. The Thrombolysis in Myocardial Infarction (TIMI) trial. Phase I findings. N Engl J Med 1985;312:932–936.
Di Pasquale P, Bucca V, Giuliano P, Maringhini G, Scalzo S, Paterna S.Advantages of immediate two-dimensional echocardiography in patients with acute cardiac ischemic events.Intern. J Cardiol 1995;51:85–91.
Cannon CP, Gibson CM, Lambrew CT, et al. Relantionship of symptom-onset–to-balloon time and door-to balloon time with mortality in patients undergoing angioplasty for acute myocardial infarction. JAMA 2000;283:2941–2947.
Stone GW, Cox D, Garcia E, et al. Normal Flow (TIMI-3) before mechanical reperfusion therapy i san independent determinant of survival in acute myocardial infarction. Circulation 2001;104:636–641.
Cannon CP. Importance of TIMI 3 flow. Circulation 2001;104:624–626.
Grines CL, Browne KF, Marco J, et al. A comparison of immediate angioplasty with thrombolytic therapy for acute myocardial infarction: the Primary Angioplasty in Myocardial Infarction study group. N Engl J Med 1993;328:673–679.
Nallamothu BK, Bates ER. Percutaneous coronary intervention versus fibrinolytic therapy in acute myocardial infarction: is timing (almost) everything? Am J Cardiol 2003;92:824–826.
Fernandez-Aviles F, et al. On behalf of GRACIA-2 investigators. Primary optimal percutaneous coronary intervention versus facilitated intervention (tenecteplase plus stenting) in patients with ST-elevated acute myocardial Infarction. Presented to European Society of Cardiology Congress2003.
LeMay MR, Wells GA, Labinaz M, et al. Combined Angioplasty and Pharmacological intervention versus thrombolytic alone in acute myocardial infarction (CAPITAL-AMI). J Am Coll Cardiol 2005;46:417–424.
Alter DA, Tu JV, Austin PC, Naylor CD. Waiting Times, Revascularization modality, and outcomes after acute myocardial infarction at hospitals with and without on-site revascularization facilities in Canada. J Am Coll Cardiol 2003:42:410–419.
Topol EJ. Reperfusion therapy for acute myocardial infarction with fibrinolytic therapy or combination reduced fibrinolytic therapy and platelet glycoprotein IIb/IIIa inhibition: the GUSTO V randomised trial. Lancet 2001 357:1905–1914.
Fernandez-Aviles F, Alonso JJ, Castro-Beiras A, et al. on behalf of the GRACIA (grupo de analisis de la Cardiopatia isquemica Aguda) Group.Routine invasive strategy within 24 hours of thrombolysis versus ischaemia-guided conservative approach for acute myocardial infarction with ST-segment elevation (GRACIA-1): a randomized controlled trial. Lancet 2004:364:1045–1053.
McClelland AJJ, Owens CG, Walsh SJ, et al. Percutaneous coronary intervention and 1 year survival in patients treated with fibrinolytic therapy for acute ST-elevation myocardial infarction. Eur Heart J 2005;26:544–548.
Van de Werf F. ASSENT-4 PCI: The Assessment of the Safety and Efficacy of a New Treatment Strategy for Acute Myocardial Infarction. Presented to ESC congress, Stockolm 3–7 september 2005.
The assessment of the safety and efficacy of a new thrombolytic (ASSENT-3) Investigators. Efficacy and safety of tenecteplase in combination with enoxaparin, abciximab, or unfractionated heparin:the ASSENT-3 randomised trial in acute myocardial infarction. Lancet 2001;358:605–613.
De Luca G, Suryapranata H, Stone GW, et al. Abciximab as adjunctive therapy to reperfusion in acute ST- segmernt elevation myocardial infarction.A meta-analysis of randomized trials. JAMA 2005:293:1759–1765.
Van de Werf F, Gore JG, Avezum A, et al. for the GRACE Investigators. Access to catheterisation facilities in patients admitted with acute coronary syndrome: multinational registry study. BMJ 2005;330:441 doi: 10.1136/ bmj. 38335.390718.82 (published 21 January 2005).
Gersh JB, Stone GW, White HD, Homes DR. Pharmacological Facilitation of primary percutaneous Coronary Intervention for acute myocardial infarction. Is the slope of the curve the shape of the future? JAMA 2005;293:979–986.
De Luca G, Sryapranata H, Ottervanger JP, Antman EM. Time delay to treatment and mortality in primary angioplasty for acute myocardial infarction. Circulation 2004;109:1223–1225.
Martines-Rios MA, Rosas M, Gonzales H, et al. For the Sastre Investigators. Comparison of reperfusion regimens with or without tirofiban in ST-Elevation Acute Myocardial infarction. Am J Cardiol 2004;93:280–287.
Dauermann HL, Sobel BE. Synergistic Treatment of ST-Segment Elevation Myocardial Infarction with pharmacoinvasive recanalization. J Am Coll Cardiol 2003;42:646–651.
Antman EM, Van de Werf F. Pharmacoinvasive therapy.The future of treatment for ST-Elevation Myocardial infarction. Circulation 2004;109:2480–2486.
Armstrong PW, Wagner G, Goodman SG, Van de Werf F, Granger C, Wallentin L, Fu Y; Assent 3, investigators. ST segment resolution in ASSENT 3; insights into the role of three different treatment strategies for acute myocardial infarction. Eur Heart J 2003;24(16):1515–1522.
Rebeiz AG, Johanson P, Green CL, et al. Comparison of ST-segment resolution with combined fibrinolityic and Glycoprotein IIb/IIIa inhibitor therapy versus fibrinolytic alone (data from four clinical trials) Am J Cardiol 2005;95:611–614.
Sarullo FM, Di Pasquale P, D’Alfonso G, Amerigo L, Cannizzaro S, Castello A. Safety and efficacy of thrombolysis with alteplase (50 mg) plus tirofiban versus alteplase (100 mg) alone in acute myocardial infarction: preliminary findings. Ital Heart J 2001;8:605–611.
Di Pasquale P, Sarullo FM, Cannizzaro S, et Al. Effects of administration of glycoprotein IIb/IIIa receptor antagonists in patients with failed thrombolysis. Clin Drug Invest 2001;21:545–553.
Martinez-Rios MA, Rosas M, Gonzalez H, et al. Comparison of reperfusion regimens with or without tirofiban in ST-elevation acute myocardial infarction. Am J Cardiol 2004;93:280–287.
Valgimigli M, Percoco G, Barbieri D, et al. The additive value of tirofiban administered with the high-dose bolus in the prevention of ischemic complications during high-risk coronary angioplasty: The advance trial. J Am Coll Cardiol 2004;44:14–19.
Johanson P, Wallentin L, Nilsson T, Bergstrand L, Lindahl B, Delborg M. ST-segment analyses and residual thrombi in the infarct-related artery: A report from the ASSENT PLUS ST-monitoring substudy. Am Heart J 2004;147:853–858.
Henriques JP, Haasdijk AP, Zijlstra F on behalf of the Zwolle Myocardial infarction study group. Outcome of primary angioplasty for acute myocardial infarction during routine duty hours versus during off-hours. J Am Coll Cardiol 2003;41:2138–2142.
Sabatine MS, Cannon CP, Gibson CM, et al. for the CLARITY–TIMI 28 Investigators. Addition of Clopidogrel to Aspirin and Fibrinolytic Therapy for Myocardial Infarction with ST-Segment Elevation. N Engl J Med 2005;352:1179–118.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pasquale, P.D., Cannizzaro, S., Parrinello, G. et al. Is delayed facilitated percutaneous coronary intervention better than immediate in reperfused myocardial infarction? Six months follow up findings. J Thromb Thrombolysis 21, 147–157 (2006). https://doi.org/10.1007/s11239-006-5733-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-006-5733-z