Abstract
Purpose
The inclusion of patient-reported outcome (PRO) instruments to record patient health-related quality of life (HRQOL) data has virtually become the norm in oncology randomised controlled trials (RCTs). Despite this fact, recent concerns have focused on the quality of reporting of HRQOL. The primary aim of this study was to evaluate the quality of reporting of HRQOL data from two common instruments in oncology RCTs.
Design
A meta-review was undertaken of systematic reviews reporting HRQOL data collected using PRO instruments in oncology randomised controlled trials (RCTs). English language articles published between 2000 and 2012 were included and evaluated against a methodology checklist.
Results
Four hundred and thirty-five potential articles were identified. Six systematic reviews were included in the analysis. A total of 70,403 patients had completed PROs. The European Organization for Research and Treatment of Cancer QLQ-C30 and Functional Assessment of Cancer Therapy-General questionnaire accounted for 55 % of RCTs. Eighty per cent of RCTs had used psychometrically validated instruments; 70 % reported culturally valid instruments and almost all reported the assessment timing (96 %). Thirty per cent of RCTS reported clinical significance and missing data. In terms of methodological design, only 25 % of RCTs could be categorised as probably robust.
Conclusion
The majority of oncology RCTs has shortcomings in terms of reporting HRQOL data when assessed against regulatory and methodology guidelines. These limitations will need to be addressed if HRQOL data are to be used to successfully support clinical decision-making, treatment options and labelling claims in oncology.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The assessment of health-related quality of life (HRQOL) in oncology randomised controlled trials (RCTs) through patient-reported outcome (PRO) instruments has seen a steady increase over the last two decades helped, in part, through the development of a number of PRO cancer-specific instruments in the 1980s and 1990s [1–4]. However, despite their use in oncology RCTs, concerns have been raised regarding the consistency and quality of reporting of HRQOL data. Recent reviews have suggested a degree of variability in the reporting quality of HRQOL data in oncology RCTs: on the one hand, criteria such as the rationale for the instrument selection, presentation of results and discussion of the findings tend to be well reported, whereas the clinical significance of results and a description of missing data are frequently not addressed [5, 6]. However, there does appear to be a trend towards a greater degree of reporting of HRQOL in oncology RCTs over time [7].
The quality of HRQOL data reported is of importance if outcomes are increasingly being employed to inform clinical decision-making processes, as well as in comparative effectiveness studies, and health policy and reimbursement decisions [8].
There remain issues regarding the methodology of RCTs in oncology in terms of the quality and completeness of the reporting of HRQOL data. Two of the commonly used PROs in oncology RCTs are the European Organization for Research and Treatment of Cancer Quality of Life Questionnaire-Core 30 questionnaire (EORTC QLQ-C30) and the Functional Assessment of Cancer Therapy-General (FACT-G) [1, 2]. What is not known is whether despite the frequent use of these instruments in clinical trials there are still issues in terms of the reporting of HRQOL data from these trials. This in turn would have significant implications in terms of clinical practice and study outcomes.
The primary aim of this study was therefore to undertake a meta-review of published systematic reviews to synthesise published data and detail any methodological shortcomings associated with the reporting of HRQOL in RCTs in oncology utilising the EORTC QLQ-C30 and/or the FACT-G. The secondary aims were to determine whether there were any similarities/differences in trial reporting between the two instruments (EORTC QLQ-C30 and FACT-G), and to evaluate the quality of HRQOL reporting against a robustness checklist [9].
Methods
A comprehensive meta-review was undertaken of systematic reviews of oncology PRO instruments used in oncology RCTs. This approach was adopted in order to maximise the synthesis of results from previously published studies and collate evidence from RCTs for different cancer types.
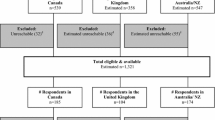
Inclusion criteria for the review were defined as systematic reviews of RCTs involving adult (≥18 years) patients with a cancer diagnosis, irrespective of stage/grade or tumour type and including any anti-cancer treatment (surgery, chemotherapy, radiotherapy, biological therapy or any combination of these) and PROs. Exclusion criteria included non-English language systematic reviews, the absence of patients-reported outcomes (including HRQOL reported by proxies or physicians). The Cochrane Library, PubMed, Ovid, PsychINFO and EMBASE databases were searched using the following broad search terms: (“neoplasm$” OR “cancer”) AND [(“quality of life” OR “HRQOL” OR “PRO$”) AND (“PRO measure$”) OR (“instrument$”)] AND (“clinical trial$ OR randomised controlled trial$) AND [(“review$”) OR (“literature review$”) OR (“systematic review$”). The publication type was restricted to full manuscripts (excluding textbooks, abstracts and unpublished manuscripts). The search was limited to systematic reviews of oncology RCTs involving HRQOL data published after 2000. An overview of the search process is shown in Fig. 1. In summary, article titles and abstracts were screened against the search criteria. Full articles were subsequently screened for inclusion (as well as full duplicate references) in the study. The reference sections of each review publication were inspected to identify any potential overlap in studies included.
The final systematic reviews were analysed recording cancer type, patient numbers, as well as the quality of HRQOL data reporting (from the EORTC QLQ-C30 and/or FACT-G)Footnote 1 which was evaluated using a standardised checklist [9]. This checklist consists of the fundamental and critical issues that a well-designed trial should include in order to produce reliable PROs. The checklist comprises four key areas: conceptual, measurement, methodology, and interpretation representing 11 criteria (see Table 2).
The total number of criteria reported were recorded and used to calculate a “robustness” score [9] The number of criteria reported for each reported study were summed to provide an overall score categorised as probably robust for scores of between 8 and 11 on the checklist, limited robustness for scores between 5 and 7, and very limited for scores between 0 and 4. Only those studies were included which reported at least 8/11 criteria. This method has been used previously to categorise the standard of reporting of HRQOL data in clinical trials [9, 10].
Results
Quality of reporting
A final 8 systematic reviews [10–17] were identified where HRQOL data had been recorded in RCTs (Fig. 1). Three reviews did not record all of the 11 criteria [10, 15, 16]. The reviews covered a variety of cancers including non-small cell lung and colorectal cancer, leukaemia, prostate and multiple myeloma, as well as surgical oncology [10]. This represented a total of 101 trials. The FACT-G had been utilised in 21/101 (20.8 %), the EORTC QLQ-C30 in 78/101 (77.2 %) and 2 trials had employed both instruments (~2 %). A total of 34,616 patients had completed the instruments (32 % FACT-G, 64 % EORTC QLQ-C30).Footnote 2 A summary of trials is shown in Table 1.
The proportions of the 11 criteria reported are shown in Table 2 for the two instruments. Given that not all the systematic reviews recorded all criteria, the proportions were adjusted for the difference in total number of trials (i.e. the denominator was adjusted); however, this had little impact on the results and these data are therefore not shown. It may be seen from this table that there was a great deal of variation in reporting the criteria: psychometric properties, adequacy of domain, timing of assessments and presentation of results were reported in more than two-thirds of trials. In contrast to this, clinical significance, rationale for instrument selection and a priori hypothesis were reported in fewer than 40 % of trials.
Efficace et al. [9] have defined the following criteria as critical in terms of reporting HRQOL data: psychometric properties, baseline compliance and missing data documentation. At least 50 % of trials across all 8 reviews included these three criteria for both instruments, and for the EORTC QLQ-C30, at least two of these criteria were reported in over 70 % of trials.
Instrument comparison
There was a considerable degree of agreement between the two instruments with 9/11 criteria falling within a 10 % difference between the two instruments. However, two criteria demonstrated large differences (>20 %), i.e., cultural verification of instruments (difference of 26 %) and baseline compliance (19 % difference). In both instances, these criteria were reported more frequently for the EORTC QLQ-C30. Although it should be noted that the 95 % confidence intervals were particularly wide for these two properties and this result should therefore be interpreted with caution.
Robustness
Robustness could be assessed in the five systematic reviews which had included all 11 criteria [11–14, 17] amounting to 75 trials [EORTC QLQ-C30, 59/75 (78.7 %); FACT-G, 16/75 (21.3 %)]. Table 3 provides a summary of the robustness scores. More trials incorporating FACT-G could be categorised as probably robust, compared to EORTC QLQ-C30 trials. On the other hand, more FACT-G trials could also be categorised as having very limited methodological quality in terms of reporting HRQOL data.
Discussion
This study reviewed and compared the reporting quality of HRQOL data captured through two common PRO instruments, the EORTC QLQ-C30 and FACT-G.
The results demonstrated that the majority of reporting criteria for a robust design are not being met for trials employing these instruments with 7/11 criteria not reported in more than 50 % of trials. Comparisons between the two instruments revealed a significant degree of agreement and that broadly speaking the criteria are being reported similarly; however, there were important differences for two domains (baseline compliance and cultural validity) on which reporting of the EORTC QLQ-C30 data was more complete. In terms of the “critical” criteria [9], the EORTC QLQ-C30 trials are reporting 2/3 criteria in more than 70 % of cases, whereas for the FACT-G, this was 1/3. The analysis of the overall robustness revealed that slightly more trials utilising the FACT-G could be classified as robust; however, fewer EORTC QLQ-C30 trials were of very limited robustness compared to the FACT-G.
These results are in line with previous studies [5, 6] and demonstrate that important criteria, such as a priori hypotheses for HRQOL and the clinical significance of results, are not being recorded in RCTs. These shortcomings in reporting of HRQOL will have to be addressed if this data are to help in supporting or informing decision-making processes. Given the widespread use of both the EORTC QLQ-C30 and the FACT-G, these results have important significance in terms of the interpretation of data for patient care in clinical practice and the interpretation of results from clinical trials.
There are a number of potential limitations with this meta-review. In terms of the robustness of trials, we were not able to assess this for all the systematic reviews which may have introduced a degree of bias into the results. Furthermore, the reviews were published by different groups and cover different time periods. There may be differences in the criteria utilised in these publications in selecting RCTs. This is to some extent inevitable where decisions (such as in/exclusion of papers) rely on judgment. However, the reviews were selected on the basis of the use of the Efficace checklist [9] and this should therefore have introduced a level of standardisation.
It is hoped that recent initiatives such as the CONSORT statement [8] and the CONSORT PRO extension [18] providing recommendations for the reporting of PROs and HRQOL in clinical trials, as well as the International Society for Quality of Life’s [19] adoption of minimum standards for PROs in comparative effectiveness research, will lead to greater levels of standardisation and improvements in the quality of trial methodology and consequently by association the potential value of the information provided by HRQOL data.
Abbreviations
- CONSORT:
-
Consolidated standards of reporting trials
- EORTC QLQ-C30:
-
European Organization for Research and Treatment of Cancer Quality of Life Questionnaire, Core 30
- FACT-G:
-
Functional Assessment of Cancer Therapy-General
- HRQOL:
-
Health-related quality of life
- PRO:
-
Patient-reported Outcome
- RCT:
-
Randomised controlled trial
References
Aaronson, N. K., Ahmedzai, S., Bergman, B., Bullinger, M., Cull, A., Duez, N. J., et al. (1993). The European Organization for Research and Treatment of Cancer QLQ-C30: A quality-of-life instrument for use in international clinical trials in oncology. Journal of the National Cancer Institute, 85, 365–376.
Cella, D. F., Tulsky, D. S., Gray, G., Sarafian, B., Linn, E., Bonomi, A., et al. (1993). The Functional Assessment of Cancer Therapy scale: Development and validation of the general measure. Journal of Clinical Oncology, 11, 570–579.
de Haes, J. C., van Knippenberg, F. C., & Neijt, J. P. (1990). Measuring psychological and physical distress in cancer patients: Structure and application of the Rotterdam symptom checklist. British Journal of Cancer, 62, 1034–1038.
Spitzer, W., Dobson, A., & Hall, J. (1981). Measuring the quality of life of cancer patients: A concise QL-index for use by physicians. Journal of Chronic Diseases, 34, 585–597.
Brundage, M., Bass, B., Davidson, J., Queenan, J., Bezjak, A., Ringash, J., et al. (2011). Patterns of reporting health-related quality of life outcomes in randomized clinical trials: Implications for clinicians and quality of life researchers. Quality of Life Research, 20, 653–664.
Cocks, K., King, M. T., Velikova, G., Fayers, P. M., & Brown, J. M. (2008). Quality, interpretation and presentation of European Organisation for Research and Treatment of Cancer quality of life questionnaire core 30 data in randomised controlled trials. European Journal of Cancer, 44, 1793–1798.
Efficace, F., Osoba, D., Gotay, C., Sprangers, M., Coens, C., & Bottomley, A. (2007). Has the quality of health-related quality of life reporting in cancer clinical trials improved over time? Towards bridging the gap with clinical decision making. Annals of Oncology, 18, 775–781.
Calvert, M., Blazeby, J., Revicki, D., Moher, D., & Brundage, M. (2011). Reporting quality of life in clinical trials: A CONSORT extension. The Lancet, 2011(378), 1684–1685.
Efficace, F., Bottomley, A., Osoba, D., Gotay, C., Flechtner, H., D’haese, S., et al. (2003). Beyond the development of health-related quality of life (HRQOL) measures: A checklist for the evaluation of HRQOL evaluation in cancer clinical trials. Journal of Clinical Oncology, 21, 3502–3511.
Blazeby, J. M., Avery, K., Sprangers, M., Pikhart, H., Fayers, P., & Donovan, J. (2006). Health-related quality of life measurement in randomized clinical trials in surgical oncology. Journal of Clinical Oncology, 24, 3178–3186.
Claassens, L., van Meerbeeck, J., Coens, C., Quiten, C., Ghislain, I., Sloan, E. K., et al. (2011). Health-related quality of life in non-small-cell lung cancer: An update of a systematic review on methodologic issues in randomized controlled trials. Journal of Clinical Oncology, 29, 2104–2120.
Efficace, F., Bottomley, A., & van Andel, G. (2004). Health related quality of life in prostate carcinoma patients: A systematic review of randomized controlled trials. Cancer, 97, 377–388.
Efficace, F., Bottomley, A., Vanvoorden, V., & Blazeby, J. M. (2004). Methodological issues in assessing health-related quality of life of colorectal cancer patients in randomised controlled trials. European Journal of Cancer, 40, 187–197.
Efficace, F., Kemmler, G., Vignetti, F., Madelli, F., Molica, S., & Holzner, B. (2008). Health-related quality of life assessment and reported outcomes in leukaemia randomised controlled trials: A systematic review to evaluate the added value in supporting clinical decision making. European Journal of Cancer, 44, 1497–1506.
Fitzsimmons, D., Gilbert, J., Howse, F., Young, T., Arrarras, J. I., Brédart, A., et al. (2009). A systematic review of the use and validation of health-related quality of life instruments in older cancer patients. European Journal of Cancer, 45, 19–32.
Gujral, S., Avery, K. N., & Blazeby, J. M. (2008). Quality of life after surgery for colorectal cancer: Clinical implications of results from randomised trials. Supportive Care in Cancer, 16, 127–132.
Kvam, A. K., Fayers, P., Hjermstad, M., Gulbrandsen, N., & Wisloff, F. (2009). Health-related quality of life assessment in randomised controlled trials in multiple myeloma: A critical review of methodology and impact on treatment recommendations. European Journal of Haematology, 83, 279–289.
Calvert, M., Blazeby, J., Altman, D. G., Revicki, D. A., Moher, D., Brundage, M. D., et al. (2013). Reporting of patient-reported outcomes in randomized trials: The CONSORT PRO extension. Journal of the American Medical Association, 309(8), 814–822.
Reeve, R. B., Wyrwich, K. W., Wu, A. W., et al. (2013). ISOQOL recommends minimum standards for patient-reported outcome measures used in patient-centered outcomes and comparative effectiveness research. Quality of Life Research. doi:10.1007/s11136-012-0344-y.
Acknowledgments
The authors are grateful to Katarina Halling, Anders Ingelgård, Anna Niklasson, Sindre Rolstad (AstraZeneca AB, Mölndal, Sweden), Chris Miller (AstraZeneca, Wilmington, USA) and Clare McGrath (AstraZeneca Pharmaceuticals Ltd., Macclesfield, UK) for their thoughtful comments and suggestions on an earlier draft of this paper. Adam B. Smith was supported through a Knowledge Transfer Partnership Grant (KTP007957) funded jointly by the UK Technology Strategy Board and AstraZeneca Ltd.
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclaimer: The views expressed herein are those of the authors and do not reflect the official policy or position of AstraZeneca Pharmaceuticals Ltd (UK) or York Health Economics Consortium.
Rights and permissions
About this article
Cite this article
Smith, A.B., Cocks, K., Parry, D. et al. Reporting of health-related quality of life (HRQOL) data in oncology trials: a comparison of the European Organization for Research and Treatment of Cancer Quality of Life (EORTC QLQ-C30) and the Functional Assessment of Cancer Therapy-General (FACT-G). Qual Life Res 23, 971–976 (2014). https://doi.org/10.1007/s11136-013-0534-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-013-0534-2