Abstract
Individuals with schizophrenia die, on average, 20 years before their peers, with ‘natural causes’ accounting for 80% of premature deaths. The aim of this narrative review is to address this phenomenon from the perspective of known factors that contribute to long life. The relevant literature from the last decade was searched in PubMed and Google Scholar databases. Four factors have been shown to be common to centarians, people who live to be a hundred: genes, life style behaviors that favor a healthy heart, social support, and a subjective purpose in life. The latter three factors are potentially modifiable but, in the context of schizophrenia, there are barriers to change, namely poverty, illness symptoms, stress, stigma, and side effects of antipsychotic medication. Barriers to change need to be addressed before substantial progress can be made in increasing the health and mortality risk of people with schizophrenia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Individuals with a diagnosis of schizophrenia die, on average, 20 years before their peers and the implications behind this statistic have rightly been called a public health scandal [1]. The high mortality rate in this population has been attributed to suicide, accidental death and injury, all understandable in the context of schizophrenic illness [2]. What is less understandable is the 80% of premature schizophrenia deaths that result from ‘natural’ causes, mainly heart disease. There have been various speculations as to their origin. Is it because antipsychotic medications predispose to weight gain, metabolic problems and cardiovascular sequelae [3, 4]? Is it because individuals with schizophrenia engage in unhealthy lifestyles – poor diet, lack of physical activity, cigarette smoking, substance abuse, lack of self-care, non-participation in illness prevention programs such as flu shots and cancer screening [5]? Is schizophrenia a disease of accelerated aging [6]? Do genes that heighten the risk for schizophrenia commonly travel with risk genes for immune, metabolic and cardiovascular problems [7, 8]? Does mental health stigma interfere with access to timely and high quality health care so that normally treatable illness is left too long unchecked [9]?
The issue of premature mortality in specific groups of individuals can be addressed by asking the question, “what allows some people to live longer than others?” This interesting question has been investigated through the study of centarians (people who live beyond age 100) and the close analysis of factors that such long-lived people share [10, 11].
The frequent observation that an important predictor of long life is being born to long-lived parents implicates inherited genes in longevity. Diet (low caloric intake), a life style that promotes heart heath, a solid support network of friends and family, and a subjective sense that life has a purpose are the factors other than longevity genes that studies of centarians have found to contribute to exceptionally long lives [12].
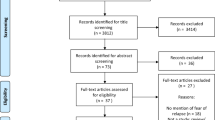
This paper will review the influence of four longevity factors (genes, diet, support network, and sense of purpose) in the lives of people with schizophrenia. The databases, PubMed and Google Scholar, were searched for studies, mainly those conducted over the last decade, which shed the most light on these influences (Fig. 1).
Findings
Longevity Genes
Between 15 and 40% (the percentages vary from study to study) of life expectancy is believed to be predetermined by the presence of specific gene variants [13, 14]. The research on long-lived populations has yielded approximately 77 candidate pro-longevity genes, chief among which are apolipoprotein E (APOE), forkhead box 03 (FOXOS), interleukin 6 (IL6), insulin-like growth factor-1 (IGF), chromosome 9P21, and 5q.33.3 [15, 16]. It is important to note that the full effect of one’s genetic inheritance may not be felt until late in life when DNA “packaging” -e.g. epigenetic DNA methylation and histone modification tends to drop off. As cells age, chromatin marks drift towards a middle ground between repressed and active, such that genes that were previously inactive begin to “leak” [16]. The corollary is that, since most people with schizophrenia die relatively young, the major determinants of longevity in this population are likely not to reside primarily in genes but more in environmental conditions alone or in products of gene-environment interactions [17].
Gene/Environment Interactions
Hormones, diet and exposure to physical and psychological stressors are important environmental influences that interact with genes, most particularly during sensitive periods of development such as fetal life and early childhood. The results of such interactions affect health throughout the lifespan. Harmful exposures during these early periods are able to directly trigger ill health or they can do so indirectly by setting off chains of adverse events. For instance, subpar parental care may lead to poor quality or short duration of schooling, subsequently to unrewarding employment and low income, to poor housing, to insufficient levels of social support, and from that to unwise health behaviors that culminate in serious illness [18]. Chains of adverse effects may not be the only routes to ill health. What matters more may be the rate and accumulation of chance noxious exposures (accidents, toxins, infections, global economic conditions, wars, natural disasters), which each work through DNA methylation and histone modification and non-coding RNA to suppress protective genes or to enhance the expression of disease genes [19].
Exposure - Prenatal Environment
While harmful exposures can occur at any time, there is evidence that what happens early in life is especially critical to future health. Fetal programming is the name given to the link between the fetal environment and later life effects on the immune, endocrine, metabolic, cardiovascular, and central nervous systems [20, 21]. When an expectant mother experiences stress, the fetus is exposed to excess glucocorticoids via placental transfer. The fetoplacental barrier to maternal glucocorticoids is not robust; high cortisol levels enter the fetal bloodstream and often lead to low infant birth weight, which, in turn, increases the risk for a variety of adult illness such as coronary heart disease, stroke, type 2 diabetes mellitus, adiposity, the metabolic syndrome, and osteoporosis [22].
There are other mechanisms by which maternal stress during pregnancy can affect the adult health of offspring. For instance, maternal undernutrition during pregnancy promotes epigenetic changes in the expression of genes involved in endothelial function, thus facilitating vascular disease [23]. Another example is maternal hyperglycemia, which leads to fetal hyperinsulinemia and fat deposition, consequently increasing the risk for metabolic disorders in offspring in adulthood [24].
One reason why fetal exposures such as maternal nutrition, stress, toxic chemicals, drugs, or diseases are of particular importance is that epigenetic processes (the influence of the local environment on gene expression) in the placenta differ from these same processes in other tissues [25], which may make their effects more durable.
Exposure - Early Childhood
Early childhood is another sensitive period for epigenetic effects. Potential noxious exposures at this time are infections, accidents, toxins, parental neglect, physical, sexual, or psychological abuse, and inadequate nutrition. Young children can also be exposed to continuing adverse circumstances such as occur with chronic illness in the family or chronic economic disadvantage or war. A recent report suggests that early childhood trauma such as this is associated with dysregulation of the immune system in adulthood [26].
Exposure -Adolescence
Significant stressors often appear during adolescence – the advent of puberty and pressures related to family, school, accidents, illnesses, peer relationships, and exposure to toxic substances. It is during adolescence that young people begin to see themselves as occupying a more or less fixed rung in the social hierarchy. Such social positioning is crucial to self-esteem and becomes a major determinant of adult goals and aspirations. It is also during adolescence that sexual preferences are solidified and sexual intimacy becomes an important motivator of behavior.
Schizophrenia generally begins at this time. This may be because the threshold for the large number of genes that need to be “turned on” in order for the symptoms and signs of illness to emerge has now been reached.
Low Caloric Intake
The association of lean body mass with exceptional longevity is corroborated by many animal studies [27]. A study in monkeys has shown that reduction of food intake delays the risk of diabetes, cancer, cardiovascular disease, and brain atrophy [28]. Studies of long lived humans confirm that eating in moderation and eating mostly plant-based diets, goat’s milk, red wine, and herbal teas in the context of adequate hydration, physical exercise, abstinence from alcohol and tobacco and maintenance of a low body mass index have been associated with longevity in humans. While reducing caloric intake extends life span, individuals with schizophrenia tend to eat a high calorie diet, high in saturated fat and low on fibre and fruit; their diet increases the risk of metabolic disease [29]. Although the high calorie diet found in schizophrenia has many explanations (substance use, medication-induced cravings, insufficient training in food preparation, general apathy, living in proximity to fast food outlets), the overall reason is probably socioeconomic disadvantage. Healthy diets cost more than unhealthy diets [30]. Foods of lower nutritional value generally cost less per calorie than nutritious food and fruit and vegetable stores are often not available in areas where the economically disadvantaged live. Low socioeconomic status, especially when coupled with low educational achievement, is known to be associated with a diet low in nutrients and high in calories [31, 32].
Social Networks
Social networks provide a) emotional support (comfort, belonging, understanding, reassurance), as well as b) informational support that assist decision-making with respect to symptoms, medication and health behaviors. They also provide c) physical support (physical comfort, nutrition, transportation) and d) practical support (financial, housekeeping), in addition to e) psychological support that augment a sense of personal control and self-esteem, and f) social support (relationships, community acceptance) and, finally, g) spiritual support - encouraging interrogation and discussion of the meaning and purpose of life [33].
Because people with schizophrenia frequently experience difficulties in developing and maintaining social relationships, they tend to have small social networks that are mainly composed of family members and care providers [34]. In a meta-synthesis of studies of the lived experience of individuals with schizophrenia [35], patients reported that their illness affected existing relationships negatively, that the relatively few relationships that were retained tended to be superficial. This is not only because of a lack of social skills. Solitude is sometimes actively sought. It reduces unwelcome arousal and serves as a protective mechanism that is often purposefully resorted to by individuals with psychotic illness [36]. Communication and cognitive difficulties, lack of social motivation and the stigma that attaches to both mental illness and to social disadvantage further contribute to the social distancing and subsequent social isolation of individuals with schizophrenia [37].
From the viewpoint of living a long life, social withdrawal is a distinct disadvantage. Active engagement with social networks and support systems confer longevity benefits because close family and friends are necessary to mobilize resources as needed, to provide spurs to healthy behavior, to help access medical care in a timely fashion, and to supervise and reward the effective self-management of symptoms [38]. Being part of a social network encourages conformity to social norms with respect to health and self-care. In addition, being part of a social network endows its members with meaningful social roles that raise self-esteem and lend purpose to life [39]. A sense of purpose, as we shall see in the next section, is itself associated with longevity. Social connections also buffer the deleterious effects of stress. This may be mediated by a reduction in sedentary time and an increase in physical activity, as has been shown in elderly populations [40].
A review of 148 studies (308,849 participants) found a 50% increased likelihood of survival over controls for participants with strong social relationships. The influence of social relationships on risk for mortality was comparable to that of cigarette smoking and exerted a greater effect than obesity or alcohol abuse [41]. Moreover, a recent meta-analysis found that social disconnection was linked with a 29% increased risk for development of coronary heart disease and a 32% increased risk for stroke [42].
Altogether, an increased mortality risk of 29%–32% has been reported for socially disconnected adults in the general population [43, 44]. A 13-year follow up found that individuals with psychosis who lived alone were more often dead at the end of the study than those who smoked cigarettes or those who suffered from metabolic syndrome [45].
Purpose in Life
As mentioned earlier, a subjective sense of meaning and purpose in life is associated in the general population with both lessened morbidity and with longer life [46, 47]. This is a frequently reported association but could be explained by the fact that healthy people are more likely to seek and find a purpose in life than are those who are frail and disabled. Nevertheless, sensing a purpose to one’s life has also been found to increase one’s ability to counter stress and to lower allostatic load (neuroendocrine, cardiovascular, immune and metabolic burden) [48, 49].
In a study from China, more centarians reported viewing themselves as useful than did younger cohorts among the elderly [50]. Despite the fact that there are many ways to find meaning in life –being useful to others, immersing oneself in spirituality, in philosophy, in science or in art, for most people, meaning is found when belonging to a community of family and friends [51].
A sense of belonging is intimately tied to the feeling that life matters [52]. Social exclusion impairs a person’s sense not only that life is worthwhile but also that one is in full control of one’s life. Being in control rather than life being determined by chance or by others is thought to prevent illness by reducing cortisol levels (a marker of stress) [53]. What is also likely is that individuals who are convinced that their life is significant pay careful attention to their health behaviors. They are more likely than others to abstain from cigarettes and alcohol, eat a healthier diet, engage in physical activity and participate in preventive programs – flu shots, daily aspirins and statins, cholesterol tests, colonoscopies, mammograms, pap smears, and prostate screening [54].
Having aspirations and pursuits and continually striving to attain goals provides life with meaning and purpose and enhances vitality. Unfortunately, those with severe mental illness are barred by symptoms, economic disadvantage, and perceived stigma from occupational activities that provide purposeful goals [55]. Many, instead, find purpose in active engagement in leisure activities [56]. For those with chronic illness, or for those living under economic constraints or for everyone as they grow older, leisure time activities become significant [57,57,58,60]. Even everyday activities can become imbued with meaning [61, 62], especially if they afford an opportunity to overcome challenges, learn new skills or help others [63,63,65].
Although taking care of other people can be both burdensome and stressful, it can also lend importance to life [66]. Many studies have confirmed that family caregivers have lower mortality rates than non-caregivers, although this may not hold across all samples of caregivers [67].
Individuals with schizophrenia do not often have the opportunity to care for others nor can they usually take part in leisure activities that are costly, such as those that involve travel or membership fees or supplies they cannot afford. Many, however, do find purpose in the arts and in religion [68, 69].
Discussion
The genes we are born with and the early exposures that negatively interact with our genes are random events over which we have little control. There is some measure of control, however, over other predictors of longevity -e.g. diet, social engagement and finding meaning in life, but economic constraints govern all three. The economic disadvantage that is tied to serious mental illness, as a consequence, plays a critical role in shortening the life of individuals with schizophrenia.
Persons with severe mental illness usually live in poverty [70]. Poverty determines where people live, what they eat, who their friends are, how they spend their time and what they do to keep healthy [71]. Poverty determines people’s attitudes towards health, the extent of their exposures to health threats, their risk behaviors, and their interactions with health providers. Poverty also governs their relative ease of access to medical care. The difficulties inherent in living in deprived economic circumstances, compounded by the stress, isolation and the stigma of poverty, are well-known barriers to timely and effective illness prevention and healthcare [72]. It is seldom possible when researching mortality risks to disentangle the role of poverty from that of illness, its treatment, and its various sequelae.
To study the effects of socioeconomics on mortality rates, Davey Smith et al. conducted an ingenious study in Glasgow, Scotland in 1992 [73]. They took advantage of the observation that Glasgow graves between 1801 and 1920 were marked with commemorative obelisks of uniform design but of different heights. The taller the obelisk, the greater it cost so that the height of the obelisk made a good proxy for the financial means of the grave occupant. Since birth and death date were indicated on the gravestone, Davey Smith and his colleagues were able to show that the higher the obelisk, the longer the person had lived. In 2000, Gould and Chappel [74] conducted a similar study in England by measuring the depth of burial of the dead body (the deeper the grave, in this case, the more it had cost). The age of death rose with increasing depth, again demonstrating a socioeconomic gradient in a particularly memorable way.
The stress that is linked to serious mental illness also plays a major role in schizophrenia mortality. Stress can come from both physiological sources -e.g. pain or hunger, and from psychological sources -e.g. social evaluation, social exclusion, or social competition [75]. Experiencing stress leads to a state of arousal that is accompanied by heightened cortisol, epinephrine and norepinephrine secretion, all of which results in a rapid heart rate, endothelial dysfunction and tissue inflammation that raise blood pressure. This varies with the intensity and the nature of the stressor as well as with the person. In general, however, cumulative stress is an important risk factor in early mortality [76, 77].
Cumulative physical stress in schizophrenia, assessed by 13 biological markers in cardiovascular, metabolic, neurendocrine, and immune systems, has been found to be significantly higher than in age peers [78]. These markers are already pathological in early disease [79] and in medication-free patients. They improve with antipsychotic treatment [80].
The very symptoms of schizophrenia –e.g. apathy, social withdrawal, cognitive problems, hostility, fear and suspicion, contribute to poor health and early mortality. Cognitive deficits make it difficult to accurately interpret the significance of medical symptoms and to appreciate behavioral risks. Motivational problems interfere with participation in preventive screening; fear and suspiciousness undermine trust in medical care [81]. Symptoms may contribute to a high rate of accidents and injuries. Also prevalent are suicidal thoughts. Suicide is 7 times as common in schizophrenia as in the general population [2].
Mental illness stigma has public health implications [82]. Not only is it a source of stress but it also interferes with timely access to services and to cutting edge treatment and quality care. It also leads to self-stigma, and loss of confidence, which consequently makes it hard for people with schizophrenia to speak up for what they need from health providers. Their tendency is to avoid people in authority. Unconscious mental illness stigma influences the medical profession as well. When faced with a patient diagnosed with schizophrenia, doctors sometimes do not take physical symptoms seriously, attributing them to the delusions of mental illness [83, 84]. In general, medical staff tend to systematically treat the physical illnesses of people with mental illness less thoroughly and less effectively than they do those they consider mentally well [1].
The day-to-day life of people with schizophrenia is often marked by sedentariness, loneliness, substance use, including cigarettes, alcohol, marijuana, and an unhealthy diet. Their life style has been held responsible for poor health and early death [2]. They are frequently the targets of violence. Death by suicide, homicide and accident together account for approximately one in every eight schizophrenia deaths [85], accidental death being twice as prevalent as suicide [2].
A critical issue is the extent to which treatment with antipsychotic drugs contributes to ill health. Antipsychotics result in weight gain and lipid and glucose dysregulation [86]. Antipsychotics may add to memory impairment, with subsequent risk-taking and accidents, lack of hygiene and inadequate self-care, perhaps explaining the high rates of infectious disease. Antipsychotics are also implicated time wise because the mortality gap between schizophrenia and the rest of the population is widening since the introduction of 2nd generation weight-inducing antipsychotic drugs [87, 88]. On the other hand, antipsychotics lower the suicide rate, reduce psychotic symptoms, and can be expected to increase social support and decrease distrust of medical intervention, perhaps explaining why markers of disease are decreased in individuals with schizophrenia after treatment [80]. Recent papers appear to exonerate antipsychotics as the cause of the high death rate in schizophrenia. The meta-analysis by Carpiniello et al. [5] strongly suggests that individuals with schizophrenia who are taking antipsychotics have a lower overall mortality rate than those not taking antipsychotics. The important question is whether the long-term use of antipsychotic medication, especially at high doses, hastens cardiovascular deaths by cumulative exposure to cardiometabolic side effects [89]. Doses and durations of exposure need to be examined. While there has been a 40% drop in death rate due to suicide in schizophrenia, from 16.2% of deaths in 1984 to 4.0% of deaths in 2014 [90], cardiovascular deaths continue to rise [91, 92].
Conclusion
Currently, individuals with schizophrenia die, on average, 20 years before their peers, with 80% of deaths resulting from ‘natural’ causes, mainly cardiovascular. The aim of this paper was to review this premature mortality from the perspective of factors known to be shared by centarians, to see whether these factors were deficient in schizophrenia. Findings were that individuals with schizophrenia generally lacked three crucial longevity factors: life behaviors that promoted heart health, sufficient social support, and a belief in a purpose to their life. These factors are potentially modifiable but there are strong barriers to change, namely poverty, symptoms specific to schizophrenia, stress, stigma, and adverse effects of antipsychotic medication. These must be addressed before effective change can take place in the duration of life in this population.
References
Thornicroft G. Physical health disparities and mental illness: the scandal of premature mortality. Br J Psychiatry. 2011;199:441–2.
Olfson M, Gerhard T, Huang C, Crystal S, Stroup TS. Premature mortality among adults with schizophrenia. JAMA Psychiat. 2015;72:1172–81.
Bak M, Fransen A, Janssen J, van Os J, Drukker M. Almost all antipsychotics result in weight gain: a meta-analysis. PLoS One. 2014;9:e94112.
Bressington D, Mui J, Tse ML, Gray R, Cheung EFC, Chien WT. Cardiometabolic health, prescribed antipsychotics and health-related quality of life in people with schizophrenia-spectrum disorders: a cross-sectional study. BMC Psychiatry. 2016;16:411.
Carpiniello B, Manchia M, Orrù MG, Pinna F. Mortality in mental disorders: are we approaching to close the gap respect to other medical specialties? The case of schizophrenia. J Psychopathol. 2019;25:39–44.
Eyler LT, Jeste DV. Aging of the body and the brain in schizophrenia. Schizophr Res. 2018;196:1–6.
Cullen AE, Holmes S, Pollak TA, Blackman G, Joyce DW, Kempton MJ, et al. Associations between non-neurological autoimmune disorders and psychosis: a meta-analysis. Biol Psychiatry. 2019;85:35–48.
Huang MH, Chen MH, Huang KL, Hsu J, Bai Y, Cheng C, et al. Increased risk of type 2 diabetes among the siblings of patients with schizophrenia. CNS Spectr. 2019:1–7. https://doi.org/10.1017/S1092852918001396.
Karim RS, Kwan MMS, Finlay AJF, Kondalsamy-Chennakesavan S, Toombs MR, Nicholson GC, et al. Mortality in hospital patients with and without mental disorders: a data-linkage cohort study. J Psychiatr Res. 2019;111:104–9.
Giuliani C, Pirazzini C, Delledonne M, Xumerl L, Descombes P, Marquis J, et al. Centenarians as extreme phenotypes: an ecological perspective to get insight into the relationship between the genetics of longevity and age-associated diseases. Mech Ageing Dev. 2017;165:195–201.
Heinz M, Cone N, Da Rosa G, Bishop AJ, Finchum T. Examining supportive evidence for psychosocial theories of aging within the oral history narratives of centenarians. Societies. 2017;7:8.
Pignolo RJ. Exceptional human longevity. Mayo Clin Proc. 2019;94:110–24.
Giefing-Kröll C, Grubeck-Loebenstein B. Improving health in later life: how a life course approach could improve health and well-being in old age. In: Walker A, editor. The future of ageing in Europe. Switzerland: Springer Nature; 2018. p. 177–215.
Murabito JM, Yuan R, Lunetta KL. The search for longevity and healthy aging genes: insights from epidemiological studies and samples of long-lived individuals. J Gerontol A Biol Sci Med Sci. 2012;67:470–9.
Giuliani C, Garagnani P, Franceschi C. Genetics of human longevity within an eco-evolutionary nature-nurture framework. Circ Res. 2018;123:745–77.
Morris BJ, Willcox BJ, Donlon TA. Genetic and epigenetic regulation of human aging and longevity. Bbadis. 2018. https://doi.org/10.1016/j.bbadis.2018.08.039.
Gianfrancesco O, Bubb VJ, Quinn JP. Treating the “E” in “G × E”: trauma-informed approaches and psychological therapy interventions in psychosis. Front Psych. 2019;10. https://doi.org/10.3389/fpsyt.2019.00009.
Pakpahan E, Hoffmann R, Kröger H. The long arm of childhood circumstances on health in old age: evidence from SHARELIFE. Adv Life Course Res. 2017;31:1–10.
Lennartsson C, sif Eyjólfsdóttir H, Keller CR, Fritzell J, Pearlin LI, Schieman S, et al. Stress, health, and the life course: some conceptual perspectives. J Health Soc Behav. 2005;46:205–19.
Hanson M, Gluckman P. Developmental origins of noncommunicable disease: population and public health implications. Am J Clin Nutr. 2011;94(suppl_6, 1):1754–8.
Xia Q, Cai H, Xiang YB, Zhou P, Li H, Yang G, et al. Prospective cohort studies of birth weight and risk of obesity, diabetes, and hypertension in adulthood in the Chinese population. J Diabetes. 2019;11:55–64.
Seckl JR, Holmes MC. Mechanisms of disease: glucocorticoids, their placental metabolism and fetal 'programming' of adult pathophysiology. Nat Clin Pract Endocrinol Metab. 2007;3:479–88.
Zelko IN, Zhua J, Roman J. Maternal undernutrition during pregnancy alters the epigenetic landscape and the expression of endothelial function genes in male progeny. Nutr Res. 2019;61:53–63.
Hillier TA, Pedula KL, Schmidt MM, Mullen JA, Charles MA, Pettitt DJ. Childhood obesity and metabolic imprinting: the ongoing effects of maternal hyperglycemia. Diabetes Care. 2007;30:2287–92.
Robinson WP, Peñaherrera MS, Konwar C, Yuan V, Wilson SL. Epigenetic modifications in the human placenta. In: Human reproductive and prenatal genetics. Leung PCK, Qiao J, eds. Academic Press, Cambridge, Mass. 2019, Ch. 13, 293–311.
Chase KA, Melbourne JK, Rosen C, McCarthy-Jones S, Jones N, Feiner BM, et al. Traumagenics: at the intersect of childhood trauma, immunity and psychosis. Psychiatry Res. 2018;273:369–77.
Speakman JR, Mitchell SE, Mazidi M. Calories or protein? The effect of dietary restriction on lifespan in rodents is explained by calories alone. Exp Gerontol. 2016;86:28–38.
Colman RJ, Beasley TM, Kemnitz JW, Johnson SC, Weindruch R, Anderson RM. Caloric restriction reduces age-related and all-cause mortality in rhesus monkeys. Nat Commun. 2014;5:3557.
Dipasquale S, Pariante CM, Dazzan P, Aguglia E, McGuire P, Mondelli V. The dietary pattern of patients with schizophrenia: a systematic review. J Psychiatr Res. 2012;47:197–207.
Darmon N, Drewnowski A. Contribution of food prices and diet cost to socioeconomic disparities in diet quality and health: a systematic review and analysis. Nutr Rev. 2015;73:643–60.
Livingstone KM, Olstad DL, Leech RM, Ball K, Meertens B, Potter J, et al. Socioeconomic inequities in diet quality and nutrient intakes among Australian adults: findings from a nationally representative cross-sectional study. Nutrients. 2017;9:E1092.
Si Hassen W, Castetbon K, Cardon P, Enaux C, Nicolaou M, Lien N, et al. Socioeconomic indicators are independently associated with nutrient intake in French adults: a DEDIPAC study. Nutrients. 2016;8:158.
Fitch MI. Supportive care framework. Can Oncol Nurs J. 2008;18:6–14.
Degnan A, Berry K, Sweet D, Abel K, Crossley N, Edge D. Social networks and symptomatic and functional outcomes in schizophrenia: a systematic review and meta-analysis. Soc Psychiatry Psychiatr Epidemiol. 2018;53:873–88.
Walsh J, Hochbrueckner R, Corcoran J, Spence R. The lived experience of schizophrenia: a systematic review and meta-synthesis. Soc Work Ment Health. 2016;14:607–24.
Seeman MV. Solitude and schizophrenia. Psychosis. 2017;9:176–83.
Green MF, Horan WP, Lee J, McCleery A, Reddy LF, Wynn JK. Social disconnection in schizophrenia and the general community. Schizophr Bull. 2018;44:242–9.
Pinto RM. Using social network interventions to improve mentally ill clients’ well-being. Clin Soc Work J. 2006;34:83–100.
Cohen S. Social relationships and health. Am Psychol. 2004;59:676–84.
Schrempft S, Jackowska M, Hamer M, Steptoe A. Associations between social isolation, loneliness, and objective physical activity in older men and women. BMC Public Health. 2019;19:74.
Holt-Lunstad J, Smith TB, Layton JB. Social relationships and mortality risk: a meta-analytic review. PLoS Med. 2010;7:e1000316.
Valtorta NK, Kanaan M, Gilbody S, Ronzi S, Hanratty B. Loneliness and social isolation as risk factors for coronary heart disease and stroke: systematic review and meta-analysis of longitudinal observational studies. Heart. 2016;102:1009–16.
Holt-Lunstad J, Smith TB, Baker M, Harris T, Stephenson D. Loneliness and social isolation as risk factors for mortality: a meta-analytic review. Perspect Psychol Sci. 2015;10:227–37.
Holt-Lunstad J. Why social relationships are important for physical health: a systems approach to understanding and modifying risk and protection. Annu Rev Psychol. 2018;69:437–58.
Keinanen J, Mantere O, Markkula N, Partti K, Perälä J, Saarni SI, et al. Mortality in people with psychotic disorders in Finland: a population-based 13-year follow-up study. Schizophr Res. 2018;192:113–8.
Boyle PA, Barnes LL, Buchman AS, Bennett DA. Purpose in life is associated with mortality among community-dwelling older persons. Psychosom Med. 2009;71:574–9.
Musich S, Wan SHS, Kraemer S, Hawkins K, Wicker E. Purpose in life and positive health outcomes among older adults. Popul Health Management. 2018;2:139–47.
Schaefer SM, Morozink Boylan J, van Reekum CM, Lapate RC, Norris CJ, Ryff CD, et al. Purpose in life predicts better emotional recovery from negative stimuli. PLoS One. 2013;8:e80329.
Zilioli S, Slatcher RB, Ong AD, Gruenewald TL. Purpose in life predicts allostatic load ten years later. J Psychosom Res. 2015;79:451–7.
Zhao Y, Fu H, Guo A, Qiu L, Cheung KSL, Wu B, et al. A comparison of perceived uselessness between centenarians and non-centenarians in China. BMC Geriatr. 2018;8:251.
Stillman TF, Baumeister RF, Lambert NM, Crescioni AW, DeWall CN, Fincham FD. Alone and without purpose: life loses meaning following social exclusion. J Exp Soc Psychol. 2009;45:686–94.
Lambert NM, Stillman TF, Hicks JA, Kamble S, Baumeister RF, Fincham FD. To belong is to matter: sense of belonging enhances meaning in life. Personal Soc Psychol Bull. 2013;39:1418–27.
Pulopulos MM, Kozusznik MW. The moderating role of meaning in life in the relationship between perceived stress and diurnal cortisol. Stress. 2018;21:203–10.
Kim ES, Strecher VJ, Ryff CD. Purpose in life and use of preventive health care services. PNAS. 2014;111:16331–6.
Wagner LC, Torres-González F, Runte Geidel A, King MB. Existential questions in schizophrenia: perceptions of patients and caregivers. Rev Saúde Pública. 2011;45:401–8.
Iwasaki Y, Messina ES, Hopper T. The role of leisure in meaning-making and engagement with life. J Posit Psychol. 2018;13:29–35.
Hutchinson SL, Nimrod G. Leisure as a resource for successful aging by older adults with chronic health conditions. Int J Aging Hum Develop. 2012;74:41–65.
Iwasaki Y, Coyle C, Shank J, Messina E, Porter H. Leisure-generated meanings and active living for persons with mental illness. Rehab Couns Bull. 2013;57:46–56.
Iwasaki Y, Messina E, Coyle C, Shank J. Role of leisure in meaning-Making for community-dwelling adults with mental illness: Inspiration for engaged life. JLR. 2015;47:538–55.
Trussell DE, Mair H. Seeking judgment free spaces: poverty, leisure, and social inclusion. JLR. 2010;42:513–33.
Twigger-Holroyd A. Perceptions and practices of dress-related leisure: shopping, sorting, making and mending. Ann Leisure Res. 2016;19:275–93.
Wensley R, Slade A. Walking as a meaningful leisure occupation: the implications for occupational therapy. Br J Occup Ther. 2012;75:85–92.
Hegarty CB, Plucker JA. Creative leisure and self-expression. Int J Creativity Problem Solving. 2012;22:63–78.
Petrou P, Bakker AB, den Heuvel M. Weekly job crafting and leisure crafting: implications for meaning-making and work engagement. JOOP. 2017;90:129–52.
Porter H, Iwasaki Y, Shank J. Conceptualizing meaning-making through leisure experiences. Soc Leisure/Loisir Soc. 2013;33:167–94.
Roth DL, Brown SL, Rhodes JD, Haley WE. Reduced mortality rates among caregivers: does family caregiving provide a stress-buffering effect? Psychol Aging. 2018;33:619–29.
Miyawaki A, Tanaka H, Kobayashi Y, Kawachi I. Informal caregiving and mortality ― who is protected and who is not? A prospective cohort study from Japan. Soc Sci Med. 2019;223:24–30.
Eneman M, Vanhee L, Liessens D, Luyten P, Sabbe B, Corveleyn J. Humanistic psychiatry and psychotherapy: listening to patients as persons in search of meaning. The case of schizophrenia. J Humanist Psychol. 2019;59:148–69.
Rosen A. Return from the vanishing point: a clinician's perspective on art and mental illness, and particularly schizophrenia. Epidemiol Psychiatr Sci. 2007;16:126–32.
Topor A, Stefansson CG, Denhov A, Bülow P, Andersson G. Recovery and economy; salary and allowances: a 10-year follow-up of income for persons diagnosed with first-time psychosis. Soc Psychiatry Psychiatr Epidemiol. 2019;54. https://doi.org/10.1007/s00127-019-01655-4.
Mood C, Jonsson JP. The social consequences of poverty: an empirical test on longitudinal data. Soc Indic Res. 2016;127:633–52.
Corrigan P. How stigma interferes with mental health care. Am Psychol. 2004;59:614–25.
Davey Smith G, Carroll D, Rankin S, Rowan D. Socioeconomic differentials in mortality: evidence from Glasgow graveyards. Br Med J. 1992;305:1554–7.
Gould EM, Chappel DB. Graveyard gleanings: socio-economic, geographical and gender inequalities in health at Tynemouth, UK, 1833-1853. J Public Health Med. 2000;22:280–6.
Pruessner JC, Dedovic K, Pruessner M, Lord C, Buss C, Collins L, et al. Stress regulation in the central nervous system: evidence from structural and functional neuroimaging studies in human populations. Psychoneuroendocrinol. 2010;35:179–91.
Chiang JJ, Turiano NA, Mroczek DK, Miller GE. Affective reactivity to daily stress and 20-year mortality risk in adults with chronic illness: findings from the National Study of daily experiences. Health Psychol. 2018;37:170–8.
Seeman TE, Crimmins E, Huang MH, Singer B, Bucur A, Gruenewald T, et al. Cumulative biological risk and socio-economic differences in mortality: MacArthur studies of successful aging. Soc Sci Med. 2004;58:1985–97.
Nugent KL, Chiappelli J, Rowland LM, Hong LE. Cumulative stress pathophysiology in schizophrenia as indexed by allostatic load. Psychoneuroendocrinol. 2015;60:120–9.
Savransky A, Chiappelli J, Fisseha F, Wisner KM, Xiaoming D, Mirmomen SM, et al. Elevated allostatic load early in the course of schizophrenia. Transl Psychiatry. 2018;8:246.
Berger M, Juster RP, Westphal S, Amminger GP, Bogerts B, Schiltz K, et al. Allostatic load is associated with psychotic symptoms and decreases with antipsychotic treatment in patients with schizophrenia and first-episode psychosis. Psychoneuroendocrinol. 2018;90:35–42.
Hooker CI, Tully LM, Verosky SC, Fisher M, Holland C, Vinogradov S. Can I trust you? Negative affective priming influences social judgments in schizophrenia. J Abnorm Psychol. 2011;120:98–107.
Link BG, Phelan JC. Stigma and its public health implications. Lancet. 2006;367:528–9.
Geiss M, Chamberlain J, Weaver T, McCormick C, Raufer A, Scoggins L, et al. Diagnostic overshadowing of the psychiatric population in the emergency department: physiological factors identified for an early warning system. J Am Psychiatr Nurses Assoc. 2018;24:327–31.
Jones S, Howard L, Thornicroft G. ‘Diagnostic overshadowing’: worse physical health care for people with mental illness. Acta Psychiatr Scand. 2008;118:169–71.
Brown S, Kim M, Mitchell C, Inskip H. Twenty-five year mortality of a community cohort with schizophrenia. Br J Psychiatry. 2010;196:116–21.
Druss BG, Chwastiak L, Kern J, Parks JJ, Ward MC, Raney LE. Psychiatry’s role in improving the physical health of patients with serious mental illness: a report from the American Psychiatric Association. Psychiatr Serv. 2018;69:254–6.
Lee EE, Liu J, Tu X, Palmer BW, Eyler LT, Jeste DV. A widening longevity gap between people with schizophrenia and general population: a literature review and call for action. Schizophr Res. 2018;196:9–13.
Walker ER, McGee RE, Druss BG. Mortality in mental disorders and global disease burden implications: a systematic review and meta-analysis. JAMA Psychiat. 2015;72:334–41.
Nemani KL, Greene MC, Ulloa M, Vincenzi B, Copeland PM, Al-Khadari S, et al. Clozapine, diabetes mellitus, cardiovascular risk and mortality: results of a 21-year naturalistic study in patients with schizophrenia and schizoaffective disorder. Clin Schizophr Relat Psychoses. 2019;12:168–76.
Onwordi E, Howes O. Trends in mortality in schizophrenia and their implications. Acta Psychiatr Scand. 2018;138:489–91.
Rødevand L, Steen NE, Elvsåshagen T, Quintana DS, Reponen EJ, Mørch RH, et al. Cardiovascular risk remains high in schizophrenia with modest improvements in bipolar disorder during past decade. Acta Psychiatr Scand. 2019;139:348–60.
Tanskanen A, Tiihonen J, Taipale H. Mortality in schizophrenia: 30-year nationwide follow-up study. Acta Psychiatr Scand. 2018;138:492–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The author declares that she has no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Seeman, M.V. Schizophrenia Mortality: Barriers to Progress. Psychiatr Q 90, 553–563 (2019). https://doi.org/10.1007/s11126-019-09645-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11126-019-09645-0