Abstract
Purpose
Growth hormone (GH) therapy has been studied as treatment for clinical manifestations of adult-onset growth hormone deficiency (AO-GHD), including cardiovascular risk, bone health, and quality of life. Patients with AO-GHD typically also have significant history of pituitary pathology and hypopituitarism, which raises the question of what proportion of their clinical presentation can be attributed to GHD alone. Currently, much of the existing data for GH therapy in AO-GHD come from uncontrolled retrospective studies and observational protocols. These considerations require careful reassessment of the role of GH as a therapeutic agent in adult patients with hypopituitarism.
Methods
We contrast results from placebo-controlled trials with those from uncontrolled and retrospective studies for GH replacement in patients with hypopituitarism. We also examine the evidence for the manifestations of AO-GHD being attributed to GHD alone, as well as the data on adults with congenital, life-long untreated isolated GHD.
Results
The evidence for increased morbidity and mortality in hypopituitary patients with GHD, and for the benefits of GH therapy, are conflicting. There remains the possibility that the described clinical manifestations of AO-GHD may not be due to GHD alone, but may also be related to underlying pituitary pathology, treatment history and suboptimal hormone replacement.
Conclusions
In the setting of inconsistent data on the benefits of GH therapy, treatment of AO-GHD remains an individualized decision. There is a need for more randomized, placebo-controlled studies to evaluate the long-term outcomes of GH therapy in adults with hypopituitarism.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The development of biosynthetic growth hormone (GH) has dramatically changed the lives of thousands of children with growth hormone deficiency (GHD) and short stature by promoting their statural growth. The widespread availability of biosynthetic GH has allowed studies of its effects in a different GHD population—adults with acquired hypopituitarism.
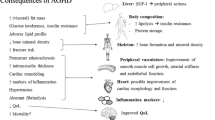
In the 1990s, two studies from Sweden found increased mortality rates in adult patients with hypopituitarism [1, 2]. Since all other hormonal deficiencies were thought to be appropriately replete, the two- to three-fold higher cardiovascular and cerebrovascular mortality rates were attributed to the untreated GH deficiency. This syndrome of adult-onset GH deficiency (AO-GHD) has subsequently been described to be associated with possible increased cardiovascular and cerebrovascular morbidity and mortality, abnormal body composition consisting of decreased lean mass and increased fat mass, unfavorable atherogenic profile, insulin resistance, decreased bone mineral density, and impaired quality of life [3]. Multiple subsequent open-label, observational studies suggested that the anabolic and lipolytic properties of GH replacement in this population improved many of the above parameters, and GH was approved by the Food and Drug Administration and international agencies for the treatment of AO-GHD.
GH therapy has been used for management of deleterious effects of GHD in patients with hypopituitarism, often due to neoplastic pituitary diseases. However, it is important to emphasize that “GH deficiency” and “hypopituitarism” are not synonymous: the latter, in addition to GHD, includes other, GH-independent, components. Some of the adverse manifestations in patients with hypopituitarism may not be due to GH deficiency per se, but rather to the nature of their organic pituitary disease and/or to the effects of its treatment (surgery, radiation, suboptimal replacement of other hormonal deficiencies), psychological burden of chronic disease, etc.
A number of prospective, randomized, placebo-controlled trials have suggested that, compared to placebo, GH therapy has not consistently improved the detrimental effects of hypopituitarism attributed to GHD. This is in contrast with the results from many uncontrolled retrospective and open-label observational studies. While placebo-controlled trials have their own deficiencies and are challenging to complete in small patient populations, these trials nevertheless provide data with fewer confounders as compared to open-label studies.
Given the preponderance of literature reviewing retrospective and observational data, this review will focus primarily on placebo-controlled studies to assess of the role of GH as a therapeutic agent in adult patients with hypopituitarism.
GH deficiency and mortality
Increased mortality rate in hypopituitarism has been hypothesized to be due to unsubstituted GHD [1, 4, 5]. This is in contrast with the observation in animal models that isolated GHD is accompanied by a 20–70% increase in life span [6]. In adults with untreated congenital GHD, normal longevity and no increased incidence of cardiovascular diseases were observed [7,8,9]. Autopsy data in patients with hypopituitarism and unsubstituted GHD showed a two-fold decrease in heart disease but a two-fold increase in cerebrovascular mortality, and in particular, a four- to five-fold increase in intracerebral hemorrhage [10]. Data on exposure to cranial radiation were not reported, but perhaps this would explain the discrepancy in effects on cerebral and coronary vasculature.
Tomlinson et al. [5] performed careful outcome analyses in 1014 hypopituitary subjects. They confirmed increased overall and vascular mortality rates in this population, but found no association with GHD. Patient sex, age, diagnosis of craniopharyngioma, unsubstituted hypogonadism and especially a history of cranial radiation were found to be the notable risk factors. Brada et al. [11] similarly identified certain patient characteristics and treatment history were risk factors for increased cerebrovascular mortality.
Cranial radiation is known to induce cerebral vasculopathy with both increased atherosclerosis and intracerebral hemorrhage [12], in agreement with the data by Kaji et al. [10]. Patients who receive pituitary radiation have been documented to develop stroke in or near the field of irradiation [13]. A Dutch study found increased risk of cerebrovascular events in men with nonfunctioning pituitary adenomas who were treated with radiotherapy compared to those who were not [14]. In two Swedish studies [1, 2] that found increased mortality rates with hypopituitarism, the majority of patients had undergone cranial radiation; in contrast, a UK series [15] in which cranial radiation was used more sparingly, found that vascular mortality rates was similar in male subjects and lower in female subjects, compared to the control populations.
The impact of GHD on malignancy risk has also been studied: Stochholm et al. [16] reported that patients with childhood-onset GHD had a 19-fold increased higher cancer mortality. However, the majority of patients in this cohort had malignant diseases as a cause of hypopituitarism, raising concern that recurrence of the original disease or predisposition for a second malignancy are more likely explanations for higher cancer mortality. In the same study, when children with isolated GHD not due to malignant disease were analyzed, the excess mortality was not seen. Other data have shown a protective effect of GHD on the development of neoplasia. Patients with hypopituitarism and unsubstituted GHD were documented to have a three-fold lower incidence of prostate cancer [17]. Shevah et al. [18] found complete absence of malignant diseases in 222 individuals with IGF-1 deficiency (due to GH insensitivity or GH deficiency), whereas 9–24% incidence of cancer was observed in their 338 first- and second-degree relatives.
Looking more broadly at risk factors for mortality in hypopituitary patients, two meta-analyses compiled the available data from 6 and 12 observational studies [19, 20]. In both studies, standardized mortality ratio was higher in patients who were female, younger, underwent transcranial surgery, and received cranial irradiation. In an earlier study by Pappachan et al. [19], GH therapy was associated with decreased standardized mortality ratio, comparable to the background population. However, the authors cautioned that interpretation of these data may be misleading given the selection bias of observation studies without untreated control groups. In a more recent larger analysis, Jasim et al. [20] noted lower standardized mortality ratio in patients treated with GH (1.24) compared to those who were untreated (1.68), but the confidence intervals of the two groups overlap without mention of statistical significance. Gaillard et al. [21] analyzed the increased standardized mortality ratios of hypopituitary patients treated with GH therapy in the KIMS database, and found contributing factors of the increased mortality to include female gender, younger age, and lower IGF-1.
Thus, in patients with hypopituitarism, increased mortality may be multifactorial and may not be attributable to GHD alone. GH therapy cannot ameliorate underlying pituitary pathology and treatment complications, which may be the actual etiologies of the observed mortality. While certain groups of patients with hypopituitarism may suffer from increased mortality, GH therapy has not been shown to reduce mortality.
Body composition, physical fitness and metabolic consequences
It was hypothesized that, in adults with GHD, administration of GH, a hormone with anabolic properties, would increase muscle mass and thus, physical strength and endurance. Concurrently, the lipolytic effect of GH should also decrease the fat mass, ameliorate metabolic syndrome and improve cardiovascular risk factors. Existing studies offer inconsistent data on both these hypotheses.
GH therapy has been associated with a measured increase in lean body mass; this may not be due to an increase in muscle fiber mass, but rather due to accumulation of water in extracellular fluid, as GH increases sodium reabsorption and plasma renin activity [22]. In one open-label prospective study, men given GH replacement for 10 years were reported to develop increased muscle strength by 5 years and were partially protected against normal age-related decline in strength in the last 5 years [23]. In contrast, other open label studies found improvements in one muscle group strength but no improvement in others [24]. In a randomized, placebo-controlled crossover trial, 60 patients who had received GH therapy for more than 3 years were assigned to continue GH or placebo for 4 months [25]. The placebo group had decreased measured thigh muscle mass (perhaps due to water loss) but without change in muscle strength.
There is some evidence that GH therapy improves aerobic and anaerobic capacity. A 22-month placebo controlled crossover study did show a significantly increased maximal oxygen uptake and a trend towards increased endurance performance that did not reach statistical significance [26]. A similar 6-month placebo-controlled trial found a positive uptrend in maximal oxygen consumption not reaching statistical significance, though baseline maximal oxygen consumption was already normal [27]. Some studies suggest that anaerobic power is impaired in AO-GHD [28]. In a 1 month placebo-controlled crossover study, GH therapy improved anaerobic power but not maximal oxygen uptake [29]. A longer, 2-year double-blind randomized trial in GHD adolescents transitioning to adulthood did not find a statistically significant change in treadmill exercise tolerance [30].
The observed improvement in exercise capacity seen in some studies has been attributed to improved cardiac function, perhaps due to increased plasma volume with GH therapy [31]. Studies of cardiac function indicate that GH improves parameters such as cardiac output, left ventricular ejection fraction, diastolic abnormalities [32,33,34]. However, the baseline cardiac function in GHD is not always abnormal: in one such study of 12 months of GH therapy, the left ventricular ejection fraction of the AO-GHD subjects were normal at baseline, 64.1%, compared with 65.8% in controls; the clinical significance of an increased to 70% after therapy is unclear [33]. In another study, 6 months of GH therapy increased stroke volume from an average of 92 mL, within normal range, to 118 mL [32].
The most consistent effect of GH administration in patients with GHD is decrease in fat mass [35], with magnitude of about 2 kg after 6 months. Fat mass does not increase further over time, and reverts to baseline with discontinuation [26]. The most recent review of 23 prospective studies found that GH does not change or increases body mass index, waist circumference, and waist-hip ratio [36]. These changes in body composition have been associated with inconsistent impact in metabolic and cardiovascular risk factors.
Some prospective and randomized controlled studies reported no impact of GH on lipid profiles, while others reported an association with improved lipid profile patterns. In a placebo-controlled 4-month crossover trial, both favorable and unfavorable lipid changes developed during the placebo period: while total cholesterol and LDL increased, HDL also increased and triglyceride levels decreased [25]. In a meta-analysis of 37 blinded randomized, placebo-controlled studies, GH replacement was reported to reduce LDL and total cholesterol in half the studies and had no effect in the others; overall, statistically significant decreases of 19.3 and 11.6 mg/dL, respectively, were seen[37]. No effect on HDL cholesterol or triglycerides was observed. Data on other markers of cardiovascular risk were mixed: there was some evidence that GH treatment decreased inflammatory markers (such as C-reactive protein, interleukin-6, TNF-α), as well as carotid intima-media thickness, a predictor of coronary disease [38]. But GH replacement was also reported to increase plasma concentrations of lipoprotein A, an independent marker of cardiovascular risk [39]. In studies where improvements in markers of cardiovascular risk were noted, there was no accompanying change in measured cardiovascular function [27, 40]. Castillo et al. [41] compared 41 patients with panhypopituitarism on no GH substitution with 37 healthy age- and sex-matched controls. Panhypopituitary patients had lower fasting glucose, serum insulin level, insulin resistance, and waist/hip ratio, but higher serum levels of CRP. The occurrence of hyperlipidemia was higher in panhypopituitary patients but the occurrence of metabolic syndrome was similar to controls.
How effective is GH substitution compared to standard HMG CoA reductase inhibitors (statins) in hypopituitary patients? Monson et al. [42] compared triglycerides, total, HDL and LDL cholesterol in statin-treated and statin-untreated hypopituitary adults before and after 12 months of treatment with GH. Baseline total cholesterol and calculated LDL in statin-untreated patients were 5.8 ± 1.2 and 3.7 ± 1.0 mmol/l (mean ± standard deviation), respectively, and in those treated with statins were significantly lower, at 5.2 ± 1.4 and 3.1 ± 1.3 mmol/l, respectively. Administration of GH to statin-untreated patients decreased LDL by 0.28 ± 0.8 mmol/l, with the resulting levels still higher than in statin-treated GH naïve patients. There were no changes in HDL cholesterol or triglycerides.
The impact of GH therapy on other cardiovascular risk factors, including insulin sensitivity and risk for diabetes, has also been studied. In some studies, administration of GH has been reported to result in glucose intolerance [43]. Some observational studies show mixed data: Svensson et al. [44] reported no change in insulin sensitivity on euglycemic clamp testing in 11 GHD patients after 7 years of GH replacement, and HypoCCS data showed increased incidence of diabetes compared to background population in the GH-treated cohorts in the US and Sweden, but not in France or Germany [45]. Analysis of KIMS observational data from 5143 patients with an average of 4 year follow-up found increased incidence of diabetes compared to age-matched background population, with highest incidence in the first year of therapy and decreasing incidence thereafter; in a subgroup of patients with annual follow-up for 6 years, fasting glucose and hemoglobin A1c levels increased continuously over the observed period [46]. In the HypoCCS trial, administration of GH induced abnormally elevated fasting blood glucose in 34.5% patients without pre-existing diabetes, but it appeared to normalize with continuation of therapy in the majority of them [47]. However, a meta-analysis of randomized placebo-controlled trials including more than 500 patients found mean fasting glucose to be normal during growth hormone treatment, with an overall minimal increase of 0.43 mmol/L [37]. Data were more consistent in double-blind placebo controlled trials: in the 4-month crossover trial, insulin sensitivity was noted to improve after stopping GH replacement versus continued GH therapy[25]. In placebo-controlled trials of 12–18 months duration [26, 37, 39], GH administration caused further increases in insulin and glucose levels, despite significant loss of truncal fat. Similarly in other trials [49,50,51], GH replacement did not improve the prevalence of metabolic syndrome, but resulted in statistically significant increases in blood pressure and fasting blood glucose; ultimately no change in metabolic syndrome was seen after 3 years of therapy [48]. The clinical significance of all these data remains difficult to interpret, as control subjects were not always followed and tested with the same intensity as the treatment group. Overall, the available data suggest GH administration does not seem to induce clinically significant alterations in glucose levels, but several studies have noted increased insulin resistance.
There is data suggesting that the “metabolic syndrome” of hypopituitarism may be not due to GH deficiency per se, but rather a consequence of inappropriate glucocorticoid replacement in these patients [49]. For decades, patients with hypopituitarism were treated with supraphysiologic doses of glucocorticoids equivalent to 25–35 mg of hydrocortisone per day. In addition, GHD enhances regeneration of cortisol from cortisone through increased 11β-HSD type 1 activity [50]. The combination of supraphysiologic glucocorticoid dosages and increased cortisol generation from cortisone brought about by GHD can result in excessive cortisol exposure for patients with hypopituitarism treated with what was considered appropriate doses of hydrocortisone [50]. In other words, in the setting of supraphysiologic glucocorticoid dosing, GH therapy decreased cortisone reduction via 11β-HSD type 1, thereby ameliorating hypercortisolism.
Data from the KIGS-KIMS database showed that many features of metabolic syndrome—increased waist circumference, higher BMI, elevated triglycerides, total and LDL cholesterol—was proportionate to the dose of their glucocorticoid replacement, and that patients taking less than 20 mg of hydrocortisone daily had no manifestations of metabolic syndrome in excess of the ACTH-sufficient group [51]. Notably, the development of new diabetes, stroke and myocardial infarction was found in the GH-treated group on glucocorticoid replacement [51]. Swords, et al. [52] showed that administration of GH to glucocorticoid-treated hypopituitary adults markedly lowered their plasma cortisol milieu. This effect alone could at least partially explain the improvements in body composition observed in hypopituitary subjects treated with GH. Danilowicz et al. [53] further found that a decrease of hydrocortisone dose from the supraphysiologic 35 mg per day to the currently accepted 15 mg per day for 6–12 months resulted in major body fat loss (7.1 kg of total body fat, 4.1 kg of abdominal body fat), trend toward increased lean body mass, and major declines in total cholesterol and triglycerides. These data suggest that optimization of glucocorticoid replacement alone, in the absence of GH supplementation, results in improved body composition and metabolic parameters in hypopituitary adults. Although the study by Danilowicz et al. cannot be replicated today, it would be valuable to study whether hypopituitary patients in the current era, treated with the hydrocortisone equivalent below 20 mg per day from the time of diagnosis, exhibit signs of metabolic syndrome in excess of the general population. Perhaps patients should first be optimized with respect to glucocorticoid dosing, followed with observation of their clinical progress, and then evaluated for the need for GH replacement.
In a study by Egger et al. [54], 10 AO-GHD patients who were either ACTH-sufficient and receiving no exogenous glucocorticoids, or those treated with physiological hydrocortisone replacement doses, had normal subcutaneous and visceral fat mass, fat-free mass and insulin sensitivity as compared to age and BMI-matched healthy controls. These findings need to be confirmed in larger studies.
Thus, in properly controlled studies in AO-GHD patients, the GH-induced increase in lean body mass is inconsistently translated into increased muscle strength but may improve endurance. The loss of body fat is not accompanied by a consistent improvement in lipid profile, but may decrease glucose tolerance. The possibility that metabolic abnormalities in hypopituitarism are related to supraphysiologic glucocorticoid replacement rather than GHD, merits further investigation.
Bone health
The impact of GH therapy on bone health has been studied extensively: GH causes an initial decrease in BMD to approximately 6 months of therapy, followed by a subsequent increase in this parameter after 12–24 months of therapy [55]. The effect may persist even after GH is discontinued [56]. The latest meta-analysis synthesized data from 1403 patients with GHD across 31 studies, which included nine randomized placebo-controlled studies [57]. Treatment period ranged from 6 to 180 months; randomized controlled studies demonstrated increases in BMD in lumbar spine (ranging from 1–7%) and femoral neck (ranging from 0.6–4%) in studies conducted for more than a year, and decreases in these parameters in studies conducted for less than 1 year; in subgroup analyses, the increases in BMD were only significant in men. In a 15-year observational follow-up of GH replacement in 126 adults, femoral neck BMD was maintained, and lumbar BMD increased by 5% compared to baseline [58]. The results are notable, though the study was too small to evaluate impact on fracture incidence.
In the prospective cohort study of fracture risk in the HypoCCS database, patient-reported fracture incidence was compared in 9641 AO-GHD individuals receiving or not receiving GH therapy [59]. Over a mean follow-up period of 4.6-years, annual facture incidence rate was lower in patients without pre-existing osteoporosis receiving GH; no difference in fracture risk was found in the subgroup of patients with pre-existing osteoporosis. The authors acknowledged notable confounding factors, including younger age, more women, lower percentage of pre-existing osteoporosis, and higher percentage of estrogen use in the GH treated group. There remains an absence of data on fracture end points from randomized controlled studies.
The effect of bisphosphonates in AO-GHD has also been studied. In a study of 30 GHD patients consisting of 15 participants with osteoporosis and 15 controls, GH replacement gradually increased BMD but plateaued after 3 to 4years, while the addition of alendronate rapidly increased BMD over an additional 3 years of treatment [60]. Biermasz et al. [61] also conducted a study in 18 patients with GHD and osteoporosis who had received GH replacement for 4 years: half were randomized to continue GH alone and half to continue GH with the addition of alendronate for 12 months. The latter group was found to have significantly increased BMD at the lumbar spine with decreased in bone turnover markers. These studies suggest that bisphosphonates may augment GH effects.
Prior to considering treatment, it is important to evaluate whether patients with GHD have inferior bone health: some studies indicate that GHD and hypopituitarism are associated with decreased BMD and increased risk of fracture [62, 63]. There is also evidence that BMD in adults with GHD is not significantly different from age and sex matched controls [64,65,66], and that the measured decreased BMD in children with GHD might be due to an artifact of a small bone size [66], as summarized and reviewed by Hogler and Shaw[67].
It is also important to determine whether the increased risk of fractures in hypopituitarism is due to GHD per se, or related to the shortcomings of other hormone replacement: undertreatment with sex steroids, and overtreatment with glucocorticoids or thyroid hormone [68, 69]. Mazziotti et al found a direct correlation between the dose of glucocorticoid replacement and the incidence of vertebral fractures in hypopituitary adults, and that treatment with GH markedly attenuated the incidence of fractures in glucocorticoid-treated subjects [70]. Similarly, radiological vertebral fractures were associated with higher doses of levothyroxine and higher serum free T4 levels in patients on GH treatment [69]. This is similar to the above-mentioned data on glucocorticoid replacement and metabolic syndrome [51].
Bouillon et al. [68] compared the prevalence of fractures in Russian adults with isolated GHD and those with multiple pituitary hormones deficiencies (MPHD) with background controls. In the study, none of the subjects with isolated GHD had ever received any GH treatment, and roughly half the subjects with MPHD had been intermittently treated with GH in childhood, ranging from 2 months to a maximum of 2 years. The average age of the isolated GHD group was 23 years, and they received no hormonal substitutions; their fracture prevalence was the same as healthy controls. In young patients with MPHD of the same average age, the prevalence of fractures was increased with an odds ratio of 3 compared to healthy controls of the same age. In older patients with MPHD of both sexes with an average age of 55, the odds ratio was even higher, 7.4 compared to healthy controls. These data were obtained from the entire group, including both male and female subjects. However, the male patients received insufficient androgen supplementation with short-acting testosterone propionate 125–250 mg once monthly, instead of the recommended dosing of 25–50 mg daily or every other day, due to its short half-life. The female subjects were treated with appropriate doses of estradiol, suggesting that the fracture odds ratios in men on subtherapeutic testosterone replacement may have been even higher. This analysis suggests that it may not be GHD alone, but rather inadequate androgen replacement, that increases fracture risk.
In addition to optimizing management of other hormonal deficiencies, there are data suggesting that GH therapy is associated with maintaining or increasing bone BMD over longer treatment duration. GH treatment is also associated with decreased fracture incidence in subgroups of patients without pre-existing osteoporosis. There are currently no data on fracture risk from randomized controlled trials, and there are undoubtedly challenges to completing long term studies for a rare condition. In the setting of conflicting data on whether GHD patients have diminished bone health, it is currently difficult to form conclusions about the utility of GH therapy for improving bone health and reducing fracture risk, beyond adequate calcium and vitamin D intake with optimal replacement of other pituitary deficiencies.
Quality of life (QoL)
Low QoL is currently the most widely used indication for GH treatment in the US and is the only indication for GH therapy in adult hypopituitarism in the UK. In multiple open-label uncontrolled studies, GH administration has been suggested to improve QoL in patients with AO-GHD [24, 71, 72]. Retrospective case series of carefully selected patients with low baseline QoL have also been found to demonstrate significant improvement after 3 years of GH treatment [73].
The subjective and self-reporting nature of QoL metrics makes this evaluation prone to placebo effect. It is notable that the degree of QoL impairment in hypopituitarism does not correlate with the severity of GHD [24], and the QoL assessment tools are not clearly able to distinguish between patients with severe GH deficiency and those with GH excess [74]. Furthermore, adults with isolated childhood-onset GHD, the most severe and long-lasting form, do not have lower QoL [75, 76]; decreased QoL in adult patients with history of childhood GHD is only seen in those with associated diseases, syndromes or cancer [77]. This finding may be explained by a study of adult GHD patients conducted by psychiatrists, who found high prevalence of major depression, dysthymia and anxiety, which could “be attributed solely to the presence of a chronic disease” [78]. Lastly, observational studies of AO-GHD patients with very low QoL and their age- and sex-matched controls suggested regression to the mean after 2 years [79].
These considerations prompted a meta-analysis of 15 published, mostly open-label, studies comprising a total of 830 patients[80]. This study found a significant QoL effect of GH after 3 months of therapy; by 6 months, the GH effects were no longer distinguishable from placebo. Some studies found efficacy of GH therapy using surrogate markers such as days of sick leave or physician visits [81]. These may also be susceptible of placebo effect. Thus, prospective, randomized, placebo-controlled studies help to mitigate the placebo effect.
Table 1 shows the summary of all randomized, placebo-controlled studies that included more than 10 adults with GHD treated with GH for at least 6 months. All QoL studies, whether placebo-controlled or open-label, are unfortunately limited by sensitivity and specificity of available assessment tools, as well as their validation for different ethnicities, but most of the listed placebo-controlled studies employed multiple tools. Interpretation of the studies is limited by a number of additional factors; some studies found normal baseline QoL, administered supraphysiologic GH dosing, or used non-validated diagnostic testing for GHD. With the exception of the study completed by Underwood et al. [82], which was conducted in young adults with childhood GHD, all other studies were conducted in AO-GHD.
In summary, in 15 placebo-controlled studies totaling 938 adults with GHD and utilizing 24 different quality of life instruments (Table 1), GH did not consistently have an advantage over placebo in improving QoL. A 21-month cross-over double blind trial found that the benefits of GH replacement was at least in part due to placebo effect; interestingly, the subjects’ spouses noted improved mood and behavior during the active drug phases of the trial [83]. Some studies utilized multiple questionnaires and/or analyzed multiple “sub-domains” of the same questionnaire. In such studies employing multiple comparisons, occasional questionnaires indicated higher efficacy for GH, but others showed higher efficacy for the placebo [84, 85]. In one study [85], the energy domain of the NHP test improved more on GH, but the reverse was true in another study [86]. The negative results of some of these studies were attributed to the normal QoL at baseline [26]; lack of GH efficacy was also found in a study in which the data from only severely impaired patients were separately analyzed [86].
The study by Miller et al. [87] stands apart as a study demonstrating superiority of GH over placebo using AGHDA score and some subdivisions of SF-36 and SQ. The population studied in this report was unique: it consisted of patients with acromegaly rendered GH deficient by radiation and/or surgery. This randomized, placebo-controlled 6-month study of 30 subjects found improvement in QoL in the treatment group. A study by van der Klaauw [88] in a similar group of patients did not reproduce these results. Still, there may be a difference in the QoL responses in GH-deficient patients who were previously chronically exposed to pathologically high GH/IGF-1 milieu. Whether certain populations, such as patients with previous acromegaly, truly benefit from GH therapy, deserves future attention.
The suggestion that GH therapy could be beneficial in patients with history of Cushing’s disease has also been studied. Feldt-Rasmussen et al. [89] found in analysis of the KIMS database that GH replacement was safe and particularly improved QoL in individuals previously treated for Cushing’s disease. However, Webb et al. [90] found in the HypoCCS cohort that, compared to those with nonfunctioning pituitary adenomas, individuals with prior Cushing’s disease treated with GH developed two- to threefold greater incidence of metabolic syndrome, cardiovascular disease, cerebrovascular disease over the 3-year study period.
Proponents of GH therapy for treatment of decreased QoL may argue that absence of a detectable improvement does not equate to absence of beneficial action. However, other medications that rely on patient self-assessment tools to evaluate for efficacy, such as antidepressants, do show measurable effect on these assessments in placebo-controlled trials. The counter-argument is that GH therapy should be held to a similar conventional efficacy standard, though this may be more challenging due to smaller patient population.
As with metabolic and bone effects of GH replacement, the potential influence of glucocorticoid therapy should also be considered. Somatic and psychiatric manifestations of Cushing’s syndrome may, at least in part, account for lower QoL at baseline and its improvement with GH replacement. In a population of 194 patients with primary adrenal insufficiency and 140 patients with secondary adrenal insufficiency due to hypopituitarism, Bleicken et al. [91] showed the deleterious effects on QoL of hydrocortisone doses greater than 30 mg per day. No difference was observed between the primary and secondary groups. A more recent study compared QoL in post-transsphenoidal surgery hypopituitary patients with untreated GHD who were on an average of hydrocortisone dose of 15 mg per day, with the control group of patients who had undergone transnasal surgery for benign sinus conditions [92]: the hypopituitary patients who had no history of radiation had similar QoL as controls, but those who had undergone both surgery as well as radiation had lower QoL. Finally, Danilowicz et al. [53] demonstrated significant improvement in QoL (AGHDA score) in panhypopituitary patients whose daily hydrocortisone replacement was decreased from 35 to 15 mg per day.
Additional studies should be performed with attention to weaknesses in existing studies, including exclusion of individuals with normal baseline QoL, appropriate GH dosing, and universally validated criteria for diagnosis of GHD.
Isolated growth hormone deficiency
Most of the studies addressing the issue of GH efficacy in adults with GHD were conducted in patients with history of pituitary disease. The relative contributions of GHD, versus history of pituitary surgery, radiation therapy, suboptimal hormonal replacement, etc., are difficult to discern. The effects of GHD are ideally studied in adult patients without history of complicating factors. In this regard, a series of studies in a Brazilian cohort have provided us with unique perspectives on GHD.
In Itabaianinha municipality, Brazil, there is a population of individuals with congenital, life-long untreated isolated GHD due to an inactivation mutation in the growth hormone-releasing hormone receptor gene [93]. Since the 1990s, the studies on more than 100 untreated individuals have provided a unique model for understanding the physiologic effects of GHD in the absence of confounding factors. The characteristic physical features of this isolated GHD population included short stature and truncal obesity. Compared to age- and gender-matched controls, they have normal longevity [9], normal QoL as evaluated by commonly used questionnaires [75], no increased risk of fractures, and superior muscle strength [94]. In the assessment of BMD, adults with isolated GHD have lower areal BMD due to smaller bone mass, but when BMD is corrected for bone size, the volumetric BMD is similar to controls[95]. These individuals do have increased truncal adiposity [96], and higher total and LDL cholesterol throughout life [97], but they do not have greater carotid intimal medial thickness or coronary atherosclerosis [7]; their cardiovascular mortality is no different from the control population [9]. Oliveira et al. [98] found that in 20 adults with isolated GHD who were treated with GH for 6 months, lipid profile and body composition improved, but carotid intimal thickness increased and carotid atherosclerotic plaques developed, with a 52-fold increased likelihood to have a carotid atherosclerotic plaque by 12 months even after discontinuation of GH therapy. 5 years after interruption of GH therapy, intima-media thickness returned to normal, but the number of atherosclerotic plaques did not change [99]. Their QoL was unchanged with GH therapy[75]. These data is in notable contrast to findings by Pfeifer et al. [100], who found that 18-month treatment with GH therapy in 11 men normalized the previously elevated intimal medial thickness of the common carotid artery and carotid bifurcation; this study did not report the incidence of plaque formation noted by Oliveira et al. The reason for the conflicting findings is unknown, but perhaps may be due to inherent differences between acquired versus congenital GHD, or the impact of using long-acting GH; this highlights the importance of further studies to better understand discrepancies in research findings such as these.
Isolated GHD is not the perfect paradigm for AO-GHD, and data in the isolated GHD population may not be directly applicable to managing the medical complexities of patients with AO-GHD. Nevertheless, the findings provide us with valuable insight on the impact of long-term GHD on human health. They suggest that perhaps the symptoms experienced by patients with hypopituitarism and GHD may be multifactorial.
Summary and Conclusions
This analysis concludes that the data supporting detrimental consequences of GHD remain inconsistent. The increased morbidity and mortality rates in patients with hypopituitarism may not be due to GHD alone, and thus, the addition of GH to the established therapeutic regimen is uncertain to benefit longevity, as long as other pituitary hormone deficiencies are appropriately replaced.
The data on benefits of GH replacement are conflicting. There is some evidence that GH may maintain and increase BMD over the long term, with possible decreased risk of fractures. Observed increases in lean mass are susceptible to measurement error, without consistent improvement in patient strength, but there is some evidence of improved aerobic and anaerobic capacity. GH has been found to increase insulin resistance and induce loss of body fat with suggestion of improved lipid profile, though improvements in actual cardiovascular outcomes have not been consistently seen. Finally, placebo-controlled studies have not demonstrated a reliable improvement in the QoL in hypopituitary patients treated with GH. Additionally, GH is costly and associated with side effects and potential risks. It is not clear that GH is cost-effective compared to current conventional therapy; for example, there is an absence of studies comparing GH therapy to statins in cardiovascular outcomes, and comparing GH therapy to bisphosphonates in bone health.
GH therapy remains open to debate, with experts in notable disagreement. Some experts have seen significant clinical benefits outweighing the risks of GH therapy [101], consistent with the Endocrine Society recommendation for GH therapy use for those with biochemical GHD [102]. Others have noted variable individual responses to therapy; as such, the National Institute for Health and Care Excellence guidelines state that GH therapy may be tried for AO-GHD patients with significantly impaired QoL [103]. Furthermore, they agree that GH therapy may be continued in those who had demonstrated improvement in QoL after 6 months of open-label GH replacement. The most recent UpToDate article does not recommend GH therapy in AO-GHD in general, though acknowledges that patient preferences may impact treatment decisions [104].
Where do we go from here?
First, there is a need for more randomized, placebo-controlled studies to evaluate the long-term outcomes of GH replacement in adults with hypopituitarism and to identify individuals that may benefit from therapy [105]. Developing an objective understanding of the role of GHD in human morbidity and mortality is necessary for appropriate clinical management in suitable patients. Lastly, the possibility that inappropriate replacement of other hormone deficiencies is the culprit of many manifestations of hypopituitarism, should be considered and evaluated in properly-constructed trials.
GH replacement currently remains an individualized decision. Patients with AO-GHD who are already on and derive benefit from GH replacement will likely continue the medication. Criteria for long-term GH therapy remain a question to be answered. Initiation of GH replacement may be limited to patients managed by experienced providers employing standardized protocols with appropriate follow-up, with full disclosure of all potential risks and benefits, and publication of the results in peer-reviewed journals.
References
Rosén T, Bengtsson BA (1990) Premature mortality due to cardiovascular disease in hypopituitarism. Lancet Lond Engl 336:285–288
Bülow B, Hagmar L, Mikoczy Z et al (1997) Increased cerebrovascular mortality in patients with hypopituitarism. Clin Endocrinol (Oxf) 46:75–81
Shalet SM, Toogood A, Rahim A, Brennan BM (1998) The diagnosis of growth hormone deficiency in children and adults. Endocr Rev 19:203–223. https://doi.org/10.1210/edrv.19.2.0329
Svensson J, Bengtsson B-A, Rosén T et al (2004) Malignant disease and cardiovascular morbidity in hypopituitary adults with or without growth hormone replacement therapy. J Clin Endocrinol Metab 89:3306–3312. https://doi.org/10.1210/jc.2003-031601
Tomlinson JW, Holden N, Hills RK et al (2001) Association between premature mortality and hypopituitarism. West Midlands Prospective Hypopituitary Study Group. Lancet Lond Engl 357:425–431
Bartke A (2005) Minireview: role of the growth hormone/insulin-like growth factor system in mammalian aging. Endocrinology 146:3718–3723. https://doi.org/10.1210/en.2005-0411
Menezes Oliveira JL, Marques-Santos C, Barreto-Filho JA et al (2006) Lack of evidence of premature atherosclerosis in untreated severe isolated growth hormone (GH) deficiency due to a GH-releasing hormone receptor mutation. J Clin Endocrinol Metab 91:2093–2099. https://doi.org/10.1210/jc.2005-2571
Krzisnik C, Grgurić S, Cvijović K, Laron Z (2010) Longevity of the hypopituitary patients from the island Krk: a follow-up study. Pediatr Endocrinol Rev 7:357–362
Aguiar-Oliveira MH, Oliveira FT, Pereira RMC et al (2010) Longevity in untreated congenital growth hormone deficiency due to a homozygous mutation in the GHRH receptor gene. J Clin Endocrinol Metab 95:714–721. https://doi.org/10.1210/jc.2009-1879
Kaji H, Chihara K (2004) Direct causes of death in Japanese patients with hypopituitarism as analyzed from a nation-wide autopsy database. Eur J Endocrinol 150:149–152
Brada M, Ashley S, Ford D et al (2002) Cerebrovascular mortality in patients with pituitary adenoma. Clin Endocrinol (Oxf) 57:713–717
O’Connor MM, Mayberg MR (2000) Effects of radiation on cerebral vasculature: a review. Neurosurgery 46:138–149. https://doi.org/10.1093/neurosurgery/46.1.138 (discussion 150–151)
Rim CH, Yang DS, Park YJ et al (2011) Radiotherapy for pituitary adenomas: long-term outcome and complications. Radiat Oncol J 29:156–163. https://doi.org/10.3857/roj.2011.29.3.156
van Varsseveld NC, van Bunderen CC, Ubachs DHH et al (2015) Cerebrovascular events, secondary intracranial tumors, and mortality after radiotherapy for nonfunctioning pituitary adenomas: a subanalysis from the Dutch National Registry of Growth Hormone Treatment in Adults. J Clin Endocrinol Metab 100:1104–1112. https://doi.org/10.1210/jc.2014-3697
Bates AS, Bullivant B, Sheppard MC, Stewart PM (1999) Life expectancy following surgery for pituitary tumours. Clin Endocrinol (Oxf) 50:315–319
Stochholm K, Gravholt CH, Laursen T et al (2006) Incidence of GH deficiency: a nationwide study. Eur J Endocrinol 155:61–71. https://doi.org/10.1530/eje.1.02191
Erfurth EM, Bulow B, Mikoczy Z, Hagmar L (2000) Low cancer incidence in patients with hypopituitarism and unsubstituted GH deficiency. Toronto, p Abst. #2037
Shevah O, Laron Z (2007) Patients with congenital deficiency of IGF-I seem protected from the development of malignancies: a preliminary report. Growth Horm IGF Res 17:54–57. https://doi.org/10.1016/j.ghir.2006.10.007
Pappachan JM, Raskauskiene D, Kutty VR, Clayton RN (2015) Excess mortality associated with hypopituitarism in adults: a meta-analysis of observational studies. J Clin Endocrinol Metab 100:1405–1411. https://doi.org/10.1210/jc.2014-3787
Jasim S, Alahdab F, Ahmed AT et al (2017) Mortality in adults with hypopituitarism: a systematic review and meta-analysis. Endocrine 56:33–42. https://doi.org/10.1007/s12020-016-1159-3
Gaillard RC, Mattsson AF, Akerblad A-C et al (2012) Overall and cause-specific mortality in GH-deficient adults on GH replacement. Eur J Endocrinol 166:1069–1077. https://doi.org/10.1530/EJE-11-1028
Ehrnborg C, Ellegård L, Bosaeus I et al (2005) Supraphysiological growth hormone: less fat, more extracellular fluid but uncertain effects on muscles in healthy, active young adults. Clin Endocrinol (Oxf) 62:449–457. https://doi.org/10.1111/j.1365-2265.2005.02240.x
Götherström G, Elbornsson M, Stibrant-Sunnerhagen K et al (2009) Ten years of growth hormone (GH) replacement normalizes muscle strength in GH-deficient adults. J Clin Endocrinol Metab 94:809–816. https://doi.org/10.1210/jc.2008-1538
Woodhouse LJ, Mukherjee A, Shalet SM, Ezzat S (2006) The influence of growth hormone status on physical impairments, functional limitations, and health-related quality of life in adults. Endocr Rev 27:287–317. https://doi.org/10.1210/er.2004-0022
Filipsson Nyström H, Barbosa EJL, Nilsson AG et al (2012) Discontinuing long-term GH replacement therapy: a randomized, placebo-controlled crossover trial in adult GH deficiency. J Clin Endocrinol Metab 97:3185–3195. https://doi.org/10.1210/jc.2012-2006
Hoffman AR, Kuntze JE, Baptista J et al (2004) Growth hormone (GH) replacement therapy in adult-onset gh deficiency: effects on body composition in men and women in a double-blind, randomized, placebo-controlled trial. J Clin Endocrinol Metab 89:2048–2056. https://doi.org/10.1210/jc.2003-030346
Newman CB, Frisch KA, Rosenzweig B et al (2011) Moderate doses of hGH (0.64 mg/d) improve lipids but not cardiovascular function in GH-deficient adults with normal baseline cardiac function. J Clin Endocrinol Metab 96:122–132. https://doi.org/10.1210/jc.2010-1204
Chikani V, Cuneo RC, Hickman I, Ho KKY (2015) Impairment of anaerobic capacity in adults with growth hormone deficiency. J Clin Endocrinol Metab 100:1811–1818. https://doi.org/10.1210/jc.2015-1006
Chikani V, Cuneo RC, Hickman I, Ho KKY (2016) Growth hormone (GH) enhances anaerobic capacity: impact on physical function and quality of life in adults with GH deficiency. Clin Endocrinol (Oxf) 85:660–668. https://doi.org/10.1111/cen.13147
Mauras N, Pescovitz OH, Allada V et al (2005) Limited efficacy of growth hormone (GH) during transition of GH-deficient patients from adolescence to adulthood: a phase III multicenter, double-blind, randomized two-year trial. J Clin Endocrinol Metab 90:3946–3955. https://doi.org/10.1210/jc.2005-0208
Christ ER, Cummings MH, Westwood NB et al (1997) The importance of growth hormone in the regulation of erythropoiesis, red cell mass, and plasma volume in adults with growth hormone deficiency. J Clin Endocrinol Metab 82:2985–2990. https://doi.org/10.1210/jcem.82.9.4199
Caidahl K, Edén S, Bengtsson BA (1994) Cardiovascular and renal effects of growth hormone. Clin Endocrinol (Oxf) 40:393–400. https://doi.org/10.1111/j.1365-2265.1994.tb03937.x
Valcavi R, Gaddi O, Zini M et al (1995) Cardiac performance and mass in adults with hypopituitarism: effects of one year of growth hormone treatment. J Clin Endocrinol Metab 80:659–666. https://doi.org/10.1210/jcem.80.2.7852533
Böger RH, Skamira C, Bode-Böger SM et al (1996) Nitric oxide may mediate the hemodynamic effects of recombinant growth hormone in patients with acquired growth hormone deficiency. A double-blind, placebo-controlled study. J Clin Investig 98:2706–2713. https://doi.org/10.1172/JCI119095
Elbornsson M, Götherström G, Bosæus I et al (2013) Fifteen years of GH replacement improves body composition and cardiovascular risk factors. Eur J Endocrinol 168:745–753. https://doi.org/10.1530/EJE-12-1083
Appelman-Dijkstra NM, Claessen KMJA, Roelfsema F et al (2013) Long-term effects of recombinant human GH replacement in adults with GH deficiency: a systematic review. Eur J Endocrinol 169:R1–R14. https://doi.org/10.1530/EJE-12-1088
Maison P, Griffin S, Nicoue-Beglah M et al (2004) Impact of growth hormone (GH) treatment on cardiovascular risk factors in GH-deficient adults: a metaanalysis of blinded, randomized, placebo-controlled trials. J Clin Endocrinol Metab 89:2192–2199. https://doi.org/10.1210/jc.2003-030840
Gazzaruso C, Gola M, Karamouzis I et al (2014) Cardiovascular risk in adult patients with growth hormone (GH) deficiency and following substitution with GH: an update. J Clin Endocrinol Metab 99:18–29. https://doi.org/10.1210/jc.2013-2394
Sesmilo G, Biller BM, Llevadot J et al (2000) Effects of growth hormone administration on inflammatory and other cardiovascular risk markers in men with growth hormone deficiency. A randomized, controlled clinical trial. Ann Intern Med 133:111–122
Gruson D, Alexopoulou O, Pasquet A et al (2012) Impact of growth hormone (GH) treatment on circulating Nt-proBNP concentrations and on cardiac function in adult GH-deficient patients. Scand J Clin Lab Investig 72:387–394. https://doi.org/10.3109/00365513.2012.685887
Castillo AR, Zantut-Wittmann DE, Neto AM et al (2018) Panhypopituitarism without GH replacement: about insulin sensitivity, CRP levels, and metabolic syndrome. Horm Metab Res Horm Stoffwechselforschung Horm Metab 50:690–695. https://doi.org/10.1055/a-0649-8010
Monson JP, Jönsson P, Koltowska-Häggström M, Kourides I (2007) Growth hormone (GH) replacement decreases serum total and LDL-cholesterol in hypopituitary patients on maintenance HMG CoA reductase inhibitor (statin) therapy. Clin Endocrinol (Oxf) 67:623–628. https://doi.org/10.1111/j.1365-2265.2007.02935.x
Rosenfalck AM, Maghsoudi S, Fisker S et al (2000) The effect of 30 months of low-dose replacement therapy with recombinant human growth hormone (rhGH) on insulin and C-peptide kinetics, insulin secretion, insulin sensitivity, glucose effectiveness, and body composition in GH-deficient adults. J Clin Endocrinol Metab 85:4173–4181. https://doi.org/10.1210/jcem.85.11.6930
Svensson J, Fowelin J, Landin K et al (2002) Effects of seven years of GH-replacement therapy on insulin sensitivity in GH-deficient adults. J Clin Endocrinol Metab 87:2121–2127. https://doi.org/10.1210/jcem.87.5.8482
Attanasio AF, Jung H, Mo D et al (2011) Prevalence and incidence of diabetes mellitus in adult patients on growth hormone replacement for growth hormone deficiency: a surveillance database analysis. J Clin Endocrinol Metab 96:2255–2261. https://doi.org/10.1210/jc.2011-0448
Luger A, Mattsson AF, Koltowska-Häggström M et al (2012) Incidence of diabetes mellitus and evolution of glucose parameters in growth hormone-deficient subjects during growth hormone replacement therapy: a long-term observational study. Diabetes Care 35:57–62. https://doi.org/10.2337/dc11-0449
Woodmansee WW, Hartman ML, Lamberts SWJ et al (2010) Occurrence of impaired fasting glucose in GH-deficient adults receiving GH replacement compared with untreated subjects. Clin Endocrinol (Oxf) 72:59–69. https://doi.org/10.1111/j.1365-2265.2009.03612.x
Attanasio AF, Mo D, Erfurth EM et al (2010) Prevalence of metabolic syndrome in adult hypopituitary growth hormone (GH)-deficient patients before and after GH replacement. J Clin Endocrinol Metab 95:74–81. https://doi.org/10.1210/jc.2009-1326
van der Klaauw AA, Biermasz NR, Feskens EJM et al (2007) The prevalence of the metabolic syndrome is increased in patients with GH deficiency, irrespective of long-term substitution with recombinant human GH. Eur J Endocrinol 156:455–462. https://doi.org/10.1530/EJE-06-0699
Stewart PM, Toogood AA, Tomlinson JW (2001) Growth hormone, insulin-like growth factor-I and the cortisol-cortisone shuttle. Horm Res 56(Suppl 1):1–6. https://doi.org/10.1159/000048126
Filipsson H, Monson JP, Koltowska-Häggström M et al (2006) The impact of glucocorticoid replacement regimens on metabolic outcome and comorbidity in hypopituitary patients. J Clin Endocrinol Metab 91:3954–3961. https://doi.org/10.1210/jc.2006-0524
Swords FM, Carroll PV, Kisalu J et al (2003) The effects of growth hormone deficiency and replacement on glucocorticoid exposure in hypopituitary patients on cortisone acetate and hydrocortisone replacement. Clin Endocrinol (Oxf) 59:613–620
Danilowicz K, Bruno OD, Manavela M et al (2008) Correction of cortisol overreplacement ameliorates morbidities in patients with hypopituitarism: a pilot study. Pituitary 11:279–285. https://doi.org/10.1007/s11102-008-0126-2
Egger A, Buehler T, Boesch C et al (2011) The effect of GH replacement therapy on different fat compartments: a whole-body magnetic resonance imaging study. Eur J Endocrinol 164:23–29. https://doi.org/10.1530/EJE-10-0702
Ohlsson C, Bengtsson BA, Isaksson OG et al (1998) Growth hormone and bone. Endocr Rev 19:55–79. https://doi.org/10.1210/edrv.19.1.0324
Biller BM, Sesmilo G, Baum HB et al (2000) Withdrawal of long-term physiological growth hormone (GH) administration: differential effects on bone density and body composition in men with adult-onset GH deficiency. J Clin Endocrinol Metab 85:970–976. https://doi.org/10.1210/jcem.85.3.6474
Barake M, Klibanski A, Tritos NA (2014) Effects of recombinant human growth hormone therapy on bone mineral density in adults with growth hormone deficiency: a meta-analysis. J Clin Endocrinol Metab 99:852–860. https://doi.org/10.1210/jc.2013-3921
Elbornsson M, Götherström G, Bosæus I et al (2012) Fifteen years of GH replacement increases bone mineral density in hypopituitary patients with adult-onset GH deficiency. Eur J Endocrinol 166:787–795. https://doi.org/10.1530/EJE-11-1072
Mo D, Fleseriu M, Qi R et al (2015) Fracture risk in adult patients treated with growth hormone replacement therapy for growth hormone deficiency: a prospective observational cohort study. Lancet Diabetes Endocrinol 3:331–338. https://doi.org/10.1016/S2213-8587(15)00098-4
Biermasz NR, Hamdy NAT, Pereira AM et al (2004) Long-term skeletal effects of recombinant human growth hormone (rhGH) alone and rhGH combined with alendronate in GH-deficient adults: a seven-year follow-up study. Clin Endocrinol (Oxf) 60:568–575. https://doi.org/10.1111/j.1365-2265.2004.02021.x
Biermasz NR, Hamdy NA, Janssen YJ, Roelfsema F (2001) Additional beneficial effects of alendronate in growth hormone (GH)-deficient adults with osteoporosis receiving long-term recombinant human GH replacement therapy: a randomized controlled trial. J Clin Endocrinol Metab 86:3079–3085. https://doi.org/10.1210/jcem.86.7.7669
Tritos NA, Greenspan SL, King D et al (2011) Unreplaced sex steroid deficiency, corticotropin deficiency, and lower IGF-I are associated with lower bone mineral density in adults with growth hormone deficiency: a KIMS database analysis. J Clin Endocrinol Metab 96:1516–1523. https://doi.org/10.1210/jc.2010-2662
Wüster C, Abs R, Bengtsson BA et al (2001) The influence of growth hormone deficiency, growth hormone replacement therapy, and other aspects of hypopituitarism on fracture rate and bone mineral density. J Bone Miner Res 16:398–405. https://doi.org/10.1359/jbmr.2001.16.2.398
Murray RD, Columb B, Adams JE, Shalet SM (2004) Low bone mass is an infrequent feature of the adult growth hormone deficiency syndrome in middle-age adults and the elderly. J Clin Endocrinol Metab 89:1124–1130. https://doi.org/10.1210/jc.2003-030685
Toogood AA, Adams JE, O’Neill PA, Shalet SM (1997) Elderly patients with adult-onset growth hormone deficiency are not osteopenic. J Clin Endocrinol Metab 82:1462–1466. https://doi.org/10.1210/jcem.82.5.3932
Murray RD, Adams JE, Shalet SM (2006) A densitometric and morphometric analysis of the skeleton in adults with varying degrees of growth hormone deficiency. J Clin Endocrinol Metab 91:432–438. https://doi.org/10.1210/jc.2005-0897
Högler W, Shaw N (2010) Childhood growth hormone deficiency, bone density, structures and fractures: scrutinizing the evidence. Clin Endocrinol (Oxf) 72:281–289. https://doi.org/10.1111/j.1365-2265.2009.03686.x
Bouillon R, Koledova E, Bezlepkina O et al (2004) Bone status and fracture prevalence in Russian adults with childhood-onset growth hormone deficiency. J Clin Endocrinol Metab 89:4993–4998. https://doi.org/10.1210/jc.2004-0054
Mazziotti G, Mormando M, Cristiano A et al (2014) Association between l-thyroxine treatment, GH deficiency, and radiological vertebral fractures in patients with adult-onset hypopituitarism. Eur J Endocrinol 170:893–899. https://doi.org/10.1530/EJE-14-0097
Mazziotti G, Porcelli T, Bianchi A et al (2010) Glucocorticoid replacement therapy and vertebral fractures in hypopituitary adult males with GH deficiency. Eur J Endocrinol 163:15–20. https://doi.org/10.1530/EJE-10-0125
Mo D, Blum WF, Rosilio M et al (2014) Ten-year change in quality of life in adults on growth hormone replacement for growth hormone deficiency: an analysis of the hypopituitary control and complications study. J Clin Endocrinol Metab 99:4581–4588. https://doi.org/10.1210/jc.2014-2892
Elbornsson M, Horvath A, Götherström G et al (2017) Seven years of growth hormone (GH) replacement improves quality of life in hypopituitary patients with adult-onset GH deficiency. Eur J Endocrinol 176:99–109. https://doi.org/10.1530/EJE-16-0875
Holdaway IM, Hunt P, Manning P et al (2015) Three-year experience with access to nationally funded growth hormone (GH) replacement for GH-deficient adults. Clin Endocrinol (Oxf) 83:85–90. https://doi.org/10.1111/cen.12691
Barkan AL (2001) The “quality of life-assessment of growth hormone deficiency in adults” questionnaire: can it be used to assess quality of life in hypopituitarism? J Clin Endocrinol Metab 86:1905–1907. https://doi.org/10.1210/jcem.86.5.7443
Barbosa JAR, Salvatori R, Oliveira CRP et al (2009) Quality of life in congenital, untreated, lifetime isolated growth hormone deficiency. Psychoneuroendocrinology 34:894–900. https://doi.org/10.1016/j.psyneuen.2009.01.001
Sandberg DE, MacGillivray MH, Clopper RR et al (1998) Quality of life among formerly treated childhood-onset growth hormone-deficient adults: a comparison with unaffected siblings. J Clin Endocrinol Metab 83:1134–1142. https://doi.org/10.1210/jcem.83.4.4712
Sommer G, Gianinazzi ME, Kuonen R et al (2015) Health-Related Quality of Life of Young Adults Treated with Recombinant Human Growth Hormone during Childhood. PLoS ONE 10:e0140944. https://doi.org/10.1371/journal.pone.0140944
Lynch S, Merson S, Beshyah SA et al (1994) Psychiatric morbidity in adults with hypopituitarism. J R Soc Med 87:445–447
Li Voon Chong JSW, Groves T, Foy P et al (2002) Elderly people with hypothalamic-pituitary disease and untreated GH deficiency: clinical outcome, body composition, lipid profiles and quality of life after 2 years compared to controls. Clin Endocrinol (Oxf) 56:175–181
Arwert LI, Deijen JB, Witlox J, Drent ML (2005) The influence of growth hormone (GH) substitution on patient-reported outcomes and cognitive functions in GH-deficient patients: a meta-analysis. Growth Horm IGF Res 15:47–54. https://doi.org/10.1016/j.ghir.2004.11.004
Saller B, Mattsson AF, Kann PH et al (2006) Healthcare utilization, quality of life and patient-reported outcomes during two years of GH replacement therapy in GH-deficient adults: comparison between Sweden, The Netherlands and Germany. Eur J Endocrinol 154:843–850. https://doi.org/10.1530/eje.1.02149
Underwood LE, Attie KM, Baptista J, Genentech Collaborative Study Group (2003) Growth hormone (GH) dose-response in young adults with childhood-onset GH deficiency: a two-year, multicenter, multiple-dose, placebo-controlled study. J Clin Endocrinol Metab 88:5273–5280. https://doi.org/10.1210/jc.2003-030204
Burman P, Broman JE, Hetta J et al (1995) Quality of life in adults with growth hormone (GH) deficiency: response to treatment with recombinant human GH in a placebo-controlled 21-month trial. J Clin Endocrinol Metab 80:3585–3590. https://doi.org/10.1210/jcem.80.12.8530603
Beshyah SA, Freemantle C, Shahi M et al (1995) Replacement treatment with biosynthetic human growth hormone in growth hormone-deficient hypopituitary adults. Clin Endocrinol (Oxf) 42:73–84
Wallymahmed ME, Foy P, Shaw D et al (1997) Quality of life, body composition and muscle strength in adult growth hormone deficiency: the influence of growth hormone replacement therapy for up to 3 years. Clin Endocrinol (Oxf) 47:439–446
Cuneo RC, Judd S, Wallace JD et al (1998) The Australian multicenter trial of growth hormone (GH) treatment in GH-deficient adults. J Clin Endocrinol Metab 83:107–116. https://doi.org/10.1210/jcem.83.1.4482
Miller KK, Wexler T, Fazeli P et al (2010) Growth hormone deficiency after treatment of acromegaly: a randomized, placebo-controlled study of growth hormone replacement. J Clin Endocrinol Metab 95:567–577. https://doi.org/10.1210/jc.2009-1611
van der Klaauw AA, Bax JJ, Roelfsema F et al (2009) Limited effects of growth hormone replacement in patients with GH deficiency during long-term cure of acromegaly. Pituitary 12:339–346. https://doi.org/10.1007/s11102-009-0186-y
Feldt-Rasmussen U, Abs R, Bengtsson B-A et al (2002) Growth hormone deficiency and replacement in hypopituitary patients previously treated for acromegaly or Cushing’s disease. Eur J Endocrinol 146:67–74. https://doi.org/10.1530/eje.0.1460067
Webb SM, Mo D, Lamberts SWJ et al (2010) Metabolic, cardiovascular, and cerebrovascular outcomes in growth hormone-deficient subjects with previous cushing’s disease or non-functioning pituitary adenoma. J Clin Endocrinol Metab 95:630–638. https://doi.org/10.1210/jc.2009-0806
Bleicken B, Hahner S, Loeffler M et al (2010) Influence of hydrocortisone dosage scheme on health-related quality of life in patients with adrenal insufficiency. Clin Endocrinol (Oxf) 72:297–304. https://doi.org/10.1111/j.1365-2265.2009.03596.x
Ajmal A, McKean E, Sullivan S, Barkan A (2018) Decreased quality of life (QoL) in hypopituitary patients: involvement of glucocorticoid replacement and radiation therapy. Pituitary 21:624–630. https://doi.org/10.1007/s11102-018-0918-y
Aguiar-Oliveira MH, Souza AHO, Oliveira CRP et al (2017) Mechanisms in endocrinology: the multiple facets of GHRH/GH/IGF-I axis: lessons from lifetime, untreated, isolated GH deficiency due to a GHRH receptor gene mutation. Eur J Endocrinol 177:R85–R97. https://doi.org/10.1530/EJE-16-1047
Andrade-Guimarães AL, Aguiar-Oliveira MH, Salvatori R et al (2019) Adult individuals with congenital, untreated, severe isolated growth hormone deficiency have satisfactory muscular function. Endocrine 63:112–119. https://doi.org/10.1007/s12020-018-1763-5
Epitácio-Pereira CC, Silva GMF, Salvatori R et al (2013) Isolated GH deficiency due to a GHRH receptor mutation causes hip joint problems and genu valgum, and reduces size but not density of trabecular and mixed bone. J Clin Endocrinol Metab 98:E1710–E1715. https://doi.org/10.1210/jc.2013-2349
Barreto-Filho JAS, Alcântara MRS, Salvatori R et al (2002) Familial isolated growth hormone deficiency is associated with increased systolic blood pressure, central obesity, and dyslipidemia. J Clin Endocrinol Metab 87:2018–2023. https://doi.org/10.1210/jcem.87.5.8474
Gleeson HK, Souza AHO, Gill MS et al (2002) Lipid profiles in untreated severe congenital isolated growth hormone deficiency through the lifespan. Clin Endocrinol (Oxf) 57:89–95
Oliveira JLM, Aguiar-Oliveira MH, D’Oliveira A et al (2007) Congenital growth hormone (GH) deficiency and atherosclerosis: effects of GH replacement in GH-naive adults. J Clin Endocrinol Metab 92:4664–4670. https://doi.org/10.1210/jc.2007-1636
Araujo VP, Aguiar-Oliveira MH, Oliveira JLM et al (2012) Arrest of atherosclerosis progression after interruption of GH replacement in adults with congenital isolated GH deficiency. Eur J Endocrinol 166:977–982. https://doi.org/10.1530/EJE-12-0062
Pfeifer M, Verhovec R, Zizek B et al (1999) Growth hormone (GH) treatment reverses early atherosclerotic changes in GH-deficient adults. J Clin Endocrinol Metab 84:453–457. https://doi.org/10.1210/jcem.84.2.5456
Jørgensen JOL, Juul A (2018) THERAPY OF ENDOCRINE DISEASE: growth hormone replacement therapy in adults: 30 years of personal clinical experience. Eur J Endocrinol 179(1):R47–R56. https://doi.org/10.1530/EJE-18-0306
Fleseriu M, Hashim IA, Karavitaki N et al (2016) Hormonal Replacement in hypopituitarism in adults: an endocrine society clinical practice guideline. J Clin Endocrinol Metab 101:3888–3921. https://doi.org/10.1210/jc.2016-2118
Evidence and interpretation | Human growth hormone (somatropin) in adults with growth hormone deficiency | Guidance | NICE. In: NICE Guid. https://www.nice.org.uk/guidance/ta64/chapter/4-Evidence-and-interpretation
Snyder PJ (2019) Growth hormone deficiency in adults: UpToDate. In: Date. https://www.uptodate.com/contents/growth-hormone-deficiency-in-adults?search=growth%20hormone%20deficiency%20in%20adults&source=search_result&selectedTitle=1~111&usage_type=default&display_rank=1
Melmed S (2019) Pathogenesis and diagnosis of growth hormone deficiency in adults. N Engl J Med 380:2551–2562. https://doi.org/10.1056/NEJMra1817346
Whitehead HM, Boreham C, McIlrath EM et al (1992) Growth hormone treatment of adults with growth hormone deficiency: results of a 13-month placebo controlled cross-over study. Clin Endocrinol (Oxf) 36:45–52
Bengtsson BA, Edén S, Lönn L et al (1993) Treatment of adults with growth hormone (GH) deficiency with recombinant human GH. J Clin Endocrinol Metab 76:309–317. https://doi.org/10.1210/jcem.76.2.8432773
Verhelst J, Abs R, Vandeweghe M et al (1997) Two years of replacement therapy in adults with growth hormone deficiency. Clin Endocrinol (Oxf) 47:485–494
Baum HB, Katznelson L, Sherman JC et al (1998) Effects of physiological growth hormone (GH) therapy on cognition and quality of life in patients with adult-onset GH deficiency. J Clin Endocrinol Metab 83:3184–3189. https://doi.org/10.1210/jcem.83.9.5112
Bollerslev J, Hallén J, Fougner KJ et al (2005) Low-dose GH improves exercise capacity in adults with GH deficiency: effects of a 22-month placebo-controlled, crossover trial. Eur J Endocrinol 153:379–387. https://doi.org/10.1530/eje.1.01971
Chihara K, Kato Y, Kohno H et al (2006) Efficacy and safety of growth hormone (GH) in the treatment of adult Japanese patients with GH deficiency: a randomised, placebo-controlled study. Growth Horm IGF Res 16:132–142. https://doi.org/10.1016/j.ghir.2006.03.012
Urushihara H, Fukuhara S, Tai S et al (2007) Heterogeneity in responsiveness of perceived quality of life to body composition changes between adult- and childhood-onset Japanese hypopituitary adults with GH deficiency during GH replacement. Eur J Endocrinol 156:637–645. https://doi.org/10.1530/EJE-07-0016
Acknowledgements
The authors would like to thank Richard J. Auchus for his critical review of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Both authors report no conflict of interest. This study was not supported by any external sources.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
He, X., Barkan, A.L. Growth hormone therapy in adults with growth hormone deficiency: a critical assessment of the literature. Pituitary 23, 294–306 (2020). https://doi.org/10.1007/s11102-020-01031-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-020-01031-5