Abstract
Since 1997 there is an online National Registry of acromegalic patients in Spain (REA). We aimed to study changes in acromegaly treatment and outcomes over the last four decades in Spain. In REA clinical and biochemical data are collected at diagnosis and updated every one to 2 years. We analyzed the first treatment received and the different treatments administered according to decade of diagnosis of acromegaly: prior to 1980, 1980–1989, 1990–1999 and 2000–2009. Surgical cure rates according to pretreatment with long-acting somatostatin receptor ligands (SRLs) were also analyzed. 1,658 patients were included of which 698 had accurate follow-up data. Treatment of acromegaly changed over time. Surgery was the main treatment option (83.8 %) and medical treatment was widely used (74.7 %) both maintained over decades, while radiation therapy declined (62.8, 61.6, 42.2 and 11.9 % over decades, p < 0.001). First treatment type also changed: surgery was the first line option up until the last decade in which medical treatment was preferred (p < 0.001). Radiotherapy was barely used as first treatment. Treatment combinations changed over time (p < 0.001). The most common treatment combination (surgery plus medical therapy), was received by 24.4, 16.4, 25.3 and 56.5 % of patients over decades. Medical treatment alone was performed in 7.3, 6, 7.2 and 14.7 % over decades. Type of medical treatment also changed, SRLs becoming the first medical treatment modality in the last decades, whereas dopamine agonist use declined (p < 0.001). Surgical cure rates improved over decades (21, 21, 36 and 38 %, p = 0.002) and were not influenced by SRL pre-surgical use. Acromegaly treatment has changed in Spain in the last four decades. Surgery has been the main treatment option for decades; however, medical therapy has replaced surgery as first line in the last decade and radiotherapy rates have clearly declined. SRLs are the most used medical treatment.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Acromegaly is a rare disease of GH hypersecretion with an estimated incidence of 2.5 cases per million per year according to national Spanish data [1, 2]. Registries are a useful tool to investigate real-life management of rare diseases. Since 1997, the Spanish Society of Endocrinology and Nutrition (SEEN) supports a national acromegaly registry (Registro Español de Acromegalia or REA). The main objective of REA is to collect clinical and biochemical data as well as treatments and outcomes of acromegaly in Spain. Data entry is prospective and retrospective. Peak data entry was recorded between 1998 and 1999, and declined thereafter. In 2004 data on 1,219 patients were analyzed and results were published [2]. In 2007, the Neuroendocrine group of the SEEN, urged for new data entry, updating of previous patients and new data analysis. More than 400 new patients have been included in the last 3 years in REA.
Treatment of acromegaly has experienced important changes in the last 20 years basically due to the development of new medical options and advances in surgical techniques. Surgery, medical treatment and radiation therapy are the current available therapies. The main aim of this paper is to define trends in acromegaly treatment over the last four decades in Spain and to explore changes in surgical cure according to pre-surgical medical treatment. We have analyzed individual treatments and treatment combinations received by patients in REA according to decade of diagnosis of acromegaly. We have also analyzed surgical cure rates along decades and the influence of pre-surgical medical treatment.
Methods
REA is an online database in which all members of the SEEN are invited to voluntarily participate. Each physician involved has a personal password to enter the database and only has access to his/her patients. Data entry can be prospective and retrospective. Variables collected include: patient demographics, diagnosis (acromegaly, gigantism or ectopic growth hormone-releasing hormone secretion), estimated date of initial symptoms and date of diagnosis, pituitary imaging (tumor size and tumor extension), tumor persistence after surgery, visual fields, baseline GH, GH after an oral glucose tolerance test (OGTT) and IGF-1 concentrations. GH and IGF-1 measurements are performed in each center, and IGF-1 absolute value as well as normality or abnormality—according to local reference values-, are also recorded. Date of diagnosis and co-morbidities are included. Medical, surgical and radiation treatments are collected as well as dates when medical treatment is started and stopped. As a recommendation, variables should be entered at baseline and every one to 2 years during follow-up. Discontinuation of the study because of death or loss to follow-up is also recorded.
Accuracy of data entry is supervised by two simultaneous database managers: an endocrinologist and a webmaster. Both of them and the statistician, are the only people who have access to the complete database. Possible inconsistencies and missing data are identified and queries sent to the reporting investigators for completion of data.
Patients
All patients diagnosed with acromegaly followed up in Spain can be entered in the registry. In 1997 the aim was to collect all acromegalic patients in the nation to estimate epidemiological data. After 2004 the aim was to collect as many patients as possible and to have accurate follow-up data. Most tertiary referral centers over the country participated in the project. All patients gave informed consent to enter the study.
Statistical analysis
The current analysis was focused on treatments received by patients and surgical cure rates. Treatments are reported considering the patient’s decade of diagnosis, although treatments could have been administered in a different decade. We analyzed the first treatment received by all patients across different decades and we also studied the treatment combinations received by patients according to decade of diagnosis. First treatment received was analyzed in the whole cohort of patients (n = 1,658). However, use of all available therapies, treatment combinations, control of the disease as well as surgical cure were only analyzed in the 698 patients with complete data follow-up (at least one entry in the last 2 years) to avoid bias caused by incomplete follow-up data. Surgical outcomes according to pre-surgical use of SRLs (both for any duration and for more than 3 months), were analyzed only in patients diagnosed after 1997 when SRLs were available.
Data were analyzed using SAS 8.2 software on an SQL database. Descriptive statistics was used to give percents, means, medians and ranges. The Chi-square test was used to compare percentages and the Mann–Whitney U test was used to compare medians between different groups. Significance was accepted at p < 0.05.
Results
Up until January 2010, 1,658 patients had been included in the registry. Seven hundred and twenty seven had been updated; of those, 99 patients died and 29 were lost to follow-up. Six hundred and ninety eight patients were considered to be updated with accurate data follow-up according to predefined database aims and rules (data entry within 2 years of statistical analysis except for those who died). Baseline characteristics as well as first treatment received were studied in the whole cohort. All other analyses were performed in the 698 patients with complete follow-up data.
Patients
Of the 1,658 patients included in the database 61 % were women and 39 % men. Mean age at diagnosis was 45.5 years (interquartile range 35–55) and estimated time of symptoms before the diagnosis was 6 ± 6 years (Table 1). Mean follow-up since acromegaly diagnosis was 12 ± 9 years. According to decade of diagnosis, there were 146 patients diagnosed prior to 1980, 419 patients diagnosed between 1980 and 1989, 700 diagnosed in 1900–1999 and 331 diagnosed in 2000–2009; in 62 patients the date of diagnosis was missing.
Acromegaly was due to a pituitary adenoma in all cases, macroadenoma in 75 % of patients, microadenoma in 25 %. Mean tumor size was 17.2 mm (interquartile range 10–22 mm). Biochemical data at diagnosis are presented in Table 1.
Changes in first treatment over time
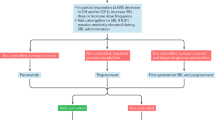
In the whole cohort the first treatment received was surgery in 895 patients (54 %), medical therapy in 702 (42.3 %), surgery + medical treatment simultaneously (received medical treatment within 1 month of surgery) in 22 (1.3 %) and radiation therapy in 15 patients (0.9 %), 1.4 % had missing data. Surgery was the first treatment received by 50, 66.5, 58.9 and 38.5 % of patients diagnosed over decades from prior to 1980 to 2000–2009 respectively. Medical treatment was given first line to 42.4, 31.3, 39.2 and 60.3 % of patients diagnosed over the four decades respectively. Medical and surgical treatment simultaneously in 1.4, 1.5, 1.4 and 1.2 % of patients over decades, while radiation was given as first line treatment to 6.2, 0.7, 0.4 and 0 % of patients diagnosed over decades. There was a significant change in the first treatment of acromegaly over time (p < 0.001) (Fig. 1).
Type of treatment over time: surgery, medical treatment and radiation therapy
Surgery was performed in 83.8 % patients overall. Over the decades: 62.8, 87.7, 88.4, and 81.1 % of patients diagnosed before 1980, in the 80s, 90s and 2000–2009 respectively (p < 0.001) had surgery for acromegaly. Medical treatment was prescribed to 74.7 % of patients (76.7, 73.9, 70.2 and 79 % respectively over decades). Globally, there were no changes in the percent of medical treatment use over time in patients according to decade of diagnosis of acromegaly (considering use or no use of medical therapy without details of which medications). Radiation therapy was administered to 36 % of patients, 62.8 % of patients diagnosed before 1980, 61.6, 42.2 and 11.9 % of patients diagnosed in the three following decades. Percent of patients receiving radiation therapy decreased over time (p < 0.001) (Fig. 2).
Treatment modalities over time and treatment combinations in individual patients
Treatment modalities and combination of treatments received did change over decades (p < 0.001) (Table 2). Surgery alone was performed in 2.4, 14.2, 24.4 and 16.4 % of patients diagnosed prior to 1980, the 80s, 90s and 2000–2009 respectively. Medical treatment alone was given to 7.3, 6, 7.2 and 15 % of patients over decades. Radiation treatment alone was performed in 12.2 % of patients diagnosed before 1980. After 1980, only one patient received radiation treatment as the only treatment modality in the eighty’s. The most common treatment combination (surgery plus medical therapy) was received by 24.4, 16.4, 25.3 and 56.5 % of patients over decades (in 35 % of the total cohort). The second most common treatment regime was surgery + medical treatment + radiation therapy (in 30 % of patients overall) and was given to 34.1, 50.7, 36.2 and 11.2 % of patients diagnosed over decades. Other treatment combinations are shown in Table 2.
Changes in first and all medical treatments received over time
For the whole cohort of patients (n = 1,658) first medical treatment was octreotide in 44 %, lanreotide in 30 %, dopamine agonists (including both bromocriptine and cabergoline) in 25 % and pegvisomant in 1 %.
Considering the 698 patients with complete data and referring treatment use to decade of patient diagnosis, dopamine agonists were used in 30.1 % of patients overall, in 67.4 % of patients diagnosed before 1980 and in 58.7, 30.2 and 11.9 % of patients diagnosed in the following 3 decades. There was a significant decrease in dopamine agonist use over time (p < 0.0001). SRLs (Octreotide and Lanreotide) were used by 63 % of patients overall: 48.8, 43.5, 64 and 76 % respectively in patients diagnosed over decades: from prior to 1980 to 2000–2009 (p < 0.001). Pegvisomant was used in 9.9 % of patients overall: 4.7, 8, 8 and 13.6 % of patients diagnosed before the 80′ and in the three following decades (Fig. 3). There were no differences in Pegvisomant use according to decade of diagnosis. However, Pegvisomant use was started in 2002 and was only used in the 2000–2009 decade (here we report treatments used related to decade of diagnosis of acromegaly).
Number of treatments received according to follow-up
Patients were followed for a mean of 13.5 (±9.4) years (n = 698 with follow-up data). A longer follow-up correlated with a greater number of treatments received (r = 0.23, p < 0.001).
Disease control and surgical cure
Control of acromegaly was defined as normal IGF-1 (reported as normal by the investigator or within the normal age-range) and was achieved in 76 % of patients (of 698 with data follow-up). Surgical cure was defined as patients with normal IGF-1 after surgical treatment who had not received any other surgical or radiation treatment and no medical treatment for more than 6 months after surgery, 32.3 % of patients were cured after first surgical treatment. Surgical cure rates clearly improved along decades (20.8, 21.1, 36.1 and 38.4 % respectively in the last four decades, p < 0.001). Pre-surgical treatment with SRLs in patients diagnosed after 1997, did not affect cure rates, whether if used at any time, or for at least 3 months.
Discussion
The present REA analysis shows how acromegaly treatment has changed over the last four decades in Spain. Surgery still remains the main treatment option (>80 % of patients) and medical therapy has also been widely used (75 % of patients). Even though rates of medical therapy have not significantly changed over time, type of medical treatment has clearly changed: SRLs have become the first option in the last decades, while dopamine agonists were the predominant option decades ago. We have also observed a change in the first treatment modality in the last decade, medical therapy being used more than surgery. Radiation therapy has experienced an important decline over time and has totally been disregarded as a first line treatment.
Important developments in acromegaly treatment have taken place in the last decades [3–13], particularly in the medical field [4–12]. In the surgical field, new surgical procedures such as computerized navigation, endoscopy, and intraoperative magnetic resonance imaging (MRI) have been implemented [13, 14]. Surgery still occupies the front line in the acromegaly treatment algorithm and, although surgical cure rates have improved over time in REA (36 and 38.4 % cure in the last two decades), the overall cure rate was poor (32.3 %), but similar to surgical cure rates in other European registries [15, 16]. Several drugs became available over the last 20 years in Spain: in 1995, subcutaneous octreotide was marketed, in 1997 lanreotide was launched [5], 1 year later, octreotide-LAR became available and Lanreotide autogel was approved in 2002 [7–9]. According to REA, long acting SRLs have displaced dopamine agonists in acromegaly treatment. Dopamine agonists were the most common medical treatment option for patients diagnosed up to 1990 (they were used in 67 and 50 % of patients diagnosed before 1980 and during the 80s respectively). After that time, SRLs have been the most frequent medical choice (used in 76 % of patients diagnosed in the last decade), whereas dopamine agonist use has fallen to a 30 and 12 % respectively in patients diagnosed in the last two decades after SRL’s became available. The poor surgical outcome has probably influenced the high rate of medical treatment use.
Another important conclusion of this analysis is the high rate of presurgical medical treatment. According to first treatment received, overall, 42 % of patients received medical treatment prior to surgery; however, in the last decade (2000–2009) 60 % of patients received medical treatment first as opposed to 38.5 % who underwent surgery first. This is a substantial increase with respect to the three prior decades in which primary medical treatment was used in 30–40 % of patients as opposed to surgery in 50–66 %. Presurgical medical treatment with SRLs has been particularly suggested for macroadenomas with low probability of surgical cure. Medical treatment may also be a useful tool while waiting for surgery in centers with a neurosurgical waiting list. Some studies indicate that pretreatment with a SRL can improve surgical cure rates [17], whereas others have found no benefits of pretreatment [18]. In REA, presurgical treatment with SRLs did not improve surgical cure rates. As seen in most acromegaly series, 75 % of patients in REA have macroadenomas [15, 19, 20] usually with a poorer surgical outcome. Costs of presurgical treatment with SRLs have been analyzed by others indicating that presurgical use of SRLs increases treatment costs by 30 % [21].
In REA 9.7 % of patients overall received medical treatment as the only therapy and this rate changed over time from 7.3 % in patients diagnosed prior to 1980 to 15 % in the last decade, indicating that despite all advances in the medical field, acromegaly is still far from being a medically treated condition.
Pegvisomant was launched in the Spanish market in 2004 [4]. Pegvisomant alone or in combination with SRLs has allowed control of the disease in previously uncontrolled patients and has contributed to change treatment algorithms, especially regarding the place of radiation therapy [3, 22, 23]. The present analysis confirms that radiation therapy rates have decreased over time and radiation is not a first line treatment in acromegaly and hasn’t been in the last three decades. Pegvisomant is not a first line medical option either; Pegvisomant use in patients diagnosed prior to 1980, in the 80s and in the 90s (in 4.7, 8 and 8 %), suggest that a percentage of patients who had been diagnosed many years before, despite the treatments available, were still not controlled in the last decade. Pegvisomant use remains low behind SRLs and dopamine agonists as it corresponds to a second line treatment.
The preferred treatment combination was surgery + medical therapy (35 % overall), and the second most common was surgery + medical therapy + radiation (30 % overall). This was particularly different in the last decade in which 56 % of patients received surgery + medical therapy versus 11 % who received surgery + medical + radiation therapy, indicating the decline in radiation therapy use.
With respect to patients characteristics, REA shows similarities with other registries [15, 19, 20]: mean time of symptoms prior to diagnosis 6 years; a higher proportion of females with respect to males (61 to 39 %) maintained since the last analysis in 2004 [2]. Other European registries show a higher proportion of females although not to this extent (German registry 54 % women [19], French registry male to female ratio of 0.8 [20], Belgian registry 51 % males [15]). Age at diagnosis is in the same range as other registries, in the mid-forties [15, 19, 20].
This study has several limitations, which include that REA is a registry that was designed in 1996, and much has been learnt since this early experience so that recent registries are much improved. Data collection as in all registries was incomplete. Number of biochemical updates entered per patients and missing data varied among centers and investigators. Moreover, due to its design, some questions like specific use of the different drugs in each decade, could not be adequately analyzed.
In conclusion, REA shows that changes in acromegaly treatment in Spain in the last four decades follow the expected direction. Surgery is the most used treatment modality but in the last decade more patients have received medical treatment as first line, radiotherapy rates have clearly declined. SRLs have displaced dopamine agonists in acromegaly treatment over decades and they are very frequently used. Despite the high use of drugs available, primary medical therapy without other treatment modalities has only been used in 15 % of patients in the last decade. Surgical cure rates were low but improved in the last two decades.
References
Etxabe J, Gaztambide S, Latorre P, Vazquez JA (1993) Acromegaly: an epidemiological study. J Endocrinol Invest 16:181–187
Mestron A, Webb SM, Astorga R, Benito P, Catala M, Gaztambide S, Gomez JM, Halperin I, Lucas-Morante T, Moreno B, Obiols G, de Pablos P, Paramo C, Pico A, Torres E, Varela C, Vazquez JA, Zamora J, Albareda M, Gilabert M (2004) Epidemiology, clinical characteristics, outcome, morbidity and mortality in acromegaly based on the Spanish Acromegaly Registry (Registro Espanol de Acromegalia, REA). Eur J Endocrinol 151:439–446
Melmed S, Colao A, Barkan A, Molitch M, Grossman AB, Kleinberg D, Clemmons D, Chanson P, Laws E, Schlechte J, Vance ML, Ho K, Giustina A (2009) Guidelines for acromegaly management: an Update. J Clin Endocrinol Metab 94:1509–1517
Trainer PJ, Drake WM, Katznelson L, Freda PU, Herman-Bonert V, van der Lely AJ, Dimaraki EV, Stewart PM, Friend KE, Vance ML, Besser GM, Scarlett JA, Thorner MO, Parkinson C, Klibanski A, Powell JS, Barkan AL, Sheppard MC, Malsonado M, Rose DR, Clemmons DR, Johannsson G, Bengtsson BA, Stavrou S, Kleinberg DL, Cook DM, Phillips LS, Bidlingmaier M, Strasburger CJ, Hackett S, Zib K, Bennett WF (2000) Davis RJ.T reatment of acromegaly with the growth hormone-receptor antagonist pegvisomant. N Engl J Med 342:1171–1177
Johnson MR, Chowdrey HS, Thomas F, Grint C, Lightman SL (1994) Pharmacokinetics and efficacy of the long-acting somatostatin analogue somatuline in acromegaly. Eur J Endocrinol 130:229–234
Hunter SJ, Shaw JA, Lee KO, Wood PJ, Atkinson AB, Bevan JS (1999) Comparison of monthly intramuscular injections of Sandostatin LAR with multiple subcutaneous injections of octreotide in the treatment of acromegaly; effects on growth hormone and other markers of growth hormone secretion. Clin Endocrinol 50:245–251
Caron P, Bex M, Cullen DR, Feldt-Rasmussen U, Pico Alfonso AM, Pynka S, Racz K, Schopohl J, Tabarin A, Valimaki MJ (2004) One-year follow-up of patients with acromegaly treated with fixed or titrated doses of lanreotide Autogel. Clin Endocrinol 60:734–740
Lucas T, Spanish-Portuguese Multicentre Autogel Study Group on Acromegaly (2006) Efficacy of lanreotide Autogel administered every 4–8 weeks in patients with acromegaly previously responsive to lanreotide microparticles 30 mg: a phase III trial. Clin Endocrinol (Oxf) 65(3):320–326
Schopohl J, Strasburger CJ, Caird D, Badenhoop K, Beuschlein F, Droste M, Plöckinger U, German Lanreotide Study Group (2011) Efficacy and acceptability of lanreotide Autogel® 120 mg at different dose intervals in patients with acromegaly previously treated with octreotide LAR. Exp Clin Endocrinol Diabetes 119(3):156–162
Biermasz NR, van den Oever NC, Frölich M, Arias AM, Smit JW, Romijn JA, Roelfsema F (2003) Sandostatin LAR in acromegaly: a 6-week injection interval suppresses GH secretion as effectively as a 4-week interval. Clin Endocrinol (Oxf) 58:288–295
Giustina A, Bonadonna S, Bugari G, Colao A, Cozzi R, Cannavo S, de Marinis L (2009) Degli Uberti E, Bogazzi F, Mazziotti G, Minuto F, Montini M, Ghigo E. High-dose intramuscular octreotide in patients with acromegaly inadequately controlled on conventional somatostatin analogue therapy: a randomised controlled trial. Eur J Endocrinol 161:331–338
Ben-Shlomo A, Melmed S (2007) Pasireotide—a somatostatin analog for the potential treatment of acromegaly, neuroendocrine tumors and Cushing’s disease. IDrugs 10:885–895
Frank G, Pasquini E (2006) Endoscopic cavernous sinus surgery with special reference to pituitary adenomas. In: Laws ER, Sheehan JP (eds) Pituitary surgery—a modern approach. Karger, Basel, pp 64–82
Fahlbusch R, Keller B, Ganslandt O, Kreutzer J, Nimsky C (2005) Transsphenoidal surgery in acromegaly investigated by intraoperative high-field magnetic resonance imaging. Eur J Endocrinol 153:239–248
Bex M, Abs R, T’Sjoen G, Mockel J, Velkeniers B, Muermans K, Maiter D (2007) AcroBel—the Belgian registry on acromegaly: a survey of the ‘real-life’ outcome in 418 acromegalic subjects. Eur J Endocrinol 157(4):399–409
Jaquet P, Cortet-Rudelli Ch, Sassolas G, Morange-Ramos I, Chanson P, Brue T, Andrieu JM, Beckers A, Bertherat J, Borson-Chazot F, Brassier G, Caron P, Cogne M, Cottier JP, Delemer B, Dufour H, Enjalbert A, Figarella-Branger D, Gaillard R, Gueydan M, Jan M, Kuhn JM, Raingeard I, Regis J, Roger P, Rohmer V, Sadoul JL, Saveanu A, Tabarin A, Travers N, French Acromegly Registry (2003) Therapeutic strategies in somatotroph adenomas with extrasellar extension: role of the medical approach, a consensus study of the French Acromegaly Registry. Ann Endocrinol (Paris) 64(6):434–441
Colao A, Ferone D, Cappabianca P, del Basso De Caro ML, Marzullo P, Monticelli A, Alfieri A, Merola B, Cali A, de Divitiis E, Lombardi G (1997) Effect of octreotide pretreatment on surgical outcome in acromegaly. J Clin Endocrinol Metab 82:3308–3314
Losa M, Mortini P, Urbaz L, Ribotto P, Castrignano T, Giovanelli M (2006) Presurgical treatment with somatostatin analogs in patients with acromegaly: effects on the remission and complication rates. J Neurosurg 104:899–906
Petersenn S, Buchfelder M, Reincke M, Strasburger CM, Franz H, Lohmann R, Quabbe HJ, Participants of the German Acromegaly Register (2008) Results of surgical and somatostatin analog therapies and their combination in acromegaly: a retrospective analysis of the German acromegaly register. Eur J Endocrinol 159(5):525–532
Fieffe S, Morange I, Petrossians P, Chanson P, Rohmer V, Cortet C, Borson-Chazot F, Brue T, The French Acromegaly Registry (2011) Diabetes in acromegaly, prevalence, risk factors, and evolution: data from the French Acromegaly Registry. Eur J Endocrinol 164(6):877–884
Biermasz NR, Roelfsema F, Pereira AM, Romijn JA (2009) Cost-effectiveness of lanreotide autogel in treatment algorithms of acromegaly. Expert Rev Pharmacoecon Outcomes Res 9:223–234
Melmed S, Colao A, Barkan A, Molitch M, Grossman AB, Kleinberg D, Clemmons D, Chanson P, Laws E, Schlechte J, Vance ML, Ho K, Acromegaly Consensus Group (2009) Guidelines for acromegaly management: an update. J Clin Endocrinol Metab 94:1509–1517
Mullan K, Sanabria C, Abram WP, McConnell EM, Courtney HC, Hunter SJ, McCance DR, Leslie H, Sheridan B, Atkinson AB (2009) Long term effect of external pituitary irradiation on IGF1 levels in patients with acromegaly free of adjunctive treatment. Eur J Endocrinol 161:547–551
Acknowledgments
We thank Novartis Oncology Spain for an unrestricted grant to support the REA database.
Conflict of interest
There is no conflict of interest that could be perceived as prejudicing the impartiality of the research reported.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
Dr. Varela recently passed away.
List of REA investigators in alphabetical order: Victoria Alcázar Lázaro, Hospital Severo Ochoa, Madrid, Javier Aller Pardo, Hospital Puerta de Hierro, Madrid, Cristina Álvarez Escolà, Hospital Universitario la Paz, Madrid, Paula Álvarez Vazquez, Complejo Hospitalario de Ourense, Orense, Ignacio Bernabeu Morón, Hospital Clínico Universitario de Santiago, Santiago de Compostela, Carmen Bernal González, Hospital 12 de Octubre, Madrid, Concepción Blanco Carrera, Hospital Principe de Asturias, Madrid, Alejandro Cámara Balda, Hospital San Pedro, Logroño, Rosa Cámara Gómez, Hospital La Fe, Valencia, Emilia Cáncer Minchot, Hospital de Fuenlabrada, Madrid, Ignasi Castells Fust, Hospital de Granollers, Barcelona, Carlos Del Pozo Picó, Hospital Mutua de Terrassa, Terrassa, Juan José Díez Gómez, Hospital Universitario la Paz, Madrid, Alberto Díez Hernández, Hospital del Bierzo, Ponferrada, León, Carmen Fajardo Montañana, Hospital de la Ribera, Alzira, Lluis Forga Llenas, Hospital de Navarra, Navarra, Rogelio García Centeno, Hospital Gregorio Marañón, Madrid, Honorato García Fernández, Hospital Son Dureta, Mallorca, Manuel Gargallo Fernandez, Hospital Virgen de la Torre, Madrid, Sonia Gaztambide Sáenz, Hospital de Cruces, Barakaldo, Irene Halperin Rabinovich, Hospital Clínic, Barcelona, Juan Angel Hernández Bayo, Hospital de la Palma, Tenerife, Miguel Angel Jaunsolo Barranechea, Hospital Severo Ochoa, Madrid, Manuel Luque Ramírez, Hospital de la Princesa, Madrid, Camelia Martí Ippoliti, Hospital de Sant Pau, Barcelona, Miguel Ángel Martínez Olmos, Hospital Clínico Universitario de Santiago, Santiago de Compostela, Francisca Mas, Hospital de Manacor, Mallorca, Alberto Moreno Carazo, Complejo Hospitalario de Jaen, Jaén, Basilio Moreno Esteban, Hospital Gregorio Marañón, Madrid, Jesus Moreno Fernandez, La Mancha Centro Endocrinología y Nutrición Ciudad Real, Gabriel Obiols Alfonso, Hospital Vall d’Hebrón, Barcelona, Herminia Pascual Saura, Hospital Morales Meseguer, Murcia, Antonio Pico Alfonso, Hospital General Universitario, Alicante, Elena Riquelme, Centro médico intergral de Henares, Madrid Mª Pilar Ruiz-Valdepeñas Herrero, Hospital 12 de Octubre, Madrid, Isabel Salinas i Vert, Hospital Germans Trias i Pujol, Barcelona, MªConcepción Sanabria Pérez, Complejo Hospitalario Ciudad Real, Ciudad Real, Piedad Santiago Fernández, Hospital General de Jaén, Jaén, Alicia Serraclara Pla, Hospital 12 de Octubre, Madrid, Gemma Sesmilo León, Institut Universitari Dexeus, Barcelona, Alfonso Soto Moreno, Hospital Universitario Virgen del Rocío, Sevilla, Elena Torres Vela, Hospital Universitario San Cecilio, Granada, César Varela, Hospital Infanta Sofía, Madrid, Eva Venegas Moreno, Hospital Universitario Virgen del Rocío, Sevilla, Almudena Vicente Delgado, Hospital Virgen de la Salud, Toledo, Carles Villabona Artero, Hospital de Bellvitge, Barcelona, Susan M Webb, Hospital de Sant Pau, Barcelona.
Rights and permissions
About this article
Cite this article
Sesmilo, G., Gaztambide, S., Venegas, E. et al. Changes in acromegaly treatment over four decades in Spain: analysis of the Spanish Acromegaly Registry (REA). Pituitary 16, 115–121 (2013). https://doi.org/10.1007/s11102-012-0384-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-012-0384-x