Abstract
To determine whether peer-reviewed consensus statements have changed clinical practice, we surveyed acromegaly care in specialist centers across the globe, and determined the degree of adherence to published consensus guidelines on acromegaly management. Sixty-five acromegaly experts who participated in the 7th Acromegaly Consensus Workshop in March 2009 responded. Results indicated that the most common referring sources for acromegaly patients were other endocrinologists (in 26% of centers), neurosurgeons (25%) and primary care physicians (21%). In sixty-nine percent of patients, biochemical diagnoses were made by evaluating results of a combination of growth hormone (GH) nadir/basal GH and elevated insulin like growth factor-I (IGF-I) levels. In both Europe and the USA, neurosurgery was the treatment of choice for GH-secreting microadenomas and for macroadenomas with compromised visual function. The most widely used criteria for neurosurgical outcome assessment were combined measurements of IGF-I and GH levels after oral glucose tolerance test (OGTT) 3 months after surgery. Ninety-eight percent of respondents stated that primary treatment with somatostatin receptor ligands (SRLs) was indicated at least sometime during the management of acromegaly patients. In nearly all centers (96%), the use of pegvisomant monotherapy was restricted to patients who had failed to achieve biochemical control with SRL therapy. The observation that most centers followed consensus statement recommendations encourages the future utility of these workshops aimed to create uniform management standards for acromegaly.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Acromegaly is a rare disease caused by a growth hormone (GH)-secreting pituitary adenoma resulting in excess circulating levels of GH and insulin like growth factor-I (IGF-I) causing increased co-morbidities and mortality [1], The estimated disease prevalence is 40–70 cases per million with an annual incidence of 3–4 new cases per million [1, 2] or higher [3, 4]. A cross-sectional study in Belgium reported the prevalence of acromegaly to be 100–130 cases per million inhabitants [3], and a study conducted in Germany measuring IGF-I levels to screen for acromegaly found the calculated population prevalence to be 1034 cases per million [4].
During the natural course of acromegaly, considerable morbidity and mortality is caused by cardiovascular, respiratory and metabolic co-morbidities [5–8]. Approaches to acromegaly management are surgery and/or medical treatment, while radiation therapy is generally restricted to a small proportion of patients [9, 10]. Each treatment approach has distinct advantages and disadvantages, but optimal treatment should reduce morbidity and normalize life expectancy. Ten years ago, consensus-driven guidelines for diagnosis and optimal management of acromegaly were not available. This led to convening of the first Acromegaly Consensus Workshop in 1999, which was followed by subsequent meetings producing seven consensus documents guiding evidence-based diagnosis and management of acromegaly [9–15].
A major aim of the regular Acromegaly Consensus Workshops is to produce recommendations of best clinical practice among endocrinology, neurosurgery and radiotherapy specialists [11]. However, in the 10 years since the first consensus statement, it is not known if these publications have influenced clinical practice. Thus far, a single analytical evaluation was restricted to the published guidelines on acromegaly cardiovascular complications [16]. Here we report results of a survey aimed to compare clinical practice in specialist centers across the globe, and determine the degree of adherence to published consensus guidelines.
Methods
A questionnaire (Appendix) was developed to assess adherence of clinical practice to consensus statements on the management of acromegaly. Questions mirrored the content of these statements. Questionnaires were issued to participating centers by December 15 2008 and those returned by email before January 31 2009 were included in the analysis. The questionnaire was answered by 65 of 73 experts that participated in the 7th Acromegaly Consensus Group meeting held in March 2009.
Results
Responses
Responses were received from representatives of 16 US centers, 12 European countries including Belgium, The Czech Republic, Denmark, France, Italy, The Netherlands, Norway, Portugal, Spain, Sweden, Turkey and the UK, as well as Australia, New Zealand, Brazil, Canada, China, Israel and Mexico. Sixty-five (89%) completed questionnaires were returned by the designated deadline, and participants are listed in the Acknowledgments section.
Patients and participating centers
Eighty-four percent of participants reported managing more than 50 patients with acromegaly at the time of the survey, 11% managed 25–50 patients, 3% managed 10–24 patients, and 2% managed fewer than 10 patients. A higher proportion of physicians managed more than 50 patients in Europe and other countries (90%) than in the USA (69%). Most European respondents managed more than 5 new patients annually (33% diagnosed >10 patients/year; 41% diagnosed 5–10 patients/year), with higher diagnosis rates of new patients in the USA (63% diagnosed >10 patients/year; 31% diagnosed 5–10 patients/year).
The most frequent referring specialists reported were other endocrinologists (in 26% of centers), neurosurgeons (25%) and primary care physicians (21%). However, there were regional differences with 64% of patients in the USA being referred by a neurosurgeon compared to 25% of patients in Europe and other countries. Most acromegaly patient referrals in Europe originated with other endocrinologists (39%) or primary care physicians (32%).
Diagnosis and treatment
The survey revealed that 69% of respondents established the biochemical diagnosis of acromegaly using results of a combination of nadir/basal GH measurements and IGF-I levels. Thirteen percent relied solely on nadir GH levels during an oral glucose tolerance test (OGTT), and 18% used only elevated IGF-I levels as the biochemical criterion.
Tumor mass and anatomic characteristics were the main factors that determined choice of treatment (79% of respondents; Fig. 1a). The second most important factor determining treatment choice was the degree of GH and IGF-I elevation (41%). Other factors such as patient preference (30%) and cardiovascular function (14%) were second-choice factors for determining treatment choice (Fig. 1b). Collectively, tumor mass characteristics and increased GH and IGF-I levels were the main determinants of treatment choice.
In both Europe and the USA, transsphenoidal surgical resection was the treatment of choice for microadenomas (90% and 94%, respectively). However, 10% of European and 6% of USA respondents opted for somatostatin receptor ligands (SRLs) as the treatment of choice for microadenoma. For macroadenomas with visual compromise, neurosurgery was equivalently ranked as the treatment of choice in both Europe (92%) and the USA (94%), and SRL therapy accounted for the remainder of responses. Responses concerning treatment of macroadenomas without visual compromise were diverse, with 53% of respondents opting for neurosurgery as the treatment of choice and 42% preferring the use of SRLs. In the USA, neurosurgery was the predominant treatment of choice (81%), whereas in Europe either neurosurgery (45%) or treatment with SRLs (49%) was considered the preferred treatment for macroadenomas without visual compromise.
Among the 75% of respondents sometimes undertaking pre-surgical treatment with SRLs, multiple reasons were offered for this approach including: reducing anesthesia risk (35% of all responses); to attain pre-surgical biochemical control (24%); delay of surgical intervention (19%); patient preference (12%); and evidence-based practice (10%). Only 2% of respondents never used pre-surgical SRL treatment, and 23% always used pre-surgical SRL treatment.
When neurosurgery was considered as the treatment of choice, the selection was based largely on the level of surgical experience with pituitary surgery (42% of all responses). Availability of an expert neurosurgeon within the respondent’s respective center, published results, and patient preference were also important factors in making the decision to proceed with neurosurgery (21, 16 and 14%, respectively).
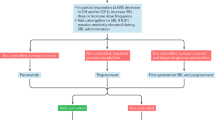
Ninety-eight percent of respondents stated that primary treatment with SRLs was indicated at least sometime in all acromegaly patients (Fig. 2a). Primary therapy with SRLs was favored in Europe and the rest of the world (2% always, 42% often, 54% sometimes) compared with the USA (19% often, 81% sometimes). The most frequent indication given for SRL primary therapy was the presence of a macroadenoma with lateral extension with or without cavernous sinus invasion (51% of all responses) (Fig. 2b).
Assessment of outcome
The most widely used method for assessment of post-operative outcome was a combined measurement of IGF-I and GH after OGTT at 3 months (35%; Fig. 3a). Among those who always relied on the same criteria to assess surgical outcome (39% of respondents), 84% used measurement of IGF-I and GH after OGTT at 3 months. SRL treatment outcomes were assessed mostly by combined IGF-I and GH measurements after 6 months (49%; Fig. 3b), and a further 15% undertook this assessment at 12 months. Most centers (61%) used a single method to evaluate the outcome of SRL treatment, and among these, 2 of 3 (67%) used combined IGF-I and GH measurements at 6 months to assess outcome.
Use of pegvisomant
Pegvisomant was used as monotherapy in 71% of the centers included in this survey. This practice was more frequent in the USA (94%) than in Europe and other countries (65%). In nearly all centers (96%), the use of pegvisomant monotherapy was restricted to patients who were not controlled by SRL therapy. No centers in Europe or the rest of the world used pegvisomant monotherapy as first-line treatment, but 13% of centers in the USA did employ this approach. Combination therapy with SRLs and pegvisomant was used in a large proportion of centers (81%) with a slightly higher prevalence in the USA (94%) than in Europe (76%). In most centers (93% USA, 97% Europe) combination therapy was used only after failed SRL therapy.
Discussion
Survey respondents included physicians who represented clinical specialties involved in the active management of patients with acromegaly, and represented centers of excellence in twelve European countries, sixteen US centers and seven countries outside of Europe and the USA. In general, despite the diversity of respondents and an uneven geographical distribution of participants, physicians included in this survey manage patients with acromegaly in a manner consistent with recent consensus statements [9–15]. Differences in patient management in the USA as compared with other countries related mainly to choice of primary medical therapy; SRL was used more frequently in Europe than in the USA, while pegvisomant was used only in the USA as first-line monotherapy.
Although clinical manifestations of acromegaly are well established, there is limited information relating to the type of medical professional who recognizes the syndrome and refers patients for specialist evaluation and management [17]. The results reported here regarding the most frequent referring specialist are interesting, with other endocrinologists, neurosurgeons and primary care physicians each accounting for about one quarter of referrals to specialist centers. There were clear global differences in referral patterns, with 64% of referrals in the USA being made by neurosurgeons compared with only 25% in Europe and the rest of the world. This was possibly due to patients in USA being referred because of the presence of a pituitary adenoma, while in Europe referrals are made due to the diagnosis of an acromegaly clinical syndrome. Alternatively, it can be hypothesized that US primary care physicians perform baseline endocrine screening tests and then refer the patient directly for surgery to the neurosurgeon bypassing an endocrinologist, while in Europe the diagnosis is more commonly made by specialist endocrinologists.
Despite acromegaly being a rare disease, most physicians included in this survey managed more than 50 patients and had at least five new patient referrals per year, reflecting the specialized nature of survey participants. Biochemical diagnoses of acromegaly were mainly made using a combination of GH nadir/basal GH and IGF-I measurements. These are appropriate, as elevated IGF-I levels and a failure to suppress GH during an OGTT confirm the diagnosis [14, 18]. In most cases, nadir GH levels of less than 1 μg/l preclude a diagnosis of acromegaly [11, 19]. However, up to 25% of cases may exhibit normal levels of GH but elevated IGF-I levels [19–21], and therefore, the notion that measuring both hormones is important, which is in line also with consensus statements [11, 14], was well accepted among respondents.
It is well recognized that transsphenoidal surgery is the treatment of choice for intrasellar microadenomas, non-invasive macroadenomas, and when the tumor causes local compression symptoms [10]. In this survey, most centers reported adherence to this principle, and tumor mass and characteristics were the main determinants for choice of treatment. However, in a few centers SRLs were used as first-line treatment in microadenomas and macroadenomas with visual compromise; a choice that is not in line with consensus guidelines [9, 10]. This probably reflects local situations (for example, unavailability of an expert neurosurgeon), patient preference and confidence in the emerging evidence of a shrinkage effect of SRLs [22]. In patients harboring macroadenomas without visual compromise, treatment with SRLs was more frequently practiced in Europe than in the USA, possibly due to a greater experience with the use of primary SRL treatments in European centers [22, 23]. Alternatively, it may be hypothesized that these regional differences (including the use of radiotherapy as primary treatment in some countries, which is not recommended in the consensus guidelines) may be influenced by differences in national health infrastructures and policies (even within Europe).
Expertise in surgical management of acromegaly is important and success rates are enhanced when surgery is performed by an experienced pituitary neurosurgeon [10, 24, 25]. This was a major determinant of treatment choice among those surveyed, and the respective surgeon’s experience strongly influenced management decisions. However, recent consensus statements recognise that first line SRL treatment is a viable alternative option to surgery in selected patients [10]. Nearly all respondents (98%) stated that primary SRL treatment prior to surgery was indicated at least sometimes for a variety of clinical indications. Such treatment was widely used at all centers, but was more frequently applied in Europe and the rest of the world compared with the USA. The most common indication for primary medical treatment was the presence of a macroadenoma with features indicative of unlikely surgical success (such as lateral extension), an approach consistent with recent consensus statements [10].
Numerous reports state that results of monitoring both GH and IGF-I levels are required to assess disease control [26–29]. Therefore, the survey included questions on methods employed to assess outcomes of surgery and of SRL treatment. Measurements of both hormones were used by most centers to assess post-operative outcome and SRL therapy. These findings are consistent with the consensus on criteria for cure of acromegaly which indicates that for patients receiving medical treatment with an SRL, IGF-I and GH measurements are required for assessment [14]. The timing of such measurements in the surveyed group (3 months post-surgery, 6–12 months after starting SRL therapy) are also broadly in line with the published guidelines [14].
Pegvisomant, a GH receptor antagonist, provides another medical treatment option for acromegaly [30]. Pegvisomant is highly effective in achieving clinical control of acromegaly following surgery, radiotherapy or medical treatment [31], and exhibits efficacy in patients who have not responded adequately to SRL treatment [32–34]. Co-administration of SRLs and pegvisomant was used in most centers surveyed here, but generally after failure of SRL therapy. However, primary pegvisomant treatment was used in the USA, and not elsewhere. This discrepancy may reflect the fact that pegvisomant is not approved for primary treatment in Europe. Recent guidelines for management of acromegaly recognize that pegvisomant and SRL combination therapy may be beneficial but point out that there are no studies directly comparing combination therapy and pegvisomant monotherapy [10].
This survey was limited to participants in the Acromegaly Consensus Group meeting in 2009, and the general adherence to consensus statements published from this group is perhaps expected. A wider survey of other centers globally could provide further valuable information. Nevertheless, this survey is the first to provide detailed information on everyday clinical practice of acromegaly specialists worldwide.
Despite clear treatment practice differences between the USA and other countries, the observation that many centers follow consensus statement recommendations is encouraging for future workshops aiming to create uniform evidence-based guidelines for diagnosing and managing acromegaly. The results indicate a high level of commitment to consensus guidelines, which will hopefully manifest in improvements in everyday lives of acromegaly patients.
References
Melmed S (2009) Acromegaly pathogenesis and treatment. J Clin Invest 119:3189–3202
Holdaway IM, Rajasoorya C (1999) Epidemiology of acromegaly. Pituitary 2:29–41
Daly AF, Rixhon M, Adam C, Dempegioti A, Tichomirowa MA, Beckers A (2006) High prevalence of pituitary adenomas: a cross-sectional study in the province of Liege, Belgium. J Clin Endocrinol Metab 91:4769–4775
Schneider HJ, Sievers C, Saller B, Wittchen HU, Stalla GK (2008) High prevalence of biochemical acromegaly in primary care patients with elevated IGF-1 levels. Clin Endocrinol (Oxf) 69:432–435
Holdaway IM, Rajasoorya RC, Gamble GD (2004) Factors influencing mortality in acromegaly. J Clin Endocrinol Metab 89:667–674
Maison P, Tropeano AI, Macquin-Mavier I, Giustina A, Chanson P (2007) Impact of somatostatin analogs on the heart in acromegaly: a metaanalysis. J Clin Endocrinol Metab 92:1743–1747
Davi MV, Dalle Carbonare L, Giustina A, Ferrari M, Frigo A, Lo Cascio V, Francia G (2008) Sleep apnoea syndrome is highly prevalent in acromegaly and only partially reversible after biochemical control of the disease. Eur J Endocrinol 159:533–540
Mazziotti G, Floriani I, Bonadonna S, Torri V, Chanson P, Giustina A (2009) Effects of somatostatin analogs on glucose homeostasis: a metaanalysis of acromegaly studies. J Clin Endocrinol Metab 94:1500–1508
Melmed S, Casanueva F, Cavagnini F, Chanson P, Frohman LA, Gaillard R, Ghigo E, Ho K, Jaquet P, Kleinberg D, Lamberts S, Laws E, Lombardi G, Sheppard MC, Thorner M, Vance ML, Wass JA, Giustina A (2005) Consensus statement: medical management of acromegaly. Eur J Endocrinol 153:737–740
Melmed S, Colao A, Barkan A, Molitch M, Grossman AB, Kleinberg D, Clemmons D, Chanson P, Laws E, Schlechte J, Vance ML, Ho K, Giustina A (2009) Guidelines for acromegaly management: an update. J Clin Endocrinol Metab 94:1509–1517
Giustina A, Barkan A, Casanueva FF, Cavagnini F, Frohman L, Ho K, Veldhuis J, Wass J, Von Werder K, Melmed S (2000) Criteria for cure of acromegaly: a consensus statement. J Clin Endocrinol Metab 85:526–529
Giustina A, Barkan A, Chanson P, Grossman A, Hoffman A, Ghigo E, Casanueva F, Colao A, Lamberts S, Sheppard M, Melmed S (2008) Guidelines for the treatment of growth hormone excess and growth hormone deficiency in adults. J Endocrinol Invest 31:820–838
Giustina A, Casanueva FF, Cavagnini F, Chanson P, Clemmons D, Frohman LA, Gaillard R, Ho K, Jaquet P, Kleinberg DL, Lamberts SW, Lombardi G, Sheppard M, Strasburger CJ, Vance ML, Wass JA, Melmed S (2003) Diagnosis and treatment of acromegaly complications. J Endocrinol Invest 26:1242–1247
Giustina A, Chanson P, Bronstein MD, Klibanski A, Lamberts S, Casanueva FF, Trainer P, Ghigo E, Ho K, Melmed S (2010) A consensus on criteria for cure of acromegaly. J Clin Endocrinol Metab 95:3141–3148
Melmed S, Casanueva FF, Cavagnini F, Chanson P, Frohman L, Grossman A, Ho K, Kleinberg D, Lamberts S, Laws E, Lombardi G, Vance ML, Werder KV, Wass J, Giustina A (2002) Guidelines for acromegaly management. J Clin Endocrinol Metab 87:4054–4058
Giustina A, Mancini T, Boscani PF, de Menis E, degli Uberti E, Ghigo E, Martino E, Minuto F, Colao A (2008) Assessment of the awareness and management of cardiovascular complications of acromegaly in Italy. The COM.E.T.A. (COMorbidities Evaluation and Treatment in Acromegaly) study. J Endocrinol Invest 31:731–738
Nachtigall L, Delgado A, Swearingen B, Lee H, Zerikly R, Klibanski A (2008) Changing patterns in diagnosis and therapy of acromegaly over two decades. J Clin Endocrinol Metab 93:2035–2041
Carmichael JD, Bonert VS, Mirocha JM, Melmed S (2009) The utility of oral glucose tolerance testing for diagnosis and assessment of treatment outcomes in 166 patients with acromegaly. J Clin Endocrinol Metab 94:523–527
Melmed S (2006) Medical progress: acromegaly. N Engl J Med 355:2558–2573
Dimaraki EV, Jaffe CA, DeMott-Friberg R, Chandler WF, Barkan AL (2002) Acromegaly with apparently normal GH secretion: implications for diagnosis and follow-up. J Clin Endocrinol Metab 87:3537–3542
Freda PU, Reyes CM, Nuruzzaman AT, Sundeen RE, Bruce JN (2003) Basal and glucose-suppressed GH levels less than 1 microg/l in newly diagnosed acromegaly. Pituitary 6:175–180
Amato G, Mazziotti G, Rotondi M, Iorio S, Doga M, Sorvillo F, Manganella G, Di Salle F, Giustina A, Carella C (2002) Long-term effects of lanreotide SR and octreotide LAR on tumour shrinkage and GH hypersecretion in patients with previously untreated acromegaly. Clin Endocrinol (Oxf) 56:65–71
Giustina A, Bonadonna S, Bugari G, Colao A, Cozzi R, Cannavo S, de Marinis L, Degli Uberti E, Bogazzi F, Mazziotti G, Minuto F, Montini M, Ghigo E (2009) High-dose intramuscular octreotide in patients with acromegaly inadequately controlled on conventional somatostatin analogue therapy: a randomised controlled trial. Eur J Endocrinol 161:331–338
Ahmed E, Stratton P, Adams W (1999) Outcome of transphenoidal surgery for acromegaly and its relationship to surgical experience. Clin Endocrinol (Oxf) 50:561–567
Bates PR, Carson MN, Trainer PJ, Wass JA (2008) Wide variation in surgical outcomes for acromegaly in the UK. Clin Endocrinol (Oxf) 68:136–142
Ayuk J, Clayton RN, Holder G, Sheppard MC, Stewart PM, Bates AS (2004) Growth hormone and pituitary radiotherapy, but not serum insulin-like growth factor-I concentrations, predict excess mortality in patients with acromegaly. J Clin Endocrinol Metab 89:1613–1617
Bianchi A, Giustina A, Cimino V, Pola R, Angelini F, Pontecorvi A, De Marinis L (2009) Influence of growth hormone receptor d3 and full-length isoforms on biochemical treatment outcomes in acromegaly. J Clin Endocrinol Metab 94:2015–2022
Kauppinen-Makelin R, Sane T, Reunanen A, Valimaki MJ, Niskanen L, Markkanen H, Loyttyniemi E, Ebeling T, Jaatinen P, Laine H, Nuutila P, Salmela P, Salmi J, Stenman UH, Viikari J, Voutilainen E (2005) A nationwide survey of mortality in acromegaly. J Clin Endocrinol Metab 90:4081–4086
Puder JJ, Nilavar S, Post KD, Freda PU (2005) Relationship between disease-related morbidity and biochemical markers of activity in patients with acromegaly. J Clin Endocrinol Metab 90:1972–1978
Colao A, Arnaldi G, Beck-Peccoz P, Cannavo S, Cozzi R, degli Uberti E, De Marinis L, De Menis E, Ferone D, Gasco V, Giustina A, Grottoli S, Lombardi G, Maffei P, Martino E, Minuto F, Pivonello R, Ghigo E (2007) Pegvisomant in acromegaly: why, when, how. J Endocrinol Invest 30:693–699
Trainer PJ, Drake WM, Katznelson L, Freda PU, Herman-Bonert V, van der Lely AJ, Dimaraki EV, Stewart PM, Friend KE, Vance ML, Besser GM, Scarlett JA, Thorner MO, Parkinson C, Klibanski A, Powell JS, Barkan AL, Sheppard MC, Malsonado M, Rose DR, Clemmons DR, Johannsson G, Bengtsson BA, Stavrou S, Kleinberg DL, Cook DM, Phillips LS, Bidlingmaier M, Strasburger CJ, Hackett S, Zib K, Bennett WF, Davis RJ (2000) Treatment of acromegaly with the growth hormone-receptor antagonist pegvisomant. N Engl J Med 342:1171–1177
Colao A, Pivonello R, Auriemma RS, De Martino MC, Bidlingmaier M, Briganti F, Tortora F, Burman P, Kourides IA, Strasburger CJ, Lombardi G (2006) Efficacy of 12-month treatment with the GH receptor antagonist pegvisomant in patients with acromegaly resistant to long-term, high-dose somatostatin analog treatment: effect on IGF-I levels, tumor mass, hypertension and glucose tolerance. Eur J Endocrinol 154:467–477
Herman-Bonert VS, Zib K, Scarlett JA, Melmed S (2000) Growth hormone receptor antagonist therapy in acromegalic patients resistant to somatostatin analogs. J Clin Endocrinol Metab 85:2958–2961
De Marinis L, Bianchi A, Fusco A, Cimino V, Mormando M, Tilaro L, Mazziotti G, Pontecorvi A, Giustina A (2007) Long-term effects of the combination of pegvisomant with somatostatin analogs (SSA) on glucose homeostasis in non-diabetic patients with active acromegaly partially resistant to SSA. Pituitary 10:227–232
Acknowledgments
The authors thank the following participants in the Seventh Acromegaly Consensus Group meeting for their kind participation in this survey in advance of the meeting: John Ayuk, Birmingham, UK; Ariel Barkan, Ann Arbor, USA; Albert Beckers, Liege, Belgium; Paolo Beck-Peccoz, Milan, Italy; Bengt-Åke Bengtsson, Gothenburg, Sweden; Anat Ben-Shlomo, Los Angeles, USA; Jérôme Bertherat, Paris, France; John Bevan, Aberdeen, UK; Beverly Biller, Boston, USA; Jens Bollerslev, Oslo, Norway; Vivien Bonert, Los Angeles, USA; Marcello Bronstein, Sao Paulo, Brazil; Thierry Brue, Marseille, France; Michael Buchfelder, Erlangen, Germany; Philippe Caron, Toulouse, France; Davide Carvalho, Porto, Portugal; Felipe Casanueva, Santiago de Compostela, Spain; Franco Cavagnini, Milan, Italy; Philippe Chanson, Le Kremlin Bicetre, France; David Clemmons, Chapel Hill, USA; Annamaria Colao, Naples, Italy; Renato Cozzi, Milan, Italy; Ettore Degli Uberti, Ferrara, Italy; Laura De Marinis, Rome, Italy; Ernesto De Menis, Italy; Eva Marie Erfurth, Lund, Sweden; Rudolph Fahlbusch, Hannover, Germany; Diego Ferone, Genoa, Italy; Pamela Freda, New York, USA; Lawrence Frohman, Chicago, USA; Monica Gadelha, Rio de Janeiro, Brazil; Rolf Gaillard, Switzerland; Ezio Ghigo, Turin, Italy; Yona Greenman, Tel Aviv, Israel; Ashley Grossmann, London, UK; Feng Gu, Beijing, China; Amir Hamrahian, Cleveland, USA; Ian Holdaway, New Zealand; Ken Ho, Sydney, Australia; Jens Otto Jorgensen, Aarhus, Denmark; David Kleinberg, New York, USA; Anne Klibanski, Boston, USA; Steven Lamberts, Rotterdam, Netherlands; Edward Laws, Boston, USA; Gaetano Lombardi, Naples, Italy; Marco Losa, Milan, Italy; Pietro Maffei, Padua, Italy; Josef Marek, Prague, Czech Republic; Gherardo Mazziotti, Mantua, Italy; Moises Mercado, Mexico City, Mexico; Francesco Minuto, Genoa, Italy; Mark Molitch, Chicago, USA; Pietro Mortini, Brescia, Italy; Robert Murray, Leeds, UK; Stephan Petersenn, Essen, Germany; Ferdinand Roelfsema, Netherlands; Richard Ross, Sheffield, UK; Roberto Salvatori, Baltimore, USA; Janet Schlechte, Iowa City, USA; Jochen Schopohl, Munich, Germany; Omar Serri, Montreal, Canada; Guenter Stalla, Munich, Germany; Brooke Swearingen, USA; Mary Lee Vance, Charlottesville, USA; Aart Jan Van Der Lely, Rotterdam, Netherlands, Massimo Terzolo, Italy; George Tolis, Greece; John Wass, Oxford, UK; Susan Webb, Barcelona, Spain; Margaret Wierman, Denver, USA; Sema Yarman, Istanbul, Turkey. Editorial assistance was provided by John Clarke and Martin Gilmour (ESP Bioscience) supported by Ipsen.
Author information
Authors and Affiliations
Corresponding author
Appendix: Survey of acromegaly global patterns of care
Appendix: Survey of acromegaly global patterns of care



Rights and permissions
About this article
Cite this article
Giustina, A., Bronstein, M.D., Casanueva, F.F. et al. Current management practices for acromegaly: an international survey. Pituitary 14, 125–133 (2011). https://doi.org/10.1007/s11102-010-0269-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-010-0269-9