Abstract
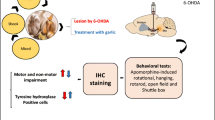
Spirulina platensis (SPI) is a cyanobacterium, presenting anti-inflammatory and antioxidant actions. Considering the importance of inflammation and oxidative stress in Parkinson’s disease (PD), SPI neuroprotective effects were evaluated in a model of PD. Male Wistar rats were divided into: sham-operated (SO), untreated 6-OHDA and 6-OHDA treated with SPI (25 and 50 mg/kg, p.o.). The 6-OHDA was injected into the right striata and SPI treatments started 24 h later for 2 weeks. The SO and untreated 6-OHDA-lesioned groups were administered with distilled water, for the same period. Afterwards, the animals were subjected to the apomorphine-induced rotational test and euthanized for striatal measurements of DA and DOPAC, nitrite and TBARS and immunohistochemistry assays for TH, DAT, iNOS and COX-2. SPI reduced the apomorphine-induced rotational behavior, DA and DOPAC depletions and nitrite and TBARS increases, at its high dose. Furthermore, TH and DAT immunoreactivities in the lesioned striatum of the untreated 6-OHDA-lesioned group were attenuated by SPI. Similarly, immunoreactivities for iNOS and COX-2 were also decreased after SPI treatments. In conclusion, we showed that behavioral and neurochemical alterations in hemiparkinsonian rats were partly reversed by SPI, characterizing the neuroprotective potential of Spirulina and stimulating translational studies focusing on its use as an alternative treatment for PD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Spirulina platensis (Nordest.) Geitler or Arthrospira platensis (Nordest.) Gomont is a multicellular filamentous cyanobacterium, presenting high contents of protein, along with high amounts of essential fatty acids and amino acids, minerals, vitamins, antioxidant pigments and polysaccharides [1, 2]. Although S. platensis is used in many countries as a nutritional supplement, based on its potential as a source of protein and vitamins, recently more attention has been paid to its therapeutic potential. S. platensis shows potent anti-inflammatory and antioxidant effects in rodents, among several other biological effects [3, 4].
A neurodegenerative process, leading to a slow and progressive dysfunction and loss of neurons and axons in the central nervous system (CNS), is a primary pathological feature of chronic neurodegenerative pathologies. Parkinson’s disease (PD) is a common, chronic, progressive, neurodegenerative disease with a multifactorial etiology, characterized by bradykinesia, rigidity, tremor and postural instability. The economic burden of the disease is substantial, but effective management of PD can minimize the disability and long-term health care costs [5].
Chronic inflammation is a major feature of PD and this neurodegenerative pathology not only encompasses deregulation of inflammatory pathways, resulting from genetic vulnerability, but also immune alterations associated with aging and activation of glia, as the result of neuronal injury [6]. Clinical post mortem studies show evidence of increased levels of pro-inflammatory molecules in brains of PD patients, as well as in the cerebrospinal fluid [7,8,9,10]. In addition, results from experimental PD models indicate that dopamine neurons are particularly vulnerable to both oxidative stress and inflammation [11, 12].
Furthermore, oxidative stress has been largely accepted to play a fundamental role in neurodegenerative diseases as PD, where aging is the most important risk factor, and cumulative oxidative stress leads to mitochondrial dysfunction and oxidative damage [13, 14]. Oxidative stress causes ROS production that can chemically interact with biological molecules, giving as a consequence changes in cell function and also cell death. Thus, neuroinflammation and mitochondrial dysfunction are common features of chronic neurodegenerative diseases. Both conditions can lead to increased oxidative stress by excessive release of ROS and RNS that further promotes neuronal damage and subsequent inflammation [15].
Considering that S. platensis presents anti-inflammatory and antioxidant properties, the objectives were to evaluate its effects on an experimental model of PD, in rats. For that, behavioral (apomorphine-induced rotation), neurochemical (DA, DOPAC, nitrite and lipid peroxidation measurements), as well as immunohistochemical (TH, DAT, iNOS and COX-2) assays in 6-OHDA-lesioned striata of animals subjected to this hemiparkinsonian model were also performed.
Materials and Methods
Drugs and Reagents
Ascorbic acid, 6-hydroxydopamine (6-OHDA) and HPLC standards were from Sigma-Aldrich (St. Louis, MO, USA); apomorphine was purchased from Tocris Bioscience (Bristol, UK); ketamine and xylazine were from Konig do Brasil (Santana do Parnaíba, São Paulo, Brazil). Rabbit polyclonal antibodies for immunohistochemistry assays were from Abcam (Cambridge, MA, USA). All other reagents were of analytical grade.
Cultivation of Spirulina platensis (SPI)
The innocula came from Antenna Technologies Foundation (Genève, Switzerland) where it was previously identified. Received as a gift from Dr. Denis von der Weid, it was cultivated in the laboratory, utilizing the Zarrouk media, and aerated with a 3000 lx illumination for a 12-h photo-period. Physical, chemical and microbiologic parameters were always determined, with a procedure aiming to control the light intensity and to decrease the rate of evaporation. After filtration, the material was weighed for determining the wet biomass and submitted to desiccation for 5 h. The dried material was weighed again to measure the dried biomass and, then, kept at −20 °C until use. It was suspended in distilled water for oral administration to the animals.
Preparation of the Aqueous Extract from Spirulina platensis for Total Phenol and Protein Contents Determinations
The 10% (w/v) aqueous Spirulina extract was prepared from a dried sample. The extraction was achieved with the aid of ultrasound for 40 min at room temperature (25 °C), and the solid residue content determined according to the Brazilian Pharmacopeia (2010) was 17.8 ± 0.98 mg/mL.
Total Phenol Contents of the Aqueous Extract from S. platensis
For the analyses of phenol contents, an aliquot (1 mL) of the 10% extract was transferred to a volumetric flask of 25 mL for dilution. Samples of the diluted extract (4 mL) were transferred to a 10 mL volumetric flask containing 0.25 mL of Folin–Ciocalteu and 4 mL of Milli-Q water. After alkalinization of the medium (3 mL 10% Na2CO3 solution), the volume was completed to 10 mL with Milli-Q water and readings performed spectrophotometrically at 785 nm. The calibration curve was prepared with standard gallic acid at concentrations ranging from 1 to 6 µg/mL. The results showed 16.5 mg/g of total phenols, expressed as gallic acid equivalent per gram of dry weight Spirulina.
Total Proteins Content of the Aqueous Extract from S. platensis
The quantification of total proteins was determined by colorimetric assay using a DC protein determination kit™ from Bio Rad (California, USA). The samples (5 µL of S. platensis extract) were transferred to a 96 well plate, followed by the addition of 25 µL of reagent A (alkaline copper tartrate) and 200 µL of reagent B (Folin) to each well, protected from light.). After 15 min at rest at room temperature (25 °C) in the dark, the total protein was quantified spectrophotometrically at 750 nm in a microplate reader. The calibration curve for the determination of proteins was prepared using bovine serum albumin (0.5; 1.0; 1.5; 2.0; 2.5, 3.0, 4.0 mg/mL).The results showed 455 mg/g (45.5%) of total protein in the aqueous extract of S. platensis.
Animals
Male Wistar rats (200–250 g) were maintained at a 24 ± 2 °C temperature, in a 12 h dark/12 h light cycle, with standard food and water ad libitum. The study was submitted to the Ethical Committee for Animal Experimentation of the Faculty of Medicine of the Federal University of Ceará (Brazil) and was approved under the number 23/2010. All experiments followed the ethical principles established in the Guide for the Care and Use of Laboratory Animals, USA, 2011.
The 6-OHDA Model of PD and the Experimental Protocol
The unilateral nigrostriatal 6-OHDA lesion is a very popular model of Parkinson's disease [16]. This classical method of intracerebral infusion of 6-OHDA involves a massive destruction of nigrostriatal dopaminergic neurons and is largely used to investigate motor and biochemical dysfunctions in Parkinson’s disease [17]. Although this neurotoxin selectively and rapidly destroys catecholaminergic neurons there are some differences between this model and the human pathology since in this last case its pathogenesis follows a progressive course and presents Lewy bodies [18]. The animals were anesthetized with the association of xylazine (20 mg/kg, i.p.) and ketamine (100 mg/kg, i.p.), submitted to shaving of the head superior region, and fixed to the stereotaxic frame by their ear canals. A longitudinal midline incision was made and the tissues were separated for bregma visualization. Then, a thin hole was performed in the skull, over the target area, and a 1 µL solution containing 6 µg 6-OHDA was injected into three different points. The following coordinates were used: 1st point: AP, +0.5; ML, −2.5; DV, +5.0; 2nd point: AP, −0.5; ML, −3.0; DV, +6.0 and 3rd point: AP, −0.9; ML, −3.7; DV, +6.5. The syringe stayed in place for 5 min for assuring the solution diffusion and, then, the incision was sutured. The sham-operated (SO) animals were subjected to all procedures, except that saline was injected into the three points. Afterwards, the animals returned to their cages for recovering. They were divided into the following groups: SO (treated by gavage with saline), 6-OHDA-lesioned (orally administered with saline), 6-OHDA-lesioned + SPI25 and 6-OHDA-lesioned + SPI50 (these last groups were orally treated by gavage with SPI, at the doses of 25 or 50 mg/kg). All treatments started 2 h before the surgical procedure and continued for 14 days, with drug volumes of 0.2 mL/100 g body weight. Then, after treatments and 1 h after the last drug administration, the animals were submitted to the behavioral tests. At the next day, they were euthanized (decapitation) and their striata removed for neurochemical studies. Four animals of each group were transcardially perfused with paraformaldehyde and processed for histological and immunohistochemical assays.
Rotational Behavior
The apomorphine induction of rotational (circling) behavior is widely used for assessing the effects of lesions to the dopaminergic system and the success of treatment strategies, in rat models of Parkinson’s disease. The number of rotations under apomorphine is related to the extent of dopamine depletion after the unilateral 6-hydroxydopamine lesion. The contralateral rotations (opposite to the lesioned right-side) induced by apomorphine (3 mg/kg, s.c.) were monitored for 1 h. The cause for this apomorphine-induced rotational behavior is related to the unbalance, in the nigrostriatal dopaminergic pathways, between the right (lesioned) and left (unlesioned) brain hemispheres. This asymmetric circling behavior, after the apomorphine administration, is a quantifiable motor deficit and an important paradigm in this model of PD [19, 20]. At day 14 and 1 h after the last SPI administration, the animals (6–13 per group) were subjected to the apomorphine-induced circling behavior test.
Neurochemical Determinations of DA and DOPAC by HPLC
The striatal contents of DA and DOPAC were determined by HPLC. Homogenates (from striatal tissue of 5–9 animals) were prepared in 10% HClO4 and centrifuged at 4 °C (20,817×g, 15 min). The supernatants were filtered and 20 µL injected into the HPLC column. For that, an electrochemical detector (model L-ECD-6A from Shimadzu, Japan) coupled to a column (Shim-Pak CLC-ODS, 25 cm) with a flux of 0.6 mL/min were employed. A mobile phase was prepared with monohydrated citric acid (150 mM), sodium octyl sulfate (67 mM), 2% tetrahydrofuran and 4% acetonitrile, in deionized water. The mobile phase pH was adjusted to 3.0 with NaOH (10 mM). Monoamines were quantified by comparison with standards, processed the same manner as the samples. The results are expressed as ng/g tissue.
Determination of Nitrite Contents
In this assay, the Griess reagent (1 part of 0.1% naphthylethylenediamine dihydrochloride in distilled water plus 1 part 1% sulfanilamide in 5% H3PO4) indicates the presence of nitrites in the sample. Striatal homogenates from 3 to 4 animals (10% in KCl buffer) were centrifuged (15,294×g for 10 min) and 100 μL supernatants were added to 100 μL Griess reagent and the mixture stayed on RT for 10 min. The standard NaNO2 curve was obtained (in spectrophotometer, at 520 nm) and used for calculating the results expressed as µmol nitrite per g tissue [21].
Determination of Lipid Peroxidation by Tiobarbituric Acid Reactive Substances (TBARS)
Lipid peroxidation expresses oxidative stress induced by ROS reactivity. A largely used method for measuring it is the determination of malondihaldehyde (MDA) in biological samples [22]. Striatal homogenates (10%) prepared from 4 to 5 animals in 1.15% KCl were added (250 μL) to 1 mL 10% TCA, followed by addition of 1 mL 0.6% thiobarbituric acid. After agitation, this mixture was maintained in a water-bath (95–100 °C) for 15 min. Then, the mixture was cooled on ice and centrifuged (2655×g/5 min). The TBARS content was determined in a plate reader, at 540 nm, with results expressed in μmol MDA per g tissue. A standard curve with several MDA concentrations was also performed.
Immunohistochemistry Assays
Four rats from each group were anesthetized with sodium pentobarbital (50 mg/kg, i.p.) and the tissues fixed by transcardial perfusion with 0.1 M phosphate-buffered saline (PBS, pH 7.2), followed by 4% paraformaldehyde (PAF) in PBS. The brains were removed, post-fixed in 4% PAF, for 24 h, and cryoprotected with 30% sucrose/0.1 M phosphate buffer. The brains were embedded in Tissue-Tek (Sakura-Americas, USA), frozen at −21 °C and cut into 50 μm coronal sections, using a cryostat. Nigral (substantia nigra pars compacta) and striatal slices were collected in series (300 μm interval) and the slices stored in 24-well plates, as free-floating sections in PBS with 0.01% NaN3. The sections were rinsed three times for 5 min in PBS and the endogenous peroxidase was inhibited, by incubating them in 3% H2O2 in PBS, for 1 h at RT. Slices were permeabilized and blocked with PBS, containing 1% Triton X-100 and 10% normal goat serum (NGS), for 1 h at RT. The sections were incubated with the appropriate primary antibody (anti-TH, anti-DAT, anti-iNOS and anti-COX-2) diluted according the manufacturers’ instructions), for 48 h at 4 °C, rinsed three times for 10 min in PBS and subsequently incubated with avidin–biotin horseradish peroxidase conjugate, for 30 min. After washing, the slices were incubated with biotinylated goat anti-rabbit secondary antibody, diluted in blocking solution (1:500). The color was developed using DAB as a chromogen. The sections were mounted in Entellan® (Merck, Germany), cover slipped and visualized under a microscope. Eight sections per animal (Olympus BX41 microscope equipped with an Olympus DP71 camera) were analyzed by the ×10 or ×40 objectives, for obtaining a rostrocaudal sampling of the striatum, and the intensity of the immunoreactivity was measured by semiquantitative densitometric analysis. The results were expressed as relative optical density by using an image analysis program (Image J software, NIH, MD, USA).
Statistical Analyses
For statistical analyses, One-way ANOVA, followed by Tukey as the post hoc test, were used for multiple comparisons. Whenever needed, the two-tailed paired or unpaired Student’s t-test was used for comparisons between two means. The photomicrographs’ data were quantified in relative optical density by the Image J software (NIH, USA). Differences were considered significant at p < 0.05.
Results
Apomorphine-Induced Rotational Behavior
The untreated 6-OHDA-lesioned group increased by more than 250-fold the number of contralateral rotations/h, related to the SO group (SO: 1.23 ± 0.871; untreated 6-OHDA-lesioned: 309.1 ± 42.33). On the other hand, treatments of the 6-OHDA-lesioned group with SPI (25 and 50 mg/kg) decreased dose-dependently this parameter (SPI25: 218.9 ± 70.83; SPI50: 157.8 ± 19.71), suggesting a neuroprotective effect (Fig. 1).
Spirulina (SPI, 25 and 50 mg/kg) treatments reverse partly the apomorphine-induced rotational behavior of the untreated 6-OHDA-lesioned groups. a vs SO, q = 10.18, p < 0.001; b vs 6-OHDA + SPI 50, q = 4.163, p < 0.05; c vs SO, q = 6.527, p < 0.001; d vs SO, q = 4.715, p < 0.05 (One-way ANOVA and Tukey as the post hoc test)
Determinations of Striatal DA and DOPAC Concentrations by HPLC
The untreated 6-OHDA-lesioned group showed around a 90% decrease of DA contents in the ipsilateral striatum, relatively to the ipsilateral side of the SO group and to its own contralateral side. A smaller decrease in DA was presented by the 6-OHDA-lesioned group, after treatments with SPI25 and SPI50 (comparatively to the ipsilateral side of the SO group or to the contralateral side of these two groups) (Fig. 2a). As far as DOPAC levels are concerned, the untreated 6-OHDA-lesioned group showed a 72% decrease, as related to the right side of the SO group, as well as to its own contralateral side. The 6-OHDA-lesioned group presented smaller decreases after SPI treatments comparatively to the ipsilateral side of the untreated 6-OHDA-lesioned group and to its own contralateral side (Fig. 2b).
Spirulina (SPI, 25 and 50 mg/kg) treatments reverse partly DA and DOPAC depletions of the untreated 6-OHDA-lesioned groups. DA: a vs SO R, q = 6.041, p < 0.01; b vs 6-OHDA L, q = 6.970, p < 0.001; c vs 6-OHDA R, t = 7.762, df = 9, p = 0.0101; d vs 6-OHDA + SPI 25 L, q = 6.068, p < 0.01; e vs 6-OHDA R, t = 3.524, df = 11, p = 0.0485; f vs 6-OHDA + SPI50 L, q = 7.441, p < 0.001. DOPAC: a vs SO R, q = 5.099, p < 0.05; b vs 6-OHDA L, q = 6.610, p < 0.001; c vs 6-OHDA R, p = 0.0315, t = 2.544, df = 9; d vs 6-OHDA R, p = 0.0264, t = 2.715, df = 8; e vs 6-OHDA + SPI50 L, p = 0.034, t = 2.911, df = 5. R right side (lesioned), L left side (One-way ANOVA and Tukey as the post hoc test and paired or unpaired two-tailed Student’s t test)
Nitrite Determinations and Lipid Peroxidation in the Rat Striata
The right (lesioned) striata from the untreated 6-OHDA-lesioned group presented a 3 times increase in nitrite contents, related to the same side of the SO group. On the other hand, values even lower than those showed by the SO group were demonstrated after SPI treatments, suggesting an antioxidant effect (Fig. 3a). In addition, a 2 times increase in MDA contents, related to the SO group, was observed in the right (lesioned) striata from the untreated 6-OHDA-lesioned group. This effect was completely reversed after SPI treatments, supporting the results seen in nitrite determination, above (Fig. 3b).
Spirulina (SPI) treatments (50 mg/kg) partially reversed the increased nitrite contents (μM) and lipid peroxidation, expressed as MDA (μg/g tissue) observed in the striatal lesioned right side from the untreated 6-OHDA group. Nitrite: a vs SO, q = 6.137, p < 0.001; b vs 6-OHDA + SPI50, q = 6.299, p < 0.001. MDA: a vs SO, q = 6.381, p < 0.001; b vs 6-OHDA + SPI50, q = 6.816, p < 0.001 (One way ANOVA and Tukey as the post hoc test)
Immunohistochemistry for Tyrosine Hydroxylase (TH) and Dopamine Transporter (DAT) in Rat Striata
The immunohistochemical data for TH and DAT were quantified by the Image J software. The results showed a 99% decrease in the TH immunoreactivity, on the lesioned striatal right side of the untreated 6-OHDA group related to the SO group. On the other hand, only a 42% decrease in TH immunostaining was observed after treatment of the 6-OHDA-lesioned group with SPI50. Similarly to the TH findings, a drastic decrease in DAT immunoreactivity (98%) was demonstrated in the lesioned right striatum of the untreated 6-OHDA-lesioned group. This reduction was partially blocked (55%) in the 6-OHDA-lesioned group after SPI treatment with the dose of 50 mg/kg (Fig. 4).
Representative photomicrographs (×400) of tyrosine hydroxylase (TH) and dopamine transporter (DAT), showing a decreased immunoreactivity in the lesioned striatum from the untreated 6-OHDA group, what was highly attenuated after the Spirulina treatment. TH: a vs SO, q = 62.05, p < 0.001; b vs 6-OHDA + SPI50, q = 26.13, p < 0.001; c vs SO, q = 35.92, p < 0.001. DAT: a vs SO, q = 23.47, p < 0.001; b vs 6-OHDA + SPI50, q = 7.525, p < 0.001; c vs SO, q = 14. 60, p < 0.001. The data were quantified by the Image J software, NIH, USA (One-way ANOVA followed by Tukey as the post hoc test)
Immunohistochemistry for the Inducible Nitric Oxide Syntase (iNOS) and Cyclooxygenase-2 (COX-2) in Rat Striata
The immunohistochemical data for iNOS and COX-2 were quantified by the Image J software. In the present study, while a 9 times increase was observed for iNOS immunoreactivity in the untreated 6-OHDA-lesioned group striatum, this went down to values even lower than those of the SO group, after the treatment with SPI (50 mg/kg). In addition, a 15 times higher immunoreactivity for COX-2 was demonstrated in the untreated 6-OHDA-lesioned group. Similarly, these values went down after SPI50, thus the immunostaining intensity was lower than that presented by the SO group (Fig. 5).
Representative photomicrographs (×400) of immunohistochemistry for iNOS and COX-2, showing an increased immunoreactivity in the lesioned striatum from the untreated 6-OHDA group, what was highly attenuated after the Spirulina treatment. iNOS: a vs SO, q = 100.4, p < 0.001; b vs 5-OHDA + SPI50, q = 103.0, p < 0.001. COX-2: a vs. SO, q = 47.68, p < 0.001; b vs 6-OHDA + SPI50, q = 49.32, p < 0.001. The data were quantified by the Image J software, NIH, USA (One-way ANOVA followed by Tukey as the post hoc test)
Discussion
Spirulina platensis is a rich source of protein, used as a nutritional supplement especially in low income countries. In the present study the Spirulina standardization shows 16.5 mg/g of total phenols and 45.5% of protein. This cyanobacterium besides being a rich source of protein, is known to present many properties, including anti-inflammatory, antioxidant and neuroprotective ones, generally needed for the treatment of chronic neurodegenerative pathologies, as Parkinson’s disease.
Furthermore, the presence of neuroinflammation and mitochondrial dysfunction, common features of these neurologic conditions, can lead to increased oxidative stress by excessive release of reactive oxygen and nitrogen species. These last alterations will further promote neuronal damage and subsequent inflammation, resulting in a feed-forward loop of neurodegeneration (15). In the present work, we evaluated the neuroprotective properties of S. platensis (SPI) in the hemiparkinsonism model, resulting from 6-OHDA striatal lesion.
In the present work, the potential neuroprotective activity of SPI was supported by the decrease of apomorphine-induced rotational behavior, related to the untreated 6-OHDA-lesioned group. Rats with unilateral 6-OHDA lesions of the nigrostriatal DA pathway are known to exhibit a contralateral rotational behavior, when challenged with DA agonists, such as apomorphine. This rotational response to apomorphine is used as a behavioral index of DA receptor supersensitivity, after unilateral 6-OHDA lesion [19], as well as for evaluating the extent of unilateral nigrostriatal denervation [23].
We showed that SPI partly recovered the DA and DOPAC depletions observed in the striatum of untreated 6-OHDA-lesioned animals. The most important neuropathological feature of Parkinson’s disease is the loss of dopaminergic neurons of the substantia nigra, leading to a severe depletion of striatal DA [24]. The striatum has a population of dopaminergic neurons that act as a source of DA. This neuronal population increases in size, in animal models of Parkinson’s disease where striatal DA levels are low [25]. The dopaminergic deficiency in Parkinson’s disease patients causes abnormalities of movement, behavior, learning and emotions [26]. Thus, SPI by partly reversing DA depletion would offer some protection for PD patients.
SPI significantly reversed the increased nitrite contents and lipid peroxidation observed in the right (lesioned) striatum of the 6-OHDA group. It is largely accepted that oxidative stress, leading to ROS production, is present in neurodegenerative diseases [27,28,29,30]. Previously, we demonstrated increased lipid peroxidation and nitrite levels in brains from AD patients [31]. These two parameters are good markers of oxidative stress and were blocked by SPI, indicating its potential as an antioxidant drug. Previously [32] the protean extract from S. platensis was shown to present a poweful antioxidant activity on SH-SY5Y neuroblastoma cells. Other results [33] observed similar effects on some cell lines, with the S. platensis water extract. In addition, a recent study [34] demonstrated that S. platensis reduced the kainic acid neuronal death in mice.
Furthermore, the striatal injection of 6-OHDA was shown [35] to lead to a massive disappearance of TH immunoreactive terminals, in a defined area within the striatum surrounding the injection site. These authors also observed a disappearance of DA cell bodies, in a small region of the ipsilateral substantia nigra pars compacta and concluded that the striatal injection of 6-OHDA leads to retrograde degeneration, as well as glial activation in the nigostriatal dopamine pathway. TH is the rate-limiting enzyme for brain catecholamine synthesis; and reduction of TH expression results in diminished DA synthesis, leading to PD, what makes TH essential in the pathogenesis of PD [36]. Thus, PD can be considered as a TH-deficiency syndrome of the striatum [37]. We showed that SPI treatment of 6-OHDA-lesioned animals produced an almost complete recovery of the drastic decrease in TH immunoreactivity. Considering the great importance of TH activity in PD, a logical and efficient therapeutic strategy for its treatment could be based on correcting TH deficiency.
We also demonstrated a drastic decrease in DAT immunoreactivity in the untreated 6-OHDA-lesioned animals, what was completely recovered after SPI treatment. The dopamine transporter (DAT) is a transmembrane protein, responsible for the reuptake of DA from the synaptic cleft and termination of dopaminergic transmission. Although it is usually accepted that parkinsonian symptoms develop when approximately 70–80% of DA neurons are lost, imaging studies have shown that a loss around 50% of DA terminals is required for the onset of symptoms in PD patients [38]. There is a decline of DAT, as the disease progresses in an exponential process, that can be revealed by DAT imaging [39]. Thus, this parameter can be considered as a marker for differentiating PD patients from healthy individuals [40].
Neuroinflammation may contribute to a variety of neurodegenerative diseases; and ROS are major regulators of this process, exerting a direct damaging effect on neurons. Nitric oxide is a highly reactive chemical messenger, playing an important role in mediating physiological as well as pathological pathways [41]. The expression of iNOS is linked to the generation of ROS which affects various cellular components and preferentially damages midbrain dopaminergic neurons in PD [42]. We showed a ninefold increase in the striatal immunoreactivity for iNOS in the untreated 6-OHDA-lesioned group, as related to the SO group. On the other hand, after SPI50 treatment, this value was even lower than that of the SO group.
An upregulation of inflammatory molecules, as iNOS and COX-2, has been suggested to play an important role in Parkinson’s disease, leading to dopaminergic neuron loss [43]. COX-2 is the enzyme responsible for the first committed step in the synthesis of several important mediators involved in the initiation and resolution of inflammation. The subsequent generation of PGs, upon activation of this inflammatory pathway, has been shown to participate in neurodegenerative processes, including those present in PD [44]. Furthermore, COX-2 is rapidly expressed in several cell types, in response to cytokines, growth factors and pro-inflammatory molecules [45]. In the present work, we demonstrated that the large increase in immunostaining for COX-2, in the striatum from the untreated 6-OHDA-lesioned group, was completely reversed after SPI treatments (50 mg/kg).
A recent study showed the neuroprotective properties of some other Spirulina species (S. fusiform) on a 6-OHDA model of PD. Spirulina improved locomotor activity and oxidative stress, as well as DA contents, in the lesioned rats [46]. Another study [47] demonstrated the protective effect of Spirulina treatment on the locomotor function and morphological damage, in the injured spinal cord model in rats. Garbuzova-Davis et al., 2010 [48], showed that a Spirulina supplemented diet significantly maintained body weight and extension reflex, and also reduced inflammatory markers and motor neuron degeneration, in a mouse model of amyotrophic lateral sclerosis.
Probably, the work by Pabon et al., 2012 [49], so far, is the only one similar to ours. These authors assumed that Spirulina was neuroprotective in the alpha-synuclein model of PD in rats, as more TH and NeuN positive cells were observed in the substantia nigra. Spirulina also decreased the numbers of activated microglial cells. Although these findings corroborate with ours and point out to the Spirulina potential in neurodegeneration, the authors used a different protocol: firstly, the administration of a diet containing 0.1% Spirulina, for a 30-day period (pretreatment) and, secondly, continuing the treatment in the presence of synuclein for 2 weeks, 1 or 4 months.
Our results suggest that Spirulina is neuroprotective in the model of 6-OHDA-induced hemiparkinsonism. This natural product presents potent anti-inflammatory and antioxidant activities, as demonstrated in acute and chronic experimental models of inflammation [50,51,52,53].
Interestingly, Spirulina was recently shown to inhibit LPS-induced inflammation, through the repression of HDAC in macrophages [54]. HDACs enzymes are known to play a role in homeostasis of protein acetylation and to regulate cellular activities, such as transcription, and their dysfunction is associated with a wide variety of brain disorders [55]. Thus, HDAC inhibitors, besides exerting anti-inflammatory effects also present a potential as neuroprotective drugs [56,57,58,59]. Recently, we demonstrated that valproic acid, in the 6-OHDA model of PD, probably exerts a neuroprotective action, in part through HDAC inhibition [60]. Valproic acid has been reported to upregulate the expression of neurotrophic factors, what could contribute to its neuroprotective effects on DA neurons [61,62,63,64]. HDAC inhibition has been hypothesized as cooperating to neuroprotection, through gene expression regulation in glial cells [65]. Furthermore, we believe that Spirulina antioxidant and anti-inflammatory effects would certainly contribute to its neuroprotective actions, as shown in the present work, suggesting this drug as a potential candidate to be included in the clinic for PD treatment.
References
Belay A, Ota Y, Miyakawa K, Shimamatsu H (1993) Current knowledge on potential health benefits of Spirulina. J Appl Phycol 5:235–241
Vonshak A (1997) Spirulina platensis (Arthrospira): physiology, cell biology and biotechnology. Taylor and Francis, London
Patro N, Sharma A, Kariaya K, Patro I (2011) Spirulina platensis protects neurons via suppression of glial activation and peripheral sensitization leading to restoration of motor function in collagen-induced arthritic rats. Indian J Exp Biol 49:739–748
Ismail M, Hossain MF, Tanu AR, Shekhar HU (2015). Effect of Spirulina intervention on oxidative stress, antioxidant status, and lipid profile in chronic obstructive pulmonary disease patients. Biomed Res Int 2015:486120
Weintraub D (2008) Dopamine and impulse control disorders in Parkinson’s disease. Ann Neurol 64(Suppl 2):S93–S100
Herrero M-T, Estrada C, Maatouk L, Vyas S (2015) Inflammation in Parkinson’s disease: role of glucocorticoids. Front Neuroanat 9:32. doi: 10.3389/fnana.2015.00032
Mogi M, Harada M, Riederer P, Narabyashi H, Fujita J, Nagatsu T (1994) Interleukin-1 beta growth factor and transforming growth factor-alpha are elevated in the brain from Parkinsonian patients. Neurosci Lett 180:147–150
Dobbs RJ, Charlett A, Purkiss AG, Dobbs SM, Weller C, Peterson DW (1999) Association of circulating TNF-alpha and IL-6 with ageing and Parkinsonism. Acta Neurol Scand 100:34–41
Reale M, Greig NH, Kamal MA (2009) Peripheral chemo-cytokine profiles in Alzheimer’s and Parkinson’s diseases. Mini Rev Med Chem 9:1229–1241
Reale M, Iarlori C, Thomas A, Gambi D, Perfetti B, Di Nicola M, Onofrj M (2009) Peripheral cytokines profile in Parkinson’s disease. Brain Behav Immun 23:55–63
McGeer PL, McGeer EG (2008) The alpha-synuclein burden hypothesis of Parkinson disease and its relationship to Alzheimer disease. Exp Neurol 212:235–238
Pott Godoy MC, Tarelli R, Ferrari CC, Sarchi MI, Pitossi FJ (2008) Central and systemic IL-1 exacerbates neurodegeneration and motor symptoms in a model of Parkinson’s disease. Brain 131:1880–1894
Gandhi S, Abramov AY (2012). Mechanism of oxidative stress in neurodegeneration. Oxidat Med Cell Longev 2012:11. doi:10.1155/2012/428010
Lin MT, Beal MF (2006) Mitochondrial dysfunction and oxidative stress in neurodegenerative diseases. Nature 443:787–795
Fischer R, Maier O (2015). Interrelation of oxidative stress and inflammation in neurodegenerative disease: role of TNF. Oxidat Med Cell Longev 2015:18. doi:10.1155/2015/610813
Jackson-Lewis V, Blesa J, Przedborski S (2012) Animal models of Parkinson’s disease. Parkinsonism Relat Disord 18(Suppl 1):S183–S185
Simola N, Morelli M, Carta AR (2007) The 6-hydroxydopamine model of Parkinson’s disease. Neurotox Res 11:151–167
Tieu K (2011) A guide to neurotoxic animal models of Parkinson’s disease. Cold Spring Harb Perspect Med 1:a009316
Waddington JL, Cross AJ, Longden A, Owen F, Poulter M (1979) Apomorphine-induced rotation in the unilateral 6-OHDA-lesioned rat: relationship to changes in striatal adenylate cyclase activity and 3H-spiperone binding. Neuropharmacology 18:643–645
Metz GA, Whishaw IQ, Metz GA, Whishaw IQ (2002) Drug-induced rotation intensity in unilateral dopamine-depleted rats is not correlated with end point or qualitative measures of forelimb or hindlimb motor performance. Neuroscience 111(2):325–336
Green LC, Wagner DA, Glogowski J, Skipper PL, Wishnok JS, Tannenbaum SR (1982) Analysis of nitrate, nitrite, and [15N]nitrate in biological fluids. Anal Biochem 126(1):131–138
Draper HH, Hadley M (1990) Malondialdehyde determination as index of lipid peroxidation. Methods Enzymol 186:421–431
Hudson JL, van Horne CG, Stromberg I, Brock S, Clayton J, Masserano J, Hoffer BJ, Gerhardt GA (1993) Correlation of apomorphine- and amphetamine-induced turning with nigrostriatal dopamine content in unilateral 6-hydroxydopamine lesioned rats. Brain Res 626:167–174
Hornykiewicz O, Kish SJ (1986) Biochemical pathophysiology of Parkinson’s disease. Adv Neurol 45:19–34
Huot P, Lévesque M, Parent A (2007) The fate of striatal dopaminergic neurons in Parkinson’s disease and Huntington’s chorea. Brain 130(Pt 1):222–232
Rodriguez-Oroz MC, Jahanshahi M, Krack P, Litvan I, Macias R, Bezard E, Obeso JA (2009) Initial clinical manifestations of Parkinson’s disease: features and pathophysiological mechanisms. Lancet Neurol 8:1128–1139
Chen X, Guo C, Kong J (2012) Oxidative stress in neurodegenerative diseases. Neural Regen Res 7(5):376–385
Kim GH, Kim JE, Rhie SJ, Yoon S (2015) The role of oxidative stress in neurodegenerative diseases. Exp Neurobiol 24(4):325–340
Sultana R, Perluigi M, Butterfield DA (2013) Lipid peroxidation triggers neurodegeneration: a redox proteomics view into the Alzheimer disease brain. Free Radic Biol Med 62:157–169
Uttara B, Singh AV, Zamboni P, Mahajan RT (2009) Oxidative stress and neurodegenerative diseases: a review of upstream and downstream antioxidant therapeutic options. Curr Neuropharmacol 7:65–74
DiCiero MM, de Bruin VM, Viana GS (2000) Lipid peroxidation and nitrite plus nitrate levels in brain tissues from patients with Alzheimer’s disease. Gerontology 46(4):179–184
Bermejo-Bescos P, Pinero-Estrada E, Villar del Fresno AM (2008) Neuroprotection by Spirulina platensis protean extract and phycocyanin against iron-induced toxicity in SH-SY5Y neuroblastoma cells. Toxicol In Vitro 22:1496–1502
Zaid AAA, Hammad DM, Sharaf EM (2015) Antioxidant and abticancer activity of Spirulina platensis water extracts. Int J Pharmacol 11:846–851
Pérez-Juárez A, Chamorro G, Alva-Sánchez C, Paniaqua-Castro N, Pacheco-Rosado J (2016) Neuroprotective effect of arthrospira (Spirulina)-platensis against kainic acid-neuronal death. Pharm Biol 54(8):1408–1412
Rodrigues RWP, Gomide VC, Chadi G (2003) Striatal injection of 6-hydroxydopamine induces retrograde degeneration and glial activation in the nigrostriatal pathway. Acta Cirúrgica Brasileira 18:272–282
Zhu Yanzhen Zhang, Jing Zeng Yanjun (2012) Overview of tyrosine hydroxylase in Parkinson’s disease. CNS Neurol Disord Drug Targets 11:350–358
Tabrez S, Jabir NR, Shakil S, Greig NH, Alam Q, Abuzenadah AM, Damanhouri GA, Kamal MA (2012) A synopsis on the role of tyrosine hydroxylase in Parkinson’s disease. CNS Neurol Disord Drug Targets 11:395–409
Varrone A, Halldin C (2010) Molecular imaging of the dopamine transporter. J Nucl Med 51:1331–1334
Antonini A, Biundo R (2014) Parkinson disease: can dopamine transporter imaging define early PD? Nat Rev Neurol 10:432–433
Bor-Seng-Shu E, Felicio AC, Braga-Neto P, Batista IS, Paiva WS, Andrade DC, Teixeira MJ, Andrade LAF, Barsottini OGP, Shih MC, Bressan RA, Ferraz HB (2014) Dopamine transporter imaging using 99mTc-TRODAT-1 SPECT in Parkinson’s disease. Med Sci Monit 20:1413–1418
Kavya R, Dikshit M (2015) Role of nitric oxide/nitric oxide synthase in Parkinson’s disease. Ann Neurosci (India) 12:1–5
Koppula S, Kumar H, Kim IS, Choi D-K (2012). Reactive oxygen species and inhibitors of inflammatory enzymes, NADPH oxidase, and iNOS in experimental models of Parkinson’s disease. Med Inflamm 2012, Article ID 823902
Okuno T, Nakatsuji Y, Kumanogoh A, Moriya M, Ichinose H, Sumi H, Fujimura H, Kikutani H, Sakoda S (2005) Loss of dopaminergic neurons by the induction of inducible nitric oxide synthase and cyclooxygenase-2 via CD 40: relevance to Parkinson’s disease. J Neurosci Res 81(6):874–882
Teismann P (2012) COX-2 in the neurodegenerative process of Parkinson’s disease. Int Un Biochem Mol Biol Inc 38:395–397
Bartels AL, Leenders KL (2010) Cyclooxygenase and neuroinflammation in Parkinson’s disease neurodegeneration. Curr Neuropharmacol 8:62–68
Chattopadhyaya I, Gupta S, Mohammed A, Mushtag N, Chauhan S, Ghosh S (2015) Neuroprotective effect of Spirulina fusiform and amantadine in the 6-OHDA induced parkinsonism in rats. BMC Complem Altern Med 15:296. doi:10.1186/s12906-015-0815-0
Aziz I, Ramli MDC, Zain NSM, Sanusi J (2014). Behavioral and histopathological study of changes in spinal cord injured rats supplemented with Spirulina platensis. Evid-Bas Complem Altern Med 2014:8. doi:10.1155/2014/871657
Garbuzova-Davis S, Bickford PC (2010) Neuroprotective effect of Spirulina in a mouse model of ALS. Open Tissue Eng Regen Med J 3:36–41
Pabon MM, Jernberg JN, Morganti J, Contreras J, Hudsen CE, Klein RL, Bickford PC (2012) A Spirulina-enhanced diet provides neuroprotection in an alpha-synuclein model of Parkinson’s disease. PLoS ONE 7(9):e45256
Pham TX, Kim B, Lee J (2013) Spirulina platensis inhibits lipopolysaccharide-induced inflammation through the repression of histone deacetylases in RAW 264.7 macrophages. FASEB 27:247.1
Yogianti F, Kunisada M, Nakano E, Ono R, Sakumi K, Oka S, Nakabeppu Y, Nishigori C (2014) Inhibitory effects of dietary Spirulina platensis on UVB-induced skin inflammatory responses and carcinogenesis. J Investig Dermatol 134:2610–2619
Muga MA, Chao Jane C-J (2014) Effects of fish oil and Spirulina on oxidative stress and inflammation in hypercholesterolemic hamsters. BMC Complement Altern Med 14:470. doi:10.1186/1472-6882-14-470
Gutiérrez-Rebolledo GA, Galar-Martínez M, García-Rodríguez RV, Chamorro-Cevallos GA, Hernández-Reyes AG, Martínez-Galero E (2015) Antioxidant effect of Spirulina (Arthrospira) maxima on chronic inflammation induced by Freund’s complete adjuvant in rats. J Med Food 18:865–871
Chuang D-M, Leng Y, Marinova Z, Kim H-J, Chiu C-T (2009) Multiple roles of HDAC inhibition in neurodegenerative conditions. Trends Neurosci 32:591–601
Halili MA, Andrews MR, Sweet MJ, Fairlie DP (2009) Histone deacetylase inhibitors in inflammatory disease. Curr Top Med Chem 9:309–319
Grabiec AM, Tak PP, Reedquist KA (2011) Function of histone deacetylase inhibitors in inflammation. Crit Rev Immunol 31:233–263
Lu J, Frerich JM, Turtzo LC, Li S, Chiang J, Yang C, Wang X, Zhang C, Wu C, Sun Z, Niu G, Zhuang Z, Brady RO, Chen X (2013) Histone deacetylase inhibitors are neuroprotective and preserve NGF-mediated cell survival following traumatic brain injury. Proc Natl Acad Sci USA 110:47–52
Coppedè F (2014) The potential of epigenetic therapies in neurodegenerative diseases. Font Gen doi:10.3389/fgene.2014.00220
Kim HJ, Rowe M, Ren M, Hong JS, Chen PS, Chuang DM (2007) Histone deacetylase inhibitors exhibit anti-inflammatory and neuroprotective effects in a rat permanent ischemic model of stroke: multiple mechanisms of action. J Pharmacol Exp Ther 321:892–901
Ximenes JC, Neves KR, Leal LK, do Carmo MR, Brito GA, Naffah-Mazzacoratti MG, Cavalheiro EA, Viana GS (2015). Valproic acid neuroprotection in the 6-OHDA model of Parkinson’s disease is possibly related to its anti-inflammatory and HDAC inhibitory properties.J Neurodegener Dis 2015:313702. doi:10.1155/2015/313702
Chen P-S, Peng G-S, Li G, Yang S, Wu X, Wang C-C, Wilson B, Lu R-B, Gean P-W, Chuang D-M, Hong J-S (2006) Valproate protects dopaminergic neurons in midbrain neuron/glia cultures by stimulating the release of neurotrophic factors from astrocytes. Mol Psychiatry 11:1116–1125
Chen P-S, Wang C-C, Bortner CD, Peng G-S, Wu X, Pang H, Lu R-B, Gean P-W, Chuang D-M, Hong J-S (2007) Valproic acid and other HDAC inhibitors induce microglial apoptosis and attenuate lipopolysaccharide-induced dopaminergic neurotoxicity. Neurosci 149:203–212
Leng Y, Wang J, Wang Z, Liao H-M, Wei M, Leeds P, Chuang D-M (2016) Valproic acid and other HDAC inhibitors upregulate FGF21 gene expression and promote process elongation in glia by inhibiting HDAC2 and 3.. Int J Neuropsychopharmacol 19(8):pyw035
Chiu C-T, Wang Z, Hubsberger JG, Chuang D-M (2013) Therapeutic potential of mood stabilizers lithium and valproic acid: beyond bipolar disorder. Pharmacol Rev 61(1):105–142
Wu X, Li S, Wu Q, Peng Y, Yu D, Wang H, Chui D, Zhao J (2013) Histone deacetylase inhibition leads to neuroprotection through regulation on glial function. Mol Neurodegen 8(Suppl 1):P49
Acknowledgements
The authors are grateful to the financial support of the Foundation for Development of Research and Innovation of the State of Ceará, Brazil (FUNCAP) and to the Brazilian National Research Council (CNPq). They thank Prof. M.O.L. Viana for the orthographic revision of the manuscript.
Author information
Authors and Affiliations
Contributions
FAVL carried most of the behavioral and neurochemical experiments; IPJ and FPJ were responsible for the cultivation of S. platensis; KRTN and MRC carried out all immunohistochemical assays; GMA performed the statistical analyses and GSBV coordinated and wrote the work. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interests.
Rights and permissions
About this article
Cite this article
Lima, F.A.V., Joventino, I.P., Joventino, F.P. et al. Neuroprotective Activities of Spirulina platensis in the 6-OHDA Model of Parkinson’s Disease Are Related to Its Anti-Inflammatory Effects. Neurochem Res 42, 3390–3400 (2017). https://doi.org/10.1007/s11064-017-2379-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-017-2379-5