Abstract
Altered redox dynamics contribute to physiological aging and Parkinson’s disease (PD). This is reflected in the substantia nigra (SN) of PD patients as lowered antioxidant levels and elevated oxidative damage. Contrary to this observation, we previously reported that non-SN regions such as caudate nucleus and frontal cortex (FC) exhibited elevated antioxidants and lowered mitochondrial and oxidative damage indicating constitutive protective mechanisms in PD brains. To investigate whether the sub-cellular distribution of antioxidants could contribute to these protective effects, we examined the distribution of antioxidant/oxidant markers in the neuropil fractions [synaptosomes, non-synaptic mitochondria and cytosol] of FC from PD (n = 9) and controls (n = 8). In the control FC, all the antioxidant activities [Superoxide dismutase (SOD), glutathione (GSH), GSH peroxidase (GPx), GSH-S-transferase (GST)] except glutathione reductase (GR) were the highest in cytosol, but several fold lower in mitochondria and much lower in synaptosomes. However, FC synaptosomes from PD brains had significantly higher levels of GSH (p = 0.01) and related enzymes [GPx (p = 0.02), GR (p = 0.06), GST (p = 0.0001)] compared to controls. Conversely, mitochondria from the FC of PD cases displayed elevated SOD activity (p = 0.02) while the GSH and related enzymes were relatively unaltered. These changes in the neuropil fractions were associated with unchanged or lowered oxidative damage. Further, the mitochondrial content in the synaptosomes of both PD and control brains was ≥five-fold lower compared to the non-synaptic mitochondrial fraction. Altered distribution of oxidant/antioxidant markers in the neuropil fractions of the human brain during aging and PD has implications for (1) degenerative and protective mechanisms (2) distinct antioxidant mechanisms in synaptic terminals compared to other compartments.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parkinson’s disease (PD) is a neurodegenerative disease clinically manifesting with movement disorders [1]. Oxidative stress and mitochondrial dysfunction contribute to the loss of dopaminergic neurons in the substantia nigra (SN) in PD [2–5]. Oxidative stress in PD manifests as lowered glutathione (GSH) [6], increased iron content and oxidative damage of cellular biomolecules [7–14], probably leading to mitochondrial dysfunction [15, 16].
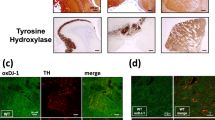
Although neurodegenerative events affect specific neuroanatomical areas such as SN, histopathological staging in PD brains revealed the initial pathology in the brainstem nuclei including the SN, extending to involve the neocortex in the late-stage of the disease [17]. To investigate whether the redox dynamics seen in the SN is evident in other neuroanatomical regions, we examined the status of oxidant and antioxidant markers in the striatum (caudate nucleus and putamen) and frontal cortex (FC) in human PD brains [18]. We observed that while SN showed higher oxidative damage, the non-SN regions displayed relatively lower oxidative and mitochondrial damage. This relative sparing of some of these areas was associated with 3–5 fold higher GSH content and elevated astrocytic proliferation [(indicated by higher expression of glial fibrillary acidic protein (GFAP)] [18].
Different sub-cellular compartments of the human brain display varied response to distinct physiological and pathological stimuli, with the synaptic terminals being more susceptible to damage. Postsynaptic regions are exposed to higher calcium influx and oxidative stress due to activated glutamate receptors which might make them more vulnerable to neurodegeneration [19]. Synaptic mitochondria are more sensitive to oxidative damage compared to non-synaptic mitochondria [20–23]. Interestingly, oxidative stress in the cytosol [4, 24] could ultimately lead to synaptic dysfunction and neurodegeneration [5, 25, 26]. Similarly, oxidative damage to nuclear DNA can influence the status of synaptic proteins [6, 12, 27, 28]. The status of the cytosolic GSH significantly influences plasma membrane function at the synaptic terminals [13, 29]. These data not only highlight that synaptic terminals are the initial targets for damage and degeneration, but also suggest that one sub-cellular compartment can influence the other. Secondly, analysis of specific markers in total extracts might not reflect the relative differential distribution in individual sub-cellular compartments. Thirdly, analysis of isolated synaptic terminals will provide neuron-specific information unlike the study on total brain extracts which might represent both neuronal and non-neuronal cell populations including vascular elements.
Since the FC in PD brains showed relatively lower oxidative damage and significantly high levels of GSH [18], the study of relative distribution of oxidant markers and antioxidant activities in different sub-cellular compartments can provide a mechanistic understanding of the neuronal function and protection of this neuroanatomical region against oxidative damage in PD. Towards this objective, in the current study, we examined the status of different oxidant and antioxidant markers in synaptosomes, non-synaptic mitochondria and cytosol in the human FC from cases of PD (n = 9) compared to age-matched control brains (n = 8).
Materials and Methods
All chemicals used were of analytical grade. Bulk chemicals were obtained from Merck (Whitehouse Station, NJ, USA) and Sisco Research Laboratories Pvt. Ltd. (Mumbai, Maharashtra, India). Nitrocellulose membrane from Millipore (Billerica, MA, U.S.A.), mouse monoclonal antibody to glial fibrillary acidic protein (GFAP) (clone GA-5) from Biogenex (San Ramon, CA, U.S.A.), horseradish peroxidase conjugated secondary antibodies from Bangalore Genei (Bangalore, Karnataka, India), anti-dinitrophenyl (DNP), rabbit polyclonal anti-β-actin and anti-3-nitrotyrosine antibodies and protease inhibitor cocktail from Sigma (Eugene, OR, U.S.A.) were obtained.
Human Tissue Samples
Brain samples from cases satisfying neurological criteria (based on the grading system of Hoehn and Yahr [1]) and neuropathological parameters (based on histology and immunohistochemistry as described previously [18]) for PD (n = 9) were obtained from the Human Brain Tissue Repository (HBTR), Department of Neuropathology, National Institute of Mental Health and Neurosciences (NIMHANS), Bangalore.
Non-PD control brains (n = 8) were from age-matched normal human subjects who succumbed to road traffic accidents (non-alcoholics, non-diabetics, not on any medication and without any known neurological or psychiatric disorders). Both diseased and control brain tissues were collected with informed consent from the close relatives of the deceased and the Institutional Ethics Committee approved the study protocol. Demographic and clinical details of all the subjects were recorded. Within 1 h of death, the body was transferred to a refrigerator maintained at 2–4 °C with a recorder and uninterrupted power supply. Following autopsy, the brains were sliced coronally and kept flat on salt-ice mixture (−15 to −18 °C) during dissection and then transferred into plastic zip lock bags and stored at −80 °C in cryo-resistant plastic boxes. The procedure of dissection of the fresh brains took 30–45 min and the brain slices were transferred immediately into the deep freezer maintained at −80 °C. The postmortem time (PMI) (the elapsed time between death and the freezing of the brain samples following autopsy and dissection) was recorded for each case. Human brain areas chosen for the study were anatomically farthest from the site of injury and without distinct edema or abnormal morphology. While the major portion of the tissue was frozen for biochemical studies, a minor portion corresponding to the mirror image bits of the stored tissue were fixed in buffered formalin. These tissues were subjected to routine histological assessment (by SKS and AM) as indicated below and the samples that maintained tissue integrity were utilized for the study (data not shown). The same procedure of autopsy, tissue handling and other protocols were uniformly maintained for all the samples in this study. Similar PD and control tissues from the human brain bank have been earlier utilized extensively in PD research [18, 30–32].
In the current study, frontal cortex (FC) region was analyzed in the PD and non-PD control brains [18]. The nigrostriatum could not be examined due to the non-availability of tissue from the cases of PD brains, following earlier studies. Table 1 shows the details related to the brain samples including age, gender, PMI and neurological score. The age of the controls [Mean (SD): 61.5 ± 14.9 years, range: 35–77 years; n = 8; 6 males, 2 females)] and PD (62.4 ± 14.1 years, range = 35–80 years; n = 9; 8 males and 1 female) are indicated. The average postmortem delay was 13.8 ± 6.4 h (range = 6–22 h) in controls and 6.1 ± 5.1 h (range = 1.5–15 h) in PD.
Isolation of Neuropil Fractions from the Brain Tissue [33]
Approximately 200 mg of brain tissue (FC) was minced in 1,000 μl of isolation Buffer (350 mM sucrose, 5 mM TES and 1 mM EGTA, pH 7.2) containing 100 μl of protease inhibitor cocktail and manually homogenized (16 strokes). The homogenate was centrifuged at 1,000×g for 5 min at 4 °C and the supernatant was stored. The pellet was homogenized again (16 strokes) on ice and centrifuged (1,000×g, 5 min at 4 °C). The supernatants from both the steps were pooled and centrifuged at 8,500×g for 10 min at 4 °C to obtain the crude mitochondrial/synaptosomal pellet. The post-mitochondrial fraction which corresponded to the cytosolic fraction was aliquoted and stored. The pellet was re-suspended in 300 μl of isolation buffer and overlaid on a discontinuous Ficoll gradient consisting of 6 % (w/v Ficoll, ρ = 1.065 g/ml, 3 ml), 9 % (w/vFicoll, ρ = 1.075 g/ml, 2 ml) and 12 % (w/v Ficoll, ρ = 1.085 g/ml, 3 ml). The gradient was centrifuged at 75,000×g for 1 h at 4 °C and the synaptosomes which formed a whitish ring in the middle of the gradient was collected, resuspended in reconstitution buffer (250 mM sucrose and 10 mM TES, pH 7.2) and stored as aliquots in −80 °C. Similarly, the mitochondria which formed the pellet were carefully resuspended in the reconstitution buffer. We previously demonstrated that the mitochondria and synaptosomes isolated from human brain samples by this method maintained purity and integrity [34–36]. All the three fractions were utilized for biochemical assays after protein estimation [37].
SDS PAGE and Western Blot
Soluble protein (50 μg) from different samples was loaded on 10 % SDS PAGE followed by western blot with either anti-GFAP or β-actin antibody [18].
Estimation of Protein Carbonyls (Oxyblot) and Protein Nitration
Oxyblots were carried out as described earlier [22, 38]. Briefly, protein extract (4 mg/ml) was derivatized by dinitrophenyl hydrazine (DNPH) in a 20 μl reaction mixture in the presence of 12 % SDS for 20 min at room temperature. The reaction was stopped by neutralization with 2 M Tris in 30 % glycerol and 5 μl of the sample was spotted in triplicate on nitrocellulose membrane and probed with anti-DNP antibody. Non-derivatized samples did not show anti-DNP immunoreactivity confirming the specificity of the antibody (data not shown).
To detect protein nitration, protein (10 μg/sample) from different samples were spotted in triplicate onto a nitrocellulose membrane and probed with polyclonal anti-3-nitrotyrosine (3-NT) antibody. Western blot signals were densitometrically quantified and normalized against the respective anti-β-actin signal [22].
Assays for Antioxidant Function and GSH Metabolism
Superoxide Dismutase (SOD) Assay
SOD activity was assayed using its inhibitory action on quercetin oxidation based on the method described earlier with minor modifications [39]. The final reaction mixture contained 30 mM Tris HCl (pH 9.1), 0.5 mM EDTA, 50 mM TEMED, 0.05 mM quercetin and 10 μl of brain extract supernatant containing 10 μg of protein. The reaction was monitored at 406 nm for 10 min. One unit of SOD activity was defined as the amount of enzyme (per mg protein) that inhibits quercetin oxidation reaction by 50 % of the maximal value.
Estimation of Total Glutathione (GSH + GSSG)
In all the samples, total glutathione (GSH + GSSG) and GSSG content were estimated. Total glutathione estimations were carried out by the 5,5′ dithio-bis-2-nitro benzoic acid recycling method as described earlier [40]. All estimations were conducted in triplicate and total glutathione concentrations were normalized per mg protein.
GSSG content in the neuropil fractions was measured by the method described previously [41] with minor modifications. Soluble extract prepared as described previously [40] was incubated first with 0.05 M N-ethylmaleimide (NEM) for 20 min to block the reduced GSH in the sample. Later, the reaction mixture containing 10 μl of sample, 180 μl of 0.1 N NaOH, and 10 μl o-phthalaldehyde (20 mg/ml) was incubated at room temperature for 15 min and the fluorescence (excitation at 350 nm and emission at 420 nm) was recorded. All the values were obtained in triplicate, compared with GSSG standards and normalized per mg protein.
Glutathione Peroxidase (GPx) Assay
GPx activity was determined by t-butyl hydroperoxide (tbHP) method [42]. The reaction mixture containing 150 μg protein (sample), 0.1 M phosphate buffer, 0.5 mM EDTA, 100 μl Glutathione reductase (0.24 U), 100 μl GSH (1 mM), and 100 μl NADPH (0.15 mM) was incubated at 37 °C for 3 min and the reaction was initiated by the addition of 100 μl tbHP (0.12 mM). Change in absorbance at 340 nm was monitored for 5 min spectrophotometrically and the activity was expressed as ηmoles of NADPH oxidized/min/mg protein (MEC = 6.22 mM−1cm−1).
Glutathione Reductase (GR)
Solubilized brain protein extract (100 μg) was assayed at 25 °C in 0.1 M Tris–HCl (pH 8.1) and 0.2 mM NADPH and the reaction was initiated by the addition of 1 mM GSSG. The enzyme activity was measured by monitoring the oxidation of NADPH, spectrophotometricallyat 340 nm [43].
Glutathione-S-Transferase (GST) Assay
GST was assayed by the 1-chloro 2-4-dinitro benzene (CDNB) method [44]. To 1 ml reaction mixture containing phosphate buffer (0.1 M, pH 6.5), 0.5 mM EDTA, CDNB (1.5 mM) and 50 μl GSH (1 mM), 30 μg protein (sample) was added and the increase in absorbance at 340 nm was monitored for 5 min. The enzyme activity was expressed as nmoles of S-2,4, dinitrophenyl glutathione formed/min/mg protein (MEC = 9.6 mM−1 cm−1).
Assays for Mitochondrial Function
3-(4,5-Dimethylthiazol-2-yl)-2,5-Diphenyltetrazolium Bromide (MTT) Assay
MTT assay, which is a colorimetric method that measures the reduction of MTT by mitochondria reductases was carried out as described previously [35, 45]. Briefly, 5 μl of the sample (~5 μg protein) was added to 1,000 μl of buffer (Mannitol-Sucrose-HEPES, 20 mM sodium succinate, 1 mM NADH, pH 7.4). To this, 15 μl of MTT (5 mg/ml) was added and incubated at 37 °C for 2 h. The formazan crystals formed, were dissolved in 100 μl SDS-dimethyl formamide (DMF) buffer (45 % DMF in distilled water and 10 % SDS, pH 4.7), and the absorbance was measured at 570 nm.
Citrate Synthase (CS)
CS activity which represents the rate of reduction of 5,5′-dithiobis-(2-nitrobenzoic) acid (DTNB) to thionitrobenzoic acid (TNB) at 412 nm was assayed as described previously [35, 46]. The reaction was initiated by the addition of 20 μl of 10 mM oxaloacetate (final concentration 0.2 mM) to the reaction mixture containing 100 mM Tris–HCl (pH 8.1), 0.2 mM DTNB, 0.1 % Triton X-100, 0.1 mM acetyl-CoA and 20 μg of mitochondrial protein. The results were expressed as nmol DTNB/min/mg protein (MEC = 13.6 mM−1cm−1).
Succinate Dehydrogenase (SDH)
SDH activity was determined as an end-point assay based on the method of Pennington [47] with minor modifications [35]. Mitochondrial sample (10 μl) was added to 70 μl of 0.01 mol/l sodium succinate solution in 0.05 mol/l phosphate buffer, pH 7.5 and incubated for 15 min at 37 °C. Next, 70 μl of 1 μg/μl p-iodonitrotetrazolium violet was added to the reaction and incubated at 37 °C for an additional 10 min. The reaction was stopped by the addition of 100 μl of a 5:5:1 (v:v:w) solution of ethyl acetate:ethanol:trichloroacetic acid and the absorbance was measured at 490 nm. The specific activity was expressed as OD/mg protein.
Malate Dehydrogenase (MDH)
Malate dehydrogenase activity was assayed as described previously [35, 48]. To 230 μl of the reaction buffer [Potassium phosphate buffer (0.1 M, pH 7.5), 0.03 ml NADH (14.3 mM) and 0.05 ml oxaloacetate (20 mM)], mitochondrial sample (10 μg) was added and the decrease in absorbance due to increased oxidation of NADH was measured for 3 min at 340 nm. The enzyme activity was expressed as nmoles NADH/min/mg protein (MEC = 6.22 × 10−6 nmol−1 cm−1).
Statistical Analysis
Quantitative data from at least three independent experiments were expressed as mean ± SD followed by analysis of variance (ANOVA). For all the quantitative data, p < 0.05 was considered to be statistically significant.
Results
Experimental evidences in PD have demonstrated significant oxidative stress and mitochondrial dysfunction in the SN [49–51]. In our previous study [18], we observed that compared to SN, non-SN regions such as FC were protected from oxidative and mitochondrial damage due to increased GSH. In the current study, we investigated the distribution of antioxidant markers in different sub-cellular fractions in FC in the brains from cases of PD compared to controls. This is physiologically relevant since the activity in total brain extract might not reflect the status of different markers in the neuropil compartments and different fractions might respond differently to oxidative stimuli. We observed this phenomenon of differential response both in control and PD brains.
In our earlier study, we had reported that the total SOD activity in non-SN regions of the brain was unaltered in PD compared to control [18]. However, the current study showed that the SOD activity in the FC from control brains were ~4 fold lower in the mitochondria (p < 0.001) and ~10 fold lower in the synaptosomes (p < 0.001) compared to the cytosolic fraction (Fig. 1a). Further, while the SOD activity in the cytosol and synaptosomes of FC tissue from PD cases was unaltered, mitochondrial SOD activity was found to be increased by ~2 fold (p = 0.017) compared to control (Fig. 1a).
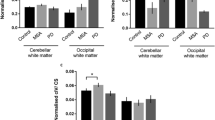
Alterations in the antioxidant activities in the neuropil fractions of FC region of human PD brains (n = 9) and controls (n = 6). Neuropil fractions (cytosol-cyto, non-synaptic mitochondria-ns mito, synaptosomes-syn) were isolated from FC. SOD activity and total GSH content in all the fractions were assayed in triplicate and the average for each sample was plotted as mean ± SD followed by ANOVA analysis and calculation of p values. The bar graph and the p values in the neuropil fractions of control and PD samples: a SOD activity (Absolute SOD activity in cytosol = 115.8 unit activity/mg protein, mitochondria = 32.7 unit activity/mg protein and synaptosome = 13.6 unit activity/mg protein. SOD activity in the respective neuropil fraction of control brains was considered as 100 % for comparison with PD samples) b Total GSH (Total GSH content in cytosol = 1.8 nmoles/mg protein, mitochondria = 0.32 nmoles/mg protein and synaptosome = 0.4 nmoles/mg protein. The total GSH in the respective neuropil fraction of control brains was considered as 100 % for comparison with PD samples). c Total GSSG (Total GSSG content in cytosol = 0.13 nmoles/mg protein, mitochondria = 0.04 nmoles/mg protein and synaptosome = 0.05 nmoles/mg protein. The total GSSG in the respective neuropil fraction of control brains was considered as 100 % for comparison with PD samples) and d GSSG/total glutathione ratio from the control and PD samples. *p < 0.05, **p < 0.01, ***p < 0.001, not significant (ns) compared to the respective controls or compared to cyto
In the control brains, total GSH displayed ~5 fold lower level in mitochondria (p < 0.01) and synaptosomes (p < 0.05) compared to cytosolic fraction (Fig. 1b). On the other hand, we observed distinct elevation in GSH content in the synaptic terminals of the FC from PD brains. Accordingly, synaptosomes from PD brains showed ~5 fold elevation in total GSH compared to control (p = 0.01), while the cytosolic GSH was elevated by ~2.5 fold compared to controls (p = 0.009). Interestingly, the mitochondrial GSH content was unaltered in PD samples (p = 0.23) (Fig. 1b).
To investigate whether the elevation in total glutathione was associated with the conversion of GSH to GSSG, we estimated the GSSG in the neuropil fractions. The GSSG content in the control samples showed a trend similar to the total glutathione (Fig. 1b, c), with the cytosolic GSSG significantly higher that the mitochondrial and synaptosomal GSSG (p < 0.05). In the PD samples, the synaptosomes showed the highest percentage increase in GSSG (p < 0.01) compared to control followed by cytosol (p < 0.001), while it was unchanged in the non-synaptic mitochondria. The ratio of GSSG to total glutathione (GSH + GSSG) in the different fractions did not show any difference between the control and PD samples indicating that the elevated total glutathione was not due to conversion of GSH to GSSG (Fig. 1d).
The GPx activity in the control brains was ~3 fold lower in mitochondria (p < 0.001) and ~5 fold lower in synaptosomes (p < 0.001) compared to cytosol (Fig. 1c, inset). On the other hand, GPx activity in the PD tissue was elevated by ~2 fold both in the cytosol (p = 0.02) and synaptosomes (p = 0.02) compared to control, while it was unaltered in mitochondria (p = 0.09) (Fig. 2a).
Alterations in the activities of GSH enzymes in the neuropil fractions of FC region of human PD brains (n = 9) and controls (n = 6). Neuropil fractions (cytosol-cyto, non-synaptic mitochondria-ns mito, synaptosomes-syn) were isolated from FC. GPx, GR and GST activities in all the fractions were assayed in triplicate and the average for each sample was plotted as mean ± SD followed by ANOVA analysis and calculation of p values. The bar graph and the p values in the neuropil fractions from control and PD samples are shown as follows: a GPx activity (Total GPx activity in cytosol = 0.03 nmoles/min/mg protein, mitochondria = 0.01 nmoles/min/mg and synaptosome = 0.005 nmoles/min/mg. The GPx activity in the respective neuropil fraction of control brains was considered as 100 % for comparison with PD samples). b GR activity (Absolute GR activity in cytosol = 0.009 nmoles/min/mg protein, mitochondria = 0.005 nmoles/min/mg and synaptosome = 0.0065 nmoles/min/mg. GR activity in the respective neuropil fraction of control brains was considered as 100 % for comparison with PD samples) c Total GST activity (Absolute GST activity content in cytosol = 0.17 nmoles/min/mg, mitochondria = 0.03 nmoles/min/mg and synaptosome = 0.006 nmoles/min/mg. The GST activity in the respective neuropil fraction of control brains was considered as 100 % for comparison with PD samples) *p < 0.05, ***p < 0.001, not significant (ns) compared to the respective controls or compared to cyto
GSH reductase activity in the control FC showed similar activity in all neuropil fractions (Fig. 2b). However, the GR activity in the FC from PD brains was elevated by ~2.5 fold in synaptosomes (p = 0.006) and by ~1.5 fold in the cytosol (p = 0.03) compared to the respective controls, while it was unaltered in mitochondria (p = 0.54) (Fig. 2a). On the other hand, GST in the control brains showed ~6 fold lower activity (p < 0.001) and >10 fold lower activity in synaptosomes (p < 0.001) compared to cytosol. GST activity in the FC from PD brains was significantly elevated on in the synaptosomes by ~3 fold (p = 0.0001) while it was unaltered in cytosolic and mitochondrial fractions (Fig. 2c).
These data indicated that (1) the antioxidant markers showed significant alteration in control brains across different sub-cellular fractions of FC with the synaptosomes showing least activity followed by mitochondria and cytosol (2) synaptosomes from FC of PD brains showed relatively increased GSH content and higher related enzyme activities compared to controls (3) mitochondria from FC of PD brains showed higher SOD activity compared to controls (Table 2).
Next, we investigated whether markers of oxidative stress in different fractions showed alteration in PD compared to age-matched controls. The mitochondrial fraction showed lowered protein nitration levels (indicated by 3-nityrotyrosine or 3-NT blot) (p < 0.01) and lowered protein oxidation (indicated by anti-dinitrophenyl or anti-DNP blot) in PD samples compared to controls (p < 0.05) (Fig. 3). Similarly, protein nitration was unaltered (p = 0.5) and protein oxidation was lowered in PD synaptosomes (p < 0.01) compared to controls (Fig. 4). The cytosolic fraction from the FC of PD brains showed lowered protein oxidation (p < 0.05), while the protein 3-NT level (p = 0.13) and GFAP expression (p > 0.05) were unaltered (Fig. 5). These observations indicate protection against oxidative damage by elevated SOD in the mitochondria and elevated GSH content in the synaptosomes and cytosolic compartments.
Analysis of markers of oxidative and nitrosative stress in non-synaptic mitochondria (ns mito) FC from human PD brains (n = 9) and controls (n = 6). Total protein extracts (100 μg) from FC (ns mito) of Control (C) and PD samples were spotted on nitrocellulose membrane followed by anti-3NT western blot. a representative anti-3NT blot from C and PD (in triplicate indicated by flower bracket) and its quantitation based on densitometric analysis are indicated in the figure. PBS corresponds to no-protein control. Total protein extract after DNP-derivatization (~10 μg) in FC from C and PD samples were spotted on nitrocellulose membrane in triplicate followed by anti-DNP western blot (Oxyblot). b Representative anti-DNP blot from C and PD (in triplicate indicated by flower bracket) and its quantitation based on densitometric analysis are shown. DNPH corresponds to the sample with DNPH only and without protein. *p < 0.05, **p < 0.01, ns not significant
Analysis of markers of oxidative and nitrosative stress in the synaptosomal fraction (syn) of FC from human PD brains (n = 9) and controls (n = 6). Total protein extracts (100 μg) from FC (synaptosmes or syn) of Control (C) and PD samples were spotted on nitrocellulose membrane followed by anti-3NT western blot. a Representative anti-3NT blot and representative western blot (from 4 samples) and dot blot for β-actin from C and PD samples (in triplicate indicated by flower bracket) followed by quantitation of anti-3NT signal normalized with β-actin signalare shown. PBS corresponds to no-protein control. Total protein extract after DNP-derivatization (~10 μg) in FC syn from C and PD samples were spotted on nitrocellulose membrane in triplicate followed by anti-DNP western blot (Oxyblot). b Representative anti-DNP blot of FC from PD and C samples and quantitation of anti-DNP signal normalized with β-actin signal are shown. DNPH corresponds to the sample with DNPH only and without protein as indicated in the figure. **p < 0.01, ns = not significant
Analysis of markers of oxidative and nitrosative stress and GFAP expression in the cytosolic fraction of FC from human PD brains (n = 9) and controls (n = 6). Total protein extracts (100 μg) from FC (cytosol) of Control (C) and PD samples were spotted on nitrocellulose membrane followed by anti-3NT western blot. a representative anti-3NT dot blot and β-actin dot blot from C and PD (in triplicate as indicated by flower bracket) and quantitation of anti-3NT signal normalized with β-actin signal are shown. PBS corresponds to no-protein control. Total protein extract after DNP-derivatization (~10 μg) in FC (PMS) from C and PD samples were spotted on nitrocellulose membrane in triplicate followed by anti-DNP western blot (Oxyblot). b Representative anti-DNP blot of FC tissue (cytosol) showing PD and C samples and quantitation of anti-DNP signal normalized with β-actin signal are shown. c Representative anti-GFAP western blot (from four samples) and dot blot of FC tissue (cytosol) showing PD and C samples and quantitation of anti-GFAP signal normalized with β-actin signal are shown. PBS corresponds to no-protein control. *p < 0.05, ns not significant
Next, we investigated whether the difference in the antioxidant status between synaptosomes and non-synaptic mitochondria is associated with the quantum of mitochondrial content and function. To address this issue, we carried out mitochondrial assays including MTT, CS, SDH and MDH in both fractions (Fig. 6). Based on these functional assays, we observed that the synaptosomes showed ≥5 fold lower mitochondrial content compared to the non-synaptic mitochondria, both in the control and PD samples.
Analysis of mitochondrial enzyme activities in the synaptic and non-synaptic mitochondria of FC region of human PD brains (n = 9) and controls (n = 6). Non-synaptic mitochondria (ns mito), synaptic mitochondria (syn mito) were isolated from FC. CS, MDH, SDH and mitochondrial reductase (MTT) activities in both the fractions were assayed in triplicate and the average for each sample was plotted as mean ± SD followed by ANOVA analysis and calculation of p values. The bar graph and the p values in the neuropil fractions from control and PD samples are shown as follows: a CS activity (expressed as nmoles of DTNB reduced/min/mg protein) b MDH activity (expressed as nmoles of NADH oxidized/min/mg protein) c SDH activity (expressed as OD/mg protein (OD as a result of reduction of p-iodonitrotetrazolium/mg protein) and d MTT values (OD as a result of reduction of MTT to formazan/mg protein). *p < 0.05, ***p < 0.001, not significant (ns) compared to the respective controls
Discussion
Even as previous studies have correlated the redox dynamics [4, 7–14] and mitochondrial status [15, 16] in PD brains compared to controls, the sub-cellular distribution of antioxidant markers in PD brains need to be investigated, as such studies in human samples are non-existent. The current study compared non-synaptic mitochondria, synaptosomes (which represent synaptic terminals) and cytosolic fractions from human PD brains. While the total extracts from the human brain represent neuronal and non-neuronal cells, analysis of synaptosomes represents only the neuronal physiology devoid of glial and vascular endothelial contribution. Since the bioenergetic capacities of neurochemically different synaptosomes do not vary significantly [52], the synaptosomes used in the current study could be considered as a homogenous population. We observed that the synaptosomes and mitochondrial fractions in the control FC showed several fold lower antioxidant activity compared to cytosol (Figs. 1, 2).This is in agreement with our previous study [36], which showed that the antioxidant activities such as SOD, GPx and GST in the neuronal cytosol and synaptosomes were altered by age. Ansari et al. [53] showed that the neuropil fractions from subjects with mild cognitive impairment and Alzheimer’s disease (AD) displayed elevated oxidative stress and antioxidant depletion, with the highest oxidative damage observed in the synaptosomes. While these data indicate the selective vulnerability of synaptosomes, elevated GSH and related activities in FC of PD brains (Figs. 1, 2) might be neuroprotective, consistent with a report [54] that elevated brain GSH protected synaptosomes against acrolein-induced damage. While higher GSH content and related enzyme activities might provide the major antioxidant defense in the synaptosomes, elevated SOD activity might play an important role in the non-synaptic mitochondria. Interestingly, most of the other activities were relatively unaltered in the non-synaptic mitochondria (Figs. 1, 2). Two previous studies [55, 56] showed that under conditions that induce cellular GSH depletion, irrespective of the in vivo GSH levels, the mitochondrial GSH pool was unaltered thus signifying the mitochondrial mechanism underlying the ability to counter oxidative stress.
These results also indicate that the data from whole cell or tissue extracts might not reflect the status of different activities in individual compartments. Hence biochemical activity from total cell extracts should be interpreted cautiously. In a relevant study on aging human brains [36], we showed that while the SOD activity and GSH content were unchanged with increasing age in total brain extracts, the parameters changed significantly in the neuropil fractions. In another study [18] carried out on the total extract of FC from PD brains, we showed that the SOD activity from PD brains was unaltered compared to controls, while the SOD activity was elevated in the non-synaptic mitochondria (Fig. 1a), consistent with a previous study [57] which demonstrated increased mitochondrial SOD activity in the motor cortex from PD cases but not in cases of amyotropic lateral sclerosis. Similarly, while the GR and GST activities in the total extract of FC were unaltered between PD and control brains[18] neuropil analysis revealed significantly elevated activities in the synaptosomes (Fig. 2b, c). Total GSH was elevated by 3 fold in total extract of FC compared to control [18] while the highest relative elevation was observed in the synaptosomes (Fig. 1b) compared to cytosol and non-synaptic mitochondria. On the other hand, the GPx activity elevated in the total extract of FC from PD brains was contributed only by the cytosolic and synaptosomal fractions while the activity was unchanged in the mitochondria (Fig. 2a).
In the human brains obtained after autopsy, pre-mortem (age, gender, agonal state) and postmortem factors [postmortem interval (PMI), storage time] might impinge on tissue integrity and quality [35, 58]. PMI might affect different biochemical parameters in the human brain tissue [22].The average PMI of the control brain samples (13.8 h) used in the current study was nearly two-fold higher than in the PD samples (6.1 h), which might affect the antioxidant activities. However, our previous studies on human brains showed that increasing PMI (2.5–26 h) did not affect the antioxidant activities, GSH content and related enzymes in FC [59]. In another study, we have demonstrated that increasing PMI did not influence the postmortem stability of glial fibrillary acidic protein (GFAP) and oxidatively damaged proteins indifferent anatomical regions of human brains including FC [58]. These studies indicate that the oxidant and antioxidant markers in FC are relatively unaffected by PMI and the differences observed between the control and PD samples in the study represent disease-related changes.
Most studies on redox dynamics in PD have concentrated on the nigrosriatum but studies on FC are limited [60].While the SN from PD brains displays GSH loss [61, 62], non-SN regions show elevated GSH content, which might protect mitochondria against oxidative damage [18]. Elevated GSH could either be due to increased synthesis or leakage of intracellular GSH or by lowered breakdown. We previously showed that the elevated GSH in FC of PD brains was due to lowered activity of gamma glutamyl transpeptidase (GGT), while the activity of the GSH synthesizing enzyme gamma glutamyl ligase (GCL) was unaltered [18]. The current study showed that the GSH elevation in FC was not due to the oxidation of GSH to GSSG since both control and PD samples showed the same GSSG/total glutathione ratio (Fig. 1c, d). Analysis of mitochondrial enzyme activities (Fig. 6) indicated that the mitochondrial content in the synaptosomal fraction was at least 5 fold lower than the non-synaptic mitochondria. Since this phenomenon was seen both in the control and PD samples, it could be concluded that the selective vulnerability of the synaptosomes to oxidative damage in the controls and the relative changes in the antioxidant activities in PD samples is not directly associated with the mitochondrial content.
In conclusion, our data indicate that (1) the relative distribution of antioxidant markers including GSH in synaptic and non-synaptic regions significantly impinges on the degenerative and protective mechanisms in PD (2) synaptosomal and mitochondrial fractions exhibit lower antioxidant activity compared to cytosol in FC from control brains indicating the susceptibility of synaptosomes against oxidative damage (3) Elevated GSH content and related enzyme activities in FC of PD brains compared to controls might contribute to neuroprotection in PD.
Abbreviations
- PD:
-
Parkinson’s disease
- SN:
-
Substantianigra
- FC:
-
Frontal cortex
- GSH:
-
Glutathione reduced
- PMI:
-
Postmortem interval
- 3-NT:
-
3-nitrotyrosine
- GFAP:
-
Glial fibrillary acidic protein
- SOD:
-
Superoxide Dismutase
- GST:
-
Glutathione-s-transferase
- GR:
-
Glutathione reductase
- GP:
-
Xglutathione peroxidase
- ns mito:
-
Non-synaptic mitochondria
- syn mito:
-
Synaptic mitochondria
- cyto:
-
Cytosol
- CS:
-
Citrate synthase
- MDH:
-
Malate dehydrogenase
- SDH:
-
Succinate dehydrogenase
- MTT:
-
3-(4,5-Dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide
References
Hoehn MM, Yahr MD (1967) Parkinsonism: onset, progression and mortality. Neurology 17(5):427–442
Adams JD Jr, Chang ML, Klaidman L (2001) Parkinson’s disease–redox mechanisms. Curr Med Chem 8(7):809–814
Beal MF (1992) Does impairment of energy metabolism result in excitotoxic neuronal death in neurodegenerative illnesses? Ann Neurol 31(2):119–130. doi:10.1002/ana.410310202
Jenner P, Dexter DT, Sian J, Schapira AH, Marsden CD (1992) Oxidative stress as a cause of nigral cell death in Parkinson’s disease and incidental Lewy body disease. The Royal Kings and Queens Parkinson’s Disease Research Group. Ann Neurol 32(Suppl):S82–S87
Sayre LM, Smith MA, Perry G (2001) Chemistry and biochemistry of oxidative stress in neurodegenerative disease. Curr Med Chem 8(7):721–738
Bharath S, Hsu M, Kaur D, Rajagopalan S, Andersen JK (2002) Glutathione, iron and Parkinson’s disease. Biochem Pharmacol 64(5–6):1037–1048. doi:10.1016/S0006-2952(02)01174-7
Alam ZI, Daniel SE, Lees AJ, Marsden DC, Jenner P, Halliwell B (1997) A generalised increase in protein carbonyls in the brain in Parkinson’s but not incidental Lewy body disease. J Neurochem 69(3):1326–1329
Dexter DT, Wells FR, Lees AJ, Agid F, Agid Y, Jenner P, Marsden CD (1989) Increased nigral iron content and alterations in other metal ions occurring in brain in Parkinson’s disease. J Neurochem 52(6):1830–1836
Floor E, Wetzel MG (1998) Increased protein oxidation in human substantia nigra pars compacta in comparison with basal ganglia and prefrontal cortex measured with an improved dinitrophenylhydrazine assay. J Neurochem 70(1):268–275
Good PF, Hsu A, Werner P, Perl DP, Olanow CW (1998) Protein nitration in Parkinson’s disease. J Neuropathol Exp Neurol 57(4):338–342
Sofic E, Paulus W, Jellinger K, Riederer P, Youdim MB (1991) Selective increase of iron in substantia nigra zona compacta of parkinsonian brains. J Neurochem 56(3):978–982
Dexter DT, Carter CJ, Wells FR, Javoy-Agid F, Agid Y, Lees A, Jenner P, Marsden CD (1989) Basal lipid peroxidation in substantia nigra is increased in Parkinson’s disease. J Neurochem 52(2):381–389
Yoritaka A, Hattori N, Uchida K, Tanaka M, Stadtman ER, Mizuno Y (1996) Immunohistochemical detection of 4-hydroxynonenal protein adducts in Parkinson disease. Proc Natl Acad Sci USA 93(7):2696–2701
Alam ZI, Jenner A, Daniel SE, Lees AJ, Cairns N, Marsden CD, Jenner P, Halliwell B (1997) Oxidative DNA damage in the parkinsonian brain: an apparent selective increase in 8-hydroxyguanine levels in substantia nigra. J Neurochem 69(3):1196–1203
Keeney PM, Xie J, Capaldi RA, Bennett JP Jr (2006) Parkinson’s disease brain mitochondrial complex I has oxidatively damaged subunits and is functionally impaired and misassembled. J Neurosci 26(19):5256–5264. doi:10.1523/JNEUROSCI.0984-06.2006
Schapira AH, Cooper JM, Dexter D, Clark JB, Jenner P, Marsden CD (1990) Mitochondrial complex I deficiency in Parkinson’s disease. J Neurochem 54(3):823–827
Braak H, Del Tredici K, Rub U, de Vos RA, Jansen Steur EN, Braak E (2003) Staging of brain pathology related to sporadic Parkinson’s disease. Neurobiol Aging 24(2):197–211
Mythri RB, Venkateshappa C, Harish G, Mahadevan A, Muthane UB, Yasha TC, Srinivas Bharath MM, Shankar SK (2011) Evaluation of markers of oxidative stress, antioxidant function and astrocytic proliferation in the striatum and frontal cortex of Parkinson’s disease brains. Neurochem Res 36(8):1452–1463. doi:10.1007/s11064-011-0471-9
Mattson MP, Furukawa K (1998) Signaling events regulating the neurodevelopmental triad. Glutamate and secreted forms of beta-amyloid precursor protein as examples. Perspect Dev Neurobiol 5(4):337–352
Brown MR, Sullivan PG, Geddes JW (2006) Synaptic mitochondria are more susceptible to Ca2+ overload than nonsynaptic mitochondria. J Biol Chem 281(17):11658–11668. doi:10.1074/jbc.M510303200
Naga KK, Sullivan PG, Geddes JW (2007) High cyclophilin D content of synaptic mitochondria results in increased vulnerability to permeability transition. J Neurosci 27(28):7469–7475. doi:10.1523/jneurosci.0646-07.2007
Chandana R, Mythri RB, Mahadevan A, Shankar SK, Srinivas Bharath MM (2009) Biochemical analysis of protein stability in human brain collected at different post-mortem intervals. Indian J Med Res 129(2):189–199
Chinta SJ, Kommaddi RP, Turman CM, Strobel HW, Ravindranath V (2005) Constitutive expression and localization of cytochrome P-450 1A1 in rat and human brain: presence of a splice variant form in human brain. J Neurochem 93(3):724–736. doi:10.1111/j.1471-4159.2005.03061.x
Cash AD, Perry G, Ogawa O, Raina AK, Zhu X, Smith MA (2002) Is Alzheimer’s disease a mitochondrial disorder? Neurosci Rev J Brin Neurobiol Neurol Psychiatry 8(5):489–496
Onyango I, Khan S, Miller B, Swerdlow R, Trimmer P, Bennett P Jr (2006) Mitochondrial genomic contribution to mitochondrial dysfunction in Alzheimer’s disease. J Alzheimers Dis 9(2):183–193
Reddy PH, Beal MF (2005) Are mitochondria critical in the pathogenesis of Alzheimer’s disease? Brain Res Brain Res Rev 49(3):618–632. doi:10.1016/j.brainresrev.2005.03.004
Forero DA, Casadesus G, Perry G, Arboleda H (2006) Synaptic dysfunction and oxidative stress in Alzheimer’s disease: emerging mechanisms. J Cell Mol Med 10(3):796–805
Urano S, Asai Y, Makabe S, Matsuo M, Izumiyama N, Ohtsubo K, Endo T (1997) Oxidative injury of synapse and alteration of antioxidative defense systems in rats, and its prevention by vitamin E. Eur J Biochem 245(1):64–70
Martinez M, Ferrandiz ML, Diez A, Miquel J (1995) Depletion of cytosolic GSH decreases the ATP levels and viability of synaptosomes from aged mice but not from young mice. Mech Ageing Dev 84(1):77–81
Karunakaran S, Saeed U, Ramakrishnan S, Koumar RC, Ravindranath V (2007) Constitutive expression and functional characterization of mitochondrial glutaredoxin (Grx2) in mouse and human brain. Brain Res 1185:8–17. doi:10.1016/j.brainres.2007.09.019
Karunakaran S, Saeed U, Mishra M, Valli RK, Joshi SD, Meka DP, Seth P, Ravindranath V (2008) Selective activation of p38 mitogen-activated protein kinase in dopaminergic neurons of substantia nigra leads to nuclear translocation of p53 in 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine-treated mice. J Neurosci 28(47):12500–12509. doi:10.1523/jneurosci.4511-08.2008
Alladi PA, Mahadevan A, Yasha TC, Raju TR, Shankar SK, Muthane U (2009) Absence of age-related changes in nigral dopaminergic neurons of Asian Indians: relevance to lower incidence of Parkinson’s disease. Neuroscience 159(1):236–245. doi:10.1016/j.neuroscience.2008.11.051
Douglas MS (1983) Rapid, quantitative isolation of mitochondria from rat liver using Ficoll gradients in vertical rotors. Anal Biochem 131(2):453–457. doi:10.1016/0003-2697(83)90198-7
Frasca JM, Parks VR (1965) A routine technique for double-staining ultrathin sections using uranyl and lead salts. J Cell Biol 25:157–161
Harish G, Venkateshappa C, Mahadevan A, Pruthi N, Bharath MM, Shankar SK (2012) Mitochondrial function in human brains is affected by pre and postmortem factors. Neuropathol Appl Neurobiol. doi:10.1111/j.1365-2990.2012.01285.x
Harish G, Venkateshappa C, Mahadevan A, Pruthi N, Bharath MM, Shankar SK (2012) Effect of pre and postmortem factors on the distribution and preservation of antioxidant activities in the cytosol and synaptosomes of human brains. Biopreserv Biobank 10(3):253–265. doi:10.1089/bio.2012.0001
Bradford MM (1976) A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem 72:248–254
Jagatha B, Mythri RB, Vali S, Bharath MM (2008) Curcumin treatment alleviates the effects of glutathione depletion in vitro and in vivo: therapeutic implications for Parkinson’s disease explained via in silico studies. Free Radic Biol Med 44(5):907–917. doi:10.1016/j.freeradbiomed.2007.11.011
Bagnyukova TV, Storey KB, Lushchak VI (2003) Induction of oxidative stress in Rana ridibunda during recovery from winter hibernation. J Therm Biol 28:21–28
Tietze F (1969) Enzymic method for quantitative determination of nanogram amounts of total and oxidized glutathione: applications to mammalian blood and other tissues. Anal Biochem 27(3):502–522
Hissin PJ, Hilf R (1976) A fluorometric method for determination of oxidized and reduced glutathione in tissues. Anal Biochem 74(1):214–226
Flohe L, Gunzler WA (1984) Assays of glutathione peroxidase. Methods Enzymol 105:114–121
Carlberg I, Mannervik B (1985) Glutathione reductase. Methods Enzymol 113:484–490
Guthenberg C, Alin P, Mannervik B (1985) Glutathione transferase from rat testis. Methods Enzymol 113:507–510
Cohen G, Farooqui R, Kesler N (1997) Parkinson disease: a new link between monoamine oxidase and mitochondrial electron flow. Proc Natl Acad Sci USA 94(10):4890–4894
Srere PA (1969) [1] Citrate synthase: [EC 4.1.3.7. Citrate oxaloacetate-lyase (CoA-acetylating)]. In: John ML (ed) Methods in enzymology, Vol 13. Academic Press, Waltham, pp 3–11
Pennington RJ (1961) Biochemistry of dystrophic muscle. Mitochondrial succinate-tetrazolium reductase and adenosine triphosphatase. Biochem J 80:649–654
Kitto GB, Lewis RG (1967) Purification and properties of tuna supernatant and mitochondrial malate dehydrogenases. Biochimica et Biophysica Acta (BBA)-Enzymol 139(1):1–15. doi:10.1016/0005-2744(67)90107-6
Albers DS, Beal MF (2000) Mitochondrial dysfunction and oxidative stress in aging and neurodegenerative disease. J Neural Transm Suppl 59:133–154
Banerjee R, Starkov AA, Beal MF, Thomas B (2009) Mitochondrial dysfunction in the limelight of Parkinson’s disease pathogenesis. Biochim Biophys Acta 1792(7):651–663. doi:10.1016/j.bbadis.2008.11.007
Lin MT, Beal MF (2006) Mitochondrial dysfunction and oxidative stress in neurodegenerative diseases. Nature 443(7113):787–795. doi:10.1038/nature05292
Choi SW, Gerencser AA, Lee DW, Rajagopalan S, Nicholls DG, Andersen JK, Brand MD (2011) Intrinsic bioenergetic properties and stress sensitivity of dopaminergic synaptosomes. J Neurosci 31(12):4524–4534. doi:10.1523/jneurosci.5817-10.2011
Ansari MA, Scheff SW (2010) Oxidative stress in the progression of Alzheimer disease in the frontal cortex. J Neuropathol Exp Neurol 69(2):155–167. doi:10.1097/NEN.0b013e3181cb5af4
Pocernich CB, Cardin AL, Racine CL, Lauderback CM, Butterfield DA (2001) Glutathione elevation and its protective role in acrolein-induced protein damage in synaptosomal membranes: relevance to brain lipid peroxidation in neurodegenerative disease. Neurochem Int 39(2):141–149
Roychowdhury S, Wolf G, Keilhoff G, Horn TF (2003) Cytosolic and mitochondrial glutathione in microglial cells are differentially affected by oxidative/nitrosative stress. Nitric Oxide 8(1):39–47
Schnellmann RG, Gilchrist SM, Mandel LJ (1988) Intracellular distribution and depletion of glutathione in rabbit renal proximal tubules. Kidney Int 34(2):229–233
Radunovic A, Porto WG, Zeman S, Leigh PN (1997) Increased mitochondrial superoxide dismutase activity in Parkinson’s disease but not amyotrophic lateral sclerosis motor cortex. Neurosci Lett 239(2–3):105–108
Harish G, Venkateshappa C, Mahadevan A, Pruthi N, Bharath MMS, Shankar SK (2011) Effect of storage time, postmortem interval, agonal state, and gender on the postmortem preservation of glial fibrillary acidic protein and oxidatively damaged proteins in human brains. Biopreserv Biobank 9(4):379–387. doi:10.1089/bio.2011.0033
Harish G, Venkateshappa C, Mahadevan A, Pruthi N, Srinivas Bharath MM, Shankar SK (2011) Glutathione metabolism is modulated by postmortem interval, gender difference and agonal state in postmortem human brains. Neurochem Int 59(7):1029–1042. doi:10.1016/j.neuint.2011.08.024
Gomez A, Ferrer I (2010) Involvement of the cerebral cortex in Parkinson disease linked with G2019S LRRK2 mutation without cognitive impairment. Acta Neuropathol 120(2):155–167. doi:10.1007/s00401-010-0669-y
Riederer BM (1989) Antigen preservation tests for immunocytochemical detection of cytoskeletal proteins: influence of aldehyde fixatives. J Histochem Cytochem 37(5):675–681
Sofic E, Lange KW, Jellinger K, Riederer P (1992) Reduced and oxidized glutathione in the substantia nigra of patients with Parkinson’s disease. Neurosci Lett 142(2):128–130
Acknowledgments
This work was financially supported by a research grant from the Indian Council of Medical Research (ICMR IRIS ID No. 2009-07710), India, to MMSB. GH is a senior research fellow of ICMR, India. We thank all the donors and their relatives for donating human brain tissue samples for this study. Human brain tissues for the study were sourced from Human Brain Tissue Repository for Neurobiological Studies (A National Research Facility), Department of Neuropathology, NIMHANS, Bangalore–560 029. We thank Dr. Uday Muthane for his help regarding neurological analysis of the PD samples used in the current study. GH and MMSB designed the study. GH carried out the biochemical work. SKS and AM provided the tissue samples and carried out the neuropathological analysis. MMSB and GH analyzed the data. MMSB wrote the paper, while the co-authors assisted in editing it.
Conflict of interest
The authors declare that there are no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Harish, G., Mahadevan, A., Srinivas Bharath, M.M. et al. Alteration in Glutathione Content and Associated Enzyme Activities in the Synaptic Terminals but not in the Non-synaptic Mitochondria from the Frontal Cortex of Parkinson’s Disease Brains. Neurochem Res 38, 186–200 (2013). https://doi.org/10.1007/s11064-012-0907-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-012-0907-x