Abstract
Long-term treatment of l-dopa for Parkinson’s disease (PD) patients induces adverse effects, including dyskinesia, on–off and wearing-off symptoms. However, the cause of these side effects has not been established to date. In the present study, therefore, 3-O-methyldopa (3-OMD), which is a major metabolite of l-dopa, was tested to determine whether it plays a role in the aforementioned adverse effects. The effects of 3-OMD on the dopaminergic nervous system in the brain were investigated, by examining behavioral, biochemical, and cellular changes in male Sprague–Dawley rats and catecholamine-producing PC12 neuronal cells. The results revealed that the intracerebroventricular (icv) injection of 1 μmol of 3-OMD impaired locomotor activities by decreasing movement time (MT), total distance (TD), and the number of movement (NM) by 70, 74 and 61%, respectively. The biochemical analysis results showed that a single administration of 1 μmole of 3-OMD decreased the dopamine turnover rate (DOPAC/DA) by 40.0% in the rat striatum. 3-OMD inhibited dopamine transporter and uptake in rat brain striatal membranes and PC12 cells. The subacute administration of 3-OMD (5 days, icv) also significantly impaired the locomotor activities and catecholamine levels. 3-OMD induced cytotoxic effects via oxidative stress and decreased mitochondrial membrane potential in PC12 cells, indicating that 3-OMD can damage neuronal cells. Furthermore, 3-OMD potentiated l-dopa toxicity and these toxic effects induced by both 3-OMD and l-dopa were blocked by vitamin E (α-tocopherol) in PC12 cells, indicating that 3-OMD may increase the toxic effects of l-dopa to some extent by oxidative stress. Therefore, the present study reveals that 3-OMD accumulation from long-term l-dopa treatment may be involved in the adverse effects of l-dopa therapy. Moreover, l-dopa treatment might accelerate the progression of PD, at least in part, by 3-OMD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
3-O-Methyldopa (3-OMD) is a major metabolite of l-dopa, which is used to increase dopamine in the therapy of PD. It is detected in high levels in the plasma as well as the cerebral spinal fluid of PD patients treated with l-dopa [1–4]. 3-OMD is formed by catecholamine-O-methyltransferase (COMT, EC 2.1.1.6, Fig. 1A and B) from l-dopa in many organs including blood, peripheral tissues, and nigrostriatal neurons [5]. l-dopa is commonly administered with dopa decarboxylase inhibitors (DDI), such as carbidopa or benserazide, to increase the availability of l-dopa in the brain, resulting in the accumulation of 3-OMD in the brain. Moreover, while the half-life of l-dopa is about 1 h, that of 3-OMD is 15 h, which leads to its accumulation in the plasma and brain of the patients in chronic l-dopa treatment [6]. As a result, the ratio of mean plasma 3-OMD to l-dopa concentration can be as high as 14:1 [7].
(A) Synthesis of 3-OMD and homocysteine in l-dopa treatment. (B) Metabolic pathway of l-dopa. Enzymes: 1: methionine adenosyltransferase; 2: catechol-O-methyltransferase; 3: SAH hydrolase; and 4: methionine synthase. Abbreviation: AADC, aromatic amino acid decarboxylase; DA, dopamine; 3-MT, 3-methoxytyramine; SAM, S-adenosylmethionine; SAH, S-adenosylhomocysteine
There is growing evidence that 3-OMD might be involved in the side effects of chronic treatment of l-dopa. The plasma levels of 3-OMD from patients with dyskinesias which is one of the side effects of l-dopa treatment [8] were significantly higher than those from patients without dyskinesias. This high 3-OMD level is possibly caused by a progressive accumulation due to its long half-life [9, 10]. In addition to the absolute higher levels of 3-OMD, high ratios of 3-OMD to l-dopa were also found to be related to dyskinesia [11] and poor response to l-dopa [12]. PD patients with the wearing-off phenomenon had higher concentrations of 3-OMD than patients without the wearing-off complication, implicating that 3-OMD might be associated with l-dopa-related motor dysfunction [13]. The proportion of 3-OMD to dopamine was much greater in patients exhibiting the wearing-off effects after l-dopa treatment.
3-OMD may interfere with l-dopa response by several different mechanisms [14, 15]. 3-OMD inhibits striatal uptake of tyrosine and the utilization of l-dopa, resulting in the inhibition of l-dopa metabolism to DA [16]. Furthermore, 3-OMD competes with l-dopa for the blood–brain barrier transporter system [17]. l-dopa treatment also decreases SAM levels and increases SAH levels due to higher methylation activity of COMT [5]. Consequently, l-methionine S-adenosyltransferase (MAT) activity was elevated in PD patients and animals with l-dopa treatment, providing evidence that COMT-mediated methylation activity was increased to metabolize excess amount of l-dopa in PD patients [18, 19]. A significant reduction in dopamine efflux from striatal tissue slices after l-dopa superfusion in the presence of 3-OMD indicates that 3-OMD might inhibit dopamine release [20].
While it remains as a primary choice for PD treatment, l-dopa may induce toxic effects by itself as well as indirectly via its metabolites, 3-OMD and/or homocysteine. Several in vitro studies have reported that l-dopa is toxic to neuronal cells, suggesting that long-term treatment of l-dopa to PD patients may exacerbate the progression of the disease [21]. However, there is controversy over whether l-dopa treatment in PD patients is toxic since some studies have reported that l-dopa is nontoxic or neuroprotective [22–24]. There is no clear demonstration of l-dopa-induced dopaminergic cell death in human Parkinsonians and l-dopa may even slow the progression of PD [25]. Nonetheless, l-dopa itself induces oxidative stress and apoptosis, leading to cell death in vitro [26]. Moreover, a chronic treatment of l-dopa to the PD patients significantly increases the levels of 3-OMD as well as homocysteine [27]. Since it is well known that homocysteine induces cardiovascular disease as well as neuronal damages [28, 29], it is of particular significance to note that PD patients with chronic l-dopa treatment retain abnormally high levels of l-dopa, homocysteine and 3-OMD [27].
Molecular and cellular mechanisms of 3-OMD action, alone or with l-dopa, have not completely been established. It has been reported that both l-dopa and 3-OMD induce oxidative DNA damage, which might lead to cell death [30]. PD patients treated with l-dopa demonstrated positive correlations between reactive oxygen species and 3-OMD levels, compared to the controls or untreated PD patients [31, 32]. This result indicates that l-dopa may promote free radical formation in PD patients and 3-OMD may also play a role in this process.
In the present study, therefore, we examined the involvement of 3-OMD in the adverse effects of chronic l-dopa treatment, focusing on the locomotor activities and the dopaminergic neurotransmission system in rats. To further investigate the cellular mechanism of 3-OMD-mediated toxic effects in l-dopa treatment, we also used PC12 cells, derived from rat pheochromocytoma, which possessed catecholaminergic neuronal characteristics.
Materials and methods
Chemicals
Homocysteine, 3-O-methyldopa, adenosine, dopamine, 3,4-dihydroxyphenylacetic acid (DOPAC), homovanillic acid (HVA), tri-n-butylphosphine, trichloroacetic acid, sodium borate, EDTA, methanol, acetonitrile, resazurin, and rhodamine 123 were obtained from Sigma Chemical Co. (St. Louis, MO, USA). 2′,7′-dichlorofluorescin diacetate (H2DCF-DA) was purchased from Molecular Probes (Eugene, OR, USA). Phosphoric acid, perchloric acid, citric acid, and other materials were obtained from Fisher Scientific (Pittsburgh, PA, USA).
Animals
Male Sprague–Dawley rats weighing 180–200 g were purchased from Harlan (Indianapolis, IN). Animals were kept in the animal care facility until the beginning of experiments and had access to food and water ad libitum, under a 12 h light/dark cycle. Temperature was maintained at 21 ± 1°C.
Cell culture
PC12 cells were purchased from American Type Culture Collection (ATCC, Rockville, MD, USA). PC12 cells are catecholamine-secreting neuronal cell lines and widely used to study neuronal toxicity mechanisms [33]. PC12 cells during their exponential phase of growth were maintained in a tissue culture flask in an atmosphere of 5% CO2/95% air in RPMI 1640 medium containing 10% horse serum, 5% fetal bovine serum, 100 U/ml penicillin, 100 μg/ml streptomycin, and 250 ng/ml amphotericin B. For the experiments, PC12 cells (5 × 105 cells/ml) were treated with 100 μg/L nerve growth factor (NGF) in collagen-coated plates for 5 days and medium was changed every 3 days until the experiments were conducted.
Cannulation of rats
Rats weighing 250–300 g were anesthesized with chloral hydrate (400 mg/kg, i.p.). A 22-guage stainless steel cannula was stereotaxically implanted for injections into the lateral ventricle of the rat brain. The position for cannula was at 1.5 mm lateral and 0.6 mm caudal with reference to the bregma from which it extended to the lateral ventricles. After the cannulations, rats were allowed to recover for 3 days before the experiments. Drugs were injected into the lateral ventricle 5 mm from the surface of the cranium through polyethylene tube (PE 20) which was attached to a 10 μl Hamilton syringe.
Measurement of locomotor activities
Phosphate buffered saline (PBS) was used as a control and homocysteine, 3-O-methyldopa, or adenosine was dissolved in PBS. After the rats were injected (icv) with PBS, homocysteine, 3-O-methyldopa, or adenosine in 5 μl of volume, rats were placed in the locomotor activity monitor. The measurement was started 5 min after the placement of animals into the monitor in a quiet isolated place with a dim light. The changes in motor activity of the animals were measured using Activity Monitor (Degiscan Instruments, Inc., Columbus, OH, USA). Movement time (MT), total distance (TD), and the number of movements (NM) were determined. The locomotor activities were determined for 40 min post-injection.
HPLC analysis
For the measurements of DA and its metabolites, DOPAC, after the last injections, animals were sacrificed and the striatal and midbrain regions were dissected. The dissected tissues were homogenized using Polytron in 0.4 M perchloric acid, centrifuged, and filtered for HPLC analysis as described previously [34]. The HPLC system (LC-10 AT, Shimadzu) was connected with an electrochemical detector (Coulochem II, ESA), using a C-18 reverse-phase column (5 μm, 250 × 4.6 mm, Whatman EQC). The mobile phase consisted of 0.1 M sodium acetate, 60 mM citric acid, 0.6 mM octanesulfonic acid sodium salt, 0.5 mM disodium EDTA, in 15% methanol in water, pH 3.5 and pumped at a rate of 1.0 ml/min.
Dopamine D1 receptor binding assay
Male Sprague–Dawley rat brains were obtained by cervical dislocation and the striatal regions were dissected out. Rat striatal tissue was manually homogenized with a Wheaton Teflon-on glass tissue homogenizer (20 up and down strockes) in 50 mM Tris–HCl buffer containing 1 mM EDTA, 5 mM KCl, 1.5 mM CaCl2, 4 mM MgCl2, and 120 mM NaCl, pH 7.4 at 4°C. Tissue homogenates in 50 volume of Tris–HCl buffer were centrifuged at 20,000 × g for 20 min at 4°C and the pellet was washed with the same buffer twice, followed by resuspension in fresh Tris–HCl buffer, pH 7.4 to a final concentration of about 50 mg/ml using previously described method with some modifications [35]. Briefly, 0.7 nM of dopamine D1 ligand [3H]SCH 23390 (85 Ci/mmol) was incubated with the rat brain striatal tissue membrane preparation (300–500 μg of protein) in 50 mM Tris–HCl buffer at pH 7.5 with various concentrations of 3-OMD in a final volume of 500 μl. SCH 23390 (1 μM) was used for non-specific binding. The reaction was carried out in a shaking water bath at 37°C for 30 min and terminated by rapid filtration on Whatman GF/B filters that were pretreated with 0.5% polyethylenimine in Tris–HCl buffer solution in Cell Harvester (Brandel, M-48TI). The filters containing the bound radioactivity were washed twice with 4 ml ice-cold 50 mM Tris–HCl buffer, pH 7.4. The membrane filters were then transferred to 5 ml liquid scintillation cocktail (Scinte Verse-E). Radioactivity was measured in a liquid scintillation counter (Beckman, LS 6500).
Dopamine transporter assay
The rat brain striatal regions were homogenized in 50 volume of buffer (50 mM Tris–HCl, 120 mM NaCl, 5 mM KCl), pH 7.9 at 4°C and tissue membrane was prepared as described previously in dopamine receptor binding section. Aliquots of striatal tissue membrane preparation were incubated with 80 nM of [3H]mazindol, 300 nM of desipramine to block norepinephrine transporters in the presence of various concentrations of 3-OMD in a final volume of 500 μl at 4°C for 1 h. The reactions were terminated by rapid filtration and the filters containing the bound radioactivity were counted in a scintillation counter as described in the dopamine binding section.
Dopamine uptake assay
Dopamine uptake assay was performed according to the method of Woodgate et al. [36] with a slight modification. PC12 cells (1 × 106 cells/ml) were plated in 6-well plates and incubated with various concentrations of 3-OMD in a total volume of 1 ml in Krebs–Ringer–HEPES (KRH) buffer, which consisted of 120 mM NaCl, 5.4 mM KCl, 1.0 mM CaCl2, 0.8 mM MgCl2, 11.1 mM glucose, 20 mM Hepes, (pH 7.4), containing [3H]dopamine (0.5 μCi/ml) for 30 min at room temperature and washed with fresh KRH buffer three times. The pellets were solubilized with 0.5 ml of 2% SDS solution and transferred to tubes. Five milliliters of scintillation fluid was added to each tube and radioactivity was counted in a scintillation counter (LS 6500, Beckman).
Cell viability assay
Cell viability was assessed by alamar blue assay using resazurin as a dye indicator. In brief, after PC12 cells (5 × 105 cells/ml) were treated with various compounds in DMEM/F12 media which contains 17.5 mM glucose in 96-well plates, resazurin dye was added to the culture media to test the cell viability. In this assay, the dye solution was added to the culture medium in a final concentration of 50 μg/ml and incubated for 4–8 h at 37°C. After incubation, the fluorescence produced by the esterase from the live cells was measured in a fluorometer (Model 7620, Cambridge Tech) with settings at 550/580 nm (excitation/emission).
Detection of intracellular ROS formation
The dye H2DCF-DA, which is oxidized to fluorescent DCF by hydroperoxides, was used to measure relative levels of cellular peroxides [37]. After PC12 cells (5 × 105 cells/ml) were incubated with compounds in 6-well plates for 24 h in low serum (2%) DMEM/F12 experimental media, cells were treated with H2DCF-DA dye in a final concentration of 25 μM for 30 min at 37°C. PC12 cells were washed twice with PBS by centrifugation at 400 × g for 10 min and cell pellets were dissolved in 1% Triton X-100. Fluorescence was measured at wavelengths of 480/530 nm (excitation/emission) in a fluorometer (Model 7620, Cambridge Tech, Watertown, MA, USA).
Measurement of mitochondrial membrane potential
The mitochondrial membrane potential in PC12 cells was measured using rhodamine 123 dye [37]. The uptake of rhodamine 123 into mitochondria is a function of the mitochondrial membrane potential [38]. After treated with compounds for the indicated period in DMEM/F12 media, PC12 cells (5 × 105 cells/ml) were incubated in 6-well plates with rhodamine 123 dye in a final concentration of 10 μM for 30 min at 37°C. Cells were washed twice with PBS by centrifugation at 400 × g for 10 min. Following aspiration of medium, cells were dissolved with 1% Triton X-100 and fluorescence was measured at sets of 480/530 nm (excitation/emission) in a fluorometer (Model 7620, Cambridge Tech, Watertown, MA, USA).
Statistical analysis
The mean and standard error of the mean (SEM) were determined for each set of data and one-way analysis of variance (ANOVA) followed by Newman–Keuls post-hoc test was used for statistical analysis to compare control and treated groups. A probability of 0.05 or less was considered significant.
Results
Effects of metabolites of l-dopa on the locomotor activities and dopamine turnover in rats
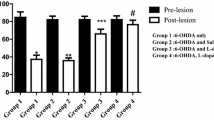
The administration of l-dopa may increase the levels of 3-OMD, adenosine and homocysteine (Fig. 1A and B). The elevation of 3-OMD and homocysteine levels in PD patients who have been taking l-dopa has been previously reported [27]. One micromole of each metabolite was injected to the lateral ventricles of rat brain (icv) and locomotor activities were measured for 40 min after 5 min post-injection. The results showed that 3-OMD among the three compounds significantly decreased the locomotor activities in rats. 3-OMD decreased movement time (MT) by 70%, number of movement (NM) by 74% and total distance (TD) by 61%, respectively (Fig. 2). Correspondingly, 3-OMD decreased dopamine turnover rate by 39.7% in rat striatum (Table 1). These results indicate that the increase of 3-OMD affects movement functions, corresponding to the alteration of dopamine turnover rate.
Effects of 3-O-methyldopa (3-OMD), homocysteine, and adenosine on movement time (MT), total distance (TD), and number of movements (NM) in rats. Each compound was dissolved in PBS and 5 μl containing 1 μmol of each compound was injected into the rat brains by icv route as described in “Materials and methods” section. Locomotor activities were recorded for 40 min, 5 min post-injection. Values are expressed as means ± SEM (N = 8). One-way ANOVA followed by Newman–Keuls test was used for statistical analysis to compare control and treated groups. *Significant decreases compared to the control (**P < 0.01).
Effect of 3-OMD on dopamine receptor/transporter binding activities and dopamine uptake
As shown in Fig. 3, 3-OMD did not alter dopamine receptor binding activity (Fig. 3A), but it inhibited dopamine transporter activity in rat brain striatal tissue preparation. Concentrations of 3-OMD at 125, 250, 500, and 1,000 μM decreased the binding activity of mazindol, which is a specific ligand for dopamine transporter, by 21.5, 27.7, 33.5, and 45.1%, respectively (Fig. 3B). 3-OMD also significantly decreased DA uptake in PC12 cells. The same range of 3-OMD concentrations decreased DA uptake by 12.65, 17.1, 32.6, and 42%, respectively (Fig. 3C).
(A) Effect of 3-OMD on [3H]SCH 23390 specific binding activities to dopamine D1 receptors in rat brain striatal membrane preparation. (B) Effect of 3-OMD on [3H]mazindol binding activities to dopamine transporter in rat brain striatal membrane preparation. For (A) and (B), various concentrations of 3-OMD were incubated with striatal tissue membrane preparation to study the effects of 3-OMD on dopamine transporter or D1 receptor activities using mazindol or SCH 23390 which is a specific ligand for dopamine transporter oe D1 receptor as described in the “Materials and methods” section. Values are means of quadruplicate determination in a representative of three experiments with standard errors. (C) Effect of 3-OMD on dopamine uptake in PC12 cells. PC12 cells (1 × 106 cells/ml) were incubated with various concentrations of 3-OMD in a total volume of 1 ml in Krebs–Ringer–HEPES (KRH) buffer, which consisted of 120 mM NaCl, 5.4 mM KCl, 1.0 mM CaCl2, 0.8 mM MgCl2, 11.1 mM glucose, 20 mM Hepes, (pH 7.4), containing [3H]dopamine (0.5 μCi/ml) for 30 min at room temperature as described in “Materials and methods” section. The values are means ± SEM of ten replicate determinations. *Significantly different form the control (*P < 0.05, one-way ANOVA test followed by Newman–Keuls post analysis)
Repeated injections of 3-OMD on locomotor activities and catecholamine levels in rat brain
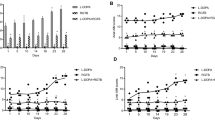
The repeated injection of 3-OMD into the rat brain decreased all the measures of locomotor activities in a dose-dependent manner (Fig. 4). The degree of decrease was less than the changes that occurred following a single administration of 3-OMD, indicating that compensating mechanism might play a role in these effects. Dopamine and its metabolite, DOPAC, were also significantly decreased by five consecutive icv injections of 3-OMD into the rat brain (Fig. 5). The 1 or 2 μmol doses of 3-OMD decreased DA in the midbrain by 8 or 65% and by 30 or 32% in the striatum. DOPAC was also dose-dependently decreased (Fig. 5).
Effect of 3-OMD on the locomotor activities after 5 days of consecutive treatments (icv) in rats. One or two micromoles of 3-OMD was injected into the rat brains by icv route daily for 5 days and 24 h after the last injection rats were placed in the locomotor activity monitor for the measurement of locomotor activities. Movement time, total distances, and the number of movements were recorded for 40 min 5 min-post injection. Values are expressed as means ± SEM (N = 6). One-way ANOVA followed by Newman–Keuls test was used for statistical analysis to compare control and treated groups. *Significantly decreased compared to the control (*P < 0.05, **P < 0.01)
Effect of 3-OMD on the levels of dopamine and its metabolite, DOPAC, after 5 days of consecutive treatments (icv) in the midbrain and striatal regions of rat brain. Two doses (1 or 2 μmol) of 3-OMD were injected into the rat brains by icv route daily for 5 days and 24 h after the last injection rats were decapitated and the midbrain and striatal regions were dissected. After sample preparations for HPLC, the levels of dopamine and DOPAC were measured in HPLC with an electrochemical detector. Values are expressed as means ± SEM (N = 6). One-way ANOVA followed by Newman–Keuls test was used for statistical analysis to compare different groups. *Significantly decreased compared to the control (*P < 0.05, **P < 0.01)
Effect of 3-OMD on PC12 catecholaminergic neuronal cells
3-OMD decreased the locomotor activities and catecholamine levels in a single as well as repeated treatment in vivo, indicative of changes occurring at the level of the dopaminergic cells. Accordingly, the effects of 3-OMD on PC12 cells were tested to determine whether 3-OMD may affect dopaminergic neurons where its concentration would accumulate high due to l-dopa metabolism in dopaminergic neurons. PC12 cells produce catecholamines, including dopamine, and are widely used to test dopaminergic functions in vitro [39]. The results showed that 3-OMD decreased cell viability in a dose-dependent manner at concentrations from about 1 mM in the present experimental conditions (Fig. 6). 3-OMD induced the formation of reactive oxygen species (ROS) significantly starting at 1 mM while decreasing mitochondrial membrane potential at concentrations from 0.5 mM, indicating that 3-OMD induces mitochondrial impairments as well as oxidative stress (Fig. 7).
Effect of 3-OMD on cell viability in PC12 cells. PC12 cells (5 × 105 cells/ml) were incubated with various concentrations of 3-OMD for the indicated time periods in 96-well plates at 37°C and cell viability was assessed by alamar blue assay using resazurin dye indicator as described in “Materials and methods” section. *Significantly decreased compared to the control (*P < 0.05, **P < 0.01, ***P < 0.001)
(A) Effect of 3-OMD on the formation of ROS in PC12 cells. After PC12 cells (1 × 106 cells/ml) were incubated with 3-OMD for 24 h at 37°C, cells were treated with H2DCF-DA in a final concentration of 25 μM for 30 min at 37°C. Cells were washed with PBS twice and solubilized with 1% triton X-100. Fluorescence was measured at 480–530 nm (excitation/emission). (B) Effect of 3-OMD on mitochondrial membrane potential in PC12 cells. After cells (1 × 106 cells/ml) were incubated with compounds for 24 h at 37°C in 6-well plates, rhodamine 123 was added into the cell culture media in a final concentration of 10 μM and incubated for 30 min at 37°C. Cells were washed with PBS twice followed by being dissolved in 1% triton X-100, and fluorescence was measured at 480–530 nm (excitation/emission). *Significantly decreased compared to the control (*P < 0.05, **P < 0.01, ***P < 0.001)
Potentiative effects of 3-OMD in l-dopa-induced toxicity in PC12 cells
This experiment was designed to determine whether 3-OMD has synergistic or additive effects with l-dopa because l-dopa is taken in large amounts by the PD patients to achieve its efficacy and both would be in high amounts in dopaminergic neurons. There is a dramatic increase of 3-OMD in plasma and CSF of PD patients following l-dopa therapy due to its 15 h long half-life and, therefore, these two compounds are coexisting in high concentrations in the body and might cause additive toxic effects [6]. As shown in Fig. 8A, 0.5 mM of 3-OMD did not show any toxic effect, but it did potentiate the toxic effect of l-dopa significantly at concentrations of 63 μM and higher. This potentiative effect of 3-OMD on l-dopa toxicity might be due to the ROS formation because the concurrent treatments of PC12 cells with 0.5 mM 3-OMD and l-dopa significantly increased ROS formation (Fig. 8B).
Potentiative effects of 3-OMD in l-dopa-induced toxicity in PC12 cells. (A) Potentiative effects of 3-OMD in l-dopa-induced cytotoxicity in PC12 cells. Cells (5 × 105 cells/ml) were incubated with 0.5 mM 3-OMD and various concentrations of l-dopa for 24 h at 37°C. Cell viability was assessed by alamar blue assay as described in “Materials and methods” section. *Significantly decreased compared to the each corresponding concentration of l-dopa alone (*P < 0.05, ***P < 0.001). (B) Potentiative effects of 3-OMD in l-dopa-induced ROS formation in PC12 cells. After PC12 cells (1 × 106 cells/ml) were incubated with 3-OMD or/and l-dopa for 24 h at 37°C, cells were treated with H2DCF-DA in a final concentration of 25°μM for 30 min at 37°C. Cells were washed with PBS twice and solubilized with 1% triton X-100. Fluorescence was measured at 480–530 nm (excitation/emission). *Significantly decreased compared to the control (**P < 0.01, ***P < 0.001)
Protective effects of α-tocopherol (vitamin E) on 3-OMD and l-dopa-induced cytoxicity in PC12 cells
This experiment was designed to determine whether antioxidants can prevent the toxic effects of 3-OMD and/or l-dopa in PC12 cells. The data showed that α-tocopherol prevented the cytotoxic effects of 3-OMD/l-dopa at concentrations from 25 μM. The results indicate that α-tocopherol is a potent antioxidant and oxidative stress might play a role in 3-OMD/l-dopa-induced toxicity mechanism (Fig. 9).
Protective effects of α-tocopherol (vitamin E) on 3-OMD and l-dopa-induced cytoxicity in PC12 cells. Cells (5 × 105/ml) were treated with 3-OMD or/and l-dopa in the presence of various concentrations of α-tocopherol for 24 h at 37°C. Cell viability was determined by resazurin dye indicator. M: mixture of l-dopa 125 μM and 3-OMD 1 mM. *Significantly different form the control (*P < 0.05, One-way ANOVA test followed by Newman–Keuls post analysis)
Discussion
The results of the present study show that 3-OMD significantly decreased the locomotor activities and dopamine turnover in rats. 3-OMD also appeared to inhibit dopamine transporters and dopamine uptake functions. These results indicate that 3-OMD, the major metabolite of l-dopa, might play a role in l-dopa-induced side effects in PD patients. Moreover, the cytotoxic effects of 3-OMD by oxidative stress, along with mitochondrial impairment and its potentiative effects on l-dopa toxicity, suggest that the accumulation of 3-OMD in l-dopa therapy may accelerate the progression of the disease.
Several clinical data have shown that 3-OMD might play a role in l-dopa-induced side effects [40]. Patients with higher COMT activity, which leads to an increase of 3-OMD formation in the erythrocytes of PD patients, showed less favorable clinical responses to l-dopa, implicating that high levels of 3-OMD might be associated with l-dopa-induced adverse effects [40]. The ratio of 3-OMD to l-dopa (3-OMD/l-dopa) in the brain and plasma might also be an important parameter because the patients who had higher 3-OMD concentration ratios to l-dopa (3-OMD/l-dopa) did not respond to l-dopa [41].
The pharmacological actions of 3-OMD in PD patients taking l-dopa may involve multiple mechanisms. 3-OMD has been suggested to compete with l-dopa for the uptake into the brain via the blood–brain barrier (BBB) [17, 42]. This idea has been challenged, however, because there was no difference in the l-dopa and DA concentrations in the brains between patients with wearing-off and patients without wearing-off. This means that if 3-OMD blocked the l-dopa transportation through BBB, resulting in the induction of l-dopa side effects, PD patients with wearing-off phenomenon would have had comparatively lower levels of l-dopa and dopamine in their brains. The levels of 3-OMD in the CSF may be a crucial factor since the 3-OMD levels of the patients with the wearing-off were twice those in PD patients without the wearing-off after medication of l-dopa/carbidopa [13]. It has also been reported that 3-OMD inhibited the uptake of tyrosine into striatum, leading to the less utilization of l-dopa [16], and caused the impediment of dopamine release [20]. Thus, 3-OMD may act at the level of the dopaminergic synthesis and function. We have tested the effects of 3-OMD on dopamine uptake and receptor binding activities in rat brain tissue membranes and PC12 cells. The results indicate that 3-OMD had no significant effect on dopamine receptor binding activity, but it inhibited dopamine transporter activity and uptake in rat brain tissue and PC12 cells.
The present study shows that 3-OMD impairs locomotor activities when it is administered directly into the brain, indicating that locally increased 3-OMD in the brain may alter locomotor activities. It has been reported that 3-OMD altered l-dopa-induced behavioral activities and diminished l-dopa efficacy [43], which supports the decrease in locomotor activities by 3-OMD treatment in the present study. This result shows the evidence of the possible role of 3-OMD in l-dopa-induced behavioral adverse effects in long-term treatment.
3-OMD may induce the neurotoxic effects. Although PC12 cells may not be the best model, they are widely used for neurotoxicology studies. PC12 cell is a catecholamine-containing cell line, derived from rat pheochromocytoma, and possesses dopamine synthesizing, storage, and releasing properties similar to neurons [44–46]. PC12 cells can be induced to differentiate into sympathetic-like neuronal cells by the addition of nerve growth factor [47], which is used in the present studies. Differentiated PC12 cells have been used in many studies of l-dopa side effects associated with PD [26, 48]. The relative high concentration of 3-OMD was required to induce toxic effects in our cell culture experiment. This might be due to the characteristics of PC12 cells which are relatively resistant to dopaminergic toxins compared to the primary culture system. Moreover, the sensitivity of PC12 cells to cytotoxins could be altered by tissue culture medium condition [49]. All these factors may explain the relative resistance of PC12 cells to 3-OMD exposure in the present cell culture system. It has been reported that 3-OMD caused toxicity, inducing oxidative DNA damage [30] highly correlated with ROS formation [31, 32], indicating that the toxicity mechanism of 3-OMD may be related to oxidative stress, which may correlate with our data revealing that 3-OMD induces neurotoxicity by increasing ROS formation and inhibiting mitochondrial membrane potentials. Moreover, the potentiative effects of 3-OMD in l-dopa-induced toxic effects, by decreasing cell viability and increasing oxidative stress, suggest the possible potentiative role of 3-OMD in l-dopa-induced toxicity. The fact that PD patients take large amounts of l-dopa (up to 8 g/day) and that the 3-OMD levels are accumulating due to its long half-life (15 h) should be underscored for the consideration of its toxic effects during the long-term l-dopa therapy. The protective effects of antioxidants, such as vitamin E on l-dopa/3-OMD-induced cytotoxic effects, suggest that concurrent treatment of l-dopa with antioxidants might be beneficial for PD patients taking l-dopa.
In conclusion, our present study showed that 3-OMD induced behavioral changes and alteration of dopaminergic neurotransmission by decreasing dopamine turnover and uptake in rat brains, implying that 3-OMD may play a role in l-dopa-induced side effects during l-dopa therapy. Moreover, the toxic effects of 3-OMD in PC12 cells by increasing ROS generation and decreasing mitochondrial membrane potential, as well as its potentiaive effects in l-dopa-induced cytotoxic effects, indicate the possible accelerating effects of 3-OMD in the progression of the disease.
References
Muenter MD, Sharpless NS, Tyce GM (1972) Plasma 3-0-methyldopa in l-dopa therapy of Parkinson’s disease. Mayo Clin Proc 47:389–395
Sharpless NS, Muenter MD, Tyce GM et al (1972) 3-methoxy-4-hydroxyphenylalanine (3-O-methyldopa) in plasma during oral l-dopa therapy of patients with Parkinson’s disease. Clin Chim Acta 37:359–369
Gervas JJ, Muradas V, Bazan E et al (1983) Effects of 3-OM-dopa on monoamine metabolism in rat brain. Neurology 33:278–282
Tohgi H, Abe T, Takahashi S (1991b) Concentrations of tyrosine, l-dihydroxyphenylalanine, dopamine, and 3-O-methyldopa in the cerebrospinal fluid of Parkinson’s disease. Neurosci Lett 127:212–214
Miller JW, Shukitt-Hale B, Villalobos-Molina R et al (1997) Effect of l-Dopa and the catechol-O-methyltransferase inhibitor Ro 41-0960 on sulfur amino acid metabolites in rats. Clin Neuropharmacol 20:55–66
Kuruma I, Bartholini G, Tissot R et al (1971) The metabolism of l-3-O-methyldopa, a precursor of dopa in man. Clin Pharmacol Ther 12:678–82
Marion MH, Stocchi F, Quinn NP et al (1986) Repeated levodopa infusions in fluctuating Parkinson’s disease: clinical and pharmacokinetic data. Clin Neuropharmacol 9:165–181
Marsden CD (1994) Problems with long-term levodopa therapy for Parkinson’s disease. Clin Neuropharmacol Suppl 2:S32–S44
Feuerstein C, Serre F, Gavend M et al (1977a) Plasma O-methyldopa in levodopa-induced dyskinesias. A bioclinical investigation. Acta Neurol Scand 56:508–524
Feuerstein C, Tauche M, Serre F et al (1977b) Does O-methyl-dopa play a role in levodopa-induced dyskinesias. Acta Neurol Scand 56:79–82
Mena MA, Muradas V, Bazan E et al (1987) Pharmacokinetics of l-dopa in patients with Parkinson’s disease. Adv Neurol 45:481–486
Blandini F, Nappi G, Fancellu R et al (2003) Modifications of plasma and platelet levels of l-DOPA and its direct metabolites during treatment with tolcapone or entacapone in patients with Parkinson’s disease. J Neural Transm 110:911–922
Tohgi H, Abe T, Kikuchi T et al (1991a) The significance of 3-O-methyldopa concentrations in the cerebrospinal fluid in the pathogenesis of wearing-off phenomenon in Parkinson’s disease. Neurosci Lett 132:19–22
Fabbrini G, Juncos JL, Mouradian MM et al (1987) 3-O-methyldopa and motor fluctuations in Parkinson’s disease. Neurology 37:856–859
Soares-da-Silva P, Parada A, Serrao P (2000) The O-methylated derivative of l-DOPA, 3-O-methyl-l-DOPA, fails to inhibit neuronal and non-neuronal aromatic l-amino acid decarboxylase. Brain Res 863:293–297
Reches A, Fahn S (1982) 3-O-methyldopa blocks dopa metabolism in rat corpus striatum. Ann Neurol 12:267–271
Benetello P, Furlanut M, Fortunato M et al (1997) Levodopa and 3-O-methyldopa in cerebrospinal fluid after levodopa-carbidopa association. Pharmacol Res 35:313–315
Cheng H, Gomes-Trolin C, Aquilonius SM et al (1997) Levels of l-methionine S-adenosyltransferase activity in erythrocytes and concentrations of S-adenosylmethionine and S-adenosylhomocysteine in whole blood of patients with Parkinson’s disease. Exp Neurol 145:580–585
Zhao WQ, Latinwo L, Liu XX et al (2001) l-dopa upregulates the expression and activities of methionine adenosyl transferase and catechol-O-methyltransferase. Exp Neurol 171:127–138
Chang WY, Webster RA (1995) Effects of 3-O-methyl on l-dopa-facilitated synthesis and efflux of dopamine from rat striatal slices. Br J Pharmacol 116:2637–2640
Mena MA, Pardo B, Paino CL et al (1993) Levodopa toxicity in foetal rat midbrain neurons in culture: modulation by ascorbic acid. Neuroreport 4:438–440
Mena MA, Casarejos MJ, Carazo A et al (1996) Glia conditioned medium protects fetal rat midbrain neurones in culture from l-DOPA toxicity. Neuroreport 7:441–445
Datla KP, Blunt SB, Dexter DT (2001) Chronic l-DOPA administration is not toxic to the remaining dopaminergic nigrostriatal neurons, but instead may promote their functional recovery, in rats with partial 6-OHDA or FeCl(3) nigrostriatal lesions. Mov Disord 16:424–434
Melamed E, Offen D, Shirvan A et al (1998) Levodopa toxicity and apoptosis. Ann Neurol 44:S149–S154
Murer MG, Dziewczapolski G, Menalled LB et al (1998) Chronic levodopa is not toxic for remaining dopamine neurons, but instead promotes their recovery, in rats with moderate nigrostriatal lesions. Ann Neurol 43:561–575
Walkinshaw G, Waters CM (1995) Induction of apoptosis in catecholaminergic PC12 cells by l-DOPA. Implications for the treatment of Parkinson’s disease. J Clin Invest 95:2458–2464
Müller T, Woitalla D, Fowler B et al (2002) 3-OMD and homocysteine plasma levels in parkinsonian patients. J Neural Transm 109:175–179
Müller T, Woitalla D, Hauptmann B et al (2001) Decrease of methionine and S-adenosylmethionine and increase of homocysteine in treated patients with Parkinson’s disease. Neurosci Lett 308:54–56
Lee ES, Chen H, Soliman KF et al (2005) Effects of homocysteine on the dopaminergic system and behavior in rodents. Neurotoxicology 26:361–371
Spencer JP, Jenner A, Aruoma OI et al (1994) Intense oxidative DNA damage promoted by l-dopa and its metabolites. Implications for neurodegenerative disease. FEBS Lett 353:246–250
Martignoni E, Blandini F, Godi L et al (1999) Peripheral markers of oxidative stress in Parkinson’s disease. The role of l-DOPA. Free Radic Biol Med 27:428–437
Blandini F, Martignoni E, Ricotti R et al (1999) Determination of hydroxyl free radical formation in human platelets using high-performance liquid chromatography with electrochemical detection. J Chromatogr B Biomed Sci Appl 732:213–220
Lee JJ, Kim YM, Yin SY et al (2003) Aggravation of l-DOPA-induced neurotoxicity by tetrahydropapaveroline in PC12 cells. Biochem Pharmacol 66:1787–1795
Lowry CA, Renner KJ, Moore FL (1996) Catecholamines and indoleamines in the central nervous system of a urodele amphibian: a microdissection study with emphasis on the distribution of epinephrine. Brain Behav Evol 48:70–93
Billard W, Ruperto V, Crosby G et al (1984) Characterization of the binding of [3H]SCH 23390, a selective D1 receptor antagonist ligand, in rat striatum. Life Sci 35:1885–1893
Woodgate A, MacGibbon G, Walton M et al (1999) The toxicity of 6-hydroxydopamine on PC12 and P19 cells. Brain Res Mol Brain Res 69:84–92
Fu W, Luo H, Parthasarathy S et al (1998) Catecholamines potentiate amyloid beta-peptide neurotoxicity: involvement of oxidative stress, mitochondrial dysfunction, and perturbed calcium homeostasis. Neurobiol Dis 5:229–243
Palmeira CM, Moreno AJ, Madeira VM et al (1996) Continuous monitoring of mitochondrial membrane potential in hepatocyte cell suspensions. J Pharmacol Toxicol Methods 35:35–43
Lee CS, Han JH, Jang YY et al (2002) Differential effect of catecholamines and MPP+ on membrane permeability in brain mitochondria and cell viability in PC12 cells. Neurochem Int 40:361–369
Reilly DK, Rivera-Calimlim L, Van Dyke D (1980) Catechol-O-methyltransferase activity: a determinant of levodopa response. Clin Pharmacol Ther 28:278–286
Rivera-Calimlim L, Tandon D, Anderson F et al (1977) The clinical picture and plasma levodopa metabolite profile of parkinsonian nonresponders. Treatment with levodopa and decarboxylase inhibitor. Arch Neurol 34:228–232
Gomes P, Soares-da-Silva P (1999) Interaction between l-DOPA and 3-O-methyl-l-DOPA for transport in immortalised rat capillary cerebral endothelial cells. Neuropharmacology 38:1371–1380
Himori N, Tanaka Y, Kurasawa M et al (1994) 3-O-methyldopa attenuates the effects of Madopar on the haloperidol-induced cataleptic behavior and the locomotor activity in the mouse. Pharmacology 48:226–233
Greene LA, Rein G (1977) Release of (3H)norepinephrine from a clonal line of pheochromocytoma cells (PC12) by nicotinic cholinergic stimulation. Brain Res 138:521–528
Schubert D, Klier FG (1977) Storage and release of acetylcholine by a clonal cell line. Proc Natl Acad Sci USA 74:5184–5188
Rebois RV, Reynolds EE, Toll L et al (1980) Storage of dopamine and acetylcholine in granules of PC12, a clonal pheochromocytoma cell line. Biochemistry 19:1240–1248
Greene LA, Tischler AS (1976) Establishment of a noradrenergic clonal line of rat adrenal pheochromocytoma cells which respond to nerve growth factor. Proc Natl Acad Sci USA 73:2424–2428
Basma AN, Morris EJ, Nicklas WJ, Geller HM (1995) l-dopa cytotoxicity to PC12 cells in culture is via its autoxidation. J Neurochem 64:825–832
Cobuzzi RJ, Neafsey EJ, Collins MA (1994) Differential cytotoxicities of N-methyl-beta-carbolinium analogues of MPP+ in PC12 cells: insights into potential neurotoxicants in Parkinson’s disease. J Neurochem 62:1503–1510
Acknowledgement
Support for this research project is provided by National Institutes of Health grants NIH/NS28432, RR03020, and GM08111.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, ES.Y., Chen, H., King, J. et al. The Role of 3-O-Methyldopa in the Side Effects of l-dopa. Neurochem Res 33, 401–411 (2008). https://doi.org/10.1007/s11064-007-9442-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-007-9442-6