Abstract
A better understanding is needed of how glutamate metabolism is affected in mesial temporal lobe epilepsy (MTLE). Here we investigated glial–neuronal metabolism in the chronic phase of the kainate (KA) model of MTLE. Thirteen weeks following systemic KA, rats were injected i.p. with [1-13C]glucose. Brain extracts from hippocampal formation, entorhinal cortex, and neocortex, were analyzed by 13C and 1H magnetic resonance spectroscopy to quantify 13C labeling and concentrations of metabolites, respectively. The amount and 13C labeling of glutamate were reduced in the hippocampal formation and entorhinal cortex of epileptic rats. Together with the decreased concentration of NAA, these results indicate neuronal loss. Additionally, mitochondrial dysfunction was detected in surviving glutamatergic neurons in the hippocampal formation. In entorhinal cortex glutamine labeling and concentration were unchanged despite the reduced glutamate content and label, possibly due to decreased oxidative metabolism and conserved flux of glutamate through glutamine synthetase in astrocytes. This mechanism was not operative in the hippocampal formation, where glutamine labeling was decreased. In neocortex labeling and concentration of GABA were increased in epileptic rats, possibly representing a compensatory mechanism. The changes in the hippocampus might be of pathophysiological importance and merit further studies aiming at resolving metabolic causes and consequences of MTLE.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Mesial temporal lobe epilepsy (MTLE) is a common type of focal epilepsy in adults and consequently a target of extensive research. This condition is often preceded by an initial precipitating injury early in life, such as febrile seizures, head trauma, or status epilepticus, followed by a latent period of several years with no apparent seizure activity [12]. Histopathologically, MTLE is often characterized by hippocampal sclerosis, which involves extensive neuronal death, gliosis, and reorganization of synaptic connections by axon sprouting [13]. The mechanisms causing MTLE are yet to be defined, but there is increasing evidence that perturbed metabolism of glucose and amino acid neurotransmitters play essential roles.
Glucose utilization is increased locally during epileptic discharge and decreased interictally [9, 23, 33, 48]. Glutamate, the main excitatory neurotransmitter in the brain, can be produced from glucose involving both neuronal and astrocytic TCA cycle. In astrocytes, glutamate is converted to glutamine by cytosolic glutamine synthetase (GS) [35] and released to the extracellular space. Glutamine is taken up into neurons and deamidated to glutamate by mitochondrial phosphate activated glutaminase (PAG) as a link in the glutamate–glutamine cycle [18, 26]. Glutamate is excitotoxic and has been shown to be involved both in cell death and initiation and maintenance of epileptic seizures [10]. During and Spencer [16] reported an increased extracellular level of glutamate within the epileptogenic hippocampus prior to and during seizures. Others have observed low glutamate content interictally in the hippocampal tissue in both humans and animals [25, 39].
Downregulation of GS and impaired glutamate–glutamine cycling have been reported in the epileptogenic, gliotic human hippocampus [17, 39]. In GABAergic neurons glutamate is converted to the inhibitory neurotransmitter GABA by glutamate decarboxylase (GAD). Both increased and decreased amounts of GABA have been observed in biopsy material from patients with MTLE [1, 38, 39].
Spatial segregation of the enzymes PAG, GAD, and GS to different cell types causes glutamate, GABA, and glutamine to be enriched in different compartments. The glutamatergic neurons contain the largest pool of glutamate, whereas GABAergic neurons hold the GABA pool [37, 47]. Both types of neurons contain PAG whereas only astrocytes contain GS. By 13C magnetic resonance spectroscopy (13C MRS), it is possible to study the metabolic interactions between different cellular compartments [45]. Thus incorporation of 13C in glutamate, GABA, and glutamine from systemically injected [1-13C]glucose reflects the metabolism in glutamatergic neurons, GABAergic neurons, and astrocytes, respectively.
The role of altered glutamate homeostasis in epilepsy needs to be clarified. Metabolic studies using 13C MRS have been performed on whole rat brain extracts one day and two weeks after kainic acid (KA) injections [31, 41], but not on specific brain regions or in the chronic phase. The present study aims at exploring whether there is an altered glucose and glutamate metabolism in specific brain regions of KA-treated rats in the chronic phase of epilepsy. This animal model has been in use for decades, reproducing many of the features of human MTLE [6]. KA, a glutamate analogue, causes status epilepticus in rats when given systemically, followed by a latent period of approximately three to four weeks before spontaneous recurrent seizures occur [5, 6, 22]. Similar to human MTLE, the brain damage in the KA model is mostly restricted to limbic areas [6], where the hippocampal formation (dentate gyrus, CA1-3, subiculum) and entorhinal cortex develop into a hyperexcitable ‘epileptic circuit’ [11]. Rats were injected systemically with either KA or vehicle. Thirteen weeks later, after development of spontaneous seizures, they were subjected to systemic [1-13C]glucose injections followed by 13C and 1H MRS of brain extracts. Three brain regions were analyzed: the hippocampal formation, the entorhinal cortex, and the neocortex.
Materials and Methods
Materials
Male Sprague Dawley rats (∼250 g) were obtained from Taconic M&B (Copenhagen, Denmark). [1-13C]glucose and D2O (99.9%) were purchased from Cambridge Isotopes Laboratories (Woburn, MA, USA); ethylene glycol from Merck (Darmstad, Germany); kainic acid from Sigma-Aldrich (St. Louis, MO, USA). All other chemicals were of the purest grade available from local commercial sources.
Animals
All animals in this study were treated in accordance with the European Convention (ETS 123 of 1986) and all protocols were approved by the Norwegian National Animal Research Authority. Animals were maintained under standard laboratory conditions at room temperature of 22°C, air humidity of 66%, and a 12/12 h light/dark cycle, with free access to food and water. The animals were adapted to the above conditions for one week before the experiment started. Furthermore, the animals’ weight and general condition were monitored throughout the study period and in case of weight loss or lack of weight gain rats were fed with water soaked chow.
Kainic Acid Treatment
Fifteen rats were injected with KA dissolved in phosphate buffered saline, adjusted to pH 7.0 and injected intraperitoneally 10 mg/kg in a volume of 10 ml/kg. Eight control rats received the same volume of phosphate buffered saline.
The rats were placed in separate plastic cages immediately after the injections and monitored for at least 4 h for behavioral seizure manifestation. Seizures were scored according to the Racine score [42]: Stage 1, facial clonus; Stage 2, nodding; Stage 3, forelimb clonus; Stage 4, forelimb clonus with rearing; Stage 5, rearing and falling. Status epilepticus was defined as continuous limbic seizures scored as class 4 or 5 seizures and lasting for more than 90 min.
Animals developing status epilepticus were further monitored for the occurrence of spontaneous recurrent seizures, marking the transition from latent to chronic phase. A DVD recorder device with a CCTV camera was used and the animals were observed 8–12 h/day 7 days a week.
Only animals developing status epilepticus and two or more spontaneous recurrent seizures were used in this study.
Tissue Preparation and Extraction
Thirteen weeks after saline or KA injection, seven control and 10 epileptic animals were injected intraperitoneally with [1-13C]glucose (5.4 mg/kg, 3 mM solution) dissolved in saline. Fifteen minutes after injection, the animals were decapitated and the heads were snap frozen in liquid nitrogen and stored at −80°C until dissection. Three regions were sampled and weighed; the hippocampal formation (subiculum, CA1-CA3, and dentate gyrus), the entorhinal cortex (including a small part of the piriform cortex) and the neocortex. The tissue was homogenized with 1 ml cold 7% perchloric acid followed by centrifugation for 10 min at 4,000 g and 4°C. The procedure was repeated with water and the combined supernatants were neutralized with 2 M KOH followed by centrifugation and lyophilization of supernatants. Samples were stored at −20°C till analyses were performed.
13C and 1H Magnetic Resonance Spectroscopy
Brain tissue extracts were dissolved in 200 μl D2O (99.9%) containing 0.1% ethylene glycol, before neutralization (pH 6.0–7.0).
MR spectra of the larger (240–430 mg) neocortical samples were acquired on a Bruker DRX 500 MHz instrument whereas those of the hippocampal and entorhinal samples (50–200 mg) were obtained on a Bruker DRX 600 MHz instrument (BRUKER Analytik GmbH, Rheinstetten, Germany). Proton decoupled 13C MR spectra were acquired with the following acquisition parameters: 30° pulse angle, acquisition time 1.3 s, and relaxation delay 0.5 s. The number of scans was typically 20,000 (neocortex), 40,000 (hippocampal formation), and 50,000 (entorhinal cortex). Correction factors for nuclear Overhauser and relaxation effects were applied to the integrals of the individual peaks.
For 1H MR spectra, the following parameters were used: 90° pulse angle, acquisition time 1.36 s, and relaxation delay 10 s; 512 scans were accumulated for each sample. Water suppression was achieved by applying a low-power presaturation pulse at the water frequency.
Data Analysis
[1-13C]glucose metabolism was analyzed by integrating peaks from relevant metabolites in the 13C MR spectra (Fig. 1). The amounts of 13C were quantified from the area under the curve of relevant peaks using ethylene glycol as an internal standard. It should be noted that this 13C can come from the 1.1% naturally abundant 13C (the rest is 12C) or from incorporation of the label from [1-13C]glucose via metabolic pathways. Total amounts of metabolites were quantified from 1H MR spectra using ethylene glycol as an internal standard. The percentage 13C enrichment in the C-4 position of glutamate and C-6 N-acetyl aspartate was calculated from the amount of 13C from 13C MR spectra corrected for the 1.1% natural abundant 13C and the compound determined by 1H MRS (for details see Badar-Goffer [4]). Percent 13C enrichment in C-6 of NAA was calculated from the amount of 13C in the C-6 position and the total amount calculated from the 1H MR spectra to monitor cell loss and viability. Differences between KA and control groups were analyzed statistically with Student’s t-test, and the significance was set at P < 0.05. Results are given as mean ± standard deviation (SD).
A typical 13C MR spectrum of hippocampal formation extract from control rat brain 13 weeks after saline injection. [1-13C]glucose was injected 15 min prior to decapitation. Peak assignment; 1: glutamate-C2; 2: glutamine-C2; 3: aspartate-C2; 4: GABA-C4; 5: aspartate-C3; 6: GABA-C2; 7: succinate-C2/C3; 8: glutamate-C4; 9: glutamine-C4; 10: glutamate-C3; 11: glutamine-C3; 12: GABA-C3; 13: NAA-C6; 14: lactate-C3; 15: alanine-C3; ppm: parts per million
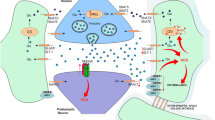
The analysis of glucose metabolism by 13C MRS is based on knowledge of the metabolic fate of [1-13C]glucose in neurons and astrocytes. Equal amounts of [1-13C]glucose are taken up in neurons and astrocytes [32]. Through glycolysis [1-13C]glucose is converted into one molecule of [3-13C]pyruvate and one molecule of unlabeled pyruvate (Fig. 2). [3-13C]pyruvate can be converted into either [3-13C]lactate or [3-13C]alanine in the cytosol, or be metabolized by pyruvate dehydrogenase (PDH) to [2-13C]acetyl CoA in neuronal and astrocytic mitochondria. [2-13C]acetyl CoA can condense with oxaloacetate and enter the TCA cycle. [4-13C]glutamate is formed from [4-13C]α-ketoglutarate from the first turn of the TCA cycle. [4-13C]glutamate either adds to the pool of metabolic constituents, or it is used as neurotransmitter in glutamatergic neurons. In astrocytes, [4-13C]glutamate is converted to [4-13C]glutamine by GS, while in GABAergic neurons it is transformed into [2-13C]GABA by GAD.
Incorporation of label from [1-13C]glucose into metabolites. Via glycolysis in cytosol of neurons and astrocytes, [1-13C]glucose is converted into one molecule of [3-13C]pyruvate and one molecule of unlabelled pyruvate, which does not contribute to labeling and is, thus, omitted. [3-13C]pyruvate can be converted into either [3-13C]lactate or [3-13C]alanine, or be further metabolized to [2-13C]acetyl CoA in mitochondria. The latter condenses with oxaloacetate and enters the TCA cycle eventually forming [4-13C]α-ketoglutarate, which can be converted to [4-13C]glutamate, and further to [4-13C]glutamine, to [2-13C]GABA, or to [2-13C]- or [3-13C]oxaloacetate/aspartate. If the 13C label stays in the TCA cycle for a second turn, [2-13C]- or [3-13C]glutamate/glutamine and [3-13C]- or [4-13C]GABA can be formed. As described in “Materials and methods” section, pyruvate carboxylation can occur in astrocytes, but is, for simplicity, not included in the figure
If [4-13C]α-ketoglutarate remains in the TCA cycle, [2-13C]- and [3-13C]oxaloacetate will eventually be formed and can give rise to [2-13C]- and [3-13C]aspartate or condense with acetyl CoA to give equal amounts of [2-13C]- and [3-13C]glutamate, [2-13C]- and [3-13C]glutamine or [3-13C]- and [4-13C]GABA in the second turn of the TCA cycle. The TCA cycling ratios for glutamate and glutamine (see Melo et al. [29]) were calculated as follows: ([3-13C]-1.1%glu or gln)/([4-13C]-1.1%glu or gln). For GABA the expression is ([3-13C]-1.1%GABA)/([2-13C]-1.1%GABA). These ratios for glutamate and further glutamine or GABA give an indication of TCA cycle activity.
In addition to PDH, astrocytes possess pyruvate carboxylase (PC) [44], which is not present in neurons. PC converts [3-13C]pyruvate into [3-13C]oxaloacetate, eventually resulting in the formation of [2-13C]glutamate which may be converted to [2-13C]glutamine, which again can serve as precursor for [2-13C]glutamate and [4-13C]GABA [30]. Label in C-2 of glutamate and glutamine (and C-4 of GABA) can also be derived from PDH if 13C from [1-13C]glucose stays in the TCA cycle for a second turn, where equal amounts of label in C-2 and C-3 positions for glutamate and glutamine (C-3 and C-4 for GABA) are formed as mentioned earlier (see also Melo et al. [29]). This can be corrected for by subtraction of 13C label in the C-3 from that in the C-2 position.
Results
Seizures
Following KA injection, animals developed a typical behavioral response starting with staring spells, followed by head nodding and periods of wet dog shakes. Within an hour after KA injection, forelimb clonus appeared and was later accompanied by rearing and falling. The limbic seizures appeared with progressively shorter time intervals and eventually developed into a status epilepticus with continuous behavioral seizure activity for several hours. Thirteen out of 15 rats experienced status epilepticus exceeding 90 min of duration. Of these, 11 rats developed spontaneous recurrent seizures, and were defined as epileptic. Ten animals were used for the 13C experiments.
Concentrations of Metabolites
We used 1H MRS to measure the concentration (μmol/g brain tissue) of total (labeled and unlabeled) glutamate, glutamine, GABA, aspartate, NAA, lactate, and alanine (Fig. 3 and Table 1) in the hippocampal formation, entorhinal cortex, and neocortex of epileptic and control rats. As shown in Fig. 3A and B (lower panels), the concentrations of glutamate and aspartate were decreased within the hippocampal formation and the entorhinal cortex of epileptic rats, while no significant changes were found in the concentrations of GABA and glutamine. In the neocortex, however, an increase in GABA was seen in epileptic rats, combined with decreased concentration of aspartate (Fig. 3C, lower panel). The epileptic animals showed a decreased concentration of NAA in all regions, but no change in lactate and alanine (Table 1).
Concentrations of 13C labeled metabolites (nmol/g tissue) derived from [1-13C]glucose are shown in (A–C) upper panels. Concentrations of total metabolites (μmol/g tissue) are shown in the lower panels. Results were obtained by 13C and 1H MRS analyses of brain extracts of hippocampal formation, entorhinal cortex and neocortex from controls and chronically epileptic animals 13 weeks after kainic acid (KA) injection. All animals (control n = 6, KA n = 7–10) were injected with [1-13C]glucose 15 min before decapitation. White bars represent saline treated control animals, grey bars represent KA-treated animals. Values are given as mean ± standard deviation. *Significantly different from control group using Student’s t-test, P < 0.05
13C Labeling of Metabolites
We performed 13C MRS to obtain more detailed information about the amino acid metabolism in neurons and astrocytes, and the interaction between the different cellular compartments. In most rats, metabolites were successfully labeled by [1-13C]glucose as seen in the typical spectrum of a control rat brain extract of the hippocampal formation in Fig. 1. As shown in Fig. 3A and B (upper panels), the amounts of [4-13C]glutamate and [3-13C]aspartate were decreased within the hippocampal formation and the entorhinal cortex of epileptic rats. Decreased labeling was also observed in the C-2 and C-3 positions of glutamate and C-2 position of aspartate (data not shown). In the hippocampal formation there was a decreased amount of [4-13C]glutamine as well, but no decrease in labeling of the C-2 and C-3 positions (data not shown). The neocortex differed from the other regions by showing a significant increase in the amount of [2-13C]GABA in epileptic rats (Fig. 3C, upper panel).
Percent 13C enrichment (more than the naturally present 1.1%) of glutamate (C-4) was significantly decreased in the hippocampal formation of KA animals compared to controls, 0.6% ± 0.2 and 1.1% ± 0.2 (P < 0.02), respectively. No such difference was detected in the entorhinal cortex or the neocortex. 13C enrichment of NAA (C-6) was detected in entorhinal cortex and neocortex, while no differences were observed between control and epileptic animals in these regions. In the hippocampal formation, only naturally abundant 13C was detected (results not shown).
Labeling of lactate and alanine was not changed in most parts of the brain of epileptic animals, with the exception of neocortex, where lactate labeling was increased. Cycling ratios for glutamate, glutamine and GABA are presented in Table 2. Glutamate and GABA had similar ratios in all areas, while in the entorhinal cortex the cycling ratio for glutamine was decreased in KA injected animals compared to control.
Discussion
The data presented suggest changes in neuronal metabolism and astrocyte–neuron interactions in the brain of KA-injected rats in the chronic phase. A complex picture emerges of mitochondrial dysfunction of glutamatergic neurons in the hippocampal formation, reduced entry of glutamate into the astrocytic TCA cycle in entorhinal cortex, and increased synthesis of GABA in the neocortex.
The adult mammalian brain depends on glucose and oxygen for energy and metabolite production. After glycolysis, [3-13C]pyruvate is converted to [3-13C]lactate by lactate dehydrogenase in the cytosol, or to [3-13C]alanine via alanine aminotransferase in the cytosol and mitochondria. In hippocampal formation and entorhinal cortex of the KA-treated rats, the amount and labeling of lactate and alanine were not altered, compared to control. However, glycolysis could well have been reduced in these areas, as decreased labeling of glutamate, aspartate and glutamine is suggestive of a reduced acetyl CoA formation from [1-13C]glucose. In neocortex no decrease was observed in the concentration or labeling of the above mentioned metabolites, or in the concentration of lactate, indicating unchanged glycolysis.
Hippocampal Formation
In the hippocampal formation, both the amount of [4-13C]glutamate and concentration of total glutamate were decreased in the epileptic rats. A major pool of glutamate in the brain is located in glutamatergic neurons [37, 47], and changes in glutamate labeling in C-4 and concentration are likely to reflect alterations in these cells. It has been shown that there is a reduced metabolism of glucose in epileptogenic hippocampal formation of humans and animals [15, 19], and that there is a reduced glutamate content in human epileptogenic hippocampus in the interictal phase [38]. A reduced glutamate concentration and an analogous decrease in the amount of labeled glutamate would occur if there was an extensive loss of glutamatergic neurons. Indeed, the hippocampal subfields CA1, CA3 and the dentate hilus display pronounced cell loss both in the KA model and in humans with MTLE [6]. A decrease in the concentration of NAA, a marker for neuronal death, was observed in the epileptic rats, consistent with neuronal loss in the hippocampal formation. However, the decreased NAA and the reduced glutamate labeling could also reflect mitochondrial dysfunction of the remaining glutamatergic neurons, not merely cell loss. To address this question, we measured the percent 13C enrichment in glutamate C-4 (see “Methods” section). The amount of glutamate derived from [1-13C]glucose within the 15 min from injection to decapitation of the rat is a measure of mitochondrial activity, as the precursor of this glutamate ([4-13C]glutamate) is the TCA cycle intermediate [4-13C]α-ketoglutarate. The reduction in the amount of [4-13C]glutamate was greater than the decrease in the total amount of glutamate in this brain area and thus it is clear that loss of neurons (measured as the decrease in the total amount of glutamate and NAA) was smaller than the decrease in glutamate C-4 labeling (decreased % 13C enrichment in glutamate C-4), indicating mitochondrial dysfunction in the remaining glutamatergic neurons.
Glutamate released from neurons is taken up into astrocytes and converted to glutamine by the astrocytic enzyme glutamine synthetase [35]. Glutamine is transported back to neurons and converted to glutamate, as a part of the glutamate–glutamine cycle [8]. Accordingly, when both [4-13C]glutamate labeling and glutamate concentration are reduced, a reduced [4-13C]glutamine labeling is expected. A decrease in [4-13C]glutamine was indeed apparent in the epileptic rats. This decrease could be secondary to a reduced release of glutamate from the neurons, but alternatively it could be due to a reduced capacity for glutamine synthesis in the astrocytes. Notably, a previous study of surgically resected hippocampi from patients with MTLE showed decreased expression and activity of GS [17]. A reduced flux of glutamate through GS (due to reduced availability of glutamate or reduced GS activity) is consistent with the finding that the glutamine level is maintained in the present study, in the face of an increased number and/or size of astrocytes [2, 24, 43, 46].
GABA labeling and concentration was unaltered in the hippocampal formation, in contrast to the situation in the pilocarpine model which shows a decreased GABA labeling [29]. The GABA synthesizing enzyme GAD is reduced during the acute phase following KA injection, but then recovers after one month [27, 46]. This is consistent with the present findings. Additionally, the number of GAD-immunoreactive neurons is unchanged in the human epileptogenic hippocampus [3].
The 13C labeling and the concentration of aspartate were also decreased in the hippocampal formation of epileptic rats. Aspartate is present both in GABAergic and glutamatergic neurons [37], but the decrease in aspartate can probably be attributed to the changes that occur in glutamatergic neurons. Thus the decrease in aspartate parallels the decrease in glutamate (Fig. 3A). A coupling of aspartate and glutamate metabolism has been demonstrated in previous studies [36].
Entorhinal Cortex
Entorhinal cortex is one of the structures involved in the epileptic circuitry, but has gained less attention than the hippocampal formation. In kainic acid-treated rats, the neuronal loss in entorhinal cortex is largely restricted to layer III [14], but in the present material the entorhinal cortex has been sampled together with parts of the extensively degenerated piriform cortex. The entorhinal cortex and hippocampal formation display many of the same metabolic changes, but differences are also apparent. As for the hippocampal formation, both 13C labeling and concentration of total glutamate were decreased in the entorhinal cortex of epileptic rats. This decrease is consistent with the cell loss in these regions, as indicated by the reduced NAA concentration. Furthermore, it is known that there is extensive cell loss in the piriform cortex [7, 34]. Hence, the small contamination from this region in the entorhinal samples may contribute to the observed reduction in glutamate and NAA. The percent 13C enrichment of both glutamate and NAA was unchanged, indicating normal TCA cycle activity of the remaining neurons in the entorhinal cortex.
As stated above, a decreased amount of [4-13C]glutamine is expected when both [4-13C]glutamate labeling and concentration of total glutamate are reduced. In contrast to the situation in the hippocampal formation, the amount of [4-13C]glutamine in entorhinal cortex was unaltered in the epileptic rats. One possible explanation is that the astrocytes respond to decreased glutamate supply by increasing their PC activity. PC refills the astrocytic TCA cycle with oxaloacetate by carboxylating pyruvate, and is essential for de novo synthesis of glutamine, glutamate, GABA, and aspartate. However, there was no evidence of increased PC activity in this region (results not shown).
Alternatively, the fact that the glutamine labeling is unaffected by the decreased availability of glutamate could be explained by a shift in the routing of glutamate within astrocytes. More specifically, the glutamine labeling could be maintained if the proportion of glutamate that is converted into glutamine (by glutamine synthetase) is increased at the expense of the proportion of glutamate that is funneled into the TCA cycle. The extent to which these pathways are active can be calculated from the TCA cycling ratio for glutamine (Hassel et al. [21]; for details see “Methods” section). The cycling ratio for glutamine was reduced in entorhinal cortex, indicating that more glutamine was formed from neuronal glutamate directly. Thus, astrocytes in entorhinal cortex could compensate for reduced glutamate availability by decreasing entry of the carbon skeleton into the TCA cycle and conserving flux through GS. This would be in line with the histological analysis of the entorhinal cortex which indicated that astrocyte morphology was well preserved (unpublished results).
Similar to the hippocampal formation, metabolism in GABAergic neurons was unaltered and labeling and amount of aspartate were reduced in the same manner as glutamate.
Neocortex
The neocortex is not involved in the generation of seizures in KA-treated rats, but rather in their spreading, and showed few metabolic changes in this study. An increase in both GABA labeling and concentration was observed. In agreement with this finding, GAD activity has been found to increase in the frontal cortex one month after KA injection [27], and in all cortical areas after six months [5].
The GABA shunt connects GABA with the TCA cycle resulting in succinate and subsequently oxaloacetate formation [28]. The latter can be transaminated with glutamate to give aspartate. In the present study, the concentration of total aspartate was decreased in neocortex. Since glutamate labeling was normal, the decreased concentration of aspartate might reflect a down regulation of GABA-transaminase (GABA-T) which will cause increase in GABA and decrease in aspartate. Indeed, both types of change were observed in the present study. GABA-T is a component of the GABA shunt and a target for antiepileptic treatment [49]. If GABA-T is downregulated in the KA-treated rats, this might be viewed as a compensatory mechanism.
Poor seizure control is associated with low brain GABA content [40], and antiepileptic drugs enhancing GABAergic transmission have proven effective in reducing seizures [20]. Hence, we suggest that the elevated GABA labeling and concentration in the neocortex of KA-treated rats may represent an endogenous antiepileptic mechanism, suppressing spread of interictal discharge beyond the hippocampal–entorhinal circuitry.
Conclusions
The reduced conversion of glucose to glutamate in hippocampal formation and entorhinal cortex of epileptic rats reflects cell loss, but also involves TCA cycle dysfunction in the surviving neurons of the hippocampal formation. In the entorhinal cortex, our data suggest that astrocytes respond to decreased glutamate availability by decreasing its conversion via the TCA cycle and maintaining flux of glutamate through glutamine synthetase. This compensatory mechanism was not operative in the hippocampal formation. The reason for TCA cycle dysfunction needs to be explored further in order to develop pharmacological strategies to prevent the progressive neurodegeneration seen in MTLE.
References
Aasly J, Silfvenius H, Aas TC, Sonnewald U, Olivecrona M, Juul R, White LR (1999) Proton magnetic resonance spectroscopy of brain biopsies from patients with intractable epilepsy. Epilepsy Res 35:211–217
Altar CA, Baudry M (1990) Systemic injection of kainic acid: gliosis in olfactory and limbic brain regions quantified with [3H]PK 11195 binding autoradiography. Exp Neurol 109:333–341
Babb TL, Pretorius JK, Kupfer WR, Crandall PH (1989) Glutamate decarboxylase-immunoreactive neurons are preserved in human epileptic hippocampus. J Neurosci 9:2562–2574
Badar-Goffer RS, Bachelard HS, Morris PG (1990) Cerebral metabolism of acetate and glucose studied by 13C-n.m.r. spectroscopy. A technique for investigating metabolic compartmentation in the brain. Biochem J 266:133–139
Baran H, Kepplinger B, Draxler M, Skofitsch G (2004) Choline acetyltransferase, glutamic acid decarboxylase and somatostatin in the kainic acid model for chronic temporal lobe epilepsy. Neurosignals 13:290–297
Ben-Ari Y (1985) Limbic seizure and brain damage produced by kainic acid: mechanisms and relevance to human temporal lobe epilepsy. Neuroscience 14:375–403
Ben-Ari Y, Tremblay E, Ottersen OP (1980) Injections of kainic acid into the amygdaloid complex of the rat: an electrographic, clinical and histological study in relation to the pathology of epilepsy. Neuroscience 5:515–528
Berl S, Clarke DD (1969) Compartmentation of amino acid metabolism. In Lajtha A (ed) Handbook of neurochemistry, vol. 2:. Plenum Press, New York, pp 447–472
Bouilleret V, Boyet S, Marescaux C, Nehlig A (2000) Mapping of the progressive metabolic changes occurring during the development of hippocampal sclerosis in a model of mesial temporal lobe epilepsy. Brain Res 852:255–262
Bradford HF (1995) Glutamate, GABA and epilepsy. Prog Neurobiol 47:477–511
Bragin A, Wilson CL, Engel J Jr (2000) Chronic epileptogenesis requires development of a network of pathologically interconnected neuron clusters: a hypothesis. Epilepsia 41(Suppl 6):S144–S152
Bruton CJ (1988) The neuropathology of temporal lobe epilepsy. Oxford University Press, Oxford
de Lanerolle NC, Lee TS (2005) New facets of the neuropathology and molecular profile of human temporal lobe epilepsy. Epilepsy Behav 7:190–203
Du F, Eid T, Lothman EW, Kohler C, Schwarcz R (1995) Preferential neuronal loss in layer III of the medial entorhinal cortex in rat models of temporal lobe epilepsy. J Neurosci 15:6301–6313
Dube C, Boyet S, Marescaux C, Nehlig A (2001) Relationship between neuronal loss and interictal glucose metabolism during the chronic phase of the lithium-pilocarpine model of epilepsy in the immature and adult rat. Exp Neurol 167:227–241
During MJ, Spencer DD (1993) Extracellular hippocampal glutamate and spontaneous seizure in the conscious human brain. Lancet 341:1607–1610
Eid T, Thomas MJ, Spencer DD, Runden-Pran E, Lai JC, Malthankar GV, Kim JH, Danbolt NC, Ottersen OP, de Lanerolle NC (2004) Loss of glutamine synthetase in the human epileptogenic hippocampus: possible mechanism for raised extracellular glutamate in mesial temporal lobe epilepsy. Lancet 363:28–37
Erecinska M, Silver IA (1990) Metabolism and role of glutamate in mammalian brain. Prog Neurobiol 35:245–296
Gaillard WD, Bhatia S, Bookheimer SY, Fazilat S, Sato S, Theodore WH (1995) FDG-PET and volumetric MRI in the evaluation of patients with partial epilepsy. Neurology 45:123–126
Gale K (1992) GABA and epilepsy: basic concepts from preclinical research. Epilepsia 33(Suppl 5):S3–12
Hassel B, Sonnewald U, Fonnum F (1995) Glial–neuronal interactions as studied by cerebral metabolism of [2-13C]acetate and [1-13C]glucose: an ex vivo 13C NMR spectroscopic study. J Neurochem 64:2773–2782
Hellier JL, Patrylo PR, Buckmaster PS, Dudek FE (1998) Recurrent spontaneous motor seizures after repeated low-dose systemic treatment with kainate: assessment of a rat model of temporal lobe epilepsy. Epilepsy Res 31:73–84
Henry TR, Mazziotta JC, Engel J Jr, Christenson PD, Zhang JX, Phelps ME, Kuhl DE (1990) Quantifying interictal metabolic activity in human temporal lobe epilepsy. J Cereb Blood Flow Metab 10:748–757
Jabs R, Paterson IA, Walz W (1997) Qualitative analysis of membrane currents in glial cells from normal and gliotic tissue in situ: down-regulation of Na+ current and lack of P2 purinergic responses. Neuroscience 81:847–860
Koyama I (1972) Amino acids in the cobalt-induced epileptogenic and nonepileptogenic cat’s cortex. Can J Physiol Pharmacol 50:740–752
Kvamme E, Torgner IA, Roberg B (2001) Kinetics and localization of brain phosphate activated glutaminase. J Neurosci Res 66:951–958
Marksteiner J, Sperk G (1988) Concomitant increase of somatostatin, neuropeptide Y and glutamate decarboxylase in the frontal cortex of rats with decreased seizure threshold. Neuroscience 26:379–385
Martin DL, Rimvall K (1993) Regulation of gamma-aminobutyric acid synthesis in the brain. J Neurochem 60:395–407
Melo TM, Nehlig A, Sonnewald U (2005) Metabolism is normal in astrocytes in chronically epileptic rats: a (13)C NMR study of neuronal–glial interactions in a model of temporal lobe epilepsy. J Cereb Blood Flow Metab 25:1254–1264
Melo TM, Nehlig A, Sonnewald U (2006) Neuronal–glial interactions in rats fed a ketogenic diet. Neurochem Int 48:498–507
Muller B, Qu H, Garseth M, White LR, Aasly J, Sonnewald U (2000) Amino acid neurotransmitter metabolism in neurones and glia following kainate injection in rats. Neurosci Lett 279:169–172
Nehlig A, Wittendorp-Rechenmann E, Lam CD (2004) Selective uptake of [14C]2-deoxyglucose by neurons and astrocytes: high-resolution microautoradiographic imaging by cellular 14C-trajectography combined with immunohistochemistry. J Cereb Blood Flow Metab 24:1004–1014
Nelissen N, Van PW, Baete K, Van LK, Palmini A, Van BH, Dupont P (2006) Correlations of interictal FDG-PET metabolism and ictal SPECT perfusion changes in human temporal lobe epilepsy with hippocampal sclerosis. Neuroimage 32:684–695
Nitecka L, Tremblay E, Charton G, Bouillot JP, Berger ML, Ben-Ari Y (1984) Maturation of kainic acid seizure-brain damage syndrome in the rat. II. Histopathological sequelae. Neuroscience 13:1073–1094
Norenberg MD, Martinez-Hernandez A (1979) Fine structural localization of glutamine synthetase in astrocytes of rat brain. Brain Res 161:303–310
Olstad E, Qu H, Sonnewald U (2007) Glutamate is preferred over glutamine for intermediary metabolism in cultured cerebellar neurons. J Cereb Blood Flow Metab 27:811–820
Ottersen OP, Storm-Mathisen J (1985) Different neuronal localization of aspartate-like and glutamate-like immunoreactivities in the hippocampus of rat, guinea-pig and Senegalese baboon (Papio papio), with a note on the distribution of gamma-aminobutyrate. Neuroscience 16:589–606
Peeling J, Sutherland G (1993) 1H magnetic resonance spectroscopy of extracts of human epileptic neocortex and hippocampus. Neurology 43:589–594
Petroff OA, Errante LD, Rothman DL, Kim JH, Spencer DD (2002) Glutamate–glutamine cycling in the epileptic human hippocampus. Epilepsia 43:703–710
Petroff OA, Rothman DL, Behar KL, Mattson RH (1996) Low brain GABA level is associated with poor seizure control. Ann Neurol 40:908–911
Qu H, Eloqayli H, Muller B, Aasly J, Sonnewald U (2003) Glial-neuronal interactions following kainate injection in rats. Neurochem Int 42:101–106
Racine RJ (1972) Modification of seizure activity by electrical stimulation. II. Motor seizure. Electroencephalogr Clin Neurophysiol 32:281–294
Roch C, Leroy C, Nehlig A, Namer IJ (2002) Magnetic resonance imaging in the study of the lithium-pilocarpine model of temporal lobe epilepsy in adult rats. Epilepsia 43:325–335
Shank RP, Bennett GS, Freytag SO, Campbell GL (1985) Pyruvate carboxylase: an astrocyte-specific enzyme implicated in the replenishment of amino acid neurotransmitter pools. Brain Res 329:364–367
Sonnewald U, Kondziella D (2003) Neuronal glial interaction in different neurological diseases studied by ex vivo 13C NMR spectroscopy. NMR Biomed 16:424–429
Sperk G, Lassmann H, Baran H, Kish SJ, Seitelberger F, Hornykiewicz O (1983) Kainic acid induced seizures: neurochemical and histopathological changes. Neuroscience 10:1301–1315
Storm-Mathisen J, Leknes AK, Bore AT, Vaaland JL, Edminson P, Haug FM, Ottersen OP (1983) First visualization of glutamate and GABA in neurones by immunocytochemistry. Nature 301:517–520
Tremblay E, Ottersen OP, Rovira C, Ben-Ari Y (1983) Intra-amygdaloid injections of kainic acid: regional metabolic changes and their relation to the pathological alterations. Neuroscience 8:299–315
Yogeeswari P, Sriram D, Vaigundaragavendran J (2005) The GABA shunt: an attractive and potential therapeutic target in the treatment of epileptic disorders. Curr Drug Metab 6:127–139
Acknowledgments
The authors thank the Norwegian Epilepsy Foundation for financial support to SA. Supported by the Norwegian Research Council (Storforsk) and the EU project GRIPANNT.
Author information
Authors and Affiliations
Corresponding author
Additional information
Special issue article in honor of Dr. Frode Fonnum.
Rights and permissions
About this article
Cite this article
Alvestad, S., Hammer, J., Eyjolfsson, E. et al. Limbic Structures Show Altered Glial–Neuronal Metabolism in the Chronic Phase of Kainate Induced Epilepsy. Neurochem Res 33, 257–266 (2008). https://doi.org/10.1007/s11064-007-9435-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-007-9435-5