Abstract
Background
Molecular glioblastomas (i.e. without the histological but with the molecular characteristics of IDH-wild-type glioblastoma) frequently lack contrast enhancement, which can wrongly lead to suspect a lower-grade glioma. Herein, we aimed to assess the diagnostic value of gyriform infiltration as an imaging marker for molecular glioblastomas.
Methods
Two independent investigators reviewed the MRI scans from patients with newly diagnosed gliomas for the presence of a gyriform infiltration defined as an elective cortical hypersignal on MRI FLAIR sequence. Diagnostic test performance of this sign for the diagnosis of molecular glioblastoma were calculated.
Results
A total of 426 patients were included, corresponding to 31 molecular glioblastoma, 294 IDH-wild-type glioblastoma, 50 IDH-mutant astrocytoma, and 51 IDH-mutant 1p19q-codeleted oligodendroglioma. A gyriform infiltration was observed in 16/31 (52%) molecular glioblastoma, 40/294 (14%) IDH-wild-type glioblastoma, and none of the IDH-mutant glioma. All the 56 gyriform-infiltration-positive tumors were IDH-wild-type and all but two had a TERT promoter mutation. The inter-rater agreement was good (κ = 0.69, p < 0.001). The sensitivity, specificity, positive predictive value and negative predictive value of the presence of a gyriform infiltration for the diagnosis of molecular glioblastoma were 52%, 90%, 29%, 96%, respectively. The median overall survival was better for gyriform-infiltration-negative patients compared to gyriform-infiltration-positive patients in the whole series and in patients with non-enhancing lesions (n = 95) (25.6 vs 16.9 months, p = 0.005 and 20.2 months vs not reached, p < 0.001).
Conclusion
Gyriform infiltration is a specific imaging marker of molecular glioblastomas that can help distinguishing these tumors from IDH-mutant lower-grade gliomas.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Several studies have shown that IDH-wild-type diffuse astrocytic gliomas display molecular features of glioblastoma (GBM) and, similar to IDH-wild-type GBM, are associated with a poor prognosis. Therefore, these tumors have been classified in the World Health Organization (WHO) 2021 classification [1] of central nervous system tumors as IDH-wild-type GBM [2, 3]. Thus, according to the latter classification, a diagnosis of IDH-wild-type GBM can be made in adults if the histo-molecular analysis finds an IDH-wild-type diffuse and astrocytic glioma with microvascular proliferation or necrosis, or a TERT promoter (TERTp) mutation, or an EGFR amplification, or a combined whole-chromosome-7 gain and chromosome-10 loss. However, in contrast to IDH-wild-type GBM diagnosed on histological characteristics (presence of microvascular proliferation or necrosis), contrast enhancement is frequently lacking in IDH-wild-type GBM diagnosed solely on the molecular profile (molecular GBM) and these tumors have a radiological presentation that can wrongly suggest a low grade glioma (LGG) [4,5,6]. Indeed, in a recent meta-analysis, 42% of grade II or III IDH-wild-type astrocytomas were found not to display contrast enhancement on magnetic resonance imaging (MRI), compared to 57% and 45% of IDH-mutant low grade astrocytomas and oligodendrogliomas, respectively [7]. Therefore, imaging biomarkers that could allow distinguishing molecular GBM from LGG would be helpful. Recently, important advances have been made in the non-invasive molecular characterization of gliomas. For example, 2-hydroxyglutarate MR spectroscopy enables to identify IDH-mutant gliomas [8] and the presence of a T2/FLAIR mismatch sign is highly specific of IDH-mutant astrocytomas [9,10,11]. Additionally, molecular GBM have been shown to frequently display areas of elective FLAIR hyperintensity limited to the cortical grey matter[4]. The aim of the present study was to assess the specificity and reproducibility of this radiological feature, designated as “gyriform infiltration”, as an imaging marker for the noninvasive detection of molecular GBM in an independent cohort of diffuse gliomas.
Methods
Patient selection
We retrospectively identified adult patients with diffuse gliomas diagnosed in the Hospices Civils de Lyon, Hôpital Neurologique, Lyon, France between September 2017 and June 2020 and reviewed their clinical, radiological, histological, and molecular characteristics. The list of patients was retrospectively obtained from the records of the neuropathology department. Patients were included if they were aged ≥ 18 years, had a diffuse glioma according to 2016 WHO brain tumor classification, had an available TERTp mutation and IDH mutation status, and had an MRI scan performed at diagnosis (before surgery or biopsy) for radiological review with T2 FLAIR and post-contrast T1-weighted sequences. Patients with glioma limited to the brainstem or cerebellum, or with a H3K27M or an H3G34 mutation, were excluded from the analysis. We defined molecular GBM as IDH-wild-type astrocytomas without histological characteristics of GBM (presence of microvascular proliferation or necrosis) but with molecular alterations (TERTp mutation and/or EGFR amplification).
Molecular data
Data regarding IDH1, IDH2, H3-3A/H3C2, BRAF V600E, and TERTp mutations, EGFR gene amplification, ATRX expression, O6-methylguanine-DNA methyltransferase (MGMT) promoter methylation, and chromosomes 1p and 19q codeletion were obtained from the records of the neuropathology department. The majority of samples were molecularly characterized using a dedicated next generation sequence (NGS) panel enabling to test genetic mutations and loss or gain of chromosomal regions characteristic of gliomas [12, 13]. TERTp mutation was tested using a droplet Polymerase Chain Reaction (PCR) using commercial probes (Biorad) and confirmed using the NGS panel [14].
Imaging protocol
Elective gyriform infiltration was defined as an area of FLAIR hyperintensity limited to the cortical grey matter, without involvement of the underlying white matter and without contrast enhancement.
Brain MRI were acquired at 1.5 T or 3.0 T and were independently reviewed by two investigators (E.M. and F.D.) for the presence of a gyriform infiltration. The two investigators were blinded to the clinical history of the patient and the molecular characteristics of the lesion during this review. If there were discordant reviews between the two investigators, both assessed the MRI sequences a second time (agreement by consensus).
Statistical analysis
Sensitivity (Se), specificity (Sp), positive predictive value (PPV), and negative predictive value (NPV) were calculated using the final score after adjudication. An inter-rater agreement analysis was performed to determine the reproducibility between the two reviewers using Cohen’s kappa statistic (κ). A κ value ≤ 0.2 indicates slight agreement, 0.21–0.4 fair agreement, 0.41–0.6 moderate agreement, and > 0.6 substantial agreement[15]. Comparisons of categorical variables were performed using the Fisher’s exact test, and comparisons of quantitative variables were performed using the Student’s t-test. The probability of survival was estimated using the Kaplan–Meier method from the date of the histological diagnosis to the date of last follow-up or death, and differences between curves were assessed using the Log-rank test. All calculations were performed using SPSS software package version 28.0 (SPSS Inc, IBM Corp, Armonk, New York), and p values < 0.05 (two-sided) were considered significant.
The design of the study was approved by the institutional review board and conducted according to the European ethical guidelines (MR004 n°20_5178).
Results
Tumor characteristics
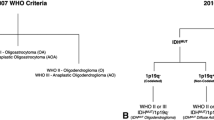
We retrospectively identified 426 patients who met the inclusion criteria (flowchart in Fig. 1). The tumor population consisted in 31 molecular GBM, 294 IDH-wild-type GBM, 50 grade II or grade III IDH-mutant astrocytomas, and 51 grade II or grade III IDH-mutant and 1p19q codeleted oligodendrogliomas (Table 1). Molecular GBM presented as an IDH-wild-type grade II astrocytoma in 10/31 (32%) patients and as an IDH-wild-type anaplastic astrocytoma in 21/31 (68%) patients, and were classified as molecular GBM because of the presence of a TERTp mutation (30/31, 97%) or/and an EGFR amplification (16/31, 52%). A T2-FLAIR mismatch was identified in 11/95 (12%) patients presenting non-enhancing tumors. All of these patients had an IDH-mutant astrocytoma (11/50; 22%).
Detection of gyriform infiltration
Gyriform infiltration was observed in 56 (13%) patients (Table 2). Representative examples are shown in Fig. 2. Blinded MRI analysis found a substantial inter-rater agreement for gyriform infiltration identification with a κ of 0.69 (p < 0.001; 95% confidence interval [0.61; 0.77]). Both reviewers identified gyriform infiltration as present in 43 (10%) cases and as absent in 351 (82%) cases; 31 (8%) cases were discordant, among these, a gyriform infiltration was identified by reviewer 1 only in 20 cases and by reviewer 2 only in 11 cases. After second assessment, no discordant case remained: the 31 discordant cases were finally considered as gyriform-infiltration-positive for 13 and gyriform-infiltration-negative for 18. In the latter cases, the reason for finally considering the gyriform as absent was related to the non-limitation of the infiltration to the cortex (it also involved the underlying white matter) or the limitation of the infiltration to the white matter (see Supplementary Figure).
Progression of gyriform infiltration
A total of 38 patients with gyriform infiltration had an MRI scan performed during follow-up for radiological review to assess the progression of the sign, which was indeed observed in 28 cases: 20 patients developed contrast enhancement at the site of the gyriform infiltration within a median time of 2 months and 8 patients developed an infiltration of the underlying white matter. Only one patient displayed a partial regression of the gyriform infiltration 6 months after radiochemotherapy. The gyriform infiltration was stable for the remaining 9 patients.
Characteristics of gyriform-infiltration-positive patients
Among the patients with a gyriform infiltration, 54/56 (96%) patients had an IDH-wild-type TERTp-mutant glioma and 2 (4%) had an IDH-wild-type TERTp-wild-type glioma. A gyriform infiltration was observed in 16/31 (52%) patients with a molecular GBM, 40/294 (14%) patients with a GBM IDH-wild-type, but in none of the patients with an astrocytoma IDH-mutant or an oligodendroglioma IDH-mutant and 1p19q codeleted. The gyriform infiltration was significantly more frequent in the subgroup of molecular GBM than in other groups (p < 0.001).
Compared to gyriform-infiltration-negative patients, gyriform-infiltration-positive patients were older at diagnosis (mean age: 63.4 vs 59.6 years, p = 0.018), had tumors less accessible to surgical resection (11% vs 39%, p < 0.001), and had more frequently an EGFR amplified (59% vs 30%, p < 0.001) or TERTp-mutant glioma (96% vs 81%, p < 0.001). Regarding radiological characteristics, compared to gyriform-infiltration-negative patients, gyriform-infiltration-positive patients were more in proportion to display multicentric or multifocal tumors (38% vs 15%, p < 0.001), which were more frequently associated with gliomatosis (64% vs 10%, p < 0.001), more frequently located in the insula (41% vs 25%, p = 0.014) and the thalamus (23% vs 6%, p < 0.001), and displayed more frequently poorly delimited edges (91% vs 72%, p = 0.002; Table 2).
Diagnostic value
The Sp, Se, PPV, and NPV of the presence of a gyriform infiltration for the diagnosis of molecular GBM were 90%, 52%, 29%, and 96%, respectively, in the whole series, and 97%, 48%, 85%, and 85%, respectively, among patients presenting non-enhancing tumors (n = 95). In the whole series, the Sp, Se, PPV, and NPV of the presence of a gyriform infiltration for the diagnosis of an IDH-wild-type TERTp-mutant glioma were 97%, 15%, 96%, and 19%, respectively. In the subgroup of patients presenting non-enhancing tumors, all the tumors displaying the gyriform infiltration sign (n = 13) were aggressive grade IV TERTp-mutant gliomas (11 molecular GBM and 2 IDH-wild-type GBM).
Impact of gyriform infiltration on outcome
At the time of analysis, 187 (44%) patients had died. The median follow-up duration was 14.9 months and the median overall survival (OS) was 23.2 months in the entire cohort. There was a significant difference in the median OS between patients with gyriform-infiltration-positive compared to gyriform-infiltration-negative diffuse gliomas (16.9 vs 25.6 months, p = 0.005). This difference was also significant in the subgroup of patients with non-enhancing tumors (20.2 months vs not reached, p < 0.001; Fig. 3) but not maintained if only IDH-wild-type gliomas were considered. Also, the difference was not observed in the subgroup of patients with IDH-wild-type GBM and molecular GBM (Fig. 3c; 16.9 months vs 16.0 months, p = 0.07).
Survival probability according to the presence of a gyriform infiltration. Kaplan–Meier overall survival curves for patients with (GI +) and without (GI-) gyriform infiltration in the entire cohort (a Log-rank test: 16.9 months vs 25.6 months, p = 0.005), in the subgroup of patients with non-enhancing lesions (b 20.2 months vs not reached, p < 0.001), and in the subgroup of patients with IDH-wild-type GBM and molecular GBM (c 16.9 months vs 16.0 months, p = 0.07)
Discussion
Early identification of poor prognosis gliomas is of utmost importance to allow rapid diagnosis and treatment. Herein we showed that the presence of a gyriform infiltration is a specific imaging marker for molecular GBM and more generally for IDH-wild-type TERTp-mutant gliomas. To the best of our knowledge, our study is the first one to analyze the gyriform infiltration diagnostic value in gliomas.
Radiological presentation of molecular glioblastomas
Molecular GBM have been previously shown to have a radiological presentation different from that of IDH-mutant LGG and IDH-wild-type GBM (diagnosis based on the presence of microvascular proliferation or necrosis), characterized by frequent temporo-insular location, thalamic involvement, gliomatosis, and gyriform infiltration [4]. The analysis of the radiological presentation of molecular glioblastomas performed in the present study using an independent cohort validates these findings, which are also consistent with those of other studies showing a high frequency of temporoinsular location, thalamic involvement, and gliomatosis in molecular GBM [16,17,18]. However, except once [4], the presence of a gyriform infiltration has not been reported as a hallmark of molecular GBM elsewhere. Some authors have reported that nearly half of IDH-wild-type GBM displayed non-enhancing cortical signal abnormalities, defined as non-enhancing FLAIR hyperintensity in the cortex contiguous with the area of tumoral enhancement, and that these cortical abnormalities could be associated in 5–10% of cases with distant non-enhancing lesions [19, 20]. However, these abnormalities generally involved both the grey and white matter adjacent to the tumor, and are therefore different from the gyriform infiltration sign reported herein, which consists in an infiltration limited to the grey matter [21]. Gyriform infiltrations have been previously reported as present in a third of molecular GBM and 15% IDH-wild-type GBM, but virtually absent in IDH-mutant astrocytomas and IDH-mutant and 1p/19q codeleted oligodendrogliomas [4]. The present study validates these findings. Another characteristic of molecular GBM is that they frequently lack contrast enhancement, which can wrongly suggest a lower-grade glioma. In the present study, 74% of molecular GBM displayed no contrast enhancement, highlighting the need for imaging biomarkers to differentiate these tumors from actual low-grade gliomas.
Diagnostic and prognostic value of the gyriform infiltration
Herein we found that gyriform infiltration was a specific biomarker for molecular GBM that could be identified with a substantial inter-rater agreement, similar to that of the recently described T2-FLAIR mismatch sign in IDH-mutant astrocytomas [9] or the Fluid attenuation sign in non-contrast-enhancing tumor, correlated with IDH glioblastoma [22]. We found that tumors displaying gyriform infiltration were more infiltrative and more frequently associated with gliomatosis likely explaining why patients with gyriform infiltration tumors more frequently underwent a biopsy than a surgical resection. However, differentiating gyriform infiltration from cortical and subcortical infiltration is not always easy on T2 FLAIR sequences, especially when the infiltration is located in the internal temporal lobe. In such cases, T2w coronal sequences may be more appropriate (see Supplementary Figure). A previous study showed that infiltration of grey matter (as patterns of non-contrast-enhancing tumor) in glioblastoma was correlated with the IDH1 mutation status [23]. In addition to its diagnostic value, we found that gyriform infiltration was associated with a poorer prognosis in the entire cohort and in the subgroup of patients presenting non-enhancing tumors. In this population, the gyriform infiltration sign could be a precious imaging marker for the early identification of non-enhancing gliomas with poor prognosis, not suitable to the wait-and-scan strategy that can be proposed for some LGG.
Consequences for radiotherapy planning
Currently, there is no recommendation regarding the inclusion of gyriform infiltration—and more generally remote unconnected and non-enhancing lesions—in the clinical target volume (CTV). One strategy could be to include these lesions and consider all FLAIR hypersignal in CTV, although it could lead to an important treatment volume. Another strategy could be to focus radiotherapy on the enhancing lesion which is the site of tumor recurrence in most cases [24, 25] and to consider that systemic treatment (temozolomide) will treat other distant non-enhancing lesions. However, in a recent study focusing on 12 patients with multicentric non-enhancing lesions in GBM, 12 of 16 identified non-enhancing lesions were included in the radiation field: during follow-up, 9 remained unchanged and 7 progressed (with the appearance of an enhancing component in 6 lesions)[20]. The 4 non-enhancing lesions not treated were all progressive within a short delay, appearing as aggressive enhancing lesions. These results, combined with ours showing a progression in 70% of cases of gyriform infiltration within a short delay, support the inclusion of gyriform infiltration in the treated volume. It could be an alternative option to surgery, which is very challenging in these cortical areas with a high risk of functional damages. When gyriform infiltration is associated with gliomatosis and multicentric lesions, a radiation protocol including the whole brain in association with temozolomide can be another strategy in selected patients [26, 27].
Limitations and perspectives
Our study is limited by its single-center design and by the fact that molecular GBM were only defined by the presence of a TERTp mutation and/or an EGFR amplification. There was no case only defined by the presence of a combined chromosome 7 gain and chromosome 10 loss. Although these cases are rare (about 10% of molecular GBM [3]), future studies are needed to determine whether these molecular GBM frequently present a gyriform infiltration. Additionally, some patients were not included in the analysis because of the lack of some MRI sequences (especially T2 FLAIR sequences). Confounding bias could be related to the prognosis value of gyriform infiltration, for example patients with tumors displaying gyriform infiltration were more in proportion to have had a biopsy rather than a complete surgery. Finally, we cannot exclude occurrence of a disease spectrum bias due to the retrospective design with missing data.
The strength of our study lies in the large sample size and in the blinded assessment of the gyriform infiltration sign. Nevertheless, future studies will be needed to validate our findings and to understand the pathophysiology of gyriform infiltration. Scherer has described invasion patterns in glioblastoma and defined “secondary structures” corresponding to mechanisms by which glioma cells spread from preexisting tissue elements [28]. We think that the gyriform infiltration could be explained by perineuronal satellitosis and surface (subpial) growth (2 of the 4 “secondary structures of Scherer”). There is probably microscopic communication between the principal tumor and this elective cortical infiltration that cannot be detected due to the imaging resolution. These hypotheses will need to be confirmed by a dedicated histopathological study.
Conclusion
An elective gyriform infiltration on T2 FLAIR MRI sequences constitutes a highly specific imaging marker of IDH-wild-type TERTp-mutant gliomas especially in the molecular GBM subgroup, with a good inter-rater agreement. This sign is associated with a poor prognosis and could be helpful to guide the clinical decision preoperatively for patients with non-enhancing tumors.
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Louis DN, Perry A, Wesseling P et al (2021) The 2021 WHO classification of tumors of the central nervous system: a summary. Neuro Oncol 23:1231–1251. https://doi.org/10.1093/neuonc/noab106
Louis DN, Wesseling P, Aldape K et al (2020) cIMPACT-NOW update 6: new entity and diagnostic principle recommendations of the cIMPACT-Utrecht meeting on future CNS tumor classification and grading. Brain Pathol 30:844–856. https://doi.org/10.1111/bpa.12832
Stichel D, Ebrahimi A, Reuss D et al (2018) Distribution of EGFR amplification, combined chromosome 7 gain and chromosome 10 loss, and TERT promoter mutation in brain tumors and their potential for the reclassification of IDHwt astrocytoma to glioblastoma. Acta Neuropathol 136:793–803. https://doi.org/10.1007/s00401-018-1905-0
Izquierdo C, Barritault M, Poncet D et al (2019) Radiological characteristics and natural history of adult IDH-wildtype astrocytomas with TERT promoter mutations. Neurosurgery 85:E448–E456. https://doi.org/10.1093/neuros/nyy513
Metellus P, Coulibaly B, Colin C et al (2010) Absence of IDH mutation identifies a novel radiologic and molecular subtype of WHO grade II gliomas with dismal prognosis. Acta Neuropathol 120:719–729. https://doi.org/10.1007/s00401-010-0777-8
Juratli TA, Tummala SS, Riedl A et al (2019) Radiographic assessment of contrast enhancement and T2/FLAIR mismatch sign in lower grade gliomas: correlation with molecular groups. J Neurooncol 141:327–335. https://doi.org/10.1007/s11060-018-03034-6
van Lent DI, van Baarsen KM, Snijders TJ, Robe PAJT (2020) Radiological differences between subtypes of WHO 2016 grade II-III gliomas: a systematic review and meta-analysis. Neuro Oncol Adv 2:vdaa04
Choi C, Ganji SK, DeBerardinis RJ et al (2012) 2-hydroxyglutarate detection by magnetic resonance spectroscopy in IDH-mutated patients with gliomas. Nat Med 18:624–629. https://doi.org/10.1038/nm.2682
Broen MPG, Smits M, Wijnenga MMJ et al (2018) The T2-FLAIR mismatch sign as an imaging marker for non-enhancing IDH-mutant, 1p/19q-intact lower-grade glioma: a validation study. Neuro Oncol 20:1393–1399. https://doi.org/10.1093/neuonc/noy048
Patel SH, Poisson LM, Brat DJ et al (2017) T2-FLAIR mismatch, an imaging biomarker for IDH and 1p/19q status in lower-grade gliomas: A TCGA/TCIA project. Clin Cancer Res 23:6078–6085. https://doi.org/10.1158/1078-0432.CCR-17-0560
Foltyn M, Nieto Taborda KN, Neuberger U et al (2020) T2/FLAIR-mismatch sign for noninvasive detection of IDH-mutant 1p/19q non-codeleted gliomas: validity and pathophysiology. Neuro Oncol Adv 2:vdaa004
Meyronet D, Esteban-Mader M, Bonnet C et al (2017) Characteristics of H3 K27M-mutant gliomas in adults. Neuro Oncol 19:1127–1134. https://doi.org/10.1093/neuonc/now274
Labussière M, Boisselier B, Mokhtari K et al (2014) Combined analysis of TERT, EGFR, and IDH status defines distinct prognostic glioblastoma classes. Neurology 83:1200–1206. https://doi.org/10.1212/WNL.0000000000000814
Simon M, Hosen I, Gousias K et al (2015) TERT promoter mutations: a novel independent prognostic factor in primary glioblastomas. Neuro Oncol 17:45–52. https://doi.org/10.1093/neuonc/nou158
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Tesileanu CMS, Dirven L, Wijnenga MMJ et al (2020) Survival of diffuse astrocytic glioma, IDH1/2 wildtype, with molecular features of glioblastoma, WHO grade IV: a confirmation of the cIMPACT-now criteria. Neuro Oncol 22:515–523. https://doi.org/10.1093/neuonc/noz200
Lee D, Riestenberg RA, Haskell-Mendoza A, Bloch O (2021) Diffuse astrocytic glioma, IDH-wildtype, with molecular features of glioblastoma, WHO grade IV: a single-institution case series and review. J Neurooncol 152:89–98. https://doi.org/10.1007/s11060-020-03677-4
Aoki K, Nakamura H, Suzuki H et al (2018) Prognostic relevance of genetic alterations in diffuse lower-grade gliomas. Neuro Oncol 20:66–77. https://doi.org/10.1093/neuonc/nox132
Lasocki A, Gaillard F, Tacey MA et al (2016) The incidence and significance of multicentric noncontrast-enhancing lesions distant from a histologically-proven glioblastoma. J Neurooncol 129:471–478. https://doi.org/10.1007/s11060-016-2193-y
Benouaich-Amiel A, Khasminsky V, Gal O et al (2021) Multicentric non-enhancing lesions in glioblastoma: a retrospective study. J Clin Neurosci 85:20–26. https://doi.org/10.1016/j.jocn.2020.11.050
Lasocki A, Gaillard F, Tacey M et al (2016) Incidence and prognostic significance of non-enhancing cortical signal abnormality in glioblastoma. J Med Imaging Radiat Oncol 60:66–73. https://doi.org/10.1111/1754-9485.12421
Patel SH, Batchala PP, Muttikkal TJE et al (2021) Fluid attenuation in non-contrast-enhancing tumor (nCET): an MRI marker for isocitrate dehydrogenase (IDH) mutation in glioblastoma. J Neurooncol 152:523–531. https://doi.org/10.1007/s11060-021-03720-y
Lasocki A, Gaillard F, Tacey M et al (2018) Morphologic patterns of noncontrast-enhancing tumor in glioblastoma correlate with IDH1 mutation status and patient survival. J Clin Neurosci 47:168–173. https://doi.org/10.1016/j.jocn.2017.09.007
Milano MT, Okunieff P, Donatello RS et al (2010) Patterns and timing of recurrence after temozolomide-based chemoradiation for glioblastoma. Int J Radiat Oncol Biol Phys 78:1147–1155. https://doi.org/10.1016/j.ijrobp.2009.09.018
Brandes AA, Tosoni A, Franceschi E et al (2009) Recurrence pattern after temozolomide concomitant with and adjuvant to radiotherapy in newly diagnosed patients with glioblastoma: correlation With MGMT promoter methylation status. J Clin Oncol 27:1275–1279. https://doi.org/10.1200/JCO.2008.19.4969
Lahmi L, Idbaih A, Rivin Del Campo E et al (2019) Whole brain radiotherapy with concurrent temozolomide in multifocal and/or multicentric newly diagnosed glioblastoma. J Clin Neurosci 68:39–44. https://doi.org/10.1016/j.jocn.2019.07.065
Showalter TN, Andrel J, Andrews DW et al (2007) Multifocal glioblastoma multiforme: prognostic factors and patterns of progression. Int J Radiat Oncol Biol Phys 69:820–824. https://doi.org/10.1016/j.ijrobp.2007.03.045
Scherer HJ (1938) Structural development in gliomas. Am J Cancer 34:333–351
Acknowledgements
We thank Helene Boyer (from DRCI department of HCL) for the review of this manuscript (English writing).
Funding
This analysis was not funded.
Author information
Authors and Affiliations
Contributions
The corresponding author certifies that all authors have made substantial contributions to all of the following: EM, FD: conception and design of the study, analysis and interpretation of data, acquisition of data, MRI analysis, EM: statistical analysis, All authors: drafting the article or revising it critically for important intellectual content, All authors: Final approval of the version to be submitted.
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mesny, E., Barritault, M., Izquierdo, C. et al. Gyriform infiltration as imaging biomarker for molecular glioblastomas. J Neurooncol 157, 511–521 (2022). https://doi.org/10.1007/s11060-022-03995-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-022-03995-9