Abstract
Citrate-coated silver nanoparticles (citrate-AgNPs) are among the most commonly used nanomaterials, widely present in industrial and biomedical products. In this study, the cytotoxicity of 30-nm citrate-AgNPs on the macrophage cell line RAW 264.7 was evaluated, using a battery of cytotoxicity endpoints (viability, oxidative stress, and cytostaticity/clastogenicity), at 24 and 48 h of exposure. Citrate-AgNPs decreased cell proliferation and viability only at 75 μg/mL, suggesting a low sensitivity of RAW cells to lower doses of these AgNPs. After 24 h of exposure, ROS content decreased in cells exposed to 60 μg/mL AgNPs (IC20 value), corroborating the high tolerance of these cells to citrate-AgNPs. However, these cells suffered an impairment of the cell cycle, shown by an increase at the sub-G1 phase. This increase of the sub-G1 population was correlated with an increase of DNA fragmentation, suggesting an increase of apoptosis. Thus, our data are important to understand the effects of low concentrations (IC20) of citrate-AgNPs on in vitro vital macrophage functions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Advances in nanotechnology have enabled great benefits in many fields, such as engineering, information technology, diagnostics, and medical treatments (for example photodynamic therapy to treat cancer) (Diaz-Diestra et al. 2015), among others (Liu 2006; Salata 2004). The antibacterial effects of silver nanoparticles (AgNPs) are well known, rendering a wide range of applications from medicine and industry to household and personal care products or clothing (Abdelhalim and Jarrar 2011; Behra et al. 2013; Benn and Westerhoff 2008; Eckhardt et al. 2013; Nowack et al. 2011; Varner et al. 2010). This extensive use of AgNPs raises the concern about their safety and possible impacts on the environment and human health (Nowack and Bucheli 2007; Oberdorster et al. 2005). Thus, it is important to study their putative toxic effects on biological systems and to improve current understanding of toxicity mechanisms in mammalian cells. Several in vitro studies have reported toxic effects of AgNPs towards different types of human cells (Li et al. 2014; Smita et al. 2012; Zhang et al. 2014), but the mechanisms of AgNP-induced toxicity are not completely understood (Browning et al. 2013). Also, the susceptibility of different cell types to AgNPs should be more deeply investigated (Zhang et al. 2015). The cell-dependent toxicity could reflect, besides inherent characteristics of the cells, differences in AgNP dissolution, cellular uptake, bioavailability, or the generation of oxidative stress (AshaRani et al. 2009; Avalos et al. 2014; Wang et al. 2014).
As often reported, AgNPs are coated to promote stability and avoid aggregation by citrate being the most commonly used reducing agent, which stabilizes the NPs by electrostatic repulsion (Sharma et al. 2009). Zhang et al. (2014) reported that citrate coating improved the stability of AgNPs while decreasing their toxicity. Nevertheless, other studies found that citrate-coated AgNPs (20 and 10 nm) could be cytotoxic to human bronchial epithelial cells at concentrations ≥6.25 μg/mL (Wang et al. 2014) and to rat brain endothelial cells at concentrations ≥10 μg/mL (Grosse et al. 2013). However, more research is needed to determine the cytotoxic potential of AgNPs with different physicochemical properties and in different cell types.
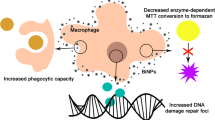
The response of macrophages to nanoparticles is an important area of investigation since these cells play a crucial role in the early-stage defense barriers against foreign objects (Park et al. 2011). In particular, macrophages play a major role in the phagocytic removal of NPs from the bloodstream, contributing to minimize their organ deposition and toxicity (Mukherjee et al. 2014).
In this report, we aimed at evaluating the effects of well-characterized citrate-coated AgNPs on macrophage’s viability, intracellular ROS production, and cell cycle profile. For that purpose, the RAW 264.7 cell line was exposed to 30-nm citrate-AgNPs. This cell line is a model macrophage cell type, which is commonly used for hazard assessment and mechanistic studies in nanotoxicology (Munusamy et al. 2015; Orr et al. 2011).
Material and methods
Chemicals
Sterile, purified, and endotoxin-free silver nanoparticles (Biopure AgNPs 1.0 mg/mL), with a diameter of 30 nm and a citrate surface, were purchased from Nanocomposix Europe (Prague, Czech Republic). Dulbecco’s modified Eagle’s medium (DMEM), fetal bovine serum (FBS), antibiotics, and phosphate buffer saline (PBS, pH 7.4) were purchased from Life Technologies (Carlsbad, CA, USA). 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) and dimethyl sulfoxide (DMSO) were obtained from Sigma-Aldrich (St. Louis, MO, USA). Dichlorodihydrofluorescein diacetate (DCFH2-DA) was purchased from Sigma-Aldrich, St. Louis, MO, USA. RNase and propidium iodide (PI) used in cell cycle assay were purchased from Sigma-Aldrich (St. Louis, MO, USA).
Physicochemical characterization of AgNPs
AgNP characterization was performed through assessment of the hydrodynamic diameter and polydispersity index (PdI) by dynamic light scattering (DLS) and of the zeta potential by electrophoretic mobility, both measurements using a Zetasizer Nano ZS (Malvern Instruments, UK).
Cell culture
The RAW 264.7 cell line was kindly provided by Dr. Philipp Seib, University of Strathclyde (Glasgow, UK). Cell culture reagents were purchased from Life Technologies (Carlsbad, CA, USA). The cells were grown in complete medium, i.e., Dulbecco’s modified Eagle’s medium, supplemented with 10% fetal bovine serum (FBS), 2 mM l-glutamine, 100 U/mL penicillin, 100 μg/mL streptomycin, and 250 μg/mL fungizone, at 37 °C in 5% CO2 humidified atmosphere. Cells were daily observed under an inverted phase-contrast Eclipse TS100 microscope (Nikon, Tokyo, Japan). For each experiment, cells were allowed to adhere for 24 h and then medium was replaced with fresh new medium containing citrate-AgNPs. The effects were measured after 24 and 48 h. Throughout the experiments, cultures were routinely visualized for confluence and cell morphology.
Viability assay
Cell viability was determined by the colorimetric MTT assay (Twentyman and Luscombe 1987). Cells were seeded in 96-well plates and cultured as described above. Cell viability was measured after 24 and 48 h of citrate-AgNP exposure at the concentrations 0, 0.5, 5, 10, 25, 50, and 75 μg/mL. Fifty microliters of MTT (1 mg/mL) in phosphate-buffered saline (PBS) were then added to each well and incubated for 4 h at 37 °C, 5% CO2. Medium was then removed, and 150 μL of DMSO was added to each well for solubilization of formazan crystals. The optical density of reduced MTT was measured at 570 nm in a microtiter plate reader (Synergy HT Multi-Mode, BioTeK, Winooski, VT). Three independent assays were performed with at least two technical replicates each and the results compared with the control (no exposure). From the MTT results, the IC50 and IC20 values (calculated through SigmaPlot) were 87 and 60 μg/mL at 24 h of exposure and 79.8 and 61.4 μg/mL at 48 h of exposure, respectively. The IC20 concentration at 24 h of exposure was selected for further assays, since we were interested in evaluating the sub-toxic effects of citrate-AgNPs to macrophages.
Intracellular ROS formation
Intracellular ROS production was assessed by flow cytometry (FCM) with the use of DCFH2-DA fluorescent probe, as described previously (Ferreira de Oliveira et al. 2014). This probe enters the cells and is deacetylated by cellular esterases producing non-fluorescent DCFH2 and diacetate. In the cytosol, DCFH2 is quickly oxidized to fluorescent DCF by intracellular ROS. Cells were plated in 6-well plates and after AgNP exposure, the medium was discarded and cells were incubated for 30 min, at 37 °C, in the dark with serum-free DMEM containing 10 mM DCFH2-DA. Cells were washed with PBS, trypsinized, and collected for analysis. Acquisitions were made using a Coulter EPICS XL flow cytometer (Coulter Electronics, Hialeah, Florida, USA) equipped with an argon laser (15 mW, 488 nm) and the SYSTEM II software v. 3.0 (Beckman Coulter, Hialeah, FL). ROS formation was estimated from the median fluorescence intensity (MFI) of DCF using the FlowJo software (Tree Star Inc., Ashland, OR-USA). For each sample, the number of events reached at least 10,000.
Cell cycle and clastogenicity analysis
Cell cycle and putative clastogenic effects were analyzed by FCM according to the method previously described (Oliveira et al. 2014). Briefly, cells were seeded in 6-well plates and after exposure, they were harvested through scrapping and centrifuged twice at 300×g for 5 min. Cells were then fixed with 85% cold ethanol and kept at −20 °C until analysis. At the time of analysis, cells were centrifuged at 300×g for 5 min, resuspended in PBS, and filtered through a 35-μm nylon mesh to separate aggregates. Then, 50 μL RNase (1 mg/mL) and 50 μL propidium iodide (PI) (1 mg/mL) were added to each sample which was then incubated for 20 min in darkness at room temperature until analysis. The relative fluorescence intensity of the stained nuclei was measured in a Coulter XL Flow Cytometer (Beckman Coulter, Hialeah, FL-USA) equipped with an argon laser (15 mW, 488 nm). Acquisitions were made using SYSTEM II software v. 3.0 (Beckman Coulter, Hialeah, FL). For each sample, the number of nuclei analyzed was approximately 5000. The percentage of nuclei in each phase of the cell cycle (G0/G1, S and G2 phases) was analyzed using the FlowJo software (Tree Star Inc., Ashland, Oregon, USA). In order to assess the putative clastogenic effects of Cit30 AgNPs, as described by Misra and Easton (1999), the coefficient of variation (CV) of the G0/G1 peak was determined.
Statistical analysis
The results are reported as mean ± standard deviation (SD) of two technical replicates in each of the three independent experiments. For all the assays, the statistical significance between control and exposed cells was performed by one-way ANOVA, followed by Dunnet and Dunn’s method (as parametric and non-parametric test, respectively), using Sigma Plot 12.5 software (Systat Software Inc.). The differences were considered statistically significant from p < 0.05.
Results
Physicochemical characterization of AgNPs
The main properties of citrate-coated AgNPs dispersed in water or in culture medium are summarized in Table 1, while a more detailed characterization has been previously reported (Bastos et al. 2016a). The increase in hydrodynamic diameter (Dh) from 43.3 nm in water to 64.8 nm in culture medium, together with the increase in zeta potential (from −42.7 to −8.5 mV), likely reflects the displacement of citrate and the formation of a protein corona.
Effects on cell growth, viability and ROS
In control conditions, RAW 264.7 cells showed a typical confluence profile and morphology (Fig. 1a, c). When cells were exposed to 75 μg/mL citrate-AgNPs, their confluence decreased (Fig. 1b, d), especially after 48 h of exposure (Fig. 1d). Moreover, there were some alterations in cellular morphology and semblance of phagosomes, including an increase of granularity and darker aspect (Fig. 1a, b).
The viability of RAW 264.7 cells was negatively affected by citrate-AgNPs (Fig. 2). In particular, cell viability was significantly reduced (p < 0.05) relatively to controls at 75 μg/mL AgNPs, after both exposure times (24 and 48 h).
Relative cell viability (%) of RAW 264.7 after exposure to 30-nm citrate-AgNPs for 24 and 48 h, measured by MTT assay. Data expressed as mean and standard deviation. Asterisk indicate significant differences between control at p < 0.05 for 24 h and number sign indicate significant differences between control at p < 0.05 for 48 h
As stated in the “Materials and methods” section, the IC20 concentration at 24 h of exposure (60 μg/mL), calculated from the MTT dose-response curve, was selected for further assays.
The intracellular ROS production is shown in Fig. 3. Citrate-AgNPs significantly decreased ROS production in RAW 264.7 cells at the concentration of 60 μg/mL after 24 h of exposure.
Cell cycle and clastogenicity
Figure 4 show that AgNPs at IC20 deeply injured the cell cycle of RAW 264.7 cells. Citrate-AgNPs induced a significant increase in the percentage of cells in sub-G1 phase and a significant decrease in the percentage of cells in S and G2 phases (p < 0.05). Furthermore, there was a significant increase in the coefficient of variation (CV) of G1 peak after exposure to AgNPs (p < 0.01). Example histograms obtained for control and 24-h-exposed (60 μg/mL AgNPs) cells are presented in Fig. 5.
Effects of 60 μg/mL citrate-AgNPs on RAW 264.7 cell cycle dynamics after 24 h of exposure, measured by flow cytometry. The results were expressed as mean and standard deviation. *Significant differences between control at p < 0.05. In the graph is represented the coefficient of variation (CV) of G0/G1 peak values of the respective conditions
Discussion
The toxicity of AgNPs to macrophages has been previously explored in some studies (e.g., Hamilton et al. 2014; Shannahan and Sowrirajan 2015). Hamilton et al. (2014) showed that, regardless of coating (citrate or PVP), smaller AgNPs (20 nm) were more toxic to THP-1 macrophages than were larger AgNPs. It was also demonstrated that macrophages internalize AgNP agglomerates via actin-dependent endocytosis mediated by scavenger receptors (Wang et al. 2012), and that the expression of some inflammatory-related transcripts was upregulated in RAW 264.7 cells and bone marrow-derived macrophages (BMDMs) exposed to 20-nm-citrate-coated AgNPs (Aldossari et al. 2015).
Our data contributes to clarify the influence of citrate-AgNPs on macrophage cells, by using a toolbox of toxicity endpoints to determine if low citrate-AgNP concentrations (IC20) affect vital macrophage functions in vitro.
As part of the immune system, white blood cells have great capacity to destroy or remove foreign matter from the body. More specifically, macrophages actively perform phagocytic functions, engulfing the particles and creating phagosomes that will fuse with lysosomes containing hydrolytic enzymes during their maturation process. The acidic environment in the lysosomes can further contribute to dissolve the AgNPs into ions. Thus, macrophages are a relevant cell model to perform nanotoxicity testing. Our results showed that RAW 264.7 cells only reduced their viability by 20% after exposure to 60 μg/mL citrate-AgNPs, showing higher tolerance to these NPs than other cell lines that we have previously investigated. For instance, our previous results showed that the IC50 values for 30-nm citrate-coated AgNPs for human keratinocytes (HaCaT) and for hepatoma (HepG2) cells were 40 μg/mL (Bastos et al. 2016a) and 11 μg/mL (Bastos et al. 2016b), respectively, while the maximum concentration tested in RAW 264.7 cells (75 μg/mL) only induced an ∼34% decrease in viability. This comparison demonstrates that different cell types have different susceptibility to AgNPs and that the toxicological profile of AgNPs should not be generalized for individual nanoparticles and instead should be determined in each different cell line. This observation that macrophages have higher tolerance towards AgNPs could be related to their phagocytic functions and their capacity to destroy or remove foreign matter from the body and is in agreement with the results found by others. For instance, Kaur and Tikoo (2013) found that RAW 264.7 macrophages presented the least cell viability reduction (21% cell death) at 100 μg/ml of TSNPs (AgNPs synthesized by reduction with tannic acid) compared with A431 (skin epithelial) and A549 (lung epithelial) cells. They also concluded that RAW 264.7 cells “engulf” AgNPs and thus resist to toxic effects. Zhang et al. (2015) exposed RAW 264.7 cells to a range of citrate-AgNP concentrations (0.1–50 μg/mL) and also obtained less than 20% of viability reduction. On the other hand, a study on the cytotoxic potential of tannic acid-modified AgNPs (13, 33, and 46 nm) reported a significant decrease on viability of RAW 264.7 cells after exposure to 2.5 μg/mL (Orlowski et al. 2013). Other studies on the toxicity of AgNPs (dispersed with silica) in the same cell type highlighted the influence of size and of Ag + ion release on their toxic potential (Pratsinis et al. 2013). The authors obtained significant viability decrease after exposure to ∼20-nm AgNPs for concentrations ≥20 μg/mL, while for ∼10-nm AgNPs, a significant decrease took place at concentrations ≥10 μg/mL. A study on the cytotoxic effects of AgNPs coated with a peptide layer on a human macrophage cell line (THP-1) reported IC50 values of 110 μg/mL for 20-nm AgNPs and 140 μg/mL for 40-nm AgNPs after 24 h of exposure; these values significantly decreased for 48-h exposures (18 and 30 μg/mL for 20- and 40-nm AgNPs, respectively), thus stressing the size and time dependence of AgNP toxicity (Haase et al. 2011).
Although the induction of ROS is a common in vitro response to AgNP exposure (Arora et al. 2008; Hussain et al. 2005), we did not find evidence of ROS induction in RAW 264.7 cells; on the contrary, a 50% decrease in ROS levels was detected upon exposure to AgNPs at IC20. Other studies also showed absence of ROS increase upon AgNP exposure. For instance, Gliga et al. (2014) found no changes in ROS generation in BEAS-2B cells exposed to AgNPs of 10–75 nm, uncoated or coated with PVP or citrate. In another study, Kaur and Tikoo (2013) found that TSNPs (AgNPs synthesized by reduction with tannic acid) at 50 μg/mL did not induce significant ROS generation in RAW macrophages while increasing in more sensitive cells (lung cell line A549 and epidermoid carcinoma cell line A-431). The hereby observed decrease of ROS levels in macrophages exposed to a low concentration of AgNPs supports the hypothesis that these cells present a good adaptive mechanism to cope with nanoparticles, possibly through the activation of multiple antioxidant mechanisms.
A significant increase in the sub-G1 population was observed in RAW 264.7 cells exposed to AgNPs, which may possibly be related to DNA fragmentation often associated with apoptosis (Kajstura et al. 2007). After exposure of RAW 264.7 cells to 1.6 μg/mL AgNPs, Park et al. (2010) also obtained a significant increase of cells at the sub-G1 phase. Concerning cell cycle dynamics, RAW 264.7 cells were deeply affected by AgNP exposure with an arrest at G0/G1 phase, which may support the observed decreases of cells in both S and G2 phases. Moreover, since the increased dispersion of nuclear DNA content in a tissue-specific cell population is considered to be diagnostic for clastogenic damage, as characterized by an increase in the coefficient of variation, the significant increase in the coefficient of variation could be related to clastogenic potential of citrate-AgNPs on RAW 264.7 cells (Misra and Easton 1999). Sasidharan et al. (2011) obtained similar histograms for the nasopharyngeal carcinoma cell line (KB) after 24 h of exposure to 200 and 300 μM ZnO nanocrystals (NCs). Similarly, RAW 264.7 cells showed a decrease in S phase and increases in G0/G1 and sub-G1 phases after exposure to 0.01 μg/mL of SiO2 NPs (10 nm). The authors indicated that, although there was no decrease in cell viability, a subpopulation of cells (between 12 and 15% at sub-G1) underwent apoptosis (Bancos et al. 2015).
In comparison with our previous studies on the cell cycle effects of the same citrate-AgNPs towards keratinocytes (HaCaT cells) (Bastos et al. 2016a) or hepatoma (HepG2) cells (Bastos et al. 2016b), it is interesting to note that only RAW 264.7 macrophages showed an increase in the sub-G1 population. Moreover, upon 24 h of exposure to the IC20 concentration, a significant decrease in the percentage of RAW 264.7 cells in both S and G2 phases was observed, while for HaCaT or HepG2 cells, a decrease in G0/G1 phase and an arrest at G2 phase were observed. This comparison demonstrates that the different cell types respond differently to exposure to the same AgNPs in what concerns cell cycle dynamics. Thus, more research is needed to determine the toxicological profile of AgNPs among cell lines with different susceptibilities.
In conclusion, this study has contributed to the further understanding of the biological effects of citrate-coated AgNPs, which are widely present in industrial and biomedical products, towards macrophages, a cell type directly interacting with nanoparticles. Particularly, our study has shown that AgNPs induced a significant decrease on the viability of RAW 264.7 cells at concentrations above 75 μg/mL. Additionally, we found that intracellular ROS production was not induced, but a decrease in ROS levels was observed instead. On the other hand, AgNPs had a great impact on the cell cycle progression of these cells. Beyond the apparent cytostatic effect, AgNPs induced a subpopulation at sub-G1 phase, which might be associated to apoptosis. Thus, and having our previous works into account, we can conclude that the toxicity of AgNPs varies with the cell type, being more cytotoxic to the HepG2 and HaCaT cell lines than to RAW 264.7 cells. Therefore, more research should be done in order to determine the toxicity profile of the different-sized and coated AgNPs in each cell type.
References
Abdelhalim MAK, Jarrar BM (2011) Renal tissue alterations were size-dependent with smaller ones induced more effects and related with time exposure of gold nanoparticles. Lipids Health Dis 10(1):1
Aldossari AA, Shannahan JH, Podila R (2015) Scavenger receptor B1 facilitates macrophage uptake of silver nanoparticles and cellular activation. J Nanopart Res 17(7):1–14
Arora S, Jain J, Rajwade JM, Paknikar KM (2008) Cellular responses induced by silver nanoparticles: in vitro studies. Toxicol Lett 179(2):93–100
AshaRani P, Low Kah Mun G, Hande M, Valiyaveettil S (2009) Cytotoxicity and genotoxicity of silver nanoparticles in human cells. ACS Nano 3(2):279–290
Avalos A, Haza AI, Mateo D, Morales P (2014) Cytotoxicity and ROS production of manufactured silver nanoparticles of different sizes in hepatoma and leukemia cells. J Appl Toxicol 34(4):413–423
Bancos S, Stevens DL, Tyner KM (2015) Effect of silica and gold nanoparticles on macrophage proliferation, activation markers, cytokine production, and phagocytosis in vitro. Int J Nanomedicine 10:183–206
Bastos V, de Oliveira JF, Brown D, Johnston H, Malheiro E, Daniel-da-Silva AL, Duarte IF, Santos C, Oliveira H (2016a) The influence of citrate or PEG coating on silver nanoparticle toxicity to a human keratinocyte cell line. Toxicol Lett 249:29–41
Bastos V, Ferreira-de-Oliveira JM, Carrola J, Daniel-da-Silva AL, Duarte IF, Santos C, Oliveira H (2016b) Coating independent cytotoxicity of citrate- and PEG-coated silver nanoparticles on a human hepatoma cell line. J Environ Sci 51:191–201
Behra R, Sigg L, Clift M, Herzog F, Minghetti M, Johnston B, Petri-Fink A, Rothen-Rutishauser B (2013) Bioavailability of silver nanoparticles and ions: from a chemical and biochemical perspective. J R Soc Interface 10(87):20130396
Benn T, Westerhoff P (2008) Nanoparticle silver released into water from commercially available sock fabrics. Environ Sci Technol 42(11):4133–4139
Browning L, Lee K, Nallathamby P, Xu X-HN (2013) Silver nanoparticles incite size- and dose-dependent developmental phenotypes and nanotoxicity in zebrafish embryos. Chem Res Toxicol 26(10):1503–1513
Diaz-Diestra D, Beltran-Huarac J, Bracho-Rincon DP, González-Feliciano JA, González CI, Weiner BR, Morell G (2015) Biocompatible ZnS: Mn quantum dots for reactive oxygen generation and detection in aqueous media. Journal of Nanopart Res 17(12):461
Eckhardt S, Brunetto P, Gagnon J, Priebe M, Giese B, Fromm K (2013) Nanobio silver: its interactions with peptides and bacteria, and its uses in medicine. Chem Rev 113(7):4708–4754
Ferreira de Oliveira JM, Costa M, Pedrosa T, Pinto P, Remédios C, Oliveira H, Pimentel F, Almeida L, Santos C (2014) Sulforaphane induces oxidative stress and death by p53-independent mechanism: implication of impaired glutathione recycling. PLoS One 9(3):e92980
Gliga A, Skoglund S, Odnevall Wallinder I, Fadeel B, Karlsson H (2014) Size-dependent cytotoxicity of silver nanoparticles in human lung cells: the role of cellular uptake, agglomeration and Ag release. Part Fibre Toxicol 11(1):1
Grosse S, Evje L, Syversen T (2013) Silver nanoparticle-induced cytotoxicity in rat brain endothelial cell culture. Toxicol in Vitro 27(1):305–313
Haase A, Tentschert J, Jungnickel H, Graf P, Mantion A, Draude F, Plendl J, Goetz ME, Galla S, Masic A, Thuenemann AF, Taubert A, Arlinghaus HF, Luch A (2011) Toxicity of silver nanoparticles in human macrophages: uptake, intracellular distribution and cellular responses. J Phys Conf Ser 304(1):012030 IOP Publishing
Hamilton RF, Buckingham S, Holian A (2014) The effect of size on Ag nanosphere toxicity in macrophage cell models and lung epithelial cell lines is dependent on particle dissolution. Int J Mol Sci 15(4):6815–6830
Hussain SM, Hess KL, Gearhart JM, Geiss KT, Schlager JJ (2005) In vitro toxicity of nanoparticles in BRL 3A rat liver cells. Toxicol in Vitro 19(7):975–983
Kajstura M, Halicka HD, Pryjma J, Darzynkiewicz Z (2007) Discontinuous fragmentation of nuclear DNA during apoptosis revealed by discrete "sub-G1" peaks on DNA content histograms. Cytometry A 71(3):125–131
Kaur J, Tikoo K (2013) Evaluating cell specific cytotoxicity of differentially charged silver nanoparticles. Food Chem Toxicol 51:1–14
Li Y, Zhang Y, Yan B (2014) Nanotoxicity overview: nano-threat to susceptible populations. Int J Mol Sci 15(3):3671–3697
Liu WT (2006) Nanoparticles and their biological and environmental applications. J Biosci Bioeng 102(1):1–7
Misra R, Easton M (1999) Comment on analyzing flow cytometric data for comparison of mean values of the coefficient of variation of the G1 peak. Cytometry 36(2):112–116
Mukherjee D, Royce SG, Sarkar S, Thorley A, Schwander S, Ryan MP, Porter AE, Chung KF, Tetley TD, Zhang J, Georgopoulos PG (2014) Modeling in vitro cellular responses to silver nanoparticles. J Toxicol 2014
Munusamy P, Wang C, Engelhard MH, Baer DR, Smith JN, Liu C, Kodali V, Thrall BD, Chen S, Porter AE, Ryan MP (2015) Comparison of 20 nm silver nanoparticles synthesized with and without a gold core: structure, dissolution in cell culture media, and biological impact on macrophages. Biointerphases 10(3):031003
Nowack B, Bucheli T (2007) Occurrence, behavior and effects of nanoparticles in the environment. Environ Pollut 150(1):5–22
Nowack B, Krug H, Height M (2011) 120 years of nanosilver history: implications for policy makers. Environ Sci Technol 45(4):1177–1183
Oberdorster G, Maynard A, Donaldson K, Castranova V, Fitzpatrick J, Ausman K, Carter J, Karn B, Kreyling W, Lai D et al (2005) Principles for characterizing the potential human health effects from exposure to nanomaterials: elements of a screening strategy. Part Fibre Toxicol 2:8
Oliveira H, Monteiro C, Pinho F, Pinho S, Ferreira de Oliveira JM, Santos C (2014) Cadmium-induced genotoxicity in human osteoblast-like cells. Mutat Res Genet Toxicol Environ Mutagen 775-776:38–47
Orlowski P, Krzyzowska M, Zdanowski R, Winnicka A, Nowakowska J, Stankiewicz W, Tomaszewska E, Celichowski G, Grobelny J (2013) Assessment of in vitro cellular responses of monocytes and keratinocytes to tannic acid modified silver nanoparticles. Toxicol in Vitro 27(6):1798–1808
Orr GA, Chrisler WB, Cassens KJ, Tan R, Tarasevich BJ, Markillie LM, Zangar RC, Thrall BD (2011) Cellular recognition and trafficking of amorphous silica nanoparticles by macrophage scavenger receptor A. Nanotoxicology 5(3):296–311
Park E-JJ, Yi J, Kim Y, Choi K, Park K (2010) Silver nanoparticles induce cytotoxicity by a Trojan-horse type mechanism. Toxicol InVitro 24(3):872–878
Park J, Lim D-HH, Lim H-JJ, Kwon T, Choi J-SS, Jeong S, Choi I-HH, Cheon J (2011) Size dependent macrophage responses and toxicological effects of Ag nanoparticles. Chem Commun (Camb) 47(15):4382–4384
Pratsinis A, Hervella P, Leroux JC, Pratsinis SE, Sotiriou GA (2013) Toxicity of silver nanoparticles in macrophages. Small 9(15):2576–2584
Salata OV (2004) Applications of nanoparticles in biology and medicine. J Nanobiotechnology 2(1):3
Sasidharan A, Chandran P, Menon D, Raman S, Nair S, Koyakutty M (2011) Rapid dissolution of ZnO nanocrystals in acidic cancer microenvironment leading to preferential apoptosis. Nano 3(9):3657–3669
Shannahan JH, Sowrirajan H (2015) Impact of silver and iron nanoparticle exposure on cholesterol uptake by macrophages. J Nanomater 501:127235
Sharma V, Yngard R, Lin Y (2009) Silver nanoparticles: green synthesis and their antimicrobial activities. Adv Colloid Interf Sci 145(1):83–96
Smita S, Gupta S, Bartonova A, Dusinska M, Gutleb A, Rahman Q (2012) Nanoparticles in the environment: assessment using the causal diagram approach. Environ Health 11(Suppl 1):S13
Twentyman P, Luscombe M (1987) A study of some variables in a tetrazolium dye (MTT) based assay for cell growth and chemosensitivity. Br J Cancer 56(3):279–285
Varner K, Sanford J, El-Badawy A, Feldhake D, Venkatapathy R (2010) State of the science literature review: everything nanosilver and more. US Environmental Protection Agency, Washington, DC, EPA/600/R-10/084
Wang H, Wu L, Reinhard BMM (2012) Scavenger receptor mediated endocytosis of silver nanoparticles into J774A.1 macrophages is heterogeneous. ACS Nano 6(8):7122–7132
Wang X, Ji Z, Chang C, Zhang H, Wang M, Liao Y-P, Lin S, Meng H, Li R, Sun B et al (2014) Use of coated silver nanoparticles to understand the relationship of particle dissolution and bioavailability to cell and lung toxicological potential. Small 10(2):385–398
Zhang T, Wang L, Chen Q, Chen C (2014) Cytotoxic potential of silver nanoparticles. Yonsei Med J 55(2):283–291
Zhang H, Wang X, Wang M, Li L, Chang CH, Ji Z, Xia T, Nel AE (2015) Mammalian cells exhibit a range of sensitivities to silver nanoparticles that are partially explicable by variations in antioxidant defense and Metallothionein expression. Small 11(31):3797–3805
Acknowledgments
This work has been funded by the European Regional Development Fund (FEDER) through the Competitive Factors Thematic Operational Programme (COMPETE) and by National Funds through the Foundation for Science and Technology (FCT), under the projects CICECO—FCOMP-01-0124-FEDER-037271 (Refª. FCT PEst-C/CTM/LA0011/2013) and FCOMP-01-0124-FEDER-021456 (Refª. FCT PTDC/SAU-TOX/120953/2010). The grants awarded by FCT to V.B. (SFRH/BD/81792/2011) and H.O. (SFRH/BPD/111736/2015) are also acknowledged. I.F.D acknowledges FCT/MCTES for a research contract under the Program “Investigador FCT” 2014.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflicting interests
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Bastos, V., Duarte, I.F., Santos, C. et al. A study of the effects of citrate-coated silver nanoparticles on RAW 264.7 cells using a toolbox of cytotoxic endpoints. J Nanopart Res 19, 163 (2017). https://doi.org/10.1007/s11051-017-3855-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11051-017-3855-1