Abstract
Neonatal candidemia can occur, however, infections caused by Candida pelliculosa are rare. Here, we describe an outbreak of candidemia caused by C. pelliculosa among babies hospitalized in a neonatal intensive care unit.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The incidence of neonatal systemic candidiasis is associated with significant morbidity and mortality [1]. Previous epidemiologic outcome studies of neonatal candidemia have reported crude mortality rates of 30–60 % and increased risk associated with low birth weight [2]. Furthermore, in addition to premature birth, common use of broad-spectrum antibiotics and intravenous catheters means that neonates are particularly prone to candidemia [3].
Among Candida species pathogenic to humans, C. albicans has been the species most often associated with neonatal infection. Recent reports, however, have indicated an increasing number of pediatric outbreaks attributable to other Candida species including Candida pelliculosa teleomorph Pichia anomala [4]. Infections caused by this yeast are rare, but has occurred in premature infants and immunocompromised patients [5]. It is frequently found in fruits, tree exudates, soil, and other organic compounds [6].
Candida pelliculosa has been identified as a cause of invasive infections, and fungemia is the most common presentation in some countries [7, 8]. Usually, such patients are treated with amphotericin B or fluconazole with good clinical outcomes. Nonetheless, treatment failures may occur as well as cases of breakthrough fungemia in patients receiving prophylaxis with fluconazole. Antifungal regimens currently used in neonates are associated with increasing fungal resistance, notable toxicity, drug–drug interactions, or a limited spectrum of activity. In this context, to determine a pathogen’s antifungal susceptibility is an important step in effective treatment [9]. Delayed initiation of appropriate antifungal therapy can raise the risk of mortality and morbidity in infants [10].
Here, we describe an outbreak of fungemia among neonates caused by C. pelliculosa, a possible clonal infection origin and the in vitro antifungal susceptibility of the strains.
Patients and Methods
The research was conducted after the approval by the research ethics committee from the Instituto de Medicina Integral Professor Fernando Figueira register CAAE0246.0.099.000-10.
Case 1
A male infant born in February 2010 with gestational age of 37.2 weeks and a weight of 3,460 g, presenting with congenital malformation, neonatal cholestasis, jaundice, and anemia was hospitalized after birth. In April 2010, a positive diagnosis was made for fungemia caused by C. pelicullosa. The patient was initially treated with fluconazole (6 mg/kg) for 10 days and for a further 15 days with amphotericin B (0.5 mg/kg). After treatment, the fungal sepsis had been overcome and the patient was discharged.
Case 2
A premature male twin neonate born in April 2010 with gestational age of 26 weeks and 4 days and weight of 830 g, presented with jaundice and respiratory distress syndrome, stayed in the NICU from April to September 2010. In May 2010, C. pelliculosa was identified in blood culture. The child was treated for 28 days with fluconazole (6 mg/kg) and for a further 21 days with amphotericin B (0.5 mg/kg). Fungal sepsis was overcome, but the baby remained hospitalized until September 2010 due to severe malnutrition been treated with good clinical outcome and was later discharged.
Case 3
A female premature newborn born in June 2010 with gestational age of 34 weeks and weight of 1,390 g was admitted 10 days after birth suffering from congenital heart disease, jaundice, and anemia. In the same month, a blood culture tested positive for C. pelliculosa. The child was treated with fluconazole (6 mg/kg) for 14 days. The infection was overcome and the patient was discharged in August, 2010.
Case 4
A premature female neonate born in June 2010 at a gestational age of 31 weeks and 3 days, weighing 1,690 g, was admitted with jaundice, pneumothorax, respiratory distress syndrome, and meningoencephalitis. In the same month, a positive diagnosis was made for candidemia caused by C. pelliculosa. The infection was treated with fluconazole (6 mg/kg) for 24 days, with a good response, and the child was discharged in July 2010.
Case 5
A premature female neonate born in June 2010 at a gestational age of 29 weeks and with weight of 840 g, low Apgar score, jaundice, meningoencephalitis, and respiratory distress syndrome, was hospitalized after birth. After 23 days, a blood culture tested positive for C. pelliculosa. Subsequently, the child was treated with fluconazole (6 mg/kg) for 20 days with a good outcome.
An overview of the cases and possible risk factors is showed in Table 1.
In all cases, two blood samples were collected in consecutive days, aseptically by arterial puncture scalp using EDTA anticoagulant from patients hospitalized in a Neonatal Intensive Care Unit (NICU) of a Public Brazilian Hospital between April 2010 and September 2010 (diagnostic and cure control cultures). The microbiological analyses were conducted in the Mycology Department from Pernambuco Federal University. They were processed by standard methods (direct examination and isolation in culture) for mycological diagnosis.
The direct examination of the clinical samples was performed without clarifying and with Giemsa staining. At the same time, cultures were prepared using Sabouraud dextrose agar plus chloranphenicol (Difco) incubated at 30 and 37 °C in an aerobic atmosphere for 15 days.
The identification of the etiological agents was done after purification of the cultures through the macroscopic characteristics (edges, texture and color of the front and back of the colonies, pigment production and growth time), microscopic (somatic and reproductive structures), physiological (ascospores formation), biochemical (assimilation carbon compounds and nitrogen fermentation of sources of carbon and acetic acid production) [11] as well as by molecular techniques involving species-specific primers (P. Anom-F 5’-GAG GGT GGT GGC TTA CCT CT-3′ and P. anom-R 5′-AAA ATA CCT CTT CTA AAC CTG AG-3′) [12].
Direct examination revealed numerous oval hyaline and budding yeast cells in all clinical samples. The growth cultures occurred in both temperatures (30 and 37 °C). The yeast cultures were identified according to morphophysiological characteristics as C. pelliculosa and confirmed based on molecular techniques as shown on Fig. 1.
For the similarity evaluation, fingerprinting analyses were performed with ISSR marker using (GTG)5 (5′-GTGGTGGTGGTGGTG-3′) and M13 (5′-AGTCAGCCAAC-3′) single primers. The variable binary similarity matrix was prepared using Jaccard coefficient by the NTSYS (Numerical Taxonomy System of multivariate program) computer program version pc2.1 [13]. Dendrograms were prepared by UPGMA (Unweighted Pair Group Method with Arithmetical average) analysis.
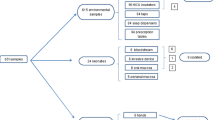
For all molecular assays, an international recommended strain of C. tropicalis ATCC750 was used as an out group. All isolates of C. pelliculosa were placed in the same branch when Primer GTG5 was used. With the primer M13, the strain from case 4 was placed on another branch. The microsatellite band patterns and the dendrograms are showed on Fig. 2.
Microsatelite band patterns and dendrogram generated from the data obtained after PCR amplification of Candida isolates using the primer GTG5 (a, b) and M13 (c, d). 1–5 isolates of Candida pelliculosa from patients hospitalized in the Neonatal Intensive Care Unit from a hospital in Recife-PE correspond to isolates 6345, 6283, 6281, 6280, 6279. Number 6 is the ATCC 750 Candida tropicalis
Antifungal susceptibility testing for amphotericin B (UnitedMedical), fluconazole (Pfizer), voriconazole (Pfizer), and anidulafungin (Pfizer) was performed by the broth microdilution method following the CLSI (Clinical laboratories and standards institute) guidelines found in the document M27-A3 [14]. Quality control was performed by testing CLSI-recommended strains C. tropicalis ATCC750, C. krusei ATCC6258, and C. parapsilosis ATCC22019. The results from the susceptibility test are demonstrated in the Table 2.
The cultured strains have been maintained at the URM Culture Collection of Department of Mycology, Federal University of Pernambuco, Brazil, with records numbers 6345, 6283, 6281, 6280, and 6279.
Discussion
There are several reports of nosocomial cross-infections due to Candida species in NICUs [4]; however, deep-seated infections due to C. pelliculosa are reported rarely [6]. Kalkanci et al. [4] in 2010 reported an outbreak of fungemia by C. pelliculosa in a Turkish hospital among four babies hospitalized in the same room; our report has some similarities as we report an outbreak with five cases of fungemia due C. pelliculosa in neonates from the same NICU. All patients acquired the infection after the admission to the NICU; the non-perinatal nosocomial transmission of C. pelliculosa suggests that the route of transmission may come from the hands of healthcare workers, hospital environment air (dispersed fungal propagules), and invasive procedures as parenteral nutrition. Molecular epidemiologic methods are required for the demonstration of the clonal relationships between the isolates [15]. Genetic analysis of the blood isolates showed that all five were positive for the marker (GTG)5, but only four were positive for the M13 marker which suggests that in our study, four of the five yeasts isolated probably had the same clonal origin.
Four of the five affected babies were premature: one of them with a birth weight of less than 2,500 g and three with very low birth weights of less than 1,500 g. In a study conducted in an Indian NICU, low birth weight was the most common risk factor for candidemia (79.09 %), followed by prematurity (67.27 %) [16]. Another research of potential risk factors for C. pelliculosa infection in neonates conducted by Chakrabarti et al. [7] showed that lower gestational age, very low birth weight, and longer duration of hospital stay were all significantly associated with fungemia.
Although C. pelliculosa is considered an emergent hematogenous yeast pathogen, data about its susceptibility to antifungal drugs are scarce [17]. A previous study C. pelliculosa strains showed good susceptibility to amphotericin B, fluconazole, and voriconazole [9]. The drug susceptibility profiles of the five isolates were similar. All of them were susceptible to amphotericin B, fluconazole, and anidulafungin, but were resistant to voriconazole. Our isolates were sensitive to anidulafungin, which could be a good therapeutic option for invasive candidiasis, although pharmacokinetics studies of this drug are still in progress and/or under development in the neonatal population [18]. In all five cases, amphotericin B and fluconazole were able to promote a healing of our patients who had fungemia caused by C. pelliculosa. The treatment instituted after antifungal susceptibility testing probably contributed for cure.
References
Zaoutis TE, Heydon K, Locali OR, Walsh TJ, Feudtner C. Outcomes attributable to neonatal candidiasis. Clin Infect Dis. 2007;44:1187–93.
Lopes JM, Goulart EM, Starling CE. Pediatric mortality due to nosocomial infection: a critical approach. Braz J Infect Dis. 2007;11:515–9.
Goel N, Ranjan PK, Aggarwal R, Chaudhary U, Sanjeev N. Emergence of nonalbicans Candida in neonatal septicemia and antifungal susceptibility: experience from a tertiary care center. J Lab Physicians. 2009;1:53–5.
Kalkanci A, Dizbay M, Turan O, Fidan I, Yalçin B, Hirfanoglu I, et al. Nosocomial transmission of Candida pelliculosa fungemia in a pediatric intensive care unit and review of the literature. Turk J Pediatr. 2010;52:42–9.
Choi S, Lee T, Kim M, Lee M, Jung J. A case of fungal arthritis caused by Hansenula anomala. Clin Orthop Surg. 2010;2:59–62.
De Hoog GS, Guarro J, Gene J, Figueras MJ. Atlas of clinical fungi. 2nd ed. Holland: CBS; 2000. p. 215–6.
Chakrabarti A, Singh K, Narang A, Batra R, Rao KLN, Ray P, et al. Outbreak of Pichia anomala infection in the pediatric service of a tertiary-care center in Northern India. J Clin Microbiol. 2001;9:1702–6.
Pasqualotto AC, Sukiennik TCT, Severo LC, Amorim ACS, Colombo AL. An outbreak of Pichia anomala fungemia in a Brazilian pediatric intensive care unit. Infect Control Hosp Epidemiol. 2005;26:553–8.
Pfaller MA, Diekema DJ. Twelve years of fluconazole in clinical practice: global trends in species distribution and fluconazole susceptibility of bloodstream isolates of Candida. Clin Microbiol Infect. 2004;10:11–23.
Matta VLR, Melhem MSC, Colombo AL, Moretti ML, Rodero L, Almeida GMD, et al. Susceptibility profile to antifungal drugs of Pichia anomala isolated from patients presenting nosocomial fungemia. Antimicrob Agents Chemother. 2007;51:1573–6.
Barnett JA, Paine RW, Yarrow D. Yeasts: characteristics and identification. Cambridge: Cambridge University Press; 2000.
Mannarelli BM, Kurtzman CP. Rapid identification of Candida albicans and other human pathogenic yeasts by using short oligonucleotides in a PCR. J Clin Microbiol. 1998;36:1634–41.
Rohlf FJ. NTSYS-PC Numerical taxonomy and multivariate analysis system. New York: Applied Biostatistics, lnc., Exeter Publishing; 1988.
Clinical and Laboratory Standards Institute (CLSI). Reference method for broth dilution antifungal susceptibility testing of yeasts; approved standard. 3rd ed. CLSI document M27-A3, Wayne, PA; 2008.
Ergon MC, Yucesoy M. Molecular epidemiology of Candida species isolated from urine at an intensive care unit. Mycoses. 2005;48:126–31.
Sardana V, Pandey A, Madan M, Goel SP, Asthana AK. Neonatal candidemia: a changing trend. Indian J Pathol Microbiol. 2012;55:132–3.
Barchiesi F, Tortorano AM, Tortorano LF, Giacometti A, Spreghini E, et al. Genotypic variation and antifungal susceptibilities of Candida pelliculosa clinical isolates. J Med Microbiol. 2005;54:279–85.
Odio CM, Araya R, Pinto LE, Castro CE, Vasquez S, Alfaro B, et al. Caspofungin therapy of neonates with invasive candidiasis. Pediatr Infect Dis J. 2004;23:1093–7.
Acknowledgments
We are particularly grateful to David Bousfield for critical reading of the manuscript. We thank the National Scientific and Technological Development Council (CNPq) for granting the fellowship and the Federal University of Pernambuco (UFPE) for providing the infrastructure.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
da Silva, C.M., de Carvalho Parahym, A.M.R., Leão, M.P.C. et al. Fungemia by Candida pelliculosa (Pichia anomala) in a Neonatal Intensive Care Unit: A Possible Clonal Origin. Mycopathologia 175, 175–179 (2013). https://doi.org/10.1007/s11046-012-9605-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-012-9605-0