Abstract
Exosomes play a role in the pathogenesis and treatment of malignancies as a double-edged sword. Recently, researchers discussed about two new roles, cardiomyocyte function impairment and cardiovascular disease (CVD) genesis. Data were collected from PUBMED at various time points up to the 2019 academic year. The related key words are listed as following; “Arsenic trioxide”, “acute promyelocytic leukemia” and “cardio toxicity” and “molecular pathway” and “biomarker”. This study has shown that exosomes secreted substances stimulate angiogenesis and cardiomyocytes repairment; cited process depended on the kinds of released substances. Generally, exosomes may involve in the pathogenesis of CVD; although CVD can prevented by identifying the pathways that induce angiogenesis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
According to the reports of World Health Organization (WHO), the rate of mortality related to hematological malignancies is increasing. Despite progression in the diagnostic method and introducing new prognostic factors many of involved patients die, as a result of disease [1]. Occurrence of cardiovascular disease (CVD) as an underlying disease or malignancy induced is much [2]. The researches which are done recently has shown that mammalian cells exosomes, have a role not only in proliferation of malignant cells but also in pathogenesis of CVD [3]. Vesicles are categorized in three size including small, media and large; the small ones are called exosomes, which contain [4] different substances such as, Micro RNAs (miRs), cytokine, chemokines and coagulant factors [5]. Given that, exosomes have both coagulation activity and releasing cytokines and chemokines; they lead to immune system function impairment. We can say that these vesicles simultaneously promote malignancy and CVD. Thus, designing proper therapies, regarding to exosomes content, can prevent CVD and malignant cells proliferation simultaneously [6, 7]. Therefore, we investigated the role of exosomes in the CVD pathogenesis in hematological malignancies.
Structure of exosomes
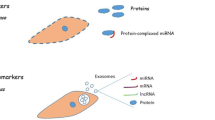
Exosomes are vesicles derived from different cells which are found in body fluids such as amnion fluid, milk, and blood; the diameter is 30–100 nm [8]. These vesicles are cup-shaped and surrounded by a series of proteins and lipids such as sphingomyelin and cholesterol [9]. They contain a variety of proteins, including chaperones, kinase and GTPase, and many CD markers such as CD81 and CD82 [10]. Furthermore, they have a number of miRs that are effective in cellular communication in normal and pathogenic states. Many of exosomes released from cardiomyocytes and other cardiac cells along with endothelial cells exosome, lead to connection between the cardiac components; the linkage will improve cardiac function and ultimately supply energy for body’s metabolic activity [11, 12]. The exosomes have a series of miRs that not only disrupt cell signaling, but also activate thrombosis and inflammation by coagulation factors. These Processes simultaneously lead to disease progression with cardiac origin.
Exosome proteins
Proteins is one of the components displaced by exosomes and are present in the external structure of exosomes. Exosomes surface proteins not only interact with other cells, but also stimulate molecular pathways by binding to receptors at the target cell surface [13, 14]. S100-A9 is one of the serum proteins secreted by Exosomes in hematological malignancies. The S100-A9 receptor is an extracellular matrix metalloproteinase inducer (EMMPRIN) which expresses on the surface of many cells [15]. In addition, S100-A9 interaction with EMMPIRIN lead to activate NF-κB (nuclear factor kappa-light-chain-enhancer of activated B cells) pathway and trigger inflammation [16]. On the opposite side, EMMPRIN expression at the surface of some exosomes and, its interaction with Matrix metalloproteinase (MMPs) can cause cardio myocytes progenitors cells (CPCs) displacement and cardio myocytes repairmen. It also increases angiogenesis through vascular endothelial growth factor (VEGF) secretion [17, 18]. Thus in hematological malignancies, CVD occurrence and progression are preventable by expressing EMMPIRIN on heart cells but not malignant cells. This finding needs to identify signaling pathways that activate EMMPRIN in cardiac tissue and prevent angiogenesis in the malignant cells. Also, when inflammatory responses are triggered by NF-κB pathway activation and the inflammatory mediators production increased, Tumor growth factor-β (TGF-β) production is increased too; these events prevent overproduction of mediators as well as damage healthy tissues [19]. During a malignancy procedure, malignant cells secrete vesicles containing TGF-β, after inflammation; they grow and proliferate by suppressing immune cells [20]. Also exosomes contain TGF-β ccccsis of cardiomyocytes and cardiomyopathy in CVD [21]. Furthermore, researches have shown that exosomes contain TGF-β are accompanied with increased expression of high-mobility group box 1 (HMGB-1); HMGB-1 enhances TGF-β production by activating NF-κB pathway [22]. Therefore, targeting HMGB-1 in malignant cells reduces the secretion of exosomes containing TGF-β. TGF-β inhibits the proliferation of malignant cells and cardiomyocytes fibrosis. Another study, emphasize on the cardio protection role of HMGB-1, the results of these studies show that HSP70 expresses on exosomes; Interaction of HSP70 with Toll-like receptor 4 (TLR4) activates the ERK/MAPK pathway which cause cardio protection by preventing apoptosis [22, 23]. HMGB-1 enhances TLR4 expression by activating the NF-κB pathway. In addition, it activates the PI3k/AKT/mTOR pathway in malignant cells. It induces the malignant cells resistance to chemotherapy; activating the PI3k/AKT/mTOR pathway by HMGB-1, promotes proliferation and growth of cardiomyocytes, in CVD condition (Fig. 1) [24, 25].
Multiple functions of exosomes associated with CVD in hematologic malignancies, with regard to their proteins, miRNAs, immunomodulators, and enzymes. According to the signaling aspect, interactions between exosome proteins, as well as secretory cytokines (such as TGF-β), induce diverse effects on cardiac tissue, angiogenesis, and malignant cell proliferation. Alongside these effects, miRNAs as a double-edged sword, are capable of stimulating leukemic cell proliferation (or even CVD development) and some of them inhibit leukemic cell proliferation by increasing their susceptibility to chemotherapy drugs. Similar to the consequences of miRNAs function, exosomal immunomodulators, despite causing leukemic cell resistance against host immune responses, are considered an appropriate strategy for repair damaged heart cells and CVD prevention. Exosomal enzymes generally affect inflammatory and apoptosis processes, which can be involved in the pathogenesis of CVD through their powerful weapons (such as ROS and NOX2). Accurate identification of each of these aspects can be useful indesigning therapeutic strategies to reduce the progression of CVD in hematologic malignancies. CVD cardiovascular disease, MIR microrna, PB peripheral blood, BM bone marrow, MI myocardial infarction, PI3K/AKT phosphoinositide 3-kinases, FOXO1 forkhead box protein O1, MCL-1 myeloid cell leukemia-1, PTEN phosphatase and tensin homologue, Bcl-2 B-cell lymphoma 2, NOX2 NADPH oxidase 2, ROS reactive oxygen species, NRF2 nuclear factor erythroid 2-related factor 2, CYTO C cytochrome c, MST1 mammalian sterile 20-like kinase 1, YAP yes-associated protein, GLUT4 glucose transporter 4, Glc glucose, CD cluster of differentiation, PRO protein, CHOL cholesterol, GTP guanosine-5′-triphosphate, MMP matrix metalloproteinase, CPC myocytes progenitors cells, NF-Κb nuclear factor kappa-light-chain-enhancer of activated B cells, HSP70 heat shock protein 70, HMGB-1 high-mobility group box 1, TGF-β tumor growth factor-β, VEGF vascular endothelial growth factor, TLR4 toll-like receptor 4, ERK extracellular-signal-regulated kinase, MAPK mitogen activated protein kinase, MTOR mammalian target of rapamycin, MDSC myeloid-derived suppressor cells, TGF-β1 transforming growth factor beta 1, NCAM1 neural adhesion molecule 1, SPHK1 sphingosine kinase 1, TIMP-1 TIMP metallopeptidase inhibitor 1, IL-1 interleukin-1, TREG T regulatory cell
Finally, we can say that HMGB-1 is a key factor at the center of signaling pathways; it has a dual role in hematologic malignancies in malignant cell proliferation and CVD. Identifying pathways that jointly Prevents cell proliferation and cardiomyocytes dysfunction could be a suitable therapeutic design for hematological malignancy patients with CVD.
Exosome microRNA
Exosomes also excrete microRNAs (miRNAs). These miRNAs involved in various processes, including cell-to-cell and cell-to-extracellular communication, as well as the association between heart and stem cells [26, 27]. MiRNAs are short noncoding RNAs which are effective in the regulation of expression as well as the translation of many mRNAs in the cell [28]. Recent studies imply that exosomes secreted miRNAs of leukemia patients, are effective in in promoting malignant cell proliferation and development of CVD. On the contrary, recent studies have reported that induction of some miRNAs by exosomes in patients, causes cardiac repair and regeneration, it prevents CVD too. For instance, miR-26a prevents cardiac cell fibrosis by reducing FoxO1 and TRIM63/MuRF1 expression. In addition, evidences suggest that miR-26a expression is decreased, in chronic lymphocytic leukemia (CLL) patients. MCL-1 inhibition induces miR-26a expression which promotes apoptosis process of leukemic cell [29,30,31]. On the other hand, miR-486-5p inhibits leukemia cell proliferation by targeting FoxO1 and increasing their susceptibility to chemotherapy drugs [32]. On the contrary, miR-486-5p by targeting PTEN and enhancing PI3K/AKT pathway induces BCL-2 expression and prevents cardiomyocyte apoptosis, in the ischemia patients [33]. MiR-134 is another miRs that increases in the serum of myocardial infarction patients; it has been introduced as a biomarker in patients with myocardial infarction [34]. MiR-134 increases blast in peripheral blood and bone marrow by preventing stem cell differentiation; its expression is associated with poor prognosis in leukemic patients [35]. MiR-132 expression is decreased in CVD patients and results in cardiomyocyte atrophy; induction of miR-132 expression leads to increased angiogenesis and prevents myocardial infraction. It is not protective on leukemic cells and leads to increased proliferation of malignant cells [36, 37]. Finally, each miRs, can both promote the proliferation of cancer cells and impair cardiomyocyte function, depending on the biological function. Some are known for the protective effect for cardiomyocytes and induces leukemic cell resistance to chemotherapy (Fig. 1) [38, 39]. Therefore, screening and detection of miRs as a prognostic marker can be used in the plasma of leukemia patients; they can predict therapy resistance and CVD incidence in the patients (Table 1).
Exosome immunosuppression mediators
Secretion of exosomes that contain immunosuppressive factors is one of the mechanisms which causes leukemia cells resistance to host immune responses; these factors provide the conditions for proliferation and development of leukemic cells, by modulating the immune system [52, 53]. For instance, studies show that increased myeloid-derived suppressor cells (MDSCs) inhibit the production of inflammatory cytokines such as IL-1 and IL-6; this mechanism prevents cardiomyocyte hypertrophy and CVD by preventing T-cell from functioning [54]. MDSCs modulate the immune system from pro-inflammatory to anti-inflammatory state by inducing T regulatory cells (Treg) differentiation and blocking access of T-cells to L-arginine [55]. TGF-β1 is another secreted immunosuppressive agent by exosomes in leukemic patients. Studies have shown that TGF-β1 secretion unlike MDSC does not induce cardiomyocyte repairing; it increases the expression of both sphingosine kinase 1 (SPHK1) and TIMP metallopeptidase inhibitor 1 (TIMP-1). These two factors cause angiogenesis and regulate metabolism, normally, but increasing expression by TGF-β1 leads to cardiomyocyte apoptosis and CVD [56]. It has been proven that, TGF-β1 leads to increased expression of neural adhesion molecule 1 (NCAM1) in CVD patients; NCAM1 expression leads to impaired cardiomyocyte adhesion and impaired cardiac function, consequently (Fig. 1) [57].
It can be concluded that some factors are protective for cardiomyocytes, although they increase leukemia cells survival and proliferation. Therefore, identifying these pathways can be a way to design a suitable treatment strategy to prevent CVD development.
Exosome enzyme
Enzymes are other factors released from exosomes secreted by leukemic cells. These factors play an important role in inflammation and apoptosis and the pathogenesis of CVD through the reactive oxygen species (ROS) production. Caspase-3 is one of the enzymes released by exosomes, which induces cardiomyocytes apoptosis by releasing cytochrome C from mitochondria [58, 59]. Mammalian sterile 20-like kinase 1 (Mst1) is a component of the Hippo signaling pathway which has a role in cell apoptosis and autophagy to regulate. Results have shown that Mst1 induces cardiomyocytes apoptosis by activating caspase-3 and inhibition of the yes-associated protein (YAP) (involved in cell cycle progression). In addition, Mst1 inhibits glucose uptake and insulin resistance by impairing Glucose transporter 4 (GLUT4) function, which results in cardiomyocyte hypertrophy and CVD, ultimately [60,61,62]. NADPH oxidase 2 (NOX2) is another effective enzyme in the CVD development due to ROS production. This enzyme induces cardiomyocyte apoptosis by increasing ROS production. Nuclear factor erythroid 2-related factor 2 (Nrf2) is one of the antioxidant factors that inhibits ROS production due to NOX2 dysfunction. Furthermore, given that Mst1 has been shown to decrease Nrf2 expression, it can be said that increased Mst1 expression by increasing ROS production lead to CVD [63, 64]. Another prominent role of Nox2 is apoptosis prevention. Nox2 inhibits apoptosis by targeting PTEN and enhancing BCL-2 expression through activating PI3K/AKT pathway [65]. According to the dual role of NOX2 in cardiomyocyte apoptosis induction and suppression, it can be said that accurate identification of signaling pathways which activated or inactivated by NOX2 could be suitable for designing a therapeutic strategy.
Conclusion
Some researchers believed that exosomes secreted substances are able to impair cardiomyocyte function and cause CVD; the events occur by stimulating the immune system as well as producing ROS. Contradictory results from other studies revealed that CVD can be prevented by angiogenesis and stimulation of cardiomyocyte precursor’s differentiation; some studies have cited that secreted miRs and lncRNAs are responsible for these events. Therefore, the reconnaissance of angiogenesis pathways can be used as an appropriate therapeutic strategy for the treatment of CVD in hematologic malignancies.
References
Ho G, Jonas BA, Li Q, Brunson A, Wun T, Keegan TH (2017) Early mortality and complications in hospitalized adult Californians with acute myeloid leukaemia. Br J Haematol 177(5):791–799
Park JY, Guo W, Al-Hijji M, El Sabbagh A, Begna KH, Habermann TM et al (2019) Acute coronary syndromes in patients with active hematologic malignancies—incidence, management, and outcomes. Int J Cardiol 275:6–12
Boyiadzis M, Whiteside T (2017) The emerging roles of tumor-derived exosomes in hematological malignancies. Leukemia 31(6):1259–1268
Kowal J, Arras G, Colombo M, Jouve M, Morath JP, Primdal-Bengtson B et al (2016) Proteomic comparison defines novel markers to characterize heterogeneous populations of extracellular vesicle subtypes. Proc Natl Acad Sci USA 113(8):E968–E977
Vlassov AV, Magdaleno S, Setterquist R, Conrad R (2012) Exosomes: current knowledge of their composition, biological functions, and diagnostic and therapeutic potentials. Biochim Biophys Acta 1820(7):940–948
Qiao L, Hu S, Liu S, Zhang H, Ma H, Huang K et al (2019) microRNA-21-5p dysregulation in exosomes derived from heart failure patients impairs regenerative potential. J Clin Investig. https://doi.org/10.1172/JCI123135
Yue Y, Wang C, Benedict C, Huang G, Truongcao M, Roy R et al (2020) Interleukin-10 deficiency alters endothelial progenitor cell-derived exosome reparative effect on myocardial repair via integrin-linked kinase enrichment. Circ Res 126(3):315–329
Crenshaw BJ, Gu L, Sims B, Matthews QL (2018) Exosome biogenesis and biological function in response to viral infections. Open Virol J 12:134
Théry C, Regnault A, Garin J, Wolfers J, Zitvogel L, Ricciardi-Castagnoli P et al (1999) Molecular characterization of dendritic cell-derived exosomes: selective accumulation of the heat shock protein hsc73. J Cell Biol 147(3):599–610
Mathivanan S, Simpson RJ (2009) ExoCarta: a compendium of exosomal proteins and RNA. Proteomics 9(21):4997–5000
Hergenreider E, Heydt S, Tréguer K, Boettger T, Horrevoets AJ, Zeiher AM et al (2012) Atheroprotective communication between endothelial cells and smooth muscle cells through miRNAs. Nat Cell Biol 14(3):249–256
Zamani P, Fereydouni N, Butler AE, Navashenaq JG, Sahebkar A (2019) The therapeutic and diagnostic role of exosomes in cardiovascular diseases. Trends Cardiovasc Med 29(6):313–323
Choi DS, Kim DK, Kim YK, Gho YS (2013) Proteomics, transcriptomics and lipidomics of exosomes and ectosomes. Proteomics 13(10–11):1554–1571
Hibino T, Sakaguchi M, Miyamoto S, Yamamoto M, Motoyama A, Hosoi J et al (2013) S100A9 is a novel ligand of EMMPRIN that promotes melanoma metastasis. Cancer Res 73(1):172–183
Prieto D, Sotelo N, Seija N, Sernbo S, Abreu C, Durán R et al (2017) S100-A9 protein in exosomes from chronic lymphocytic leukemia cells promotes NF-κB activity during disease progression. Blood 130(6):777–788
Vrijsen K, Sluijter J, Schuchardt M, Van Balkom B, Noort W, Chamuleau S et al (2010) Cardiomyocyte progenitor cell-derived exosomes stimulate migration of endothelial cells. J Cell Mol Med 14(5):1064–1070
Wang Q, Zhou X, Zhao Y, Xiao J, Lu Y, Shi Q et al (2018) Polyphyllin I ameliorates collagen-induced arthritis by suppressing the inflammation response in macrophages through the NF-κB pathway. Front Immunol 9:2091
Ren X-S, Tong Y, Qiu Y, Ye C, Wu N, Xiong X-Q et al (2020) MiR155-5p in adventitial fibroblasts-derived extracellular vesicles inhibits vascular smooth muscle cell proliferation via suppressing angiotensin-converting enzyme expression. J Extracell Vesicles 9(1):1698795
Huang F, Wan J, Hu W, Hao S (2017) Enhancement of anti-leukemia immunity by leukemia-derived exosomes via downregulation of TGF-β1 expression. Cell Physiol Biochem 44(1):240–254
Ke X, Yang D, Liang J, Wang X, Wu S, Wang X et al (2017) Human endothelial progenitor cell-derived exosomes increase proliferation and angiogenesis in cardiac fibroblasts by promoting the mesenchymal–endothelial transition and reducing high mobility group box 1 protein B1 expression. DNA Cell Biol 36(11):1018–1028
Shi Y, Zhang L, Teng J, Miao W (2018) HMGB1 mediates microglia activation via the TLR4/NF-κB pathway in coriaria lactone induced epilepsy. Mol Med Rep 17(4):5125–5131
Davidson SM, Riquelme JA, Zheng Y, Vicencio JM, Lavandero S, Yellon DM (2018) Endothelial cells release cardioprotective exosomes that may contribute to ischaemic preconditioning. Sci Rep 8(1):1–9
Vicencio JM, Yellon DM, Sivaraman V, Das D, Boi-Doku C, Arjun S et al (2015) Plasma exosomes protect the myocardium from ischemia-reperfusion injury. J Am Coll Cardiol 65(15):1525–1536
Li S, Jiang J, Yang Z, Li Z, Ma X, Li X (2018) Cardiac progenitor cell-derived exosomes promote H9C2 cell growth via Akt/mTOR activation. Int J Mol Med 42(3):1517–1525
Chen Y, Zhou X, Qiao J, Bao A (2017) MiR-142-3p overexpression increases chemo-sensitivity of NSCLC by inhibiting HMGB1-mediated autophagy. Cell Physiol Biochem 41(4):1370–1382
Shantikumar S, Angelini GD, Emanueli C (2014) Diabetes, microRNAs and exosomes: les liaisons dangereuses. J Mol Cell Cardiol 74:196–198
Bang C, Batkai S, Dangwal S, Gupta SK, Foinquinos A, Holzmann A et al (2014) Cardiac fibroblast-derived microRNA passenger strand-enriched exosomes mediate cardiomyocyte hypertrophy. J Clin Investig 124(5):2136–2146
Cheng M, Zhao X, Wu B, Mao X, Yi G, Zeng Q et al (2014) Circulating exosomal miR-1a is markedly induced by myocardial infarction and downregulates CXCR4 expression in the bone marrow mononuclear cells. Circulation 130(Suppl_2):A18383
Wang B, Zhang A, Wang H, Klein JD, Tan L, Wang Z-M et al (2019) miR-26a limits muscle wasting and cardiac fibrosis through exosome-mediated microRNA transfer in chronic kidney disease. Theranostics 9(7):1864
Gao J, Li L, Wu M, Liu M, Xie X, Guo J et al (2013) MiR-26a inhibits proliferation and migration of breast cancer through repression of MCL-1. PLoS ONE 8(6):e65138
Wang L, Jia Q, Xinnong C, Xie Y, Yang Y, Zhang A et al (2019) Role of cardiac progenitor cell-derived exosome-mediated microRNA-210 in cardiovascular disease. J Cell Mol Med 23(11):7124–7131
Liu H, Ni Z, Shi L, Ma L, Zhao J (2019) MiR-486-5p inhibits the proliferation of leukemia cells and induces apoptosis through targeting FOXO1. Mol Cell Probes 44:37–43
Sun X-H, Wang X, Zhang Y, Hui J (2019) Exosomes of bone-marrow stromal cells inhibit cardiomyocyte apoptosis under ischemic and hypoxic conditions via miR-486-5p targeting the PTEN/PI3K/AKT signaling pathway. Thromb Res 177:23–32
Zhou J, Chen L, Chen B, Huang S, Zeng C, Wu H et al (2018) Increased serum exosomal miR-134 expression in the acute ischemic stroke patients. BMC Neurol 18(1):1–9
Lin X, Rice K, Buzzai M, Hexner E, Costa F, Kilpivaara O et al (2013) miR-433 is aberrantly expressed in myeloproliferative neoplasms and suppresses hematopoietic cell growth and differentiation. Leukemia 27(2):344–352
Tavolaro S, Colombo T, Chiaretti S, Peragine N, Fulci V, Ricciardi MR et al (2015) Increased chronic lymphocytic leukemia proliferation upon IgM stimulation is sustained by the upregulation of miR-132 and miR-212. Genes Chromosom Cancer 54(4):222–234
Ma T, Chen Y, Chen Y, Meng Q, Sun J, Shao L et al (2018) MicroRNA-132, delivered by mesenchymal stem cell-derived exosomes, promote angiogenesis in myocardial infarction. Stem Cells Int. https://doi.org/10.1155/2018/3290372
Hou Z, Qin X, Hu Y, Zhang X, Li G, Wu J et al (2019) Longterm exercise-derived exosomal miR-342-5p: a novel exerkine for cardioprotection. Circ Res 124(9):1386–1400
Gollmann-Tepeköylü C, Pölzl L, Graber M, Hirsch J, Nägele F, Lobenwein D et al (2019) miR-19a-3p containing exosomes improve function of ischaemic myocardium upon shock wave therapy. Cardiovasc Res. https://doi.org/10.1093/cvr/cvz209
Zhu L-P, Tian T, Wang J-Y, He J-N, Chen T, Pan M et al (2018) Hypoxia-elicited mesenchymal stem cell-derived exosomes facilitates cardiac repair through miR-125b-mediated prevention of cell death in myocardial infarction. Theranostics 8(22):6163
Jiang L, Deng T, Wang D, Xiao Y (2018) Elevated serum exosomal miR-125b level as a potential marker for poor prognosis in intermediate-risk acute myeloid leukemia. Acta Haematol 140(3):183–192
Sun H, Zhong D, Jin J, Liu Q, Wang H, Li G (2018) Upregulation of miR-215 exerts neuroprotection effects against ischemic injury via negative regulation of Act1/IL-17RA signaling. Neurosci Lett 662:233–241
Ohyashiki K, Umezu T, Katagiri S, Kobayashi C, Azuma K, Tauchi T et al (2016) Downregulation of plasma miR-215 in chronic myeloid leukemia patients with successful discontinuation of imatinib. Int J Mol Sci 17(4):570
Al-Hayali MA, Sozer V, Durmus S, Erdenen F, Altunoglu E, Gelisgen R et al (2019) Clinical value of circulating microribonucleic acids miR-1 and miR-21 in evaluating the diagnosis of acute heart failure in asymptomatic type 2 diabetic patients. Biomolecules 9(5):193
Taverna S, Fontana S, Monteleone F, Pucci M, Saieva L, De Caro V et al (2016) Curcumin modulates chronic myelogenous leukemia exosomes composition and affects angiogenic phenotype via exosomal miR-21. Oncotarget 7(21):30420
Li H, Zhang P, Li F, Yuan G, Wang X, Zhang A et al (2019) Plasma miR-22-5p, miR-132-5p, and miR-150-3p are associated with acute myocardial infarction. BioMed Res Int 2019:1–13
Xu D-D, Zhou P-J, Wang Y, Zhang Y, Zhang R, Zhang L et al (2016) miR-150 suppresses the proliferation and tumorigenicity of leukemia stem cells by targeting the nanog signaling pathway. Front Pharmacol. https://doi.org/10.3389/fphar.2016.00439
Khanaghaei M, Tourkianvalashani F, Hekmatimoghaddam S, Ghasemi N, Rahaie M, Khorramshahi V et al (2016) Circulating miR-126 and miR-499 reflect progression of cardiovascular disease; correlations with uric acid and ejection fraction. Heart Int 11(1):e1–e9
Taverna S, Amodeo V, Saieva L, Russo A, Giallombardo M, De Leo G et al (2014) Exosomal shuttling of miR-126 in endothelial cells modulates adhesive and migratory abilities of chronic myelogenous leukemia cells. Mol Cancer 13(1):169
Sassi Y, Avramopoulos P, Ramanujam D, Grüter L, Werfel S, Giosele S et al (2017) Cardiac myocyte miR-29 promotes pathological remodeling of the heart by activating Wnt signaling. Nat Commun 8(1):1614
Butrym A, Rybka J, Baczyńska D, Poręba R, Kuliczkowski K, Mazur G (2016) Clinical response to azacitidine therapy depends on microRNA-29c (miR-29c) expression in older acute myeloid leukemia (AML) patients. Oncotarget 7(21):30250
Hong C-S, Sharma P, Yerneni SS, Simms P, Jackson EK, Whiteside TL et al (2017) Circulating exosomes carrying an immunosuppressive cargo interfere with cellular immunotherapy in acute myeloid leukemia. Sci Rep 7(1):1–10
Liu S, Chen J, Shi J, Zhou W, Wang L, Fang W et al (2020) M1-like macrophage-derived exosomes suppress angiogenesis and exacerbate cardiac dysfunction in a myocardial infarction microenvironment. Basic Res Cardiol 115(2):1–17
Wang Y-G, Xiong X, Chen Z-Y, Liu K-l, Yang J-H, Wen Q et al (2015) Expansion of myeloid-derived suppressor cells in patients with acute coronary syndrome. Cell Physiol Biochem 35(1):292–304
Zhang Y, Zhang M, Li X, Tang Z, He L, Lv K (2017) Expansion of CD11b+ Ly-6C+ myeloid-derived suppressor cells (MDSCs) driven by galectin-9 attenuates CVB3-induced myocarditis. Mol Immunol 83:62–71
Wang S, Zhang Q, Wang Y, You B, Meng Q, Zhang S et al (2018) Transforming growth factor β1 (TGF-β1) appears to promote coronary artery disease by upregulating sphingosine kinase 1 (SPHK1) and further upregulating its downstream TIMP-1. Med Sci Monit 24:7322
Ackermann MA, Petrosino JM, Manring HR, Wright P, Shettigar V, Kilic A et al (2017) TGF-β1 affects cell-cell adhesion in the heart in an NCAM1-dependent mechanism. J Mol Cell Cardiol 112:49–57
Vardaki I, Sanchez C, Fonseca P, Olsson M, Chioureas D, Rassidakis G et al (2016) Caspase-3-dependent cleavage of Bcl-xL in the stroma exosomes is required for their uptake by hematological malignant cells. Blood 128(23):2655–2665
Li H, Liao Y, Gao L, Zhuang T, Huang Z, Zhu H et al (2018) Coronary serum exosomes derived from patients with myocardial ischemia regulate angiogenesis through the miR-939-mediated nitric oxide signaling pathway. Theranostics 8(8):2079
Ikeda S, Mizushima W, Sciarretta S, Abdellatif M, Zhai P, Mukai R et al (2019) Hippo deficiency leads to cardiac dysfunction accompanied by cardiomyocyte dedifferentiation during pressure overload. Circ Res 124(2):292–305
Hu J, Wang S, Xiong Z, Cheng Z, Yang Z, Lin J et al (1864) (2018), Exosomal Mst1 transfer from cardiac microvascular endothelial cells to cardiomyocytes deteriorates diabetic cardiomyopathy. Biochim Biophys Acta 1864(11):3639–3649
Yamamoto S, Yang G, Zablocki D, Liu J, Hong C, Kim S-J et al (2003) Activation of Mst1 causes dilated cardiomyopathy by stimulating apoptosis without compensatory ventricular myocyte hypertrophy. J Clin Investig 111(10):1463–1474
Song H, Wang M, Xin T (2019) Mst1 contributes to nasal epithelium inflammation via augmenting oxidative stress and mitochondrial dysfunction in a manner dependent on Nrf2 inhibition. J Cell Physiol 234(12):23774–23784
Ren Y, Chen X, Li P, Zhang H, Su C, Zeng Z et al (2019) Si-Miao-Yong-An decoction ameliorates cardiac function through restoring the equilibrium of SOD and NOX2 in heart failure mice. Pharmacol Res 146:104318
Hervera A, De Virgiliis F, Palmisano I, Zhou L, Tantardini E, Kong G et al (2018) Reactive oxygen species regulate axonal regeneration through the release of exosomal NADPH oxidase 2 complexes into injured axons. Nat Cell Biol 20(3):307–319
Acknowledgements
We wish to thank all our colleagues in Golestan Hospital and Allied Health Sciences School, Ahvaz Jundishapur University of Medical Sciences.
Author information
Authors and Affiliations
Contributions
HR has conceived the manuscript and revised it. FJZ and SB wrote the manuscript. MM and ND design table and figure. YGH did revise and edited grammar.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zadeh, F.J., Ghasemi, Y., Bagheri, S. et al. Do exosomes play role in cardiovascular disease development in hematological malignancy?. Mol Biol Rep 47, 5487–5493 (2020). https://doi.org/10.1007/s11033-020-05453-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-020-05453-z