Abstract
We investigated the effects of AT-101/cisplatin combination treatment on the expression levels of apoptotic proteins and epigenetic events such as DNA methyltransferase (DNMT) and histone deacetylase (HDAC) enzyme activities in OVCAR-3 and MDAH-2774 ovarian cancer cells. XTT cell viability assay was used to evaluate cytotoxicity. For showing apoptosis, both DNA Fragmentation and caspase 3/7 activity measurements were performed. The expression levels of apoptotic proteins were assessed by human apoptosis antibody array. DNMT and HDAC activities were evaluated by ELISA assay and mRNA levels of DNMT1 and HDAC1 genes were quantified by qRT-PCR. Combination of AT-101/cisplatin resulted in strong synergistic cytotoxicity and apoptosis in human ovarian cancer cells. Combination treatment reduced some pivotal anti-apoptotic proteins such as Bcl-2, HIF-1A, cIAP-1, XIAP in OVCAR-3 cells, whereas p21, Bcl-2, cIAP-1, HSP27, Clusterin and XIAP in MDAH-2774 cells. Among the pro-apoptotic proteins, Bad, Bax, Fas, phospho-p53 (S46), Cleaved caspase-3, SMAC/Diablo, TNFR1 and Cytochrome c were induced in OVCAR-3 cells, whereas, Bax, TRAILR2, FADD, p27, phospho-p53 (S46), Cleaved caspase-3, Cytochrome c, SMAC/Diablo and TNFR1 were induced in MDAH-2774 cells. Combination treatment also inhibited both DNMT and HDAC activities and also mRNA levels in both ovarian cancer cells. AT-101 exhibits great potential in sensitization of human ovarian cancer cells to cisplatin treatment in vitro, suggesting that the combination of AT-101 with cisplatin may hold great promise for development as a novel chemotherapeutic approach to overcome platinum-resistance in human ovarian cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The gold standard of care for advanced ovarian cancer is currently a combination of platinum and taxane. However, the disease almost invariably progresses to a platinum-resistant state, and unfortunately, second or third line chemotherapy regimens do not provide sufficient results [1–3]. Thus, for platinum-resistant ovarian cancer patients, new agents or their combinations with current chemotherapeutic agents with different cellular targets are urgently needed.
Failure of drug-induced apoptosis have been suggested to underlie the phenomenon of drug resistance in cancer treatment, in addition to alterations in DNA repair, drug uptake, cell cycle related genes and also epigenetic events [4–6]. Thus, in recent years, therapies triggering apoptosis in drug resistant cancer cells are currently undergoing clinical trials to overcome drug resistance phenomenon [7].
Cisplatin causes the formation of DNA adducts, consequentially triggering apoptosis in cancer cells. However, toxicity to normal cells and development of drug resistance are the significant problems during cisplatin treatment [8]. The addition of new agents that can sensitize tumor cells to cisplatin with minimal toxicity to normal cells might suggest an important strategy to overcome platinum-resistance in ovarian cancer treatment.
Chemoresistance of ovarian cancer has been previously attributed to the expression and activation of Bcl-2 family proteins. BH3-mimetic molecules possessing potential anticancer activity are able to inhibit anti-apoptotic Bcl-2 family proteins. AT-101, the (−)- enantiomer of gossypol, a natural BH3-mimetic molecule, has been identified as a small molecule inhibitor of anti-apoptotic Bcl-2 family proteins. It has been shown that it induces apoptosis in a wide range of tumor cell lines and enhances chemotherapy- and radiation-induced cytotoxicity [9]. AT-101 has shown anti-tumor activity as a single agent and in combination with standard anticancer therapies in a variety of tumor models [10, 11].
Moreover, it is also suggested that aberrant epigenetic mechanisms may also play a crucial role in drug resistance by interfering with tumor growth regulatory pathways and pro-apoptotic programs in different types of cancer [12]. It is reported that a large number of genes involved in drug resistance are either silenced or activated by aberrant modulation of DNA methyltransferases (DNMTs) and histone acetylase/deacetylases (HDACs) in cancer cells [13]. Unlike genetic mutations, epigenetic alterations are reversible and, therefore, drugs targeting the activities of the executing enzymes like DNMTs and HDACs are attractive drug targets for novel therapies.
Based on these data, in the present study, we investigated the possible synergistic/additive cytotoxic effects of AT-101 in combination with cisplatin in human ovarian cancer cells, OVCAR-3 and MDAH-2774. OVCAR-3 is a highly metastatic, cisplatin resistant human ovarian carcinoma cell line, and thus it is an ideal model to study the effects and mechanisms of various anticancer agents [14]. MDAH-2774 represents an example of slow-growing tumor type and was chosen a reciprocal experimental effect when used with OVCAR-3. To obtain insights into its mechanism of action, we examined the effects of AT-101/cisplatin combination treatment on the expression levels of several apoptotic proteins by protein array method. In addition, we investigated whether this combination has any effect on the epigenetic events in ovarian cancer cells, such as DNMT and HDAC enzyme activities by ELISA and qRT-PCR assays.
Materials and methods
Cell lines and reagents
Human OVCAR-3 and MDAH-2774 ovarian cancer cells were obtained from ICLC (Genova, Italy). The cells were grown as monolayers in adherent cell lines and were routinely cultured in RPMI 1640 supplemented with 10 % heat-inactivated fetal bovine serum (FBS), 1 % l-glutamine, 1 % penicillin–streptomycin in 75 cm2 polystyrene flasks (Corning Life Sciences, UK) and maintained at 37 °C in a humidified atmosphere with 5 % CO2. AT-101 was a generous gift from Ascenta Therapeutics (Malvern, PA, USA). Cisplatin was obtained from Sigma Chemical Co (St. Louis, MO, USA). The stock solutions of AT-101 (10 mM) and cisplatin (10 mM) were prepared in DMSO and stored at −20 °C. The final dilutions were made immediately before use, and new stock solutions were made for each experiment. The DMSO concentration in the assay did not exceed 0.1 % and was not cytotoxic to the tumor cells. All other chemicals, unless mentioned, were purchased from Sigma.
XTT viability assay
After verifying cell viability using trypan blue dye exclusion test by Cellometer automatic cell counter (Nexcelom Inc., Lawrence, MA, USA), cells were seeded at ~1 × 104 cells/well in a final volume of 200 μl in 96-well flat-bottom microtiter plates with or without various concentrations of the drugs. 100 μl of XTT (2,3-bis (2-methoxy-4-nitro-5-sulfophenyl)-5-[(phenylamino)carbonyl]-2H-tetrazolium hydroxide) (Roche Applied Science, Mannheim, Germany) was added to each well, and cytotoxicity was evaluated as described in our previous study [15].
The live/dead viability/cytotoxicity assay
After incubating OVCAR-3 cells with AT-101/cisplatin combination for 72 h, cells were treated with the live/dead viability/cytotoxicity assay kit (Invitrogen, Carlsbad, CA) according to the instruction’s manual. The labeled cells viewed under the fluorescence microscope (Leica Microsystems, Germany).
Evaluation of apoptosis by DNA fragmentation and caspase 3/7 enzyme activity assay
Apoptosis was evaluated by enzyme-linked immunosorbent assay (ELISA) using Cell Death Detection ELISA Plus Kit (Roche Applied Science, Mannheim, Germany) according to the instruction’s manual. The relative amounts of mono- and oligonucleosomes generated from the apoptotic cells were quantified using monoclonal antibodies directed against DNA and histones by ELISA. Absorbance was measured at 405 nm with a reference wavelength at 490 nm (DTX 880 Multimode Reader, Beckman Coulter, FL, USA). Detection of apoptosis was verified by measuring caspase 3/7 enzyme activity as described in our previous study [15].
Examining the expression levels of apoptotic proteins by protein antibody array
To determine the effects of combined treatment with AT-101 and cisplatin on the expression levels of apoptosis related proteins in ovarian cancer cells, a R&D Human Apoptosis Array Kit (R&D Systems, Abingdon, OX, UK) was used according to the instruction’s manual. The principle of the method comprised a nitrocellulose membrane that was coated with specific antibodies for each protein, forming an array. After blocking the membrane, the sample was added and incubated at room temperature. Protein detection was completed by incubation with a biotinylated antibody followed by horseradish peroxidase-conjugated streptavidin. The signals were detected using chemiluminescence in the Kodak® Gel Logic 1500 imaging system (Carestream Molecular Imaging, Newhaven, CT, USA).
DNA Methyltransferase and histone deacetylase activity assays
Total DNMT and HDAC activities were measured using EpiQuik DNA Methyltransferase Activity/Inhibition Assay and EpiQuik HDAC Activity/Inhibition Assay kits, respectively (Epigentek, Brooklyn, NY, USA). Nuclear extracts were isolated using the EpiQuik Nuclear Extraction Kit (Epigentek, Brooklyn, NY, USA) and 3 μl of nuclear extract was added to each reaction well, according to the manufacturer’s protocol. Absorbance was determined using a microplate spectrophotometer at 450 nm (DTX 880 Multimode Reader, Beckman Coulter, FL, USA).
Real time quantitative PCR (qRT-PCR) assay
To validate our enzyme activity assay results, quantitative real-time PCR was performed on DNMT1 and HDAC1 genes. Glyceraldehyde-3-phosphate dehydrogenase (GAPDH) was used as a positive control by using Real-Time™ qPCR Primer Assay (SABioscience, Frederick, MD, USA) on Light Cycler 480 instrument (Roche Applied Science, Mannheim, Germany). Total RNA of 4 μg was extracted from cell samples using an Array Grade Total RNA isolation kit (SuperArray, Frederick, MD, USA) and quantitated by UV spectroscopy using a biophotometer. The integrity and quality of isolated RNA was determined by running the RNAs on agarose gel electrophoresis. PCR reaction mix was prepared 25 μl final volume containing 12.5 μl RT2 SYBR Green qPCR Master Mix, 10.5 μl DNAase-RNaseFree water, 1.0 μl gene-specific 10 μM PCR primer pair stock and finally 1,0 μl diluted cDNA samples for each primer (SABioscience, Frederick, MD, USA). Universal cycling conditions (10 min at 95 °C, 15 s at 95 °C, 1 min 60 °C for 40 cycles) were carried out.
Statistical analysis
The results of the study were expressed as mean ± SD and data was analyzed by using one way analysis of variance test (ANOVA) followed by Dunnett’s t test for multiple comparisons. Values with p < 0.05 were considered as significant. Determination of the synergistic cytotoxic effects of the combined treatment of cells with AT-101 and cisplatin was assessed by Biosoft CalcuSyn 2.0 software (Ferguson, MO, USA). The Combination index (CI) was used to express additive effect (CI = 1), antagonism (CI > 1), synergism (CI < 1), and strong synergism (CI < 0.5) [16]. Data analysis and graphs were done by Graphpad Prism 5.0 software (La Jolla, CA, USA).
Results
Combination of AT-101 and cisplatin resulted in strong synergistic cytotoxicity as compared to any agent alone in human ovarian cancer cells
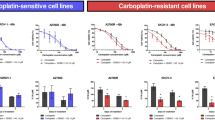
To evaluate the cytotoxic effects of AT-101 or cisplatin on the viability of human ovarian cancer cells, OVCAR-3 and MDAH-2774 cells were exposed to increasing concentrations of AT-101 (1–10 μM) or cisplatin (1–10 μM) or in combination for 24, 48 and 72 h, and XTT cell viability assay was performed.
AT-101 and cisplatin alone decreased the cell viability in a time- and dose dependent manner both in OVCAR-3 and MDAH-2774 cells (Fig. 1a, b). Highest cytotoxicity was observed at 72 h for both agents. IC50 values were calculated from cell proliferation plots and found to be 4.6 and 5.8 μM for cisplatin, 4.8 and 3.9 μM for AT-101 in OVCAR-3 and MDAH-2774 cells, respectively.
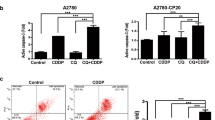
To study the possible synergistic/additive effects of AT-101 and cisplatin combination, OVCAR-3 and MDAH-2774 cells were exposed to different concentrations of each agent alone, and in combination of both for 72 h. Our results indicate that 0.5 μM AT-101 and 1 μM cisplatin showed 6 and 26 % decreases, respectively, in the viability of OVCAR-3 cells but the combination of both resulted in 75 % decrease in the cell viability (Fig. 2a). In MDAH-2774 cells, 1 μM AT-101 and 0.5 μM cisplatin showed 8 and 22 % decreases, respectively, in the viability of MDAH-2774 cells but the combination of both resulted in 79 % decrease in the cell viability (Fig. 2b). All of the concentrations for each combination found to be synergistic/strong synergistic in ovarian cancer cells are presented in Table 1.
Sequential administration of the agents were carried out to see if either of these agents enhance the other one’s effect and to understand whether the synergism depended on which agent applied first. Experiment results showed that synergistic cytotoxicity was observed no matter which agent applied first in both cells.
Combination treatment induced both DNA Fragmentation and caspase 3/7 activity in human ovarian cancer cells
To examine the induction of apoptosis, we incubated these cells in the presence of AT-101 or cisplatin alone or in combination for 72 h and then we quantified the levels of mono-oligo nucleosome fragments by Cell Death Detection Plus Kit (Roche Applied Science, Mannheim, Germany). Our results clearly showed that both AT-101 and cisplatin alone induced apoptosis in human ovarian cancer cells but combination treatment resulted in synergistic induction of apoptosis by DNA fragmentation analysis at 72 h (Fig. 3a, b).
In parallel with the DNA fragmentation analyses, combination treatment resulted in synergistic induction of caspase 3/7 enzyme activity both in OVCAR-3 and MDAH-2774 cells, confirming the previous data (data not shown).
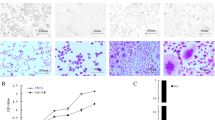
The immunofluorescence images using live/dead cell reagent in OVCAR-3 and MDAH-2774 cells were shown in Fig. 4. The cell death was increased in AT-101/cisplatin combination treated ovarian cancer cells when compared to any agent alone and untreated control.
Immunofluorescence images of OVCAR-3 and MDAH-2774 cells using live/dead cell reagent. After incubating the cells with AT-101/cisplatin combination (1 μM AT-101 and 0.5 μM cisplatin:CP) for 72 h, cells were treated with 1 μL calcein AM/1 mL of D-PBS. The cell death was increased when compared to untreated control. The red and green fluorescence are the markers of dead and live cells, respectively. The Live/Dead Viability/Cytotoxicity Assay Kit (Invitrogen) allows determination of live and dead cells with two probes using calcein AM and ethidium homodimer (EthD-1). Live cells are distinguished by the presence of ubiquitous intracellular esterase activity, determined by the enzymatic conversion of the virtually nonfluorescent cell-permeant calcein AM to the intensely fluorescent calcein. The polyanionic dye calcein is well retained within live cells, producing an intense uniform green fluorescence in live cells (ex/em ~495 nm/~515 nm). EthD-1 enters cells with damaged membranes and undergoes a 40-fold enhancement of fluorescence upon binding to nucleic acids, thereby producing a bright red fluorescence in dead cells (ex/em ~495 nm/~635 nm). EthD-1 is excluded by the intact plasma membrane of live cells. (Color figure online)
Changes in apoptosis-related protein expressions in human ovarian cancer cells exposed to AT-101/cisplatin combination
Combination treatment with AT-101 (1 μM) and cisplatin (0.5 μM) caused significant changes in some of the critical apoptosis-related proteins in ovarian cancer cells (p < 0.05). The data for apoptosis-related proteins after treatment with either AT-101 or cisplatin alone or in combination in OVCAR-3 and MDAH-2774 are given as fold changes in Table 2.
Pro-apoptotic proteins which play important roles in carcinogenesis were significantly induced in both cell lines. Bad, Bax, Fas, phospho-p53 (S46), Cleaved caspase-3, SMAC/Diablo, TNFR1 and Cytochrome c were induced by—2.5-, 10.5-, 1.6-, 4.8-, 7.4-, 6.2-, 2.9- and 5.1-fold in OVCAR-3 cells respectively, whereas, Bax, TRAILR2, FADD, p27, phospho-p53 (S46), Cleaved caspase-3, Cytochrome c, SMAC/Diablo and TNFR1 were induced by—8.7-, 2.1-, 1.8-, 2.0-, 4.2-, 8.2-, 69-, 8.4- and 2.3-fold in MDAH-2774 cells, respectively. Among the anti-apoptotic proteins, Bcl-2, HIF-1A, cIAP-1, XIAP were reduced by—4.6-, 2.3-, 4.5-, and 4.8-fold in OVCAR-3 cells, whereas p21, Bcl-2, cIAP-1, HSP27, Clusterin and XIAP were reduced by—2.6-, 5.5-, 6.2-, 2.5-, 5.3-, and 5.8-fold in MDAH-2774 cells, respectively.
AT-101/cisplatin combination inhibited both DNMT and HDAC enzyme activities in ovarian cancer cells
Exposure to combination treatment for 72 h resulted in a dose dependent inhibition of both DNMT and HDAC enzyme activities in human ovarian cancer cells, as compared to agents alone (Fig. 5a, b). We also evaluated the alterations in the mRNA levels of DNMT1 and HDAC1 enzymes by qRT-PCR Assay. There were 2.4-and 4.8-fold decreases in the mRNA levels of DNMT1 and HDAC1 enzymes in ovarian cancer cells exposed to combination treatment, as compared to agents alone (data not shown).
Effects of AT-101/cisplatin combination on the global epigenetic patterns of DNA methylation and histone deacetylation in OVCAR-3 (a) and MDAH-2774 (b) cells at 72 h. The results are the mean of three independent experiments. Cells treated with cisplatin/AT-101 alone or in combination reduced the DNMT and HDAC enzyme activities as compared to untreated controls (p < 0.05)
Discussion
Due to the toxic side effects and treatment-induced resistance in cancer cells, usage of cisplatin may be limited in ovarian cancer treatment. Thus, new strategies are needed for chemosensitization of cancer cells.
Some bioactive compounds derived from natural sources have been reported to have chemosensitizing effect in ovarian cancer cells. For example, curcumin, the active component of turmeric, has been suggested to sensitize ovarian cancer cells to docetaxel therapy [17]. Also, in our previous studies, different enantiomers of gossypol in combination with various chemotherapeutics synergistically induced cytotoxicity and apoptosis in different type of human cancer cell lines [11, 18–20]. In the literature, it has been shown that cisplatin resistance was reversed by AT-101 in head and neck cancer cells [10].
AT-101 is a small molecule with a BH-3 mimetic structure that binds and inhibits the anti-apoptotic members of the Bcl-2 family proteins [21]. It has potent anticancer activity in many types of human cancers, with negligible toxicity for normal cells, making this agent an attractive agent for cancer treatment [22, 23]. This promising molecule as a single agent and in combination with various agents has now being studied widely in different types of human cancers in phase II trials [24, 25].
In our study, we applied subtoxic doses of AT-101(1 μM) together with a low dosage of cisplatin (0.5 μM) to minimize the side effects of combination treatment, which may be critical in clinical studies to follow. We found that addition of AT-101 to cisplatin reduced the cell viability and induced apoptosis in human ovarian cancer cells as compared to untreated controls. By using apoptosis protein array we tried to elucidate which of the apoptosis related proteins are affected by this combination treatment. We found that, combination treatment resulted in significant changes in the expression levels of some pivotal apoptotic proteins in ovarian cancer cells, which play important roles in regulating the apoptotic responses to chemotherapeutics.
Among the pro-apoptotic proteins, Bax was induced in both ovarian cancer cells. Bax is found in the cytosol of a cell in an inactive form and by a stimulus, such as cytotoxic agents, it undergoes conformational changes and inserts into the mitochondrial outer membrane and forms pores that causes releasing of proapoptotic proteins such as cytochrome c and Smac into the cytosol [26, 27]. Parallel with this data, beside Bax induction, Cytochrome c and Smac protein levels were also induced by the combination treatment in both OVCAR-3 and MDAH-2774 cells.
Bcl-2 is another anti-apoptotic protein which is inhibited by the combination treatment in ovarian cancer cells. In ovarian cancer cells, Bcl-2 is an important modulator of drug-induced apoptosis and chemoresistance [28]. The survival of the cell that is regulated by the IAPs was comparable to that regulated by anti-apoptotic proteins, such as Bcl-2. cIAP-1 and XIAP are the anti-apoptotic proteins which are the members of the inhibitor apoptosis (IAP) gene family. Combination treatment decreased the levels of these apoptosis suppressor proteins. This indicates that this combination treatment is a significant inducer of apoptosis in ovarian cancer cells, as well as a good candidate to overcome the drug resistance phenomenon in ovarian cancer. IAPs can inhibit caspase-3 and caspase-7 cell death proteases which are downstreams of many proapoptotic signaling pathways [29, 30]. As revealed by enzyme activity assay, caspase 3/7 activation was also obviously induced in both ovarian cancer cells as proved by protein array.
Among the proteins that are induced by the combination treatment; p53 has a unique role in tumor progression and drug resistance. It is known that phosphorylation of p53 at serine- 46 [(phospho-p53 (S46)] induces apoptosis, which was also induced in both ovarian cancer cells suggesting that p53 is involved in the apoptotic response of the combination treatment [31].
Induction of phospho-p53 levels by the combination treatment was accompanied by decreased p21 levels in MDAH-2774 cells. The cyclin-dependent kinase inhibitor p21 is involved in p53 mediated growth arrest and regulation of cell growth [32]. Besides anti-apoptotic and pro-survival role, p21 appears to play a key role in cellular resistance of tumors during treatment with anticancer agents including cisplatin, doxorubicin and paclitaxel [33]. The inhibition of anti-apoptotic p21 levels by combination treatment represents a favorable molecular mode of action.
In this study, we demonstrated that by acting in different apoptotic targets within ovarian cancer cells, this novel combination therapy may achieve to overcome drug resistance in platinum-resistant ovarian cancer.
Epigenetic alterations can regulate sensitivity to chemotherapeutic drugs in ovarian cancer. Thus, targeting epigenetic modifications could also provide novel treatment options for ovarian cancer [34, 35]. The most widely studied epigenetic changes in cancer cells are DNA methylation/demethylation and histone acetylation/deacetylation. DNA methylation is catalyzed by DNMTs whereas acetylation/deacetylation of histones is catalyzed by HATs/HDACs. In this study, we have evaluated the effect of AT-101/cisplatin combination on both DNMT and HDAC enzyme activities and also mRNA levels in ovarian cancer cells. We found that combination treatment resulted in inhibition of both DNMT and HDAC activities and also mRNA levels in ovarian cancer cells. Since epigenetic alterations play important roles in carcinogenesis and drug response, reversal of these changes should be one of the goals of cancer treatment.
In conclusion, AT-101 exhibits a great potential in sensitization of human ovarian cancer cells to cisplatin treatment in vitro by effecting pivotal apoptotic proteins and also essential epigenetic events. Up to best our knowledge, this is the first study demonstrating strong synergism between AT-101 and cisplatin in ovarian cancer, and may easily be translated to clinical approach with further studies. Since, cisplatin is the cornerstone of treatment strategy; we strongly suggest that the combination of AT-101 with cisplatin may hold great promise for development as a novel chemotherapeutic approach in human ovarian cancer.
References
Herzog TJ, Sill MW, Walker JL et al (2011) A phase II study of two topotecan regimens evaluated in recurrent platinum-sensitive ovarian, fallopian tube or primary peritoneal cancer: a Gynecologic Oncology Group Study (GOG 146Q). Gynecol Oncol 120:454–458
Rakowski JA, Ahmad S, Holloway RW (2012) Use of pegylated liposomal doxorubicin in the management of platinum-sensitive recurrent ovarian cancer: current concepts. Expert Rev Anticancer Ther 12:31–40
Dear RF, Gao B, Harnett P (2010) Recurrent ovarian cancer: treatment with pegylated liposomal doxorubicin; a Westmead Cancer Care Centre experience. Asia Pac J Clin Oncol 6:66–73
Broxterman HJ, Gotink KJ, Verheul HM (2009) Understanding the causes of multidrug resistance in cancer: a comparison of doxorubicin and sunitinib. Drug Resist Updat 12:114–126
Luqmani YA (2005) Mechanisms of drug resistance in cancer chemotherapy. Med Princ Pract 14(Suppl 1):35–48
Balch C, Huang TH, Brown R et al (2004) The epigenetics of ovarian cancer drug resistance and resensitization. Am J Obstet Gynecol 191:1552–1572
Reed JC (2006) Drug insight: cancer therapy strategies based on restoration of endogenous cell death mechanisms. Nat Clin Pract Oncol 3:388–398
Galluzzi L, Senovilla L, Vitale I et al (2012) Molecular mechanisms of cisplatin resistance. Oncogene 31:1869–1883
Zerp SF, Stoter R, Kuipers G et al (2009) AT-101, a small molecule inhibitor of anti-apoptotic Bcl-2 family members, activates the SAPK/JNK pathway and enhances radiation-induced apoptosis. Radiat Oncol 4:47
Bauer JA, Trask DK, Kumar B et al (2005) Reversal of cisplatin resistance with a BH3 mimetic, (−)-gossypol, in head and neck cancer cells: role of wild-type p53 and Bcl-xL. Mol Cancer Ther 4:1096–1104
Kisim A, Atmaca H, Cakar B et al (2012) Pretreatment with AT-101 enhances tumor necrosis factor-related apoptosis-inducing ligand (TRAIL)-induced apoptosis of breast cancer cells by inducing death receptors 4 and 5 protein levels. J Cancer Res Clin Oncol 138:1155–1163
Zeller C, Brown R (2010) Therapeutic modulation of epigenetic drivers of drug resistance in ovarian cancer. Ther Adv Med Oncol 2:319–329
Asadollahi R, Hyde CA, Zhong XY (2010) Epigenetics of ovarian cancer: from the lab to the clinic. Gynecol Oncol 118:81–87
Hamilton TC, Young RC, McKoy WM et al (1983) Characterization of a human ovarian carcinoma cell line (NIH: OVCAR-3) with androgen and estrogen receptors. Cancer Res 43:5379–5388
Erten C, Karaca B, Kucukzeybek Y et al (2009) Regulation of growth factors in hormone- and drug-resistant prostate cancer cells by synergistic combination of docetaxel and octreotide. BJU Int 104:107–114
Chou TC, Talalay P (1984) Quantitative analysis of dose-effect relationships: the combined effects of multiple drugs on enzyme inhibitors. Adv Enzyme Regul 22:27–55
Lin YG, Kunnumakkara AB, Nair A et al (2007) Curcumin inhibits tumor growth and angiogenesis in ovarian carcinoma by targeting the nuclear factor-kappaB pathway. Clin Cancer Res 13:3423–3430
Atmaca H, Gorumlu G, Karaca B et al (2009) Combined gossypol and zoledronic acid treatment results in synergistic induction of cell death and regulates angiogenic molecules in ovarian cancer cells. Eur Cytokine Netw 20:121–130
Sanli UA, Gorumlu G, Erten C et al (2009) Targeting apoptosis in the hormone- and drug-resistant prostate cancer cell line, DU-145, by gossypol/zoledronic acid combination. Cell Biol Int 33:1165–1172
Cengiz E, Karaca B, Kucukzeybek Y et al (2010) Overcoming drug resistance in hormone- and drug-refractory prostate cancer cell line, PC-3 by docetaxel and gossypol combination. Mol Biol Rep 37:1269–1277
Hu W, Wang F, Tang J et al (2012) Proapoptotic protein Smac mediates apoptosis in cisplatin-resistant ovarian cancer cells when treated with the anti-tumor agent AT101. J Biol Chem 287:68–80
Moretti L, Li B, Kim KW et al (2010) AT-101, a Pan-Bcl-2 inhibitor, leads to radiosensitization of non-small cell lung cancer. J Thorac Oncol 5:680–687
Liu G, Kelly WK, Wilding G et al (2009) An open-label, multicenter, phase I/II study of single-agent AT-101 in men with castrate-resistant prostate cancer. Clin Cancer Res 15:3172–3176
Ready N, Karaseva NA, Orlov SV et al (2011) Double-blind, placebo-controlled, randomized phase 2 study of the proapoptotic agent AT-101 plus docetaxel, in second-line non-small cell lung cancer. J Thorac Oncol 6:781–785
Heist RS, Fain J, Chinnasami B et al (2010) Phase I/II study of AT-101 with topotecan in relapsed and refractory small cell lung cancer. J Thorac Oncol 5:1637–1643
Nie C, Tian C, Zhao L et al (2008) Cysteine 62 of Bax is critical for its conformational activation and its proapoptotic activity in response to H2O2-induced apoptosis. J Biol Chem 283:15359–15369
Mohan J, Gandhi AA, Bhavya BC et al (2006) Caspase-2 triggers Bax-Bak-dependent and -independent cell death in colon cancer cells treated with resveratrol. J Biol Chem 281:17599–17611
Eliopoulos AG, Kerr DJ, Herrod J et al (1995) The control of apoptosis and drug resistance in ovarian cancer: influence of p53 and bcl-2. Oncogene 11:1217–1228
Daveraux QL, Takahashi R, Saivesen QS et al (1997) X-linked IAP is a direct inhibitor of cell-death proteases. Nature 388:300–303
Roy N, Deveraux QL, Takahashi R et al (1997) The c-IAP-1 and c-IAP-2 proteins are direct inhibitors of specific caspases. EMBO J 16:6914–6925
Liu HF, Hsiao PW, Chao C (2008) Celecoxib induces p53-PUMA pathway for apoptosis in human colorectal cancer cells. Chem Biol Interact 176:48–57
Li R, Hannon GJ, Beach D, Stillman B (1996) Subcellular distribution of p21 and PCNA in normal and repair-deficient cells following DNA damage. Curr Biol 6:189–199
Stangelberger A, Schally AV, Rick FG et al (2012) Inhibitory effects of antagonists of growth hormone releasing hormone on experimental prostate cancers are associated with upregulation of wild-type p53 and decrease in p21 and mutant p53 proteins. Prostate 72:555–565
Balch C, Fang F, Matei DE et al (2009) Minireview: epigenetic changes in ovarian cancer. Endocrinology 150:4003–4011
Glasspool RM, Teodoridis JM, Brown R (2006) Epigenetics as a mechanism driving polygenic clinical drug resistance. Br J Cancer 94:1087–1092
Conflict of interest
No conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Karaca, B., Atmaca, H., Bozkurt, E. et al. Combination of AT-101/cisplatin overcomes chemoresistance by inducing apoptosis and modulating epigenetics in human ovarian cancer cells. Mol Biol Rep 40, 3925–3933 (2013). https://doi.org/10.1007/s11033-012-2469-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-012-2469-z