Abstract
Parkinson’s disease (PD) is one of the most common neurodegenerative diseases after Alzheimer’s disease (AD), afflicting adults above the age of sixty irrespective of gender, race, ethnicity, and social status. PD is characterized by motor dysfunctions, displaying resting tremor, rigidity, bradykinesia, and postural imbalance. Non-motor symptoms, including rapid eye movement (REM) behavior disorder, constipation, and loss of sense of smell, typically occur many years before the appearance of the PD motor symptoms that lead to a diagnosis. The loss of dopaminergic neurons in the substantia nigra, which leads to the motor symptoms seen in PD, is associated with the deposition of aggregated, misfolded α-Synuclein (α-Syn, SNCA) proteins forming Lewy Bodies. Additionally, dysregulation of miRNA (a short form of mRNA) may contribute to the developing pathophysiology in PD and other diseases such as cancer. Overexpression of α-Syn and miRNA in human samples has been found in PD, AD, and dementia. Therefore, evaluating these molecules in urine, present either in the free form or in association with extracellular vesicles of biological fluids, may lead to early biomarkers for clinical diagnosis. Collection of urine is non-invasive and thus beneficial, particularly in geriatric populations, for biomarker analysis. Considering the expression and function of α-Syn and miRNA, we predict that they can be used as early biomarkers in the diagnosis and prognosis of neurodegenerative diseases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parkinson’s disease (PD), sometimes referred to as “paralysis agitans,” is an idiopathic and genetic disease of the nervous system characterized by motor and non-motor dysfunctions. This is a chronic, progressive neurodegenerative disease that appears predominantly in persons over the age of sixty while remaining rare among people under the age of forty (Kempster et al. 2010). PD is the second most common neurodegenerative disease behind Alzheimer’s disease (AD), affecting ten million people worldwide. A record one million Americans are currently suffering from PD, with approximately 60,000 new cases occurring each year (Chou 2016; Parkinson’s Disease Foundation: Statistics on Parkinson’s 2016; Sherer et al. 2012). Many symptoms are debilitating, including visual hallucinations, fluctuations in consciousness, sleep disturbances, falls, and depression, all leading to loss of independence, disability, and a significant burden for caregivers.
Environmental and genetic factors can both contribute to the prevalence of PD. A genetic association is minor, as most cases are idiopathic; however, it has been well established that constitutive translation of the SNCA gene mediated by a 5′ untranslated region (5’-UTR) has an integral role in PD pathology (Koukouraki and Doxakis 2016). The protein, α-Synuclein (α-Syn), accumulates to form toxic, pathological forms such as α-Syn oligomers (Atik et al. 2016). Thus, recent studies on α-Syn oligomers and other toxic species of α-Syn (such as A53T, H50Q mutations) have led to the emergence of potential biomarkers in brain diseases (Kalia et al. 2013; Kasten and Klein 2013; Shalash et al. 2017). Another promising biomarker, miRNAs, are short regulatory RNAs that control gene expression through interacting with the UTR of target messenger RNA, causing translational repression or RNA destabilization (Filipowicz et al. 2008; Filipowicz et al. 2005). miRNA as a signature novel biomarker has been studied in colorectal cancer, Crohn’s disease, and cardiomyopathy (Liu et al. 2013; Luo et al. 2011; Miyamoto et al. 2015; Zahm et al. 2011). Moreover, miRNA such as miR-135b-3p, miR-30e-5p, miR-223-3p, which have inflammatory pathway targets, are dysregulated in the blood, brain, and other body fluids in a broad range of diseases in adults, including neurodegenerative diseases PD, AD, and dementia (Cheng et al. 2015; Mancuso et al. 2019; Zeng et al. 2019).
The immune cells of the brain, microglia, have a considerable role in neurodegenerative diseases. They surveil the brain and are activated due to neuronal damage, misfolded proteins, viruses, and more. Microglial activation causes cytokine release and thus neuroinflammation, which, when chronic, results in cell death, as shown in Fig. 1 (Ouchi et al. 2009). It is still controversial as to whether neuroinflammation is a cause or a result of PD. Moreover, misfolded, oligomeric, and other unusual forms of α-Syn activate microglia; Increased microglia were found in the area of the brain most affected in PD, the Substantia Nigra (Lim et al.) of PD postmortem brain sections (Wakade et al. 2014). This suggested the infiltration of immune cells crossing the blood-brain barrier (BBB) (Banati et al. 1998; McGeer et al. 1988). Microglia can release anti-inflammatory cytokines and rescue injured cells, or they can take up dead or damaged cells, utilizing both autophagy and exosomes for clearance (Zhao and Wang 2019). The over-the-counter vitamin, niacin, was found to induce macrophage polarization and anti-inflammatory cytokines in PD (Wakade et al. 2014; Wakade et al. 2018). An in vitro study showed the ameliorative effect of niacin in regulating inflammatory cytokine through G protein-coupled receptor GPR109A via nuclear factor-kappa B (NF-kB) (Giri et al. 2019; Seamon et al. 2020). Reducing neuroinflammation is an important target for slowing or halting PD progression. The appearance of signature molecular events that can be seen in the body fluids, such as with neuroinflammation, could be observed much earlier than PD’s clinical symptoms (Fig. 2).
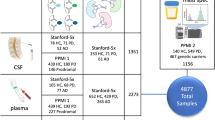
Schematic representation of the biomarker resources for clinical diagnosis. The miRNAs and α-Syn oligomers, which are elevated in biological fluids such as saliva, plasma, urine, and CSF, could provide useful biomarkers for early diagnosis, prognosis, and therapeutic invention of Parkinson’s disease
Here, in this review, we discuss important considerations for urine as a biospecimen to identify early biomarkers. To provide further background information and justification for detecting the above molecules, we discuss the scope of available methods and instruments available for urinary analysis. We further present numerous urine assays currently used clinically, including high throughput methods and their importance to healthcare and clinical diagnosis, with a particular focus on microfluidic urine assays. Together, this review discusses the prospective candidate biomarkers, α-Syn, and miRNA, particularly in urine (a non-invasive method) which may have the ability to detect crucial warning signs, allow for earlier intervention and care, or reduce the risk of permanent or life-threatening damage of chronic neurodegenerative diseases.
Urine as a source of biomarkers
Early biomarker identification using liquid biopsy is key for timely, earlier diagnosis and to find preventative measures for the progression of PD, further neuronal loss, dementia, and disability. Moreover, non-invasive biospecimen collection methods are more attractive in geriatric subjects than healthy adult subjects due to the availability of healthy, accessible veins. Thus, urinary analysis has great potential in this respect, considering its biological richness and its capacity to be a convenient and cost-effective method for disease diagnosis/prognosis. A large volume of urine is produced daily by the average person: 6–7 urinations totaling 400 to 2000 mL; therefore, samples are abundant for collection and analysis (Lepowsky et al. 2017). It has been reported that urine contains more than 3000 biological molecules. A complete set of 2651 confirmed human metabolites and their structure has been documented (Bouatra et al. 2013). Even chronic diseases like cancer and coronary heart diseases use urine as a means of specific disease identifications (Brindle et al. 2002; Chan et al. 2011). Urine is also commonly used for clinical assessment in urinary tract infections (UTI), kidney function, diabetes, and pregnancy testing, but not in the context of brain diseases. This may be due to urine being conventionally regarded as an inappropriate source of biospecimens for neurodegenerative diseases since it is anatomically distant from the brain. The circulatory α-Syn oligomer and miRNA have no boundary (Table 1 & 2) as evidenced by the literature review. Several studies have indicated the overexpression of key proteins including α-Syn and miRNA, in biofluids of PD patients (Atik et al. 2016). These two molecules are promising potential candidates for early biomarkers in urine, allowing for screening and diagnosis that would enable the patients to receive proper care for brain diseases promptly (Simerville et al. 2005). Particularly for PD, early intervention enabled by early diagnosis could reduce the risk of neurological complications, motor function failure, or even death, all of which are associated with chronic neurodegenerative diseases.
α-Synuclein as a potential biomarker in PD
PD is considered a synucleinopathy that develops slowly; however, there is no efficient early diagnosis method, nor is there a cure. Mainly three different types of synucleinopathies exist, PD, dementia with Lewy bodies (DLB), and Multiple System Atrophy (Ng et al. 2011), which are characterized by the aberrant accumulation of the presynaptic protein α-Syn (SNCA), resulting in toxic α-Syn oligomers or Lewy Bodies (Ioanna Chalatsa et al. 2020). Different types of biofluids considered for the identification of candidate biomarkers such as blood, CSF, urine, and saliva have been summarized in Table 1 (Cao et al. 2019; Chang et al. 2019; Chen et al. 2020; Devic et al. 2011; Ioanna Chalatsa et al. 2020; Lee et al. 2006; Lin et al. 2017; Mollenhauer et al. 2019b; Mollenhauer et al. 2011; Nam et al. 2020; Pchelina et al. 2011; Shahnawaz et al. 2017; Tokuda et al. 2010; Vivacqua et al. 2019; Wang et al. 2015; Waragai et al. 2010). Several studies have reported evaluation of α-Syn in blood and CSF using commercially available Enzyme-linked immunosorbent assays (Psihogios et al.) kits and semi-quantitative immunoblot analysis in PD subjects (Lee et al. 2006; Waragai et al. 2010). On the contrary, some investigators failed to detect α-Syn in CSF (Jakowec et al. 1998; Ohrfelt et al. 2009). This suggests α-Syn is not a good candidate biomarker in CSF samples. Moreover, CSF sample collection is a cumbersome and painful method for geriatric subjects, particularly PD subjects with motor and non-motor dysfunction. A larger multicenter trial (MCT) may be needed to obtain specificity and sensitivity to detect α-Syn protein in CSF. However, plasma samples may offer better opportunities to identify α-Syn as a biomarker for PD. In this context, Lee et al. were able to identify α-Syn in the blood of PD and MSA patients (Lee et al. 2006). The distribution of α-Syn in various body fluids and methods of detection has been given in Table 1. Several factors may account for the discrepancy in the results, including variations in specificity, sensitivity, and accuracy of each experimental method. This raises the question of how many samples were used in the assays and assay format capabilities for clinical diagnosis. Therefore, the concentration of analytes in clinical specimens is essential for evaluating molecules of interest.
We also believe, based on literature reviews by others, that there is a considerable variation in the concentrations of metabolites in urine, mainly due to the influence of many factors including age, gender, genetic background, health status, activity level, and diet (Guneral and Bachmann 1994; Psihogios et al. 2008; Zuppi et al. 1997). However, urine is a notable non-invasive biospecimen that could be available in a copious amount with no limitations for clinical diagnosis. α-Syn is constitutively expressed in various cells and transported across all peripheral tissue and body fluids (Shin et al. 2000). Recent studies showed α-Syn to be associated with many pathways, including endocytosis, Golgi homeostasis, ER-to-Golgi transport, and presynaptic trafficking for intercellular communications through exosomes (Loov et al. 2016; Wang and Hay 2015). Moreover, it exists in different forms, i.e., monomeric, oligomeric, and phosphorylated forms in different cells and the extracellular matrix (Surguchov 2016). The ubiquitous presence of α-Syn may offer an opportunity to evaluate its presence in non-invasive samples for clinical diagnosis.
Recently, several studies reported α-Syn was contained in and secreted through exosomes as a cargo vehicle to distant tissues and/or for communication and excretion through the skin, saliva, blood, and CSF (Mollenhauer et al. 2019a; Mollenhauer et al. 2019b; Mollenhauer et al. 2019c). Ho, et al. showed increased levels of DJ-1 and LRRK2 proteins detected in the exosomes isolated from urine samples from PD patients, but they were not able to detect α-Syn in the urine exosomes (Ho et al. 2014). Ioanna et al. found that Lewy Bodies in PD pathology are mostly made up of α-Syn that has been excessively phosphorylated, proposing phosphorylated α-Syn as another potential early biomarker (Ioanna Chalatsa et al. 2020). The precise and site-specific measurements of α-Syn expression levels may be relevant to disease specificity and are necessary for detecting the quality and quantity of this protein for clinical diagnosis. The existence of the differing forms of α-Syn may reflect specific disease activities, and the availability of urine could be obtained easily from any patients, including PD subjects. Identifying and quantifying the different forms of α-Syn in urine may be a novel method to discriminate brain diseases from other unrelated neurological disorders for clinical diagnosis and to implement early intervention measures for delayed progression of the disease.
α-Synuclein determination in urine samples
Urine was conventionally regarded as an inappropriate source of biomarkers for neurodegenerative diseases because it is anatomically distant from the brain compared to peripheral blood and CSF (Reed et al.). However, recent studies have suggested that urine could be utilized as a source of brain disease biomarkers if an appropriate marker is predetermined by immunoassay approaches in PD subjects’ urine (Nam et al. 2020). Studies have also demonstrated an accumulation of α-Syn in the urine of animals and humans under both physiological and pathological states (Seol et al. 2020). A few urinary biomarkers already found such as formaldehyde and 8-OHdG, show a correlation with severity of the disease (Nam et al. 2020; Seol et al. 2020). There are limited studies using urine to evaluate α-Syn as a biomarker.
Next-generation technologies will lead to developing affordable and accessible healthcare. However, the advent of recent sophisticated technology includes proteomics and paper-based detection systems, which may be applied in the identification and analysis of α-Syn and alterations of protein levels in urine relative to the severity of the disease. Mass spectrometry provides the best sensitivity, selectivity, and quantitative identification capabilities to determine the bioactive compounds with accuracy (Beasley-Green 2016). (Psihogios et al.) already tested and validated by Nam et al. also have the sensitivity to quantitatively detect α-Syn oligomers in urine in PD subjects compared to age-matched control groups (Table 1) (Nam et al. 2020). Moving forward in the development of paper-based microfluidic urine analysis would be beneficial for promoting efficient, effective, and affordable diagnosis. In this context, Lepowsky et al. described the paper-based urine analysis methods as a point of care diagnosis (Lepowsky et al. 2017). It is predicted that α-Syn oligomers could be identified using paper-based technology with more sensitivity and specificity than classical immunoassays and immunoblots for clinical diagnosis and prognosis of PD and other synucleopathic diseases.
Circulating miRNAs as potential biomarkers for PD
miRNAs regulate gene expression at the post-transcriptional level has been well established. They have recently emerged as prominent transcriptional regulators of various cellular processes, including neurodevelopment. They are abundantly present in the brain, and their dysfunction has been implicated in an array of neuropathological conditions, including PD, AD, and dementia. miRNAs exist in the tissues and have also been found to circulate in several body fluids, including plasma or serum, CSF, urine, and saliva. There are significant differences between the circulating miRNA expression profiles of healthy individuals and those of PD patients. The importance of miRNA in biological processes has been recently recognized for its potential role in regulating approximately 33% of human genes (Ambros 2004; Lewis et al. 2005; Lim et al. 2003). Changes in miRNA expression have been associated with the development and progression of diseases (Tili et al. 2007). Recent studies evaluated miRNAs as a potential for diagnostics in many clinical applications, including cancer. However, there are limitations of miRNA-based diagnostics in brain diseases due to the impracticality of sampling brain tissues from living humans. Difficulties also occur with obtaining CSF and blood samples from aged populations. Growing evidence based on several studies revealed miRNA to be a novel class of biomarkers for disease diagnosis and prognosis in PD (Du et al. 2009; Guerau-de-Arellano et al. 2012; Otaegui et al. 2009). There are two notable reasons why miRNA should be considered as potential biomarkers for disease identification: the expression level of miRNAs that are specific to the disease’s activities and the availability of miRNAs in a large number of samples, including tissue biopsies, whole blood, blood cells, serum, plasma, urine, and even exosomes.
Urine is considered one of the prominent extracellular human body fluids obtained in large volumes using simple, non-invasive methods and is easy to obtain in large volumes for clinical diagnosis and disease identifications. Even chronic diseases like cancer and coronary heart diseases use urine as a means of specific disease identifications (Brindle et al. 2002; Chan et al. 2011). Recently, several miRNAs have been detected in urine samples (Hanke et al. 2010). Several supporting articles identify more than 40 urinary miRNAs related to specific urological pathologies, including intrinsic kidney disease, renal cell carcinoma, and bladder cancer (Sun and Lerman 2019; Thorsen et al. 2012; Zahm et al. 2011). There is a significant concern about the stability of miRNA in the harsh urinary milieu; However, the miRNA can also be tightly packed in exosomes which are protected from the harsh conditions of urine (Street et al. 2017). The exosome not only provides protection but also keeps miRNA in a concentrated form, making robust detection quantitative for disease identifications with accuracy.
Table 2 shows the expression of disease-specific miRNA profiles targeting proteins of interest unique to various neurological diseases. Specifically, several miRNAs, such as miR-21, miR-192, miR-200, and miR-29, are upregulated in renal diseases described by Chung et al. (Chung et al. 2013; Sun and Lerman 2019). Moreover, miRNAs profiles are not limited to renal diseases and are also found in the blood, CSF, saliva, and urine in response to central nervous system injury (Sun et al. 2018). Several miRNAs (e.g., miR-497, Let-7f, miR-181, miR-15a/16–1, miR-23a, miR-424, miR-124, miR-122, miR-21, others) that are altered after CNS injuries have been reported, relating to neuroinflammation in nervous systems (Sun et al. 2018). Microarray would be ideal for capturing miRNA changes related to disease type and severity (Jimenez-Avalos et al. 2020). miRNAs are not only used for diagnostic parameters, but it has a potential role in gene therapy for regulating disease-modifying genes of interest (Hashemi and Gorji-Bahri 2020; Thorsen et al. 2012; Zhao and Wang 2019). With the development of the latest innovative technology, including paper-based microfluidic technology, LC-MS/MS, inductively coupled plasma mass spectrometry, and high-performance liquid chromatography (HPLC), numerous metabolic molecules can be determined both qualitatively and quantitatively with accuracy in very short periods of time (Bouatra et al. 2013).
Despite the challenges, a miRNA-based diagnosis has become a promising strategy for neurodegenerative disease identifications either at point-of-care diagnosis or with sophisticated instruments in laboratory settings. Much remains to be discovered in order to utilize miRNA-based approaches and identify candidate miRNAs as potential biomarkers in brain diseases. Successful clinical identification and validations of miRNAs in urine will undoubtedly enhance the future of this nascent field.
Conclusion
In general, PD itself does not cause death but is associated with an increased risk of morbidity and mortality worldwide (Hirsch et al. 2003; Lindqvist et al. 2012). Despite the numerous research studies, clinical diagnosis and management of PD are still in their infancy by suboptimal detection and prognosis methods. There are no optimized, validated biomarkers available with high enough sensitivity and specificity for early disease identification before the canonical PD motor symptoms occur. Early diagnosis of the disease is essential for enhanced maintenance of PD subjects’ health through clinical interventions. Here we highlighted both α-Syn oligomers and miRNAs as potential biomarkers for disease diagnosis and explored the use of urine as a potential non-invasive biospecimen sample to identify biomarkers for neurodegenerative diseases, specifically PD. Recent technological advances allow for the systematic, holistic, and unbiased identifications and characterization of miRNAs and α-Syn oligomers in the urine, ensuring the promising potential of approaches in biomarker discovery. Developing optimal miRNA and α-Syn oligomer identification tools for clinical validation may pave the way for novel biomarkers in PD diagnosis and prognosis.
Data availability
Not Applicable.
References
Ambros V (2004) The functions of animal microRNAs. Nature 431:350–355. https://doi.org/10.1038/nature02871
Atik A, Stewart T, Zhang J (2016) Alpha-Synuclein as a biomarker for Parkinson's disease. Brain Pathol 26:410–418. https://doi.org/10.1111/bpa.12370
Banati RB, Daniel SE, Blunt SB (1998) Glial pathology but absence of apoptotic nigral neurons in long-standing Parkinson's disease. Movement disorders : official journal of the Movement Disorder Society 13:221–227. https://doi.org/10.1002/mds.870130205
Beasley-Green A (2016) Urine proteomics in the era of mass spectrometry. Int Neurourol J 20:S70–S75. https://doi.org/10.5213/inj.1612720.360
Beck KE, Kay JG, Braun JE (2006) Rdj2, a J protein family member, interacts with cellular prion PrP(C) biochemical and biophysical research communications 346:866-871 doi:https://doi.org/10.1016/j.bbrc.2006.05.185
Bhattacharyya NP, Banerjee M, Majumder P (2008) Huntington's disease: roles of huntingtin-interacting protein 1 (HIP-1) and its molecular partner HIPPI in the regulation of apoptosis and transcription. FEBS J 275:4271–4279. https://doi.org/10.1111/j.1742-4658.2008.06563.x
Bouatra S, Aziat F, Mandal R, Guo AC, Wilson MR, Knox C, Bjorndahl TC, Krishnamurthy R, Saleem F, Liu P, Dame ZT, Poelzer J, Huynh J, Yallou FS, Psychogios N, Dong E, Bogumil R, Roehring C, Wishart DS (2013) The human urine metabolome. PLoS One 8:e73076. https://doi.org/10.1371/journal.pone.0073076
Brindle JT, Antti H, Holmes E, Tranter G, Nicholson JK, Bethell HWL, Clarke S, Schofield PM, McKilligin E, Mosedale DE, Grainger DJ (2002) Rapid and noninvasive diagnosis of the presence and severity of coronary heart disease using 1H-NMR-based metabonomics. Nat Med 8:1439–1444. https://doi.org/10.1038/nm1202-802
Cao Z, Wu Y, Liu G, Jiang Y, Wang X, Wang Z, Feng T (2019) Alpha-Synuclein in salivary extracellular vesicles as a potential biomarker of Parkinson's disease. Neurosci Lett 696:114–120. https://doi.org/10.1016/j.neulet.2018.12.030
Chan EC, Pasikanti KK, Nicholson JK (2011) Global urinary metabolic profiling procedures using gas chromatography-mass spectrometry. Nat Protoc 6:1483–1499. https://doi.org/10.1038/nprot.2011.375
Chang CW, Yang SY, Yang CC, Chang CW, Wu YR (2019) Plasma and serum alpha-Synuclein as a biomarker of diagnosis in patients with Parkinson's disease. Front Neurol 10:1388. https://doi.org/10.3389/fneur.2019.01388
Chen NC et al. (2020) Plasma levels of alpha-Synuclein, Abeta-40 and T-tau as biomarkers to predict cognitive impairment in Parkinson's disease front aging Neurosci 12:112 doi:https://doi.org/10.3389/fnagi.2020.00112
Cheng L et al (2015) Prognostic serum miRNA biomarkers associated with Alzheimer's disease shows concordance with neuropsychological and neuroimaging assessment. Mol Psychiatry 20:1188–1196. https://doi.org/10.1038/mp.2014.127
Chou KL (2016) Clinical manifestations of Parkinson disease
Chung AC, Yu X, Lan HY (2013) MicroRNA and nephropathy: emerging concepts. Int J Nephrol Renovasc Dis 6:169–179. https://doi.org/10.2147/IJNRD.S37885
Devic I, Hwang HJ, Edgar JS, Izutsu K, Presland R, Pan C, Goodlett DR, Wang Y, Armaly J, Tumas V, Zabetian CP, Leverenz JB, Shi M, Zhang J (2011) Salivary alpha-synuclein and DJ-1: potential biomarkers for Parkinson's disease. Brain : a journal of neurology 134:e178. https://doi.org/10.1093/brain/awr015
Du C et al (2009) MicroRNA miR-326 regulates TH-17 differentiation and is associated with the pathogenesis of multiple sclerosis. Nat Immunol 10:1252–1259. https://doi.org/10.1038/ni.1798
Filipowicz W, Bhattacharyya SN, Sonenberg N (2008) Mechanisms of post-transcriptional regulation by microRNAs: are the answers in sight? Nat Rev Genet 9:102–114. https://doi.org/10.1038/nrg2290
Filipowicz W, Jaskiewicz L, Kolb FA, Pillai RS (2005) Post-transcriptional gene silencing by siRNAs and miRNAs. Curr Opin Struct Biol 15:331–341. https://doi.org/10.1016/j.sbi.2005.05.006
Geng L, Zhang T, Liu W, Chen Y (2018) miR-494-3p modulates the progression of in vitro and in vivo Parkinson's disease models by targeting SIRT3. Neurosci Lett 675:23–30. https://doi.org/10.1016/j.neulet.2018.03.037
Giri B, Belanger K, Seamon M, Bradley E, Purohit S, Chong R, Morgan JC, Baban B, Wakade C (2019) Niacin ameliorates Neuro-inflammation in Parkinson's disease via GPR109A. Int J Mol Sci 20. https://doi.org/10.3390/ijms20184559
Guerau-de-Arellano M, Alder H, Ozer HG, Lovett-Racke A, Racke MK (2012) miRNA profiling for biomarker discovery in multiple sclerosis: from microarray to deep sequencing. J Neuroimmunol 248:32–39. https://doi.org/10.1016/j.jneuroim.2011.10.006
Guneral F, Bachmann C (1994) Age-related reference values for urinary organic acids in a healthy Turkish pediatric population. Clin Chem 40:862–866
Hanke MHK, Merz H, Feller AC, Kausch I, Jocham D, Warnecke JM, Sczakiel G (2010) A robust methodology to study urine microRNA as tumor marker: microRNA-126 and microRNA-182 are related to urinary bladder cancer. Jurolonc 28(6):6
Hashemi A, Gorji-Bahri G (2020) MicroRNA: promising roles in Cancer therapy. Curr Pharm Biotechnol 21:1186–1203. https://doi.org/10.2174/1389201021666200420101613
Hirsch EC, Breidert T, Rousselet E, Hunot S, Hartmann A, Michel PP (2003) The role of glial reaction and inflammation in Parkinson's disease. Ann N Y Acad Sci 991:214–228
Ho DH, Yi S, Seo H, Son I, Seol W (2014) Increased DJ-1 in urine exosome of Korean males with Parkinson's disease. Biomed Res Int 2014:704678–704678. https://doi.org/10.1155/2014/704678
Hwang JY, Zukin RS (2018) REST, a master transcriptional regulator in neurodegenerative disease. Curr Opin Neurobiol 48:193–200. https://doi.org/10.1016/j.conb.2017.12.008
Ioanna Chalatsa KM, Emmanouilidou E, Vekrellis K (2020) Assessment of cerebrospinal fluid α-synuclein as a potential biomarker in Parkinson’s disease and synucleinopathies. Neuroimmunol Neuroinflammation 7:8
Jakowec MW, Petzinger GM, Sastry S, Donaldson DM, McCormack A, Langston JW (1998) The native form of alpha-synuclein is not found in the cerebrospinal fluid of patients with Parkinson's disease or normal controls. Neurosci Lett 253:13–16. https://doi.org/10.1016/s0304-3940(98)00599-0
Jimenez-Avalos JA, Fernandez-Macias JC, Gonzalez-Palomo AK (2020) Circulating exosomal MicroRNAs: new non-invasive biomarkers of non-communicable disease. Mol Biol Rep 48:961–967. https://doi.org/10.1007/s11033-020-06050-w
Johnson R, Zuccato C, Belyaev ND, Guest DJ, Cattaneo E, Buckley NJ (2008) A microRNA-based gene dysregulation pathway in Huntington's disease. Neurobiol Dis 29:438–445. https://doi.org/10.1016/j.nbd.2007.11.001
Kalia LV, Kalia SK, McLean PJ, Lozano AM, Lang AE (2013) Alpha-Synuclein oligomers and clinical implications for Parkinson disease. Ann Neurol 73:155–169. https://doi.org/10.1002/ana.23746
Kasten M, Klein C (2013) The many faces of alpha-synuclein mutations. Movement disorders : official journal of the Movement Disorder Society 28:697–701. https://doi.org/10.1002/mds.25499
Kempster PA, O'Sullivan SS, Holton JL, Revesz T, Lees AJ (2010) Relationships between age and late progression of Parkinson's disease: a clinico-pathological study. Brain : a journal of neurology 133:1755–1762. https://doi.org/10.1093/brain/awq059
Kim J, Inoue K, Ishii J, Vanti WB, Voronov SV, Murchison E, Hannon G, Abeliovich A (2007) A MicroRNA feedback circuit in midbrain dopamine neurons. Science 317:1220–1224. https://doi.org/10.1126/science.1140481
Koukouraki P, Doxakis E (2016) Constitutive translation of human alpha-synuclein is mediated by the 5′-untranslated region. Open Biol 6:160022. https://doi.org/10.1098/rsob.160022
Kume K et al (2018) Serum microRNA expression profiling in patients with multiple system atrophy Mol med rep 17:852-860. https://doi.org/10.3892/mmr.2017.7995
Lau P, Bossers K, Janky R', Salta E, Frigerio CS, Barbash S, Rothman R, Sierksma ASR, Thathiah A, Greenberg D, Papadopoulou AS, Achsel T, Ayoubi T, Soreq H, Verhaagen J, Swaab DF, Aerts S, de Strooper B (2013) Alteration of the microRNA network during the progression of Alzheimer's disease. EMBO Mol Med 5:1613–1634. https://doi.org/10.1002/emmm.201201974
Lee PH, Lee G, Park HJ, Bang OY, Joo IS, Huh K (2006) The plasma alpha-synuclein levels in patients with Parkinson's disease and multiple system atrophy. J Neural Transm 113:1435–1439. https://doi.org/10.1007/s00702-005-0427-9
Lee ST, Chu K, Jung KH, Ban JJ, Im WS, Jo HY, Park JH, Lim JY, Shin JW, Moon J, Lee SK, Kim M, Roh JK (2015) Altered expression of miR-202 in cerebellum of multiple-system atrophy. Mol Neurobiol 51:180–186. https://doi.org/10.1007/s12035-014-8788-4
Lepowsky E, Ghaderinezhad F, Knowlton S, Tasoglu S (2017) Paper-based assays for urine analysis. Biomicrofluidics 11:051501. https://doi.org/10.1063/1.4996768
Lewis BP, Burge CB, Bartel DP (2005) Conserved seed pairing, often flanked by adenosines, indicates that thousands of human genes are microRNA targets. Cell 120:15–20. https://doi.org/10.1016/j.cell.2004.12.035
Lim LP, Glasner ME, Yekta S, Burge CB, Bartel DP (2003) Vertebrate microRNA genes. Science 299:1540. https://doi.org/10.1126/science.1080372
Lin CH, Yang SY, Horng HE, Yang CC, Chieh JJ, Chen HH, Liu BH, Chiu MJ (2017) Plasma alpha-synuclein predicts cognitive decline in Parkinson's disease. J Neurol Neurosurg Psychiatry 88:818–824. https://doi.org/10.1136/jnnp-2016-314857
Lindqvist D, Kaufman E, Brundin L, Hall S, Surova Y, Hansson O (2012) Non-motor symptoms in patients with Parkinson's disease - correlations with inflammatory cytokines in serum. PLoS One 7:e47387. https://doi.org/10.1371/journal.pone.0047387
Liu F, Xiong Y, Zhao Y, Tao L, Zhang Z, Zhang H, Liu Y, Feng G, Li B, He L, Ma J, Qin S, Yang Y (2013) Identification of aberrant microRNA expression pattern in pediatric gliomas by microarray. Diagn Pathol 8:158. https://doi.org/10.1186/1746-1596-8-158
Loov C, Scherzer CR, Hyman BT, Breakefield XO, Ingelsson M (2016) Alpha-Synuclein in extracellular vesicles: functional implications and diagnostic opportunities. Cell Mol Neurobiol 36:437–448. https://doi.org/10.1007/s10571-015-0317-0
Luo X, Burwinkel B, Tao S, Brenner H (2011) MicroRNA signatures: novel biomarker for colorectal cancer? Cancer Epidemiol Biomark Prev 20:1272–1286. https://doi.org/10.1158/1055-9965.EPI-11-0035
Mancuso R, Agostini S, Hernis A, Zanzottera M, Bianchi A, Clerici M (2019) Circulatory miR-223-3p discriminates between Parkinson's and Alzheimer's patients scientific reports 9:9393 doi:https://doi.org/10.1038/s41598-019-45687-x
Marti E et al (2010) A myriad of miRNA variants in control and Huntington's disease brain regions detected by massively parallel sequencing. Nucleic Acids Res 38:7219–7235. https://doi.org/10.1093/nar/gkq575
McGeer PL, Itagaki S, Boyes BE, McGeer EG (1988) Reactive microglia are positive for HLA-DR in the substantia nigra of Parkinson's and Alzheimer's disease brains. Neurology 38:1285–1291
Miyamoto SD, Karimpour-Fard A, Peterson V, Auerbach SR, Stenmark KR, Stauffer BL, Sucharov CC (2015) Circulating microRNA as a biomarker for recovery in pediatric dilated cardiomyopathy. J Heart Lung Transplant 34:724–733. https://doi.org/10.1016/j.healun.2015.01.979
Mollenhauer B, Bowman FDB, Drake D, Duong J, Blennow K, el-Agnaf O, Shaw LM, Masucci J, Taylor P, Umek RM, Dunty JM, Smith CL, Stoops E, Vanderstichele H, Schmid AW, Moniatte M, Zhang J, Kruse N, Lashuel HA, Teunissen C, Schubert T, Dave KD, Hutten SJ, Zetterberg H (2019a) Antibody-based methods for the measurement of alpha-synuclein concentration in human cerebrospinal fluid - method comparison and round robin study. J Neurochem 149:126–138. https://doi.org/10.1111/jnc.14569
Mollenhauer B, Caspell-Garcia CJ, Coffey CS, Taylor P, Singleton A, Shaw LM, Trojanowski JQ, Frasier M, Simuni T, Iranzo A, Oertel W, Siderowf A, Weintraub D, Seibyl J, Toga AW, Tanner CM, Kieburtz K, Chahine LM, Marek K, Galasko D, for the PPMI study (2019b) Longitudinal analyses of cerebrospinal fluid alpha-Synuclein in prodromal and early Parkinson's disease. Movement disorders : official journal of the Movement Disorder Society 34:1354–1364. https://doi.org/10.1002/mds.27806
Mollenhauer B, Locascio JJ, Schulz-Schaeffer W, Sixel-Doring F, Trenkwalder C, Schlossmacher MG (2011) Alpha-Synuclein and tau concentrations in cerebrospinal fluid of patients presenting with parkinsonism: a cohort study. Lancet Neurol 10:230–240. https://doi.org/10.1016/S1474-4422(11)70014-X
Mollenhauer B, Zimmermann J, Sixel-Döring F, Focke NK, Wicke T, Ebentheuer J, Schaumburg M, Lang E, Friede T, Trenkwalder C, on behalf of the DeNoPa Study Group (2019c) Baseline predictors for progression 4 years after Parkinson's disease diagnosis in the De novo Parkinson cohort (DeNoPa). Movement disorders : official journal of the Movement Disorder Society 34:67–77. https://doi.org/10.1002/mds.27492
Montag J, Hitt R, Opitz L, Schulz-Schaeffer WJ, Hunsmann G, Motzkus D (2009) Upregulation of miRNA hsa-miR-342-3p in experimental and idiopathic prion disease. Mol Neurodegener 4:36. https://doi.org/10.1186/1750-1326-4-36
Mouradian MM (2012) MicroRNAs in Parkinson's disease. Neurobiol Dis 46:279–284. https://doi.org/10.1016/j.nbd.2011.12.046
Muller M, Kuiperij HB, Claassen JA, Kusters B, Verbeek MM (2014) MicroRNAs in Alzheimer's disease: differential expression in hippocampus and cell-free cerebrospinal fluid. Neurobiol Aging 35:152–158. https://doi.org/10.1016/j.neurobiolaging.2013.07.005
Nam D, Lee JY, Lee M, Kim J, Seol W, Son I, Ho DH (2020) Detection and assessment of alpha-Synuclein oligomers in the urine of Parkinson's disease patients. J Parkinsons Dis 10:981–991. https://doi.org/10.3233/JPD-201983
Nelson PT, Wang WX, Rajeev BW (2008) MicroRNAs (miRNAs) in neurodegenerative diseases. Brain Pathol 18:130–138. https://doi.org/10.1111/j.1750-3639.2007.00120.x
Ng DC et al (2011) Opposing actions of extracellular signal-regulated kinase (ERK) and signal transducer and activator of transcription 3 (STAT3) in regulating microtubule stabilization during cardiac hypertrophy. J Biol Chem 286:1576–1587. https://doi.org/10.1074/jbc.M110.128157
Ohrfelt A, Grognet P, Andreasen N, Wallin A, Vanmechelen E, Blennow K, Zetterberg H (2009) Cerebrospinal fluid alpha-synuclein in neurodegenerative disorders-a marker of synapse loss? Neurosci Lett 450:332–335. https://doi.org/10.1016/j.neulet.2008.11.015
Otaegui D, Baranzini SE, Armañanzas R, Calvo B, Muñoz-Culla M, Khankhanian P, Inza I, Lozano JA, Castillo-Triviño T, Asensio A, Olaskoaga J, de Munain AL (2009) Differential micro RNA expression in PBMC from multiple sclerosis patients. PLoS One 4:e6309. https://doi.org/10.1371/journal.pone.0006309
Ouchi Y, Yagi S, Yokokura M, Sakamoto M (2009) Neuroinflammation in the living brain of Parkinson's disease. Parkinsonism Relat Disord 15(Suppl 3):S200–S204. https://doi.org/10.1016/S1353-8020(09)70814-4
Parkinson's Disease Foundation: Statistics on Parkinson's. (2016)
Pchelina SN, Emelyanov AK, Yakimovskii AF, Miller DW, Shabalina IG, Drozdova AS, Schwarzman AL (2011) Reduced content of alpha-synuclein in peripheral blood leukocytes of patients with LRRK2-associated Parkinson's disease. Bull Exp Biol Med 150:679–681. https://doi.org/10.1007/s10517-011-1221-3
Pietrzak M, Papp A, Curtis A, Handelman SK, Kataki M, Scharre DW, Rempala G, Sadee W (2016) Gene expression profiling of brain samples from patients with Lewy body dementia Biochem. Biophys Res Commun 479:875–880. https://doi.org/10.1016/j.bbrc.2016.09.114
Psihogios NG, Gazi IF, Elisaf MS, Seferiadis KI, Bairaktari ET (2008) Gender-related and age-related urinalysis of healthy subjects by NMR-based metabonomics. NMR Biomed 21:195–207. https://doi.org/10.1002/nbm.1176
Reed ER, Latourelle JC, Bockholt JH, Bregu J, Smock J, Paulsen JS, Myers RH, PREDICT-HD CSF ancillary study investigators (2018) MicroRNAs in CSF as prodromal biomarkers for Huntington disease in the PREDICT-HD study. Neurology 90:e264–e272. https://doi.org/10.1212/WNL.0000000000004844
Saba R, Goodman CD, Huzarewich RL, Robertson C, Booth SA (2008) A miRNA signature of prion induced neurodegeneration. PLoS One 3:e3652. https://doi.org/10.1371/journal.pone.0003652
Scott HL, Tamagnini F, Narduzzo KE, Howarth JL, Lee YB, Wong LF, Brown MW, Warburton EC, Bashir ZI, Uney JB (2012) MicroRNA-132 regulates recognition memory and synaptic plasticity in the perirhinal cortex. Eur J Neurosci 36:2941–2948. https://doi.org/10.1111/j.1460-9568.2012.08220.x
Seamon M, Purohit S, Giri B, Baban B, Morgan JC, Chong R, Wakade C (2020) Niacin for Parkinson's disease. Clinical & Experimental Neuroimmunology 11:10
Seol W, Kim H, Son I (2020) Urinary biomarkers for neurodegenerative. Diseases Exp Neurobiol 29:325–333. https://doi.org/10.5607/en20042
Shahnawaz M, Tokuda T, Waragai M, Mendez N, Ishii R, Trenkwalder C, Mollenhauer B, Soto C (2017) Development of a biochemical diagnosis of Parkinson disease by detection of alpha-Synuclein Misfolded aggregates in cerebrospinal fluid. JAMA Neurol 74:163–172. https://doi.org/10.1001/jamaneurol.2016.4547
Shalash A et al. (2017) Elevated serum α-Synuclein autoantibodies in patients with Parkinson’s disease relative to Alzheimer’s disease and controls. Front Neurol
Sherer TB, Chowdhury S, Peabody K, Brooks DW (2012) Overcoming obstacles in Parkinson's disease. Movement disorders : official journal of the Movement Disorder Society 27:1606–1611. https://doi.org/10.1002/mds.25260
Shin EC, Cho SE, Lee DK, Hur MW, Paik SR, Park JH, Kim J (2000) Expression patterns of alpha-synuclein in human hematopoietic cells and in Drosophila at different developmental stages. Mol Cells 10:65–70. https://doi.org/10.1007/s10059-000-0065-x
Simerville JA, Maxted WC, Pahira JJ (2005) Urinalysis: a comprehensive review. Am Fam Physician 71:1153–1162
Street JM, Koritzinsky EH, Glispie DM, Star RA, Yuen PS (2017) Urine Exosomes: an emerging trove of biomarkers. Adv Clin Chem 78:103–122. https://doi.org/10.1016/bs.acc.2016.07.003
Sun IO, Lerman LO (2019) Urinary microRNA in kidney disease: utility and roles. Am J Physiol Renal Physiol 316:F785–F793. https://doi.org/10.1152/ajprenal.00368.2018
Sun P, Liu DZ, Jickling GC, Sharp FR, Yin KJ (2018) MicroRNA-based therapeutics in central nervous system injuries. Journal of cerebral blood flow and metabolism : official journal of the International Society of Cerebral Blood Flow and Metabolism 38:1125–1148. https://doi.org/10.1177/0271678X18773871
Surguchov A (2016) Parkinson's Disease: Assay of Phosphorylated alpha-Synuclein in Skin Biopsy for Early Diagnosis and Association with Melanoma. Brain Sci:6. https://doi.org/10.3390/brainsci6020017
Thorsen SB, Obad S, Jensen NF, Stenvang J, Kauppinen S (2012) The therapeutic potential of microRNAs in cancer. Cancer J 18:275–284. https://doi.org/10.1097/PPO.0b013e318258b5d6
Tili E, Michaille JJ, Gandhi V, Plunkett W, Sampath D, Calin GA (2007) miRNAs and their potential for use against cancer and other diseases. Future Oncol 3:521–537. https://doi.org/10.2217/14796694.3.5.521
Tokuda T, Qureshi MM, Ardah MT, Varghese S, Shehab SAS, Kasai T, Ishigami N, Tamaoka A, Nakagawa M, el-Agnaf OMA (2010) Detection of elevated levels of alpha-synuclein oligomers in CSF from patients with Parkinson disease. Neurology 75:1766–1772. https://doi.org/10.1212/WNL.0b013e3181fd613b
Valera E, Spencer B, Mott J, Trejo M, Adame A, Mante M, Rockenstein E, Troncoso JC, Beach TG, Masliah E, Desplats P (2017) MicroRNA-101 modulates autophagy and Oligodendroglial alpha-Synuclein accumulation in multiple system atrophy. Front Mol Neurosci 10:329. https://doi.org/10.3389/fnmol.2017.00329
Vivacqua G, Suppa A, Mancinelli R, Belvisi D, Fabbrini A, Costanzo M, Formica A, Onori P, Fabbrini G, Berardelli A (2019) Salivary alpha-synuclein in the diagnosis of Parkinson's disease and progressive Supranuclear palsy. Parkinsonism Relat Disord 63:143–148. https://doi.org/10.1016/j.parkreldis.2019.02.014
Wakade C, Chong R, Bradley E, Thomas B, Morgan J (2014) Upregulation of GPR109A in Parkinson's disease. PLoS One 9:e109818. https://doi.org/10.1371/journal.pone.0109818
Wakade C, Giri B, Malik A, Khodadadi H, Morgan JC, Chong RK, Baban B (2018) Niacin modulates macrophage polarization in Parkinson's disease. J Neuroimmunol 320:76–79. https://doi.org/10.1016/j.jneuroim.2018.05.002
Wang G, van der Walt JM, Mayhew G, Li YJ, Züchner S, Scott WK, Martin ER, Vance JM (2008a) Variation in the miRNA-433 binding site of FGF20 confers risk for Parkinson disease by overexpression of alpha-synuclein. Am J Hum Genet 82:283–289. https://doi.org/10.1016/j.ajhg.2007.09.021
Wang L, Zhang L (2020a) Circulating Exosomal miRNA as diagnostic biomarkers of neurodegenerative diseases. Front Mol Neurosci 13:53. https://doi.org/10.3389/fnmol.2020.00053
Wang R, Zhang J (2020b) Clinical significance of miR-433 in the diagnosis of Alzheimer's disease and its effect on Abeta-induced neurotoxicity by regulating JAK2. Exp Gerontol 141:111080. https://doi.org/10.1016/j.exger.2020.111080
Wang T, Hay JC (2015) Alpha-synuclein toxicity in the early secretory pathway: how it drives Neurodegeneration in Parkinsons disease. Front Neurosci 9:433. https://doi.org/10.3389/fnins.2015.00433
Wang WX, Rajeev BW, Stromberg AJ, Ren N, Tang G, Huang Q, Rigoutsos I, Nelson PT (2008b) The expression of microRNA miR-107 decreases early in Alzheimer's disease and may accelerate disease progression through regulation of beta-site amyloid precursor protein-cleaving enzyme 1. J Neurosci 28:1213–1223. https://doi.org/10.1523/JNEUROSCI.5065-07.2008
Wang X, Yu S, Li F, Feng T (2015) Detection of alpha-synuclein oligomers in red blood cells as a potential biomarker of Parkinson's disease. Neurosci Lett 599:115–119. https://doi.org/10.1016/j.neulet.2015.05.030
Waragai M, Sekiyama K, Sekigawa A, Takamatsu Y, Fujita M, Hashimoto M (2010) Alpha-Synuclein and DJ-1 as potential biological fluid biomarkers for Parkinson's disease. Int J Mol Sci 11:4257–4266. https://doi.org/10.3390/ijms11114257
Wu Q, Ye X, Xiong Y, Zhu H, Miao J, Zhang W, Wan J (2016) The protective role of microRNA-200c in Alzheimer's disease pathologies is induced by Beta amyloid-triggered endoplasmic reticulum stress. Front Mol Neurosci 9:140. https://doi.org/10.3389/fnmol.2016.00140
Yu L, Li H, Liu W, Zhang L, Tian Q, Li H, Li M (2020) MiR-485-3p serves as a biomarker and therapeutic target of Alzheimer's disease via regulating neuronal cell viability and neuroinflammation by targeting AKT3. Mol genet genomic med:e1548. https://doi.org/10.1002/mgg3.1548
Zahm AM, Thayu M, Hand NJ, Horner A, Leonard MB, Friedman JR (2011) Circulating microRNA is a biomarker of pediatric Crohn disease. J Pediatr Gastroenterol Nutr 53:26–33. https://doi.org/10.1097/MPG.0b013e31822200cc
Zeng R, Luo DX, Li HP, Zhang QS, Lei SS, Chen JH (2019) MicroRNA-135b alleviates MPP(+)-mediated Parkinson's disease in in vitro model through suppressing FoxO1-induced NLRP3 inflammasome and pyroptosis. J Clin Neurosci 65:125–133. https://doi.org/10.1016/j.jocn.2019.04.004
Zhao L, Wang Z (2019) MicroRNAs: game changers in the regulation of alpha-Synuclein in Parkinson's disease. Parkinsons Dis 2019:1743183–1743110. https://doi.org/10.1155/2019/1743183
Zhu Y, Li C, Sun A, Wang Y, Zhou S (2015) Quantification of microRNA-210 in the cerebrospinal fluid and serum: implications for Alzheimer's disease. Exp Ther Med 9:1013–1017. https://doi.org/10.3892/etm.2015.2179
Zuppi C, Messana I, Forni F, Rossi C, Pennacchietti L, Ferrari F, Giardina B (1997) 1H NMR spectra of normal urines: reference ranges of the major metabolites. Clin Chim Acta 265:85–97. https://doi.org/10.1016/s0009-8981(97)00110-1
Acknowledgments
We are grateful to Augusta University and the CSRA Parkinson’s Support Groups of Georgia, USA for providing support. There is no financial conflict of interest.
Code availability
Not Applicable.
Funding
The Central Savannah River Area (CSRA) Parkinson’s Support Group awarded grant PSG00037 to Dr. Banabihari Giri for Parkinson’s Research.
Author information
Authors and Affiliations
Contributions
Idea Development, BG, MS.
Literature Search, BG, MS, AB, SC, JM.
Draft, BG, MS, AB.
Revisions, BG, MS, AB, SC, MCW, JM, SP, BB.
Corresponding author
Ethics declarations
Ethics approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Conflict of interests
The authors declare no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Giri, B., Seamon, M., Banerjee, A. et al. Emerging urinary alpha-synuclein and miRNA biomarkers in Parkinson’s disease. Metab Brain Dis 37, 1687–1696 (2022). https://doi.org/10.1007/s11011-021-00735-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-021-00735-2