Abstract
Hyperglycaemia during pregnancy is the main reason for developing diabetes mediated vascular complications. Advanced glycation end products (AGEs) are formed due to non-enzymatic glycation of proteins, lipids and nucleic acids during hyperglycaemia. It has the potential to damage vasculature by modifying the substrate or by means of AGEs and receptor of AGE (RAGE) interaction. It has been linked with the pathogenesis of various vascular diseases including coronary heart disease, atherosclerosis, restenosis etc. This study was carried out to investigate the role of AGEs-EGR-1 pathway in gestational diabetes mellitus (GDM) vascular inflammation. Human umbilical vein endothelial cells (HuVECs) isolated from normal glucose tolerant mothers were subjected to various treatments including high glucose, silencing of early growth response (EGR)-1, blockade of protein kinase C (PKC) β, blocking extracellular signal-regulated protein kinases 1 and 2 (ERK1/2), and treatment with AGEs and assayed for EGR-1, tissue factor (TF) and soluble intercellular adhesion molecule (sICAM)-1. Similarly, umbilical vein endothelial cells isolated from normal and GDM mothers were assayed for EGR-1, TF, and sICAM-1. There was a significant increase in EGR-1 and TF levels in HuVECs isolated form GDM mother’s umbilical cord and normal HuVECs treated with high glucose condition. This was accompanied by elevated levels of sICAM-1 in high glucose treated cells. Our results revealed AGE-mediated activation of EGR-1 and its downstream genes via PKC βII and ERK1/2 signaling pathway. The present study demonstrated a novel mechanism of AGEs/ PKC βII/ ERK1/2/EGR-1 pathway in inducing vascular inflammation in GDM.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
GDM is characterized by hyperglycaemia and insulin resistance that affects 14% of pregnancies worldwide [1, 2]. The occurrence of Gestational diabetes [3] and childhood obesity [4] has increased dramatically in the last few decades in India. Many studies have been carried out to explain the role of fetal nutrition and its effect on diabetes and cardiovascular complications [5]. A proper intra-uterine environment is necessary for the normal growth and development of the fetus. There are evidence demonstrating that adverse intra-uterine environment (both less and high nutrient conditions) affects the fetus pancreatic vascular development and response to insulin leading to adult-onset of type 2 diabetes mellitus (T2DM) and/or GDM. An altered inflammatory state was reported to be seen in GDM [6,7,8,9,10].
One of the predominant factors which affect the vascular integrity is the increased concentration of AGEs. AGEs stem from a non-enzymatic reaction of reducing sugars with free amino groups of proteins, lipids, and nucleic acids [11]. For several years, the research in diabetes is mainly focused on establishing the physiological function of AGEs and their effects. AGEs are known to be involved in the pathophysiology of ischemia/reperfusion injury, inflammation, and cardiovascular dysfunctions by activation of various transcription factors. Among the various AGEs studied, N ε-Carboxymethyl Lysine (CML) is regarded as one of the major form of AGEs formed during various pathological conditions including diabetes [12, 13]. CML is a product of glycoxidation and lipoxidation due to irreversible binding of carbohydrates or lipids with proteins. Increased concentration of CML is observed during atheroma and microvascular complications of diabetes [14,15,16]. AGEs exert its cellular effects via binding to its receptor the RAGE [17, 18]. EGR-1 is a major transcription factor reported to a play critical role in vascular complications of type 2 diabetes [19, 20]. EGR-1 exerts its role in various disease conditions via activation of various inflammatory genes like tumor necrosis factor (TNF)-α, ICAM-1, interleukin (IL)-13, IL-6, TF, monocyte chemoattractant protein (MCP)-1, and plasminogen activator inhibitor (PAI) -1 [21,22,23,24,25,26,27,28,29,30]. Researchers have demonstrated a link between EGR-1 and both acute and chronic vascular stress, such as hypoxia, ischemia/reperfusion, mechanical stress, shear stress, emphysema, atherosclerosis, and acute vascular injury [31,32,33,34]. EGR-1 activation has been observed in microvascular endothelial cells of placental villi when vascular disease is present [35].
However, the role of AGEs (CML), RAGE, and EGR-1 on vascular inflammation in GDM is not known. The present study was aimed at investigating the role of the AGE-EGR-1 pathway in causing vascular inflammation in umbilical vein tissues procured from normal glucose tolerant and GDM mothers and primary HuVECs isolated from these tissues were subjected to hyperglycaemia treatment.
Materials and methods
Sample collection and GDM screening
Samples of umbilical cord were collected after delivery from participant enrolled in K.A.P. Viswanatham government medical college, Trichy and Kovai Medical Center and Hospital (KMCH), Coimbatore. Institutional ethical committee approval was obtained prior to the sample collection (MCRC.IEC#001, 2015 and EC/AP/432/12/2015). The pregnant mothers with polycystic ovary syndrome (PCOS), pre-diabetes, previous pregnancy diabetes, chronic diseases, and preeclampsia were excluded from the study. The pregnant mothers were considered to have GDM based on the IADPSG (International Association for Diabetes in Pregnancy Study Group) criteria, if they exceed 2 or more glucose values as follows: fasting blood glucose ≥ 92 mg/dl, a 1-h blood glucose ≥ 180 mg/dl, and a 2-h blood glucose ≥ 153 mg/dl after taking a 75 g oral glucose tolerance test. The patients eligible for this present study were identified during 32 weeks of pregnancy and their clinical parameters including age, body mass index, baby birth weight, blood pressure, blood glucose levels (OGTT values), were noted down for further investigation.
Isolation and culture of HuVECs from the umbilical vein
Primary HuVECs was cultured as described earlier [36]. Briefly, the two ends of the umbilical cord was cut neatly. After a wash with PBS, collagenase-II (0.2%) was injected through one end of the vein while the other end is tightly clamped with a clip. The cord was incubated in PBS for 15 min at 37 °C. The cord was gently squeezed and flushed with sterile PBS after incubation. The cells were further centrifuged at 1000 RPM for 10 min, and the supernatant was discarded, and cell pellet was suspended in EGM-2 medium (Lonza) with 10% fetal calf serum. The isolated cells were then plated in a T25 flask and incubated at 37 °C with 5% CO2 until it reaches confluence. The cells were then stored in liquid nitrogen until further use.
Treatment conditions
HuVECs passage between 5 to7 was used for this current study [36]. All the treatments were done in 6 well plates. The cells were seeded at a concentration of 0.2 × 106 cells. The treatments included in this study are as follows: (1) Normal glucose—5.5 mM glucose acts as control, (2) High glucose (HG)—25 mM glucose + 80 nM insulin [37].These treatments were followed by EGR-1-siRNA transfection, PKC β and ERK1/2 inhibitors treatment, and AGEs treatment studies with and without EGR-1-siRNA and inhibitors.
For siRNA transfection studies, the HuVECs were treated with EGR-1-siRNA and scrambled siRNA at concentrations of 25 pmol and 0.5 µmol, respectively in the presence of Lipofectamine-3000 (Invitrogen) for 24 h followed by HG treatment as described above. The optimum EGR-1-siRNA concentration was measured in HuVECs (Supplementary Fig. 1). For inhibitor study, the cells were treated with PKC β and ERK1/2 inhibitors (Ruboxistaurin and FR180204) at concentrations of 6 nM/L and 0.3 µM/L respectively and incubated for 1 h followed by HG treatment for 24 h. For AGEs treatment, cells were treated with CML at a concentration of 100 µmol for 1 h followed by HG treatment for 24 h. In another set of transfection studies, the cells were transfected with siEGR-1 and scrRNA for 24 h and then treated with CML and PKC β inhibitor separately for one hour, followed by HG treatment for 24 h.
Gene expression studies
HuVECs isolated from umbilical vein tissues and HuVECs post treatment was directly lysed in TRIzol reagent (TaKaRa, Germany) for isolation of RNA. Total RNA was quantified using Nanodrop 2000/20000 spectrophotometer instrument (Thermo Fisher Scientific, USA). 2000 ng of total RNA was used for the synthesis of complementary DNA (cDNA). cDNA was synthesized using Bio-Rad cDNA synthesis kit. Semi-quantitative real-time PCR was performed to quantify the gene expressions of EGR-1, ICAM-1 and TF using Sybr green (Roche) in Master Cycler Realplex instrument (Eppendorf). The cycle condition includes 95 °C for 5 min, 95 °C for 20 s, followed by 40 cycles of annealing temperature (Tm) of respective primers (EGR-1 Tm-62 °C, TF Tm-61 °C, ICAM-1 Tm-62 °C, 18 s Tm-59 °C) and then 76 °C for 30 s. All gene expression data were normalized against 18 s rRNA expression. The primer sequence specific for EGR-1, ICAM-1, and TF are given in Supplementary Table-1.
Western blotting
Total protein from HuVECs isolated from human umbilical vein and HuVECs after treatments were separated using cell lysis buffer (V8571, Promega, USA) containing protease inhibitor cocktail purchased from Sigma, USA (P8340). The cells were incubated for 30 min as per the manufacturer’s instructions for cell lysis. The cells 50 µg of protein from all the cell lysates was loaded onto a 10% SDS gel and ran at a power of 110V. The protein in the gel was shifted to immune-blot polyvinylidene difluoride (PVDF) membrane (1620112, Bio-Rad) at 100V for 1 h using Trans-Blot Turbo Transfer System (Bio-Rad). The following antibodies were used for the detection of EGR-1, TF, PKC βII, ERK1/2, pERK1/2, and RAGE protein: anti- EGR-1 rabbit polyclonal antibody (sc-110, Santa Cruz, USA), anti-TF rabbit polyclonal antibody (sc-210, Santa Cruz, USA), rabbit polyclonal PKC βII antibody (sc-30201, Santa Cruz, USA), monoclonal anti-ERK1/2 antibody produced in mouse (SAB1305560, Sigma Aldrich),anti-phospho-ERK1/2 (pThr202/Tyr204) antibody produced in rabbit (SAB4301578, Sigma Aldrich), and anti-RAGE Antibody produced in mouse (sc-365154, Santa Cruz, USA). The protein levels were normalized to β-Actin. The monoclonal β-Actin antibody was purchased from Santa Cruz, USA. HRP conjugated mouse anti-rabbit IgG antibody (sc-2357, Santa Cruz, USA) and HRP conjugated anti-mouse IgG antibody (A9044, dilution Sigma Aldrich) were used as secondary antibodies. Chemiluminescence signals from the membrane after adding the substrate (#1705060-Clarity Western ECL Substrate, Bio-rad) was detected using Chemi Doc XRS system, Bio-Rad.
Enzyme-linked immunosorbent assay (ELISA)
ICAM-1 levels in cell culture supernatant in all the treatment conditions were measured by commercially available ELISA kit (K7161, BioVision, USA). ELISA was carried out according to the manufacturer’s protocol.
Statistical analysis
Statistical calculations were performed using SPSS software. Clinical data from umbilical cord samples and RT-PCR data of EGR-1 and its targeted pro-inflammatory genes were expressed as mean ± SD (standard deviation). Two-tailed student t-test was used for comparing two individual groups. One-way ANOVA was used to test the significant difference in ICAM-1 levels. p < 0.05 was significant.
Results
Clinical characteristics and anthropometric measures of the study participants are given in Table 1. No significant difference was observed in age, body mass index (BMI), systolic and diastolic blood pressure (BP), and baby birth weight between individuals. There was a significant difference in the fasting blood sugar (FBS) levels and post prandial blood sugar (PPBS) levels in the venous blood of GDM mothers when compared with normal glucose tolerant mothers.
EGR-1 and its target gene TF was elevated in HuVECs isolated from human umbilical vein tissue
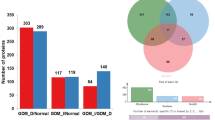
The mRNA and protein expressions of EGR-1 and TF in HuVECs isolated from normal glucose tolerant mothers and GDM mother’s umbilical cord and in HuVECs treated with normal glucose and HG are shown in Fig. 1. In the GDM study group, the EGR-1 mRNA expression was significantly elevated (8.22-fold expression) when compared with normoglycemic mothers (2.06-fold expression) (Fig. 1a). The fold expressions were calculated via comparative CT (ΔΔCT) method and all the values were normalized against 18 s mRNA expression. The TF mRNA levels were elevated in GDM study group (14.32-fold change) when compared with normal glucose tolerant mothers group (1.55-fold change) (Fig. 1b). Consistent with the mRNA expression, the EGR-1 as well as TF protein expression was increased in GDM study group when compared with normal study group (Fig. 1c, d).
mRNA and protein expression of EGR-1 and TF in umbilical vein endothelial cells isolated from normal glucose tolerance (NGT, n = 19) and GDM mothers (n = 20) umbilical cord. a EGR-1 mRNA expression, b TF mRNA expression, c EGR-1 protein, d TF protein expression The data here represented are from three independent experiments. *p < 0.05 significant with HuVECs isolated from NGT mother’s umbilical vein
To validate the above results in-vitro, HuVECs isolated from umbilical cord was treated with normal glucose and HG conditions for 24 h. EGR-1 and TF gene transcripts and protein expressions were preferentially elevated in HG treated HuVECs cells when compared with normal glucose treated cells (Fig. 2a, b, d, e). We observed that ICAM-1 mRNA levels in HG treated cells and sICAM-1 levels in HG treated cell supernatant were increased when compared with normal glucose treated cells (Fig. 2c, f).
Protein and mRNA expression of EGR-1 and its downstream genes TF and ICAM-1 in primary HuVEC treated with high glucose insulin (HG) and normal glucose (NG). a EGR-1 mRNA expression, b TF mRNA expression, c ICAM-1 mRNA expression, d total protein expression of EGR-1 in HG treated cells, e immunoblot of TF, f sICAM-1 levels in cells treated supernatant. The data here represented are from three independent experiments. *p < 0.05 significant with NG treated HuVECs
Silencing of EGR-1 by siRNA decreases TF and ICAM-1 expression
To ascertain whether EGR-1 regulates the expression of TF and ICAM-1 during hyperglycaemia, HuVECs was transfected with EGR-1 targeted siRNA and control scrambled siRNA. We observed a significant decrease in EGR-1 gene as well as protein expression, confirming the knockdown of EGR-1 (Fig. 3a, b). In addition, Q-PCR and western blotting revealed that the transcript levels of TF were decreased in EGR-1 silenced HuVECs when compared with scrambled siRNA as well as HG treated HuVECs (Fig. 3c, d). We also found a significant decrease in ICAM-1 mRNA levels in EGR-1 siRNA treated HuVECs. sICAM-1 levels in EGR-1-siRNA treated media was also decreased when compared with HG and scrambled siRNA treated HuVECs (Fig. 3e, f). Altogether, these findings suggest that TF and ICAM-1 are direct downstream targets of EGR-1 and knockdown of EGR-1 may prevent vascular inflammation.
Expression of EGR-1 and its downstream target gene TF and ICAM-1 after silencing for Egr-1 in primary HuVEC treated with high glucose insulin (HG) and normal glucose (NG). a EGR-1 mRNA expression, b EGR-1 protein expression, c TF mRNA expression, d TF immunoblot, e ICAM-1 mRNA expression, f sICAM-1 levels in cell treated supernatant. Significant mRNA and protein results are represented as fold change and arbitrary units with regard to NG treated cells (*p < 0.05). The data here represented are from three independent experiments
Elevated EGR-1 expression is mediated via PKC βII-ERK1/2 activation
When HuVECs were treated with HG alone (Fig. 4a, b), we observed that there was a significant elevation in the PKC βII and ERK1/2 protein levels. Furthermore, in the cells treated with PKC β inhibitor, there was reduced expression of ERK1/2 (Fig. 4b). Whereas in the cells treated with ERK1/2 inhibitor, the protein expression of PKC βII remained unaltered while ERK1/2 protein expression was decreased (Fig. 4a). These results suggest that ERK1/2 lies downstream of PKC βII. We further examined the expression of EGR-1 when the HuVECs were treated with the PKC or ERK1/2 inhibitors. The experiment showed a predominant decrease in EGR-1 protein levels in both PKC βII and ERK1/2 specific inhibitors treated conditions when compared with cells treated with HG alone (Fig. 4c). Reduction in EGR-1 expression was shown t o decrease the protein expression of TF and sICAM-1 in HG (Fig. 4d, e). These findings demonstrate that HG mediated rise in EGR-1 expression is mediated, in part, through PKC-βII/ERK1/2 axis.
Effects of ruboxistaurin and FR180204 on EGR-1, TF and sICAM-1 expression was analyzed by western blotting and ELISA in HuVECs treated with normal glucose (5.5 mM), high glucose insulin (HG) + DMSO, HG, HG + rubosistaurin and HG + FR180204. a immunoblotting of PKC β II protein, b ERK1/2 immunoblot, c EGR-1 immunoblot, d TF western blotting, e sICAM-1 levels in cell treated supernatant. Significant protein results are represented as arbitrary units with regard to normal glucose treated HuVECs and arbitrary units represented here are average of three different experiments (*p < 0.05)
AGEs mediate hyperglycaemia induced EGR-1 expression
We investigated the activation of EGR-1 via PKC βII and ERK1/2 pathway in HuVECs treated with CML. We found that there was a significant increase in EGR-1 expression in CML and HG treated HuVECs when compared with normal glucose treated HuVECs (Fig. 5a). In addition, we assayed the protein levels of RAGE to further investigate AGE-RAGE interaction in activating EGR-1 during HG condition. As shown in Fig. 5b, the HG and CML treated groups displayed significant increase in RAGE protein expression when compared with normal glucose treated group. To support this finding, we then performed RAGE western blotting analysis in HuVECs isolated from GDM mothers and NGT mothers. We saw elevated levels of RAGE protein in GDM mothers HuVECs alone (Fig. 5c).
Effects of CML on EGR-1, RAGE, TF and sICAM-1, PKC βII and ERK1/2 expression was analyzed by western blotting and ELISA in HuVECs. a EGR-1 immunoblot, b RAGE protein expression in CML treated HuVECs, c RAGE protein expression in HuVECs isolated from umbilical vein tissue, d TF immunoblot, e PKC β II protein expression, f ERK1/2 protein expression, g sICAM-1 levels in cell grown media. Significant mRNA and protein results are represented as fold change and arbitrary units with regard to NG treated cells (*p < 0.05). All the data are representative of three individual experiments
We also found that PKC βII and ERK1/2 was also elevated in CML and HG treated cells (Fig. 5d, e). However, in PKC βII inhibitor treated cells there was a decrease in EGR-1 protein expression even in the presence of CML. These results demonstrates that CML mediates EGR-1 expression via PKC βII mediated pathway during hyperglycaemic and hyperinsulinemia condition. Furthermore, we found that expression of TF and sICAM-1 was low in cells treated with CML + EGR-1 siRNA and CML + PKC β inhibitor (Fig. 5f, g). These results conclude that AGEs trigger increased expression of EGR-1 via RAGE-PKC βII/ERK1/2 pathway.
Discussion
GDM pregnancy is a pathological state caused due to altered insulin sensitivity by placental hormones. Several studies have revealed vascular activation during GDM [38]. It is associated with increased oxidative stress and inflammatory cytokines, which might lead to endothelial dysfunction [39]. Nevertheless, the exact pathological mechanism/factor causing vascular disease in GDM is not clearly understood. Our study unravels the mechanism behind vascular inflammation in GDM. We have demonstrated that EGR-1 up-regulation via AGEs mediates vascular changes that are seen in GDM pathophysiology. The study also unravels the molecular mechanisms associated with endothelial inflammation that is seen during GDM.
EGR-1 is a major transcription factor expressed in various cell types including smooth muscle cells, fibroblast, and leukocytes and endothelial cells, and expressed significantly high in response to oxidative stress, growth factors, hypoxia, inflammation, and vascular injury [40]. There is evidence that EGR-1 overexpression during hyperglycaemic condition accelerates pro-inflammatory genes expressions, such as ICAM-1, TNF-α, TGF β, IL-6, TF [21,22,23,24,25,26,27,28]. Recent studies demonstrated that EGR-1 not only correlates with cell proliferation and differentiation but also contributes to develop atherosclerotic lesions [41, 42]. In addition to this, Karthikkeyan et al., proposed that hyperglycaemia induced EGR-1 expression illustrates an early step in promoting diabetes mediated vascular complications [43]. We have showed a significant elevation of this transcription factor in HuVECs isolated from GDM mothers and in HuVECs when exposed to HG condition in-vitro.
In this study, the downstream targets of EGR-1 such as TF and ICAM-1 mRNA expression were significantly elevated in the HuVECs treated with HG and HuVECs isolated from GDM patients alone. sICAM-1 which is pointed as a predictor for vascular dysfunction in type 2 diabetes [44, 45], was found to be significantly increased in HG treated cells supernatant. We also saw an increase in sICAM-1 levels the plasma isolated from GDM mothers (results under publication). These results suggest the presence of vascular dysfunction during hyperglycaemic condition in GDM. TF is a membrane-bound prothrombotic factor which triggers the extrinsic pathway for the coagulation of blood [46] was also elevated in hyperglycaemic condition in this study, indicates the presence of prothrombiotic environment during hyperglycaemia. There is little evidence, about the role of TF and sICAM-1 in hyperglycaemia [47, 48]. Elżbieta et al., showed an increase in the concentration of sICAM-1 in GDM which characterizes the activation of the endothelial cells [49]. Egr-1 modulates TF and ICAM-1 expressions, in different disease conditions [20, 23, 24, 31, 50].
There is increasing evidence that hyperglycaemia is associated with increased levels of pro-inflammatory molecules (C-reactive protein, TNF-α, IL-6), pro-coagulatory molecules and increased oxidative stress and decrease in anti-inflammatory molecules such as IL-10 and adiponectin, which might illustrate the link between GDM and vascular activation and these, might increase the risk for development of CVD [51,52,53,54,55,56,57,58,59].
It is a well-known fact that diabetes accelerates the formation of AGEs [11, 60]. Our lab has found elevated levels of AGEs in the plasma of GDM mothers compared to the normal mothers during third trimester of pregnancy (data not shown). Hence, we treated the HuVECs cells with AGEs apart from HG condition to study their importance in activation of EGR-1. AGEs are capable of activating various cytokines, transcription factors and inflammation and oxidative stress when it binds to its receptor RAGE [61,62,63]. For example, Lappas et al., in 2007 proposed that glycated bovine serum albumin (BSA) are capable of inducing prostaglandins and pro-inflammatory cytokines in tissue explants of the human placenta [64]. Serum levels of AGEs were found to be increased in pre-eclamptic women placenta [65]. Elevation of PKC isoforms and increased glycation of intra and extracellular proteins (formation of AGEs) are major mechanistic pathways included in the diabetic vascular pathogenesis [66].
AGEs have been reported to activate PKC βII and EGR-1 in various disease models [67,68,69]. According to the study conducted by Chang and his colleagues, RAGE regulates expression of EGR-1 via PKC βII and c-Jun N-terminal kinase (JNK) signaling in murine aortic endothelial cells of RAGE knockout mice [70]. They have also shown that mDia-1 and RAGE interaction activates PKC βII, ERK1/2, and c-JUN signaling pathways which are necessary for hypoxia-mediated EGR-1 expression [71]. Zeng et al. identified that RAGE modifies EGR-1 expression in hepatic ischemia–reperfusion injury [72]. Our study is the first to demonstrate the role of AGEs-RAGE interaction mediated EGR-1 expression in hyperglycaemic similar to GDM.
Based on the cell type, cytokine, growth factor and disease, diverse signaling pathways activates Egr-1, which includes the MAPK/ERK1/2 pathway, PKC mediated ERK1/2 pathway, and ERK1/2 – JNK pathway [73,74,75]. Hasan et al., proposed that glucose-induced EGR-1 expression was intervened via PKC activation [76]. Amidst various signaling molecules, MAPKs and PKC βII mediated pathways have surfaced as mediators of EGR-1 expression in endothelial cells. Hence, we checked the expression of PKC βII in our study. The present study demonstrated the elevated levels of PKC βII and ERK1/2 protein levels under hyperglycaemic condition. By inhibition of PKC β using ruboxistaurin, we found that there was a decrease in ERK1/2 and EGR-1 expression. However, when we inhibited ERK1/2 instead of PKC βII using its inhibitor FR180204, there was no alteration in PKC βII expression but EGR-1 expression. From these results it is understood that PKC βII is an upstream regulator of ERK1/2 and EGR-1. These results authenticate the fact that EGR-1 is activated in endothelial cells of GDM vasculature via PKC βII-ERK1/2 pathway.
In conclusion, we have demonstrated the importance of AGE/EGR-1 axis in GDM pathophysiology. High glucose and/or AGEs mediated RAGE activation may cause changes in fetal endothelial EGR-1 gene expression, which leads to pro-inflammatory state and may have a profound effect on the developing fetus. Understanding of the significance of EGR-1 in GDM pathophysiology needs to be further investigated to understand its role in long-term impact of GDM in chronic diseases.
Change history
15 December 2021
A Correction to this paper has been published: https://doi.org/10.1007/s11010-021-04310-2
References
International Diabetes Federation. IDF Diabetes Atlas, 8th edn. (2017) Brussels, Belgium: International Diabetes Federation. http://www.diabetesatlas.org
Buchanan TA, Xiang A, Kjos SL, Watanabe R (2007) What is gestational diabetes? Diabetes Care 30(Supplement 2):105–111
Seshiah V, Balaji V, Madhuri SB, Sanjeevi CB, Green A (2004) Gestational diabetes mellitus in India. J Assoc Physicians India 52:707–711
Midha T, Nath B, Kumari R, Rao YK, Pandey U (2012) Childhood obesity in India: a meta-analysis. Indian J Pediatr 79(7):945–948
Yajnik CS, Deshmukh US (2008) Maternal nutrition, intrauterine programming and consequential risks in the offspring. Rev Endocr Metab Disord 9(3):203–211
Kleiblova P, Dostalova I, Bartlova M et al (2010) Expression of adipokines and estrogen receptors in adipose tissue and placenta of patients with gestational diabetes mellitus. Mol Cell Endocrinol 314(1):150–156
Kirwan JP, Hauguel-De Mouzon S, Lepercq J et al (2002) TNF-alpha is a predictor of insulin resistance in human pregnancy. Diabetes 51(7):2207–2213
Pantham P, Aye ILMH, Powell TL (2015) Inflammation in maternal obesity and gestational diabetes mellitus. Placenta 36(7):709–715
Atègbo JM, Grissa O, Yessoufou A (2006) Modulation of adipokines and cytokines in gestational diabetes and macrosomia. J Clin Endocrinol Metab 91(10):4137–4143
Morisset AS, Dubé MC, Côté JA, Robitaille J, Weisnagel SJ, Tchernof A (2011) Circulating interleukin-6 concentrations during and after gestational diabetes mellitus. Acta Obstet Gynecol Scand 90(5):524–530
Singh VP, Bali A, Singh N, Jaggi AS (2014) Advanced glycation end products and diabetic complications. Korean J Physiol Pharmacol 18(1):1–14
Ikeda K, Higashi T, Sano H, Jinnouchi Y, Yoshida M, Araki T, Ueda S, Horiuchi S (1996) N (epsilon)-(carboxymethyl)lysine protein adduct is a major immunological epitope in proteins modified with advanced glycation end products of the Maillard reaction. Biochemistry 35:8075–8083
Lieuw-A-Fa MLM, van Hinsbergh VWM, Teerlink T, Barto R, Twisk J, Stehouwer CDA, Schalkwijk CG (2004) Increased levels of Nε-(carboxymethyl)lysine and Nε-(carboxyethyl)lysine in type 1 diabetic patients with impaired renal function: correlation with markers of endothelial dysfunction. Nephrol Dial Transpl 19:631–636
Ghanem AA, Elewa A, Arafa LF (2011) Pentosidine and N-carboxymethyl-lysine: biomarkers for type 2 diabetic retinopathy. Eur J Ophthalmol 21(1):48–54
Wautier MP, Massin P, Guillausseau PJ, Huijberts M, Levy B, Boulanger E, Laloi-Michelin M, Wautier JL (2003) N(carboxymethyl)lysine as a biomarker for microvascular complications in type 2 diabetic patients. Diabetes Metab 29(1):44–52
Ahmed KA, Muniandy S, Ismail IS (2007) Role of Nε-(Carboxymethyl) lysine in the development of ischemic heart disease in Type 2 diabetes mellitus. J Clin Biochem Nutr 41(2):97–105
Yamagishi S (2011) Role of advanced glycation end products (AGEs) and receptor for AGEs (RAGE) in vascular damage in diabetes. Exp Gerontol 46:217–224
Yamagishi S, Imaizumi T (2005) Diabetic vascular complications: pathophysiology, biochemical basis and potential therapeutic strategy. Curr Pharm Des 11:2279–2299
Yan SF, Harja E, Andrassy M, Fujita T, Schmid AM (2009) Protein kinase C β/early growth response-1 pathway: a key player in ischemia, atherosclerosis, and restenosis. J Am Coll Cardiol 48(9):A47–A55
Vedantham S, Thiagarajan D, Ananthakrishnan R et al (2014) Aldose reductase drives hyperacetylation of Egr-1 in hyperglycemia and consequent upregulation of proinflammatory and prothrombotic signals. Diabetes 63(2):761–774
Shi L, Kishore R, McMullen MR, Nagy LE (2002) Lipopolysaccharide stimulation of ERK1/2 increases TNF-alpha production via Egr-1. Am J Physiol Cell Physiol 282(6):1205–1211
Yao J, Mackman N, Thomas S, Edgington, Fan S (1997) Lipopolysaccharide induction of the tumor necrosis factor-a promoter in human monocytic cells. Regulation by Egr-1, c-Jun, and NF-kB transcription factor. J Biol Chem 272(28):17795–17801
Zhang K, Cao J, Dong R, Du J (2013) Early growth response protein 1 promotes restenosis by upregulating intercellular adhesion molecule-1 in vein graft. Oxid Med Cell Longev. https://doi.org/10.1155/2013/432409
Maltzman JS, Carman JA, Monroe JG (1996) Transcriptional regulation of the Icam-1 gene in antigen receptor- and phorbol ester-stimulated B lymphocytes: role for transcription factor EGR1. J Exp Med 83:1747–1759
Cho SJ, Kang MJ, Homer RJ et al (2006) Role of early growth response-1 (Egr-1) in interleukin-13-induced inflammation and remodeling. J Biol Chem 281:8161–8168
Pawlinski R, Pedersen B, Kehrle B, Aird WC, Frank RD, Guha M, Mackman N (2003) Regulation of tissue factor and inflammatory mediators by Egr-1 in a mouse endotoxemia model. Blood 101(10):3940–3947
Meng Y, Chen C, Tian C, Du J, Li H (2015) Angiotensin II-induced Egr-1 expression is suppressed by peroxisome proliferator-activated receptor-γ ligand 15d-PGJ2 in macrophages. Cell Physiol Biochem 35:689–698
Dickinson MG, Bartelds B, Molema G et al (2011) Egr-1 expression during neointimal development in flow-associated pulmonary hypertension. Am J Pathol 179(5):2199–2209
Liu C, Yao J, Mercola D, Adamson E (2000) The transcription factor EGR-1 directly transactivates the fibronectin gene and enhances attachment of human glioblastoma cell line U251. J Biol Chem 275:20315–20323
Liao H, Hyman MC, Lawrence DA, Pinsky DJ (2006) Molecular regulation of the PAI-1 gene by hypoxia: contributions of Egr-1, HIF-1alpha, and C/EBP alpha. FASEB J 21(3):935–949
Yan SF, Zou YS, Gao Y et al (1998) Tissue factor transcription driven by Egr-1 is a critical mechanism of murine pulmonary fibrin deposition in hypoxia. Proc Natl Acad Sci USA 95:8298–8303
Yan SF, Lu J, Zou YS et al (1999) Hypoxia-associated induction of early growth response-1 gene expression. J Biol Chem 274:15030–15040
Lo L, Cheng J, Chiu J, Wung B, Liu Y, Wand DL (2001) Endothelial exposure to hypoxia induces Egr-1 expression involving PKCa-mediated Ras/Raf-1/ERK1/2 pathway. J Cellu Physiol 188:304–312
McCaffrey TA, Fu C, Du B et al (2000) High-level expression of Egr-1 and Egr-1–inducible genes in mouse and human atherosclerosis. J Clin Invest 105(5):653–662
Wang X, Athayde N, Trudinger B (2006) Egr-1 transcription activation exists in placental endothelium when vascular disease is present. Int J Obst Gynaec 683–687
Liao H, He H, Chen Y, Zeng F, Huang J, Wu L, Chen Y (2014) Effects of long-term serial cell passaging on cell spreading, migration, and cell-surface ultrastructures of cultured vascular endothelial cells. Cytotechnology 66:229–238
Nigris VD, Pujadas G, Sala LL, Testa R, Genovese S, Ceriello (2015) A short-term high glucose exposure impairs insulin signaling in endothelial cells. Cardiovasc Diabetol 14:114
Leiva A, Pardo F, Ramírez MA, Farías M, Casanello P, Sobrevia L (2011) Fetoplacental vascular endothelial dysfunction as an early phenomenon in the programming of human adult diseases in subjects born from gestational diabetes mellitus or obesity in pregnancy. Exp Diabetes Res. https://doi.org/10.1155/2011/349286
González M, Muñoz E, Puebla C et al (2011) Maternal and fetal metabolic dysfunction in pregnancy diseases associated with vascular oxidative and nitrative stress. In: Matata BM, Elahi M (eds) The molecular basis for origin of fetal congenital abnormalities and maternal health: an overview of association with oxidative stress. Bentham USA. Chapter 8, pp 98–115
Silverman ES, Collins T (1999) Pathways of Egr-1-mediated gene transcription in vascular biology. Am J Pathol 154:665–670
Gururajan M, Simmons A, Dasu T, Spear BT, Calulot C et al (2008) Early growth response regulate B cell development, proliferation, and immune response. J Immunol 181:4590–4602
Du B, Fu C, Kent KC (2000) Elevated Egr-1 in human atherosclerotic cells transcriptionally represses the transforming growth factor-β type II receptor. J Biol Chem 275:39039–39047
Karthikkeyan G, Nagaraj NR, Seeneevasan A, Natarajan SK, Vedantham S, Coral K (2018) Hyperglycemia induced early growth response-1 regulates vascular dysfunction in human retinal endothelial cells. Microvasc Res 117:37–43
Kulkarni H, Mamtani M, Peralta J (2016) Soluble forms of intercellular and vascular cell adhesion molecules independently predict progression to type 2 diabetes in Mexican American families. PLoS ONE 11(3):0151177. https://doi.org/10.1371/journal.pone.0151177
Blann AD, McCollum CN (1998) Circulating ICAM-1 in peripheral arterial disease as a predictor of adverse events. The Lancet 351:1135
Mackman N (2004) Role of tissue factor in hemostasis, thrombosis, and vascular development. Arterioscler Thromb Vasc Biol 24:1015–1022
Boganov VY, Osterund B (2010) Cardiovascular complications of diabetes mellitus: the tissue factor perspective. Thromb Res 125:112–118
Avci1 E, Uzeli S (2016) The role of adhesion molecules and cytokines in patients with diabetic nephropathy. Biomed Res Special Issue: S343-S348
Elżbieta P, Mierzyński R, Szymula D, Bożena L, Oleszczuk L (2016) Intercellular adhesion molecule and endogenous NOS inhibitor: asymmetric dimethylarginine in pregnant women with gestational diabetes mellitus. J Diabetes Res. https://doi.org/10.1155/2016/1342643
Bavendiek U, Libby P, Kilbride M, Reynolds R, Mackman N, Schönbeck U (2002) Induction of tissue factor expression in human endothelial cells by CD40 ligand is mediated via activator protein 1, nuclear factor κB, and Egr-1. J Biol Chem 277:25032–25039
Fasshauer M, Blüher M, Stumvoll M (2014) Adipokines in gestational diabetes. Lancet Diabetes Endocrinol 2:488–499
Lowe LP, Metzger BE, Lowe WL, Dyer AR, McDade TW, McIntyre HD (2010) Inflammatory mediators and glucose in pregnancy: results from a subset of the hyperglycemia and adverse pregnancy outcome (HAPO) study. J Clin Endocrinol Metab 95:5427–5434
Boden G, Vaidyula VR, Homko C, Cheung P, Rao AK (2007) Circulating tissue factor procoagulant activity and thrombin generation in patients with type 2 diabetes: effects of insulin and glucose. J Clin Endocrinol Metab 92:4352–4358
Ceriello A (1993) Coagulation activation in diabetes mellitus: the role of hyperglycaemia and therapeutic prospects. Diabetologia 36(11):1119–1125
Stegenga ME, van der Crabben SN, Levi M, de Vos AF, Tanck MW, Sauerwein HP, van der Poll T (2006) Hyperglycemia stimulates coagulation, whereas hyperinsulinemia impairs fibrinolysis in healthy humans. Diabetes 55(6):1807–1812
Lappas M, Hiden U, Desoye G, Froehlich J, Hauguel-de Mouzon S, Jawerbaum A (2011) The role of oxidative stress in the pathophysiology of gestational diabetes mellitus. Antioxid Redox Signal 15(12):3061–3100
Monnier L, Mas E, Ginet C, Michel F, Villon L, Cristol JP, Colette C (2006) Activation of oxidative stress by acute glucose fluctuations compared with sustained chronic hyperglycemia in patients with type 2 diabetes. JAMA 295(14):1681–1687
Yaghini N, Mahmoodi M, Asadikaram R, Hassanshahi H, Khoramdelazad H, Arababadi MK (2011) Serum levels of interleukin 10 (IL-10) in patients with type 2 diabetes. Iran Red Crescent Med J 13(10):752
Lindberg S, Jensen JS, Pedersen SH, Galatius S, Frystyk J, Flyvbjerg A, Bjerre M, Mogelvang R (2014) Low adiponectin levels and increased risk of type 2 diabetes in patients with myocardial infarction. Diabetes Care 37(11):3003–3008
Basta G, Schmidt AM, Caterina R (2004) Advanced glycation end products and vascular inflammation: implications for accelerated atherosclerosis in diabetes. Cardiovasc Res 63:582–592
Yang K, Wang XQ, He YS, Lu L, Chen QJ, Liu J, Shen AT (2010) Advanced glycation end products induce chemokine/cytokine production via activation of p38 pathway and inhibit proliferation and migration of bone marrow mesenchymal stem cells. Cardiovasc Diabetol 9:66
Ramasamy R, Yan SF, Schmidt AM (2011) Receptor for AGE (RAGE): signaling mechanisms in the pathogenesis of diabetes and its complications. Ann N Y Acad Sci 1243:88–102
Yamamoto Y, Yamamoto H (2011) Receptor for advanced glycation end-products-mediated inflammation and diabetic vascular complications. J Diabetes Investig 2(3):155–157
Lappas M, Permezel M, Rice GE (2007) Advanced glycation endproducts mediate pro-inflammatory actions in human gestational tissues via nuclear factor-kappaB and extracellular signal-regulated kinase ½. J Endocrinol 193(2):269–277
Chekir C, Nakatsuka M, Noguchi S, Konishi H, Kamada Y, Sasaki A, Hao L, Hiramatsu Y (2006) Accumulation of advanced glycation end products in women with preeclampsia: possible involvement of placental oxidative and nitrative stress. Placenta 27(2–3):225–233
Scivittaro V, Ganz MB, Weiss MF (2000) AGEs induce oxidative stress and activate protein kinase C-βII in neonatal mesangial cells. Am J Physiol-Renal Physiol 278:676–683
Harja E, Hudson BI, Zou YS, Lu Y, Schmidt AM, Yan SF (2005) PKC beta/Egr-1: a central axis in atherosclerosis. FASEB J 19:387.20
Rong J, Qiu HX, Wang SP (2000) Advanced glycosylation end products, protein kinase C and renal alterations in diabetic rats. Chin Med J (Engl) 113(12):1087–1091
Yoon YW, Kang TS, Lee BK et al (2008) Pathobiological role of advanced glycation endproducts via mitogen-activated protein kinase dependent pathway in the diabetic vasculopathy. Exp Mol Med 40(4):398–406
Chang JS, Wendt T, Qu W, Kong L, Zou YS, Schmidt AM, Yan SF (2008) Oxygen deprivation triggers upregulation of early growth response-1 by the receptor for advanced glycation end products. Circ Res 102(8):905–913
Xu Y, Toure F, Qu W et al (2010) Advanced glycation end product (AGE)-receptor for AGE (RAGE) signaling and up-regulation of Egr-1 in hypoxic macrophages. J Biol Chem 285(30):23233–23240
Zeng S, Dun H, Ippagunta N, Rosario R, Zhang QY, Lefkowitch J, Yan SF, Schmidt AM, Emond JC (2009) Receptor for advanced glycation end product (RAGE)-dependent modulation of early growth response-1 in hepatic ischemia/reperfusion injury. J Hepatol 50(5):929–936
Yu X, Shen N, Zhang ML, Pan FY, Wang C, Jia WP, Liu C, Gao Q, Gao X, Xue B, Li CJ (2011) Egr-1 decreases adipocyte insulin sensitivity by tilting PI3K/Akt and MAPK signal balance in mice. EMBO J 30:3754–3765
Fujita T, Asai T, Andrassy M, Stern DM, Pinsky DJ, Zou YS, Okada M, Naka Y, Schmidt AM, Yan SF (2004) PKC beta regulates ischemia/reperfusion injury in the lung. J Clin Invest 113(11):1615–1623
Yoon YJ, Kim DK, Yoon CM, Park J, Kim YK, Roh TY, Gho YS (2014) Egr-1 activation by cancer-derived extracellular vesicles promotes endothelial cell migration via ERK1/2 and JNK signaling pathways. PLoS ONE 9(12):115170
Hasan RN, Phukan S, Harada S (2003) Differential regulation of early growth response gene-1 expression by insulin and glucose in vascular endothelial cells. Arterioscler Thromb Vasc Biol 23:988–993
Acknowledgements
We would like to thank our project (SB/FT/LS-432/2012) funding agency - Department of Science and Technology India and TRR fund from SASTRA University for supporting this research. We thank all the nursing staff, physician assistants for helping us with the sample collection as well as for providing patient’s clinical details.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Rajaraman, B., Ramadas, N., Krishnasamy, S. et al. Hyperglycaemia cause vascular inflammation through advanced glycation end products/early growth response-1 axis in gestational diabetes mellitus. Mol Cell Biochem 456, 179–190 (2019). https://doi.org/10.1007/s11010-019-03503-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-019-03503-0