Abstract
The aim of this study was to investigate protective effects of the lipophilic vitamin C derivative, 6-o-palmitoylascorbate (PlmtVC), against X-ray radiation-induced damages including cell death, DNA double-strand breaks (DSBs), lipid peroxidation, and protein carbonylation in human lymphocytes HEV0082, and the stability of PlmtVC under cell-cultured or cell-free condition. Irradiation with X-ray (1.5 Gy) diminished the cell viability and induced apoptosis, both of which were protected by pre-irradiational administration with PlmtVC. Gamma-H2A.X foci as a hallmark of DSBs were markedly enhanced in the irradiated cells. PlmtVC prevented X-ray-induced DSBs more appreciably than l-ascorbic acid (l-AA). Intracellular ROS production, lipid peroxidation, and protein carbonylation in HEV0082 cells were increased by X-ray at 1.5 Gy, all of which were significantly repressed by PlmtVC. PlmtVC also elevated endogenous reduced glutathione (GSH) in HEV0082 cells, and prevented X-ray-induced GSH depletion that are more appreciably over l-AA. Thus, PlmtVC prevents X-ray-induced cell death through its antioxidative activity. Stability tests showed that after being kept under physiological conditions (pH 7.4, 37 °C) for 14 days, vitamin C residual rates in PlmtVC solutions (62.2–82.0 %) were significantly higher than those in l-AA solutions (20.5–28.7 %). When PlmtVC or l-AA was added to HEV0082 lymphocytes, intracellular vitamin C in l-AA-treated cells was not detectable after 24 h, whereas PlmtVC-treated cells could keep a high level of intracellular vitamin C, suggesting an excellent stability of PlmtVC. Thus, X-ray-induced diverse harmful effects could be prevented by PlmtVC, which was suggested to ensue intrinsically from the persistent enrichment of intracellular vitamin C, resulting in relief to X-ray-caused oxidative stress.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ionizing radiation (IR) induces various lesions in mammalian cells that result in a series of overlapping consequences including growth arrest, cell death, and malignant transformation. IR can react with critical biomolecules in cells, such as lipids, proteins, and DNA, through direct and indirect actions of radiation [1–5]. For radiations with low linear energy transfer (LET) such as X-ray or gamma particles, cellular molecules are mainly damaged by indirect action through hydroxyl (•OH) radicals, which are produced by the radiolysis of water (the main component of cells) [6, 7]. IR-induced cellular lesions include DNA double-strand breaks (DSBs, breaks in the phosphodiester backbone of both strands of the DNA) [8], lipid peroxidation (oxidative breakdown of the polyunsaturated fatty acids that are part of the cell and subcellular membranes) [9, 10], and protein carbonylation (a reaction of hydroxyl radicals with accessible side chains of certain amino acids) [11, 12]. These lesions independently or compliantly cause cell death and malignant transformation [13]. Among these lesions, DSBs have been considered to be the most deleterious and major actor responsible for apoptotic cell death. If misrepaired or unrepaired, DSBs may also lead to mutations and cancer in mammals [14, 15]. As another important lesion induced by IR, lipid peroxidation not only disintegrates the cell membrane but also reacts with DNA and proteins [16]. Additionally, an IR-induced irreversible oxidative damage, protein carbonylation plays a major role in cell dysfunction, the delayed lethality (especially across generations), and bystander effect [17].
Bdelloid rotifers, the super radioresistant invertebrates, have the extreme capacity for scavenging reactive molecular species generated by IR, suggesting that antioxidative ability of cells is very important for radioprotection [18]. Exposure of cells to ionizing radiation also results in depletion of intracellular antioxidant stores, prominently a reduced form of glutathione (GSH). Enhancement of endogenous GSH and exogenous administration of antioxidant vitamins (A, C, and E) has shown some protective effects against IR-induced cell death [19–22]. In human, vitamin C scavenges free radicals, thereby reducing risk of oxidative stress-involved diseases, such as cancer, arteriosclerosis, cardiovascular, and inflammatory diseases [23]. Administration of l-ascorbic acid (water-splible vitamin C) at higher doses decreases mutagens-induced genomic toxicity such as chromosomal aberrations, micronuclei, and DSBs [24]. A recent report showed that l-ascorbic acid promotes the chemical repair of gamma-radiation-induced DNA lesions [25].
However, l-ascorbic acid is chemically active, labile, and unstable; degradation is markedly increased under physiological conditions (pH 7.4, 37 °C). In biological systems, l-ascorbic acid can be rapidly oxidized reversibly to dehydroascrobic acid (DHA) at the first oxidation, and then irreversibly to 2,3-diketogulonic acid (2,3-DKG) at the second one together with loss of the antioxidant property. These degradation products react with proteins resulting in structurally deleterious, non-enzymatic modifications of proteins that might contribute to the onset of a variety of diseases including senile cataract, diabetes, and Alzheimer’s disease [26]. Therefore, it become an essential issue to search stable l-ascorbic acid derivatives that are able to protect cells from oxidative stress induced by IR or other mutagens.
l-Ascorbyl 6-palmitate (also named ascorbyl palmitate, or 6-palmitoyl-l-ascorbic acid) is a fat-soluble acyl derivative of ascorbate which combined ascorbic acid and palmitic acid. The mono-palmitoyl form of PlmtVC is advantageous over dipalmitoyl form which is difficult to be dispersed because of the marked hydrophobicity, from a viewpoint of biomembrane permeability. In contrast, its mono-stearoyl form, being shorter in molecular-chain length by two carbon atoms, is inferior to the mono-palmitoyl form, suggesting that PlmtVC has an adequate molecular hydrophilicity-lipophilicity balance. On the other hand, a mere equimolar mixture of free ascorbic acid and free palmitic acid or palmitoyl methylester is almost ineffective, showing the necessity for a covalent bond joining between the ascorbyl moiety and the palmitoyl moiety. Thus, PlmtVC is an excellent lipophlic vitamin C derivative after choice among diverse acylascorbate derivatives. When PlmtVC is administered orally, the palmitic acid is separated by hydrolysis due to cellular esterase in the stomach, and the now active antioxidant (ascorbic acid) is distributed to tissue stores. Previous reports showed that PlmtVC could protect cells and cellular membranes from oxidative damage [27–29].
Here, we investigated cytoprotective effects of PlmtVC on IR-induced cell death, DNA damage, lipid peroxidation, and protein carbonylation in human lymphocytes. We also compared the stabilities of PlmtVC with l-AA under both cellular and cell-free conditions.
Materials and methods
Materials
6-o-Palmitoylascorbate (Ascorbyl palmitate, PlmtVC) was purchased from DSM Nutritional Products Ltd., Germany. General chemicals were purchased from Sigma-Aldrich (Tokyo), tissue culture medium from Life Technologies (Tokyo), and tissue culture plastics from Corning Costar Ltd. (NY, USA), unless otherwise stated.
Cell culture
HEV0082 cells were purchased from Riken Bio Resource Center [30]. Cells were maintained in RPMI 1640 medium (Gibco) supplemented with 20 % fetal bovine serum (FBS) (JRH Biosciences, Lenexa, KS, USA) and 1 % Gibco® GlutaMAX™ Supplement (Life Technologies) in a 5 % CO2 atmosphere. Cells were passaged twice a week.
Alamar blue assay
Cell viability was measured with AlamarBlue® (Life Technologies) according the standard protocol. HEV0082 cells were seeded into the maintenance medium in 96-well microplates at a density of 5,000 cells/well. After treatment or X-ray radiation, cells were incubated for 4 h with the addition of 10 vol% AlamarBlue®. The AlamarBlue® reduction by the cells was expressed as fluorescence intensity units and was measured on a fluorescence microplate reader (SH-9000Lab, HITACHI, Tokyo) with excitation at 530 nm and emission 585 nm.
X-ray radiation
The cells were pretreated with different concentrations of l-AA or PlmtVC at 37 °C in a humidified atmosphere of 5 % CO2 for 3 h and then radiated with X-ray. X-ray radiation was performed using an apparatus generator (MBR-1520R-3, HITACHI) operating at 100 kV, 20 mA with a filter (aluminum 0.3 mm/copper 0.2 mm) at a dose rate of 0.35 Gy/min at room temperature. The distance of the radiation stage is about 455 mm.
Analysis of apoptosis
Early-stage apoptosis determination
Detection of cells destined to apoptosis was performed with CellEvent™ Caspase-3/7 Green ReadyProbes™ Reagent (Life Technologies) according to the manufacturer’s recommended protocol. Activation of caspase-3 in cells was analyzed with the Tali® Image Cytometer (Life Technologies) and observed with a confocal laser scanning microscope (LSM 700, Carl Zeiss Microscopy Co., Ltd.). To avoid the situation that cell volume-dependent signal density influences Tali cytometric analysis, we excluded cells with sizes below 8 and over 9 μm (similar to the rest experiments).
Late-stage apoptosis determination
Late apoptosis was determined by the terminal deoxynucleotidyl transferase-mediated deoxyuridine triphosphate-biotin nick-end labeling (TUNEL) assay using the apoptosis detection TUNEL kit (TakaraBio, Shiga) according to the manufacturer’s recommended protocol. The apoptotic cells were calculated with a Guava EasyCyte flow cytometer (Millipore). Green fluorescence of 5,000 cells was detected by gating and acquiring the cell population. Data are expressed as the percentage of positive cells corresponding to the mean fluorescence intensity in each experiment. Cell images were taken with a laser scanner microscope (LSM).
Determination of gamma-H2A.X foci formation
Gamma-H2A.X foci formation was detected by immunofluorescence staining using the Tali® Image Cytometer. Immunofluorescence staining was performed with a Histostain™ kit (Life Technologies) according to manufacturer’s protocol. Briefly, HEV0082 cells were gently fixed with 90 % methanol at −10 °C. Cells were incubated with 0.5 % (w/v) BSA/PBS (–) for 10 min to suppress non-specific binding of IgG, and then incubated for 60 min with saturated levels of anti-gamma H2A.X (phospho S139) antibody (Abcam, ab26350). After washing with 0.5 % (w/v) BSA/PBS (–) for three times, cells were then reacted with a fluorochrome-conjugated secondary antibody (Life Technologies, A11001) diluted to 2 µg/ml in PBS with 0.5 % (w/v) BSA/PBS (–). Expression of gamma-H2A.X in HEV0082 cells was then analyzed on the Tali® Image Cytometer. The nuclei were stained with propidium iodide (PI). Images were taken by LSM.
Cellular ROS detection
At 30 min after X-ray, cellular ROS generation was detected with the CellROX® Variety Pack (including CellROX® Green, Deep Red and Orange Reagent) (Life Technologies) according to the manufacturer’s recommended protocol. ROS production in cells was analyzed with the Tali® Image Cytometer and observed by LSM.
Detection of lipid peroxidation
At 2 h after X-ray, lipid peroxidation in HEV0082 cells was detected with the Image-iT® Lipid Peroxidation Kit (Life Technologies) according to the manufacturer’s recommended protocol and then analyzed with the Tali® Image Cytometer. Cell images were observed by LSM.
Protein carbonyl colorimetric assay
Protein quantification was performed with Protein Assay Rapid kit (Wako, 293-56101) by the attached protocol. Protein carbonylation was detected using a protein carbonyl colorimetric assay kit (Cayman Chemical, 10005020) according to the manufacturer’s recommended protocol. After the final step of the assay, the absorbance was measured at a wavelength of 370 nm using a microplate reader (SH-9000Lab, HITACHI).
Glutathione detection
Intracellular reduced glutachione (GSH) was detected with ThiolTracker™ Violet (Life Technologies) according the standard protocol. Briefly, HEV0082 cells (5 × 105 cells) were harvested after final treatment by centrifugation and then washed two times with Dulbecco’s phosphate buffered saline, containing Ca++ and Mg++, glucose, and sodium pyruvate (D-PBS with C/M). Cells were then reacted with the ThiolTracker™ Violet dye working solution (20 μM) for 30 min at 37 °C. After the reaction was stopped, cells were fixed with 4 % formaldehyde solution. Intracellular fluorescence was measured using a fluorescence microplate reader (SH-9000Lab, HITACHI, Tokyo) with excitation at 404 nm and emission 526 nm.
Ascorbate assays
o-Phenylenediamine (OPDA) ascorbate assay
For cell-free experiments, vitamin C determination is performed by an o-phenylenediamine (OPDA)-mediated enzymatic procedure with an ascorbate assay kit (Cayman Chemical, 700420) according to the manufacturer’s recommended protocol. PlmtVC or l-AA was solved in 1 N NaOH solution at first, and immediately neutralized with 5.4 % meta-phosphoric acid until the pH reaches 7.4. The solutions were kept in tubes without lids and exposed in a humidified atmosphere at 37 °C until the assay was performed. After the final step of the assay, the fluorescence of end products was analyzed using an excitation wavelength of 340 nm and an emission wavelength of 420 nm with a microplate reader (SH-9000Lab, HITACHI).
2,4-Dinitrophenylhydrazine (DNPH) ascorbate assay
DNPH ascorbic acid assay was used for the determination of cellular vitamin C with a vitamin C detection kit (Shima Laboratories Co. Ltd.). After incubated with PlmtVC or l-AA, about 1 × 107 cells were collected and homogenized on ice in 0.5 ml of cold 5.4 % phosphoric acid solution. After the final step of the assay, the absorbance of end products was measured at a wavelength of 530 nm using a microplate reader (SH-9000Lab, HITACHI).
Statistical analysis
All data, expressed as mean ± standard deviation, were processed statistically by SPSS11.5 for Windows. One-way ANOVA followed by LSD test (equal variances assumed) or Dunnett’s T3 test (equal variances not assumed) was used for statistical analysis. The differences of the data were considered especially when p < 0.05.
Results
Cytotoxicity of PlmtVC in human lymphocytes HEV0082
Before performing the series tests of radioprotection of PlmtVC, we evaluated the cell viability of HEV0082 cells, to which PlmtVC or l-AA was administered for 48, 72, and 96 h. Previous epidemiological and clinical long-term studies showed that protective plasma vitamin C concentration for the minimum risk of free-radical-related diseases is higher than 50 μM [31]. The vitamin C plasma level at about 100 μM showed significant prevention on lipid peroxidation in plasma as well as in lymphocytes in an elderly population [32]. Therefore, we equated cytotoxicity of PlmtVC below 200 μM. As shown in Fig. 1, after cultured in medium containing PlmtVC or l-AA of diverse concentrations, it was found that the survival rates of HEV0082 cells were not decreased even at a high concentration of 200 μM after 48, 72, and 96 h. The left panel of Fig. 1 showed that cell viability was significantly increased in PlmtVC-treated cells at concentrations of 50, 75, 100, and 150 μM after 48 h of cultivation, suggesting that PlmtVC could stimulate cell growth under certain conditions. This finding suggests that PlmtVC has no cytotoxicity to human lymphocytes as well as l-AA even at higher concentrations after a long-term treatment. Therefore, as an antioxidant, PlmtVC is as safe as l-AA.
Effect of PlmtVC on cell proliferation in human lymphocytes HEV0082. HEV0082 cells were seeded into 96-well plates at a density of 3,200 cells/well. PlmtVC or l-ascorbic acid was added in the medium at the same time. After 48, 72, and 96 h of incubation, cell viability was measured by Alamar Blue assay. The data showed that PlmtVC had stimulative effects on cell growth at 48 h after incubation. PlmtVC did not affect cell viability after 72- and 96-h incubation even at high concentrations. Data represent the mean ± SD of three independent experiments. PVC PlmtVC, LAA l-ascorbic acid (identical wording for the rest). **p < 0.01, ***p < 0.001 vs. 0
Preventive effects of PlmtVC on X-ray-induced death and apoptosis in human lymphocytes
To examine the cytoprotective effect of PlmtVC, at 72 h after X-ray irradiation, we determined cell viabilities of HEV0082 cells which were pre-administered with PlmtVC at different concentrations. Because PlmtVC has stimulative effect on cell growth at 48 h post administration as shown in Fig. 1, we choose 72 h for the test. We first examined a 50 % lethal dose (LD50) of X-ray on HEV0082 cells. As shown in Fig. 2a, cell viability was decreased in a dose-dependent manner. LD50 is about 1.536 Gy according to the linear equation. Therefore, we selected 1.5 Gy for the rest experiments. Figure 2b shows that X-ray (1.5 Gy) decreased cell viability to about 50 %. When the cells were pretreated with PlmtVC at 30, 60, 120, and 200 μM, the cell viability was significantly increased. l-AA showed significant protection only at doses as high as 60 and 120 μM.
Protection of PlmtVC on X-ray-induced cell death in HEV0082 cells. a LD50 of X-ray on HEV0082 cells. HEV0082 cells were seeded into 4-well plates at a density 5.0 × 104 cells/well. After 3 h of cultivation, cells were irradiated with X-ray at gradual doses of 0, 0.1, 0.5, 1.0, and 2.0 Gy. After further cultivated for 72 h, cell viability was measured by Alamar Blue assay. According to the linear equation, LD50 of X-ray is about 1.536 Gy. b PlmtVC or l-ascorbic acid was added in the medium. After 3 h of treatment, cells were irradiated with X-ray (1.5 Gy) and further cultivated for 72 h. Cell viability was measured by Alamar Blue assay. Data represent the mean ± SD of three independent experiments. NC, sham-irradiation; PC, X-ray without treatment (identical wording for the rest). The viability of irradiated cells was decreased over 50 % of sham-irradiated control cells. Pretreatment of LAA or PVC at high concentrations protected cells from X-ray-induced cell death as seen from increased cell viability in LAA or PVC pretreated samples. **p < 0.01, ***p < 0.001 versus PC
Since both PlmtVC and l-AA have cytoprotective effects against X-ray in common at concentrations of 60 and 120 μM, we chose 120 μM to compare their radioprotection for the rest experiments. We then examined repressive effects of PlmtVC and l-AA on X-ray-induced early- and late-stage apoptosis in HEV0082 cells. The apoptosis-associated molecule, caspase-3 is considered as an early indicator of apoptosis when being activated. As shown in Fig. 3a, at 12 h after irradiated with X-ray, caspase 3 was activated in HEV0082 cell without treatment (the middle panel). Pretreatment with PlmtVC (120 μM) markedly inhibited X-ray-induced caspase 3 activation (the right panel). Tali cytometric analysis showed that PlmtVC significantly decreased X-ray-caused early apoptosis (p < 0.01), whereas l-AA did not show a significant inhibitory effect (Fig. 3b). TUNEL assay detects DNA fragmentation that results from apoptotic signaling cascades. Flow cytometric analysis presented that at 24 h after X-ray, about 90 % cells underwent late apoptosis (Fig. 3c, the middle panel) which was reduced to approximately 45 % by l-AA and 40 % by PlmtVC, respectively (Fig. 3d).
Protection of PlmtVC on X-ray-induced apoptosis in HEV0082 cells. HEV0082 cells were seeded into 4-well plates and treated with PlmtVC (120 μM) or l-ascorbic acid (120 μM) as same as we described in Fig. 2. After treatment, cells were irradiated with X-ray (1.5 Gy) and further cultivated for 12 h. Early apoptosis was detected with CellEvent™ Caspase 3/7 Green ReadyProbes® reagent. Sham-irradiated cells have minimal fluorescence, while irradiated cells without vitamin C treatment have a significant increase in fluorescence in the cytoplasm (shown in green) indicating early apoptosis. LAA or PVC pretreatment decreases the early apoptotic cells as seen from decreased green signals in LAA or PVC pretreated samples. Nuclei were stained with Hoechest 33342 (blue). Cell images were taken by LSM (a) and analyzed with the Tali® Image Cytometer (b). Late apoptotic cells were stained by TUNEL assay and counted by flow cytometry 24 h after irradiation. Typical FCM histograms represent one of three independent experiments (c, d). Data represent the mean ± SD of three independent experiments. The data showed that about 90 % irradiated cells underwent late apoptosis that was prevented by LAA or PVC pretreatment **p < 0.01; ***p < 0.001 versus PC. (Color figure online)
These results suggest that PlmtVC could protect HEV0082 lymphocytes from X-ray-induced cell death and apoptosis. PlmtVC showed better effect than l-AA.
Inhibition of PlmtVC on X-ray-induced DNA damage in human lymphocytes
We then examined inhibitory effect of PlmtVC on X-ray-induced DSB by gamma-H2A.X antibody-based immunostaining. We observed that gamma-H2A.X foci occurred in irradiated HEV0082 cells even at a low dose of 0.1 Gy and increased in a dose-dependent manner (data not shown). As shown in Fig. 4, compared to the sham-ray control, cells without treatment formed higher amounts of DSB. Either l-AA or PlmtVC obviously reduced DSBs at a concentration of 120 μM (p < 0.001). The inhibition of PlmtVC on DSB was significantly better than l-AA (p < 0.001). The data indicate that PlmtVC could prevent X-ray-induced DNA damages.
Effect of PlmtVC on X-ray-induced DNA double-strand breaks in HEV0082 cells. HEV0082 cells (3 × 105/dish) were seeded into 35-mm dishes. PlmtVC (120 μM) or l-ascorbic acid (120 μM) was added in the medium at the same time. After 3 h of cultivation, cells were irradiated with X-ray (1.5 Gy). 30 min later, cells were fixed with 90 % ice-cold methanol and stained with anti-gamma-H2A.X antibody. Nuclei were stained by propidium iodide (PI). Cell images were taken by LSM (a) and analyzed with the Tali® Image Cytometer (b). Green gamma-H2A.X; Red nuclei (PI). Gamma-H2A.X foci (green spots) indicate DNA double-strand breaks. After irradiation, HEV0082 cells generated higher amounts of gamma-H2A.X foci than that in the sham-ray control. Either l-ascorbic acid or PlmtVC reduced DSBs at a concentration of 120 μM as seen the decreased green spots. Data represent the mean ± SD of three independent experiments. ***p < 0.001 versus PC; ### p < 0.001 versus LAA. (Color figure online)
Scavenging effect of PlmtVC on X-ray-induced intracellular ROS generation in human lymphocytes
To examine whether PlmtVC has an antioxidant activity at degrees similar to those of l-AA, we quantified the intracellular ROS after X-ray. We have tested CellROX® Green, Deep red, and Orange Reagents that were purchased from Life Technologies. According to Tali cytometric analysis, there were no differences between the sham-irradiated control and the irradiated cells using CellROX® Green and Deep red Reagents. Only the Orange Reagent was able to detect intracellular ROS that generated by X-ray. We then used the Orange Reagent to perform the experiment. As shown in Fig. 5a, at 30 min after X-ray, significant accumulation of intracellular ROS in non-pretreated cells was observed. In the cells pretreated with PlmtVC at 120 μM, the ROS level was markedly reduced. Cytometric analysis showed that either PlmtVC or l-AA significantly inhibited intracellular ROS production (p < 0.001) (Fig. 5b). The data suggest that PlmtVC and l-AA have equal ROS scavenging ability.
Effect of PlmtVC on X-ray-induced generation of cellular ROS in HEV0082 cells. HEV0082 cells (3 × 105 cells/dish) were seeded into 35-mm dishes and treated with PlmtVC (120 μM) or l-acsorbic acid (120 μM) as same as we described in Fig. 4. After 3 h of cultivation, cells were irradiated with X-ray (1.5 Gy). 30 min later, cellular ROS were detected by the CellROX® Orange Reagent. Nuclei were stained with Hoechest 33342. Cell images were taken by LSM (a) and analyzed with the Tali® Image Cytometer (b). Orange ROS products; blue nuclei. After irradiation, HEV0082 cells generated higher amounts of ROS than that in the sham-ray control. Either l-ascorbic acid or PlmtVC reduced cellular ROS at a concentration of 120 μM. Typical histograms represent one of three independent experiments. Data represent the mean ± SD of three independent experiments. ***p < 0.001 versus PC. Scale bar = 50 μm. (Color figure online)
Inhibitory effects of PlmtVC on X-ray-induced lipid peroxidation in human lymphocytes
Lipid is one of the main targets attacked by ROS. The reaction between lipid and ROS such as •OH and H2O2 causes lipid peroxidation, resulting in damages of cell membranes. It has been reported that 6-o-palmitoylascorbate could protect lipid bilayers and micelles against lipid peroxidation probably due to its ability to interact with phospholipid mono-layers [33]. We observed that at 2 h after X-ray, most of the non-pretreated cells suffered from lipid peroxidation in the membranes, whereas there were much fewer cells with lipid peroxidation in either sham-irradiated or PlmtVC-pretreated samples. Tali cytometric analysis showed that PlmtVC significantly inhibited lipid peroxidation as well as l-AA (p < 0.001), suggesting that PlmtVC could prevent X-ray-induced oxidative degradation of lipids (Fig. 6).
Effect of PlmtVC on X-ray-induced lipid peroxidation in HEV0082 cells. HEV0082 cells (3 × 105 cells/dish) were seeded into 35-mm dishes and treated with PlmtVC (120 μM) or l-acsorbic acid (120 μM) as same as we described in Fig. 4. Cells were irradiated with X-ray (1.5 Gy) and further cultivated for 2 h. Cells were then stained with 10 μM Lipid Peroxidation Sensor for 30 min in complete growth medium at 37 °C. Nuclei were stained with Hoechst 33342 (blue). The cells were imaged by LSM. Upon oxidation, the reagent shifts fluorescence emission peak from ~590 nm (red) to ~510 nm (green) (a). The signal was then quantitated using the Tali® Image Cytometer, and the ratios of the signal from the 510 to 590 channels were used to quantify lipid peroxidation in cells. In control cells (NC), most of the signal was in red channel, and the ratio of 510/590 was low. When the cells were irradiated with X-ray (PC), the ratios were much higher. LAA or PVC pre-treatment decreases the lipid peroxidation in cells as seen from decreased ratios in LAA or PVC pre-treated samples (b). Data represent the mean ± SD of three independent experiments. ***p < 0.001 versus PC. Scale bar = 20 μm. (Color figure online)
Inhibitory effects of PlmtVC on X-ray-induced protein carbonylation in human lymphocytes
As same as lipids, proteins are other important targets for oxidative damage. It has been reported that ionizing radiation-induced protein carbonylation is related to survival more closely than to DNA damage in organism [34]. We demonstrated that in non-irradiated HEV0082 cells, the amount of protein carbonyls was about 5.1 nmol/ml/107 cells. Immediately after X-ray, the amount of protein carbonyls was increased to 9.8 nmol/ml/107 cells in non-pretreated cells (PC). In l-AA- or PlmtVC-pretreated samples, protein carbonyls were 6.5 and 4.9 nmol/ml/107 cells, respectively. There was a significant difference between the positive control group and PlmtVC group (p < 0.05) but not l-AA group (Fig. 7). The data suggest that PlmtVC has inhibitory effects on X-ray-caused protein carbonylation that is more markedly than l-AA.
Effect of PlmtVC on X-ray-induced protein carbonylation in HEV0082 cells. HEV0082 cells (1 × 107 cells/flask) were seeded into 75-cm2 flasks and cultivated overnight. PlmtVC (120 μM) or l-ascorbic acid (120 μM) was added in the medium at the next day. After 3 h of cultivation, cells were irradiated with X-ray (1.5 Gy). Cells were then immediately homogenized on ice in 0.5 ml cold 50 mM MES buffer (pH 6.7, contain 1 mM EDTA). About 0.5 mg protein was obtained by extraction. Protein carbonyl was measured with the protein carbonyl colorimetric assay kit. In control cells (NC), concentration of protein carbonyl was low. In X-ray-irradiated cells (PC), the concentration was increased near two times. PVC pretreatment significantly decreased protein carbonylation in cells. Data represent the mean ± SD of three independent experiments. *p < 0.05 versus PC
PlmtVC elevates intracellular GSH levels in human lymphocytes preferentially over l-AA
As an important intracellular antioxidant, GSH plays a central role in protecting of mammalian cells against damage incurred by oxidative stress [19]. Since reduced glutathione represents the majority of intracellular free thiols in cells, ThiolTracker™ Violet dye can be used in estimating the cellular level of reduced glutathione. We then examined if PlmtVC could elevate intracellular GSH levels in HEV0082 cells with ThiolTracker™ Violet dye. As shown in Fig. 8a, after 3 h of treatment, intracellular GSH significantly increased in PlmtVC-treated cells at diverse concentrations (p < 0.001). l-AA treatment also pointedly increased intracellular GSH levels at doses of 30 and 120 μM, whereas the enhancement was significantly lower than PlmtVC at the same concentration. We further observed the effect of X-ray irradiation on intracellular GSH at different time points. Figure 8b shows that intracellular GSH levels did not obviously decreased by X-ray at 10 min and 5 h after irradiation. However, at the time points of 24 h (which is the time point that X-ray-induced terminal apoptosis-associated symptoms are expressed) and 48 h (which is the time point that X-ray-induced cell death occurs) after irradiation GSH levels were decreased to about 66.4 and 20 % of that in negative control (NC), respectively. We then chose the time point of 24 h after irradiation to evaluate the effect of PlmtVC on X-ray-induced exhaustion of GSH in HEV0082 cells. Figure 8c shows that PlmtVC significantly elevated intracellular GSH levels in X-ray-irradiated cells at different concentrations (p < 0.001). l-AA treatment slightly increased intracellular GSH levels at 30 and 60 μM whereas the enhancement was significantly lower than PlmtVC at the same concentration (p < 0.001). Our data suggested that PlmtVC could elevate intracellular GSH levels in human lymphocytes irradiated with X-ray or not, preferentially over l-AA.
Effect of PlmtVC on intracellular GSH levels in HEV0082 cells irradiated with X-ray or not. a HEV0082 cells (3 × 105 cells/dish) were seeded into 35-mm dishes and incubated with PlmtVC or l-ascorbic acid at diverse concentrations for 3 h. Then, the cells were harvested and washed 2 times with DPBS with C/M. Intracellular GSH levels were detected with ThiolTracker™ Violet and analyzed with a fluorescence microplate reader. b HEV0082 cells (3 × 105 cells/dish) were seeded into 35-mm dishes and irradiated by X-ray at 1.5 Gy. Intracellular GSH was detected at different time points after X-ray. c HEV0082 cells were seeded and pretreated with PlmtVC or l-ascorbic acid as in (a). Cells were then irradiated with X-ray (1.5 Gy) after 3 h of pretreatment. Intracellular GSH was measured at 24 h after X-ray. Data presented are the mean ± SD of results from three independent experiments (***p < 0.001 versus 0; ## p < 0.01; ### p < 0.001 versus LAA-treated cells at the same concentration)
Comparison of stability between PlmtVC and l-AA
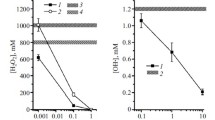
Vitamin C is the less stable vitamin which can be rapidly oxidized at physiological temperatures and pH. To investigate whether PlmtVC is stable at the physiological conditions, we performed both cell-free and cellular studies. Figure 9 shows that, under the cell-free conditions, 1 day after incubation, residual vitamin C rates in l-AA solutions were 111.1 % of the fresh solution at 20 μM, 87.0 % at 40 μM and 62.0 % at 60 μM. Residual vitamin C rates in PlmtVC solutions were 57.0 % at 20 μM, 88.8 % at 40 μM and 84.4 % at 60 μM. 14 days later, vitamin C in l-AA solutions were degraded to 28.7 % (20 μM), 20.5 % (40 μM) and 22.5 % (60 μM). In contrast, residual vitamin C rates in PlmtVC solutions were 82.0 % (20 μM), 62.2 % (40 μM) and 65.6 % (60 μM), which were significant higher than in l-AA solutions (p < 0.001).
Stability of PlmtVC solution under physiological conditions (pH 7.4, 37 °C). PlmtVC or l-ascorbic acid was solved in 1 N NaOH solution first, and immediately neutralized with 5.4 % meta-phosphoric acid until the pH reaches 7.4. Then, the solutions were kept in a humidified environment at 37 °C. After 1 and 14 days, the concentration of vitamin C was measured with OPDA ascorbate assay. LAA-F, fresh solution of LAA; LAA-37-1d, LAA solution was kept at 37 °C for 1 day. LAA-37-14d, LAA solution was kept at 37 °C for 14 days. PVC-F fresh solution of PVC; PVC-37-1d PVC solution was kept at 37 °C for 1 day. PVC-37-14d PVC solution was kept at 37 °C for 14 days. Data represent the mean ± SD of three independent experiments. # p < 0.05; ## p < 0.01; ### p < 0.001 versus LAA-treated cells at the same concentration
The intracellular vitamin C tests (Fig. 10) showed that after cultivated with l-AA for 1.5 h, intracellular vitamin C reached the highest concentration of 38.5 μmol/107 cells and then gradually decreased. After 24 h intracellular vitamin C could not be detected in the l-AA-treated cells indicating that vitamin C was degraded. In PlmtVC-treated samples, intracellular vitamin C reached the peak concentration of 86.9 μmol/107 cells at 4 h after cultivation. Even at 24 h later, there still considerate vitamin C (62.8 μmol/107 cells) remained. The concentrations of vitamin C in PlmtVC-treated cells were significantly higher than that in l-AA-treated samples (p < 0.01 at 3 h, p < 0.001 at 4 and 24 h) suggesting that PlmtVC could enhance intracellular vitamin C level and prevent vitamin C degradation.
Uptake of PlmtVC into HEV0082 cells and time-dependent change of intracellular vitamin C. HEV0082 cells (1 × 107 cells/flask) were seeded into 75-cm2 flasks. PlmtVC (500 μM) or l-ascorbic acid (500 μM) was added in the medium at the same time. After 0.5, 1.5, 3, 4, and 24 h of cultivation, about 1 × 107 cells were harvested and homogenized. Intracellular vitamin C was measured by DNPH ascorbate assay. Data represent the mean ± SD of three independent experiments. ## p < 0.01; ### p < 0.001 versus LAA
These data indicate that PlmtVC has excellent stabilities under both cell-free and cellular physiological conditions.
Discussion
The present study investigated radioprotection of the lipophilic ascorbate PlmtVC on X-ray-induced damages in human lymphocytes HEV0082 compared with water-soluble l-AA. Because of the hydrophobic palmitate side chain, PlmtVC molecule positions itself into cell membranes that might undergo a harmful effect on cell viability under certain conditions [35]. To clarify if PlmtVC is toxic to HEV0082 lymphocytes, we first examined the cytotoxicity of PlmtVC. PlmtVC showed stimulative effects on cell growth in HEV0082 cells after 48 h cultivation, indicating that PlmtVC can promote cell proliferation. Since PlmtVC elevates intracellular GSH (which is very important for cell growth and viability) in HEV0082 cells, we considered that PlmtVC-enhanced cell proliferation is related to the enhancement of endogenous GSH. PlmtVC did not reduce cell viability after 72 and 96 h of cultivation at concentrations from 10 to 200 μM, suggesting that PlmtVC is very safe. The LD50 of X-ray in HEV0082 cells was approximately 1.5 Gy. Apoptotic analysis showed that, 12 h after X-ray, caspase-3 was activated. 24 h later, cells underwent terminal-stage apoptosis. PlmtVC significantly protected HEV0082 cells against X-ray-induced cell death and apoptosis as shown by Alamar Blue assay, caspase 3 activation indicator, and TUNEL assay. DNA damage, lipid peroxidation, and protein carbonylation are considered as important contributors for X-ray-induced lethality. Among them, DNA damage is the most responsible for X-ray-induced cell death. Our results showed that at 30 min after X-ray (1.5 Gy), the hallmark of DBSs, gamma-H2A.X foci were plentifully detected in HEV0082 cells, indicating serious DNA damage. PlmtVC prevented HEV0082 cells from X-ray-induced DSBs that were more markedly than l-AA.
Because DSBs are mainly caused by X-ray-generated hydroxyl radicals, it needs to confirm the antioxidative activities of PlmtVC. We first tested the effect of PlmtVC on intracellular ROS which was generated by X-ray at 1.5 Gy. The data showed that PlmtVC-scavenged X-ray-caused intracellular ROS as well as l-AA. Lipid peroxidation is the oxidative membrane damage. It has been reported that, although ascorbyl-6-palmitate reduced intracellular ROS levels following ultraviolet B (UVB) irradiation, it intensely promoted UVB-induced lipid peroxidation, unexpectedly in keratinocytes [36]. It was examined in the present study whether PlmtVC has any effects on X-ray-induced lipid peroxidation in lymphocytes or not. Our data showed that lipid peroxidation was prevented by PlmtVC in X-ray-irradiated cells. So why PlmtVC promoted UVB-induced lipid peroxidation in cultured keratinocytes, but, in contract, inhibited X-ray-induced lipid peroxidation in lymphocytes? The reason is considered that cellular non-specific esterase activity is different between keratinocytes and lymphocytes. It has been reported that an esterase activity in the freshly isolated human keratinocytes decreased along with culture time [37], whereas lymphocytes have a distinctive esterase activity. It is possible that because the cultured keratinocytes have limited abilities to hydrolyze esters of PlmtVC, its hydrophobic palmitate side chain remains in the cell membranes. UVB-generated ROS easily attacked the palmital side chain incorporated disturbed cell membrane to cause lipid peroxidation. In contrast, lymphocytes have abundant esterase which hydrolyzes palmitate side of PlmtVC, release active non-esterified ascorbic acid molecules, and therefore reduce lipid peroxidation.
Additionally, protein carbonylation as the ionizing radiation-mediated irreversible oxidative damage was obviously reduced by PlmtVC pretreatment in HEV0082 cells, further confirming the antioxidative activity of PlmtVC. PlmtVC also elevated endogenous antioxidant GSH in HEV0082 cells and prevented X-ray-induced GSH depletion, both of which were preferential over l-AA. Noticeably, PmtVC exhibited much better stability under physiological conditions. In the cellular level, PlmtVC was demonstrated to enhance intracellular accumulation of vitamin C, assumedly through esterolytic conversion to ascorbic acid (Asc), more markedly than administration with Asc itself being susceptible to oxidative degradation reversibly to dehydroascorbic acid and further irreversibly to diketogulonic acid.
Based on the data described here, we propose a hypothetical mechanism of preventive effect of PlmtVC on X-ray-induced damage in HEV0082 cells in Fig. 11. In this hypothesis, X-ray-generated hydroxyl radicals cause lipid peroxidation, protein carbonylation, and DSBs. Lipid peroxidation damages the plasma and intracellular membranes, protein carbonylation causes structural and functional damage, and DSBs lead to genome rearrangements. These three lethal injuries independently or cooperatively induce cell death. The water-soluble l-AA depends on the glucose transporter 1 (GLUT1) to enter into the cells as the oxidated form diketogulonic acid. l-AA can be rapidly oxidized and lose its antioxidative activity before entering into the cells. In contrast, fat-soluble PlmtVC can easily pass the plasma and intracellular membranes through passive diffusion. The fatty acid ester of ascorbate molecules can prevent the 2,3-enediol moiety in a VC molecule from oxidative degradation through the buried interior form, within micro micelle aggregates, which is separately isolated from the extramolecular bulk space being abundant for soluble oxygen molecules. Therefore, PlmtVC is more stable inside the cell than l-AA. Once PlmtVC entered into cells, the PlmtVC molecules are hydrolytically separated into VC molecules and PlmtVC moieties by cellular esterase. Non-oxidized VC molecules scavenge X-ray-generated hydroxyl radicals and prevent lipid peroxidation, protein carbonylation, and DSBs thereby inhibit cell death.
References
Tusher VG, Tibshirani R, Chu G (2001) Significance analysis of microarrays applied to the ionizing radiation response. Proc Natl Acad Sci USA 98:5116–5121
Varshney R, Kale RK (1990) Effects of calmodulin antagonists on radiation-induced lipid peroxidation in microsomes. Int J Radiat Biol 58:733–743
Krisko A, Radman M (2010) Protein damage and death by radiation in Escherichia coli and Deinococcus radiodurans. Proc Natl Acad Sci USA 107:14373–14377. doi:10.1073/pnas.1009312107
Sutherland BM, Bennett PV, Sidorkina O, Laval J (2000) Clustered DNA damages induced in isolated DNA and in human cells by low doses of ionizing radiation. Proc Natl Acad Sci USA 97:103–108
Sokolov M, Neumann R (2013) Lessons learned about human stem cell responses to ionizing radiation exposures: a long road still ahead of us. Int J Mol Sci 14:15695–15723. doi:10.3390/ijms140815695
Thornalley PJ, Vasák M (1985) Possible role for metallothionein in protection against radiation-induced oxidative stress. Kinetics and mechanism of its reaction with superoxide and hydroxyl radicals. Biochim Biophys Acta 827:36–44
Ward JF, Blakely WF, Joner EI (1985) Mammalian cells are not killed by DNA single-strand breaks caused by hydroxyl radicals from hydrogen peroxide. Radiat Res 103:383–392
Cadet J, Douki T, Ravanat JL (2010) Oxidatively generated base damage to cellular DNA. Free Radic Biol Med 49:9–21. doi:10.1016/j.freeradbiomed.2010.03.025
Manda K, Ueno M, Anzai K (2007) AFMK, a melatonin metabolite, attenuates X-ray-induced oxidative damage to DNA, proteins and lipids in mice. J Pineal Res 42:386–393
Corre I, Niaudet C, Paris F (2010) Plasma membrane signaling induced by ionizing radiation. Mutat Res 704:61–67. doi:10.1016/j.mrrev.2010.01.014
Daly MJ, Gaidamakova EK, Matrosova VY, Vasilenko A, Zhai M, Leapman M, Lai B, Ravel B, Li SM, Kemner KM, Fredrickson JK (2007) Protein oxidation implicated as the primary determinant of bacterial radioresistance. PLoS Biol 5:e92. doi:10.1371/journal.pbio.0050092
Haro KJ, Sheth A, Scheinberg DA (2012) Dysregulation of IRP1-mediated iron metabolism causes gamma ray-specific radioresistance in leukemia cells. PLoS ONE 7:e48841. doi:10.1371/journal.pone.0048841
Smutná M, Beňová K, Dvořák P, Nekvapil T, Kopřiva V, Maté D (2013) Protein carbonyls and traditional biomarkers in pigs exposed to low-dose γ-radiation. Res Vet Sci 94:214–218. doi:10.1016/j.rvsc.2012.09.002
Wright EG (2000) Inducible genomic instability: new insights into the biological effects of ionizing radiation. Med Confl Surviv 16:117–130
Vignard J, Mirey G, Salles B (2013) Ionizing-radiation induced DNA double-strand breaks: a direct and indirect lighting up. Radiother Oncol 108:362–369. doi:10.1016/j.radonc.2013.06.013
Lomax ME, Folkes LK, O’Neill P (2013) Biological consequences of radiation-induced DNA damage: relevance to radiotherapy. Clin Oncol 25:578–585. doi:10.1016/j.clon.2013.06.007
Prasad NR, Menon VP, Vasudev V, Pugalendi KV (2005) Radioprotective effect of sesamol on gamma-radiation induced DNA damage, lipid peroxidation and antioxidants levels in cultured human lymphocytes. Toxicology 209:225–235
Buonanno M, de Toledo SM, Pain D, Azzam EI (2011) Long-term consequences of radiation-induced bystander effects depend on radiation quality and dose and correlate with oxidative stress. Radiat Res 175:405–415. doi:10.1667/RR2461.1
Chatterjee A (2013) Reduced glutathione: a radioprotector or a modulator of DNA-repair activity? Nutrients 5:525–542
Krisko A, Leroy M, Radman M, Meselson M (2012) Extreme anti-oxidant protection against ionizing radiation in bdelloid rotifers. Proc Natl Acad Sci USA 109:2354–2357. doi:10.1073/pnas.1119762109
Vorotnikova E, Tries M, Braunhut S (2004) Retinoids and TIMP1 prevent radiation-induced apoptosis of capillary endothelial cells. Radiat Res 161:174–184
Singh VK, Wise SY, Singh PK, Posarac A, Fatanmi OO, Ducey EJ, Bolduc DL, Elliott TB, Seed TM (2013) Alpha-tocopherol succinate-mobilized progenitors improve intestinal integrity after whole body irradiation. Int J Radiat Biol 89:334–345. doi:10.3109/09553002.2013.762137
Rahman K (2007) Studies on free radicals, antioxidants, and co-factors. Clin Interv Aging 2:219–236
Sram RJ, Binkova B, Rossner P Jr (2012) Vitamin C for DNA damage prevention. Mutat Res 733:39–49. doi:10.1016/j.mrfmmm.2011.12.001
Fujii Y, Kato TA, Ueno A, Kubota N, Fujimori A, Okayasu R (2010) Ascorbic acid gives different protective effects in human cells exposed to X-rays and heavy ions. Mutat Res 699:58–61. doi:10.1016/j.mrgentox.2010.04.003
Hata K, Urushibara A, Yamashita S, Shikazono N, Yokoya A, Katsumura Y (2013) Chemical repair of base lesions, AP-sites, and strand breaks on plasmid DNA in dilute aqueous solution by ascorbic acid. Biochem Biophys Res Commun 434:341–345. doi:10.1016/j.bbrc.2013.03.075
Simpson GL, Ortwerth BJ (2000) The non-oxidative degradation of ascorbic acid at physiological conditions. Biochim Biophys Acta 1501:12–24
Miwa N, Yamazaki H (1986) Potentiated susceptibility of ascites tumor to acyl derivatives of ascorbate caused by balanced hydrophobicity in the molecule. Exp Cell Biol 54:245–249
May JM, Qu ZC, Cobb CE (1996) Accessibility and reactivity of ascorbate 6-palmitate bound to erythrocyte membranes. Free Radic Biol Med 21:471–480
Ross D, Mendiratta S, Qu ZC, Cobb CE, May JM (1999) Ascorbate 6-palmitate protects human erythrocytes from oxidative damage. Free Radic Biol Med 26:81–89
Iwakawa M, Goto M, Noda S, Sagara M, Yamada S, Yamamoto N, Kawakami Y, Matsui Y, Miyazawa Y, Yamazaki H, Tsuji H, Ohno T, Mizoe J, Tsujii H, Imai T (2005) DNA repair capacity measured by high throughput alkaline comet assays in EBV-transformed cell lines and peripheral blood cells from cancer patients and healthy volunteers. Mutat Res 588:1–6
Gey KF (1995) Ten-year retrospective on the antioxidant hypothesis of arteriosclerosis: threshold plasma levels of antioxidant micronutrients related to minimum cardiovascular risk. J Nutr Biochem 6:206–236
Srám RJ, Rössner P, Smerhovský Z (2004) Cytogenetic analysis and occupational health in the Czech Republic. Mutat Res 566:21–48
Mottola M, Wilke N, Benedini L, Oliveira RG, Fanani ML (2013) Ascorbyl palmitate interaction with phospholipid monolayers: electrostatic and rheological preponderancy. Biochim Biophys Acta 1828:2496–2505. doi:10.1016/j.bbamem.2013.06.016
Daly MJ (2009) A new perspective on radiation resistance based on Deinococcus radiodurans. Nat Rev Microbiol 7:237–245. doi:10.1038/nrmicro2073
Meves A, Stock SN, Beyerle A, Pittelkow MR, Peus D (2002) Vitamin C derivative ascorbyl palmitate promotes ultraviolet-B-induced lipid peroxidation and cytotoxicity in keratinocytes. J Invest Dermatol 119:1103–1108
Barker CL, Clothier RH (1997) Human keratinocyte cultures as models of cutaneous esterase activity. Toxicol In Vitro 11:637–640
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xiao, L., Tsutsui, T. & Miwa, N. The lipophilic vitamin C derivative, 6-o-palmitoylascorbate, protects human lymphocytes, preferentially over ascorbate, against X-ray-induced DNA damage, lipid peroxidation, and protein carbonylation. Mol Cell Biochem 394, 247–259 (2014). https://doi.org/10.1007/s11010-014-2101-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-014-2101-8