Abstract
After peripheral nerve injury, Schwann cells are rapidly activated to participate in the regenerative process and modulate local immune reactions. Tumor necrosis factor-α (TNF-α), one of the major initiators of the inflammatory cascade, has been known to exert pleiotropic functions during peripheral nerve injury and regeneration. In this study, we aimed to investigate the in vitro effects of TNF-α on peripheral neural cells. First, gene-microarray analysis was applied to the RNA samples extracted from injured peripheral nerves, providing the information of gene interactions post nerve injury. Then, after primary cultured Schwann cells were treated with increasing dosages (0–40 ng/ml) of TNF-α, cell proliferation and migration were examined by EdU incorporation and a transwell-based assay, and cell apoptosis was observed and quantified by electron microscopy and Annexin V-FITC assay, respectively. The results showed that lower dosages of TNF-α increased cell proliferation and migration, whereas higher dosages of TNF-α decreased cell proliferation and migration and enhanced cell apoptosis. The tests using a chemical inhibitor of TNF-α further confirmed the above effects of TNF-α. To understand how TNF-α produced the dose-dependent dual effects on primary cultured Schwann cells, we performed co-immunoprecipitation, Western blot analysis, and immunocytochemistry to decipher the complex network of biochemical pathways involving many signaling molecules, i.e., TNF receptor-associated death domain, Fas-associated death domain, receptor interacting protein, JNK, NF-κB p65, and caspases, thus assuming the mechanisms by which TNF-α activated the death and survival pathways and achieved a balance between the two opposite actions in primary cultured Schwann cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Peripheral nerve injury is a common clinical problem, and various nerve repair techniques have been developed. Until now, however, the therapeutic outcomes are still far from ideal, especially functional recovery remains unsatisfactory. To improve peripheral nerve regeneration, it is required to have an in-depth insight into the process of peripheral nerve injury and regeneration, which may involve multiple complex interactions among different cells and a diverse array of cytokines [1].
Schwann cells are the principal glial cells of the peripheral nervous system. They are rapidly activated after peripheral nerve injury and differentiate into myelinating cells. Following nerve injury, successful remyelination of damaged axons by Schwann cells depends on a combination of signals that Schwann cells receive from the demyelinated axons with the inflammatory response. These signals prompt Schwann cells to first re-enter the cell cycle and then differentiate into myelinating cells [2]. More importantly, if axonal regrowth is initiated, Schwann cells not only receive signals from axons, but also, in turn, regulate how axons respond [3, 4]. Moreover, the extracellular molecules of the basal lamina and their receptors are also involved in both axonal elongation and remyelination [5].
Tumor necrosis factor-α (TNF-α) is one of the pro-inflammatory cytokines produced in activated macrophages in response to pathogens and other noxious stimuli. The cytokine usually initiates the inflammatory cascade and exerts pleiotropic functions in physiological and pathological conditions by binding to its receptors, type I (TNFRI) and type II (TNFRII). Following peripheral nerve injury, TNF-α can be released by Schwann cells as well as by macrophages [6, 7]. If axonally derived trophic support is decreased, TNF-α release will be enhanced to promote the reversion of mature to immature Schwann cells [8, 9]. This phenotype reversion, together with an increase in p75NTR expression, could make Schwann cells more susceptible to pro-apoptotic molecular mechanisms [10].
We recently noticed an involvement of TNF-α-related signaling molecules, including Birc2, Birc3, and TNFRI, in the anti-apoptosis process of injured peripheral nerves, implying that a higher dosage of TNF-α could induce apoptosis of Schwann cells in vitro while a lower dosage of TNF-α could not [11]. Our findings are consistent with the results of several previous studies [10, 12], but the mechanism underlying the pleiotropic functions of TNF-α in peripheral nerve injury is still unclear. The aim of our study is to confirm the dose-dependent dual effects of TNF-α on Schwann cells, and to help understand the possible mechanism. We used primary cultured Schwann cells as a cell model, tested Schwann cell proliferation, migration, and morphological changes after treatment with different dosages of TNF-α, and examined the involvement of several apoptosis-related signaling molecules.
Materials and methods
Microarray and gene network analysis
The gene-microarray procedures were performed as previously described [11]. Briefly, under deep anesthesia, male Sprague–Dawley rats (180–220 g) underwent surgical axotomy of the left sciatic nerve. At 0, 0.5, 1, 3, 6, and 9 h after surgery, the proximal nerve segments were harvested for RNA extraction with a mirVana™ miRNA Isolation Kit (Ambion, Austin, TX) according to the manufacturer’s instructions, followed by purification and quantification of RNA samples.
A cDNA microarray (Agilent Technology, Tokyo, Japan) was used to screen the RNA samples collected at different time points post-surgery. The labeling and hybridization of RNA samples were performed by the Shanghai Biochip Company (Shanghai, China). Agilent Scan Control software was used for scanning the microarray slides, and Agilent Feature Extraction software version 9.5.3 was used for image analysis. Microarray data were analyzed using GeneSpring GX v11.0 software (Agilent Technology).
Following microarray analysis, the mRNA expression was compared among different time points. The significance and false discovery rate were calculated using the adjusted F-test with the random variation model [13], and the differential gene expressions at different time points were identified.
For bioinformatic analysis, gene ontology and Kyoto encyclopedia of genes and genomes databases were applied to analyze the pathways related to differentially expressed genes, and a dynamic gene regulatory network was constructed according to gene fold expression and gene interaction in pathways.
Cell culture and treatment
Primary cultured Schwann cells were obtained as previously described [14] with minor modifications. Briefly, sciatic nerves were harvested from Sprague–Dawley rats (1–3-day-old) and enzymatically dissociated by incubation at 37 °C sequentially with 1 % collagenase and 0.125 % trypsin for 30 and 10 min, respectively. The mixture was triturated, centrifuged, and resuspended in Dulbecco’s modified Eagle’s medium (DMEM) supplemented with 10 % (v/v) fetal calf serum. The cell pellets were plated on poly-l-lysine pre-coated dishes (35 mm) for incubation in the same medium. On the following day, 10 μM cytosine arabinoside was added and allowed to incubate for additional 48 h to remove fibroblasts. The cell culture was maintained subsequently in DMEM supplemented with 10 % FBS, 2 μM forskolin (Sigma, St Louis, MO), and 2 ng/ml heregulin (HRG, Sigma) to stimulate Schwann cell proliferation. For further purification, the cell culture was gently trypsinized, pelleted, and incubated with anti-Thy1 antibody (AbD Serotec, Raleigh, NC) on ice for 2 h, followed by incubation in complement (Jackson Immuno, West Grove, PA) for additional 2 h. All media and supplements were bought from Gibco-Invitrogen (Carlsbad, CA).
Primary Schwann cells with 90 % confluency were treated, respectively, with increasing dosages (0–40 ng/ml) of soluble recombinant rat TNF-α (Peprotech, endotoxin level < 1 EU/μg) for 24 h. The cells were also treated with a chemical inhibitor of TNF-α, 6,7-dimethyl-3-((methyl-(2-(methyl-(1-(3-trifluoromethyl-phenyl)-1H-indol-3-ylmethyl)-amino)-ethyl)-amino)-methyl)-chromen-4-one, diHCl (Merck, Germany), which was dissolved in DMSO with different concentrations (10, 50, 100, and 500 nM), in the presence of 2 or 40 ng/ml of TNF-α.
Cell proliferation assay
Schwann cells were resuspended in fresh pre-warmed (37 °C) complete medium, counted and plated at a density of 2 × 105 cells/ml on 0.01 % poly-l-lysine-coated 96-well plates. At the indicated time point after treatment with TNF-α or with TNF-α plus its chemical inhibitor, 50 μM 5-ethynyl-2-deoxyuridine (EdU) was added to allow culture for additional 2 h. Then, Schwann cells were fixed with 4 % formaldehyde in phosphate buffered saline for 30 min, followed by assay using Cell-Light™ EdU DNA Cell Proliferation Kit (Ribobio Guangzhou, China) according to the manufacturer’s protocol. The percentage of EdU-positive cells was calculated from five random fields obtained on a DMR fluorescence microscope (Leica Microsystems, Bensheim, Germany). Assays were done three times using triplicate wells.
Cell migration assay
Migration of Schwann cells was examined in a 6.5 mm Transwell chamber with 8 μm pores (Costar, Cambridge, MA) as described previously [15]. The bottom surface of each membrane was coated with 10 μg/ml fibronectin. 100 μl Schwann cells (106 cells/ml) resuspended in DMEM was transferred to the top chambers of each transwell and allowed to migrate at 37 °C in 5 % CO2, and 600 μl of complete medium was injected into the lower chambers. The upper surface of each membrane was cleaned with a cotton swab at the indicated time point. Cells adhering to the bottom surface of each membrane were stained with 0.1 % crystal violet, imaged, and counted using a DMR inverted microscope (Leica Microsystems). Assays were carried out three times using triplicate wells.
Electron microscopy and Annexin V-FITC assay
After treatment with different dosages of TNF-α, Schwann cells were fixed in 4 % glutaraldehyde, post-fixed with 1 % OsO4, and dehydrated stepwise in increasing concentrations of ethanol. A portion of samples was dried in a critical point drier (Hitachi, Tokyo, Japan) for coating with gold, followed by observation under a scanning electron microscope (JEM-T300, JEOL, Japan). And other samples were embedded in Epon 812 epoxy resin to make ultrathin sections, which were stained with lead citrate and uranyl acetate, followed by observation under a transmission electron microscope (JEM-1230, JEOL, Japan).
The apoptosis rate was determined by Annexin V-FITC apoptosis assay according to the manufacturer’s instructions (Invitrogen). In brief, primary Schwann cells on 96-well plate were treated with TNF-α or with TNF-α plus its chemical inhibitor, and then allowed to incubate with Annexin-binding buffer (containing 10 μl Annexin V conjugate) for 15 min at 22–25 °C. After washes, Annexin-V staining was visualized under an inverted Leica DM3000 epifluorescence microscope (Leica, Wetzlar, Germany). Two images were taken per well and the number of Annexin-V-positive cells was counted.
Western blot analysis
Protein was extracted from Schwann cells with a buffer containing 1 % SDS, 100 mM Tris–HCl, 1 mM PMSF, and 0.1 mM β-mercaptoethanol. Protein concentration was detected by the Bradford method to maintain the same loads. Protein extracts were heat denatured at 95 °C for 5 min, electrophoretically separated on 10 or 12 % SDS-PAGE, and transferred to PVDF membranes. The membranes were subjected to the reaction at 4 °C overnight with rabbit antibodies against cleaved caspase-7 (Asp198), cleaved caspase-8 (18C8), phosphor-NF-κB P65 (Ser536), phosphor-p44/42 MAPK (JNK, Thr202/Tyr204, 197G2), or a mouse antibody against cleaved caspase-9 (Asp353), respectively, in which all antibodies were obtained from Cell Signaling (Beverly, MA) and used with 1:1,000 dilution in TBS buffer. Then, the secondary antibody conjugated with horseradish peroxidase (HRP): goat anti-rabbit HRP (1:1,000) or goat anti-mouse HRP dilution (1:1000, both from Santa Cruz, Santa Cruz, CA) was added to allow incubation at room temperature for 2 h. After the membrane was washed, the HRP activity was detected using an ECL kit. The image was scanned with a GS800 Densitometer Scanner (Bio-Rad), and the data were processed using a PDQuest 7.2.0 software (Bio-Rad). β-actin (1:5,000) was used as an internal control.
Immunocytochemistry
After treatment with 40 ng/ml of TNF-α, Schwann cells were fixed with 4 % paraformaldehyde and incubated with rabbit antibodies against cleaved caspase-7 (Asp198), cleaved caspase-8 (18C8), or a mouse antibody against cleaved caspase-9 (Asp353), respectively, in which all antibodies were obtained from Cell Signaling and used with 1:100 dilution in TBS buffer, or rabbit antibody against S100β (1:500, Sigma, St. Louis, MO) at 4 °C for 24 h, and were further reacted with the FITC labeled secondary antibody goat anti-mouse IgG (1:200, Santa Cruz), FITC labeled secondary antibody goat anti-rabbit IgG (1:200 dilution, Santa Cruz), or TRITC labeled secondary antibody goat anti-rabbit IgG (1:200 dilution, Santa Cruz) at 4 °C overnight. After being labeled with Hoechst 33342 (5 μg/ml), sections were mounted in fluorescent mounting medium and observed under a confocal laser scanning microscope (Leica, Heidelberg, Germany).
Coimmunoprecipitation
After treatment with different dosages of TNF-α, Schwann cells were lysed in a lysis buffer (0.025 M Tris, 0.15 M NaCl, 0.001 M EDTA, 1 % NP-40, and 5 % glycerol, pH 7.4) containing protease and phosphatase inhibitors. The immunoprecipitation was performed following the protocol of a Pierce® Classic IP Kit (Pierce). Afterward, cell samples were subjected to Western blot analysis through the above mentioned procedures, but using primary antibodies against TNF receptor-associated death domain (TRADD, 1:500, Rabbit, Abcam, Cambridge, UK), Fas-associated death domain (FADD, 1:500, mouse, Santa Cruz), and receptor interacting protein (RIP, 1:500, mouse, Abcam, Cambridge, UK) instead.
Statistics
The data were expressed as mean ± SD and analyzed by one-way analysis of variance (ANOVA) followed by post hoc Scheffé test. All statistical analyses were carried out by the aid of STATA 7.0 software package (Stata Corp., College Station, TX), and differences were considered statistically significant at p < 0.05.
Results
Gene expression profile
The differential expressions of some apoptosis- or survival-related genes were determined by microarray analysis. After rat sciatic nerves were transected, both pro-apoptosis genes, such as FADD, JNK, caspase-3, -6, -7, -8, and -9, and anti-apoptosis genes, such as RIP, NF-κB p65, Birc2 (also named cIAP 1), and Birc3 (also named cIAP 2), underwent time-dependent expression changes in the proximal nerve (Table 1). These data initiate an assumption that peripheral nerve injury might simultaneously activate both pro-apoptosis and anti-apoptosis signaling pathways. In fact, our previous study [11] revealed that the TNF-α level gradually increased with time after sciatic nerve injury, suggesting that TNF-α was likely to exert dual effects on neural cells. The following tests were conducted to test this assumption.
Effects of TNF-α on proliferation and migration of primary Schwann cells
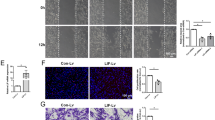
EdU (red)/Hoechst (blue) immunostaining compared the cell proliferation rate of primary Schwann cells when they were treated with different dosages of TNF-α. Statistics indicated that as compared to non-treatment (control), treatment with 2 ng/ml TNF-α resulted in a significant increase in the cell proliferation rate of Schwann cells, and treatment with 5 ng/ml of TNF-α induced no significant change, but treatment with 10, 20, or 40 ng/ml of TNF-α caused a significant decrease (Fig. 1a–g). We also tested cell proliferation after primary Schwann cells were treated with TNF-α at dosages lower than 2 ng/ml (0.01, 0.1, and 1.0 ng/ml). Although each of these low dosages of TNF-α led to an increased cell proliferation as compared to that of non-treatment (data not shown), only 1.0 and 2.0 ng/ml of TNF-α significantly increased cell proliferation, and so 2.0 ng/ml of TNF-α was selected as a typical low dosage for other experiments.
Effects of different dosages of TNF-α on cell proliferation and migration of primary cultured Schwann cells. Merges of EdU staining (red) and Hoechst 33342 staining (blue) for the cells treated with 0 (a, control), 2 (b), 5 (c), 10 (d), 20 (e), and 40 (f) ng/ml of TNF-α, respectively. Scale bar 50 μm. Bar chart (g) showing the cell proliferation rate (expressed as the percentage of EdU-positive cells to total cells, and normalized to control) of primary cultured Schwann cells after treatment with different dosages of TNF-α. Images showing that the cells migrated to the bottom of the transwell chamber after treatment with 0 (h, control), 2 (i), 5 (j), 10 (k), 20 (l), and 40 (m) ng/ml of TNF-α, respectively. Scale bar 50 μm. Bar chart (n) showing the cell migration rate (normalized to control) of primary cultured Schwann cells after treatment with different dosages of TNF-α. *p < 0.05 and **p < 0.01 versus control (non-treatment). (Color figure online)
The cell migration assay demonstrated that as compared to non-treatment, treatment with 2 or 5 ng/ml of TNF-α resulted in no significant change in the migration rate of primary Schwann cells, while treatment with 10, 20, or 40 ng/ml of TNF-α caused a significant decrease (Fig. 1h–n). Both the above results reinforce the previous findings about the dose-dependent dual effects of TNF-α on cell behaviors of primary Schwann cells.
Effects of TNF-α on cell morphology of primary Schwann cells
Transmission electron microscopy showed the cell morphology of primary Schwann cells after treatment with different dosages of TNF-α (Fig. 2). Primary Schwann cells treated with 2 or 5 ng/ml of TNF-α had no obvious change in their cell morphology as compared to untreated cells. In contrast, primary Schwann cells treated with 10, 20, or 40 ng/ml of TNF-α demonstrated some morphological features of apoptosis, as characterized by the condensation of nuclear chromatin, cytoplasmic blebbing and vacuolization, or the formation of a few apoptotic bodies (Fig. 2d–f). The cell apoptosis rate was significantly higher after treatment with 10, 20, or 40 ng/ml of TNF-α than that after non-treatment, while treatment with 2 or 5 ng/ml of TNF-α led to little change in the cell apoptosis rate (Fig. 2g).
Effects of different dosages of TNF-α on cell survival/apoptosis of primary cultured Schwann cells. Representative transmission electron micrographs (a–f) comparing the cell morphology of primary cultured Schwann cells after treatment with 0 (a), 2 (b), 5 (c), 10 (d), 20 (e), and 40 (f) ng/ml of TNF-α, respectively. Scale bar 2 μm. Solid and open arrows and an arrow head indicate the condensation of nuclear chromatin, cytoplasmic blebbing and vacuolization, or the formation of a few apoptotic bodies, respectively. Bar chart (g) showing the apoptosis rate of primary cultured Schwann cells after treatment with different dosages (0–40 ng/ml) of TNF-α. **p < 0.01 versus control (non-treatment)
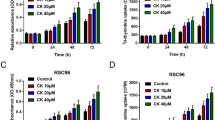
To confirm the dose-dependent dual effects of TNF-α on cell proliferation and apoptosis of primary Schwann cells, a chemical inhibitor of TNF-α was used to affect the cell behaviors in the presence of 2 or 40 ng/ml of TNF-α. Intriguingly, addition of a chemical inhibitor of TNF-α reduced cell proliferation as compared to treatment with 2 ng/ml TNF-α alone, but enhanced cell proliferation as compared to treatment with 40 ng/ml TNF-α alone (Fig. 3a), and the influences of a chemical inhibitor of TNF-α exhibited a concentration-dependent pattern. On the other hand, addition of a chemical inhibitor of TNF-α reduced cell apoptosis in a concentration-dependent manner as compared to treatment with 40 ng/ml TNF-α alone (Fig. 3b). Because 2 ng/ml TNF-α did not substantially affect cell apoptosis, the influences of a chemical inhibitor of TNF-α were not tested. All the results suggested that the effects of TNF-α on cell proliferation and apoptosis of primary Schwann cells could be alleviated through TNF-α inhibition.
Cell proliferation (a) and apoptosis (b) of primary cultured Schwann cells after treatments with different concentrations of a chemical inhibitor of TNF-α in the presence of 2 or 40 ng/ml of TNF-α. The cell proliferation or apoptosis rate was quantified by EdU incorporation or Annexin V-FTTC assay, respectively. Scale bar 50 μm (a, b). *p < 0.05 and **p < 0.01 versus control (treatment with 2 or 40 ng/ml of TNF-α alone)
Effects of TNF-α on protein expressions of caspase-7, -8, and -9 in primary Schwann cells
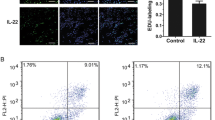
Western blot analysis revealed that protein expressions of cleaved caspase-7, -8, and -9 (activated forms) were changed in primary Schwann cells after treatment with different dosages of TNF-α. As compared to control (non-treated cells), primary Schwann cells treated with 2 or 5 ng/ml of TNF-α showed no significant changes in protein expression of cleaved caspase-7, -8, and -9 except for cleaved caspase-7 in the cells treated with 5 ng/ml of TNF-α, whereas primary Schwann cells treated with 10, 20, or 40 ng/ml of TNF-α induced significantly increased expressions of cleaved caspase-7, -8, and -9 (Fig. 4a). Immunocytochemistry provided further evidence that Schwann cells obviously expressed apoptosis-related factors, caspase-7, -8, and -9, following treatment with 40 ng/ml TNF-α (Fig. 4b), confirming the apoptosis-promoting functions of higher dosages of TNF-α in primary Schwann cells.
Effects of TNF-α on the expression of apoptosis-related molecules in primary cultured Schwann cells. a Bar chart showing the protein expression of cleaved caspase-7, -8, and -9 in primary cultured Schwann cells after treatment with different dosages of TNF-α, respectively. Also shown are representative Western blot images, in which β-actin served as a protein load control. b Immunostaining of primary cultured Schwann cells treated with 40 ng/ml of TNF-α with antibodies against cleaved caspase-7, -8, and -9 (green), or with anti-S100 β (red), and Hoechst 33342 staining (blue) of the cell nuclei. Also shown are the corresponding merges. Scale bar 50 μm. **p < 0.01 versus control (non-treatment). (Color figure online)
Effects of TNF-α on death- or survival-pathway in primary Schwann cells
To gain insights into the signaling events involved in the dual effects of TNF-α on primary Schwann cells, we performed co-immunoprecipitation experiments to investigate the protein interactions of TRADD (an adapter molecule) with either of two adaptor molecules, FADD or RIP. After pull-down with TRADD, Western blot analysis compared the expression level of FADD or RIP in Schwann cells treated with different dosages of TNF-α. Co-immunoprecipitation showed that either FADD or RIP was able to bind to TRADD and form a protein complex in primary Schwann cells. Western blot analysis demonstrated that the protein level of FADD bound to TRADD was elevated with increase in the dosage of added TNF-α; in contrast, the protein level of RIP bound to TRADD reached a maximum value when cells were treated with 2 ng/ml of TNF-α, and was then dramatically decreased when cells were treated with 5–40 ng/ml of TNF-α (Fig. 5a). Western blot analysis also revealed that the expression level of phosphorylated- (p-) JNK or p-NF-κB p65 changed in a fashion similar to that of FADD or RIP, respectively, in response to treatment with different dosages of TNF-α (Fig. 5b). It should be mentioned that the total protein level of TRADD, FADD, or RIP was found to be kept constant in primary Schwann cells irrespective of the dosages of added TNF-α (data not shown).
Signaling analysis for dual effects of TNF-α on primary cultured Schwann cells. Bar charts showing the protein level of FADD or RIP, which was bound to TNF receptor-associated death domain (TRADD), after primary cultured Schwann cells had been treated with different dosages of TNF-α and subjected to pull-down by TRADD (a), or the protein level of phosphorylated- (p-) JNK or p-NF-κB p65 (b). *p < 0.05 and **p < 0.01 versus control (non-treatment). Also shown are representative Western blot images, in which β-actin served as a protein load control
Discussion
Upon peripheral nerve injury, degeneration of damaged axons and myelin sheaths will occur in the injured nerve segment [16]. During nerve degeneration, Schwann cells first dedifferentiate and proliferate, and then redifferentiate and remyelinate newly grown axons in response to axon-derived signals, thus triggering a process of nerve regeneration [17]. Axonal myelination is of utmost importance for functional recovery of injured peripheral nerves, especially for rapid saltatory impulse conduction by allowing faster conduction velocity of action potentials [18, 19]. To better understand the orchestration of cell behaviors of Schwann cells, including cell proliferation, migration, and survival/apoptosis, during peripheral nerve injury and regeneration [20], we focused on the influences of multiple growth factors and cytokines on neural cells.
In this study, we used microarray and gene network analysis to determine the mRNA expression profile in injured nerve segments, and noticed that both pro- and anti-apoptosis genes in the injured nerves showed time-dependent expression patterns, and among them, the TNF-α expression was constantly altered during nerve regeneration. These analyses inspired us to investigate the possible effects of TNF-α on neural cells, exclusively on primary cultured Schwann cells, and further to explore the involvement of both pro- and anti-apoptosis signaling pathways in the effects of TNF-α.
To achieve these goals, we performed EdU incorporation and a transwell-based assay to, respectively, monitor the rate of proliferation and migration of primary cultured Schwann cells following treatment with different dosages of TNF-α. Since different cell behaviors are interwoven with each other, for instance, the cell proliferation or migration is usually linked to the cell susceptibility to apoptosis [21], we also observed and quantified cell apoptosis in primary cultured Schwann cells after treatment with different dosages of TNF-α. We noted that higher dosages (10, 20, and 40 ng/ml) of TNF-α enhanced the cell apoptosis of primary Schwann cells, while low dosages (2 and 5 ng/ml) of TNF-α induced less influences on cells. Obviously, the impacts of different dosages of TNF-α on the cell apoptosis were in parallel with those on the proliferation and migration. Collectively, these results were consistent with the previous finding [22], being suggestive of the dose-dependent dual effects of TNF-α on Schwann cells in vitro. The experiments using the TNF-α inhibitor confirmed the above observation.
Western blot analysis and immunocytochemistry indicated that treatment with higher dosages (10, 20, and 40 ng/ml) of TNF-α significantly increased the expression of cleaved caspase-7, -8, and -9 in primary Schwann cells. As is known, apoptosis is executed by a family of aspartate-specific cysteine proteases (caspases) which can be activated by various apoptogenic signals. Caspase family consists of initiator caspases (such as caspase-8, -9) and executioner caspases (caspase-3, -6, -7) in terms of their function and their sequence of activation [23]. The signaling pathways involving the activation of cleaved caspase-7, -8, and -9 are discussed below.
Accumulating evidence shows that TNF-α exerts its functions by binding to its cognate receptors TNFR1 and 2, two members of TNFR superfamily [24]. TNFR 1 and 2, respectively, mediate the majority of apoptotic or survival effects [25]. It has been known that TNFR1 trimerization induces the release from an inhibitory protein, called silencer of death domains which allows for the recruitment of TRADD, an adapter protein, followed by the recruitment of FADD, another adapter protein. These recruitments eventually lead to activation of caspase-8/10, even of caspase-3, -6, and -7. A subsequent pathway of death in primary Schwann cells is concomitantly initiated through TNFR-associated factor 2 (TRAF2) to TRADD, which up-regulates the expression of pro-apoptotic members of Bcl-2 family through the activation of ASK 1 and JNK or p38, thereby causing cell apoptosis [24–29].
Our experimental results concerning treatment of primary Schwann cells with higher dosages of TNF-α seemed to follow the pro-apoptotic cascade process, as evidenced by the up-regulation of FADD and p-JNK, which suggested the interaction of TRADD with FADD and the subsequent activation of JNK [24].
Despite the pro-apoptotic potential of TNF-α, researchers still suggest that TNF-α could mediate anti-apoptotic effects [30]. Due to the actions of TNFR1, TRADD is able to bind TRAF2 and another adaptor protein called RIP. Both TRAF2 and RIP promote cell survival by activating the NF-κB pathway, mainly by recruiting a protein kinase complex composed of NF-κB essential modulator, inhibitor κB (IκB) kinase (IKK)α and IKKβ. Activation of this complex activates the cytoplasmic NF-κB heterotrimer composed of p50, p65, and IκB. Specifically, the complex phosphorylates IκB and renders it for ubiquitination and thereby proteosomal degradation. As a result, the remaining NF-κB dimer is activated and translocates to the nucleus to transcribe numerous genes, among which a subset inhibits apoptosis [25, 26, 28, 29, 31].
Our experimental results concerning treatment of primary Schwann cells with lower dosages of TNF-α seemed to follow the anti-apoptotic cascade process, as evidenced by the up-regulation of RIP and p-NF-κB p65, which suggested the interaction of TRADD with RIP and the subsequent activation of NF-κB p65 [24].
We conceive that an antagonism or a balance may exist between the pro- and anti-apoptotic actions of TNF-α when TNF-α is used to stimulate primary Schwann cells, and the net result of these two opposite actions may depend on the dosage of TNF-α used.
In summary, based on the information provided by gene array analysis, we tested and confirmed that TNF-α induced dose-dependent dual effects on the cell behaviors of primary cultured Schwann cells, including cell proliferation, migration, and survival/apoptosis. To understand how TNF-α could act as a pleiotropic cytokine during peripheral nerve injury, we performed co-immunoprecipitation, Western blot analysis, and immunocytochemistry to decipher the complex network of biochemical pathways involving signaling molecules, such as TRADD, FADD, RIP, JNK, NF-κB p65, and caspase-7, -8, and -9.
References
Joung YK, Bae JW, Park KD (2008) Controlled release of heparin-binding growth factors using heparin-containing particulate systems for tissue regeneration. Expert Opin Drug Del 5:1173–1184
Akassoglou K, Yu WM, Akpinar P, Strickland S (2002) Fibrin inhibits peripheral nerve remyelination by regulating Schwann cell differentiation. Neuron 33:861–875
Gumy LF, Bampton ETW, Tolkovsky AM (2008) Hyperglycaemia inhibits Schwann cell proliferation and migration and restricts regeneration of axons and Schwann cells from adult murine DRG. Mol Cell Neurosci 37:298–311
Chen YY, McDonald D, Cheng C, Magnowski B, Durand J, Zochodne DW (2005) Axon and Schwann cell partnership during nerve regrowth. J Neuropathol Exp Neurol 64:613–622
Lino MM, Atanasoski S, Kvajo M, Fayard B, Moreno E, Brenner HR, Suter U, Monard D (2007) Mice lacking protease nexin-1 show delayed structural and functional recovery after sciatic nerve crush. J Neurosci 27:3677–3685
Wagner R, Myers RR (1996) Schwann cells produce tumor necrosis factor alpha: expression in injured and non-injured nerves. Neuroscience 73:625–629
Mulleman D, Mammou S, Griffoul I, Watier H, Goupille P (2006) Pathophysiology of disk-related low back pain and sciatica. II. Evidence supporting treatment with TNF-α antagonists. Joint Bone Spine 73:270–277
Schäfers M, Geis C, Brors D, Yaksh TL, Sommer C (2002) Anterograde transport of tumor necrosis factor-α in the intact and injured rat sciatic nerve. J Neurosci 22:536–545
Pollheimer J, Knöfler M (2005) Signalling pathways regulating the invasive differentiation of human trophoblasts: a review. Placenta 26:S21–S30
Boyle K, Azari MF, Cheema SS, Petratos S (2005) TNF [alpha] mediates Schwann cell death by upregulating p75NTR expression without sustained activation of NF [kappa] B. Neurobiol Dis 20:412–427
Wang Y, Tang X, Yu B, Gu Y, Yuan Y, Yao D, Ding F, Gu X (2012) Gene network revealed involvements of Birc2, Birc3 and Tnfrsf1a in anti-apoptosis of injured peripheral nerves. PLoS ONE 7:e43436
Tao T, Ji Y, Cheng C, Yang H, Liu H, Sun L, Qin Y, Yang J, Wang H, Shen A (2009) Tumor necrosis factor-alpha inhibits Schwann cell proliferation by up-regulating Src-suppressed protein kinase C substrate expression. J Neurochem 111:647–655
Wright GW, Simon RM (2003) A random variance model for detection of differential gene expression in small microarray experiments. Bioinformatics 19:2448–2455
Brockes JP, Fields KL, Raff MC (1979) Studies on cultured rat Schwann cells. I. Establishment of purified populations from cultures of peripheral nerve. Brain Res 165:105–118
Mantuano E, Inoue G, Li X, Takahashi K, Gaultier A, Gonias SL, Campana WM (2008) The hemopexin domain of matrix metalloproteinase-9 activates cell signaling and promotes migration of Schwann cells by binding to low-density lipoprotein receptor-related protein. J Neurosci 28:11571–11582
Mirsky R, Jessen KR (2001) Embryonic and early postnatal development of Schwann cells. In: Jessen KR, Richardson WD (eds) Glial cell development: basic principles and clinical relevance. Oxford University Press, Oxford, pp 1–20
Harrisingh MC, Perez-Nadales E, Parkinson DB, Malcolm DS, Mudge AW, Lloyd AC (2004) The Ras/Raf/ERK signalling pathway drives Schwann cell dedifferentiation. EMBO J 23:3061–3071
Mirsky R, Parmantier E, McMahon AP, Jessen KR (1999) Schwann cell-derived desert Hedgehog signals nerve sheath formation. Ann N Y Acad Sci 883:196–202
Chen ZL, Strickland S (2003) Laminin γ1 is critical for Schwann cell differentiation, axon myelination, and regeneration in the peripheral nerve is critical for Schwann cell differentiation, axon myelination, and regeneration in the peripheral nerve. J Cell Biol 163:889–899
Yoshifumi T, Martin K (2011) Axonal outgrowth is associated with increased ERK 1/2 activation but decreased caspase 3 linked cell death in Schwann cells after immediate nerve repair in rats. BMC Neurosci 12:12. doi:10.1186/1471-2202-12-12
Joy AM, Beaudry CE, Tran NL, Ponce FA, Holz DR, Demuth T, Berens ME (2003) Migrating glioma cells activate the PI3-K pathway and display decreased susceptibility to apoptosis. J Cell Sci 116:4409–4417
Yuan Q, Yang H, Cheng C, Li C, Wu X, Huan W, Sun H, Zhou Z, Wang Y, Zhao Y, Lu X, Shen A (2012) Beta-1,4-galactosyltransferase I involved in Schwann cells proliferation and apoptosis induced by tumor necrosis factor-alpha via the activation of MAP kinases signal pathways. Mol Cell Biochem 365:149–158
Thornberry NA, Lazebnik Y (1998) Caspases: enemies within. Science 281:1312–1316
Profyris C, Cheema SS, Zang DW, Azari MF, Boyle K, Petratos S (2004) Degenerative and regenerative mechanisms governing spinal cord injury. Neurobiol Dis 15:415–436
Gupta S (2002) A decision between life and death during TNF-alpha-induced signaling. J Clin Immunol 22:185–194
Chen G, Goeddel DV (2002) TNF-R1 signaling: a beautiful pathway. Sci Signal 296:1634
Harris CA, Johnson EM Jr (2001) BH3-only Bcl-2 family members are coordinately regulated by the JNK pathway and require Bax to induce apoptosis in neurons. J Biol Chem 276:37754–37760
Gupta S (2002) Tumor necrosis factor-alpha-induced apoptosis in T cells from aged humans: a role of TNFR-I and downstream signaling molecules. Exp Gerontol 37:293–299
Waiwut P, Shin MS, Inujima A, Zhou Y, Koizumi K, Saiki I Sakurai H (2011) Gomisin N enhances TNF-α-induced apoptosis via inhibition of the NF-κB and EGFR survival pathways. Mol Cell Biochem 350:169–175
Kim GM, Xu J, Song SK, Yan P, Ku G, Xu XM, Hsu CY (2001) Tumor necrosis factor receptor deletion reduces nuclear factor-kappaB activation, cellular inhibitor of apoptosis protein 2 expression, and functional recovery after traumatic spinal cord injury. J Neurosci 21:6617–6625
Yin X, Krikorian P, Logan T, Csizmadia V (2010) Induction of RIP-2 kinase by proinflammatory cytokines is mediated via NF-kB signaling pathways and involves a novel feed-forward regulatory mechanism. Mol Cell Biochem 333:251–259
Acknowledgments
We thank Professor Jie Liu for assistance in manuscript preparation. This study was supported by National Natural Science Foundation of China (Grant Nos. 81130080, 81000678, and 81171457) and the Priority Academic Program Development of Jiangsu Higher Education Institutions (PAPD).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tang, X., Wang, Y., Zhou, S. et al. Signaling pathways regulating dose-dependent dual effects of TNF-α on primary cultured Schwann cells. Mol Cell Biochem 378, 237–246 (2013). https://doi.org/10.1007/s11010-013-1614-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-013-1614-x