Abstract
Remodeling by its very nature implies synthesis and degradation of extracellular matrix components (such as elastin, collagen, and connexins). Most of the vascular matrix metalloproteinase (MMP) are latent because of the presence of constitutive nitric oxide (NO). However, during oxidative stress peroxinitrite (ONOO–) activates the latent MMPs and instigates vascular remodeling. Interestingly, in mesenteric artery, homocysteine (Hcy) decreases the NO bio-availability, and folic acid (FA, an Hcy-lowering agent) mitigates the Hcy-mediated mesentery artery dysfunction. Dimethylarginine dimethylaminohydrolase-2 (DDAH-2) and endothelial nitric oxide synthase (eNOS) increases NO production. The hypothesis was that the Hcy decreased NO bio-availability, in part, activating MMP, decreasing elastin, DDAH-2, eNOS and increased vasomotor response by increasing connexin. To test this hypothesis,the authors used 12-week-old C57BJ/L6 wild type (WT) and hyperhomocysteinemic (HHcy)-cystathione beta synthase heterozygote knockout (CBS+/−) mice. Blood pressure measurements were made by radio-telemetry. WT and MMP-9 knockout mice were administered with Hcy (0.67 mg/ml in drinking water). Superior mesenteric artery and mesenteric arcade were analyzed with light and confocal microscopy. The protein expressions were measured by western blot analysis. The mRNA levels for MMP-9 were measured by RT-PCR. The data showed decreased DDAH-2 and eNOS expressions in mesentery in CBS−/+ mice compared with WT mice. Immuno-fluorescence and western blot results suggest increased MMP-9 and connexin-40 expression in mesenteric arcades of CBS−/+ mice compared with WT mice. The wall thickness of third-order mesenteric artery was increased in CBS−/+ mice compared to WT mice. Hcy treatment increased blood pressure in WT mice. Interestingly, in MMP-9 KO, Hcy did not increase blood pressure. These results may suggest that HHcy causes mesenteric artery remodeling and narrowing by activating MMP-9 and decreasing DDAH-2 and eNOS expressions, compromising the blood flow, instigating hypertension, and acute abdomen pain.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Clinical studies has shown that the increased homocysteine (Hcy) levels are a significant risk factor for cardiovascular disease, stroke, and mesenteric thrombosis [1, 2]. Hcy is auto-oxidized to reactive oxygen species (ROS), causing inflammatory response leading to endothelial dysfunction. Hcy greatly affects NO bioproduction and NO bioavailability [3]. Hyperhomocysteinemia (HHcy) affects responsiveness of both vascular smooth muscle and endothelium to vasomotor agonists [4].Vasomotor alterations and systemic redistribution of the blood flow, are known to have a crucial role in the development of progressive organ dysfunction [4, 5].
Connexins play a critical role in providing a conduit for the membrane structures, which permits direct intercellular passage of ions and small molecules, and which plays a role both in electrical coupling and intercellular communication during patterning and development. Also, connexins contribute to the maintenance and modulation of vasomotor tone [6]. Connexin-40 is essentially required for normal transmission of endothelium-dependent vasodilator response [7]. Interestingly, Connexin-40 promoter polymorphism has been associated with an increased risk of hypertension in men [8, 9].
High plasma Hcy levels induce a reduction in arterial distensibility and compliance [10]. Previous studies of our lab showed that Hcy causes constrictive vascular remodeling, and hence causes narrowing of arteriolar/artery lumen [11]. Hcy levels are independently associated with increased arterial wall thickness [12–14]. MMPs involved in Hcy induced vascular remodeling and further caused ECM proteolysis, and myoendothelial uncoupling [15, 16]. Hcy-induced activation of latent MMP has been previously shown, and it causes increased oxidative stress (ROS and nitrotyrosine) by differential expressions of Thioredoxin, Nox1, and NOS in MVEC [23]. The chronic exposure of blood vessels to homocysteine causes disruption elastic laminae, and hence causes elastinolysis [17]. Also, Hhcy causes endothelial nitric oxide synthase dysfunction. This can further be explained by dimethylarginine dimethylaminohydrolase (DDAH), an enzyme involved in the regulation of nitric oxide synthase (NOS) by metabolizing the free endogenous arginine derivatives N(omega)-methyl-l-arginine (MMA) and N(omega),N(omega)-dimethyl-l-arginine (ADMA) [18]. Interestingly, DDAH expression in the vasculature was found to colocalize at all sites of expression isoform of NOS [19]. Furthermore, tissue-specific downregulation of DDAH in HHcy has been reported [18]. Hcy interferes with methylation modification of DDAH-2 gene resulting in elevation of ADMA [20]. Consequently, this ADMA further competively inhibits eNOS, and hence decreases bio-availability of NO [21].
The authors hypothesize that Hcy decreases NO bio-availability, in part, by activating MMP, decreasing elastin, DDAH-2, eNOS, and increases vasomotor response by increasing connexins in mesenteric vasculature, HHcy causes thickening superior mesenteric artery which may affect the distensibility.
Methods
Antibodies and reagents
Rabbit polyclonal antibodies to MMP-2, MMP-9, and eNOS were purchased from Abcam (Cambridge, MA), rabbit polyclonal antibodies to DDAH-2, connexin-40, and 43 were purchased from Chemicon. GAPDH antibody and other analytical reagents were from Sigma-Aldrich (St. Louis, MO). Horseradish peroxidase-linked anti-rabbit IgG antibody was from Santa Cruz Biotechnology (Santa Cruz, CA). PVDF membrane was from Bio-Rad (Hercules, CA).
Animal model
Male C57BL/6 J wild-type mice (8–10-wk old) and heterozygous CBS (+/−) a model for Hhcy, were obtained from Jackson Laboratory (Bar Harbor, ME) WT (C57BL/6 J), and kept in the animal care facility of University of Louisville where ambient environmental conditions (12:12-h light:dark cycle, 22–24°C) were maintained. The animals were fed standard chow and water ad libitum. All animal procedures were reviewed and approved by the Institutional Animal Care and Use Committee of the University of Louisville, School of Medicine in accordance with animal care and use program guidelines of the National Institutes of Health.
Blood pressure
For blood pressure measurements by radio-telemetry, animals were divided into four groups: WT group, Male C57BL/6 J wild-type mice (8–10-week old) were given drinking water; Hcy group, Male C57BL/6 J wild-type(4–5-week old) were given homocysteine in drinking water for 6–8-weeks; MMP-9 group, MMP-9 knock out mice given; MMP-9 knockout mice were administered Hcy (0.67 mg/ml) in drinking water. Direct radiotelemetric measurements of systolic/diastolic blood pressure were measured continuously during the experiment with a DSI (Data Sciences International; St.Paul, MN) telemetric system using a pressure transducer (PA-C20) surgically implanted into the aortic arch through the left common carotid artery as we described previously [22], starting after 1-week surgical recovery period. The data were analyzed with DSI Dataquest ART 3.1software.
Video microscopy and digital image processing
A Nikon Diaphot 200 inverted microscope optimized was utilized. Observations were made with a Nikon fluorite ×20 (numerical aperture = 0.75) objective and/or a Nikon fluorite oil × 40 objective (numerical aperture = 1.30–0.80). A multi-image module (beam-splitting device) was connected to Hamamatsu intensified CCD camera system. Mesenteric third-order artery diameter and wall thickness were measured on-line with a video caliper device.
Cryosectioning
The mesenteric tissue was excised, cryopreserved in Peel-A-Way disposable plastic tissue-embedding molds (Polysciences, Warrington, PA) containing tissue-freezing media (Triangle Biomedical Sciences, Durham, NC). These molds were kept frozen (–70°C) until serial 5-μm tissue sections were made in Cryocut 1800 (Reichert-Jung). Cryosections were placed on Superfrost/plus microscope slides and air dried.
Immunoflourescence
Immunofluorescence staining was performed on 5-μm thick frozen sections of the superior mesenteric artery. Anti-connxin-40, 43, eNOS, and anti-MMP-2, secondarily conjugated with Texas Red (Chemicon International, St. Charles, MO) were used for immunodetection of these two proteins, respectively.
Western blot analyses of MMP-2, & 9, DDAH-2, eNOS, Connexin-40
Western blot analyses were performed on mesenteric tissue homogenates using 10% SDS-PAGE. BCA method was used to estimate total protein, and 25 μg of protein was loaded in each well of electrophoresis gels. After electrophoresis, proteins were transferred to polyvinylidene difluoride membrane (PVDF), blocked with 5% fat-free milk, and blotted with respective antibodies. As a loading control, GAPDH was used. The bands were normalized with GAPDH controls.
In situ Zymography
MMP activity in the media and intima of frozen mesenteric sections was measured by in situ zymography using a gelatinolytic fluorogenic substrate. Vessel sections were incubated in dark humidified chambers with 1.0 μg/ml DQ gelatin in Tris–CaCl2 Buffer for 1 h. The sections were examined using confocal microscope, and the image was captured at 60× magnification. The proteolytic activity was detected as bright green fluorescence, which indicates gelatin breakdown, which was quantified using the Image Pro software. The gelatinolytic activity was assessed by quantifying the intensity of green fluorescence from ten fields selected around the vessel circumference. Phenanthroline at 0.1 mmol l−1 inhibited MMPs activity in the mesenteric sections served as negative control.
RNA isolation and expression study
Total RNA from the mouse mesenteric arcade was isolated using Trizol Reagent (Gibco BRL) according to the instructions provided by the manufacturer. The cDNA was prepared using the Promega kit. The reverse transcription program was 25°C for 10 min, 42°C for 50 min, and then 70°C for 15 min. PCR was performed using 2 μl of each RT product (cDNA), with a total reaction volume of 20 μl. The PCR thermalcycle was 94°C for 6 min, 35 cycles at 94°C for 50 s, 60°C for 1 min, and 72°C for 1 min, finally 72°C for 10 min, which gives a product of ~320 bp. Primers for GAPDH (116 bp product) were sense (5-GATGCAGGGATGATGTTCTG-3) and antisense (5-ACAACTTTGGCATTGTGGAA-3). The PCR thermal cycle for GAPDH was 94°C for 2 min,30 cycles at 94°C for 30 s, 57°C for 30 s, and 72°C for 1 min, finally 72°C for 2 min. All of the primers were obtained from Invitrogen (Carlsbad, CA).
Nitrite assay
NO metabolites such as nitrite production was measured fluorimetricaly using commercially available kit from Biovision. Results expressed as nanomole of nitrite produced per mg of protein.
Statistical analysis
All data are expressed as mean ± SE. Data were analyzed using a one-way analysis of variance (ANOVA) to test for treatment effect. The level of significance was accepted at P < 0.05.
Results
Mesenteric remodeling
In Fig. 1, tissue elastin in WT mesenteric artery appeared to be more when compared to CBS+/− SMA. This suggested greater distensibility in the WT than CBS+/− mouse mesentery. Severe elastin breakdown and irregularities in the smooth muscle layer as observed in the histological section of SMA from CBS+/−. This suggested remodeling in mesenteric artery. Videomicroscopic data revealed significant increase (P ≤ 0.05) in third-order mesenteric artery wall thickness in CBS−/+ mice than WT mice (Fig. 2b). This may suggest that CBS−/+ mesenteries are more prone to become stiffer and further priming these to ischemic events than the mesenteries from WT mice.
Histological analysis of frozen superior mesenteric artery (SMA) from wild type (a) and CBS+/− mice (b), stained with van Gieson for elastin. Images were visualized using light microscopy and Q capture software. Note: the non uniform smooth muscle layer as well as thinning of the elastin lamina in CBS+/− SMA. (c) Bar graph presentation of quantification of elastin using image-pro software. The y-axis represents arbitrary scan unit (n = 4 in each group); * P < 0.05 compared to WT control
Histological analysis with H and E staining of frozen superior mesenteric artery (SMA) from wild type (a) and CBS+/− (b) mice, respectively, showing increased lamilar thickness of SMA in CBS+/− mice compared to WT mice. (c) Graph showing Mesenteric 3rd order artery wall thickness, measured using video caliper Nikon Diaphot 200 inverted microscope from WT and CBS+/− mice. Values are mean ± SEM. n = 4 in each animal group; * P < 0.05 compared to WT control
To determine whether the decrease in elastin in CBS−/+ mesentery is due to increase in metalloproteinases,the authors measured elastinolytic MMP-2 and -9. The results suggested that although there was the tendency to increase in MMP-2, MMP-9 was robust in CBS−/+ mesentery than WT mesentery (Fig. 3). These results support the concept that MMP-2 is constitutively expressed, and which plays a constitutive role by increase in during compensatory remodeling. However, MMP-9 is inducible and detrimental and activated during pathological remodeling in HHcy. Furthermore, the authors checked gelatinolytic activity of MMPs using in situ zymography (Fig. 4). Micrograph from normal vessels (Fig. 4a) showed no gelatinolytic activity (green) (arrows). However, there was increased gelatinolytic activity (green) in CBS+/− HHcy vessel (Fig. 4b). In addition, quantification using image pro software corroborated respective results (Fig. 4d).
Effect of Hcy on MMP-2 protein (a) MMP-9 protein (b) and MMP-9 mRNA (c) in mesenteric tissue. The protein was blotted with MMP-2, -9 and GAPDH antibodies. The mRNA was amplified using MMP-9 and GAPDH primers. The bands for MMP-2 and MMP-9 expression were quantified using densitometry and expressed fold change from wild type. The bar graphs represent MMP over GAPDH expression. Values are mean ± SEM. n = 4 in each animal group; * P < 0.05 compared to WT control
a Western Blot analysis of connexin-40 in tissue lysate from mesenteric arcade. The bar graphs represent and connexin-40 expression over GAPDH. Values are mean ± SEM. n = 4 in each animal group; * P < 0.05 compared to WT control. b Connexin-40 labeling in WT mesentery using immunofluorescence; c connexin-40 labeling in CBS−/+ mesentery; and d negative control using secondary antibody, without connexin-40 antibody
The cell–cell connexins are involved in endothelial cells as well as smooth muscle cells. The authors measured the levels of connexin-40, connexin-43 in SMA sections using immunofluorecence. The result suggests increase in connexin-40, 43 levels in CBS−/+ mesentery than WT (Figs. 5b–e, 6a–d). These results may indicate the increase in gap junction communication in CBS−/+ mesentery than WT. This may explain why Hhcy arteries are more prone to become hypertrophied (Fig. 6).
Immunohistochemical staining using an antibody against connexin-43 in SMA sections from a: WT C57BL/6 J mice; b from CBS+/− mice; c negative control using secondary antibody, without connexin-40 antibody. d Bar graph presentation of quantification of connexin-43 per unit area using image-pro software. Values are mean ± SEM. n = 4 in each animal group; * P < 0.05 compared to WT control
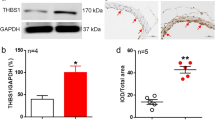
Effects of Hcy on the expression of dimethylarginine dimethylaminohydrolase (DDAH-2) in the mesenteric tissue. Results are presented as the mean ± SEM (n = 4). a Immunohistochemical staining with the use of an antibody against DDAH-2 protein showing SMA sections from WT C57BL/6 J mice; b from CBS+/− mice. c Immuno-blots of mesenteric arcade from WT and CBS−/+ mice. Note: abundant DDAH-2 positive cells in the medial layer of the SMA from C57BL/6 J WT mice than CBS−/+ mice
Levels of DDAH-2 and eNOS
To examine the effect of Hhcy on the production and bio-availability of NO in mesenteric arcade as well as SMA, the authors measured DDAH-2 and eNOS levels. The immunohistochemistery data showed abundant expressions of DDAH-2 in SMA sections from C57BL/6 J mice when compared to CBS+/− mice (Fig. 7a, b). DDAH-2 expression was down regulated as can be seen in immunoblots from mesenteric tissue from CBS+/− mice (Fig. 7c). The similar results were obtained for eNOS expression (Fig. 8).
Effects of homocysteine on the expression of endothelial nitric oxide synthase (eNOS) in mesenteric tissue: a Fluorescence immunohistochemical assays for eNOS in SMA sections from C57BL/6 J WT; b CBS+/− mice; and c negative control without primary antibody. All panels are representative of three independent experiments. d Western Blot analysis of eNOS in tissue lysate from mesenteric arcade of C57BL/6 J and CBS+/− mice. Bars are mean ± SEM (n = 4)
Blood pressure (BP) measurement using telemetric DSI system in real time. WT, C57BL/6 J mice treated with vehicle; Hcy, C57BL/6 J mice treated with homocysteine; MMP-9, MMP-9 knock out mice treated with vehicle; MMP9 + Hcy, MMP-9 knock out mice treated with Homocysteine. Values are means ± SE; n = 4 animals in each group. * P < 0.05 Systolic BP compared to WT control. # P < 0.05, Diastolic BP compared to WT control
Arterial blood pressure, systolic and diastolic, in the Hcy-treated group was significantly greater than in WT controls. Also, pulse pressure, the difference between systolic and diastolic blood pressures was more in comparison with WT controls. Interestingly, this increase was attenuated in MMP-9 knockout mice, when treated with Hcy (Fig. 9).
Mesenteric sections show MMP-2 and -9 activity using in situ zymography: Cryosections were incubated with DQ-gelatin-FITC substrate for 3 h. a Representative micrograph shows no gelatinolytic activity (green) in normal vessels (arrows) b Representative micrograph shows increase in gelatinolytic activity (green) in CBS+/− HHcy vessels (arrows) c Using MMPs inhibitor (phenanthroline) as a negative control d Quantification using image pro software revealed a two- to four-fold increase in MMP activity in CBS−/+ mouse vessels (* P < 0.05, n = 5 animals/group). (Color figure online)
Levels of nitrite
To elucidate the role of homocysteine in NO bio-availability, the authors measured NO metabolite nitrite levels in mesenteric arcade as well as plasma. The graph (Fig. 10) shows the decreased NO metabolite levels in mesenteric tissue as well as plasma samples of CBS+/− mice when compared with control.
Discussion
Hcy depletes folic acid that leads to depletion of tetrahydrobiopterin, an essential co-factor of eNOS, thereby causing uncoupling of eNOS and decreasing bio-availability of NO, therefore, activates MMP-9 and connexin-40, leading to vascular remodeling and hypertension [23]. To substantiate the hypothesis that Hcy decreases NO bio-availability by activating MMP, decreasing elastin, DDAH-2, eNOS and increases vasomotor response by increasing connexin, and to provide a cause-effect relationship between down regulation of eNOS and MMP-9 activation in CBS+/− mice, the authors measured metabolites of NO (nitrite) in mesentery vasculature as well as in plasma (Fig. 10). This delineates the role of NO in modulating MMP activities and vascular remodeling and addresses the detrimental effect of Hcy in mesenteric vasculature of CBS−/+ mice.
Pathological vascular remodeling of mesenteric arteries leads to endothelial dysfunction and also wall thickening. Interestingly, blockade of angiotensin-2 receptor causes receptor decreased MMP activity and increased elastin content in small mesenteric arteries [23]. Furthermore, HHcy is associated with smooth muscle cell proliferation by activating cyclin-dependent kinases [24].
In this article showed elastin degradation in superior mesenteric arteries. Also, further evidences indicate altered properties of the elastin network in arteries cultured with physiological and pathological concentrations of homocysteine [25]. Moreover, long-term elevated blood pressure causes cellular and matrix “remodeling” in mesenteric vessels [26]. Mild hyperhomocysteinemia is associated with stiffer and smaller arteries with increased collagen deposition in the media [12]. Also, a linear correlation between Hcy levels and systolic hypertension was demonstrated previously [27]. There has been a direct connection between aortic wall thickness and plasma Hcy levels [28].
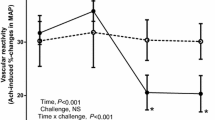
Symon et al. [29] showed Hhcy produced dysfunction in mesenteric circulation, and also showed low folate diet associated with compromised in mesenteric vasculature function. Interestingly, folic acid and magnesium decrease Hcy-induced MMP secretion [30]. Previous studies have shown in CBS+/− (mild Hhcy model) endothelium-dependent vasodilator function was decreased in mesenteric arterioles and was associated with an increased in expression of P-selectin, indicating inflammation [31]. In addition, Hhcy exposure resulted in impaired vascular reactivity of the superior mesenteric artery to the endothelium-dependent vasodilators acetylcholine, but not to the endothelium-independent vasodilator sodium nitroprusside [19].
The authors have shown Hhcy induces a decline in eNOS and DDAH-2 expressions in mesenteric arcade as well as SMA. It is consistent with the previous report that DDAH-2 expression is required for EDRF/NO responses in mesenteric vessels [32]. DDAH may play an important role in the regulation of extravillous trophoblast function via its effects on ADMA and NO productions [4]. DDAH plays a pivotal role in maintenance of endothelial function and is also a potential target for treating diseases associated with decreased NO bio-availability [33, 34].
A critical role of connexin-40 inhibition in EDHF (endothelium-derived hyperpolarizing factor)-mediated dilation of rat mesenteric arteries [35]. In addition, Cx40 is essentially required for normal transmission of endothelium-dependent vasodilator response [18]. Hence, Cx40 plays a crucial role in maintaining vasomotor tone. In this article, the authors showed elevated connexin-40, 43 expression in HHcy mesenteric tissue which is consistent with previous findings showing Hcy-induced upregulation of Cx43 transcript in HUVEC [36, 37]. On the contrary, some other authors have shown down regulation of connexin-40 in endothelial cells of the HHcy rat [12]. This suggests differential heterogeneity in connexins isoform in various vasculatures in HHcy. The results of this study show for the first time Hcy-induced MMP-9 activation in mesenteric vasculature. Altered vascular reactivity in mesenteric arteries from hypertensive mice due to vascular hypertrophy has been suggested [38]. Also, altered vasomotor function and systemic redistribution of the blood flow, have been suggested to play a crucial role in the development of progressive organ dysfunction [4, 5].
Reports from the authors lab showed Hcy associated thickening of the aortic wall, and hence causes constrictive remodeling in arteries [22, 39]. Interestingly, a marked thickening of intima and media in the mesenteric arterioles of hypertensive rats was observed [40]. Also, one of the major findings in the present study, showed elevated blood pressure in HHcy mice which was decreased in MMP-9 KO mice treated with Hcy. Moreover, pressure alone stimulates wall stress as well as protooncogene expression in mesenteric arteries [41]. This further contributes toward stress, one of the signaling parameter and other cascade events in hypertension when arteries are tonically constricted. In previous reports showed distinct temporal and mechanistic responses to hypertensive injury in different vascular beds, which is indicative of differential susceptibility of organs to a hypertensive stimulus with mesentery and heart, exhibiting the greatest sensitivity to damage [42]. Furthermore, Hcy-mediated endothelial dysfunction can be ameliorated by peroxisome proliferator-activated receptor (PPAR) agonists [43].
In summary, the results of this study suggests that the Hcy-induced arterial hypertension leads to mesenteric arterial remodeling, mediated by MMPs and connexin’s activation, elastin degradation, dowregulation of DDAH-2, eNOS which may be attenuated in MMP-9 KO mice treated with homocysteine. Moreover, the authors previously reported the role of negative and positive remodelings in vascular diseases. Because the associated mechanism is yet obscure, further research is required to gain new insights into homocysteine induced negative remodeling in mesenteric arteries and the roles of different connexins isoforms.
References
Gradman WS, Daniel J, Miller B, Haji-Aghaii M (2001) Homocysteine-associated acute mesenteric artery occlusion treated with thrombectomy and bowel resection. Ann Vasc Surg 15(2):247–250
Alexander T, Rajnish R, Balakrishnan R, Shallam JF (2005) Hyperhomocysteinemia presenting as superior mesenteric artery thrombosis. Indian J Gastroenterol 24(2):78–79
Fu WY, Dudman NP, Perry MA, Wang XL (2002) Homocysteine attenuates hemodynamic responses to nitric oxide in vivo. Atherosclerosis 161(1):169–176
Chen C, Conklin BS, Ren Z, Zhong DS (2002) Homocysteine decreases endothelium-dependent vasorelaxation in porcine arteries. J Surg Res 102(1):22–30
Turini GA (1983) [Physiopathology of the state of shock]. Schweiz Med Wochenschr 113(33):1118–1123
Christ GJ, Brink PR, Zhao W, Moss J, Gondre CM, Roy C et al (1993) Gap junctions modulate tissue contractility and alpha 1 adrenergic agonist efficacy in isolated rat aorta. J Pharmacol Exp Ther 266(2):1054–1065
de Wit C, Roos F, Bolz SS, Kirchhoff S, Kruger O, Willecke K et al (2000) Impaired conduction of vasodilation along arterioles in connexin40-deficient mice. Circ Res 86(6):649–655
Firouzi M, Kok B, Spiering W, Busjahn A, Bezzina CR, Ruijter JM et al (2006) Polymorphisms in human connexin40 gene promoter are associated with increased risk of hypertension in men. J Hypertens 24(2):325–330
Grayson TH (2006) Is Cx40 a marker for hypertension? J Hypertens 24(2):279–280
Arcaro G, Fava C, Dagradi R, Faccini G, Gaino S, Degan M et al (2004) Acute hyperhomocysteinemia induces a reduction in arterial distensibility and compliance. J Hypertens 22(4):775–781
Mujumdar VS, Tummalapalli CM, Aru GM, Tyagi SC (2002) Mechanism of constrictive vascular remodeling by homocysteine: role of PPAR. Am J Physiol Cell Physiol 282(5):C1009–C1015
Neves MF, Endemann D, Amiri F, Virdis A, Pu Q, Rozen R et al (2004) Small artery mechanics in hyperhomocysteinemic mice: effects of angiotensin II. J Hypertens 22(5):959–966
Smilde TJ, van den Berkmortel FW, Boers GH, Wollersheim H, de Boo T, van Langen H et al (1998) Carotid and femoral artery wall thickness and stiffness in patients at risk for cardiovascular disease, with special emphasis on hyperhomocysteinemia. Arterioscler Thromb Vasc Biol 18(12):1958–1963
Voutilainen S, Alfthan G, Nyyssonen K, Salonen R, Salonen JT (1998) Association between elevated plasma total homocysteine and increased common carotid artery wall thickness. Ann Med 30(3):300–306
Moshal KS, Tyagi N, Henderson B, Ovechkin AV, Tyagi SC (2005) Protease-activated receptor and endothelial-myocyte uncoupling in chronic heart failure. Am J Physiol Heart Circ Physiol 288(6):H2770–H2777
Tyagi N, Moshal KS, Lominadze D, Ovechkin AV, Tyagi SC (2005) Homocysteine-dependent cardiac remodeling and endothelial-myocyte coupling in a 2 kidney, 1 clip Goldblatt hypertension mouse model. Can J Physiol Pharmacol 83(7):583–594
Tummalapalli CM, Tyagi SC (1999) Responses of vascular smooth muscle cell to extracellular matrix degradation. J Cell Biochem 75(3):515–527
Dayal S, Rodionov RN, Arning E, Bottiglieri T, Kimoto M, Murry DJ et al (2008) Tissue-specific downregulation of dimethylarginine dimethylaminohydrolase in hyperhomocysteinemia. Am J Physiol Heart Circ Physiol 295(2):H816–H825
Tojo A, Welch WJ, Bremer V, Kimoto M, Kimura K, Omata M et al (1997) Colocalization of demethylating enzymes and NOS and functional effects of methylarginines in rat kidney. Kidney Int 52(6):1593–1601
Zhang JG, Liu JX, Li ZH, Wang LZ, Jiang YD, Wang SR (2007) Dysfunction of endothelial NO system originated from homocysteine-induced aberrant methylation pattern in promoter region of DDAH2 gene. Chin Med J (Engl) 120(23):2132–2137
Stuhlinger MC, Tsao PS, Her JH, Kimoto M, Balint RF, Cooke JP (2001) Homocysteine impairs the nitric oxide synthase pathway: role of asymmetric dimethylarginine. Circulation 104(21):2569–2575
Ovechkin AV, Tyagi N, Sen U, Lominadze D, Steed MM, Moshal KS et al (2006) 3-Deazaadenosine mitigates arterial remodeling and hypertension in hyperhomocysteinemic mice. Am J Physiol Lung Cell Mol Physiol 291(5):L905–L911
Brassard P, Amiri F, Schiffrin EL (2005) Combined angiotensin II type 1 and type 2 receptor blockade on vascular remodeling and matrix metalloproteinases in resistance arteries. Hypertension 46(3):598–606
Lubec B, Labudova O, Hoeger H, Muehl A, Fang-Kircher S, Marx M et al (1996) Homocysteine increases cyclin-dependent kinase in aortic rat tissue. Circulation 94(10):2620–2625
Samouillan V, Lamy E, Dandurand J, Foucault-Bertaud A, Chareyre C, Lacabanne C et al (2010) Changes in the physical structure and chain dynamics of elastin network in homocysteine-cultured arteries. J Biomed Mater Res A 93(2):696–703
McGuffee LJ, Little SA (1996) Tunica media remodeling in mesenteric arteries of hypertensive rats. Anat Rec 246(2):279–292
Sutton-Tyrrell K, Bostom A, Selhub J, Zeigler-Johnson C (1997) High homocysteine levels are independently related to isolated systolic hypertension in older adults. Circulation 96(6):1745–1749
Bortolotto LA, Safar ME, Billaud E, Lacroix C, Asmar R, London GM et al (1999) Plasma homocysteine, aortic stiffness, and renal function in hypertensive patients. Hypertension 34(4 Pt 2):837–842
Symons JD, Rutledge JC, Simonsen U, Pattathu RA (2006) Vascular dysfunction produced by hyperhomocysteinemia is more severe in the presence of low folate. Am J Physiol Heart Circ Physiol 290(1):H181–H191
Guo H, Lee JD, Uzui H, Yue H, Wang J, Toyoda K et al (2006) Effects of folic acid and magnesium on the production of homocysteine-induced extracellular matrix metalloproteinase-2 in cultured rat vascular smooth muscle cells. Circ J 70(1):141–146
Weiss N, Heydrick S, Zhang YY, Bierl C, Cap A, Loscalzo J (2002) Cellular redox state and endothelial dysfunction in mildly hyperhomocysteinemic cystathionine beta-synthase-deficient mice. Arterioscler Thromb Vasc Biol 22(1):34–41
Wang D, Gill PS, Chabrashvili T, Onozato ML, Raggio J, Mendonca M et al (2007) Isoform-specific regulation by N(G), N(G)-dimethylarginine dimethylaminohydrolase of rat serum asymmetric dimethylarginine and vascular endothelium-derived relaxing factor/NO. Circ Res 101(6):627–635
Pope AJ, Karrupiah K, Kearns PN, Xia Y, Cardounel AJ (2009) Role of dimethylarginine dimethylaminohydrolases in the regulation of endothelial nitric oxide production. J Biol Chem 284(51):35338–35347
Ayling LJ, Whitley GS, Aplin JD, Cartwright JE (2006) Dimethylarginine dimethylaminohydrolase (DDAH) regulates trophoblast invasion and motility through effects on nitric oxide. Hum Reprod 21(10):2530–2537
Mather S, Dora KA, Sandow SL, Winter P, Garland CJ (2005) Rapid endothelial cell-selective loading of connexin 40 antibody blocks endothelium-derived hyperpolarizing factor dilation in rat small mesenteric arteries. Circ Res 97(4):399–407
Li H, Brodsky S, Kumari S, Valiunas V, Brink P, Kaide J et al (2002) Paradoxical overexpression and translocation of connexin43 in homocysteine-treated endothelial cells. Am J Physiol Heart Circ Physiol 282(6):H2124–H2133
Heil SG, De Vriese AS, Kluijtmans LA, Mortier S, Den HM, Blom HJ (2004) The role of hyperhomocysteinemia in nitric oxide (NO) and endothelium-derived hyperpolarizing factor (EDHF)-mediated vasodilatation. Cell Mol Biol (Noisy -le-grand) 50(8):911–916
Hassona MD, Abouelnaga ZA, Elnakish MT, Awad MM, Alhaj M, Goldschmidt-Clermont PJ, et al. (2010) Vascular hypertrophy-associated hypertension of profilin1 transgenic mouse model leads to functional remodeling of peripheral arteries. Am J Physiol Heart Circ Physiol
Sood HS, Hunt MJ, Tyagi SC (2003) Peroxisome proliferator ameliorates endothelial dysfunction in a murine model of hyperhomocysteinemia. Am J Physiol Lung Cell Mol Physiol 284(2):L333–L341
Westwood FR, Iswaran TJ, Greaves P (1990) Pathologic changes in blood vessels following administration of an inotropic vasodilator (ICI 153, 110) to the rat. Fundam Appl Toxicol 14(4):797–809
Allen SP, Liang HM, Hill MA, Prewitt RL (1996) Elevated pressure stimulates protooncogene expression in isolated mesenteric arteries. Am J Physiol 271(4 Pt 2):H1517–H1523
Kantachuvesiri S, Fleming S, Peters J, Peters B, Brooker G, Lammie AG et al (2001) Controlled hypertension, a transgenic toggle switch reveals differential mechanisms underlying vascular disease. J Biol Chem 276(39):36727–36733
Hunt MJ, Tyagi SC (2002) Peroxisome proliferators compete and ameliorate Hcy-mediated endocardial endothelial cell activation. Am J Physiol Cell Physiol 283(4):C1073–C1079
Acknowledgment
A part of this study was supported by NIH Grants: HL-71010 and NS-51568.
Author information
Authors and Affiliations
Corresponding author
Additional information
Givvimani S, and Qipshidze N contributed equally to this study.
Rights and permissions
About this article
Cite this article
Munjal, C., Givvimani, S., Qipshidze, N. et al. Mesenteric vascular remodeling in hyperhomocysteinemia. Mol Cell Biochem 348, 99–108 (2011). https://doi.org/10.1007/s11010-010-0643-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-010-0643-y