Abstract
The expression and function of calcium-sensing receptor (CaSR) in differentiated THP-1 (human acute monocytic leukemia cell line) cells are unknown currently. This study investigated above-mentioned issues using TRAP staining, immunofluorescence staining, Western blotting, ELISA, and Laser Confocal Scanning Microscopy techniques. We found that CaSR protein was expressed, and mainly located in the membrane and cytoplasm in differentiated THP-1 cells. Elevated extracellular calcium or GdCl3 (an agonist of CaSR) raised intracellular calcium concentration. And this increase was inhibited or abolished by NPS2390 (an inhibitor of CaSR), U73122 (a specific inhibitor of phospholipase C, PLC) or thapsigargin (a Ca2+-ATPase inhibitor). The extracellular GdCl3 elevation stimulated both of IL-1β and TNFα release, and this effect of GdCl3 was inhibited by NPS2390. In conclusion, CaSR is functionally expressed in differentiated THP-1 cells, and the activated CaSR contributes to intracellular calcium increment through Gq-PLC- inositol triphosphate (IP3) pathway and commits to cytokine secretion. These results suggest that CaSR might be involved in a variety of pathological processes mediated by activated monocyte-macrophages.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
As a member of G protein-coupled receptor superfamily, calcium-sensing receptor (CaSR) has been detected in a variety of tissues and cells, and plays an essential role in cell differentiation, proliferation, apoptosis, hormone secretion, etc., in addition to maintaining Ca2+ homeostasis in the body [1–4]. In previous studies, we have found that CaSR is involved in rat cardiac ischemia/reperfusion injury, apoptosis and hypertrophy, and that CaSR expression of myocardium in atherosclerotic rat was elevated, resulting in hypersensitivity to acute myocardial infarction [5, 6].
Monocytes-macrophages, as scavenger cells in the body, participate in the non-specific immunity as well as in many diseases and pathological processes [7–9], especially, atherosclerosis and multiple organ failure. Yamaguchi et al. have previously detected the expression of CaSR in human and murine monocytes isolated from peripheral blood [10–12]. However, the effect of CaSR activation on cytokine secretion and the pathway by which intracellular calcium was elevated by CaSR activation were not clarified in these studies.
THP-1, a human acute monocytic leukemia cell line, has been extensively used as a model for studying the differentiation of monocytes and macrophages in vitro [13]. When treated with phorbol-12-myristate-13-acetate (PMA), the THP-1 cells (monocyte-like) can differentiate into cells with macrophages-like phenotype [14–16]. Compared to other human myeloid cell lines, such as HL-60, U937, KG-1, or HEL cell lines, the differentiated THP-1 cells behave more like native monocyte-derived macrophages. For example, THP-1 cell line is the only cell line capable of producing lipoprotein lipase (LPL) in several human leukemia cell lines [15].
The imbalance of Ca2+ homeostasis is closely related with cardiovascular diseases such as hypertension, atherosclerosis, and coronary artery disease [17–19]. It is well known that monocytes-macrophages play important roles in onset and deterioration of atherosclerosis, shock, multiple organ failure, etc. [20–22]. Whether the monocyte/macrophage-mediated pathological processes are related with activation of CaSR remains unclear so far.
In this study, we determined whether CaSR is expressed in differentiated THP-1 cells stimulated with PMA, by which signal transduction pathway the CaSR activation induced increase of intracellular calcium concentration, and what effect CaSR activation had on cytokine release.
Materials and methods
Chemicals
LPS, GdCl3, NPS2390, PMA, NiCl2, CdCl2, U73122, U73343 and thapsigargin (TG) were purchased from Sigma Chemical Co. (St. Louis, MO, USA). Fluo-3/Am was purchased from Invitrogen Life Technologies (Carlsbad, CA, USA).
Cell line and cell cultures
The human acute monocytic leukemia cell line THP-1 was obtained from the American Type Culture Collection (Rockville, MD).THP-1 cells were maintained in RPMI 1640 (Thermo, Grand Island, NY), supplemented with 10% FBS (GIBCO, Grand Island, NY, USA) at pH 7.4, 37°C in a 5% CO2 atmosphere. THP-1 cells (5 × 105 cells per 35-mm dish) were differentiated by stimulation with PMA (160 nmol/ml, final concentration) for 3 days to obtain a macrophage-like phenotype, which closely resembles human monocyte-derived macrophages, as previously reported [12, 14].
Morphological examination
THP-1 cells were plated in 24-well plates. After 24, 48 and 72 h of treatment with PMA (160 nM), the cells were examined with an optical phase-contrast microscope (Olympus, Japan) after washing thrice with PBS.
Tartrate resistant acid phosphatase staining
Tartrate resistant acid phosphatase (TRAP) staining was performed according to the manufacturer’s instructions of the TRAP kit (Sigma, St. Louis, MO, USA). The THP-1 or differentiated THP-1 cells adhering to slides were fixed in Fixative Solution for 30 s and rinsed thoroughly in deionized water. These cells were divided into two groups. One group was incubated in solution A (Deionized water prewarmed 45 ml; Diazotized Fast Garnet GBC Solution 1.0 ml; Naphthol AS-Bl Phosphate Solution 0.5 ml; Acetate Solution 2.0 ml), the other group was incubated in solution B (Tartrate Solution 1.0 ml was added into solution A above mentioned) for 1 h in 37°C from light. The groups incubated in solution B was negative control. Then the cells were counterstained 2 min in hematoxylin solution, and rinsed several minutes in alkaline tap water to blue nuclei. The cells were then examined and photographed microscopically.
Western blotting for CaSR in THP-1 cells
Total proteins of the 293 cells, differentiated or undifferentiated THP-1 cells were prepared according to the manufacturer’s instructions as described [23]. Samples of 40 μg of protein from different experimental groups were separated by 10% SDS–PAGE and transferred to nitrocellulose membranes by electro-blotting. The membranes were blocked in TBS-T [137 mM NaCl, 20 mM Tris (pH 7.6), and 0.1% (v/v) Tween 20] containing 5% (w/v) skimmed milk at 37°C for 1 h. The membranes were then incubated overnight at 4°C with antibody against CaSR (Alomone Labs Ltd, Israel, 1:200). The membranes were incubated with secondary antibody AP-IgG (Promega) (diluted 1:5000 in TBS-T) for 1 h at room temperature. The lysate of 293 cells was the positive control. A peptide pre-absorption experiment was the negative control. β-actin was used as an internal control for a semi-quantitative assay.
Immunofluorescence staining of differentiated THP-1 cells for CaSR
The differentiated THP-1 cells plated at a density of 3.5–5 × 105 cells/ml onto cover slips, fixed with 4% paraformaldehyde, were treated with 3% BSA for 1 h and then incubated overnight at 4°C with CaSR primary antibody (1:50, Alomone). After washing the cells three times with 0.5% bovine serum albumin in PBS for 10 min, FITC-coupled, goat anti-rabbit IgG (1:100, Santa Cruz) was added and incubated for 1 h at room temperature. A peptide pre-absorption experiment was the negative control. The cells were then washed with PBS three times for 10 min. The cells were then examined and photographed using a fluorescence microscope (Olympus, Japan).
Measurement of intracellular free Ca2+ concentration
The differentiated THP-1 cells were loaded with 10 μM Fluo-3/AM for 30 min at 37°C, then rinsed with PBS for three times to remove the extracellular Fluo-3/AM. First, the cells were treated with various concentration of Ca2+ (0–30 mM) or Gd3+ (0–3 mM) to observe the effect of CaSR agonist on increase of intracellular free Ca2+ concentration ([Ca2+]i). According these results, Ca2+ (10 mM) or Gd3+ (1 mM) was used in the following experiments. These cells were randomly divided into CaCl2 challenge group and GdCl3 challenge group. Other intervention agents, for sample, NPS2390 (10 μM, a specific CaSR inhibitor), NiCl2 (100 μM, an inhibitor of Na+/Ca2+ exchanger), CdCl2 (20 μM, an inhibitor of L-type calcium channel), U73122 (10 μM, a PLC specific blocker), U73343 (10 μM, an inactivated analogue of U73122), thapsigargin (10 μM, TG, Ca2+-ATPase inhibitor), were added into media for 30 min before 10 mM Ca2+ or 1 mM GdCl3 challenge (see Fig. 4 in detail).
[Ca2+]i was detected at 488 nm using Laser Confocal Scanning Microscope (Leica Corporation, Germany). Following a 15 s baseline recording, cells were exposed to 10 mM Ca2+ or 1 mM Gd3+ and then recorded for 6 min. [Ca2+]i changes were showed with fluorescence intensity which represented FI and normalized to initial fluorescence intensity (FI0) [24].
Cytokine ELISA assays
Differentiated THP-1 cells were rinsed with PBS for three times before the experiments. Afterward, the cells were incubated in fresh serum-free medium containing 1 mg/L LPS, 10 μM NPS2390, GdCl3 (0–2 mM), or 1 mM GdCl3 together with 10 μM NPS2390, respectively, for 24 h.
Cytokine assays were performed with the following commercially available kits with a sensitivity (>10pg/ml): IL-1β and TNF-α human enzyme-linked immune absorbent assay (ELISA) system (Genetimes Technology Inc, Shanghai, China), according to the manufacturer’s instructions. Briefly, 100 μl of supernatant or recombinant protein standards were added to each well coated with primary antibodies against the specific cytokine, rinsed with buffer, incubated with the corresponding biotinylated secondary antibodies, and rinsed again before adding the streptavidin-horseradish peroxidase solution and developing the reaction with the tetramethylbenzidine (TMB) substrate solution. Absorbance of end products was determined at 450 nm within 10 min after developing the color.
Statistical analysis
All the data were obtained from at least three independent experiments that were replicated two or four times for each condition. All values are expressed as means ± SE. Comparisons among the groups were performed using one-way variance (ANOVA) followed by LSD test or Dunnett’s test. Values of P < 0.05 were considered statistically significant.
Results
Differentiation of THP-1 to macrophage-like cells
Morphological examination
After stimulated with PMA for 24 h (160 nmol/l), most of THP-1 cells adhered to dish surface, aggregated, and followed by elongation and pseudopodia formation in a time-dependent manner. More macrophage-like phenotypes appeared with time (Fig. 1).
TRAP staining
The red staining, which indicated positive TRAP expression, was observed in the differentiated THP-1 cells induced by PMA for 72 h. There was no red staining in the undifferentiated THP-1 cells (Fig. 2).
Tartrate resistant acid phosphatase staining. TRAP staining was used for identification of macrophages differentiation derived from THP-1 cells. In the negative groups, the cells were incubated in the solution containing the tartrate (Fig. 2)
CaSR expression in differentiated THP-1 cells
The protein expression of CaSR with two bands at 110 and 130 kD was detected in differentiated THP-1 cells and 293 cells (positive control) using Western blotting. In the negative control group, no bands could be observed (Fig. 3a).
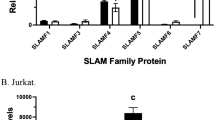
The expression of calcium-sensing receptor (CaSR) in THP-1 cells. a Protein expression of CaSR in 293 cells (lanes 1, 6), undifferentiated (lanes 3, 4) or differentiated THP-1 cells (lane2, 5) was detected by western blot. A peptide pre-absorption experiment was the negative control (lanes 1, 2, 3). b The nuclei were stained with 4′-6-diamidino-2-phenylindole (DAPI). A peptide pre-absorption experiment was the negative control (a).The immunofluorescence staining in differentiated THP-1 cells showed that CaSR was mainly expressed on the membrane and in the cytoplasm (b)
Subcellular localization of CaSR in differentiated THP-1 cells was determined by an immunoflurescence staining method. Excited FITC emits green fluorescence. Nuclei stained with 4′-6-diamidino-2-phenylindole (DAPI) display blue fluorescence. Strong green fluorescence was observed on the differentiated THP-1 cell surface and cytosol, indicating the expression of CaSR protein across the plasma membrane and inside the cells. In the negative control group, no green fluorescence could be observed (Fig. 3b).
Increase of [Ca2+]i induced by CaSR activation via G-PLC pathway
We found that extracellular Ca2+ and Gd3+ could induce increase of [Ca2+]i in differentiated THP-1 cells in concentration dependent manner at [Ca2+]o ranging from 0 to 30 mM and [Gd3+]o ranging from 0 to 3 mM (Fig. 4a, b).
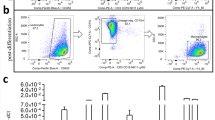
The effects of different agents on increase of intracellular calcium ([Ca2+]i) induced by extracellular Ca2+ or Gd3+ in differentiated THP-1 cells. a The cells in the group were exposed to various concentration of CaCl2. b The cells in the group were exposed to various concentration of GdCl3. c The cells in the experimental group were pretreated with NiCl2 (100 μM) and CdCl2 (20 μM) in the absence or presence of NPS2390 (10 μM), U73122 (10 μM), U73343 (10 μM) or TG (10 μM) for 30 min, then they were exposed consecutively to CaCl2 (10 mM). d The cells in experimental groups were exposed to GdCl3 (1 mM) with or without pre-exposure to NPS2390 (10 μM), U73122 (10 μM), U73343 (10 μM) or TG (10 μM) for 30 min. The cells in control group were incubated in Ca2+-free Krebs buffer (118 mM NaCl, 4.7 mM KCl, 1.2 mM KH2PO4, 1.2 mM MgSO4, 4.2 mM NaHCO3, 10 mM glucose, 10 mM Hepes, pH 7.4) (c, d). The intracellular calcium record was performed for 6 min (c, d)
The pre-treatment of 100 μM NiCl2(an inhibitor of Na+/Ca2+ exchanger)and 20 μM CdCl2 (an inhibitor of L-type calcium channel) for 30 min significantly diminished the increase of [Ca2+]i induced by 10 mM Ca2+, but could not be restored [Ca2+]i to the basal level. Meanwhile, NPS2390 (an antagonist of CaSR) completely abolished the increase of [Ca2+]i induced by 10 mM Ca2+ or 1 mM Gd3+(Fig. 4c, d).
Under the normal condition, the intracellular Ca2+ is from extracellular Ca2+ entry and release of intracellular Ca2+ store. To verify whether the change of [Ca2+]i induced by CaSR activation is dependent on intracellular Ca2+ store, cells were pretreated with 10 μM thapsigargin (TG, Ca2+-ATPase inhibitor) or 10 μM U73122 (a PLC specific blocker) for 30 min. The results showed that both TG and U73122 eliminated the increase of [Ca2+]i caused by extracellular 10 mM Ca2+ or 1 mM Gd3+. On the other hand, pretreatment with 10 μM U73334 (an inactivated analogue of U73122) did not prevent this increase of [Ca2+]i (Fig. 4c, d).
Treatment with NiCl2 + CdCl2, NPS2390, TG, and U73122 alone had no effect on [Ca2+]i of differentiated THP-1 Cells (The data were not supplied).
The increase of TNF-α and IL-1β release in differentiated THP-1 macrophages induced by GdCl3
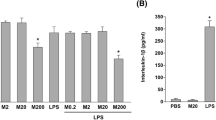
ELISA assays showed that GdCl3 increased IL-1β and TNF-α in the centrifuged supernatant depending on the GdCl3 concentration, and 1 mM GdCl3 induced the secretion of IL-1β and TNF-α significantly, as well as LPS (1 mg/l). The increase of IL-1β and TNF-α induced by GdCl3 was attenuated by 10 μM NPS2390. Treatment with NPS2390 alone did not affect secretion of IL-1β and TNF-α (Fig. 5).
Effect of GdCl3 loading on IL-1β and TNF-α release in differentiated THP-1 cells. Differentiated THP-1 cells were incubated in serum-free medium for 4 h at 37°C. Then cells were incubated with LPS (1 mg/l), or various concentration of GdCl3 (0–2 mM) for 24 h, or pre-treated with 10 μM NPS2390 for 1 h before adding GdCl3. The concentration of IL-1β (a, c) and TNF-α (b, d) in the culture media was detected with ELISA kit. Results are expressed as mean ± SE of four independent experiments. * P < 0.05 versus control group, ** P < 0.01 versus control group, # P < 0.05 versus 1 mM GdCl3 group, $ P > 0.05 versus control group
Discussion
Systemic inflammatory response is involved in many diseases and pathological processes, for example, atherosclerosis, shock, diabetes, organ failure. The cytokines released by monocyte/macrophage play important roles in systemic inflammatory response. Whether the more like native macrophages derived from THP-1 express CaSR functionally remains unclear so far.
To confirm the existence of functional CaSR expression in some tissues, the following evidence must be provided: (1) the existence of CaSR mRNA and protein in these tissues or cells; (2) the increase of [Ca2+]i is owing to extracellular calcium ([Ca2+]o) increment; (3) the [Ca2+]o-induced increase of [Ca2+]i is dependent on the release of Ca2+ from intracellular stores, but not on the calcium influx via voltage-dependent calcium channel; (4) the CaSR agonist- Gd3+ can cause similar response induced by an elevation of [Ca2+]o [25–28].
In this study, the morphological observation and TRAP staining indicated that THP-1 cells treated with PMA could differentiate into cells with the phenotype of macrophages. Western blotting analysis showed that the two specific protein bands at 110 and 130 kD, which represented as the precursor and mature form of CaSR, were displayed in differentiated THP-1. It is generally agreed that bands of 130–170 kDa are fully glycosylated mature form of the CaSR [28, 29]. The size of CaSR protein detected by western blotting varies considerably depending on the tissue and cell type, cellular fraction analyzed (membrane or cytoplasm), and the degree of posttranslational modification (glycosylation) of the CaSR protein. In our experiment, the same bands were detected in 293 cell expressing CaSR cDNA and did not appear in the peptide pre-absorption group. These results demonstrated that the 110- and 130-kDa bands were specific to CaSR. Meanwhile, the immunofluorescence staining indicated that CaSR proteins were located in the membrane and cytoplasm of differentiated THP-1 cells. Based on these data, we defined the expression of CaSR in differentiated THP-1 cells. Yamaguchi et al. reported that the CaSR expression exists in peripheral blood monocytes and several mononuclear cell strains, such as, human leukemia cell line HL-60 [30].
Wang and Xu have reported that the increase of [Ca2+]o or other CaSR agonists (Gd3+, spermine, etc.) caused the release of calcium from sarcoplasmic reticulum and led to a quick multiplication of [Ca2+]i via the G protein-PLC-IP3 signaling transduction pathway [31].
In this study, we observed that extracellular Ca2+ and Gd3+ could induce increase of [Ca2+]i in differentiated THP-1 cells in concentration-dependent manner, and the increase of [Ca2+]i caused by 10 mM Ca2+ could be partially inhibited by NiCl2 (100 μM) + CdCl2 (20 μM) or abolished by NiCl2 + CdCl2 with NPS2390 (10 μM), U73122 (10 μM) or thapsigargin (10 μM). In GdCl3 challenge group, we obtained similar results. Besides activating CaSR, Gd3+ shows calcium-related functions, such as acting on stretch-activated and other calcium channels, so we chose NPS2390 (a specific inhibitor of CaSR) as an approach to evaluate the specificity of this activity on CaSR in this study.
As we all know, extracellular calcium entry is a triggering factor, and calcium release from endoplasmic reticulum is critical for increase of [Ca2+]i. Therefore, TG inhibiting the endoplasmic reticulum ATP-ase (that pumps Ca2+ into the ER) would elevate [Ca2+]i transiently, but a continuous inhibition of Ca2+ pump on ER could induce calcium exhaustion in ER, and resulte in decrease of [Ca2+]i. IP3 receptor-dependent calcium release from ER is also an important mechanism for increase of [Ca2+]i. The activated phospholipase C (PLC) could hydrolyze phosphatidylinositol 4,5-bisphosphate(PIP2) into IP3 and DAG, which can cause IP3 receptor-dependent calcium release from ER and extracellular calcium entry through L-type of calcium channel, respectively. U73122 is a special inhibitor of PLC, so pretreatment with U73122 could induce decline of [Ca2+]i. NiCl2 (an inhibitor of Na+/Ca2+ exchanger) and CdCl2 (an inhibitor of L-type calcium channel) could decrease extracellular calcium entry. These data suggest that the increase of intracellular calcium induced by activation of CaSR in differentiated THP-1 cells is through the G protein-PLC-IP3 signaling transduction pathway, although Na+/Ca2+ exchanger and L-type calcium channel are also involved in the increase of [Ca2+]i caused by increased [Ca2+]o.
The production and release of inflammatory factors and cytokines are an important function of monocyte-macrophages. Sugimoto reported that elevated [Ca2+]o contributes to the augmentation of peripheral blood mononuclear cells chemotaxis [32]. In this study, we found that GdCl3 treatment, as well as LPS, could induce an increase of IL-1β and TNFα level in the supernatant of THP-1 cells with concentration- dependent manner, and that NPS2390 could partially inhibit the Gd-induced IL-1β and TNF-α release in the cells, while this drug had pretty efficiency on blocking the Gd-induced increase of intracellular calcium. How to interpret such a discrepancy if cytokine secretion is mainly mediated by the CaSR? We think that Gd3+ is not only an agonist of CaSR, but also a kind of heavy metal which is harmful to body and can activate immune system. There might be other way, besides CaSR activation, by which Gd3+ induces IL-1β and TNFα release in THP-1 cells. Wermuth et al. reported that Gd3+ could induce expression and release of numerous cytokines [33]. Therefore, NPS2390, as an antagonist of CaSR, could only inhibit release of cytokines induced by Gd3+ via activating CaSR.
In conclusion, this study demonstrated that CaSR was functionally expressed in differentiated THP-1 cells with the phenotype of macrophages and that the activation of CaSR could promote the secretion of IL-1β and TNFα in differentiated THP-1 cells. These results suggested that CaSR was involved in a variety of mononuclear macrophage related diseases possibly, and that it should be considered as a promising and potential therapeutic target.
References
Tu CL, Chang W, Xie Z, Bikle DD (2008) Inactivation of the calcium sensing receptor inhibits E-cadherin-mediated cell-cell adhesion and calcium-induced differentiation in human epidermal keratinocytes. J Biol Chem 283:3519–3528
Molostvov G, Fletcher S, Bland R, Zehnder D (2008) Extracellular calcium-sensing receptor mediated signalling is involved in human vascular smooth muscle cell proliferation and apoptosis. Cell Physiol Biochem 22:413–422
Kantham L, Quinn SJ, Egbuna OI, Baxi K, Butters R, Pang JL, Pollak MR, Goltzman D, Brown EM (2009) The calcium-sensing receptor (CaSR) defends against hypercalcemia independently of its regulation of parathyroid hormone secretion. Am J Physiol Endocrinol Metab 297:E915–E923
Chattopadhyay N, Brown EM (1997) Calcium-sensing receptor: roles in and beyond systemic calcium homeostasis. Biol Chem 378:759–768
Guo J, Li HZ, Zhang WH, Wang LC, Wang LN, Zhang L, Li GW, Li HX, Yang BF, Wu L, Wang R, Xu CQ (2010) Increased expression of calcium-sensing receptors induced by ox-LDL amplifies apoptosis of cardiomyocytes during simulated ischaemia/reperfusion. Clin Exp Pharmacol Physiol 37:e128–e135
Wang LN, Wang C, Lin Y, Xi YH, Zhang WH, Zhao YJ, Li HZ, Tian Y, Lv YJ, Yang BF, Xu CQ (2008) Involvement of calcium-sensing receptor in cardiac hypertrophy-induced by angiotensinII through calcineurin pathway in cultured neonatal rat cardiomyocytes. Biochem Biophys Res Commun 369:584–589
Woollard KJ, Geissmann F (2010) Monocytes in atherosclerosis: subsets and functions. Nat Rev Cardiol 7:77–86
Sayed D, Amin NF, Galal GM (2010) Monocyte-platelet aggregates and platelet micro-particles in patients with post-hepatitic liver cirrhosis. Thromb Res 125:e228–e233
Whitfield JF (2009) Calcium, calcium-sensing receptor and colon cancer. Cancer Lett 275:9–16
House MG, Kohlmeier L, Chattopadhyay N, Kifor O, Yamaguchi T, LeBoff MS, Glowacki J, Brown EM (1997) Expression of an extracellular calcium-sensing receptor in human and mouse bone marrow cells. J Bone Miner Res 12:1959–1970
Yamaguchi T, Olszak I, Chattopadhyay N, Butters RR, Kifor O, Scadden DT, Brown EM (1998) Expression of extracellular calcium (Ca 2+o )-sensing receptor in human peripheral blood monocytes. Biochem Biophys Res Commun 246:501–506
Yamaguchi T, Kifor O, Chattopadhyay N, Bai M, Brown EM (1998) Extracellular calcium ([Ca2+]o)-sensing receptor in amouse monocyte-macrophage cell line (J774): potential mediator of the actions of [Ca2+]o on the function of J774 cells. J Bone Miner Res 13:1390–1397
Llaverias G, Lacasa D, Vázquez-Carrera M, Sánchez RM, Laguna JC, Alegret M (2005) Cholesterol regulation of genes involved in sterol trafficking in human THP-1 macrophages. Mol Cell Biochem 273:185–191
Auwerx J, Staels B, Van Vaeck F, Ceuppens JL (1992) Changes in IgG Fc receptor expression induced by phorbol 12-myristate 13-acetate treatment of THP-1 monocytic leukemia cells. Leuk Res 16:317–327
Auwerx J (1991) The human leukemia cell line, THP-1: a multifacetted model for the study of monocyte-macrophage differentiation. Experientia 47:22–31
Daigneault M, Preston JA, Marriott HM, Whyte MK, Dockrell DH (2010) The identification of markers of macrophage differentiation in PMA-stimulated THP-1 cells and monocyte-derived macrophages. PLoS One 5:e8668
Xu C, Lu Y, Tang G, Wang R (1999) Expression of voltage-dependent K+ channel genes in mesenteric artery smooth muscle cells. Am J Physiol 277:G1055–G1063
Zheng XD, Li Q, Tang XB, Liang SJ, Chen LP, Zhang S, Wang ZG, Guo L, Zhang R, Zhu DL (2008) Source of the elevation Ca2+ evoked by 15-HETE in pulmonary arterial myocytes. Eur J Pharmacol 601:16–22
Deeks ED, Keating GM, Keam SJ (2009) Clevidipine: a review of its use in the management of acute hypertension. Am J Cardiovasc Drugs 9:117–134
Alexopoulos N, Raggi P (2009) Calcification in atherosclerosis. Nat Rev Cardiol 6:681–688
Molostvov G, Bland R, Zehnder D (2009) Expression and role of the calcium-sensing receptor in the blood vessel wall. Curr Pharm Biotechnol 10:282–288
Libby P, Okamoto Y, Rocha VZ, Folco E (2010) Inflammation in atherosclerosis: transition from theory to practice. Circ J 74:213–220
Tabas I (2010) Macrophage death and defective inflammation resolution in atherosclerosis. Nat Rev Immunol 10:36–46
Antoniades CG, Berry PA, Wendon JA, Vergani D (2008) The importance of immune dysfunction in determining outcome in acute liver failure. J Hepatol 49:845–861
Wonneberger K, Scofield MA, Wangemann P (2000) Evidence for a calcium-sensing receptor in the vascular smooth muscle cells of the spiral modiolar artery. J Membr Biol 175:203–212
Ray JM, Squires PE, Curtis SB, Meloche MR, Buchan AM (1997) Expression of the calcium-sensing receptor on human antral gastrin cells in culture. J Clin Investig 99:2328–2333
Sanders JL, Chattopadhyay N, Kifor O, Yamaguchi T, Butters RR, Brown EM (2000) Extracellular calcium-sensing receptor expression and its potential role in regulating parathyroid hormone-related peptide secretion in human breast cancer cell lines. Endocrinology 141:4357–4364
Ziegelstein RC, Xiong Y, He C, Hu Q (2006) Expression of a functional extracellular calcium-sensing receptor in human aortic endothelial cells. Biochem Biophys Res Commun 342:153–163
Molostvov G, James S, Fletcher S, Bennett J, Lehnert H, Bland R, Zehnder D (2007) Extracellular calcium-sensing receptor is functionally expressed in human artery. Am J Physiol Renal Physiol 293:F946–F955
Yamaguchi T, Ye C, Chattopadhyay N, Sanders JL, Vassilev PM, Brown EM (2000) Enhanced expression of extracellular calcium sensing receptor in monocyte-differentiated versus undifferentiated HL-60 cells: potential role in regulation of a nonselective cation channel. Calcif Tissue Int 66:375–382
Wang R, Xu CQ, Zhao WM, Zhang J, Cao K, Yang BF, Wu LY (2003) Calcium and polyamine regulated calcium-sensing receptors in cardiac tissues. Eur J Biochem 270:2680–2688
Sugimoto T, Kanatani M, Kano J, Kaji H, Tsukamoto T, Yamaguchi T, Fukase M, Chihara K (1993) Effects of high calcium concentration on the functions and interactions of osteoblastic cells and monocytes and on the formation of osteoclast-like cells. J Bone Miner Res 8:1445–1452
Wermuth PJ, Del Galdo F, Jiménez SA (2009) Induction of the expression of profibrotic cytokines and growth factors in normal human peripheral blood monocytes by gadolinium contrast agents. Arthritis Rheum 60:1508–1518
Acknowledgments
This work was supported by the National Basic Research Program of China (973 Program, grant number 2007CB512000); National Natural Science Foundation of China (30871012, 30470688 and 30700288); Specialized Research Found for the Doctoral Program of Higher Education (20070226012); Harbin Medical University found for younger scientists (060016) and Technology Research Foundation of the Department of Education of Heilongjiang Province (11521078).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xi, Yh., Li, Hz., Zhang, Wh. et al. The functional expression of calcium-sensing receptor in the differentiated THP-1 cells. Mol Cell Biochem 342, 233–240 (2010). https://doi.org/10.1007/s11010-010-0489-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-010-0489-3