Abstract
The parotid glands are highly active secretory systems subjected to continuous stress, which in turn, can lead to several pathophysiological conditions. Damage of the parotid glands are caused by radical oxygen species (ROS) as by-products of oxygen metabolism. This study investigated the effect of hydrogen peroxide (H2O2) on Carbachol (CCh)-evoked secretory responses and caspase-3 activity in the isolated rat parotid gland to understand the role of oxidative stress on the function of the gland. Amylase secretion, cytosolic calcium concentration ([Ca2+]i) and caspase-3 activity in parotid gland tissue were measured using fluorimetric methods. H2O2 had little or no effect on amylase secretion compared to basal level. Combining H2O2 with CCh resulted in an attenuation of the CCh-evoked amylase secretion compared to the effect of CCh alone. CCh can evoke a large increase in [Ca2+]i comprising an initial peak followed by a plateau. In a Ca2+-free medium containing 1 mM EGTA, CCh evoked only the initial peak of [Ca2+]i. H2O2 alone evoked a gradual and dose-dependent increase in [Ca2+]i. Combining H2O2 with CCh resulted in a decrease in [Ca2+]i compared to the effect of CCh alone. In a Ca2+-free medium, H2O2 still evoked a small increase in [Ca2+]i, but this response was less compared to the results obtained with H2O2 in normal [Ca2+]0. Combining H2O2 with CCh resulted in only a small transient increase in [Ca2+]i. Following CCh stimulation, H2O2 application resulted in a large increase in [Ca2+]i in normal [Ca2+]0. This effect of H2O2 was partially abolished in a nominally free Calcium medium containing EGTA. H2O2 can stimulate caspase-3 activity in parotid gland tissue. Similar response was obtained with betulinic acid and thapsigargin (TPS) on caspase-3 activity compared to basal. The results have demonstrated that like CCh, H2O2 can also mobilise Ca2+ from intracellular stores and facilitate its influx into the cell from extracellular medium. This effect of H2O2 may be due to its activity to induce apoptosis in the parotid gland, since H2O2 can stimulate the activity of caspase-3, a marker of cellular apoptosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Oxidative stress is a major risk factor, which induces dysfunction of several tissues and organs of the body [1]. Aerobic organisms, which obtain their energy from the reduction of oxygen (O2), are continuously at risk from the damaging action of small amounts of oxygen free radicals (O−), hydroxyl ion (OH−) and hydrogen peroxide (H2O2), which are the by-products of O2 metabolism [2, 3]. In biological systems, these free radicals are referred to as reactive O2 species (ROS), which have a remarkable capacity to cause extensive damage to physiological systems [4, 5]. Often, the ROS can induce apoptosis, a highly complex and toughly regulated process, which plays a major role in maintaining tissue homeostasis [6]. H2O2-induced oxidative stress has been demonstrated with modifications of calcium (Ca2+) homeostasis, amylase secretion and filament polymerisation in different tissues [7–11].
More recently, ROS have been recognised as intracellular messengers, which are required for the activation of a larger number of signal transduction mechanisms [12, 13]. In relation to cellular Ca2+ homeostasis, the H2O2-induced increase in intracellular Ca2+ concentration ([Ca2+]i) has been attributed to either mobilisation from intracellular stores [14], Ca2+ influx across plasma membrane [15] or both [16]. Moreover, H2O2-evoked Ca2+ release from intracellular stores may also be due to either inhibition of the sarcoplasmic reticulum calcium-ATPase pump (SERCA) [17] or activation of Ca2+ release channel [7]. Other studies have shown that extremely high concentrations of H2O2 (1 mM) can cause severe oxidative stress in most cells, with the release of Ca2+ from the mitochondrial and non-mitochondrial intracellular stores [18]. Although the effect of H2O2 on secretory responses and apoptosis have been demonstrated in several epithelial cell types including pancreatic acinar cells [9, 19] and gastric cells [20], very little is known about the action of H2O2 and its combination with secretagogues in parotid acinar cells. Since the salivary glands are similar in structure and function as the exocrine pancreas, this study now investigates the effect of oxidative condition in amylase secretion, Ca2+ mobilisation and caspase-3 activity in parotid gland tissues.
Materials and methods
Materials and chemicals
The specific caspase-3 fluorogenic substrate (AC-DEVD-AMC) and other chemicals were purchased from Sigma (Spain), except collagenase, which was obtained from Worthington Biochemical Corporation (New Jersey, USA), and fura-2 AM, which was obtained from Molecular Bioprobes Europe (The Netherlands).
Experimental procedure
Young adult male Wistar rats weighting 200–300 g were used in this study. All the rats were in good health and were given food and water ad libitum. They were kept in 12–12 h day cycle. The animals were starved 24 h before the use of the parotid glands. All the rats were humanely killed by a blow to the head followed by cervical dislocation. An incision was made in the right and left sides of the neck and the parotid glands were located, rapidly excised and placed in Krebs–Henseleit (KH) solution containing (in mM): NaCl 118; KCl 4.76; CaCl2 2.56; MgCl2 1.1; NaHCO3 25.0; NaH2PO4 1.15; d-glucose 1.8; sodium puruvate 4.9; sodium fumarate 2.7 and sodium glutamate 4.9. The solution was adjusted and kept at pH 7.4 while being continuously gassed with a mixture of 95% O2: 5% CO2 and maintained at 37°C. All the work had relevant ethical clearance from the University of Central Lancashire (UK), the University of Lisbon (Portugal) and University of Extremadura (Spain).
Online fluorimetric determination of parotid amylase
The parotid glands were dissected free of any fatty and connective tissues and cut into small segments (5–10 mg) and a total weight of about 175–250 mg was placed in a Perspex flow chamber (volume 1 ml) and superfused with oxygenated KH solution at 37°C at a flow rate of 1.8 ml min−1. The amylase concentration in the effluent from the chamber was measured continuously using an online fluorimetric method. This method was previously described by Mata et al. [21] and is a modification of the original technique described previously by Rinderknecht et al. [22] and subsequently by Michalek et al. [23]. Using a modified Technicon auto-analyser system, the effluent from the flow chamber was mixed with the substrate solution. After passing through two glass mixing coils (27 and 14 turns, respectively) submerged in a thermostatically heated water bath (37°C), the reaction products were dialysed through a cuphrane membrane (Technicon part No. 933.0225.01) embedded in a 12″ dry operated dialyser (Bran-Luebbe, Germany) with a recipient stream buffer (NaCl, 0.05 M and Triton-X-100, 0.1% v/v, at pH 7.0). The air segmented recipient stream, which contains the released fluorochrome, was then pumped via a de-bubbler through a 37°C thermostated removable 750 μl quartz flow cell cuvette placed in a Perkin Elmer LS 50 B fluorimeter. The fluorescence was monitored with excitation and emission wavelengths of 343 nm and 414 nm, respectively, at a fixed intensity scale of 0.1 [23]. Excitation and emission slits were set at 5 nm. Continuous α-amylase output fluorescence intensity data were collected directly into a computer and processed via a Winlab Software. After each experiment, the tissue was removed from the chamber, blotted dry and weighed. α-amylase (Sigma type II-A) (30 Units ml−1 amylase) was used as a standard to calibrate each experiment. The standard and KH solution, which contained either H2O2, carbachol (CCh) or a combination of H2O2 and CCh, were perfused through the system for 6 min. Either H2O2, CCh or a combination of H2O2 and CCh was added directly to the superfusing KH solution at appropriate concentrations and output was expressed as Units ml−1 above basal (per 100 mg of tissue).
Isolation of parotid acinar cells
The parotid gland was dissociated into acinar cells with collagenase in two stages after a period of 75 min by an established method [21, 24]. Briefly, the parotid was incubated in the presence of modified Hanks’ balanced salt solution (HBSS) containing (in mM): NaCl, 137; KCl, 5.4; MgSO4, 0.81; CaCl2, 2.5; Na2HPO4, 0.33; KH2PO4, 0.44; glucose, 5.6; Hepes, 33, supplemented by 0.1% (w/v) bovine serum albumine (BSA), 0.1 mg ml−1 soyabean trypsin inhibitor (STBI) and 50 Units ml−1 of CLPSA collagenase. The solution was gassed with 100% oxygen and the pH was adjusted to 7.4. When the experiments were performed in a calcium-free medium, calcium was omitted and EGTA (1 mM) was added. Cell viability monitored with trypan blue was always greater than 95%.
Cell loading and Ca2+ signal analysis
Cell suspensions from the parotid glands were loaded with 2 μM of fura-2 acetylmethoxy ester (AM) for 40 min at room temperature (20°C) in a dark room, with gentle shaking every 10 min. After the loading procedure, cells were centrifuged and re-suspended in an incubating medium containing (in mM): NaCl, 137; KCl, 5.4; MgCl2, 1.1; CaCl2, 1.28; Na2HPO4, 0.33; KH2PO4, 0.44; glucose, 5.6; Hepes, 33; pH 7.4; 0.1% w/v bovine serum albumin for 60 min at 37°C for complete desterification of the probe. Cells were used within 2–3 h.
For determination of fluorescence, a small volume (250 μl) of parotid cell suspension was placed on a thin glass cover slip attached to a Perspex perfusion chamber. Thin glass cover slips were imbedded and coated with Polly-lysine (20 μg ml−1) and let to dry in open air, to promote cell attachment. Perfusion (approximately 1 ml min−1) at room temperature (22°C) was started after a 2-min period to allow spontaneous attachment of the cells to the glass cover slip. The chamber was placed on the stage of an inverted fluorescence-equipped microscope (Nikon Diaphot 300) equipped with a Fluor 40× fluorescence objective.
The cells were alternatively excited at 340 nm and 380 nm by a computer-controlled filter wheel (Lamda-2, Shutter Instruments), and the emission fluorescence was detected at 510 nm. The emitted images were captured by a cooled digital CCD camera (C-6790, Hamamatsu Photonics) and recorded using dedicated software (Aqua-Cosmos, Hamamatsu Photonics). Traces were expressed as 340/380 ratio fluorescence variations [18]. Clusters of four to six cells were selected and fluorescence from individual cells was measured during each experiment.
Caspase-3 activity assay
Aliquots of parotid acinar cell suspensions were incubated in a shaking water bath at 37°C for 1 h either alone (control) or with either 10 μM, 100 μM or 1 mM H2O2, 10 μg ml−1 betulinic acid or 1 μM thapsigargin. Following incubation, each sample was centrifuged at 250g and the cell pellet was used to measure caspase-3 activity. In order to determinate caspase-3 activity, stimulated or resting cells were sonicated and cell lysates were incubated with 2 ml of substrate solution (20 mM N-(2-hydroxylthyl) piperazine-N′-(2-ethanesulfonic acid (HEPES), pH 7.4, 2 mM EDTA, 0.1% 3-[(3-cholamidopropyl) dimethyammonio]-1-propanesulfonate (CHAPS), 5 mM DTT and 8.25 μM of caspase-3 substrate) for 2 h at 37°C as previously described [25]. Substrate cleavage was measured with a fluorescence spectrophotometer with an excitation wavelength of 360 nm and emission at 460 nm. The activity of caspase was calculated from the cleavage of the specific fluorogenic substrate (AC-DEVD-AMC). The data were calculated as fluorescence units mg−1 protein and presented as percentage relative to control.
Statistical analysis
All data provided are expressed as mean ± standard error of mean (SEM). Data were analysed using Student’s unpaired t-test and a one-way analysis of variance (ANOVA) test using SPSS 15 statistical software. Only values with P < 0.05 were accepted as significant.
Results
Effects of H2O2 on amylase secretion
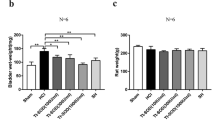
Basal amylase secretion in this series of experiments was 4.41 ± 0.35 U ml−1 (100 mg tissue)−1, (n = 46). Superfusion of parotid gland tissues with 1 mM H2O2 resulted in a small decrease in amylase output compared to control. Typical amylase output reduced from 4.41 ± 0.35 U ml−1 (100 mg tissue)−1 (n = 46) to 3.98 ± 0.31 U ml−1 (100 mg tissue)−1 (n = 26). These results show that 1 mM H2O2 had either little or no statistical effect on amylase secretion compared to control. Figure 1a shows original chart recordings of amylase output from parotid gland segments following superfusion with 10−4 M and 10−5 M CCh alone and in combination with 1 mM H2O2. Mean peak (±SEM) values of amylase output above basal levels for CCh alone and in combination with H2O2 are shown in Fig. 1b. The results show that CCh can elicit marked increases in amylase secretion compared to basal. In the presence of H2O2, the CCh-evoked amylase output significantly (P < 0.05) decreased especially at 10−5 M CCh.
(a) Original chart recordings show the effect of 10−5 M and 10−4 M CCh on amylase output in the absence and presence of 1 mM H2O2. Traces are typical of 18–24 experiments taken from eight to ten rats. (b) Bar charts showing amylase output above basal for either 10−4 M or 10−5 M CCh in the absence or presence of 1 mM H2O2. Data (taken from original traces) are mean (±SEM), n = 18–24; *P < 0.05 for c compared to d. Note that a and b are not significantly different from one another
Effects of CCh on [Ca2+]i
Since H2O2 can elicit a reduction in CCh-evoked amylase secretion in parotid gland segments, it was decided to measure [Ca2+]i, since Ca2+ is an important mediator of CCh-evoked amylase output [18]. Figure 2a shows time course chart traces of [Ca2+]i in fura-2 loaded parotid acinar cells in basal condition and following stimulation with 10−4 M CCh in a medium with normal concentration of Ca2+ ([Ca2+]0 = 1.28 mM) and in a Ca2+-free medium containing 1 mM EGTA ([Ca2+]0 = 0 mM). The mean (±SEM) data for changes in the [Ca2+]i transient are shown in Fig. 2b. The results show that in normal [Ca2+]0, CCh elicit a marked transient increase in [Ca2+]i comprising an initial rise (peak) followed by a gradual decrease, which subsequently levels off to a plateau phase (plateau) above basal level. In the absence of [Ca2+]0, basal [Ca2+]i was reduced and CCh evoked only a transient rise (peak) in [Ca2+]i followed by a rapid decline to basal level. The plateau response was abolished in the Calcium free medium when compared to responses obtained in normal [Ca2+]0, suggesting that extra-cellular [Ca2+]0 is required to maintain the sustained plateau phase of the CCh-evoked [Ca2+]i response. The results in Fig. 2b also show that free Calcium medium caused a significant (P < 0.05) decrease in both the peak and plateau phase (measured 100 and 200 s after peak response) of the CCh-evoked [Ca2+]i compared to the responses obtained in normal [Ca2+]0.
(a) Original chart recordings showing basal and CCh (10−4 M)-evoked changes in [Ca2+]i in fura 2-loaded single parotid acinar cells during perfusion with a physiological salt solution containing either 1.28 mM [Ca2+]0 or 0 mM [Ca2+]0 plus 1 mM EGTA. Traces are typical of 15–20 cells taken from eight to ten different animals. Note that basal [Ca2+]i decreases in low [Ca2+]0 compared to normal [Ca2+]0. (b) Mean (±SEM) % [Ca2+]i above basal in fura 2-loaded parotid acinar cells in 1.28 mM and 0 mM [Ca2+]0 at the peak, 100 s and 200 s following CCh application. Values are expressed as % fluorescence above basal, n = 15–20 cells taken from eight to ten animals. Single value t-test was performed to compare all test values with 100% (basal) and all of them were significantly (*P < 0.05) different
Effect of H2O2 on [Ca2+]i
Since H2O2 can reduce CCh-evoked amylase output, it was decided to measure CCh-evoked [Ca2+]i in the absence and presence of H2O2 to determine what effect H2O2 may exert on cellular Ca2+ mobilisation. The results for these experiments in normal and in Ca2+-free medium containing 1 mM EGTA are shown as original time courses traces of [Ca2+]i in Fig. 3a and b, respectively. The results show that in normal [Ca2+]0, either 100 μM or 1 mM H2O2 can elicit a gradual increase in [Ca+]i, compared to a steady state basal [Ca2+]i in the absence of H2O2. The effect of 1 mM H2O2 was more effective in increasing [Ca2+]i compared to 100 μM. In the continuous presence of H2O2, CCh (10−4 M) evoked a rapid rise in [Ca2+]i followed by a plateau that remained above basal level, but this response was attenuated by the H2O2. Similarly, in the absence of H2O2, CCh evoked a large transient increase in [Ca2+]i followed by a plateau phase. Figure 3c shows the mean (±SEM) % fluorescence above basal at 100, 300, 500 and 750 s of different concentrations of H2O2 in basal condition prior to CCh application.
(a) Original time course chart recordings showing the effect either of 100 μM (trace b) or 1 mM H2O2 (trace a) on [Ca2+]i in fura-2 loaded parotid acinar cells in normal [Ca2+]0 in the absence and presence of 10−4 M CCh. The effect of 10−4 M CCh alone on [Ca2+]i is also shown in the figure for comparison (trace c). (b) Original chart recordings showing the effect of either 100 μM H2O2 (trace c) or 1 mM H2O2 (trace d) on [Ca2+]i in the absence and presence of 10−4 M CCh in a nominally free [Ca2+]0 containing 1 mM EGTA. The effect of 10−4 M CCh alone in low Ca2+ is also shown for comparison (trace f). Traces in a and b are typical of 15–20 cells taken from six to eight different animals. The arrows indicate the point when CCh was exposed to the cell. (c) Mean (±SEM) of time course fluorescence ratios above basal in fura 2-loaded parotid acinar cells in 1.28 mM (normal) and zero mM [Ca2+]0 either in 100 μM or 1 mM H2O2. Values are expressed as % fluorescence ratios above basal, n = 15–20 cells taken from six to eight animals. *P < 0.05 when compared to basal
Typically, prior to CCh application, perfusion of different concentrations (100 μM–1 mM) of H2O2 resulted in an increase in [Ca2+]i above basal (21.66 ± 1.00% and 49.40 ± 0.69%, respectively). Similarly, in a Ca2+-free solution containing 1 mM EGTA, the increase was 7.93 ± 0.84% and 31.58 ± 1.54% in 100 μM and 1 mM H2O2 prior to CCh simulation. The results show that the reactive oxygen species induced a significant increase (P < 0.05) in [Ca2+]i in both a normal and a Ca2+-free medium for 100 μM and 1 mM H2O2.
Figure 4 shows the mean (±SEM) increases in percentage of [Ca2+]i fluorescence at the peak and plateau phase (100 s and 200 s after peak) above basal (absence or presence of either 100 μM or 1 mM H2O2) and following stimulation of fura-2 loaded parotid acinar cells with 10−4 CCh in a normal and a Ca2+-free medium. In the absence of H2O2, CCh evoked much larger increases in [Ca2+]i compared to the responses obtained in either 100 μM or 1 mM H2O2 in normal [Ca2+]0. Similar responses were obtained for CCh in a Ca2+-free medium, but the magnitude of the responses was markedly reduced, especially the plateau phase. Together, these results suggest that H2O2 is mobilising [Ca2+]0 from the same intracellular pool(store) compared to CCh, and that [Ca2+]0 is required to replenish the intracellular Ca2+ pool.
Mean (±SEM) time course increases in [Ca2+]i ratio units (expressed as % above basal either in the absence or the presence of either 100 μM or 1 mM H2O2) in fura-2 loaded parotid acinar cells following stimulation with 10−4 M CCh in normal (a) and in a normally low (+1 mM EGTA) Calcium medium (b). n = 15–20 cells taken from eight to ten animals. *P < 0.05 when compared to 0 μM [H2O2]0
In another series of experiments (Fig. 5), fura-2 parotid acinar cells were stimulated with 10−4 M CCh alone and following its removal, the cells were exposed to either 100 μM or 1 mM H2O2 in a normal and a nominally calcium free (+1 mM EGTA) medium. The results show that CCh can evoke a large transient increase in [Ca2+]i (peak) followed by a sustained plateau phase. On removal of CCh, [Ca2+]i gradually decreased to almost basal level. Exposure of fura-2 parotid acinar cells to either 100 μM or 1 mM H2O2 resulted in a gradual increase in [Ca2+]i. The percentage of fluorescence of [Ca2+]i above basal, 750 s after H2O2 application, was 35.02 ± 1.98 and 27.60 ± 2.96% for 100 μM and 1 mM of H2O2, respectively, compared to 125.52 ± 3.95% for CCh-evoked initial peak response. In contrast, in a nominally free Calcium medium containing 1 mM EGTA, CCh (10−4 M) evoked only the initial peak response followed by a rapid decline to the basal level. On removal of CCh and application of either 100 μM or 1 mM H2O2, there were small, but detectable changes in the percentage of fluorescence of [Ca2+]i compared to basal. In the presence of 100 μM and 1 mM H2O2, the percentage of fluorescence of [Ca2+]i above basal was 7.15 ± 1.00 and 26.24 ± 1.51, respectively, compared to 77.31 ± 2.24% in CCh alone. Together, these results clearly indicate that H2O2 is stimulating Ca2+ influx into the parotid acinar cells from the extra cellular medium and possibly its release from intracellular store since [Ca2+]i increased slightly in a nominally free [Ca2+]0 medium containing EGTA.
Mean (±SEM) of % fluorescence ratio units above basal in fura 2-loaded parotid acinar cells in 1.28 mM and 0 mM Calcium medium after CCh (10−4 M)-induced calcium store depletion. Values are expressed as % fluorescence above basal, n = 15–20 cells taken from eight to ten animals. *P < 0.01 when compared to basal, which is taken as 100%. Note that H2O2 can still elevate [Ca2+]i in a nominally low Calcium medium
Effects of H2O2 on caspase-3 activity
Figure 6 shows the mean (±SEM) % caspase-3 activity above control level following stimulation of parotid acinar cells with different concentrations of either H2O2, betulinic acid (10 μg ml−1) or thapsigargin (TPS) (1 μM) as positive controls. The results show that the reactive oxygen species induced a significant (P < 0.05) and dose-dependent increase in % caspase-3 activity. The results also show that both the depletion of intracellular Ca2+ stores by administration of 1 μM TPS or betulinic acid, an agent that opens the permeability transition pore of the mitochondria, can also induce significant (P < 0.05) increases in caspase-3 activity compared to control.
Histograms showing mean (±SEM) % changes in caspase-3 activity (expressed per μg total protein above control level) following stimulation of parotid acinar cells with either different concentrations (10−3–10−5 M) of H2O2, 10 μg/ml of betulinic acid (BA) or 10−6 M of thapsigargin (TPS) during 60 min of incubation. Values are expressed as caspase-3 activity in μM total protein, n = 8–20 taken from 16 to 30 animals. * P < 0.05 when compared to control
Discussion
The results of this study have shown that CCh can evoke large increases in amylase secretion, while exposure of the gland tissue to H2O2 resulted in decrease in CCh-evoked amylase secretion (Fig. 1). Cellular Ca2+ plays a major physiological role in the stimulus-secretion coupling process in epithelial cells including those from the parotid gland [26, 27]. Cytosolic Ca2+ can come from two sources to elicit a physiological response. These include the intracellular stores such as the endoplasmic reticulum (ER) and the mitochondria and the extra-cellular medium [28–30]. Once the intracellular stores are depleted, Ca2+ will enter the cell, and subsequently, the store, by a process called capacitative Ca2+ entry (CCE). The present study was designed to investigate the effect of H2O2 on a basal and CCh-evoked Ca2+ mobilisation in parotid acinar cells. The results clearly show, as demonstrated previously [31], that the cholinergic agonist at a supramaximal dose can elicit a large transient increase in [Ca2+]i followed by a sustained plateau in normal [Ca2+]0. However, when [Ca2+]0 was nominally reduced and 1 mM EGTA was present, CCh only evoked the initial peak response (Fig. 2). This finding clearly indicates that [Ca2+]0 is required to maintain the plateau phase, and moreover, the initial peak response is due to Ca2+ released from an intracellular store [31]. When parotid acinar cells were exposed to H2O2 in normal [Ca2+]0, there was a gradual increase in [Ca2+]i and this response was significantly reduced in a nominally free Calcium medium containing 1 mM EGTA (Figs. 3, 4). In the continuing presence of H2O2, CCh evoked a much smaller increase in [Ca2+]i compared to the response obtained with CCh alone in the absence of H2O2. In free Calcium medium, the CCh-evoked [Ca2+]0 was significantly reduced compared to the responses obtained with CCh alone in normal [Ca2+]0 (Fig. 5). These results suggest that like CCh, H2O2 is gradually releasing Ca2+ from an intracellular store and the store(s) may be the same that is activated by CCh. However, the small increase in cellular Ca2+ does not seem adequate enough to increase amylase output from parotid segments.
Second, this study investigated further whether H2O2 is actually inducing Ca2+ entry into parotid acinar cells. Initially, parotid acinar cells were stimulated with CCh in either a normal or a nominally free Calcium medium containing 1 mM EGTA and on removal of CCh, the cells were exposed to H2O2. The results show that CCh can evoke large increases in [Ca2+]i comprising of the initial peak followed by a plateau. On the removal of CCh and exposure to H2O2, [Ca2+]i gradually increased above CCh stimulated level (Fig. 6). These results suggest that H2O2 is probably stimulating Ca2+ influx into parotid acinar cells. In order to test this interesting finding, the experiments were repeated in a nominally free Calcium medium containing 1 mM EGTA. In this case, CCh only evoked the initial transient (peak) increase in [Ca2+]i followed by a rapid decline to basal level. On exposure of the cells to H2O2, there was only a smaller change in [Ca2+]i compared to the response in a normal [Ca2+]0 medium. Together, the results clearly indicate that H2O2 is facilitating Ca2+ influx and its release from intracellular stores into parotid acinar cells. The cellular mechanism to this H2O2-evoked increase in Ca2+ influx is not understood. It is possible that H2O2 is disrupting the plasma membrane via oxygen free radical, which, in turn, leads to Ca2+ influx. Alternatively, the generation of free radicals may lead to the activation of capacitative calcium entry. If H2O2 is generating ROS, then it should produce by-products of apoptotic mechanism. Interestingly, the results of this study have shown that H2O2 can also stimulate the activity of caspase-3 in parotid gland tissue and this effect of H2O2 was dose-dependent. Similar response was obtained with either betulinic acid, a substance which is known to induce apoptosis in a number of cell types [32], or with thapsigargin, which is known to deplete intracellular Ca2+ stores [33, 34] (Fig. 6).
The results of this study corroborate the findings of other similar studies employing either platelets or pancreatic acinar cells [9, 13, 18, 33]. ROS via H2O2 can stimulate the release of cytochrome C, which interacts with the apoptotic protease activating factor 1 (Apaf-1). This, in turn, activates caspase-3 leading to apoptosis [34, 35]. In addition, oxidative stress induced by H2O2 can lead to the re-organisation of the actin cytoskeleton in secretory acinar cells [9]. Actin filament arrangement is a key modulator of secretion via exocytosis in epithelial cells, and thus a possible explanation for the secretagogue-evoked reduced responses induced by H2O2.
In conclusion, the results of this study have demonstrated that H2O2 can attenuate CCh-evoked amylase secretion and [Ca2+]i, which may be due to its stimulating effect on intracellular stores and on the capacitative Ca2+ entry mechanism either directly or via the process of apoptosis.
References
Forsberg L, de Faire U, Morgenstern R (2001) Oxidative stress, human genetic variation, and disease. Arch Biochem Biophys 389:84–93
Cross CE, Halliwell B, Borish ET, Pryor WA, Ames BN, Saul RL, McCord JM, Harman D (1987) Oxygen radicals and human disease. Ann Intern Med 107:526–545
Halliwell B, Gutteridge JM (1984) Oxygen toxicity, oxygen radicals, transition metals and disease. Biochem J 219:1–14
Holbrook NJ, Ikeyama S (2002) Age-related decline in cellular response to oxidative stress: links to growth factor signaling pathways with common defects. Biochem Pharmacol 64:999–1005
Ryter SW, Kim HP, Hoetzel A et al (2007) Mechanisms of cell death in oxidative stress. Antioxid Redox Signal 9:49–89
Curtin JF, Donovan M, Cotter TG (2002) Regulation and measurement of oxidative stress in apoptosis. J Immunol Methods 265:49–72
Favero TG, Zable AC, Abramson JJ (1995) Hydrogen peroxide stimulates the Ca2+ release channel from skeletal muscle sarcoplasmic reticulum. J Biol Chem 270:25557–25563
Redondo PC, Salido GM, Pariente JA, Rosado JA (2004) Dual effect of hydrogen peroxide on store-mediated calcium entry in human platelets. Biochem Pharmacol 67:1065–1076
Rosado JA, Gonzalez A, Salido GM, Pariente JA (2002) Effects of reactive oxygen species on actin filament polymerisation and amylase secretion in mouse pancreatic acinar cells. Cell Signal 14:547–556
Supinski GS, Callahan LA (2005) Diaphragmatic free radical generation increases in an animal model of heart failure. J Appl Physiol 99:1078–1084
Sweiry JH, Shibuya I, Asada N et al (1999) Acute oxidative stress modulates secretion and repetitive Ca2+ spiking in rat exocrine pancreas. Biochim Biophys Acta 1454:19–30
Granados MP, Salido GM, Pariente JA et al (2004) Generation of ROS in response to CCK-8 stimulation in mouse pancreatic acinar cells. Mitochondrion 3:285–296
Rosado JA, Redondo PC, Salido GM et al (2004) Hydrogen peroxide generation induces pp60src activation in human platelets: evidence for the involvement of this pathway in store-mediated calcium entry. J Biol Chem 279:1665–1675
Wang X, Takeda S, Mochizuki S et al (1999) Mechanisms of hydrogen peroxide-induced increase in intracellular calcium in cardiomyocytes. J Cardiovasc Pharmacol Ther 4:41–48
Korzets A, Chagnac A, Weinstein T et al (1999) H2O2 induces DNA repair in mononuclear cells: evidence for association with cytosolic Ca2+ fluxes. J Lab Clin Med 133:362–369
Krippeit-Drews P, Haberland C, Fingerle J et al (1995) Effects of H2O2 on membrane potential and [Ca2+]i of cultured rat arterial smooth muscle cells. Biochem Biophys Res Commun 209:139–145
Moreau VH, Castilho RF, Ferreira ST et al (1998) Oxidative damage to sarcoplasmic reticulum Ca2+-ATPase at submicromolar iron concentrations: evidence for metal-catalyzed oxidation. Free Radic Biol Med 25:554–560
Pariente JA, Camello C, Camello PJ et al (2001) Release of calcium from mitochondrial and nonmitochondrial intracellular stores in mouse pancreatic acinar cells by hydrogen peroxide. J Membr Biol 179:27–35
Weber H, Roesner JP, Nebe B et al (1998) Increased cytosolic Ca2+ amplifies oxygen radical-induced alterations of the ultrastructure and the energy metabolism of isolated rat pancreatic acinar cells. Digestion 59:175–185
Kim MH, Cho HS, Jung M et al (2005) Extra-cellular signal-regulated kinase and AP-1 pathways are involved in reactive oxygen species-induced urokinase plasminogen activator receptor expression in human gastric cancer cells. Int J Oncol 26:1669–1674
Mata A, Marques D, Mesquita MF, Singh J (2002) Effect of extra-cellular magnesium on secretagogue-evoked amylase secretion in the isolated rat parotid gland segments. Mag Res 15:161–165
Rinderknecht H, Marbach EP (1970) A new automated method for the determination of serum-amylase. Clinica et Chemica Acta 29:107–110
Michalek R, Templeton D (1987) Description of an automated assay for measurement of alpha-amylase in vitro from rat parotid gland slices. Gen Pharmacol 18:555–558
Baum BJ, Ambudkar IS, Helman J et al (1990) Dispersed salivary gland acinar cell preparations for use in studies of neuroreceptor-coupled secretory events. Methods Enzymol 192:26–37
Bejarano I, Lozano GM, Ortiz A, García JF, Paredes SD, Rodríguez AB, Pariente JA (2008) Caspase 3 activation in human spermatozoa in response to hydrogen peroxide and progesterone. Fertil Steril (In press). doi:10.1016/j.fertnstert.2007.08.069
Petersen OH (1992) Stimulus-secretion coupling: cytoplasmic Ca2+ signals and control of ion channels in exocrine acinar cells. J Physiol 448:1–51
Schulz I, Streb H, Bayerdorffer E, Thevenod F (1985) Stimulus-secretion coupling in exocrine glands: role of inositol 1,4,5-trisphosphate, calcium and cAMP. Curr Eye Res 4:467–473
Ambudkar IS, Lockwich T, Hiramatsu Y et al (1992) Calcium entry in rat parotid acinar cells. Mol Cell Biochem 114:73–77
Ambudkar IS (2004) Cellular domains that contribute to Ca2+ entry events. Sci STKE 2004:pe32
Baum BJ, Ambudkar IS (1988) Regulation of calcium handling by rat parotid acinar cells. Mol Cell Biochem 82:67–73
Mata AD (2003) Influence of magnesium on salivary gland secretion: physiological and pathophysiological studies. PhD Thesis, University of Central Lancashire, Preston, United Kingdom
Fulda S, Scaffidi C, Susin SA et al (1998) Activation of mitochondria and release of mitochondrial apoptogenic factors by betulinic acid. J Biol Chem 273:33942–33948
González-Matheos A, Camello PJ, Salido GM et al (2001) Effect of xanthine oxidase-catalyzed reactive oxygen species generation on secretagogue-evoked calcium mobilization in mouse pancreatic acinar cells. Biochem Pharmacol 62(12):1621–1627
Chakraborti T, Das S, Mondal M et al (1999) Oxidant, mitochondria and calcium: an overview. Cell Signal 11:77–85
Jacobson J, Duchen MR (2002) Mitochondrial oxidative stress and cell death in astrocytes-requirement for stored Ca2+ and sustained opening of the permeability transition pore. J Cell Sci 115:1175–1188
Acknowledgments
This work was supported by MEC-DGI Grant BFU2007-60091.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Mata, A., Marques, D., Martínez-Burgos, M.A. et al. Effect of hydrogen peroxide on secretory response, calcium mobilisation and caspase-3 activity in the isolated rat parotid gland. Mol Cell Biochem 319, 23–31 (2008). https://doi.org/10.1007/s11010-008-9873-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-008-9873-7