Abstract
Promoting patient care is a priority for all healthcare providers with the overall purpose of realising a high degree of patient satisfaction. A medical centre server is a remote computer that enables hospitals and physicians to analyse data in real time and offer appropriate services to patients. The server can also manage, organise and support professionals in telemedicine. Therefore, a remote medical centre server plays a crucial role in sustainably delivering quality healthcare services in telemedicine. This article presents a comprehensive review of the provision of healthcare services in telemedicine applications, especially in the medical centre server. Moreover, it highlights the open issues and challenges related to providing healthcare services in the medical centre server within telemedicine. Methodological aspects to control and manage the process of healthcare service provision and three distinct and successive phases are presented. The first phase presents the identification process to propose a decision matrix (DM) on the basis of a crossover of ‘multi-healthcare services’ and ‘hospital list’ within intelligent data and service management centre (Tier 4). The second phase discusses the development of a DM for hospital selection on the basis of integrated VIKOR-Analytic Hierarchy Process (AHP) methods. Finally, the last phase examines the validation process for the proposed framework.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Remote healthcare services can be beneficial to patients in isolated communities and remote regions by enabling them to receive care from doctors or specialists far away without having to travel to visit them [1,2,3,4,5,6]. Remote healthcare systems in telemedicine have gained considerable attention due to their significant role in the lives of people [2, 3]. For remote patients, continuous monitoring from a distant hospital is highly desirable to ensure adequate care and provide suitable guidelines for proper medication [4]. In current telemedicine systems, data are processed through three main tiers, namely, sensors (Tier 1), gateway (Tier 2) and medical centre server (Tier 3) [2, 5, 7], as illustrated in Fig. 1. Tier 1 involves gathering individual health vital signs through interoperable medical devices, such as electrocardiography (ECG), blood pressure (BP) and blood oxygen saturation level (SpO2) sensors. These devices send the collected data to Tier 2. Tier 2 aggregates the data collected from all monitoring devices and transmits the data to the remote server through an external gateway that provides long-range communication. Tier 3 (medical centre server) is a remote computer located in the medical institution for data real-time monitoring by physicians or a database for post-processing.
In this context, the requirement of telemedicine should consist of three tiers: Tiers 1, 2 and 3. Tiers 1 and 2 can represent the client side [2, 6, 7], whereas Tier 3 represents a medical centre connected with remote hospitals and medical professionals to provide healthcare services [8, 9]. A compressive review of literature is essential to highlight and scrutinise healthcare service provision in telemedicine applications and medical centre servers in detail. Further investigations also need to highlight the challenges and open issues in providing healthcare services through the medical centre server in telemedicine applications. In addition, the methodological aspects for providing healthcare services within the medical centre server need to be highlighted to manage and control healthcare service provision for patients and overcome the related challenges in telemedicine architecture. Figure 2 demonstrates the literature review framework for the medical centre server. The remaining parts of this article are composed of three sections as follows: “Comprehensive review” Section presents the comprehensive review studies, “Methodology” section reports the methodological aspects of the three distinct and successive phases and “Conclusion” Section presents the conclusion.
Comprehensive review
This section presents a detailed description of a literature review background for this article. A systematic review protocol for the area of telemedicine systems is presented in the next section.
Systematic review protocol
Method
The scope of this study is covered by the most significant keywords, which are ‘telemedicine’, ‘triage’, ‘priority’ and ‘sensor’, and excludes any other studies on telemedicine, such as surveys and reviews. Moreover, the scope is limited to English literature but considers all health-related areas. Three reliable databases were selected to search for target articles: (1) ScienceDirect, (2) IEEE Xplore and (3) Web of Science (WoS). These particular databases were selected to cover the scientific and technical literature and provide extensive insight into researchers’ efforts in a wide yet relevant range of disciplines. Study selection consisted of searching the literature sources, followed by three iterations of screening and filtering. In the first iteration, duplicate articles were excluded and only articles from the (2012–2017) were collected. In the second iteration, filtering was carried out by reading titles and abstracts and excluding articles out of our domain. In the third iteration, articles were filtered after a thorough full-text reading and articles out of our domain and criteria were excluded, as shown in Fig. 3. All iterations applied the same eligibility criteria followed by screening and reviewing. The search was conducted on January 2017 by using the search boxes of the ScienceDirect, IEEE Xplore and WoS databases. A mix of keywords were used containing ‘medical system’, ‘telemonitoring’, ‘e-health’, ‘telemedicine’, ‘telehealth’, ‘healthcare services’, ‘remote monitoring’ and ‘mobile doctor’ in different variations, combined by the ‘OR’ and ‘AND’ operators; followed by ‘triage’ and ‘priority’ in different variations, combined by the ‘OR’ and ‘AND’ operators; followed by ‘sensor’. The explicit query text is shown at the top of Fig. 3. Other additional options were used in each search engine to ignore book chapters and other types of reports other than journal and conference articles. We choose journals and conference articles because these two venues are the most likely to include up-to-date and appropriate scientific works pertinent to our survey on this emergent trend of telemedicine. Any article that satisfied our criteria, which are listed in Fig. 3, was included in this research. This research set an initial target of mapping the space of research on our title into a general and coarse-grained taxonomy consisting of three categories derived from a previous study on the literature with no restrictions. After the initial removal of duplicate articles between databases, we excluded articles that did not achieve our eligibility criteria in three iterations of filtering and screening. The exclusion criteria included the following: (1) the article is not written in the English language; (2) the article focuses on a particular part of telemedicine technology; and (3) the target is general telemedicine technology, whereas our focus is on healthcare service provision, patient prioritisation, patient triage, healthcare service management, disaster management, network failure, sensors in telemedicine and security of telemedicine [10,11,12,13,14,15,16,17,18].
Taxonomy analysis
The initial query search resulted in 3064 articles: 911 from ScienceDirect, 1496 from IEEE Xplore and 657 from WoS, for the years 2007–2017. Unfortunately, we could not download 2 scientific articles from WoS due to accessibility issues. Articles were filtered following the sequence adopted in this article and three classes were adopted. A total of 1612 papers were collected from (2012–2017), of which 65 were duplicate papers amongst the mentioned databases, resulting in 1547 papers. After the titles and abstracts were scanned, 1264 additional papers were excluded, resulting in 283 papers. The last full-text reading excluded 164 papers, leaving 119 papers in the final set. These remaining articles were read thoroughly for the major purpose of determining a general map for the research conducted on this emerging topic. The final set of articles is divided into three major categories: sensor based, gateway based and medical centre server. As a result of the taxonomy analysis, specific patterns and general categories were observed in the telemedicine area. Figure 4 illustrates the mapping and domains of telemedicine applications (yellow mapping refers to the scope of this research):
Sensor based (Tier 1)
This section describes and summarises the technologies and issues of sensors in telemedicine which can provide reliable and continuous monitoring for patients. Wireless body area networks (WBANs) consist of wireless sensors that consider tiny intelligent hardware for collecting and transmitting the vital signals of patients [19]. In the literature, the sensor-based category (Tier 1) has been studied in numerous domains, namely, reliability, energy efficiency, quality of service (QoS), security- and privacy-based sensors, evaluation- and assessment-based sensors and ontology-based sensors.
In the first domain, numerous studies have addressed the reliability of sensor technologies except in four main areas: link quality and packet delay, congestion control, electromagnetic interference (EMI) and false alarm detection (FAD).
Various studies on link quality and packet delay are available. The study by [20] developed real-time publish-subscribe middleware functions into the healthcare system and maintained a set of QoS to support real-time data transmission. Another study introduced two scheduling algorithms to fulfil the QoS requirements in WBANs and surpass the starvation mode of packets without the highest priority [21]. In [22], an architecture was presented to handle the dynamic behaviour and heterogeneous traffic in WBANs for the system related to the healthcare domain. Another study presented a new traffic-sensitive WBAN by adopting a non-preemptive priority queue discipline [23]. The study by [24] proposed a media access control (MAC) protocol for considering the priorities of multiple bio signs with a number of characteristics and setting up a low packet delay time to ensure the effectiveness of the data. The study by [25] focused on the healthcare monitoring scheme and the structure of sensors with simulation results. In [26], an infrastructure-based method was presented to enhance the quality of telehealth applications by managing the distributions and qualities of Internet traffic amongst the devices connected in home area network environments. The study by [27] improved the performance of the MAC protocol of WBAN that adopted traffic prioritisation and an adaptive resource allocation on the basis of users’ medical condition and channel conditions. The last study in this area by [28] presented a compositional probabilistic response time analysis approach to probabilistic real-time systems in BASNs with fixed priority preemptive scheduling.
A few studies have been carried out on the second area in reliability, that is, congestion control of sensor technologies. The study by [29, 30] focused on controlling the protocol and congestion detections for the remote monitoring of user healthcare condition through WBAN. The study by [31, 32] presented a protocol to manage the congestion in wireless sensor network (WSN) healthcare applications. In [33], a hybrid scheme for priority-based congestion avoidance was presented for WSN to avoid congestion problems and save energy by providing an efficient mechanism.
Some studies have also been carried out EMI, which is the third area in reliability. The study by [34] reduced the number of patients who are forced to disconnect from the network while keeping the EMI on sensors at a needed level. In [35], a priority scheme was introduced for nonmedical and medical devices, and effective wireless healthcare service systems were enhanced.
The last area in reliability is FAD. FAD detects and reduces false alarms generated by medical sensors related to the monitoring of patients and is expected to achieve the best efficiency, accuracy and smart alarm system. In the study by [36], a novel FAD architecture was presented in cyber-physical systems (CPS) for healthcare application to overcome the confusion that generates a large number of false alarms and minimises the efficiency of the overall healthcare service.
The second domain addressed in Tier 1 is the energy efficiency of sensors in telemedicine technologies. Numerous studies have addressed the energy efficiency of sensor technologies in two perspectives: traffic routing and transmission data packet. In the traffic routing perspective, [37,38,39,40,41,42] focused on high energy efficiency and robust data transmission by reducing energy consumption, prolonging network lifetime and guaranteeing on-time task execution by increasing system predictability. In [43,44,45], priority-based time slot allocation scheme was presented for WBAN to achieve energy efficiency. The study by [46] presented green cloud-assisted healthcare services on WBANs and considered the sensory frequency of the physiological signals of different body components and the data transmission amongst the sensor nodes of WBANs. The study by [47] focused on the transmission data packet perspective, which ensures reliable traffic dissemination and customised channel access for intra−/inter-body communication.
The third domain addressed the QoS of sensors in telemedicine technologies. The studies by [19, 48,49,50,51] focused on QoS for WBAN, which is a provisioning parameter to extract QoS performance metrics such as packet loss rate, throughput and delay.
The fourth domain of sensors addressed the security and privacy of sensor data in telemedicine technologies. The study by [52] presented a prototype biomedical sensor application that implemented TinyECC to secure the wireless communications amongst sensor nodes and study the feasibility of using TinyECC in real-time sensor networks. The study by [53] improved the secure logging of information gathered from the nodes in a wireless sensor network. Meanwhile, the study by [54] provided multiple levels of security to achieve encryption and a distance bounding test to deny long-distance attacks; the method is used in body area networks (BANs) for medical devices where security is imperative. The study by [55] presented a cryptographic hash algorithm to preserve and protect data integrity. After analysing the features of X73PHD (specially its built-in security), integrating healthcare enterprise (IHE) profiles related to these applications and other research works, [56] proposed a comprehensive IHE that was dependent on an X73PHD extension containing additive layers adapted to various e-health and mobile health (mHealth) applications.
The fifth domain addressed the evaluation- and assessment-based sensors in telemedicine technologies. Some studies conducted the performance evaluations of the standard IEEE 802.15.6. The study by [57] evaluated this standard in terms of packet delivery rate, latency and power efficiency at the MAC layer while satisfying the ISO/IEEE 11073 requirement. Meanwhile, the study by [58] evaluated this standard in the performance of IEEE 802.15.6 when applied on different sensors from the Cane Network eHealth Project. The study by [59] assessed the effectiveness of wearable health-monitoring devices in minimising the loading of primary care patients and enhancing the communications amongst different healthcare parts. The study by [60] presented an evaluation of a miniature wireless vital signal monitoring for potential trauma triage in the intensive care unit (ICU). Finally, the last domain in Tier 1, namely, ontology-based sensors, describes wearable sensor platforms. A novel method called mainstream magnetic and inertial measurement unit was presented by [61] to describe the characteristics and capabilities of wearable body sensor platforms.
Gateway based (Tier 2)
Gateway in the telemedicine environment is a general term for the use of mobile phones (handheld devices) and other wireless technologies and communication devices to inform users or consumers about preventive healthcare services in medical care [7, 62].
In the literature, gateway-based sensor (Tier 2) was studied in various domains, such as disaster management, network management, ambient assisted living (AAL), integration and aggregation, treatment support and disease surveillance, mobile user interfaces (MUI) adaptation, decision support system (DSS) and evaluation- and assessment-based gateway.
In the first domain, numerous studies have addressed treatment support and disease surveillance. Some of them [63, 64] conducted studies to monitor and manage patients with chronic diseases, as well as the BP, heart rate (HR) and body temperature, either by using biometrics, such as mobile machine learning model, or a new device, namely, Arduino Mega micro-system. Other studies [65, 66] introduced applications that can adapt to other diseases, including high BP, diabetes and fever, through biometric devices such as thermometer, glucometer and densitometer. In another study [67], a new scheduling technique was presented to transmit the patient’s information from an Android application based on the sensitivity of the user’s status. The study by [68] presented a social media system, such as a software application to track the vaccination coverage of children in the rural community. In the study by [69], a system was developed to prevent dengue disease in Asian regions, especially in Sri Lanka. The study by [70] investigated a mechanism that focused on major depression diseases by providing personalised and adaptive daily interactive sessions to treat patients with the mentioned disease. The study by [71] presented a continuous, non-invasive and wireless monitoring for Parkinson disease patients. The study by [72] presented a coaching approach known as Personal Coaching Systems which uses on-body sensing integrated with context-aware feedback and smart reasoning.
A few studies have addressed disaster management, which is the second domain in the gateway category. The study by [73, 74] presented an mHealth system by using tsunami-stricken disaster scenarios and introduced a platform for developing a field accident and emergency centre intelligent monitoring system. Another study by [75] proposed a real-time assessment system for patients which uses mobile electronic triaging integrated with crowd source and sensor information. Another system was introduced in [76] to provide a situational awareness in indoor/outdoor settings for rescue operations and urban searches. The study by [77] focused on tracking pilgrims who are under safe conditions in case of natural disasters in the holy area. The study by [78] presented a Ripple Project that created a medical BAN of sensors used in disasters to provide assistance in triage and gather physiological data of patients.
A few studies have likewise addressed integration and aggregation area, which belongs to the third domain in the gateway category. The study by [79] presented a linear sequential data modelling approach (i.e. GUDM) with an expert-centric priority-based approach. Another study by [80] proposed a theory-based approach and highlighted the design of decisions amongst architecture, technology and algorithmic solution. In [81], ubiquitous healthcare environments were integrated in virtual organisations. Another study by [82] focused on aggregation data by proposing a cloud-assisted WBAN-based architecture. The study by [83] introduced a priority-based health data aggregation scheme for cloud-assisted WBANs with privacy preservation.
Moreover, several studies have addressed network management, which is the fourth domain in the gateway category. One of these studies [84] focused beyond WBAN communications either by proposing a radio resource allocation scheme or introducing a priority-aware pricing-based capacity sharing scheme. The study by [85] proposed a multiple-attribute decision-making handover algorithm, which assists the mobile patient and dynamically selects the best network by providing a ranking order amongst available candidates. Another study by [86] proposed an incentive-compatible mechanism for transmission scheduling in e-health networks with delay-sensitive medical packets. In the study by [87], a multi-user sharing scheme was proposed with diverse medical information. The study by [88] investigated an approach dependent on mobile ad hoc networks to solve the challenges of enhancing communication reliabilities related with patient monitoring.
The fifth domain addressed in the gateway category is AAL. Few studies have addressed this domain. In the study by [89], a ubiquitous system was developed involving the processing of video and audio that automatically support fall detection for patients. Another study by [90] designed and implemented a semantic, data-driven and cloud-based back-end platform by offering knowledge-based services and information. The study by [91] modelled the activities of a single human inhabitant in a home environment to simulate a daily activity. The developments in information and communication technologies (ICTs), such as in IoT and CPS, was the last study in this domain [92].
Only a couple of studies have addressed the DSS, which is the sixth domain in the gateway category. One such study [93] proposed a model for enhancing the quality of decisions in mHealth. Another study by [94] introduced a lightweight rule-based reasoning system that was designed and optimised to build knowledge-based DSSs that are efficiently embeddable in mobile devices.
Only one study [95], which focused on a context- and rule-based approach for designing adaptable MUIs in mHealth, addressed the MUI adaptation, which is the seventh domain in the gateway category. Moreover, only one study has addressed the evaluation- and assessment-based gateway, which is the eighth domain in the gateway category. In [96], the feasibility of medical alarm dissemination through mobile phones was evaluated in an urban environment when congestions or failures occur in the infrastructure of the networks.
Medical centre server (Tier 3): an overview
Medical centre server is a remote computer that helps medical staff and hospitals analyse and monitor vital signs and provide appropriate services to patients in real time. The server can also manage, organise and support professionals in telemedicine. It normally comprises a medical institution server, patient history and database and service generation [2].
In the literature, medical centre server (Tier 3) has been studied in seven domains in accordance with the features and contributions offered in the server side of telemedicine, which are environmental management, evaluation and assessment, collaboration fields, security- and privacy-based server, big data analysis, patient triage and providing healthcare services.
The first domain is evaluation- and assessment-based server. In the literature, few studies focused on evaluation and assessment in the medical centre server of telemedicine. The studies by [97, 98] evaluated the features and effectiveness of common telehealthcare systems, which aim to establish user-friendly, ubiquitous and patient-centred systems for caregivers and their patients, dependent on the continuous applications of clinical guidelines and semantically combined electronic health records. Another study by [99] evaluated the effectiveness of a Web-based healthcare system that helps patients record measurements of BP, weight and steps walked per day.
Security- and privacy-based server is the second domain in telemedicine servers. In the literature, few studies have addressed security and privacy in the medical centre server of telemedicine. A study by [100] focused on the security of medical data generated by medical sensor networks by using the proposed mechanism that ensures confidentiality, integrity and fine-grained access control to outsourced medical information. The study by [101] addressed e-healthcare society security by using the proposed low-cost-and-secure communications system and demonstrated how the different actors in e-healthcare societies could interact with one another in a secure manner.
The third domain in telemedicine server is collaboration fields. This domain describes and reviews different activities and collaboration fields that communicate with one another in the medical centre server of telemedicine. In the literature, many studies have addressed collaboration fields in all but two areas: cooperative environment and tele-expertise between professionals. In particular, cooperative environment area means integrating a u-healthcare environment in the virtual organisation. Hence, individual physical environments share information gathered from the sensors and computers or devices through WSN. The study by [8] focused on decentralised data, where the PHRs can be stored and accessed by distributed data centres with high performance. Another study by [102] improved healthcare information systems to provide a good level of information and introduce distributed and heterogeneous resource access solutions that perfectly meet user requirements in various situations. Furthermore, numerous studies have presented tele-expertise between professionals, which is the second area in collaboration fields. These studies [103,104,105,106] focused on tele-expertise that assists medical and health professionals in collaborating with one another to treat and diagnose patients and appropriately decide, by sharing knowledge and expert advice that can be used as explanation elements for medical professionals in their decision-making process.
Big data analysis is the fourth domain in telemedicine servers. Big data as a concept refer to data that exceed the processing capacity of conventional database systems [107]. The data move rapidly, are large and do not fit the structures of conventional database architectures [108]. In the healthcare domain, big data refers to electronic health datasets so large and complex that they are difficult to manage with traditional or common data management methods and traditional software and/or hardware [109]. Big data characteristics can be defined by six Vs [110,111,112,113,114,115,116], namely, volume, value, variety, velocity, variability and veracity. In the literature, some studies involved big data analysis in the server of telemedicine. In the study by [117], a new algorithm was proposed to discover frequent activities in a smart home history log adopting temporal relationships amongst sensor activations. The study by [118] presented an integrated and comprehensive framework for big data analytics services in smart healthcare networks, namely, SmartHealth, which addresses the challenging concerns in the processing and storage of data from different sensors by leveraging cloud computing technologies.
Finally, the last three main domains in the server category, namely, patient triage, environment management, and providing healthcare services, will be discussed in the following subsections.
Environment management
Environment management is important for healthcare institutions to focus on managing health organisations because of various reasons, such as dynamic processes and distributed hospital organisation. Therefore, these institutions need to review the process of managing emergency facilities [22].
In the literature, few studies involved environment management in the medical centre server of telemedicine. In the study by [119], a cognitive radio network, along with the hospital management system, was designed. This study developed a new algorithm/network called Bio Cog for the implementation of cognitive networks to transmit medical data which uses efficient frequency spectrum allocation method. In the study by [120], a multi-agent system (MAS) was proposed and used to manage, monitor and collect vital signs of sensors, such as BP, (HR), body temperature and respiratory rate in hospitals. The gathered data are then stored in a database. The proposed MAS consists of four agents, namely, admin, control, query and data agents, which perform data reduction using Epsilon approximation. The study in this domain by [121] developed and implemented a management DSS that can assist medical professionals in managing their organisations and anticipating the feature of overcrowding, as well as optimising the paediatric emergency department (PED) function characterised by stochastic arrivals of patients leading to service overload.
Patient triage
The term ‘triage’ comes from the French word ‘trier’, which means ‘to sort’. The concept was first used in warfare when a system was needed to prioritise all casualties and provide immediate care to the most seriously injured. According to [122], in the hospital domain, triage has traditionally relied on the ability of nurses to prioritise cases, which involves initially sorting patients who arrive at the ED by quickly identifying those who require immediate care due to urgent, life-threatening conditions.
An experienced triage nurse evaluates a patient’s status, notes any changes and determines the patient’s priority for admission to the ED and for important treatments [123]. Triage is the system of sorting patients by order of treatment necessity in large-scale emergencies [124, 125]. Triage protocols are used to detect the priority of a patients’ diagnoses depending on the severity of their status [42, 126]. In accordance with medical guidelines [127], the triage system is performed by a triage officer and/or designee(s), when possible. Triaged patients are moved to appropriate treatment areas. A triage area with designated spaces may be necessary to separate patients recently moved from the incident site from those already triaged and those ready to be moved to the suitable treatment area. The triage personnel needs to keep a tally of the total number of patients triaged and the number assigned to all categories. Furthermore, the triage officer has to repeat the triage sequence at regular intervals to monitor the changes in patients’ conditions.
In the literature, numerous studies have addressed triage but in different areas: triage inside the ED and triage outside the ED.
For inside the ED perspective, overcrowding in EDs is a growing worldwide issue [128]. A medicine committee institute in the USA has described ED overcrowding as a national crisis [128] because it compromises the safety of patients and timeliness (time to appropriate treatment) [129]. The study by [130] developed a constant and remote monitoring system of vital signals that allows measuring HR, respiratory rate and body temperature in the emergency room to assist in the patient triage process. The system keeps track of the patient’s condition for suitable treatments during emergency situations by processing the data gathered from a temperature sensor and a photoplethysmograph. The study by [131, 132] developed a WSN for the remote monitoring of the HR of patients for triage purpose inside the ED to help the medical team track and treat the status of the patients depending on the severity of their conditions. Studies in this perspective were conducted by doctors and nurses to either increase the knowledge of triage nurses or improve the triaging scoring guidelines. These studies are applicable in the hospital setting, specifically in the ED, and are not directly related to our research scope. However, the summary is provided in the interest of completeness and to show how the medical side (doctors/nurses) improved the triage process in the ED.
The second perspective is triage outside the ED in the telemedicine environment, where patients are physically far from hospitals and EDs. The improvement of triage processing is a cooperative research between computer engineering and medical guidelines, given that the triage process involves implementing certain computing algorithms in portable devices on the basis of medical guidelines [133].
The study by [134] introduced a lightweight and low-cost wearable electronic triage device with a sensing system to monitor the vital signs of each casualty and classify them based on the severity of their conditions, such as minor, delayed and major. The study by [135] proposed automatic self-tagging methodology that adopts body sensor networks (BSNs) transmitting relevant vital signals, such as HR, mental status and respiratory rate. The proposed approaches help patients in the surgery department and elderlies at home. Another study by [136] presented an approach to assist in triage during mass casualty incidents (MCIs) and provide the tactical planning of rescue operations with constant updates on triage information. Another study by [2] proposed the multi sources healthcare architecture (MSHA) framework to improve the efficiency of healthcare challenges, such as scalability, and improve the processes of remote triage and patient priority.
Providing healthcare services
Different techniques and methods were used to improve the provision of healthcare services. In the literature, various studies have addressed healthcare services by using different systems. The study by [137] presented a 3D real-time interactive system, namely, physical therapy as a service (PTaaS), to help therapists remotely monitor patients’ performance within an exercise balance assessment program, adopt the features in the PTaaS interface and offer verbal, auditory and visual cues to achieve suitable exercise movements. The study by [138] proposed a framework that consists of WBSNs, service-oriented architecture and services based on the Web to provide healthcare services to patients, caregivers and doctors in both clinical and non-clinical settings. These services include alert emergency service, medication, video conferencing and general information, such as providing emergency numbers, information about nearby hospitals in the patient’s locality, mail IDs and caregiver detail for fast health status intimation. The study by [139] proposed a hierarchical particle swarm optimisation algorithm with ortho cyclic circles that work efficiently in dynamic environments. The algorithm receives the request in cloud from different resources, employs multi-swarm interaction and implements cyclic and orthogonal properties in a hierarchical manner to provide the nearest optimal solution. Service provision refers to the delivery of alert SMS about the patients’ status (in case of abnormality) to the registered physicians. The details of the SMS are as follows: ID of the patient, value of abnormal parameters, abnormality, gender, age and name. The study by [140] developed an architecture dependent on the ontology ability of monitoring the workout routine and healthcare recommendation to patients with chronic diseases. This architecture enables patients with chronic diseases to improve their workout routine and eating habits. In the study by [141], a people-centric sensing framework was presented for monitoring and providing healthcare services to people, especially the elderly and disabled, with service-oriented emergency response in the case of an abnormal health status. Relatives can visualise the status of alarm, abnormal physiological parameters and location of disabled patient. The study by [142] developed a data-driven platform for clinical DSSs. It presented a DDS that supported an ambulance emergency medical service for patients with acute coronary syndrome (ACS). The service was provided by selecting a near and appropriate specialised hospital and the available physician depending on the patient condition. The study by [143] proposed a novel e-healthcare model combined with a cloud computing platform to provide healthcare services in internet of vehicles (IoV) environments on the fly while traveling. This model is dependent on theoretical game approaches to calculate payoff and VM scheduling mechanisms and handle the resources on the clouds. The study by [144] presented an architecture that combined telehealth and telecare monitoring, namely, inCASA, which supports simultaneous healthcare follow-up, mental health and evaluation of the psychological condition of elderly people dependent on monitoring a set of parameters for each disease, tracking patients in home environments and profiling/diagnosing patient’s habits and activities. The study by [145] presented a remote-monitoring system for monitoring HR and transmitting the vital signs to the monitoring centre to generate fast-acting and alert medical teams and physicians if the health of the elderly patient is at the risk level. The study by [146] developed an e-health consultancy system utilising cloud computing, namely, On-Cloud Healthcare Clinic, which assists physicians and caregivers to provide recommendations, suggestions and treatment of non-communicable diseases in remote and rural communities in Bangladesh. The study by [147] presented an architecture for first aid operations depending on two phases: firstly, the ambulance collects and sends up to three outdoor ambient videos of paramedics providing first aid to the patient, and secondly, a patient in the second stage (after being loaded on the ambulance) is being visited with an ultrasonography. The main idea of the study [148] is remote monitoring and updating patients with information on new medicine, which can be performed by a prescriber by using the Web according to the scheduling and condition of the patient. The data are gathered remotely from the sensor side, and then the alarm will generate based on the emergency level. Through the Web, the system can help save future references and update drug information in accordance with the need after comparing the drug-taking habits of patients. The study by [149] described SERVANDO, a distributed open platform that manages the therapy prescribed to patients with visual difficulties through simple notifications of doses and drugs. The study by [150] presented a wireless transmission system for physiological healthcare by adopting ZigBee technology. The proposed system can be used by groups or individuals. It can diagnose the general status of patients anytime, conduct long-term tracking for daily measurement of patients in hospitals and be used for self-examination and tracking of nurses to minimise the incidence of fatigue-related mistakes. The study by [151] presented health-monitoring approaches for patient’s emergency care and an ambulance alert alarm under mobile cloud-based telecare and community cloud controller systems. The procedure of the system is for a nurse to identify the emergency level of the patient inside the ambulance, then move the patient to the available physician and nearest appropriate specialised hospital and transmit the capture image from the camera to the doctors.
Healthcare service scalability challenges
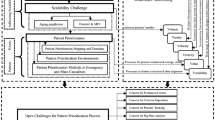
Numerous challenges exist in healthcare service provision, such as medical centre failure and scalability in ageing population and disasters [2, 7, 152, 153]. However, the scope of this work is related to the scalability, triaging and provision of healthcare services, which caused another major problem, which is, reducing the available healthcare services provided through the accurate system. Figure 5 explains the mentioned challenges (in yellow).
Scalability is a challenge in healthcare service provision in disaster scenes and population ageing (i.e., increase in demand for healthcare services and online doctor visits) [2, 154, 155]. The rising costs of healthcare services and the aging of the global population add to the restrictions in applying telemedicine networks to the delivery of common healthcare services [156, 157]. Increases in the number of patients lead to major problems, which in turn increase the demand for healthcare services provided to users on the basis of the triage level. Healthcare services in hospitals are affected by various issues, so the availability of services can be decreased at any time in accordance with patients’ demand [142, 153, 158, 159]. As the number of patients continuously increases in accordance with disaster scenes and population ageing, healthcare services and medical resources will reduce in the hospital, causing less availability of healthcare services. Moreover, as the number of patients continuously increases, the medical centre should effectively use any developed system to accommodate this growing system demand. Increasing healthcare service demands have likewise led to the urgent need for effective and scalable healthcare services [152, 160].
Healthcare systems should connect with several hospitals to increase the healthcare service availability by managing and balancing these services in real time. According to [152], scalability identifies how research could respond innovatively and contribute towards efficient and effective healthcare service provision systems. Additional healthcare services will be needed, especially those provided outside of the hospitals. The increase in the number of users is expected to occur in several aspects, such as population ageing [2, 153, 161, 162], disasters and MCIs [163], as shown in Fig. 6 and described in the following subsections.
Population ageing
Ubiquitous healthcare services are becoming increasingly popular, especially under the urgent demand of the global ageing issue [7, 164]. Population ageing is regarded as the main problem in healthcare services [165] because the number of patients continuously increases. This problem constitutes a challenge that needs to be faced in all developed countries. The current demographic changes are the main reasons that lead to the gradual and persistent growth of older generation groups [166], which cause permanent and serious problems, including the incidence of ageing diseases and economic and social burdens [166,167,168]. Numerous age-related chronic disease problems have emerged from the momentary increase in the ageing phenomena, and they are directly affected and define the determination of medical care expenses [169,170,171]. Chronic diseases that increase with the surge of population ageing (e.g. diabetes, hypertension and heart failure) render healthcare management a highly relevant issue for health systems all over the world [169]. An ageing population suffering from long-term adverse conditions is a challenge to global healthcare systems in terms of quality of care delivery [171, 172]. Therefore, any accretion in the number of ageing population patients is considered a challenge in telemedicine systems [2]. Rapid population ageing increases the amount and severity of chronic diseases, requiring healthcare researchers to reconsider existing healthcare models [173]. Therefore, researchers have begun to examine how healthcare service provision systems can be improved in response to the population ageing problem.
Disasters and MCIs
Disasters are sudden calamitous events that seriously disrupt the functioning of a society or community and cause human, economic and material or environmental losses that force a community to cope and help vulnerable individuals affected by these disasters by utilising available resources [174]. According to [175], MCIs, including earthquakes, floods, stampedes, wildfires, mass road accidents, cave mishaps and building collapse accidents, usually result in a large number of casualties. During MCIs, the emergency medical service resources, including personnel and equipment, can be easily overwhelmed by the number and severity of casualties. MCIs can engage many types of responders and agencies, such as paramedics, ambulances, the police or firefighters; consequently, a high level of logistics is necessary to coordinate all of them [7, 136].
Healthcare service during disasters is different from routine services in numerous ways. Firstly, patients are triaged according to their severity and survival probability [176, 177]. Given large numbers of critical patients, those who are dead or expected to die should not be offered attempted resuscitation. Furthermore, disasters extensively require quality communication amongst healthcare caregivers and gathering facilities such as surge-capacity care venues, operating rooms and EDs [178,179,180]. Disasters also cause a large scale of victims, some uninjured bystanders and others with minor injuries. Although disasters occur infrequently, they raise the need for pre-hospital care providers equipped with the skills of triage and treatments not used in routine practice [181]. Scholars have compared the different strategies of triage and applied technologies to track patients during disasters [182, 183]. Monitoring patients remotely has been recommended to enhance the decision making of clinicians during disasters [181, 184].
In conclusion, the increasing demand for healthcare services due to an ageing population and disasters engenders major challenges [152] because the temporarily explosive number of patients during disasters and MCIs cause a temporary need for services. This scenario poses a significant challenge and reduces the available healthcare services in certain hospitals, hence requiring an efficient system to accommodate such a growing demand for services.
Critical review and analysis
The increasing number of users of remote monitoring systems per unit area because of ageing population and disasters is considered a major problem for providers of healthcare services [2, 152, 153]. Furthermore, the number of available healthcare services and medical resources will reduce in certain hospitals and render services insufficient due to scalability challenges [153].
The analysis in “Environment management” Section demonstrates that several studies have presented systems that healthcare institutions may use to manage the dynamic processes of the health organisation, managing the patients in ED and managing the process of emergency facilities and proposed measures to preserve the quality of care for consumers. However, no study has presented solutions for managing and controlling the load on healthcare services amongst hospitals.
The analyses in “Patient triage” and “Providing healthcare services” sections show that several systems and methods have been designed in the literature to provide healthcare services, focusing on patients who require healthcare services provided by an individual provider of healthcare services (e.g. hospital, professional and medical centre) [138, 139, 141, 145, 146, 148]. Some of the proposed systems provide recommendations and suggestions on the basis of limited data of patients (i.e. vital signs) without triage level, other systems issue an alert when the vital signs become abnormal, and others only provide directions to the nearest hospital.
Therefore, healthcare services should be provided to patients through distributed hospitals, and the growing demand for these services should be managed amongst hospitals to avoid the insufficient availability of healthcare services in each one [153]. In the field of healthcare research, systems that can accommodate the variation in health conditions and provide healthcare services to users in large-scale areas are important [2]. The required system should also triage patients and provide healthcare services remotely [2]. Such a system, if made appropriately, can save lives, amongst other advantages.
Furthermore, previous studies [142] and [2] are considered important in this field of research. In [142], a clinical DSS of an ambulance was proposed to select a proper hospital for patients with ACS. The data and information obtained from the patients are classified into two: therapy patient at home and transport patient to a hospital or leave recommendations for a patient to visit hospital by taxi. In case of transportation, the proper hospital is selected on the basis of the number of patients in queue for therapy in each hospital. In the diagnosis process, the patients do not undergo a triage process; therefore, the accuracy of healthcare services is poor. Moreover, the process of hospital selection does not consider the availability of services in each hospital. To ensure accuracy, the process of hospital selection should be done according to the number of available services because these services vary from one hospital to another. In the selection process, the number of available services is a more important factor than the number of patients in each hospital.
Reference [2] addresses patient triage in the mHealth environment by using a multisource data fusion module to calculate the triage level and consequently sort patients in the server. However, [2] did not investigate the use of an accurate engine in the medical centre server in providing healthcare services. Furthermore, the author mentioned that the multisource data fusion module can determine the compatible package of tips; these tips can be displayed directly through the mHealth graphical user interface. Therefore, no clear engine exists on the server side (Tier 3) to represent the service-providing process for each patient.
In conclusion, data and service management systems should connect with hospitals and telemedicine systems to share medical resources and avoid the acute shortage of healthcare services in case of an increased demand for healthcare services. In such as case, a healthcare service management system can manage the load on healthcare services amongst hospitals as well identify an appropriate hospital to handle and provide accurate services to the patients. Moreover, chronic heart disease in a remote monitoring environment has been set as a case study in this research as proof of concept. Further investigation on chronic heart disease in the remote monitoring environment is demonstrated in the following section.
Chronic diseases in remote healthcare monitoring
A chronic disease is a permanent, nonreversible condition that may require a long period of supervision, observation, or care and that interferes with a person’s physical, psychological, and social functioning [185]. Several remote monitoring strategies that involve telephone interviews, IoT-based technologies or other sophisticated systems have been presented [186]. Chronic diseases have become amongst the hottest issues in telemedicine applications over the world [2]. For example, the clinical expenses for chronic diseases in the United States are projected to reach 80% of the overall healthcare expenses [160], and 100 million Americans in 1995 were affected with one or more chronic conditions [185]. Furthermore, more than 150 million humans could experience chronic conditions by 2020 [160], and chronic diseases account for 70% of all deaths and are the leading causes of disabilities amongst persons older than 15 [185]. Chronic diseases also impose a considerable burden on individuals and health systems because of frequent unscheduled visits to the ED and lengthy hospital admissions [5, 154]. Healthcare researchers and developers have focused on out-of-hospital health monitoring, specifically in the home setting where telemedicine is used, because the continuous and daily monitoring of physiological data (e.g. ECG or BP signals) is significant in the surveillance of chronic diseases [187]. Homecare is a vital and effective mode of managing chronic illnesses [188]. An essential need exists for home management of patients using telemedicine [189], which is a popular and efficient approach that could ensure care continuity, especially for chronic diseases [190]. Remote patients, who live far from hospitals and use telemedicine, may suffer from different chronic conditions, such as diabetes, chronic heart disease, chronic BP and other diseases [160, 191, 192]. However, heart disease has been set as a case study in the current research.
Cardiovascular diseases are the principal causes of deaths worldwide [193, 194]. The World Health Organization estimated that 12 million deaths occur worldwide yearly because of heart disease [195]. Chronic heart disease includes several types of diseases, the symptoms of which can be manifested in patients. According to the American Heart Association [160], approximately 55% of patients with heart disease die because of arrhythmia, which is the serious type of heart disease. Moreover, another type of chronic heart disease is heart failure, which does not mean that the heart stops beating but actually means the heart is not pumping blood as well as it should. According to [194], in 2013, 1 in 9 death certificates (284,388 deaths) in the United States mentioned heart failure. The automatic diagnosis of heart disease is a huge real-world medical problem that affects the health and working performance of patients, especially the elderly [195]. Telemedicine has a vital role in the efficient delivery of patient healthcare with different types of cardiovascular diseases [196]. Several studies have been conducted on remote monitoring for the management of cardiac diseases and cardiac home cures, demonstrating its potential for cost savings but with the same health outcome [169]. Furthermore, e-healthcare techniques have displayed considerable impacts on chronic heart failure care [197]. In home telemonitoring, both mortality and hospitalisation reductions were reported [197,198,199]. In addition, vital signs, including SpO2, BP and ECG, have been proven very necessary in triage because they offer an objective complement to the triage decision and improve inter-rater consistency [122].
Sources used to measure patients’ medical vital signs
Many medical sensors are utilised to measure patients’ vital signs. Vital signs are useful in monitoring and detecting medical problems and can be measured in medical units, at homes or elsewhere [200]. Medical sensors devices play a vital role in telemedicine and remote healthcare monitoring. Continuous health monitoring requires the sensors of a system to be active round the clock [152]. Currently, a persuasive demand exists for the integration and exploitation of heterogeneous biomedical information to enhance medical research, point of care and clinical practice [201]. As the focus of the current research is chronic heart disease, the medical sources related thereto are presented in Table 1. References [2] and [158] identify and validate four medical sources related to chronic heart disease. These sources comprise one text source and three signal sources.
On the one hand, BP, ECG and SPO2 sensors are significant, and they need to be employed in this research. On other hand, nonsensory data are also necessary in remote healthcare monitoring [2, 153]. Text data (i.e. complaints) can be used as another medical source to improve the accuracy of triage and healthcare services [2]. Furthermore, the connection amongst the vital signs and the complaints are operationalised as the changing relative importance of vital signs [204].
Integrating a group of heterogeneous sources related to chronic heart disease in one healthcare platform is important in healthcare monitoring [2, 153, 201].
In conclusion, multisensor and nonsensory data (text data) should be used for the prioritisation and triage of patients with chronic heart disease. Patients should be prioritised according to these sources and the related features to ensure that the treatment is given in an appropriate and timely manner. The patient prioritisation methods and techniques are described further and summarised in the next section.
Patient prioritisation methods and techniques
Patient prioritisation is important for all types of diseases, especially chronic heart disease [2, 153]. Different prioritisation methods and techniques were reviewed in previous studies. These prioritisation methods and techniques are being used in different countries all over the world. The most important studies that explored the improvement of the prioritisation methods and techniques are presented in Table 2.
As shown in Table 2, the majority of the studies target patients on the incidence scene/site or disaster, whereas only [2, 133, 205, 207, 208, 210] target patients remotely. Furthermore, the majority of the studies did not address scalability as a challenge except [2, 205, 214]. Only two studies, namely [2] and [202] focused on chronic disease as a long-term status related to remote patients, whereas the majority of studies focused on illnesses or injuries in general during MCIs and disasters. However, amongst the studies on remote healthcare monitoring, only [205] proposed a prioritisation system and ordered a large scale of patients by comparing each patient with others to offer compatible healthcare services based on the emergency status, whereas the other studies prioritised patients as categories and groups.
To overcome the limitations of the other studies, the present research adopts the methodology proposed in [205] (integrated back-forward adjustment for weight computation and technique for order performance by similarity to ideal solution) to rank a large scale of patients with chronic heart disease and consequently provide services and treatments based on the triage level. After the patients are prioritised, the present research proposes that the healthcare services and treatment to be provided to patients with chronic heart disease should depend on the emergency status; thus, we need to explore and investigate triage standards and guidelines which are described in the next section.
Triage system standards and guidelines
Different triage system standards and guideline were reviewed in previous studies. These triage systems are being used in different countries all over the world. However, they are discrete. The majority of these triage systems are presented in Table 3.
Table 3 shows that 13 of the 15 triage systems reviewed are paper-based triage systems, whereas only two are digital triage systems. Furthermore, the majority of these systems have been used as traditional triage EDs, whereas only START, JumpSTART, PTT, STM and Military Triage have been used during MCIs and disasters. Moreover, six of these triage systems, namely ATS, CTAS, METTS, ESI, MSHA and MTS used five categories; three triage systems, namely EWS, START and JumpSTART, use four categories; and only MEWS uses three categories. The categories of the remaining triage systems are not specified in the literature. Although paper triage tags are often used, they exhibit the following disadvantages [133]: (i) triaging is performed by officers only, (ii) triage for patients who are using telemedicine and are far from triage officers and EDs is not addressed, (iii) collecting data on physiological conditions is difficult and (iv) real-time monitoring is provided. Therefore, The trend remarkably points to the digitalisation the triage systems, such as MSHA and eMEWS [2]. According to [2], triage digitalisation has become a necessary trend to provide patients with healthcare services based on the severity of their triage level. Digital triage should satisfy the following requirements: firstly, remote patients, wherever they are, should be triaged. Secondly, new symptoms and features should be used for triaging users. Thirdly, the guideline scores for chronic diseases should be improved with the use of sensory data and text. Finally, the accuracy of triaging should be improved with an efficient mathematical theory so that the triaging level is selected by an efficient algorithm and not by human opinion. In view of these requirements, MSHA algorithm is more efficient than eMEWS. Moreover, MSHA is one of the significant algorithms for triaging and categorising patients. Table 4 illustrates the evaluation of the performance of the MSHA algorithm and the requirements that should be adopted in the present research.
Table 4 presents a general description and general technical review of the performance and contribution of MSHA. On the basis of the requirements for our work, MSHA has several disadvantages compared with our work. To overcome these disadvantages, the MSHA algorithm must be requalified to develop accurate triage and package localisation systems and consequently satisfy our requirements. After the prioritisation and triage processes, healthcare services should be provided to patients who are in the most critical condition and according to the patients’ triage level. The healthcare services packages are described and summarised in the next section.
Healthcare services packages
As mentioned in “Providing healthcare services” section, many studies have focused on improving service efficiency in specific emergency conditions. Furthermore, healthcare services should be provided as rapidly and accurately as possible to patients with the most urgent emergency case. The analysis of the previous studies shows that various services are provided to patients with various kinds of diseases, including those that related to patients with chronic heart disease. According to [2], healthcare services for chronic disease can be divided into five packages based on the severity of patients. Thus, the present research adopts this concept to provide compatible healthcare services according to the five triage levels and emergency cases. The packages and related services according to each triage level are discussed in succeeding subsections.
Package1 (Alarm)
Providing healthcare services, especially to patients with risk level (red colour), are considered the greatest challenges for healthcare systems. Patients at the risk level will not survive if not treated soon enough; thus, they should receive prompt medical attention [229]. A person with a severe chronic heart disease is classified as red. Amongst many services, surgery room, team and doctor are prepared for patients with risk level. Table 5 presents the different service packages.
Package 2 (Alarm)
Patients at the urgent level (orange) require medical attention, which is not necessarily prompt. Injuries are potentially life threatening, but they can wait until the patients at the risk level (Package 1) are stabilised and evacuated [229]. This package includes many services similar to the patient at the risk level, as shown in Table 6.
Package 3 (Directions)
Patients at the sick level (yellow) do not require ambulance transport. They require medical attention when all higher-priority patients have been served, treatment when practical and transport and/or discharge when possible. Services in this section are presented in Table 7.
Package 4 (Directions)
Patients at the cold state level (blue) require minor treatment and advice for supervised medication. They do not require ambulance transport. Services in Package 4 are shown in Table 8.
Package 5 (Directions)
Patients at the normal level (green) do not require treatment. Their vital signs or their conditions are stable. The services for these patients are enumerated in Table 9.
In conclusion, the number of available healthcare services in a package vary from one hospital to another [142, 153, 158, 159]. The data and service management centre aims to manage the wide variation in service availability in different hospitals. Managing and providing healthcare services from an appropriate hospital on the basis of the number of available services represent a multi-attribute complex decision problem. Thus, a multi-decision-making method should be used to solve the intricate task of specifying the appropriate hospital on the basis of the number of available services.
Recommended solution and pathway
The distinct recommended solution in this article is explained in this section. The process of choosing an appropriate hospital from which to receive treatment after the evaluation of the number of available services is known as hospital selection [153]. Hospital selection is required to avoid the insufficiency and reduction in the number of healthcare services in hospitals [142, 153]. Such a selection process involves the simultaneous consideration of the number of healthcare services from multiple attributes generate a data variation that considered as a multi-attribute decision problem. Thus, the process of hospital management and selection to manage the load on healthcare services amongst hospitals and select the appropriate hospital to provide healthcare services for chronic heart disease patients is a complex multi-attribute decision problem. As such, decision-based methods should be used for hospital selection to deal with this complex problem. In this section, multicriteria decision-making (MCDM) methods are presented as a recommended pathway and solution to deal with multi-attribute decision problem of hospital management and selection.
MCDM: Definition and importance
The book by Keeney and Raiffa [235] defines MCDM as ‘an extension of decision theory that covers any decision with multiple objectives. A methodology for assessing alternatives on individual, often conflicting criteria, and combining them into one overall appraisal’. Another important definition was given by Stewart and Belton [236]: ‘an umbrella term to describe a collection of formal approaches, which seek to take explicit account of multiple criteria in helping individuals or groups explore decisions that matter.’
MCDM is the most well-known decision-making method, and it is a part of the operations research that deals with decision problems with respect to various criteria [237, 238]. MCDM involves structuring, planning and solving this type of problems [237]. The purpose of MCDM is to assist decision makers who are facing such problems [239]. The use of MCDM is rapidly becoming popular because of its ability to improve the quality of the decisions through a process that is more rational, more explicit and more efficient than conventional processes [240]. Table 10 shows an example of a multi- attribute problem with alternatives and criteria.
In Table 7, Y1, Y2, …, Ym are suitable alternatives that decision makers should rank; in this research, they are the hospitals. In the same table, X1, X, …, Xn are the attributes/criteria against which the performances of all the alternatives are evaluated; in this research, they represent the healthcare services. The objectives of MCDM are as follows: (1) to prioritise the alternatives in decreasing order of performance, (2) to classify the viable alternatives amongst a set of others and (3) to assist data miners in selecting the appropriate alternative [241]. Accordingly, the appropriate and best alternative(s) will be scored. Thus, unsurprisingly, MCDM in the healthcare field has rapidly become familiar and popular [242,243,244,245,246,247,248,249]. Through the several existing MCDM techniques, decision makers of healthcare can promote their decision-making process by systematically acquiring the appropriate solution [250, 251].
MCDM techniques and methods
Several MCDM theories have been explored. Figure 7 shows the most commonly used MCDM techniques, which use different notations [244, 252].
The advantages and disadvantage of the popular MCDM methods shown in Fig. 7 are provided in Fig. 8 [234, 190, 237,238,239,240,241, 249, 250, 251].
According to our analysis, none of the discussed methods have been used to rank distributed hospitals to manage and control the process of healthcare service provision in a telemedicine system. However, TOPSIS and VIKOR are applicable to cases with numerous alternatives and criteria. Both methods are also specifically convenient to use when quantitative or objective data are given. TOPSIS determines a solution with the shortest distance to the ideal solution and the greatest distance from the negative-ideal solution, but it does not consider the relative importance of these distances [242]. By contrast, VIKOR is functionally related to discrete-alternative problems. This technique is one of the most practical routes for solving real-world problems. The benefit of VIKOR is its capability to find the best alternative rapidly. Thus, VIKOR is appropriate for situations with many alternatives and attributes [242].
However, the primary shortcoming of VIKOR is the lack of provision for weight elicitation and judgment consistency checking [242]. Therefore, VIKOR requires an effective technique to obtain the relative importance of various criteria with respect to the objective, and AHP provides such a technique. However, AHP is used to set weights for objectives on the basis of the preferences of stakeholder [253], and it is significantly restricted by the human capacity for processing the information; therefore, the 7 ± 2 would be the comparison ceiling [254]. The most recent trend regarding MCDM techniques is the integration of two or more techniques to compensate for the weaknesses of a single technique [255,255,257]. AHP and VIKOR have become a commonly accepted integrated MCDM method in many studies (e.g. [258,258,259,260,262]).
As a conclusion, an integrated VIKOR–AHP method is recommended to manage and control the process of healthcare service provision in hospitals. It ranks distributed hospitals and selects the best hospital according to the number of healthcare services based on the triage level of patients with chronic heart disease.
Methodology
This section presents an overview and explanation of the three-phase methodology of the hospital selection in the telemedicine environment. The first phase (identification) is designed to identify the target telemedicine tier in the telemedicine architecture (“Identification phase” section). In view of the many limitations of the existing architecture, a new design of telemedicine architecture is proposed for providing healthcare services. This phase also includes a case study of chronic heart disease and the dataset (“Identification of patients with chronic heart disease and data set” section). Moreover, this phase also includes a new four-level remote triage and package localisation (4LRTPL) within Tier 4. This phase also includes dummy data to represent a dataset for the numbers of available services in hospitals, and distributed hospitals as healthcare providers. The resulting decision matrix (DM) is dependent on the crossover of ‘multi-healthcare services’ and ‘hospital list’ in the intelligent data and service management centre (Tier 4) within the new design of telemedicine architecture. The second phase (development) involves developing a decision-making solution for hospital selection based on the integrated AHP–VIKOR method (“Development phase” section). Finally, the third phase (validation) validates the performance of the proposed hospital selection methodology objectively (“Validation phase” section). The mentioned phases are demonstrated in Fig. 9.
Identification phase
This phase aims to propose a new design of telemedicine architecture (Tier 1–Tier 2–Tier 3–Tier 4) and identify the target tier. This phase also aims to identify a new four-level remote triage and package localisation (4LRTPL), the chronic heart disease patients and dataset, dummy dataset for three healthcare service packages as proof of concept and distributed hospitals. The information acquired from the given analysis is used to propose a DM based on ‘multi-healthcare services’ and ‘hospital list’ in Tier 4 within the new telemedicine architecture.
Identify the target tier within the telemedicine architecture
The current telemedicine architecture contains three tiers: sensor based (Tier 1); gateway based (Tier 2), which represent the client side; and medical centre server (Tier 3), which represent remote server. Data from the medical sensors and manual inputs (text) are collected from the patient on the client side (Tier 1 and Tier 2). All data are then sent to the server for further processing. In the medical centre server (Tier 3), distributed hospitals are connected and controlled. Tier 3 involves a remote computer, which is connected to the distributed hospitals for real-time monitoring. Figure 10 shows the healthcare service flow from the distributed hospitals to the medical centre server. The vital signs originate from the user in a sensor (Tier 1) to the gateway (Tier 2) and then transmitted to the medical centre server (Tier 3).
Propose a new design of telemedicine architecture (Tier 1–Tier 2–Tier 3–Tier 4)
This research aims to propose a new design of telemedicine architecture by produce intelligent data and service management centre (Tier 4) to the current design. The existing telemedicine architecture has various limitations in relation to healthcare service provision [153]. Furthermore, as mentioned in “Critical review and analysis” section, various challenges exist in healthcare service provision. The healthcare services in a hospital are affected by many factors; thus, the availability of services can decrease at any time because of scalability challenges. Consequently, healthcare services and medical resources will reduce in the hospital and result in insufficient availability of healthcare services.
The increasing demand for healthcare services have highlighted the essential need for an effective and scalable design of telemedicine architecture to cope with such a growing demand [7, 263]. References [153] and [263] asserted that healthcare services amongst hospitals should be managed and balanced in case of scalability challenges. Therefore, this research aims to manage and control the healthcare services load amongst hospitals by proposing a new design of telemedicine architecture for providing healthcare services. As mentioned, this design includes an intelligent data and service management centre (Tier 4), which is connected to telemedicine systems to share the medical resources and avoid the acute shortage of healthcare services in case of increased demand for these services. In such a case, Tier 4 receives vital signals from three biomedical sensors (SpO2, BP and ECG) and text input (Text data) from the patient on the client side (Tier 1 and Tier 2) in each city. Subsequently, Tier 4 can manage the load of healthcare services amongst hospitals that are connected to the medical centre server (Tier 3) and identify an appropriate hospital, on the basis of the patient’s city, to handle and provide accurate healthcare services.
Figure 11 shows telemedicine systems exist in n cities. Each telemedicine system has a certain number of users per unit area. Tier 4 is connected to the telemedicine systems to share the medical resources and avoid the acute shortage of healthcare services. Therefore, Tier 4 can manage the load on healthcare services amongst hospitals that are connected to Tier 3 and identify an appropriate hospital to handle and provide high-quality and accurate healthcare services to patients.
In this research, the intelligent data and service management centre (Tier 4) is the part in which all processes and decisions are occurring. Several issues and problems in the current telemedicine architecture need to be resolved. The issues and healthcare service challenges that must be addressed in Tier 4 are as follows:
-
Scalability: The increasing demand for healthcare services must be accommodated and managed by managing and controlling the load on healthcare services amongst hospitals. Tier 4 can select and rank distributed hospitals to offer healthcare services to patients with chronic heart disease.
-
Services Weighting: A specific weight should be assigned to each service in the healthcare packages to evaluate the hospitals by a set of expert and decision-making techniques.
-
Ranking the hospitals: The hospitals should be ranked and ordered the according to their available services and they should be queued according to the number of healthcare services in each package in these hospitals.
Identification of patients with chronic heart disease and data set
In this step, the type and number of patients have been specified. Owing to this research’s significance over others, patients identified are remote patients with chronic heart diseases. Sensors and texts were used to transfer patients’ vital signs and complaints to Tier 4 for monitoring and assessing their situation. Considering the scalability issue, a large scale of 500 patients will be involved in this research. The data set is adopted from the studies in the remote prioritisation and triage area [2, 149].
Identify patient prioritisation
As mentioned in “Patient prioritisation methods and techniques” section, several prioritisation techniques have been analysed and discussed. The study by [205] was identified as the best and novel methodology to be adopted in the present research. Figure 12 illustrates the prioritisation method, which has been implemented within Tier 4, receives vital signals (SpO2, ECG and BP) and text data from 500 patients (client side) with chronic heart diseases and then ranks the patients in real time based on integrated BFAWC and TOPSIS method. More details and explanation about the prioritisation process are available in [205].
Identification of new four-level remote triage and package localisation within Tier 4 (4LRTPL)
According to the new design of telemedicine architecture presented in Fig. 11, the analysis in “Triage system standards and guidelines” section, identifying a new four-level remote triage and package localisation which can categorise many patient conditions is essential within Tier 4. A new triage known as the four-level remote triage (4LRTPL) is identified to solve these problems. As mentioned previously, the new triage can be derived from the study [2], and the presented research will re-qualify most steps of MSHA algorithm and keep the other steps which are meant to be adaptive with the scope of the requirement. The entire process of identifying and developing MSHA algorithm can be found in the reference of [2], whereas this section will provide a detailed explanation about the updated and new steps that are only relevant to re-qualifying MSAH, resulting in the new 4LRTPL that will be presented in this section.
Requirements for constructing a new triage and package localisation (4LRTPL)
The requirement tiers for new triage (4LRTPL) are client side and intelligent data and service management centre.
-
Client side: In this stage, data of patient (sensors and text) are collected and sent to Tier 4.
-
Tier 4: This is the process stage which involves a data and service management centre for real-time monitoring. This tier will analyse the data collected from client side (Tiers 1 and 2) and then calculate the triage level and compatible services for patients. Some requirements in Tier 4 should be fulfilled.
-
Manage and compute the data received from client side (Tiers 1 and 2)
-
Capability to estimate the medical status of user
-
Provide a computation method for triage and package localisation
-
4LRTPL workflow
All data from the sensors are collected by gateway and then sent to Tier 4. As mentioned previously, 500 patients (Client side) have been prioritised in Tier 4; thus, the new triage has calculated the triage level for patient according to their order. In this case, data are fused in the fusion module. The output of this module is an estimate of the emergency level of the patient, resulting in four outputs: triage level, triage code (TC) and healthcare service packages.
The module in Tier 4 processes all collected data and TC value and mimics a triage system which categorises patients based on the severity of their status. TC value is used for linking with appropriate healthcare service packages.
Data fusion module
The (4LRTPL) fusion is also based on the fundamentals of data fusion. The presented research keeps the data fusion module as in the study by [2] which are feature extraction, data alignment and association and state estimation and prediction. Figure 13 illustrates the process of identifying triage level for prioritised patients in Tier 4 by using data set of the patient with heart chronic disease. These triage levels are linked with healthcare service packages.
Output of the data fusion module
Three types of decisions resulting from this stage contain the following: triage level, TC value and healthcare service packages in Table 11.
-
TC: This value can be calculated by the sum of all the scores of the features in the MSHA. The TC value is a parameter used for triaging patients based on their emergency status.
-
Triage Level: Four triage levels are presented in this research. According to [2], the conclusion for all features range from 0 to 100. These numbers are used in the evidence theory method to determine the triage level.
-
Package Localisation: The four appropriate healthcare service packages are as follows: Package 1 for patients with risk level, Package 2 for patients with urgent level, Package 3 for patients with sick level and Package 4 for patients with normal situation.
Based on the TC value and the triage level, the ‘multi-source data fusion module’ can locate the most compatible healthcare service package. Four levels of triaging patients linked with three healthcare service packages are related to the new triage according to the literature, as discussed in “Healthcare services packages” section and according to medical symptoms and guidelines of the MSHA algorithm. The presented research combines the cold state and normal levels in one level because the patients in these levels do not need healthcare services from hospitals; in this situation, the patient is only informed that ‘You are in good health. You do not need a hospital ☺.’
4LRTPL algorithm
In data fusion techniques, evidence theory is suitable for combining information from different sources. In this section, the sequence of the processing data of 4LRTPL algorithm is presented. The mathematical representation of the 4LRTPL uses evidence theory and if-then statements according to the mathematical representation of the Dempster–Shafer theory.
If-then statements are used to define the four triage levels linked with healthcare service packages. The consequence of the if-then statements is the triage level (Y), which was explained previously in Table 11 and healthcare service packages. To describe the data processing in the new triage and package localisation algorithm (4LRTPL), the new algorithm replaces Stage 3, integrates evidence theory fusion with if-then statement and excludes the fuzzy c-means (FCM) to avoid complexity. In addition, the process of FCM is not needed because the fuzzy role is a reasoning system in which the notions of truth and falsehood are considered in a graded fashion, whereas the process of using FCM in MSHA considers classical logic conclusions which are either true or false to link TC value with packages. The order of the sequences of 4LRTPL algorithm are as follows:
-
1.
Feature extraction stage
-
2.
Evidence theory fusion stage, which includes the establishment of the score values
-
3.
If-then statement stage
Triage level calculation linking with healthcare service packages
In this stage, the if-then statements are applied. The input of this stage is a decimal value for all the triage levels, and the outputs are the final triage level and the appropriate healthcare service packages. Table 12 presents the eight sets of designed clusters. Rules 1 to 4 in the first four clusters are used to determine the three triage levels. Rules 5 to 8 in the second four clusters are used to package localisation by defining the three healthcare service packages. The description for each package of healthcare services is explained in Table 11. The updated healthcare service algorithm in terms of functions is presented in Table 13.
Identification of dummy data for healthcare services in distributed hospitals
Dummy data can be used as placeholder for both testing and operational purposes. For testing, dummy data can also be used as stubs or pad to avoid software testing issues by ensuring that all variables and data fields are occupied. In this research, the numbers of available healthcare services in distributed hospitals cannot be represented by real data because the availability and number of healthcare services in the proposed system can be derived only when such system connects with real hospitals in the real environment and works in real-time processing healthcare services provided by hospitals. In addition, dummy data are widely used in numerous areas [264, 265] as well as in telemedicine [149, 266, 267]. Therefore, in this section, the use of dummy data acts as the numbers of available healthcare services in hospitals. This factor is represented as a criterion in the DM of this research. As mentioned in “Output of the data fusion module” section, three packages are provided for patients with chronic disease. According to a disparity in the number of these services in hospitals owing to the capacity and crowding of each hospital, the dummy data will generate virtual numbers for these services for each hospital. This process can be represented by using dummy data. Tables 14, 15, and 16 show the representation of dummy data for the three packages in each hospital.
Distributed hospitals
This research adopted 12 hospitals as a ‘proof of concept’, which represents the alternatives in the DM. Each hospital contains three packages, and the services of these packages are illustrated in “Identification of dummy data for healthcare services in distributed hospitals” section. These hospitals, which are connected to the medical centre server, are controlled and managed through Tier 4. The process of hospital selection is based on the number and available services considered as multi-attribute DM. The proposed DM will be explained in the next section.
Propose a DM within Tier 4
The overall architecture and the design of Tier 4 is shown in Fig. 14.
Several hospitals are used to provide healthcare services for patients with heart chronic disease according to their triage level. Medically, providing an accurate healthcare service for all patients from the individual hospital is insufficient because the hospital may be exposed to acute shortage of services and medical resources in case of increasing demand for health services. Therefore, as mentioned in “Distributed hospitals” section, the focus of this research is to manage and control 12 hospitals through Tier 4 as a data centre management and provide healthcare services from the appropriate hospital. In this research, all services provided to the patient according to the triage level are simultaneously gathered and assessed for each hospital by a computer algorithm. The hospitals are then compared with one another based on the number of available services according to the designed method. One way to achieve this aim is to propose a DM based on a crossover of ‘multi-services’ and ‘hospital lists’ according to the number of available services for each hospital.
Identify DM
In this research, three DMs are identified within Tier 4 for Packages 1, 2 and 3 according to the triage level of patients with heart chronic disease. As mentioned in “Identification of dummy data for healthcare services in distributed hospitals” section, six healthcare services in Package 1 will be provided to the patient in risk level, six healthcare services in Package 2 will be provided to the patient in urgent level and four healthcare services in Package 3 will be provided to the patient in sick level. These services are provided by 12 hospitals. Hospitals send the number of available services to the medical centre server and then to Tier 4 as a record for saving and updating in the database. Although Tier 4 can calculate the triage level of each patient to identify the appropriate package, the hospitals are compared with one another based on the number of available services of the selected package in the database of Tier 4. In this context, the DM of Packages 1, 2 and 3 are shown in Tables 17, 18 and 19, respectively.
Evaluation of DM
This section presents a description of DM evaluation for hospital selection. Tier 4 receives the datasets of patients. After identifying the priority for each patient and determining the triage level for the selected patient, Tier 4 can identify the appropriate package for the patient. As mentioned in “Distributed hospitals” section, Tier 3 is connected with 12 hospitals, and Tier 4 is controlled and managed by the hospitals connected with Tier 3. To provide healthcare services from an appropriate hospital, these hospitals contain three packages as discussed in “Distributed hospitals” section. Each package has a different number of services. Tables 11, 17 and 19 illustrate the DM that shows all the hospitals must be ranked according to the number and available services in each one. In this DM, the hospitals represent the alternatives, while the healthcare services represent the multi-criteria used to evaluate the hospitals. However, these services have a different effect on hospital evaluation. The ranking of the hospitals represents a multi-criteria problem because this process involves simultaneous consideration of multiple services with respect to the proper weight assigned for each service to score the hospitals according to the number and availability of the services. Thereafter, the final decision that represents the hospital selection according to the numbers of available services is difficult and cannot be determined in a normal case. A decision-making algorithm and computer-based approach are significant for mitigating hospital selection complexity. Figure 15 shows the framework of identification DM for hospital selection through Tier 4. The development of a decision-making solution for hospital selection will be presented in the following section.
Development phase
Problems emerge when each hospital that provides healthcare services to patients has several attributes (services), and each DM can provide diverse weights for these attributes. In typical situations, weights can be assigned by experts (cardiologists). This situation is attributed to the varied opinions of experts on the criteria that influence the focus on the hospitals. Therefore, hospital selection according to the number of available services is often difficult. In addition, a Tier 4 which aims to give a score for a hospital might give more weight to the service rather than to other less important services.
In this instance, the experts are required to set weights that represent various cases. Six evaluators are used to set the preference weight for services in three packages. This scenario is recommended for servers that rank hospitals according to the number of available services. Thus, those with a high number of services have high rank levels, whereas those who have few services have low rank levels.
The method involves the integrated MCDM methods for ranking hospitals in Tier 4. The integrated MCDM methods require AHP to calculate attribute weights regarding to the goal to identify how each of them contributes to this decision. The VIKOR technique is then utilised to rank the hospitals based on quantitative information through which criteria are measured. As a final point, the hospitals are ranked according to their number of available services from the highest to the lowest levels. The structure of the integrated AHP–VIKOR method for ranking hospitals is shown in Fig. 16.
AHP
In this stage, several steps are involved to assign proper weights to the multi-service criteria using AHP [268]. The AHP procedure includes the following steps [269, 270].
-
Step 1:
To start the AHP procedure, the problem is modelled as a hierarchy containing the decision goal and the criteria must be designed. The hierarchy of the criteria used in the AHP pairwise for three packages is demonstrated in Fig. 17.
Figure 17 shows the hierarchy (tree) of the AHP (for each package) that was utilised in this article to obtain the weights. The first level of the hierarchy acts as the goal, while the lower level represents the criteria.
Package 1 has six criteria, namely, prepare surgery room, prepare surgery team, prepare doctor, prepare O2 supplier, send an ambulance and provide medications. Package 2 has six criteria, namely, prepare emergency room, prepare consultant section, prepare doctor, prepare O2 supplier, send an ambulance and provide medications. Package 3 has four criteria, namely, prepare consultant section, prepare doctor, prepare O2 supplier and provide medications. To obtain the weights, a pairwise comparison between the criteria (of each package) will be achieved with respect to the main goal.
-
Step 2:
To determine a decision, AHP builds the pairwise matrix comparison in the following Eq. (3.1):
The comparisons (relative importance) of each criterion are measured according to a numerical scale from 1 to 9 [271, 272]. These relative scales (1 to 9), as shown in Table 20, are used to show the experts’ (cardiologists) judgments for each comparison. Each cardiologist decisively sets these judgments based on their knowledge and experience.
-
Step 3:
To show the relative importance of all the attributes in each package, a pairwise comparison questionnaire is designed and distributed to a geographically diverse convenience sample of experts in heart diseases (cardiologist). The experts show their judgments on the criteria of each package (services) through the nine scales to compare them and show the relative importance for each. A sample of the attribute pairwise comparisons in the evaluation form distributed to the experts is illustrated in Fig. 18.
NPC = n × (n − 1) /2, where NPC is the number of required pairwise comparisons, and n is the number of criteria.
In this stage, the decision-making team will be set up. The AHP extracts the weight of importance of each service from the pairwise comparison using a preference and judgments from the decision-making team. In this research, six experts are selected to show their preferences and judgments on the services used in the AHP. The selection was made based on the idea that having the hospital selection depend exclusively on the number of services is not reasonable without giving more importance to one service over another.
Six copies of evaluation forms for each package are revised by the experts, with 15 comparisons for the services of Package 1, 15 comparisons for the services of Package 2 and 6 comparisons for the services of Package 3. These pairwise comparisons are presented to the experts, and their responses are obtained. At this point, all the comparisons for services of each package are performed.
-
Step 4:
Every element of matrix A is normalised by dividing each element in a column by the sum of the elements in the same column to create a normalised pairwise comparison matrix Anorm. Anorm is the normalised matrix of A(1), where A(xij) is given by Eq. (3.2), Anorm (aij), such that
-
Step 5:
In this step, the AHP pairwise uses mathematical calculations to convert the judgments and give weights for each service (in each package). After attaining the responses on pairwise comparisons, the reciprocal matrix is created from the pairwise comparisons, and the AHP pairwise derives the priorities for each service (in each package) which represent the importance of each service with respect to the goal. The weights of the decision factor i can be calculated as in Eq. (3.4):
where n is the number of compared elements. The AHP measurement steps are designed to gain the weight according to the evaluator’s preference. Table 21 presents the AHP steps for the weight preferences used for six evaluators for Package 3. The other designs of MLAHP steps for weight preferences for Packages 1 and 2 are shown in the appendix (Tables 22 and 23).
-
Step 6:
In this step, the CR that expresses the internal consistency of the judgments that will be entered are calculated. [273] defined the following terms to develop a quantitative measure of the degree of inconsistency within a pairwise comparison matrix. We define the CI that is calculated by Eq. (3.5) as follows:
The RI is calculated by Eq. (3.6) as follows:
CI measures the degree of inconsistency. RI is the corresponding measure of the degree of inconsistency of a pairwise comparison matrix. The CR is defined in Eq. (3.7) as follows:
CR is the ratio of CI to RI. CR is the quantitative measure, proposed by [254, 273], of the degree of inconsistency of a pairwise comparison matrix. A pairwise comparison matrix with a corresponding CR of no more than 10% or 0.1 is acceptable [254, 273, 274]. If the level of inconsistency is unacceptable, then the decision maker should revise the pairwise comparisons; otherwise, it will be ignored.
Adaptive VIKOR method for hospital ranking
In this stage, VIKOR is used to rank hospitals because it is suitable for cases with many attributes and alternatives and can rapidly identify the most suitable option. Moreover, the overall weights will be driven from the AHP to tackle the major weakness of VIKOR, which is its lack of provision for weight elicitation and consistency checking for judgments.
The available alternative scores are ranked in decreasing order, and the hospitals are ranked based on the number of available services using VIKOR method. The Q value provides an idea of which hospitals have high numbers of available services, which, according to this technique, will have the lowest Q value compared with others. The steps of VIKOR method are described in the following [242, 275].
-
Step 1:
Determine the best f∗i and worst f−i values of all criterion functions, i = 1; 2; ...; n. If the ith function represents a benefit, then
-
Step 2:
In this process, the weights for each attribute are computed based on the AHP model. A set of weights w = w1, w2, w3, ⋯, wj, ⋯, wn from the decision maker is accommodated in the DM; this set is equal to 1. The resulting matrix can also be calculated as illustrated in Eq. (3.9).
This process will produce a weighted matrix as follows:
-
Step 3:
Compute the values Sj and Rj, j = 1,2,3,….,J, i = 1,2,3,…,n by using the following equations:
where wi are the weights of criteria expressing their relative importance.
-
Step 4:
Compute the values Qj, j = (1, 2, ⋯, J) by the following relation:
where
v is introduced as the weight of the strategy of ‘the majority of criteria’ (or ‘the maximum group utility’); here, v = 0.5
-
Step 5:
The set of alternatives (hospitals) can now be ranked by sorting the values S, R and Q in decreasing order. The lowest value indicates the optimal performance.
-
Step 6:
Propose as a compromise solution the alternative (a′), which is ranked the best by the measure Q (minimum) if the following two conditions are satisfied:
-
C1. ‘Acceptable advantage:’
where (a") is the alternative at second position in the ranking list by Q, DQ = 1/(J − 1) J is the number of alternatives.
C2. ‘Acceptable stability in decision making’: Alternative a′ must also be the best ranked by S and/or R. This compromise solution is stable within a decision-making process, which could be ‘voting by majority rule’ (v > 0:5), ‘by consensus’ (v≅0.5) or ‘with veto’ (v < 0.5). Here, v is the weight of the decision-making strategy ‘the majority of criteria’ (or ‘the maximum group utility’).
Validation phase
Hospital selection is a complicated process owing to the availability of healthcare services which vary amongst hospitals. The number and type of services have important roles in the accuracy of these processes. Validation of the hospital selection results is done by utilising objective validation, as shown in the following section.
Objective validation
In this stage, statistical methods (mean ± standard deviation) are used to ensure that the hospital selection undergoes systematic ranking. The ranking results of the ranked hospitals are divided into four equal groups (as in the study of [149, 276]) and expressed as the mean ± standard deviation for each group. Mean (\( \overline{x} \)) is the average and is computed as the sum of all the observed outcomes from the sample divided by the total number, as presented in Eq. (3.14):
Standard deviation (s) is a measure that is used to quantify the amount of variation or dispersion of a set of data values, as presented in Eq. (3.15):
In practice, mean ± SD are utilised to ensure that the four groups of hospitals undergo systematic ranking. Based on the above test, hospital scoring is divided into four groups according to the prioritisation result on the integrated MCDM method to validate the result. Each group consists of an equal number of hospitals (three hospitals) that are selected based on the scoring values from the prioritisation results. The validation process is achieved using two methods based on a statistical platform, which proves that the first group should reach the highest scoring value by measuring the mean and SD. If the first group has the highest mean and SD, then comparison with the three others groups will be considered to validate the result. The second group’s means and SD results must be lower than or equal to those of the first group. The third group’s means and SD result must be lower than those of the first and second groups or equal to the second group. Lastly, the fourth group’s means and SD must be lower than those of the first, second and third groups or equal to the third group. According to the systematic ranking results, the first group should be proven statistically to be the highest group amongst other groups. The process aims to validate the hospital ranking for one patient. The scope of this research is to rank hospitals individually for 500 patients. Accordingly, 500 validation processes are achieved for 500 patients, given 1 for each valid process; otherwise, given 0. The final value of the validation process for ranking hospitals can be obtained by Eq. (3.16) as follows:
where Sum(x) is the summation of valid process, fv is the final Validation and 500 is the number of patients.
Conclusion
The number of studies on telemedicine continues to increase. However, the studies related to healthcare service provision in telemedicine applications and medical centre server have limitations that remain unaddressed. Medical centre server in telemedicine involves a remote computer for real-time monitoring to analyse the data in real time and provide patients with compatible services. The server is an attractive part of telemedicine architecture that warrants further investigation. The main contribution of this article is a comprehensive review of studies related to the topic. The systematic review protocol was conducted for the area of healthcare services in telemedicine application to determine the gaps and main challenges in providing healthcare services through a medical centre server (Tier 3). Telemedicine technologies were discussed in detail by showing their applications and architecture. As a result of the taxonomy analysis, specific patterns and general categories were observed in telemedicine. The related articles were divided into three major categories: sensor based (Tier 1), gateway based (Tier 2) and medical centre server (Tier 3). We intensively analysed environment management, patient triage and healthcare service provisions to highlight the open issues and challenges related to medical centre server in telemedicine and address the gaps. However, an increase in the number of patients is expected to occur in several aspects, such as population ageing, disasters and mass casualty incidences, all of which may give rise to a scalability challenge and reduce the accuracy of healthcare service systems. Increasing the number of users of the remote monitoring systems per unit area because of ageing population and disaster scenes is considered a major problem by providers of healthcare services. Most of these challenges are linked to medical centre server in telemedicine architecture, such as (i) the issue for managing and controlling the loading of healthcare services amongst hospitals, (ii) the individual provider of healthcare services and (iii) the acute shortage of healthcare services and medical resources. On the other hand, remote monitoring was discussed, and chronic heart diseases were identified as a case study. Moreover, different sources, namely, sensory (ECG, SpO2 and BP) and non-sensory (text data) sources were discussed and proven to be very important in prioritising and triaging patients with chronic heart diseases. Many prioritisation and triage methods were also defined and discussed thoroughly to identify the best and accurate approach. Consequently, healthcare service packages for chronic heart disease which were identified from literature were addressed in detail. This review also summarised and outlined the methodological aspects in providing healthcare services during the mentioned issues. The methodological aspects were presented based on three main phases, with each phase corresponding to a major distinct step in conducting and producing the anticipated output. The first phase (identification) was designed to identify the targeted telemedicine tier in telemedicine architecture. On the basis of the many drawbacks in the existing architecture, a new design of telemedicine architecture for providing healthcare services was proposed in phase. This phase also lists the major steps of the identification process to propose a DM based on a crossover of multi-service and hospitals lists in the intelligent data and services management centre (Tier4) within a new design of telemedicine architecture. The second phase (development) involved developing a decision-making solution for hospital selection based on integrated AHP–VIKOR methods. Thereafter, the last phase was proposed to validate the resulting framework. The proposed framework will be simulated and implemented in the future to serve as a guide for providing healthcare services within a new Tier 4 during the mentioned challenges and issues.
References
Gilpin, R., and Gilpin, J. M., The challenge of global capitalism: The world economy in the 21st century. 5th edition. Princeton: Princeton University Press, 2000.
Salman, O. H., Rasid, M. F. A., Saripan, M. I., and Subramaniam, S. K., Multi-Sources Data Fusion Framework for Remote Triage Prioritization in Telehealth. J. Med. Syst. 38(9):103, 2014.
T. H. Sanders, A. Devergnas, T. Wichmann, and M. A. Clements, Remote stphone monitoring for management of Parkinson’s Disease. in Proceedings of the 6th International Conference on PErvasive Technologies Related to Assistive Environments. 42, 2013.
J. Mirkovic, H. Bryhni, and C. M. Ruland, A framework for the development of ubiquitous patient support systems. in Pervasive Computing Technologies for Healthcare (PervasiveHealth), 2012 6th International Conference on. 81–88, 2012.
Chowdhury, M., Mciver, W., and Light, J., Data association in remote health monitoring systems. IEEE Commun. Mag. 50(6):144–149, 2012.
Acampora, G., Cook, D. J., Rashidi, P., and Vasilakos, A. V., A Survey on Ambient Intelligence in Health Care.. Proc. IEEE. Inst. Electr. Electron. Eng. 101(12):2470–2494, 2013.
A. S. Albahri et al., Real-Time Fault-Tolerant mHealth System: Comprehensive Review of Healthcare Services, Opens Issues, Challenges and Methodological Aspects. J. Med. Syst., 42(8), 2018.
Wang, J., Qiu, M., and Guo, B., Enabling real-time information service on telehealth system over cloud-based big data platform. J. Syst. Archit. 72:69–79, 2017.
Chang, M.-Y., Pang, C., Tarn, J. M., Liu, T.-S., and Yen, D. C., Exploring user acceptance of an e-hospital service: An empirical study in Taiwan. Comput. Stand. Interfaces 38:35–43, 2015.
Alanazi, H. O., Zaidan, A. A., Zaidan, B. B., Mat Kiah, M. L., and Al-Bakri, S. H., Meeting the security requirements of electronic medical records in the ERA of high-speed computing. J. Med. Syst. 39(1):1–14, 2015.
Alanazi, H. O., Alam, G. M., Zaidan, B. B., and Zaidan, A. A., Securing electronic medical records transmissions over unsecured communications: An overview for better medical governance. J. Medi. Plants Res. 4(19):2059–2074, 2010.
Hussain, M., Al-Haiqi, A., Zaidan, A., Zaidan, B., Kiah, M. M., Anuar, N. B., and Abdulnabi, M., The rise of keyloggers on stphones: A survey and insight into motion-based tap inference attacks. Pervasive Mob. Comput. 25:1–25, 2016.
Mat Kiah, M. L., Al-Bakri, S. H., Zaidan, A. A., Zaidan, B. B., and Hussain, M., Design and develop a video conferencing framework for real-time telemedicine applications using secure group-based communication architecture. J. Med. Syst. 38(10):1–13, 2014c.
Mat Kiah, M. L., Nabi, M. S., Zaidan, B. B., and Zaidan, A. A., An enhanced security solution for electronic medical records based on AES hybrid technique with SOAP/XML and SHA-1. J. Med. Syst. 37(5):1–16, 2013.
Abdulnabi, M., Al-Haiqi, A., Kiah, M. L. M., Zaidan, A. A., Zaidan, B. B., and Hussain, M., A distributed framework for health information exchange using stphone technologies. J. Biomed. Inform. 69:230–250, 2017.
Zaidan, B. B., Zaidan, A. A., and Mat Kiah, M. L., Impact of data privacy and confidentiality on developing telemedicine applications: A review participates opinion and expert concerns. Int. J. Pharm. 7(3):382–387, 2011.
Hussain, M., Ahmed, A.-H., Zaidan, A. A., and Zaidan, B. B., M Kiah, Salman Iqbal, S Iqbal, Mohamed Abdulnabi "a security framework for mHealth apps on android platform". Comput. Sec. 45:191–217, 2018.
Zaidan, A. A., Zaidan, B. B., Al-Haiqi, A., Kiah, M. L. M., Hussain, M., and Abdulnabi, M., Evaluation and selection of open-source EMR software packages based on integrated AHP and TOPSIS. J. Biomed. Inform. 53(0):390–404, 2015.
Bradai, N., Charfi, E., Fourati, L. C., and Kamoun, L., Priority consideration in inter-WBAN data scheduling and aggregation for monitoring systems. Trans. Emerg. Telecomm. Technol. 27(4):589–600, 2016.
Almadani, B., Saeed, B., and Alroubaiy, A., Healthcare systems integration using Real Time Publish Subscribe (RTPS) middleware. Comput. Electr. Eng. 50:67–78, 2016.
Bradai, N., Chaari Fourati, L., and Kamoun, L., WBAN data scheduling and aggregation under WBAN/WLAN healthcare network. Ad Hoc Netw. 25(PA):251–262, 2015.
S. Gambhir and M. Kathuria, DWBAN: Dynamic priority based WBAN architecture for healthcare system. 2016 3rd International Conference on Computing for Sustainable Global Development (INDIACom). 3380–3386, 2016.
Gündoğdu, K., and Çalhan, A., An Implementation of Wireless Body Area Networks for Improving Priority Data Transmission Delay. J. Med. Syst. 40(3):75, 2016.
Rae Hyun Kim, Pyung Soo Kim, and Jeong Gon Kim, An effect of delay reduced MAC protocol for WBAN based medical signal monitoring. in 2015 IEEE Pacific Rim Conference on Communications, Computers and Signal Processing (PACRIM), 2015. 2015; 434–437, 2015.
Y. Zhao and H. G. Kerkhoff, Design of an Embedded Health Monitoring Infrastructure for Accessing Multi-processor SoC Degradation. in 2014 17th Euromicro Conference on Digital System Design, pp. 154–160, 2015.
M. A. Shah, J. Kim, M. H. Khadra, and D. Feng, Home Area Network for Optimizing Telehealth Services- Empirical Simulation Analysis. 36th Annu. Int. Conf. IEEE Eng. Med. Biol. Soc., pp. 1370–1373, 2014.
Rezvani, S., and Ghorashi, S. A., Context aware and channel-based resource allocation for wireless body area networks. IET Wirel. Sens. Syst. 3(1):16–25, 2013.
Ren, J., Wu, G., Li, X., Pirozmand, P., and Obaidat, M. S., Probabilistic response-time analysis for real-time systems in body area sensor networks. Int. J. Commun. Syst. 28(16):2145–2166, 2015.
S. Ghanavati, J. Abawaji, and D. Izadi, A Congestion Control Scheme Based on Fuzzy Logic in Wireless Body Area Networks. in 2015 IEEE 14th International Symposium on Network Computing and Applications. 235–242, 2015.
S. Ghanavati, J. Abawajy, and D. Izadi, ECG rate control scheme in pervasive health care monitoring system. in 2016 IEEE International Conference on Fuzzy Systems (FUZZ-IEEE). 2265–2270, 2016.
Rezaee, A. A., Yaghmaee, M. H., and Rahmani, A. M., Optimized Congestion Management Protocol for Healthcare Wireless Sensor Networks. Wirel. Pers. Commun. 75(1):11–34, 2014.
Rezaee, A. A., Yaghmaee, M. H., Rahmani, A. M., and Mohajerzadeh, A. H., HOCA: Healthcare aware optimized congestion avoidance and control protocol for wireless sensor networks. J. Netw. Comput. Appl. 37(1):216–228, 2014.
J. Kaur, K. S. Saini, and R. Grewal, Priority based congestion avoidance hybrid scheme for Wireless Sensor Network. in 2015 1st International Conference on Next Generation Computing Technologies (NGCT. (ember):158–165, 2015.
Lin, D., Labeau, F., Yao, Y., Vasilakos, A. V., and Tang, Y., Admission control over internet of vehicles attached with medical sensors for ubiquitous healthcare applications. IEEE J. Biomed. Heal. Info. 20(4):1195–1204, 2016.
I. Al Mamoon, A. K. M. Muzahidul-Islam, S. Baharun, S. Komaki, and A. Ahmed, Architecture and communication protocols for cognitive radio network enabled hospital. in 2015 9th International Symposium on Medical Information and Communication Technology (ISMICT). 2015; 170–174, 2015.
Haque, S. A., and Aziz, S. M., False alarm detection in cyber-physical Systems for Healthcare Applications. AASRI Procedia 5:54–61, 2013.
X. Yuan, C. Li, Y. Song, L. Yang, and S. Ullah, On energy-saving in e-healthcare: A directional MAC protocol for WBAN. in 2015 IEEE Globecom Workshops, GC Wkshps 2015 - Proceedings, 2015.
Sudha, G. F., Karthik, S., and Ku, N. S., Activity aware energy efficient priority based multi patient monitoring adaptive system for body sensor networks. Technol. Health Care 22(2):167–177, 2014.
Rodrigues, E. M. G., Godina, R., Cabrita, C. M. P., and Catalão, J. P. S., Biomedical signal processing and control experimental low cost reflective type oximeter for wearable health systems. Biomed. Sig. Proces. Control 31:419–433, 2017.
N. Li, K. Lin, S. Yong, X. Chen, X. Wang, and X. Zhang, Design and implementation of a MAC protocol for a wearable monitoring system on human body. in 2015 IEEE 11th International Conference on ASIC (ASICON). 1–4, 2015.
Li, C., Yuan, X., Yang, L., and Song, Y., A Hybrid Lifetime Extended Directional Approach for WBANs. Sensors 15(12):28005–28030, 2015.
Hwang, T. H., Kim, D. S., and Kim, J. G., An on-time power-aware scheduling scheme for medical sensor SoC-based WBAN systems. Sensors (Switzerland) 13(1):375–392, 2013.
T. Puri, R. K. Challa, and N. K. Sehgal, Energy efficient QoS aware MAC layer time slot allocation scheme for WBASN. in 2015 International Conference on Advances in Computing, Communications and Informatics (ICACCI. 966–972, 2015.
Misra, S., and Sarkar, S., Priority-Based Time-Slot Allocation in Wireless Body Area Networks During Medical Emergency Situations: An Evolutionary Game-Theoretic Perspective. IEEE J. Biomed. Heal. Info. 19(2):541–548, 2015.
Ru Kong, C. Chen, W. Yu, B. Yang, and X. Guan, Data priority based slot allocation for Wireless Body Area Networks. in 2013 International Conference on Wireless Communications and Signal Processing. 1–6, 2013.
Chiang, H., Lai, C., and Huang, Y., A green cloud-assisted health monitoring service on wireless body area networks. Inf. Sci. (Ny). 284:118–129, 2014.
Ben Elhadj, H., Elias, J., Chaari, L., and Kamoun, L., A Priority based Cross Layer Routing Protocol for healthcare applications. Ad Hoc Netw. 42:1–18, 2016.
Sevin, A., Bayilmis, C., and Kirbas, I., Design and implementation of a new quality of service-aware cross-layer medium access protocol for wireless body area networks. Comput. Electr. Eng. 56:145–156, 2016.
Iftikhar, M., Al Elaiwi, N., and Aksoy, M. S., Performance analysis of priority queuing model for low power wireless body area networks (WBANs). Proc. Comput. Sci. 34:518–525, 2014.
Iftikhar, M., and Ahmad, I., A el analytical model for provisioning QoS in body area sensor networks. Proc. Comput. Sci. 32:900–907, 2014.
Hu, L., Zhang, Y., Feng, D., Hassan, M. M., Alelaiwi, A., and Alamri, A., Design of QoS-Aware Multi-Level MAC-Layer for Wireless Body Area Network. J. Med. Syst. 39(12):192, 2015.
D. Baehr, S. McKinney, A. Quirk, and K. Harfoush, On the practicality of elliptic curve cryptography for medical sensor networks. in 2014 11th Annual High Capacity Optical Networks and Emerging/Enabling Technologies (Photonics for Energy). 41–45, 2014.
de la Piedra, A., Braeken, A., Touhafi, A., and Wouters, K., Secure event logging in sensor networks. Comput. Math. Appl. 65(5):762–773, 2013.
D. S. Hedin, D. T. Kollmann, P. L. Gibson, T. H. Riehle, and G. J. Seifert, Distance bounded energy detecting ultra-wideband impulse radio secure protocol. in 2014 36th Annual International Conference of the IEEE Engineering in Medicine and Biology Society. 2014; 6619–6622, 2014.
Perera, C., Zaslavsky, A., Christen, P., and Georgakopoulos, D., Sensing as a service model for st cities supported by Internet of Things. Trans. Emerg. Telecomm. Technol. 25(1):81–93, 2014.
Rubio, Ó. J., Trigo, J. D., Alesanco, Á., Serrano, L., and García, J., Analysis of ISO/IEEE 11073 built-in security and its potential IHE-based extensibility. J. Biomed. Inform. 60:270–285, 2016.
T. Benmansour, T. Ahmed, and S. Moussaoui, Performance Evaluation of IEEE 802.15.6 MAC in Monitoring of a Cardiac Patient. in 2016 IEEE 41st Conference on Local Computer Networks Workshops (LCN Workshops), . 241–247, 2016.
H. Fourati, H. Idoudi, T. Val, A. Van Den Bossche, and L. A. Saidane, Performance evaluation of IEEE 802.15.6 CSMA/CA-based CANet WBAN. in 2015 IEEE/ACS 12th International Conference of Computer Systems and Applications (AICCSA). 1–7, 2015.
Radhakrishnan, S., Duvvuru, A., and Kathi, S. V., Investigating discrete event simulation method to assess the effectiveness of wearable health monitoring devices. Procedia. Econ. Fin. 11(14):838–856, 2014.
Meizoso, J. P. et al., Evaluation of Miniature Wireless Vital Signs Monitor in a Trauma Intensive Care Unit. Mil. Med. 181(5S):199–204, 2016.
Villalonga, C., Poes, H., Rojas, I., and Banos, O., MIMU-Wear: Ontology-based sensor selection for real-world wearable activity recognition. Neurocomputing 250(2017):76–100, 2017.
M. Hussain et al., Conceptual framework for the security of mobile health applications on Android platform. Telemat .Info. 2018.
Fezari, M., Rasras, R., and El Ey, I. M. M., Ambulatory Health Monitoring System Using Wireless Sensors Node. Proc. Comput. Sci. 65(Iccmit):86–94, 2015.
Boursalie, O., Samavi, R., and Doyle, T. E., M4CVD: Mobile Machine Learning Model for Monitoring Cardiovascular Disease. Proc. Comput. Sci. 63(Icth):384–391, 2015.
Villarreal, V., Fontecha, J., Hervas, R., and Bravo, J., Mobile and ubiquitous architecture for the medical control of chronic diseases through the use of intelligent devices: Using the architecture for patients with diabetes. Futur. Gener. Comput. Syst. 34:161–175, 2014.
Sebillo, M., Tortora, G., Tucci, M., Vitiello, G., Ginige, A., and Di Giovanni, P., Combining personal diaries with territorial intelligence to empower diabetic patients. J. Vis. Lang. Comput. 29:1–14, 2015.
Hindia, M. N., Rahman, T. A., Ojukwu, H., Hanafi, E. B., and Fattouh, A., Enabling Remote Health-Caring Utilizing IoT Concept over LTE-Femtocell Networks. PLoS One 11(5):e0155077, 2016.
Katib, A., Rao, D., Rao, P., Williams, K., and Grant, J., A prototype of a el cell phone application for tracking the vaccination coverage of children in rural communities. Comput. Methods Prog. Biomed. 122(2):215–228, 2015.
Lwin, M. O. et al., A 21st century approach to tackling dengue: Crowdsourced surveillance, predictive mapping and tailored communication. Acta Trop. 130:100–107, 2014.
Bresó, A., J. tínez-Miranda, E. Fuster-García, and J. M. García-Gómez, A el approach to improve the planning of adaptive and interactive sessions for the treatment of Major Depression. Int. J. Hum. Comput. Stud. 87:80–91, 2016.
Chakraborty, S., Ghosh, S. K., Jamthe, A., and Agrawal, D. P., Detecting Mobility for Monitoring Patients with Parkinson’s Disease at Home using RSSI in a Wireless Sensor Network. Proc. Comput. Sci. 19:956–961, 2013.
Hermens, H., op den Akker, H., Tabak, M., Wijsman, J., and Vollenbroek, M., Personalized Coaching Systems to support healthy behavior in people with chronic conditions. J. Electromyogr. Kinesiol. 24(6):815–826, 2014.
C. Beck and J. Georgiou, A wearable, multimodal, vitals acquisition unit for intelligent field triage. in 2016 IEEE International Symposium on Circuits and Systems (ISCAS). 2016; 1530–1533, 2016.
S. Adibi, A mobile health network disaster management system. in 2015 Seventh International Conference on Ubiquitous and Future Networks. 424–428, 2015.
L. I. Besaleva and A. C. Weaver, Mobile electronic triaging for emergency response improvement through crowdsourced and sensor-detected information. in Proceedings of the 2013 IEEE/ACM International Conference on Advances in Social Networks Analysis and Mining - ASONAM ‘13. 1092–1093, 2013.
Ganz, A., Schafer, J. M., Tang, J., Yang, Z., Yi, J., and Ciottone, G., Urban search and rescue situational awareness using DIORAMA disaster management system. Procedia Eng. 107:349–356, 2015.
S. Gunasekaran and M. Suresh, A el control of disaster protection (NCDP) for pilgrims by pan technology. in 2014 IEEE 8th International Conference on Intelligent Systems and Control (ISCO). 103–107, 2014.
A. Renner et al., RIPPLE: Scalable medical telemetry system for supporting combat rescue. in NAECON 2014 - IEEE National Aerospace and Electronics Conference. 2015; 228–232, 2014.
Ali, R. et al., GUDM: Automatic Generation of Unified Datasets for Learning and Reasoning in Healthcare. Sensors 15(12):15772–15798, 2015.
Gaynor, M., and Waterman, J., Design framework for sensors and RFID tags with healthcare applications. Heal. Policy Technol. 5(4):357–369, 2016.
Kim, H.-K., Convergence agent model for developing u-healthcare systems. Futur. Gener. Comput. Syst. 35:39–48, 2014.
Misra, S., and Chatterjee, S., Social choice considerations in cloud-assisted WBAN architecture for post-disaster healthcare: Data aggregation and channelization. Inf. Sci. (Ny). 284:95–117, 2014.
Zhang, K., Liang, X., Baura, M., Lu, R., and Shen, X., PHDA: A priority based health data aggregation with privacy preservation for cloud assisted WBANs. Inf. Sci. (Ny). 284:130–141, 2014.
Yi, C., Zhao, Z., Cai, J., and Lobato de Faria, R., G. (Michael) Zhang, Priority-aware pricing-based capacity sharing scheme for beyond-wireless body area networks. Comput. Netw. 98:29–43, 2016.
Ben Elhadj, H., Elias, J., Chaari, L., and Kamoun, L., Multi-Attribute ision Making Handover Algorithm for Wireless Body Area Networks. Comput. Commun. 81:97–108, 2016.
Yi, C., Alfa, A. S., and Cai, J., An Incentive-Compatible Mechanism for Transmission Scheduling of Delay-Sensitive Medical Packets in E-Health Networks. IEEE Trans. Mob. Comput. 15(10):2424–2436, 2016.
Zhang Yi et al., Emergency treatment in st terminal-based e-healthcare networks. in 2015 4th International Conference on Computer Science and Network Technology (ICCSNT). (Iccsnt):1178–1181, 2015.
Sneha, S., and Varshney, U., A framework for enabling patient monitoring via mobile ad hoc network. Sup. Syst. 55(1):218–234, 2013.
Bouakaz, S. et al., CIRDO: St companion for helping elderly to live at home for longer. IRBM 35(2):100–108, 2014.
De Backere, F., Bonte, P., Verstichel, S., Ongenae, F., and De Turck, F., The OCarePlatform: A context-aware system to support independent living. Comput. Methods Prog. Biomed. 140:111–120, 2017.
B. Kormanyos and B. Pataki, Multilevel simulation of daily activities: Why and how?. in 2013 IEEE International Conference on Computational Intelligence and Virtual Environments for Measurement Systems and Applications (CIVEMSA). 1–6, 2013.
Rahmani, A. M. et al., Exploiting st e-Health gateways at the edge of healthcare Internet-of-Things: A fog computing approach. Futur. Gener. Comput. Syst. 78:641–658, 2017.
Varshney, U., A model for improving quality of isions in mobile health. Sup. Syst. 62:66–77, 2014.
Minutolo, A., Esposito, M., and De Pietro, G., Design and validation of a light-weight reasoning system to support remote health monitoring applications. Eng. Appl. Artif. Intell. 41:232–248, 2015.
Alnanih, R., Ormandjieva, O., and Radhakrishnan, T., Context-based and rule-based adaptation of mobile user interfaces in mHealth. Proc. Comput. Sci. 21:390–397, 2013.
Fratini, A., and Caleffi, M., Medical emergency alarm dissemination in urban environments. Telemat. Info. 31(3):511–517, 2014.
Peleg, M. et al., Assessment of a personalized and distributed patient guidance system. Int. J. Med. Inform. 101:108–130, 2017.
Tawfik, H., and Anya, O., Evaluating practice-centered awareness in cross-boundary telehealth ision support systems. Telemat. Info. 32(3):486–503, 2015.
Tamura, T. et al., Assessment of participant compliance with a Web-based home healthcare system for promoting specific health checkups. Biocybern. Biomed. Eng. 34(1):63–69, 2014.
Lounis, A., Hadjidj, A., Bouabdallah, A., and Challal, Y., Healing on the cloud: Secure cloud architecture for medical wireless sensor networks. Futur. Gener. Comput. Syst. 55:266–277, 2016.
Saleem, K., Derhab, A., Al-Muhtadi, J., and Shahzad, B., Human-oriented design of secure Machine-to-Machine communication system for e-Healthcare society. Comput. Hum. Behav. 51:977–985, 2015.
Nageba, E., Rubel, P., and Fayn, J., Towards an intelligent exploitation of heterogeneous and distributed resources in cooperative environments of eHealth. IRBM 34(1):79–85, 2013.
Sene, A., Kamsu-foguem, B., and Rumeau, P., Telemedicine framework using case-based. Comput. Methods Prog. Biomed. 121(1):21–35, 2015.
Doumbouya, M. B., Kamsu-Foguem, B., Kenfack, H., and Foguem, C., Telemedicine using mobile telecommunication: Towards syntactic interoperability in teleexpertise. Telemat. Info. 31(4):648–659, 2014.
Urovi, V., Jimenez-del-Toro, O., Dubosson, F., Ruiz Torres, A., and Schumacher, M. I., COMPOSE: Using temporal patterns for interpreting wearable sensor data with computer interpretable guidelines. Comput. Biol. Med. 81:24–31, 2017.
Tegegne, T., and van der Weide, T. P., Enriching queries with user preferences in healthcare. Inf. Process. Manag. 50(4):599–620, 2014.
V. Yeguas and R. Casado, Big data issues in computational chemistry. in Proceedings - 2014 International Conference on Future Internet of Things and Cloud, FiCloud 2014. 389–392, 2014.
Wolfe, P. J., Making sense of big data. Proc. Natl. Acad. Sci. 110(45):18031–18032, 2013.
Archenaa, J., and Anita, E. A. M., A survey of big data analytics in healthcare and government. Proc. Comput. Sci. 50(4):408–413, 2015.
P. Bellini, M. di Claudio, P. Nesi, and N. Rauch, Tassonomy and Review of Big Data Solutions Navigation. in Big Data Computing, no. ember. 57–101, 2013.
Y. Demchenko, P. Grosso, C. de Laat, and P. Membrey, Addressing big data issues in Scientific Data Infrastructure. in 2013 International Conference on Collaboration Technologies and Systems (CTS). 48–55, 2013.
F. M. Megahed and L. A. Jones-Farmer, Statistical Perspectives on ‘Big Data,’” in Frontiers in Statistical Quality Control 11, vol. 11th ed, Cham: Springer International Publishing. 29–47, 2015.
M. Minelli, M. Chambers, and A. Dhiraj, Big Data Analytics - Emerging BI and Analitics trends for today’s businesses. 2013.
H. Rahman, S. Begum, and M. U. Ahmed, Ins and Outs of Big Data : A Review. 18–19, 2016.
Wang, L., and Alexander, C. A., Big data in medical applications and health care. Am. Med. J. 6(1):1–8, 2015.
Kalid, N., Zaidan, A. A., Zaidan, B. B., Salman, O. H., Hashim, M., and Muzammil, H., Based real time remote health monitoring systems: A review on patients prioritization and related" big data" using body sensors information and communication technology. J. Med. Syst. 42(2):30, 2018.
M. T. Moutacalli, V. Men, A. Bouzouane, and B. Bouchard, Activity pattern mining using temporal relationships in a st home. in 2013 IEEE Symposium on Computational Intelligence in Healthcare and e-health (CICARE). 83–87, 2013.
Sakr, S., and Elgammal, A., Towards a Comprehensive Data Analytics Framework for St Healthcare Services. Big Data Res. 4:44–58, 2016.
Bharatula, S., and Meenakshi, M., Design of Cognitive Radio Network for Hospital Management System. Wirel. Pers. Commun. 90(2):1021–1038, 2016.
Vaidehi, V., Vardhini, M., Yogeshwaran, H., Inbasagar, G., Bhargavi, R., and Hemalatha, C. S., Agent Based Health Monitoring of Elderly People in Indoor Environments Using Wireless Sensor Networks. Proc. Comput. Sci. 19(Ant):64–71, 2013.
Ben Othman, S., Zgaya, H., Hammadi, S., and Quilliot, A., A. tinot, and J.-M. Renard, Agents endowed with uncertainty management behaviors to solve a multiskill healthcare task scheduling. J. Biomed. Inform. 64:25–43, 2016.
Westergren, H., Ferm, M., and Häggström, P., First evaluation of the paediatric version of the Swedish rapid emergency triage and treatment system shows good reliability. Acta Paediatr. 103(3):305–308, 2014.
Seising, R., and Tabacchi, M., Fuzziness and medicine: Philosophical reflections and application Systems in Health Care, vol. 302. Berlin: Springer Berlin Heidelberg, 2013.
M. Jentsch and L. Ramirez, The reconfiguration of triage by introduction of technology. in Proceedings of the 15th international conference on Human-computer interaction with mobile devices and services (MobileHCI ‘13), 2013. 55–64, 2013.
Innes, K., Plummer, V., and Considine, J., Nurses’ perceptions of their preparation for triage. Australas. Emerg. Nurs. J. 14(2):81–86, 2011.
A. B. Rn, C. Nurse, D. E. C. Rn, and A. Dean, Reducing uncertainty in triaging mental health presentations : Examining triage ision-making. Int. Emerg. Nurs.. 1–5, 2013.
Godfrey, B. et al, Emergency Medical Guidelines. Sun. Act. Flo. (3):245, 2000.
Ritchie, C., and Lai, R., A systematic review of the scientific evidence for the efficacy of a palliative care approach in dementia A systematic review of the scientific evidence. Int. Psychogeriatr. 17:31–40, 2005.
Bernstein, S. L., and D’Onofrio, G., Public Health in the Emergency Department: Academic Emergency Medicine Consensus Conference Executive Sumy. Acad. Emerg. Med. 16(11):1037–1039, 2009.
S. Moreno, A. Quintero, C. Ochoa, M. Bonfante, R. Villareal, and J. Pestana, Remote monitoring system of vital signs for triage and detection of anomalous patient states in the emergency room. in 2016 XXI Symposium on Signal Processing, Images and Artificial Vision (STSIVA). 1–5, 2016.
M. Niswar et al., Performance evaluation of ZigBee-based wireless sensor network for monitoring patients’ pulse status. in 2013 International Conference on Information Technology and Electrical Engineering (ICITEE). 291–294, 2013.
J. R. B. Dos Santos, G. Blard, A. S. R. Oliveira, and N. B. De Carvalho, Wireless Sensor Tag and Network for Improved Clinical Triage. in 2015 Euromicro Conference on Digital System Design. 399–406, 2015.
Sakanushi, K. et al., Electronic triage system for continuously monitoring casualties at disaster scenes. J. Ambient. Intell. Humaniz. Comput. 4(5):547–558, 2013.
M. Niswar et al., The design of wearable medical device for triaging disaster casualties in developing countries. in 2015 5th International Conference on Digital Information Processing and Communications, ICDIPC 2015. 207–212, 2015.
F. Ullah, A. Khelil, A. A. Sheikh, E. Felemban, and H. M. A. Bo, Towards automated self-tagging in emergency health cases. in 2013 IEEE 15th International Conference on e-Health Networking, Applications and Services (Healthcom 2013). (Healthcom):658–663, 2013.
D. Rodriguez, S. Heuer, A. Guerra, W. Stork, B. Weber, and M. Eichler, Towards automatic sensor-based triage for individual remote monitoring during mass casualty incidents. in 2014 IEEE International Conference on Bioinformatics and Biomedicine (BIBM). 544–551, 2014.
Calyam, P. et al., Synchronous Big Data analytics for personalized and remote physical therapy. Pervasive Mob. Comput. 28:3–20, 2016.
Ganapathy, K., Priya, B., Priya, B., Dhivya, V. P., and Vaidehi, V., SOA Framework for Geriatric Remote Health Care Using Wireless Sensor Network. Proc. Comput. Sci. 19(Fams):1012–1019, 2013.
Ganapathy, K., Vaidehi, V., Kannan, B., and Murugan, H., Hierarchical Particle Swarm Optimization with Ortho-Cyclic Circles. Expert Syst. Appl. 41(7):3460–3476, 2014.
Gómez, J., Oviedo, B., and Zhuma, E., Patient Monitoring System Based on Internet of Things. Proc. Comput. Sci. 83(Ant):90–97, 2016.
Hussain, A., Wenbi, R., da Silva, A. L., Nadher, M., and Mudhish, M., Health and emergency-care platform for the elderly and disabled people in the St City. J. Syst. Softw. 110:253–263, 2015.
Kovalchuk, S. V., Krotov, E., Smir, P. A., Naso, D. A., and Yakovlev, A. N., Distributed data-driven platform for urgent ision making in cardiological ambulance control. Futur. Gener. Comput. Syst. 79:144–154, 2016.
Ku, N., Kaur, K., Jindal, A., and Rodrigues, J. J. P. C., Providing healthcare services on-the-fly using multi-player cooperation game theory in Internet of Vehicles (IoV) environment. Digit. Commun. Netw. 1(3):191–203, 2015.
Lamprinakos, G. C. et al., An integrated remote monitoring platform towards Telehealth and Telecare services interoperability. Inf. Sci. (Ny). 308(ch):23–37, 2015.
J. Mendes, H. Simões, P. Rosa, N. Costa, C. Rabadão, and A. Pereira, Secure Low-cost Solution for Elder’s eCardio Surveillance. Proc. Comput. Sci., vol. 27, no. Dsai 2013, pp. 46–56, 2014.
Miah, S. J., Hasan, J., and Gammack, J. G., On-Cloud Healthcare Clinic: An e-health consultancy approach for remote communities in a developing country. Telemat. Info. 34(1):311–322, 2017.
Moretti, S., Cicalò, S., Mazzotti, M., Tralli, V., and Chiani, M., Content/context-aware multiple camera selection and video adaptation for the support of m-health services. Proc. Comput. Sci. 40:206–213, 2014.
Zanjal, S. V., and Talmale, G. R., Medicine Reminder and Monitoring System for Secure Health Using IOT. Proc. Comput. Sci. 78:471–476, 2016.
Teijeiro, T., Félix, P., Presedo, J., and Zarón, C., An open platform for the protocolization of home medical supervision. Expert Syst. Appl. 40(7):2607–2614, 2013.
Sung, W., and Chang, K., Health parameter monitoring via a el wireless system. Appl. Soft Comput. 22:667–680, 2014.
Rajku, R., and Sriman Narayana Iyengar, N. C., Dynamic Integration of Mobile JXTA with Cloud Computing for Emergency Rural Public Health Care. Osong Public Heal. Res. Perspect. 4(5):255–264, 2013.
Rocha, A. et al., Inations in health care services: The CAALYX system. Int. J. Med. Inform. 82(11):1–14, 2013.
Kalid, N. et al., Based on Real Time Remote Health Monitoring Systems: A New Approach for Prioritization ‘Large Scales Data’ Patients with Chronic Heart Diseases Using Body Sensors and Communication Technology. J. Med. Syst. 42(4):69, 2018.
van Dyk, L., A review of telehealth service implementation frameworks. Int. J. Environ. Res. Public Health 11(2):1279–1298, 2014.
Jeong, S., Youn, C.-H., Shim, E. B., Kim, M., Cho, Y. M., and Peng, L., An integrated healthcare system for personalized chronic disease care in home–hospital environments. IEEE Trans. Inf. Technol. Biomed. 16(4):572–585, 2012.
Zaidan, A. A., Zaidan, B. B., Kadhem, Z., Larbani, M., Lakulu, M. B., and Hashim, M., Challenges, Alternatives, and Paths to Sustainability: Better Public Health Promotion Using Social Networking Pages as Key Tools. J. Med. Syst. 39(2):7, 2015.
Kiah, M. L. M., Zaidan, B. B., Zaidan, A. A., Nabi, M., and Ibraheem, R., MIRASS: Medical informatics research activity support system using information mashup network. J. Med. Syst. 38(4):37, 2014.
Busse, R., Schreyögg, J., and Smith, P. C., Variability in healthcare treatment costs amongst nine EU countries–results from the HealthBASKET project. Health Econ. S1:17, 2008.
L. H. Wizig, Method and system for providing a user-selected healthcare services package and healthcare services panel customized based on a user’s selections.” Google Patents, 2004.
Baig, M. M., and Gholamhosseini, H., St health monitoring systems: an overview of design and modeling. J. Med. Syst. 37(2):9898, 2013.
Li, S. H., Cheng, K. A., Lu, W. H., and Lin, T. C., Developing an active emergency medical service system based on WiMAX technology. J. Med. Syst. 36(5):3177–3193, 2012.
Fernandes, C. M., Wuerz, R., Clark, S., and Djurdjev, O., How reliable is emergency department triage? Ann. Emerg. Med. 34(2):141–147, 1999.
Culley, J. M., Svendsen, E., Craig, J., and Tavakoli, A., A validation study of 5 triage systems using data from the 2005 Graniteville, South Carolina, chlorine spill. J. Emerg. Nurs. 40(5):453–460, 2014.
He, C., Fan, X., and Li, Y., Toward Ubiquitous Healthcare Services With a el Efficient Cloud Platform. IEEE Trans. Biomed. Eng. 60(1):230–234, 2013.
Mazomenos, E. B. et al., A low-complexity ECG feature extraction algorithm for mobile healthcare applications. IEEE J. Biomed. Heal. Info. 17(2):459–469, 2013.
B. Klimova, Mobile Health Devices for Aging Population Groups: A Review Study. vol. 9847, M. Younas, I. Awan, N. Kryvinska, C. Strauss, and D. van Thanh, Eds. Cham: Springer International Publishing. 295–301, 2016.
Chung, Y., and Liu, C., Design of a Wireless Sensor Network Platform for Tele-Homecare. Sensors 13(12):17156–17175, 2013.
Sun, J., Guo, Y., Wang, X., and Zeng, Q., mHealth For Aging China: Opportunities and Challenges. Aging Dis. 7(1):53, 2016.
G. Palozzi, D. Binci, and A. Appolloni, E-Health and Co-production: Critical Drivers for Chronic Diseases Management Models, Strategies, Tools. 2017.
Sparks, R., Celler, B., Okugami, C., Jayasena, R., and Varnfield, M., Telehealth Monitoring of Patients in the Community. J. Intell. Syst. 25(1):37–53, 2016.
Touati, F., and Tabish, R., U-healthcare system: State-of-the-art review and challenges. J. Med. Syst. 37(3):9949, 2013.
Kaiser Family Foundation, Trends in Health Care Costs and Spending. Health Care (Don. Mills). 650:1–2, 2009.
C. for M. and M. Services, The Affordable Care Act: helping providers help patients: a menu of options for improving care. 2015.
IFRC, Disaster and crisis management. International Federation of Red Cross and Red Crescent Societies, 2015. [Online]. Available: https://www.ifrc.org/en/what-we-do/disaster-management/. [Accessed: 02--2017].
Merin, O., Miskin, I. N., Lin, G., Wiser, I., and Kreiss, Y., Triage in mass-casualty events: The Haitian experience. Prehosp. Disaster Med. 26(5):386–390, 2011.
Cross, K. P., and Cicero, M. X., Head-to-Head Comparison of Disaster Triage Methods in Pediatric, Adult, and Geriatric Patients. Ann. Emerg. Med. 61(6):668–676.e7, 2013.
E. B. Lerner et al., Mass Casualty Triage: Universal Versus Specific: Lerner et al reply. Disaster Med. Public Health Prep. 3, 2009.
Kanter, R. K., Strategies to improve pediatric disaster surge response: Potential mortality reduction and tradeoffs. Crit. Care Med. 35(12):2837–2842, 2007.
Kelen, G. D. et al., Creation of Surge Capacity by Early Discharge of Hospitalized Patients at Low Risk for Untoward Events. Disaster Med. Public Health Prep. 3:S10–S16, 2009.
Nager, A. L., and Khanna, K., Emergency department surge: Models and practical implications. J. Trauma Acute Care Surg. 67(2):S96–S99, 2009.
Cicero, M. X. et al., Do you see what i see? Insights from using Google glass for disaster telemedicine triage. Prehosp. Disaster Med. 30(1):4–8, 2015.
Chung, S., and Shannon, M., Reuniting children with their families during disasters: A proposed plan for greater success. Am. J. Disaster Med. 2(3):113–117, 2007.
Wallis, L. A., and Carley, S., Comparison of paediatric major incident priy triage tools. Emerg. Med. J. 23(6):475–478, 2006.
Xiong, W., Bair, A., Sandrock, C., Wang, S., Siddiqui, J., and Hupert, N., Implementing telemedicine in medical emergency response: Concept of operation for a regional telemedicine hub. J. Med. Syst. 36(3):1651–1660, 2012.
Nodhturft, V. et al., Chronic disease self-management. Nurs. Clin. North. Am. 35:507–518, 2000.
A. A. Zaidan et al., A survey on communication components for IoT-based technologies in st homes. Telecom. Syst. 1–25, 2018.
Patel, S., Park, H., Bonato, P., Chan, L., and Rodgers, M., A review of wearable sensors and systems with application in rehabilitation. J. Neuroeng. Rehabil. 9(1):21, 2012.
Sockolow, P. S., Bowles, K. H., Adelsberger, M. C., Chittams, J. L., and Liao, C., Impact of homecare electronic health record on timeliness of clinical documentation, reimbursement, and patient outcomes. Appl. Clin. Inform. 5(2):445, 2014.
Durisko, C., McCue, M., Doyle, P. J., Dickey, M. W., and Fiez, J. A., A flexible and integrated system for the remote Acquisition of Neuropsychological Data in stroke research. Telemed. e-Health 22(12):1032–1040, 2016.
Bernocchi, P. et al., Healthcare continuity from hospital to territory in Lombardy: TELEMACO project. Am. J. Manag. Care 18(3):101–108, 2012.
Okura, T. et al., The Importance of Walking for Control of Blood Pressure: Proof Using a Telemedicine System. Telemed. e-Health 22(12):1019–1023, 2016.
Alsalem, M. A. et al., A review of the automated detection and classification of acute leukaemia: Coherent taxonomy, datasets, validation and performance measurements, motivation, open challenges and recommendations. Comput. Methods Prog. Biomed. 158:93–112, 2018.
Miao, F., Cheng, Y., He, Y., He, Q., and Li, Y., A Wearable Context-Aware ECG Monitoring System Integrated with Built-in Kinematic Sensors of the Stphone. Sensors 15(5):11465–11484, 2015.
Cohn, J. N., Current therapy of the failing heart. Circulation 78(5):1099–1107, 1988.
Nguyen, T., Khosravi, A., Creighton, D., and Nahavandi, S., Classification of healthcare data using genetic fuzzy logic system and wavelets. Expert Syst. Appl. 42(4):2184–2197, 2015.
Brunetti, N. D. et al., Telemedicine for cardiovascular disease continuum: A position paper from the Italian Society of Cardiology Working Group on Telecardiology and informatics. Int. J. Cardiol. 184:452–458, 2015.
Winkler, S. et al., A new telemonitoring system intended for chronic heart failure patients using mobile telephone technology—Feasibility study. Int. J. Cardiol. 153(1):55–58, 2011.
Klersy, C., De Silvestri, A., Gabutti, G., Regoli, F., and Auricchio, A., A meta-analysis of remote monitoring of heart failure patients. J. Am. Coll. Cardiol. 54(18):1683–1694, 2009.
Zhang, J., Goode, K. M., Cuddihy, P. E., and Cleland, J. G. F., Predicting hospitalization due to worsening heart failure using daily weight measurement: Analysis of the trans-European network-home-care management system (TEN-HMS) study. Eur. J. Heart Fail. 11(4):420–427, 2009.
A. A. Zaidan et al., A review on stphone skin cancer diagnosis apps in evaluation and benchking: coherent taxonomy, open issues and recommendation pathway solution. Health Technol. (Berl). 1–16, 2018.
Azeez, D., Ali, M. A. M., Gan, K. B., and Saiboon, I., Comparison of adaptive neuro-fuzzy inference system and artificial neutral networks model to categorize patients in the emergency department. Springerplus 2(1):416, 2013.
Brunetti, N. D., Dellegrottaglie, G., Di Giuseppe, G., Antonelli, G., and Di Biase, M., All for one, one for all: Remote telemedicine hub pre-hospital triage for public Emergency Medical Service 1–1-8 in a regional network for priy PCI in Apulia, Italy. Eur. Res. Telemedicine/La Rech. Eur. en Téléméine 3(1):9–15, 2014.
Merzougui, R., Adaptation of an intelligent mobile assistant medical (IMAM) of the heterogeneous data for the telemedicine services: Design and implementation. Wirel. Pers. Commun. 84(4):3091–3107, 2015.
Ashour, O. M., and Okudan, G. E., Fuzzy AHP and utility theory based patient sorting in emergency departments. Int. J. Collab. Enterp. 1(3–4):332–358, 2010.
Salman, O. H., Zaidan, A. A., and Zaidan, B. B., Naserkalid, and M. Hashim, el Methodology for Triage and Prioritizing Using ‘Big Data’ Patients with Chronic Heart Diseases Through Telemedicine Environmental. Int. J. Inf. Technol. is. Mak. 16(05):1211–1245, 2017.
Kamali, B., Bish, D., and Glick, R., Optimal service order for mass-casualty incident response. Eur. J. Oper. Res., 2017.
M. Mandava, C. Lubamba, A. Ismail, A. Bagula, and H. Bagula, Cyber-healthcare for public healthcare in the developing world. in Proceedings - IEEE Symposium on Computers and Communications. 2016; 14–19. 2016.
A. Bagula, C. Lubamba, M. Mandava, H. Bagula, M. Zennaro, and E. Pietrosemoli, CLOUD BASED PATIENT PRIORITIZATION AS SERVICE IN PUBLIC HEALTH CARE ISAT Laboratory , Computer Science Department , University of The Western Cape ( UWC ), Private Bag X17 , Bellville , 7535 , South Africa. Email : abagula@uwc.ac.za Department of Public. 2016.
Mills, A. F., A simple yet effective ision support policy for mass-casualty triage. Eur. J. Oper. Res. 253(3):734–745, 2016.
P. Sarkar and D. Sinha, An approach to continuous pervasive care of remote patients based on priority based assignment of nurse. in IFIP International Conference on Computer Information Systems and Industrial Management. 327–338, 2014.
Childers, A. K., Orga, M. E., and Taaffe, K. M., Prioritization strategies for patient evacuations. Health Care Manag. Sci. 17(1):77–87, 2014.
Mills, A. F., Argon, N. T., and Ziya, S., Resource-based patient prioritization in mass-casualty incidents. Manuf. Serv. Oper. Manag. 15(3):361–377, 2013.
Sung, W.-T., and Chang, K.-Y., Evidence-based multi-sensor information fusion for remote health care systems. Sensors Actuators A Phys. 204:1–19, 2013.
Jacobson, E. U., Argon, N. T., and Ziya, S., Priority assignment in emergency response. Oper. Res. 60(4):813–832, 2012.
A. Kashiyama, A. Uchiyama, and T. Higashino, Depth Limited Treatment Planning and Scheduling for Electronic Triage System in MCI. in Wireless Mobile Communication and Healthcare, Springer. 224–233, 2012.
A. Childers, G. Visagamurthy, and K. Taaffe, Prioritizing patients for evacuation from a health-care facility. Transp. Res. Rec. J. Transp. Res. Board. (2137): 38–45, 2009.
Argon, N. T., Ziya, S., and Righter, R., Scheduling impatient jobs in a clearing system with insights on patient triage in mass casualty incidents. Probab. Eng. Info. Sci. 22(03):301–332, 2008.
Christensen, D., Jensen, N. M., Maaløe, R., Rudolph, S. S., Belhage, B., and Perrild, H., Nurse-administered early warning score system can be used for emergency department triage. Dan. Med. Bull. 58(6):A4221, 2011.
Hung, C. Y., Chang, P. Y., and Huang, Y. H., Comparison of fuzzy-based MCDM and non-fuzzy MCDM in setting a new fee schedule for orthopedic procedures in Taiwan’s national health insurance program. WSEAS Trans. Math. 5(1):149–153, 2006.
R. Beveridge et al., Implementation Guidelines for The Canadian Emergency Department Triage & Acuity Scale ( CTAS ) - endorsed by the Canadian Association of Emergency Physicians, the National Emergency Nurses Affiliation of Canada, and l’association des meins d’urgence du. Can. Assoc. Emerg. Physicians. 1–32, 1998.
Zarabzadeh, A. et al., Variation in health care providers’ perceptions: ision making based on patient vital signs. J. Syst. 22(3):168–189, 2013.
Widgren, B. R., and Jourak, M., Medical Emergency Triage and Treatment System (METTS): A New Protocol in Priy Triage and Secondary Priority ision in Emergency Medicine. J. Emerg. Med. 40(6):623–628, 2011.
Zachariasse, J. M. et al., Validity of the Manchester triage system in emergency care: A prospective observational study. PLoS One 12(2):1–14, 2017.
D. Christensen, N. M. Jensen, R. Maaløe, S. S. Rudolph, B. Belhage, and H. Perrild, Low compliance with a validated system for emergency department triage. Dan. Med. Bull. 58(6):A4294, 2011.
Lerner, E. B. et al., Mass casualty triage: An evaluation of the science and refinement of a National Guideline. Disaster Med. Public Health Prep. 5(02):129–137, 2011.
Benson, M., Koenig, K. L., and Schultz, C. H., Disaster triage: START, then SAVE—A new method of dynamic triage for victims of a catastrophic earthquake. Prehosp. Disaster Med. 11(02):117–124, 1996.
Hodgetts, T. J., Hall, J., Maconochie, I., and St, C., Paediatric triage tape. Pre-hospital Immed. Care 2:155–159, 1998.
Wiseman, D. B., Ellenbogen, R., and Shaffrey, C. I., Triage for the neurosurgeon.. Neurosurg. Focus 12(3):E5, 2002.
N. Gilboy, P. Tanabe, D. Travers, and A. M. Rosenau, Emergency Severity Index (ESI): a triage tool for emergency department care, version 4. Implement. Handb. 12–14, 2012.
P. Moore, A. Thomas, T. Qassem, N. Bessis, and B. Hu, Monitoring Patients with Mental Disorders. in 2015 9th International Conference on Inative Mobile and Internet Services in Ubiquitous Computing. 65–70, 2015.
W. H. Organization, Surgical care at the district hospital. World Health Organization, 2003.
C. D. Johnson and I. Taylor, Recent Advances in Surgery 27, vol. 27. CRC Press, 2004.
“best dors.” [Online]. Available: https://bestdors.com/. [Accessed: 05--2017].
Zanjal, S. V., and Talmale, G. R., Medicine reminder and monitoring system for secure health using IOT. Proc. Comput. Sci. 78(3):471–476, 2016.
R. L. Keeney and H. Raiffa, Decisions with multiple objectives: preferences and value trade-offs. Cambridge university press, 1993.
Belton, V., and Stewart, T. J., Multiple criteria ision analysis. Boston: Springer US, 2002.
J. Malczewski, GIS and multicriteria ision analysis. Wiley, 1999.
S. Petrovic-Lazarevic and A. Abraham, Hybrid fuzzy-linear programming approach for multi criteria ision making problems. arXiv Prepr. cs/0405019, 2004.
Zionts, S., MCDM—If not a roman numeral, then what? Interfaces (Providence). 9(4):94–101, 1979.
M. Oliveira, D. B. M. M. Fontes, and T. Pereira, Multicriteria ision making: a case study in the automobile industry. in International Symposium on Operational Research and Applications (ISORAP2013), 2013.
A. Jadhav and R. Sonar, Analytic Hierarchy Process (AHP), Weighted Scoring Method (WSM), and Hybrid Knowledge Based System (HKBS) for Software Selection: A Comparative Study. in Emerging Trends in Engineering and Technology (ICETET), 2009 2nd International Conference on. 991–997, 2009.
Diaby, V., Campbell, K., and Goeree, R., Multi-criteria ision analysis (MCDA) in health care: A bibliometric analysis. Oper. Res. Heal. Care 2(1):20–24, 2013.
Thokala, P. et al., Multiple criteria ision analysis for health care ision making—An introduction: Report 1 of the ISPOR MCDA emerging good practices task force. Value Health 19(1):1–13, 2016.
Adunlin, G., Diaby, V., and Xiao, H., Application of multicriteria ision analysis in health care: A systematic review and bibliometric analysis. Health Expect. 18(6):1894–1905, 2015.
Jumaah, F. M., Zadain, A. A., Zaidan, B. B., Hamzah, A. K., and Bahbibi, R., ision-making solution based multi-measurement design parameter for optimization of GPS receiver tracking channels in static and dynamic real-time positioning multipath environment. Measurement 118:83–95, 2018.
Yas, Q. M., Zaidan, A. A., Zaidan, B. B., Rahmatullah, B., and Abdul Karim, H., Comprehensive insights into evaluation and benchking of real-time skin detectors: Review, open issues & challenges, and recommended solutions. Measurement 114:243–260, 2018.
Zaidan, B. B., Zaidan, A. A., Abdul Karim, H., and Ahmad, N. N., A new approach based on multi-dimensional evaluation and benchking for data hiding techniques. Int. J. Inf. Technol. is. Mak.:1–42, 2017.
Zaidan, B. B., and Zaidan, A. A., Software and hardware FPGA-based digital waterking and steganography approaches: Toward new methodology for evaluation and benchking using multi-criteria ision-making techniques. J. Circuits, Syst. Comput. 26(07):1750116, 2017.
Zaidan, B. B., and Zaidan, A. A., Comparative study on the evaluation and benchking information hiding approaches based multi-measurement analysis using TOPSIS method with different normalisation, separation and context techniques. Measurement 117:277–294, 2018.
Mühlbacher, A. C., and Kaczynski, A., Making good isions in healthcare with multi-criteria ision analysis: The use, current research and future development of MCDA. Appl. Health Econ. Health Policy 14(1):29–40, 2016.
Abdullateef, B. N., Elias, N. F., Mohamed, H., Zaidan, A. A., and Zaidan, B. B., An evaluation and selection problems of OSS-LMS packages. Springerplus 5(1):248, 2016.
Zhu, G., Hu, J., Qi, J., Gu, C., and Peng, Y., An integrated AHP and VIKOR for design concept evaluation based on rough number. Adv. Eng. Inform. 29(3):408–418, 2015.
F. M. Jumaah, A. A. Zaidan, B. B. Zaidan, R. Bahbibi, M. Y. Qahtan, and A. Sali, Technique for order performance by similarity to ideal solution for solving complex situations in multi-criteria optimization of the tracking channels of GPS baseband telecommunication receivers. Telecomm. Syst. 1–19, 2017.
Kiah, M. L. M., Haiqi, A., Zaidan, B. B., and Zaidan, A. A., Open source EMR software: Profiling, insights and hands-on analysis. Comput. Methods Prog. Biomed. 117(2):360–382, 2014.
Yas, Q. M., Zadain, A. A., Zaidan, B. B., Lakulu, M. B., and Rahmatullah, B., Towards on develop a framework for the evaluation and benchking of skin detectors based on artificial intelligent models using multi-criteria ision-making techniques. Int. J. Pattern Recognit. Artif. Intell. 31(03):1759002, 2017.
Opricovic, S., and Tzeng, G.-H., Compromise solution by MCDM methods: A comparative analysis of VIKOR and TOPSIS. Eur. J. Oper. Res. 156(2):445–455, 2004.
Nilsson, H., Nordström, E.-M., and Öhman, K., ision support for participatory forest planning using AHP and TOPSIS. Forests 7(5):100, 2016.
Saaty, T. L., and Ozdemir, M. S., Why the magic number seven plus or minus two. Math. Comput. Model. 38(3–4):233–244, 2003.
Ortíz, M. A., Cómbita, J. P., la Hoz, Á. l. A. D., De Felice, F., and Petrillo, A., An integrated approach of AHP-DEMATEL methods applied for the selection of allied hospitals in outpatient service. Int. J. Med. Eng. Inform. 8(2):87–107, 2016.
Barrios, M. A. O., De Felice, F., Negrete, K. P., Romero, B. A., Arenas, A. Y., and Petrillo, A., An AHP-Topsis integrated model for selecting the most appropriate tomography equipment. Int. J. Inf. Technol. is. Mak. 15(04):861–885, 2016.
Çalışkan, H., Selection of boron based tribological hard coatings using multi-criteria ision making methods. Mater. Des. 50:742–749, 2013.
Fu, H.-P., Chu, K.-K., Chao, P., Lee, H.-H., and Liao, Y.-C., Using fuzzy AHP and VIKOR for benchking analysis in the hotel industry. Serv. Ind. J. 31(14):2373–2389, 2011.
Albahri, O. S. et al., Systematic Review of Real-time Remote Health Monitoring System in Triage and Priority-Based Sensor Technology: Taxonomy, Open Challenges, Motivation and Recommendations. J. Med. Syst. 42(5):80, 2018.
Ilangkuan, M., Sasirekha, V., Anojku, L., and Raja, M. B., Machine tool selection using AHP and VIKOR methodologies under fuzzy environment. Int. J. Model. Oper. Manag. 2(4):409, 2012.
Aktan, H. E., and Samut, P. K., Agricultural performance evaluation by integrating fuzzy AHP and VIKOR methods. Int. J. Appl. Sci. 6(4):324, 2013.
Y. Yamamoto, Adding a dummy data or discarding a portion of data in a bus repeater buffer memory for a second data transfer to a second bus. Google Patents, 2002.
J.-M. Lee, H.-G. Lee, S.-C. Lee, H. Cho, and S.-T. Kim, Liquid crystal display with dummy data driving to produce edge column compensation. Google Patents, 1999.
V. Sherekar, M. Tatikonda, and M. Student, Impact of Factor Affecting on Labour Productivity in Construction Projects by AHP Method. Int. J. Eng. Sci. Comput. 6, 2016.
Miyahara, S., Tsuji, M., Iizuka, C., Hasegawa, T., and Taoka, F., On the evaluation of economic benefits of Japanese telemedicine and factors for its promotion. Telemed. J. e-Health 12(6):691–697, 2006.
Connell, F. A., Diehr, P., and Hart, L. G., The use of large data bases in health care studies. Annu. Rev. Public Health 8(1):51–74, 1987.
Lahby, M., Cherkaoui, L., and Adib, A., A el ranking algorithm based network selection for heterogeneous wireless access. JNW 8(2):263–272, 2013.
Saksrisathaporn, K., Bouras, A., Reeveerakul, N., and Charles, A., Application of a ision model by using an integration of AHP and TOPSIS approaches within humanitarian operation life cycle. Int. J. Inf. Technol. is. Mak. 15(04):887–918, 2016.
Saaty, T. L., A scaling method for priorities in hierarchical structures. J. Math. Psychol. 15(3):234–281, 1977.
Wind, Y., and Saaty, T. L., keting applications of the analytic hierarchy process. Manag. Sci. 26(7):641–658, 1980.
T. L. Saaty, The Analytic Hierarchy Process, New York: McGrew Hill. Int. Transl. to Russ. Port. Chinese, Revis. Ed. Paperb. (1996, 2000), Pittsburgh RWS Publ., 1980.
Further Reading
Mohaghar, A., Fathi, M. R., Zarchi, M. K., and Omidian, A., A Combined VIKOR – Fuzzy AHP Approach to keting Strategy Selection. Bus. Manag. Strateg. 3:1, 1969.
Chang, T.-H., and method, F. V. I. K. O. R., A case study of the hospital service evaluation in Taiwan. Inf. Sci. (Ny). 271:196–212, 2014.
Qader, M. A., Zaidan, B. B., Zaidan, A. A., Ali, S. K., Kamaluddin, M. A., and Radzi, W. B., A methodology for football players selection problem based on multi-measurements criteria analysis. Meas. J. Int. Meas. Confed. 111:38–50, 2017.
Zaidan, A. A., Zaidan, B. B., Al-Haiqi, A., Kiah, M. L. M., Hussain, M., and Abdulnabi, M., Evaluation and selection of open-source EMR software packages based on integrated AHP and TOPSIS. J. Biomed. Inform. 53:390–404, 2015.
M. Mansooreh and J. Pet-Edwards, Technical Briefing: Making Multiple-Objective isions. Inst. Electr. ve Electron. Eng. Inc., IEEE Comput. Soc. Press. USA, 1997.
Triantaphyllou, E., Multi-criteria ision making methods: A comparative study. 44th edition. Boston: Springer US, 2000.
Aruldoss, M., Lakshmi, T. M., and Venkatesan, V. P., A survey on multi criteria ision making methods and its applications. Am. J. Inf. Syst. 1(1):31–43, 2013.
K. P. Yoon and C.-L. Hwang, Multiple attribute ision making: an introduction, vol. 104. Sage publications, 1995.
Triantaphyllou, E., Shu, B., Sanchez, S. N., and Ray, T., Multi-criteria ision making: an operations research approach. Encycl. Electr. Electron. Eng. 15(1998):175–186, 1998.
Funding
This study was funded by UPSI grant No: 2017–0179–109-01.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study
Additional information
This article is part of the Topical Collection on Systems-Level Quality Improvement
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Albahri, O.S., Zaidan, A.A., Zaidan, B.B. et al. Real-Time Remote Health-Monitoring Systems in a Medical Centre: A Review of the Provision of Healthcare Services-Based Body Sensor Information, Open Challenges and Methodological Aspects. J Med Syst 42, 164 (2018). https://doi.org/10.1007/s10916-018-1006-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10916-018-1006-6