Abstract
Although cervical cancer rates in the United States have declined sharply in recent decades, certain groups of women remain at elevated risk, including middle-aged and older women in central Appalachia. Cross-sectional baseline data from a community-based randomized controlled trial were examined to identify barriers to cervical cancer screening. Questionnaires assessing barriers were administered to 345 Appalachian women aged 40–64, years when Papanicolaou (Pap) testing declines and cervical cancer rates increase. Consistent with the PRECEDE/PROCEED framework, participants identified barriers included predisposing, enabling, and reinforcing factors. Descriptive and bivariate analyses are reported, identifying (a) the most frequently endorsed barriers to screening, and (b) significant associations of barriers with sociodemographic characteristics in the sample. Recommendations are provided to decrease these barriers and, ultimately, improve rates of Pap tests among this traditionally underserved and disproportionately affected group.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Invasive cervical cancer (ICC) is one of the most common cancers affecting women in the United States. Approximately 12,170 cases of ICC and 4,220 deaths are expected in 2012 [1]. While its incidence and mortality rates appear modest compared to other cancers, ICC remains a high priority for several reasons. First, with screening via Papanicolaou (Pap) tests, nearly all ICC cases can be prevented. Further, the Pap test is a well-established, low cost, and generally widely available screening test. Finally, the burden of ICC mortality falls most heavily on certain traditionally underserved populations [2].
The US Preventive Services Task Force strongly advocates using Pap tests for early detection of ICC. Early detection and treatment of abnormalities has proved successful in preventing the development of ICC. Fifty to seventy percent of new ICC cases occur in rarely or never screened women [3], and screening reduces the likelihood of ICC onset by 90 % for up to 3 years [4]. This level of efficacy led Healthy People 2010 to set the goal of a 97 % 3-year screening rate for women age 18+, and Healthy People 2020 has retained this goal with modifications [5, 6]. While this level of screening has yet to be attained, screening rates have increased over the past several decades [7, 8].
The Burden of Cervical Cancer in Appalachia
Although ICC mortality has decreased over recent decades [9], certain groups continue to experience a disproportionate burden from this disease. Surveillance, Epidemiology, and End Results (SEER) data from Appalachia reveal ICC incidence rates 40 % higher than the national average [10]. Appalachian Kentucky in particular has an ICC incidence rate (15.0/100,000) approximately 67 % above the national average (9.0/100,000) [11, 12]. Moreover, differences emerge in ICC mortality rates within Appalachia, with Appalachian Kentucky and West Virginia having notably higher ICC mortality than Appalachia as a whole [13].
One key contributor to the high rates of ICC incidence and mortality in Appalachian Kentucky is the suboptimal use of Pap tests. Inadequate Pap screening, including lack of and lapses in screening, likely contributes to the elevated ICC rates among middle-aged and older Appalachian women. Recent data reveal that in 2002, nearly one-third of Kentucky women aged 50 and over had not had a Pap test within the prior 3 years [14].
Theoretical Framework: PRECEDE/PROCEED
Factors implicated in low rates of ICC screening include those identified through conceptual frameworks like PRECEDE/PROCEED. Although this framework is not necessarily intended to predict factors associated with health behaviors, it is useful in conceptualizing barriers to Pap test use [15–20].
The PRECEDE/PROCEED framework posits that predisposing, enabling, and reinforcing factors shape whether an individual engages in a particular behavior, broadly uniting social, epidemiologic, behavioral, environmental, educational, and organizational perspectives of a health problem within a community context [21, 22]. This framework allows for the influence of environmental factors that may affect screening behavior, as well as individual- and system-level variables. Predisposing factors include an individual’s reasons, beliefs, or attitudes underlying a behavior, as well as personal characteristics affecting the likelihood that a health behavior will be performed. Predisposing factors previously found to impede various types of screening include demographic characteristics (e.g., old age, low educational attainment), knowledge deficits, and negative attitudes. For example, older age and rural residence were associated with lack of ICC screening in a nationally representative sample [23], as were beliefs that screening was unnecessary in the absence of feeling ill, among South African women [24].
Enabling factors, including structural issues which make it possible for screening to occur, have repeatedly demonstrated powerful effects on screening rates. Enabling factors including not having a usual source of care [25], low income [16], and competing demands [26], have all been identified as decreasing the likelihood of preventive health care services such as cancer screening.
Finally, reinforcing factors occur after a behavior is initiated and encourage maintaining that behavior. Examples of reinforcing factors previously found to correlate with screening status include social support for the behavior [27] and recommendation from a medical care provider [28]. Overall, however, few studies have examined the role of reinforcing factors in the receipt of Pap tests within the PRECEDE-PROCEED framework.
Barriers Experienced by Appalachian Women
Previous investigations of barriers to cervical cancer screening experienced by rural Appalachian women have described contextually and culturally specific barriers. These include structural and environmental challenges like inadequate provider availability (particularly in rural health care shortage areas), difficulty scheduling appointments, and lengthy waiting times [29, 30]. Other studies have described barriers pertaining to attitudes and beliefs, such as embarrassment or modesty during gynecological examinations; reluctance to interact with a male physician, originating either from the woman herself or her partner; and perceived associations among cervical cancer, sexual activity, and immoral behavior. Still others have suggested that strong traditions of religion and fatalism in Appalachia have adversely affected women’s screening and follow-up, such that “God’s will” rather than proactive behavior directs ICC outcomes [31–33].
Unfortunately, many of these research efforts were undertaken 10–25 years ago, and notable limitations existed in methodological approaches. Specifically, most existing studies exploring barriers to ICC screening among rural women either relied on telephone contacts (a serious limitation in a region in which women highlight concerns about privacy regarding personal topics) or were conducted with small samples [34, 35].
In the present study, a comprehensive survey instrument of barriers was developed, pre-tested, and administered by local interviewers to women who had not been screened for ICC according to the recommended guidelines at the time of study initiation. Aims of the current study were (a) to explore a wide range of barriers preventing middle-aged and older rural Appalachian women from obtaining ICC screening, and (b) to apply the conceptual PRECEDE/PROCEED framework to identify the most frequently endorsed barriers and their sociodemographic correlates.
Methods
All research activities were approved by the University of Kentucky Institutional Review Board, and all participants provided informed consent. The study comprised two stages: qualitative work developing the survey instrument, and quantitative assessment of barriers reported by a sample of Appalachian women. Data for the quantitative stage were obtained from the baseline assessment of participants enrolled in a randomized controlled trial (RCT) investigating an intervention to increase ICC screening rates in four Appalachian Kentucky counties.
Development and Pre-testing of the Survey Instrument
Several qualitative activities were conducted over 18 months to capture Appalachian women’s perspectives on ICC and screening. First, to offer insights about the general barriers and facilitators of ICC screening, 25 rarely- or never-screened (i.e., last Pap test 5 or more years ago, or never) Appalachian women participated in in-depth interviews. These semi-structured interviews provided updated perspectives on screening determinants and framed the interview guide for the second qualitative activity: focus group interviews. The focus groups were conducted to confirm the findings of the in-depth interviews, pretest a pilot survey instrument, and brainstorm about an upcoming intervention to increase ICC screening among Appalachian women. Ten focus groups were undertaken: five with women who had been screened according to American Cancer Society guidelines at the time, and five with women who fell outside of the screening guidelines. Following subsequent revisions of the instrument, it was again pilot-tested with 10 middle-aged and older Appalachian women to ensure that the questionnaire comprehensively and appropriately encapsulated barriers to ICC screening. Qualitative analyses of these data have been previously reported [36].
Baseline Assessment of Appalachian Women’s Barriers to Cervical Cancer Screening
Sample Recruitment
Members of the targeted study population—women between the ages of 40–64 who fall outside of ICC screening guidelines—are often considered among the most likely to forgo Pap tests [37]. Additionally, Appalachian women are often perceived as difficult to reach due to geographical isolation, traditions of self-reliance, and other factors [38, 39]. To address these circumstances and adhere to community preferences, this project involved churches as the focal point for participant recruitment for the parent study, a RCT testing an intervention to increase ICC screening. Twenty-nine denominations, approximating the denominational characteristics of the counties in which the project was conducted, were recruited into the study using snowball sampling. The specifics of the faith-placed recruitment and intervention procedures are discussed elsewhere [36]. In brief, all members of a congregation were invited to an informational meeting about cancer prevention, at which attendees were screened for eligibility. Inclusion criteria of the parent intervention study limited the potential participants to women who (a) spoke English; (b) were aged 40–64; (c) had no history of ICC; (d) had not undergone hysterectomy; and (e) had not had a Pap test within the past 12 months (in line with screening recommendations at the time of study initiation). Women who were eligible and willing to participate provided informed consent and completed the survey instrument as a baseline assessment. To mitigate limited literacy, interviewers orally administered all documents, unless requested otherwise.
Measures
The 88-item questionnaire developed for this study collected the following data: last Pap test date; knowledge, attitudes, and behaviors regarding ICC and screening; and other potential barriers identified during the foundational qualitative studies, described above. Additionally, sociodemographic characteristics and general perceptions of health status were collected.
In line with the PRECEDE/PROCEED framework, barriers to ICC screening were represented by items reflecting predisposing (21 items), enabling (26 items), and reinforcing (13 items) factors related to obtaining Pap tests, for a total of 60 possible barriers to screening. Items assessing beliefs and attitudes were in Likert-type formats with 5 response options (1 = strongly disagree; 2 = disagree; 3 = unsure; 4 = agree; 5 = strongly agree).
Predisposing factors included self-efficacy toward Pap testing, risk perception regarding ICC, and other knowledge, attitudes, and beliefs related to ICC screening. Enabling factors included structural variables, such as having a usual source of medical care, health insurance status, and expected financial expense of being screened. Reinforcing factors included variables such as perceived influence of one’s physician’s medical advice, perceived influence of family members or friends regarding health care decisions, and perceived quality of experiences with health care providers.
Data Analyses
Descriptive statistics were used to summarize sample characteristics and responses to the questionnaire items. Likert-type item responses were dichotomized to reflect agreement or disagreement with each potential barrier. Frequencies and percentages of participants endorsing each item as a barrier were calculated. Items were ranked to indicate the most frequently reported barriers to cervical cancer screening among this sample of Appalachian women. Rankings were obtained overall as well as within each theoretical category (i.e., across and within predisposing, enabling, and reinforcing factors, respectively). Finally, unadjusted odds ratios (OR) were calculated to estimate the associations between specific participant characteristics and the most frequently reported barriers overall. The four demographic characteristics included age, education, perceived income adequacy, and health insurance status. The two health-related characteristics included screening history and perceived health status. Statistical significance was set at the 0.05 probability level. All analyses were conducted with Stata/IC 10.1 for Windows.
Results
Sample Characteristics
Participants’ (N = 345) mean age was 51 years (SD = 7), with a range from 40 to 64 years. See Table 1 for detailed characteristics. Nearly all (95 %) participants were non-Hispanic Caucasian, reflecting the demographics of this region [40]. In general, participants reported indicators of low socioeconomic status, including unemployment (50 %), lack of health insurance (32 %), and high school education or less (64 %). Just over half of participants described their health status positively (ranging from good to excellent), while 15 % reported poor health status. Regarding ICC screening history, the majority of the sample (66 %) had been screened more than 1 but less than 5 years ago; however, 33 % reported having their last Pap test 5 or more ago, and 1 % reported never having had a Pap test.
Prevalence of Reported Barriers
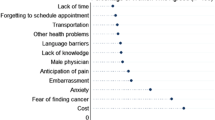
Percentages of participants reporting each barrier are presented in Table 2 (predisposing factors), Table 3 (enabling factors), and Table 4 (reinforcing factors), and barriers are ranked by frequency of endorsement across the three categories of factors. Endorsement of specific barriers ranged from 4 to 78 %, with only 8 of the 60 possible barriers being reported by a majority (>50 %) of participants. These top 8 reported barriers included: “I think that a test to find polyps or cancer makes people worry” (78 %); “I cannot use public transportation to get to my medical appointments” (71 %); “I am afraid of a cancer being found” (67 %); “I would be more likely to screen if I could use a home kit” (66 %); “I would be more likely to have a Pap test if the procedure was completely paid for by my insurance company” (65 %); “I would be more likely to get tested if I could choose whether the doctor doing the test is a man or woman” (64 %); “Pap tests are too embarrassing” (56 %); and “I believe a person with cervical cancer would have symptoms” (52 %). Notably, half of the top 8 barriers reported were predisposing factors (see Table 2), while half were enabling factors (see Table 3); the highest percentage of participants reporting a reinforcing factor as a barrier to cervical cancer screening was only 43 % (“I do not know a lot of people who have had Pap tests in the past year”).
Barriers reported by 10 % or fewer of participants included: “My risk of getting cancer is too low to have a screening” (10 %); “I do not believe I can get a Pap test” (10 %); “Cervical cancer is not curable if it is detected early” (10 %); “My doctor’s advice is not important in my health decisions” (8 %); “You do not need to do the Pap test if feeling fine” (7 %); “I don’t have a telephone” (6 %); and “I do not know where to get a Pap test” (4 %). Over half of these infrequently reported barriers were predisposing factors, while two were enabling and one was a reinforcing factor.
Correlates of Reported Barriers
Unadjusted ORs and 95 % confidence intervals (CIs) of each of the 8 most frequently endorsed barriers given participants’ characteristics are reported in Table 5. All barriers but two (i.e., being more likely to screen with a home kit or if able to choose the sex of the physician performing the test) were significantly associated with at least one participant characteristic.
Demographic Characteristics: Education, Age, Perceived Income Adequacy, and Type of Health Insurance Coverage
In the current sample, educational level was significantly associated with only one barrier: being unable to use public transportation for medical appointments, an enabling factor. Participants with some college education (OR = 1.95, 95 % CI: 1.00–3.78) and those with a college education or more (OR = 5.94, 95 % CI: 1.94–18.17) had significantly higher odds of reporting this barrier, compared to those with less than a high school education. Similarly, participant age was significantly associated with only a single barrier: feeling embarrassed by Pap tests, a predisposing factor. Participants who were 45–54 years old had lower odds of reporting embarrassment associated with Pap tests as a barrier to screening (OR = 0.49, 95 % CI: 0.27–0.89), compared to their counterparts 40–44 years old.
Participants’ perceived income adequacy, however, was significantly associated with four barriers: belief that Pap tests cause worry, being afraid of cancer being found, inability to use public transportation, and not having health insurance coverage for the screening procedure. For the former two predisposing factors, participants reporting higher levels of perceived income adequacy were much less likely to report these barriers than those who struggled to have their financials needs met. As for the latter two enabling factors, participants reporting having just enough income to get by had significantly higher odds of reporting the public transportation barrier, compared to the lowest perceived income group (OR = 1.75, 95 % CI: 1.05–2.91). In contrast, those in the highest perceived income group had significantly lower odds of reporting lack of insurance as a barrier to screening, compared to the lowest perceived income group (OR = 0.29, 95 % CI: 0.11–0.75).
In addition, participants’ type of health insurance coverage was also significantly associated with two enabling (i.e., being unable to use public transportation for medical appointments and lack of insurance coverage of screening) and two predisposing factors (i.e., being afraid of cancer being found and belief that a person with cervical cancer would have symptoms). More specifically, those with employer-provided insurance had much higher odds of reporting the barrier of not being able to use public transportation to get to their medical appointments (OR = 2.09, 95 % CI: 1.13–3.85), compared to those without health insurance coverage. Conversely, those with employer-provided insurance had lower odds of reporting fear of finding cancer (OR = 0.45, 95 % CI: 0.26–0.78) and lack of health insurance coverage (OR = 0.49, 95 % CI: 0.29–0.85) as barriers, compared to those with no insurance. Participants covered by Medicaid had much lower odds of reporting not being able to use public transportation (OR = 0.46, 95 % CI: 0.24–0.88) and much higher odds of believing that a person with ICC would have symptoms (OR = 2.68, 95 % CI: 1.37–5.23) compared to uninsured participants.
Health-Related Characteristics: Screening History and Perceived Health Status
Participants’ ICC screening status was not significantly associated with any of the eight most frequently reported barriers at baseline. However, participants’ perceived health status was significantly associated with three predisposing and two enabling factors. Regarding predisposing factors, compared to those in poor health, participants perceiving their health status as fair had significantly higher odds of reporting that Pap tests were embarrassing (OR = 2.37, 95 % CI: 1.17–4.81). Those reporting very good health had significantly lower odds of reporting a fear of cancer being found (OR = 0.18, 95 % CI: 0.07–0.44) and believing that a person with ICC would have symptoms (OR = 0.37, 95 % CI: 0.16–0.85), compared to those with poor health status. Participants reporting excellent health also had significantly lower odds of reporting a fear of cancer being found (OR = 0.24, 95 % CI: 0.07–0.87) than those with poor health. Regarding enabling factors, participants perceiving their health status as only fair had significantly higher odds of reporting the inability to use public transportation (OR = 2.13, 95 % CI: 1.02–4.48) compared to those with poor health. In contrast, participants perceiving themselves to be in very good health had lower odds of identifying health insurance coverage as a barrier to screening (OR = 0.42, 95 % CI: 0.18–0.97), compared to those in poor health.
Discussion
Efforts to reduce the disproportionate disease burden of ICC in Appalachian Kentucky [11, 12] require an enhanced understanding of the complex ways in which socioeconomic, cultural, emotional, and logistic factors affect screening decisions in this region [41, 42]. Two major and intersecting study findings merit discussion: (a) the frequent identification of predisposing and enabling—but not reinforcing—factors as barriers to ICC screening, and (b) the associations between specific identified barriers to screening and several demographic and health-related characteristics of participants.
Predisposing, Enabling, or Reinforcing?
Of 60 possible barriers generated through developmental qualitative work in the region, 8 were endorsed by a majority of participants. Four were classified as predisposing factors (i.e., beliefs and attitudes about screening) and four as enabling factors (i.e., resources and situations influencing screening), using the PRECEDE/PROCEED framework. No reinforcing factors were endorsed by a majority of participants.
Predisposing Factors
The most frequently endorsed predisposing factors included items tapping negative emotions (fear, worry, and embarrassment) and erroneous beliefs (that a person with ICC would have symptoms). Frequent participant endorsement of these barriers to screening demonstrates the salience of emotions and beliefs in this vulnerable population. Like other traditionally underserved groups, middle-aged and older women in Appalachian Kentucky may experience misperceptions, apprehension, and negativity regarding ICC screening in part due to infrequent exposure to Pap tests [39]. In particular, the fear of cancer being detected was strongly associated with several participant characteristics. Those with lowest perceived income adequacy, lack of health insurance coverage, and worse perceived health status were more likely to report this fear than those with higher perceived income adequacy, employer-provided insurance coverage, and very good or excellent perceived health status, respectively. Thus, some of the most vulnerable participants in the study—those with the greatest financial and health stressors—also disproportionately reported a significant emotional barrier to obtaining ICC screening.
Enabling Factors
Given the limited resources in the region, the frequent endorsement of several enabling factors as barriers to Pap tests was unsurprising. Participants identified barriers with regard to access to health care facilities, health insurance coverage, and testing costs. All four of the counties in which this study was conducted are designated Health Professional Shortage Areas, where the primary care physician-to-population ratio is less than 1:4,000 [43]. Approximately one-third of participants reported having no health insurance, and an equal proportion relied on Medicare or Medicaid, possibly limiting opportunities to obtain high quality preventive services [44]. Inadequate access to providers could help explain erroneous beliefs, worry, and lack of provider recommendations for screening.
An enabling factor frequently mentioned as impeding access to screening in high-risk areas [45, 46] —limited transportation—may be more nuanced than generally conceived. Although most participants (71 %) in the current study indicated that they cannot use public transportation to get to health care appointments, this item may not have discriminated between those who do versus do not need public transportation. In the counties in which this research was conducted, household income is used to determine eligibility for use of most, if not all, public transportation to medical appointments [47]. Participants with higher educational levels, higher perceived income sufficiency, and employer-sponsored health insurance appeared more likely to endorse this item; however, they likely did not qualify for public transportation in their counties precisely because they did not need it. Other items, endorsed by fewer participants, may have more accurately reflected transportation barriers: for example, “the roads make traveling hard to get to medical appointments” (endorsed by 21 %), “not having a car makes it hard to get to medical appointments” (20 %), and “it’s hard for me to get transportation to my medical appointments” (18 %).
Reinforcing Factors
Interestingly, none of the most frequently reported barriers to ICC screening were reinforcing factors (i.e., events or situations promoting the continuation of screening—e.g., negative medical experiences or perceived influence of physician advice). Since study participants were out of compliance with screening guidelines at the time of the study, it is possible that they also were not receiving other recommended health services. In the absence of regular Pap tests and overall health care, participants may not have had many medical experiences—positive or negative—to influence their screening behaviors. Previous studies have demonstrated that a key determinant of receiving preventive services, including Pap tests, is undergoing other types of preventive screening [48, 49]. Levy and colleagues found, for instance, that rural residents with health maintenance visits in the preceding 26 months were significantly more likely to undergo colorectal cancer screening than those without such visits [50]. For the participants in the current study, lack of endorsement of reinforcing factors related to medical care history and communication with physicians may signal an absence of influential interactions with health care providers. In fact, over one-third of participants in this study reported the lack of physician recommendation, an especially concerning finding since previous findings suggest that physician recommendation is a major—if not the most—significant predictor of obtaining screening [50–54].
Another potential reinforcing factor barrier, the role played by socially significant others, is complex. While many participants indicated that they knew others who had been screened for ICC, that family and friends’ advice were important, or that people close to them advised them to get needed medical care, such social support may not be compelling enough to override the predisposing and enabling barriers that obstruct cancer screening. This finding is a departure from several studies demonstrating an association between Pap test screening and encouragement from socially supportive individuals [51, 55]. Allen and colleagues described a slightly different picture of the role of social support and social networks’ influence on cancer screening, one that may converge with the current results [52]. In their study, mammogram use was positively associated with participant perception that such screening was normative and encouraged among their peers; however, explicit encouragement of mammogram use was negatively associated with screening.
Implications for Policy and Practice
Although many of the barriers assessed in this study were endorsed by only a minority of participants, the additive effects of several barriers experienced by one individual may relegate screening to a lower priority [56]. In other cases, a single endorsed item may suggest several underlying barriers. Multiple and intersecting barriers may prove more challenging to overcome than one commonly experienced barrier to screening. For example, 66 % of participants endorsed the item, “I would be more likely to screen if I could use a home kit.” This barrier actually may encompass multiple other barriers: enabling factors like transportation challenges, limited clinic hours, and time constraints, as well as predisposing factors such as concerns about privacy and feelings of embarrassment. Thus, it is unlikely that addressing any single barrier alone will substantially increase ICC screening rates among underserved Appalachian women. Instead, a focus on combinations of the most prevalent barriers in this high risk population—particularly related to financial challenges, negative emotions, and lack of knowledge—may facilitate inroads to increase screening rates.
Addressing financial barriers that impede Pap tests is a perpetual challenge in this Appalachian community and in most underserved environments. Health care reform initiatives may very well increase insurance coverage or bolster preventive service capacity among these women, some of whom, in the pre-reform system, may have just enough resources to disqualify them for Medicaid. However, another approach to reducing financial barriers involves increased publicity regarding local resources that provide not only Pap tests, but also follow-up care, with adjusted or even no fees. Such programs, including the National Breast and Cervical Cancer Early Detection Program often conducted through local health departments or federally qualified health centers, will not necessarily curtail all expenses associated with Pap tests (e.g., time off from work, costs associated with travel and child- or adult-care, and others), but may alleviate some financial strain.
Targeting knowledge deficits and negative emotions may be the “lowest hanging fruit” in the intervention orchard. As is intuitive and well-documented, those with greater knowledge of cancer, or “cancer literacy,” are more likely to engage in screenings [41, 57, 58]. Women in the current study, as found in previous studies in Appalachia, experienced several knowledge deficits that may be associated with inadequate screening [59]. These frequently endorsed barriers could be remediated by improving participants’ understanding of (a) the asymptomatic nature of the early stages of ICC; (b) the way that tests can be conducted to minimize embarrassment and discomfort; (c) the potential for screening tests to actually lessen worry; and (d) the curable nature of early stage ICC [60]. Many participants were not aware that early detection and treatment of ICC is linked with increased long-term survival. Thus, providing clear and sensitive information might ease the worry and fears associated with screening.
In addition, fear and embarrassment might be mitigated with repeated exposure to ICC screening: a situation that once was mortifying or worrisome soon could become merely a little unpleasant once routinized [23]. Indeed, ample research demonstrates that once an individual overcomes barriers so that screenings become normative, repeat screenings are common. For example, in their analyses of nearly 1,600 women from NCI’s HINTS panel, Rakowski et al. [61] found that 88.5 % of women who obtained a recent mammogram also reported having a prior mammogram on schedule.
Study Limitations
Several limitations merit discussion. Participant recruitment was targeted to a single region of Appalachia, and findings may not be representative of other Appalachian areas. Appalachian Kentucky is, however, one of the regions in the United States most disproportionately affected by ICC. In addition, the sample was comprised predominately of White participants, though this is reflective of the demographics of the region. With regard to screening status, no comparison was possible with women who were in compliance with Pap test recommendations, due to the intervention inclusion criteria targeting only those women who had not had a Pap test within a recommended time frame. Finally, the cross-sectional nature of these baseline data precludes any causal conclusions regarding barriers and ICC screening. Future work will investigate relationships between barriers reported by participants at baseline and the eventual receipt of Pap tests following an intervention delivered by local lay health advisors.
Conclusions
Women in Appalachia, and specifically in Appalachian Kentucky, continue to carry a disproportionate burden of ICC incidence and mortality. This inequity is likely due to inadequate rates of cervical cancer screening. Barriers to screening identified by participants in the current study include a range of issues which can be characterized as predisposing, enabling, and reinforcing factors. The most commonly endorsed barriers in the current study highlight financial impediments, inadequate knowledge, and negative emotions about ICC screening. While some approaches to reduce these barriers must involve political, economic, and structural interventions (e.g., health care system reform), other potentially effective methods will require direct interactions with women at risk for ICC: providing education about existing affordable and accessible screening programs; improving knowledge regarding ICC screening and treatment; and addressing worry, fear, and embarrassment associated with screening. In planning and delivering such interventions in Appalachia, attention to cultural preferences is vitally important. Several strategies have been suggested, both by participants in the qualitative portion of the current study, and by previous research—for example, drawing on local patient navigators to more clearly explain the Pap test process; employing trusted local lay health advisors for educational services; and, consistent with local traditions of imparting knowledge, using storytelling to meld educational material with emotional and inspirational messages [35, 36]. In the Appalachian region, creative approaches to reduce barriers to screening, designed and delivered in partnership with local communities, stand an excellent chance of eliminating a cancer that should no longer end the life of any woman [60].
References
Cancer facts and figures 2012. (2012). Atlanta: American Cancer Society. Accessed 3 September, 2011, available at http://www.cancer.org/Research/CancerFactsFigures/CancerFactsFigures/cancer-facts-figures-2012.
Cancer advances in focus: Cervical cancer. (2010). Bethesda, MD: National Cancer Institute. Accessed 3 September, 2012, available at http://www.cancer.gov/cancertopics/factsheet/cancer-advances-in-focus/cervical.
Blackman, D. K., Bennett, E. M., & Miller, D. S. (1999). Trends in self-reported use of mammograms (1989–1997) and Papanicolaou tests (1991–1997)—behavioral risk factor surveillance system. Morbidity and Mortality Weekly Report, 48(SS-6), 1–22.
IARC Working Group on Evaluation of Cervical Cancer Screening Programmes. (1986). Screening for squamous cervical cancer: Duration of low risk after negative results of cervical cytology and its implication for screening policies. British Medical Journal (Clinical Research Edition), 293(6548), 659–664.
Healthy People Consortium Meeting. (1998). Community implementation micro-grants. Healthy people 2010. Washington, DC: US Department of Health and Human Services, Office of Disease Prevention and Health Promotion.
Developing Healthy People 2020. Washington, DC: US Department of Health and Human Services, Office of Disease Prevention and Health Promotion. Accessed September 3, 2012, available at http://healthypeople.gov/2020/topicsobjectives2020/objectiveslist.aspx?topicId=5.
Anderson, L. M., & May, D. S. (1995). Has the use of cervical, breast, and colorectal cancer screening increased in the United States? American Journal of Public Health, 85(6), 840–842.
Solomon, D., Breen, N., & McNeel, T. (2007). Cervical cancer screening rates in the United States and the potential impact of implementation of screening guidelines. CA: A Cancer Journal for Clinicians, 57(2), 105–111.
Ries, L. A. G., Eisner, M. P., Kosary, C. L., et al. (2000). National Cancer Institute. SEER cancer statistics review, 1973–1997. Bethesda, MD: US Department of Health and Human Services.
Appalachian Regional Commission. (1999). Demographic diversity and economic change. Accessed August 8, 2010, available at http://www.arc.gov/index.
Hopenhayn, C., Bush, H., Christian, A., & Shelton, B. J. (2005). Comparative analysis of invasive cervical cancer incidence rates in three Appalachian states. Preventive Medicine, 41(5–6), 859–864.
Ries, L. A. G., Eisner, M. P., Kosary, C. L., et al. (2005). Cancer Statistics Review, 1975–2002. Bethesda, MD: National Cancer Institute.
Kentucky Cancer Registry. (2010). Cancer inquiry system. Accessed August 8, 2010, available at http://www.cancer-rates.info/ky/index.php. Accessed 8 Aug, 2010.
Jenkins, T. (2002). Unpublished data from BRFSS, 2002.
Arnsberger, P., Fox, P., Ryder, P., Nussey, B., Zhang, X., & Otero-Sabogal, R. (2006). Timely follow-up among multicultural women with abnormal mammograms. American Journal of Health Behavior, 30(1), 51–61.
Documét, P. I., Green, H., Adams, J., Weil, L. A., Stockdale, J., & Hyseni, Y. (2008). Perspectives of African American, Amish, Appalachian and Latina women on breast and cervical cancer screening: Implications for cultural competence. Journal of Health Care for the Poor and Underserved, 19(1), 56–74.
Ahmed, N. U., Fort, J. G., Elzey, J. D., & Bailey, S. (2004). Empowering factors in repeat mammography: Insights from the stories of underserved women. The Journal of Ambulatory Care Management, 27(4), 348–355.
Brouse, C. H., Basch, C. E., Wolf, R. L., & Shmukler, C. (2004). Barriers to colorectal cancer screening: An educational diagnosis. Journal of Cancer Education, 19(3), 170–173.
Tarasenko, Y. T., Wackerbarth, S. B., Love, M. M., Joyce, J. M., & Haist, S. A. (2011). Colorectal cancer screening: Patients’ and physicians’ perspectives on decision-making factors. Journal of Cancer Education, 26(2), 285–293.
Palmer, R. C., Lynn, A. M., & Dankwa, I. (2008). Colorectal cancer screening and African Americans: Findings from a qualitative study. Cancer Control: Journal of the Moffitt Cancer Center, 15(1), 72–79.
Gielen, A. C., & McDonald, E. M. (2002). Using the PRECEDE/PROCEED planning model to apply health behavior theories. In K. Glanz, F. M. B. K. Rimer, & F. M. Lewis (Eds.), Health behavior and health education: Theory, research and practice, 3rd edn (pp. 409–436). San Francisco: Jossey-Bass.
Green, L. W., & Kreuter, M. W. (1999). Health promotion planning: An educational and environmental approach (3rd ed.). Mountain View, CA: Mayfield.
Leach, C. R., & Schoenberg, N. E. (2007). The vicious cycle of inadequate early detection: A complementary study on barriers to cervical cancer screening among middle aged and older women. Preventing Chronic Disease, 4(4), A95.
Lartey, M., Joubert, G., & Cronje, H. (2003). Knowledge, attitudes and practices of rural women in South Africa regarding the Pap smear. International Journal of Gynaecology and Obstetrics, 83(3), 315–316.
Meissner, H. I., Breen, N., Taubman, M. L., Vernon, S. W., & Graubard, B. I. (2007). Which women aren’t getting mammograms and why? (United States). Cancer Causes and Control: CCC, 18(1), 61–70.
Hislop, T., Deschamps, M., Taylor, V., et al. (2003). Facilitators and barriers to cervical cancer screening among Chinese Canadian women. Canadian Journal of Public Health, 94(1), 68–73.
Kelsey, K. S., Campbell, M. K., DeVellis, B., et al. (2000). Social support and health behaviors among blue collar workers. American Journal of Health Behavior, 24(6), 434–443.
DuBard, C. A., Schmid, D., Yow, A., Rogers, A. B., & Lawrence, W. W. (2008). Recommendations for and receipt of cancer screenings among Medicaid recipients 50 years and older. Archives of Internal Medicine, 168(18), 2014–2021.
McPhee, S. J., Richard, R. J., & Solkowitz, S. N. (1986). Performance of cancer screening in a university general internal medicine practice: Comparison with the 1980 American Cancer Society Guidelines. Journal of General Internal Medicine, 1(5), 275–281.
Paskett, E. D., Tatum, C. M., D’Agostino, R., et al. (1999). Community-based interventions to improve breast and cervical cancer screening: Results of the Forsyth County Cancer Screening (FoCaS) Project. Cancer Epidemiology, Biomarkers and Prevention, 8(5), 453–459.
Mayo, R. M., Ureda, J. R., & Parker, V. G. (2001). Importance of fatalism in understanding mammography screening in rural elderly women. Journal of Women and Aging, 13(1), 57–72.
Paskett, E. D., Carter, W. B., Chu, J., & White, E. (1990). Compliance behavior in women with abnormal Pap smears. Developing and testing a decision model. Medical Care, 28(7), 643–656.
Pachter, L. M. (1994). Culture and clinical care. Folk illness beliefs and behaviors and their implications for health care delivery. JAMA: The Journal of American Medical Association, 271(9), 690–694.
Schoenberg, N. E., Hopenhayn, C., Christian, A., Knight, E., & Rubio, A. (2006). An in-depth and updated perspective on determinants of cervical cancer screening among central Appalachian women. Women and Health, 42(2), 89–105.
Katz, M. L., Wewers, M. E., Single, N., & Paskett, E. D. (2007). Key informants’ perspectives prior to beginning a cervical cancer study in Ohio Appalachia. Qualitative Health Research, 17(1), 131–141.
Schoenberg, N., Hatcher, J., Dignan, M., Shelton, B., Wright, S., & Dollarhide, K. (2009). Faith moves mountains: An Appalachian cervical cancer prevention program. American Journal of Health Behavior, 33(6), 627–638.
Kerner, J. (2001). Excess cervical cancer mortality: Inevitable or avoidable? Paper presented at the reducing health disparities in high cervical cancer mortality regions. Bethesda, MD: National Cancer Institute.
Behringer, B., & Friedell, G. H. (2006). Appalachia: Where place matters in health. Preventing Chronic Disease, 3(4), A113–A118.
Elnicki, D. M., Morris, D. K., & Shockcor, W. T. (1995). Patient-perceived barriers to preventive health care among indigent, rural Appalachian patients. Archives of Internal Medicine, 155(4), 421–424.
Data reports, 2010. (2010). Appalachian Regional Commission. Accessed August 8, 2010, available at http://www.arc.gov/data.
Chavez, L. R., McMillan, J. M., Mishra, S. L., & Hubbell, F. A. (2001). Beliefs matter: Cultural beliefs and the use of cervical cancer-screening tests. American Anthropologist, 103(4), 1114–1129.
Harlan, L. C., Bernstein, A. B., & Kessler, L. G. (1991). Cervical Cancer screening: Who is not screened and why? American Journal of Public Health, 81(7), 885–890.
An analysis of disparities in health status and access to health care in the Appalachian region, 2007. (2007). Appalachian Regional Commission. Accessed May 3, 2010, available at http://www.arc.gov/index.do?nodeId=2378.
An analysis of the financial conditions of health care institutions in the Appalachian region and their economic impacts, 2002. (2002). Appalachian Regional Commission. Accessed June 1, 2007, available at http://www.arc.gov/index.do?nodeId=1647.
Daley, E., Alio, A., Anstey, E. H., Chandler, R., Dyer, K., & Helmy, H. (2011). Examining barriers to cervical cancer screening and treatment in Florida through a socio-ecological lens. Journal of Community Health, 36(1), 121–131.
Coronado, G. D., Thompson, B., Koepsell, T. D., Schwartz, S. M., & McLerran, D. (2004). Use of Pap test among Hispanics and non-Hispanic whites in a rural setting. Preventive Medicine, 38(6), 713–722.
Community Action Council (L.K.L.P.). Accessed 8 August, 2010. http://www.lklp.org/Programs/PublicTransportation/tabid/137/Default.aspx.
Amonkar, M. M., & Madhavan, S. (2002). Compliance rates and predictors of cancer screening recommendations among Appalachian women. Journal of Health Care for the Poor and Underserved, 13(4), 443–460.
Lyttle, N. L., & Stadelman, K. (2006). Assessing awareness, knowledge of breast, cervical cancer among Appalachian women. Preventing Chronic Disease, 3(4), A125.
Levy, B. T., Dawson, J., Hartz, A. J., & James, P. A. (2006). Colorectal cancer testing among patients cared for by Iowa family physicians. American Journal of Preventive Medicine, 31(3), 193–201.
Taylor, V. M., Yasui, Y., Burke, N., et al. (2004). Pap testing adherence among Vietnamese American women. Cancer Epidemiology, Biomarkers and Prevention, 13(4), 613–619.
Allen, J. D., Sorensen, G., Stoddard, A. M., Peterson, K. E., & Colditz, G. (1999). The relationship between social network characteristics and breast cancer screening practices among employed women. Annals of Behavioral Medicine, 21(3), 193–200.
Klabunde, C. N., Frame, P. S., Meadow, A., Jones, E., Nadel, M., & Vernon, S. W. (2003). A national survey of primary care physicians’ colorectal cancer recommendations and practices. Preventive Medicine, 36(3), 352–362.
Winawer, S. J. (2001). A quarter century of colorectal cancer screening: Progress and prospects. Journal of Clinical Oncology, 19(18 Suppl), 6S–12S.
Otero-Sabogal, R., Stewart, S., Sabogal, F., Brown, B. A., & Perez-Stable, E. J. (2003). Access and attitudinal factors related to breast and cervical cancer rescreening: Why are Latinas still underscreened? Health Education and Behavior, 30(3), 337–359.
O’Malley, A. S., Beaton, E., Yabroff, K. R., Abramson, R., & Mandelblatt, J. (2004). Patient and provider barriers to colorectal cancer screening in the primary care safety-net. Preventive Medicine, 39(1), 56–63.
Pearlman, D. N., Clark, M. A., Rakowski, W., & Ehrich, B. (1999). Screening for breast and cervical cancers: The importance of knowledge and perceived survivability. Women and Health, 28(4), 93–112.
Xu, Y., Ross, M. C., Ryan, R., & Wang, B. (2005). Cancer risk factors of Vietnamese Americans in rural South Alabama. Journal of Nursing Scholarship, 37(3), 237–244.
Shell, R., & Tudiver, F. (2004). Barriers to cancer screening by rural Appalachian primary care providers. The Journal of Rural Health, 20(4), 368–373.
Cervical cancer, 2009. Bethesda, MD: National Cancer Institute. Accessed January 22, 2010, available at http://www.cancer.gov/cancertopics/types/cervical/.
Rakowski, W., Meissner, H., Vernon, S. W., Breen, N., Rimer, B., & Clark, M. A. (2006). Correlates of repeat and recent mammography for women ages 45 to 75 in the 2002 to 2003 Health Information National Trends Survey (HINTS 2003). Cancer Epidemiology, Biomarkers and Prevention, 15(11), 2093–2101.
Acknowledgments
This project was supported by the National Cancer Institute (R01CA108696). We acknowledge and thank all Faith Moves Mountains’ community and scientific staff and participants. Last, but not least, we wish to express our appreciation to the community members who have offered extensive support to this project.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Studts, C.R., Tarasenko, Y.N. & Schoenberg, N.E. Barriers to Cervical Cancer Screening Among Middle-Aged and Older Rural Appalachian Women. J Community Health 38, 500–512 (2013). https://doi.org/10.1007/s10900-012-9639-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10900-012-9639-8