Abstract
Generalized anxiety disorder (GAD) has been associated with significant impairment and estimates of human and economic burden associated with the disorder are substantial. Little has been done, however, to examine impairment associated with subthreshold presentations of the disorder in medically underserved populations. This study compared primary care patients with GAD (n = 30), subthreshold GAD (n = 21), worry (n = 79), and no worry (n = 199) on measures of human and economic burden. On measures of human burden, all three symptomatic groups reported poorer perceived physical health, greater stress, and sleep difficulty. Worried and subthreshold groups also reported lower social support. For economic burden, GAD and worry groups reported a greater number of prescription medications. However, when co-morbid depression was accounted for the effect was no longer significant. Groups did not differ on employment status, number of visits to the clinic in the last 90 days, or physical health. Results are discussed in terms of identification, prevention, and intervention for GAD in primary care settings.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The hallmark feature of Generalized Anxiety Disorder (GAD) is chronic, uncontrollable worry about a number of events or activities in daily life. In addition, the diagnosis requires three of the following six associated symptoms: restlessness, fatigue, difficulty concentrating, irritability, muscle tension, and difficulty sleeping (American Psychiatric Association, 2000). Recent studies have found that individuals with GAD frequently present to their primary care provider rather than a mental health clinic (Roy-Byrne & Wagner, 2004), with the prevalence rates in primary care clinics ranging from a low of 3.7% to a high of 14.8% (Olfson et al., 1997; Olfson, 2000). Further, GAD is the most common anxiety disorder seen in primary care and accounts for more than 50% of all anxiety disorders in that setting (Wittchen & Hoyer, 2001). GAD is associated with significant impairment, and the disability due to GAD is comparable to that of major depressive disorder (MDD; Kessler, DuPont, Berglund, & Wittchen, 1999). Individuals with GAD show significant interference in functioning, including adjustment to daily routine, energy input and performance, contact with others at work, and other daily activities. When GAD is present for at least a month, associated disability equals that of chronic somatic diseases, including diabetes, arthritis, cardiovascular disease, cancer, tuberculosis, asthma, and HIV-positive illness (Maier, Gänsicke, Freyberger, Linz, Heun, & Lecrubier, 2000). In contrast to the well documented interference associated with GAD, little has been done to investigate subthreshold presentations of GAD and associated impairment in primary care, although subthreshold presentations of the disorder are common (Pini, Perkonnig, Tansella, & Wittchen, 1999; Rucci et al., 2003). If significant impairment exists, increasing recognition of symptoms and increasing referrals for appropriate treatment could reduce human and economic burden substantially.
The disability and interference related to GAD has been conceptualized as both human and economic burden. The human burden has been defined as impairment in social, family, and occupational functioning; perceived emotional and physical health; well-being; and satisfaction with daily life (Hoffman, Dukes, & Wittchen, 2008). Estimates suggest that the disorder significantly impairs quality of life. Individuals with GAD report poorer overall well-being and greater dissatisfaction with their main activity and family life than those without GAD, even after adjusting for lifetime dysthymia, age, gender, and social class (Stein & Heimberg, 2004). A review found that individuals with GAD and/or MDD in a community sample reported lower quality of life in multiple domains (i.e., physical functioning, role limitations due to physical health problems, bodily pain, social functioning, general mental health, role limitations due to emotional problems, vitality, energy or fatigue, and general health perceptions) compared to those with no disorder (Hoffman et al., 2008). Primary care studies show similar results. In a sample of low-income, uninsured African American females, those with GAD reported lower health-related quality of life compared to both those with other Axis I diagnoses and those with no diagnosis (Jones, Ames, Jeffries, Scarinci, & Brantley, 2001). Other examinations of primary care samples indicate that individuals with GAD experience poorer family and social role functioning than individuals with no disorder (Ansseau, Fischler, Dierick, Mignon, & Leyman 2005; Oflson et al., 2000; Olfson & Gameroff, 2007).
The economic burden of GAD has been examined in terms of decreased work productivity and increased health care utilization, including more emergency room visits, referrals to specialists, diagnostic tests, and medication (Hoffman et al., 2008). GAD is associated with an increased health care cost of $2,138 per individual (Marciniak et al., 2005), and estimated health costs for individuals with GAD are 64% higher than those without GAD (Olfson & Gameroff, 2007). GAD is much more prevalent in primary care settings compared to the general population, indicative of overuse of the health care system by this group (Roy-Byrne & Wagner, 2004), which may be due in part to poorer perceived health. For example, Hoffman et al. (2008) found that, controlling for sociodemographic factors and other comorbid psychiatric diagnoses, those with GAD and/or MDD were more likely to report fair/poor health than those with no disorder. GAD has also been associated with more emergency room visits compared to those without GAD (Jones et al., 2001; Olfson & Gameroff, 2007). Individuals with GAD are more likely to be unemployed or to depend on government assistance compared to those without GAD (Leon, Portera, & Weissman, 1995; Massion, Warshaw, & Keller, 1993) and in primary care those with GAD were more likely to have missed at least 1 day of work within the last month compared to individuals with no disorder (Oflson, 2000). Another study estimated that GAD is associated with 9.9 days of work lost over the last month, compared to 1.9 days for individuals without GAD or MDD (Wittchen, 2002).
Although the impact of GAD is well understood in general primary care populations, the burden on medically underserved populations remains understudied. This is especially important because low economic status has been shown to increase the risk for GAD (Grant et al., 2005). In addition, it has been suggested that medically underserved and low income populations may utilize medical services differently than those of higher economic status (Jones et al., 2001). The combination of high risk for GAD and potentially different patterns of service utilization suggest that it may be especially beneficial to understand burden and impairment in this population.
There is also a lack of information about impairment in groups who fail to meet diagnostic criteria for the disorder. Subthreshold syndromes generally are not well studied; however, limited data indicate that subthreshold presentation of GAD is common. Subthreshold GAD and MDD are the most common presentations in primary care settings (Pini et al., 1999; Rucci et al., 2003). For example, a study found that 3.6% of individuals reported at least subthreshold symptoms of GAD within the last year, and 7.8% reported a period of at least 1 month where they felt worried, tense, or anxious most of the time (Carter, Wittchen, Pfister, & Kessler, 2001). A primary care study found that presentations of subthreshold GAD and depression were common, and were in fact more common than the threshold presentation of the disorders (8.3–7.6% for GAD and 9.9 and 4.6% for depressive episode, respectively) (Rucci et al., 2003).
Subthreshold presentations of disorders are also associated with significant impairment. The burden of subthreshold depressive disorders or “minor depressions” is comparable to that of other medical disorders, although less than that of major depression (De Gruy & Pincus, 1996; Wells, Burnham, Rogers, Hays, & Camp, 1992), and subthreshold depressive symptoms have been linked with high rates of service utilization and health care costs (Johnson, Weissman, & Klerman, 1992). Subthreshold depression, anxiety, obsessive compulsive disorder (OCD), and drug and alcohol use is associated with more impairment, recent loss of work, marital distress, and use of medical services compared to those who reported no symptoms (Olfson et al., 1996). Pini et al. (1999) also found that threshold and subthreshold disorders (including depressive, anxiety somatoform, and alcohol-related disorders) were comparable in terms of employment status, frequency of medical consultation in the last year, health perception, or physical status. Rucci et al. (2003) examined four levels of symptoms across a range of disorders, including depressive episodes, dysthymia, GAD, panic disorder, agoraphobia, somatization disorder, neurasthenia, and hypochondriasis. Results showed that, for all disorders, the symptomatic, subthreshold, and full criteria groups reported significantly more psychological distress and lower perceptions of health compared to the healthy group. Interestingly, subthreshold disorders did not differ significantly from full criteria disorders on the three variables of interest. Specifically, subthreshold GAD was associated with poor health perception and psychological distress, but not physical disability. Relatedly, Maier et al. (2000) found that even after reducing the minimum number of associated symptoms required for a full diagnosis of GAD, individuals reported marked social disability greater than those with chronic somatic diseases.
It should be noted that there is significant overlap between GAD and MDD. GAD and MDD are frequently comorbid (Kessler, Chiu, Demler, & Walters, 2005) and rates in primary care are particularly high. For example, one study showed that 53% of a primary care GAD sample met criteria for a depressive disorder (Jones et al., 2001). In addition, GAD shares four of six somatic criteria with MDD (American Psychiatric Association, 2000) and worry has been linked with both anxiety and depression. One study found that a worry induction task elicited 60% anxious and 40% depressed mood (Andrews & Borkovec, 1988). Mennin, Heimberg, Fresco, and Ritter (2008) suggest that it is unclear whether the shared symptom constellations best represent GAD, MDD, or both, and in fact the two have been shown to load onto a higher order factor of negative affect (see Mennin et al., 2008 for a discussion). Statistically and conceptually, it is difficult to address this issue and no one solution seems optimal. As discussed by Miller and Chapman (2001), controlling for depression is inappropriate, as removing variance associated with MDD would undoubtedly remove a large portion of variance associated with worry and/or GAD. In this study we examined effects of levels of worry and GAD initially, followed by additional analyses aimed toward identifying effects more specific to worry by including both MDD and worry groups.
Previously reviewed work shows that GAD is common and associated with significant impairment in social, family, and occupational domains, representing serious human and economic burdens. Emerging work suggests that subthreshold levels of anxiety are even more common than threshold disorders and are also related to impairment (Rucci et al., 2003). However, the burden associated with subthreshold presentations of GAD remains understudied, especially in medically underserved populations that may be at increased risk for the disorder. Additional information about relationships between levels of GAD symptoms and impairment could provide an avenue to lessen the human and economic burden not only by addressing the burden of subthreshold GAD, but also by intervening to prevent subthreshold individuals from advancing to GAD. In the current study, individuals from a primary care sample were classified into four groups based on report of GAD symptoms: GAD, subthreshold GAD, worried, and nonworried. Impairment measures consisted of estimates of both human and economic burden. We hypothesized that impairment would increase with symptom level and that individuals in all three symptomatic groups would report impairment greater than that of the no worry group.
Method
Sample and Participant Selection
Participants were adults recruited from a University-based urban ambulatory internal care medical clinic. The clinic provides medical treatment to adults and has a Medically Underserved Area designation from the Shortage Designation Branch of the Bureau of Health Professions (BHPR), Department of Health and Human Services (DHHS). This designation is assigned to areas with a low ratio of primary care providers to patients, a high infant mortality rate, a significant percentage of the population living below the poverty level, and/or a large population over the age of 65 years.
Participants were patients attending one of three half-day clinics. Patients were screened by clinical psychology trainees and/or a clinical psychologist for psychosocial risk factors and self-reported health status using a brief screener adapted from the Primary Care Evaluation of Mental Disorders (PRIME-MD) Patient Questionnaire (Spitzer, Williams, Kroenke, & Linzer, 1994). Patients were approached as part of their routine visit or by physician’s request. Over 15 months, 534 patients were approached at three half-day clinics; 455 patients gave informed consent and were administered the screener.
Measures
Demographics
Medical chart review was used to extract standard demographics, including age, gender, ethnicity, marital status, employment, and whether or not the individual had health insurance.
GAD Symptoms
The PRIME-MD (Spitzer et al., 1994) is a two-step diagnostic instrument used to assess psychological disorders in primary care settings. In the first step, individuals complete a 26-item self-report form, the Patient Questionnaire (PQ), which screens for common symptoms of depression, anxiety, substance abuse, and eating disorder. For this study a 13-item abbreviated version of the PQ was used, eliminating items 1 through 13 which assess specific physical symptoms (e.g., back pain, menstrual pain or problems, chest pain, nausea, gas, indigestion) and including a global rating of perceived stress and social isolation. The screener also includes a 5-point Likert-type self-reported rating of global health ranging from “poor” to “excellent.” Positive patient endorsements on the screener trigger the administration of one or more interview modules which assess major depression, dysthymia, panic disorder, GAD, possible eating disorder, and alcohol abuse. Specific interview modules were administered, when feasible, after positive endorsement of corresponding screener items. For the purpose of this study, only responses to the GAD interview module were included in analyses.
The PRIME-MD has been validated on a sample of 1,000 patients at four primary care sites in the United States. The measure also shows good sensitivity and specificity for anxiety disorders. Sensitivity for any anxiety disorder is estimated at .69 (Spitzer et al., 1994) and specificity ranges from .91 (Anxiety NOS) to .99 (Panic Disorder). For GAD specifically, studies have estimated sensitivity from .57 to .92, specificity from .90 to 97, and overall accuracy at .90 (Loerch, Szegedi, Kohnen, & Benkert, 2000; Spitzer et al., 1994). An examination of the measure’s test–retest reliability indicated that GAD had moderate agreement over a 1 week period (kappa = .59), the highest level of agreement of any anxiety disorder (Bakker, Terluin, van Marwjk, van Mechelen, & Stalmna, 2009).
Symptom Groups
Participant responses to the PRIME-MD were used to form four groups based on GAD symptoms. The GAD group consisted of individuals who met full DSM-IV criteria for GAD. The subthreshold GAD group endorsed Criterion A (excessive worry occurring more days than not), in addition to one or two of the following criteria: B (uncontrollability of the worry), C (three or more physiological symptoms associated with worry), or E (worry causes significant distress and impairment). We also created a worried group, comprised of individuals who endorsed Criterion A but no other GAD symptoms, to examine potential impact of excessive worry in the absence of other GAD symptoms. It could be that worry alone is related to impairment and using a simple one item screening question could be useful in primary care settings. The fourth group denied Criterion A and was considered the no worry group.
Economic Burden
Economic burden is defined as decreased work productivity and increased health care utilization, including more emergency room visits, referrals to specialists, diagnostic tests, and medication. Economic burden was measured by number of visits to the clinic in the last 90 days, number of medications, employment status, and physical health. Physical health was measured by an illness burden score, which was quantified by using disability weights drawn from the World Health Organization Global Burden of Disease (GBD) project (Murray & Lopez, 1996; World Health Organization, 1990). For the purposes of the GBD project, healthcare providers assigned values ranging from 0 (equivalent to state of perfect health) to 1 (equivalent to death) to a variety of mental and physical conditions to indicate states of living with various illnesses. Values approaching 1 indicate that a condition is more severely disabling. Individuals with multiple diagnoses received multiple weights which were summed for a total disability score.
Human Burden
The human burden relates to impairment in social, family, and occupational functioning, poor perceived emotional and physical health, well-being, and low satisfaction with daily life. The human burden was measured by responses to questions about perceived health and stress, social support and sleep trouble. Perceived health was measured from the PRIME-MD item assessing self-reported health. Participants rated health from 1 (excellent) to 5 (poor). Perceived stress was measured by a single item added to the PRIME-MD screener. Participants were asked to rate their level of stress using a 10 point Likert-type scale ranging from 0 (no stress) to 10 (most possible stress). Social isolation was measured by a single yes–no item added to the PRIME-MD screener. The item (“Do you feel you have as much contact as you would like with someone you feel close to, someone you can trust and confide in?”) was based on the work of Williams et al. (1992) and has been found to be associated with decreased survival in patients with coronary artery disease. Sleep trouble was measured by a yes/no response to the question “Have you been having trouble sleeping?” on the screener.
Procedure
Patients were screened in one of two ways: (1) A clinical psychology graduate student or doctoral-level psychologist approached patients waiting for their physician appointment; or (2) patients were referred by clinic resident or attending physicians due to current or potential behavioral health issues (e.g., smoking, medication nonadherence, suspected depression and/or anxiety). Researchers escorted patients to a private examination room where they were informed about the study and invited to participate. All procedures were conducted in compliance with the Institutional Review Board (The University of Louisville's IRB provided approval for the study) standards and participants provided informed consent prior to participation. Upon consent, patients were provided with a modified version of the PRIME-MD screener. If participants appeared to have difficulty with the reading level of the screener, the clinical psychology graduate student or doctoral-level psychologist assisted by reading the items aloud. Positive endorsements of items from the anxiety or depression items from the screener were followed by administration of the interview modules of the PRIME-MD, when feasible (e.g., on occasion participants were called for their appointment with their physician prior to completion of the interview modules). The current study focused on responses to the PRIME-MD GAD interview module.
Results
Sample Characteristics
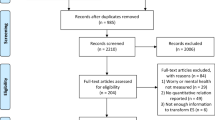
The initial sample included 455 participants. Seven participants did not respond to the initial worry query and were removed from the sample. One hundred nineteen individuals had missing data from the GAD module and were removed from the sample, resulting in a final sample of 329 individuals. Missing data were most commonly the result of patients being called in by their physician before data collection was completed.
Individuals with missing data were compared to those with complete data to determine if the groups differed. An analysis of demographic variables showed no differences by sex, ethnicity, age, marital status, education, or employment. Groups did not differ on measures of economic burden (including number of visits to the clinic in the last 90 days, physical health, or number of medications) or human burden estimates of sleep trouble or social support. However, groups differed significantly on perceived stress, F (1, 430) = 12.51, p < .001, partial η 2 = .03, with those with missing GAD data reporting greater levels of perceived stress, M = 6.45, SD = 2.71, compared to those with complete GAD data, M = 5.06, SD = 3.8. Groups also differed in their perceived health, F (1, 443) = 4.12, p = .04, partial η 2 = .009, with the incomplete data group reporting better health, M = 3.83, SD = .85, than the complete data group, M = 3.62, SD = .98.
Total sample size for each group included 199 for the no worry group, 79 for the worried group, 21 for the subthreshold GAD group, and 30 for the GAD group. Demographic characteristics of each group are presented in Table 1. Overall, the sample was primarily female (n = 198) and nearly equally split between European American and African American (47% for both). Age ranged from 22 to 88 years, with a mean of 53 years. In terms of marital status, 38% (n = 124) were single, 20% (n = 67) were married, 17% (n = 55) were divorced, 9% (n = 29) were widowed, 3% (n = 11) were separated, 7% (n = 22) declined to answer, and 6% (n = 21) were missing. The median level of education was 12 years. Eighty-five percent of the sample (n = 265) was unemployed.
Demographic Analyses
Demographic analyses were first conducted across the four GAD groups to examine potential differences based on symptoms. Chi square analyses showed no differences across the four groups for sex, χ2 (3, N = 312) = 4.16, p = .25, education, χ2 (6, N = 206) = 3.40, p = .76, or marital status, χ2 (6, N = 308) = 4.65, p = .59. There was a significant association between GAD symptom group and ethnicity, χ2 (6, N = 312) = 12.80, p = .046, with 15% of the European American sample, compared to only 4% of the African American sample, meeting criteria for GAD. An ANOVA showed a significant effect for age, F (3, 307) = 10.35, p < .001, partial η 2 = .09, and follow up pairwise Bonferrnoi adjusted comparisons showed that the GAD group (M = 43; SD = 12.45) was significantly younger than the no worry (M = 55; SD = 12.59) and worry groups (M = 51; SD = 10.48), p < .001, p = .02, but did not differ from than subthreshold group (M = 49; SD = 11.45), p = .44. Finally, the four groups differed in the prevalence of MDD, χ2 (3, N = 329) = 102.14, p < .001, with 73% of the full GAD group, 57% of the subthreshold GAD group, 28% of the worried group, and 5% of the no worry group meeting criteria for MDD. See Table 1 for a summary of demographics in each group. Age and ethnicity were entered as covariates for analyses of human and economic burden.
GAD Symptom Presentation
Symptoms of GAD and worry were common in this sample. Twenty-four percent of the sample reported worry about a number of events or activities in daily life and 6% reported symptoms consistent with subthreshold GAD. Nine percent of the total sample met diagnostic criteria for GAD.
Human Burden
First, we examined differences by groups on measures of human burden, including perceived physical health, perceived stress, sleep trouble, and social support. For all ANCOVAs Levene’s test of equality of error variances showed no significant differences between groups, p > .05, indicating that the homogeneity of variances assumption had not been violated. Results showed significant differences between groups for perceived health, F(3, 304) = 9.26, p < .001, partial η2 = .08 and follow up analyses showed that the GAD, subthreshold, and worry groups reported poorer perceived physical health compared to the no worry group (p = .001, .03, and .001, respectively). Groups differed in terms of perceived stress, F(3, 297) = 30.89, p < .001, partial η2 = .24. The GAD, subthreshold, and worry groups reported more stress than the no worry group, p < .001 for all three pairwise tests. See Table 2 and Fig. 1 for means and pairwise comparisons. A binary logistic regression indicated that GAD symptoms also affected sleep trouble, χ2 (3, N = 329) = 24.48, p < .001.Wald statistics for the worried group, W = 14.40, p < .001, the subthreshold group, W = 4.42, p = .04, and the GAD group, W = 9.89, p = .002, were significant. The odds of reporting difficulty sleeping increased by 3.09 (CI = 1.73, 5.54) for the worried group, 2.96 (CI = 1.08, 8.09) for the subthreshold group, and 5.32 (CI = 1.88, 15.06) for the GAD group. Group membership also significantly predicted social support, χ2 (3, N = 329) = 8.13, p = .04. Significant Wald statistics were found for the worry and subthreshold groups, W = 3.94, p = .047, and W = 5.87, p = .02, respectively. The no worry group was twice as likely as the worry group (OR = .53, CI = .28, .99) to report adequate social support. The no worry group was also more likely to report adequate social support compared to the subthreshold GAD group (OR = .30, CI = .11, .80).
Economic Burden
Next we examined the effect of group on measures of economic burden. ANCOVAs were conducted on the previously described continuous variables. Again, Levene’s test of the equality of error variances were nonsignificant for both analyses, p > .05. There was no significant difference between groups for number of visits to the clinic in the last 90 days, F(3, 277) = .31, p = .82, partial η2 = .003, or physical health, F(3, 305) = .91, p = .43, partial η2 = .009. Groups differed in number of medications, F(3, 279) = 4.96, p = .002, partial η2 = .05. The GAD and worry groups were prescribed more medications than the nonworried group (p = .046 and .007, respectively). See Table 2 and Fig. 1 for means and pairwise comparisons. The relationship between group status and employment status was examined using a binary logistic regression with the no worry group set as the reference category. The block with GAD group was not significant, χ2 (3, N = 329) = .59, p = .90.
Unique Effects of Worry
A set of follow up analyses were conducted to better understand the unique impact of the presence of worry on the outcome measures, separate from the effects of depression. A new dichotomous categorical variable was created, with patients who endorsed worry in one group (including the worry, subthreshold, and GAD groups) and patients who denied worry in the other group. This variable and a depression group variable, with patients who met criteria for MDD and those who did not, were included as independent variables and hypotheses re-examined. Age and ethnicity were included as covariates. Measures of human burden were examined first. The ANCOVA for perceived health showed significant effects for both worry and depression group, F(1, 304) = 4.62, p = .03, partial η2 = .02 and F (1, 304) = 11.42, p = .001, partial η2 = .04, respectively, with both the worried and depressed groups reporting poorer perceived health. Similar results were found for perceived stress, with significant effects for both worry and depression group, F(1, 304) = 20.94, p < .001, partial η2 = .07, and F(1, 304) = 9.56, p = .002, partial η2 = .03, and both symptomatic groups reported higher levels of stress. Binary logistic regressions were also conducted to examine effects of group membership on sleep trouble and social support. As before, ethnicity and age were entered in Block 1 and the worry and depression groups entered into Block 2. Block 2 was significant, χ2 (2, N = 329) = 39.80, p < .001, and Wald statistics for both worry and depression group were significant, W = 12.94, p < .001, and W = 4.18, p = .04. The logistic regression for social support showed that Block 2 failed to reach significance, although the Wald statistic for worry group was significant, W = 4.55, p = .03.
Follow up analyses for estimates of economic burden were conducted next, using the same method outlined above. Results showed no effect for worry or depression group for number of visits to the clinic in the last 90 days, F(1, 277) = 1.54, p = .06, partial η2 < .01, and F(1, 277) = .14, p = .71, partial η2 < .01, or physical health, F(1, 305) = .41, p = .52, η = .001, and F(1, 305) = 4.06, p = .05, η = .01. Results for number of medications showed significant effects for depression group, F(1, 279) = 5.06, p = .03, partial η 2 = .02, but not worry group, F(1, 279) = 1.67, p = .20, partial η 2 = .01, with the depressed group reporting more medications. The regression model for employment was significant, χ2 (5, N = 329) = 14.98, p = .01, but Block 2 failed to reach significance, χ2 (2, N = 329) = 88, p = .64
Discussion
The current study examined the impact of three severity levels of GAD on both human and economic burden measures in a medically underserved, primary care sample. Overall, our results suggest that subthreshold presentations of GAD, in and of themselves, are associated with significant impairment, primarily on measures of human burden. In addition, our results provide additional support for the finding that subthreshold and threshold presentations of GAD are common in primary care. This work builds on and extends previous work examining subclinical presentations of GAD and associated characteristics in primary care, with a particular emphasis on medically underserved groups who may be at greater risk for GAD.
Several important demographic differences emerged. Overall, worry and GAD symptoms were common in this sample. The symptomatic groups differed in terms of age and ethnicity, with the GAD group younger than the no worry and worry groups. Further, GAD was more common in European American individuals. These results are consistent with those of other studies showing higher prevalence of GAD in middle adulthood (Brenes, Knudson, McCall, Williamson, Miller, & Stanley, 2008; Kessler et al., 2005). Symptom groups did not differ by sex, education or marital status, in contrast to previous work (Ansseau, Fischler, Dierick, Albert, Leyman, & Mignon, 2008). Our findings are in line, however, with other work (Jones et al., 2001) that found that GAD groups were younger than individuals without a psychiatric diagnosis, but there were no differences in terms of income, gender, marital status, insurance status, or number of chronic illnesses. The sample used in the study by Jones et al. (2001) was comprised predominantly of low income, middle-aged, uninsured African American females and perhaps more similar to our sample than other primary care samples.
The hypothesis that the symptomatic groups would describe a greater human burden compared to those with no worry was generally supported. The presence of any GAD symptom was related to a significant decrease in perceived health. Each of the three symptomatic groups reported lower perceived health than the no worry group, although previous analyses revealed no significant difference between the groups on measures of physical health. Catastrophic thoughts associated with worry may contribute to this perception, as individuals who worry are perhaps more likely to generate negative thoughts about their own health and potentially worsening physical health in the future. Other work has shown that individuals with GAD in primary care are more likely to describe vague somatic illnesses (Wittchen, 2002). It may be that worry in the absences of GAD is also associated with such complaints, although no known work has investigated this. All three symptomatic groups also reported significantly higher perceptions of stress compared to the no worry group. Interestingly, the three symptomatic groups did not differ from one another and responses were comparable. GAD symptoms were also associated with sleep trouble, with all three symptomatic groups showing higher odds ratios compared to the nonworried group. Worry also was associated with the quality of perceived social support. Subthreshold GAD and worry were associated with a significant decrease in perceived social support, while GAD was not. This finding is partially in line with other work suggesting that individuals with GAD report a great deal of worry about interpersonal things and also describe greater severity of interpersonal problems (Eng & Heimberg, 2006; Roemer, Molina, & Borkovec, 1997). However, the finding that the presence of GAD did not significantly impact perceived social support is difficult to explain. It may be that a high level of worry interferes with accurate reporting of social support, as worried individuals likely spend a great deal of time internally focused on their worries. These individuals may not be as sensitive to interpersonal difficulties as those with lower levels of worry. Statistical power may have also limited our ability to detect such differences, if they exist. Future work examining this issue might consider incorporating an additional informant for more accurate data.
Our hypothesis that symptomatic groups would represent a greater economic burden compared to those with no worry was not supported. Of four measures of economic burden, groups differed only in number of medications, with the threshold and worried groups reporting more medications than the nonworried group. However, follow up analyses examining unique effects of worry and depression clarify this finding. Results suggest that this effect is more likely associated with depression or some of the shared characteristics of GAD and MDD, as the MDD factor was significant and the worry factor was not. The groups did not differ in employment status, number of visits to the clinic, or physical health. A failure to find significant differences between the GAD group and the nonworried group was especially surprising and contradictory to a large body of work (Hoffman et al., 2008; Leon et al., 1995; Massion et al., 1993; Roy-Byrne & Wagner, 2004). This could be specific to the medically underserved sample in the study, which included a large proportion of individuals living below the poverty level and/or a large population over the age of 65 years. In a sample of individuals mostly from low socioeconomic backgrounds with limited access to healthcare and generally poor health across all groups, variability on these measures may be low.
Follow up analyses including MDD group to examine effects specific to worry suggested that even after accounting for the effects of MDD, the worry group was associated with significant impairment on measures of human burden. The worry group was significantly related to perceived stress and health, difficulty sleeping, and perceived social support. However, as discussed previously, the depression group accounted for the findings associated with greater number of prescription medications.
Overall, our results suggest that GAD is associated with increased human burden and that this effect can be seen even at milder symptom levels. Results from this study suggest that the level of economic burden associated with subclinical presentations, however, is less severe. Worry group membership appeared to influence only number of medications, and follow up analyses examining the influence of depression suggest that this finding is due to comorbid depressive symptoms.
The current study suggests that subclinical presentations of GAD are associated with impairment in their own right. This is further underscored by data showing that subthreshold GAD may be a precursor to GAD (Rucci et al., 2003), and that physician recognition of subthreshold anxiety remains low (Pini et al., 1999). Our data indicate that worried and subthreshold individuals present with greater levels of impairment than non-worried individuals and on some variables (perceived health and stress) report levels comparable to that of those with GAD. As such, it may be worthwhile to treat subthreshold forms of the disorder to alleviate current symptoms and associated burden. To date, however, there are no known data on the treatment of subthreshold GAD. Future work might pursue this line of reasoning on a small scale to determine if such intervention approaches are effective for amelioration of symptoms as well as longitudinally for the prevention of GAD. Our results also indicate that worry and subclinical presentations of GAD are common in primary care. These findings are consistent with those of other work on subthreshold disorders (Pini et al., 1999; Rucci et al., 2003), and given the number of individuals at risk, further underscore the importance of early intervention and prevention.
The study has several limitations. First, the results of the study could be limited to a sample of this nature, specifically a sample of primarily unemployed, low income females from an urban area. Although it is informative to understand the impact of GAD in this sample, it is important to note that findings may not generalized to samples of higher SES or samples with a greater proportion of males. Second, the relatively small sample size of the subthreshold and GAD groups reduced power and may have limited our ability to detect other differences between groups. Third, the use of single item measures is not ideal from a psychometric standpoint. Although such measures have good clinical utility, measures with multiple items representing the constructs would be ideal. The use of the PRIME-MD as a diagnostic measure may also have influenced the findings. Using longer interviews or clinician determined diagnoses would have provided an additional measure of diagnostic groups and may have resulted in different diagnostic or symptom group classification. Additionally, others have noted that the PRIME-MD has a high risk for false positives (Boyer, Bsserbe, & Weller, 1998). Finally, the correlational nature of the study design precludes any causal conclusions. It could be that the differences found in human and economic burden lead to worry and GAD, or vice versa. Future longitudinal work could better address these issues and examine the temporal relationships of impairment, worry, and GAD.
References
American Psychiatric Association. (2000). Diagnostic and statistical manual of mental disorders (4th ed.). Washington, DC: Author. (text revision).
Andrews, V. H., & Borkovec, T. D. (1988). The differential effects of inductions of worry, somatic anxiety, and depression on emotional experience. Journal of Behavior Therapy and Experimental Psychiatry, 19, 21–26.
Ansseau, M., Fischler, B., Dierick, M., Albert, A., Leyman, S., & Mignon, A. (2008). Socioeconomic correlates of generalized anxiety disorder and major depression in primary care: The GADIS II study (generalized anxiety and depression impact survey II). Depression and Anxiety, 25, 506–513.
Ansseau, M., Fischler, B., Dierick, M., Mignon, A., & Leyman, S. (2005). Prevalence and impact of generalized anxiety disorder and major depression in primary care in Belgium and Luxemburg: The GADIS study. European Psychiatry, 20, 229–235.
Bakker, I. M., Terluin, B., van Marwjk, H. W., van Mechelen, W., & Stalmna, W. A. B. (2009). Test-retest reliability of the PRIME-MD: Limitations in diagnosing mental disorders in primary care. Eupropean Journal of Public Health, 19, 303–307.
Boyer, P., Bsserbe, J., & Weller, E. (1998). How efficient is a screener? A comparison of the PRIME-MD patient questionnaire with the SDDS-PC screen. International Journal of Methods in Psychiatric Research, 7, 27–32.
Brenes, G. A., Knudson, M., McCall, W. V., Williamson, J. D., Miller, M. E., & Stanley, M. A. (2008). Age and racial differences in the presentation and treatment of generalized anxiety disorder in primary care. Journal of Anxiety Disorders, 22, 1128–1136.
Carter, R. M., Wittchen, H. U., Pfister, H., & Kessler, R. C. (2001). One-year prevalence of subthreshold and threshold DSM-IV generalized anxiety disorder in a nationally representative sample. Depression and Anxiety, 13, 78–88.
De Gruy, F. V., & Pincus, H. A. (1996). The DSM-IV-PC: A manual for diagnosing mental disorders in the primary care setting. Journal of the American Board of Family Practice, 9, 271–281.
Eng, W., & Heimberg, R. G. (2006). Interpersonal correlates of generalized anxiety disorder: Self versus other perception. Journal of Anxiety Disorders, 20, 380–387.
Grant, B. F., Hasin, D. S., Stinson, F. S., Dawson, D. A., Ruan, W. J., Goldstein, R. B., et al. (2005). Prevalence, correlates, co-morbidity, and comparative disability of DSM-IV generalized anxiety disorder in the USA: Results from the national epidemiologic survey on alcohol and related conditions. Psychological Medicine: A Journal of Research in Psychiatry and the Allied Sciences, 35, 1747–1759.
Hoffman, D. L., Dukes, E. M., & Wittchen, H. U. (2008). Human and economic burden of generalized anxiety disorder. Depression and Anxiety, 25, 72–90.
Johnson, J., Weissman, M. M., & Klerman, G. L. (1992). Service utilization and social morbidity associated with depressive symptoms in the community. JAMA, 267, 1478–1483.
Jones, G. N., Ames, S. C., Jeffries, S. K., Scarinci, I. C., & Brantley, P. J. (2001). Utilization of medical services and quality of life among low-income patients with generalized anxiety disorder attending primary care clinics. International Journal of Psychiatry in Medicine, 31, 183–198.
Kessler, R. C., Chiu, W. T., Demler, O., & Walters, E. E. (2005). Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the national comorbidity survey replication. Archives of General Psychiatry, 62, 617–627.
Kessler, R. C., DuPont, R. L., Berglund, P., & Wittchen, H. U. (1999). Impairment in pure and comorbid generalized anxiety disorder and major depression at 12 months in two national surveys. American Journal of Psychiatry, 156, 1915–1923.
Leon, A. C., Portera, L., & Weissman, M. M. (1995). The social costs of anxiety disorders. British Journal of Psychiatry, 166, 19–22.
Loerch, B., Szegedi, A., Kohnen, R., & Benkert, O. (2000). The Primary Care Evaluation of Mental Disorders (PRIME-MD), German version: A comparison with the CIDI. Journal of Psychiatric Research, 34, 211–220.
Maier, W., Gänsicke, M., Freyberger, H. J., Linz, M., Heun, R., & Lecrubier, Y. (2000). Generalized anxiety disorder (ICD-10) in primary care from a cross-cultural perspective: A valid diagnostic entity? Acta Psychiatrica Scandinavica, 101, 29–36.
Marciniak, M. D., Lage, M. J., Dunayevich, E., Russell, J. M., Bowman, L., Landbloom, R. P., et al. (2005). The cost of treating anxiety: The medical and demographic correlates that impact total medical costs. Depression and Anxiety, 21, 178–184.
Massion, A. O., Warshaw, M. G., & Keller, M. B. (1993). Quality of life and psychiatric morbidity in panic disorder and generalized anxiety disorder. American Journal of Psychiatry, 150, 600–607.
Mennin, D. S., Heimberg, R. G., Fresco, D. M., & Ritter, M. R. (2008). Is generalized anxiety disorder an anxiety or mood disorder? Considering multiple factors as we ponder the fate of GAD. Depression and Anxiety, 25, 289–299.
Miller, G. A., & Chapman, J. P. (2001). Misunderstanding analyses of covariance. Journal of Abnormal Psychology, 110, 40–48.
Murray, C. J. L., & Lopez, A. D. (1996). The global burden of disease: A comprehensive assessment of mortality and disability from diseases, injuries, and risk factors in 1990 and projected to 2020. Cambridge: Harvard University Press.
Olfson, M. (2000). Impairment in generalized anxiety disorder. American Journal of Psychiatry, 157, 2060–2061.
Olfson, M., Broadband, E. W., Weissman, M. M., Leon, A. C., Farber, L., Hoven, C., et al. (1996). Subthreshold psychiatric symptoms in a primary care group practice. Archives of General Psychiatry, 53, 880–886.
Olfson, M., Fireman, B., Weissman, M., Leon, A. C., Sheehan, D. V., Kathol, R. G., et al. (1997). Mental disorders and disability among patients in a primary care group practice. American Journal of Psychiatry, 154, 1734–1740.
Olfson, M., & Gameroff, M. J. (2007). Generalized anxiety disorder, somatic pain and health care costs. General Hospital Psychiatry, 29, 310–316.
Pini, S., Perkonnig, A., Tansella, M., & Wittchen, H. U. (1999). Prevalence and 12-month outcome of threshold and subthreshold mental disorders in primary care. Journal of Affective Disorders, 56, 37–48.
Roemer, L., Molina, S., & Borkovec, T. D. (1997). An investigation of worry content among generally anxious individuals. Journal of Nervous and Mental Disease, 185, 314–319.
Roy-Byrne, P. P., & Wagner, A. (2004). Primary care perspectives on generalized anxiety disorder. Journal of Clinical Psychiatry, 65, 20–26.
Rucci, P., Gherardi, S., Tansella, M., Piccinelli, M., Berardi, D., Bisoffi, G., et al. (2003). Subthreshold psychiatric disorders in primary care: Prevalence and associated characteristics. Journal of Affective Disorders, 76, 171–181.
Spitzer, R. L., Williams, J. B. W., Kroenke, K., & Linzer, M. (1994). Utility of a new procedure for diagnosing mental disorders in primary care: The PRIME-MD 1000 study. JAMA, 272, 1749–1756.
Stein, M. B., & Heimberg, R. G. (2004). Well-being and life satisfaction in generalized anxiety disorder: Comparison to major depressive disorder in a community sample. Journal of Affective Disorders, 79(1), 161–166.
Wells, K. B., Burnham, M. A., Rogers, W., Hays, R., & Camp, P. (1992). The course of depression in adult outpatients. Archives of General Psychiatry, 489, 788–794.
Williams, R. B., Barefoot, H. C., Califf, R. M., Haney, T. L., Saunders, W. B., Pryor, D. B., et al. (1992). Prognostic importance of social and economic resources among medically under treated patients with angiographically documented coronary artery disease. JAMA, 267, 520–524.
Wittchen, H. U. (2002). Generalized anxiety disorder: Prevalence, burden, and cost to society. Depression and Anxiety, 16, 162–171.
Wittchen, H. U., & Hoyer, J. (2001). Generalized anxiety disorder: Nature and course. Journal of Clinical Psychiatry, 62, 15–19.
World Health Organization. (1990). Global burden of disease 1990 disability weights. Retrieved August 26, 2005, from http://www.who.int/healthinfo/bodreferencesdisabilityweights.xls .
Acknowledgment
This research was supported by a Health Resources and Services Administration, Department of Health and Human Services GPE Grant #1D40HP00001.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kertz, S.J., Woodruff-Borden, J. Human and Economic Burden of GAD, Subthreshold GAD, and Worry in a Primary Care Sample. J Clin Psychol Med Settings 18, 281–290 (2011). https://doi.org/10.1007/s10880-011-9248-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10880-011-9248-1