Abstract
Purpose
Splenectomy is associated with increased risk of overwhelming post-splenectomy infections despite proper anti-pneumococcal vaccination. As most studies concentrated on vaccination-induced humoral immunity, the cellular immune responses triggered in splenectomized patients are not yet well studied. The present study aims to investigate this area as it can contribute to the development of more effective vaccination strategies.
Methods
Five healthy and 14 splenectomized patients were vaccinated with pneumococcal conjugate polysaccharide vaccine (PCV) followed by pneumococcal polysaccharide vaccine according to the guidelines established by Advisory Committee on Immunization Practices. PBMC samples collected 0, 8, and 12 weeks after PCV immunization were in vitro stimulated with PCV. Levels of lymphoproliferation, TH cell differentiation, and cytokine release were assessed by carboxyfluorescein succinimidyl ester labeling, intracellular cytokine staining, and ELISA, respectively.
Results
While TH1-dominated immune response was detected in both groups, asplenic individuals generated significantly lower levels of TH1 cells following in vitro stimulation. Similarly, levels of IFN-γ, IL-4, and IL-17 release and lymphoproliferation were significantly lower in asplenic patients.
Conclusions
According to our data, splenectomy negatively influences the levels of PCV-induced lymphoproliferation, TH1 differentiation, and cytokine release. Besides, PCV failed to induce TH17-dominant immune response which is crucial for protection against extracellular pathogens.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Splenectomy is associated with increased risk of overwhelming post-splenectomy infection (OPSI), which is mainly caused by Streptococcus pneumoniae (50–90% of cases) [1, 2]. Two types of pneumococcal vaccines are currently recomended for protection: the 23-valent pneumococcal polysaccharide vaccine (PPV-23) which induces T cell-independent immune responses and 13-valent pneumococcal conjugate vaccines (PCV-13) which, because of their conjugated nature to a carrier protein, can induce T cell-dependent immune responses characterized by immunological memory, affinity maturation, and extensive antibody subclass switching [3]. Among those, for more than two decades, PPV-23 has been recommended for both immunocompromised individuals and the elderly people [4]. However, PPV-23-driven hyporesponsiveness [5, 6] provided further support for the idea that new PCV-13 + PPV-23 combined schedules should be recommended for individuals at risk since 2012 (Advisory Committee on Immunization Practices-ACIP-2012) [7].
As antibody-secreting B cells are thought to occupy a central role for the protection against encapsulated organisms, impairment of humoral response is considered the main cause for OPSI, and accordingly, most of the studies in literature concentrated on the vaccine-induced humoral immunity [8,9,10,11,12,13,14,15]. On the other hand, despite the fact that splenectomy was shown to influence unprimed T cells and/or their precursors by previous sudies [16, 17], vaccination-induced cellular immune responses in asplenic patients have not received enough attention.
Our aim in this study is to examine the effect of splenectomy on the levels of cell-mediated immune responses initiated against the anti-pneumococcal vaccination by measuring the levels of vaccine-specific PBMC proliferation; TH1, TH2, and TH17 subpopulations generated; and IFN-γ, IL-4, and IL-17 secreted. Our results can contribute to the development of more effective vaccination strategies in order to protect splenectomized individuals from OPSI, as it can affect even those with appropriate immunization [18,19,20].
Methods
Subjects and Vaccination
Fourteen splenectomized patients who were splenectomized in Hitit University Corum Training and Research Hospital in Corum province of Turkey and five healthy patients were enrolled in this study. This study was approved by the ethics committee of Numune Training and Research Hospital in Ankara/Turkey (E-14-285). After getting all patients’ informed consents, patients’ database (clinical history, reason for splenectomy, vaccination status) was obtained from the hospital information system. All patient and control subjects were white and Caucasian.
Vaccination Schedule
All participants were vaccinated according to the updated Advisory Committee on Immunization Practices guidelines that recommend combined schedule of PCV-13 (Pfizer, Lot No. 305010) followed by PPV-23 (Merck, Lot No. K0 10839) vaccination 8 weeks later [7]. All individuals were vaccinated subcutaneously with one dose of the PCV-13 containing 2.2 μg of capsular PS 1, 3, 4, 5, 6A, 7F, 9V, 14, 18C, 19A, 19F, 6B, and 23F serotypes and 32 μg of CRM197 (a nontoxic, single-amino acid mutant of diphtheria toxin). After 8 weeks, the same patients were subcutaneously vaccinated with PPV-23 containing 25 μg of each 1, 2, 3, 4, 5, 6B, 7F, 8, 9N, 9V, 10A, 11A, 12F, 14, 15B, 17F, 18C, 19F, 19A, 20, 22F, 23F, and 33F serotypes.
Collection of Blood Samples and Isolation of Peripherial Blood Mononuclear Cells
Blood samples (20 ml) were collected before vaccination, 8 weeks after PCV-13 vaccination (PCV-13) and 4 weeks after PPV-23 vaccination (PCV-13 + PPV-23). PBMCs were isolated from peripherial venous blood by lymphocyte separation medium histopaque (Genaxxon, C4754.0100) and suspended in RPMI 1640 medium supplemented with 10% fetal calf serum (FCS), 100 IU/ml penicillin and streptomycin, and L-glutamine.
Lymphocyte Proliferation Assay
Previously described protocol was followed for lymphocyte proliferation assay [21]. Briefly, 2 × 106 cells were labeled with 10 μM carboxyfluorescein succinimidyl ester (CFSE) (Biolegend, 423801) in 1× PBS. Cells were incubated at 37 °C for 30 min. Labeling process was terminated by the addition of cell culture media, after which cells were centrifuged at 300×g for 5 min. Cells were then suspended in 500-μl cell culture media, and 5 × 105 cells in 0.125-ml media was transferred onto 96-well plates. For all patients, the following treatments were performed:
-
Experimental group: anti-CD28 (2 μg/ml, Biolegend, 302933) + anti-CD49b (2 μg/ml, Biolegend, 359304) + PCV-13 (1:100).
-
Positive control: anti-CD28 (2 μg/ml) + anti-CD49b (2 μg/ml) + anti-CD3 (2 μg/ml).
-
Negative control: anti-CD28 (2 μg/ml) + anti-CD49b (2 μg/ml) but not with vaccine.
Cells were incubated with stimulants for 120 h, and CFSE positivity was analyzed with BD Accuri C6 flow cytometer.
Analysis of Vaccine-Specific TH1, TH2, and TH17 Subpopulations
TH1, TH2, and TH17 subpopulations were analyzed by following the protocol previously described [17, 22, 23]. PBMCs were diluted to 4 × 106 cells/ml, and 5 × 105 cells (in 0.125-ml media) were seeded into 96-well cell culture plate. For all patients, the following treatments were performed on PBMC samples collected:
-
Experimental group: anti-CD28 (2 μg/ml) + anti-CD49b (2 μg/ml) + PCV-13 (1:100).
-
Positive control: PMA (50 ng/ml) + ionomycin (1 μg/ml).
-
Negative control: anti-CD28 (2 μg/ml) + anti-CD49b (2 μg/ml) but not with vaccine.
For helper T cell analysis, cells were treated with brefeldin A (Biolegend, 420601) at 5 μg/ml concentration at 16th hour of incubation and then incubated for 6 h. After 24 h of incubation, cells were collected, fixed, permeabilized, and stained against CD4, IFN-γ, IL-4, and IL-17 by using Human Th1/Th2/Th17 Phenotyping Kit (BD Biosciences, 560751) by following the manufacturer’s guidelines. Cells were analyzed with BD Accuri C6 flow cytometer.
Analysis of Cytokine Secretion in Lymphocyte Culture Supernatants
For cytokine ELISA [24], cells were incubated with anti-CD28 (2 μg/ml), anti-CD49b (2 μg/ml), and PCV-13 (1:100) for 72 h. As positive control, PBMCs were stimulated with PMA (50 ng/ml) and ionomycin (1 μg/ml), while cells incubated with antibodies but not with vaccine were used as negative control. Supernatant was collected, and IFN-γ, IL-4, and IL-17 concentrations were measured with IFN-γ ELISA kit (Biolegend, 430104), IL-4 ELISA kit (Biolegend, 430304), and IL-17 ELISA kit (Biolegend, 433914), respectively, by following guidelines provided by the manufacturer.
Statistical Analysis
Descriptive statistics were calculated and provided throughout the text. Mean ± standard error of mean. Within group and between group comparisons were performed using two-way repeated measures analysis of variance test. Between group comparisons were adjusted for errors by using Sidak’s multiple comparisons test, while for within group comparisons, Tukey post hoc test was applied. Level of significance was accepted to be 0.05. All statistical analyses were performed, and graphs were drawn with GraphPad Prism (Version 7.00) software package.
Results
Characteristics of Study Groups
For all 14 splenectomized patients who were included in this study, the main reason for splenectomy was trauma. The study group consisted of 11 (79%) men and 3 (21%) women with a mean age of 37 ± 9.1 years (20–53 years). Mean weight and body mass index (BMI) were 74.8 ± 6.3 kg (64–80 kg) and 24.98 ± 2.02 kg/m2 (22.1–27.5 kg/m2), respectively. Mean time since splenectomy was 12.7 years, with a range of 3–36 years. All study individuals were healthy acccording to the physical examination and routine laboratory parameters. Control group included five individuals: two women and men men, with mean age 36 ± 9.7 years (25–48 years) who did not receive any pneumococcal vaccination before this study. Mean weight and BMI were 73.5 ± 7.12 kg (57–82 kg) and 23.81 ± 1.88 kg/m2 (19.8–27.3 kg/m2), respectively. There was no any acute illness or any other severe diseases detected in control groups.
Lymphocyte Proliferative Responses
In order to examine the effect of splenectomy on the anti-pneumococcal vaccination-induced cellular immune responses, at first, lymphoproliferative responses were compared. For this purpose, PBMC samples isolated from pre-vaccinated and post-vaccinated control and experiment groups were treated with PCV-13 in vitro. PCV-13 was chosen as the in vitro stimulant since PPV-23 is not able to induce cell-mediated immune responses [25].
In pre-vaccinated samples isolated from both groups, there was no any significant level of PCV-13-induced lymphocyte proliferation. This was reversed in the samples collected after PCV-13 vaccination and PPV-23 vaccination following the initial PCV-13 shot (PCV-13 + PPV-23). Removal of spleen seemed to have a negative impact on the lymphocyte proliferation as there is a significant reduction in the level observed in asplenic individuals (Fig. 1, Table 1).
Level of lymphoproliferation in response to PCV-13 treatment in vitro. PBMCs were collected 8 weeks following the initial PCV-13 vaccination (PCV-13) and 4 weeks after the second PPV-23 vaccination (PCV-13 + PPV-23) for both groups. Isolated PBMC samples were labeled with 10 μM CFSE and treated with anti-CD28, anti-CD49b, and PCV-13. For positive control, cells were stimulated with anti-CD3, anti-CD28, and anti-CD49b (data not shown). For negative control, cells were incubated anti-CD28 and anti-CD49b only (data not shown). The asterisks, and section signs signify significant differences against pre-vaccinated control and pre-vaccinated patient values (within group comparison), respectively. The dagger signifies significant difference between control and patient group values in pre-vaccinated, post-PCV-13-vaccinated and post-PCV-13 + PPV-23-vaccinated samples (between group comparison). *, §, † represent p < 0.05; **, §§, †† represent p < 0.01; ***, §§§, ††† represent p < 0.001; and ****, §§§§, †††† represent p < 0.0001
On the other hand, time since the cellular immune response activation by the first PCV-13 vaccination shot did not seem to influence the PCV-induced lymphoproliferation levels, since in both control and experiment groups, there was no any significant difference between the samples collected 8 weeks (PCV-13) and 12 weeks (PCV-13 + PPV-23) after the PCV-13 vaccination (Fig. 1, Table 1).
Vaccine-Specific TH1, TH2, and TH17 Subpopulations
The effect of spleen on the cell-mediated immunity was further investigated by monitoring the levels of CD4+ T cell subsets generated in response to PCV-13 stimulation in vitro. The subset levels were screened following the addition of brefeldin that is able to block the secretion of cytokines required for the detection of cell subsets by flow cytometry [22].
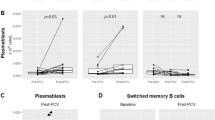
Pre-vaccinated samples from both groups did not generate any significant level of CD4+ T cell subsets monitored, following the PCV stimulation. In contrast, PBMCs collected from PCV-13 and PCV-13 + PPV-23-vaccinated individuals (from both groups) displayed enhanced levels of TH1 and TH17 cells, while TH1 cells were reported to be the dominant cell population (Fig. 2, Table 2). Spleen seems to influence the CD4+ T cell differentiation since significantly lower level of TH1 cell population was detected when PCV-13-vaccinated asplenic patient PBMCs were used for in vitro stimulation. However, this significant difference is lost in case of PCV-13 + PP23-vaccinated samples (Fig. 2a, Table 2 (A)).
The levels of CD4+ TH cell subsets—TH1 (a), TH2 (b), and TH17 (c)—induced by PCV-13 treatment in vitro. PBMCs were isolated from splenic and asplenic patients 8 weeks following the initial PCV-13 vaccination (PCV-13) and 4 weeks after the second PPV-23 vaccination (PCV-13 + PPV-23). Isolated PBMC samples were stimulated with anti-CD28, anti-CD49b, and PCV-13. For positive control, PBMCs were stimulated with PMA and ionomycin (data not shown), while cells incubated with antibodies but not with vaccine were used as negative control (data not shown). The asterisks and section signs signify significant differences against pre-vaccinated control and pre-vaccinated patient values (within group comparison), respectively. The dagger signifies significant difference between control and patient group values in pre-vaccinated, post-PCV-13-vaccinated, and post-PCV-13 + PPV-23-vaccinated samples (between group comparison). *, §, † represent p < 0.05; **, §§, †† represent p < 0.01; ***, §§§, ††† represent p < 0.001; and ****, §§§§, †††† represent p < 0.0001
On the other hand, in contrast to asplenic group, in which samples from both PCV-13 and PCV-13 + PPV-23 individuals showed significantly enhanced TH2 levels, this change was significiant only in PCV-13 + PPV-23-vaccinated samples for the control group (Fig. 2b, Table 2 (B)).
Vaccine-Specific IFN-γ, IL-4, and IL-17 Levels
Cytokines play a major role in adaptive immune responses by both influencing naive T cell differentiation into various CD4+ TH cell subsets and mediating downstream immunological T cell effector functions. Because of this dual role in T cell-mediated immune responses, cytokines can be categorized into groups depending on which TH cell-mediated immune response they are associated with. In our study, the effect of splenectomy on the PCV-13-mediated cellular immune response was further studied by monitoring the levels of IFN-γ (TH1), IL-4 (TH2), and IL-17 (TH17) cytokine release in response to PBMC stimulation by PCV-13 in vitro.
As with vaccine-specific lymphoproliferation and TH cell subset results above, there was no any significant level of cytokine release in response to PCV-13 stimulation of unvaccinated patient and control group PBMCs. PBMCs collected from asplenic individuals after PCV-13 and PCV-13 + PPV-23 vaccination displayed significantly reduced levels of IFN-γ, IL-4, and IL-17 cytokines in comparison to that from the control group (Fig. 3, Table 3). In accord with the vaccine-specific TH cell subset results above, IFN-γ (TH1) seemed to be the predominant cytokine induced by anti-pneumococcal vaccination, since the corrosponding levels were higher than those for IL-4 and IL-17 in the same serum samples used (Fig. 3, Table 3).
The levels of IFN-γ (a), IL-4 (b), and IL-17 (c) cytokine release induced by PCV-13 treatment in vitro. PBMCs were collected from both groups, 8 weeks following the initial PCV-13 vaccination (PCV-13) and 4 weeks after the second PPV-23 vaccination (PCV-13 + PPV-23). Isolated PBMC samples were incubated with anti-CD28, anti-CD49b, and PCV-13. As positive control, PBMCs were stimulated with PMA and ionomycin (data not shown). For negative control, cells were incubated with antibodies but not with vaccine (data not shown). ELISA kits are used to measure IFN-γ (a), IL-4 (b), and IL-17 (c) concentrations in the supernatants collected. The asterisks and section signs signify significant differences against pre-vaccinated control and pre-vaccinated patient values (within group comparison), respectively. The dagger signifies significant difference between control and patient group values in pre-vaccinated, post-PCV-13-vaccinated, and post-PCV-13 + PPV-23-vaccinated samples (between group comparison). *, §, † represent p < 0.05; **, §§, †† represent p < 0.01; ***, §§§, ††† represent p < 0.001; and ****, §§§§, †††† represent p < 0.0001
Furthermore, as observed in lymphoproliferative results, there was no any significant difference between the post-PCV-13 and post-PCV-13 + PPV-23 control/asplenic patient PBMCs in the cytokine levels detected (Fig. 3, Table 3).
Discussion
Splenectomy is associated with lifelong risk of pneumococcal infections which are the most common cause of OPSI syndrome [1, 2]. Today, ACIP recommends initial PCV-13 vaccination followed by immunization with PPV-23 8 weeks later [7]. The PCV vaccination is able to trigger T cell-mediated immune response characterized by immunological memory, affinity maturation, and extensive antibody subclass switching [3, 25, 26], while PPV-23 vaccination triggers exclusively humoral immunity [17, 27].
Individuals who have undergone post-traumatic splenectomy were previously reported to have negative effect on humoral and cellular branches of immunity [8, 9, 16, 28]. However, the effects on anti-pneumococcal vaccine-induced cell-mediated responses are not yet investigated. The current study aims to investigate the effect of splenectomy on the persistence and effectiveness of cellular immune responses triggered by the anti-pneumococcal vaccination, which fail to give optimum level of protection after splenectomy [18,19,20].
For the first time in literature, our results showed that splenectomy has a negative effect on the levels of lymphoproliferation, TH1 cell differentiation, and cytokine (IFN-γ, IL-4, and IL-17) release stimulated by PCV treatment in vitro. This is in correlation with a previous study by Balsalobre and Carbonell-Tatay that showed defective cutanous delayed hypersensitivity reaction in splenectomized patients [29].
Among the cytokines and CD4+ TH cell subsets investigated, IFN-γ and TH1 cells are known to provide protection especially against intracellular bacteria by eliciting macrophage activation, while IL-4 and TH2 cells are protective against extracellular parasites via humoral immune responses [30]. Together with ELISA results, flow cytometry analysis revealed that the PCV-13 vaccination induces TH1-dominant immune response which was negatively influenced by splenectomy. Having reduced TH1 cell and IFN-γ levels in aplenic patients is in correlation with another study by Kuranaga et al. that suggested spleen as an important organ for TH1 immune responses against bacterial infections [31].
On the other hand, IL-17, which was the other cytokine investigated, is considered to be essential for protection against extracellular pathogens, including those that can cause OPSI [32]. Accordingly, protective immunity against pneumococcal colonization was previously shown to be mediated by IL-17A production by TH17 cells [33, 34]. Furthermore, in contrast to IFN-γ and IL-4-deficient mice, animals lacking IL-17 receptor expression were not able to develop protection against pneumococci [30]. Therefore, we suggest that development of TH17, rather than TH1, dominant immune response-inducing vaccination strategies may provide a better protection for splenectomized patients.
One such strategy involves intranasal administration of polysaccharides with mucosal adjuvant which was previously shown to confer resistance against nasopharyngeal colonization by capsulated S. pneumoniae via CD4+ T cells and IL-17 activity [35]. Furthermore, quite recently, new protein candidates that provide complete protection from pneumococcal colonization via a TH17-mediated immune response has been identified [36]. As splenectomized patients can be considered as immunocompromised [37], and S. pneumoniae remain risk factors for invasive pneumococcal disease as long as they are colonized [38], reduction in bacterial colonization can have a vital role in conferring optimum level of protection against OPSI. Future studies correlating the bacterial colonization with the vaccination-induced IL-17 and TH17 levels can further help to enlighten this area of research.
Our results also showed that lymphoproliferation is negatively influenced by splenectomy. This together with ELISA and flow cytometry results suggests that, respectively, lower level of antigen-specific memory cells may be generated in asplenic patients since memory T cells were shown to be the predominant T cell responding to recall antigens in vitro [39, 40]. Further studies on the levels of memory cells generated upon vaccination in asplenic patients are still ongoing in our laboratory.
On the other hand, our data is in contrast to Wolf et al. which did not detect a significant difference in the level of recall antigen-mediated lymphoproliferation between splenic and asplenic patients [17]. The conflicting data can be explained, at least partially, by the differences in the methodology utilized. For instance, while 3H-thymidine incorporation assay was used to monitor lymphoproliferation by Wolf et al., in our work, CFSE staining was preferred. Among those, the former measures DNA synthesis during S phase, while the latter detects cells at the M phase of the cell cycle during which daughter cells are generated [41]. Since DNA synthesis can be triggered during processes independent of cell divison, such as gene duplication, repair, or apoptosis, 3H-thymidine incorporation assay measures the level of DNA synthesis and not of cell division [42]. Accordingly, CFSE staining was recently reported to be more sensitive for lymphocyte proliferation assays than 3H-thymidine incorporation [41].
Another important aspect investigated by our study is the effect of time since the initial PCV shot on the conjugated vaccine-induced cellular responses. For this purpose, PBMCs collected 4 weeks after PPV vaccination (i.e., 12 weeks after the PCV-13 immunization) were used, and detected responses were compared with that obtained from post-PCV-13 samples (i.e., 8 weeks after the PCV-13 immunization). PPV vaccination cannot boost any cellular immune response [17, 24], and therefore, cellular immune responses initiated by the PCV-13 vaccination are not affected by PPV vaccination in PCV-PPV samples.
Our results showed that there was no significant difference between splenic and asplenic patients in the levels of immune responses (i.e., lymphoproliferation, CD4+ TH subset differentiation, and cytokine release levels) detected 8 and 12 weeks after the initial PCV-13 vaccination. This was in correlation with a previous study showing increased level of lymphoproliferation and IFN-γ production 4 weeks following PCV vaccination that persists until week 24 [43].
The only exception was the TH1 cell levels. Even though the levels did not seem to significantly differ between week 8 and week 12 post-PCV vaccination in both control and asplenic patients, the significant difference that was observed between control and asplenic patients in post-PCV-vaccinated samples is lost in post-PCV + PPV samples. This can be due to the low sample numbers used, which is a limitation of our study. This can also explain why the difference in TH2 levels between unvaccinated and PCV-13-vaccinated samples did not reach the significant level, even though significantly high level of IL-4 was produced.
Conclusions
In conclusion, splenectomy negatively influences the anti-pneumococcal vaccine-induced immune responses including lymphocyte proliferation, CD4+ TH cell differentiation, and cytokine release. This may be as a result of reduced level of memory cells generated in asplenic patients following anti-pneumococcal vaccination, which is an area for further investigation. Our results also showed that PCV-13 vaccination induces TH1, rather than TH17, dominant immune response which is in general important for protection against rather intracellular microbes. Future vaccine development strategies to reverse splenectomy-associated effects and/or induce TH17-dominant immune responses may help to minimize risk of OPSI in asplenic individuals.
References
Holdsworth RJ, Irving AD, Cuschieri A. Postsplenectomy sepsis and its mortality rate: actual versus perceived risks. Br J Surg. 1991;78:1031–8. Available from: http://www.ncbi.nlm.nih.gov/pubmed/1933181
Di Sabatino A, Carsetti R, Corazza GR. Post-splenectomy and hyposplenic states. Lancet. 2011:86–97.
Mawas F, Feavers IM, Corbel MJ. Serotype of Streptococcus pneumoniae capsular polysaccharide can modify the Th1/Th2 cytokine profile and IgG subclass response to pneumococal-CRM197 conjugate vaccines in a murine model. Vaccine. 2000;19:1159–66.
Center for Disease Control and Prevention. Updated recommendations for prevention of invasive pneumococcal disease among adults using the 23-valent pneumococcal polysaccharide vaccine (PPSV23). MMWR Morb Mortal Wkly Rep. 2010;59:1102–6.
Huss A, Scott P, Stuck AE, Trotter C, Egger M. Efficacy of pneumococcal vaccination in adults: a meta-analysis. CMAJ. 2009;180:48–58.
Poolman J, Borrow R. Hyporesponsiveness and its clinical implications after vaccination with polysaccharide or glycoconjugate vaccines. Expert Rev Vaccines. 2011;10:307–22.
Report MW. Use of 13-valent pneumococcal conjugate vaccine and 23-valent pneumococcal polysaccharide vaccine for adults with immunocompromising conditions: recommendations of the advisory committee on immunization practices (ACIP). Am J Transplant. 2013;13:232–5.
Meerveld-Eggink A, de Weerdt O, van Velzen-Blad H, Biesma DH, Rijkers GT. Response to conjugate pneumococcal and Haemophilus influenzae type b vaccines in asplenic patients. Vaccine. 2011;29:675–80.
Stanford E, Print F, Falconer M, Lamden K, Ghebrehewet S, Phin N, et al. Immune response to pneumococcal conjugate vaccination in asplenic individuals. Hum Vaccin. 2009;5:85–91. Available from: http://www.ncbi.nlm.nih.gov/pubmed/18758242
Uslu A, Yetis H, Aykas A, Karagoz A, Dogan M, Simsek C, et al. The efficacy and immunogenecity of Pneumo-23 and ACT-HIB in patients undergoing splenectomy. Turkish J Trauma Emerg Surg. 2006;12:277–81.
Forstner C, Plefka S, Tobudic S, Winkler HM, Burgmann K, Burgmann H. Effectiveness and immunogenicity of pneumococcal vaccination in splenectomized and functionally asplenic patients. Vaccine. 2012;30:5449–52. doi:10.1016/j.vaccine.2012.06.048.
Hansen K, Singer DB. Asplenic-hyposplenic overwhelming sepsis: postsplenectomy sepsis revisited. Pediatr Dev Pathol. 2001:105–21.
Nived P, Jørgensen CS, Settergren B. Vaccination status and immune response to 13-valent pneumococcal conjugate vaccine in asplenic individuals. Vaccine. 2015;33:1688–94.
Issekutz A, Top K, McKelvie B, Issekutz T, Letenyi D, McCusker C. Fatal pneumococcal sepsis/meningitis in seven-year-old girl with IRAK-4 deficiency despite antibiotic prophylaxis and repeated pneumococcal vaccination. J Clin Immunol. 2012;32:S93. Available from: http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L71302027%5Cn. http://sfx.library.uu.nl/utrecht?sid=EMBASE&issn=02719142&id=doi:&atitle=Fatal+pneumococcal+sepsis%2Fmeningitis+in+seven-year-old+girl+with+IRAK-4+deficiency+despite+antib
Schutz K, Hughes RG, Parker A, Quinti I, Thon V, Cavaliere M, et al. Kinetics of IgM and IgA antibody response to 23-valent pneumococcal polysaccharide vaccination in healthy subjects. J Clin Immunol. 2013;33:288–96.
Karakantza M, Theodorou GL, Mouzaki A, Theodori E, Vagianos C, Maniatis A. In vitro study of the long-term effects of post-traumatic splenectomy on cellular immunity. Scand J Immunol. 2004;59:209–19.
Wolf HM, Eibl MM, Georgi E, Samstag A, Spatz M, Uranüs S, et al. Long-term decrease of CD4+CD45RA+ T cells and impaired primary immune response after post-traumatic splenectomy. Br J Haematol. 1999;107:55–68.
Cullingford GL, Watkins DN, Watts ADJ, Mallon DF. Severe late postsplenectomy infection. Br J Surg. 1991:716–21.
Waghorn DJ, Mayon-White RT. A study of 42 episodes of overwhelming post-splenectomy infection: is current guidance for asplenic individuals being followed? J Inf Secur. 1997;35:289–94.
Cameron PU, Jones P, Gorniak M, Dunster K, Paul E, Lewin S, et al. Splenectomy associated changes in IgM memory B cells in an adult spleen registry cohort. PLoS One. 2011;6.
Venken K, Thewissen M, Hellings N, Somers V, Hensen K, Rummens J-L, et al. A CFSE based assay for measuring CD4+CD25+ regulatory T cell mediated suppression of autoantigen specific and polyclonal T cell responses. J Immunol Methods. 2007;322(1–2):1–11.
Poccia F, Gioia C, Montesano C, Martini F, Horejsh D, Castilletti C, et al. Flow cytometry and T-cell response monitoring after smallpox vaccination. Emerg Infect Dis. 2003;9:1468–70. Available from: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=14718095
Hobeika AC, Morse MA, Osada T, Ghanayem M, Niedzwiecki D, Barrier R, et al. Enumerating antigen-specific T-cell responses in peripheral blood: a comparison of peptide MHC Tetramer, ELISpot, and intracellular cytokine analysis. J Immunother. 2005;28:63–72. Available from: http://eutils.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&id=15614046&retmode=ref&cmd=prlinks%5Cnpapers2://publication/uuid/B7F13126-EFFC-41C6-A345-F187D0C57E72 .
Zhang Y, Bliska JB. YopJ-promoted cytotoxicity and systemic colonization are associated with high levels of murine interleukin-18, gamma interferon, and neutrophils in a live vaccine model of Yersinia pseudotuberculosis infection. Infect Immun. 2010;78:2329–41.
Wuorimaa T, Kayhty H, Eskola J, Bloigu A, Leroy O, Surcel HM. Activation of cell-mediated immunity following immunization with pneumococcal conjugate or polysaccharide vaccine. Scand J Immunol. 2001;53:422–8.
Kamboj KK, Kirchner HL, Kimmel R, Greenspan NS, Schreiber JR. Significant variation in serotype-specific immunogenicity of the seven-valent Streptococcus pneumoniae capsular polysaccharide-CRM197 conjugate vaccine occurs despite vigorous T cell help induced by the carrier protein. J Infect Dis. 2003;187:1629–38.
Harding CV, Roof RW, Allen PM, Unanue ER. Effects of pH and polysaccharides on peptide binding to class II major histocompatibility complex molecules. Proc Natl Acad Sci U S A. 1991;88:2740–4. Available from: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=51314&tool=pmcentrez&rendertype=abstract
Müller C, Zielinski CC, Klepetko W, Knoflach P, Wolf HEM. Phenotypic and functional analysis of cellular cytotoxicity after splenectomy. Int Arch Allergy Appl Immunol. 1988;87:76–88.
Balsalobre C-T. Cellular immunity in splenectomized patients. J Investig Allergol Clin Immunol. 1991;1:235–8.
D’Elios MM, et al. T-cell response to bacterial agents. J Infect Dev Ctries. 2011;5:640–5. Available from: http://www.jidc.org/index.php/journal/article/view/21918304
Kuranaga N, Kinoshita M, Kawabata T, Shinomiya N, Seki S. A defective Th1 response of the spleen in the initial phase may explain why splenectomy helps prevent a Listeria infection. Clin Exp Immunol. 2005;140:11–21.
Onishi RM, Gaffen SL. Interleukin-17 and its target genes: mechanisms of interleukin-17 function in disease. Immunology. 2010:311–21.
Lu YJ, Gross J, Bogaert D, Finn A, Bagrade L, Zhang Q, et al. Interleukin-17A mediates acquired immunity to pneumococcal colonization. PLoS Pathog. 2008;4.
Hoe E, Boelsen LK, Toh ZQ, Sun GW, Koo GC, Balloch A, et al. Reduced IL-17A secretion is associated with high levels of pneumococcal nasopharyngeal carriage in Fijian children. PLoS One. 2015;10
Malley R, Srivastava A, Lipsitch M, Thompson CM, Watkins C, Tzianabos A, et al. Antibody-independent, interleukin-17A-mediated, cross-serotype immunity to pneumococci in mice immunized intranasally with the cell wall polysaccharide. Infect Immun. 2006;74:2187–95.
Moffitt KL, Gierahn TM, Lu YJ, Gouveia P, Alderson M, Flechtner JB, et al. TH17-based vaccine design for prevention of streptococcus pneumoniae colonization. Cell Host Microbe. 2011;9:158–65.
Jirillo E, Mastronardi ML, Altamura M, Munno I, Miniello S, Urgesi G, et al. The immunocompromised host: immune alterations in splenectomized patients and clinical implications. Curr Pharm Des. 2003;9:1918–23. Available from: http://www.ncbi.nlm.nih.gov/pubmed/12871175
Musher DM, Groover JE, Reichler MR, Riedo FX, Schwartz B, Watson DA, et al. Emergence of antibody to capsular polysaccharides of Streptococcus pneumoniae during outbreaks of pneumonia: association with nasopharyngeal colonization. Clin Infect Dis. 1997;24:441–6.
Sanders ME, Makgoba MW, Shaw S. Human naive and memory T cells: reinterpretation of helper-inducer and suppressor-inducer subsets. Immunol Today. 1988;9:195–9
Akbar AN, Salmon M, Janossy G. The synergy between naive and memory T cells during activation. Immunol Today. 1991;12(6):184–8.
Lašťovička J, Rataj M, Bartůňková J. Assessment of lymphocyte proliferation for diagnostic purpose: comparison of CFSE staining, Ki-67 expression and 3H-thymidine incorporation. Hum Immunol. 2016;77:1215–22. Available from: http://linkinghub.elsevier.com/retrieve/pii/S0198885916304360
Duque A, Rakic P. Different effects of BrdU and 3 H-thymidine incorporation into DNA on cell proliferation, position and fate. J Neurosci. 2011;31:997–1003.
Rabian C, Tschöpe I, Lesprit P, Katlama C, Molina J-M, Meynard J-L, et al. Cellular CD4 T cell responses to the diphtheria-derived carrier protein of conjugated pneumococcal vaccine and antibody response to pneumococcal vaccination in HIV-infected adults. Clin Infect Dis. 2010;50:1174–83.
Acknowledgements
We thank Thorvacs for the technical support and Hitit University Scientific Research Projects/Corum/Turkey for the financial funding (grant number 19001.15.001).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This study was approved by the ethics committee of Numune Training and Research Hospital in Ankara/Turkey (E-14-285).
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Karasartova, D., Gazi, U., Tosun, O. et al. Anti-Pneumococcal Vaccine-Induced Cellular Immune Responses in Post-Traumatic Splenectomized Individuals. J Clin Immunol 37, 388–396 (2017). https://doi.org/10.1007/s10875-017-0397-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10875-017-0397-3