Abstract
Purpose
Autosomal recessive deficiencies of DNMT3B or ZBTB24 account for two-thirds of cases of immunodeficiency, centromeric instability and facial dysmorphism (ICF syndrome). This primary immunodeficiency (PID) is characterized mainly by an antibody deficiency, facial abnormalities and centromeric instability. We analyzed the national cohort of patients with ICF syndrome with the aim of providing a more detailed description of the phenotype and management of patients with ICF syndrome.
Methods
Demographic, genetic, immunological, and clinical features were recorded for each patient.
Results
In the French cohort, seven of the nine patients carried DNMT3B mutations, six of which had never been described before. One patient had compound heterozygous ZBTB24 mutations. All patients were found to lack CD19+CD27+ memory B cells. This feature is a major diagnostic criterion for both ICF1 and ICF2. Patients suffered both bacterial and viral infections, and three patients developed bronchiectasis. Autoimmune manifestations (hepatitis, nephritis and thyroiditis) not previously reported in ICF1 patients were also detected in two of our ICF1 patients. The mode of treatment and outcome of the French patients are reported, by genetic defect, and compared with those for 68 previously reported ICF patients. Immunoglobulin (Ig) replacement treatment was administered to all nine French patients. One ICF1 patient presented severe autoimmune manifestations and pancytopenia and underwent allogeneic hematopoietic stem cell transplantation (HSCT), but she died from unknown causes 6 years post-transplant.
Conclusion
Autoimmune signs are uncommon in ICF syndrome, but, when present, they affect patient outcome and require immunosuppressive treatment. The long-term outcome of ICF patients has been improved by the combination of IgG replacement and antibiotic prophylaxis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The immunodeficiency-centromeric instability-facial anomalies (ICF) syndrome is a rare autosomal recessive (AR) disorder, first described in 1978 [1]. Most patients have mild facial anomalies and delayed developmental milestones, with various degrees of cognitive impairment. They present with recurrent infections due to profound panhypogammaglobulinemia, with no detectable impairment of immunoglobulin (Ig) class-switch recombination in vitro [2], a lack of memory (CD19+CD27+) B cells in peripheral blood and a variable cellular deficiency [3]. Only a limited number of studies have explored T-cell function in these patients, despite suggestive infections and evidence for T-cell abnormalities in mouse models of ICF [4]. Rearrangements of chromosome structure associated with DNA hypomethylation in the heterochromatic regions of chromosomes 1, 9 and 16 are a hallmark of this disease [5–8]. About 50 % of patients carry AR mutations of the DNA methyltransferase 3B (DNMT3B) gene and are considered to have ICF type 1 [9, 10]. These mutations mostly affect the catalytic activity of the enzyme, significantly modifying the DNA methylation landscape and, thus, the expression of many genes, including some critical for immune function and development [11]. AR ZBTB24 mutations have been found in almost 30 % of the remaining ICF patients. These patients are considered to have ICF type 2 [12]. ZBTB24 belongs to the zinc finger and BTB domain family of transcription factors, several of which are involved in various stages of B-cell differentiation [13, 14]. The function of ZBTB24 is unknown, but this protein has been localized to heterochromatin and may be involved in controlling heavily methylated regions [15]. Clinically, intellectual disabilities are the most marked signs in ICF2 patients, whereas antibody deficiency tends to be more pronounced in ICF1 patients [16]. More recently, ICF3 and ICF4 patients have been described with mutations in CDCA7 and HELLS, emphasizing the genetic heterogeneity of this syndrome [17].
Since 1978, up to 70 ICF patients have been reported in individual case reports, national or international series [1, 3, 12, 15, 16, 18–50]. However, the nature and severity of the infectious events, the impact of prophylaxis, age at diagnosis and clinical outcome remain poorly characterized. In the face of the heterogeneity of the features of ICF syndrome, we decided to carry out a thorough clinical, immunological and genetic description of the largest national cohort reported to date, comprising nine ICF patients included in the French registry (CEREDIH) for primary immune deficiencies. We also document the first described cases of autoimmune signs in ICF1 patients and highlight the impact of prophylaxis on the clinical outcome of the patients.
Methods
Patients and Clinical Definitions
The patients consulted at various French hospitals and were identified through the CEREDIH (Centre de Référence des Déficits Immunitaires Héréditaires) at Necker Children’s Hospital, Paris, France. The physicians caring for the patients completed a detailed questionnaire; clinical and biological data were collected from birth until August 2015. The median age of the cohort at the time of the study was 15 years (range: 8 months to 34 years). Approval for this study was obtained from the institutional review board of Necker Hospital and informed consent was obtained from all patients or their families (for minors), in accordance with the Helsinki Declaration (CNIL authorization: no. 908,256, October 14th, 2008).
Genetic Analysis
Genomic DNA was prepared from the blood samples of patients by the standard phenol-chloroform extraction method. The exons of DNMT3B and their flanking intron sequences were amplified by PCR with specific oligonucleotide primers (available on request) and sequenced with the Applied Biosystems Big Dye terminator kit v1.1 (AB Foster City California) and an ABI Prism 3130xl Analyzer (Applied Biosystems). PolyPhen-2 (polymorphism phenotyping) (http://genetics.bwh.harvard.edu/pph2/), a bioinformatics method for predicting the possible impact of an amino-acid substitution on the structure and function of a protein, was used to estimate the effect of the newly identified mutations. Mutations in ZBTB24 and CDCA7 were identified as described in [15, 51].
Immunological Investigations
Immunological investigations were based on those described in previous studies and/or the questionnaires sent to physicians [52, 53]. All antibody determinations were performed before Ig treatment. The normal ranges for lymphocyte numbers and Ig levels were determined from laboratory data [54].
Statistical Analysis
The data were analyzed with Microsoft Excel® and GraphPad Prism® software. When necessary, data were compared in Mann-Whitney tests. A p value <0.05 was considered significant.
Results
Epidemiologic Features of the Cohort
We studied nine ICF syndrome patients from eight kindreds (6 female and 3 male patients). All but two (P7 and P8) of the patients were alive at the time of reporting, after a median follow-up of 7.5 years. P6 is lost from follow-up. Five patients were born to consanguineous parents (Table 1).
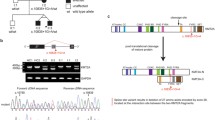
We identified AR mutations of DNMT3B in seven of the nine patients. We found homozygous DNMT3B mutations in four consanguineous kindreds, and compound heterozygote mutations in the other three patients. Five mutations were missense mutations (c.1747G > A, c.1964C > T, c.2162 T > C, c.2324C > T, c.2450 A > G) affecting amino acids located in the catalytic domain of the DNMT3B protein and were classified as “probably damaging” by polyPhen-2. Others were nonsense mutations (n = 2, c.C310T and c.158dupT) or splice-site mutations (n = 3, c.143-22del, c.1252 + 13 T-G and c.2302-212 T > C). A composite heterozygous mutation of ZBTB24 was described in P4 (c.A787T/980_981delGT) [15]. Patient P6 carried a homozygous mutation in CDCA7 (c.911G > A) [17]. The details are presented in Table 1.
The first clinical signs, mostly recurrent infections (n = 6) or a failure to thrive (n = 3), occurred at a median age of 4 months (range: 1 to 12 months). Hypogammaglobulinemia was diagnosed at a median age of 3.3 years (range: 2 months to 11 years), whereas the diagnosis of ICF on the basis of cytogenetic hallmarks occurred at a median age of 5.2 years (range: 1 month to 11.4 years). We assessed the typical facial anomalies in each patient, as reported at diagnosis. The following abnormalities were found: high forehead with frontal bossing (P3, 5 and 7), hypertelorism (P3, 5 and 7), epicanthus (P7 and P8), low-set ears (P3 and 7), macroglossia (P3 and 7). A few other abnormalities, including hyperpigmented spots (P5), macrocrania (P5), sparse hair (P5) and short limbs (P7), were also recorded. No dysmorphic features were reported for three patients at diagnosis and later during childhood (Table 1). Clinical examination revealed hypospadias in one ICF1 patient (P3). This malformation has already been reported in ICF patients [3].
Delayed Growth and Mental Retardation
Five (P1, 2, 6, 7 and 9) of the patients with adequate birth records had birth weights below the 10th percentile, and three patients (P2, P6 and P9) had birth heights below the 10th percentile. Eight patients displayed a failure to thrive, at a mean age of 4.5 months (range: 3 months to 10 years). One of these patients (P3) required growth hormone treatment and the failure to thrive of two other patients was related to chronic diarrhea. Gastrointestinal problems were common in our ICF patients (n = 6). For instance, P3 had two episodes of Salmonella sp. gastroenteritis requiring hospitalization and fluoroquinolone treatment before Ig replacement. Three patients had severe, protracted bouts of diarrhea (P6, P7 and P8) temporarily requiring parenteral nutrition. P7 developed chronic cholestasis and sub-occlusion, requiring treatment by jejunostomy. Another patient presented nodular gastritis and colon stenosis associated with an infiltration of CD3+ lymphocytes (P8). Finally, a gastroesophageal reflux was detected in four patients (P3, P4, P8 and P9). Five patients presented developmental delay. Four of these patients presented a slight cognitive and motor developmental delay in the first few years of life, but they subsequently displayed age-appropriate development and attended ordinary schools (Table 1). Only P4, who carries mutations of ZBTB24, displayed marked mental retardation requiring attendance at a specialized institution. Four of the patients in this series (P3, P4, P6 and P8) were highly sensitive or aggressive impairing the interpersonal relationship, notably the interactions with the healthcare team. Such symptoms may affect the patient care and the follow-up.
Infections
Infections, mostly respiratory infections (recurrent otitis, bronchitis) were a prominent clinical feature in eight patients, and three patients had bronchiectasis (Table 2). P9, the sister of P1, developed no infections, owing to early diagnosis [54], leading to early intravenous immunoglobulin (IVIgG) replacement. Diverse pathogens were responsible for the infections observed in these patients: bacteria (encapsulated or not, Table 2), viruses, fungi and parasites (Table 3).
Autoimmune and Immune-Mediated Manifestations in ICF1 Patients
Two patients (P3 and 8) with DNMT3B mutations developed severe autoimmune signs. P3 developed autoimmune hepatitis with high levels of alkaline phosphatase and gamma-glutamyl-transferase in the serum, but without detectable autoantibodies at the age of 12 years. Liver biopsy revealed a significant infiltration of the portal area by inflammatory cells, including a few macrophages and CD8+ T cells, in particular. Strikingly, flare-ups of the disease were marked by an increase in levels of CD8+CD45RA−CCR7− effector memory T cells in the peripheral blood. Since the age of 14 years, this patient has received immunosuppressive therapy combining tacrolimus and corticosteroids, followed by anti-CTLA4 agents and corticosteroids, leading to a partial control of hepatitis. He developed progressive renal failure at age 19. Renal biopsy showed massive interstitial infiltration by lymphocytes with the same phenotype as the liver infiltrate. At time of writing, P3 was undergoing pulsed steroids. Recently, such autoimmune phenomena were reported in an ICF2 patient [51]. P8 developed autoimmune thyroiditis with anti-thyroid peroxidase antibodies, at the age of 16 years. Of note, this patient showed other immune-mediated diseases as idiopathic psoriasis. She had psoriatic lesions at the age of 4 years and was initially treated with topical corticosteroids and then with retinoids, with a favorable outcome. This patient also displayed arthritis associated with synovitis. Neutrophils were abundant in the sterile synovial fluid and a synovial biopsy showed inflammatory lesions. The patient was treated with oral anti-inflammatory drugs, intra-articular steroids and a higher dose of IVIG, with beneficial effects. A non-septic arthritis has already been reported in ICF patient [22]. Finally, P8 experienced chronic anemia associated with thrombopenia, partially due to nodular regenerative hyperplasia. Because no other underlying cause was detected, including bone marrow investigations, these cytopenia have been linked to immune disorders.
Immunological and Hematological Investigations
We analyzed the peripheral blood B-cell populations of the nine patients. B-cell immunity was severely impaired in all patients, with an absence of CD27+ memory B cells (0.2 to 1 % of total B cells), contrasting with normal numbers of circulating B lymphocytes (Table 5, normal ranges from [55]). B-cell defects have been associated with hypogammaglobulinemia in ICF patients [2]. We therefore investigated B-cell function in vitro (n = 5, Table 4). B cells from all ICF1 patients tested showed a weak response to CD40 activation or no response at all, and an absence of Ig class-switch recombination. These features were not found in the ICF2 patient. Consistent with these findings, serum Ig levels were low for age in all ICF1 patients, whereas IgG levels were almost normal in the ICF2 patient. We assessed the production of immunoglobulins in vivo, by testing for antibodies against protein antigens after regular immunization (n = 5, Table 4). All of the patients displayed an absence of specific antibodies against recall antigens (Table 4).
CD4+ and CD8+ T-cell counts and percentage were normal in all but three of the patients (P3, P7 and P9; Table 5). Naive CD45RA+CD31+CD4+ T-cell counts were low in all patients, whereas naive CD8+ T-cell counts were normal in all but one patient (P3). T-cell function was assessed in vitro for eight patients. In all but one of these patients (P7), normal T-cell proliferation was observed in response to phytohemagglutinin (PHA) stimulation. By contrast, six patients displayed low levels of T-cell proliferation in response to antigens such as candidin and tetanus toxoid (P1, 3, 4, 5, 7 and 8).
Treatment and Outcome
All patients had been on polyvalent IgG replacement therapy since a mean age of 5 years (range: 3 months to 15 years) and antibacterial prophylaxis since a mean age of 4.1 years (range: 3 months to 11 years, Table 1). Prophylaxis greatly decreased the incidence of ENT and systemic infections, indeed only two systemic infections occurred in patients on IgG substitution: one case of sepsis (P2) and one of systemic CMV infection (P1) treated with ganciclovir. Attempts to decrease the dose of preventive treatment systematically resulted in a recurrence of ENT infections. For instance, P7 developed pneumonia when the interval between IgG infusions was increased. Physiotherapy helped to attenuate respiratory symptoms in two patients. All the ICF1 patients required iron supplementation due to iron-deficiency anemia. Such supplementation was not required for the ICF2 patient.
In this series, P8 was the only patient to undergo HSCT, to treat severe cytopenia and autoimmune signs. She received stem cells from a related HLA-matched donor at the age of 17, after conditioning with alemtuzumab, fludarabine and melphalan. Cyclosporine treatment was administered to prevent graft-versus-host-disease. Three months after HSCT, the rate of donor chimerism was almost 97 %, and IVIgG treatment was stopped 1 year later. However, severe refractory psoriasis recurred 2 years after HSCT, necessitating anti-TNF therapy; pancytopenia persisted (1160/mm3 neutrophils, 11 g/dl hemoglobin, 14,000/mm3 platelets). P8 died, of unknown causes, at the age of 22 years, 6 years after HSCT.
Discussion
We provide here a detailed description of the genetic, clinical and immunological features and outcomes of nine patients with ICF syndrome followed in France. We identified six previously unknown mutations of DNMT3B, all of which were predicted to decrease its methyltransferase activity. In mice, Dnmt3b knockout is lethal early in embryonic development [56], whereas hypomorphic mutations similar to those found in ICF1 patients lead to developmental defects at later stages [4, 57]. Consistent with these data, the only nonsense mutation identified here (c.310C > T) was heterozygous, as already reported for other ICF1 patients [19, 21, 35]. By contrast, most ICF2 patients harbor nonsense mutations. No relevant genotype-phenotype association could be established in ICF1 patients, but missense mutations in ICF2 patients were found to be correlated with higher serum Ig levels and lower frequencies of infection [15, 27]. Several clinical features also differed between ICF1 and ICF2 patients. First, the ICF1 patients tended to be diagnosed earlier than the ICF2 patients, probably due to the higher incidence of infections and slightly more severe hypogammaglobulinemia in ICF1 than in ICF2 patients. The roles of DNMT3B and ZBTB24 in antibody production have not yet been investigated in vivo.
Second, ICF2 patients suffer from more severe mental retardation than ICF1 patients: in our series, only the ICF2 patient required education at a specialized institution, and all but one of the other ICF2 patients reviewed displayed mild or severe mental retardation, whereas almost 70 % of the ICF1 patients were of normal intelligence. ZBTB transcription factors have been implicated in the differentiation of the hippocampal neurons playing a key role in cognition and memory [58, 59]. Studies of the contribution of ZBTB24 to neurogenesis may improve our understanding of the neurological signs in ICF2 patients.
We report here, for the first time, the occurrence of autoimmune and immune-mediated signs in ICF1 patients outside the context of HSCT [60] or granulomatous phenomena [51]. Consistent with these findings, longer CDR3 domains harboring larger numbers of positive charges, which have been associated with autoreactivity and autoimmune diseases, were found in ICF1 patients [2, 61–64]. This observation suggested that clonal deletion might be defective in ICF patients, leading to autoimmune signs [2]. However, B cells do not seem to play such a prominent role in ICF autoimmunity. First, autoimmunity appears to be uncommon in ICF syndrome, whereas B-cell deficiency is frequent in the various cohorts of ICF patients. Second, in our study, autoimmune hepatitis was linked to T-cell disorders with an absence of antibody detection, highlighting a possible role of cellular immunity. T-cells seem also involved in autoimmune signs previously reported in one ICF2 patient. Indeed, periportal CD8+ T-cells infiltrates were observed in repeated liver biopsies [51]. Autoimmune manifestations and inflammatory disorders in both ICF1 and ICF2 patients could reflect a break of T-cell tolerance or defects in regulatory T-cell populations [65, 66].
Our study also confirmed the absence of CD19+CD27+ memory B cells in ICF1 and ICF2 patients. The lack of long-lived memory B cells and plasma cells may result from a terminal B-cell differentiation block, activation or a survival defect in long-lived memory B cells. CD27 is widely associated with B-cell activation and differentiation, and low levels of CD27 expression, due to methylation defects, have been found in ICF lymphoblasts [11, 67–69]. The propensity of ICF B cells to undergo apoptosis in vitro is consistent with the hypothesis of a survival defect [2]. Moreover, it has been shown that the DNMT3B mutations underlying ICF lead to the apoptosis of murine thymocytes [4]. However, a deficiency of CD19+CD27+ memory B cells does not mean a total absence of memory B cells. It remains unknown whether CD27− memory B cells are present in ICF patients, but such cells have been identified in normal and pathological circumstances [70, 71].
We have described the therapeutic strategies and follow-up of the French ICF cohort. All patients received IgG substitution, which helped to decrease the rate of ENT and pulmonary infections. Indeed, IgG replacement is the mainstay for the treatment of antibody deficiencies [72]. In litterature, 18 ICF patients were reported to be on IgG treatment, and 16 of these patients experienced beneficial effects. ICF patients also presented an impairment of mucosal immunity, with low levels of IgA. Thus, IgG replacement does not prevent gastrointestinal manifestations, such as diarrhea [72, 73]. Two patients in our cohort (P7 and P8) suffered persistent diarrhea. Antibiotic prophylaxis was used in addition to IVIgG, in eight of our patients. By contrast to the findings for our cohort, only five of the other ICF patients reviewed were reported to be on antibiotic prophylaxis. Notwithstanding the lack of detail provided in publications relating to previous cases, this difference highlights heterogeneity in patient care and the need for practical guidelines. The early initiation of Ig infusions totally prevented infections in P9. We therefore propose new molecular markers, to facilitate early diagnosis [52]. Five ICF patients (including one from our cohort) have undergone HSCT, which may be the last resort in terms of treatment options. Pancytopenia persisted in our patient, and two other patients developed autoimmune signs after HSCT [60]. As three patients recovered and achieved immune reconstitution, HSCT may be considered for patients with disease uncontrolled patients on IVIgG and antibiotic prophylaxis.
Abbreviations
- AR:
-
autosomal recessive
- DNMT3B:
-
DNA methyltransferase 3B
- ENT:
-
ear-nose-throat
- HSCT:
-
hematopoietic stem cell transplantation
- ICF:
-
immunodeficiency, centromeric instability, facial anomalies
- IVIG:
-
intravenous immunoglobulin
- P:
-
patient
- PID:
-
primary immunodeficiency
References
Tiepolo L, Maraschio P, Gimelli G, Cuoco C, Gargani GF, Romano C Multibranched chromosomes 1, 9, and 16 in a patient with combined IgA and IgE deficiency. Hum Genet. 1979;51:127–37.
Blanco-Betancourt CE, Moncla A, Milili M, Jiang YL, Viegas-Pequignot EM, Roquelaure B, Thuret I, Schiff C Defective B-cell-negative selection and terminal differentiation in the ICF syndrome. Blood. 2004;103:2683–90.
Franceschini P, Martino S, Ciocchini M, Ciuti E, Vardeu MP, Guala A, Signorile F, Camerano P, Franceschini D, Tovo PA Variability of clinical and immunological phenotype in immunodeficiency-centromeric instability-facial anomalies syndrome. Report of two new patients and review of the literature. Eur J Pediatr. 1995;154:840–6.
Ueda Y, Okano M, Williams C, Chen T, Georgopoulos K, Li E Roles for Dnmt3b in mammalian development: a mouse model for the ICF syndrome. Development. 2006;133:1183–92.
Kondo T, Bobek MP, Kuick R, Lamb B, Zhu X, Narayan A, Bourc'his D, Viegas-Pequignot E, Ehrlich M, Hanash SM Whole-genome methylation scan in ICF syndrome: hypomethylation of non-satellite DNA repeats D4Z4 and NBL2. Hum Mol Genet. 2000;9:597–604.
Miniou P, Bourc'his D, Molina Gomes D, Jeanpierre M, Viegas-Pequignot E Undermethylation of Alu sequences in ICF syndrome: molecular and in situ analysis. Cytogenet Cell Genet. 1997;77:308–13.
Miniou P, Jeanpierre M, Bourc'his D, Coutinho Barbosa AC, Blanquet V, Viegas-Pequignot E alpha-satellite DNA methylation in normal individuals and in ICF patients: heterogeneous methylation of constitutive heterochromatin in adult and fetal tissues. Hum Genet. 1997;99:738–45.
Jeanpierre M, Turleau C, Aurias A, Prieur M, Ledeist F, Fischer A, Viegas-Pequignot E An embryonic-like methylation pattern of classical satellite DNA is observed in ICF syndrome. Hum Mol Genet. 1993;2:731–5.
Xu GL, Bestor TH, Bourc'his D, Hsieh CL, Tommerup N, Bugge M, Hulten M, Qu X, Russo JJ, Viegas-Pequignot E Chromosome instability and immunodeficiency syndrome caused by mutations in a DNA methyltransferase gene. Nature. 1999;402:187–91.
Jiang YL, Rigolet M, Bourc'his D, Nigon F, Bokesoy I, Fryns JP, Hulten M, Jonveaux P, Maraschio P, Megarbane A, et al. DNMT3B mutations and DNA methylation defect define two types of ICF syndrome. Hum Mutat. 2005;25:56–63.
Jin B, Tao Q, Peng J, Soo HM, Wu W, Ying J, Fields CR, Delmas AL, Liu X, Qiu J, et al. DNA methyltransferase 3B (DNMT3B) mutations in ICF syndrome lead to altered epigenetic modifications and aberrant expression of genes regulating development, neurogenesis and immune function. Hum Mol Genet. 2008;17:690–709.
de Greef JC, Wang J, Balog J, den Dunnen JT, Frants RR, Straasheijm KR, Aytekin C, van der Burg M, Duprez L, Ferster A, et al. Mutations in ZBTB24 are associated with immunodeficiency, centromeric instability, and facial anomalies syndrome type 2. Am J Hum Genet. 2011;88:796–804.
Yoon HS, Scharer CD, Majumder P, Davis CW, Butler R, Zinzow-Kramer W, Skountzou I, Koutsonanos DG, Ahmed R, Boss JM ZBTB32 is an early repressor of the CIITA and MHC class II gene expression during B cell differentiation to plasma cells. J Immunol. 2012;189:2393–403.
Dent AL, Shaffer AL, Yu X, Allman D, Staudt LM Control of inflammation, cytokine expression, and germinal center formation by BCL-6. Science. 1997;276:589–92.
Nitta H, Unoki M, Ichiyanagi K, Kosho T, Shigemura T, Takahashi H, Velasco G, Francastel C, Picard C, Kubota T, et al. Three novel ZBTB24 mutations identified in Japanese and Cape Verdean type 2 ICF syndrome patients. J Hum Genet. 2013;58:455–60.
Weemaes CM, van Tol MJ, Wang J, van Ostaijen-ten Dam MM, van Eggermond MC, Thijssen PE, Aytekin C, Brunetti-Pierri N, van der Burg M, Graham Davies E, et al. Heterogeneous clinical presentation in ICF syndrome: correlation with underlying gene defects. Eur J Hum Genet. 2013;21:1219–25.
Thijssen PE, Ito Y, Grillo G, Wang J, Velasco G, Nitta H, Unoki M, Yoshihara M, Suyama M, Sun Y, et al. Mutations in CDCA7 and HELLS cause immunodeficiency-centromeric instability-facial anomalies syndrome. Nat Commun. 2015;6:7870.
Brown DC, Grace E, Sumner AT, Edmunds AT, Ellis PM ICF syndrome (immunodeficiency, centromeric instability and facial anomalies): investigation of heterochromatin abnormalities and review of clinical outcome. Hum Genet. 1995;96:411–6.
Hagleitner MM, Lankester A, Maraschio P, Hulten M, Fryns JP, Schuetz C, Gimelli G, Davies EG, Gennery A, Belohradsky BH, et al. Clinical spectrum of immunodeficiency, centromeric instability and facial dysmorphism (ICF syndrome). J Med Genet. 2008;45:93–9.
Colucci M, Cocito L, Capello E, Mancardi GL, Serrati C, Cinque P, Schenone A Progressive multifocal leukoencephalopathy in an adult patient with ICF syndrome. J Neurol Sci. 2004;217:107–10.
Shirohzu H, Kubota T, Kumazawa A, Sado T, Chijiwa T, Inagaki K, Suetake I, Tajima S, Wakui K, Miki Y, et al. Three novel DNMT3B mutations in Japanese patients with ICF syndrome. Am J Med Genet. 2002;112:31–7.
Schuetz C, Barbi G, Barth TF, Hoenig M, Schulz A, Moeller P, Smeets D, de Greef JC, van der Maarel SM, Vogel W, et al. ICF syndrome: high variability of the chromosomal phenotype and association with classical Hodgkin lymphoma. Am J Med Genet A. 2007;143A:2052–7.
Kaya N, Al-Muhsen S, Al-Saud B, Al-Bakheet A, Colak D, Al-Ghonaium A, Al-Dhekri H, Al-Mousa H, Arnaout R, Al-Owain M, et al. ICF syndrome in Saudi Arabia: immunological, cytogenetic and molecular analysis. J Clin Immunol. 2011;31:245–52.
Kloeckener-Gruissem B, Betts DR, Zankl A, Berger W, Gungor T A new and a reclassified ICF patient without mutations in DNMT3B and its interacting proteins SUMO-1 and UBC9. Am J Med Genet A. 2005;136:31–7.
Pezzolo A, Prigione I, Chiesa S, Castellano E, Gimelli G, Pistoia V A novel case of immunodeficiency, centromeric instability, and facial anomalies (the ICF syndrome): immunologic and cytogenetic studies. Haematologica. 2002;87:329–31.
Bjorck EJ, Bui TH, Wijmenga C, Grandell U, Nordenskjold M Early prenatal diagnosis of the ICF syndrome. Prenat Diagn. 2000;20:828–31.
Cerbone M, Wang J, Van der Maarel SM, D'Amico A, D'Agostino A, Romano A, Brunetti-Pierri N Immunodeficiency, centromeric instability, facial anomalies (ICF) syndrome, due to ZBTB24 mutations, presenting with large cerebral cyst. Am J Med Genet A. 2012;158A:2043–6.
Chouery E, Abou-Ghoch J, Corbani S, El Ali N, Korban R, Salem N, Castro C, Klayme S, Azoury-Abou Rjeily M, Khoury-Matar R, et al. A novel deletion in ZBTB24 in a Lebanese family with immunodeficiency, centromeric instability, and facial anomalies syndrome type 2. Clin Genet. 2012;82:489–93.
De Ravel TJ, Deckers E, Alliet PL, Petit P, Fryns JP The ICF syndrome: new case and update. Genet Couns. 2001;12:379–85.
Gimelli G, Varone P, Pezzolo A, Lerone M, Pistoia V ICF syndrome with variable expression in sibs. J Med Genet. 1993;30:429–32.
Makay B, Anal O, Kose G, Bozkaya O, Ozer E, Bora E, Ulgenalp A, Ercal D Lymphoid tissue histology in a patient with ICF syndrome. J Investig Allergol Clin Immunol. 2012;22:220–1.
Maraschio P, Zuffardi O, Dalla Fior T, Tiepolo L Immunodeficiency, centromeric heterochromatin instability of chromosomes 1, 9, and 16, and facial anomalies: the ICF syndrome. J Med Genet. 1988;25:173–80.
Rigolet M, Gregoire A, Lefort G, Blanchet P, Courbes C, Rodiere M, Sarda P, Viegas-Pequignot E Early prenatal diagnosis of ICF syndrome by mutation detection. Prenat Diagn. 2007;27:1075–8.
Sawyer JR, Swanson CM, Wheeler G, Cunniff C Chromosome instability in ICF syndrome: formation of micronuclei from multibranched chromosomes 1 demonstrated by fluorescence in situ hybridization. Am J Med Genet. 1995;56:203–9.
Schuffenhauer S, Bartsch O, Stumm M, Buchholz T, Petropoulou T, Kraft S, Belohradsky B, Hinkel GK, Meitinger T, Wegner RD DNA, FISH and complementation studies in ICF syndrome: DNA hypomethylation of repetitive and single copy loci and evidence for a trans acting factor. Hum Genet. 1995;96:562–71.
Reisli I, Yildirim MS, Koksal Y, Avunduk MC, Acar A A case with ICF syndrome lost to rubella pneumonitis. Turk J Pediatr. 2005;47:85–8.
van den Brand M, Flucke UE, Bult P, Weemaes CM, van Deuren M Angiosarcoma in a patient with immunodeficiency, centromeric region instability, facial anomalies (ICF) syndrome. Am J Med Genet A. 2011;155A:622–5.
Kieback P, Wendisch H, Lorenz P, Hinkel K ICF syndrome. Immunodeficiency, chromosomal centromere instability, facial anomalies. Case report and literature review. Monatsschr Kinderheilkd. 1992;140:91–4.
Kubota T, Furuumi H, Kamoda T, Iwasaki N, Tobita N, Fujiwara N, Goto Y, Matsui A, Sasaki H, Kajii T ICF syndrome in a girl with DNA hypomethylation but without detectable DNMT3B mutation. Am J Med Genet A. 2004;129A:290–3.
Smeets DF, Moog U, Weemaes CM, Vaes-Peeters G, Merkx GF, Niehof JP, Hamers G ICF syndrome: a new case and review of the literature. Hum Genet. 1994;94:240–6.
Turleau C, Cabanis MO, Girault D, Ledeist F, Mettey R, Puissant H, Prieur M, de Grouchy J Multibranched chromosomes in the ICF syndrome: immunodeficiency, centromeric instability, and facial anomalies. Am J Med Genet. 1989;32:420–4.
Valkova G, Ghenev E, Tzancheva M Centromeric instability of chromosomes 1, 9 and 16 with variable immune deficiency. Support of a new syndrome. Clin Genet. 1987;31:119–24.
Fasth A, Forestier E, Holmberg E, Holmgren G, Nordenson I, Soderstrom T, Wahlstrom J Fragility of the centromeric region of chromosome 1 associated with combined immunodeficiency in siblings. A recessively inherited entity? Acta Paediatr Scand. 1990;79:605–12.
Tauris P, Hansen PW Functional studies on lymphocytes from two siblings with congenital hypogammaglobulinaemia. Scand J Haematol. 1983;30:117–24.
Ostergaard PA A girl with recurrent infections, low IgM and an abnormal chromosome number 1. Acta Paediatr Scand. 1973;62:211–5.
Carpenter NJ, Filipovich A, Blaese RM, Carey TL, Berkel AI Variable immunodeficiency with abnormal condensation of the heterochromatin of chromosomes 1, 9, and 16. J Pediatr. 1988;112:757–60.
Fryns JP, Azou M, Jaeken J, Eggermont E, Pedersen JC, Van den Berghe H Centromeric instability of chromosomes 1, 9, and 16 associated with combined immunodeficiency. Hum Genet. 1981;57:108–10.
Howard PJ, Lewis IJ, Harris F, Walker S Centromeric instability of chromosomes 1 and 16 with variable immune deficiency: a new syndrome. Clin Genet. 1985;27:501–5.
Wijmenga C, van den Heuvel LP, Strengman E, Luyten JA, van der Burgt IJ, de Groot R, Smeets DF, Draaisma JM, van Dongen JJ, De Abreu RA, et al. Localization of the ICF syndrome to chromosome 20 by homozygosity mapping. Am J Hum Genet. 1998;63:803–9.
Andre N, Roquelaure B, Caillez M, Chrestian M, Moncla A, Blanco-Betancourt C, Schiff C Macrophage activation syndrome mimicking life-threatening infection in a patient with variable immunodeficiency, centromeric instability, and facial anomalies. Pediatrics. 2004;114:1127.
von Bernuth H, Ravindran E, Du H, Frohler S, Strehl K, Kramer N, Issa-Jahns L, Amulic B, Ninnemann O, Xiao MS, et al. Combined immunodeficiency develops with age in Immunodeficiency-centromeric instability-facial anomalies syndrome 2 (ICF2). Orphanet J Rare Dis. 2014;9:116.
Chandesris MO, Melki I, Natividad A, Puel A, Fieschi C, Yun L, Thumerelle C, Oksenhendler E, Boutboul D, Thomas C, et al. Autosomal dominant STAT3 deficiency and hyper-IgE syndrome: molecular, cellular, and clinical features from a French national survey. Medicine (Baltimore). 2012;91:e1–19.
Gardes P, Forveille M, Alyanakian MA, Aucouturier P, Ilencikova D, Leroux D, Rahner N, Mazerolles F, Fischer A, Kracker S, et al. Human MSH6 deficiency is associated with impaired antibody maturation. J Immunol. 2012;188:2023–9.
Velasco G, Walton EL, Sterlin D, Hedouin S, Nitta H, Ito Y, Fouyssac F, Megarbane A, Sasaki H, Picard C, et al. Germline genes hypomethylation and expression define a molecular signature in peripheral blood of ICF patients: implications for diagnosis and etiology. Orphanet J Rare Dis. 2014;9:56.
Duchamp M, Sterlin D, Diabate A, Uring-Lambert B, Guerin-El Khourouj V, Le Mauff B, Monnier D, Malcus C, Labalette M, Picard C B-cell subpopulations in children: National reference values. Immun Inflammation Dis. 2014;2:131–40.
Okano M, Bell DW, Haber DA, Li E DNA methyltransferases Dnmt3a and Dnmt3b are essential for de novo methylation and mammalian development. Cell. 1999;99:247–57.
Velasco G, Hube F, Rollin J, Neuillet D, Philippe C, Bouzinba-Segard H, Galvani A, Viegas-Pequignot E, Francastel C Dnmt3b recruitment through E2F6 transcriptional repressor mediates germ-line gene silencing in murine somatic tissues. Proc Natl Acad Sci U S A. 2010;107:9281–6.
Nielsen JV, Thomassen M, Mollgard K, Noraberg J, Jensen NA Zbtb20 defines a hippocampal neuronal identity through direct repression of genes that control projection neuron development in the isocortex. Cereb Cortex. 2014;24:1216–29.
Mitchelmore C, Kjaerulff KM, Pedersen HC, Nielsen JV, Rasmussen TE, Fisker MF, Finsen B, Pedersen KM, Jensen NA Characterization of two novel nuclear BTB/POZ domain zinc finger isoforms. Association with differentiation of hippocampal neurons, cerebellar granule cells, and macroglia. J Biol Chem. 2002;277:7598–609.
Gennery AR, Slatter MA, Bredius RG, Hagleitner MM, Weemaes C, Cant AJ, Lankester AC Hematopoietic stem cell transplantation corrects the immunologic abnormalities associated with immunodeficiency-centromeric instability-facial dysmorphism syndrome. Pediatrics. 2007;120:e1341–4.
Crouzier R, Martin T, Pasquali JL Heavy chain variable region, light chain variable region, and heavy chain CDR3 influences on the mono- and polyreactivity and on the affinity of human monoclonal rheumatoid factors. J Immunol. 1995;154:4526–35.
Bas S, Djavad N, Schwager J, Vischer T, Roosnek E Relation between the heavy chain complementarity region 3 characteristics and rheumatoid factor binding properties. Autoimmunity. 1998;27:191–9.
Henry-Bonami RA, Williams JM, Rachakonda AB, Karamali M, Kendall PL, Thomas JW B lymphocyte “original sin” in the bone marrow enhances islet autoreactivity in type 1 diabetes-prone nonobese diabetic mice. J Immunol. 2013;190:5992–6003.
Cho MJ, Lo AS, Mao X, Nagler AR, Ellebrecht CT, Mukherjee EM, Hammers CM, Choi EJ, Sharma PM, Uduman M, et al. Shared VH1-46 gene usage by pemphigus vulgaris autoantibodies indicates common humoral immune responses among patients. Nat Commun. 2014;5:4167.
Carneiro-Sampaio M, Coutinho A Early-onset autoimmune disease as a manifestation of primary immunodeficiency. Front Immunol. 2015;6:185.
Baroudjian B, Viguier M, Battistella M, Beneton N, Pages C, Gener G, Begon E, Bachelez H Psoriasis associated with idiopathic CD4+ T-cell lymphopenia: a regulatory T-cell defect? Br J Dermatol. 2014;171:186–9.
Tangye SG, Liu YJ, Aversa G, Phillips JH, de Vries JE Identification of functional human splenic memory B cells by expression of CD148 and CD27. J Exp Med. 1998;188:1691–703.
Klein U, Rajewsky K, Kuppers R Human immunoglobulin (Ig)M + IgD+ peripheral blood B cells expressing the CD27 cell surface antigen carry somatically mutated variable region genes: CD27 as a general marker for somatically mutated (memory) B cells. J Exp Med. 1998;188:1679–89.
Ehrlich M, Sanchez C, Shao C, Nishiyama R, Kehrl J, Kuick R, Kubota T, Hanash SM ICF, an immunodeficiency syndrome: DNA methyltransferase 3B involvement, chromosome anomalies, and gene dysregulation. Autoimmunity. 2008;41:253–71.
Fecteau JF, Cote G, Neron S A new memory CD27-IgG+ B cell population in peripheral blood expressing VH genes with low frequency of somatic mutation. J Immunol. 2006;177:3728–36.
Wirths S, Lanzavecchia A ABCB1 transporter discriminates human resting naive B cells from cycling transitional and memory B cells. Eur J Immunol. 2005;35:3433–41.
Cunningham-Rundles C Key aspects for successful immunoglobulin therapy of primary immunodeficiencies. Clin Exp Immunol. 2011;164(Suppl 2):16–9.
Oksenhendler E, Gerard L, Fieschi C, Malphettes M, Mouillot G, Jaussaud R, Viallard JF, Gardembas M, Galicier L, Schleinitz N, et al. Infections in 252 patients with common variable immunodeficiency. Clin Infect Dis. 2008;46:1547–54.
Acknowledgments
We thank the patients and their families for participating in this study. We also thank the technicians and physicians of the CEREDIH network.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sterlin, D., Velasco, G., Moshous, D. et al. Genetic, Cellular and Clinical Features of ICF Syndrome: a French National Survey. J Clin Immunol 36, 149–159 (2016). https://doi.org/10.1007/s10875-016-0240-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10875-016-0240-2