Abstract
Background
Busulfan treatment as a chemotherapeutic agent has been considered an alternative approach in xenograft model because it offers a simple, convenient, effective, and less toxic conditioning regimen.
Objective and methods
To investigate busulfan effects on the reconstitution of human immune cells and the generation of immune response to foreign antigens, we generated humanized NOD/SCID/IL-2Rγnull (NSG) mice conditioned either busulfan or total body irradiation (TBI) with hCD34+ CB cells.
Results
Busulfan resulted in a high survival rate and effective reconstitution of human immune cells including B, T, macrophage, and dendritic cells in humanized NSG mice, compared to that of TBI. Moreover, the humanized NSG mice conditioned busulfan showed effective B cell development and thereby the high production of human antibody against immunized antigen.
Conclusion
Humanized mice conditioned by busulfan provide a powerful and versatile tool for studying the entire process of human B-lymphocyte development and for producing specific human antibodies
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Humanized mice are considered a valuable tool for developing new therapeutics and for studying human immune responses to pathogen infections, as well as the development of human immune cells, etc. [1–5]. More than 20 years after the first successful engraftment of human leukocytes and hematopoietic organs in mice [6], many different humanized mice have been reported and used for a variety of purposes. A number of modified severe combined immunodeficient (SCID) models have been proposed for reconstitution of human immune cells [7]. Additionally, T and B cell-deficient Prkdc scid and recombination activating gene Rag1−/− and Rag2−/− mutant mice have been used as recipients in xenotransplantation [8–10]. However, these models exhibit low efficacy in engraftment levels because of the remaining innate immunity of the host animals. Nonobese diabetic/SCID (NOD/SCID) mice harboring either a null allele at the β2-microglobulin gene (NOD/SCID/β2 m−/−) or a truncated common cytokine receptor γ chain (γc) lacking its cytoplasmic region (NOD/SCID/γ −/−c ) were recently developed and used in the generation of humanized mice [11–13]. To further optimize humanized mice for clinical applications in biomedical research, several important issues, such as the hematopoietic stem cell (HSC) source, cell dose, and graft composition, should be considered.
Another important issue is to generate preconditioned mice before transplantation of HSC. This might be critical to achieve high-level, efficient human cell engraftment in the xenograft model. Total body irradiation (TBI) has been used extensively in xenograft research, including in humanized mice [14–16]. However, there are several problems with this method; for example, the high mortality and care of animals following TBI absolutely requires autoclaved cages and chow, antibiotic administration, high-efficiency particulate air-filtered airflow, and pathogen-free conditions when handling the animals. These clinical and scientific hurdles must be overcome in order to use the xenograft model in biomedical research. The use of chemotherapeutic agents such as busulfan has therefore been considered an alternative approach because it offers a simple, convenient, effective, and less toxic conditioning regimen [17–20]. A recent study showed that busulfan can induce efficient human cell engraftment in NOD/LtSz-Scid/IL2Rγnull (NOD/SCID/IL-2Rγnull, NSG) mice [21]. However, several important issues about the reconstitution of human immune cells and the functional capacity for foreign antigens have not been fully evaluated.
In this study, we show that busulfan induces effective reconstitution of human immune cells in humanized NSG mice. Additionally, the humanized mice conditioned with busulfan exhibit the ability to produce T-dependent antigen-specific antibody against immunized dinitrophenol–keyhole limpet hemocyanin (DNP-KLH) compared to TBI-induced humanized mice. Interestingly, pregerminal center, germinal center, and memory B cells, which are phenotypically represented by hCD19+hCD38+hIgD+, hCD19+hCD38+hIgD−, and hCD19+hCD38−hIgD+hIgM+hCD27+, respectively [22–24], were markedly more abundant in humanized mice. Taken together, the data strongly demonstrate that treatment with busulfan might be a very useful tool for studying the entire process of human B-lymphocyte development and the production of specific human antibodies.
Methods
Mice
NOD.Cg-Prkdc scid Il2rg tm1Wjl/SzJ (NSG) mice were obtained from the Jackson Laboratory (Bar Harbor, ME, USA). All mice were maintained under specific pathogen-free conditions in accordance with ethical guidelines for the care of these mice at the Laboratory Animal Research Center of the Samsung Biomedical Research Institute in Seoul, South Korea. Mice were 6 weeks old at the time of transplant.
Isolation of Human CD34+ Cells from Cord Blood
Human cord blood (hCB) samples were acquired from normal full-term deliveries after obtaining informed parental consent according to guidelines established by the Samsung Medical Center, Seoul, South Korea. Mononuclear cells (MNCs) were isolated from hCB using Ficoll-Hypaque density gradient centrifugation, and then hCD34+ cells were purified further by positive selection using the MACS human CD34 MicroBead Kit (Miltenyi Biotec, GlodBach, Germany) and autoMACS™ Cell Separator (Miltenyi Biotec) according to the manufacturer’s instructions. The purity of hCD34+ cells was estimated by flow cytometry analysis using antibodies specific for hLin, hCD34, and hCD38 molecules (hLin: anti-human lineage cocktail 1, BD, CA, USA; hCD34: BD Pharmingen™, CA, USA; hCD38: eBioscience, San Diego, CA, USA). hLin−CD34+CD38− cells were used in this study and the purity was over 95%.
Pretreatment with Busulfan or Irradiation and Transplantation of hCD34+ CB Cells
Busulfex (busulfan, Ben Benue Laboratories, Inc., Bedford, OH, USA) was dissolved in dimethyl sulfoxide (Sigma Chemical Co., St. Louis, MO, USA) and diluted with 0.9% saline. The liquid busulfan solution was intraperitoneally injected into NSG mice at various doses (20, 30, and 40 mg/kg body weight) in a total volume of 250 μl. Another NSG group was whole-body irradiated with 2.4 Gy for comparison with busulfan-treated mice. The next day, hCD34+ cells (1 × 105 in 100 μl phosphate-buffered saline (PBS)) purified from hCB were transplanted intravenously into the NSG mice via the tail vein.
Assessment of Survival Rate in Humanized NSG Mice
Humanized NSG (hu-NSG) mice were monitored every 2 weeks. Moribund or dead mice were counted and the survival ratio was calculated as a percentage.
Flow Cytometric Analysis
After hCD34+ CB cell transplantation, peripheral blood (PB) was collected from tail vein at 4-week intervals and treated with 1× RBC Lysis Buffer (eBioscience, San Diego, CA, USA) according to the manufacturer’s instructions. At 24 weeks after transplantation, all hu-NSG mice were sacrificed and the spleen, bone marrow, lymph node, and PB cells were collected. Cells were prepared from the samples and suspended in 1× PBS (HyClone, South Logan, UT, USA) containing 2 mM ethylenediaminetetraacetic acid (Sigma) and 2% fetal bovine serum (Hyclone). For flow cytometric analysis, the following human-specific monoclonal antibodies were used: CD3-, CD4-, CD45-, CD138-, and IgD-fluorescein isothiocyanate conjugates; CD11c-, CD19-, CD27-, and CD56-phycoerythrin (PE) conjugates; CD3-, CD19-, CD20-, and CD45-peridinin chlorophyll protein-cyanine (Cy)5.5 conjugates; CD3-, CD11b-, CD20-, and CD38-PE-Cy7 conjugates; CD8α-, CD14-, CD19-, and IgM-allophycocyanin conjugates from eBioscience. The cells (0.1 to 1 × 106 cells) were stained with appropriate antibodies in 100 μl of 1× PBS containing 0.2% bovine serum albumin (BSA; Invitrogen, Carlsbad, CA, USA) and 0.05% sodium azide for 30 min on ice. Stained cells were analyzed on FACSAria (BD Biosciences, San Jose, CA, USA). Ten thousand to million events were acquired per sample and analyzed by the Flow-jo™ 8.3 flow cytometry analysis program (Tree-star, Ashland, OR, USA) and FACSDiva (BD Biosciences, San Jose, CA, USA).
Histological Analysis
At 24 weeks after transplantation, hu-NSG mouse spleen and mesenteric lymph node were embedded in paraffin. The paraffin-embedded tissue sections were stained with hematoxylin and eosin (H&E). Dual immunohistochemical staining was performed on 4-μm tissue sections fixed on slide glass after deparaffinization with xylene and rehydration with ethanol. Antigen epitope retrieval was performed by heating in 0.01 M citrate buffer (pH 6.0) in the microwave for 20 min and cooling at room temperature. Endogenous peroxidase was inhibited with 8% H2O2 in 1× PBS for 30 min at room temperature. The slides were washed with 1× Tris-buffered saline (TBS) containing 0.1% Tween-20 and bound with the following primary antibodies: monoclonal mouse anti-human CD11c (5D11; Leica Microsystems, UK), monoclonal mouse anti-human CD20cy antibody (L26; DAKO, Glostrup, Denmark), and monoclonal mouse anti-human CD68 antibody (KP1; DAKO) and incubated at 4°C overnight. The next day, the slides were washed and treated with Dako Real™ Envision™ horseradish peroxidase (HRP) rabbit/mouse (DAKO) kit. Dako Cytomation EnVision labeled polymer-alkaline phosphatase (AP) mouse/rabbit (DAKO) kit was also used for visualization by the peroxidase substrate Vector SG kit (black) and the AP substrate kit (red) from Vector Laboratories, Burlingame, CA, USA. Stained slides were observed using an Olympus BX40 light microscope (Olympus, Japan) with ×10/22 numeric aperture and ×40/0.75 numeric aperture objectives, and photographic images were collected with a digital camera DP50 (Olympus) and Image-Pro Plus 5.1 software.
Immunization
Hu-NSG mice were immunized by intramuscular injection of the hind leg with 1 mg/ml of DNP-KLH (Calbiochem, Merck, Germany) in 1× PBS from 14 weeks after transplantation with hCD34+ CB cells, and the immunization was boosted biweekly until 18 weeks after transplantation. Finally, DNP-KLH was directly injected into the spleen at 20 weeks after transplantation. Four weeks after the final boost, all hu-NSG mice were sacrificed and sera were collected. The levels of total plasma human immunoglobulins (hIgM and hIgG), DNP-KLH-specific hIgG, and hIgM were measured by enzyme-linked immunosorbent assay (ELISA).
Enzyme-Linked Immunosorbent Assay
Total and DNP-KLH-specific human immunoglobulins (hIgs), hIgM and hIgG, levels in sera were measured with the hIgM and hIgG ELISA Quantitation kit (Bethyl Laboratories, Montgomery, TX, USA). In brief, goat anti-hIgM- and anti-hIgG affinity-purified antibodies were diluted in 0.05 M carbonate–bicarbonate buffer (pH 9.6) and added to the appropriate wells of 96-well immunoplates (NUNC™, Roskilde, Denmark). After 1-h incubation at room temperature, the plates were washed five times and blocked with 1% BSA in TBS for 30 min at room temperature. Hu-NSG total serum diluted 10-fold in TBS containing 1% BSA, and 0.05% Tween-20 was loaded onto the plates and incubated for an hour at room temperature. After incubation, HRP-conjugated hIgM and hIgG detection antibodies (Bethyl Laboratories) were added and incubated for an hour at room temperature. Finally, the substrate solution, tetramethylbenzidine, was added to the plates, and then the reaction was stopped with 0.18 M H2SO4. For antigen-specific antibodies detection, each well was coated with 5 μg/ml DNP-KLH, and DNP-KLH-specific antibodies were measured using the same procedure described above. The hIg concentrations were determined from human reference serum provided in the ELISA kit.
Statistical Analysis
Data in the experiments are expressed as mean ± standard deviation of the mean. The Student’s t test was used to calculate statistical differences, and significance was defined by p < 0.05.
Results and Discussion
Determination of Busulfan Dose in the Generation of Humanized NSG Mice
To determine the optimal dose of busulfan in the generation of humanized mice, NSG mice were preconditioned with different doses of busulfan (Fig. 1a: group 2 pretreated with 20 mg/kg, group 3 pretreated with 30 mg/kg, and group 4 pretreated with 40 mg/kg) or TBI at 2.4 Gy, which is the previously established dose for the xenograft model [14–16], for comparison (Fig. 1a, group 1). Human CD34+ CB cells purified from human cord blood cells were then transplanted into the conditioned NSG mice. After transplantation with CD34+ CB cells, the survival rate was monitored for 24 weeks, as indicated in Fig. 1b. The TBI group showed 50% survival from 7 to 19 weeks after transplantation, and the survival rate gradually decreased to 33% after 24 weeks (Fig. 1b, diamond). However, both 20 and 30 mg/kg busulfan-injected mice showed 100% survival for up to 24 weeks after transplantation (Fig. 1b: square, 20 mg/kg; triangle, 30 mg/kg), whereas 40 mg/kg busulfan-injected mice all died 7 weeks after injection (Fig. 1b, inverted triangle). These results indicated that, although high-dose busulfan (40 mg/kg) showed highly toxic effects, both 20 and 30 mg/kg busulfan induced sufficient safety. Moreover, these doses were more effective than TBI in terms of mouse survival.
Schemes for the generation of humanized mice by busulfan and TBI treatment and assessment of survival rate. a Four different groups of humanized mice were generated in NSG mice: Group 1 (n = 10) conditioned by total body irradiation (TBI) at 2.4 Gy was injected via tail vein with 1 × 105 cells of isolated human CD34+ cells from umbilical cord blood; group 2 (n = 10), group 3 (n = 10), and group 4 (n = 10) were conditioned with 20, 30, and 40 mg/kg busulfan, respectively, then injected via tail vein with 1 × 105 cells of isolated human CD34+ cells from umbilical cord blood. b Assessment of percent survival of humanized mice. Ten humanized mice in each group were monitored weekly from a week after human CD34+ cells injection (2.4 Gy, diamond; 20 mg/kg, square; 30 mg/kg, triangle; 40 mg/kg, inverted triangle)
Reconstitution of Human T and B Cells in Humanized NSG Mice Conditioned with Busulfan
Based on Fig. 1, we assessed whether busulfan induces reconstitution of human immune cells in the humanized NSG mice and then compared that with the reconstitution in humanized mice conditioned by TBI. As shown in Fig. 1a, humanized NSG mice were generated by conditioning with 20 and 30 mg/kg busulfan and 2.4 Gy TBI. Peripheral blood mononuclear cells were isolated from the tail vein of each mouse at different intervals, as indicated in Fig. 2. The cells were stained with antibody specific for human CD45. The percentage of human CD45+ cells in the humanized NSG mice conditioned with busulfan rose significantly in a time-dependent manner: 11 ± 3%, 13 ± 3%, 19 ± 4%, 34 ± 5%, and 40 ± 4% with 20 mg/kg busulfan and 29 ± 5%, 26 ± 4%, 50 ± 6%, 50 ± 6%, and 64 ± 4% with 30 mg/kg busulfan (Fig. 2b, c). The reconstitution was significantly more effective with 30 mg/kg busulfan compared to those of other humanized mice (Fig. 2a, 2.4 Gy TBI; Fig. 2b, 20 mg/kg busulfan).
Kinetic analysis of the reconstitution of human CD45+ cells in humanized NSG mice. Peripheral blood was sampled from the tail of each group of humanized NSG mice (n = 5) at different times as indicated (a 2.4 Gy, b 20 mg/kg, c 30 mg/kg). Peripheral blood mononuclear cells were isolated and stained with antibody specific for human CD45, as described in the “Methods”. The results were analyzed by flow cytometry. Data are mean ± SEMs in humanized mice
Next, we assessed reconstitution of human immune cells in periphery, spleen, lymph node, and bone marrow. As shown in Fig. 2, the reconstitution rate was the highest at 24 weeks after transplantation. Thus, we sacrificed all humanized mice and isolated peripheral blood lymphocyte (PBL), splenocytes, MNCs from periphery, lymph node, and bone marrow. After the cells were counted, they were stained with antibodies specific for hCD45, hCD3, hCD14, hCD11b, hCD19, hCD20, hCD4, and hCD8. As shown in Figs. 3c and 4c, the absolute number of hCD45+ cells in both spleen and lymph node of busulfan-treated mice was significantly higher than that in 2.4 Gy treated mice, whereas no significant changes could be detected in PBL and bone marrow, indicating that busulfan treatment effectively induces the increase of reconstitution rates of human CD45+ cells derived from hCD34+ CB cells in lymphoid organs of humanized mice. In hCD45+hCD3+ T cells, the percent of cells was significantly increased up to >2-fold in both PBL and bone marrow of busulfan-treated mice (Fig. 3a, 27% in 2.4 Gy versus 61% in 20 mg/kg and 61% in 30 mg/kg busulfan; Fig. 4a, 11% in 2.4 Gy versus 34% in 20 mg/kg and 55% in 30 mg/kg), whereas little differences could be detected in spleen and lymph node (Figs. 3b and 4b). However, marked changes were detected in the absolute number of cells. The absolute cells of hCD45+hCD3+ T cells in both spleen and lymph node were markedly higher in busulfan-treated mice than in those of 2.4 Gy treated mice (Fig. 3d in spleen and Fig. 4d in lymph node), indicating quantitative effects of busulfan on the reconstitution of human T cells in lymphoid organs. Interestingly, busulfan showed both qualitative and quantitative effects on the reconstitution of human B cells in lymphoid organs. In hCD45+CD19+ B cells, the percent was elevated up to proximal 2-fold in both spleen and lymph node of busulfan-treated mice (Fig. 3b, 26% in 2.4 Gy versus 39% in 20 mg/kg; Fig 4b, 17% in 2.4 Gy versus 34% in 20 mg/kg or 25% in 30 mg/kg busulfan), but not in PBL and bone marrow (Figs. 3a and 4a). Moreover, the absolute number of B cells in both spleen and lymph node were higher in busulfan-treated mice than in those of 2.4 Gy treated mice, whereas no significant changes could be detected in both PBL and bone marrow (Figs. 3d and 4d), indicating that busulfan facilitates the reconstitution of B cells in lymphoid organs. We next compared the reconstitution of human macrophages in humanized mice conditioned by irradiation or busulfan. As shown in Figs. 3b and 4b, the percent of human macrophages represented by hCD45+CD11b+CD14+ were significantly increased in both spleen and lymph node of busulfan-treated mice, compared to that of 2.4 Gy treated mice (Fig. 3b, 4% in 2.4 Gy versus 7% in 20 mg/kg or 14% in 30 mg/kg busulfan; Fig 4b, 7% in 2.4 Gy versus 13% in 20 mg/kg or 22% in 30 mg/kg busulfan). Moreover, the absolute number of cells was greatly elevated in both spleen and lymph node of busulfan-treated mice (Figs. 3d and 4d). Taken together, these results suggest that busulfan has more potential effects on the reconstitution of human T, B cells, and macrophages in lymphoid organs than 2.4 Gy irradiation.
Reconstitution of human T and B cells in peripheral blood and spleen of humanized mice at 24 weeks post-transplantation with human CD34+ CB cells. a, b Mononuclear cells were isolated from peripheral blood and spleen of humanized mice, as described in “Methods”, and stained with antibodies specific for hCD45, hCD3, hCD4, CD8, hCD14, hCD11b, hCD19, and hCD20. After hCD45+ cells were gated in a dot plot of SSC versus hCD45, the gated cells were further analyzed by the expression of hCD3 versus hCD19 or hCD20 versus hCD19 and hCD11b versus hCD14. hCD45+hCD3+ cells were gated in a dot plot of hCD45 versus hCD3, and then the gated cells were further analyzed by the expression of hCD4 versus hCD8. Representative results are shown in a and b. The percent and absolute number of hCD45+ cells, hCD45+hCD3+, hCD45+hCD19+, and hCD45+hCD11b+hCD14+ cells are presented in c and d. Data are mean ± SEMs in humanized mice (n = 5, each group)
Reconstitution of human T and B cells in bone marrow and lymph node of humanized mice after post-transplanted 24 weeks with human CD34+ CB cells. a, b Mononuclear cells were isolated from bone marrow and lymph node of humanized mice, as described in “Methods” and stained with antibodies specific for hCD45, hCD3, hCD4, hCD8, hCD14, hCD11b, hCD19, and hCD20. After hCD45+ cells were gated in a dot plot of SSC versus hCD45, the gated cells were further analyzed by the expression of hCD3 versus hCD19 or hCD20 versus hCD19 and hCD11b versus hCD14. hCD45+hCD3+ cells were gated in a dot plot of hCD45 versus hCD3, and then the gated cells were further analyzed by the expression of hCD4 versus hCD8. Representative results are shown in a and b. The percent and absolute number of hCD45+ cells, hCD45+hCD3+, hCD45+hCD19+, and hCD45+hCD11b+hCD14+ cells are presented in c and d. Data are mean ± SEMs in humanized mice (n = 5, each group)
Histological Analysis of Human B, T, Monocyte, and Dendritic Cell Engraftment in Spleen of Humanized NSG Mice
To test whether humanized NSG mice conditioned with busulfan also facilitate other immune cells in spleen and mesenteric lymph node, samples were assessed by immunohistochemical staining. Figure 5 shows representative serial sections of organs from the humanized mice conditioned with busulfan or 2.4 Gy, stained with H&E, anti-hCD3hCD20, anti-hCD3hCD68, and anti-hCD3hCD11c. Under the H&E staining, follicle-like structures were observed in spleens of 30 mg/kg busulfan-treated mice (Fig. 5a indicated as asterisk). In contrast, follicles were not detected in the spleens of 2.4 Gy irradiated mice. As shown in Fig. 5a, b, moreover, reconstituted human CD20+ B cells indicated by red color were highly appeared in both spleen and mesenteric lymph node of 30 mg/kg busulfan-treated mice. Interestingly, human CD68+ monocytes and human CD11b+ dendritic cells represented by red color were markedly higher in both spleens and mesenteric lymph nodes of 30 mg/kg busulfan-treated mice than in that of others. These results suggest that busulfan treatment effectively induces reconstitutions of human monocytes and dendritic cells in lymphoid organs, along with reconstitutions of T and B cells as shown in Figs. 3 and 4. These histological results demonstrate that busulfan induces the formation of follicle-like structures in spleen and also induces the efficient engraftment of human immune cells, such as monocytes and dendritic cells, in the humanized mice conditioned by busulfan.
Histological analysis of structural and cellular reconstitution in spleen and mesenteric lymph nodes in humanized NSG mice. Spleen (a) and mesenteric lymph nodes (b) were isolated from humanized mice conditioned with 2.4 Gy irradiation, 20 mg/kg, or 30 mg/kg busulfan. Immunohistochemical staining was performed as described in “Methods”. Sections were visualized and photographed using an Olympus microscope. H&E images were collected at ×200 magnification and immunohistochemical images were collected at ×400 magnification
T Cell-Dependent Production of Human Antibodies in Humanized NSG Mice Conditioned with Busulfan
Since busulfan effectively induced reconstitution of human immune cells, especially B and T cells, in lymphoid organs, we tested whether humanized mice conditioned with busulfan allowed the production of T cell-dependent antibodies against T-dependent antigen [25]. We immunized humanized mice conditioned by busulfan or 2.4 Gy irradiation with DNP-KLH according to the immunization schedule (Fig. 6a). At 24 weeks after transplantation, samples were collected from peripheral blood, and the levels of secreted total human IgM and IgG were determined by ELISA. As shown in Fig. 6b, the antibody levels were significantly increased in 30 mg/kg busulfan-induced mice immunized with DNP-KLH compared to those in 20 mg/kg busulfan-induced or 2.4 Gy induced mice immunized with DNP-KLH. Moreover, when we measured specific hIgM and hIgG antibodies against DNP-KLH, the levels of specific antibodies were markedly elevated in 30 mg/kg busulfan-induced humanized mice compared to those in other humanized mice (Fig. 6c). These data show clearly that humanized mice conditioned with 30 mg/kg busulfan effectively produce T cell-dependent antigen-specific human antibodies.
Schemes of immunization with DNP-KLH and measurement of secreted total and DNP-KLH-specific human IgM and IgG. a NSG mice were preconditioned by 2.4 Gy irradiation (n = 20), 20 mg/kg busulfan (n = 10), and 30 mg/kg busulfan (n = 10). Humanized NSG mice were then generated by the procedure described in Fig. 1a. Considering the survival rate after 2.4 Gy irradiation, 20 NSG mice were initially used to generate humanized NSG mice. The humanized mice were immunized with DNP-KLH as mentioned in the “Methods”. b, c At 24 weeks, serum samples were collected from humanized mice, and the levels of total human IgM and IgG were measured by ELISA as described in the “Methods” (b). Additionally, secreted DNP-KLH-specific human IgM and IgG in each group were also measured by ELISA (c). Data are the mean ± SEMs in samples of humanized mice (n = 10 per group). *p < 0.05
Since distinct follicle-like structures were detected in 30 mg/kg busulfan-induced humanized mice (Fig. 5a), we next asked whether the production of specific antibodies is due to the effective generation of B cell subsets that produce antibodies. Mononuclear cells from bone marrow were harvested and stained with antibodies specific for hCD19, hIgM, hCD79a, hCD10, hCD20, hCD34, hCD27, and hIgD. Among hCD19−hIgM− cells, hCD10+hCD79a+ early B cells were significantly increased in 30 mg/kg busulfan-induced humanized mice (Fig. 7; hCD19−hIgM− gated). In addition, a slight difference in the distribution of pro-B and pre-B represented by hCD19+hIgM−hCD20+hCD34− and hCD19+hIgM−hCD20−hCD34−, respectively, was also detected in busulfan-induced humanized mice (Fig. 7, hCD19+hIgM− gated). Interestingly, hIgM+ memory B cells represented by hCD19+hIgM+hCD27+hIgD− were markedly increased in busulfan-induced humanized mice (Fig. 7, hCD19+hIgM+ gated).
Phenotypic analysis of early stages of human B cell development in bone marrow of humanized NGS mice. Humanized mice were immunized as described in Fig. 6a; a 2.4 Gy irradiated; b 20 mg/kg busulfan-treated; c 30 mg/kg busulfan-treated mice. MNCs were isolated from bone marrow cells of immunized mice and stained with antibodies specific for hCD19, hIgM, hCD79a, hCD10, hCD20, and hCD34. To identify early B cells, CD19+hIgM− cells were further analyzed by the expression of hCD79a versus hCD10. To discriminate between pro-B and pre-B cells, CD19+hIgM− cells were further analyzed by the expression of hCD20 versus hCD34. For the identification of IgM+ memory B, IgM+IgD+ activated or non-switched memory B, immature B, and naïve B cells, CD19+hIgM+ cells were further analyzed by the expression of hCD27 versus hIgD
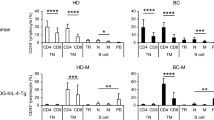
We further assessed whether busulfan effectively induces B cell development in spleen. Splenocytes were isolated from humanized mice immunized with DNP-KLH and stained with antibodies specific for hCD19, hIgD, hCD38, hIgM, and hCD27. As shown in Fig. 8a, pregerminal center and germinal center B cells represented by hCD19+hIgD+hCD38+ and hCD19+hIgD−hCD38+, respectively, were markedly increased in 30 mg/kg busulfan-induced humanized mice. Moreover, memory B cells represented by hIgD+hCD38−hIgM+hCD27+ were also significantly enhanced in 30 mg/kg busulfan-induced humanized mice (Fig. 8b). These data suggest that, although the cellular and molecular environments facilitating B cell response in busulfan-induced humanized mice remain to be investigated, busulfan effectively induces B cell responses by facilitating the formation of cellular structure in lymphoid organs (Fig. 5) and inducing multiple B cell developmental stages to antigen (Figs. 6, 7, and 8).
Analysis of human B development in spleen of humanized mice. a Humanized mice conditioned by 2.4 Gy irradiation, 20 mg/kg busulfan, and 30 mg/kg busulfan were immunized as described in Fig. 6a. Splenocytes were isolated from the mice and stained with antibodies specific for hCD19, hIgD, and hCD38. To identify pregerminal center B and germinal center B cells, hCD19+ cells were analyzed by the expression of hIgD versus hCD38. Their absolute cell numbers are presented as mean ± SEMs in samples of humanized mice (n = 5 per group). b Splenocytes were stained with antibodies specific for hIgD, hCD38, hIgM, and hCD27. To identify naïve, mature naïve, and memory B cells, hIgD+hCD38− cells were analyzed by the expression of hIgM versus hCD27. Their absolute cell numbers are presented as mean ± SEMs in samples of humanized mice (n = 5 per group)
Conclusions
Although busulfan is commonly used in hematopoietic stem cell transplant (HCT) patients because of its narrow toxicity, its hematoxic effect causing bone marrow failure has been reported when used inappropriately [26–29]. The side effect seems to be related to significant defects in hematopoietic stem cell proliferation. Similarly, it has been reported that busulfan therapy results in a chronic latent marrow aplasia characterized by normal peripheral blood neutrophil numbers, normal hematocrit, and marrow cellularity but reduced numbers of pluripotent hematopoietic stem cells and colony-forming unit granulocyte–macrophage, indicating that busulfan can induce qualitative defect in either the hemopoietic stem cells, the stromal-forming elements, or both [28, 29]. Nevertheless, busulfan has still potential advantages in HCT study. Many reports have shown that busulfan has little toxicity in HCT patients, when either orally or intravenously administrated [17–20, 26]. These studies have demonstrated that the optimal busulfan target range is mostly important and determined by considering the conditioning regimen, the age of the HCT recipients, and their underlying disease. Therefore, the use of busulfan in therapeutics have to consider multiple conditions to be appeared in recipient and also carefully monitor possible toxicities on hematopoietic stem cell, stroma, and supporting tissues of lymphoid organs.
Our results demonstrate in this study that humanized mice conditioned with busulfan can efficiently induce reconstitution and differentiation of human immune cells derived from transplanted CD34+ CB cells. Moreover, the humanized mice can induce effective B cell development and thereby mount strong T cell-dependent antigen-specific B cell responses against immunized DNP-KLH. This is a powerful humanized model for the in vivo study of human B cell development, human immune system, and their functions. Because of the simple, convenient, effective, and less toxicity, busulfan-induced humanized mice might be also a valuable tool for producing humanized antibodies that can be applied to various biomedical fields.
References
Shultz LD, Ishikawa F, Greiner DL. Humanized mice in translational biomedical research. Nat Rev Immunol. 2007;7:118–30.
Manz MG. Human-hemato-lymphoid-system mice: opportunities and challenges. Immunity. 2007;26:537–41.
Macchiarini F, Manz MG, Palucka AK, Shultz LD. Humanized mice: are we there yet? J Exp Med. 2005;202:1307–11.
Payne KJ, Crooks GM. Immune-cell lineage commitment: translation from mice to humans. Immunity. 2007;26:674–7.
Melkus MW, Estes JD, Padgett-Thomas A, Gatlin J, Denton PW, Othieno FA, et al. Humanized mice mount specific adaptive and innate immune responses to EBV and TSST-1. Nat Med. 2006;12:1316–22.
Mosier DE, Gulizia RJ, Baird SM, Wilson DB. Transfer of a functional human immune system to mice with severe combined immunodeficiency. Nature. 1988;335:256–9.
Kaneshima H, Namikawa R, McCune JM. Human hematolymphoid cells in SCID mice. Curr Opin Immunol. 1994;6:327–33.
Pflumio F, Izac B, Katz A, Shultz LD, Vainchenker W, Coulombel L. Phenotype and function of human hematopoietic cells engrafting immune-deficient CB17-severe combined immunodeficiency mice and nonobese diabetic-severe combined immunodeficiency mice after transplantation of human cord blood mononuclear cells. Blood. 1996;88:3731–40.
Shultz LD, Lang PA, Christianson SW, Gott B, Lyons B, et al. NOD/LtSz-Rag1null mice: an immunodeficient and radioresistant model for engraftment of human hematolymphoid cells, HIV infection, and adoptive transfer of NOD mouse diabetogenic T cells. J Immunol. 2000;164:2496–507.
Goldman JP, Blundell MP, Lopes L, Kinnon C, Di Santo JP, Thrasher AJ. Enhanced human cell engraftment in mice deficient in RAG2 and the common cytokine receptor gamma chain. Br J Haematol. 1998;103:335–42.
Kollet O, Peled A, Byk T, Ben-Hur H, Greiner D, Shultz L, et al. β2 Microglobulin-deficient (B2mnull) NOD/SCID mice are excellent recipients for studying human stem cell function. Blood. 2000;95:3102–5.
Ito M, Hiramatsu H, Kobayashi K, Suzue K, Kawahata M, et al. NOD/SCID/γ nullc mouse: an excellent recipient mouse model for engraftment of human cells. Blood. 2002;100:3175–82.
Hiramatsu H, Nishikomori R, Heike T, Ito M, Kobayashi K, Katamura K, et al. Complete reconstitution of human lymphocytes from cord blood CD34+ cells using the NOD/SCID/γ nullc mice model. Blood. 2003;102:873–80.
Haddow A, Timmis GM. Myleran in chronic myeloid leukaemia; chemical constitution and biological action. Lancet. 1953;31:207–8.
Shultz LD, Lyons BL, Burzenski LM, Gott B, Chen X, et al. Human lymphoid and myeloid cell development in NOD/LtSz-scid IL2R gamma null mice engrafted with mobilized human hemopoietic stem cells. J Immunol. 2005;174:6477–89.
Ishikawa F, Yasukawa M, Lyons B, Yoshida S, Miyamoto T, et al. Development of functional human blood and immune systems in NOD/SCID/IL2 receptor γ chainnull mice. Blood. 2005;106:1565–73.
Ciurea SO, Andersson BS. Busulfan in hematopoietic stem cell transplantation. Biol Blood Marrow Transplant. 2009;15:523–36.
Mauch P, Down JD, Warhol M, Hellman S. Recipient preparation for bone marrow transplantation. I. Efficacy of total-body irradiation and busulfan. Transplantation. 1988;46:205–10.
Down JD, Ploemacher RE. Transient and permanent engraftment potential of murine hematopoietic stem cell subsets: differential effects of host conditioning with gamma radiation and cytotoxic drugs. Exp Hematol. 1993;21:913–21.
Hsieh MM, Langemeijer S, Wynter A, Phang OA, Kang EM, Tisdale JF. Low-dose parenteral busulfan provides an extended window for the infusion of hematopoietic stem cells in murine hosts. Exp Hematol. 2007;35:1415–20.
Hayakawa J, Hsieh MM, Uchida N, Phang O, Tisdale JF. Busulfan produces efficient human cell engraftment in NOD/LtSz-Scid IL2Rγ null mice. Stem Cells. 2009;27:175–82.
Shapiro-Shelef M, Calame K. Regulation of plasma-cell development. Nat Rev Immunol. 2005;5:230–42.
Allman D, Pillai S. Peripheral B cell subsets. Curr Opin Immunol. 2008;20:149–57.
Carsetti R, Rosado MM, Wardmann H. Peripheral development of B cells in mouse and man. Immunol Rev. 2004;197:179–91.
Tonomura N, Habiro K, Shimizu A, Sykes M, Yang YG. Antigen-specific human T-cell responses and T cell-dependent production of human antibodies in a humanized mouse model. Blood. 2008;111:4293–6.
McCune JS, Holmberg LA. Busulfan in hematopoietic stem cell transplant setting. Expert Opin Drug Metab Toxicol. 2009;8:957–69.
Chen J. Animal models for acquired bone marrow failure syndromes. Clin Med Res. 2005;2:102–8.
Sauer M, Zeidler C, Meissner B, Rehe K, Hanke A, Welte K, et al. Substitution of cyclophosphamide and busulfan by fludarabine, treosulfan and melphalan in a preparative regimen for children and adolescents with Shwachman–Diamond syndrome. Bone Marrow Transplant. 2007;39:143–7.
Boyd RL, Caro J, Halka KG, Erslev AJ. Granulopoiesis in long-term culture by marrow from mice with busulfan-induced chronic latent aplasia. Int J Cell Cloning. 1986;4:357–67.
Acknowledgment
This work was supported by Mid-career Researcher Program through NRF grant funded by the MEST (2009-0084573; to K.-Y.L.), the Korea Health 21 R&D Project, Ministry of Health and Welfare (A080568; to S.J.K.), and by Medical Research Foundation of Samsung Biomedical Research Institute (SBRI) grant (C-A6-407-1; to S.J.K.).
Author information
Authors and Affiliations
Corresponding authors
Additional information
Bongkum Choi, Eunyoung Chun, and Miyoung Kim are equally contributed to this work
Rights and permissions
About this article
Cite this article
Choi, B., Chun, E., Kim, M. et al. Human B Cell Development and Antibody Production in Humanized NOD/SCID/IL-2Rγnull (NSG) Mice Conditioned by Busulfan. J Clin Immunol 31, 253–264 (2011). https://doi.org/10.1007/s10875-010-9478-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10875-010-9478-2