Abstract
The use of calcium silicate (CS) cement holds great promise for bone substitute biomaterials. However, the effects of CS on osteoblast and macrophage cells are not fully understood. This study examines cell proliferation and differentiation of mono- or co-cultured MC3T3-E1 and Raw 264.7 cells on CS cement. Very few studies to date have looked at the effects of osteoblast and macrophages on biomaterial-regulated osteogenesis. In this study the proliferation and differentiation of MC3T3-E1, Raw 264.7 and co-cultured MC3T3-E1/Raw 264.7 on CS cements have been analyzed using a PrestoBlue kit and ELISA. In addition, the effect of macrophages on CS-coordinated osteogenesis of MC3T3-E1 has been investigated. Results show that MC3T3-E1, Raw 264.7 and co-cultured MC3T3-E1/Raw 264.7 adhere to and proliferate well on the CS cement. In a co-culture, the CS cements inhibit receptor activator of nuclear factor kappa B ligand expression of both genes and proteins in Raw 264.7 cells when compared to those grown in mono-cultured system. Ca deposition of MC3T3-E1 in the co-culture is higher than that of cells in a mono-culture. Bone morphogenetic protein 2 (BMP2) is also significantly up-regulated by the CS cement stimulation, indicating that macrophages may participate in the CS stimulated osteogenesis. Interestingly, when macrophage are cultured with BMP2 receptor-blocking MC3T3-E1 on the CS cements, the osteogenesis differentiation of the cells is significantly inhibited, indicating the important role of macrophages in biomaterial-induced osteogenesis via BMP2 receptors. It is assumed that it is an increase in the secretion of the BMP2 from the Raw 264.7 cell that is primarily involved in the promotion of the osteogenesis of the MC3T3-E1. These results provide valuable insights into both the mechanism of CS-stimulated osteogenesis, and strategies to optimize the evaluation system for the in vitro osteogenesis capacity of bone substitute biomaterials.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
Natural Bone is a composite with outstanding material properties and therefore serves as a model for bone replacement biomaterials. Bone remodeling is regulated by the replacement of old bone with new bone through sequential osteoclastic resorption and osteoblastic bone formation [1]. Recently, several studies have investigated whether osteoblast cells constitutively express osteogenesis cytokines and growth factors, such as collagen I, osteopontin, alkaline phosphatase, osteocalcin, and anti-inflammatory cytokines [2]. Mature osteoblast-related cells produce osteoprotegerin (OPG) and the receptor activator of nuclear factor kappa B ligand (RANKL), which has opposing effects on osteoclasts [3].
Recently, a calcium silicate-based (CS) material has been investigated as a bioactive material for bone substitution [4–6]. CS has been reported to exhibit excellent in vitro bioactivity, and it leads to the precipitation of a bone-like apatite layer, which may assist the material to integrate into living tissue [7, 8]. Ions released from CS-based cements have been shown to stimulate the proliferation and osteogenic differentiation of osteoblasts and promote mineral deposition at the material–dentine interface [9, 10]. Restoration of periodontal attachment requires not only the formation of the alveolar bone but also new cementum regeneration to substitute for the diseased root surfaces contaminated with bacterial endotoxins [11]. Therefore, CS-based cements have been formulated into dentin replacement restorative materials in dentistry [12, 13]. Moreover, Lin et al. demonstrated that the bioactive Si ions released from CS can support a preferential extracellular environment for directing osteogenic differentiation of human mesenchymal stem cells (hMSCs), and promote human umbilical vein endothelial cell (HUVEC) proliferation and angiogenesis even in the absence of extra osteogenic and angiogenic reagents. However, as described by Bohner in his leading opinion paper, until now, no clear link has been made between the enhanced biological performance of Si-based materials and Si release [14].
It has recently been reported that the osteogenesis of bone cells is greatly promoted by being co-cultured with HUVEC in 3D ceramic scaffolds [15, 16]. These studies have confirmed that the extent of cell–cell communication between bone cells and HUVEC in a co-culture system in combination with secreted cytokines, such as bone morphogenetic proteins (BMP), endothelial growth factor (VEGF) and fibroblast growth factor (FGF), may promote the osteogenic differentiation of hMSCs. Interestingly, a paracrine effect through osteogenic factors has also been observed in the indirect contact co-culture of macrophage cells and bone cells in previous studies [17, 18]. However, implantation of any material into tissue evokes a host inflammatory and immune reaction generally described as the foreign body response. Several pro-inflammatory cytokines secreted by macrophages are immediately up-regulated post- injury in the presence of a foreign materials [19–21]. These soluble growth factors are recognized by the same cells in autocrine, and neighboring cells in paracrine [20]. Macrophages and osteoblasts during bone formation via soluble autocrine and paracrine signals as well as juxtacrine signals associated with direct cell–cell contacts [17].
Therefore, the aims of this study are to confirm the hypothesis that the stimulation of osteogenesis of co-cultured macrophage cells and osteoblast by calcium silicate cements occur through paracrine effects, and to identify the role of the BMP2 in this biomaterial-induced process of osteogenesis. In addition, we also investigate and compare macrophages and osteoblasts in vitro co-cultures to elucidate and distinguish cytokine signaling between these cell types and determine more representative instances of in vitro cellular responses to in vivo models; ideally we hope to provide evidence for confounding in vitro cell behavior. CS cement is used as a model biomaterial to investigate the interactions between bone substitute and macrophages, and to further reveal whether macrophages participate in the material-stimulated osteogenic differentiation.
2 Materials and methods
2.1 Preparation of specimens
The method used here for the preparation of CS powder has been described elsewhere [22]. In brief, reagent grade 25 % SiO2 (High Pure Chemicals, Saitama, Japan), 65 % CaO (Sigma-Aldrich, St. Louis, MO), and 10 % Al2O3 (Sigma-Aldrich) powders were used as matrix materials. The oxide mixtures were then sintered at 1400 °C for 2 h using a high-temperature furnace and then ball-milled in ethyl alcohol using a centrifugal ball mill (S 100, Retsch, Hann, Germany) for 6 h. The sintered powder was mixed using a liquid/powder ratio of 0.35 mL/g. After mixing with water, the cements were shaped in a Teflod mold (diameter: 10 mm, height: 2 mm). All samples were stored in an incubator at 100 % relative humidity and 37 °C for 1 day of hydration.
2.2 Ion concentration
The Ca, Si, and P ion concentrations released from the cement on DMEM were determined using an inductively coupled plasma-atomic emission spectrometer (ICP-AES; Perkin-Elmer OPT 1MA 3000DV, Shelton, CT, USA) after the samples had been immersed in DMEM for various periods of time. Three samples were measured for each data point and the results were obtained in triplicate from three separate samples for each test.
2.3 Cell culture
RAW 264.7 macrophage cells (Mac) and MC3T3-E1 osteoblast cells (OB) (American Type Culture Collection, Manassas, VA) were cultured in Dulbecco’s Modified Eagle Medium (DMEM, Caisson Laboratories, North Logan, UT) containing 10 % fetal bovine serum (GeneDireX, Las Vegas, NV), 100 U/mL penicillin/100 μg/mL streptomycin (Caisson) at 37 °C in a humidified atmosphere of 5 % CO2. The culture medium was changed every 3 days. Cells (5 × 104 cell/mL) were seeded on covered glass or calcium silicate cements for 24 h, and transferred to 6-well plates (GeneDireX) with cultured medium. Before performing the cell experiments, the cover glass and materials were sterilized by immersion in 75 % ethanol followed by exposure to ultraviolet (UV) light for 6 h. The 24-well plates are equipped with cover glasses (mono-culture: MC3T3-E1 or RAW264.7 on cover glass or cement; co-culture: two cover glasses, one MC3T3-E1, and the other RAW264.7 on cements). A full description of the culture process implemented for each signaling condition is presented in the supplementary materials.
2.4 Proliferation Assays
After being cultured for the various predetermined periods of time, cell proliferation was evaluated using the PrestoBlue® assay (Invitrogen, Grand Island, NY). Briefly, at the end of the appointed time, the cover glasses or cements were transferred to a new 24-well plate and washed with PBS three times. Each well was then filled with 300 µL solution (PrestoBlue®: DMEM = 1: 9) and incubated at 37 °C for 30 min after which the solution in each well was transferred to a new 96-well plate (GeneDireX). Plates were read in a multiwell spectrophotometer (Hitachi, Tokyo, Japan) at 570 nm with a reference wavelength of 600 nm. The results were obtained in triplicate from three separate experiments for each test.
2.5 ELISA analysis
RANKL and OPG protein are secretions from MC3T3-E1 cells cultured under a tensile or normal incubator for various numbers of days and collected the cultured medium. A RANKL ELISA assay kit (Abcam, Cambridge, MA) and OPG ELISA assay kit (Sigma-Aldrich, St. Louis, MO) were used to determine the protein concentration following the manufacturer’s instructions. The protein concentration was measured by correlation with a standard curve. Analyses of blank disks served as controls. All experiments were done in triplicate.
2.6 Tartrate-resistant acid phosphatase (TRAP) Activity
After being cultured for different numbers of days, the cells on the covering glass were fixed with 4 % formalin for 15 min and 95 % EtOH for 3 min in order to measure TRAP activity. Later, the cover glasses were immersed in 10 mM citrate buffer (pH 4.6) containing 10 mM sodium tratrate and p-nitrophenylphosphate. After incubation for 1 h, the reaction mixtures were transferred to a new 24-well tray. The reaction was stopped by the addition of 5 N NaOH and quantified by absorbance at 405 nm. All experiments were done in triplicate for each of the three separate experiments comprising each test.
In addition, we also confirmed the TRAP gene expression. The total RNA of all groups was extracted using TRIzol reagent (Invitrogen) after being cultured and analyzed by RT- qPCR. The total RNA (500 ng) was used for the synthesis of complementary DNA using a cDNA Synthesis Kit (GenedireX) following the manufacturer’s instructions. TRAP primers: Forward: 5′-AGCAGCCAAGGAGGACTACGTT-3′ and reverse: 5′- TCGTTGATGTCGCACAGAGG-3′ were designed based on cDNA sequences from the NCBI Sequence database. SYBR Green qPCR Master Mix (Invitrogen) was used for detection and the target mRNA expressions were assayed on the ABI Step One Plus real-time PCR system (Applied Biosystems, Foster City, California, USA). Each sample was performed in triplicate.
2.7 Mineralization
The accumulated calcium deposition was analyzed after 14 days using Alizarin Red S staining, as in a previous study [23]. In brief, the cells were fixed with 4 % paraformadedyde (Sigma-Aldrich) for 15 min and then incubated in 0.5 % Alizarin Red S (Sigma-Aldrich) at pH 4.0 for 15 min at room temperature in an orbital shaker (25 rpm). After the cells were washed with PBS, photographs were taken using an optical microscope (BH2-UMA, Olympus, Tokyo, Japan) equipped with a digital camera (Nikon, Tokyo, Japan) at 200x magnification. To quantify the stained calcified nodules after staining, samples were immersed with 1.5 mL of 5 % SDS in 0.5 N HCl for 30 min at room temperature. After that, the tubes were centrifuged at 5000 rpm for 10 min and the supernatant was transferred to the new 96-well plate; absorbance was measured at 405 nm (Hitachi).
2.8 Osteogenic protein secretion from macrophage cells
After treatment for 3 and 7 days, the BMP2 protein released from the cells to the cultured medium was collected and analyzed using an enzyme-linked immunosorbent assay kit (ELISA, Invitrogen) following the manufacturer’s instructions. The protein concentration was measured by correlation with a standard curve. All experiments were done in triplicate.
2.9 BMPR2 expression of bone cells
To investigate the activation of the BMP2 signaling pathway in bone cells, the bone morphogenetic protein receptor type II (BMPR2) gene was analyzed using an RT-qPCR as described in Sect. 2.6. BMPR2 primers: Forward: 5′-GGCAGCAGTATACAGATAGGTG-3′ and reverse: 5′-CTGCCCTGTTACTGCCATTATT-3′ were designed based on cDNA sequences from the NCBI Sequence database.
2.10 BMPR2 on osteogenesis
To further clarify the role of BMPR2 on osteogenesis, the cells were incubated with 10 mg/mL blocking antibodies (Genetex) against BMPR2 for 30 min on ice before being seeded on substrates. After being cultured for 3 and 7 days, the alkaline phosphatase (ALP) and osteocalcin (OC) were measured. The process of ALP activity was as follows: the cells were lysed from discs using 0.2 % NP-40 and centrifuged for 10 min at 2000 rpm after washing with PBS. ALP activity was determined using p-nitrophenyl phosphate (pNPP, Sigma) as the substrate. Each sample was mixed with pNPP in 1 M diethanolamine buffer for 15 min, after which the reaction was stopped by the addition of 5 N NaOH and quantified by absorbance at 405 nm. The OC protein was determined from the cells following the manufacturer’s instructions, an osteocalcin enzyme-linked immunosorbent assay kit (Invitrogen) was used to determine the OC protein content. The OC protein concentration was measured by correlation with a standard curve. Six measurements were done for each group.
2.11 Statistical analysis
One-way analysis of variance (ANOVA) statistical analysis was used to evaluate the significance of the differences between the mean values in comparison with those of the controls. Scheffe’s multiple comparison testing was used to determine the significance of the deviations in the data for each specimen. In all cases, the results were considered statistically significant with a p value <0.05.
3 Results and discussion
3.1 Release of ions from CS substrates
The release profiles of Ca, Si and P ions from the CS specimens in DMEM are presented in Fig. 1. After 1 day, the Ca ion concentration in the CS cement medium was seen to have decreased to approximately 1.4 mM (Fig. 1a), which is lower than the baseline Ca concentration of DMEM (1.8 mM) (P < 0.05). As for the P ion concentration of DMEM, it also showed a decrease after 1 day of immersion (Fig. 1c). The bioactivity of calcium silicate materials indicates that the presence of PO43− ions in the composition is not an essential requirement for the development of an apatite layer, which consumes calcium and phosphate ions [7, 8, 24]. Si ion concentrations increase along with an increase in the culturing time. Si ion concentrations reach levels of 1.15, 2.27, and 3.22 mM after immersion for 1, 3, and 7 days, respectively. Si ions are released during the hydration of the cement paste providing favorable sites for nucleation of apatite crystals, while the released Ca ions induce the super saturation of the DMEM solution [10, 25]. Calcium silicate cement undergoes hydrolysis on immersion, and Si ion dissolves during incubation [5, 26]. In addition, certain amounts of Si released from silicate-based materials seem to promote desired cell behaviors [18, 27, 28]. The current CS gives the ability to control the rate at which soluble Si ions affect cell adhesion and proliferation [13, 29].
3.2 Cell proliferation
The proliferation of the Raw 264.7 cells and MC3T3-E1 cells cultivated as a mono-culture as well as a co-culture with CS have been calculated using a PrestoBlue® assay (Fig. 2). Cell viability of Raw 264.7 was not significant (P > 0.05) in any of the four groups at any of the time-points at which measurements were made (Fig. 2a). The growth rate of the RAW 264.7 cells was not affected in different substrates. In a previous study, it was found that an Si ion concentration lower than 4 mM did not have a growth stimulatory effect on RAW 264.7 cells [30]. However, it was found that CS caused a higher growth rate of MC3T3-E1 cells (Fig. 2b) than Ctl for all analyzed periods of time. Interestingly, the MC3T3-E1 cells cultured on CS had a greater number of cells than Ctl (P < 0.05) in the co-culture system on day 7.
3.3 OPG and RANKL secretion
The secretion of RANKL and OPG was also detected, and the results are shown in Figs. 3. OPG protein secretion from MC3T3-E1 cells cultured with CS was nearly 1.4- and 1.5-times higher than Ctl (P < 0.05) in the mono-culture and co-culture systems, respectively (Fig. 3a). Moreover, the amount of OPG from MC3T3-E1 in co-cultured system is higher than in the mono-cultured one. In addition, the CS cement had a significant inhibiting effect (P < 0.05), leading to a decrease of 23 and 37 % in RANKL synthesis compared with Ctl in the mono-cultured and co-cultured systems, respectively (Fig. 3b). A Reduction in the pre-osteoblast secretion of RANKL or antagonizing RANKL actions on pre-osteoclasts might be a protective mechanism for preventing excessive osteoclast differentiation [31]. Pre-osteoclast maturation and osteoclast activation were affected negatively since, by binding to OPG, RANKL is segregated and unavailable to bind to pre-osteoclastic receptors, RANK [32]. Calcium silicate cements have the potential to antagonize RANKL actions and bone resorption by enhanced osteogenesis and the production of anti-osteoclastogenic cytokines [30, 33]. These results indicate that CS up-regulated the secretion of OPG and inhibited RANKL synthesis.
3.4 TRAP activity
The differentiation of RAW264.7 into osteoclasts has been estimated through the detection of TRAP activity and TRAP gene expression in the mono-culture as well as in the co-culture with MC3T3-E1 (Fig. 4). TRAP activity and gene expression of the RAW264.7 cells increased from day 3 to day 7 in co-cultured system and the cells increased significantly more than in the mono-cultured system (P < 0.05), which stimulated the differentiation to form osteoclasts. However, there was no TRAP secretion from MC3T3-E1 cells present in the mono-culture with CS for any of the measured culture times (data not shown). In the co-cultured system, a significant (P < 0.05) decrease of 51 and 43 % was found for TRAP synthesis in RAW264.7 cells cultured on CS in comparison with the control group at 3, and 7 days, respectively (Fig. 4a). In addition, the results of the TRAP activity in the co-cultured system decreased strongly and significantly in comparison with the mono-culture on CS for each of the measured incubation periods. To substantiate this cytochemical observation, gene expression results were performed for TRAP using the RT-PCR. These data showed similar results to TRAP activity (Fig. 4b). In Recent research it has been shown that both silicon/silicate-based components and polymeric phosphate, when combined in a complex with calcium, have the potential to act as anti-osteoporotic agents [34]. An unanticipated finding is that Si, in the form of bio-silica, causes a differential gene expression and promotes OPG expression while, simultaneously, RANKL expression remains unchanged [35]. Moreover, osteoblastic cells in vitro not only produce more OPG but also less osteoclast-activating RANKL secretion, which inhibits the RANKL-RANK interaction on osteoclasts on CS in the co-cultured system.
3.5 Mineralization
Alizarin Red S staining showed evidence of calcium deposition and nodule formation. Mineralized nodules formation was observed in all groups (Fig. 5a). According to the literature, CS promotes cells in higher osteogenesis activity and a trend toward higher mineral deposition [36]. After being cultured for 3 and 7 days, more distinct nodules were observed in MC3T3-E1 cells cultured with Raw 264.7 cells than in the osteoblast cells alone (P < 0.05) (Fig. 6b). In a previous study, the lipopolysaccharide activated macrophages induced pre-osteoblast cells to differentiate and contribute osteogenic cytokines to promote osteogenesis [37]. After being cultured on materials, the macrophage cells participate in both ends, via secreting several cytokines. They may contribute osteoinductive and osteogenic cytokines (BMP2, VEGF) to enhance osteogenesis while also assisting inflammatory and fibrous agents (TNF-α, VEGF, TGF-β) to affect pathological fibrosis [38]. Therefore, the conclusion still could not be made whether nor not macrophages play a major role in affecting osteogenesis. An effective and adequate switch in macrophage phenotype might be of great importance for enhancing osteogenesis.
3.6 BMP2 and BMP2R expression
The potentially osteogenic-enhancing effect of materials needs to be further demonstrated in vivo; the in vitro and in vivo biological behavior to biomaterials are not always similar, due to the lack of immune cells in vitro [39, 40]. BMP2 protein secretion was up regulated by the stimulation of CS (P < 0.05) (Fig. 6a). The BMP2 secretions from macrophage cells in mono- or co-cultured system with CS were increased to levels 41 and 58 % (P < 0.05) more than the macrophage cell used for the Ctl for 7 days, respectively. To further explore the mechanisms promoting osteogenesis, we considered the gene expressions of BMP2R signaling pathways (Fig. 6b). MC3T3-E1 cells on CS alone could not up-regulate the BMP2R genes, unlike the co-cultured system. Moreover, the BMP2R gene expression of MC3T3-E1 cells cultured with CS is higher than the Ctl in the co-cultured system. The stimulated macrophages also up-regulate BMP2 protein expression, which activates the BMP2 signaling pathway in MC3T3-E1 cells, leading to osteogenic differentiation. However, the results of biological responses to CS-based materials stimulation are not always consistent, due to the lack of immune cells in vitro [41]. BMP2 is a founding member of the BMP family, and acts as an osteoinductive agent [42]. CS materials-treatment itself is not sufficient to promote the osteogenic effect of MC3T3-E1, although macrophages can release osteogenic cytokines in the co-cultured system, thereby promoting the osteogenesis effect of hPDLs, which is more consistent with in vivo results. The confirmation that macrophage cells behave actively during the osteogenic differentiation caused by CS-based materials is meaningful: macrophages play an important role in regulating osteogenic differentiation [17]. An effective and adequate switch in macrophage phenotype might be of great importance for promoting osteogenesis.
3.7 Effect of BMPR on osteogenesis
The effect of cell osteogenesis for MC3T3-E1 in mono- and co-cultured system after BMP2R blocking is presented in Fig. 7. When BMP2R blocking occurs, all specimens showed a significant reduction in their ALP activity. However, the samples cultured on Ctl showed no significant differences (P > 0.05) between the mono-cultured and co-cultured systems (Fig. 7a). The BMP2R antibody blocking against for BMP2R had no effect on the ALP level in the mono-cultured system. By contrast, the ALP activity of MC3T3-E1 after BMP2R blocking was decreased 26.9 and 37.9 % on CS in the co-cultured system after 3 and 7 days, respectively, significantly lower (P < 0.05) than in the other group. It can be seen in the OC results shown in Fig. 7b that it is similar to ALP, both showing BMP2R-blocking inhibited in the co-cultured system with CS (P < 0.05). Accordingly, CS may stimulate BMP2 release from Raw 264.7 cells and promote osteogenesis of MC3T3-E1 cells through a BMP2R-responsive mechanism. In previous research, the detailed mechanism by which Si ions released from CS materials promoted cell behavior was reported, and it was proposed that a MAPK cascade of ERK and p38 pathways was playing an important role in facilitating cell functions [22, 33, 43]. In addition, we also demonstrated that fibroblast growth factor receptor stimulates cell proliferation and differentiation through the ERK/MAPK pathway in hDPCs [10]. It is not surprising that the pretreatment of cells with inhibitors of ERK (PD98059) significantly inhibits mineralization in the cells on CS. This suggests that CS materials control the lineage allocation of human dental pulp cells from the fibroblast to the osteoblast lineage via mechanisms involving activation of FGFR/ERK/MAPK signaling. Thus, although there are several studies that look at the in vitro and in vivo osteogenic of CS materials, the effect of CS on the biological behavior of macrophages is still unclear, and the effect of macrophages on CS-coordinated osteogenesis of bone cell has not been investigated. In this study, the results show the stimulated Raw 264.7 cells also up-regulate BMP2 gene expression, which activates the BMP2 signaling pathway in MC3T3-E1, leading to osteogenic differentiation.
Effect of anti-BMP2R antibody on a ALP activity and b OC protein of MC3T3-E1 cultured on CS under mono- and co-cultured system for 7 and 14 days. The untreated groups were used as the 100 % reference level. *A significant difference (P < 0.05) compared with Ctl. #A significant difference (P < 0.05) compared with mono-cultured
4 Conclusion
The data showed here underscore that calcium silicate cement displays a significant enhancement of the osteogenic-related genes and a distinct reduction of the differentiation potential of RAW 264.7 macrophage cells that differentiate into osteoclast-like cells in vitro. In addition, the macrophage cells are shown to play important roles in CS-induced osteogenesis. CS elicits significant effects on macrophages that inhibit inflammation and promote the osteogenic differentiation of MC3T3-E1. Adequately activated macrophages are vital for the success of material-stimulated bone regeneration. The interaction with macrophage cells should be elucidated when evaluating the in vitro osteogenic capacity of a bone substitute.
References
Eriksen EF. Cellular mechanisms of bone remodeling. Rev Endocr Metab Disord. 2010;11:219–27.
Huang TH, Lu YC, Kao CT. Low-level diode laser therapy reduces lipopolysaccharide (LPS)-induced bone cell inflammation. Lasers Med Sci. 2012;27:621–7.
Singh PP, van der Kraan AGJ, Xu J, Gillespie MT, Quinn JMW. Membrane-bound receptor activator of NFκB ligand (RANKL) activity displayed by osteoblasts is differentially regulated by osteolytic factors. Biochem Biophys Res Commun. 2012;422:48–53.
Kao CT, Huang TH, Chen YJ, Hung CJ, Lin CC, Shie MY. Using calcium silicate to regulate the physicochemical and biological properties when using β-tricalcium phosphate as bone cement. Mater Sci Eng C Mater Biol Appl. 2014;43:126–34.
Su CC, Kao CT, Hung CJ, Chen YJ, Huang TH, Shie MY. Regulation of physicochemical properties, osteogenesis activity, and fibroblast growth factor-2 release ability of β-tricalcium phosphate for bone cement by calcium silicate. Mater Sci Eng C Mater Biol Appl. 2014;37:156–63.
Lin K, Xia L, Li H, Jiang X, Pan H, Xu Y, et al. Enhanced osteoporotic bone regeneration by strontium-substituted calcium silicate bioactive ceramics. Biomaterials. 2013;34:10028–42.
Liu CH, Huang TH, Hung CJ, Lai WY, Kao CT, Shie MY. The synergistic effects of fibroblast growth factor-2 and mineral trioxide aggregate on an osteogenic accelerator in vitro. Int Endod J. 2014;47:843–53.
Hung CJ, Kao CT, Shie MY, Huang TH. Comparison of host inflammatory responses between calcium-silicate base material and intermediate restorative material. J Dent Sci. 2014;9:158–64.
Shie MY, Ding SJ, Chang HC. The role of silicon in osteoblast-like cell proliferation and apoptosis. Acta Biomater. 2011;7:2604–14.
Liu CH, Hung CJ, Huang TH, Lin CC, Kao CT, Shie MY. Odontogenic differentiation of human dental pulp cells by calcium silicate materials stimulating via FGFR/ERK signaling pathway. Mater Sci Eng C Mater Biol Appl. 2014;43:359–66.
Zhou Y, Wu C, Xiao Y. Silicate-based bioceramics for periodontal regeneration. J Mater Chem B. 2014;2:3907.
Chen CL, Kao CT, Ding SJ, Shie MY, Huang TH. Expression of the inflammatory marker cyclooxygenase-2 in dental pulp cells cultured with mineral trioxide aggregate or calcium silicate cements. J Endod. 2010;36:465–8.
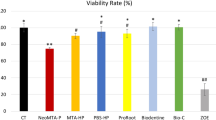
Wei W, Qi Y, Nikonov SY, Niu L, Messer RLW, Mao J, et al. Effects of an experimental calcium aluminosilicate cement on the viability of murine odontoblast-like cells. J Endod. 2012;38:936–42.
Bohner M. Silicon-substituted calcium phosphates—a critical view. Biomaterials. 2009;30:6403–6.
Li H, Chang J. Bioactive silicate materials stimulate angiogenesis in fibroblast and endothelial cell co-culture system through paracrine effect. Acta Biomater. 2013;9:6981–91.
Kang Y, Kim SH, Fahrenholtz M, Khademhosseini A, Yang YJ. Osteogenic and angiogenic potentials of monocultured and co-cultured human-bone-marrow-derived mesenchymal stem cells and human-umbilical-vein endothelial cells on three-dimensional porous beta-tricalcium phosphate scaffold. Acta Biomater. 2013;9:4906–15.
Chen Z, Wu C, Gu W, Klein T, Crawford R, Xiao Y. Osteogenic differentiation of bone marrow MSCs by β-tricalcium phosphate stimulating macrophages via BMP2 signalling pathway. Biomaterials. 2014;35:1507–18.
Schröder HC, Wang XH, Wiens M, Diehl-Seifert B, Kropf K, Schloßmacher U, et al. Silicate modulates the cross-talk between osteoblasts (SaOS-2) and osteoclasts (RAW 264.7 cells): inhibition of osteoclast growth and differentiation. J Cell Biochem. 2012;113:3197–206.
Holt DJ, Chamberlain LM, Grainger DW. Cell–cell signaling in co-cultures of macrophages and fibroblasts. Biomaterials. 2010;31:9382–94.
Schutte RJ, Xie L, Klitzman B, Reichert WM. In vivo cytokine-associated responses to biomaterials. Biomaterials. 2009;30:160–8.
Hsu TT, Yeh CH, Kao CT, Chen YW, Huang TH, Yang JJ, et al. Antibacterial and odontogenesis efficacy of mineral trioxide aggregate combined with CO2 laser treatment. J Endod. 2015;41:1073–80.
Wu BC, Kao CT, Huang TH, Hung CJ, Shie MY, Chung HY. Effect of verapamil, a calcium channel blocker, on the odontogenic activity of human dental pulp cells cultured with silicate-based materials. J Endod. 2014;40:1105–11.
Su YF, Lin CC, Huang TH, Chou MY, Yang JJ, Shie MY. Osteogenesis and angiogenesis properties of dental pulp cell on novel injectable tricalcium phosphate cement by silica doped. Mater Sci Eng C Mater Biol Appl. 2014;42:672–80.
Kao CT, Shie MY, Huang TH, Ding SJ. Properties of an accelerated mineral trioxide aggregate-like root-end filling material. J Endod. 2009;35:239–42.
Correa D, Almirall A, García-Carrodeguas R, Alberto Dos Santos L, De Aza AH, Parra J, et al. β-Dicalcium silicate-based cement: synthesis, characterization and in vitro bioactivity and biocompatibility studies. J Biomed Mater Res, Part A. 2013;102:3693–703.
Silva EJNL, Rosa TP, Herrera DR, Jacinto RC, Gomes BPFA, Zaia AA. Evaluation of cytotoxicity and physicochemical properties of calcium silicate-based endodontic sealer MTA fillapex. J Endod. 2013;39:274–7.
Torabinejad M, Parirokh M. Mineral trioxide aggregate: a comprehensive literature review—Part II: leakage and biocompatibility investigations. J Endod. 2010;36:190–202.
Eid AA, Niu L, Primus CM, Opperman LA, Pashley DH, Watanabe I, et al. In vitro osteogenic/dentinogenic potential of an experimental calcium aluminosilicate cement. J Endod. 2013;39:1161–6.
Lai WY, Chen YW, Kao CT, Hsu TT, Huang TH, Shie MY. Human dental pulp cells responses to apatite precipitation from dicalcium silicates. Materials. 2015;8:4491–504.
Hung CJ, Kao CT, Chen YJ, Shie MY, Huang TH. Antiosteoclastogenic activity of silicate-based materials antagonizing receptor activator for nuclear factor kappaB ligand–induced osteoclast differentiation of murine marcophages. J Endod. 2013;39:1557–61.
Henriksen K, Neutzsky-Wulff AV, Bonewald LF, Karsdal MA. Local communication on and within bone controls bone remodeling. Bone. 2009;44:1026–33.
Wada T, Nakashima T, Hiroshi N, Penninger JM. RANKL–RANK signaling in osteoclastogenesis and bone disease. Trends Mol Med. 2006;12:17–25.
Hung CJ, Hsu HI, Lin CC, Huang TH, Wu BC, Kao CT, et al. The role of integrin αv in proliferation and differentiation of human dental pulp cell response to calcium silicate cement. J Endod. 2014;40:1802–9.
Müller WEG, Wang X, Diehl-Seifert B, Kropf K, Schloßmacher U, Lieberwirth I, et al. Inorganic polymeric phosphate/polyphosphate as an inducer of alkaline phosphatase and a modulator of intracellular Ca2+ level in osteoblasts (SaOS-2 cells) in vitro. Acta Biomater. 2011;7:2661–71.
Wiens M, Wang X, Schröder HC, Kolb U, Schloßmacher U, Ushijima H, et al. The role of biosilica in the osteoprotegerin/RANKL ratio in human osteoblast-like cells. Biomaterials. 2010;31:7716–25.
Huang MH, Kao CT, Chen YW, Hsu TT, Shieh DE, Huang TH, et al. The synergistic effects of chinese herb and injectable calcium silicate/b-tricalcium phosphate composite on an osteogenic accelerator in vitro. J Mater Sci Mater Med. 2015;26:161.
Hsieh WH, Chen YJ, Hung CJ, Huang TH, Kao CT, Shie MY. Osteogenesis differentiation of human periodontal ligament cells by CO2 laser-treatment stimulating macrophages via BMP2 signalling pathway. Laser Phys. 2014;24:115607.
Nomura K, Yamaguchi M, Abiko Y. Inhibition of interleukin-1beta production and gene expression in human gingival fibroblasts by low-energy laser irradiation. Lasers Med Sci. 2001;16:218–23.
Lai WY, Kao CT, Hung CJ, Huang TH, Shie MY. An evaluation of the inflammatory response of lipopolysaccharide-treated primary dental pulp cells with regard to calcium silicate-based cements. Int J Oral Sci. 2014;6:94–8.
Hsu TT, Kao CT, Chen YW, Huang TH, Yang JJ, Shie MY. The synergistic effects of CO2 laser treatment with calcium silicate cement of antibacterial, osteogenesis and cementogenesis efficacy. Laser Phys Lett. 2015;12:055602.
Chen Z, Mao X, Tan L, Friis T, Wu C, Crawford R, et al. Osteoimmunomodulatory properties of magnesium scaffolds coated with β-tricalcium phosphate. Biomaterials. 2014;35:8553–65.
Jensen ED, Pham L, Billington CJ, Espe K, Carlson AE, Westendorf JJ, et al. Bone morphogenic protein 2 directly enhances differentiation of murine osteoclast precursors. J Cell Biochem. 2010;109:672–82.
Huang SC, Wu BC, Kao CT, Huang TH, Hung CJ, Shie MY. Role of the p38 pathway in mineral trioxide aggregate-induced cell viability and angiogenesis-related proteins of dental pulp cell in vitro. Int Endod J. 2015;48:236–45.
Acknowledgments
The authors acknowledge receipt of a grant from the Ministry of Science and Technology grants (MOST 102-2314-B-039-014) of Taiwan.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Additional information
Ming-Gene Tu and Yi-Wen Chen have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Tu, MG., Chen, YW. & Shie, MY. Macrophage-mediated osteogenesis activation in co-culture with osteoblast on calcium silicate cement. J Mater Sci: Mater Med 26, 276 (2015). https://doi.org/10.1007/s10856-015-5607-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10856-015-5607-z