Abstract
Rapid and efficient animal models are needed for evaluating the effectiveness of many new candidate bone regenerative materials. We developed an in vivo model screening for calvarial bone regeneration in lipopolysaccharide (LPS)-treated mice, in which materials were overlaid on the periosteum of the calvaria in a 20 min surgery and results were detectable in 1 week. Intraperitoneal LPS injection reduced spontaneous bone formation, and local application of basic fibroblast growth factor (bFGF) increased the bone-forming activities of osteoblasts. A novel synthetic collagen gel, alkali-treated collagen (AlCol) cross-linked with trisuccinimidyl citrate (TSC), acted as a reservoir for basic substances such as bFGF. The AlCol–TSC gel in conjunction with bFGF activated osteoblast activity without the delay in osteoid maturation caused by bFGF administration alone. The AlCol–TSC gel may slow the release of bFGF to improve the imbalance between osteoid formation and bone mineralization. These findings suggest that our model is suitable for screening bone regenerative materials and that the AlCOl–TSC gel functions as a candidate reservoir for the slow release of bFGF.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
Rodents with cranial defects are generally used as in vivo models for regeneration of craniofacial bone tissue [1, 2]. These models are considered to be the most reliable for investigating the effectiveness of materials for repairing membranous bone. However, it takes several months to repair bone defects, and it requires some skill to prepare such calvarial models without damaging the dura and the underlying brain and rodent survival is essential for evaluation. Spontaneous bone formation from cranial defects can make it difficult to determine the efficiency of bone regenerative materials. Furthermore, the scaffold, a spacer that causes probably more harm than use in the protease rich environment of a large defect, may render cytokines such as FGF inactive.
Many candidate bone regenerative materials have recently been introduced. Efficient and short-term animal models are needed for screening these candidate materials such that only promising candidates are investigated further. Lipopolysaccharide (LPS) is a well-known endotoxin that plays an important role in the progression of bone-resorptive diseases such as periodontitis [3]. By reducing spontaneous bone formation in calvaria, LPS can improve recognition of the bone regenerative effects of materials. Herein, we present an in vivo model for screening bone regenerative materials in LPS-treated mice, in which materials were overlaid on the periosteum of the calvaria. We have used this model to demonstrate the effects of a novel synthetic collagen gel, alkali-treated collagen (AlCol) cross-linked with trisuccinimidyl citrate (TSC), on bone function [4]. The AlCol–TSC gel was used in conjunction with basic fibroblast growth factor (bFGF), a well-known bone-forming growth factor in vivo [5].
2 Materials and methods
2.1 Materials
AlCol derived from pig tissues was provided by Nitta Gelatin Inc. (Osaka, Japan). Citric acid (CA), N-hydroxysuccinimide (HOSu), tetrahydrofuran (THF), dimethyl sulfoxide (DMSO), ethanol, tert-butyl alcohol, HCl, acetic acid, 2-[4-(2-hydroxyethyl)-1-piperazinyl]ethanesulfonic acid, 10 % formalin solution, NaOH, and methyl methacrylate were purchased from Wako Pure Chemical Industrials Ltd. (Osaka, Japan). Dicyclohexylcarbodiimide (DCC) was purchased from Kokusan Chemical Co., Ltd. (Tokyo, Japan). LPS from Salmonella minnesota was purchased from Sigma-Aldrich (MO, USA). Recombinant human bFGF was purchased from R&D systems (MN, USA).
2.2 Preparation of the AlCol–TSC gel
TSC was prepared by previously reported methods [4, 6]. In brief, CA was first dissolved in THF, and then HOSu and DCC were added. The resulting mixture was stirred for 30 min and then concentrated with rotary evaporation under reduced pressure to remove THF. The final mixture was recrystallized in ethanol to yield pure TSC. Characterization of the resulting TSC was performed using 1H-NMR spectroscopy (JEOL EX-300) and elemental analysis as follows: TSC: 1H-NMR (DMSO-d6) d = 2.8 (s, 12H, succinimidyl ester’s CH2 × 6), 3.4 (s, 4H, CH2 × 2), 7.2 (s, 1H, OH). C18H17N3O13: Calcd. C 44.73, H 3.55, N 8.69; Found C 44.83, H 3.45, N 8.58.
AlCol (30 % w/v) was first dissolved in DMSO, and then 30 mM TSC solution was added. The mixture was stirred and placed in a mold with a 0.5-mm-thick silicone rubber spacer between two glass plates for 24 h at 37 °C. The AlCol–TSC gel was subsequently immersed in excess pure water for 48 h at 37 °C to remove DMSO from the AlCol–TSC matrices.
The AlCol–TSC gel was gently dried to remove excess moisture and immersed in 20 μl (29 μg) of bFGF or the bFGF solvent [10 mM sodium phosphate and 0.3 M glycerol (pH 7.0) containing 50 μg of bovine serum albumin] overnight. The total amount of bFGF or solvent was absorbed into the AlCol–TSC gel.
2.3 ELISA for bFGF released from the AlCol–TSC gel
The AlCol–TSC gel was immersed overnight in 20 μl (29 μg) of bFGF, then transferred to 20 μl of PBS, and incubated at 37 °C for 7 days. The gel was transferred to fresh PBS again at 1, 3, 12, 24, 48 and 96 h. bFGF in PBS was quantified using a bFGF ELISA kit (R&D) according to the manufacturer’s instructions.
2.4 Animals
After measuring the body weight, LPS (10 mg/kg body weight) was injected intraperitoneally in 7-week-old BALB/c mice just before the surgery. Prior to the main experiments, 12 LPS-injected mice were weighed at 0, 1, and 2 week to determine the systemic effects of LPS. These mice were sacrificed after 14 days. In every group of the main experiments, skin incision was made and skin flaps were raised under anesthesia induced by injection with pentobarbital (50 mg/kg weight).
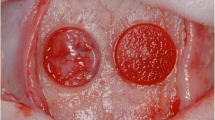
After incision of the calvarial skin, the AlCol–TSC gel (3 mm diameter) with or without bFGF was overlaid on the periosteum of the calvaria of LPS-treated mice (n = 8 or 7, respectively). In a second experimental group, 20 μl of bFGF was injected between the skin and the periosteum of the calvaria after incision (n = 7). The third experimental group was the control calvaria without gel or local bFGF application (n = 6). Sufficient exfoliation of skin around the incision was performed in order to suture the wound without tension, which may cause physical damage to calvaria. Mice were sacrificed after 1 week and used for histological analysis. All animal experiments were performed according to the guidelines of the International Association for the Study of Pain [7]. In addition, the experimental protocol was reviewed and approved by the Animal Care Committee of the University of Tokyo.
The calvaria were removed from the mice and fixed with 70 % ethanol. They were stained with Villanueva bone stain for 7 days, dehydrated in ascending grades of ethanol, defatted in an acetone/methyl methacrylate monomer mixture (1:2), and embedded in methyl methacrylate without decalcification. Cross sections (200 μm thick) were ground to a thickness of 15 μm.
Some tissue samples were fixed overnight in formalin and then decalcified in 10 % EDTA for 7 days. After the decalcification was complete, the tissues were embedded in paraffin using a standard procedure and sectioned into 5 μm slices, and the sections were deparaffinized and stained with hematoxylin and eosin.
Bone histomorphometric measurements of the calvaria without decalcification were performed using a semiautomatic image analyzing system (System Supply, Nagano, Japan) and a fluorescent microscope (Optiphot; Nikon, Tokyo, Japan) set at a magnification of 200×. Bone histomorphometric measurements are validated in the analysis of bone metabolism, and the standard bone histomorphometrical nomenclature, symbols, and units are according to the report of the ASBMR Histomophometry Nomenclature Committee [8]. The outer membranes of calvaria were used for measuring the direct effects of materials on bone.
2.5 Statistical analysis
All results are expressed as mean ± SD. Statistical analysis was performed with GraphPad Prism Software ver.5.0. The statistical significance of differences among more than three groups was determined by the Tukey’s post t test. The statistical significance of differences between two groups was determined by the two-tailed Student’s t test. Differences were considered statistically significant at P values of <0.05.
3 Results
3.1 Characterization of AlCol–TSC gel
We have previously reported the general characterization of AlCol–TSC gel [4, 9]. TSC can cross-link biopolymers such as collagen and exhibits cytocompatibility [4]. The amounts of residual carboxyl groups in AlCol gels increase with increasing TSC concentrations [4, 9]. Other properties such as pH-responsive swelling behavior of AlCol–TSC gel is also recognized [9].
The release of bFGF from the AlCol–TSC gel is shown in Fig. 1. The release rate, i.e., the slope of the percentage of cumulative release, was the greatest from 0 to 1 h. A certain amount of bFGF was still released from 1 to 48 h. Therefore, it is suggested that bFGF in the AlCol–TSC gel that was overlaid on the mouse calvaria may be released for a longer duration compared with injected bFGF. A total of 30 % of the initially loaded bFGF remained in the AlCol–TSC gel after 1 week, and this bFGF is expected to be available after degradation of the AlCol–TSC gel in vivo.
3.2 Effects of LPS on murine calvaria
Mouse body weights were used to determine the systemic effects of LPS. All mice survived after LPS injection. Most mice lost body weight 7 days after LPS injection, but all regained the weight after 14 days. These findings suggested that LPS has only temporary systemic effects.
We next examined the effects of the intraperitoneal LPS injection on bone formation. In the mice injected with phosphate buffer saline (PBS) injection instead of LPS, the osteoid thickness (O.Th) and bone formation rate per bone surface (BFR/BS) on the outer membranes of calvaria were 3.65 ± 0.39 mcm and 0.44 ± 0.06 mm3/mm2/year, respectively (Fig. 2a, b), indicating that spontaneous bone formation had occurred. The osteoblast surface per unit of bone surface (Ob.S/BS) was 21.65 ± 23.56 %, with the high SD indicating substantial individual differences among the specimens (Fig. 2c). No osteoclast was observed (Fig. 2d), showing that bone resorption had not occurred. On the outer membranes of calvaria from the LPS-injected mice, the O.Th and BFR/BS were 2.95 ± 0.43 mcm and 0.35 ± 0.04 mm3/mm2/year, respectively (Fig. 2a, b). The Ob.S/BS was 7.93 ± 3.19 % and appeared to be reduced compared with the PBS-injected mice (Fig. 2c), although the wide range of values from the PBS-injected mice obscured any differences. Similar to the PBS-injected mice, no osteoclast was observed on the outer membranes of the calvaria (Fig. 2d). These findings demonstrated that intraperitoneal LPS injection reduces spontaneous uneven bone formation without enhancing bone resorption, indicating that this model would be useful for investigating the bone-forming effects of materials without bone resorption.
Histomorphometric analysis of the outer membranous region of the calvaria in lipopolysaccharide (LPS)- and PBS-injected mice. The osteoid thickness (O.Th); a bone formation rate per unit of bone surface (BFR/BS); b osteoblast surface per unit of bone surface (Ob.S/BS); c and number of multinuclear osteoclasts per unit of bone surface (N.Mu.Oc/BS); d are shown. −, mice injected with PBS; +, mice injected with LPS; *P < 0.05 versus mice injected with PBS (n = 6/group)
3.3 Effects of bFGF on bone formation in the LPS-treated mouse calvaria
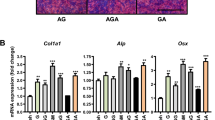
We examined the effects of local application of bFGF without a gel on bone formation to verify the effectiveness of our model. The O.Th and Ob.S/BS of the mouse calvaria with bFGF application after LPS injection increased more than those of the control calvaria without local bFGF application (Fig. 3a, b). Osteoid maturation time (Omt) of the bFGF-treated calvaria also increased more than that of the control calvaria (Fig. 3c). The BFR/BS of the bFGF-treated calvaria was similar to that of the control (Fig. 3d). The number of multinuclear osteoclasts per unit of bone surface (N.Mu.O/BS) of the bFGF-treated calvaria was not significantly different from that of the control (Fig. 3e). These results showed that bFGF increases the number of osteoblasts, but not osteoclasts, and stimulates osteoid production. Thus, bFGF did not enhance the bone formation rate (the rate of bone mineralization), and osteoid maturation was delayed.
Histomorphometric analysis of the outer membranous region of the calvaria from LPS-injected mice with and without basic fibroblast growth factor (bFGF) and/or alkali-treated collagen–trisuccinimidyl citrate (AlCol–TSC) gel. Control, no overlaid material; Gel, overlaid alkali-treated collagen–trisuccinimidyl citrate (AlCol–TSC) gel without basic fibroblast growth factor (bFGF); FGF, bFGF applied alone; Gel+FGF, AlCol–TSC gel with bFGF; O.Th, osteoid thickness (a); Ob.S/BS, osteoblast surface per unit of bone surface (b); Omt, maturation time (c); BFR/BS, bone formation rate per unit of bone surface (d); N.Mu.Oc/BS, number of multinuclear osteoclasts per unit of bone surface (e); Po.Ar/Tt.Cr, porosity area per total cranium (f); *P < 0.05 versus control; # P < 0.05 versus groups indicated by bars (n = 6–8/group)
3.4 Effects of the AlCol–TSC gel with or without bFGF on bone formation in LPS-treated mouse calvaria
The O.Th, Ob.S/BS, Omt, BFR/BS, and N.Mu.O/BS of the calvaria with the overlain AlCol–TSC gel without bFGF did not differ significantly from those of the control (Fig. 3a–e, respectively). The porosity area per total core (Po.Ar/Tt.Cr) of the AlCol–TSC gel-overlain calvaria increased more than that of the control calvaria (Fig. 3f), without affecting the bone-forming activity.
In contrast, the O.Th and Ob.S/BS of the mouse calvaria with the overlaid AlCol–TSC gel with bFGF increased more than those of the control calvaria (Fig. 3a, b). The Ob.S/BS and Omt were decreased compared with those of the mouse calvaria with bFGF alone (Fig. 3b, c). In particular, Omt was reduced to the control level. BFR/BS and N.Mu.O/BS did not differ significantly from those of the control (Fig. 3d, e).
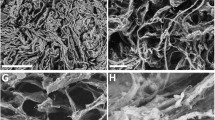
It has been reported that four types of osteoblasts occur in a regular sequence that correlates with osteoid thickness [10]. Among these, type I cells are preosteoblasts, and their presence adjacent to osteoid is considered to be an artifact of sectioning obliquity. There were few osteoblasts and a thin osteoid in the control calvaria (Ob.S/BS, 7.93 ± 3.09 %; O.Th, 2.95 ± 0.43 mcm; Figs. 3a and b, 4, upper left). Type IV osteoblasts, which are lining osteoblasts characterized by extremely thin cytoplasm, and a thin osteoid appeared in the calvaria with the overlain AlCol–TSC (Fig. 4, upper right). Type II osteoblasts, which are active osteoblasts characterized by cuboidal shapes with nuclear clear zones, and a thick osteoid appeared in the calvaria to which bFGF had been applied locally after LPS injection (Fig. 4, lower left). Type III osteoblasts, which are active osteoblasts characterized by columnar shapes without a nuclear clear zone, and a rather thick osteoid appeared in the calvaria with the overlain AlCol–TSC gel with bFGF (Fig. 4, lower right). These results suggested that activated osteoblasts play a role in osteoid production.
Representative images of osteoblasts on the calvaria. Arrowheads and arrows indicate osteoblasts and osteoid, respectively. Note the differences in the types of osteoblasts and osteoid thickness among the experimental groups. Control, no overlaid material; Gel, overlaid AlCol–TSC gel bFGF; FGF, bFGF applied alone; Gel+FGF, AlCol–TSC gel with bFGF; bar, 10 μm
To evaluate the animal model, we observed our model for long-term period. We measured the width of the calvarial bone including the osteoid zone (the distance from the outer surface to the inner surface of the calvaria at a point 2 mm away from the cranial suture, where the bone-forming effects seemed the most obvious) using decalcified specimens from LPS-injected mice to identify the basal phenotype of the bone from mice sacrificed after 1 week and after 3 weeks. Although the calvarial width measured using the decalcified specimens is not officially included in the parameters of bone morphometry, where specimens without decalcification are normally used, we believe that it is a convenient method of determining the basal phenotype of the bone. As shown in Fig. 5a, we found a significant difference in the calvarial width between the calvaria overlaid with the AlCol–TSC gel without bFGF (n = 7) and that overlaid with the AlCol–TSC gel with bFGF (n = 8) in mice sacrificed after 1 week. However, no difference was observed in the calvarial width between the mouse calvaria overlaid with the AlCol–TSC gel without bFGF (n = 6) and that overlaid with the AlCol–TSC gel with bFGF (n = 7) in mice sacrificed after 3 weeks (Fig. 5b). Based on the variability in the calvarial width in mice sacrificed after 3 weeks, the difference was found to be insignificant. These findings suggest that the data from mice sacrificed after 1 week are more reliable than those after 3 weeks. The variability in the calvarial width in mice sacrificed after 3 weeks may be due to reactivation of the unsteady spontaneous bone remodeling because of the lack of LPS effects after 3 weeks.
The distance from the outer surface to the inner surface at a point 2 mm away from the cranial suture (where the bone-forming effects seemed the most obvious) of the calvaria overlaid with the AlCol–TSC gel with and without bFGF from LPS-injected mice −, without bFGF; +, with bFGF. After 1 week of LPS injection a; after 3 weeks of LPS injection b; *P < 0.05 versus the group overlaid with the gel without bFGF (n = 6–8/group)
4 Discussion
Many candidate bone regenerative materials are being introduced, and each material must be examined for appropriate physical properties such as rigidity. Furthermore, the proper combination of materials must be selected. Thus, an efficient screening method for bone regenerative materials is desirable. The proposed model for screening cranial bone regenerative materials is an easy and time-saving method for narrowing the candidate bone regenerative materials. Although models of rodents with cranial defects are reliable for studying bone regenerative materials [1, 2], the surgical procedure takes approximately 30 min, with approximately 2 h of perioperative care for each animal, and several months are required to detect the repair of bone defects [2]. Local injection of liquid growth factors such as bFGF over the rodent calvaria is sometimes used to investigate the effects of growth factors on bone formation [11], and this is a simple procedure. Applying solid material on bone requires incising the skin and laying the material; Separation of the periosteum from the calvarial bone leads to injury of osteoblasts in the periosteum most adjacent to the bone. However, it is easy to apply the material on the calvaria covered with periosteum when there is sufficient exfoliation of skin around the incision with the periosteum remaining intact. Both liquid and solid materials can be in contact with intact osteoblasts from outside of the osteoblast lineage. Taken together, our model appears to be appropriate for the initial screening of bone regenerative materials prior to critical investigations using models of calvarial bone defects in rodents and/or larger animals that are more closely related to humans in size and bone characteristics.
LPS, a major constituent of gram-negative bacteria, has been suggested to be a potent stimulator of bone loss in inflammatory bone diseases such as periodontitis, osteomyelitis, and bacterial arthritis [3]. LPS stimulates osteoblasts to secrete factors such as interleukin (IL)-1, IL-6, and prostaglandin E2, and LPS-induced production of these factors by osteoblasts may be involved in the mechanism of bone resorption [12]. In contrast, osteoclast differentiation is counterintuitive because direct LPS stimulation on osteoclast precursors inhibits receptor activator of nuclear factor kappa-B ligand-mediated osteoclastogenesis [3, 13]. In our model, intraperitoneal LPS injection decreased spontaneous uneven calvarial bone formation without enhancing bone resorption compared with PBS injection. It is important to decrease spontaneous variant formation for judging the net bone forming effects of materials. It is not known whether this is a result of the lack of osteoclasts on the calvaria or a result of the indirect effects of systemically administered LPS. In either case, this model should be useful for screening the bone-forming effects of materials.
An in vivo rodent model, in which bone formation is precisely restrained, is often used to investigate the effects of growth factors or materials on bone metabolism. For example, the effects of bFGF on bone formation was reported in a diabetic rodent model [14], and bone anabolic effects of bFGF were investigated in ovariectomized rats [15]. Vascular endothelial growth factor scaffolds enhanced angiogenesis and bone regeneration in irradiated osseous defects [16]. Thus, LPS-injected models appear to be appropriate for the investigation of bone formation.
bFGF has been reported to have both stimulatory and inhibitory effects on bone formation in vitro [5]. FGF increases proliferation of immature osteoblasts, whereas FGF signaling inhibits expression of alkaline phosphatase and blocks mineralization in differentiated osteoblasts [5, 17]. In contrast, multiple studies have shown that FGF signaling enhances bone formation in vivo [5, 14, 18, 19]. Local application of bFGF with or without the careers for bone damage has been reported to have the osteogenic properties both in animal models [14, 18] and in human patients [19]. Our results demonstrate that local administration of bFGF remarkably increases osteoid thickness and the number of osteoblasts, but does not change the rate of bone mineralization within the period observed. Bone mineralization lags behind osteoid production, occurring at a distance of 8–10 μm from the osteoblasts [20]. Delayed osteoid maturation by local administration of bFGF may be due to the imbalance between osteoid production and bone mineralization.
We previously reported that the AlCol–TSC gel has effects on neovascular ingrowth [21, 22], wound healing [23], and antithrombotics [6]. The AlCol–TSC gel is able to retain its scaffold structure and act as a reservoir of bFGF [21, 22]. bFGF can be physically absorbed into the matrix of this composite. Furthermore, positively charged bFGF can form ionic bonds with the negatively charged AlCol–TSC gel [24], thereby fixing bFGF inside the gel. Therefore, bFGF would be physically released from the matrix at first, and it would be then released gradually as this composite degrades in vivo. In our model, AlCol–TSC gel appeared to act as a reservoir of bFGF and to enhance bone formation. This slow-release system using a reservoir may be very beneficial because it enables bFGF to exert its activities locally for a long period and induce anabolic effects on tissues including bone [18]. In our model, the combination of the AlCol–TSC gel and bFGF increases osteoid thickness and the number of osteoblasts without delaying osteoid maturation. The balance between osteoid production and mineralization may be moderated by this slow-release bFGF system.
The AlCol–TSC gel itself may have a biological effect on bone. AlCol–TSC gels increase the porosity of calvaria without changing the bone-forming activity. This increase in Po.Ar/Tt.Cr does not necessarily mean a reduction in bone strength when bone-forming activity is maintained. The porous body serves as a cushion that reduces shock due to impact [25]. At a minimum, the AlCol–TSC gel does not have inhibitory effects on bone formation.
Taken together, our results demonstrated within a 1 week experimental period that the AlCol–TSC gel may act as a reservoir for bFGF and that the slow release of bFGF may improve the imbalance between osteoid formation and bone mineralization, resulting in appropriate bone formation. With these results, we can undertake critical investigations using rodent models of calvarial bone defects and/or large animal models. Our findings suggest that this model is appropriate for screening bone regenerative materials.
5 Conclusions
We have demonstrated an efficient in vivo murine model for screening cranial bone-regenerative materials. This model should be useful for investigating the bone-forming effects of materials.
We also created a gel consisting of alkali-treated collagen and cross-linked trisuccinimidyl citrate. In vivo evaluation using our model showed that the combination of the AlCol–TSC gel and bFGF induced bone-forming activities without delaying osteoid maturation at 1 week after the surgery. These findings suggest that the AlCol–TSC gel functions as a reservoir of bFGF.
References
Takagi K, Urist M. The reaction of the dura to bone morphogenetic protein (BMP) in repair of skull defects. Ann Surg. 1982;196:100–9.
Spicer PP, Kretlow JD, Young S, Jansen JA, Kasper FK, Mikos AG. Evaluation of bone regeneration using the rat critical size calvarial defect. Nat Protocols. 2012;7:1918–29.
Lorenzo J, Horowitz M, Choi Y. Osteoimmunology: interactions of the Bone and Immune System. Endocr Rev. 2008;29:403–40.
Taguchi T, Saito H, Uchida Y, Sakane M, Kobayashi H, Kataoka K, et al. Bonding of soft tissues using a novel tissue adhesive consisting of a citric acid derivative and collagen. Mater Sci Eng, C. 2004;24:775–80.
Towler D. Fibroblast growth factor (FGF) and FGF families in bone. In: Bilezikian J, Raisz L, Martin T, editors. Principles of bone biology. 3rd edn., vol 2 San Diego: Academic Press; 2008. p. 1103–1132.
Inoue M, Sasaki M, Nakasu A, Takayanagi M, Taguchi T. An antithrombogenic citric acid-crosslinked gelatin with endothelialization activity. Adv Healthc Mater. 2012;1:573–81.
Zimmermann M. Ethical guidelines for investigations of experimental pain in conscious animals. Pain. 1983;16:109–10.
Parfitt A, Drezner M, Glorieux F, Kanis J, Malluche H, Meunier P, et al. Bone histomorphometry: standardization of nomenclature, symbols, and units. Report of the ASBMR Histomorphometry Nomenclature Committee. J Bone Miner Res. 1987;2:595–610.
Saito H, Taguchi T, Aoki H, Murabayashi S, Mitamura Y, Tanaka J, et al. pH-responsive swelling behavior of collagen gels prepared by novel crosslinkers based on naturally derived di- or tricarboxylic acids. Acta Biomater. 2007;3:89–94.
Villanueva A, Mathews C, Parfitt A. Relationship between the size and shape of osteoblasts and the width of osteoid seams in bone. In: Takahashi H, editor. Handbook of bone morphometry. 1st ed. Niigata: Nishimura; 1983. p. 191–6.
Morinobu M, Nakamoto T, Hino K, Tsuji K, Shen Z-J, Nakashima K, et al. The nucleocytoplasmic shuttling protein CIZ reduces adult bone mass by inhibiting bone morphogenetic protein-induced bone formation. J Exp Med. 2005;201:961–70.
Kikuchi T, Matsuguchi T, Tsuboi N, Mitani A, Tanaka S, Matsuoka M, et al. Gene expression of osteoclast differentiation factor is induced by lipopolysaccharide in mouse osteoblasts via toll-like receptors. J Immunol. 2001;166:3574–9.
Takami M, Kim N, Rho J, Choi Y. Stimulation by toll-like receptors inhibits osteoclast differentiation. J Immunol. 2002;169:1516–23.
Kawaguchi H, Kurokawa T, Hanada K, Hiyama Y, Tamura M, Ogata E, et al. Stimulation of fracture repair by recombinant human basic fibroblast growth factor in normal and streptozotocin-diabetic rats. Endocrinology. 1994;135:774–81.
Liang H, Pun S, Wronski TJ. Bone anabolic effects of basic fibroblast growth factor in ovariectomized rats. Endocrinology. 1999;140:5780–8.
Kaigler D, Wang Z, Horger K, Mooney D, Krebsbach P. VEGF scaffolds enhance angiogenesis and bone regeneration in irradiated osseous defects. J Bone Miner Res. 2006;21:735–44.
Mansukhani A, Bellosta P, Sahni M, Basilico C. Signaling by fibroblast growth factors (Fgf) and fibroblast growth factor receptor 2 (Fgfr2)-activating mutations blocks mineralization and induces apoptosis in osteoblasts. J Cell Biol. 2000;149:1297–308.
Tabata Y, Yamada K, Miyamoto S, Nagata I, Kikuchi H, Aoyama I, et al. Bone regeneration by basic fibroblast growth factor complexed with biodegradable hydrogels. Biomaterials. 1998;19:807–15.
Kawaguchi H, Oka H, Jingushi S, Izumi T, Fukunaga M, Sato K, et al. A local application of recombinant human fibroblast growth factor 2 for tibial shaft fractures: a randomized, placebo-controlled trial. J Bone Miner Res. 2010;25:2735–43.
Manolagas SC. Birth and death of bone cells: basic regulatory mechanisms and implications for the pathogenesis and treatment of osteoporosis. Endocr Rev. 2000;21:115–37.
Nagayoshi M, Taguchi T, Koyama H, Takato T, Miyata T, Nagawa H. Enhanced neovascular formation in a novel hydrogel matrix consisting of citric acid and collagen. Ann Vascular Dis. 2011;4:196–203.
Takayama T, Taguchi T, Koyama H, Sakari M, Kamimura W, Takato T, et al. The growth of a vascular network inside a collagen-citric acid derivative hydrogel in rats. Biomaterials. 2009;30:3580–7.
Chikazu D, Taguchi T, Koyama H, Hikiji H, Fujihara H, Suenaga H, et al. Improvement in wound healing by a novel synthetic collage-gel dressing in genetically diabetic mice. Asian J Oral Maxillofac Surg. 2010;22:61–7.
Saito H, Murabayashi S, Mitamura Y, Taguchi T. Unusual cell adhesion and antithrombogenic behavior of citric acid-cross-linked collagen matrices. Biomacromolecules. 2007;8:1992–8.
Ehlers W, Karajan N, Markert B. A porous media model describing the inhomogeneous behaviour of the human intervertebral disc. Materialwiss Werkstofftech. 2006;37:546–51.
Acknowledgments
This study was supported in part by the Industrial Technology Research Grant Program of the New Energy and Industrial Technology Development Organization (NEDO) of Japan. This work was also supported in part by Grants-in-Aid for Scientific Research from the Ministry of Education, Culture, Sports, Science and Technology of Japan (to H.H.).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hikiji, H., Tomizuka, K., Taguchi, T. et al. An in vivo murine model for screening cranial bone regenerative materials: testing of a novel synthetic collagen gel. J Mater Sci: Mater Med 25, 1531–1538 (2014). https://doi.org/10.1007/s10856-014-5185-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10856-014-5185-5