Abstract
Introduction
Definitive therapy of idiopathic right ventricular arrhythmias (VA) remains a challenge in interventional electrophysiology. The aim of this study was to evaluate the utility of EnSite Velocity system in the catheter ablation of RV tachycardia in children.
Methods
Thirty-five children with idiopathic right VA underwent catheter ablation procedure using the EnSite Velocity system guidance.
Results
The mean patient age was 12.0 ± 3.7 years and the mean patient weight was 43.6 ± 18.7 kg. The origin of right VA was divided into right ventricular outflow tract (RVOT) (30 patients) and other right ventricular localizations (five patients). The mean procedure and fluoroscopy times were 175 ± 67 min and 2.35 ± 1.89 min, respectively. No fluoroscopy was used in 19 patients. Acute success was achieved in 29 patients (83 %). The focus of VA was epicardial in three failed procedures. Cryocatheter (6-mm or 8-mm tip) was used in six patients, radiofrequency ablation (RFA) (4-mm or 8-mm tip) in 26 patients, and 4-mm tip irrigated RFA in three patients. During a mean follow-up of 15.9 ± 7.1 months, ventricular tachycardia recurred in six patients (20 %). There were three complications (transient atrioventricular block developed in one patient during parahissian cryoablation and two patients developed transient complete right bundle branch block).
Conclusions
Catheter ablation of idiopathic right VA in children can be performed safely and effectively with limited fluoroscopy using the EnSite Velocity system.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Idiopathic ventricular arrhythmia (VA) is a clinical entity observed in children and adults without any structural heart disease detected by conventional diagnostic evaluations. Idiopathic VA has been reported to have a good prognosis, but there is a small risk of sudden cardiac death or congestive heart failure [1]. Most of the data from the electrophysiological findings of idiopathic VA have been obtained from adult patients [2]. In children, the reported experience of catheter ablation using electroanatomical mapping systems in idiopathic VA is limited.
There are few studies of catheter ablation of idiopathic VA in pediatric populations [3–7]. These studies focused on outflow tract VAs. However, in this study, we report our experience of ablation of idiopathic right VAs using EnSite Velocity system to limit or eliminate radiation exposure. The aim of this study was to review the clinical picture of idiopathic VA and evaluate the efficacy and safety of catheter ablation therapy of idiopathic right VA using EnSite Velocity system in children.
2 Methods and materials
2.1 Study population
This is a single-center study performed in children with idiopathic right VA between July 2012 and January 2015. All patients underwent non-invasive cardiac evaluation including history (family history of sudden cardiac death), physical examination, resting 12-lead ECG, ECG-Holter recording, exercise test, and echocardiography before the procedure. Indications for ablation in children with idiopathic right VA were episodes of symptomatic ventricular tachycardia, frequent VA burden with ventricular dilation or dysfunction, VA in suspected arrhyhtmogenic cardiomyopathy, and VA increased or unsuppressed with exercise. Idiopathic VA was defined as VT or premature ventricular complexes (PVC) without structural heart disease or any identifiable predisposing causes [8]. VT was defined as three or more consecutive ventricular beats at a rate >120 bpm [9]. EnSite Velocity system (St. Jude Medical, St Paul, MN, USA) was used to facilitate mapping and to reduce or eliminate the fluoroscopy.
2.2 Electrophysiologic study and ablation
All patients and/or their legal guardians gave verbal and written consent for the procedure. Antiarrhythmic medications were discontinued at least five half-lives before electrophysiological procedure. Deep sedation without intubation using propofol infusion with occasional combinations of ketamine, midazolam, and meperidine were used during majority of the procedures. For adolescent patients, procedures were started with midazolam in order to prevent suppression of VA with deep sedative agents.
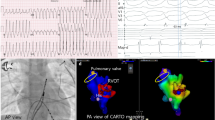
The procedure was started without using fluoroscopy by inserting a 7-Fr sheath into the right femoral vein and two 5- or 6-Fr sheaths into the left femoral veins. A steerable quadripolar catheter was positioned in the right atrium. Following electroanatomical reconstruction of cardiac anatomy including the right atrium and coronary sinus, a steerable decapolar catheter was inserted into the coronary sinus for a positional reference. All patients underwent a basic electrophysiological study. The 12-lead ECGs of all patients were reviewed for any ventricular ectopy and non-sustained or sustained VT in order to ensure that the targeted morphology was identical to the clinical morphology. Activation and pace mappings were utilized as needed. If spontaneous arrhythmia was not present during the procedure, appropriate pacing maneuvers (burst and programmed stimulations from both the atria and ventricle) and if necessary, orciprenaline bolus and dobutamine infusion at low doses (5 mg/kg/min) were used in some cases. The ablation site was chosen when local activation time preceded the surface QRS complex by 20–50 ms, and the QS morphology was with steep negative deflection was observed in the unipolar recording from the catheter tip (Fig. 1). In addition to three-dimensional activation mapping, pace mapping was also used during the electrophysiological study. Acute ablation success was defined as a lack of inducibility of VT or absence of ectopic beats with and without electrophysiologic stimulation and orciprenaline bolus immediately and 30 min after the last energy application. If the endpoints were achieved, the procedure was terminated and catheters were removed.
In regions in close proximity to the His bundle, cryoablation (Freezor Cryocath, Medtronic, Inc., Minneapolis, USA) was utilized. In other regions, radiofrequency energy (RF Mariner 4 mm and 8 mm catheters, Medtronic, Inc., Minneapolis, USA) was used. In patients with ineffective ablation with RFA and suspected epicardial origin, irrigated RF catheter ablation was used. Epicardial VA was suspected when there was a prolonged precordial maximum deflection index (MDI > 0.55) along with ineffective cryo or RF ablation result [10].
2.3 Follow-up
All patients underwent continuous telemetry monitoring, a 12-lead ECG, 24-h ECG-Holter, and if necessary echocardiography before they were discharged. All patients were hospitalized for 1 day following the ablation procedure. Patients were assessed at 10 days and 3 and 6 months after the procedure and then every 12 months. At each visit, 12-lead ECG and 24-h ECG-Holter recordings were performed.
2.4 Statistical analysis
Data were analyzed using SPSS software version 15.0 (SPSS, Chicago, IL, USA) and presented as mean ± standard deviation and median ± interquartile range in normal distributed and non-normal distributed patients, respectively. The distribution of the variables was analyzed with the Kolmogorov–Smirnow test.
3 Results
Demographic and clinical characteristics of the study population are depicted in Table 1. The mean patient age and weight were 12.0 ± 3.7 years and 43.6 ± 18.7 kg, respectively. Most of the patients were symptomatic and palpitation was the most common symptom (Table 1). Mean PVC burden in a 24-h ECG-Holter was 36 ± 10 %.
3.1 Electrophysiologic study and ablation
Idiopathic PVC/VT originated from the right ventricular outflow tract (RVOT) in 30 patients and from other RV regions in five patients. Four patients had epicardial origin of VA. Radiofrequency energy application was applied in the majority of patients (Table 2). Irrigated RF was used only in three patients. The median number of energy applications was 9.5 (min 1, max 34 lesions). Mean local early activation time was 35.1 ± 9.4 ms. Fluoroscopy was used in 16 patients and the mean fluoroscopy time was 2.35 ± 1.89 min. The mean procedure duration was 175 ± 67 min. Acute procedural success was achieved in 29 patients (83 %) (Table 2). There were three complications during the procedure: one was transient complete AV block during ablation of parahissian VA, and the other two were development of transient complete RBBB.
Ablation failed in six patients (Table 3). The location of VA was epicardial in 3 of 6 (50 %) failed procedures. In two patients, the origin of VA was adjacent to the His bundle and RF or irrigated RF ablation was not preferred to prevent injury to the bundle. In one patient, right ventricular outflow tract ablation failed and due to the age and weight (5 years, 20 kg) retrograde approach via aorta was not done to assess the possibility of left ventricular outflow tract focus. The majority of the patients with failed procedures were males (Table 3).
3.2 Follow-up
During a mean follow-up of 15.9 ± 7.1 months, VA recurred in six patients (20 %). Of the patients with recurrence, only one patient underwent repeated ablation with irrigated RF catheter; however, the rest of the patients (five patients) were treated with antiarrhythmic drugs.
4 Discussion
This study demonstrates that catheter ablation of idiopathic right VA in children can be performed with very low fluoroscopy exposure using an electroanatomical system guidance. In our study, fluoroscopy was used in only 16 patients and the mean fluoroscopy time was lower compared to what is reported in previous but not all studies [7, 13].
The incidence of VA in children is low (0.2–0.8 per 10,000 children in school-based heart screening) compared to that in adults and the most of the pediatric cases are idiopathic without an underlying heart disease [1, 11]. Most of the VAs originate from right ventricle in children. There are many studies of right ventricular tachycardia in adult patients, however relatively few data on the electrophysiological findings have been reported in pediatric patients. Catheter ablation is a therapeutic option with the possibility of complete elimination of the idiopathic VA. The largest VT study in pediatric patients was reported by Pfammatter et al. [1]. They concluded that most of the VA in children originated from the RVOT (70 %). In our study, similar to the literature, RVOT was the most common origin of idiopathic right VA (85 %). Acute and chronic success rate of ablation varies in pediatric patients. With conventional and electroanatomical mapping systems, acute success rate of ablation varies between 60 and 90 % [3–7, 12]. The earliest data were reported by Smeets et al. [3] and in that study, ablation was performed in six children and was successful in 5 (83 %). Morwood et al. [12] reported a long-term success rate of catheter ablation of 60 % in children and young adults with idiopathic right and left VT using conventional mapping techniques. However, with the help of new mapping and ablation techniques, success rate has improved. Studies performed among children showed a success rate of 60 % with conventional ablation methods and up to 90 % with the use of electroanatomical mapping systems (EnSite and CARTO) [4–7, 12–14]. In our study, acute success rate was similar to the literature (acute procedural success of 83 %).
Acute success with non-contact mapping system is higher than both electroanatomical and conventional systems. Friedman et al. [15] reported successful ablation in 9 of 10 adult patients (90 %) with RVOT VT with non-contact mapping technique. Schneider and colleagues [4] also demonstrated a high acute success rate (94 %) in children. A comparative study between non-contact and conventional mapping in adults with RVOT VT demonstrated a higher success rate of 100 % with only one recurrence in the group treated with non-contact mapping versus 71.5 % acute success in the group in whom conventional mapping was performed [16]. However, in pediatric patients the main limitations of non-contact mapping are the requirement of a larger sheath, the need of careful anticoagulation and a large stiff-mapping balloon, all which lead to difficulty of application in younger children.
The main causes of failed VA ablation and high recurrence rates can be listed as follows: (a) the inability to find the critical ablation zone using conventional mapping due to lack of sufficient ventricular ectopy, (b) high-risk localization of VA origin near His region, (c) deep endocardial and epicardial localization of VA origin, (d) inability to perform ablation because of unstable VT, (e) multifocal origin in some patients, and (f) insufficient evaluation before the procedure in small number of patients who might have underlying disease like structural heart disease and/or genetic rhythm disorders. Some important clues to achieve higher success rate of ablation include the use of irrigated tip RF catheter, targeting unipolar electrocardiograms, epicardial access via subxiphoid puncture, and utility of electroanatomical systems. Of these clues, the usefulness of unipolar potential for targeting the successful ablation site has been demonstrated. QS-pattern V-uni is a simple, very useful sign, and should be closely scrutinized when determining the optimum target site. In patients with idiopathic outflow tachycardia, the incidence of a QS-pattern ventricular unipolar potential at the successful ablation sites was 100 % and at the unsuccessful sites was 25 %. Soejima and colleagues [17] found sensitivity and specificity of QS unipolar in RVOT patients as 100 and 89 %, respectively [17]. During our early experience, we did not use unipolar electrocardiograms for ablation of the idiopathic VT, thereby possibly reducing procedural success. In the last few years, we routinely use unipolar electrocardiograms.
In our study, the common feature of children with failed procedure was presence of male gender, near the His bundle localization, and epicardial origin. Tanaka and colleagues [18] demonstrated similar results in adult patients with idiopathic VA; they found gender and localization differences in terms of predictors of a successful catheter ablation. In a univariate analysis, female gender, in contrast to our study, and near the His bundle localization of VA were predictors of unsuccessful catheter ablation, however in the multivariate analysis, both findings did not reach statistical significance. Epicardial origin of VA is another important cause of unsuccessful ablation [18]. In an adult study performed by Tung et al. [19], acute success rate of epicardial ablation in patients with idiopathic ventricular arrhythmias was found as 50 %. Successful endocardial ablation was achieved in 3 of 6 patients with epicardial foci in our study. However, we did not attempt to proceed with epicardial ablation in the failed ones.
5 Limitations
Several limitations need to be mentioned. First, this is a single-center study with a small sample size of patients; however most of the pediatric studies reported have smaller sample sizes. Patients with VA comprise only about 1.8 % of children undergoing ablation; therefore it is difficult to obtain larger pediatric cohorts [20].
6 Conclusions
Catheter ablation of idiopathic VAs in pediatric population can be performed safely and effectively with very limited fluoroscopy using the EnSite Velocity system. Procedural success of epicardial origin or parahissian VA is substantially low and new procedural techniques (mapping and ablation) need to be improved.
References
Pfammater JP, Paul T. Idiopathic ventricular tachycardia in infancy and childhood: a multicenter study on clinical profile and outcome: working group on dysrhythmias and electrophysiology of the Association for European Pediatric Cardiology. J Am Coll Cardiol. 1999;33:2067–72.
Iwai S, Cantillon DJ, Kim RJ, et al. Right and left ventricular outflow tract tachycardias: evidence for a common electrophysiologic mechanism. J Cardiovasc Electrophysiol. 2006;17:1052–8.
Smeets JLRM, Rodrigues LM, Tımmermans C, Wellens HJJ. Radiofrequency catheter ablation of idiopathic ventricular tachycardias in children. PACE. 1997;20:2068–71.
Schneider HE, Kriebel T, Jung K, Gravenhorst VD, Paul T. Catheter ablation of idiopathic left and right ventricular tachycardias in the pediatric population using noncontact mapping. Heart Rhythm. 2010;7:731–9.
Baksiene D, Sileikiene R, Sileikis V, et al. Idiopathic ventricular tachycardia in children: curative therapy with radiofrequency ablation. Med (Kaunas). 2007;43(10).
Miszcak-Knecht M, Szumowski L, Posadowska M, et al. Idiopathic ventricular arrhythmia in children and adolescents: early effectiveness of radiofrequency current ablation. Kardiol Pol. 2014;72:1148–55.
Ozyilmaz I, Ergul Y, Akdeniz C, Tanidir IC, Tuzcu V. Catheter ablation of idiopathic ventricular tachycardia in children using the EnSite NavX system with/without fluoroscopy. Cardiol Young. 2014;24:886–92.
Wang S, Zhu W, Hamilton RM, Kirsh JA, Stephenson EA, Gross GJ. Diagnosis-specific characteristics of ventricular tachycardia in children with structurally normal hearts. Heart Rhythm. 2010;7:1725–31.
Grimm W, Marchlinski FE. Accelerated idioventricular rhythm: bidirectional ventricular tachycardia. In: Zipes DPJ, editor. Cardiac electrophysiology: from cell to bedside. Philadelphia, PA: Saunders; 2004. p. 700–4.
Daniels DV, Lu YY, Morton JB, et al. Idiopathic epicardial left ventricular tachycardia originating remote from the sinus of Valsalva: electrophysiological characteristics, catheter ablation, and identification from the 12-lead electrocardiogram. Circulation. 2006;113:1659–66.
Iwamoto M, Niimura I, Shibata T, Yasui K, Takigiku K, Nishizawa T. Long-term course and clinical characteristics of ventricular tachycardia detected in children by school-based heart disease screening. Circ J. 2005;69:273–6.
Morwood JG, Triedman JK, Berul CI, et al. Radiofrequency catheter ablation of ventricular tachycardia in children and young adults with congenital heart disease. Heart Rhythm. 2004;301–8.
Von Bergen NH, Bansal S, Gingerich J, Law IH. Nonfluoroscopic and radiation-limited ablation of ventricular arrhythmias in children and young adults: a case series. Pediatr Cardiol. 2011;32:743–7.
Junji Fukuhara MD, Naokata Sumitomo. Electrophysiological characteristics of idiopathic ventricular tachycardia in children. Circ J:(75).
Friedman PA, Asirvatham SJ, Grice S, et al. Non-contact mapping to guide ablation of right ventricular outflow tachycardia. J Am Coll Cardiol. 2002;39:1808–12.
Ribbing M, Wasmer K, Monnig G, et al. Endocardial mapping of right ventricular outflow tract tachycardia using noncontact activation mapping. J Cardiovasc Electrophysiol. 2003;14:602–8.
Soejima Y, Aonuma K, Iesaka Y, Isobe M. Ventricular unipolar potential in radiofrequency catheter ablation of idiopathic Non-reentrant ventricular outflow tachycardia. Jpn Heart J. 2004;45:749–60.
Tanaka Y, Tada H, Ito S, et al. Gender and age differences in candidates for radiofrequency catheter ablation of idiopathic ventricular arrhythmias. Circ J. 2011;75:1585–91.
Tung R, Michowitz Y, Yu R. Epicardial ablation of VT: an institutional experience of safety and efficacy. Heart Rhythm. 2013;10:490–8.
Brugada J, Blom N, Sarquella-Brugada G, et al. Pharmacological and non-pharmacological therapy for arrhythmias in the pediatric population: EHRA and AEPC-arrhythmia working group joint consensus statement. Europace. 2013;1:1337–82.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All patients and/or their legal guardians gave verbal and written consent for the procedure.
Conflict of interest
The manuscript, as submitted or its essence in another version, is not under consideration for publication elsewhere, and will not be published elsewhere while under consideration by Journal of Interventional Cardiac Electrophysiology. The authors have no commercial associations or sources of support that might pose a conflict of interest. All authors have made substantive contributions to the study, and all authors endorse the data and conclusions.
Rights and permissions
About this article
Cite this article
Akdeniz, C., Gul, E.E., Celik, N. et al. Catheter ablation of idiopathic right ventricular arrhythmias in children with limited fluoroscopy. J Interv Card Electrophysiol 46, 355–360 (2016). https://doi.org/10.1007/s10840-016-0133-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-016-0133-6