Abstract
It is well established that the tumor necrosis factor-α (TNF-α) plays a dominant role in rheumatoid arthritis (RA). Calcium channel is recently reported to be closely associated with various inflammatory diseases. However, whether chronic calcium channel blocker verapamil plays a role in RA still remains unknown. To investigate the role of verapamil in antagonizing TNF-α-mediated inflammation reaction and the underlying mechanisms, bone marrow-derived macrophages (BMDM) cells were cultured with stimulation of TNF-α, in the presence or absence of verapamil. Inflammation-associated cytokines, including IL-1, IL-6, inducible nitric oxide synthase 2 (NOS-2), and cyclooxygenase-2 (COX-2), were assessed, and verapamil suppressed TNF-α-induced expression of inflammatory cytokines. Furthermore, collagen-induced arthritis (CIA) mice models were established, and arthritis progression was evaluated by clinical and histological signs of arthritis. Treatment of verapamil attenuated inflammation as well as joint destruction in arthritis models. In addition, activity of NF-kB signaling pathway was determined both in vitro and in mice arthritis models, and verapamil inhibited TNF-α-induced activation of NF-kB signaling both in vitro and in mice models. Collectively, chronic calcium channel blocker verapamil may shed light on treatment of inflammatory arthritis and provide a potential therapeutic instrument for RA in the future.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Rheumatoid arthritis (RA) is a chronic autoimmune disease characterized by pain, joint inflammation, progressive cartilage damage, and bone erosion. Inflammatory cytokines produced by innate immune cells, in particular tumor necrosis factor α (TNF-α), play a critical role in the pathogenesis of inflammatory arthritis [1, 2]. Indeed, several approved biological agents, including anti-TNF antibodies (infliximab, adalimumab) and a recombinant soluble TNF receptor–Fc fusion protein (etanercept) showed promising therapeutic effects in patients with RA and other inflammatory diseases [3]. However, considering the cost of such biologic agents, potential resistance of these agents, and their limited efficacy, there is still a great need for the investigation of novel therapeutic mechanisms and agents [4, 5].
Calcium channel is expressed extensively within organism and plays a vital role in various diseases [6, 7]. Recently, it was reported that an inhibitor of store-operated calcium channel (SOC), an ion channel which displays selective permeability to calcium ions, attenuated rheumatoid arthritis in mice models [8]. However, it is unknown whether inhibitor of another calcium channel, chronic calcium channel, also protects against RA development. Verapamil is a commonly accepted chronic calcium channel inhibitor in cardiac diseases [9]. Recently, verapamil was reported to antagonize production as well as function of TNF-α and protect against inflammation reaction [10–12]. It is well-established that nuclear factor-kappa B (NF-kB) signaling plays a detrimental role in progress of inflammation [13] and is closely associated with RA development. It is known that verapamil inhibits activation of NF-kB signaling [14]. Recently, it was reported that verapamil protects against cartilage destruction in mice osteoarthritis models [15]. However, whether verapamil acts as a potential treatment of RA remains to be elucidated. The purpose of this study is to determine (1) whether verapamil is able to block the inflammatory function of TNF-α and has therapeutic effect in inflammatory arthritis and, if so, (2) what underlying mechanisms are involved.
MATERIAL AND METHODS
Mice
All animal studies were performed in accordance with institutional guidelines and with approval by the Institutional Animal Care and Use Committee of Shandong University. DBA/1J mice were obtained from Jackson Laboratories.
Isolation and Culture of Bone Marrow-Derived Macrophages
Bone marrow-derived macrophages (BMDM) cells were isolated from wild-type mice as previously reported [16]. Cells were isolated of bone marrow cells from mouse femurs and tibias. And, BMDM cells were cultured with DMEM containing 10 % fetal bovine serum, 1 % penicillin and streptomycin, and 15 % L929 conditioned media. Cells were differentiated to macrophages after 7 days of incubation at 37 °C.
CIA model
The collagen-induced arthritis (CIA) mice model was established as we have previously reported [17, 18]. Briefly, 10-week-old male DBA1/J mice were immunized via a 0.1-ml intradermal injection at the base of the tail with 100-μg chicken type II collagen (Chondrex, LLC, Seattle, WA) emulsified with an equal volume of complete Freund’s adjuvant (CFA) containing 4 mg/ml heat denatured mycobacterium (Chondrex, LLC, Seattle, WA) (day 0). A second injection was given subsequently after 21 days as previously reported [18]. To determine protective effects, 20 mg/kg verapamil [19] was administered intraperitoneally every day starting on day 21 [20, 21].
Evaluation for Clinical Arthritis
Clinical signs of arthritis in CIA mice models were evaluated to determine arthritis incidence. Each paw was evaluated and scored individually using a 0 to 4 scoring system. The paw scores were summed to yield individual mouse scores, with a maximum score of 16 for each animal as published previously [17].
Histopathological Examination of Joints
Following routine fixation, decalcification, and paraffin embedding, tissue sections were prepared and stained with hematoxylin and eosin. Decalcification procedure was performed as previously reported [18]. Briefly, paw samples from mice were put into 10 % EDTA, and the decalcification procedure lasts for demineralization. All slides were coded and submitted for evaluation by investigators blinded to the experimental conditions. The extent of synovitis, pannus formation, and bone/cartilage destruction was determined using a graded scale as follows: grade 0, no signs of inflammation; grade 1, mild inflammation with hyperplasia of the synovial lining without cartilage destruction; and grades 2 through 4, increasing degrees of inflammatory cell infiltrate and bone destruction. Sections were also stained with 0.1 % Safranin O to study the joint pathologic features. PG depletion was scored on an arbitrary scale of 0–3, where 0 = normal, 1 = fully stained cartilage, 2 = detained cartilage, and 3 = completely depleted of PGs. The degree of chondrocyte death was scored on a scale of 0–3, where 0 = no empty lacunae and 3 = complete loss of chondrocytes in the cartilage layer. Cartilage surface erosion was scored on a scale of 0–3, where 0 = no cartilage loss and 3 = complete loss of articular cartilage. All the analyses of cartilage destruction were done as previously reported [22, 23]. Histopathologic changes were scored on five semi-serial sections, spaced 140 mm apart. Scoring was performed in a blinded manner by two independent observers. In addition, TRAP staining was performed for detection of osteoclast activity as previously reported [13].
Western Blot
Bone marrow-derived macrophages (BMDM) cells were isolated from wild-type mice and stimulated with 10 ng/ml TNF-α, in the presence or absence of indicated doses of verapamil. At different time points, total cell lysate or cytoplasmic and nuclear extracts were prepared following our published protocol [19]. Cell extracts (∼30 μg) were resolved on a 10 % SDS-PAGE gel and probed using specific antibodies against total as well as phosphorylated IkBα, NF-kB p65, and NOS-2. Synovium from knee joints of CIA models was harvested and homogenized, followed by Western blot for NOS-2. β-Tubulin was used as internal control in all this set of experiments.
Reporter Gene Assay
To examine whether verapamil inhibits TNF-mediated transactivation of NF-kB-dependent reporter genes, reporter gene assay was performed in a method as described before with modifications [24]. Briefly, BMDM cells grown to ∼50 % confluence were transfected with 1 μg of the p6XNF-kB-Luc reporter plasmid and 1 μg of the pSVGal plasmid (internal control), using Lipofectamine 2000 Reagent (Invitrogen). Forty-eight hours following transfection, the cells were starved overnight and then stimulated for 6 h with 10 ng/ml TNF-α in the presence or absence of various doses of verapamil. Luciferase activity was then measured.
Immunofluorescence Staining of NF-kB p65
BMDM cells were cultured on coverslips, stimulated with 10 ng/ml TNF-α in the presence or absence of verapamil for 1 h. Then, immunofluorescence staining of NF-kB p65 was performed on these cells as described previously and examined using a confocal fluorescence microscope system [22].
Immunohistochemistry
The metatarsal joints of CIA mice treated with PBS or verapamil were sectioned, deparaffinized, rehydrated, and incubated in Tris buffer (10 Mm Tris–HCl (pH 8.0), 150 mM NaCl). The samples were then incubated with rabbit anti-mouse phosphorylated IkBα (1:100) at 4 °C overnight. Then, the sections were incubated for 30 min with biotinylated anti-rabbit IgG (Vector, Burlingame, CA) and subsequently stained using a biotin-streptavidin-peroxidase protocol (Vector). Horseradish peroxidase (HRP) activity was detected using 3,3′-diaminobenzidine and H2O2. Slides were counterstained with 0.5 % methyl green.
Real-Time PCR
Total RNA was extracted from synovium of knee joint in PBS or verapamil-treated CIA models, and BMDM cells stimulated with TNF-α (10 ng/ml) in the presence or absence of verapamil (5 μM) for 4 h using RNeasy kit (Qiagen), and first-strand complementary DNA (cDNA) was generated with ImProm-II reverse transcription system (Promega). Real-time PCR was performed with SYBR Green I dye used to monitor DNA synthesis. Data from each sample were normalized to GAPDH. Primers used for real-time RT-PCR were designed to generate products between 100 and 200 bp in length. Oligonucleotides used as the specific primers to amplify mouse genes are as follows: Total mRNA was isolated from. Then, they were reverse-transcribed to cDNA. Real-time PCR was performed with the following sequence-specific primers: 5′-TACAAGCTGGCTGGTGGGGA-3′ and 5′-GTCGCGGGTCTCAGGACCTT-3′ for NF-kB2; 5′-AATCTCACAGCAGCACATCA-3′ and 5′-AAGGTGCTCATGTCCTCATC-3′ for interleukin-1β (IL-1β); 5′-CCTTCCTACCCCAATTTCCAAT-3′ and 5′-GCCACTCCTTCTGTGACTCCAG-3′ for IL-6; 5′-ACA GGAGGGGTTAAAGCTGC-3′ and 5′-TTGTCTCCAAGGGACCAGG-3′ for NOS-2; 5′-AAT GCT GAC TAT GGC TAC AAA A-3′ and 5′-AAA ACT GAT GCG TGA AGT GCT G-3′ for COX-2; 5′-CTTCACCACCATGGAGAAGGC-3′ and 5′ GACGGACACATTGGGGGTAG-3′ for GAPDH. The presence of a single-specific PCR product was verified by melting curve analysis, and for each gene, the experiments were repeated three times.
Micro-CT
The microstructure destruction of metatarsal bones was measured using a Scanco μCT40 scanner (Scanco Medical AG, Basserdorf, Switzerland) as we have previously reported [13, 25]. A threshold of 300 was used for evaluation of all scans. The whole hind paw was scanned, and 3-D reconstruction was performed to evaluate bone erosion of metatarsal joints.
Assays for Circulating IL-1β and IL-6
Serum was collected from CIA model, and levels of IL-1β as well as IL-6 were assayed through ELISA as previously reported [24]. IL-1β and IL-6 were assayed using a commercial kit (eBioscience), according to the instructions of the manufacturer.
Statistical Analysis
For comparison of treatment groups, we performed unpaired t tests (Mann–Whitney), paired t tests, and one-way or two-way ANOVA (where appropriate). For ANOVA, we used Bonferroni post hoc analysis to compare treatment groups. All statistical analysis was performed using GraphPad Prism Software (version 4.01). Statistical significance was achieved when P < 0.05.
RESULTS
Verapamil Attenuated Inflammatory Reaction Induced by TNF-α In Vitro
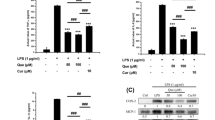
To determine whether verapamil antagonizes TNF-α function in vitro, BMDM cells were stimulated with 10 ng/ml TNF-α for 4 h in the presence or absence of 5 or 20 μM verapamil, followed by real-time RT-PCR assay. As shown in Fig. 1a–d, TNF-α-mediated inflammatory cytokine production, including IL-1β, IL-6, NOS-2, and COX-2, was largely abolished by additional use of verapamil in a dose-dependent manner. Furthermore, BMDM cells were cultured with 10 ng/ml TNF-α for 24 h, with or without treatment of 5 or 20 μM verapamil, followed by Western blot assay. Figure 1e shows that TNF-α significantly elevated expression levels of NOS-2 and COX-2, while this effect of TNF-α was remarkably diminished by additional treatment of verapamil dose dependently. Moreover, levels of interleukin (IL)-1 and IL-6 in conditional medium of the indicated groups were measured through ELISA. As shown in Fig. 1f–g, both mentioned inflammatory mediators were greatly antagonized by administration of 5 and 20 μM verapamil.
Verapamil antagonizes TNF-α-induced inflammatory reaction in BMDM cells. a–d Verapamil inhibited TNF-α-mediated production of IL-1β, IL-6, NOS-2, and COX-2 in BMDM cells, assayed by real-time RT-PCR. BMDM cells were incubated with TNF-α (10 ng/ml) in the presence or absence of verapamil (5 or 20 μM) for 4 h, cell extract was then harvested and assessed by real-time PCR. e Expression of NOS-2 as well as COX-2 in PBS and verapamil (5 or 20 μM) treatment group following TNF-α stimulation, assayed by Western blot. Protein extracts were collected from BMDM cells 24 h following TNF-α (10 ng/ml) stimulation in indicated treatment groups, and Western blot was performed. f, g Expression levels of IL-1β and IL-6 in TNF-α (10 ng/ml)-stimulated BMDM cells were significantly diminished by verapamil (5 or 20 μM), as measured through ELISA. Conditional media were collected from all the indicated groups of BMDM cells, and ELISA was performed for IL-1β and IL-6. The values are the mean ± SD. *P < 0.05; **P < 0.01; ***P < 0.005 vs. PBS treatment group.
Verapamil Protects Against Development of Arthritis in CIA Mice Models
To define the protective role of verapamil in vivo, we induced CIA model in 8–10-week-old male DBA/1J mice. Twenty-one days after immunization, the mice were divided into two groups based on their treatments: the CIA control group (PBS, n = 7) and the experimental groups (verapamil, 20 mg/kg, n = 7). Intraperitoneal injection of each agent was performed every day, and macrograph of hind paw (Fig. 2a) as well as clinical score of arthritis (Fig. 2b) implied inflammation in CIA model, while administration of verapamil remarkably attenuated development of arthritis. Forty-two days following immunization, samples of metatarsal joints from each group were collected and histological analyses as well as micro CT assay were performed. As shown in Fig. 2c, d, HE staining of metatarsal joints indicated severe synovitis, pannus, and erosion sites in CIA models. By contrast, verapamil dramatically alleviated inflammation in the arthritis model. Furthermore, synovium samples of metatarsal joints were collected from each group, and messenger RNA (mRNA) and protein were isolated. As revealed in Fig. 2e–h, mRNA levels of inflammation-associated molecules in CIA model, including IL-1β, IL-6, NOS-2, and COX-2, were significantly reduced by verapamil treatment. Figure 2i, j indicates that verapamil markedly reduced expression of NOS-2 and COX-2 compared with PBS group in CIA model. Moreover, serum was collected from each group, and IL-1β and IL-6 levels were assayed through ELISA. Figure 2k, l shows that circulating levels of both inflammatory molecules were greatly diminished in CIA with treatment of verapamil. Collectively, this set of experiments suggests that verapamil plays a protective role in CIA.
Verapamil protects against CIA development. a Representative photographs of hind paws from normal control and CIA mice treated with PBS or verapamil. DBA/1J mice were induced for CIA model. Twenty-one days after immunization, PBS (negative control, n = 7) or verapamil (n = 7) were administered every day in a dose of 20 mg/kg body weight through intraperitoneal injection until day 42. b Clinical arthritis scores in PBS or verapamil-treated CIA mice. The experiment process is the same as a. Data are presented as the mean clinical score ± s.e.m. *P < 0.05; **P < 0.01; ***P < 0.001 versus the PBS group. c Verapamil attenuates severity of inflammation in metatarsal joints of CIA models, as indicated by HE staining. Scale bar = 100 μm. d Evaluation of synovitis, pannus formation, and erosion of tarsal joints in CIA mice. e–h IL-1β, IL-6, NOS-2, and COX-2 gene levels in synovium of CIA model treated with PBS or verapamil, assayed by real-time RT-PCR. RNA extracts were collected from PBS and verapamil-treated CIA model, and real-time RT-PCR was performed. i, j Protein levels of NOS-2 and COX-2 in synovium samples of indicated groups, as measured by Western blot. k, l Serum levels of IL-1β and IL-6, as measured by ELISA. Forty-two days after primary immunization and different treatments (started at day 21), serum was taken from normal untreated control mice as well as CIA model of each treatment group, and ELISA was performed for IL-1β and IL-6. Values are mean ± s.d. of three independent experiments. *P < 0.05; **P < 0.01; ***P < 0.001 versus the control PBS group.
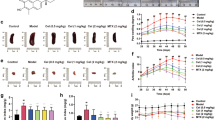
Cartilage destruction and inflammatory bone resorption are well accepted characteristics of rheumatoid arthritis [26, 27]. In this study, metatarsal joints were collected from each group, and Safranin O staining was performed. As indicated in Fig. 3a, serious destruction of cartilage was observed in CIA model, while the destruction was dramatically protected through verapamil. Based on Safranin O staining, severity of cartilage destruction was further testified through a histological scoring system. Figure 3b–d reveals that cartilage PG depletion, chondrocyte death, and cartilage surface erosion in CIA model were greatly attenuated in verapamil treatment group. ADAMTS-5 and MMP-13 are well accepted molecules for cartilage destruction in arthritis [28, 29]. In the current study, metatarsal joints were collected and real-time PCR was performed. Figure 3e shows that levels of ADAMTS-5 and MMP-13 were both diminished in verapamil treatment group. It is reported that calcium channel inhibitors, including verapamil, are associated with osteoclastogenesis [30, 31]. To determine the protective role of verapamil for inflammatory osteoporosis in CIA models, metatarsal joints from each group were isolated, and micro-CT and TRAP staining were performed. Figure 3f, g indicates that verapamil remarkably protected against inflammatory bone erosion as well as osteoclastogenesis in CIA models. Furthermore, mRNA was collected from bony tissue of metatarsal joints, and Fig. 3h, i reveals that the levels of osteoclast-associated molecules, including TRAP and Cathepsin K were significantly reduced by administration of verapamil.
Verapamil treatment protects against bone erosion and cartilage destruction in CIA model. a Verapamil treatment protected cartilage from destruction, assayed by Safranin O staining. Metatarsal joints from both verapamil and PBS-treated CIA model were dissected at day 42 and Safranin O staining was performed. Scale bar, 100 μm. b–d Results of histological analysis to determine irreversible cartilage destruction in mice metatarsal joints. On the basis of Safranin O staining, histological scores were determined for the extent of cartilage proteoglycan (PG) depletion, chondrocyte death, and cartilage surface erosion in metatarsal joints from PBS or verapamil treatment group of CIA model. e Verapamil treatment diminished expression levels of MMP-13 and ADAMTS-5 in CIA model, as detected by real-time PCR. Metatarsal joints from CIA mice were collected at day 42 and real-time PCR was performed. f Verapamil therapy attenuated bone erosion in CIA model, assessed by micro-CT. Then, hind paws from each group were dissected and micro-CT was performed. g Verapamil suppressed inflammatory osteoclastogenesis in CIA model, assayed by TRAP staining. Hind paws from a were performed with TRAP staining, and osteoclast activity was compared between verapamil and PBS group. Scale bar, 50 μm. h, i Verapamil treatment diminished osteoclastic biomarkers TRAP and Cathepsin K in CIA model, as assayed by real-time PCR. Values are mean ± s.d. of three independent experiments. *P < 0.05; **P < 0.01; ***P < 0.001 versus the control PBS group.
Verapamil Blocks NF-kB Signaling Pathway Both In Vitro and in the CIA Model
NF-kB pathway is a critical signaling pathway in various diseases and plays a pivotal role in development and progression of inflammatory arthritis [32]. To investigate whether verapamil inhibits TNF-α-induced stimulation of NF-kB pathway, BMDM cells were cultured for 3 h in the presence of TNF-α (10 ng/ml), with or without pretreatment of 5 μM verapamil. Thereafter, cell extract was collected, and real-time PCR was performed. As shown in Fig. 4a, additional use of verapamil suppressed TNF-α-mediated expression of NF-kB2, a critical composite of NF-kB signaling pathway. Besides, plasma and nuclear proteins were collected respectively as described before for testing nuclei translocation of NF-kB p65. Figure 4b demonstrates that verapamil inhibited TNF-α-induced nuclei translocation of NF-kB p65. To further assess the role of verapamil in inhibiting activation of NF-kB signaling, immunostaining for NF-kB p65 was performed on BMDM cells cultured in the presence of 10 ng/ml TNF-α for 1 h, in the absence or presence of verapamil. As indicated in Fig. 4c, verapamil inhibited TNF-α-mediated activation of NF-kB-dependent reporter gene by measuring the luciferase activity of increasing concentrations of verapamil (1, 5, 20 μM) used in BMDM cells. Figure 4d reveals that verapamil suppressed nuclei translocation of NF-kB p65. Additionally, activation of NF-kB signaling in the synovium fibroblast of tarsal joint in CIA model was assessed through immunohistochemistry of pIkB-α. As shown in Fig. 4e, verapamil suppressed expression level of NF-kB2 in prevention experiment of CIA model was measured by real-time PCR. Figure 4f indicates the protective role of verapamil in the activation of NF-kB signaling in CIA model by histopathological examination.
Verapamil inhibits TNF-α-mediated activation of NF-kB signaling. a Verapamil inhibited TNF-α-induced NF-kB2 expression. BMDM cells were incubated with TNF-α (10 ng/ml) in the presence or absence of verapamil (5 μM) for 4 h, and cell extract was then harvested and assessed by real-time PCR. b Verapamil impaired TNF-α-mediated activation of NF-kB signaling, assayed by Western blot. BMDM cells were incubated and treated as Fig. 4a for indicated time points. Then, cytoplasmic (CE) and nuclear (NE) protein extracts were harvested and detected by Western blot. β-Tubulin and lamin A served as cytoplasmic and nuclear controls, respectively. c Verapamil inhibited TNF-α-mediated activation of NF-kB-dependent reporter gene. BMDM cells transfected with the NF-kB-dependent reporter construct were incubated with TNF-α (10 ng/ml) in the presence of increasing concentrations of verapamil (1, 5, 20 μM), and the luciferase activity was measured. Values are mean ± s.d. *P < 0.05; **P < 0.01; ***P < 0.001 versus TNF-α-stimulated cells. d Verapamil suppressed TNF-α-induced nuclear translocation of NF-kB p65, assayed by immunofluorescence. BMDM cells were stimulated with TNF-α for 4 h, with treatment of PBS or 5 μM verapamil, then cells were fixed and the location of NF-kB was visualized by p65 antibody, and the nuclei were stained with DAPI. e Verapamil suppressed expression level of NF-kB2 in prevention experiment of CIA model, as measured by real-time PCR for NF-kB2. Metatarsal joints of normal control and CIA mice were collected on day 42 after primary immunization with treatment of PBS or verapamil (start on day 21), and then real-time PCR for NF-kB2 was performed. f Verapamil suppressed expression level of pIkBα in prevention experiment of CIA model, as measured by immunohistochemistry for p-IkBα. Metatarsal joints of normal control and CIA mice with treatment of PBS or verapamil (start on day 21) were collected on day 42 after primary immunization, and then immunohistochemistry for p-IkBα was performed. Values are mean ± s.d. *P < 0.05; **P < 0.01; ***P < 0.001 versus PBS treatment group. Scale bar, 25 μm.
DISCUSSION
Verapamil has been widely used and is well-established in clinic for the safety and efficacy in various diseases [33]. Recently, it was reported that verapamil was able to antagonize inflammation in several pathological conditions and present protective effect [34, 35]. TNF-α is a critical cytokine to induce other inflammation-associated molecules, which further leads to development of inflammatory diseases [36, 37]. TNF-α also promotes osteoclastogenesis and leads to bone erosion in various inflammatory diseases such as rheumatoid arthritis or inflammatory bowel disease [38, 39]. As a predominant inflammatory cytokine, TNF-α activates NF-kB inflammatory signaling pathway, stimulates production of other inflammatory cytokines such as IL-1 and IL-6, and enhances tissue destruction in joints, contributing to the aggravating lesion of RA [40]. To date, TNF-α inhibition has become a well-accepted therapeutic strategy for RA [41, 42]. TNF-α neutralizing therapies, including anti-TNF-α monoclonal antibody and soluble TNFR, are well-established instruments in clinic for treatment of rheumatoid arthritis [43–45]. In this study, we have shown that administration of verapamil suppressed the inflammation reaction induced by TNF-α in vitro. It is known that macrophage plays a pivotal role in the progression of various inflammatory diseases [46, 47]. Macrophage, especially when activated by TNF-α, can strongly exaggerate severity of RA for further production of inflammatory cytokines such as COX-2, NOS-2, IL-1, and IL-6 [48, 49]. In the present study, we took use of BMDM macrophage and indicated that verapamil suppressed the elevation of the mentioned cytokines mediated by TNF-α, suggesting its protective role in inflammatory reaction.
NF-kB signaling pathway is a pleiotropic pathway in development of inflammatory diseases and plays an important role in inflammation-associated molecules including NOS-2 as well as COX-2 in RA. Production of these molecules results in further activation of NF-kB signaling. Indeed, persistent NF-kB activation has been observed in both human and animal models of RA. It is reported that verapamil inhibited NF-kB signaling pathway in the liver [14]. Moreover, the other calcium channel blocker such as nifedipine plays a positive role in vascular inflammation by NF-kB signaling [50]. In the present study, we found that verapamil affected not only the expression level of NF-kB signaling but also the production of downstream molecules related with NF-kB signaling pathway in inflammatory arthritis mice models, which implies the amelioration of verapamil on the RA and other inflammatory diseases.
It is well accepted that cartilage destruction is one feature of RA [51]. Moreover, verapamil is known to protect against osteoarthritis in mice models [15]. In the current study, we established CIA mice models to further verify the chondroprotective role of verapamil in vivo. We demonstrated that treatment of verapamil significantly attenuated breakdown of cartilage and reduced the levels of MMP13 as well as ADAMTS-5, which are known to be associated with cartilage degradation in arthritis. Together with the reduced matrix loss of metatarsal joints in verapamil treatment group, all the data suggested the protective effect of verapamil on cartilage matrix in CIA models. Another characteristic of RA is enhanced osteoclastogenesis and bone erosion [52]. Herein, we testified that classical inflammatory osteoclastogenesis and osteolysis in CIA model were greatly attenuated by administration of verapamil. Collectively, these data implied that verapamil may shed light on CIA treatment and serve a potential target for rheumatoid arthritis in the future.
CIA is a most frequently used animal model to study the effect of new therapeutics for RA. Although there are similarities between these conditions, human arthritis conditions still remain to be elucidated. Therefore, CIA only can simulate RA to a certain degree. Furthermore, though verapamil works well in inflammatory arthritis in mice, there is no investigation concerning the improvement of RA symptoms in the patients who used verapamil for other conditions. Further studies are required to determine whether the finding in mice also works well in human. And, this is the limitation in our study.
References
Tang, W., Y. Lu, Q.Y. Tian, Y. Zhang, F.J. Guo, G.Y. Liu, N.M. Syed, Y. Lai, E.A. Lin, L. Kong, et al. 2011. The growth factor progranulin binds to TNF receptors and is therapeutic against inflammatory arthritis in mice. Science 332: 478–484.
Cuchacovich, R., R. Perez-Alamino, A.H. Zea, and L.R. Espinoza. 2014. Distinct genetic profile in peripheral blood mononuclear cells of psoriatic arthritis patients treated with methotrexate and TNF-inhibitors. Clinical Rheumatology 33: 1815–1821.
Hoffmann, J.H., C. Knoop, A.H. Enk, and E.N. Hadaschik. 2014. Baseline anti-dsDNA concentrations and previous treatments predict response to Adalimumab and Etanercept: A retrospective investigation of 146 psoriasis patients. Journal of Dermatological Science 76: 180–185.
Eng, G.P., K. Bendtzen, H. Bliddal, M. Stoltenberg, M. Szkudlarek, V. Fana, H.M. Lindegaard, E. Omerovic, P. Hojgaard, E.K. Jensen, and P.N. Bouchelouche. 2015. Antibodies to infliximab and adalimumab in patients with rheumatoid arthritis in clinical remission: A cross-sectional study. Arthritis 2015: 784825.
Viatte, S., D. Plant, B. Han, B. Fu, A. Yarwood, W. Thomson, D.P. Symmons, J. Worthington, A. Young, K.L. Hyrich, et al. 2015. Association of HLA-DRB1 haplotypes with rheumatoid arthritis severity, mortality, and treatment response. JAMA 313: 1645–1656.
Delaney, B., J. Loy, and A.M. Kelly. 2011. The relative efficacy of adenosine versus verapamil for the treatment of stable paroxysmal supraventricular tachycardia in adults: A meta-analysis. European Journal of Emergency Medicine 18: 148–152.
Paulis, G., G. Cavallini, G.D. Giorgio, S. Quattrocchi, T. Brancato, and R. Alvaro. 2013. Long-term multimodal therapy (verapamil associated with propolis, blueberry, vitamin E and local diclofenac) on patients with Peyronie’s disease (chronic inflammation of the tunica albuginea). Results of a controlled study. Inflammation & Allergy Drug Targets 12: 403–409.
Gao, X.H., R. Gao, Y.Z. Tian, P. McGonigle, J.E. Barrett, Y. Dai, and H. Hu. 2015. A store-operated calcium channel inhibitor attenuates collagen-induced arthritis. British Journal of Pharmacology 172: 2991–3002.
Vicente J, Johannesen L, Mason JW, Crumb WJ, Pueyo E, Stockbridge N, Strauss DG. Comprehensive T wave morphology assessment in a randomized clinical study of dofetilide, quinidine, ranolazine, and verapamil. J Am Heart Assoc 2015, 4.
Cuschieri, J., D. Gourlay, I. Garcia, S. Jelacic, and R.V. Maier. 2002. Slow channel calcium inhibition blocks proinflammatory gene signaling and reduces macrophage responsiveness. The Journal of Trauma 52: 434–442.
Chen, Y.L., Y.S. Chen, H.H. Lin, C.W. Chan, S.C. Chen, and C.H. Chen. 2007. Immunostimulatory flagellin from Burkholderia pseudomallei effects on an increase in the intracellular calcium concentration and up-regulation of TNF-alpha by mononuclear cells. Microbiology and Immunology 51: 81–86.
Geoghegan-Morphet, N., D. Burger, X. Lu, V. Sathish, T. Peng, S.M. Sims, and Q. Feng. 2007. Role of neuronal nitric oxide synthase in lipopolysaccharide-induced tumor necrosis factor-alpha expression in neonatal mouse cardiomyocytes. Cardiovascular Research 75: 408–416.
Zhao, Y.P., Q.Y. Tian, S. Frenkel, and C.J. Liu. 2013. The promotion of bone healing by progranulin, a downstream molecule of BMP-2, through interacting with TNF/TNFR signaling. Biomaterials 34: 6412–6421.
Li, G., X.P. Qi, X.Y. Wu, F.K. Liu, Z. Xu, C. Chen, X.D. Yang, Z. Sun, and J.S. Li. 2006. Verapamil modulates LPS-induced cytokine production via inhibition of NF-kappa B activation in the liver. Inflammation Research 55: 108–113.
Takamatsu, A., B. Ohkawara, M. Ito, A. Masuda, T. Sakai, N. Ishiguro, and K. Ohno. 2014. Verapamil protects against cartilage degradation in osteoarthritis by inhibiting Wnt/beta-catenin signaling. PLoS ONE 9: e92699.
Ekpenyong, A.E., S.M. Man, S. Achouri, C.E. Bryant, J. Guck, and K.J. Chalut. 2013. Bacterial infection of macrophages induces decrease in refractive index. Journal of Biophotonics 6: 393–397.
Tian, Q., Y. Zhao, J.J. Mundra, E. Gonzalez-Gugel, J. Jian, S.M. Uddin, and C. Liu. 2014. Three TNFR-binding domains of PGRN act independently in inhibition of TNF-alpha binding and activity. Front Biosci (Landmark Ed) 19: 1176–1185.
Bevaart, L., M.J. Vervoordeldonk, and P.P. Tak. 2010. Collagen-induced arthritis in mice. Methods in Molecular Biology 602: 181–192.
El-Azab, M.F., and Y.M. Moustafa. 2012. Influence of calcium channel blockers on anticonvulsant and antinociceptive activities of valproic acid in pentylenetetrazole-kindled mice. Pharmacological Reports 64: 305–314.
Jung, E.G., K.I. Han, S.G. Hwang, H.J. Kwon, B.B. Patnaik, Y.H. Kim, and M.D. Han. 2015. Brazilin isolated from Caesalpinia sappan L. inhibits rheumatoid arthritis activity in a type-II collagen induced arthritis mouse model. BMC Complement Altern Med 15: 124.
Zhao, X.X., Y. Bi, X.Y. Yin, and R. Min. 2016. Suppression of collagen-induced arthritis by lipopolysaccharide in DBA/1 mice. European Review for Medical and Pharmacological Sciences 20: 441–446.
Koenders, M.I., E. Lubberts, B. Oppers-Walgreen, L. van den Bersselaar, M.M. Helsen, J.K. Kolls, L.A. Joosten, and W.B. van den Berg. 2005. Induction of cartilage damage by overexpression of T cell interleukin-17A in experimental arthritis in mice deficient in interleukin-1. Arthritis and Rheumatism 52: 975–983.
Nabbe, K.C., A.B. Blom, A.E. Holthuysen, P. Boross, J. Roth, S. Verbeek, P.L. van Lent, and W.B. van den Berg. 2003. Coordinate expression of activating Fc gamma receptors I and III and inhibiting Fc gamma receptor type II in the determination of joint inflammation and cartilage destruction during immune complex-mediated arthritis. Arthritis and Rheumatism 48: 255–265.
Li, W., Y. Zhao, X. Xu, W. Ma, P. Gao, Y. Wang, K. Liang, and R. Li. 2015. Rebamipide suppresses TNF-alpha mediated inflammation in vitro and attenuates the severity of dermatitis in mice. The FEBS Journal 282: 2317–2326.
Zhao, Y.P., B. Liu, Q.Y. Tian, J.L. Wei, B. Richbourgh, and C.J. Liu. 2015. Progranulin protects against osteoarthritis through interacting with TNF-alpha and beta-Catenin signalling. Annals of the Rheumatic Diseases 74: 2244–2253.
Gravallese, E.M. 2002. Bone destruction in arthritis. Annals of the Rheumatic Diseases 61(Suppl 2): i84–i86.
Goldring, S.R. 2002. Bone and joint destruction in rheumatoid arthritis: What is really happening? Journal of Rheumatology Supplement 65: 44–48.
Imada, K., N. Lin, C. Liu, A. Lu, W. Chen, M. Yano, T. Sato, and A. Ito. 2008. Nobiletin, a citrus polymethoxy flavonoid, suppresses gene expression and production of aggrecanases-1 and −2 in collagen-induced arthritic mice. Biochemical and Biophysical Research Communications 373: 181–185.
Jungel, A., C. Ospelt, M. Lesch, M. Thiel, T. Sunyer, O. Schorr, B.A. Michel, R.E. Gay, C. Kolling, C. Flory, et al. 2010. Effect of the oral application of a highly selective MMP-13 inhibitor in three different animal models of rheumatoid arthritis. Annals of the Rheumatic Diseases 69: 898–902.
Klar, R.M., R. Duarte, T. Dix-Peek, C. Dickens, C. Ferretti, and U. Ripamonti. 2013. Calcium ions and osteoclastogenesis initiate the induction of bone formation by coral-derived macroporous constructs. Journal of Cellular and Molecular Medicine 17: 1444–1457.
Redlich, K., P. Pietschmann, T. Stulc, and M. Peterlik. 1997. Comparative study on the effect of calcium channel blockers on basal and parathyroid hormone-induced bone resorption in vitro. Pharmacology and Toxicology 80: 262–265.
Lee, H.S., S.J. Woo, H.W. Koh, S.O. Ka, L. Zhou, K.Y. Jang, H.S. Lim, H.O. Kim, S.I. Lee, and B.H. Park. 2014. Regulation of apoptosis and inflammatory responses by insulin-like growth factor binding protein 3 in fibroblast-like synoviocytes and experimental animal models of rheumatoid arthritis. Arthritis Rheumatol 66: 863–873.
Abd Allah, E.S., M.A. Ahmed, and A.F. Abdel Mola. 2014. Comparative study of the effect of verapamil and vitamin D on iron overload-induced oxidative stress and cardiac structural changes in adult male rats. Pathophysiology 21: 293–300.
Park, H.W., H. Park, I.A. Semple, I. Jang, S.H. Ro, M. Kim, V.A. Cazares, E.L. Stuenkel, J.J. Kim, J.S. Kim, and J.H. Lee. 2014. Pharmacological correction of obesity-induced autophagy arrest using calcium channel blockers. Nature Communications 5: 4834.
Matsumura, C.Y., A. Pertille, T.C. Albuquerque, H. Santo Neto, and M.J. Marques. 2009. Diltiazem and verapamil protect dystrophin-deficient muscle fibers of MDX mice from degeneration: A potential role in calcium buffering and sarcolemmal stability. Muscle and Nerve 39: 167–176.
Abbott, R., R. Whear, V. Nikolaou, A. Bethel, J.T. Coon, K. Stein, and C. Dickens. 2015. Tumour necrosis factor-alpha inhibitor therapy in chronic physical illness: A systematic review and meta-analysis of the effect on depression and anxiety. Journal of Psychosomatic Research 79: 175–184.
Urbano, P.C., V.T. Soccol, and V.F. Azevedo. 2014. Apoptosis and the FLIP and NF-kappa B proteins as pharmacodynamic criteria for biosimilar TNF-alpha antagonists. Biologics 8: 211–220.
Park, Y.J., J.Y. Kim, J. Park, J.J. Choi, W.U. Kim, and C.S. Cho. 2014. Bone erosion is associated with reduction of circulating endothelial progenitor cells and endothelial dysfunction in rheumatoid arthritis. Arthritis Rheumatol 66: 1450–1460.
Milia, A.F., L. Ibba-Manneschi, M. Manetti, G. Benelli, S. Generini, L. Messerini, and M. Matucci-Cerinic. 2011. Evidence for the prevention of enthesitis in HLA-B27/hbeta(2)m transgenic rats treated with a monoclonal antibody against TNF-alpha. Journal of Cellular and Molecular Medicine 15: 270–279.
Yeremenko, N., K. Zwerina, G. Rigter, D. Pots, J.E. Fonseca, J. Zwerina, G. Schett, and D. Baeten. 2015. Tumor necrosis factor and interleukin-6 differentially regulate Dkk-1 in the inflamed arthritic joint. Arthritis Rheumatol 67: 2071–2075.
Yokoyama, W., H. Kohsaka, K. Kaneko, M. Walters, A. Takayasu, S. Fukuda, C. Miyabe, Y. Miyabe, P.E. Love, N. Nakamoto, et al. 2014. Abrogation of CC chemokine receptor 9 ameliorates collagen-induced arthritis of mice. Arthritis Research and Therapy 16: 445.
Yoshida, Y., A. Ogata, S. Kang, K. Ebina, K. Shi, S. Nojima, T. Kimura, D. Ito, K. Morimoto, M. Nishide, et al. 2015. Semaphorin 4D contributes to rheumatoid arthritis by inducing inflammatory cytokine production: Pathogenic and therapeutic implications. Arthritis Rheumatol 67: 1481–1490.
van Vollenhoven, R.F., M. Ostergaard, M. Leirisalo-Repo, T. Uhlig, M. Jansson, E. Larsson, F. Brock, and K. Franck-Larsson. 2016. Full dose, reduced dose or discontinuation of etanercept in rheumatoid arthritis. Annals of the Rheumatic Diseases 75: 52–58.
Emery, P., A. Deodhar, W.F. Rigby, J.D. Isaacs, B. Combe, A.J. Racewicz, K. Latinis, C. Abud-Mendoza, L.J. Szczepanski, R.A. Roschmann, et al. 2010. Efficacy and safety of different doses and retreatment of rituximab: A randomised, placebo-controlled trial in patients who are biological naive with active rheumatoid arthritis and an inadequate response to methotrexate (Study Evaluating Rituximab’s Efficacy in MTX iNadequate rEsponders (SERENE)). Annals of the Rheumatic Diseases 69: 1629–1635.
Smolen, J.S., J. Kay, E.L. Matteson, R. Landewe, E.C. Hsia, S. Xu, Y. Zhou, and M.K. Doyle. 2014. Insights into the efficacy of golimumab plus methotrexate in patients with active rheumatoid arthritis who discontinued prior anti-tumour necrosis factor therapy: Post-hoc analyses from the GO-AFTER study. Annals of the Rheumatic Diseases 73: 1811–1818.
Lissner, D., M. Schumann, A. Batra, L.I. Kredel, A.A. Kuhl, U. Erben, C. May, J.D. Schulzke, and B. Siegmund. 2015. Monocyte and M1 Macrophage-induced Barrier Defect Contributes to Chronic Intestinal Inflammation in IBD. Inflammatory Bowel Diseases 21: 1297–1305.
Bruck, N., A. Schnabel, and C.M. Hedrich. 2015. Current understanding of the pathophysiology of systemic juvenile idiopathic arthritis (sJIA) and target-directed therapeutic approaches. Clinical Immunology 159: 72–83.
Li, J., H.C. Hsu, Y. Ding, H. Li, Q. Wu, P. Yang, B. Luo, A.L. Rowse, D.M. Spalding, S.L. Bridges Jr., and J.D. Mountz. 2014. Inhibition of fucosylation reshapes inflammatory macrophages and suppresses type II collagen-induced arthritis. Arthritis Rheumatol 66: 2368–2379.
Vogelpoel, L.T., I.S. Hansen, T. Rispens, F.J. Muller, T.M. van Capel, M.C. Turina, J.B. Vos, D.L. Baeten, M.L. Kapsenberg, E.C. de Jong, and J. den Dunnen. 2014. Fc gamma receptor-TLR cross-talk elicits pro-inflammatory cytokine production by human M2 macrophages. Nature Communications 5: 5444.
Gao, X.Y., Q. Yu, S.K. Liu, F.Q. Lu, S.M. Zhou, and S.T. Zhang. 2010. Nifedipine attenuates vascular inflammation via inhibin NF-kappaB activity. Zhonghua Xin Xue Guan Bing Za Zhi 38: 1025–1030.
Feng ZY, He ZN, Zhang B, Li YQ, Guo J, Xu YL, Han MY, Chen Z. 2015. Adenovirus-mediated osteoprotegerin ameliorates cartilage destruction by inhibiting proteoglycan loss and chondrocyte apoptosis in rats with collagen-induced arthritis. Cell Tissue Res.
Denninger, K.C., T. Litman, T. Marstrand, K. Moller, L. Svensson, T. Labuda, and A. Andersson. 2015. Kinetics of gene expression and bone remodelling in the clinical phase of collagen-induced arthritis. Arthritis Research and Therapy 17: 43.
Acknowledgments
This research was supported partially by the National Natural Science Foundation of China (81501880 to Yunpeng Zhao); this research was also supported by the Natural Science Foundation of Shandong Province (BS2014YY048 to Yunpeng Zhao) and Scientific Research foundation of Qilu Hospital (26010175616073 to Yunpeng Zhao).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
None.
Additional information
Wenhan Wang and Zhong Li contributed equally to this work.
Rights and permissions
About this article
Cite this article
Wang, W., Li, Z., Meng, Q. et al. Chronic Calcium Channel Inhibitor Verapamil Antagonizes TNF-α-Mediated Inflammatory Reaction and Protects Against Inflammatory Arthritis in Mice. Inflammation 39, 1624–1634 (2016). https://doi.org/10.1007/s10753-016-0396-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-016-0396-1