Abstract
Microglial activation has been reported to play an important role in neurodegenerative diseases by producing pro-inflammatory cytokines. Bisphenol A (BPA, 2,2-bis (4-hydroxyphenyl) propane), known as a ubiquitous endocrine-disrupting chemical, is reported to perform both mimic- and anti-estrogen properties; however, whether it affects cytokine production or immune response in central nervous system remains unclear. The present study was aimed to explore whether BPA was involved in inflammatory action and to investigate the potential mechanisms in microglial cells. BV2, the murine microglial cell line, was used in the present work as the cell model. BPA-associated morphologic changes, cytokine responses, and signaling events were examined using immunofluorescence analysis, real-time PCR, enzyme-linked immunosorbent assay, and western blot. Our results indicated that BPA increased BV2 cells activation and simultaneously elevated tumor necrosis factor-α and interleukin 6 expression, which could be partially reversed by estrogen receptor antagonist, ICI182780. In addition, the c-Jun N-terminal protein kinase (JNK) inhibitor (SP600125), rather than ERK1/2 blocker (PD98059), displayed anti-inflammatory properties on BPA-elicited cytokine responses. Moreover, the inflammatory transcription factor NF-κB was specifically activated by BPA as well. These results, taken together, suggested that BPA may have functional effects on the response of microglial cell activation via, in part, the estrogen receptor, JNK, ERK mitogen-activated protein kinase, and NF-κB signaling pathways with its subsequent influence on pro-inflammatory action.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Recently, exogenous environmental pollutants exposure has gained more attention on their endocrine-disrupting effects and other human health impacts [1–5]. This concern was highlighted by a recent survey of 1,442 French male newborns perinatally exposed to environmental chemicals, revealing a potential link between pollutants biochemical effects and occurrence of diseases [6]. Bisphenol A (BPA), one of the endocrine disrupting chemicals (EDCs), is widely used in the manufacture of epoxy resins and polycarbonates, and thus, is a substance ubiquitously found in consumer products, like polycarbonate food containers and utensils, dental sealants, protective coatings, and water supply pipes [7, 8]. Reports available now suggest that BPA can interfere with hormone synthesis and hormone receptor expression, specifically alter gene activities in target tissues, which might influence potential genetic embryo stability and immune homeostasis [9–11]. According to the latest study, measurable levels of BPA were detected in maternal blood in the USA population, close to a nanomole scale [12]. In addition, BPA was also reported to penetrate the blood–brain barrier (BBB), which makes central nervous system (CNS) a potentially sensitive target [13]. However, it is still poorly understood how BPA exerts immunomodulatory effects on the brain.
In present days, studies have focused on the contrasting role of mimic and anti-effects BPA played on the steroid hormones, one related kind of which, estrogen, is well researched for its anti-inflammatory property, so there lies the necessity to clarify the actual influence and possible mechanisms of BPA on the genesis and progression of host immunity [14–18]. Microglial cells (MG), the local macrophage-like residential cells in the brain, have been proposed to perform critical roles in the innate immune response of the central nervous system [19, 20]. MG act as phagocytes to remove dead cells and tissue debris, protecting CNS from microbial pathogens of various infectious diseases [21]. However, once overactivated, the microglial cells secret excessive pro-inflammatory factors, like nitric oxide (NO), prostaglandin E2 (PGE 2), tumor necrosis factor-α (TNF-α), and reactive oxygen species (ROS), which are believed to be responsible for various forms of neurodegenerative processes, such as Parkinson’s disease, Alzheimer’s disease, multiple sclerosis, and amyotrophic lateral sclerosis (ALS) [22–24]. Considering the importance of microglial cells, and its role as the frontline of the immune response, which makes it a possible target of EDCs, we investigated the in vitro effects of BPA on the generation of two regulatory cytokines: TNF-α and interleukin 6 (IL-6) in BV2 microglial cell line. Since EDCs are able to serve as inflammatory inducers partially via the estrogen receptor, the regulatory effect of estrogen receptor (ER) was discussed [25]. Furthermore, extensive studies have demonstrated interference with differentiation and proliferation of neuronal cells, which closely involves differential activation of mitogen-activated protein kinase (MAPKs) and NF-κB pathways, may be a critical factor in cell survival and death process. However, it is still unknown whether MAPKs and NF-κB were participated in BPA-mediated inflammatory reaction in microglial cells [26, 27].
The results herein provide evidence supporting the influence of EDCs on the function of BV2 cells involving, in part, an ER-dependent mechanism and activation of MAPKs and NF-κB, with subsequent TNF-α and IL-6 expression.
MATERIALS AND METHODS
Reagents and Antibodies
Bisphenol A (purity >98 %), 3-(4, 5-dimethylthiazol-2-yl)-2, 5-diphenyl tetrazolium bromide (MTT), and lipopolysaccharide (LPS) were purchased from Sigma (St. Louis, MO, USA). The rabbit anti-mouse antibodies for ERK1/2 and phosphorylated (p)-ERK1/2, JNK and p-JNK, NF-κB and p-NF-κB, PD98059, SP600125, and ICI182780 were obtained from Cell Signaling (Danvers, MA, USA). The rabbit anti-mouse CD11b monoclonal antibody, the rabbit anti-mouse Estrogen Receptor alpha monoclonal antibody, the rabbit anti-mouse Estrogen Receptor beta polyclonal antibody (Abcam Inc., Cambridge, MA, USA), and TRITC-conjugated goat anti-rabbit-IgG secondary antibody (Sigma) were used. Dulbecco’s Modified Eagle Medium (DMEM), fetal bovine serum (FBS), penicillin, and streptomycin were obtained from HyClone Laboratories Inc. (Legan, Utah, USA).
Cell Culture and Sample Treatment
The murine BV2 microglial cell line was obtained from Shanghai Cell Research Center (Shanghai, China). These cells were grown at 37 °C in DMEM supplemented with 10 % FBS, penicillin (100 units/ml), and streptomycin sulfate (100 μg/ml) in a humidified atmosphere of 5 % CO2. Cells were incubated with BPA at concentrations of 10, 100, and 1000 nM/l. The final concentration of DMSO did not exceed 0.05 %.
Cell Viability Assay
Cell viability was measured based on the formation of blue formazan metabolized from MTT by mitochondrial dehydrogenases, which are active only in live cells. BV2 cells were plated in 96-well plates at a density 8 × 10^3 cells per well for stability. After cultured in DMEM without FBS for 12 h, cells were treated with various concentrations of BPA (0.01 nM/l–100 μM/l) for 12 or 24 h and then incubated in 0.5 mg/ml MTT solution. Viabilities were determined using colorimetric MTT assay on microplate reader.
Immunofluorescence Analysis
Glass bottom dishes containing 100–200 cells/mm2 were fixed with 4 % paraformaldehyde for 20 min followed by treatment with 0.2 % Triton (−20 °C) for 15 min and three rinses in phosphate-buffered saline. Samples were blocked with 5 % bovine serum albumin in phosphate-buffered saline-Tween-20 (PBST) for 30 min and incubated in PBST containing 1 % bovine serum albumin rabbit anti-mouse CD11b monoclonal antibody (1:1,000) overnight, 4 °C. Dishes were further incubated with TRITC-conjugated goat anti-rabbit-IgG secondary antibody (1:100) for 2 h (37 °C). After three rinses in PBS (5 min each), DAPI was finally incubated. The samples were mounted and observed under a ZEISS confocal laser scanning microscope 700.
Isolation of Total RNA and Real-Time PCR
BV2 microglial cells were treated with the indicated concentrations of BPA for 6 or 12 h and total RNA was extracted by using TRIZOL (TaKaRa Bio, Inc., Japan) according to the manufacturer’s instruction. One microgram RNA was reverse-transcribed using PrimeScriptTM RT Master Regent (TaKaRa). Then cDNA was amplified by PCR using specific primer CD11b (forward 5′-TATGGAGCATCAATAGCCAGCCT-3′ and reverse 5′-GAGATCCTTACCCCCACTCAGAGAC-3′), CD68 (forward 5′-TCTGATCTTGCTAGGACCGCTTATA-3′ and reverse 5′-TGTGAACTGTGACATTTCCGTGACT-3′), TNF-α (205 bp) (forward 5′-GACCCTCACACTCAGATCAT-3′ and reverse 5′-TTGAAGAGAACCTGGGAGTA-3′), IL-6 (265 bp) (forward 5′-GAGGATACCACTCCCAACAGACC-3′ and reverse 5′-AAGTGCATCATCGTTGTTCATACA-3′), and β-actin (263 bp) (forward 5′-ATGTACGTAGCCATCCAGGC-3′ and reverse 5′-AGGAAGGAAGGCTGGAAGAG-3′) according to SYBR Premix Ex TaqTM (TaKaRa) manufacturer’s instruction. The temperature profile was as follows: initial denaturation at 95 °C for 30 s, 40 cycles of PCR step at 95 °C for 5 s and then 60 °C for 31 s. β-Actin was used as an internal control to evaluate relative expression of IL-6 and TNF-α.
Enzyme-Linked Immunosorbent Assay
Levels of TNF-α and IL-6 in the culture media were quantified using enzyme-linked immunosorbent assay (ELISA) kits (R&D Systems, Minneapolis, MN, USA). Quantification of ELISA results was performed using the microplate reader set to a test wavelength of 450 nm and corrected for the absorbance at 540 nm, according to the manufacturer’s instructions.
Western Blot Analysis
BV2 microglial cells were treated with the indicated concentrations of BPA for specific hours and then cells were harvested, washed once with ice-cold PBS, and gently lysed for 20 min in protein lysis buffer, RIPA (Sigma). Lysates were centrifuged at 15,000 rpm at 4 °C for 15 min to obtain the supernatants. Then, supernatants were collected and protein concentrations were determined using Pierce BCA protein assay reagent (Thermo Scientific Rockford, IL, USA). Samples with the equal amounts of protein were loaded onto 10 % sodium dodecyl sulfate–polyacrylamide gels, subjected to electrophoresis, and subsequently blotted onto 0.20 μM PVDF membrane (Millipore, USA). The immunoblot was incubated for 2 h with blocking solution (5 % nonfat milk or 5 % BSA in TBS-T for phosphorylated protein) at room temperature, followed by incubation overnight with a primary antibody at 4 °C. Membranes were washed three times with Tween 20/Tris-buffered saline (TBST) and incubated with a 1:50,000 dilution of secondary antibody (Sigma) for 2 h at room temperature. Membranes were again washed five times with TBST and then developed by Chemiluminescent HRP Substrate (Millipore Corporation, Billerica, MA, USA). Band densities were normalized to β-actin in each sample.
Statistical Analysis
Results were expressed as the mean ± standard deviation. Statistically significant values were compared using Student’s t test, ANOVA, and Dunnett’s post hoc test, and P values of less than 0.05 were considered statistically significant. All statistical analyses were performed using SPSS v.17.0 statistical analysis software (SPSS Inc., USA).
RESULTS
Effects of BPA on Cell Viability in BV2 Cells
BV2 cells were incubated with varied concentration (0.01 nM/l–100 μM/l) of BPA for 12 and 24 h, and then cell injury was evaluated by MTT assay. As shown in Fig. 1, 0.01 nM–10 μM BPA did not obviously affect the cell viability; however, 100 μM BPA dramatically contributed to microglial cell injury with approximately 60 % reduction of cell viability compared with control group. To rule out the cell death mediated by BPA, 10 nM/l to 1 μM/l BPA were selected for the subsequent experiments.
Effects of BPA on cell viability in BV2 microglial cells. Cells were treated with the indicated concentrations of BPA (10^−2–10^5 nM/l) for 12 and 24 h, then cell viability was measured by MTT assay. The results were shown as the percentage of surviving cells compared with control cells. Data are expressed as the mean ± S.E. of three independent experiments, performed in triplicate. Statistical significance was determined by ANOVA and Dunnett’s post hoc test (**P < 0.01 vs. the control group).
Effects of BPA on Microglial Activation
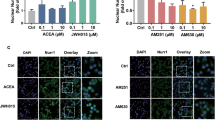
The morphologic change in glial cell is considered as a hallmark of glial activation, giving credit to its secretion of cytokine mediators. Also, increased expression of CD11b, the beta-integrin marker of microglial, as well as CD68, represents microglial activation during neurodegenerative inflammation [28]. To explore whether BPA treatment contributed to activation of BV2 cells, immunoflurescence analysis and real-time PCR were performed to determine the resting or activated state of MG qualitatively and quantitatively. Figure 2a represented red fluorescence labeled by rabbit anti-mouse CD11b monoclonal antibody, as this was observed in normal resting BV2 cells. As the positive control, LPS-stimulated cells demonstrated rather high expression of CD11b protein along with typical morphologic changes of activation. Figure 2c presented kinds of process-bearing cell types, both bipolar and tripolar, and also amoeboid types with swelling round cell bodies. BPA-treated cells in Fig. 2b also showed signs of activation with ramified shape and higher level of CD11b expression, compared to the control group. This was confirmed by real-time PCR analysis that significant enhancement in CD11b and CD68 mRNA were observed in BPA-treated groups (Fig. 2d, e). All these results suggested that BPA might lead to MG activation at a nanomole scale in BV2 cells.
Effects of BPA on microglial activation in BV2 cells. Cells were cultured on glass bottom dishes at a density of 100–200 cells/mm2. All cells were fixed and stained with rabbit anti-mouse CD11b monoclonal antibody (red) and DAPI (blue). a The negative control group treated with non-FBS DMEM. b Representative photos of cells treated with BPA (100 nM/l) for 12 h. c Representative photos of cells incubated with LPS (0.5 μg/ml) for 12 h. Laser scanning microscope (oil scope) ×630. d, e Total RNA was prepared for the real-time PCR analysis of CD11b and CD68 gene expression from BV2 microglial cells treated with BPA (10, 100, 1,000 nM/l) for 12 h. Data are expressed as the mean ± S.E. of three independent experiments, performed in triplicate. Statistical significance was determined by ANOVA and Dunnett’s post hoc test (*P < 0.05, **P < 0.01 vs. the control group).
Effects of BPA on IL-6 and TNF-α in BV2 Cells
Based on the typical changes in microglial morphology and phenotype, we then evaluated the effects of BPA on pro-inflammatory cytokines, using real-time PCR analysis and ELISA. As depicted in Fig. 3, treatment of BPA markedly up-regulated IL-6 and TNF-α mRNA expression (Fig. 3a, b). As mRNA level is not always corresponded with protein expression, we next investigated the effects of BPA on IL-6 and TNF-α expression by ELISA. Similarly, it suggested that BPA specifically facilitated IL-6 and TNF-α expression in a dose-dependent manner (Table 1).
Effects of BPA on IL-6 (a) and TNF-α (b) mRNA expression in BV2 microglial cells. Total RNA was prepared for the real-time PCR analysis of IL-6 and TNF-α gene expression from BV2 microglial cells treated with BPA (10, 100, 1,000 nM/l) for 6 h. Data are expressed as the mean ± S.E. of three independent experiments, performed in triplicate. Statistical significance was determined by ANOVA and Dunnett’s post hoc test (*P < 0.05, **P < 0.01 vs. the control group).
Effects of Estrogen Receptor on BPA-Induced IL-6 and TNF-α
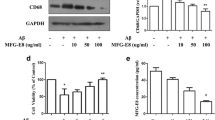
Because EDCs are able to serve as inflammatory inducers partially via the estrogen receptor, we examined whether ER was involved in the regulatory activity of BPA [25]. As shown in Fig. 4, the addition of ER-specific antagonist ICI182780 (10 μM) was able to partially suppress BPA-induced TNF-α production (Fig. 4a) and was capable of blocking IL-6 secretion in the presence of BPA (Fig. 4b). With the western blot assay (Fig. 4c), BV2 cells expressed only detectable levels of ERβ, so it was convincible that the suppressive effects of ICI182780 on CK might primarily mediated by ERβ [29].
Effects of estrogen receptor pathway on BPA mediated IL-6 and TNF-α expression. After 1 h pretreatment with ICI182780 (10 μM/L), BV2 cells were incubated with (100 nM/l) BPA for 24 h. Supernatants were collected for protein analysis of IL-6 (a) and TNF-α (b) by ELISA. Data are expressed as the mean ± S.E. of three independent experiments, performed in triplicate. Statistical significance was determined by ANOVA and Dunnett’s post hoc test (**P < 0.01 vs. the control group; ##P < 0.01 vs. the BPA treated group). c Western blot were performed to identify the subunit of estrogen receptor (ERα and ERβ).
Effects of BPA on ERK1/2 and JNK Activation in BV2 Cells
MAPK family has long been studied with its relation to inflammatory reaction. Therefore, we next explored whether MAPKs signal pathways were involved in BPA-mediated IL-6 and TNF-α expression. As shown in Fig. 5, BPA obviously activated ERK1/2 and JNK pathways. It was worth mentioning that nanomolar BPA (10–1,000 nM) elicited a rapid phosphorylation of ERK1/2 in a dose-dependent manner (Fig. 5b). Meanwhile, BPA significantly activated ERK1/2 within 10 min. It rose rapidly to a peak between 10 and 30 min and then gradually returned to a steady level (Fig. 5a). In addition, the appearance of JNK as well as p-JNK fragments was also quantified by western blot. Similarly, our data showed that a rapid phosphorylation of JNK was first detectable at 10 min and started to decline by 60 min. As we speculated, BPA activated the JNK pathway in a dose-dependent manner, which manifested a specific effect of BPA on JNK signaling pathway (Fig. 5c, d).
Effects of BPA on p-ERK, ERK, p-JNK, JNK expression in BV2 microglial cells. a Effects of 100 nM/l BPA on ERK1/2 pathway at different time points (10 min, 20 min, 30 min, 1 h, 3 h, 6 h, 12 h) or b effects of BPA on ERK1/2 pathway with various concentrations (10, 100, 1,000 nM/l) for 12 h. c Effects of 100 nM/l BPA on JNK pathway at different time points (10 min, 20 min, 30 min, 1 h, 3 h, 6 h, 12 h) or d effects of BPA on JNK pathway with varied concentrations (10, 100, 1,000 nM/l) for 12 h. β-Actin levels performed in parallel served as controls. The experiments were repeated three times, and similar results were obtained. Statistical significance was determined by ANOVA and Dunnett’s post hoc test (**P < 0.01 vs. the control group).
Having determined the specific effects of BPA on ERK1/2 and JNK in BV2 cells, we then consequently asked whether ERK1/2 and JNK pathways were involved in BPA-mediated inflammatory reaction. The BV2 cells were incubated with PD98059 (ERK1/2 antagonist) and SP600125 (JNK inhibitor) for 1 h prior to BPA exposure, then TNF-α and IL-6 expression was subjected to real-time PCR assay and ELISA. As shown in Fig. 6, SP600125 obviously suppressed TNF-α and IL-6 mRNA expression in BV2 cells, whereas PD98059 markedly inhibited TNF-α expression and slightly decreased IL-6 level though the data showed no significant differences. The ELISA analyses showed that both PD98059 and SP600125 were capable to attenuate the production of TNF-α and slightly decreased IL-6 secretion. The inconformity of mRNA and protein expression suggested a post-transcriptional regulation might function via activation of MAPK cascades.
Effects of ERK1/2 and JNK pathways on BPA mediated IL-6 and TNF-α expression. Total RNA was prepared for the real-time PCR analysis of IL-6 (a) and TNF-α (b) mRNA expression from BV2 microglial cells pretreated with PD98059 or SP600125 1 h and then incubated 100 nM/l BPA for 6 h. In parallel, the protein level of IL-6 and TNF-α was detected by ELISA following PD98059 or SP600125 treatment. Cells were treated with BPA (100 nM/l) for 24 h, then the culture media was collected. Levels of IL-6 (c) and TNF-α (d) in the supernatants were quantified using ELISA kits. Data are expressed as the mean ± S.E. of three independent experiments, performed in triplicate. Statistical significance was determined by ANOVA and Dunnett’s post hoc test (*P < 0.05, **P < 0.01 vs. the control group; #P < 0.05, ##P < 0.01 vs. the BPA-treated group).
Effects of BPA on NF-κB Activation in BV2 Cells
Since the MAPKs pathways are known to be involved in Iκκ-dependent NF-κB activation and NF-κB is known to exert transcriptional regulation of TNF-α and other pro-inflammatory cytokines genes, we then focused on NF-κB transcription and activation. As depicted in Fig. 7, BPA significantly increased levels of phosphorylated NF-κB p65 in a time- and dose-dependent manner, the maximum expression levels were observed at 12 h and 1 μM, respectively. These results suggested that NF-κB might be involved in BPA-mediated inflammatory reaction in BV2 cells.
Effects of BPA on p-NF-κB, NF-κB protein expression in BV2 microglial cells. Cells were treated with 100 nM/l BPA at varied time points (15 min, 30 min, 1 h, 3 h, 6 h, 12 h) or various concentrations of BPA (10, 100, 1,000 nM/l) for 12 h, respectively. Then, the cell lysates were prepared and western blot were performed to analyze time course (a) or dose response (b) of phosphorylated NF-κB and total NF-κB. β-Actin levels performed in parallel served as controls. The experiments were repeated three times, and similar results were obtained. Statistical significance was determined by ANOVA and Dunnett’s post hoc test (**P < 0.01 vs. the control group).
DISCUSSION
Microglial cells have been recognized as the major frontline guardian of immune defense in the central nervous system and exert their regulatory functions, in part, through the release of cytokines after activation and/or inflammatory insults [20, 21]. Results from recent epidemiologic and experimental studies have suggested the potential role of exposure to EDCs in modifying the immune homeostatic state [11]. Therefore, understanding the target and regulatory pathways of EDCs, particularly in MG, would contribute to advancing knowledge about EDC involvement in the development of immunologic neurodegenerative diseases. In the present study, we found BPA, one of the most common EDCs, targeted and regulated cytokine responses of BV2 cells via ERβ signaling, MAPK activation, and NF-κB pathway.
The role of microglial cells play on immunity reaction as well as neurodegeneration diseases has long been discussed [21]. Our study showed BPA-stimulated BV2 cells displayed in the process-bearing form, which was reported to exhibit further progressive activation with highly proliferative activity [30, 31]. We also found BPA de novo did not perform cytotoxicity of BV2 cells under indicated concentrations, so the releasing of pro-inflammatory mediators should be subsequent to the activation of microglial cells, which in turn could contribute to the immunoregulatory effects on central nervous system. In vitro studies, Yamashita reported that treatment of BPA (0.01 to 1 μM) contributed to secretion of a higher level of IL-1, IL-6, TNF, and MCP-1 compared to the control group in murine spleen cells and thymus cells, which was in accordance with our study in BV2 cells [32]. Whereas higher level of BPA (1 to 50 μM) exerted a potential ability to decrease NO and TNF-α induced by LPS in macrophage cells [33], suggesting that diverse cell types and doses may lead to differential inflammation consequences. In the present study, we found that the IL-6 and TNF-α mRNA expression after BPA exposure did not show characteristic dose-dependent manner, this may explained by Laura’s reports that non-monotonic dose response curves (NMDRCs) are common in the BPA in vitro literature [34]. However, further detailed work is needed to address these issues. Also, of interest, the TNF-α and IL-6 mRNA expression was not totally corresponded with protein excretion; it might be due to the post-transcriptional regulation, which contains a time-delayed component [35].
The ability of estrogen to modulate microglial inflammatory capacity via interaction with ERs (mainly ERα and ERβ) has been extensively established [36–38]. As one kind of EDCs, BPA is described to perform both anti- and/or mimic estrogen properties and it acts as cell type-specific agonists (≥10 nM) or antagonists (≤10 nM) dependent on differential treatments [39]. To examine the involvement of the ER axis, our data demonstrated that BPA could exert modulatory effects on inflammatory factors expression via interactions with ERβ (ERα is naturally undetectable in BV2 cell line), or a compensatory mechanism for the lack of ERα expression, on account that ICI182780 could cause significant reduction in TNF-α and IL-6 production. The selectively suppressive effects of ER antagonist on CK secretion were observed in other EDCs, like 4-OP and NP [40]. The classic ERE-dependent mechanisms may lie in estrogenic IL-6 secretion, since previous study sustained the fact that in human osteoblastic cells, the IL-6 promoter is inhibited by E2 in the absence of a functional ER binding site, which is mediated via down-regulation of NF-κB and C/EBP [41]. Additionally, physiologically high concentration of 17β-estradiol and ERβ elevated TNF-α expression by direct enhancement of NF-κB activity on human T cells [42]. EDCs may also act in non-ERE-dependent mechanism, evidence indicates that E2 and estrogenic EDCs (NP, 4-OP, BPA) may induce rapid ERK phosphorylation and PI3K activation via genomic responses in MCF-7 [43–45]. The further mechanisms linking ERs to MAPKs and NF-κB signaling pathway in BPA-evoked MG activation need to be fully addressed.
Inflammatory cytokines are regulated in multiple levels: transcriptional, post-transcriptional, and post-translational. Transcriptional regulation of TNF-α and other cytokines is complex, which is involving a number of transcriptional factors (TFs), including NF-κB, AP-1, and various members of the C/EBP, ATF/CREB, and STAT family [46–48]. Of all, NF-κB is considered a widely use strategy to suppress the inflammatory reaction and as the critical factor to link the cytoplasmic and nuclear signal transduction. In unstimulated cells, NF-κB is retained in the cytoplasm by binding to IκB-α. Once activated, NF-κB, via phosphorylated its endogenous inhibitors IκB-α, results in nuclear translocation, which is considered as a key process to regulate the gene of certain cytokines genes, like iNOS, COX-2, and TNF-alpha [49, 50]. Lee et al. reported that the treatment of BPAF (with similar chemical structure as BPA) at the concentration of 200 μM/l caused IκB-α to decrease while NF-κB continued to increase in HT-22 cells (murine hippocampal cell line) [51], showing a close correspondence with our study. Other research also determined that BPA could change the transcriptional capacity of NF-κB by modifying various transcriptional factors, like sp1 which influenced the combining site of NF-κB [39]. All these results supported our speculation that at least, in microglial cells, NF-κB might be participated in BPA-mediated inflammatory reaction.
The MAPK family has been implicated as a classic mediator of signal transduction pathways related to inflammatory responses. ERK is stimulated primarily by growth factors and tumor promoters, and JNK is activated in response to inflammatory agents and environmental stress [52]. In our study, ERK1/2 and JNK pathways could be rapidly activated in 30 min, reaching a relatively high level when compared to the control group, and both proteins displayed a dose-dependent manner. Corresponding to this, in cerebellar granule cells, BPA increased ERK1/2 phosphorylation within 2–4 min with simultaneous neural impairment [53]. Consistent with the findings aforementioned, we found that SP600125, a JNK inhibitor, could partially retard BPA-induced TNF-α production, suggesting JNK’s crucial function in this inflammatory process. p38 MAPK, as another vital member of MAPK pathway, is widely studied as a modulating factor of cell impairment procedure, while in our study, phosphorylated p38 was not detectable (data not shown), which might result from trivial BPA-evoked microglial toxicity. In addition, the impact of BPA on MAPK was observed within seconds to minutes, while NF-κB p65 persistently elevated in observed period within 12 h, as is reported that each of the three MAPKs modules has the potential to elicit transcriptional activation via phosphorylation of different sets of TFs, the actual mechanistic link between them remains to be fully addressed [27, 54, 55].
In summary, our findings represent the demonstration that BPA possesses glial activation and exerts its action on inflammatory response in microglial cells, the inflammatory reaction mediated by BPA were partially via ER signaling, MAPKs and NF-κB pathways. Further studies are necessary to elucidate the immunomodulatory effects in vivo models.
REFERENCES
Schug, T.T., A. Janesick, B. Blumberg, and J.J. Heindel. 2011. Endocrine disrupting chemicals and disease susceptibility. The Journal of Steroid Biochemistry and Molecular Biology 127: 204–215.
Casals-Casas, C., and B. Desvergne. 2011. Endocrine disruptors: from endocrine to metabolic disruption. Annual Review of Physiology 73: 135–162.
DiVall, S.A. 2013. The influence of endocrine disruptors on growth and development of children. Current Opinion in Endocrinology Diabetes and Obesity 20: 50–55.
Crisp, T.M., E.D. Clegg, R.L. Cooper, W.P. Wood, D.G. Anderson, K.P. Baetcke, J.L. Hoffmann, M.S. Morrow, D.J. Rodier, J.E. Schaeffer, L.W. Touart, M.G. Zeeman, and Y.M. Patel. 1998. Environmental endocrine disruption: an effects assessment and analysis. Environmental Health Perspectives 106(Suppl 1): 11–56.
Fernandez, M.F., B. Olmos, A. Granada, M.J. Lopez-Espinosa, J.M. Molina-Molina, J.M. Fernandez, M. Cruz, F. Olea-Serrano, and N. Olea. 2007. Human exposure to endocrine-disrupting chemicals and prenatal risk factors for cryptorchidism and hypospadias: a nested case-control study. Environmental Health Perspectives 115(Suppl 1): 8–14.
Elsworth, J.D., J.D. Jentsch, C.A. Vandevoort, R.H. Roth, D.E. Jr, and C. Leranth. 2013. Prenatal exposure to bisphenol A impacts midbrain dopamine neurons and hippocampal spine synapses in non-human primates. Neurotoxicology 35: 113–120.
Maffini, M.V., B.S. Rubin, C. Sonnenschein, and A.M. Soto. 2006. Endocrine disruptors and reproductive health: the case of bisphenol-A. Molecular and Cellular Endocrinology 254–255: 179–186.
Richter, C.A., L.S. Birnbaum, F. Farabollini, R.R. Newbold, B.S. Rubin, C.E. Talsness, J.G. Vandenbergh, D.R. Walser-Kuntz, and F.S. vom Saal. 2007. In vivo effects of bisphenol A in laboratory rodent studies. Reproductive Toxicology 24: 199–224.
Kim, M.E., H.R. Park, E.J. Gong, S.Y. Choi, H.S. Kim, and J. Lee. 2011. Exposure to bisphenol A appears to impair hippocampal neurogenesis and spatial learning and memory. Food and Chemical Toxicology: An International Journal Published for the British Industrial Biological Research Association 49: 3383–3389.
Yang, L., L. Luo, W. Ji, C. Gong, D. Wu, H. Huang, Q. Liu, B. Xia, G. Hu, W. Zhang, Q. Zhang, J. Liu, and Z. Zhuang. 2013. Effect of low dose bisphenol A on the early differentiation of human embryonic stem cells into mammary epithelial cells. Toxicology Letters 218: 187–193.
Rogers, J.A., L. Metz, and V.W. Yong. 2013. Review: Endocrine disrupting chemicals and immune responses: a focus on bisphenol-A and its potential mechanisms. Molecular Immunology 53: 421–430.
Meeker, J.D., and K.K. Ferguson. 2011. Relationship between urinary phthalate and bisphenol A concentrations and serum thyroid measures in U.S. adults and adolescents from the National Health and Nutrition Examination Survey (NHANES) 2007-2008. Environmental Health Perspectives 119: 1396–1402.
Kubo, K., O. Arai, M. Omura, R. Watanabe, R. Ogata, and S. Aou. 2003. Low dose effects of bisphenol A on sexual differentiation of the brain and behavior in rats. Neuroscience Research 45: 345–356.
Liu, C., W. Duan, R. Li, S. Xu, L. Zhang, C. Chen, M. He, Y. Lu, H. Wu, H. Pi, X. Luo, Y. Zhang, M. Zhong, Z. Yu, and Z. Zhou. 2013. Exposure to bisphenol A disrupts meiotic progression during spermatogenesis in adult rats through estrogen-like activity. Cell Death and Disease 4: e676.
Spence, R.D., A.J. Wisdom, Y. Cao, H.M. Hill, C.R. Mongerson, B. Stapornkul, N. Itoh, M.V. Sofroniew, and R.R. Voskuhl. 2013. Estrogen mediates neuroprotection and anti-inflammatory effects during EAE through ERalpha signaling on astrocytes but not through ERbeta signaling on astrocytes or neurons. The Journal of Neuroscience: the Official Journal of the Society for Neuroscience 33: 10924–10933.
Gosselin, D., and S. Rivest. 2011. Estrogen receptor transrepresses brain inflammation. Cell 145: 495–497.
Spence, R.D., and R.R. Voskuhl. 2012. Neuroprotective effects of estrogens and androgens in CNS inflammation and neurodegeneration. Frontiers in Neuroendocrinology 33: 105–115.
Loram, L.C., P.W. Sholar, F.R. Taylor, J.L. Wiesler, J.A. Babb, K.A. Strand, D. Berkelhammer, H.E. Day, S.F. Maier, and L.R. Watkins. 2012. Sex and estradiol influence glial pro-inflammatory responses to lipopolysaccharide in rats. Psychoneuroendocrinology 37: 1688–1699.
Graeber, M.B., W. Li, and M.L. Rodriguez. 2011. Role of microglia in CNS inflammation. FEBS Letters 585: 3798–3805.
Zhang, W., K. Phillips, A.R. Wielgus, J. Liu, A. Albertini, F.A. Zucca, R. Faust, S.Y. Qian, D.S. Miller, C.F. Chignell, B. Wilson, V. Jackson-Lewis, S. Przedborski, D. Joset, J. Loike, J.S. Hong, D. Sulzer, and L. Zecca. 2011. Neuromelanin activates microglia and induces degeneration of dopaminergic neurons: implications for progression of Parkinson's disease. Neurotoxicity Research 19: 63–72.
Glass, C.K., K. Saijo, B. Winner, M.C. Marchetto, and F.H. Gage. 2010. Mechanisms underlying inflammation in neurodegeneration. Cell 140: 918–934.
Glezer, I., A.R. Simard, and S. Rivest. 2007. Neuroprotective role of the innate immune system by microglia. Neuroscience 147: 867–883.
Choi, Y., M.K. Lee, S.Y. Lim, S.H. Sung, and Y.C. Kim. 2009. Inhibition of inducible NO synthase, cyclooxygenase-2 and interleukin-1beta by torilin is mediated by mitogen-activated protein kinases in microglial BV2 cells. British Journal of Pharmacology 156: 933–940.
Cordle, A., and G. Landreth. 2005. 3-Hydroxy-3-methylglutaryl-coenzyme A reductase inhibitors attenuate beta-amyloid-induced microglial inflammatory responses. The Journal of Neuroscience: the Official Journal of the Society for Neuroscience 25: 299–307.
Tabb, M.M., and B. Blumberg. 2006. New modes of action for endocrine-disrupting chemicals. Molecular Endocrinology 20: 475–482.
Carnevale, D., R. De Simone, and L. Minghetti. 2007. Microglia-neuron interaction in inflammatory and degenerative diseases: role of cholinergic and noradrenergic systems. CNS & Neurological Disorders Drug Targets 6: 388–397.
Bhat, N.R., P. Zhang, J.C. Lee, and E.L. Hogan. 1998. Extracellular signal-regulated kinase and p38 subgroups of mitogen-activated protein kinases regulate inducible nitric oxide synthase and tumor necrosis factor-alpha gene expression in endotoxin-stimulated primary glial cultures. The Journal of Neuroscience : the Official Journal of the Society for Neuroscience 18: 1633–1641.
Roy, A., Y.K. Fung, X. Liu, and K. Pahan. 2006. Up-regulation of microglial CD11b expression by nitric oxide. The Journal of Biological Chemistry 281: 14971–14980.
Baker, A.E., V.M. Brautigam, and J.J. Watters. 2004. Estrogen modulates microglial inflammatory mediator production via interactions with estrogen receptor beta. Endocrinology 145: 5021–5032.
Laurenzi, M., C. Arcuri, R. Rossi, P. Marconi, and V. Bocchini. 2001. Effects of microenvironment on morphology and function of the microglial cell line BV-2. Neurochemical Research 26: 1209–1216.
Glenn, J.A., S.A. Ward, C.R. Stone, P.L. Booth, and W.E. Thomas. 1992. Characterisation of ramified microglial cells: detailed morphology, morphological plasticity and proliferative capability. Journal of Anatomy 180(Pt 1): 109–118.
Yamashita, U., T. Sugiura, Y. Yoshida, and E. Kuroda. 2005. Effect of endocrine disrupters on macrophage functions in vitro. Journal of UOEH 27: 1–10.
Young Kim, J., and H. Gwang Jeong. 2003. Down-regulation of inducible nitric oxide synthase and tumor necrosis factor-α expression by bisphenol A via nuclear factor-κB inactivation in macrophages. Cancer Letters 196: 69–76.
Vandenberg, L.N. 2014. Non-monotonic dose responses in studies of endocrine disrupting chemicals: bisphenol a as a case study. Dose-Response 1: 1–18.
Wang, H., Q. Wang, U.J. Pape, B. Shen, J. Huang, B. Wu, and X. Li. 2010. Systematic investigation of global coordination among mRNA and protein in cellular society. BMC Genomics 11: 364.
Straub, R.H. 2007. The complex role of estrogens in inflammation. Endocrine Reviews 28: 521–574.
Vegeto, E., C. Bonincontro, G. Pollio, A. Sala, S. Viappiani, F. Nardi, A. Brusadelli, B. Viviani, P. Ciana, and A. Maggi. 2001. Estrogen prevents the lipopolysaccharide-induced inflammatory response in microglia. The Journal of Neuroscience: the Official Journal of the Society for Neuroscience 21: 1809–1818.
Bruce-Keller, A.J., J.L. Keeling, J.N. Keller, F.F. Huang, S. Camondola, and M.P. Mattson. 2000. Antiinflammatory effects of estrogen on microglial activation. Endocrinology 141: 3646–3656.
Li, Y., K.A. Burns, Y. Arao, C.J. Luh, and K.S. Korach. 2012. Differential estrogenic actions of endocrine-disrupting chemicals bisphenol A, bisphenol AF, and zearalenone through estrogen receptor alpha and beta in vitro. Environmental Health Perspectives 120: 1029–1035.
Hung, C.H., S.N. Yang, P.L. Kuo, Y.T. Chu, H.W. Chang, W.J. Wei, S.K. Huang, and Y.J. Jong. 2010. Modulation of cytokine expression in human myeloid dendritic cells by environmental endocrine-disrupting chemicals involves epigenetic regulation. Environmental Health Perspectives 118: 67–72.
Stein, B., and M.X. Yang. 1995. Repression of the interleukin-6 promoter by estrogen receptor is mediated by NF-kappa B and C/EBP beta. Molecular and Cellular Biology 15: 4971–4979.
Hirano, S., D. Furutama, and T. Hanafusa. 2007. Physiologically high concentrations of 17beta-estradiol enhance NF-kappaB activity in human T cells. American Journal of Physiology. Regulatory, Integrative and Comparative Physiology 292: R1465–R1471.
Bulayeva, N.N., B. Gametchu, and C.S. Watson. 2004. Quantitative measurement of estrogen-induced ERK 1 and 2 activation via multiple membrane-initiated signaling pathways. Steroids 69: 181–192.
Watson, C.S., N.N. Bulayeva, A.L. Wozniak, and R.A. Alyea. 2007. Xenoestrogens are potent activators of nongenomic estrogenic responses. Steroids 72: 124–134.
Cobb, M.H., and E.J. Goldsmith. 1995. How MAP kinases are regulated. Journal of Biological Chemistry 270: 14843–14846.
Hohmann, H.P., M. Brockhaus, P.A. Baeuerle, R. Remy, R. Kolbeck, and A.P. van Loon. 1990. Expression of the types A and B tumor necrosis factor (TNF) receptors is independently regulated, and both receptors mediate activation of the transcription factor NF-kappa B. TNF alpha is not needed for induction of a biological effect via TNF receptors. The Journal of Biological Chemistry 265: 22409–22417.
Classen, A., B.N. Kalali, C. Schnopp, C. Andres, J.A. Aguilar-Pimentel, J. Ring, M. Ollert, and M. Mempel. 2011. TNF receptor I on human keratinocytes is a binding partner for staphylococcal protein A resulting in the activation of NF kappa B, AP-1, and downstream gene transcription. Experimental Dermatology 20: 48–52.
Jongeneel, C.V. 1995. Transcriptional regulation of the tumor necrosis factor α gene. Immunobiology 193: 210–216.
Beg, A.A., S.M. Ruben, R.I. Scheinman, S. Haskill, C.A. Rosen, and A.S. Baldwin. 1992. I kappa B interacts with the nuclear localization sequences of the subunits of NF-kappa B: a mechanism for cytoplasmic retention. Genes & Development 6: 1899–1913.
Oeckinghaus, A., M.S. Hayden, and S. Ghosh. 2011. Crosstalk in NF-kappaB signaling pathways. Nature Immunology 12: 695–708.
Lee, S., Y.K. Kim, T.Y. Shin, and S.H. Kim. 2013. Neurotoxic effects of bisphenol AF on calcium-induced ROS and MAPKs. Neurotoxicity Research 23: 249–259.
Cargnello, M., and P.P. Roux. 2011. Activation and function of the MAPKs and their substrates, the MAPK-activated protein kinases. Microbiology and Molecular Biology Reviews MMBR 75: 50–83.
Belcher, S.M., H.H. Le, L. Spurling, and J.K. Wong. 2005. Rapid estrogenic regulation of extracellular signal- regulated kinase 1/2 signaling in cerebellar granule cells involves a G protein- and protein kinase A-dependent mechanism and intracellular activation of protein phosphatase 2A. Endocrinology 146: 5397–5406.
Guma, M., D. Stepniak, H. Shaked, M.E. Spehlmann, S. Shenouda, H. Cheroutre, I. Vicente-Suarez, L. Eckmann, M.F. Kagnoff, and M. Karin. 2011. Constitutive intestinal NF-kappaB does not trigger destructive inflammation unless accompanied by MAPK activation. The Journal of Experimental Medicine 208: 1889–1900.
Olajide, O.A., M.A. Aderogba, and B.L. Fiebich. 2013. Mechanisms of anti-inflammatory property of Anacardium occidentale stem bark: inhibition of NF-kappaB and MAPK signalling in the microglia. Journal of Ethnopharmacology 145: 42–49.
ACKNOWLEDGMENTS
This work was supported by the National Natural Science Foundation of China (81273115, 81072329, and 81202230) and the Priority Academic Program Development (PAPD) of Jiangsu Higher Education Institutions.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Jingying Zhu and Lei Jiang have contributed equally to this study.
Rights and permissions
About this article
Cite this article
Zhu, J., Jiang, L., Liu, Y. et al. MAPK and NF-κB Pathways Are Involved in Bisphenol A-Induced TNF-α and IL-6 Production in BV2 Microglial Cells. Inflammation 38, 637–648 (2015). https://doi.org/10.1007/s10753-014-9971-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-014-9971-5