Abstract
In previous study, the anti-inflammatory effect of morin had been found. In this study, we investigated anti-inflammatory effects of morin on acute lung injury using lipopolysaccharide (LPS)-induced acute lung injury (ALI) mouse model. The cell counting in the bronchoalveolar lavage fluid (BALF) was measured. The animal lung edema degree was evaluated by wet/dry weight (W/D) ratio. The superoxidase dismutase (SOD) activity and myeloperoxidase (MPO) activity were assayed by SOD and MPO kits, respectively. The levels of inflammatory mediators including tumor necrosis factor-α (TNF-α), interleukin (IL)-1β, IL-18, and IL-6 were assayed by enzyme-linked immunosorbent assay method. Pathological changes of lung tissues were observed by hematoxylin and eosin (HE) staining. The protein level of lung NACHT, LRR, and PYD domains-containing protein 3 (NLRP3) inflammasome was measured by Western blotting. The data showed that treatment with the morin markedly attenuated inflammatory cell numbers in the BALF, decreased lung NLRP3 inflammasome protein level, and improved SOD activity and inhibited MPO activity. Histological studies demonstrated that morin substantially inhibited LPS-induced neutrophils in lung tissue compared with model group. The results indicated that the morin had a protective effect on LPS-induced ALI in mice.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Acute lung injury (ALI), or its more severe form, acute respiratory distress syndrome (ARDS), characterized by severe hypoxemia, pulmonary edema, and neutrophil accumulation in the lung, is a common clinical problem associated with significant morbidity and mortality in shock, sepsis, and ischemia reperfusion, etc. [1, 2]. ALI is a major clinical problem that has a high mortality rate of 30 to 40 % despite significant advances in antimicrobial therapy and supportive care made in the past few decades. There are still few effective measures or specific medicines to treat it [3]. The inflammatory process played a key role in the development of ALI, and the main pathological change of ALI was acute leakage inflammatory response with leakage of protein into the alveolar space, inflammatory cell accumulation, interstitial edema, and disruption of epithelial integrity [4]. Therefore, it was significant that anti-inflammatory drugs were used to reduce lung injury at early stage of ALI.
The intratracheal administration of lipopolysaccharide (LPS) had been extensively used to study the pathogenesis and intervention of ALI. As a bacterial cell membrane component, LPS was known to induce the production of numerous inflammatory cytokines and chemokines [5, 6].
Highly inflammatory cytokines of the interleukin (IL)-1 family, including IL-1β and IL-18, are central to processes mediating lung inflammation. The proteolytic activation of these cytokines is under the control of several innate immune receptors that are able to form large multiprotein signaling platforms, termed inflammasomes. The inflammasome-formed downstream of the receptor NACHT, LRR, and PYD domains-containing protein 3 (NLRP3; alias NALP3) can be activated not only by pathogens but also in response to sterile tissue damage or metabolic stress, resulting in sustained inflammatory reactions. This observation led to the discovery that the NLRP3 inflammasome is central to the pathogenesis of a wide variety of chronic inflammatory diseases, including several common metabolic disorders. The NLRP3 inflammasome is currently the most fully characterized inflammasome, which responds to numerous physically and chemically diverse stimuli, and leads to a series of diseases when out of control. The NLRP3 inflammasome is the most intensively studied of the inflammasomes, and it can be activated by a variety of microbial-, stress-, or danger-induced substances [7]. The products of NLRP3 inflammasome activation, IL-1β and IL-18, have been shown to be protective in a variety of infections [8, 9]. Emerging genetic and pharmacological evidence suggests that NLRP3 inflammasome activation is critical for driving acute lung inflammation aiding in the clearance of viral or bacterial infections.
Morin, a flavonoid constituent of many Chinese herbs and fruits, exhibits significant antioxidant and anti-inflammatory activity [10]. Despite the several known effects of morin, no work on ALI prevention promoted by this compound has been reported to date. The present study was designed to examine the effect of morin on LPS-induced inflammatory in acute lung injury and its possible mechanism.
In this study, the LPS-induced mouse ALI models were used to evaluate the effects of the morin.
METHODS AND MATERIALS
Reagents
Morin (pure 99 %) were purchased from National Institutes for Food and Drug Control (Beijing, China). Dexamethasone was purchased from Xiansheng Drug Store (Nanjing, China). LPS was purchased from Sigma-Aldrich (St. Louis, MO, USA). SOD, MPO, and Wright–Giemsa staining (Nanjing Jiancheng Bioengineering Institute, Nanjing, China) were purchased from the Institute of Jiancheng Bioengineering (Nanjing, China). The enzyme-linked immunosorbent assay (ELISA) kits for determination of tumor necrosis factor-α (TNF-α), IL-1β, IL-18, and IL-6 were produced by Nanjing KeyGen Biotech. Co., Ltd. (Nanjing, China).
Animals
Animal experiment was carried out in accordance with the Guidelines for Animal Experimentation of China Pharmaceutical University, China Pharmaceutical University. A total of 50 female BALB/c mice (18–22 g) obtained from the Experimental Animal Center of China Pharmaceutical University (Nanjing, China). Mice were maintained in an animal facility under standard laboratory conditions for 1 week prior to experiments and provided with water and standard chow ad libitum. All experimental procedures were carried out in accordance with the NIH Guidelines for the Care and Use of Laboratory Animals, and animal handling followed the dictates of the National Animal Welfare Law of China.
Model of Acute Lung Inflammation
The intratracheal instillation was done as previously described [11]. Female BALB/c mice were randomly divided into five groups with ten mice in each group: (1) control group (saline), (2) LPS group, (3) LPS + dexamethasone (LPS + Dex, 2 mg/kg), (4) LPS + morin (20 mg/kg), and (5) LPS + morin (40 mg/kg). The animals were administered with the saline or drugs intragastrically. After 15 min of treatment, mice were anesthetized with chloraldurate (3 %), and 20 μg of LPS in 50 μL phosphate-buffered saline (PBS) was administrated intratracheally to induce acute lung injury. Control group mice were given 50 μL PBS intratracheally.
Bronchoalveolar Lavage
Six hours after intratracheal instillation, the animal was killed and bronchoalveolar lavage (n = 10) was performed three times through a tracheal cannula with 0.5 mL (total volume 1.5 mL) of autoclaved PBS to obtain the bronchoalveolar lavage fluid (BALF). The total leukocyte count was determined using a hemocytometer. BALF samples were centrifuged at 1,500 rpm for 10 min at 4 °C; the supernatants were stored in −80 °C for analysis of cytokine concentrations and SOD activity (Nanjing Jiancheng Bioengineering Institute, Nanjing, China), and the pellet was resuspended in 100 μL of saline, centrifuged onto slides, and stained for 8 min with Wright–Giemsa staining (Nanjing Jiancheng Bioengineering Institute, Nanjing, China). The slides were quantified for macrophages, neutrophils, and lymphocytes by counting a total of 200 cells/slide at × 40 magnification as the differential cell count.
MPO Activity in Lung Homogenates and SOD Levels in BALF
MPO activity in 10 % lung homogenized and SOD activities in the BALF were determined using test kits purchased from Nanjing Jiancheng Bioengineering Institute (Nanjing, China); all procedures were according to the manual. MPO activity was determined by using o-dianisidine as peroxidase substrates, and data were presented as units per gram (U/g) tissue. Total SOD activity included Cu–Zn and Mn SOD activity and was determined by hydroxylamine assay developed from xanthine oxidase, and data were expressed as units per milligram (U/mg) protein. The absorbance at 460 nm was measured with Multiskan Spectrum Microplate Photometers (Thermo Fisher Scientific, 81 Wyman Street, Waltham, MA, USA).
Cytokine in BALF
BALF levels of TNF-α, IL-1β, IL-18, and IL-6 were measured by ELISA according to the manufacturer’s instructions (R&D, Minneapolis, MN, USA). All measurements were performed in duplicate.
Lung Wet/Dry Weight Ratios
The right lungs were removed at the end of the experiment. The trachea and esophagus were separated from the lungs by blunt dissection, and the wet weight of the latter was determined. Subsequently, the lungs were incubated at 60 °C for 3 to 4 days to remove all moisture, and then the dry weight was measured and the ratio of wet-to-dry weight calculated.
Histological Assessment
In order to evaluate tissue inflammation, hematoxylin and eosin (HE) staining was performed on paraffin-embedded sections. The hematoxylin and eosin staining process was previously described [12]. Lung cell count based on a 5-point scoring system was performed as previously described to estimate the severity of leukocyte infiltration. The scoring system was as follows: 0, no cells; 1, a few cells; 2, a ring of cells one cell layer deep; 3, a ring of cells two to four cell layers deep; and 4, a ring of cells more than four cell layers deep.
Western Blotting of NLRP3 Inflammasome
The lung tissues were homogenized, washed with PBS, and incubated in lysis buffer in addition to a protease inhibitor cocktail (Sigma, St. Louis, MO) to obtain extracts of lung proteins. The samples were loaded to 10 % SDS-PAGE gels and were electrotransferred to nitrocellulose. The blots were incubated with the appropriate concentration of specific antibody. After washing, the blots were incubated with horseradish peroxidase-conjugated second antibody. The membranes were stripped and reblotted with anti-actin antibody (Sigma) to verify the equal loading of protein in each lane.
Statistical Analysism
The results were expressed as means ± SDs and analyzed by one-way ANOVA, with the Statistical Product and Service Solutions (SPSS 17.0, USA). P < 0.05 was taken as statistically significant.
RESULTS
Effects of Morin in BALF
To confirm the efficacy of LPS exposure, total leukocyte and neutrophil numbers in BALF were determined at the end of the intratracheal LPS protocol. Meanwhile, SOD activity was determined. Instillation of LPS into the lungs produced a significant recruitment of neutrophils into the alveolar space compared with the control group (Fig. 1). Total leukocyte number and neutrophil number in BALF raised rapidly by 2.64 times and 5.1 times, while SOD activity decreased by 2.26 times compared with the control group (P < 0.01), respectively. Morin (20 and 40 mg/kg) could dose-dependently reduce the total leukocyte cell number and neutrophil number (P < 0.01) (Fig. 1a) and increase SOD activity in BALF (Fig. 1b). After Dex treatment, total leukocyte cell number, neutrophil number, and total protein content in BALF were also obviously decreased (P < 0.01) and increase SOD activity in BALF.
a Total leukocyte number and neutrophil number in BALF. Values are expressed as means ± SDs. Compared with control # P < 0.05, ## P < 0.01; compared with model *P < 0.05, **P < 0.01. b SOD activity in BALF. Values are expressed as means ± SDs. Compared with control # P < 0.05, ## P < 0.01; compared with model *P < 0.05, **P < 0.01.
Effects of Morin on Cytokine in BALF and MPO Activity in Lung Homogenate
The levels of the cytokines TNF-α, IL-1β, IL-18, and IL-6 in BALF were dramatically increased by intratracheal LPS administration (Fig. 2). Morin (20 and 40 mg/kg) can downregulate the TNF-α, IL-1β, IL-18, and IL-6 levels in dose-dependent manners, respectively. Dex also downregulates the TNF-α, IL-1β, IL-18, and IL-6 levels in BALF. With lung neutrophil burden measured as MPO activity, which morin reduced MPO activity in dose-dependent manners, Dex also significantly inhibited the MPO activity (P < 0.01).
Effects of Morin on Lung Wet/Dry Weight Ratio
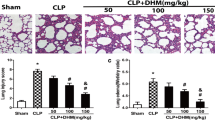
To independently evaluate LPS-induced changes in pulmonary vascular permeability to water, lung wet/dry weight ratios were used. LPS instilled for 6 h caused a significant increase in lung wet/dry weight ratio compared with control (P < 0.01). As shown in Fig. 3, both morin and Dex exhibited variability on lung wet/dry weight ratio when compared with the LPS group; those differences achieved statistical significance (P < 0.01).
Effects of Morin on Lung Histology
Histological evaluation of lungs (Figs. 4 and 5) by light microscopy demonstrated a large number of neutrophil sequestration and infiltration around the pulmonary vessel and airway, distributed in the alveolar and interstitial after intratracheal LPS. Treatment groups significantly reduced the degree of inflammatory cell infiltration (P < 0.05). The results indicate that morin can reduce the degree of pathological inflammation in lung tissues in acute lung injury (P < 0.05).
Pathological changes of lung tissues observed by HE staining. (Light microscopy, ×200) a control, b model, c dexamethasone (2 mg/kg), d morin (20 mg/kg), and e morin (40 mg/kg). Values are expressed as means ± SDs. Compared with control # P < 0.05, ## P < 0.01; compared with model *P < 0.05, **P < 0.01.
Effect of Morin on LPS-Induced NLRP3 Inflammasome Protein Expression in Mice
The expression of inflammation-related protein NLRP3 inflammasome was changed by LPS in lung. As shown in Fig. 6, compared with the control group, the protein level of NLRP3 inflammasome in the model group was significantly increased (P < 0.05). In morin (20 and 40 mg/kg), the protein level of NLRP3 inflammasome was significantly decreased in a dose-dependent manner compared to the model group, respectively (P < 0.05).
DISCUSSION
One of the most important components of the initial innate immune response in the lung against bacterial infection is the vigorous recruitment of neutrophils. In ALI, neutrophils are the earliest immune cells to be recruited to the site of injury and express multiple cytotoxic products [13]. In endotoxemia-induced ALI, the neutrophils accumulated in the lungs express proinflammatory cytokines, such as IL-1β and TNF-α, and finally lead to the pulmonary injury [14]. In this study, we found that the neutrophils increased evidently in lung tissues after LPS exposure. As expected, morin pretreatment significantly decreased the neutrophils in lung tissues. MPO is a major constituent of neutrophil cytoplasmic granules. The total activity of MPO in a tissue is therefore a direct measure of neutrophil sequestration in that tissue [15]. In this study, we found that the MPO activity increased evidently in lung tissues after LPS exposure. As expected, morin pretreatment significantly decreased the MPO activity in lung tissues. In addition, histopathological study also indicated that morin pretreatment markedly attenuated the neutrophil infiltration in lungs.
LPS is known to induce the production of several inflammatory and chemotactic cytokines. TNF-α, IL-1β, and IL-6 are characterized cytokines involved in the inflammatory process of acute lung injury [16-18]. These cytokines, as well as other proinflammatory compounds, initiate, amplify, and perpetuate the inflammatory response in acute lung injury. TNF-α is the earliest and primary endogenous mediator of the process of an inflammatory reaction. TNF-α, mainly produced by monocytes/macrophages, can elicit the inflammatory cascade, cause damage to the vascular endothelial cells, and induce alveolar epithelial cells to produce other cellular factors, such as IL-6 [19]. In this study, we found that the TNF-α, IL-1β, IL-18, and IL-6 increased evidently in BALF after LPS exposure. As expected, morin pretreatment significantly decreased the TNF-α, IL-1β, IL-18, and IL-6 in BALF. Lung wet/dry weight (W/D) ratio was evaluated as an index of pulmonary edema, which is a typical symptom of inflammation not only in systemic inflammation but also in local inflammation [20]. In the present study, it was found that morin could decrease the LPS-induced lung W/D ratio. These results suggested that morin has a protective effect on LPS-induced ALI.
The NLRP3 inflammasome is currently the most fully characterized inflammasome, which responds to numerous physically and chemically diverse stimuli, and leads to a series of diseases when out of control. The NLRP3 inflammasome is the most intensively studied of the inflammasomes, and it can be activated by a variety of microbial-, stress-, or danger-induced substances. The products of NLRP3 inflammasome activation, IL-1β and IL-18, have been shown to be protective in a variety of infections. In the present study, it was found that morin could decrease the protein level of NLRP3 inflammasome; the result suggested that morin has a protective effect on LPS-induced ALI through regulating NLRP3 inflammasome.
In this paper, we have established that morin may exert some of its anti-inflammatory and pharmacological effects by affecting the activity of NLRP3 inflammasome in LPS-induced acute lung injury in mice. Although NLRP3 inflammasome activation is critical for driving acute lung inflammation aiding in the clearance of viral or bacterial infections, and morin can inhibit NLRP3 inflammasome, the underlying immunological mechanisms are not clear; thus, the mechanisms need to be clarified in the future.
In previous study, the anti-inflammatory effect of morin had been found. In this study, we investigated anti-inflammatory effects of morin on acute lung injury using lipopolysaccharide (LPS)-induced acute lung injury (ALI) mouse model. The cell counting in the bronchoalveolar lavage fluid (BALF) was measured. The animal lung edema degree was evaluated by W/D ratio. The superoxidase dismutase (SOD) activity and myeloperoxidase (MPO) activity were assayed by SOD and MPO kits, respectively. The levels of inflammatory mediators including tumor necrosis factor-α (TNF-α), IL-1β, IL-18, and IL-6 were assayed by enzyme-linked immunosorbent assay method. Pathological changes of lung tissues were observed by HE staining. The protein level of lung NLRP3 inflammasome was measured by Western blotting. The data showed that treatment with the morin markedly attenuated inflammatory cell numbers in the BALF, decreased lung NLRP3 inflammasome protein level, and improved SOD activity and inhibited MPO activity. Histological studies demonstrated that morin substantially inhibited LPS-induced neutrophils in lung tissue compared with model group. The results indicated that the morin had a protective effect on LPS-induced ALI in mice.
References
Rubenfeld, G.D. 2003. Epidemiology of acute lung injury. Critical Care Medicine 31: S276–S284.
Zhang, X.M., K.J. Song, H.Z. Xiong, H.Y. Li, X. Chu, and X.M. Deng. 2009. Protective effect of florfenicol on acute lung injury induced by lipopolysaccharide in mice. International Immunopharmacology 9: 1525–1529.
Matthay, M.A., G.A. Zimmerman, C. Esmon, J. Bhattacharya, B. Coller, C.M. Doerschuk, et al. 2003. Future research directions in acute lung injury summary of a National Heart Lung and Blood Institute Working Group. American Journal of Respiratory and Critical Care Medicine 167: 1027–1035.
Chen, Z., X. Zhang, X. Chu, X. Zhang, K. Song, Y. Jiang, L. Yu, and X. Deng. 2010. Preventive effects of valnemulin on lipopolysaccharide-induced acute lung injury in mice. Inflammation 33: 306–314.
Itoh, T., H. Obata, S. Murakami, K. Hamada, K. Kangawa, H. Kimura, and N. Nagaya. 2007. Adrenomedullin ameliorates lipopolysaccharide-induced acute lung injury in rats. American Journal of Physiology 293: L446–L452.
Riedemann, M.E., H.S. Murphy Murphy, and P.A. Ward. 2003. Regulatory effects of iNOS on acute lung inflammatory responses in mice. American Journal of Pathology 163: 2319–2328.
Strowig, T., J. Henao-Mejia, E. Elinav, and R. Flavell. 2012. Inflammasomes in health and disease. Nature 481: 278–286.
Dinarello, C.A., and G. Fantuzzi. 2003. Interleukin-18 and host defense against infection. Journal of Infectious Diseases 187(Suppl 2): S370–S384.
Dinarello, C.A. 2009. Immunological and inflammatory functions of the interleukin-1 family. Annual Review of Immunology 27: 519–550.
Wang, L., Y.C. Tu, T.W. Lian, J.T. Hung, J.H. Yen, and M.J. Wu. 2006. Distinctive antioxidant and antiinflammatory effects of flavonols. Journal of Agricultural and Food Chemistry 54: 9798–9804.
Kumazawa, Y., K. Kawaguchi, and H. Takimoto. 2006. Immunomodulating effects of flavonoids on acute and chronic inflammatory responses caused by tumor necrosis factor alpha. Current Pharmaceutical Design 12: 4271–4279.
Yunhe, Fu., Liu Bo, Feng Xiaosheng, et al. 2012. The effect of magnolol on the toll-like receptor 4/nuclear factor kappa B signaling pathway in lipopolysaccharide-induced acute lung injury in mice. European Journal of Pharmacology 689: 255–261.
Nanashima, N., M. Akita, T. Yamada, T. Shimizu, H. Nakano, Y. Fan, et al. 2008. The hairless phenotype of the Hirosaki hairless rat is due to the deletion of an 80-kb genomic DNA containing five basic keratin genes. Journal of Biological Chemistry 283: 16868–16875.
Parsey, M.V., R. Tuder, and E. Abraham. 1998. Neutrophils are major contributors to intraparenchymal lung IL-1β expression after hemorrhage and endotoxemia. Journal of Immunology 160: 1007–1101.
Shenkar, R., and E. Abraham. 1999. Mechanisms of lung neutrophil activation after hemorrhage or endotoxemia: roles of reactive oxygen intermediates, NF-κB, and cyclic AMP response element binding protein. Journal of Immunology 163: 954–962.
Bradley, P.P., D.A. Priebat, R.D. Christensen, and G. Rothstein. 1982. Measurement of cutaneous inflammation: estimation of neutrophil content with an enzyme marker. The Journal of Investigative Dermatology 78: 206–209.
Bhatia, M., and S. Moochhala. 2004. Role of inflammatory mediators in the pathophysiology of acute respiratory distress syndrome. Journal of Pathology 202: 145–156.
Cribbs, S.K., M.A. Matthay, and G.S. Martin. 2010. Stem cells in sepsis and acute lung injury. Critical Care Medicine 38: 2379–2385.
Goodman, R.B., J. Pugin, J.S. Lee, and M.A. Matthay. 2003. Cytokine-mediated inflammation in acute lung injury. Cytokine and Growth Factor Reviews 14: 523–535.
Giebelen, I.A., D.J. van Westerloo, G.J. LaRosa, A.F. de Vos, and T. van der Poll. 2007. Local stimulation of alpha7 cholinergic receptors inhibits LPS-induced TNF-alpha release in the mouse lung. Shock 28: 700–703.
Acknowledgments
This work was supported by a project funded by the Priority Academic Program Development of Jiangsu Higher Education Institutions.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tianzhu, Z., Shihai, Y. & Juan, D. The Effects of Morin on Lipopolysaccharide-Induced Acute Lung Injury by Suppressing the Lung NLRP3 Inflammasome. Inflammation 37, 1976–1983 (2014). https://doi.org/10.1007/s10753-014-9930-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-014-9930-1