Abstract
To investigate whether oligomerization domains (NODs) are involved in Porphyromonas gingivalis-induced interleukin (IL)-6, IL-8, and vascular cell adhesion molecule (VCAM)-1 expression beyond Toll-like receptors (TLRs), we investigated the role of NOD1/2 in P. gingivalis-induced IL-6, IL-8, and VCAM-1 expression in human gingival fibroblasts (hGFs) and periodontal ligament cells (hPDLCs). The mechanism was explored by activation and silence of NODs, electrophoretic mobility shift assay (EMSA), and pathway blockade assays. Results showed that P. gingivalis could induce NOD1, NOD2, IL-6, IL-8, and VCAM-1 expression in hGFs and hPDLs at mRNA and protein levels. Activation of NOD1/2 by agonists could clearly upregulate the expression of these genes, while silence of NOD1/2 could remarkably attenuate them. EMSA and blockade of NF-κB and extracellular-signal-regulated kinase (ERK)1/2 pathway assays also verified that the two pathways were involved in NOD1/2-mediated IL-6, IL-8, and VCAM-1 expression. In conclusion, our findings demonstrated that P. gingivalis induced IL-6, IL-8, and VCAM-1 expression in hGFs and hPDLCs through NOD1/2-mediated NF-κB and ERK1/2 signaling pathways beyond TLRs.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Periodontitis is a chronic inflammatory disorder involving the inflammation of the periodontium and results in the destruction of soft and hard tissues. Porphyromonas gingivalis (P. gingivalis) has long been known to be one of the major pathogens involved in this inflammatory disease [1, 2]. It has the property of invading into the periodontal connective tissue [3] and acting with periodontal residential cells such as human gingival fibroblasts (hGFs) and human periodontal ligament cells (hPDLCs). The ability of these periodontal residential cells to recognize such pathogens renders them crucial in dealing with microbial invasion. These cells can release several inflammatory cytokines including interleukins, chemokines, and adhesion molecules, so as to play active roles in the host defense [4, 5].
Interleukin (IL)-6 and IL-8 are important inflammatory cytokines in the initiation of periodontitis. Increased presence of IL-6 and IL-8 secreted by fibroblasts has been detected in periodontitis lesions [6]. In addition, adhesion molecules are also involved in this process. Vascular cell adhesion molecule (VCAM)-1 (CD106), belonging to the transmembrane immunoglobulin superfamily of adhesion molecules [7], can bind to its ligand lymphocyte function-associated antigen-4 and mediate the influx of leukocytes into the local inflammatory tissue [8, 9]. Thus, it is reported to take part in the pathogenesis of several inflammatory diseases, such as rheumatoid arthritis [10] and coronary atherosclerosis [11, 12]. Some studies showed that soluble VCAM-1 in gingival crevicular fluid of subjects with periodontitis was increased [13], but other studies found the opposite result [14]. Therefore, the regulation of this adhesion molecule in infectious condition needs more investigation.
Previous studies have showed that Toll-like receptor (TLR) signal was one of the pathways to mediate IL-6, IL-8, and VCAM-1 expression by P. gingivalis [15–17]. TLRs are the first discovered subfamily of pattern recognition receptors (PRRs), which mainly locate on the membrane and recognize several pathogen-associated molecule patterns including lipopolysaccharides. Recently, another kind of PRRs, namely nucleotide-binding oligomerization domain (NOD)-containing protein-like receptors (NLRs), has been discovered to play pivotal roles in the immune response against pathogens. Unlike TLRs, NLRs are a group of receptors that is located in the cytoplasm. NOD1 and NOD2 are representative NLRs. They consist of an N-terminal caspase recruitment domain, an intermediate NOD, and a C-terminal leucine-rich repeat domain [18] and recognize peptidoglycan from the cell wall of bacteria. NOD1 and NOD2 can be detected in various human periodontal cells, including gingival epithelial cells [19], gingival fibroblasts [20], periodontal ligament cells [21], and cementoblasts [22]. It is demonstrated that activation of NOD1 and (or) NOD2 in hGFs and/or hPDLCs in vitro could mediate the release of IL-6 and IL-8 through inflammatory pathways including the nuclear factor kappaB (NF-κB) and mitogen-activated protein kinases (MAPKs) signaling pathway [20, 21, 23]. However, up to now, little is known whether NODs regulate VCAM-1 expression in these cells. We previously discovered that NOD1/2 mediated another adhesion molecule ICAM-1 expression in periodontal fibroblasts [24]. Given that these two adhesion molecules belong to the same family, and the similar regulations of which they are through, we hypothesized that NOD1/2 could play a role in VCAM-1 production in hGFs and hPDLCs.
In this present study, the functions of NOD1 and NOD2 in hGFs and hPDLCs were assessed. The relationship of NOD1/2 and VCAM-1 by P. gingivalis stimulation was mainly investigated by activation and silence of NODs, electrophoretic mobility shift assay (EMSA), and pathway blockade assays, while NOD1/2-mediated IL-6 and IL-8 expression were taken as positive control.
MATERIAL AND METHODS
Cell culture and reagents
hPDLCs and hGFs were obtained from four healthy individuals (two male and two female, age range from 20 to 30 years old) who underwent the third molar extraction at the Department of Oral and Maxillofacial Surgery in Peking University School and Hospital of Stomatology, which was also approved by the Medical Ethical Committee of this hospital (ethics approval no. PKUSSIRB-2012017), and written informed consents were obtained from all the donors before tooth extraction. All the donors at the time of enrollment were systemically and periodontally healthy. The individuals were nonsmoker and had no antimicrobial or any other medicine treatment in the previous 6 months. The third molars were fully erupted and had no tooth defect. Extracted teeth and gingival tissues surrounding the extraction socket were rinsed three times with D-hanks solution. The PDL tissue from the mid-one-third of root surfaces and gingival tissue were cut into small fragments (1 mm3) in Dulbecco's Modified Eagle's Medium (DMEM, Gibco, Paisley, Scotland, UK) containing 10 % fetal bovine serum (FBS; HyClone, Logan, UT) and were cultured in 35-mm dishes. All cultures were maintained at 37 °C with a humidified gas mixture of 5 % CO2/95 % air. The cells from each donor were cultured and utilized individually and identified by immunohistochemistry for the expression of vimentin (mesenchymal marker) and cytokeratin (CK)-14 (epithelial markers) (Supplementary Fig. 1) and were used in all experiments at four to eight passages. The agonists, d-glutamyl-meso-diaminopimelic acid (Tri-DAP, NOD1 ligand) and muramyldipeptide (MDP, NOD2 ligand) were purchased from InvivoGen (San Diego, CA, USA). NF-κB signal inhibitor pyrrolidine dithiocarbamate (PDTC) and ERK1/2 MAPK signal inhibitor U0126 were purchased from Sigma-Aldrich (St. Louis, MO, USA).
Bacterial strain and culture conditions
P. gingivalis W83 was kindly provided by Prof. Chenxiong Lai of the Kaohsiung Medical University in Taiwan. Bacteria were grown in brain heart infusion (BHI, Bacto, Sparks, MD, USA) broth agar plates (supplemented with 5 % fetal bovine serum, 5 μg/ml hemin and 0.4 μg/ml menadione) in an anaerobic system (5 % CO2, 10 % H2, and 85 % N2) at 37 °C for 5 to 7 days. The cultures were then inoculated into fresh BHI broth (supplemented with 5 μg/ml hemin and 0.4 μg/ml menadione) and grown for 24 h or until the optical density at 600 nm reached 1.0.
Bacteria challenge
P. gingivalis W83 was grown to an optical density of 1.0, pelleted by centrifugation, washed three times with PBS (pH 7.2), and resuspended in DMEM with 10 % FBS at a final concentration of 108 cells/ml [25]. Bacterial suspensions were added to confluent fibroblast monolayers at an indicated multiplicity of infection (MOI) for the indicated times at 37 °C in 5 % CO2. Control cultures were incubated with medium alone. The cells were then harvested and used in subsequent experiments. The viabilities of the fibroblasts were assessed by a 0.2 % trypan blue exclusion test, and were >90 %. All assays were performed in triplicate.
RNA interference
NOD1, NOD2 small-interfering (si) RNA, and control siRNA were obtained from Invitrogen Biotechnology (Invitrogen, San Diego, CA, USA). Transfection of siRNA was performed using Lipofectamine 2000 (Invitrogen, Carlsbad, CA, USA), according to the manufacturer's instructions. A 100-pM siRNA was transfected into hPDLCs and hGFs for 48 h. The relative expression levels of VCAM-1 and NOD1/2 were then determined by real-time PCR and western blot. The efficiency of the transfection and viability were also detected using BLOCK-iT™ Fluorescent Oligo and trypan blue exclusion tests, respectively.
RNA extraction and cDNA synthesis
Total RNA was extracted from cells by using the TRIzol reagent (Invitrogen, Carlsbad, CA, USA), according to the manufacturer's instructions. The RNA concentration was measured spectrophotometrically. Total RNA (2 μg) was then reverse-transcribed into single-stranded cDNA by using M-MLV reverse transcriptase (Promega, Madison, WI, USA) and oligo(dT)15 primers, according to the manufacturer's protocol.
Quantitative real-time polymerase chain reaction
Quantitative real-time polymerase chain reaction (qPCR) was performed in an ABI Prism 7000 Sequence Detection System (Applied Biosystems, LifeTechnologies, Warrington, UK) using SYBR Green Reagent (Roche, Indianapolis, IN, USA). β-actin was used as the endogenous control gene. The primers for each gene were listed in Table 1. The standard PCR conditions were 10 min at 95 °C, followed by 40 cycles of 95 °C for 15 s, and 60 °C for 1 min. All reactions were performed in triplicate. The expression levels of the target transcripts in each sample were calculated by the comparative 2−ΔΔCt method after normalization to the expression of β-actin.
Western blot
The cells were harvested and lysed in RIPA buffer (Applygen, Beijing, China) containing proteinase inhibitors and phosphatase inhibitors. After measuring the protein concentration by the BCA Kit (Thermo, Rockford, IL, USA), equal amounts of protein samples were separated by 10 % sodium dodecyl sulfate–polyacrylamide gel electrophoresis and transferred to polyvinylidene difluoride membranes by wet blotting. The membranes were blocked in 5 % nonfat dry milk for 1 h and probed with antibodies against NOD1 (Cell Signaling Technology, Danvers, MA, USA); NOD2 (Abgent, San Diego, CA, USA); VCAM-1 (Santa Cruz, CA, USA); phospho-P65 and total P65; phospho-p38 MAPK and total p38 MAPK; phospho-JNK and total JNK; phospho-ERK1/2 and total ERK1/2; and β-actin (ZSGB-BIO, Beijing, China) separately at 4 °C overnight. All anti-P65 and anti-MAPK antibodies were purchased from Cell Signaling Technology (Danvers, MA, USA). After incubation with peroxidase-linked secondary antibodies, the ECL Reagent (Thermo, Rockford, IL, USA) was used to visualize the immunoreactive proteins.
Electrophoretic mobility shift assay
Nuclear extraction and EMSA were performed as described by Zhou et al.[26]. Periodontal fibroblasts were incubated for 24 h with either 10 μg/ml Tri-DAP or 10 μg/ml MDP. After washing three times with ice-cold PBS, nuclear extracts from periodontal fibroblasts were prepared using the Nuclear–Cytosol Extraction Kit (Applygen Technology, Shanghai, China), according to the manufacturer's instruction. Aliquots of the extract were immediately frozen at −80 °C.
Nuclear extracts (5 μg each) were prepared and subjected to EMSA by using a chemiluminescence-labeled NF-κB oligonucleotide probe (5′-AGTTGAGGGGACTTTCCC AGGC-3′). A binding reaction was performed using the LightShift Chemiluminescent EMSA Kit (Pierce, Rockford, IL, USA). The DNA–protein complex samples were analyzed on a 6 % polyacrylamide gel.
Statistical analysis
Data were expressed as the means ± SD. Cells from four different donors were used for statistical analysis by multivariate ANOVA of SPSS. The level of significance (P) was set as <0.05.
RESULTS
P. gingivalis increased TLR2, NOD1/2, IL-6, IL-8 as well as VCAM-1 expression in hGFs and hPDLCs
P. gingivalis W83, as one of the major periodontal pathogens, was used in vitro to simulate the infectious conditions on periodontal fibroblasts. As expected, this microbe increased TLR2, NOD1, and NOD2 expressions in hPDLCs and hGFs in a concentration-dependent manner (Fig. 1a) as well as in a time-dependent manner (Fig. 1b). However, it did not affect TLR4 expression (Supplementary Fig. 2). The expression of IL-6, IL-8, and VCAM-1 was also upregulated after P. gingivalis stimulation at mRNA (P < 0.05) and (or) protein levels. When P. gingivalis infection was applied at MOI of 1:100 for 8 h, the mRNA level of IL-6 was 15.2 ± 2.5 fold in hPDLCs (P < 0.001) and 23 ± 2.4 fold in hGFs (P < 0.001) compared to their untreated controls. For IL-8, the increased fold was up to 43.1 ± 4.6 fold in hPDLCs (P < 0.001) and 58.6 ± 6.8 fold in hGFs (P < 0.001); VCAM-1 mRNA was upregulated to 3.2 ± 2.0 fold in hPDLCs and 6.6 ± 1.8 fold in hGFs (P < 0.001).
P. gingivalis W83 increased TLR2, NOD1, NOD2, IL-6 and IL-8, and VCAM-1 expression levels in hPDLCs and hGFs. hPDLCs and hGFs were treated with P. gingivalis W83 at the indicated concentrations for 4 h. Real-time PCR and western blot were used to detect TLR2, NOD1, NOD2, IL-6, IL-8, and VCAM-1 expression. The expression levels of these molecules were all upregulated by P. gingivalis W83 at both mRNA level and (or) protein levels (a). hPDLCs and hGFs were treated with P. gingivalis W83 at multiplicity of infection of 1:100 for indicated times. TLR2, NOD1, NOD2, IL-6, IL-8, and VCAM-1 were also increased by P. gingivalis infection in a time-dependent manner (b). *P < 0.05; **P < 0.01; ***P < 0.001 as compared with their corresponding untreated controls.
Activation of NOD1 or NOD2 upregulated IL-6, IL-8, and VCAM-1 expression in hPDLCs and hGFs
Since it was known that TLR2 could mediate IL-6, IL-8, and VCAM-1 expressions in periodontal fibroblasts, we focused on the role of NOD1/2 in regulating these cytokines in hGFs and hPDLCs. The results showed that Tri-DAP (an agonist for NOD1) successfully activated NOD1 expression at mRNA as well as protein level (Fig. 2a). Activation of NOD1 significantly increased IL-6, IL-8, and VCAM-1 expression in these two fibroblasts in a dose-dependent manner (Fig. 2a). Specially, Tri-DAP at 10 μg/ml increased IL-6 mRNA level by 3.3 ± 0.8 fold in hPDLCs (P < 0.01) and by 6.4 ± 1.5 fold in hGFs (P < 0.001); increased IL-8 mRNA level by 5.7 ± 1.3 fold in hPDLCs (P < 0.001) and 9.2 ± 1.2 fold in hGFs (P < 0.001); and increased VCAM-1 mRNA level by 2.56 ± 0.86 fold in hPDLCs (P < 0.01) and by 1.89 ± 0.65 fold in hGFs (P < 0.01).
Tri-DAP and MDP upregulated IL-6, IL-8, and VCAM-1 expression in a dose-dependent manner. A 10-μg/ml Tri-DAP (NOD1 ligand) or 10 μg/ml MDP (NOD2 ligand) was applied to hPDLCs and hGFs at the indicated doses for 24 h. The specific agonist activated their targets (NOD1 or NOD2) in a dose-dependent manner in hGFs and hPDLCs at mRNA level (a, b). Either Tri-DAP (a) or MDP (b) increased the expression of IL-6, IL-8, and VCAM-1. Western blot showed and confirmed these results in both hPDLCs and hGFs. *P < 0.05; **P < 0.01; ***P < 0.001 as compared with their corresponding untreated controls.
In addition, MDP (the agonist for NOD2) could activate NOD2 in both of periodontal fibroblasts (Fig. 2b). It also remarkably upregulated IL-6, IL-8, and VCAM-1 expression at mRNA level (P < 0.05). The results were further confirmed by western blot (Fig. 2b).
Silencing of NOD1 or NOD2 decreased P. gingivalis-induced IL-6, IL-8, and VCAM-1 expression in hPDLCs and hGFs
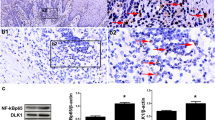
To determine whether NOD1 or NOD2 mediated VCAM-1 expression, RNA interference (RNAi) targeting of NOD1/2 mRNA was performed on hPDLCs and hGFs, respectively. Real-time PCR and western blot clearly showed that siNOD1 or siNOD2, respectively, downregulated NOD1or NOD2 expression in the two periodontal fibroblasts stimulated by P. gingivalis at mRNA level (P < 0.05, Fig. 3a, b) and protein level (Fig. 3f). Downregulation of NOD1 or NOD2 suppressed P. gingivalis-induced mRNA production of IL-6 to 30–50 % (P < 0.01, Fig. 3c) and IL-8 to 25–45 % (P < 0.01, Fig. 3d) in both of fibroblasts. Furthermore, either si-NOD1 or si-NOD2 could successfully attenuate P. gingivalis-induced VCAM-1 mRNA to approximately 70 % in hPDLCs (P < 0.01) and to 60 % in hGFs (P < 0.01, Fig. 3e). The results were confirmed at protein level by western blot (Fig. 3f).
Silencing of NOD1 and NOD2 attenuated IL-6, IL-8, and VCAM-1 expression induced by P. gingivalis W83. Small interfering RNAs (siRNAs) targeting NOD1 and NOD2 were used in both types of fibroblasts followed by 10 μg/ml of Tri-DAP or 10 μg/ml of MDP treatment. The relative quantities of NOD1 and NOD2 mRNA decreased by their specific siRNA (a, b). IL-6 (c), IL-8 (d), and VCAM-1 expression (e) were also suppressed by siNOD1 or siNOD2 compared with the group transfected with scrambled siRNA in hGFs and hPDLCs. The protein levels were consistent with mRNA changes (f). *P < 0.05; **P < 0.01; ***P < 0.001 as compared with their corresponding scrambled siRNA controls.
Effects of Tri-DAP and MDP on NF-κB and ERK1/2 activities in hPDLCs and hGFs
The signaling pathways involved in the effect of NOD1/2 activation were then assessed. We investigated NF-κB activity by using Tri-DAP or MDP treatment in both fibroblasts. As shown in EMSA assays, compared with the nontreated group, the NF-κB DNA-binding activity remarkably increased in both hPDLCs and hGFs when treated with 10 μg/ml Tri-DAP or MDP (Fig. 4a). Furthermore, the immunoblotting results of phosphorylated (p)-P65 confirmed these results. p-P65 expression was higher in hPDLCs and hGFs treated by either Tri-DAP or MDP, while the total P65 level was the same among all the samples (Fig. 4b).
Tri-DAP and MDP activated NF-κB and ERK1/2 MAPK signals in hPDLCs and hGFs. Cells were incubated with 10 μg/ml of Tri-DAP or 10 μg/ml of MDP for 24 h, and NF-κB signal and MAPK signals were examined in hPDLCs and hGFs. By verifying the banding specificity with cold competition in EMSA assay, the results showed that the DNA-binding protein activities of p-P65 were remarkably higher in the two fibroblasts triggered by Tri-DAP or MDP than that in the untreated cells (a). Western blot showed that phosphorylated-P65 was increased in the groups treated with Tri-DAP or MDP, while the total P65 level was the same in the treated and untreated groups (b). Western blot showed that ERK1/2 signals were activated by NOD1 and NOD2 agonists, while P38 MAPK and JNK MAPK did not take part in this process in hPDLCs and hGFs (c).
Meanwhile, we examined the activated forms of P38, ERK1/2, and JNK MAPK. p-ERK1/2 expression was remarkably upregulated after stimulation either by Tri-DAP or MDP, while total ERK1/2 was not significantly different between the treated and untreated groups (Fig. 4c). However, p-P38 and p-JNK did not show any significant changes compared with their corresponding total P38, and total JNK (Fig. 4c). The results indicated that the agonists of NOD1/2 could activate the NF-κB and ERK1/2 signaling cascade in hPDLCs and hGFs, but not including JNK and P38 MAPK.
NF-κB- and ERK1/2-mediated IL-6, IL-8, and VCAM-1 expression by Tri-DAP and MDP in hPDLCs and hGFs
The ligands of NOD1/2 could activate NF-κB and ERK1/2 signals in hGFs and hPDLCs; therefore, the effects of these two signaling pathways on IL-6, IL-8, and VCAM-1 expression were determined. The cells were treated with 5 μg/ml PDTC (an inhibitor of NF-κB) or 10 μM U0126 (an inhibitor of ERK1/2) for 30 min before incubation of 10 μg/ml Tri-DAP or 10 μg/ml MDP for 24 h. The results showed that p-P65 was significantly decreased in inhibitor-treated hGFs and hPDLs (Fig. 5c, d). Meanwhile, IL-6, IL-8, and VCAM-1 were reduced to about 20 ~ 40 % in hPDLCs and to25 ~ 50 % in hGFs compared with those treated by Tri-DAP alone (Fig. 5a, c, d). Similarly, blockade of NF-κB signal by PDTC successfully and significantly decreased MDP-induced IL-6, IL-8, and VCAM-1 products in hPDLCs and hGFs (Fig. 5b–d). In addition, pretreatment of U0126 also successfully attenuated the agonist-induced IL-6, IL-8, and VCAM-1 expression (Fig. 5 a–d). These results suggested that NOD1/2-mediated IL-6, IL-8, and VCAM-1 expression depended on NF-κB and ERK1/2 signals in periodontal fibroblasts.
Blocking of either the NF-κB or ERK1/2 signal pathway attenuated NOD1/2-mediated IL-6, IL-8, and VCAM-1 productions. The fibroblasts were treated with PDTC (an inhibitor of NF-κB signaling) and U0126 (an inhibitor of ERK1/2 signaling) for 30 min, respectively, followed by Tri-DAP or MDP treatment at 10 μg/ml for 24 h in hPDLCs and hGFs. The expression of IL-6, IL-8, and VCAM-1 were examined. Real-time PCR showed that Tri-DAP-induced expression of IL-6, IL-8, and VCAM-1 were all partly attenuated after blockade of either NF-κB or ERK1/2 signaling in the two fibroblasts compared with unblocked controls (a). Similarly, MDP-induced expression of these three cytokines were partly decreased when blocking the either of two signaling pathways (b). Western blotting results confirmed real-time PCR, showing that compared with Tri-DAP or MDP treatment alone, VCAM-1 expression was attenuated when NF-κB and ERK1/2 signals were blocked by their own inhibitors in hPDLCs and hGFs (c, d). *P < 0.05; **P < 0.01; ***P < 0.001 as compared with their corresponding controls (Tri-DAP or MDP-alone-treated fibroblasts).
DISCUSSION
In this study, we utilized P. gingivalis strain W83 to challenge hGFs and hPDLCs in vitro, showing that this strain successfully activates NOD1/2 in periodontal fibroblasts. Although the activity of P. gingivalis to induce inflammation is weakest among the periodontal pathogens [27], even weaker than the commensal bacteria Escherichia coli [27, 28], this bacterium is recognized as the predominant causal agent involved in chronic periodontitis, which belongs to the “red” complex of pathogens. Considering the similar cell wall construction of the gram-negative microbe, it is reasonable to speculate that other periodontal pathogens, such as Aggregatibacter actinomycetemcomitans and Fusobacterium nucleatum, also have the ability to trigger NOD1/2 expression in periodontal fibroblasts and induce the inflammatory response. Owing to the capability of P. gingivalis to penetrate into connective tissue through degrading the barrier junctions of gingival epithelium [3, 29], we chose this microbe as the representative stimuli to challenge periodontal fibroblasts in this in vitro study. Our results demonstrated that P. gingivalis could increase IL-6 and IL-8 expression in hGFs and hPDLCs though NOD1/2 signaling pathways, which was in line with previous studies [20, 21]. IL-6 and IL-8 are pivotal cytokines and mediators to modulate the inflammatory cascade in chronic periodontitis [30]. The high level of IL-8 could also induce the chemotaxis in its target cells, thus leading to periodontal inflammation and tissue destruction [31]. Furthermore, these pro-inflammatory cytokines were shown to play a role in stimulating osteoclast activity [32]. The evidence of NOD1/2-mediated IL-6 and IL-8 expression in hPDLCs and hGFs not only further demonstrates the selective pathological roles of NOD1/2 in periodontitis but also confirms the immune behavior of periodontal fibroblasts.
In addition, to confirm the relationship between NOD1/2 and IL-6, and IL-8, which is more important, our data further expanded the roles of NOD1/2, showing that activation of NOD1/2 could also upregulate VCAM-1 expression in hGFs and hPDLCs. So far, to the best of our knowledge, this is the first evidence linking NOD1/2 with VCAM-1 in periodontal fibroblasts. For a long time, VCAM-1 is thought to be mainly expressed in endothelial cells of blood vessels and can be a biomarker for activation of the endothelium. Recently, it is also reported that VCAM-1 can be detected in hPDLCs and hGFs [33–35], and its regulation in such cells by inflammation is very complicated [34]. Tumor necrosis factor-α and interferon-γ are shown to enhance VCAM-1 expression, while TGF-β1 inhibits its expression. Therefore, the regulation of VCAM-1 in inflammation seems to depend on the types and levels of stimuli. Our data indicated that P. gingivalis was an activating factor in regulating VCAM-1 expression, which was supported by other studies [36, 37]. The high level of VCAM-1 in periodontal fibroblasts can promote lymphocyte infiltration and binding to periodontal fibroblasts, and this binding can trigger fibroblasts to secrete inflammatory cytokines, such IL-1α and IL-13 [38]. In addition to attract the immune cells, recent studies have discovered another role of VCAM-1, showing that it could recruit monocytic osteoclast progenitors and elevate local osteoclast activity [39]. Periodontitis is a complex inflammatory disease involving destruction of soft tissue and loss of hard tissue, and osteoclasts play a critical role in the absorption of alveolar bone. The NOD1/2-regulated VCAM-1 expression makes it sensible to speculate that NOD1/2 may not only play the functional immune receptors role in periodontal fibroblasts, but also take part in the bone remodeling. Further studies are needed to support this hypothesis.
Both of NODs and TLRs are innate immune receptors responding to microbe challenges. It is discovered that, rather than function respectively, interaction with each other would be more likely to be the ways of the two receptors regulating the immune response [20, 40]. In this study, TLR2, NOD1, and NOD2 were all activated by P. gingvalis stimulation, indicating that both of TLRs and NODs were the functional receptors in hGFs and hPDLCs. They may synergistically induce IL-6, IL-8, and VCAM-1 expression. That may be a possible reason that knockdown of NOD1/2 only attenuated P. gingvalis-induced VCAM-1 expression by 30–40 % in this study.
NF-κB is an ubiquitous effector in transduction pathways of the inflammatory response. NOD1 and NOD2 act as sensors to trigger activation of the NF-κB signaling pathway [41]. The production of pro-inflammatory cytokines, such as IL-6, IL-8, and monocyte chemoattractant protein-1, induced by NOD1 and NOD2 ligands, is significantly inhibited by an RNA interference assay targeted to p65 in gingival fibroblasts [20]. The present study confirmed the role of NF-κB in the immune response, showing that the activation of the NF-κB pathway is also responsible for NOD1/2-mediated VCAM-1 expression. In parallel to the activation of NF-κB, we also found that ERK1/2 MAPK signaling pathway was also involved in NOD-triggered production of these pro-inflammatory cytokines. ERK1/2 belongs to the MAPK signaling pathways and is first identified to be responsible for cell proliferation and activation [42]. Actually, this pathway is also involved in regulating inflammatory molecules such as ICAM-1, IL-6, IL-8, and MMP9 in response to different stimuli such as IL-17 and IL-20 [43–45]. The downregulation of IL-6, IL-8, and VCAM-1 by PDTC and U0126 in P. gingivalis-challenged periodontal fibroblasts confirmed the pro-inflammatory properties of NF-κB and ERK1/2 MAPK.
CONCLUSIONS
In conclusion, this study suggests that NOD1 and NOD2 are the functional receptors to modulate inflammation in the periodontal fibroblasts. Our findings demonstrate P. gingivalis-induced IL-6, IL-8, and VCAM-1 expression in hGFs and hPDLCs through NOD1/2-mediated NF-κB and ERK1/2 signaling pathways beyond TLRs, indicating that NOD1/2 can be a new potential therapeutic target for treating periodontitis in the future.
References
Socransky, S.S., A.D. Haffajee, M.A. Cugini, C. Smith, and R.L. Kent Jr. 1998. Microbial complexes in subgingival plaque. Journal of Clinical Periodontology 25(2): 134–144.
Nishihara, T., and T. Koseki. 2004. Microbial etiology of periodontitis. Periodontology 2000(36): 14–26.
Kim, Y.C., Y. Ko, S.D. Hong, K.Y. Kim, Y.H. Lee, C. Chae, and Y. Choi. 2010. Presence of Porphyromonas gingivalis and plasma cell dominance in gingival tissues with periodontitis. Oral Diseases 16(4): 375–381.
Sun, Y., R. Shu, C.L. Li, and M.Z. Zhang. 2010. Gram-negative periodontal bacteria induce the activation of Toll-like receptors 2 and 4, and cytokine production in human periodontal ligament cells. Journal of Periodontology 81(10): 1488–1496.
Chang, L.C., H.C. Kuo, S.F. Chang, H.J. Chen, K.F. Lee, T.H. Lin, T.Y. Huang, C.S. Choe, L.T. Lin, and C.N. Chen. 2013. Regulation of ICAM-1 expression in gingival fibroblasts infected with high-glucose-treated P. gingivalis. Cellular Microbiology 15(10): 1722–34. doi:10.1111/cmi.12146.
Dongari-Bagtzoglou, A.I., and J.L. Ebersole. 1998. Increased presence of interleukin-6 (IL-6) and IL-8 secreting fibroblast subpopulations in adult periodontitis. Journal of Periodontology 69(8): 899–910.
Osborn, L., C. Hession, R. Tizard, C. Vassallo, S. Luhowskyj, G. Chi-Rosso, and R. Lobb. 1989. Direct expression cloning of vascular cell adhesion molecule 1, a cytokine-induced endothelial protein that binds to lymphocytes. Cell 59(6): 1203–1211.
Springer, T.A. 1994. Traffic signals for lymphocyte recirculation and leukocyte emigration: the multistep paradigm. Cell 76(2): 301–314.
van Wetering, S., N. van den Berk, J.D. van Buul, F.P. Mul, I. Lommerse, R. Mous, J.P. ten Klooster, J.J. Zwaginga, and P.L. Hordijk. 2003. VCAM-1-mediated Rac signaling controls endothelial cell-cell contacts and leukocyte transmigration. American Journal of Physiology. Cell physiology 285(2): C343–352.
Klimiuk, P.A., M. Fiedorczyk, S. Sierakowski, and J. Chwiecko. 2007. Soluble cell adhesion molecules (sICAM-1, sVCAM-1, and sE-selectin) in patients with early rheumatoid arthritis. Scandinavian Journal of Rheumatology 36(5): 345–350.
Guray, U., A.R. Erbay, Y. Guray, M.B. Yilmaz, A.A. Boyaci, H. Sasmaz, S. Korkmaz, and E. Kutuk. 2004. Levels of soluble adhesion molecules in various clinical presentations of coronary atherosclerosis. International Journal of Cardiology 96(2): 235–240.
Cybulsky, M.I., K. Iiyama, H. Li, S. Zhu, M. Chen, M. Iiyama, V. Davis, J.C. Gutierrez-Ramos, P.W. Connelly, and D.S. Milstone. 2001. A major role for VCAM-1, but not ICAM-1, in early atherosclerosis. The Journal of Clinical Investigation 107(10): 1255–1262.
Hannigan, E., D.P. O'Connell, A. Hannigan, and L.A. Buckley. 2004. Soluble cell adhesion molecules in gingival crevicular fluid in periodontal health and disease. Journal of Periodontology 75(4): 546–550.
Lester, S.R., J.L. Bain, F.G. Serio, B.D. Harrelson, and R.B. Johnson. 2009. Relationship between gingival angiopoietin-1 concentrations and depth of the adjacent gingival sulcus. Journal of Periodontology 80(9): 1447–1453.
Morandini, A.C., P.P. Chaves Souza, E.S. Ramos-Junior, D.T. Brozoski, C.R. Sipert, C.A. Souza Costa, and C.F. Santos. 2013. Toll-like receptor 2 knockdown modulates interleukin (IL)-6 and IL-8 but not stromal derived factor-1 (SDF-1/CXCL12) in human periodontal ligament and gingival fibroblasts. Journal of Periodontology 84(4): 535–544.
Herath, T.D., R.P. Darveau, C.J. Seneviratne, C.Y. Wang, Y. Wang, and L. Jin. 2013. Tetra- and penta-acylated lipid A structures of Porphyromonas gingivalis LPS differentially activate TLR4-mediated NF-kappaB signal transduction cascade and immuno-inflammatory response in human gingival fibroblasts. PloS One 8(3): e58496.
Hajishengallis, G., H. Sojar, R.J. Genco, and E. DeNardin. 2004. Intracellular signaling and cytokine induction upon interactions of Porphyromonas gingivalis fimbriae with pattern-recognition receptors. Immunological Investigations 33(2): 157–172.
Inohara, Chamaillard, C. McDonald, and G. Nunez. 2005. NOD-LRR proteins: role in host-microbial interactions and inflammatory disease. Annual Review of Biochemistry 74: 355–383.
Chung, W.O., J.Y. An, L. Yin, B.M. Hacker, M.G. Rohani, H. Dommisch, and D.H. DiJulio. 2010. Interplay of protease-activated receptors and NOD pattern recognition receptors in epithelial innate immune responses to bacteria. Immunology Letters 131(2): 113–119.
Uehara, A., and H. Takada. 2007. Functional TLRs and NODs in human gingival fibroblasts. Journal of Dental Research 86(3): 249–254.
Jeon, D.I., S.R. Park, M.Y. Ahn, S.G. Ahn, J.H. Park, and J.H. Yoon. 2012. NOD1 and NOD2 stimulation triggers innate immune responses of human periodontal ligament cells. International Journal of Molecular Medicine 29(4): 699–703.
Nemoto, E., T. Honda, S. Kanaya, H. Takada, and H. Shimauchi. 2008. Expression of functional Toll-like receptors and nucleotide-binding oligomerization domain proteins in murine cementoblasts and their upregulation during cell differentiation. Journal of Periodontal Research 43(5): 585–593.
Hosokawa, I., Y. Hosokawa, K. Ozaki, H. Yumoto, H. Nakae, and T. Matsuo. 2010. Proinflammatory effects of muramyldipeptide on human gingival fibroblasts. Journal of Periodontal Research 45(2): 193–199.
Liu, J., J. Duan, Y. Wang, and X. Ouyang. 2013. ICAM-1 is Regulated by Porphyromonas Gingivalis Through NOD1 and NOD2 Molecules in Periodontal Fibroblasts. Journal of Periodontology. doi:10.1902/jop.2013.130152.
Deshpande, R.G., M.B. Khan, and C.A. Genco. 1998. Invasion of aortic and heart endothelial cells by Porphyromonas gingivalis. Infection and Immunity 66(11): 5337–5343.
\Zhou, S., J. Zhang, H. Zheng, Y. Zhou, F. Chen, and J. Lin. 2013. Inhibition of mechanical stress-induced NF-kappaB promotes bone formation. Oral Diseases 19(1): 59–64.
Okugawa, T., T. Kaneko, A. Yoshimura, N. Silverman, and Y. Hara. 2010. NOD1 and NOD2 mediate sensing of periodontal pathogens. Journal of Dental Research 89(2): 186–191.
Liu, R., T. Desta, M. Raptis, R.P. Darveau, and D.T. Graves. 2008. P. gingivalis and E. coli lipopolysaccharides exhibit different systemic but similar local induction of inflammatory markers. Journal of Periodontology 79(7): 1241–1247.
Katz, J., V. Sambandam, J.H. Wu, S.M. Michalek, and D.F. Balkovetz. 2000. Characterization of Porphyromonas gingivalis-induced degradation of epithelial cell junctional complexes. Infection and Immunity 68(3): 1441–1449.
Lin, S.J., Y.L. Chen, M.Y. Kuo, C.L. Li, and H.K. Lu. 2005. Measurement of gp130 cytokines oncostatin M and IL-6 in gingival crevicular fluid of patients with chronic periodontitis. Cytokine 30(4): 160–167.
Garlet, G.P., M.J. Avila-Campos, C.M. Milanezi, B.R. Ferreira, and J.S. Silva. 2005. Actinobacillus actinomycetemcomitans-induced periodontal disease in mice: patterns of cytokine, chemokine, and chemokine receptor expression and leukocyte migration. Microbes and Infection/Institut Pasteur 7(4): 738–747.
Bendre, M.S., D.C. Montague, T. Peery, N.S. Akel, D. Gaddy, and L.J. Suva. 2003. Interleukin-8 stimulation of osteoclastogenesis and bone resorption is a mechanism for the increased osteolysis of metastatic bone disease. Bone 33(1): 28–37.
Joe, B.H., J.L. Borke, M. Keskintepe, P.J. Hanes, J.M. Mailhot, and B.B. Singh. 2001. Interleukin-1beta regulation of adhesion molecules on human gingival and periodontal ligament fibroblasts. Journal of Periodontology 72(7): 865–870.
Hosokawa, Y., I. Hosokawa, K. Ozaki, H. Nakae, and T. Matsuo. 2006. Cytokines differentially regulate ICAM-1 and VCAM-1 expression on human gingival fibroblasts. Clinical and Experimental Immunology 144(3): 494–502.
Hosokawa, Y., I. Hosokawa, K. Ozaki, H. Nakae, and T. Matsuo. 2006. Proinflammatory effects of tumour necrosis factor-like weak inducer of apoptosis (TWEAK) on human gingival fibroblasts. Clinical and Experimental Immunology 146(3): 540–549.
Park, H.J., S.K. Jeong, S.R. Kim, S.K. Bae, W.S. Kim, S.D. Jin, T.H. Koo, H.O. Jang, I. Yun, K.W. Kim, and M.K. Bae. 2009. Resveratrol inhibits Porphyromonas gingivalis lipopolysaccharide-induced endothelial adhesion molecule expression by suppressing NF-kappaB activation. Archives of Pharmacal Research 32(4): 583–591.
Chou, H.H., H. Yumoto, M. Davey, Y. Takahashi, T. Miyamoto, F.C. Gibson 3rd, and C.A. Genco. 2005. Porphyromonas gingivalis fimbria-dependent activation of inflammatory genes in human aortic endothelial cells. Infection and Immunity 73(9): 5367–5378.
Murakami, S., Y. Shimabukuro, T. Saho, E. Hino, D. Kasai, T. Hashikawa, H. Hirano, and H. Okada. 1997. Immunoregulatory roles of adhesive interactions between lymphocytes and gingival fibroblasts. Journal of Periodontal Research 32(1 Pt 2): 110–114.
Lu, X., E. Mu, Y. Wei, S. Riethdorf, Q. Yang, M. Yuan, J. Yan, Y. Hua, B.J. Tiede, B.G. Haffty, K. Pantel, J. Massague, and Y. Kang. 2011. VCAM-1 promotes osteolytic expansion of indolent bone micrometastasis of breast cancer by engaging alpha4beta1-positive osteoclast progenitors. Cancer Cell 20(6): 701–714.
Tang, L., X.D. Zhou, Q. Wang, L. Zhang, Y. Wang, X.Y. Li, and D.M. Huang. 2011. Expression of TRAF6 and pro-inflammatory cytokines through activation of TLR2, TLR4, NOD1, and NOD2 in human periodontal ligament fibroblasts. Archives of Oral Biology 56(10): 1064–1072.
Hitotsumatsu, O., R.C. Ahmad, R. Tavares, M. Wang, D. Philpott, E.E. Turer, B.L. Lee, N. Shiffin, R. Advincula, B.A. Malynn, C. Werts, and A. Ma. 2008. The ubiquitin-editing enzyme A20 restricts nucleotide-binding oligomerization domain containing 2-triggered signals. Immunity 28(3): 381–390.
Kim, E.K., and E.J. Choi. 2010. Pathological roles of MAPK signaling pathways in human diseases. Biochimica et Biophysica Acta 1802(4): 396–405.
Xu, Y., X. Xu, H. Jin, X. Yang, Q. Gu, and K. Liu. 2013. Effects of a thrombomodulin-derived peptide on monocyte adhesion and intercellular adhesion molecule-1 expression in lipopolysaccharide-induced endothelial cells. Molecular Vision 19: 203–212.
Zhang, H., J. Chen, X. Liu, L. Awar, A. McMickle, F. Bai, S. Nagarajan, and S. Yu. 2013. IL-17 induces expression of vascular cell adhesion molecule through signalling pathway of NF-kappaB, but not Akt1 and TAK1 in vascular smooth muscle cells. Scandinavian Journal of Immunology 77(4): 230–237.
Lee, S.J., S.C. Cho, E.J. Lee, S. Kim, S.B. Lee, J.H. Lim, Y.H. Choi, W.J. Kim, and S.K. Moon. 2013. Interleukin-20 promotes migration of bladder cancer cells through extracellular signal-regulated kinase (ERK)-mediated MMP-9 protein expression leading to nuclear factor (NF-kappaB) activation by inducing the up-regulation of p21(WAF1) protein expression. The Journal of Biological Chemistry 288(8): 5539–5552.
Acknowledgments
We thank Prof. Chenxiong Lai from the Kaohsiung Medical University in Taiwan for generously providing P. gingivalis W83. This study is supported by National Natural Science Foundation of China (no. 181271150).
Conflict of Interest
The authors declare there is no conflict of interests.
Author information
Authors and Affiliations
Corresponding authors
ELECTRONIC SUPPLEMENTARY MATERIAL
Below is the link to the electronic supplementary material.
Supplementary figure 1
Characterization of hPDLCs and hGFs. The fibroblasts were identified by immunohistochemistry of mesenchymal marker vimentin and epithelial markers cytokeratin (CK)-14. Both of hPDLCs and hGFs were typically spindle-shaped and were positive for the mesenchymal marker vimentin (C & D) and negative for the epithelial marker cytokeratin 14, CK (A & B). (JPEG 237 kb)
Supplementary figure 2
mRNA expression of TLR4 in P. gingivalis-challenged hPDLCs and hGFs. Cells were treated with P. gingivalis at indicated MOI for indicated time. Real-time PCR was applied to detect TLR4 expression. No significant change of its expression level was revealed before and after bacterial challenge (A & B). (JPEG 23 kb)
Rights and permissions
About this article
Cite this article
Liu, J., Wang, Y. & Ouyang, X. Beyond Toll-Like Receptors: Porphyromonas gingivalis Induces IL-6, IL-8, and VCAM-1 Expression Through NOD-Mediated NF-κB and ERK Signaling Pathways in Periodontal Fibroblasts. Inflammation 37, 522–533 (2014). https://doi.org/10.1007/s10753-013-9766-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-013-9766-0