Abstract
Baicalein shows anti-inflammatory effects in human rheumatoid arthritis fibroblast-like synoviocytes (RAFLS). Considering its anti-proliferatory effects on various cancer cells, we investigated the effects of baicalein on interleukin-1 beta (IL-1β)-induced proliferation of human RAFLS. Cell proliferation was examined by 3H-thymidine incorporation assay. Western blot analysis was performed to assess the phosphorylation of extracellular regulating kinase (ERK), p38, and c-Jun N-terminal kinase, and nuclear translocation of nuclear factor kappa B (NF-κB) subunit p65. Notably, baicalein significantly suppressed IL-1β-mediated RAFLS proliferation (P < 0.05), along with reduced ERK1/2 and p38 phosphorylation. The IL-1β-induced p65 nuclear translocation and NF-κB DNA binding activity was significantly decreased by baicalein. Additionally, the inhibitory effects of baicalein on IL-1β-induced proliferation of RAFLS were dose-dependently reversed by the addition of recombinant macrophage migration inhibitory factory (MIF). Our results indicate that baicalein inhibits IL-1β-induced RAFLS proliferation, which involves suppression of NF-κB transcriptional activity and MIF-mediated signaling.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Rheumatoid arthritis (RA) is a systemic autoimmune disease characterized by chronic synovitis and progressive destruction of joint cartilage and bone [1]. The histological characterization of RA joints is chronic inflammation with hyperplasia of synovial lining cells [2]. Rheumatoid arthritis fibroblast-like synoviocytes (RAFLS), located in the lining of the joints, participate in all of the pathological events of RA [3]. The imbalance between fibroblast-like synoviocytes (FLS) proliferation and apoptosis confers to RA synovial hyperplasia [4]. The aggressive proliferation of FLSs in RA joints forms a pannus, which secret inflammatory factors, such as cytokines, matrix metalloproteinases (MMPs), and cyclooxygenase-2 [1, 2]. Interleukin-1β (IL-1β) is thought as one of the most important cytokines in the inflammatory responses in RA through inducing proliferation of RAFLS and promoting the secretion of MMPs and prostaglandin E2 by RAFLS [5].
Macrophage migration inhibitory factor (MIF) is a well-recognized cytokine in the regulation of immune and inflammatory diseases, such as human rheumatoid arthritis (RA) [6]. Produced by synovial macrophages and FLS and enhanced in RA serum, synovial fluid, and FLS [6], MIF is involved in most of the pathological processes of RA, including synovial leukocyte recruitment, induction of mitogen-activated protein kinase (MAPK) activation in synoviocytes, impairment of synoviocyte apoptosis, activation of matrix metalloproteinase and cyclooxygenase expression, and amplification of cytokines, including tumor necrosis factor-alpha (TNF-α), interleukin-6 (IL-6), interleukin-1 (IL-1), and interleukin-8 [7]. All of these studies suggested that MIF plays an important role in RA.
Baicalein (5,6,7-trihydroxy-2-phenyl-4H-1-benzopyran-4-one), an active flavonoid extracted from the root of Scutellaria baicalensis, has anticancer, antibacterial, antiviral, and anti-inflammatory properties [8, 9]. Baicalein has been shown to inhibit cell proliferation and induce cell apoptosis in different types of cancer [10–12]. Recent studies showed that baicalein, together with ketorolac tromethamine, inhibits the production of TNF-α, IL-6, and IL-1β in human RAFLS [13]. In the present study, we sought to investigate the effects of baicalein on the IL-1β-induced proliferation of human RAFLS.
MATERIAL AND METHODS
Isolation
FLSs were obtained from the synovium of patients undergoing joint replacement surgery, who fulfilled the American College of Rheumatology Criteria for RA [14]. FLSs were as previously described [15]. Fresh synovial tissues were chopped into fragments and digested with 1 mg/mL collagenase 1 (Sigma-Aldrich, St. Louis, MO, USA) in phosphate-buffered saline (PBS). The resulting cell suspension was filtered through a 70-μm cell strainer, and cultured in 10-cm culture plates with Dulbecco’s modified Eagle’s medium (DMEM; Invitrogen, Carlsbad, CA) containing 10 % fetal calf serum (FCS; Invitrogen) at 37 °C in a 5 % CO2 humidified incubator. FLSs used in this study were from 3–9 passages, and were morphologically homogeneous with typical fibroblastoid configuration under inverse microscopy. The purity of FLSs was measured by flow cytometry with fluorescein isothiocyanate-conjugated anti-CD3, phycoerythrin-conjugated anti-CD90, and allophycocyanin-conjugated anti-CD14 mAb (BD Pharmingen, San Diego, CA). Informed consent was obtained from all patients, and the study protocol was approved by the Ethical Committee of the 97th Hospital of People’s Liberation Army.
Proliferation Assay
The effects of baicalein on IL-1β or MIF-induced proliferation of RAFLS were determined by [3H]-thymidine incorporation [6]. RAFLS were seeded at 5,000 cells/well in 96-well plates in DMEM/10 % FCS complete medium for 12 h and then serum-deprived for 24 h. The cells were stimulated with human recombinant IL-1β (0 or 0.1 ng/ml), baicalein (0, 10, 20, or 40 μM), and/or human recombinant MIF (0, 12.5, 25, 50 ng/ml) for 54 h prior to incubation with 1 μCi/ml [3H]-thymidine (Shanghai Institute of Nuclear Research, Shanghai, China) for another 18 h. Incorporated radioactivity was counted with a liquid scintillation counter (Beckman Coulter Inc., Brea, CA, USA).
Preparation of Nuclear Extracts
RAFLS with indicated treatments were collected and ground with a mortar and homogenized. Protease inhibitor cocktail (Sigma) was added and centrifuged at 2,000 r/min for 30 s. Supernatant was incubated on ice for 5 min and centrifuged at 5,000 r/min for 5 min. Pelleted nuclei were resuspended in 50–100 μl of lysis buffer and incubated on ice for 20 min. The lysed nuclei were transferred into a microcentrifuge tube and centrifuged at 12,000 r/min for 15 min. The supernatant was collected and stored at −80 °C.
Western Blot Analysis
RAFLS (5 × 105) cultured in 60-mm dishes were starved in serum-free medium overnight and incubated with IL-1β (10 ng/ml) for 30 min in the presence or absence of baicalein (20 μm). The cells were subsequently washed twice in PBS and incubated with 50-μl lysis buffer (20 mmol/l Tris-Cl [pH 8.0], 150 mmol/l NaCl, 1 mmol/l EDTA, 1 % Triton X-100, 20 μg/ml chymostatin, 2 mmol/l phenylmethylsuphonyl fluoride, 10 μmol/l leupeptin, and 1 mmol/l 4-[2-aminoethyl] benzenesulfonyl fluoride). RAFLS were scraped by a rubber policeman before another 50-μl lysis buffer was added. The cells were transferred into a microcentrifuge tube, incubated with lysis buffer on ice for 30 min and centrifuged at 14,000 rpm for 15 min. The supernatant was collected for protein concentration analysis by a Bio-Rad Protein Assay Kit (Bio-Rad, Hercules, CA, USA). Twenty micrograms of total protein extract were boiled in 5 × loading buffer (Laemmli sample buffer) for 5 min and separated by 12 % SDS-PAGE and transferred to a nitrocellulose membrane (Amersham, Arlington Heights, IL, USA). The membranes were blocked with 5 % nonfat milk in Tris-buffered saline with Tween 20 (TBST) (10 mmol/l Tris-Cl [pH 8.0], 150 mmol/l NaCl, 0.05 % Tween 20). The blots were probed with the primary antibodies for phosphorylated extracellular regulating kinase (ERK) 1/2 (p-ERK1/2), total ERK 1/2, phosphorylated p38 (p-p38), total p38, phosphorylated c-Jun N-terminal kinase (p-JNK), total JNK, nuclear factor kappa B (NF-κB), subunit p65, and histone (Cell Signaling Technology, Beverly, MA, USA) for 1 h. Blots were washed with 1 × TBST for three times and incubated with secondary antibodies coupled with horseradish peroxidase. Immunoreactive proteins were visualized by an enhanced chemiluminescent detection system (Amersham Biosciences). Blots were scanned on the Fluor-S MAX MultiImager (Bio-Rad), and signal intensities were densitometrically determined by Quantity One image software (Bio-Rad).
Electrophoretic Mobility Shift Assay
Five × 106 RASFs were stimulated with IL-1β (5 ng/ml) in the presence or absence of baicalein for 1 h. Cells were collected and washed with cold PBS. Nuclear extracts were prepared and used for analyze the activation of NF-κB and AP-1 by a gel mobility shift assay [16]. An oligonucleotide containing NF-κB binding site (5′-CCGGTTAACAGAGGGGGCTTTCCGAG-3′) or AP-1 binding site (5′-CGCTTGATGAGTCAGCCGGAA-3′) was synthesized and used as a probe. These two probes were annealed and labeled with [γ32P]-dATP. Labeled-oligonucleotides incubated with 10 mg of nuclear extracts, and binding buffer (10 mM Tris–HCl, pH 7.6, 500 mM KCl, 10 mM EDTA, 50 % glycerol, 100 ng poly (dI-dC), 1 mM dithiothreitol) for 30 min at room temperature in a final volume of 20 ml. The reaction mixtures were examined by electrophoresis on 4 % polyacrylamide gels. The gels were then dried and examined by autoradiography. Specific binding was controlled by competition with a 100-fold excess of cold NF-κB or AP-1 oligonucleotide.
Statistical Analysis
Statistical analysis was carried out by SPSS.11 software (SPSS, Chicago, IL, USA). Data are expressed as means ± SD. All P values were calculated using one-way analysis of variance followed by the Tukey test. A value of P < 0.05 was considered significant.
RESULTS
Baicalein Inhibits IL-1β-Induced Proliferation of RAFLS
IL-1β stimulation significantly enhanced the growth of RAFLS compared with control cells (Fig. 1; P < 0.01). Baicalein had no obvious effect on the proliferation of RAFLS with IL-1β treatment at the concentration of 10 μM (Fig. 1; P > 0.05). However, 20 μM of baicalein significantly attenuated IL-1β-enhanced proliferation of RAFLS (P < 0.05). Forty micrometers of baicalein did not provoke further suppression of IL-1β-induced proliferation of RAFLS.
The effects of baicalein on IL-1β-stimulated proliferation of human RAFLS. RAFLS were seeded with DMEM/10 % FCS complete medium for 12 h and starved for another 24 h. RAFLS were stimulated with human recombinant IL-1β (0.1 ng/ml) and baicalein (0, 10, 20, or 40 μm) for 54 h prior to incubation with 1 μCi/ml [3H]-thymidine. Data are expressed as mean ± SD of six separate experiments. cpm counts per minute. * P < 0.05, ** P < 0.01 versus indicated control.
Baicalein Decreases IL-1β-Mediated Phosphorylation of ERK and p38 in RAFLS
IL-1β treatment markedly increased the phosphorylation levels of ERK 1/2, p38 and JNK (Fig. 2). Baicalein significantly decreased IL-1β-induced phosphorylation of ERK 1/2 (P < 0.01) and p38 (P < 0.01), but not JNK (Fig. 2).
The effects of baicalein on IL-1β-induced MAPK signaling pathways. Human RAFLS were starved in serum-free medium overnight and stimulated with IL-1β (10 ng/ml) for 30 min in the presence or absence of baicalein (20 μm). The cells were collected and subjected to Western blot analysis for the phosphorylation of ERK1/2, p38 and JNK. Representative blots are shown in the left panels. Quantitative analysis of the phosphorylation of ERK1/2, p38 and JNK are shown in the right panels. Data are expressed as mean ± SD of three separate experiments. ** P < 0.01 versus indicated control.
Baicalein Attenuates IL-1β-Induced NF-κB DNA Binding Activity
IL-1β treatment enhanced the translocation of NF-κB p65 subunit into the nucleus of RAFLS (Fig. 3a; P < 0.01) and increased the NF-κB DNA binding activity (Fig. 3b), which were markedly suppressed by baicalein. IL-1β stimulation also led to a substantial increase in the AP-1 DNA binding activity (Fig. 3c). Baicalein had no effects on IL-1β-stimulated AP-1 DNA binding activity (Fig. 3c).
The effects of baicalein on IL-1β-induced activation of NF-κB and AP-1 signaling pathways. Human RAFLS were incubated with IL-1β (5 ng/ml) in the presence or absence of baicalein for 1 h. Cells were collected and washed with cold PBS. Nuclear extracts were prepared and used for analyze the activation of NF-κB by Western blot analysis (a) and EMSA (b), and the activation of AP-1 by EMSA (c). a Nuclear translocation of NF-κB subunit p65 was measured by Western blot analysis. Representative blots are shown in the left panels. Quantitative analyses of the expression of p65 in nucleus are shown in the right panels. CO cold oligonucleotide. Data are present as mean ± SD of three independent experiments. ** P < 0.01 versus indicated control.
Baicalein Attenuates IL-1β-Induced NF-κB DNA Binding Activity
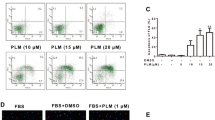
Figure 4a showed that MIF stimulation markedly enhanced the proliferation of RAFLS (Fig. 4a; P < 0.01). The proliferation of RAFLS stimulated by MIF was suppressed dose-dependently by baicalein (Fig. 4a). Figure 4b showed that baicalein profoundly inhibited IL-1β-mediated RAFLS proliferation (P < 0.05), which was reversed by MIF treatment in a dose-dependent manner (Fig. 4b).
The effects of baicalein on MIF-stimulated proliferation of human RAFLS. RAFLS were seeded with DMEM complete medium for 12 h and starved for another 24 h. a RAFLS were stimulated with human recombinant MIF (50 ng/ml), and baicalein (0, 10, 20, or 40 μm) for 54 h prior to incubation with 1 μCi/ml [3H]-thymidine. b The cells were stimulated with human recombinant IL-1β (0.1 ng/ml), baicalein (20 μm), and human recombinant MIF (0, 12.5, 25, 50 ng/ml) for 54 h prior to incubation with 1 μCi/ml [3H]-thymidine. Data are expressed as mean ± SD of six separate experiments. cpm counts per minute. * P < 0.05, ** P < 0.01 versus indicated control.
DISCUSSION
In the present study, we found that baicalein exhibited inhibitory effects on IL-1β-induced RAFLS proliferation. Baicalein decreased the phosphorylation of ERK1/2 and p38, attenuated NF-κB p65 translocation into the nucleus and lowered NF-κB DNA binding activity in IL-1β-stimulated RAFLS. Interestingly, baicalein-mediated suppressive effects on IL-1β-induced RAFLS proliferation were recovered dose-dependently by MIF, indicating that baicalein inhibits IL-1β-induced RAFLS growth through dampening MIF signaling pathway. Our results indicate that baicalein shows therapeutic potential in RA.
IL-1β is one important cytokine involved in the pathogenesis of inflammatory synovitis joint destruction [5, 17]. It has been suggested that IL-1β induces the proliferation of RAFLS, which plays a pivotal role in the physiopathology of RA via participating in inflammation and joint destruction [5]. Meanwhile, IL-1β level has been shown to be enhanced in synovial fluid and sera of patients with RA [18]. IL-1β inhibition has been suggested as one possible strategy for RA treatment [19–22]. In the present study, we found that baicalein-inhibited IL-1β-induced proliferation of RAFLS. Yang et al. showed that ketorolac baicalein in combination with tromethamine decreases the levels of inflammatory factors in human synoviocytes [13]. Both results indicate that baicalein possesses therapeutic potency for RA treatment.
IL-1β, as an important factor for the induction of cell growth, acts at least partially through the activation of NF-κB and MAPKs signal transduction pathways [23]. NF-κB and MAPKs participate in the inflammation and destruction of joints in RA [24]. MAPKs have been suggested to play a critical role in the pathogenesis of RA [23]. Three major MAPK family members are JNK, ERK, and p38 kinase [25], which are expressed in cultured RAFLS and readily activated by IL-1β [26]. To define the mechanisms of how baicalein inhibits IL-1β-induced RAFLS proliferation, the activation of MAPKs and NF-κB was measured. Our data showed that baicalein inhibits IL-1β-induced NF-κB activation and phosphorylation of ERK, p38, but not JNK. Accumulating evidence has been suggested that MAPKs or NF-κB inhibition attenuates synovial inflammation, bone destruction, and cartilage damage in animal models of arthritis [24, 27]. Thus, the inhibition of IL-1β-mediated NF-κB activation and phosphorylation of ERK, p38 by baicalein indicates that baicalein might be a potential therapeutic approach for RA treatment. IL-1β has been demonstrated to activate AP-1 via activation of MAPKs [28]. IL-1β-stimulated activation of AP-1 was also assessed in baicalein-treated RAFLS. Consistent with the effects of baicalein on the phosphorylation of JNK, baicalein did not show overt effects on AP-1 DNA binding activity.
MIF exerts proinflammatory effects on RAFLS and regulates RA synovial hyperplasia by acting directly and via the involvement in the effects of IL-1β and TNF-α [6]. The effects of MIF on RAFLS proliferation and activation are dependent on MAPKs/ERK signaling pathway [6]. It has been suggested that MIF antagonism has an important therapeutic potential in RA [6]. We analyzed the effects of baicalein on MIF-induced proliferation of RAFLS. We found that baicalein suppressed MIF-induced RAFLS proliferation. Interestingly, addition of MIF significantly reversed baicalein-mediated proliferation-inhibitory effects on IL-1β-stimulated RAFLS (P < 0.01), which indicates that MIF inhibition might confer baicalein-mediated suppression of IL-1β-induced RAFLS growth. Our results suggested that MIF inhibition might be another mechanism for baicalein-mediated inhibition of RAFLS proliferation.
TNF-α is an important mediator in the pathogenesis of RA [29]. High levels of TNF-α in RA synovium play an important role in the synovial hyperplasia of RA by suppressing apoptosis and promoting proliferation of synoviocytes through activation of NF-κB and MAPK pathways [29, 30]. In the present study, we found that baicalein decreased IL-1β-mediated RAFLS proliferation through inhibition of NF-κB and MAPK/ERK/p38 signaling pathways. It would be very interesting to investigate the effects of baicalein on TNF-α-mediated RAFLS proliferation and activation of NF-κB and MAPK signaling pathways. As the ability of IL-1β and TNF-α to induce RAFLS proliferation is dependent on MIF [6], it is also worth exploring the role of baicalein on MIF signaling pathway in TNF-α-stimulated RAFLS.
Our data revealed that baicalein inhibits IL-1β-induced RAFLS proliferation through inactivation of NF-κB, lowering the phosphorylation of MAPK/ERK/p38 and inhibition of MIF signaling pathway.
References
Li, H., and A. Wan. 2013. Apoptosis of rheumatoid arthritis fibroblast-like synoviocytes: possible roles of nitric oxide and the thioredoxin 1. Mediators of Inflammation 2013: 953462.
Han, M.K., J.S. Kim, B.H. Park, J.R. Kim, B.Y. Hwang, H.Y. Lee, E.K. Song, and W.H. Yoo. 2003. NF-kappaB-dependent lymphocyte hyper adhesiveness to synovial fibroblasts by hypoxia and reoxygenation: potential role in rheumatoid arthritis. Journal of Leukocyte Biology 73: 525–529.
Firestein, G.S. 1996. Invasive fibroblast-like synoviocytes in rheumatoid arthritis. Passive responders or transformed aggressors? Arthritis and Rheumatism 39: 1781–1790.
Firestein, G.S., M. Yeo, and N.J. Zvaifl er. 1995. Apoptosis in rheumatoid arthritis synovium. Journal of Clinical Investigation 96: 1631–1638.
Choy, E.H., and G.S. Panayi. 2001. Cytokine pathways and joint inflammation in rheumatoid arthritis. The New England Journal of Medicine 344: 907–916.
Lacey, D., A. Sampey, R. Mitchell, R. Bucala, L. Santos, M. Leech, and E. Morand. 2003. Control of fibroblast-like synoviocyte proliferation by macrophage migration inhibitory factor. Arthritis and Rheumatism 48: 103–109.
Ayoub, S., M.J. Hickey, and E.F. Morand. 2008. Mechanisms of disease: macrophage migration inhibitory factor in SLE, RA and atherosclerosis. Nature Clinical Practice Rheumatology 4: 98–105.
So, F.V., N. Guthrie, A.F. Chambers, and K.K. Carroll. 1997. Inhibition of proliferation of estrogen receptor-positive MCF-7 human breast cancer cells by flavonoids in the presence and absence of excess estrogen. Cancer Letters 112: 127–133.
Lin, C.C., and D.E. Shieh. 1996. The anti-inflammatory activity of Scutellaria rivularis extracts and its active components, baicalin, baicalein and wogonin. The American Journal of Chinese Medicine 24: 31–36.
Wong, B.C., W.P. Wang, C.H. Cho, X.M. Fan, M.C. Lin, H.F. Kung, and S.K. Lam. 2001. 12-Lipoxygenase inhibition induced apoptosis in human gastric cancer cells. Carcinogenesis 22: 1349–1354.
Chen, J., Z. Li, A.Y. Chen, X. Ye, H. Luo, G.O. Rankin, and Y.C. Chen. 2013. Inhibitory effect of baicalin and baicalein on ovarian cancer cells. International Journal of Molecular Sciences 14: 6012–6025.
Zhang, H.B., P. Lu, Q.Y. Guo, Z.H. Zhang, and X.Y. Meng. 2013. Baicalein induces apoptosis in esophageal squamous cell carcinoma cells through modulation of the PI3K/Akt pathway. Oncology Letters 5: 722–728.
Yang, J.H., M.Y. Yun, N.H. Lee, D.K. Kim, Y.I. Kim, Y.H. Noh, T.Y. Kim, S.W. Yoon, and S.C. Shin. 2008. The effects of ketorolac tromethamine and baicalein on the levels of inflammatory factors in human synoviocytes. Archives of Pharmacal Research 31: 1517–1523.
Arnett, F.C., S.M. Edworthy, D.A. Bloch, D.J. McShane, J.F. Fries, N.S. Cooper, L.A. Healey, S.R. Kaplan, M.H. Liang, H.S. Luthra, et al. 1988. The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis and Rheumatism 31: 315–324.
Lee, H.Y., H.S. Jeon, E.K. Song, M.K. Han, S.I. Park, S.I. Lee, H.J. Yun, J.R. Kim, J.S. Kim, Y.C. Lee, S.I. Kim, H.R. Kim, J.Y. Choi, I. Kang, H.Y. Kim, and W.H. Yoo. 2006. CD40 ligation of rheumatoid synovial fibroblasts regulates RANKL-mediated osteoclastogenesis: evidence of NF-kappaB-dependent, CD40-mediated bone destruction in rheumatoid arthritis. Arthritis and Rheumatism 54: 1747–1758.
Noh, E.M., J.S. Kim, H. Hur, B.H. Park, E.K. Song, M.K. Han, K.B. Kwon, W.H. Yoo, I.K. Shim, S.J. Lee, H.J. Youn, and Y.R. Lee. 2009. Cordycepin inhibits IL-1beta-induced MMP-1 and MMP-3 expression in rheumatoid arthritis synovial fibroblasts. Rheumatology (Oxford, England) 48: 45–48.
Gitter, B.D., J.M. Labus, S.L. Lees, and M.E. Scheetz. 1989. Characteristics of human synovial fibroblast activation by IL-1 beta and TNF alpha. Immunology 66: 196–200.
Symons, J.A., T.L. McDowell, F.S. di Giovine, N.C. Wood, S.J. Capper, and G.W. Duff. 1989. Interleukin 1 in rheumatoid arthritis: potentiation of immune responses within the joint. Lymphokine Research 8: 365–372.
Williams, A.S., S.G. Jones, R.M. Goodfellow, N. Amos, and B.D. Williams. 1999. Interleukin-1beta (IL-1beta) inhibition: a possible mechanism for the anti-inflammatory potency of liposomally conjugated methotrexate formulations in arthritis. British Journal of Pharmacology 128: 234–240.
Geiger, T., H. Towbin, A. Cosenti-Vargas, O. Zingel, J. Arnold, C. Rordorf, M. Glatt, and K. Vosbeck. 1993. Neutralization of interleukin-1 beta activity in vivo with a monoclonal antibody alleviates collagen-induced arthritis in DBA/1 mice and prevents the associated acute-phase response. Clinical and Experimental Rheumatology 11: 515–522.
Van den BERG, W.B., L.A.B. JOOSTEN, M. HELSEN, and F.A.J. Van de LOO. 1994. Amelioration of established murine collagen-induced arthritis with anti-IL-1 treatment. Clinical and Experimental Immunology 95: 237–243.
Lee, E.G., S.L. Lee, H.J. Chae, S.J. Park, Y.C. Lee, and W.H. Yoo. 2010. Ethyl acetate fraction from Cudrania tricuspidata inhibits IL-1β-induced rheumatoid synovial fibroblast proliferation and MMPs, COX-2 and PGE2 production. Biological Research 43: 225–231.
Inoue, H., M. Takamori, N. Nagata, T. Nishikawa, H. Oda, S. Yamamoto, and Y. Koshihara. 2001. An investigation of cell proliferation and soluble mediators induced by interleukin 1beta in human synovial fibroblasts: comparative response in osteoarthritis and rheumatoid arthritis. Inflammation Research 50: 65–72.
McIntyre, K.W., D.J. Shuster, K.M. Gillooly, D.M. Dambach, M.A. Pattoli, P. Lu, X.D. Zhou, Y. Qiu, F.C. Zusi, and J.R. Burke. 2003. A highly selective inhibitor of I kappa B kinase, BMS-345541, blocks both joint inflammation and destruction in collagen-induced arthritis in mice. Arthritis and Rheumatism 48: 2652–2659.
Robinson, M.J., and M.H. Cobb. 1997. Mitogen-activated protein kinase pathways. Current Opinion in Cell Biology 9: 180–185.
Han, Z., D.L. Boyle, L. Chang, B. Bennett, M. Karin, L. Yang, A.M. Manning, and G.S. Firestein. 2001. c-Jun N-terminal kinase is required for metalloproteinase expression and joint destruction in inflammatory arthritis. Journal of Clinical Investigation 108(1): 73–81. Erratum in: J. Clin. Invest. 108:1883.
Nishikawa, M., A. Myoui, T. Tomita, K. Takahi, A. Nampei, and H. Yoshikawa. 2003. Prevention of the onset and progression of collagen-induced arthritis in rats by the potent p38 mitogen-activated protein kinase inhibitor FR167653. Arthritis and Rheumatism 48: 2670–2681.
Han, Z., D.L. Boyle, A.M. Manning, and G.S. Firestein. 1998. AP-1 and NF-kB regulation in rheumatoid arthritis and murine collagen-induced arthritis. Autoimmunity 28: 197–208.
Youn, J., H.Y. Kim, J.H. Park, S.H. Hwang, S.Y. Lee, C.S. Cho, and S.K. Lee. 2002. Regulation of TNF-alpha-mediated hyperplasia through TNF receptors, TRAFs, and NF-kappaB in synoviocytes obtained from patients with rheumatoid arthritis. Immunology Letters 83: 85–93.
Huber, L.C., O. Distler, I. Tarner, R.E. Gay, S. Gay, and T. Pap. 2006. Synovial fibroblasts: key players in rheumatoid arthritis. Rheumatology (Oxford, England) 45: 669–675.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chen, S., Yang, Y., Feng, H. et al. Baicalein Inhibits Interleukin-1β-Induced Proliferation of Human Rheumatoid Arthritis Fibroblast-like Synoviocytes. Inflammation 37, 163–169 (2014). https://doi.org/10.1007/s10753-013-9725-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-013-9725-9