Abstract
Hypersensitivity and autoimmunity are the main features of immune system-related diseases such as type 2 diabetes (T2D), multiple sclerosis (MS), and asthma. It has been established that chemokines play key roles in the activation and regulation of immune cell migration which is important in the pathogenesis of the diseases mentioned. CC chemokines receptor 5 or CCR5 is a receptor for RANTES, MIP-1α, and MIP-1β and is expressed by several immune cells including NK cells, T lymphocytes, and macrophages. It plays key roles in the regulation of migration and activation of the immune cells during immune responses against microbe and self-antigens during autoimmunity and hypersensitivity disorders. Therefore, any alteration in the sequence of CCR5 gene or in its expression could be associated with immune system-related diseases. Previous studies revealed that a 32-base pair deletion (Δ 32) in exon 1 of the CCR5 gene led to downregulation of the gene. Previous studies demonstrated that not only CCR5 expression was altered in autoimmune and hypersensitivity disorders, but also that the mutation is associated with the diseases. This review addresses the recent information regarding the association of the CCR5 Δ 32 mutation in immune-related diseases including T2D with and without nephropathy, MS, and asthma. Based on the collected data, it seems that the CCR5 Δ 32 mutation can be considered as a risk factor for MS, but not asthma and T2D with and without nephropathy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
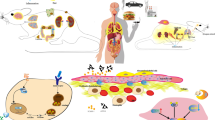
Immune responses are the main defense against tumors and infectious diseases [1, 2]. Uncontrolled immune responses against self and foreign antigens are described as autoimmunity and hypersensitivity, respectively [3]. It has been shown that chemokines play key roles in the regulation of immune responses which are important in the pathogenesis of both autoimmunity- and hypersensitivity-based diseases [4]. Chemokine receptor 5 (CCR5) is located on the short arm of chromosome 3 (3p21.31), which is a locus for multiple chemokine receptor genes [5]. CCR5 is a receptor for the MIP-1α/CCL3, MIP-1β/CCL4, and RANTES/CCL5 chemokines and is expressed by several immune cells including NK cells, T lymphocytes, macrophages, and immature dendritic cells and is upregulated by proinflammatory cytokines [6, 7] as well as nuclear factor kappa-light-chain-enhancer (NF-κB) [8]. It can also be regulated by the cAMP response element-binding protein pathway [9]. CCR5 belongs to the heterotrimeric G protein family and can inhibit cAMP production, while stimulating Ca2+ release and promote activation of the PI3-kinase, mitogen-activated protein (MAP) kinases, and other tyrosine kinase cascades including FAK and Pyk2, which play important roles in cell movement and migration [10]. CCL3, 4, and 5 also activate the three main members of the MAP kinase family (ERK1/2, p38, and SAPK/JNK), Rho GTPase, and protein kinase B (PKB) via CCR5, which are proposed to be crucial for T cell proliferation and expression of inflammatory cytokines [11]. Activation of JAK/STAT pathways by CCL5/CCR5 interactions was also reported by Wong et al. [12]. Therefore, it appears that CCR5 plays a key role in immune responses ranging from infiltration to activation of immune cells (Fig. 1) [13]. It has been established that the deletion of 32 nucleotides in exon 1 of the CCR5 gene (known as the Δ 32 mutation) leads to decreased expression and dysfunction of CCR5 receptor [13-16]. Interestingly, recent evidence demonstrated that this mutation is polymorphic in different ethnic and geographical populations [17, 18]. Furthermore, it has been documented that CCR5 acts as a co-receptor for HIV-1 and is critical for its transmission [19]. Interestingly, previous studies demonstrated that the CCR5 Δ 32 mutation can affect infection of T lymphocytes by HIV-1 [20]. In contrast to HIV infection, CCR5 and its known mutation play different roles in different immune-related diseases, including multiple sclerosis (MS), type 2 diabetes (T2D), and asthma [21-23].
The figure illustrates the CCR5 receptor structure and its signaling pathways. CCR5 is shown as cellular receptor with seven transmembrane domains. CCL3, 4, and 5 bind to the extracellular domain of CCR5 and lead to the activation of intracellular pathways. The conserved amino acids (DRYLAVHA) within the first intracellular loop are essential for interactions with G proteins (α, β, and γ). The CCR5/ligand interaction induces G protein dissociation and consequently the activation of intracellular pathways including JAK/STATs, phospholipase Cβ (PLCβ), phosphoinositide 3-kinase (PI-3K), diacylglycerol (DAG), triphosphoinositol (IP 3 ), calcium ions (Ca 2+), protein kinase C (PKC), proline-rich tyrosine kinase 2 (PYK2), extracellular signal-regulated kinase (ERK1/2), p38 and c-Jun N-terminal kinase (JNK), protein kinase B (PKB), Rho GTPase, and adenylyl cyclase (AC). Adapted from Sorce et al. [11].
Furthermore, the exact role of the Δ 32 mutation is confounded by factors such as a patient's immunological status and genetic and epigenetic factors. Individually or combined, all these factors can alter the response by a patient to the different immune system-related diseases. This is further confounded by ethnic and geographical populations which may carry polymorphisms in the genes that interact with CCR Δ 32, thereby subtly changing the biological activity of the protein. Evaluating the association of the CCR5 Δ 32 mutation to immunological disorders or disease, within a specific population, may avail us to the first clues that will unravel the function of the gene and its mutation. It has been documented that the CCR5 Δ 32 mutation leads to a much greater change in expression of the receptor in the homozygotic form when it is compared to the heterozygotic form. The immune cells of affected CCR5 individuals (carrying the CCR5 Δ 32 mutation) are unable to elicit a complete response to CCL3, 4, and 5. Therefore, it seems that CCR5 Δ 32 mutation may affect an individual's immune responses; hence, evaluation of the mutation can be rationalized to better understand immune-related disease mechanisms.
It has also been demonstrated that there is a positive correlation between asthma [24, 25], MS [26-28], T2D without nephropathy [29-32], and T2D with nephropathy [32, 33] with immune system factors. Therefore, it is plausible that genetic variations within CCR5 may be correlated to T2D with and without nephropathy, MS, and asthma. On the other hand, previous studies demonstrated that the epidemiology of the CCR5 Δ 32 mutation is different among ethnic populations. The rate of CCR5 Δ 32 mutations is high among the northern European population, while its value is low among the southeastern Asian population; hence, evaluation of the relation between the CCR5 Δ 32 mutation and immune-related diseases may be more important in some ethnic populations and less in others. Therefore, the aim of this review was to collate the current information regarding the correlation between the CCR5 Δ 32 mutation with these diseases. Demographic data and supporting information regarding the reported studies are summarized in Table 1.
THE STATUS OF THE CCR5 Δ 32 MUTATION IN TYPE 2 DIABETES
It has been well documented that parameters that influence or regulate the immune system can be associated with T2D and its complications [32-36]. Previous studies have revealed that adiponectin can upregulate expression of CCL3, 4, and 5, while downregulating surface CCR5 expression [37]. In addition, previous studies demonstrated that T2D alters CCR5 expression on the immune cells [38, 39]. The expression of adiponectin is changed in T2D pathology, and the data suggest that the expression of CCR5 is suboptimal in these patients. The presence of the CCR5 Δ 32 mutation may exacerbate disease progression in T2D patients carrying this mutation. Additionally, infiltration of immune cells within the pancreas has been documented in T2D [37]. Some studies proposed that CCR5 can be involved in the recruitment of immune cells to the pancreas; hence, it seems that the genetic and epigenetic factors that alter CCR5 expression, including the CCR5 Δ 32 mutation, can be considered as an important risk factor in the pathogenesis of T2D and its complications including nephropathy. Our previous findings demonstrated that the CCR5 Δ 32 mutation was not prevalent in either southeast Iranian T2D patients without nephropathy or T2D patients with nephropathy [36]. The control group in our study also carried a very low prevalence of this mutation (0.66 %) [36]. In agreement with our previous results, Kalev and colleagues reported that there was no association between the CCR5 Δ 32 mutation and native Estonian T2D patients [40]. Interestingly, Muntinghe et al. reported that the CCR5 Δ 32 mutation is associated with better survival in T2D patients [21]. They concluded that the protective potential of pharmacological blockage of CCR5 can be considered as a therapeutic method in type 2 diabetic patients [21]. Ahluvalia et al. revealed that homozygotic CCR5 Δ 32 mutations (Δ32/Δ32) were more prevalent in a North Indian nephropathic T2D group [41]. These results are in contrast with the Bogdanski et al. study [39] who demonstrated that CCR5 expression is increased on immune cells in T2D [39]. Due to the fact that CCR5 Δ 32 mutation leads to decrease expression of CCR5, it could be assumed that the patients that were evaluated in the Bogdanski et al. study did not carry the CCR5 Δ 32 mutation. To the best of our knowledge, there are only a limited number of studies regarding other polymorphisms within the CCR5 gene among T2D patients; however, several studies have demonstrated that polymorphisms within other regions of the CCR5 gene are significantly associated with T2D [5, 8, 9]. In summary, an increased expression of CCR5 on immune cells of T2D patients with and without nephropathy was reported by several researchers [38, 39]. It seems that the CCR5 Δ 32 mutation cannot be considered as a potential risk factor for initiating T2D in select populations, but there may be a relation between other polymorphisms with T2D in patients with and without nephropathy; however, this can only be validated by more studies. It should also be noted that the discrepancy between reports may be related to the different ethnicity and geographical backgrounds of the studied populations.
THE STATUS OF THE CCR5 Δ 32 MUTATION IN MULTIPLE SCLEROSIS
Multiple sclerosis is considered a complex immune system-related disorder [28, 42] and the most prevalent symptoms of MS are the loss of myelin and inflammation of the central nervous system [43], but the mechanisms of its pathology have yet to be completely clarified [44]. It has been established that immune cells, including T lymphocytes, NK cells, and dendritic cells, infiltrate and cause inflammation of the central nervous system (CNS) in MS patients [27, 45]. CCL3, 4, and 5 chemokines are the main chemotactic agents that induce recruitment of the immune cells to the CNS via interaction with their corresponded receptor (CCR5) [46]. Based on the important role of CCR5 in recruitment of the immune cells to the CNS in MS patients, we have collected reports regarding the prevalence of CCR5 Δ 32 mutations among MS patients. Our research team evaluated the CCR5 Δ 32 mutation in Iranian patients previously and found that this mutation was not prevalent among southeast Iranian MS patients [47]. Similar results were reported by Bennets et al. [48]. They revealed that the CCR5 Δ 32 mutation is not associated with MS in an Australian population [48]. Additionally, investigators from the USA and Ireland also demonstrated that CCR5 Δ 32 mutations are not related to MS [49, 50]. In parallel with these results, Haase et al. reported that CCR5 Δ 32 mutations are not associated with MS in Germany [51]. Sellebjerg et al. revealed that 22 and 1.5 % of cases with possible onset symptoms of multiple sclerosis carried CCR5 ∆ 32 mutations in heterozygotic (wild-type (wt)/∆32) and homozygotic (∆32/∆32) forms, respectively [22]. Interestingly, they have shown that in cases with clinically definite multiple sclerosis, the frequencies of heterozygotic and homozygotic (∆32/∆32) forms were 21 and 0 %, respectively. They also revealed that the CCR5 ∆ 32 mutation is not related to MS in DRB1 1501-negative and DRB1 1501-positive cases [22]. In a subsequent paper, Sellebjerg et al. also revealed that 1 % of MS patients and 2 % of controls carried CCR5 ∆ 32 mutation in the homozygotic (∆32/∆32) state and that 19 % of MS patients and 22 % of controls carry heterozygotic alleles while 80 % of patients and 76 % of controls carried wild-type CCR5 [52]. Their original results from 2000 demonstrated that the differences were not significant between the study groups [22] and the authors reconfirmed their results by repeating their study in 2002 [53]. However, some publications have demonstrated that the CCR5 Δ 32 mutation may affect MS. For instance, a conflicting report by Shahbazi et al. indicated high a prevalence of this mutation in MS patients from northeast of Iran [54]. Although Shahbazi and his colleagues evaluated patients from the Iranian population, the ethnic background of the subjects differed from our previous studied population. Our study group focused on Fars, while the patients studied by Shahbazi et al. were Turk; hence, the discrepancy may be related to different population genetics. The association of the CCR5 Δ 32 mutation with short patient survival was also reported by Gade and colleagues [55]. A study on HLA-DR4-positive Russian populations revealed that the CCR5 Δ 32 mutation could be associated with MS [56]. D'Angelo et al. reported that the presence of the CCR5 Δ 32 mutation is significantly frequent in MS patients with an expanded disability status scale score [57]. Pulkkinen et al. compared the frequencies of CCR5 genotypes and its relation to CCR5 mRNA in peripheral blood mononuclear cells [58]. In all MS patients, the ∆32/∆32 genotype was found in 6.7 % of patients, while it was present in only 0.8 % of the controls [58]. Interestingly, they reported that the ∆32/∆32 genotype was increased among primary progressive MS patients, in comparison to other MS subtypes and controls [58].
Therefore, it seems that there is no consensus regarding the association of the CCR5 Δ 32 mutation with MS. Once again, the discrepancy in the reports may reflect the differences in the studied populations in terms of genetic background as well as their exposure to environmental factors. Although it has been revealed that CCR5 expression is significantly increased in MS patients [46] it would appear that, in addition to the CCR5 Δ 32 mutation, there are other polymorphisms or haplotypes as well as other genetic and epigenetic factors that may be important for CCR5 expression in MS patients.
THE STATUS OF THE CCR5 Δ 32 MUTATION IN ASTHMA
Asthma is an airway obstructive respiratory disease caused by acute and chronic bronchial inflammation [59]. The main characteristics that are associated with the asthma phenotype are bronchial hyperresponsiveness, increased total serum IgE levels, and infiltration of eosinophils and Th2 lymphocytes [60]. Due to the fact that a hyperactive immune response is seen in asthma [61], it is reasonable to assess the factors that regulate the immune system to determine if they can influence asthma pathogenesis [62]. Previous studies revealed that Th2 lymphocytes infiltrate the inflamed bronchus via responses initiated by CCR5 and its ligands (CCL3, 4, and 5) [23]. Interestingly, increased expression of the chemokines has been reported by our research team (unpublished data); hence, it seems that CCR5 and its related Δ 32 mutation can be associated with asthma. Similar to MS and T2D, our previous studies demonstrated that CCR5 Δ 32 mutations are rare in southeast Iranian asthmatic patients and, interestingly, none of the asthmatic patients that we studied carried the CCR5 Δ 32 mutation [62]. Based on these results, it appears that CCR5 Δ 32 mutations are not related to asthma in the southeastern Iranian population [62].
Similar to these findings, Mitchell and colleagues demonstrated that there were no associations between the CCR5 Δ 32 mutations in atopy or asthma [63]. Szalai et al. were also unable to find the mutation in asthmatic patients [64]. Sandford et al. also reported that the CCR5 Δ 32 mutation was not significantly related to asthma and its severity in the UK population [59]. They revealed that of 87 mild-to-moderate asthma patients, 75 % carried homozygous wild-type, 24 % heterozygous, and 1 % homozygous CCR5 Δ 32 mutations. They also showed that 73 % of fatal or near-fatal asthmatic patients carried homozygous wild-type, 24 % heterozygous, and 3 % homozygous CCR5 Δ 32 mutations [59]. Nagy et al. showed that among 118 asthmatic children, 80.5 % carried the wt allele, 16.1 % heterozygous (∆32/wt), and 3.4 % were homozygous for the CCR5 Δ 32 mutation [65]. They also showed that of 145 non-asthmatic children with atopy, 80.0 % carried CCR5 wt, 17.9 % heterozygous (∆32/wt), and 2.1 % homozygous alleles [65]. Additionally, they have shown that 79.2, 19.1, and 1.7 % of children without atopy or asthma carried CCR5 wt, heterozygous (∆32/wt), and homozygous alleles, respectively [65]. Therefore, it is likely that, similar to our study population, the CCR5 Δ 32 mutation was not associated with atopy and asthma in UK population [65]. Similarly, McGinnis et al. showed that in English patients diagnosed as asthma, 46 (83 %) had CCR5 wt, 17 % carried the heterozygous genotype (∆32/wt), and no patients were homozygous for CCR5 Δ 32 mutations [66]. They also reported that the non-asthmatic group (n = 109) carried 62, 35, and 3 % CCR5 wt, heterozygous (∆32/wt), and homozygous CCR5 Δ 32 mutations, respectively [66]. The authors also revealed that the CCR5 Δ 32 mutation was not associated with asthma in the Germany population [66]. These results were confirmed in a study by Srivastava et al., which was carried out on the British population [67]. They reported that among 77 children asthmatic samples, 70 cases (90.9 %) carried CCR5 wt/wt, 7 (9.1 %) ∆32/wt, and 0 (0 %) were homozygous for the CCR5 Δ 32 mutation [67]. Their study on adult patients emerged with similar results [67]. In contrast to the mentioned studies, Hall et al. identified that there was a negative correlation between the CCR5 Δ 32 mutation and the development of asthma [68]. They proposed that CCR5 Δ 32 mutations are protective against asthma due to the reduced responsiveness to CCL3, CCL4, and CCL5, as a result of decreased CCR5 expression [68].
According to the studies surveyed here, it seems that there is no association between CCR5 Δ 32 mutations with asthma and it cannot be considered as a risk factor in all populations. It may be a candidate for some populations carrying specific genetic backgrounds such as those patients from Northern Europe, an endemic region for the CCR5 Δ 32 mutation.
CONCLUSION
The CCR5 Δ 32 mutation was not associated with MS patients in our studies and those of several other groups. However, there are a few reports regarding its correlation with MS; therefore, it may be concluded that this mutation could be associated with MS, but this needs to be evaluated with more studies in endemic regions, especially the northern region of Europe. From the data of the combined reports on T2D (with and without nephropathy) as well as asthma, it can be concluded that CCR5 Δ 32 mutations cannot be considered as a risk factor for these diseases. Potentially, other genetic and epigenetic factors may lead to an increase in CCR5 expression on the immune cells of T2D patients (both with and without nephropathy) as well as asthma. However, there is a lack of information regarding the presence of other polymorphisms and their roles in regulating CCR5 expression. The discrepancies between the reported studies may be due to differences in the evaluated populations that originated from varying ethnic groups with different genetic backgrounds. CCR5/ligand interactions lead to immune cell survival, activation, cellular adhesion, and motility [11] (Fig. 1). Therefore, it is difficult to reconcile a model in which CCR5 Δ 32 mutations, which appear to downregulate CCR5 expression, could give rise to asthma and T2D which are inflammatory diseases. On the other hand, it seems that MS, which is an autoimmune disease, may be associated with the CCR5 Δ 32 mutation, especially in the populations where the mutation is prevalent (i.e., Northern Europe). In these populations, the expression of chemokines may be perturbed as a result of the mutation and the subsequent downregulation of CCR5. Previous studies revealed that when expression of CCR5 is decreased, the expression levels of CCL3, 4, and 5 will be increased. Based on the fact that CCL3, 4, and 5 can use other receptors, including CCR1 and CCR3, it is possible that overexpression of the chemokines may lead to immune cell activation and migration leading to inflamed CNS in MS patients. Therefore, it seems that evaluating the expression of CXCR1 and CXCR3 as well as CCL3, 4, and 5 should be considered in future studies of MS patients. Finally, due to the fact that chemokines and their receptors form a complex regulatory network, it will be important to study the presence of polymorphisms within the regulatory regions of genes of the inflammatory and anti-inflammatory chemokines and their related receptors before the complicated multigenic aspects of these diseases can be resolved.
References
Chiang, Y.J., H.K. Kole, K. Brown, et al. 2000. Cbl-b regulates the CD28 dependence of T-cell activation. Nature 403: 216–220.
Arababadi M. K., Ahmadabadi B. N., Kennedy D. 2012. Current information on the immunological status of occult hepatitis B infection. Transfusion 52: 1819–1826.
van Eden, W., A. Koets, P. van Kooten, et al. 2003. Immunopotentiating heat shock proteins: negotiators between innate danger and control of autoimmunity. Vaccine 21: 897–901.
Miyara, M., K. Wing, and S. Sakaguchi. 2009. Therapeutic approaches to allergy and autoimmunity based on FoxP3+ regulatory T-cell activation and expansion. J Allergy Clin Immunol 123: 749–755. quiz 756–747.
Al-Abdulhadi, S.A., and M.W. Al-Rabia. 2010. Linkage and haplotype analysis for chemokine receptors clustered on chromosome 3p21.3 and transmitted in family pedigrees with asthma and atopy. Ann Saudi Med 30: 115–122.
Lehner, T. 2002. The role of CCR5 chemokine ligands and antibodies to CCR5 coreceptors in preventing HIV infection. Trends Immunol 23: 347–351.
Ahmadabadi, B.N., G. Hassanshahi, H. Khoramdelazad, et al. 2012. Down-regulation of CCR5 expression on the peripheral blood CD8+ T cells of South-Eastern Iranian patients with chronic hepatitis B infection. Inflammation. doi:10.1007/s10753-012-9528-4.
Song, J.K., M.H. Park, D.Y. Choi, et al. 2012. Deficiency of C-C chemokine receptor 5 suppresses tumor development via inactivation of NF-kappaB and upregulation of IL-1Ra in melanoma model. PLoS One 7: e33747.
Kuipers, H.F., P.J. Biesta, L.J. Montagne, et al. 2008. CC chemokine receptor 5 gene promoter activation by the cyclic AMP response element binding transcription factor. Blood 112: 1610–1619.
Blanpain, C., F. Libert, G. Vassart, et al. 2002. CCR5 and HIV infection. Receptors Channels 8: 19–31.
Sorce, S., R. Myburgh, and K.H. Krause. 2011. The chemokine receptor CCR5 in the central nervous system. Prog Neurobiol 93: 297–311.
Wong, M., S. Uddin, B. Majchrzak, et al. 2001. Rantes activates Jak2 and Jak3 to regulate engagement of multiple signaling pathways in T cells. J Biol Chem 276: 11427–11431.
Arababadi, M.K., A.A. Pourfathollah, A. Jafarzadeh, et al. 2010. Decreased expression of CCR5 on the NK cells in occult HBV infected patients. LabMedicine 41: 735–738.
Jin, Q., L. Agrawal, L. Meyer, et al. 2008. CCR5Delta32 59537-G/A promoter polymorphism is associated with low translational efficiency and the loss of CCR5Delta32 protective effects. J Virol 82: 2418–2426.
Singh, H., R. Sachan, M. Jain, et al. 2008. CCR5-Delta32 polymorphism and susceptibility to cervical cancer: association with early stage of cervical cancer. Oncol Res 17: 87–91.
Nahon, P., A. Sutton, P. Rufat, et al. 2008. Chemokine system polymorphisms, survival and hepatocellular carcinoma occurrence in patients with hepatitis C virus-related cirrhosis. World J Gastroenterol 14: 713–719.
Guerini, F.R., S. Delbue, M. Zanzottera, et al. 2008. Analysis of CCR5, CCR2, SDF1 and RANTES gene polymorphisms in subjects with HIV-related PML and not determined leukoencephalopathy. Biomed Pharmacother 62: 26–30.
Abousaidi, H., R. Vazirinejad, M.K. Arababadi, et al. 2011. Lack of association between chemokine receptor 5 (CCR5) delta32 mutation and pathogenesis of asthma in Iranian patients. South Med J 104: 422–425.
Richardson, M.W., J. Jadlowsky, C.A. Didigu, et al. 2012. Kruppel-like factor 2 modulates CCR5 expression and susceptibility to HIV-1 infection. J Immunol 189: 3815–3821.
Liu, S., C. Kong, J. Wu, et al. 2012. Effect of CCR5-Delta32 heterozygosity on HIV-1 susceptibility: a meta-analysis. PLoS One 7: e35020.
Muntinghe, F.L., S. Gross, S.J. Bakker, et al. 2009. CCR5Delta32 genotype is associated with outcome in type 2 diabetes mellitus. Diabetes Res Clin Pract 86: 140–145.
Sellebjerg, F., H.O. Madsen, C.V. Jensen, et al. 2000. CCR5 delta32, matrix metalloproteinase-9 and disease activity in multiple sclerosis. J Neuroimmunol 102: 98–106.
Bisset, L.R., and P. Schmid-Grendelmeier. 2005. Chemokines and their receptors in the pathogenesis of allergic asthma: progress and perspective. Curr Opin Pulm Med 11: 35–42.
Cookson, W. 1999. The alliance of genes and environment in asthma and allergy. Nature 402: B5–11.
Orihara, K., N. Dil, V. Anaparti, et al. 2011. What's new in asthma pathophysiology and immunopathology? Expert Rev Respir Med 4: 605–629.
Sawcer, S., G. Hellenthal, M. Pirinen, et al. 2011. Genetic risk and a primary role for cell-mediated immune mechanisms in multiple sclerosis. Nature 476: 214–219.
Arababadi, M.K., R. Mosavi, H. Khorramdelazad, et al. 2010. Cytokine patterns after therapy with Avonex(R), Rebif(R), Betaferon(R) and CinnoVex in relapsing-remitting multiple sclerosis in Iranian patients. Biomark Med 4: 755–759.
Arababadi M. K., Mosavi R., Teimori H., et al. 2011. Association of IL-4 polymorphisms with multiple sclerosis in south-eastern Iranian patients. Ann Saudi Med 32: 127–130.
Yaghini N., Mahmoodi M., Asadikaram G., et al. 2012. Genetic variation of IL-12B (+1188 region) is associated with its decreased circulating levels and susceptibility to type 2 diabetes: a study on south-eastern Iranian diabetic patients. Biomark Med 6: 89–95.
Cruz, M., C. Maldonado-Bernal, R. Mondragon-Gonzalez, et al. 2008. Glycine treatment decreases proinflammatory cytokines and increases interferon-gamma in patients with type 2 diabetes. J Endocrinol Invest 31: 694–699.
Yaghini N., Mahmoodi M., Asadikaram G., et al. 2011. Serum levels of Interleukin 10 (IL-10) in patients with type 2 diabetes. Iran Red Cres Med J 13: 752.
Arababadi, M.K., R. Nosratabadi, G. Hassanshahi, et al. 2009. Nephropathic complication of type-2 diabetes is following pattern of autoimmune diseases? Diabetes Res Clin Pract 87: 33–37.
Arababadi, M.K. 2010. Interleukin-4 gene polymorphisms in type 2 diabetic patients with nephropathy. Iran J Kidney Dis 4: 302–306.
Arababadi, M.K., A.A. Pourfathollah, S. Daneshmandi, et al. 2009. Evaluation of relation between IL-4 and IFN-g polymorphisms and type 2 diabetes. Iran J Bas Med Sci 12: 100–104.
Nosratabadi, R., M.K. Arababadi, V.A. Salehabad, et al. 2010. Polymorphisms within exon 9 but not intron 8 of the vitamin D receptor are associated with the nephropathic complication of type-2 diabetes. Int J Immunogenet 37: 1–5.
Arababadi, M.K., N. Naghavi, G. Hassanshahi, et al. 2009. Is CCR5-Delta32 mutation associated with diabetic nephropathy in type 2 diabetes? Ann Saudi Med 29: 413.
Neumeier, M., S. Bauer, H. Bruhl, et al. 2011. Adiponectin stimulates release of CCL2, -3, -4 and -5 while the surface abundance of CCR2 and -5 is simultaneously reduced in primary human monocytes. Cytokine 56: 573–580.
Venza, I., M. Visalli, M. Cucinotta, et al. 2010. Proinflammatory gene expression at chronic periodontitis and peri-implantitis sites in patients with or without type 2 diabetes. J Periodontol 81: 99–108.
Bogdanski, P., D. Pupek-Musialik, J. Dytfeld, et al. 2007. Influence of insulin therapy on expression of chemokine receptor CCR5 and selected inflammatory markers in patients with type 2 diabetes mellitus. Int J Clin Pharmacol Ther 45: 563–567.
Kalev, I., K. Oselin, P. Parlist, et al. 2003. CC-chemokine receptor CCR5-del32 mutation as a modifying pathogenetic factor in type I diabetes. J Diabetes Complications 17: 387–391.
Ahluwalia, T.S., M. Khullar, M. Ahuja, et al. 2009. Common variants of inflammatory cytokine genes are associated with risk of nephropathy in type 2 diabetes among Asian Indians. PLoS One 4: e5168.
Ascherio, A., K.L. Munger, and K.C. Simon. 2010. Vitamin D and multiple sclerosis. Lancet Neurol 9: 599–612.
Teunissen, C.E., J. Killestein, and G. Giovannoni. 2007. Biomarker research in multiple sclerosis: addressing axonal damage and heterogeneity. Biomark Med 1: 111–119.
Glass, C.K., K. Saijo, B. Winner, et al. 2010. Mechanisms underlying inflammation in neurodegeneration. Cell 140: 918–934.
Gandhi, R., A. Laroni, and H.L. Weiner. 2010. Role of the innate immune system in the pathogenesis of multiple sclerosis. J Neuroimmunol 221: 7–14.
Szczucinski, A., and J. Losy. 2007. Chemokines and chemokine receptors in multiple sclerosis. Potential targets for new therapies. Acta Neurol Scand 115: 137–146.
Arababadi, M.K., G. Hassanshahi, H. Azin, et al. 2010. No association between CCR5-Δ 32 mutation and multiple sclerosis in patients of south-eastern of Iran. LabMedicine 41: 31–33.
Bennetts, B.H., S.M. Teutsch, M.M. Buhler, et al. 1997. The CCR5 deletion mutation fails to protect against multiple sclerosis. Hum Immunol 58: 52–59.
Kantarci, O.H., Y. Morales, P.A. Ziemer, et al. 2005. CCR5Delta32 polymorphism effects on CCR5 expression, patterns of immunopathology and disease course in multiple sclerosis. J Neuroimmunol 169: 137–143.
Silversides, J.A., S.V. Heggarty, G.V. McDonnell, et al. 2004. Influence of CCR5 delta32 polymorphism on multiple sclerosis susceptibility and disease course. Mult Scler 10: 149–152.
Haase, C.G., S. Schmidt, and P.M. Faustmann. 2002. Frequencies of the G-protein beta3 subunit C825T polymorphism and the delta 32 mutation of the chemokine receptor-5 in patients with multiple sclerosis. Neurosci Lett 330: 293–295.
Sellebjerg, F., T.B. Kristiansen, P. Wittenhagen, et al. 2007. Chemokine receptor CCR5 in interferon-treated multiple sclerosis. Acta Neurol Scand 115: 413–418.
Sellebjerg, F., G. Giovannoni, A. Hand, et al. 2002. Cerebrospinal fluid levels of nitric oxide metabolites predict response to methylprednisolone treatment in multiple sclerosis and optic neuritis. J Neuroimmunol 125: 198–203.
Shahbazi, M., H. Ebadi, D. Fathi, et al. 2009. CCR5-delta32 allele is associated with the risk of developing multiple sclerosis in the Iranian population. Cell Mol Neurobiol 29: 29.
Gade-Andavolu, R., D.E. Comings, J. MacMurray, et al. 2004. Association of CCR5 delta32 deletion with early death in multiple sclerosis. Genet Med 6: 126–131.
Favorova, O.O., T.V. Andreewski, A.N. Boiko, et al. 2002. The chemokine receptor CCR5 deletion mutation is associated with MS in HLA-DR4-positive Russians. Neurology 59: 1652–1655.
D'Angelo, R., C. Crisafulli, C. Rinaldi, et al. 2011. CCR5Delta32 polymorphism associated with a slower rate disease progression in a cohort of RR-MS Sicilian patients. Mult Scler Int 2011: 153282.
Pulkkinen, K., M. Luomala, H. Kuusisto, et al. 2004. Increase in CCR5 Delta32/Delta32 genotype in multiple sclerosis. Acta Neurol Scand 109: 342–347.
Sandford, A.J., S. Zhu, T.R. Bai, et al. 2001. The role of the C-C chemokine receptor-5 Delta32 polymorphism in asthma and in the production of regulated on activation, normal T cells expressed and secreted. J Allergy Clin Immunol 108: 69–73.
Zietkowski, Z., M.M. Tomasiak, R. Skiepko, et al. 2008. RANTES in exhaled breath condensate of stable and unstable asthma patients. Respir Med 102: 1198–1202.
Moore, K.W., R. de Waal Malefyt, R.L. Coffman, et al. 2001. Interleukin-10 and the interleukin-10 receptor. Annu Rev Immunol 19: 683–765.
Abousaidi H., Vazirinejad R., Arababadi M. K., et al. 2011. Lack of association between chemokine receptor 5 (CCR5) C32 mutation and pathogenesis of Asthma: A Study on Iranian Asthma Patients. South Med J 104: 422–425.
Mitchell, T.J., A.J. Walley, J.E. Pease, et al. 2000. Delta 32 deletion of CCR5 gene and association with asthma or atopy. Lancet 356: 1491–1492.
Szalai, C., A. Bojszko, G. Beko, et al. 2000. Prevalence of CCR5delta32 in allergic diseases. Lancet 355: 66.
Nagy, A., G.T. Kozma, A. Bojszko, et al. 2002. No association between asthma or allergy and the CCR5Delta 32 mutation. Arch Dis Child 86: 426.
McGinnis, R., F. Child, S. Clayton, et al. 2002. Further support for the association of CCR5 allelic variants with asthma susceptibility. Eur J Immunogenet 29: 525–528.
Srivastava, P., P.J. Helms, D. Stewart, et al. 2003. Association of CCR5Delta32 with reduced risk of childhood but not adult asthma. Thorax 58: 222–226.
Hall, I.P., A. Wheatley, G. Christie, et al. 1999. Association of CCR5 delta32 with reduced risk of asthma. Lancet 354: 1264–1265.
Acknowledgments
This project was supported by a grant from the Rafsanjan University of Medical Sciences.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ghorban, K., Dadmanesh, M., Hassanshahi, G. et al. Is the CCR5 Δ 32 Mutation Associated with Immune System-Related Diseases?. Inflammation 36, 633–642 (2013). https://doi.org/10.1007/s10753-012-9585-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-012-9585-8