Abstract
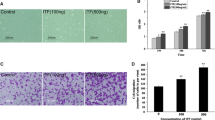
Intestinal barrier dysfunction plays an important role in the pathogenesis of inflammatory bowel disease (IBD). To evaluate the effect of intestinal trefoil factor (ITF) on increased intestinal permeability and its association with tight junction proteins, an in vitro intestinal epithelia barrier model was established with Caco-2 cells and treated with platelet-activating factor (PAF). We found that exposing cells to 0.3 M ITF (30 min before or 30 min after PAF treatment) attenuated the PAF-induced changes in transepithelial electrical resistance and Lucifer yellow flux. A quantitative RT-PCR and western blot analysis revealed that ITF suppressed PAF-induced downregulation of tight junction proteins claudin-1 and ZO-1 expression; furthermore, an abnormal localization and distribution of these proteins was inhibited, as assessed by immunofluorescence staining. These results suggest that ITF decreases mucosal permeability and shows potential as a therapy for treating IBD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Intestinal barrier dysfunction is considered to be the initiating event in the pathogenesis of inflammatory bowel disease (IBD) [1–3]. An increased permeability of the intestinal mucosa barrier allows toxic substances and microorganisms to cross the intestinal wall, thereby inducing an inflammatory response. The intestinal mucosa barrier in IBD is characterized by a significantly increased permeability of the paracellular space [4], which is restricted primarily by the tight junction. The proteins claudin-1 and zona occludens-1 (ZO-1) maintain tight junction integrity and intestinal barrier function. In an animal model in which an epithelial tight junction protein is knocked out, the gene-deficient animals exhibit intestinal pathology changes similar to IBD [5], indicating that abnormal distribution or expression of tight junction proteins in epithelial cells may be involved in IBD pathogenesis. Hence, improving intestinal barrier function is the focus of pathophysiology research regarding IBD and one of the goals of IBD treatment.
The intestinal trefoil factor (ITF) is a member of the trefoil peptide family reported to protect and repair the gastrointestinal mucosa through the maintenance of intestinal epithelial cell integrity and restoration of normal intestinal permeability [6–8], but if ITF has protect and repair effects on the IBD, they are not so well-known. In this study, we characterized the protective effect of ITF on tight junctions at the cellular level. Our findings have provided evidence for the clinical application in treating IBD.
MATERIALS AND METHODS
Cell Culture
To generate the in vitro model of the human intestinal epithelium, Caco-2 cells (American Type Culture Collection, USA) were cultured at 37°C in Dulbecco’s modified Eagle’s medium (DMEM) containing 15% fetal bovine serum in an atmosphere of 5% CO2 and 90% relative humidity. Parental cells were split at a ratio of 1:2 and seeded (5 × 104 cells per square centimeter) into Transwell cell culture inserts (0.4 μm, 6.5 mm, 0.33 cm2 growth surfaces; Corning, USA). Experiments were performed at least 2 weeks postconfluence.
To determine the optimal concentration of PAF (Sigma, USA), we incubated postconfluent monolayers of Caco-2 cells with different concentrations (0, 50, 100, 200 nM) for 24 h. To determine the appropriate duration of treatment, we evaluated Caco-2 monolayers incubated with 100 nM PAF for 0, 2, 4, 8, 12, 24, or 48 h. The effects of ITF were assessed by adding 0.3 M ITF 30 min before or 30 min after PAF (100 nM) treatment and incubating cells for 24 h. The barrier integrity (permeability) and tight junction proteins claudin-1 and ZO-1 were assessed as described as below.
Transepithelial Electrical Resistance Measurements
Caco-2 cells were cultured in Transwell plates until the confluent monolayer achieved a transepithelial electrical resistance (TEER) >300 Ω cm2 (about 15–18 days), demonstrating a tight monolayer. TEER was measured using a voltmeter (Millicell-ERS; Millipore, USA) as described by Hidalgo et al. [9]: TEER (ohms per square centimeter) = (Total resistance − Blank resistance) (ohms) × Area (square centimeter).
Determination of Barrier Integrity by Transport of Paracellular Marker
The integrity of the monolayer barrier was assessed by a widely used and validated technique that measures the apical to basolateral paracellular flux of the fluorescent marker Lucifer yellow (LY, 0.55 kDa). Briefly, 600 μL of fresh phenol-free DMEM was placed into the lower (basolateral) chamber and 100 μL of DMEM containing LY (0.08 M) was placed in the upper (apical) chamber. Aliquots (50 μL) were obtained from the upper and lower chambers at baseline and subsequent time points, and fluorescent signals were quantitated using a fluorescence spectrophotometer (HITACHIF-4500, Japan). The excitation and emission spectra for LY are 427 and 536 nm, respectively. Clearance was calculated using the following formula: \( {\text{Clearance}}\left( {\text{nanoliters per hour per square centimeter}} \right) = {\text{Lab}}/\left( {\left[ {\text{LY}} \right]{\text{a}} \times S} \right), \) where Lab is the apical to basolateral flux of LY (light units per hour), [LY]a is the concentration at baseline (light units per nanoliter), and S is the surface area (0.33 cm2). Controls were included in each experiment.
Quantitative Reverse Transcription-Polymerase Chain Reaction Analysis of Claudin-1 and ZO-1 Expression
The total cellular RNA was extracted with TRIzol one-step extraction and was used as a template for cDNA. Reverse transcription was carried out at 37°C for 15 min and terminated by heating to 85°C for 5 s. Amplification was carried out using an SYBR Green I PCR kit (TaKaRa Biotechnology, Japan) according to the manufacturer’s instructions. Thermal cycling conditions were 95°C for 10 s, followed by 40 cycles of 95°C for 5 s and 60°C for 34 s. To quantify mRNA levels, standard curves were generated for the target genes (claudin-1, ZO-1 gene) and a housekeeping gene (glyceraldehyde 3-phosphate dehydrogenase, GAPDH). Target gene expression was then normalized to that of the housekeeping gene. Primers were obtained from TaKaRa Biotechnology and sequences are shown in Table 1.
Western Blot Analysis of Changes in Claudin-1, ZO-1 Protein Expression
The total protein was extracted with the KGI total protein extraction kit (Nanjing KeyGen Biotech Co., Ltd., China), and proteins were quantified using the BCA method. Equal amounts of protein from each sample (about 50 μg) were separated by SDS-PAGE (claudin-1, 15% gel; ZO-1, 5% gel) at 100 V for 150 min. The proteins were then transferred to the PVDF membrane (200 mA, 2 h). The membranes were washed with Tris-buffered saline (TBS) for 5 min, blocked with skim milk powder for 2 h, washed twice with TBS–Tween (TTBS) for 5 min, and then incubated with polyclonal rabbit antibodies against claudin-1 (1:500 dilution) and ZO-1 (1:200 dilution; Zymed, USA) at 4°C overnight. The next day, membranes were washed three times with TTBS for 5 min and then incubated with horseradish peroxidase-labeled goat anti-rabbit IgG (1:5,000; Santa Cruz, USA) at room temperature for 2 h. After washing three times with TTBS for 5 min, proteins were detected with ECL reagents. After stripping the membrane for 30 min, it was washed with TBS for 5 min, blocked with skim milk powder for 2 h, and hybridized with a mouse anti-β-actin antibody (loading control) and goat anti-mouse antibody (Santa Cruz, USA), followed by ECL detection. An image analysis was then performed.
Immunofluorescent Localization of Claudin-1 and ZO-1
Following the incubation with PAF, with or without ITF, the cells were adhered on a slide, fixed for 10 min with 4% paraformaldehyde, and then permeabilized with 0.5% Triton X-100 for 5 min. Following a brief wash in phosphate-buffered saline (PBS), the fixed cells were incubated with 1% bovine serum albumin for 1 h to reduce non-specific staining. The cell monolayers were incubated with claudin-1 or ZO-1 antibody (1:50 dilution, Zymed, USA) for 1 h at room temperature, and then incubated with FITC-conjugated anti-rabbit IgG (1:100 dilution, Santa Cruz, USA) for 1 h at room temperature. Finally, the slides were washed twice with PBS. A coverslip was mounted on the slide with 10 μL of PBS and glycerol (1:1, v/v), and the coverslip edges were sealed with clear nail polish. The slides were examined under a fluorescence microscope (Olympus BX61, Japan), and the images were examined in a blinded fashion for overall morphology, orientation, and disruption. A tight junction integrity in Caco-2 cells was considered abnormal or injured based on the following microscopic changes: fragmentation, kinking, or loss of cell to cell contact.
Statistical Analysis
The results were expressed as mean ± standard error of the mean (SEM). A one-way analysis of variance was used to compare groups. P < 0.05 was considered significant. All data analyses were conducted with an SPSS 13.0 software package.
RESULTS
Protective Effect of ITF on PAF-Induced Changes in TEER
We tested various concentrations of PAF and found that 100 nM produced the strongest effects on TEER (P < 0.01). Exposure to 100 nM PAF for various durations significantly decreased TEER, with the most substantial decrease observed at 24 h (P < 0.01) (Fig. 1). We, therefore, treated cells with 100 nM of PAF for 24 h in subsequent experiments testing ITF. We found that treating cells with ITF (0.3 M) 30 min before or 30 min after adding PAF (100 nM) significantly increased TEER values (P < 0.05) (Fig. 2).
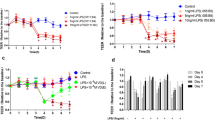
The concentration–course and time–course of TEER induced by PAF in Caco-2 monolayers. a Caco-2 monolayers were incubated with different concentrations of PAF for 24 h. b Caco-2 monolayers were exposed to 100 nM of PAF for different durations. Results were expressed as mean ± SEM (n = 4). ∆ P < 0.05, ∆∆ P < 0.01 vs control.
Effects of ITF on decreased TEER in Caco-2 monolayers induced by PAF. PAF, Caco-2 monolayers were treated with PAF (100 nM) for 24 h; ITF pre, Caco-2 monolayers were treated with ITF (0.3 M) 30 min before adding PAF; ITF post, Caco-2 monolayers were treated with ITF (0.3 M) 30 min after adding PAF. Results were expressed as mean ± SEM (n = 4). ∆ P < 0.05, ∆∆ P < 0.01 vs control; *P < 0.05 vs PAF group.
Effects of ITF on PAF-Induced Paracellular Marker Transport
Lucifer yellow (LY) is a paracellular marker; therefore, the unidirectional flux of LY can be used to determine mucosal permeability. We found that LY clearance was significantly higher in the Caco-2 cell monolayers incubated with 100 nM PAF compared with the control, and reached the peak at 24 h (P < 0.01) (Fig. 3). However, the ITF (0.3 M) added to the cell culture 30 min before or 30 min after adding PAF (100 nM) significantly decreased the clearance of LY (P < 0.05) (Fig. 4).
The concentration–course and time–course of clearance of LY induced by PAF in Caco-2 monolayers. a Caco-2 monolayers were incubated with different concentrations of PAF for 24 h. b Caco-2 monolayers were exposed to 100 nM PAF for different durations. Results were expressed as mean ± SEM (n = 4). ∆ P < 0.05, ∆∆ P < 0.01 vs control.
Effects of ITF on PAF-induced increase of unidirectional flux of LY in Caco-2 monolayers. PAF, Caco-2 monolayers were treated with PAF (100 nM) for 24 h; ITF pre, Caco-2 monolayers were treated with ITF (0.3 M) 30 min before adding PAF. ITF post, Caco-2 monolayers were treated with ITF (0.3 M) 30 min after adding PAF. Results were expressed as mean ± SEM (n = 4). ∆ P < 0.05, ∆∆ P < 0.01 vs control; *P < 0.05 vs PAF group.
Effect of ITF on PAF-Mediated Downregulation of Claudin-1, ZO-1
To determine mRNA levels of claudin-1 and ZO-1, we generated standard curves of these target genes and the internal control GAPDH; correlation coefficients were 0.99, 0.995, and 0.992, respectively, showing good linear relationships. The melting curve analysis showed good primer specificity. Our results demonstrated that claudin-1 and ZO-1 mRNA levels were reduced in cells treated with PAF (P < 0.01). Treatment with 0.3 M ITF for 24 h (added 30 min before or 30 min after 100 nM PAF) attenuated the downregulation of these tight junction proteins (P < 0.01) (Fig. 5).
Effects of PAF and ITF on claudin-1 and ZO-1 mRNA expression evaluated by qRT-PCR. a, b PAF (50–200 nM) downregulated claudin-1 and ZO-1 mRNA expression. c, d ITF attenuated the downregulation of claudin-1 and ZO-1 mRNA expression induced by PAF. PAF, Caco-2 monolayers were treated with PAF (100 nM) for 24 h; ITF pre, Caco-2 monolayers were treated with ITF (0.3 M) 30 min before adding PAF; ITF post, Caco-2 monolayers were treated with ITF (0.3 M) 30 min after adding PAF. Results are expressed as mean ± SEM (n = 4). ∆ P < 0.05, ∆∆ P < 0.01 vs control; *P < 0.05, **P < 0.01 vs PAF group.
Effect of PAF and ITF on Claudin-1, ZO-1 Protein Expression
Claudin-1 function requires serine and threonine residues phosphorylation, which increases its molecular weight from 20 to 25 kDa. Treating Caco-2 cells with PAF did not affect the levels of the 20-kDa claudin-1 protein (P = 0.99), but reduced the level of the 25-kDa claudin-1protein compared with the control (P < 0.01). Similarly, a 24-h treatment with 100 nM of PAF decreased the level of 220-kDa ZO-1 protein compared with the control (P < 0.01). Co-treatment with ITF (added 30 min before or 30 min after 100 nM of PAF) inhibited the PAF-induced downregulation of protein expression, which was consistent with the results of the mRNA analysis (Figs. 6 and 7).
Effects of PAF and ITF on the expression of claudin-1 and ZO-1 evaluated by western blot. a, b PAF (50–200 nM) downregulated claudin-1 and ZO-1 protein expression. c, d ITF attenuated the downregulation of claudin-1 and ZO-1 protein expression induced by PAF. PAF, Caco-2 monolayers were treated with PAF (100 nM) for 24 h; ITF pre, Caco-2 monolayers were treated with ITF (0.3 M) 30 min before adding PAF; ITF post, Caco-2 monolayers were treated with ITF (0.3 M) 30 min after adding PAF. Results are expressed as mean ± SEM (n = 4). ∆ P < 0.05, ∆∆ P < 0.01 vs control; *P < 0.05, **P < 0.01 vs PAF group.
Effect of PAF and ITF on Claudin-1 and ZO-1 Protein Localization and Distribution
Claudin-1 and ZO-1 are distributed primarily near the cell membrane in epithelial cells in untreated Caco-2 cells, which were tightly arranged with smooth edges and showed a typical cobblestone shape. After the treatment with 50 nM of PAF, the cellular edges became serrated and changes were observed at sites of cell to cell contact. Increasing the PAF concentration to 100 nM exacerbated these changes: gaps between cells were apparent, the claudin-1 network pattern was disrupted, and claudin-1 staining was found in the cytoplasm. Further increases in PAF concentration did not increase its effect. Alterations in ZO-1 localization were similar to that of claudin-1. These results suggest that PAF causes abnormal distribution of these tight junction proteins and translocation from the membrane. Treatment with ITF (30 min before or 30 min after PAF was added) attenuated but did not completely prevent the PAF-induced changes in claudin-1 and ZO-1 localization and cell morphology. Pretreatment with ITF produced better effects than posttreatment with ITF (Fig. 8).
Immunofluorescent staining in Caco-2 cell monolayers against claudin-1 (a–d) and ZO-1 (e–h). a, e Untreated. b, f Incubated with PAF (100 nM) for 24 h. c, g Pretreated with ITF (0.3 M) 30 min before PAF (100 nM) was added, then incubated for 24 h. d, h Posttreated with ITF (0.3 M) 30 min after adding PAF (100 nM), then incubated for 24 h.
DISCUSSION
ITF is a member of the trefoil peptide family [10, 11] and was discovered in 1991 [12]. Previous studies demonstrated an important role of ITF in the protection and restoration of the gastrointestinal mucosa. It appears to stimulate cell migration and proliferation, promote epithelial cell reparation, and stabilize the mucus gel [10]. Recent studies report that the functional and structural changes of the apical junctional complexes contribute to ITF-induced modulation of gastrointestinal epithelia. In HT29/B6 and MDCK cells, stable transfection with FLAG-tagged human ITF increases epithelial resistance [13].
Poritz et al. [14] reported that the loss of ZO-1 and increased permeability preceded the development of significant intestinal inflammation in colitis induced by dextran sulfate sodium. Weber’s research [15] showed that claudin-1 and claudin-2 expression is increased in active IBD and may contribute to carcinogenesis. These studies demonstrate that protecting tight junction proteins in the IBD is very important.
Whether ITF can be a potential factor in the treatment of IBD and its mechanisms associated with maintaining intestinal permeability and tight junction proteins function is still unknown. In the present study, we established an in vitro model of the intestinal epithelial barrier with Caco-2 cells and treated with PAF. PAF is a well-recognized mediator of inflammation in intestinal injury [16]. Previous studies show PAF is constitutively expressed at low levels in normal rat intestinal tissue [17], and several intestinal epithelial cell lines synthesize PAF in vitro [18]. Furthermore, both human and rat intestinal epithelial cells [19] and several human intestinal epithelial cell lines [20] express the PAF receptor. At levels lower than those that cause intestinal injury, PAF induces transcription of cytokines in the intestine, suggesting an additional role for protein in regulating intestinal mucosal permeability.
To determine the direct effect of PAF on mucosal permeability and furthermore the protective effect of ITF, TEER and LY flux were detected in this study. We found that exposing cells to 0.3 M ITF attenuated the PAF-induced changes in TEER and Lucifer yellow flux. These results prove that ITF can decrease mucosal permeability. Similarly, Kubes et al. [21] demonstrated that low doses of PAF that did not cause histological injury of the small intestine could increase intestinal permeability to low-molecular weight substances such as 51Cr-EDTA (51 kDa).
The permeability of the intestinal mucosa is restricted primarily by the tight junction, which is regulated by a variety of proteins, (e.g., claudin-1, -2, -3, -4, -7, -15, occludin, ZO-1, ZO-2, ZO-3) [22–24]. A previous study showed the expression of some of these tight junction proteins declined when applied with TNF-α or a cytokine mixture (TNF-α, IFN-γ, IL-1β) as the stimulus [25–27]. We evaluated the expression and localization of claudin-1 and ZO-1 as markers of the increased permeability induced by PAF. Quantitative RT-PCR and western blot analysis revealed that ITF suppressed PAF-induced downregulation of tight junction proteins claudin-1 and ZO-1 expression.
In addition, we evaluate claudin-1 and ZO-1 protein localization using immunofluorescence staining. Claudin-1 and ZO-1 are normally localized on the surface of the cell membrane, forming a network. After exposure to PAF, claudin-1 and ZO-1 translocated beneath the membrane, and fluorescence signals showed a serrated pattern. This result is consistent with the findings of Han and Sappington [26, 27]. Although pretreatment or posttreatment with ITF did not completely prevent these changes, it did attenuate the abnormal localization and distribution of claudin-1 and ZO-1 protein induced by PAF.
To investigate the molecular mechanisms by which ITF regulates monolayer barrier integrity and paracellular permeability, much work should be done, but the present study provided evidence showing that ITF induces recovery of tight junction protein changes, which contributed to the ITF-mediated stabilization and maintenance of intestinal epithelial barrier function. These results may provide new insight into the protective functions of ITF on epithelial cells and demonstrate its potential for the treatment of IBD.
References
McGuckin, M.A., R. Eri, L.A. Simms, T.H. Florin, and G. Radford-Smith. 2009. Intestinal barrier dysfunction in inflammatory bowel diseases. Inflammatory Bowel Diseases 15: 100–113.
Xavier, R.J., and D.K. Podolsky. 2007. Unravelling the pathogenesis of inflammatory bowel disease. Nature 448: 427–434.
Buhner, S., C. Buning, J. Genschel, K. Kling, D.A. HerrmannD, I. Kuechler, S. Krueger, H.H. Schmidt, and H. Lochs. 2006. Genetic basis for increased intestinal permeability in families with Crohn’s disease: role of CARD15 3020insC mutation? Gut 55: 342–347.
Su, L., L. Shen, D.R. Clayburgh, S.C. Nalle, E.A. Sullivan, J.B. Meddings, C. Abraham, and J.R. Turner. 2009. Targeted epithelial tight junction dysfunction causes immune activation and contributes to development of experimental colitis. Gastroenterology 136: 551–563.
Hermiston, M.L., and J.I. Gordon. 1995. Inflammatory bowel disease and adenomas in mice expressing a dominant negative N-cadherin. Science 270: 1203–1207.
Renes, I.B., M. Verburg, D.J. Van Nispen, H.A. Büller, J. Dekker, and A.W. Einerhand. 2002. Distict epithelial responses in experimental colitis:implications for ion uptake and mucosal protection. American Journal of Physiology. Gastrointestinal and Liver Physiology 283: G169–G179.
Chen, L.P., B.H. Zhang, Y. Li, G.R. Mai, and Z.X. Liu. 2003. The effect and significance of intestinal trefoil factor IL-8 and MDA for neonatal rat model for hypoxia-induced intestinal injury. Chinese Journal of Perinatal Medicine 36: 306–309.
Li, J., L.F. Xu, M. Sun, Q. Li, H. Gao, and W.G. Jiang. 2006. Protective effects of recombinant intestinal trefoil factor against intestinal injuries induced by endotoxin in young rats. Chinese Journal of Contemporary Pediatrics 8: 425–428.
Hidalgo, I.J., T.J. Raub, and R.T. Borchardt. 1989. Characterization of the human colon carcinoma cell line (Caco-2) as a model system for intestinal epithelial permeability. Gastroenterology 96: 736–749.
Thim, L. 1997. Trefoil peptides: From structure to function. Cellular and Molecular Life Sciences 53: 888–903.
Thim, L. 1994. Trefoil peptides: A new family of gastrointestinal molecules. Digestion 55: 353–360.
Suemori, S., K. Lynch-Devaney, and D.K. Podolsky. 1991. Identification and characterization of rat intestinal trefoil factor: Tissue and cell-specific. Proceedings of the National Academy of Sciences of the United States of America 88: 11017–11021.
zum Büschenfelde Meyer, D., R. Tauber, and O. Huber. 2006. TFF3-peptide increases transepithelial resistance in epithelial cells by modulating claudin-1 and -2 expression. Peptides 27: 3383–3390.
Poritz, L.S., K.I. Garver, C. Green, L. Fitzpatrick, F. Ruggiero, and W.A. Koltun. 2007. Loss of the tight junction protein ZO-1 in dextran sulfate sodium induced colitis. The Journal of Surgical Research 140: 12–19.
Weber, C.R., S.C. Nalle, M. Tretiakova, D.T. Rubin, and J.R. Turner. 2008. Claudin-1 and claudin-2 expression is elevated in inflammatory bowel disease and may contribute to early neoplastic transformation. Laboratory Investigation 88: 1110–1120.
Hsueh, W., M.S. Caplan, X. Sun, X. Tan, W. MacKendrick, and F. Gonzalez-Crussi. 1994. Platelet-activating factor, tumor necrosis factor, hypoxia and necrotizing enterocolitis. Acta Paediatrica. Supplement 396: 11–17.
Qu, X., L. Huang, T. Burthart, S.E. Crawford, M.S. Caplan, and W. Hsueh. 1996. Endotoxin induces PAF production in the rat ileum: quantitation of tissue PAF by an improved method. Prostaglandins 51: 249–262.
Guerrant, R.L., G.D. Fang, N.M. Thielman, and M.C. Fonteles. 1994. Role of platelet activating factor in the intestinal epithelial secretory and chinese hamster ovary cell cytoskeletal responses to cholera toxin. Proceedings of the National Academy of Sciences of the United States of America 91: 9655–9658.
Kotelevets, L., V. Noë, E. Bruyneel, E. Myssiakine, E. Chastre, M. Mareel, and C. Gespach. 1998. Inhibition by platelet-activating factor of src- and hepatocyte growth factor-dependent invasiveness of intestinal and kidney epithelial cells. Phosphatidylinositol 3'-kinase is a critical mediator of tumor invasion. Journal of Biological Chemistry 273: 14138–14145.
Merendino, N., M.B. Dwinell, N. Varki, L. Eckmann, and M.F. Kagnoff. 1999. Human intestinal epithelial cells express receptors for platelet-activating factor. The American Journal of Physiology 277: G810–G818.
Kubes, P., K.E. Arfors, and D.N. Granger. 1991. Platelet-activating factor-induced mucosal dysfunction: role of oxidants and granulocytes. The American Journal of Physiology 260: G965–G971.
Huber, J.D., K.A. Witt, S. Hom, R.D. Egleton, K.S. Mark, and T.P. Davis. 2001. Inflammatory pain alters blood-brain barrier permeability and tight junctional protein expression. American Journal of Physiology. Heart and Circulatory Physiology 280: H1241–H1248.
Luabeya, M.K., L.M. Dallasta, C.L. Achim, C.D. Pauza, and R.L. Hamilton. 2000. Blood-brain barrier disruption in simian immunodeficiency virus encephalitis. Neuropathology and Applied Neurobiology 26: 454–462.
Song, L., S. Ge, and J.S. Pachter. 2007. Caveolin-1 regulates expression of junction- associated proteins in brain microvascular endothelial cells. Blood 109: 1515–1523.
McCarthy, K.M., I.B. Skare, M.C. Stankewich, M. Furuse, S. Tsukita, R.A. Rogers, R.D. Lynch, and E.E. Schneeberger. 1996. Occludin is a functional component of the tight junction. Journal of Cell Science 109: 2287–2298.
Han, X., M.P. Fink, and R.L. Delude. 2003. Proinflammatory cytokines cause NO-dependent and -independent changes in expression and localization of tight junction proteins in intestinal epithelial cells. Shock 19: 229–237.
Sappington, P.L., X. Han, R. Yang, R.L. Delude, and M.P. Fink. 2003. Ethyl pyruvate ameliorates intestinal epithelial barrier dysfunction in endotoxemic mice and immunostimulated caco-2 enterocytic monolayers. The Journal of Pharmacology and Experimental Therapeutics 304: 464–476.
Acknowledgments
This work was supported by a research fund for the doctoral program from the National Ministry of Education (RFDP, 20092104110010), Educational Commission of Liaoning Province (L2010624), Doctorial Start Fund of Liaoning Province (20101147), and Science and Technology Planning Project of Shenyang (F10-205-1-45).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xu, Lf., Teng, X., Guo, J. et al. Protective Effect of Intestinal Trefoil Factor on Injury of Intestinal Epithelial Tight Junction Induced by Platelet Activating Factor. Inflammation 35, 308–315 (2012). https://doi.org/10.1007/s10753-011-9320-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-011-9320-x