Abstract
Heart failure (HF) with preserved ejection fraction (HFpEF) has emerged as an important public health issue in recent years. It represents the most common type of HF in ambulatory setting, and it has been recognized as a different entity from the reduced ejection fraction (EF) form. In HFpEF, continuous growing attention has been focused on the role of the left atrium (LA) in preserving good ventricular function and asymptomatic condition of the patient since the very first stages of diastolic dysfunction (DD). Non-invasive and complete echocardiographic evaluation of diastolic phase cannot exempt from accurately analyzed LA size, mostly LA volume, and its function, in particular LA myocardial deformation by speckle tracking echocardiography (STE). This review examines the expanding role of the LA in DD and HFpEF and the importance of its complete assessment in various settings, from diagnosis to correlation with major cardiovascular events.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Background
In recent years, greater attention has been focused on patients with typical heart failure (HF) signs and symptoms but with normal values of left ventricular (LV) ejection fraction (EF) usually >50% [1]. This subset represents the half of subjects that access the emergency room and even more in ambulatory setting [2]. Prevalence of HF with preserved EF (HFpEF) is increasing. Morbidity and mortality are still elevated [3], and differently from HF with reduced EF (HFrEF), outcomes have not improved in last decades, mainly because of under diagnosis and lacks of effective therapies [4].
The pathophysiological mechanism that leads from asymptomatic diastolic dysfunction (DD) to HFpEF is still not completely clear. Despite a maintained cardiac output, left-sided cardiac chambers go through important remodeling which alters cardiomyocytes and interstitial ultrastructure [5] and then filling function [6]. In particular, a key role in preserving diastolic phase and preventing the onset of HF symptoms seems to be played by the left atrium (LA). Echocardiography allows to accurately and non-invasively evaluate LA dimensions and function. This could improve correct diagnosis, therapy and prognostication in patients with DD and HFpEF.
The purpose of this review is to highlight the importance of LA function in patients suffering from DD and HFpEF and to describe the usable methods for its assessment. We base our paper on the research on PubMed literature, using mainly the following terms: “left atrial function”, “left atrium and diastolic dysfunction”, “left atrial strain and diastolic dysfunction”, “left atrium and heart failure preserved ejection fraction”, “left atrium and diastolic heart failure”, “left atrial strain and heart failure preserved ejection fraction”, “left atrial strain and diastolic heart failure”, “left atrium heart failure symptoms”, and “left atrium heart failure prognosis”. We did not decide to pose a time limit in this research, selecting the most appropriate and innovative papers.
Left atrium in diastolic dysfunction
The LA is considered a reservoir and a conduit of blood, placed between pulmonary and systemic circulation, and ensures correct ventricular filling without raising pulmonary venous pressure. The LA cavity is in direct contact with the LV cavity when the mitral valve opens, during diastolic phase, so it is exposed to LV pressures during every diastole. For this reason, increase in LA size and alteration in its function could represent a picture of average LV pressure history and may indicate an index of DD [7, 8] differently from E/E′ ratio that can be considered a snapshot of pressures at the time of the evaluation [9]. In patients with normal LV filling pressure at rest, it has been demonstrated how LA volume index can predict rise in filling pressures during exercise echocardiography, supporting the hypothesis of a cumulative effect [10]. Therefore, LA volume has been defined as the “glycosylated hemoglobin of diastolic dysfunction”.
Evaluation of left atrium size
Transthoracic echocardiogram represents the most used method for assessing LA dimensions. The most commonly used linear dimension is LA anteroposterior measurement that could be obtained in M-mode or, preferably, two-dimensions (2D) in parasternal long-axis view. Despite its high reproducibility, anteroposterior dimension is considered inaccurate because it might not be representative of the real LA size [11] and should never be assessed as the only LA dimensional parameter. The LA area, measured in apical two- or four-chamber view, may be obtained but barely used in common practice. LA volume, in particular, LA volume index (that is, LA volume indexed to BSA, body surface area), is the preferable method for its evaluation because it relies on minor geometric assumptions and permits to detect enlargements along different space axes. The American Society of Echocardiography recommends the assessment of LA volumes in two- and four-chamber apical views by Simpson’s method, with an upper normal revised cut-off value of 34 ml/m2 [12]. In patients with raised LV filling pressures, LA dimensions tend to increase, as already mentioned. While in grade I DD, LA volume is still normal, the atrial chamber dilates in higher grades. It has been widely demonstrated how LA volume expresses the intensity and the chronicity of DD [13] and proportionally increases with increasing severity of DD as defined by invasive hemodynamic study [14]. LA macroscopic remodeling is fundamental because it guarantees the best ventricular filling despite elevated wall stiffness and high diastolic pressures, until very advanced stages of dysfunction. On the other hand, the LA preserves pulmonary capillary circulation from hemodynamic overload [15] for a long time and, consequently, preserves the patients from symptoms’ onset. Exertional dyspnoea is the typical clinical presentation in subjects with DD; between all echocardiographic variables, LA volume index has been shown to be an independent predictor of exercise capacity [16].
Assessment of left atrium function
LA physiology during every cardiac cycle consists of three different phases that modulate LV filling. The reservoir phase starts with mitral valve closure: the LA fills up also thanks to the movement of atrial floor towards the heart apex. As LA pressure falls, its volume increases facilitating the passage of blood from the pulmonary circulation. After mitral valve opening, during early LV filling, the energy stored in LA walls is transferred to the LV and, jointly with the suction effect exerted from the ventricle itself, allows blood flow to the LV and the reduction of LA volume. At the same time, a direct flow from pulmonary veins through the LA into the LV occurs (conduit phase). In the last phase (atrial systole), the LA contracts determining the motion of mitral valve plan towards the ventricular apex and the additional transfer of blood into the ventricular chamber. LA function can be evaluated by measuring chamber volumes during cardiac cycle in different time points that reflect the mentioned phases (at end-systole, before mitral valve opening, that is maximal volume; at the onset of P wave on ECG, that is pre-atrial contraction volume; at end-diastole, before mitral valve closure, that is minimal volume) and calculating, with specific formulas, its reservoir, conduit and pump fractions [17]. In addition to volumetric evaluation, Doppler echocardiography has been used for the same purpose. Peak A wave by transmitral pulsed-wave (PW) Doppler is considered an index of LA function [18], but it is influenced by loading conditions and patient’s age [19]. Also, tissue Doppler imaging (TDI) A′ wave has been correlated to atrial function in numerous studies, proportionally with the grade of DD [20, 21]. However, this approach does not allow to evaluate regional LA function.
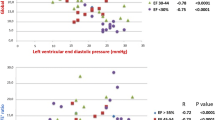
Speckle tracking echocardiography (STE)-derived LA strain currently constitutes the best method to assess atrial function. The software was born for the application to the LV, to analyze its longitudinal, radial and circumferential deformation, but STE has demonstrated great feasibility and reproducibility also when applied to the LA chamber [22]. It represents a direct measurement of intrinsic LA myocardial deformation, relatively independent of loading conditions and geometric assumptions [23]. After the acquisition of atrial 2D images in apical four and two chambers, strain curves are obtained by an off-line semi-automated analysis using specific software. In the current ASE/EAE consensus [24], two different techniques have been proposed to quantify atrial deformation by STE. The most widely applied method is performed using QRS onset as a reference point. According to this measurement, LA strain is composed of two peaks that trace atrial activity during cardiac cycle. During reservoir phase, the LA fills and stretches so strain increase, reaching a positive peak at the end of chamber filling: at this point, it is possible to measure peak atrial longitudinal strain (PALS); after mitral valve opening, the LA quickly empties and its volume falls so strain decreases up to a plateau, in diastasis phase. Then, in the short period before atrial contraction, only in patients with sinus rhythm, LA strain increases again up to a second positive peak, that is peak atrial contraction strain (PACS) [22] (Fig. 1). The other modality of quantification has been proposed by Saraiva et al. and considers P wave as a reference point: it measures a first negative peak atrial longitudinal strain curve (atrial systole, called ε negative), a second positive peak atrial strain curve (corresponding to reservoir function, ε positive) and their sum [25]. It has been widely demonstrated how LA function, assessed by STE, deteriorates even without chamber dilation [26], and then, a reduction in strain value suggests the presence of a microstructural remodeling that appears long before macroscopic one. Once extensive fibrosis has developed, the remodeling process might become irreversible so it is fundamental to detect it very early in order to intervene therapeutically. LA strain has been correlated with the degree of atrial fibrosis evaluated by Masson trichrome staining on an LA tissue sample [27]. Cardiac magnetic resonance (CMR) with late Gadolinium enhancement (CMR) allows to evaluate the presence of myocardial inflammation and fibrosis thanks to the relative accumulation of Gadolinium as the result of a slower washout and an increased extracellular volume [28]. The detection of fibrosis with CMR is challenging for the LA mostly because of its thin walls; however, experts suggest that new 3D CMR sequences, despite being time consuming and technically difficult, have obtained better results [29]. Interesting data have emerged on the inverse correlation between LA strain and the amount of LA fibrosis detected by 3D CMR [30], but they require further evaluation and validation. DD is characterized by altered LV relaxation and reduced compliance that lead to an increase in LV end-diastolic pressure, mean LA pressure and pulmonary capillary wedge pressure (PCWP), all referred to as LV filling pressures [31]. PALS represents a great tool in the non-invasive evaluation of these pressures (Fig. 2), with the greatest diagnostic accuracy among all other echocardiographic parameters [32–34]. Moreover, LA strain can be used to estimate LA stiffness, both invasively, with PCWP, obtained by heart catheterization, and non-invasively, with E/E′ ratio, got by PW Doppler and TDI. A low atrial function is an independent predictor of estimated metabolic equivalents (METs) in patients with DD [35].
Assessment of peak atrial longitudinal strain (PALS) at the end of reservoir phase and peak atrial contraction strain (PACS) before the atrial contraction. The dashed curve represents the average atrial longitudinal strain during the cardiac cycle [51]
Left atrial strain and ventricular filling pressure: differences in pulsed-wave Doppler of mitral flow velocities, tissue Doppler imaging and strain between a patient with normal filling pressures (above) and one with increased ones (below) [24]
Left atrium role in HFpEF
HFpEF may represent the evolution of a chronic DD, but completely understanding its pathophysiology still represents a work in progress. In fact, while DD has a high prevalence in the community and increases with age, the main part of these patients does not successively evolve towards HF with typical signs and symptoms [36]. Comorbidities, as age, hypertension, diabetes and coronary artery disease, play an important role in HFpEF [37]. Making an accurate diagnosis of HFpEF remains a challenging topic too. For a long period of time, in HF patients, attention has been focused on LV structure, dimensions and function, relegating the LA to a marginal position. In recent years, however, the atrial chamber has acquired increasing importance and its fundamental role has been shown both in modulating ventricular filling and in providing diagnostic and prognostic clues.
Since the very first stages of LV filling impairment, the LA tries to implement a sort of compensating action in order to support the dysfunctional ventricle chamber. Over time, nevertheless, the remodeling process profoundly alters the atrium, so much that compensatory mechanisms fail and a real “LA failure” appears [38]. This is the moment in which HFpEF becomes evident.
The LA is frequently dilated in HF patients if compared with controls, despite a preserved EF [39], and its size tends to increase proportionately with LV mass [40] and stiffness [41]. Atrial chamber volume is more useful in detecting patients with HFpEF than TDI E′-related parameters [42], and subjects with bigger LA show higher risk of developing HF [43]. Clearly, finding an enlarged LA can be secondary to other causes such as mitral regurgitation [44], atrial fibrillation [45], anemia [46], age and obesity, but in subjects with sinus rhythm and without mitral valve diseases, it is mostly related to elevated filling pressures.
On the other hand, in front of a normal volume, it cannot be excluded that the LA function has already begun to deteriorate. In DD, raised LV filling pressures cause a progressive increase in atrial chamber wall, stretch atrial cardiomyocytes, determine natriuretic peptide secretion and lead to LA dysfunction [47]. LA strain shows diagnostic accuracy in this setting. HFpEF patients have lower LA reservoir, conduit and pump function than healthy controls, and strain decreases independently from LA size or history of atrial fibrillation (AF) [48] (Fig. 3). Moreover, PALS is able to distinguish between subjects with DD and those with HFpEF; LA stiffness is typically elevated in patients with DD and even more in HFpEF [49]. LA strain is an important correlate of symptoms’ appearance [50]. Atrial dysfunction has been pointed out, in particular, in patients with new-onset dyspnoea; therefore, it is mandatory to conduct a non-invasive evaluation of strain in this setting in order to guarantee a correct differential diagnosis [51].
Left atrial strain in diastolic dysfunction and heart failure with preserved ejection fraction: comparison of peak atrial longitudinal strain (PALS) between a hypertensive subject (left) and a patient accessing the emergency room because of worsening dyspnoea with following diagnosis of HFpEF (right)
Atrial chamber beyond HF diagnosis
Heart failure severity, recurrence and mortality
LA strain has shown a good correlation with functional capacity during effort [52], a decreased peak oxygen consumption (peak VO2) at cardiopulmonary exercise testing [53], NHYA class [50] and NT-proBNP plasma levels [54]. Then, atrial dysfunction could represent a real marker of severity [48]. One of the main goals of HF therapy is to prevent recurrence of symptoms and hospital admissions. The discharge from a HF hospitalization is followed by a readmission within a month in almost 24% of cases [55], and the readmission rate in patients with preserved EF is not less than those with reduced EF forms [56]. Subjects already diagnosed with HF show different clinical courses depending on the LA reshaping: higher volumes and non-reversible remodeling with specific treatments correlate with major recurrence of HF during follow-up [57]. LA volume index is capable to predict hospital admission similarly to LV EF [58]. Also, LA-impaired function independently predicts re-hospitalization and might be useful for HF risk stratification [59]. A recent large meta-analysis demonstrated a strong association between LA enlargement and HF mortality, also after adjustment for EF, PW Doppler pattern, symptom status and age [60]; nevertheless, strain during reservoir phase has appeared to be superior to any other echocardiographic parameter in predicting cardiovascular death [61] also after adjustment for atrial fibrillation, LA volume and LV mass [53].
Major cardiovascular events
In addition to hospitalization and mortality, HF patients are exposed to a high risk of other cardiovascular events, mainly AF, stroke, transient ischemic attack (TIA) and myocardial infarction (MI). LA volume index is a more robust marker of patients’ outcome over and above LA area or diameter [62]. In general, the higher the LA volume, the poorer the prognosis [13, 38, 63], and atrial size should always be considered into the risk stratification of the patient [64]. However, the LA represents an additional prognostic tool in this setting, as strongly demonstrated in an important prospective study, extending previous results [61] (Fig. 4). AF is the most common consequence of LA remodeling: reactive deposition of collagen fibers in the interstitium causes massive wall fibrosis [65], with consequent alterations in normal electrical conduction [66], and then, increasing progressively, determines evolution to permanent form. Assessment of the grade of fibrosis by Gadolinium late enhancement CMR has high costs and side effects [67]. As mentioned before, an inverse relationship has been assessed between the grade of atrial fibrosis detected by 3D CMR and LA strain, so this could be a promising tool that requires further investigations, for a non-invasive and rapid evaluation [30]. Consequently to the onset of AF, these patients have high risk to develop a stroke. PALS has been used to predict atrial stasis [68] and is typically reduced in subjects with history of ischemic events, being independently associated with stroke [69]. Lastly, atrial function evaluated by STE is an important predictor of AF recurrence both after cardioversion [70] and ablation [71, 72].
Left atrial strain and prognosis: Kaplan–Meier event-free survival curves in patients with different values of global PALS [51]
Limitations and future perspectives
Assessment of LA function by STE could represent the missing added value for a correct evaluation of patients with DD and HFpEF. Limitations include the lack of dedicated software for the analysis of atrial strain and the presence on market of software supplied by vendors that use different analysis algorithms and may create biases. Moreover, LA shape could be difficult to obtain if the acoustic view of the patient is suboptimal and signal components arising from structures placed around LA may contaminate the feasibility of the analysis. However, application of STE analysis is continuously growing in different systemic fields and heart disease. LA strain could be included in diagnostic algorithm to ensure a correct diagnosis both in DD (Fig. 5) and HFpEF (Fig. 6), in addition to the current standard echocardiographic indexes. The promising results of LA strain obtained in DD and HFpEF should be expanded for diagnostic, therapeutic and prognostic aims. Numerous studies and trials regarding HFpEF therapy and drug efficacy are still ongoing. Precise target values of PALS might help in the assessment of the efficacy of a pharmacological strategy in reducing high filling pressures and in reversing the adverse remodeling process. In prognostication field, extension of previous promising studies regarding the correlation between major cardiovascular events and LA strain will rise accuracy of patient management.
Algorithm for the echocardiographic prediction of elevated left ventricular filling pressures (modified from Nagueh et al. [31])
Conclusion
The LA has shown to play a major role in patients from DD to HFpEF. Shifting the focus from the LV, it can be understood how the LA is not a passive chamber but it is capable to guarantee a correct ventricular diastolic filling also in advanced stage of dysfunction and, at the same time, to protect pulmonary capillary circulation from raised pressures. In order to carry out all these functions, the LA goes through an important remodeling until its wall structure is so altered that it starts to lose function and typical HF symptoms appear. Assessment of atrial size and, even more, myocardial deformation by STE allows a complete evaluation of patients in many steps, from diagnosis to prognostication, risk assessment and prediction of major events. Despite a great improvement in HFrEF outcome, thanks to target therapeutic strategies, no treatment has been shown to reduce morbidity and mortality in patients with HFpEF [73]. It is now clear how preserving a correct LA function represents a goal in these subjects and both pharmacological and non-pharmacological therapies to invert chamber remodeling should be investigated.
References
Paulus WJ, Tschope C, Sanderson JE, Rusconi C, Flachskampf FA, Rademakers FE, Marino P, Smiseth OA, De Keulenaer G, Leite-Moreira AF, Borbely A, Edes I, Handoko ML, Heymans S, Pezzali N, Pieske B, Dickstein K, Fraser AG, Brutsaert DL (2007) How to diagnose diastolic heart failure: a consensus statement on the diagnosis of heart failure with normal left ventricular ejection fraction by the Heart Failure and Echocardiography Associations of the European Society of Cardiology. Eur Heart J 28(20):2539–2550. doi:10.1093/eurheartj/ehm037
Dhingra A, Garg A, Kaur S, Chopra S, Batra JS, Pandey A, Chaanine AH, Agarwal SK (2014) Epidemiology of heart failure with preserved ejection fraction. Curr Feart Fail Rep 11(4):354–365. doi:10.1007/s11897-014-0223-7
Owan TE, Hodge DO, Herges RM, Jacobsen SJ, Roger VL, Redfield MM (2006) Trends in prevalence and outcome of heart failure with preserved ejection fraction. N Engl J Med 355(3):251–259. doi:10.1056/NEJMoa052256
Komajda M, Lam CS (2014) Heart failure with preserved ejection fraction: a clinical dilemma. Eur Heart J 35(16):1022–1032. doi:10.1093/eurheartj/ehu067
van Heerebeek L, Borbely A, Niessen HW, Bronzwaer JG, van der Velden J, Stienen GJ, Linke WA, Laarman GJ, Paulus WJ (2006) Myocardial structure and function differ in systolic and diastolic heart failure. Circulation 113(16):1966–1973. doi:10.1161/CIRCULATIONAHA.105.587519
Zile MR, Brutsaert DL (2002) New concepts in diastolic dysfunction and diastolic heart failure: part II: causal mechanisms and treatment. Circulation 105(12):1503–1508
Douglas PS (2003) The left atrium: a biomarker of chronic diastolic dysfunction and cardiovascular disease risk. J Am Coll Cardiol 42(7):1206–1207
Yamada H, Klein AL (2010) Diastology 2010: clinical approach to diastolic heart failure. J Echocardiogr 8(3):65–79. doi:10.1007/s12574-010-0055-8
Nagueh SF, Mikati I, Kopelen HA, Middleton KJ, Quiñones MA, Zoghbi WA (1998) Doppler estimation of left ventricular filling pressure in sinus tachycardia. A new application of tissue Doppler imaging. Circulation 98(16):1644–1650
Hammoudi N, Achkar M, Laveau F, Boubrit L, Djebbar M, Allali Y, Komajda M, Isnard R (2014) Left atrial volume predicts abnormal exercise left ventricular filling pressure. Eur J Heart Fail 16(10):1089–1095. doi:10.1002/ejhf.131
Wade MR, Chandraratna PA, Reid CL, Lin SL, Rahimtoola SH (1987) Accuracy of nondirected and directed M-mode echocardiography as an estimate of left atrial size. Am Jf Cardiol 60(14):1208–1211
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L, Flachskampf FA, Foster E, Goldstein SA, Kuznetsova T, Lancellotti P, Muraru D, Picard MH, Rietzschel ER, Rudski L, Spencer KT, Tsang W, Voigt JU (2015) Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr 28(1):1–39 e14. doi:10.1016/j.echo.2014.10.003
Tsang TS, Barnes ME, Gersh BJ, Bailey KR, Seward JB (2002) Left atrial volume as a morphophysiologic expression of left ventricular diastolic dysfunction and relation to cardiovascular risk burden. Am J Cardiol 90(12):1284–1289
Matsuda M, Matsuda Y (1996) Mechanism of left atrial enlargement related to ventricular diastolic impairment in hypertension. Clin Cardiol 19(12):954–959
Lancellotti P, Henri C (2014) The left atrium: an old ‘barometer’ which can reveal great secrets. Eur J Heart Fail 16(10):1047–1048. doi:10.1002/ejhf.155
Ratanasit N, Karaketklang K, Chirakarnjanakorn S, Krittayaphong R, Jakrapanichakul D (2014) Left atrial volume as an independent predictor of exercise capacity in patients with isolated diastolic dysfunction presented with exertional dyspnea. Cardiovasc Ultrasound 12:19. doi:10.1186/1476-7120-12-19
Blume GG, McLeod CJ, Barnes ME, Seward JB, Pellikka PA, Bastiansen PM, Tsang TS (2011) Left atrial function: physiology, assessment, and clinical implications. Eur J Echocardiogr 12(6):421–430. doi:10.1093/ejechocard/jeq175
Vasan RS, Larson MG, Levy D, Galderisi M, Wolf PA, Benjamin EJ, National Heart L, Blood Institute NIoH (2003) Doppler transmitral flow indexes and risk of atrial fibrillation (the Framingham Heart Study). Am J Cardiol 91(9):1079–1083
Choong CY, Herrmann HC, Weyman AE, Fifer MA (1987) Preload dependence of Doppler-derived indexes of left ventricular diastolic function in humans. J Am Coll Cardiol 10(4):800–808
Hesse B, Schuele SU, Thamilasaran M, Thomas J, Rodriguez L (2004) A rapid method to quantify left atrial contractile function: Doppler tissue imaging of the mitral annulus during atrial systole. Eur J Echocardiogr 5(1):86–92
Gulel O, Yuksel S, Soylu K, Kaplan O, Yilmaz O, Kahraman H, Sahin M (2009) Evaluation of left atrial functions by color tissue Doppler imaging in adults with body mass indexes ≥30 kg/m2 versus those <30 kg/m2. Int J Cardiovasc Imaging 25(4):371–377. doi:10.1007/s10554-008-9403-4
Cameli M, Caputo M, Mondillo S, Ballo P, Palmerini E, Lisi M, Marino E, Galderisi M (2009) Feasibility and reference values of left atrial longitudinal strain imaging by two-dimensional speckle tracking. Cardiovasc Ultrasound 7:6. doi:10.1186/1476-7120-7-6
Zhang Q, Yip GW, Yu CM (2008) Approaching regional left atrial function by tissue Doppler velocity and strain imaging. Europace 10(Suppl 3). doi:10.1093/europace/eun237
Mor-Avi V, Lang RM, Badano LP, Belohlavek M, Cardim NM, Derumeaux G, Galderisi M, Marwick T, Nagueh SF, Sengupta PP, Sicari R, Smiseth OA, Smulevitz B, Takeuchi M, Thomas JD, Vannan M, Voigt JU, Zamorano JL (2011) Current and evolving echocardiographic techniques for the quantitative evaluation of cardiac mechanics: ASE/EAE consensus statement on methodology and indications endorsed by the Japanese Society of Echocardiography. Eur J Echocardiogr 12(3):167–205. doi:10.1093/ejechocard/jer021
Saraiva RM, Demirkol S, Buakhamsri A, Greenberg N, Popović ZB, Thomas JD, Klein AL (2010) Left atrial strain measured by two-dimensional speckle tracking represents a new tool to evaluate left atrial function. J Am Soc Echocardiogr 23(2):172–180. doi:10.1016/j.echo.2009.11.003
Mondillo S, Cameli M, Caputo ML, Lisi M, Palmerini E, Padeletti M, Ballo P (2011) Early detection of left atrial strain abnormalities by speckle-tracking in hypertensive and diabetic patients with normal left atrial size. J Am Soc Echocardiogr 24(8):898–908. doi:10.1016/j.echo.2011.04.014
Cameli M, Lisi M, Righini FM, Massoni A, Natali BM, Focardi M, Tacchini D, Geyer A, Curci V, Di Tommaso C, Lisi G, Maccherini M, Chiavarelli M, Massetti M, Tanganelli P, Mondillo S (2013) Usefulness of atrial deformation analysis to predict left atrial fibrosis and endocardial thickness in patients undergoing mitral valve operations for severe mitral regurgitation secondary to mitral valve prolapse. Am J Cardiol 111(4):595–601. doi:10.1016/j.amjcard.2012.10.049
Salemi VM, Rochitte CE, Shiozaki AA, Andrade JM, Parga JR, de Ávila LF, Benvenuti LA, Cestari IN, Picard MH, Kim RJ, Mady C (2011) Late gadolinium enhancement magnetic resonance imaging in the diagnosis and prognosis of endomyocardial fibrosis patients. Circ Cardiovasc Imaging 4(3):304–311. doi:10.1161/CIRCIMAGING.110.950675
Donal E, Lip GY, Galderisi M, Goette A, Shah D, Marwan M, Lederlin M, Mondillo S, Edvardsen T, Sitges M, Grapsa J, Garbi M, Senior R, Gimelli A, Potpara TS, Van Gelder IC, Gorenek B, Mabo P, Lancellotti P, Kuck KH, Popescu BA, Hindricks G, Habib G, Cardim NM, Cosyns B, Delgado V, Haugaa KH, Muraru D, Nieman K, Boriani G, Cohen A (2016) EACVI/EHRA Expert Consensus Document on the role of multi-modality imaging for the evaluation of patients with atrial fibrillation. Eur Heart J Cardiovasc Imaging 17(4):355–383. doi:10.1093/ehjci/jev354
Kuppahally SS, Akoum N, Burgon NS, Badger TJ, Kholmovski EG, Vijayakumar S, Rao SN, Blauer J, Fish EN, Dibella EV, Macleod RS, McGann C, Litwin SE, Marrouche NF (2010) Left atrial strain and strain rate in patients with paroxysmal and persistent atrial fibrillation: relationship to left atrial structural remodeling detected by delayed-enhancement MRI. Circ Cardiovasc Imaging 3(3):231–239. doi:10.1161/CIRCIMAGING.109.865683
Nagueh SF, Smiseth OA, Appleton CP, Byrd BF III, Dokainish H, Edvardsen T, Flachskampf FA, Gillebert TC, Klein AL, Lancellotti P, Marino P, Oh JK, Popescu BA, Waggoner A (2016) Recommendations for the evaluation of left ventricular diastolic function by echocardiography: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr 29(4):277–314. doi:10.1016/j.echo.2016.01.011
Cameli M, Mandoli GE, Loiacono F, Dini FL, Henein M, Mondillo S (2015) Left atrial strain: a new parameter for assessment of left ventricular filling pressure. Heart Fail Rev. doi:10.1007/s10741-015-9520-9
Cameli M, Sparla S, Losito M, Righini FM, Menci D, Lisi M, D'Ascenzi F, Focardi M, Favilli R, Pierli C, Fineschi M, Mondillo S (2015) Correlation of left atrial strain and Doppler measurements with invasive measurement of left ventricular end-diastolic pressure in patients stratified for different values of ejection fraction. Echocardiography 33(3):398–405. doi:10.1111/echo.13094
Cameli M, Lisi M, Mondillo S, Padeletti M, Ballo P, Tsioulpas C, Bernazzali S, Maccherini M (2010) Left atrial longitudinal strain by speckle tracking echocardiography correlates well with left ventricular filling pressures in patients with heart failure. Cardiovasc ultrasound 8:14. doi:10.1186/1476-7120-8-14
Kusunose K, Motoki H, Popovic ZB, Thomas JD, Klein AL, Marwick TH (2012) Independent association of left atrial function with exercise capacity in patients with preserved ejection fraction. Heart 98(17):1311–1317. doi:10.1136/heartjnl-2012-302007
Abhayaratna WP, Marwick TH, Smith WT, Becker NG (2006) Characteristics of left ventricular diastolic dysfunction in the community: an echocardiographic survey. Heart 92(9):1259–1264. doi:10.1136/hrt.2005.080150
Kane GC, Karon BL, Mahoney DW, Redfield MM, Roger VL, Burnett JC Jr, Jacobsen SJ, Rodeheffer RJ (2011) Progression of left ventricular diastolic dysfunction and risk of heart failure. JAMA 306(8):856–863. doi:10.1001/jama.2011.1201
Rossi A, Gheorghiade M, Triposkiadis F, Solomon SD, Pieske B, Butler J (2014) Left atrium in heart failure with preserved ejection fraction: structure, function, and significance. Circ Heart Fail 7(6):1042–1049. doi:10.1161/CIRCHEARTFAILURE.114.001276
Rossi A, Cicoira M, Florea VG, Golia G, Florea ND, Khan AA, Murray ST, Nguyen JT, O'Callaghan P, Anand IS, Coats A, Zardini P, Vassanelli C, Henein M (2006) Chronic heart failure with preserved left ventricular ejection fraction: diagnostic and prognostic value of left atrial size. Int J Cardiol 110(3):386–392. doi:10.1016/j.ijcard.2005.08.049
Gerdts E, Oikarinen L, Palmieri V, Otterstad JE, Wachtell K, Boman K, Dahlof B, Devereux RB, Losartan Intervention For Endpoint Reduction in Hypertension S (2002) Correlates of left atrial size in hypertensive patients with left ventricular hypertrophy: the Losartan Intervention For Endpoint Reduction in Hypertension (LIFE) Study. Hypertension 39(3):739–743
Briguori C, Betocchi S, Losi MA, Manganelli F, Piscione F, Pace L, Boccalatte M, Gottilla R, Salvatore M, Chiariello M (1998) Noninvasive evaluation of left ventricular diastolic function in hypertrophic cardiomyopathy. Am J Cardiol 81(2):180–187
Yoshida C, Nakao S, Goda A, Naito Y, Matsumoto M, Otsuka M, Shimoshikiryo M, Eguchi A, Lee-Kawabata M, Tsujino T, Masuyama T (2009) Value of assessment of left atrial volume and diameter in patients with heart failure but with normal left ventricular ejection fraction and mitral flow velocity pattern. Eur J Echocardiogr 10(2):278–281. doi:10.1093/ejechocard/jen234
Gottdiener JS, Kitzman DW, Aurigemma GP, Arnold AM, Manolio TA (2006) Left atrial volume, geometry, and function in systolic and diastolic heart failure of persons > or =65 years of age (the cardiovascular health study). Am J Cardiol 97(1):83–89. doi:10.1016/j.amjcard.2005.07.126
Rossi A, Golia G, Gasparini G, Prioli MA, Anselmi M, Zardini P (1999) Left atrial filling volume can be used to reliably estimate the regurgitant volume in mitral regurgitation. J Am Coll Cardiol 33(1):212–217
Sanfilippo AJ, Abascal VM, Sheehan M, Oertel LB, Harrigan P, Hughes RA, Weyman AE (1990) Atrial enlargement as a consequence of atrial fibrillation. A prospective echocardiographic study. Circulation 82(3):792–797
Hammoudi N, Charbonnier M, Levy P, Djebbar M, Stankovic Stojanovic K, Ederhy S, Girot R, Cohen A, Isnard R, Lionnet F (2015) Left atrial volume is not an index of left ventricular diastolic dysfunction in patients with sickle cell anaemia. Arch Cardiovasc Dis 108(3):156–162. doi:10.1016/j.acvd.2014.09.010
Hoit BD, Shao Y, Gabel M, Walsh RA (1995) Left atrial mechanical and biochemical adaptation to pacing induced heart failure. Cardiovasc Res 29(4):469–474
Santos AB, Kraigher-Krainer E, Gupta DK, Claggett B, Zile MR, Pieske B, Voors AA, Lefkowitz M, Bransford T, Shi V, Packer M, McMurray JJ, Shah AM, Solomon SD, Investigators P (2014) Impaired left atrial function in heart failure with preserved ejection fraction. Eur J Heart Fail 16(10):1096–1103. doi:10.1002/ejhf.147
Kurt M, Wang J, Torre-Amione G, Nagueh SF (2009) Left atrial function in diastolic heart failure. Circ Cardiovasc Imaging 2(1):10–15. doi:10.1161/CIRCIMAGING.108.813071
Rosca M, Popescu BA, Beladan CC, Calin A, Muraru D, Popa EC, Lancellotti P, Enache R, Coman IM, Jurcut R, Ghionea M, Ginghina C (2010) Left atrial dysfunction as a correlate of heart failure symptoms in hypertrophic cardiomyopathy. J Am Soc Echocardiogr 23(10):1090–1098. doi:10.1016/j.echo.2010.07.016
Sanchis L, Gabrielli L, Andrea R, Falces C, Duchateau N, Perez-Villa F, Bijnens B, Sitges M (2015) Left atrial dysfunction relates to symptom onset in patients with heart failure and preserved left ventricular ejection fraction. Eur Heart J Cardiov Imaging 16(1):62–67. doi:10.1093/ehjci/jeu165
Morris DA, Gailani M, Vaz Pérez A, Blaschke F, Dietz R, Haverkamp W, Ozcelik C (2011) Left atrial systolic and diastolic dysfunction in heart failure with normal left ventricular ejection fraction. J Am Soc Echocardiogr 24(6):651–662. doi:10.1016/j.echo.2011.02.004
Freed BH, Daruwalla V, Cheng JY, Aguilar FG, Beussink L, Choi A, Klein DA, Dixon D, Baldridge A, Rasmussen-Torvik LJ, Maganti K, Shah SJ (2016) Prognostic utility and clinical significance of cardiac mechanics in heart failure with preserved ejection fraction: importance of left atrial strain. Circ Cardiovasc Imaging. 9(3). doi: 10.1161/CIRCIMAGING.115.003754.
Kurt M, Tanboga IH, Aksakal E, Kaya A, Isik T, Ekinci M, Bilen E (2012) Relation of left ventricular end-diastolic pressure and N-terminal pro-brain natriuretic peptide level with left atrial deformation parameters. Eur Heart J Cardiov Imaging 13(6):524–530. doi:10.1093/ejechocard/jer283
Desai AS, Stevenson LW (2012) Rehospitalization for heart failure: predict or prevent? Circulation 126(4):501–506. doi:10.1161/CIRCULATIONAHA.112.125435
Bhatia RS, Tu JV, Lee DS, Austin PC, Fang J, Haouzi A, Gong Y, Liu PP (2006) Outcome of heart failure with preserved ejection fraction in a population-based study. N Engl J Med 355(3):260–269. doi:10.1056/NEJMoa051530
Yamaguchi K, Yoshitomi H, Ito S, Ito S, Adachi T, Sato H, Watanabe N, Kodani N, Sugamori T, Endo A, Takahashi N, Tanabe K (2014) Left atrial remodeling and recurrence of congestive heart failure in patients initially diagnosed with heart failure. Echocardiography 31(8):936–940. doi:10.1111/echo.12497
Ristow B, Ali S, Whooley MA, Schiller NB (2008) Usefulness of left atrial volume index to predict heart failure hospitalization and mortality in ambulatory patients with coronary heart disease and comparison to left ventricular ejection fraction (from the Heart and Soul Study). Am J Cardiol 102(1):70–76. doi:10.1016/j.amjcard.2008.02.099
Welles CC, Ku IA, Kwan DM, Whooley MA, Schiller NB, Turakhia MP (2012) Left atrial function predicts heart failure hospitalization in subjects with preserved ejection fraction and coronary heart disease: longitudinal data from the Heart and Soul Study. J Am Coll Cardiol 59(7):673–680. doi:10.1016/j.jacc.2011.11.012
Rossi A, Temporelli PL, Quintana M, Dini FL, Ghio S, Hillis GS, Klein AL, Marsan NA, Prior DL, Yu CM, Poppe KK, Doughty RN, Whalley GA, Me RGEHFC (2009) Independent relationship of left atrial size and mortality in patients with heart failure: an individual patient meta-analysis of longitudinal data (MeRGE Heart Failure). Eur J Heart Fail 11(10):929–936. doi:10.1093/eurjhf/hfp112
Cameli M, Lisi M, Focardi M, Reccia R, Natali BM, Sparla S, Mondillo S (2012) Left atrial deformation analysis by speckle tracking echocardiography for prediction of cardiovascular outcomes. Am J Cardiol 110(2):264–269. doi:10.1016/j.amjcard.2012.03.022
Tsang TS, Abhayaratna WP, Barnes ME, Miyasaka Y, Gersh BJ, Bailey KR, Cha SS, Seward JB (2006) Prediction of cardiovascular outcomes with left atrial size: is volume superior to area or diameter? J Am Coll Cardiol 47(5):1018–1023. doi:10.1016/j.jacc.2005.08.077
Tamura H, Watanabe T, Nishiyama S, Sasaki S, Arimoto T, Takahashi H, Shishido T, Miyashita T, Miyamoto T, Nitobe J, Hirono O, Kubota I (2011) Increased left atrial volume index predicts a poor prognosis in patients with heart failure. J Card Fail 17(3):210–216. doi:10.1016/j.cardfail.2010.10.006
Hoit BD (2014) Left atrial size and function: role in prognosis. J Am Coll Cardiol 63(6):493–505. doi:10.1016/j.jacc.2013.10.055
Burstein B, Nattel S (2008) Atrial fibrosis: mechanisms and clinical relevance in atrial fibrillation. J Am Coll Cardiol 51(8):802–809. doi:10.1016/j.jacc.2007.09.064
Nattel S, Burstein B, Dobrev D (2008) Atrial remodeling and atrial fibrillation: mechanisms and implications. Circulation Arrhythm Electrophysiol 1(1):62–73. doi:10.1161/CIRCEP.107.754564
Grobner T (2006) Gadolinium—a specific trigger for the development of nephrogenic fibrosing dermopathy and nephrogenic systemic fibrosis? Nephrol Dial Transplant 4:1104–1108. doi:10.1093/ndt/gfk062
Providencia R, Faustino A, Ferreira MJ, Goncalves L, Trigo J, Botelho A, Barra S, Boveda S (2013) Evaluation of left atrial deformation to predict left atrial stasis in patients with non-valvular atrial fibrillation—a pilot-study. Cardiovasc Ultrasound 11:44. doi:10.1186/1476-7120-11-44
Shih JY, Tsai WC, Huang YY, Liu YW, Lin CC, Huang YS, Tsai LM, Lin LJ (2011) Association of decreased left atrial strain and strain rate with stroke in chronic atrial fibrillation. J Am Soc Echocardiogr 24(5):513–519. doi:10.1016/j.echo.2011.01.016
Shaikh AY, Maan A, Khan UA, Aurigemma GP, Hill JC, Kane JL, Tighe DA, Mick E, McManus DD (2012) Speckle echocardiographic left atrial strain and stiffness index as predictors of maintenance of sinus rhythm after cardioversion for atrial fibrillation: a prospective study. Cardiovasc ultrasound 10:48. doi:10.1186/1476-7120-10-48
Motoki H, Negishi K, Kusunose K, Popovic ZB, Bhargava M, Wazni OM, Saliba WI, Chung MK, Marwick TH, Klein AL (2014) Global left atrial strain in the prediction of sinus rhythm maintenance after catheter ablation for atrial fibrillation. J Am Soc Echocardiogr 27(11):1184–1192. doi:10.1016/j.echo.2014.08.017
Sarvari SI, Haugaa KH, Stokke TM, Ansari HZ, Leren IS, Hegbom F, Smiseth OA, Edvardsen T (2015) Strain echocardiographic assessment of left atrial function predicts recurrence of atrial fibrillation. Eur Heart J Cardiov Imaging. doi:10.1093/ehjci/jev185
McMurray JJ, Adamopoulos S, Anker SD, Auricchio A, Bohm M, Dickstein K, Falk V, Filippatos G, Fonseca C, Gomez-Sanchez MA, Jaarsma T, Kober L, Lip GY, Maggioni AP, Parkhomenko A, Pieske BM, Popescu BA, Ronnevik PK, Rutten FH, Schwitter J, Seferovic P, Stepinska J, Trindade PT, Voors AA, Zannad F, Zeiher A, Guidelines ESCCfP (2012) ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure 2012: the Task Force for the Diagnosis and Treatment of Acute and Chronic Heart Failure 2012 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association (HFA) of the ESC. Eur Heart J 33(14):1787–1847. doi:10.1093/eurheartj/ehs104
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Cameli, M., Mandoli, G.E. & Mondillo, S. Left atrium: the last bulwark before overt heart failure. Heart Fail Rev 22, 123–131 (2017). https://doi.org/10.1007/s10741-016-9589-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10741-016-9589-9