Abstract
Sirtuins (SIRTs) are NAD+-dependent enzymes that catalyze deacylation of protein lysine residues. In mammals, seven sirtuins have been identified, SIRT1–7. SIRT3–5 are mainly or exclusively localized within mitochondria and mainly participate in the regulation of energy metabolic pathways. Since mitochondrial ATP regeneration is inevitably linked to the maintenance of cardiac pump function, it is not surprising that recent studies revealed a role for mitochondrial sirtuins in the regulation of myocardial energetics and function. In addition, mitochondrial sirtuins modulate the extent of myocardial ischemia reperfusion injury and the development of cardiac hypertrophy and failure. Thus, targeting mitochondrial sirtuins has been proposed as a novel approach to improve myocardial mitochondrial energetics, which is frequently impaired in cardiac disease and considered an important underlying cause contributing to several cardiac pathologies, including myocardial ischemia reperfusion injury and heart failure. In the current review, we present and discuss the available literature on mitochondrial sirtuins and their potential roles in cardiac physiology and disease.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The heart is highly dependent on continuous delivery of ATP to maintain contractile function. 95 % of cardiomyocyte ATP regeneration stems from oxidative metabolism of fatty acids and carbohydrates within mitochondria, with minor contributions from ketone bodies, amino acids, and other substrates, depending on their availability in the blood serum [1]. Due to the large amount of myocardial ATP turnover (≈6 kg per day) and the necessity of metabolic flexibility to adapt to acute and chronic changes in energy demand and serum energy substrate levels, cardiac energetics is the subject of intense regulation by a number of different mechanisms. These mechanisms include hormonal regulation, posttranslational mechanisms, intracellular signaling, transcriptional regulation by transcription factors and transcriptional coactivators, and functional modulation and structural reorganization of chromatin, among others [1, 2].
A recently discovered class of regulators of energy metabolism that receives increasing attention is the sirtuin family of NAD+-dependent deacylases [3]. The founding member of the sirtuin family, Saccharomyces cerevisiae Sir2, is a histone deacetylase that mediates life span extension by calorie restriction in S. cerevisiae, C. elegans, and D. melanogaster [4–7]. Seven mammalian orthologs have been described, SIRT1–7, and SIRT3–5 appear to be mainly or even exclusively located within mitochondria. Protein deacylation by sirtuins requires NAD+, which is converted to nicotinamide (NAM) and 2′-O-Acyl-ADP-ribose during the enzymatic reaction. Besides the classical deacetylation reaction that is catalyzed by several sirtuins, a number of other posttranslational modifications (or lysine deacylations) have been identified that are catalyzed by sirtuins, including demalonylation, desuccinylation, deglutarylation, and delipoylation [8–11]. Since sirtuin function is essentially dependent on the NAD+/NADH ratio, it is believed that this family of proteins may serve as sensors of the cellular energy status. This may be particularly important within mitochondria, which host a high number of acylated proteins and contain high levels of NAD+ and NADH [12, 13].
Mitochondrial dysfunction contributes to a number of cardiac pathologies, including pathological hypertrophy, diabetic cardiomyopathy, ischemia reperfusion (IR) injury, and heart failure [14–16]. Despite intense investigation, the underlying mechanisms of mitochondrial dysfunction in cardiac pathologies remain incompletely understood, and the development of therapeutics to improve mitochondrial function turned out to be challenging. In the following article, we will present and discuss the available literature on mitochondrial sirtuins and their role in cardiac physiology and disease.
SIRT3 in cardiac physiology and disease
SIRT3 is the most well-characterized mitochondrial sirtuin to date, which catalyzes the classical sirtuin deacetylation reaction. Using quantitative mass spectrometry, Hebert et al. [17] detected a vast number (~400) of mitochondrial acetyl sites increasing more than twofold in the absence of SIRT3. Bioinformatic analysis of protein networks and biological processes identified an enrichment of acetylated proteins in major mitochondrial processes, including fatty acid metabolism, tricarboxylic acid (TCA) cycle activity, and electron transport. Among these, a number of enzymes have been confirmed to be deacetylated by SIRT3, including isocitrate dehydrogenase 2, glutamate dehydrogenase, complex I (Ndufa9 subunit), and long-chain acyl-CoA dehydrogenase (LCAD) [18–22]. Compatible with predicted and proven metabolic targets of SIRT3, functional studies showed increased mitochondrial respiration rates in HIB1B brown adipocytes overexpressing SIRT3 [23]. Conversely, SIRT3−/− mice exhibit decreased hepatic fatty acid oxidation rates, hepatic ATP production, LCAD activity, OXPHOS complex I–III activity, and ATP levels in kidney and liver [10, 12, 18, 24, 25]. Besides effects on energy metabolism, the mitochondrial antioxidant enzyme manganese superoxide dismutase 2 (MnSOD or SOD2) has also been identified as a SIRT3 target [26, 27]. SIRT3 deacetylates several lysine residues of MnSOD, thereby increasing MnSOD activity and detoxification of superoxide radicals [26, 27]. Thus, it is likely that SIRT3 serves to increase oxidative ATP regeneration by coordinated activation of mitochondrial metabolic pathways, and to increase mitochondrial ROS detoxification.
SIRT3 is highly expressed in the heart [20, 23]. Rates of fatty acid oxidation, glucose oxidation, oxygen consumption, mitochondrial respiration rates, ATP levels, ATP synthesis, and activities of OXPHOS complexes were decreased in hearts of SIRT3−/− mice, accompanied by increased acetylation of numerous proteins of the fatty acid oxidation spiral, TCA cycle, and OXPHOS chain [18, 28]. Based on studies in other tissues and cells and the assumption that deacetylation of SIRT3 generally increases enzymatic activity of its target proteins, these metabolic alterations may suggest that SIRT3 is required to maintain oxidative metabolism in the heart, and that increased acetylation of various metabolic enzymes due to the lack of SIRT3 activity may downregulate oxidative metabolism. This conclusion needs to be drawn carefully though since many proteins are potential SIRT3 targets but the functional effect of SIRT3-mediated deacetylation remains to be tested experimentally for many of them. In addition, although some studies investigated specific lysine residues by site-directed mutagenesis and demonstrated the functional consequence for enzyme activity, most proteins contain several lysine acetylation sites, but not all acetylation sites have been tested for their functional impact on the enzyme activity [18, 19]. In fact, increased acetylation of LCAD in SIRT3−/− tissue has been reported to be increased or decreased [19, 29].
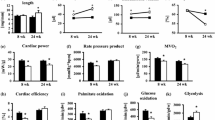
The above-mentioned myocardial metabolic alterations in SIRT3−/− mice are associated with a mild cardiac dysfunction in ex vivo perfused hearts at early ages, which may not yet be readily detectable in vivo by echocardiography due to neurohumoral compensatory mechanisms [28, 30]. When SIRT3−/− mice age, cardiac dysfunction is more pronounced and also detectable by echocardiography [28]. When subjecting SIRT3−/− mice to a chronic increase in energy demand by transverse aortic constriction, the development of cardiac dysfunction is accelerated compared to WT mice, supporting the conclusion that compromised energy substrate utilization may be causally involved in the development of contractile defects in SIRT3−/− mice [28]. SIRT3 may serve as redox-sensitive rheostat that regulates ATP-generating metabolic pathways by coordinated changes in lysine acetylation of various energy metabolic enzymes. Changes in myocardial energy demand would transiently alter the myocardial NAD+/NADH ratio, and SIRT3 may serve to translate these changes into appropriate changes in protein acetylation to synchronize ATP regeneration with ATP demand. Such changes in energy demand may include physical exercise or physiological changes in blood pressure. NAD+ levels also oscillate in a circadian fashion in many cell types to synchronize oxidative metabolic pathways with the 24-h fasting and feeding cycle [31]. Thus, it can be speculated that SIRT3 may even be involved in the synchronization of myocardial energetics with changes in physical activity during day and night times.
A number of studies suggest that SIRT3 may play a role in the development of cardiac hypertrophy and heart failure. Mice lacking SIRT3 develop spontaneous cardiac hypertrophy [28, 32]. In addition, SIRT3−/− mice show exacerbated cardiac hypertrophy following transverse aortic constriction or treatment with hypertrophy agonists such as phenylephrine, isoproterenol, or angiotensin II, accompanied by increased cardiac fibrosis [28, 30, 32, 33]. Furthermore, agonist-induced cardiac hypertrophy and fibrosis can be blocked by overexpression or activation of SIRT3, suggesting that SIRT3 is needed to prevent stress-induced cardiac hypertrophy [32, 34]. A number of mechanisms may be responsible for exacerbation and inhibition of cardiac hypertrophy by SIRT3 deficiency and overexpression, respectively. One obvious mechanism may be energy depletion due to the impairment of metabolic substrate oxidation, resulting in energy depletion and the inability to adapt to increased energy demands [18, 28]. Another mechanism may include attenuation of the ROS-sensitive mitogen-activated protein kinase (MAPK)/extracellular-signal regulated kinase (ERK) pathway and phosphatidylinositol-4,5-bisphosphate 3-kinase (PI3K)/Akt pathways by SIRT3, which are known to play a major role in the development of cardiac hypertrophy [32, 35–38]. Activation and nuclear translocation of forkhead box protein 3a (Foxo3a) into the nucleus and subsequently enhanced expression of MnSOD and catalase may reduce ROS and may thus attenuate signaling of the above-mentioned pathways [32]. Furthermore, SIRT3 may protect from cardiac hypertrophy by activating AMP-activated protein kinase (AMPK). AMPK upregulates catabolic ATP-regenerating pathways in the heart, such as glycolysis and fatty acid oxidation, and simultaneously inhibits anabolic ATP-consuming pathways [39]. AMPK is also capable of inhibiting mTOR, thereby decreasing protein synthesis and inhibiting hypertrophic growth, whereas cardiomyocyte-specific deletion of the AMPK upstream kinase, liver kinase B1 (LKB1), decreases AMPK activity and induces cardiac hypertrophy and dysfunction [40–43]. Pillai et al. [30] demonstrated that SIRT3 can interact with and deacetylate LKB1 in the heart, resulting in the activation of LKB1 and AMPK. Activation of AMPK by exogenous supplementation of NAD+ rescued the heart from ATP depletion and blocked the activation of pro-hypertrophic Akt signaling [30]. Finally, SIRT3−/− but not SIRT3-overexpressing mice develop age-associated cardiac fibrosis, likely due to impaired deacetylation and thus inhibition of glycogen synthase kinase 3β (GSK3β) and subsequent induction of profibrotic transforming growth factor β1 (TGF-β1) signaling [34].
The dependence of SIRT3 on the NAD+/NADH ratio may determine the function of SIRT3 during hypertrophy and heart failure. The NAD+/NADH ratio seems to be increased during compensated cardiac hypertrophy, which should increase SIRT3 activity and may potentially even contribute to induction of SIRT3 in these hearts [28, 44]. This adaptation is likely beneficial and may reflect a feedback mechanism to increase and maintain high rates of ATP synthesis in order to adapt to increased energy demands. In contrast, overactivation of the NAD+-consuming DNA repair enzyme poly(ADP-ribose)-polymerase 1 (PARP-1) may lead to increased consumption and thus depletion of NAD+ during decompensated hypertrophy and heart failure [45]. Indeed, lysine acetylation is increased in human failing hearts, even accompanied by reduced SIRT3 expression [45, 46]. Another attractive hypothesis for decreased NAD+ levels and decreased SIRT3 activity in heart failure may be drawn from the study published by Karamanlidis et al. [47] who generated a mouse model of mitochondrial dysfunction by inactivation of the Ndufs4 gene, resulting in defective complex I activity and heart failure in response to pressure overload stress. Decreased NADH oxidation by complex I resulted in a decreased NAD+/NADH ratio and thus impaired SIRT3 activity, and supplementation with the NAD+ precursor nicotinamide mononucleotide (NMN) normalized the NAD+/NADH ratio, the protein hyperacetylation, and the SIRT3-mediated increase in mPTP sensitivity [47]. Therefore, it may be concluded that a preexisting mitochondrial dysfunction, in this case complex I dysfunction, may lead to a relative decrease in NAD+ depletion, thereby impairing SIRT3 activity and further exacerbating mitochondrial dysfunction. Whatever may be the cause of NAD+ depletion, the resulting impairment in SIRT3 activity and/or reduced SIRT3 expression may exacerbate mitochondrial dysfunction and thus accelerate the development of cardiac failure. Indeed, several studies demonstrated increased hypertrophy, accelerated development of cardiac dysfunction, and decreased survival of SIRT3−/− mice following transverse aortic constriction [28, 32, 33]. Furthermore, exogenous application of NAD+ was capable of maintaining intracellular NAD+ levels and of blocking agonist-induced cardiac hypertrophy, and honokiol treatment, which increases expression and activity of SIRT3, blocked the agonist-induced and pressure overload-induced cardiac hypertrophic response in mice [34]. Thus, prevention of NAD+ depletion during development of heart failure deserves to be explored as a potentially novel and clinically applicable therapeutic strategy [30].
SIRT3 may also modulate the extent of myocardial IR injury. In the Langendorff model, seven-month-old mice with heterozygous deletion of SIRT3 (SIRT3+/−) showed impaired recovery of cardiac function and larger infarct size following 25 min of ischemia [48]. Interestingly, recovery from IR injury in seven-month-old SIRT3+/− hearts was similar as in 18-month-old wild-type hearts [48]. Similarly, the extent of increased mitochondrial protein acetylation was similar in seven-month-old SIRT3+/− and 18-month-old wild-type hearts, suggesting that myocardial SIRT3 activity is similar in aged wild-type mice and younger SIRT3+/− mice [48]. In contrast, recovery of contractile function following IR and myocardial infarct size following LAD ligation in vivo were not different between eight-week-old homozygous SIRT3−/− and wild-type mice [49]. These findings may suggest that compensatory mechanisms may attenuate IR injury in homozygous SIRT3−/− mice, or that SIRT3 deficiency may actually not increase IR injury. However, the rather contradictory results of the above-mentioned studies may be compatible when considering the age difference in the animals and the mechanism by which SIRT3 may modulate IR injury, as follows.
SIRT3 has been shown to deacetylate the regulatory component of the mPTP, cyclophilin D (CypD), on lysine 166 [33]. Increased acetylation of cyclophilin D in the absence of SIRT3 is believed to promote interaction of cyclophilin D with the mPTP pore, thereby increasing the sensitivity for mPTP opening [33]. Opening of the mPTP is an essential determinant of myocardial IR injury, and mice lacking SIRT3 exhibit an age-dependent increase in mitochondrial swelling, associated with increased mPTP opening [33]. Bochaton et al. [50] recently showed that SIRT3 overexpression prevented cyclophilin D acetylation, limited mPTP opening, and reduced cell death in H9C2 cells subjected to hypoxia–reoxygenation. They also showed that cardiac ischemic postconditioning could not reduce infarct size and cyclophilin D acetylation in SIRT3−/− mice [50]. These studies support the conclusion that impairment in SIRT3 may increase the sensitivity for mPTP opening and thereby modulate myocardial IR injury. Of interest, a number of studies reported of increased sensitivity of cardiac mitochondria for mPTP opening in aged animals, and in parallel the susceptibility of the heart to damage from IR injury also increases with age [51–58]. In addition, numerous studies demonstrated additional mitochondrial alterations in aged hearts, including structural derangements, increased ROS generation and oxidative damage, and impairment in mitochondrial function [59, 60]. Among others, increased ROS generation is also a powerful trigger for mPTP opening [15]. Thus, it is tempting to speculate that absence of SIRT3 per se may not yet be sufficient to increase the vulnerability to IR injury in young mice. However, in the presence of generally increased susceptibility for mPTP opening and the presence of additional age-related changes in mitochondrial function such as increased mitochondrial oxidative stress, a decrease in SIRT3 activity may predispose the aged heart for increased opening of the mPTP, in particular following IR.
During postischemic reperfusion of the heart, mitochondrial NAD+ levels decrease, suggesting that SIRT3 activity may be compromised during reperfusion and may contribute to the extent of IR injury [61, 62]. A number of mechanisms that contribute to IR injury may be contributed to by decreased SIRT3 activity. First, as discussed above, impairment in SIRT3 activity may increase mPTP opening due to decreased deacetylation of cyclophilin D [33]. Second, impairment in SIRT3 activity may result in decreased deacetylation and thus inhibition of MnSOD, thereby impairing detoxification of superoxide. As a consequence, mitochondrial oxidative stress will be increased, which will promote mPTP opening and oxidative damage within mitochondria [26]. Third, decreased SIRT3 activity may lead to a concerted downregulation of mitochondrial oxidative capacity due to hyperacetylation of numerous enzymes participating in the major pathways of mitochondrial metabolic substrate oxidation, resulting in delayed recovery of ATP synthesis during reperfusion and potentially a further increase in ROS generation during reenergization of a defective electron transport chain. Thus, preventing myocardial mitochondrial NAD+ depletion during IR may represent a useful approach to ameliorate detrimental effects of myocardial IR. Indeed, increasing myocardial NAD+ content by overexpression of the rate-limiting enzyme for NAD+ synthesis, nicotinamide phosphoribosyltransferase (Nampt), or by administration of NMN, resulted in reduced myocardial infarct size in response to ischemia reperfusion [63, 64].
Taken together, the available studies on SIRT3 in the heart suggest potentially protective effects of endogenous SIRT3 or SIRT3 activation in the heart. SIRT3 may protect against the development of pathological hypertrophy and may prevent decompensation to overt heart failure. SIRT3 may also protect against IR injury in the heart. These potentially beneficial effects of SIRT3 and SIRT3 activation as well as proposed underlying mechanisms of these beneficial effects are summarized in Fig. 1.
Potential protective/therapeutic effects of SIRT3 in the heart. NAD+ supplementation and/or activation of SIRT3 and/or induction of SIRT3 expression may protect against the development of cardiac hypertrophy and failure by increasing mitochondrial oxidative capacity, increasing nuclear translocation of Foxo3a and detoxification of ROS, inhibition of prohypertrophic Erk and Akt signaling, activation of AMPK, and inhibition of profibrotic TGF-β1 signaling. Protection against IR injury may be mediated by desensitization of mPTP opening, increased detoxification of ROS, and increased mitochondrial oxidative capacity. OXPHOS oxidative phosphorylation, FAO fatty acid oxidation, GO glucose oxidation
SIRT4 in cardiac physiology and disease
Much fewer studies have been published on SIRT4. In contrast to SIRT3, the in vitro deacetylation activity seems to be much lower; however, other posttranslational modifications have been reported for SIRT4, such as delipoylation and ADP-ribosylation, although the latter one is thought to be a side reaction of the main deacylation activity without significant physiological relevance [8, 65–68]. Similar to SIRT3, SIRT4 exerts a number of effects on energy metabolism. SIRT4 has been shown to inhibit glutamate dehydrogenase in pancreatic beta-cells by ADP-ribosylation, resulting in decreased insulin secretion in response to amino acids [67]. SIRT4 also coimmunoprecipitates with insulin-degrading enzyme and may thereby suppress insulin secretion in response to glucose, suggesting that SIRT4 regulates systemic glucose disposal by modulating insulin secretion [66]. Furthermore, SIRT4 enzymatically hydrolyzes the lipoamide cofactors from the E2 component dihydrolipoyllysine acetyltransferase (DLAT) of the pyruvate dehydrogenase (PDH) complex, thereby diminishing PDH activity and compromising intracellular glucose oxidation [8]. Interestingly, the authors also showed that SIRT4 catalytic efficiency for lipoyl–lysine and biotinyl–lysine modifications may be superior to its deacetylation activity. Besides effects on glucose disposal and utilization, SIRT4 also regulates lipid metabolism due to the ability to deacetylate malonyl-CoA decarboxylase (MCD) at K471, thereby inhibiting its activity and increasing malonyl-CoA levels [69]. Conversely, mice lacking SIRT4 display elevated MCD activity, decreased malonyl-CoA levels, resulting in increased fatty acid oxidation and decreased lipogenesis in skeletal muscle and white adipose tissue [69]. These mice show increased exercise tolerance and are protected against diet-induced obesity [69]. Similarly, knockdown of SIRT4 also resulted in increased fatty acid oxidation and cellular respiration in liver and muscle cells, maybe driven by increased expression of genes encoding for enzymes of fatty acid oxidation [70]. Interestingly, SIRT4−/− mice display increased rates of fatty acid oxidation and increased expression of PPARα and fatty acid oxidation genes in the liver, and increased oxidation rates seem to require functional SIRT1, suggesting a cross talk between mitochondrial and nuclear sirtuins [71]. Finally, it has been shown that SIRT4 expression is induced by numerous genotoxic agents and represses the metabolism of glutamine into the TCA cycle, thereby impairing TCA cycle anaplerosis [72]. Thus, the metabolic role of SIRT4 may be to inhibit oxidation of glucose and fatty acids, and may impair TCA cycle anaplerosis and function, which should result in impaired ATP synthesis and energy depletion.
Although SIRT4 is highly expressed in the heart, studies investigating the metabolic function of SIRT4 in the heart are lacking. Nevertheless, some studies suggest that SIRT4 may modulate the outcome following myocardial ischemia reperfusion. Liu and colleagues demonstrated in H9C2 rat heart myoblasts that hypoxia downregulates the expression of SIRT4 [73]. In this study, knockdown of SIRT4 decreased cell viability, increased caspase activation, and increased the amount of apoptotic cells, whereas SIRT4 overexpression increased cell viability, inhibited caspase activation, and decreased the amount of apoptotic cells, suggesting that downregulation of SIRT4 during hypoxia may contribute to increased apoptotic cell death in response to hypoxia and ischemia reperfusion [73, 74]. In contrast, suppression of SIRT4 by siRNA protects against induction of mPTP opening and mPTP-dependent ROS production in HeLa cells, suggesting that suppression of SIRT4 may exert beneficial effects during hypoxia and ischemia reperfusion injury [75]. The impact of SIRT4 suppression during hypoxia and ischemia reperfusion on mitochondrial oxidative capacity and cardiac recovery remains speculative. Inhibition of SIRT4 activity could be adaptive since recovery of myocardial energetics may be improved following hypoxia and ischemia due to disinhibition of glucose and fatty acid oxidation. In contrast, increased oxidative capacity may increase mitochondrial ROS generation during reenergization of the electron transport chain shortly after the onset of reperfusion and may thereby exaggerate IR injury. Studies investigating myocardial IR injury in mice with genetic manipulation of SIRT4 expression are much needed to understand the role of SIRT4 in the context of IR in the heart.
SIRT5 in cardiac physiology and disease
Similar to SIRT4, SIRT5 posseses only weak deacetylase activity. SIRT5 has been found to deacetylate carbamoyl phosphate synthetase 1 (CPS1), thus participating in the detoxification of ammonia [76]. Cytochrome c and peroxiredoxin 1 were identified as further deacetylation targets of SIRT5, potentially suggesting a role for SIRT5 in apoptosis, mitochondrial respiration, and redox regulation [22, 77, 78]. More importantly though, SIRT5 has been shown to function as an efficient protein lysine desuccinylase and demalonylase [79–81]. Park and colleagues identified 2565 succinylation sites on 779 proteins using systematic profiling of the mammalian succinylome, and Rardin et al. identified 1190 succinyllysine sites on 252 proteins, 56 % of which seem to be SIRT5 target proteins [13, 81]. Pathway analyses revealed that many proteins identified to be SIRT5 targets are involved in mitochondrial metabolic pathways, including amino acid degradation, the TCA cycle, fatty acid oxidation, pyruvate decarboxylation, and ATP synthesis [13, 81]. Regarding malonylation, Nishida et al. identified 1137 malonyllysine sites across 430 proteins, with 120 proteins that also showed increased malonylation in SIRT5−/− animals. A pathway analysis identified glycolysis as the top SIRT5-regulated pathway [82]. While numerous potential SIRT5 targets have been identified, elucidation of the functional consequences and physiological relevance appears challenging, and controversial results have been reported. Lack of SIRT5 was shown to decrease palmitate oxidation in mouse embryonic fibroblasts and primary hepatocytes of SIRT5−/− mice, and to impair the activity of enoyl-CoA hydratase α (ECHA) in the heart, suggesting that SIRT5 may serve to increase fatty acid oxidation [83]. Less conclusive are data on mitochondrial respiration and glucose utilization. Overexpression of SIRT5 increased ATP production and oxygen consumption in HepG2 cells, but a higher mitochondrial respiration rate was also observed in hepatocytes of SIRT5−/− mice and in 293T cells with SIRT5 knockdown [13, 84]. Regarding glucose utilization, decreased glycolytic flux was reported in primary hepatocytes from SIRT5−/− mice, maybe due to increased malonylation of glyceraldehyde-3-phosphate dehydrogenase, whereas knockdown of SIRT5 increased PDH activity due to increased succinylation of multiple PDH subunits [13, 82]. Besides metabolism, SIRT5 desuccinylated and activated superoxide dismutase 1 (SOD1) and may thus boost cellular antioxidant activity [85]. Finally, SIRT5 has been shown to catalyze protein lysine glutarylation. Tan et al. identified 229 proteins with hyperglutarylation in liver tissue of SIRT5−/− mice, and a biological pathway analysis of the lysine glutarylome revealed again fatty acid metabolism, TCA cycle, and aerobic respiration as major pathways, although the functional consequences for each pathway remain to be elucidated [9].
Similar to the other mitochondrial sirtuins, SIRT5 is highly expressed in cardiac tissue. A very recent study by Sadhukhan et al. [83] revealed that succinyl-CoA is the most abundant acyl-CoA molecule in the heart, suggesting that lysine succinylation may be relevant for cardiac physiology. Indeed, mice with deletion of SIRT5 showed cardiac contractile dysfunction, pathologic hypertrophy, and increased fibrosis [83]. Analysis of the cardiac succinylome in SIRT5−/− mice also suggested mitochondrial energy metabolic pathways to be regulated by SIRT5, and that myocardial energy depletion may contribute to cardiac dysfunction in SIRT5−/− mice, potentially contributed to by hypersuccinylation and inhibition of ECHA [83]. Thus, similar to SIRT3, SIRT5 may be required to maintain cardiac function and energetics. The study also implies that SIRT5 may protect from the development of cardiac hypertrophy, although gain-of-function studies need to be conducted for further conclusions.
Again similar to SIRT3, lack of SIRT5 exacerbates IR injury. Myocardial infarct size was increased, and recovery of contractile function was impaired in hearts of SIRT5−/− mice following IR [86]. IR injury was restored to WT levels by inhibition of succinate dehydrogenase, which was hypersuccinylated and probably more active in SIRT5−/− hearts [13, 86]. Since succinate accumulates during ischemia and drives mitochondrial ROS generation at the onset of reperfusion by increasing reverse electron transport in the electron transport chain, the authors proposed that inhibition of SDH may restore IR injury to WT levels by reducing succinate-driven ROS production [86, 87]. Interestingly, SIRT5 is downregulated in cardiomyocytes upon oxidative stress, and SIRT5 knockdown results in a marked reduction in cell viability, a significant increase in the number of apoptotic cells, and increased activity of caspase 3 activity [73]. Oxidative stress and apoptosis are frequently observed in cardiac pathologies, such as IR injury and heart failure. Thus, although only few studies are available on SIRT5 in the heart, the currently available data strongly suggest a significant role for SIRT5 in cardiac physiology and pathology that needs to be investigated.
Conclusions
Mitochondrial function and energetics are essential for cardiac function and integrity, and impairment in mitochondrial biology contributes to cardiac pathologies such as IR injury and heart failure. Mitochondrial sirtuins are major regulators of mitochondrial energetics and modulate ROS detoxification and permeability transition, and several studies suggest that mitochondrial sirtuins modulate the cardiac response to IR and various stressors. SIRT3 may exert protective effects during IR and the development of cardiac hypertrophy and failure. Few data are available on SIRT4 and SIRT5 in the heart. Nevertheless, these studies suggest that SIRT5 may also exert beneficial effects during IR, whereas the role of SIRT4 during IR remains to be elucidated. While pharmacological modulation of mitochondrial sirtuins appears like a promising therapeutic approach, a number of unresolved issues remain to be addressed. Many potential targets that have been identified in loss-of-function models and using screening assays for posttranslational modifications need to be confirmed as definite targets of mitochondrial sirtuins. Although quite laborious, it would be desirable to elucidate the functional consequence of each lysine acylation (e.g., aceytlation, succinylation, or malonylation) on a single and promising target protein to elucidate the functional modulation due to altered lysine acylation. Some studies reported opposite functional effects by posttranslational modifications of the same protein (e.g., LCAD), which may potentially be related to distinct acylation patterns of the same protein, resulting in different functional outcomes [19, 29]. Furthermore, we do not understand why the mitochondrion hosts three different sirtuins which, at least in part, seem to have targets in similar mitochondrial pathways. The NAD+ dependence of all mitochondrial sirtuins may suggest that SIRT3–5 may comprise an enzymatic system which may serve as a redox-sensitive rheostat that adapts cellular energy production to energy demand, among other functions. The relative and functional contribution of each sirtuin remains however unresolved to date. Understanding of their interplay is important though if modulation of sirtuins should be considered as a therapeutic option. Nonetheless, modulation of mitochondrial sirtuin activity may represent a promising approach to alter mitochondrial biology in cardiac disease and may promote further research in the field of mitochondrial medicine.
References
Stanley WC, Recchia FA, Lopaschuk GD (2005) Myocardial substrate metabolism in the normal and failing heart. Physiol Rev 85(3):1093–1129. doi:10.1152/physrev.00006.2004
Keating ST, El-Osta A (2015) Epigenetics and metabolism. Circ Res 116(4):715–736. doi:10.1161/CIRCRESAHA.116.303936
Guarente L, Picard F (2005) Calorie restriction—the SIR2 connection. Cell 120(4):473–482. doi:10.1016/j.cell.2005.01.029
Imai S, Armstrong CM, Kaeberlein M, Guarente L (2000) Transcriptional silencing and longevity protein Sir2 is an NAD-dependent histone deacetylase. Nature 403(6771):795–800. doi:10.1038/35001622
Rogina B, Helfand SL (2004) Sir2 mediates longevity in the fly through a pathway related to calorie restriction. Proc Natl Acad Sci USA 101(45):15998–16003. doi:10.1073/pnas.0404184101
Kaeberlein M, McVey M, Guarente L (1999) The SIR2/3/4 complex and SIR2 alone promote longevity in Saccharomyces cerevisiae by two different mechanisms. Genes Dev 13(19):2570–2580
Tissenbaum HA, Guarente L (2001) Increased dosage of a sir-2 gene extends lifespan in Caenorhabditis elegans. Nature 410(6825):227–230. doi:10.1038/3506563835065638
Mathias RA, Greco TM, Oberstein A, Budayeva HG, Chakrabarti R, Rowland EA, Kang Y, Shenk T, Cristea IM (2014) Sirtuin 4 is a lipoamidase regulating pyruvate dehydrogenase complex activity. Cell 159(7):1615–1625. doi:10.1016/j.cell.2014.11.046
Tan M, Peng C, Anderson KA, Chhoy P, Xie Z, Dai L, Park J, Chen Y, Huang H, Zhang Y, Ro J, Wagner GR, Green MF, Madsen AS, Schmiesing J, Peterson BS, Xu G, Ilkayeva OR, Muehlbauer MJ, Braulke T, Muhlhausen C, Backos DS, Olsen CA, McGuire PJ, Pletcher SD, Lombard DB, Hirschey MD, Zhao Y (2014) Lysine glutarylation is a protein posttranslational modification regulated by SIRT5. Cell Metab 19(4):605–617. doi:10.1016/j.cmet.2014.03.014
Hirschey MD, Zhao Y (2015) Metabolic regulation by lysine malonylation, succinylation, and glutarylation. Mol Cell Proteom MCP 14(9):2308–2315. doi:10.1074/mcp.R114.046664
Du J, Zhou Y, Su X, Yu JJ, Khan S, Jiang H, Kim J, Woo J, Kim JH, Choi BH, He B, Chen W, Zhang S, Cerione RA, Auwerx J, Hao Q, Lin H (2011) Sirt5 is a NAD-dependent protein lysine demalonylase and desuccinylase. Science 334(6057):806–809. doi:10.1126/science.1207861
Kim SC, Sprung R, Chen Y, Xu Y, Ball H, Pei J, Cheng T, Kho Y, Xiao H, Xiao L, Grishin NV, White M, Yang XJ, Zhao Y (2006) Substrate and functional diversity of lysine acetylation revealed by a proteomics survey. Mol Cell 23(4):607–618. doi:10.1016/j.molcel.2006.06.026
Park J, Chen Y, Tishkoff DX, Peng C, Tan M, Dai L, Xie Z, Zhang Y, Zwaans BM, Skinner ME, Lombard DB, Zhao Y (2013) SIRT5-mediated lysine desuccinylation impacts diverse metabolic pathways. Mol Cell 50(6):919–930. doi:10.1016/j.molcel.2013.06.001
Bugger H, Abel ED (2014) Molecular mechanisms of diabetic cardiomyopathy. Diabetologia 57(4):660–671. doi:10.1007/s00125-014-3171-6
Murphy E, Steenbergen C (2008) Mechanisms underlying acute protection from cardiac ischemia–reperfusion injury. Physiol Rev 88(2):581–609. doi:10.1152/physrev.00024.2007
Bayeva M, Gheorghiade M, Ardehali H (2013) Mitochondria as a therapeutic target in heart failure. J Am Coll Cardiol 61(6):599–610. doi:10.1016/j.jacc.2012.08.1021
Hebert AS, Dittenhafer-Reed KE, Yu W, Bailey DJ, Selen ES, Boersma MD, Carson JJ, Tonelli M, Balloon AJ, Higbee AJ, Westphall MS, Pagliarini DJ, Prolla TA, Assadi-Porter F, Roy S, Denu JM, Coon JJ (2013) Calorie restriction and SIRT3 trigger global reprogramming of the mitochondrial protein acetylome. Mol Cell 49(1):186–199. doi:10.1016/j.molcel.2012.10.024
Ahn BH, Kim HS, Song S, Lee IH, Liu J, Vassilopoulos A, Deng CX, Finkel T (2008) A role for the mitochondrial deacetylase Sirt3 in regulating energy homeostasis. Proc Natl Acad Sci USA 105(38):14447–14452. doi:10.1073/pnas.0803790105
Hirschey MD, Shimazu T, Goetzman E, Jing E, Schwer B, Lombard DB, Grueter CA, Harris C, Biddinger S, Ilkayeva OR, Stevens RD, Li Y, Saha AK, Ruderman NB, Bain JR, Newgard CB, Farese RV Jr, Alt FW, Kahn CR, Verdin E (2010) SIRT3 regulates mitochondrial fatty-acid oxidation by reversible enzyme deacetylation. Nature 464(7285):121–125. doi:10.1038/nature08778
Lombard DB, Alt FW, Cheng HL, Bunkenborg J, Streeper RS, Mostoslavsky R, Kim J, Yancopoulos G, Valenzuela D, Murphy A, Yang Y, Chen Y, Hirschey MD, Bronson RT, Haigis M, Guarente LP, Farese RV Jr, Weissman S, Verdin E, Schwer B (2007) Mammalian Sir2 homolog SIRT3 regulates global mitochondrial lysine acetylation. Mol Cell Biol 27(24):8807–8814. doi:10.1128/MCB.01636-07
Yu W, Dittenhafer-Reed KE, Denu JM (2012) SIRT3 protein deacetylates isocitrate dehydrogenase 2 (IDH2) and regulates mitochondrial redox status. J Biol Chem 287(17):14078–14086. doi:10.1074/jbc.M112.355206
Schlicker C, Gertz M, Papatheodorou P, Kachholz B, Becker CF, Steegborn C (2008) Substrates and regulation mechanisms for the human mitochondrial sirtuins Sirt3 and Sirt5. J Mol Biol 382(3):790–801. doi:10.1016/j.jmb.2008.07.048
Shi T, Wang F, Stieren E, Tong Q (2005) SIRT3, a mitochondrial sirtuin deacetylase, regulates mitochondrial function and thermogenesis in brown adipocytes. J Biol Chem 280(14):13560–13567. doi:10.1074/jbc.M414670200
Cimen H, Han MJ, Yang Y, Tong Q, Koc H, Koc EC (2010) Regulation of succinate dehydrogenase activity by SIRT3 in mammalian mitochondria. Biochemistry 49(2):304–311. doi:10.1021/bi901627u
Kim HS, Patel K, Muldoon-Jacobs K, Bisht KS, Aykin-Burns N, Pennington JD, van der Meer R, Nguyen P, Savage J, Owens KM, Vassilopoulos A, Ozden O, Park SH, Singh KK, Abdulkadir SA, Spitz DR, Deng CX, Gius D (2010) SIRT3 is a mitochondria-localized tumor suppressor required for maintenance of mitochondrial integrity and metabolism during stress. Cancer Cell 17(1):41–52. doi:10.1016/j.ccr.2009.11.023
Tao R, Coleman MC, Pennington JD, Ozden O, Park SH, Jiang H, Kim HS, Flynn CR, Hill S, Hayes McDonald W, Olivier AK, Spitz DR, Gius D (2010) Sirt3-mediated deacetylation of evolutionarily conserved lysine 122 regulates MnSOD activity in response to stress. Mol Cell 40(6):893–904. doi:10.1016/j.molcel.2010.12.013
Qiu X, Brown K, Hirschey MD, Verdin E, Chen D (2010) Calorie restriction reduces oxidative stress by SIRT3-mediated SOD2 activation. Cell Metab 12(6):662–667. doi:10.1016/j.cmet.2010.11.015
Koentges C, Pfeil K, Schnick T, Wiese S, Dahlbock R, Cimolai MC, Meyer-Steenbuck M, Cenkerova K, Hoffmann MM, Jaeger C, Odening KE, Kammerer B, Hein L, Bode C, Bugger H (2015) SIRT3 deficiency impairs mitochondrial and contractile function in the heart. Basic Res Cardiol 110(4):36. doi:10.1007/s00395-015-0493-6
Alrob OA, Sankaralingam S, Ma C, Wagg CS, Fillmore N, Jaswal JS, Sack MN, Lehner R, Gupta MP, Michelakis ED, Padwal RS, Johnstone DE, Sharma AM, Lopaschuk GD (2014) Obesity-induced lysine acetylation increases cardiac fatty acid oxidation and impairs insulin signalling. Cardiovasc Res 103(4):485–497. doi:10.1093/cvr/cvu156
Pillai VB, Sundaresan NR, Kim G, Gupta M, Rajamohan SB, Pillai JB, Samant S, Ravindra PV, Isbatan A, Gupta MP (2010) Exogenous NAD blocks cardiac hypertrophic response via activation of the SIRT3-LKB1-AMP-activated kinase pathway. J Biol Chem 285(5):3133–3144. doi:10.1074/jbc.M109.077271
Peek CB, Affinati AH, Ramsey KM, Kuo HY, Yu W, Sena LA, Ilkayeva O, Marcheva B, Kobayashi Y, Omura C, Levine DC, Bacsik DJ, Gius D, Newgard CB, Goetzman E, Chandel NS, Denu JM, Mrksich M, Bass J (2013) Circadian clock NAD + cycle drives mitochondrial oxidative metabolism in mice. Science 342(6158):1243417. doi:10.1126/science.1243417
Sundaresan NR, Gupta M, Kim G, Rajamohan SB, Isbatan A, Gupta MP (2009) Sirt3 blocks the cardiac hypertrophic response by augmenting Foxo3a-dependent antioxidant defense mechanisms in mice. J Clin Investig 119(9):2758–2771. doi:10.1172/JCI39162
Hafner AV, Dai J, Gomes AP, Xiao CY, Palmeira CM, Rosenzweig A, Sinclair DA (2010) Regulation of the mPTP by SIRT3-mediated deacetylation of CypD at lysine 166 suppresses age-related cardiac hypertrophy. Aging (Albany NY) 2(12):914–923. doi:10.18632/aging.100252
Pillai VB, Samant S, Sundaresan NR, Raghuraman H, Kim G, Bonner MY, Arbiser JL, Walker DI, Jones DP, Gius D, Gupta MP (2015) Honokiol blocks and reverses cardiac hypertrophy in mice by activating mitochondrial Sirt3. Nat Commun 6:6656. doi:10.1038/ncomms7656
Sugden PH, Clerk A (2000) Activation of the small GTP-binding protein Ras in the heart by hypertrophic agonists. Trends Cardiovasc Med 10(1):1–8
Sawyer DB, Siwik DA, Xiao L, Pimentel DR, Singh K, Colucci WS (2002) Role of oxidative stress in myocardial hypertrophy and failure. J Mol Cell Cardiol 34(4):379–388. doi:10.1006/jmcc.2002.1526
Sugden PH, Clerk A (2006) Oxidative stress and growth-regulating intracellular signaling pathways in cardiac myocytes. Antioxid Redox Signal 8(11–12):2111–2124. doi:10.1089/ars.2006.8.2111
Tan WQ, Wang K, Lv DY, Li PF (2008) Foxo3a inhibits cardiomyocyte hypertrophy through transactivating catalase. J Biol Chem 283(44):29730–29739. doi:10.1074/jbc.M805514200
Young LH (2008) AMP-activated protein kinase conducts the ischemic stress response orchestra. Circulation 117(6):832–840. doi:10.1161/CIRCULATIONAHA.107.713115
Chan AY, Dolinsky VW, Soltys CL, Viollet B, Baksh S, Light PE, Dyck JR (2008) Resveratrol inhibits cardiac hypertrophy via AMP-activated protein kinase and Akt. J Biol Chem 283(35):24194–24201. doi:10.1074/jbc.M802869200
Meng RS, Pei ZH, Yin R, Zhang CX, Chen BL, Zhang Y, Liu D, Xu AL, Dong YG (2009) Adenosine monophosphate-activated protein kinase inhibits cardiac hypertrophy through reactivating peroxisome proliferator-activated receptor-alpha signaling pathway. Eur J Pharmacol 620(1–3):63–70. doi:10.1016/j.ejphar.2009.08.024
Ikeda Y, Sato K, Pimentel DR, Sam F, Shaw RJ, Dyck JR, Walsh K (2009) Cardiac-specific deletion of LKB1 leads to hypertrophy and dysfunction. J Biol Chem 284(51):35839–35849. doi:10.1074/jbc.M109.057273
Heineke J, Molkentin JD (2006) Regulation of cardiac hypertrophy by intracellular signalling pathways. Nat Rev Mol Cell Biol 7(8):589–600. doi:10.1038/nrm1983
Opie LH, Owen P (1975) Effects of increased mechanical work by isolated perfused rat heart during production or uptake of ketone bodies. Assessment of mitochondrial oxidized to reduced free nicotinamide-adenine dinucleotide ratios and oxaloacetate concentrations. Biochem J 148(3):403–415
Pillai JB, Isbatan A, Imai S, Gupta MP (2005) Poly(ADP-ribose) polymerase-1-dependent cardiac myocyte cell death during heart failure is mediated by NAD + depletion and reduced Sir2alpha deacetylase activity. J Biol Chem 280(52):43121–43130. doi:10.1074/jbc.M506162200
Grillon JM, Johnson KR, Kotlo K, Danziger RS (2012) Non-histone lysine acetylated proteins in heart failure. Biochim Biophys Acta 1822(2):607–614. doi:10.1016/j.bbadis.2011.11.016
Karamanlidis G, Lee CF, Garcia-Menendez L, Kolwicz SC Jr, Suthammarak W, Gong G, Sedensky MM, Morgan PG, Wang W, Tian R (2013) Mitochondrial complex I deficiency increases protein acetylation and accelerates heart failure. Cell Metab 18(2):239–250. doi:10.1016/j.cmet.2013.07.002
Porter GA, Urciuoli WR, Brookes PS, Nadtochiy SM (2014) SIRT3 deficiency exacerbates ischemia-reperfusion injury: implication for aged hearts. Am J Physiol Heart Circ Physiol 306(12):H1602–H1609. doi:10.1152/ajpheart.00027.2014
Koentges C, Pfeil K, Meyer-Steenbuck M, Lother A, Hoffmann MM, Odening KE, Hein L, Bode C, Bugger H (2016) Preserved recovery of cardiac function following ischemia-reperfusion in mice lacking SIRT3. Can J Physiol Pharmacol 94(1):72–80. doi:10.1139/cjpp-2015-0152
Bochaton T, Crola-Da-Silva C, Pillot B, Villedieu C, Ferreras L, Alam MR, Thibault H, Strina M, Gharib A, Ovize M, Baetz D (2015) Inhibition of myocardial reperfusion injury by ischemic postconditioning requires sirtuin 3-mediated deacetylation of cyclophilin D. J Mol Cell Cardiol 84:61–69. doi:10.1016/j.yjmcc.2015.03.017
Mather M, Rottenberg H (2000) Aging enhances the activation of the permeability transition pore in mitochondria. Biochem Biophys Res Commun 273(2):603–608. doi:10.1006/bbrc.2000.2994
Petrosillo G, Moro N, Paradies V, Ruggiero FM, Paradies G (2010) Increased susceptibility to Ca(2 +)-induced permeability transition and to cytochrome c release in rat heart mitochondria with aging: effect of melatonin. J Pineal Res 48(4):340–346. doi:10.1111/j.1600-079X.2010.00758.x
Hofer T, Servais S, Seo AY, Marzetti E, Hiona A, Upadhyay SJ, Wohlgemuth SE, Leeuwenburgh C (2009) Bioenergetics and permeability transition pore opening in heart subsarcolemmal and interfibrillar mitochondria: effects of aging and lifelong calorie restriction. Mech Ageing Dev 130(5):297–307. doi:10.1016/j.mad.2009.01.004
Di Lisa F, Bernardi P (2005) Mitochondrial function and myocardial aging. A critical analysis of the role of permeability transition. Cardiovasc Res 66(2):222–232. doi:10.1016/j.cardiores.2005.02.009
Fernandez-Sanz C, Ruiz-Meana M, Castellano J, Miro-Casas E, Nunez E, Inserte J, Vazquez J, Garcia-Dorado D (2015) Altered FoF1 ATP synthase and susceptibility to mitochondrial permeability transition pore during ischaemia and reperfusion in aging cardiomyocytes. Thromb Haemost 113(3):441–451. doi:10.1160/TH14-10-0901
Korzick DH, Lancaster TS (2013) Age-related differences in cardiac ischemia-reperfusion injury: effects of estrogen deficiency. Pflugers Arch 465(5):669–685. doi:10.1007/s00424-013-1255-7
Lesnefsky EJ, Gallo DS, Ye J, Whittingham TS, Lust WD (1994) Aging increases ischemia-reperfusion injury in the isolated, buffer-perfused heart. J Lab Clin Med 124(6):843–851
Sussman MA, Anversa P (2004) Myocardial aging and senescence: Where have the stem cells gone? Ann Rev Physiol 66:29–48. doi:10.1146/annurev.physiol.66.032102.140723
Karbowski M, Kurono C, Wozniak M, Ostrowski M, Teranishi M, Nishizawa Y, Usukura J, Soji T, Wakabayashi T (1999) Free radical-induced megamitochondria formation and apoptosis. Free Radic Biol Med 26(3–4):396–409
Sachs HG, Colgan JA, Lazarus ML (1977) Ultrastructure of the aging myocardium: a morphometric approach. Am J Anat 150(1):63–71. doi:10.1002/aja.1001500105
Di Lisa F, Menabo R, Canton M, Barile M, Bernardi P (2001) Opening of the mitochondrial permeability transition pore causes depletion of mitochondrial and cytosolic NAD + and is a causative event in the death of myocytes in postischemic reperfusion of the heart. J Biol Chem 276(4):2571–2575 Epub 2000 Nov 2579
Zhu J, Rebecchi MJ, Tan M, Glass PS, Brink PR, Liu L (2010) Age-associated differences in activation of Akt/GSK-3beta signaling pathways and inhibition of mitochondrial permeability transition pore opening in the rat heart. J Gerontol A Biol Sci Med Sci 65(6):611–619. doi:10.1093/gerona/glq035
Hsu CP, Oka S, Shao D, Hariharan N, Sadoshima J (2009) Nicotinamide phosphoribosyltransferase regulates cell survival through NAD+ synthesis in cardiac myocytes. Circ Res 105(5):481–491. doi:10.1161/CIRCRESAHA.109.203703
Yamamoto T, Byun J, Zhai P, Ikeda Y, Oka S, Sadoshima J (2014) Nicotinamide mononucleotide, an intermediate of NAD + synthesis, protects the heart from ischemia and reperfusion. PLoS ONE 9(6):e98972. doi:10.1371/journal.pone.0098972
Du J, Jiang H, Lin H (2009) Investigating the ADP-ribosyltransferase activity of sirtuins with NAD analogues and 32P-NAD. Biochemistry 48(13):2878–2890. doi:10.1021/bi802093g
Ahuja N, Schwer B, Carobbio S, Waltregny D, North BJ, Castronovo V, Maechler P, Verdin E (2007) Regulation of insulin secretion by SIRT4, a mitochondrial ADP-ribosyltransferase. J Biol Chem 282(46):33583–33592. doi:10.1074/jbc.M705488200
Haigis MC, Mostoslavsky R, Haigis KM, Fahie K, Christodoulou DC, Murphy AJ, Valenzuela DM, Yancopoulos GD, Karow M, Blander G, Wolberger C, Prolla TA, Weindruch R, Alt FW, Guarente L (2006) SIRT4 inhibits glutamate dehydrogenase and opposes the effects of calorie restriction in pancreatic beta cells. Cell 126(5):941–954. doi:10.1016/j.cell.2006.06.057
Gertz M, Steegborn C (2016) Using mitochondrial sirtuins as drug targets: disease implications and available compounds. CMLS, Cell Mol Life Sci. doi:10.1007/s00018-016-2180-7
Laurent G, German NJ, Saha AK, de Boer VC, Davies M, Koves TR, Dephoure N, Fischer F, Boanca G, Vaitheesvaran B, Lovitch SB, Sharpe AH, Kurland IJ, Steegborn C, Gygi SP, Muoio DM, Ruderman NB, Haigis MC (2013) SIRT4 coordinates the balance between lipid synthesis and catabolism by repressing malonyl CoA decarboxylase. Mol Cell 50(5):686–698. doi:10.1016/j.molcel.2013.05.012
Nasrin N, Wu X, Fortier E, Feng Y, Bare OC, Chen S, Ren X, Wu Z, Streeper RS, Bordone L (2010) SIRT4 regulates fatty acid oxidation and mitochondrial gene expression in liver and muscle cells. J Biol Chem 285(42):31995–32002. doi:10.1074/jbc.M110.124164
Laurent G, de Boer VC, Finley LW, Sweeney M, Lu H, Schug TT, Cen Y, Jeong SM, Li X, Sauve AA, Haigis MC (2013) SIRT4 represses peroxisome proliferator-activated receptor alpha activity to suppress hepatic fat oxidation. Mol Cell Biol 33(22):4552–4561. doi:10.1128/MCB.00087-13
Jeong SM, Xiao C, Finley LW, Lahusen T, Souza AL, Pierce K, Li YH, Wang X, Laurent G, German NJ, Xu X, Li C, Wang RH, Lee J, Csibi A, Cerione R, Blenis J, Clish CB, Kimmelman A, Deng CX, Haigis MC (2013) SIRT4 has tumor-suppressive activity and regulates the cellular metabolic response to DNA damage by inhibiting mitochondrial glutamine metabolism. Cancer Cell 23(4):450–463. doi:10.1016/j.ccr.2013.02.024
Liu B, Che W, Xue J, Zheng C, Tang K, Zhang J, Wen J, Xu Y (2013) SIRT4 prevents hypoxia-induced apoptosis in H9c2 cardiomyoblast cells. Cell Physiol Biochem 32(3):655–662. doi:10.1159/000354469
Scarabelli TM, Gottlieb RA (2004) Functional and clinical repercussions of myocyte apoptosis in the multifaceted damage by ischemia/reperfusion injury: old and new concepts after 10 years of contributions. Cell Death Differ 11(Suppl 2):S144–S152. doi:10.1038/sj.cdd.4401544
Verma M, Shulga N (1827) Pastorino JG Sirtuin-4 modulates sensitivity to induction of the mitochondrial permeability transition pore. Biochim Biophys Acta 1:38–49. doi:10.1016/j.bbabio.2012.09.016
Nakagawa T, Lomb DJ, Haigis MC, Guarente L (2009) SIRT5 deacetylates carbamoyl phosphate synthetase 1 and regulates the urea cycle. Cell 137(3):560–570. doi:10.1016/j.cell.2009.02.026
Fischer F, Gertz M, Suenkel B, Lakshminarasimhan M, Schutkowski M, Steegborn C (2012) Sirt5 deacylation activities show differential sensitivities to nicotinamide inhibition. PLoS ONE 7(9):e45098. doi:10.1371/journal.pone.0045098
Rauh D, Fischer F, Gertz M, Lakshminarasimhan M, Bergbrede T, Aladini F, Kambach C, Becker CF, Zerweck J, Schutkowski M, Steegborn C (2013) An acetylome peptide microarray reveals specificities and deacetylation substrates for all human sirtuin isoforms. Nat Commun 4:2327. doi:10.1038/ncomms3327
Peng C, Lu Z, Xie Z, Cheng Z, Chen Y, Tan M, Luo H, Zhang Y, He W, Yang K, Zwaans BM, Tishkoff D, Ho L, Lombard D, He TC, Dai J, Verdin E, Ye Y, Zhao Y (2011) The first identification of lysine malonylation substrates and its regulatory enzyme. Mol Cell Proteom 10(12):M111-012658. doi:10.1074/mcp.M111.012658
Zhang Z, Tan M, Xie Z, Dai L, Chen Y, Zhao Y (2011) Identification of lysine succinylation as a new post-translational modification. Nat Chem Biol 7(1):58–63. doi:10.1038/nchembio.495
Rardin MJ, He W, Nishida Y, Newman JC, Carrico C, Danielson SR, Guo A, Gut P, Sahu AK, Li B, Uppala R, Fitch M, Riiff T, Zhu L, Zhou J, Mulhern D, Stevens RD, Ilkayeva OR, Newgard CB, Jacobson MP, Hellerstein M, Goetzman ES, Gibson BW, Verdin E (2013) SIRT5 regulates the mitochondrial lysine succinylome and metabolic networks. Cell Metab 18(6):920–933. doi:10.1016/j.cmet.2013.11.013
Nishida Y, Rardin MJ, Carrico C, He W, Sahu AK, Gut P, Najjar R, Fitch M, Hellerstein M, Gibson BW, Verdin E (2015) SIRT5 regulates both cytosolic and mitochondrial protein malonylation with glycolysis as a major target. Mol Cell 59(2):321–332. doi:10.1016/j.molcel.2015.05.022
Sadhukhan S, Liu X, Ryu D, Nelson OD, Stupinski JA, Li Z, Chen W, Zhang S, Weiss RS, Locasale JW, Auwerx J, Lin H (2016) Metabolomics-assisted proteomics identifies succinylation and SIRT5 as important regulators of cardiac function. Proc Natl Acad Sci USA 113(16):4320–4325. doi:10.1073/pnas.1519858113
Buler M, Aatsinki SM, Izzi V, Uusimaa J, Hakkola J (2014) SIRT5 is under the control of PGC-1alpha and AMPK and is involved in regulation of mitochondrial energy metabolism. FASEB J 28(7):3225–3237. doi:10.1096/fj.13-245241
Lin ZF, Xu HB, Wang JY, Lin Q, Ruan Z, Liu FB, Jin W, Huang HH, Chen X (2013) SIRT5 desuccinylates and activates SOD1 to eliminate ROS. Biochem Biophys Res Commun 441(1):191–195. doi:10.1016/j.bbrc.2013.10.033
Boylston JA, Sun J, Chen Y, Gucek M, Sack MN, Murphy E (2015) Characterization of the cardiac succinylome and its role in ischemia-reperfusion injury. J Mol Cell Cardiol 88:73–81. doi:10.1016/j.yjmcc.2015.09.005
Chouchani ET, Pell VR, Gaude E, Aksentijevic D, Sundier SY, Robb EL, Logan A, Nadtochiy SM, Ord EN, Smith AC, Eyassu F, Shirley R, Hu CH, Dare AJ, James AM, Rogatti S, Hartley RC, Eaton S, Costa AS, Brookes PS, Davidson SM, Duchen MR, Saeb-Parsy K, Shattock MJ, Robinson AJ, Work LM, Frezza C, Krieg T, Murphy MP (2014) Ischaemic accumulation of succinate controls reperfusion injury through mitochondrial ROS. Nature 515(7527):431–435. doi:10.1038/nature13909
Acknowledgments
This study was supported by Grants of the German Research Foundation (Bu2126/2-1 and Bu2126/3-1).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they do not have any conflict of interest related to this manuscript.
Rights and permissions
About this article
Cite this article
Bugger, H., Witt, C.N. & Bode, C. Mitochondrial sirtuins in the heart. Heart Fail Rev 21, 519–528 (2016). https://doi.org/10.1007/s10741-016-9570-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10741-016-9570-7