Abstract
The aim of this study was to evaluate the therapeutic efficacy of caffeic acid phenethyl ester (CAPE) with an experimental traumatic brain injury (TBI) model in rats. Twenty-four adult male Sprague–Dawley rats were randomly divided into three groups of 8 rats each: control, TBI, and TBI + CAPE treatment. In TBI and TBI + CAPE treatment groups, a cranial impact was delivered to the skull from a height of 7 cm at a point just in front of the coronal suture and over the right hemisphere. Rats were sacrificed at 4 h after the onset of injury. Brain tissues were removed for biochemical and histopathological investigation. To date, no biochemical and histopathological changes of neurodegeneration in the frontal cortex after TBI in rats by CAPE treatment have been reported. The TBI significantly increased tissue malondialdehyde (MDA) levels, and significantly decreased tissue superoxide dismutase (SOD) and glutathione peroxidase (GPx) activities, but not tissue catalase (CAT) activity, when compared with controls. The administration of a single dose of CAPE (10 μmol/kg) 15 min after the trauma has shown protective effect via decreasing significantly the elevated MDA levels and also significantly increasing the reduced antioxidant enzyme (SOD and GPx) activities, except CAT activity. In the TBI group, severe degenerative changes, shrunken cytoplasma and extensively dark picnotic nuclei in neurons, as well as vacuolization indicating tissue edema formation. The morphology of neurons in the CAPE treatment group was well protected. The number of neurons in the trauma alone group was significantly less than that of both the control and TBI +CAPE treatment groups. The caspase 3 immunopositivity was increased in degenerating neurons of the traumatic brain tissue. Treatment of CAPE markedly reduced the immunoreactivity of degenerating neurons. TBI caused severe degenerative changes, shrunken cytoplasma, severely dilated cisternae of endoplasmic reticulum, markedly swollen mitochondria with degenerated cristae and nuclear membrane breakdown with chromatin disorganization in neurons of the frontal cortex. In conclusion, the CAPE treatment might be beneficial in preventing trauma-induced oxidative brain tissue damage, thus showing potential for clinical implications. We believe that further preclinical research into the utility of CAPE may indicate its usefulness as a potential treatment on neurodegeneration after TBI in rats.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
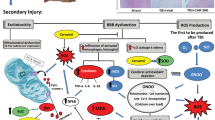
Traumatic brain injury (TBI) is one of the leading causes of death in children and young adults and results in a significant society burden throughout the world (Langlois et al. 2006; Marshall 2000a, b; Teasdale and Graham 1998). The pathology associated with TBI can be divided into two parts: the primary injury which is associated with the initial mechanical insult, and the secondary injury which is caused by an incompletely understood and complex cascade of physiology and biochemistry mechanism (Nortje and Menon 2004; Bramlett and Dietrich 2004; Gaetz 2004). Although they have significant impact on tissue necrosis and progressive neuronal cell death that follows after TBI, these secondary mechanisms of delayed post-traumatic neuronal cell death are still poorly understood. It is generally accepted that the overall pathology of TBI often associate with apoptosis of neurons (Clark et al. 1999; Keane et al. 2001). Both proapoptotic and anti-apoptotic signaling pathways can be activated after TBI (Keane et al. 2001; Stoica and Faden 2010). It is clear that the key effector of apoptosis is caspase-3, activation of which leads to programmed neuronal cell death after TBI (Erhardt 1996; Clark et al. 2000).
Oxygen free radicals and lipid peroxidation are believed to play crucial roles in secondary brain injury (Ikeda and Long 1990; McCall et al. 1987). Gray matter trauma causes tissue damage and increases Ca21 in the intracellular space. Ca21 then activates phospholipases and destroys membrane phospholipids, including arachidonic acid, which stimulates the generation of oxygen free radicals and lipid peroxidation. Previous reports of increased lipid peroxidation end products after head injury, and of the protective effects of free-radical scavengers and lipid antioxidants, are consistent with the proposed role of oxygen free radicals and lipid peroxidation in secondary brain injury (McCall et al. 1987; Marshall et al. 1998). There is extensive experimental support for the pathophysiological importance of early oxygen radical formation and cell membrane lipid peroxidation in the injured nervous system (Ikeda and Long 1990; McCall et al. 1987).
Caffeic acid phenethyl ester (CAPE) is an active component of honeybee propolis extracts and has been used for many years as a folk medicine. It has anti-inflammatory, immunomodulatory, antiproliferative, and antioxidant properties and have been shown to inhibit lipo-oxygenase activities as well as to suppress lipid peroxidation (Hepsen et al. 1997; Ilhan et al. 1999; Koltuksuz et al. 1999). However, to our best knowledge, there is no experimental study concerning the protective effects of CAPE against neuronal damage in the frontal cortex induced by TBI.
Therefore, the present study aimed to examine the neuronal damage of TBI on frontal cortex and to investigate the protective effects of CAPE against these effects at biochemical, light and electron microscopic, and immunohistochemical levels.
Materials and methods
Animals
Thirty-six adult male Sprague–Dawley rats (3 month-old), weighing 280–320 g, were used in this study. Rats were provided by the Experimental Research Center of the Medical Faculty of Trakya University. The rats were kept in a windowless animal quarter where temperature (21 ± 1°C) and illumination were automatically controlled (light on at 07 am and off at 09 pm: 14 h light/10 h dark cycle). Humidity ranged from 50 to 55%. The Ethical Committee of Trakya University approved all animal procedures and the experimental protocol. Efforts were made to minimize animal suffering and reduce the number of animals used in experimental groups. All animals received proper care according to the criteria outlined in the Guide for the Care and Use of Laboratory Animals as prepared by the National Academy of Sciences and published by the National Institutes of Health.
Surgical technique
Animals were divided randomly into three groups of 8 rats each: control, TBI and TBI + CAPE treatment groups. CAPE (10 μmol/kg/i.p.) was applied 15 min after trauma. Rats were anesthetized with an intraperitoneal injection of ketamine hydrochloride (70 mg/kg) and xylazin hydrochloride (7 mg/kg). The animals maintained spontaneous breathing. The heads of the animals were fixed into the head injury device with the chin resting firmly on the bottom plane. The application of the closed head injury was made according to the modified method described by Shapira et al. (1988). In TBI and TBI + CAPE treatment groups, the cranial impact was induced to a point on the right hemisphere 2 mm lateral to the midline and just in front of the coronal suture. The free fall occurred from a height of 7 cm, preferable for producing impact energy of 0.5 J over the skull. The rats were decapitated 4 h after the onset of the injury. Frontal brain tissues were removed for biochemical and histopathological investigation.
Biochemical procedures
Measurement of malondialdehyde (MDA) level
Tissue samples were frozen at) 70°C and irrigated well with a solution of NaCl (0.9%). By admixing it with KCl (1.5%), homogenization at a ratio of 1:10 was achieved. The DIAX9000 Homogenizer (Heidolph Instruments, Germany) was used to homogenize the tissue samples. The lipid peroxide level in the centrifuged tissue homogenates was measured according to the method described by Ohkawa et al. (1979). The reaction product was assayed spectrophotometrically (Shimadzu UV-1700, Japan) at 532 nm. The lipid peroxide level was expressed as the nmol of MDA per mg of cerebral tissue protein. Protein levels were measured according to the method described by Lowry et al. (1951).
Measurement of tissue superoxide dismutase (SOD) activity
The SOD activity was determined according to the method of Sun et al. (1988). The principle of the method is based on the inhibition of NBT reduction by the xanthine–xanthine oxidase system as a superoxide generator. Activity was assessed in the ethanol phase of the lyzate after 1.0 ml ethanol/chloroform mixture (5/3, v/v) was added to the same volume of sample and centrifuged. One unit of SOD was defined as the enzyme amount causing 50% inhibition in the NBT reduction rate. SOD activity was also expressed as units per mg protein.
Measurement of tissue glutathione peroxidase (GPx) activity
GPx activity was measured by the method of Paglia and Valentine (1967). The enzymatic reaction was initiated in a tube, which contained the following items: NADPH, reduced glutathione (GSH), sodium azide, and glutathione reductase by addition of H2O2 and the change in absorbance at 340 nm were monitored by a spectrophotometer. Activity was given in units per gram protein. All samples were assayed in duplicates.
Measurement of tissue catalase (CAT) activity
CAT activity was determined according to Aebi’s method (1974). The principle of the method was based on the determination of the rate constant (s−1, k) of the H2O2 decomposition rate at 240 nm. Results were expressed as k (rate constant) per mg protein.
Histological examinations
The brain specimens were individually immersed in 10% neutral buffered formalin, dehydrated in alcohol and embedded in paraffin. Sections of 5 μm were obtained, deparaffinized and stained with hematoxylin and eosin (H&E). The brain tissue was examined and evaluated in random order under blindfold conditions with standard light microscopy.
Immunohistochemical procedures
Harvested frontal brain tissues were fixed in 10% neutral buffered formalin, embedded in paraffin, and sectioned at 5 μm thickness. Immunohistochemical reactions were performed according to the ABC technique described by Hsu et al. (1981). Specific a rabbit polyclonal anti-caspase-3 antibody (Cat. #RB-1197-P, Neomarkers, USA) was applied at a dilution of 1:50. The procedure involved the following steps: (1) endogenous peroxidase activity was inhibited by 3% H2O2 in distilled water for 30 min; (2) the sections were washed in tap water for 30 min, and in distilled water for 10 min; (3) nonspecific binding of antibodies was blocked by incubation with normal goat serum (DAKOX 0907, Carpinteria, CA) with PBS, diluted 1:4; (4) sections were incubated with monoclonal mouse antisera against human insulin protein, diluted 1:400 for 2 h, and then at room temperature; (5) sections were washed in PBS 3·3 min; (6) sections were incubated with biotinylated anti-mouse IgG (DAKO LSAB 2 Kit; (7) sections were washed in PBS 3 × 3 min; (8) sections were incubated with ABC complex (DAKO LSAB 2 Kit); (9) sections. were washed in PBS 3 × 3 min; (10) peroxidase was detected with diaminobenzidine as substate; (11) sections were washed in tap water for 10 min and then dehydrated; (12) nuclei were stained with hematoxylin; and (13) sections were mounted in DAKO paramount.
Histological specimens of the frontal cortex were examined under light microscopy, with the examination carried out at a magnification of ×400 and the counts of neurons determined per square millimeter with the use of a standardized ocular grid. Apoptotic cells (caspase-3-immunopositive) were counted. The distribution of neurons was examined in the sections from the specimens were subjected by immunohistochemical method (caspase-3 antibody). Tissue sections were examined under light microscopy (×400) and the number of the neurons counted within random high-power fields using a Nikon Optiphot 2 light microscope incorporating a square graticule in the eyepiece (eyepiece × 10, objective × 40, a total side length of 0.25 μm2).
Electron microscopy
For electron microscopy, frontal cortex tissue specimens were fixed with 2.5% glutaraldehyde in 0.1 M sodium phosphate buffer (pH 7.2) for 3 h at 4°C, washed in the same buffer for 1 h at 4°C, and post-fixed with 1% osmium tetraoxide in sodium phosphate buffer for 1 h at 4°C. The tissues were then dehydrated in graded series of ethanol starting at 50% each step for 10 min and, after two changes in propylene oxide. The tissue specimens were embedded in araldite. Ultrathin sections were prepared with Mg-uranyl acetate and lead citrate for the electron microscopic (Jeol JEM 1010) evaluation.
Statistical analysis
All statistical analyses were carried out using SPSS statistical software (SPSS for windows, version 11.0). All data was presented in mean (±) standard deviations (SD). Differences in measured parameters among the three groups were analyzed with a Kruskal–Wallis test. Dual comparisons between groups exhibiting significant values were evaluated with a Mann–Whitney U-test. These differences were considered significant when probability was less than 0.05.
Results
Biochemical findings
The values of the MDA levels and SOD, GPx, and CAT activities are shown in Table 1 respectively. The TBI significantly increased the tissue MDA levels (P < 0.05) and significantly decreased the tissue SOD and GPx activities (P < 0.05) when compared with controls. The changes in the tissue CAT activity were not statistically significant. The administration of a single dose of CAPE (10 μmol/kg) 15 min after the trauma has shown protective effect via decreasing significantly (P < 0.05) the elevated MDA levels and also significantly (P < 0.05) increasing the reduced antioxidant enzyme activities (SOD and GPx), except CAT activity.
Histological findings
In control group, the morphology of neurons in the brain tissue was normal (Fig. 1a). In TBI group, the most consistent findings occurring in the histological tissue sections stained with hematoxylin-eosin were those indicating severe degenerative changes, shrunken cytoplasma and extensively dark picnotic nuclei in neurons, as well as vacuolization indicating tissue edema formation (Fig. 1b). In the CAPE-treated rat brains, the intensity of traumatic changes was less than in the traumatized group. The dark stained nucleus and the distorted nerve cells were mainly absent in the CAPE-treated traumatized rats. In this group, the severity of degenerative changes in the cytoplasma and especially in the nuclei of cells (Fig. 1c) was less than that in the TBI group.
Representative light microphotographs showing the morphology (a–c) of the frontal cortex tissue after trauma by hematoxylin-eosin. Brain tissue histology in control group was normal (a). Severe degenerative changes in neurons with shrunken cytoplasma and extensively dark picnotic nuclei, and vacuolization indicating tissue edema formation are seen in traumatized rats (b). In the CAPE-treated rats brain tissue, intensity of traumatic changes was less as compared to the traumatized group (c). (H&E, scale bar, 50 μm)
Immunohistochemical findings
Light micrographs showed apoptotic cortical neurons after trauma by caspase-3 immunohistochemistry (Fig. 2). The caspase-3 immunoreactivity of neurons was not evident in the frontal brain tissue in control group (Fig. 2a). The caspase-3 immunopositivity was increased in neurons of frontal brain tissue at 4 h following trauma (Fig. 2b; Table 2). Treatment of CAPE markedly reduced the immunoreactivity of degenerating neurons after trauma (Fig. 2c).
Light micrographs showing apoptotic cortical neurons after trauma by caspase-3 immunohistochemistry (a–c). The caspase-3 immunoreactivity of neurons was not evident in the frontal brain tissue in control group (a). The caspase-3 immunopositivity was increased in neurons of frontal brain tissue at 4 h following trauma (b). Treatment of CAPE markedly reduced the immunoreactivity of degenerating neurons after trauma (c). (Immunoperoxidase, hematoxylin counterstain, scale bar 50 μm)
Ultrastructural findings
In control group, the ultrastructure of neurons in the frontal cortex tissues was normal (Fig. 3a). In TBI group, the most consistent findings occurring in the ultrathin sections stained with Mg-uranyl acetate and lead citrate were those indicating severe degenerative changes, shrunken cytoplasma, severely dilated cisternae of endoplasmic reticulum and markedly swollen mitochondria resulting in loss of matrix density with degenerated cristae were observed in neurons of the frontal cortex. The nucleus of these cells seem to have increased evidence of nuclear membrane breakdown with chromatin disorganization and severely shrunken appearance, all signs of advanced cell death (Fig. 3b). Although CAPE treatment was effective in preventing the dilatation of endoplasmic reticulum, mitochondrial degeneration and irregularly shaped nuclei, the irregularly shaped chromatin clumps and moderately mitochondrial swollen was still observed in neurons (Fig. 3c).
Representative transmission electron microphotographs showing the ultrastructure of neurons in the frontal cortex tissues after trauma (a–c). (a) Control rats: The ultrastructure of cytoplasma and cytoplasmic organelles showed a normal appearance. (b) Traumatized rats: Disintegrating neuron containing shrunken cytoplasma, severely dilated cisternae of endoplasmic reticulum and markedly swollen mitochondria resulting in loss of matrix density in varying stages of destruction were observed. Typical necrotic neurons had smaller clumps of irregularly shaped, condensed chromatin with nuclear membrane breakdown. (c) Traumatized rats with CAPE: Although CAPE treatment was effective preventing the above mentioned findings, slightly dilated cisternae of endoplasmic reticulum was still observed. (thick arrow: nucleolus, N: nucleus, thin arrow: cisternae of endoplasmic reticulum, M: mitochondria) (scale bar, a: 1 μm, b:1 μm, c: 0.2 μm)
Discussion
Closed head trauma causes acute morphological changes and dysfunctions of neuronal and glial cells and elicits a series of secondary events after hours to days, causing necrotic and apoptotic cell death and impaired neurological function (Lewén et al. 2001; McIntosh et al. 1998a). Immediate early genes coding for transcription factors are activated, and locally generated autacoids, pro-inflammatory cytokines, and reactive oxygen species are formed and contribute to the secondary damage (McIntosh et al. 1998b).
Brain trauma causes primary and secondary injury to neural tissue (Siesjo 1993; Marshall 2000a, b; Ozsuer et al. 2005). Oxygen free radicals and lipid peroxidation are believed to play crucial roles (Ikeda and Long 1990; McCall et al. 1987). Indeed, a number of experimental studies suggest that excitatory amino acids and lipid peroxidation interact with each other and lead to cell death as a chain reaction (Baethmann et al. 1989; Scatton et al. 1991). Ozsuer et al. (2005) showed that MDA increases significantly in the injured hemisphere, starting from 30 min after the trauma and reaching a maximum level at 2 h, after which it gradually declines. Experimental and clinical studies also demonstrate early increases in MDA after head injury (Cristofori et al. 2001; Ustun et al. 2001; Vagnozzi et al. 1999). SOD represents the first line of defense against oxidative stres catalyzing the dismutation reaction of superoxide anion to hydrogen peroxide (McCord and Fridovich 1969), while GSH-Px converts peroxides into nontoxic forms, stable alcohols and water (Paglia and Valentine 1967). Therefore, SOD and GSH-Px constitute the major defense enzymes against superoxide radicals. In our study, treatment with CAPE increased the reduced antioxidant enzyme activities (SOD, CAT and GPx); however, the increase in the CAT activity was not significant.
CAPE is an active component of honeybee propolis extracts and it has been shown to be a pharmacologically safe compound with anti-inflammatory, anti-mitogenic, anti-carcinogenic, anti-oxidant and immunomodulatory effects (Nagaoka et al. 2002; Montpied et al. 2003; Russo et al. 2002). Previous experimental studies have shown that lipid peroxidation can be prevented by CAPE in spinal cord and kidney after ischemia–reperfusion (Ilhan et al. 1999; Ozyurt et al. 2001). Ozen et al. (2004) have shown that CAPE administration prevents cisplatin-induced nephrotoxicity in rats. Similarly, Fadillioglu et al. (2004) have reported that CAPE inhibits cardiotoxicity induced by doxorubicin in rat. Additionally, it has been reported that CAPE has protective effects against oxidative damage in various tissues (Kus et al. 2004; Ogeturk et al. 2005). Moreover, Fadillioglu et al. (2010) have reported that CAPE prevents hioacetamide-induced hepatic encephalopathy in rats. CAPE has these protective effects on the basis of anti-oxidant actions, but the exact mechanisms of anti-oxidant properties of CAPE are not known yet. However, it has been speculated that CAPE may affect transcription and/or translation of genes and gene products of anti-oxidant enzymes (Ozen et al. 2004). Although CAPE has antioxidant effects (Irmak et al. 2001; Ozyurt et al. 2001), its effect in TBI has not been investigated to date. The object of the present study was therefore to investigate the effects of CAPE on lipid peroxidation, antioxidant enzyme activity and neuronal protection in TBI injury of rat brain.
Our histological results demonstrate that even a TBI can cause diffused neuronal damage. These results correlate well with the literatures (Hicdonmez et al. 2006; Rink et al. 1995; Thomale et al. 2006; Shapira et al. 1988). In our study, the most consistent findings in histological sections of neuron regions amongst the TBI group involved severe degenerative changes, shrunken cytoplasma and extensively dark picnotic nuclei. The dark stained nucleus and the distorted nerve cells were mainly absent in the TBI group of CAPE-treated traumatized rats. In this group, the severity of degenerative changes in the cytoplasma and especially in the nuclei of cells was less than that in the TBI group.
In a study, Ozisik et al. (2007) observed there was severe damage of the cytoskeleton 24 h after trauma, that was characterized by mitochondrial swelling with loss of cristae and cytoplasmic edema, together with the development of empty zones located within myelin sheaths adjacent to the axon and loss of microtubules and neurofilaments. In our study, the ultrastructural examination of traumatized brain specimens clearly showed severe degenerative changes, shrunken cytoplasma, severely dilated cisternae of endoplasmic reticulum, markedly swollen mitochondria with degenerated cristae and nuclear membrane breakdown with chromatin disorganization in neurons of the frontal cortex. These changes was fairly well reduced after the administration of CAPE treatment.
Caspase-3 immunostaining was observed in neurons distributed around the lesioned area at 24 h after TBI and the number of immunopositive neurons increased at 48 and 72 h post-injury. In rats receiving prophylactic or post-injury treatment of aminoguanidine (AG), the number of caspase-3 immunopositive neurons was reduced in the cerebrum compared with those receiving saline injection (Lu et al. 2003). Cernak et al. (2002) have demonstrated an increased expression of active caspase-3 protein as early as 24 h after diffuse injury and persisting for almost 1 week. Moreover, the decrease in pro-caspase-3 levels suggests a conversion to the active form may have occurred as early as 4 h after injury. Thus, apoptosis seems activated early after diffuse traumatic brain injury and continues for at least 5 days post-trauma. While some caspases can be activated during events unrelated to apoptosis, caspase-3 activity is considered to be specific to the apoptotic pathway and thus a marker for apoptosis (Porter and Janicke 1999), Caspase-3 activity has been shown to be increased after ischemic insults, as well as following both experimental (Yakovlev et al. 1997; Clarket al. 2000) and clinical traumatic brain injury (Clarket al. 2000). The occurrence of apoptosis in the cortex and the hippocampus following experimental focal brain trauma was correlated with the induction of caspase-3 mRNA expression which showed significant elevation as early as 4 h after TBI continuing for at least 3 days posttrauma (Nicholson 1999). Moreover, Khan et al. (2007) have reported that CAPE treatment inhibited apoptotic cell death by down-regulating caspase 3 in rat brain following transient focal cerebral ischemia. In our study, the caspases-3 immunopositivity was increased in neurons of frontal brain tissue at 4 h following trauma. Treatment of CAPE markedly reduced the immunoreactivity of degenerating neurons after trauma. Our results support findings of the above-mentioned literature reports on apoptosis in terms of neuronal survival.
In conclusion, our findings suggest that a single dose of CAPE given 15 min after trauma might be effective on lipid peroxidation, antioxidant enzyme activity and neuronal protection in brain injury following TBI. We suggest that this would be more relevant clinically when considering the possible therapeutic use of CAPE in emergency conditions amongst human subjects with cerebral injuries.
References
Aebi H (1974) Catalase in vitro. Methods Enzymol 105:121–126
Baethmann A, Maier-Hauff K, Schürer L, Lange M, Guggenbichler C, Vogt W, Jacob K, Kempski O (1989) Release of glutamate and free fatty acids in vasogenic brain edema. J Neurosurg 70:578–591
Bramlett HM, Dietrich WD (2004) Pathophysiology of cerebral ischemia and brain trauma: similarities and differences. J Cereb Blood Flow Metab 24:133–150
Cernak I, Chapman SM, Hamlin GP, Vink R (2002) Temporal characterisation of pro- and anti-apoptotic mechanisms following diffuse traumatic brain injury in rats. J Clin Neurosci 9:565–572
Clark RS, Kochanek PM, Chen M, Watkins SC, Marion DW, Chen J, Hamilton RL, Loeffert JE, Graham SH (1999) Increases in Bcl-2 and cleavage of caspase-1 and caspase-3 in human brain after head injury. FASEB J 13:813–821
Clark RS, Kochanek PM, Watkins SC, Chen M, Dixon CE, Seidberg NA, Melick J, Loeffert JE, Nathaniel PD, Jin KL, Graham SH (2000) Caspase-3 mediated neuronal death after traumatic brain injury in rats. J Neurochem 74:740–753
Cristofori L, Tavazzi B, Gambin R, Vagnozzi R, Vivenza C, Amorini AM, Di Pierro D, Fazzina G, Lazzarino G (2001) Early onset of lipid peroxidation after human traumatic brain injury: a fatal limitation for the free radical scavenger pharmacological therapy. J Investig Med 49:450–458
Erhardt L (1996) Biochemical markers in acute myocardial infarction—the beginning of a new era? Eur Heart J 17:1781–1782
Fadillioglu E, Oztas E, Erdogan H, Yagmurca M, Sogut S, Ucar M, Irmak MK (2004) Protective effects of caffeic acid phenethyl ester on doxorubicin-induced cardiotoxicity in rats. J Appl Toxicol 24:47–52
Fadillioglu E, Gursul C, Iraz M (2010) Effects of caffeic acid phenethyl ester on thioacetamide-induced hepatic encephalopathy in rats. Prog Neuropsychopharmacol Biol Psychiatr 34(8):1440–1445
Gaetz M (2004) The neurophysiology of brain injury. Clin Neurophysiol 115:4–18
Hepsen IF, Bayramlar H, Gultek A, Ozen S, Tilgen F, Evereklioglu C (1997) Caffeic acid phenethyl ester to inhibit posterior capsule opacification in rabbits. J Cataract Refract Surg 23:1572–1576
Hicdonmez T, Kanter M, Tiryaki M, Parsak T, Cobanoglu S (2006) Neuroprotective effects of N-acetylcysteine on experimental closed head trauma in rats. Neurochem Res 31:473–481
Hsu SM, Raine L, Fanger H (1981) Use of avidin-biotin-peroxidase complex (ABC) in immunperoxidase techniques: a comparison between ABC and unlabeled antibody (PAP) procedures. J Histochem Cytochem 29:577–580
Ikeda Y, Long DM (1990) The molecular basis of brain injury and brain edema: the role of oxygen free radicals. Neurosurgery 27:1–11
Ilhan A, Koltuksuz U, Ozen S, Uz E, Ciralik H, Akyol O (1999) The effects of caffeic acid phenethyl ester (CAPE) on spinal cord ischemia/reperfusion injury. Eur J Cardiothorac Surg 16:458–463
Irmak MK, Koltuksuz U, Kutlu NO, Yağmurca M, Ozyurt H, Karaman A, Akyol O (2001) The effect of caffeic acid phenethyl ester on ischaemia-reperfusion injury in comparison with alpha-tocopherol in rat kidneys. Urol Res 29:190–193
Keane RW, Kraydieh S, Lotocki G, Alonso OF, Aldana P, Dietrich WD (2001) Apoptotic and antiapoptotic mechanisms after traumatic brain injury. J Cereb Blood Flow Metab 21:1189–1198
Khan M, Khan M, Elango C, Ansari MA, Singh I, Singh AK (2007) Caffeic acid phenethyl ester reduces neurovascular inflammation and protects rat brain following transient focal cerebral ischemia. J Neurochem 102(2):365–377
Koltuksuz U, Ozen S, Uz E, Aydinç M, Karaman A, Gültek A, Akyol O, Gürsoy MH, Aydin E (1999) Caffeic acid phenethyl ester prevents intestinal reperfusion injury in rats. J Pediatr Surg 34:1458–1462
Kus I, Colakoglu N, Pekmez H, Seckin D, Ogeturk M, Sarsilmaz M (2004) Protective effects of caffeic acid phenethyl ester (CAPE) on carbon tetrachloride-induced hepatotoxicity in rats. Acta Histochem 106:289–297
Langlois JA, Rutland-Brown W, Wald MM (2006) The epidemiology and impact of traumatic brain injury: a brief overview. J Head Trauma Rehabil 21:375–378
Lewén A, Skoglösa Y, Clausen F, Marklund N, Chan PH, Lindholm D, Hillered L (2001) Paradoxical increase in neuronal DNA fragmentation after neuroprotective free radical scavenger treatment in experimental traumatic brain injury. J Cereb Blood Flow Metab 21:344–350
Lowry OH, Rosebrough NJ, Farr AL, Randall RI (1951) Protein measurement with the folin phenol reagent. J Biol Chem 193:265–275
Lu J, Moochhala S, Shirhan M, Ng KC, Teo AL, Tan MH, Moore XL, Wong MC, Ling EA (2003) Neuroprotection by aminoguanidine after lateral fluid-percussive brain injury in rats: a combined magnetic resonance imaging, histopathologic and functional study. Neuropharmacology 44:253–263
Marshall LF (2000a) Epidemiology and cost of central nervous system injury. Clin Neurosurg 46:105–112
Marshall LF (2000b) Head injury: recent past, present, and future. Neurosurgery 47:546–561
Marshall LF, Maas AI, Marshall SB, Bricolo A, Fearnside M, Iannotti F, Klauber MR, Lagarrigue J, Lobato R, Persson L, Pickard JD, Piek J, Servadei F, Wellis GN, Morris GF, Means ED, Musch B (1998) A multicenter trial on the efficacy of using tirilazad mesylate in cases of head injury. J Neurosurg 89:519–525
McCall JM, Braughler JM, Hall ED (1987) Lipid peroxidation and the role of oxygen radicals in CNS injury. Acta Anaesthesiol Belg 38:279–373
McCord JM, Fridovich I (1969) Superoxide dismutase. An enzymic function for erythrocuprein (hemocuprein). J Biol Chem 244(22):6049–6055
Mcintosh TK, Juhler M, Wieloch T (1998a) Novel pharmacologic strategies in the treatment of experimental traumatic brain injury. J Neurotrauma 15:731–769
McIntosh TK, Saatman KE, Raghupathi R, Graham DI, Smith DH, Lee VM, Trojanowski JQ (1998b) The Dorothy Russell Memorial Lecture. The molecular and cellular sequelae of experimental traumatic brain injury: pathogenetic mechanisms. Neuropathol Appl Neurobiol 24:251–267
Montpied P, De Bock F, Rondouin G, Niel G, Briant L, Courseau AS, Lerner-Natoli M, Bockaert J (2003) Caffeic acid phenethyl ester (CAPE) prevents inflammatory stress in organotypic hippocampal slice cultures. Mol Brain Res 115:111–120
Nagaoka T, Banskota AH, Tezuka Y, Saiki I, Kadota S (2002) Selective antiproliferative activity of caffeic acid phenethyl ester analogues on highly liver-metastatic murine colon 26–L5 carcinoma cell line. Bioorg Med Chem 10:3351–3359
Nicholson DW (1999) Caspase structure, proteolytic substrates, and function during apoptotic cell death. Cell Death Differ 6:1028–1042
Nortje J, Menon DK (2004) Traumatic brain injury: physiology, mechanisms, and outcome. Curr Opin Neurol 17:711–718
Ogeturk M, Kus I, Colakoglu N, Zararsiz I, Ilhan N, Sarsilmaz M (2005) Caffeic acid phenethyl ester protects kidneys against carbon tetrachloride toxicity in rats. J Ethnopharmacol 97:273–280
Ohkawa H, Ohishi N, Yagi K (1979) Assay for lipid peroxides in animal tissues by thiobarbituric acid rection. Anal Biochem 95:351–358
Ozen S, Akyol O, Iraz M, Sogut S, Ozugurlu F, Ozyurt H, Odacı E, Yildirim Z (2004) Role of caffeic acid phenethyl ester, an active component of propolis, against cisplatin-induced nephrotoxicity in rats. J Appl Toxicol 24:27–35
Ozisik PA, Oruckaptan H, Ozdemir Geyik P, Misirlioglu M, Sargon MF, Kivanc K, Ozgen T (2007) Effect of erythropoietin on brain tissue after experimental head trauma in rats. Surg Neurol 68:547–555
Ozsüer H, Görgülü A, Kiriş T, Cobanoğlu S (2005) The effects of memantine on lipid peroxidation following closed-head trauma in rats. Neurosurg Rev 28:143–147
Ozyurt H, Irmak MK, Akyol O, Sogut S (2001) Caffeic acid phenethyl ester changes the indices of oxidative stress in serum of rats with renal ischemia-reperfusion injury. Cell Biochem Funct 19:259–263
Paglia DE, Valentine WN (1967) Studies on the quantitative and qualitative characterisation of erythrocyte glutathione peroxidase. J Lab Clin Med 70:158–169
Porter AG, Janicke RU (1999) Emerging roles of caspase-3 in apoptosis. Cell Death Differ 6:99–104
Rink A, Fung KM, Trojanowski JQ, Lee VM, Neugebauer E, McIntosh TK (1995) Evidence of apoptotic cell death after experimental traumatic brain injury in the rat. Am J Pathol 47:1575–1583
Russo A, Longo R, Vanella A (2002) Antioxidant activity of propolis: role of caffeic acid phenethyl ester and galangin. Fitoterapia 73:21–29
Scatton B, Carter C, Benavidas J, Giroux C (1991) N-methyl-D-aspartate receptor antagonists: a novel therapeutic perspective for the treatment of ischemic brain injury. Cerebrovasc Dis 1:121–135
Shapira Y, Shohami E, Sidi S, Soffer D, Freeman S, Cotev S (1988) Experimental closed head injury in rats: mechanical, pathophysiologic and neurologic properties. Crit Care Med 16:258–265
Siesjo BK (1993) Basic mechanisms of traumatic brain damage. Ann Emerg Med 22:959–969
Stoica BA, Faden AI (2010) Cell death mechanisms and modulation in traumatic brain injury. Neurotherapeutics 7:3–12
Sun Y, Oberley LW, Li Y (1988) A simple method for clinical assay of superoxide dismutase. Clin Chem 34:497–500
Teasdale GM, Graham DI (1998) Craniocerebral trauma: protection and retrieval of the neuronal population after injury. Neurosurgery 43:723–738
Thomale UW, Griebenow M, Kroppenstedt SN, Unterberg AW, Stover JF (2006) The effect of N-acetylcysteine on posttraumatic changes after controlled cortical impact in rats. Intensive Care Med 32:149–155
Ustun ME, Gürbilek M, Ak A, Vatansev H, Duman A (2001) Effect of magnesium sulfate on tissue lactate and malondialdehyde levels in experimental head trauma. Intensive Care Med 27:264–268
Vagnozzi R, Marmarou A, Tavazzi B, Signoretti S, Di Pierro D, del Bolgia F, Amorini AM, Fazzina G, Sherkat S, Lazzarino G (1999) Changes of cerebral energy metabolism and lipid peroxidation in rats leading to mitochondrial dysfunction after diffuse brain injury. J Neurotrauma 16:903–913
Yakovlev AG, Knoblach SM, Fan L, Fox GB, Goodnight R, Faden AI (1997) Activation of CPP32-like caspases contributes to neuronal apoptosis and neurological dysfunction after traumatic brain injury. J Neurosci 17:7415–7424
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kerman, M., Kanter, M., Coşkun, K.K. et al. Neuroprotective effects of Caffeic acid phenethyl ester on experimental traumatic brain injury in rats. J Mol Hist 43, 49–57 (2012). https://doi.org/10.1007/s10735-011-9376-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10735-011-9376-9