Abstract
Cognitive impairment is an important hallmark of dementia, but deterioration of cognition also occurs frequently in non-demented elderly individuals. In more than 3,000 non-demented persons, aged 45–99 years, from the population-based Rotterdam Study we studied cross-sectional age effects on cognitive function across various domains. All participants underwent an extensive cognitive test battery that tapped into processing speed, executive function, verbal fluency, verbal recall and recognition, visuospatial ability and fine motor skills. General cognitive function was assessed by the g-factor, which was derived from principal component analysis and captured 49.2 % of all variance in cognition. We found strongest associations for age with g-factor [difference in z-score −0.59 per 10 years; 95 % confidence interval (CI) −0.62 to −0.56], fine motor skill (−0.53 per 10 years; 95 % CI −0.56 to −0.50), processing speed (−0.49 per 10 years; 95 % CI −0.51 to −0.46), and visuospatial ability (−0.48 per 10 years; 95 % CI −0.51 to −0.45). In contrast, the effect size for the association between age and immediate recall was only −0.25 per 10 years (95 % CI −0.28 to −0.22), which was significantly smaller than the relation between age and fine motor skill (P < 0.001). In conclusion, in non-demented persons of 45 years and older, general cognition deteriorates with aging. More specifically, fine motor skill, processing speed and visuospatial ability, but not memory, are affected most by age.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Normal aging, as well as various clinical diseases, such as for example dementia, are accompanied by a deterioration of cognitive function. Even though memory decline is a hallmark of dementia, other cognitive domains, like executive function and processing speed are also often affected [1]. Many studies focus on persons in pre-clinical stages of dementia, i.e. mild cognitive impairment, and therefore are not always generalizable to community-dwelling elderly [2–4]. Still, cognitive aging has also been investigated extensively outside the context of dementia. Age effects have been documented on several cognitive domains, such as spatial orientation, inductive reasoning, memory, verbal and number skills, and in a variety of populations [5, 6]. However, different rates of cognitive decline across cohorts have also been reported and age effects on cognition could be altered over time due to changes in a population with regard to, for example, education, environment, health factors, or employment [7–9]. Therefore, more contemporary data on aging effects on cognition are needed.
In order to gain a comprehensive understanding of cognitive function in non-demented elderly, it is essential to study a broad range of cognitive domains in unselected community-dwelling persons. Furthermore, in addition to studying separate domains, it is equally important to investigate global cognition. The rationale for this is that cognition consists of a general underlying construct that is domain-independent and reflects an individual’s general cognitive function. This construct is linked to intelligence and can be quantified as a general cognitive factor, or g-factor. The g-factor is a stable concept, comprising the shared variance between cognitive tests, and can be interpreted as a common underlying factor to a variety of cognitive domains [10–12]. The g-factor has even been shown to be independent of cognitive test batteries used, and can therefore be easily generalized to other studies [13].
The aim of this study was to investigate patterns of cognitive function in middle-aged and elderly community-dwelling persons. We specifically studied both general cognition, using the g-factor, as well as specific cognitive domains.
Methods
Setting
The study is embedded within the Rotterdam Study, a population-based cohort study in middle-aged and elderly participants that started in 1990 and aims to investigate frequency, causes and determinants of chronic diseases [14]. The initial cohort encompassed 7,983 persons and was expanded by 3,011 persons in 2000 and by 3,932 persons in 2005. In-persons examinations take place every 3–4 years and consists of home interview and three center visits. The institutional review board of Erasmus MC approved the study and participants gave written informed consent.
Study population
Table 1 shows the number of participants from each cohort used in this study. Also, age at time of invitation to the study, sex and if available level of education are given for participants and non-participants to the study (Supplementary table 1). Additionally, we show age and sex of participants by year (Supplementary Table 2). The current cross-sectional study focuses on the period from January 1st 2008 onwards, because only then the full cognitive test battery in its current format was implemented. From the persons who responded to the invitation to participate in the study (n = 7,963), persons with a stroke (n = 325) or prevalent dementia (n = 73) were excluded from the sample used in this study. Sixteen persons had both a stroke and dementia and were excluded. For dementia, the assessment is based on a two-step procedure, which has been published before [15]. It involves screening by mini-mental state examination (MMSE), additional work-up by CAMDEX, informant interview, additional neuropsychological assessment, imaging, and final diagnosis in a consensus meeting led by a neurologist. For stroke, the assessment is based on self-report, family doctor files, and files of medical specialists, which are all discussed in a consensus panel led by a neurologist [16]. Also, neuroimaging is used if required.
Until February 29th 2012, cognitive tests were performed in 3,706 up to 4,176 persons. In case of technical problems, refusal of participation, physical limitations, or deviation from instructions, test results were excluded. This explains the range in number of subjects that performed various cognitive tests. The number of persons in the study who completed a valid cognitive test result on any of the tests used was 4,422 (Table 1). The complete cognitive test battery was available in 3,021 persons.
Cognitive test battery
During two separate center visits a cognitive test battery was administered, which included MMSE [17], Stroop test [18], letter-digit substitution task (LDST) [19], verbal fluency test [20], 15-word verbal learning test (15-WLT) [21], design organization test (DOT) [22] and Purdue pegboard test [23]. A description of the cognitive tests, test demands and latent skills measured is given in Table 2. Level of education was obtained and categorized into seven levels, ranging from primary to university education. Higher scores indicate a better performance on all cognitive tests, except for the Stroop task in which a higher score indicates a worse performance. Scores for the Stroop task were thus inverted for better comparison to other tests. The DOT is a test which is based on and highly correlated to WAIS-III block design, but is administered in two rather than 10 min and is less dependent on motor skills than the block design test [22]. Test score on the DOT has a range from 0 to 56 points for each subject.
G-factor [12]
To calculate a general cognitive factor (g-factor) we performed a principal component analysis incorporating color-word interference subtask of the Stroop test, LDST, verbal fluency test, delayed recall score of the 15-WLT, DOT and Purdue pegboard test. For tests with multiple subtasks we chose only one subtask in order to prevent highly correlated tasks distorting the factor loadings. Principal component analysis was performed on complete case data of 3,021 persons. The g-factor was identified as the first unrotated component of the principal component analysis and explained 49.2 % of all variance in the cognitive tests. This is a typical amount of variance accounted for by the g-factor [12].
Statistical analysis
To aid comparison across cognitive tests we first calculated z-scores for cognitive test scores. The MMSE score was not standardized due to its skewed nature. We used analysis of covariance to compare scores between men and women, adjusting for level of education. We used linear regression models to investigate the continuous association between age and cognitive test score, corrected for level of education. In additional analyses we used subcohort as an extra covariate to the linear regression model to test for cohort effects. We used Z tests to formally test differences of age effects between cognitive tests. We tested interaction effects between age and sex and explored non-linear effects of age on cognition. All analyses were performed using the statistical software package SPSS version 20.0 for Windows. Results are presented with 95 % confidence intervals (CI).
Results
Mean age was 71.9 years (SD = 9.7), with 57.5 % women (Table 3). Men scored better than women on the DOT, whereas women scored better on Stroop color naming, immediate recall, delayed recall and recognition parts of the 15-WLT, and Purdue pegboard test (Table 3). Pearson correlation coefficients between all cognitive test scores are shown in Supplementary table 3.
Figure 1 illustrates MMSE score and g-factor in 5-year strata of age. MMSE score stayed stable until age 70 and then showed a rapid decline. In contrast, the g-factor showed decline in scores already from age 45 onwards. The mean decline in g-factor per 10 year increase in age was −0.59 (95 % CI −0.62 to −0.56). For both MMSE score and g-factor we also found a quadratic effect of age (Table 4).
Age effects on global cognitive scores. The x-axis represents age per 5 years and the y-axis represents the MMSE-score or z-score of the g-factor. Error bars represent 95 % confidence intervals. Estimates are adjusted for level of education. MMSE mini mental state examination, g-factor general cognitive factor
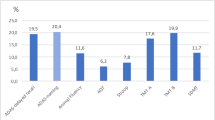
Figure 2 shows mean test scores in 5-year strata of age. We found the strongest decline for Purdue pegboard, LDST, DOT and Stroop interference task (Table 5). In contrast, smaller effects of age were found for 15-WLT immediate recall (−0.25 per 10 years; 95 % CI −0.28 to −0.22), delayed recall (−0.23 per 10 years; 95 % CI −0.26 to −0.20) and recognition (−0.09 per 10 years; 95 % CI −0.12 to −0.05). These differences in age effects between the memory subtasks versus Purdue pegboard, LDST, DOT and Stroop were confirmed by formal statistical testing (Z tests). For example, the age effects on the Purdue pegboard test or DOT were both significantly larger than the effect on immediate recall (P < 0.001). Still, the strongest effects of age were on the g-factor, rather than any individual cognitive test.
Finally, we found that for the Purdue pegboard test and LDST, age effects were stronger in women than men. Also, quadratic effects of age on cognition were found for the Stroop tasks, the LDST, verbal fluency, and the Purdue pegboard test. Adding subcohort as an extra covariate to the model did not reduce the effects of age on cognitive scores.
Discussion
In a large community-dwelling cohort of persons 45 years and older, we found that age strongly affects general cognitive function, measured by the g-factor. The effect of age on general cognitive function was already apparent from 45 years onwards. Investigating separate cognitive domains, we found strongest associations of age with fine motor skill, processing speed, and visuospatial ability.
Strengths of this study include the large community-dwelling study sample and availability of multiple cognitive tests. An important limitation to the interpretation of our results is the cross-sectional design. Also, relations between age and cognition could partly be influenced by cohort effects. However, differences in age effects across cognitive tests are comparable since all analyses were performed on the same group of persons. Another problem is that not all cognitive tests were completed by all participants to our study and that participants are younger and usually in better health compared to non-participants [24]. Therefore, in our g-factor analyses, we selected a sample with fully available cognitive data. We should keep in mind that this may have introduced some selection bias and has may reduce the generalizability of the results. We also note that in order to summarize the different cognitive tests into one g-factor, we selected six cognitive test variables under the assumption that these are representatives of various cognitive domains (executive function, processing speed, verbal fluency, memory, visuospatial ability, and fine motor skill), which are frequently used in cognitive aging research. Other studies may select different tests to construct a g-factor and will possibly get a slightly different outcome. However, it was previously found that g-factors constructed from variable test batteries result in factors that are highly correlated [13]. Thus, the g-factor is likely to be a stable concept. It is comprised of shared variance between tests, and can be interpreted as a factor which is common to a variety of cognitive domains.
In this study sample, we showed that the g-factor is affected already from age 45 onwards. Also, compared to the other cognitive tests in our battery, the g-factor was most strongly related to age. The strength of relation between age and cognition was consistent with those found by others [25, 26]. MMSE score only showed a decline from age 70 onwards. The MMSE is often used to test global cognitive function in older adults, yet it has frequently been criticised for its ceiling effect [27, 28]. In agreement with a large study of healthy elderly, we did not find strong effects of age on MMSE score [29].
Among our other cognitive tests, we found that fine motor skill, processing speed and visuospatial ability were most affected by age. In agreement with the observed relation between age and visuospatial ability, WAIS-III block design performance starts to decline from the mid-forties onward [12]. Other studies have also suggested a more prominent role for decline in visuospatial ability in aging research [30, 31]. One study reported a composite score of visuospatial ability to be a significant predictor of developing cognitive decline [2]. However, another large cohort study reported relatively small effects of age on visuospatial ability [4]. Already in the youngest age groups we found an effect of age on performance on the Purdue pegboard test. Population studies in the healthy elderly that looked into age effects on fine motor skills are scarce. The relatively large age effects on the LDST are in line with previous studies showing strong age effects on processing speed [9, 32]. Interestingly, these findings are supported by indirect evidence from neuroimaging studies which found that white matter declined faster than grey matter and white matter deterioration was associated with decline in motor skill and tasks of processing speed [33–35]. However, others concluded there is a relative stability of white matter volume in aging [36, 37]. The effect size we found relating age to memory was small compared to age effects on other cognitive scores. Again, this is in line with evidence showing that memory function is more dependent on grey matter which decreases gradually with aging [38, 39]. Furthermore, we found that women scored better on memory tests than men, which is in accordance with previous findings that women have better verbal memory than men [40, 41]. No difference in age effects on memory was found between men and women. It is expected that memory would be more strongly affected in dementia rather than normal aging. The exclusion of prevalent dementia cases from our study possibly contributed to the small negative effects of age on memory. However, there is a continuum between normal cognitive aging and dementia, and persons in the preclinical stages of dementia were not excluded from the study population. Normal cognitive aging research has often found that the more frontal brain functions such as attention and executive function are affected earlier than memory [42–44]. The relatively smaller effect on the verbal fluency test may reflect the fact that we used a category fluency test rather than a phonemic fluency test. Category fluency places a larger demand on memory performance rather than frontal lobe function [45, 46]. Furthermore, we found a stronger effect on the color-word interference subtask of the Stroop, compared to the reading and naming subtasks. The Stroop color-word interference task requires more cognitive control than the first two subtasks and is more dependent on executive function, specifically on attention and inhibition [19].
In conclusion, in persons of 45 years and older, age is most strongly related general cognitive function. Our findings also suggest that not memory, but fine motor skill, processing speed, and visuospatial ability are affected most by advancing age.
References
Albert MS. Changes in cognition. Neurobiol Aging. 2011;32(Suppl 1):S58–63.
Johnson DK, Storandt M, Morris JC, Galvin JE. Longitudinal study of the transition from healthy aging to Alzheimer disease. Arch Neurol. 2009;66(10):1254–9.
Hedden T, Oh H, Younger AP, Patel TA. Meta-analysis of amyloid-cognition relations in cognitively normal older adults. Neurology. 2013;80(14):1341–8.
Bennett DA, Wilson RS, Schneider JA, Evans DA, Beckett LA, Aggarwal NT, et al. Natural history of mild cognitive impairment in older persons. Neurology. 2002;59(2):198–205.
Tucker-Drob EM. Global and domain-specific changes in cognition throughout adulthood. Dev Psychol. 2011;47(2):331–43.
Ylikoski R, Ylikoski A, Keskivaara P, Tilvis R, Sulkava R, Erkinjuntti T. Heterogeneity of cognitive profiles in aging: successful aging, normal aging, and individuals at risk for cognitive decline. Eur J Neurol. 1999;6(6):645–52.
Finkel D, Reynolds CA, McArdle JJ, Pedersen NL. Cohort differences in trajectories of cognitive aging. J Gerontol Ser B Psychol Sci Soc Sci. 2007;62(5):P286–94.
Gerstorf D, Ram N, Hoppmann C, Willis SL, Schaie KW. Cohort differences in cognitive aging and terminal decline in the Seattle Longitudinal study. Dev Psychol. 2011;47(4):1026–41.
Finkel D, Reynolds CA, McArdle JJ, Pedersen NL. Age changes in processing speed as a leading indicator of cognitive aging. Psychol Aging. 2007;22(3):558–68.
Deary IJ, Johnson W, Starr JM. Are processing speed tasks biomarkers of cognitive aging? Psychol Aging. 2010;25(1):219–28.
Johnson DK, Storandt M, Morris JC, Langford ZD, Galvin JE. Cognitive profiles in dementia: Alzheimer disease vs healthy brain aging. Neurology. 2008;71:1783–9.
Deary IJ. Intelligence. Annu Rev Psychol. 2012;63:453–82.
Johnson W, te Nijenhuis J, Bouchard TJ Jr. Still just 1 g: consistent results from five test batteries. Intelligence. 2008;36(1):81–95.
Hofman A, van Duijn CM, Franco OH, Ikram MA, Janssen HL, Klaver CC, et al. The Rotterdam Study: 2012 objectives and design update. Eur J Epidemiol. 2011;26(8):657–86.
Schrijvers EM, Verhaaren BF, Koudstaal PJ, Hofman A, Ikram MA, Breteler MM. Is dementia incidence declining? Trends in dementia incidence since 1990 in the Rotterdam Study. Neurology. 2012;78(19):1456–63.
Wieberdink RG, Ikram MA, Hofman A, Koudstaal PJ, Breteler MM. Trends in stroke incidence rates and stroke risk factors in Rotterdam, the Netherlands from 1990 to 2008. Eur J Epidemiol. 2012;27(4):287–95.
Folstein MF, Folstein SE, McHugh PR. “Mini-mental state”: a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12(3):189–98.
Houx PJ, Jolles J, Vreeling FW. Stroop interference: aging effects assessed with the Stroop color-word test. Exp Aging Res. 1993;19(3):209–24.
Lezak MD, Howieson DB, Loring DW. Neuropsychological assessment. New York: Oxford University Press; 2004.
Welsh KA, Butters N, Mohs RC, Beekly D, Edland S, Fillenbaum G, et al. The consortium to establish a registry for Alzheimer’s disease (CERAD). Part V. A normative study of the neuropsychological battery. Neurology. 1994;44(4):609–14.
Bleecker ML, Bolla-Wilson K, Agnew J, Meyers DA. Age-related sex differences in verbal memory. J Clin Psychol. 1988;44(3):403–11.
Killgore W, Glahn D, Casasanto D. Development and validation of the design organization test (DOT): a rapid screening instrument for assessing visuospatial ability. J Clin Exp Neuropsychol. 2005;27:449–59.
Tiffin J, Asher EJ. The Purdue pegboard; norms and studies of reliability and validity. J Appl Psychol. 1948;32(3):234–47.
van Rossum CT, van de Mheen H, Witteman JC, Hofman A, Mackenbach JP, Grobbee DE. Prevalence, treatment, and control of hypertension by sociodemographic factors among the Dutch elderly. Hypertension. 2000;35(3):814–21.
Wilson RS, Beckett LA, Bennett DA, Albert MS, Evans DA. Change in cognitive function in older persons from a community population: relation to age and Alzheimer disease. Arch Neurol. 1999;56(10):1274–9.
Hayden KM, Reed BR, Manly JJ, Tommet D, Pietrzak RH, Chelune GJ, et al. Cognitive decline in the elderly: an analysis of population heterogeneity. Age Ageing. 2011;40(6):684–9.
Mungas D, Reed BR. Application of item response theory for development of a global functioning measure of dementia with linear measurement properties. Stat Med. 2000;19(11–12):1631–44.
Glymour MM, Tzourio C, Dufouil C. Is cognitive aging predicted by one’s own or one’s parents’ educational level? Results from the three-city study. Am J Epidemiol. 2012;175(8):750–9.
Starr JM, Deary IJ, Inch S, Cross S, MacLennan WJ. Age-associated cognitive decline in healthy old people. Age Ageing. 1997;26(4):295–300.
Jenkins L, Myerson J, Joerding JA, Hale S. Converging evidence that visuospatial cognition is more age-sensitive than verbal cognition. Psychol Aging. 2000;15:157–75.
Klencklen G, Despres O, Dufour A. What do we know about aging and spatial cognition? Reviews and perspectives. Ageing Res Rev. 2012;11(1):123–35.
Salthouse TA. The processing-speed theory of adult age differences in cognition. Psychol Rev. 1996;103(3):403–28.
Sullivan EV, Rohlfing T, Pfefferbaum A. Quantitative fiber tracking of lateral and interhemispheric white matter systems in normal aging: relations to timed performance. Neurobiol Aging. 2010;31:464–81.
Sachdev PS, Wen W, Christensen H, Jorm AF. White matter hyperintensities are related to physical disability and poor motor function. J Neurol Neurosurg Psychiatr. 2005;76(3):362–7.
Vernooij MW, Ikram MA, Vrooman HA, Wielopolski PA, Krestin GP, Hofman A, et al. White matter microstructural integrity and cognitive function in a general elderly population. Arc Gen Psychiatr. 2009;66:545–53.
Deary IJ, Corley J, Gow AJ, Harris SE, Houlihan LM, Marioni RE, et al. Age-associated cognitive decline. Br Med Bull. 2009;92:135–52.
Sullivan EV, Pfefferbaum A. Diffusion tensor imaging and aging. Neurosci Biobehav Rev. 2006;30(6):749–61.
Ikram MA, Vrooman HA, Vernooij MW, den Heijer T, Hofman A, Niessen WJ, et al. Brain tissue volumes in relation to cognitive function and risk of dementia. Neurobiol Aging. 2010;31(3):378–86.
Ikram MA, Vrooman HA, Vernooij MW, van der Lijn F, Hofman A, van der Lugt A, et al. Brain tissue volumes in the general elderly population. The Rotterdam Scan Study. Neurobiol Aging. 2008;29(6):882–90.
Herlitz A, Nilsson LG, Backman L. Gender differences in episodic memory. Mem Cognit. 1997;25(6):801–11.
Herlitz A, Yonker JE. Sex differences in episodic memory: the influence of intelligence. J Clin Exp Neuropsychol. 2002;24(1):107–14.
Buckner RL. Memory and executive function in aging and AD: multiple factors that cause decline and reserve factors that compensate. Neuron. 2004;44(1):195–208.
Raz N, Rodrigue KM. Differential aging of the brain: patterns, cognitive correlates and modifiers. Neurosci Biobehav Rev. 2006;30(6):730–48.
DeCarli C, Massaro J, Harvey D, Hald J, Tullberg M, Au R, et al. Measures of brain morphology and infarction in the framingham heart study: establishing what is normal. Neurobiol Aging. 2005;26:491–510.
Baldo JV, Schwartz S, Wilkins D, Dronkers NF. Role of frontal versus temporal cortex in verbal fluency as revealed by voxel-based lesion symptom mapping. J Int Neuropsychol Soc. 2006;12(6):896–900.
Schwartz S, Baldo J, Graves RE, Brugger P. Pervasive influence of semantics in letter and category fluency: a multidimensional approach. Brain Lang. 2003;87(3):400–11.
Acknowledgments
JN van der Geest was supported by the Princes Beatrix Fonds. The Rotterdam Study is sponsored by the Erasmus Medical Center and Erasmus University Rotterdam, The Netherlands Organization for Scientific Research (NWO), The Netherlands Organization for Health Research and Development (ZonMW), the Research Institute for Diseases in the Elderly (RIDE), The Netherlands Genomics Initiative, the Ministry of Education, Culture and Science, the Ministry of Health, Welfare and Sports, the European Commission (DG XII), and the Municipality of Rotterdam.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Hoogendam, Y.Y., Hofman, A., van der Geest, J.N. et al. Patterns of cognitive function in aging: the Rotterdam Study. Eur J Epidemiol 29, 133–140 (2014). https://doi.org/10.1007/s10654-014-9885-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10654-014-9885-4