Abstract
Background
Dextran sodium sulphate (DSS) is commonly used to induce intestinal inflammation in rodents. Despite its continuing importance as a model system for examining IBD pathogenesis, the mucosal and systemic immune responses have not been comprehensively documented.
Aims
The purpose of this study was to dissect functional and phenotypic changes in both immune compartments associated with acute and chronic DSS-induced colitis.
Methods
C57BL/6 mice were exposed to 3% DSS for 6 days followed by 20 days of water, and organs (spleens, MLN and colons) were harvested during both acute and chronic phases of colitis to examine innate and adaptive cell populations.
Results
As early as 1 day post DSS, significant changes in the percentage, distribution and activation status of all innate cell populations examined were noted. These striking differences continued in systemic and mucosal lymphoid tissues throughout the acute phase (days 5–12). Significantly, during the late acute and chronic phases T and B cells accumulated in the colon. In contrast, in the spleens of chronically inflamed mice T and B cells were significantly decreased whereas neutrophils, macrophages, and IL-6 and IL-17 positive cells were increased.
Conclusions
Our data provides important insights into the mucosal and systemic immune responses induced by DSS administration. Notably, we show that adaptive immune responses are induced during both acute and chronic colitis. This will facilitate a more informed and sophisticated use of this model both for investigating basic mechanisms of intestinal inflammation and for the evaluation of potential new therapeutic agents for IBD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Human inflammatory bowel disease (IBD), consisting of Crohn’s disease (CD) and ulcerative colitis (UC), is a multifactorial chronic condition characterised by acute exacerbations followed by remissions [1, 2]. Unfortunately, despite many years of extensive research implicating immune dysfunction, genetic susceptibility, and bacterial flora within the intestinal environment as possible factors associated with development of the disease, its pathogenesis is still poorly understood [3].
Animal models of intestinal inflammation have contributed greatly to our understanding of IBD pathogenesis and are essential for pre-clinical drug testing [4]. A widely used experimental model of colitis involves oral consumption of dextran sulphate sodium (DSS) dissolved in drinking water. This produces/provokes acute and chronic colitis in rodents by inducing inflammation and recruitment of immune cells and their subsequent activation directly through epithelial cell damage and/or altered macrophage function. As previously described, BALB/c mice develop an acute form of colitis when exposed to DSS, whereas the C57BL/6 mouse strain has been shown to develop acute colitis which later progresses to chronic inflammation [5].
The DSS model has many advantages including convenient induction of disease (administration in drinking water), low mortality risk (strain and batch dependent) as well as defined onset of disease. As a result, this model is widely used in the evaluation of new therapeutic strategies for IBD, in addition to unravelling basic immune pathways and associated intestinal pathology. Despite its continued use, this model is still not fully characterised with regard to both mucosal and systemic immune responses. Thus, in this study we comprehensively characterised the percentage, distribution, activation status and cytokine profile of innate and adaptive cell subsets within the colon, mesenteric lymph node (MLN) and the spleen during acute and chronic phases of DSS-induced colitis.
Materials and Methods
Animals
Female C57BL/6OlaHsD mice (10–12 weeks) from Harlan, UK were used in all animal experiments. All animals were given food and water ad libitum. Mice were sacrificed by cervical dislocation. Animal husbandry and experimental procedures were approved by the University College Cork ethics committee.
DSS-Induced Colitis
Mice were given 3% DSS (45 kDa; TdB Consultancy, Uppsala, Sweden) ad libitum in their drinking water for 6 days followed by water for the remainder of the study. We defined the stages of colitis as follows: days 1, 3, 5 and 8 as early colitis (characterised by considerable neutrophil influx into the colon), day 12 as late acute (reduction in neutrophil numbers and increase in adaptive cells), and transition into chronic colitis on day 25 (still significant numbers of T and B cells). Mice were divided into groups of 6–12 mice and were sacrificed at these time-points. In the control group (day 0), animals received only water. Fresh DSS solution was prepared daily. Body mass, fur texture, posture, stool consistency and faecal bleeding was measured. Disease activity index (DAI) comprised fur texture, animal posture and stool consistency.
Histology
Colons were removed and 3 cm of the distal colon was snap frozen in liquid nitrogen before being sectioned (6 μm). After fixing the slides for 5 min in ice-cold 3:1 ratio of acetone/ethanol, they were stained with haematoxylin and eosin according to standard histological procedures.
Immunofluorescent Staining
Frozen colon in 6-μm sections from mice sacrificed at the different time-points were stained with primary monoclonal antibody (mAb) as specified in Table 1. Where required purified mAb were revealed using the appropriate Alexa Fluor488- or 568-conjugated anti-Ig antibodies (Invitrogen, UK). Hoechst (Invitrogen) was used as a nuclear counterstain.
Flow Cytometry Analysis of Intracellular and Surface Antigens
Single cell suspensions from the spleen and MLN of individual mice were prepared. A final concentration of 2 × 105 cells/well were resuspended in blocking buffer (1 × PBS/1% BSA/0.05% sodium azide/1% rat, hamster and mouse serum). Then 50 μl of each mAb dye mix was added with incubation in the dark at 4°C for 30 min. The mAb used for flow cytometry are listed in Table 1. Cells were washed twice with blocking buffer and finally resuspended in 200 μl 1% paraformaldehyde. To perform flow cytometric analyses and measure relative fluorescence intensities a LSRII cytometer and BD Diva software (Becton Dickinson, UK) were used. For each sample 20,000–200,000 events were recorded. The percentage of cells labelled with each mAb was calculated in comparison with cells stained with isotype control antibody. Background staining was controlled by labelled isotype controls (BD Biosciences, Caltag and Serotec, UK) and FMO (fluorescence minus one). The results represent the percentage of positively stained cells in the total cell population exceeding the background staining signal. For determination of intracellular cytokine production by leukocytes, cells were incubated for 6 h at 37°C with BD Leukocyte Activation Cocktail with BD GolgiPlug (BD Biosciences). Cells were then fixed and saponin-permeabilised (Perm/fix solution, BD Biosciences) and incubated with mAb listed in Table 1 or isotypic control mAb. After 30 min cells were twice washed in permeabilisation buffer (BD Biosciences) and then analysed by flow cytometry as described above.
Statistical Analysis
Experimental results were plotted and analysed for statistical significance with Prism4 software (GraphPad Software Inc, CA, USA). P < 0.05 was considered statistically significant.
Results
Clinical and Macroscopic Signs of Inflammation
Percentage change in body weight, DAI, colon length, weight and histology of colonic sections of DSS treated and healthy animals are shown in Fig. 1. Liquid bloody stools and significantly poorer (P < 0.01) fur texture and posture (i.e. DAI) were observed in the colitis group after administration of 3% DSS for 4 days (Fig. 1a). Significant weight loss (P < 0.01) was observed by day 6 which peaked at day 11 of the study (Fig. 1b). Thereafter, mice administered DSS began to recover their original body weight and DAI. However, these clinical indices were still significantly lower (P < 0.01) than observed in control animals up to day 25. DSS treated animals had significantly shorter colons and significantly heavier (P < 0.01) distal colons 5 days post-DSS administration in comparison to those mice only receiving water (Fig. 1c,d). These macroscopic findings continued to be significantly different (P < 0.01) than those observed in control animals up until the end of the study. Finally, histological examination of the colonic sections from DSS-induced colitis mice showed typical inflammatory changes in colonic architecture, such as ulcerations, crypt dilation, and goblet cell depletion preferentially in the acute phase, as well as a mixed cell infiltration when compared to healthy control animals (Fig. 1e). These results are in agreement with previous studies using 3% DSS and C57BL/6 mice [5].
Clinical and macroscopic indices. C57BL/6 mice received DSS for 6 days followed by 20 days of water. Day 0 represents control/healthy mice (i.e., mice receiving only tap water throughout the study). a Disease activity index (DAI) score included stool consistency, fur texture and animal posture. b Daily changes in body weight in C57BL/6 mice. Body weight change was calculated by dividing body weight on the specified day by body weight at day 0 (starting body weight) and expressed as a percentage. c Colon length. d Colon weight (3 cm distal) determined at seven different time-points including acute (days 1, 3, 5, 8 and 12) and chronic phases (day 25) of colitis. Data represents the average of 6–12 individual mice ± SD. The difference in clinical indices, compared to healthy control is indicated by two asterisks (**) where P < 0.01 by the Kruskal-Wallis test followed by Dunn’s multiple comparison test. e Representative histology tissue sections of inflamed colons. Sections were stained with H&E from healthy control mice (D0) and mice that received DSS (D1, D3, D5, D8, D12 and D25). Original magnification ×20. Scale bar is 200 μm
DSS-Induced Colitis Induces Significant Changes in the Percentage and Activation Status of Immune Cell Populations Within Both the MLN and Spleen
To determine what immune cells are recruited and activated after DSS administration MLN and spleens were removed and analysed by flow cytometry. As described previously [5], spleens from mice treated with DSS had significantly more (P < 0.001) cells (50.2 ± 8.1 vs. 25.7 ± 6.6 × 106, P < 0.001) from day 12 onwards when compared to control animals. In addition, we also observed significantly more MLN cells from day 8 onwards in DSS-induced animals when compared to healthy controls (data not shown).
As shown in Fig. 2a, from as early as day 1 in DSS-treated mice we observed significant (P < 0.001) percentage changes in all cell types examined (i.e. CD11c+ dendritic cells [DC], F4/80+ macrophages [MΦ], CD19+ B cells and CD4+ and CD8+ T cells), with the exception of Ly6G+ neutrophils, in both the MLN and spleen when compared to healthy control mice. We also determined the activation status of the various immune populations including CD69, CD86 and MHC II in spleens and MLN from control and DSS exposed (Fig. 3). We did not observe an increase in the percentage and CD69 mean fluorescence intensity (MFI) of Ly6G+ cells until 3 days post-DSS administration within the spleen, where percentages continued to be significantly higher (P < 0.01) than control animals up until the end of the study. Within the MLN we first noted a significant increase (P < 0.001) in CD69 MFI on days 5 and 8, but significant decrease in the percentage of Ly6G+ cells on day 8 (which was also seen in the spleen); however, at day 25 neutrophil percentages were significantly higher (P < 0.001) than control animals. DSS-treated animals were observed to have significantly less (P < 0.01) CD11c+ DC within their spleens from day 5 up until day 12, but increased (P < 0.05) MHC II MFI during early acute colitis. Within the MLN, we observed significantly more (P < 0.05) CD11c+ cells with increased MHC II MFI on their surface also during acute colitis. F4/80+ MΦ percentages were significantly lower (P < 0.001) 1 day post-DSS administration within the spleen when compared to healthy controls. Thereafter, we observed significant increases (P < 0.05) in the percentages and MFI of MHC II on F4/80+ cells in both the spleen and MLN up until day 25. For CD19+ B cells we observed significant increases (P < 0.001) in percentage, during the entire study, and increased (P < 0.05) CD86 MFI on days 5, 8 and 12, within the MLN of DSS-treated animals when compared to healthy mice. Conversely, within the spleens of colitis mice we noted a significant decrease (P < 0.001) in B cell percentage on day 25, but a significant increase (P < 0.05) in CD86 MFI on day 12. Finally, for T cells (both CD4+ and CD8+) we observed significantly lower percentages (P < 0.001) within MLN of mice administered with DSS during both acute (days 1, 3, 8 and 12) and chronic phases (day 25) of colitis. Within the spleens of DSS-treated animals we first observed a significant increase (P < 0.001) in T cells percentages (day 1 for CD8+ cells and day 3 for CD4+ cells). CD8+ T cells were found to have significantly higher (P < 0.001) MFI of CD69 within the MLN of DSS-treated mice as early as days 1, 3 and 12; we also observed this in the splenic population on days 3 and 12. We observed a steady decline in both T cell populations were they reached their lowest percentage at the end of the study on day 25 when compared to control animals. This dramatic decrease in adaptive immune cells (both B and T cells) and conversely dramatic increase in percentage of both neutrophil and MΦ from the spleens of chronic colitis animals can be seen in Fig. 2b from their scatter profile. Whereas none of the innate immune populations were activated in the lymphoid tissues of chronic colitis animals, we did observe that both CD4+ and CD8+ T cells had significantly higher (P < 0.001) MFI of CD69 at day 25 (Fig. 3).
Percentage of immune cells in spleen and MLN during DSS colitis. a Cells were isolated from spleens and MLN of DSS-treated mice or healthy control C57BL/6 mice on days 1, 3, 5, 8, 12 and 25, and stained with flurochrome-labelled mAb. They were analysed by flow cytometry in which 20,000 events were recorded. Data represents the mean percentage of Ly6G (neutrophils), CD11c (DC), F4/80 (MΦ), CD19 (B cells), CD4 and CD8 (T cells) positive cells at different time-points during DSS colitis. Error bars show SD from between 6 and 12 mice. The asterisks (*) indicate significant values of * P < 0.05, ** P < 0.01, and *** P < 0.001 as determined by one-way ANOVA followed by Bonferroni’s multiple comparison test compared to controls (day 0). b Representative side-scatter (SSC) and forward-scatter (FSC) plots shown are representative of six mice on day 25 of study from both DSS-treated and control mice
Activation status of leukocyte populations in DSS-induced colitis. Cells were isolated from the spleens and MLN of control (day 0) and DSS-treated animals on days 1, 3, 5, 8, 12 and 25. Data represents the mean percentage of expression ± SD from groups of 6–12 individual mice. The mean percentage values indicating the frequency of CD69+ were calculated individually for each gated cell population expressing the corresponding surface markers (Ly6G+, CD4+ and CD8+). CD86 marker gates were set on the CD19+ population and MHC II was calculated for CD11c+ and F4/80+ cells. Cells were then analysed for expression of activation markers on Ly6G+, CD11c+, F4/80+, CD4+ and CD8+ cells. Data are presented as percent MFI change of DSS-treated mice over control mice MFI ± SD from groups of 6–12 individual mice. The asterisks (*) indicate significant values of * P < 0.05, ** P < 0.01, and *** P < 0.001 as determined by one-way ANOVA followed by Bonferroni’s multiple comparison test compared to controls (day 0)
Number of Cytokine Producing Cells During Acute and Chronic Phases of Colitis
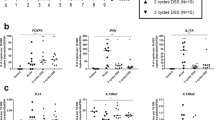
Cytokine positive cells were characterised by flow cytometry using stimulated spleen and MLN cells recovered from both control and DSS-treated mice on days 1, 3, 8, 12 and 25 (Table 2). During DSS colitis the percentage of cells producing TNF-α was found to be significantly higher from day 1 in both tissues. This continued for the reminder of the study within the MLN, but numbers returned to control levels within the spleens of DSS treated mice from day 12 onwards. The total percentage of IL-6+ cells was significantly higher (P < 0.01) in both the spleen and MLN at every time-point, with the exception of day 1, when compared to healthy controls. The percentage of IL-17+ cells was also significantly higher (P < 0.01) at day 1 within both organs of DSS-treated mice, which was again observed at days 12 and 25. Notably at day 8 we found that levels of IL-17 producing cells were significantly lower (P < 0.01) than those seen in control mice within the MLN of DSS treated animals. IFN-γ producing cells were found to be significantly higher (P < 0.05) from as early as day 1 post-DSS up until day 8 in both the spleens and MLN, returning to control levels on days 12 and 25. For IL-10+ cells we observed significant increases in percentages by day 3 up until day 12 while levels of IL-4+ cells were only observed to be significantly higher (P < 0.001) on day 12 when compared to healthy controls in both lymphoid tissues.
Number and Distribution of Colonic Immune Cell Populations During DSS-Induced Colitis
In order to identify the colonic cellular populations involved during DSS colitis, serial frozen colonic sections of control (day 0) and DSS-treated mice were investigated for the distribution (Fig. 4a) and number (Fig. 4b) of Ly6G+ neutrophils, CD11c+ DC, F4/80+ MΦ, CD3+ T cells and CD19+ B cells at the different time-points.
In situ visualisation and morphometry analysis of leukocytes within the colon during DSS colitis. C57BL/6 mice were treated with water (healthy controls) or DSS. Colons were collected on days 1, 3, 5, 8, 12 and 25. Tissue sections from six individual mice were analysed at each time-point by fluorescent microscopy. a Serial frozen sections (6 μm) were fixed in acetone/ethanol and stained for Ly6G, CD11c or F4/80 (green), and co-stained with CD3 (red) and nuclei (blue). Sections were also stained with CD19 (red) and nuclei (blue). A representative picture for each group is shown. (Original magnification, ×20). Scale bar is 200 μm. BZ stands for B cell zone, E indicates epithelium and SM shows submucosa. b Bars represent means ± SD of the total number of positive cells per field of view. Values are based on 3–4 mice/time-point, measuring 5–10 fields at ×20 magnification of distal colons. The asterisks (*) indicate significant values of * P < 0.05, ** P < 0.01, and *** P < 0.001 as determined by one-way ANOVA followed by Bonferroni’s multiple comparison test compared to controls (day 0)
In control animals, few neutrophils were present and those observed were within the lamina propria (LP) of the colon. After DSS administration we noted that neutrophils were located in the LP, but also in the submucosa and crypts. Neutrophils were also more closely associated with T cells; this interaction was most apparent by day 8 and 12 in the epithelium. Neutrophils did not co-localise to B cell zones (BZ) at any time-point and on day 25 these cells were again located within the LP. In control mice, colonic DC formed a loose network throughout the crypts mostly near the luminal surface (Fig. 4a). By day 1 and up until day 5 post-DSS, DC lined the basement membrane of colonic crypts and were also loosely located within the LP and submucosa. Indeed, DC were observed to be in closer proximity to T cells as well as co-localising to within BZ. On day 8 we noted considerable destruction of colonic crypts and diffuse infiltration of DC throughout the colon. By day 12 many DC located along with T cells into BZ, whose number and size were highly increased. By day 25, DC were localised towards the top of crypts, although many DC were still seen within BZ. In contrast to the DC population, MΦ were mostly located within the colonic LP of control mice. From day 1 onwards we observed that along with LP associated MΦ, some cells were now located within the submucosa and lined colonic crypts. On day 8 the MΦ population were distributed throughout the damaged colon and were in close contact to T cells. As described for neutrophils, very few MΦ were located within the large number of BZ observed on day 12 and those present were found to mostly locate to the LP and within the basement membrane of crypts. On day 25, MΦ distribution was similar to that observed in control animals, i.e. within the LP. As already discussed the vast majority of B cells were found in BZ after DSS administration. However, a very small number were located within the crypts and the LP. In control animals T cells were located throughout the basement membrane of the crypts and were not associated with any of the other cell types tested. As already highlighted, the colonic T cell population in those animals receiving DSS were observed in different areas of the colon including the LP and submucosa and were closely associated with other cellular populations.
Morphometry analysis demonstrated that from as early as 1 day post-DSS administration the number of neutrophils was significantly increased within the distal colons when compared to healthy controls (Fig. 4b). Numbers continued to be significantly higher at all time-points examined, reaching their peak at day 8. Colonic DC and MΦ numbers were found to be significantly greater than those observed in control animals from day 5 onwards, where MΦ numbers reached their highest at day 8 and DC reached their peak by day 12. Examining adaptive immune cell populations we observed that both B cells and T cell numbers were significantly higher than those seen in healthy controls from day 8 onwards, both peaking on day 12, with numbers still remaining significantly higher on day 25.
Discussion
Oral administration of DSS to rodents induces a colonic inflammation with many similarities to human IBD and has become a useful tool for evaluating disease pathophysiology and pre-clinical studies. The model is easily induced and reproducible and follows a predicable time course that is similar to the clinical inflammatory course during acute phases of colitis as in human IBD patients. However, even though this model has been extensively used, an integrated picture of immune responses engendered during DSS-induced colitis has not been established. Our study addresses these gaps in knowledge by characterising changes in defined cell populations, their activation status and cytokine profile during both acute and chronic phases following DSS administration. This study expands our current understanding of the nature of immune responses generated in both the systemic and mucosal compartments during DSS-induced colitis. This is crucial for our evolving understanding of immune dysfunction in IBD and the continuing application of this model for screening new IBD therapeutics.
DSS is a physical agent with an intrinsic capacity to alter the epithelial cell barrier, causing normal mucosal microflora substances to activate mucosal innate cell populations, which in turn produce immunomodulatory cytokines [6–8]. Therefore, it is no surprise that DC, MΦ and neutrophils appear to be the first wave of cellular responders as early as 1 day post DSS administration within the organs tested. We observed a significant early influx of neutrophils into the colon which correlated with the severe colonic destruction observed in these mice at day 8 possibly through their cytokine production and respiratory burst activity [9, 10]. Indeed, disease activity in patients with IBD is linked to an influx and transepithelial migration of neutrophils into the mucosal epithelium (cryptitis) and subsequently into the intestinal lumen resulting in the formation of so-called crypt abscesses, which we also observed in DSS-treated mice [11–13]. During early acute colitis we also observed neutrophils co-localising with T cells, suggesting their involvement in activation of this adaptive population and possibly furthering the damage of the colonic mucosa. Whereas we observed a continuing reduction in colonic neutrophils, which coincides with improved colonic healing on days 12 and 25, we surprisingly detected a substantial increase in the percentages of splenic and MLN neutrophils. This may correlate to the changing cytokine profile observed at these time-points (high IL-17 and IL-6) as previous studies have shown that IL-17 production from lymphocytes contributes to neutrophil recruitment through stimulation of neutrophil-mobilising cytokines such as IL-6 and chemokines [14–16].
Antigen presenting DC are inducers and regulators of immune responses. As early as day 1 post DSS we observed a significant influx of DC into the MLN which was also accompanied by their increased activation, which is similar to that observed in UC patients and animal models of colitis [17, 18]. From day 5 onwards we see a steady decline in both MLN and splenic DC populations, although this might signify their movement into the colon as we observe concurrent significant increases within this tissue also from these time-points. In contrast to the other innate population examined, DC appear to be the main cell type involved in interactions with B cells. Interactions of these DC within BZ would be expected to lead to the generation of plasma cells and consequent antibody production. In addition, the observed significant increase in IL-6+ cells throughout the study also enforces this idea as IL-6 is a known potent inducer of B cell differentiation and antibody class switching [19]. Indeed, a higher detection of plasma cells within the LP is evident in human IBD patients and in this model [5, 20, 21].
MΦ play an essential role in maintaining homeostasis and epithelial renewal in the normal intestine. However, intestinal MΦ from IBD patients differ markedly from those present physiologically, exhibiting heightened inflammatory and bactericidal activities, and contributing to the tissue damage [22]. Influx of this cellular population to the colon, and significant increases and activation status within both the spleens and MLN correlates with increasing tissue damage. In addition, MΦ appeared to be in close contact to T cells within the colon of colitis mice from day 8, highlighting the activation role MΦ may be playing which in turn may lead to further destruction of the colonic mucosa. Whereas we observed mucosal MΦ populations falling from day 12 onwards within the systemic compartment, numbers continued to increase until they reached their peak on day 25; however, these cells do not appear to be activated. This accumulation of inactivated MΦ may correlate with the reduction of IL-10+ cells within the spleen from day 12 onwards as IL-10 is known to suppress MΦ as well as neutrophil accumulation within healthy tissues by induction of apoptosis [23, 24].
Whereas we observe a steady decrease of colonic neutrophil and MΦ numbers from day 8 onwards, T cell levels steadily increased reaching their peak on day 12 and remaining high on day 25. This influx of T cells into the colon of DSS mice at these time-points appears to correlate with a concurrent decrease of both splenic and MLN T cells. In addition, their elevated CD69 profile suggests that these T cells are activated before trafficking to the colon. Although we observe epithelial regeneration from day 12 onwards the architecture had still not recovered to that observed in control mice. The significant levels of colonic T cells suggest they may be playing a positive role during the chronic regenerative phase of DSS-induced acute colitis. In agreement with this recent work in DSS-induced lymphotoxin beta receptor deficient mice indicates a protective role for T cells in DSS-induced intestinal inflammation [25]. These T cells may be producing IL-6 and IL-17 (TH17 phenotype) as these were the only cytokines tested that were still significantly increased at these later time-points [5]. Both IL-6 and IL-17 are normally associated with driving pro-inflammatory responses; however, recent data also suggest their involvement in mediating healing processes [26–28]. Previous studies have suggested that contributions from the adaptive immune system appear to be secondary in this model, since T and B lymphocyte-deficient severe combined immunodeficiency (Prkdc scid /Prkdc scid) mice also develop DSS-induced lesions [29]. However, this was based on the finding of acute colitis induced by seven days of DSS, whereas in chronic colitis induced by multiple cycles of DSS or in the recovery phase of exaggerated colitis induced by DSS, T cells play an important role [25, 30]. It is also important to note that these studies were performed in a more resistant background, whereas our study has investigated responses in the more susceptible C57BL/6 mouse [5, 29]. Our data clearly indicates a role for both B and T cells in DSS-induced chronic colitis as observed through the increased colonic numbers and heightened activation status. Thus, DSS-induced colitis is mediated by different mechanisms corresponding to innate and adaptive immune responses at different phases of the disease.
In conclusion, we provide new insights into the interplay between innate and adaptive immune response within both systemic and mucosal tissues that result in localised inflammation at mucosal surfaces in the DSS-induced colitis model. Characterisation of the immune response mechanisms throughout DSS-induced colitis will increase the understanding and utility of this popular IBD animal model. This will ultimately provide researchers with a clearer and more informed platform for studying basic immune mechanisms and assessment of new therapeutics for this increasingly important inflammatory disease. Notably, we show that adaptive immune populations are activated during both acute and chronic phases of colitis and for the first time we observed that innate cellular populations accumulate within the systemic compartment during chronic stages of colitis. Future studies will address the significance of these changes in the distribution of immune populations for the pathophysiology of IBD.
References
Korzenik JR, Podolsky DK. Evolving knowledge and therapy of inflammatory bowel disease. Nat Rev Drug Discov. 2006;5:197–209.
Cho JH. The genetics and immunopathogenesis of inflammatory bowel disease. Nat Rev. 2008;8:458–466.
Xavier RJ, Podolsky DK. Unravelling the pathogenesis of inflammatory bowel disease. Nature. 2007;448:427–434.
Byrne FR, Viney JL. Mouse models of inflammatory bowel disease. Curr Opin Drug Discov Dev. 2006;9:207–217.
Melgar S, Karlsson A, Michaelsson E. Acute colitis induced by dextran sulfate sodium progresses to chronicity in C57BL/6 but not in BALB/c mice: correlation between symptoms and inflammation. Am J Physiol. 2005;288:G1328–G1338.
Ni J, Chen SF, Hollander D. Effects of dextran sulphate sodium on intestinal epithelial cells and intestinal lymphocytes. Gut. 1996;39:234–241.
Kitajima S, Takuma S, Morimoto M. Changes in colonic mucosal permeability in mouse colitis induced with dextran sulfate sodium. Experimental Anim. 1999;48:137–143.
Okayasu I, Hatakeyama S, Yamada M, Ohkusa T, Inagaki Y, Nakaya R. A novel method in the induction of reliable experimental acute and chronic ulcerative colitis in mice. Gastroenterology. 1990;98:694–702.
Kuhl AA, Kakirman H, Janotta M, et al. Aggravation of different types of experimental colitis by depletion or adhesion blockade of neutrophils. Gastroenterology. 2007;133:1882–1892.
Farooq SM, Stillie R, Svensson M, Svanborg C, Strieter RM, Stadnyk AW. Therapeutic effect of blocking CXCR2 on neutrophil recruitment and dextran sodium sulfate-induced colitis. J Pharmacol Exp Ther. 2009;329:123–129.
Teahon K, Smethurst P, Pearson M, Levi AJ, Bjarnason I. The effect of elemental diet on intestinal permeability and inflammation in Crohn’s disease. Gastroenterology. 1991;101:84–89.
Keshavarzian A, Price YE, Peters AM, Lavender JP, Wright NA, Hodgson HJ. Specificity of indium-111 granulocyte scanning and fecal excretion measurement in inflammatory bowel disease—an autoradiographic study. Dig Dis Sci. 1985;30:1156–1160.
Costa F, Mumolo MG, Ceccarelli L, et al. Calprotectin is a stronger predictive marker of relapse in ulcerative colitis than in Crohn’s disease. Gut. 2005;54:364–368.
Miyamoto M, Prause O, Sjostrand M, Laan M, Lotvall J, Linden A. Endogenous IL-17 as a mediator of neutrophil recruitment caused by endotoxin exposure in mouse airways. J Immunol. 2003;170:4665–4672.
Laan M, Prause O, Miyamoto M, et al. A role of GM-CSF in the accumulation of neutrophils in the airways caused by IL-17 and TNF-alpha. Eur Respir J. 2003;21:387–393.
Lee JW, Wang P, Kattah MG, et al. Differential regulation of chemokines by IL-17 in colonic epithelial cells. J Immunol. 2008;181:6536–6545.
Malmstrom V, Shipton D, Singh B, et al. CD134 l expression on dendritic cells in the mesenteric lymph nodes drives colitis in T cell-restored SCID mice. J Immunol. 2001;166:6972–6981.
Niess JH. Role of mucosal dendritic cells in inflammatory bowel disease. World J Gastroenterol. 2008;14:5138–5148.
Hirano T. Interleukin-6 and its relation to inflammation and disease. Clin Immunol Immunopathol. 1992;62:S60–S65.
Dorn I, Schlenke P, Mascher B, Stange EF, Seyfarth M. Lamina propria plasma cells in inflammatory bowel disease: intracellular detection of immunoglobulins using flow cytometry. Immunobiology. 2002;206:546–557.
Siegmund B, Zeitz M. Clinical aspects of inflammatory bowel disease. Eur J Immunol. 2009;39:2026–2030.
Heinsbroek SE, Gordon S. The role of macrophages in inflammatory bowel diseases. Expert Rev Mol Med. 2009;11:e14.
Keel M, Ungethum U, Steckholzer U, et al. Interleukin-10 counterregulates proinflammatory cytokine-induced inhibition of neutrophil apoptosis during severe sepsis. Blood. 1997;90:3356–3363.
Wang ZQ, Bapat AS, Rayanade RJ, Dagtas AS, Hoffmann MK. Interleukin-10 induces macrophage apoptosis and expression of CD16 (FcgammaRIII) whose engagement blocks the cell death programme and facilitates differentiation. Immunology. 2001;102:331–337.
Jungbeck M, Stopfer P, Bataille F, Nedospasov SA, Mannel DN, Hehlgans T. Blocking lymphotoxin beta receptor signalling exacerbates acute DSS-induced intestinal inflammation—opposite functions for surface lymphotoxin expressed by T and B lymphocytes. Mol Immunol. 2008;45:34–41.
Lin ZQ, Kondo T, Ishida Y, Takayasu T, Mukaida N. Essential involvement of IL-6 in the skin wound-healing process as evidenced by delayed wound healing in IL-6-deficient mice. J Leukoc Biol. 2003;73:713–721.
O’Connor W Jr, Kamanaka M, Booth CJ, et al. A protective function for interleukin 17a in T cell-mediated intestinal inflammation. Nat Immunol. 2009;10:603–609.
Ogawa A, Andoh A, Araki Y, Bamba T, Fujiyama Y. Neutralization of interleukin-17 aggravates dextran sulfate sodium-induced colitis in mice. Clin Immunol. 2004;110:55–62.
Dieleman LA, Ridwan BU, Tennyson GS, Beagley KW, Bucy RP, Elson CO. Dextran sulfate sodium-induced colitis occurs in severe combined immunodeficient mice. Gastroenterology. 1994;107:1643–1652.
Dieleman LA, Palmen MJ, Akol H, et al. Chronic experimental colitis induced by dextran sulphate sodium (DSS) is characterized by Th1 and Th2 cytokines. Clin Exp Immunol. 1998;114:385–391.
Acknowledgments
The Alimentary Pharmabiotic Centre is a research centre funded by Science Foundation Ireland (SFI), through the Irish Government’s National Development Plan. The authors and their work were supported by SFI (grant no.s 02/CE/B124 and 07/CE/B1368) and by additional grants from industry including GlaxoSmithKline Ltd.
Conflict of interest statement
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hall, L.J., Faivre, E., Quinlan, A. et al. Induction and Activation of Adaptive Immune Populations During Acute and Chronic Phases of a Murine Model of Experimental Colitis. Dig Dis Sci 56, 79–89 (2011). https://doi.org/10.1007/s10620-010-1240-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-010-1240-3