Abstract
Background
Helicobacter pylori infection is known to be associated with chronic atrophic gastritis, peptic ulcers, and gastric malignancies. However, the effects of other Helicobacter species have not been investigated extensively. In mice, a close relationship is observed between Helicobacter hepaticus and hepatocellular carcinoma, and Helicobacter species can be found in humans, most commonly in extragastric organs. There have also been reports that H. bilis may be associated with biliary malignancies in humans. The effect of H. bilis infection on a human bile duct cancer cell line was investigated in this study.
Methods
We prepared HuCCT-1, the human bile duct cancer cell line, which was cocultured with H. bilis and cultured alone as a control. HuCCT-1 with and without H. bilis were transfected with the NF-κB, E2 transcription factor (E2F), and cyclic AMP response element (CRE) luciferase vectors. The activity of NF-κB between H. bilis and the infected and noninfected HuCCT-1 cells was also measured by dual luciferase reporter assay. The concentration of vascular endothelial growth factor (VEGF) in the cocultured medium and control medium were measured by ELISA. To investigate the effect of H. bilis infection on HuCCT-1 with regard to human umbilical vein endothelial cell (HUVEC) tube formation, HUVECs and fibroblasts were cocultured in 24-well plates with and without the conditioned medium.
Results
NF-κB, E2F and CRE activity, production of VEGF, and angiogenesis in H. bilis-infected cell lines were enhanced compared with controls.
Conclusions
H. bilis infection in a human bile duct cancer cell line activates transcript factors such as NF-κB that stimulate production of VEGF and lead to enhancement of angiogenesis. H. bilis infection may play an important role in malignancies in the biliary tract.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Helicobacter pylori infection is widely accepted as the most common cause of gastritis and is etiologically involved in gastric ulcer, duodenal ulcer, gastric adenocarcinoma [1], and gastric mucosa-associated lymphoid tissue lymphoma [2]. Other kinds of Helicobacter infection of extragastric organs have not been extensively investigated; however, in 1992, a high rate of liver tumors in mouse colonies was noted at the US National Cancer Institute [3]. An extensive search for the cause of these tumors revealed that the livers of the mice were infected with Helicobacter hepaticus, which induced chronic hepatic inflammation and subsequent liver cancer in a large population of the mouse colony. According to a previous report, Helicobacter bilis isolated from the bile, liver, and intestines of mice [4] showed a 97.4% similarity to H. hepaticus and a 93.4% similarity to H. pylori based on 16S rRNA sequence comparison. H. bilis was thus found to be closely related to H. hepaticus, which plays a role in hepatobiliary malignancies. Helicobacter was subsequently detected by PCR in the liver [5], gallbladder [6], and bile [7] of human samples. Two reports have shown a significantly higher positive rate for H. bilis in Japanese and Thai patients with bile duct and gallbladder cancer [8, 9], and H. bilis has also been found in the bile, liver, and intestines of mice [10]. It is known to be responsible for chronic hepatitis and hepatocellular tumors in mice and may play a major role in cholesterol gallstone formation [11]. However, a direct association between H. bilis and bile duct cancer has not been established yet. The aim of this study was to examine the influence of H. bilis infection on a bile duct cancer cell line.
Methods
Bacteria
The ATCC 51630 H. bilis strain was used in this study. It was cultured at 37°C under microaerobic conditions in Brucella broth (Becton Dickinson, Cockeysville, MD) supplemented with 3% heat-inactivated fetal bovine serum. Bacteria were harvested from the broth culture by centrifugation and resuspended at the indicated concentrations in antibiotic-free RPMI 1640 (Sigma Chemical Co., St Louis, MO).
Cell Culture and Materials
The human bile duct cancer cell line HuCC-T1 was obtained from Health Science Research Resources Bank (Osaka, Japan). The cells were maintained in RPMI 1640 medium supplemented with 10% fetal calf serum at 37°C in 5% CO2 and 95% air.
Dual Luciferase Reporter Assay
Luciferase is a highly sensitive enzymatic reporter that can be assayed using standard luciferase detection methods. We used the pNF-κB-Luc, pE2F-Luc, and pCRE-Luc reporter vectors, which are designed for monitoring induction of NF-κB, E2F, and CRE. These three vectors were designed to measure binding of transcription factors to the enhancer, thus providing a direct measurement of activation for this pathway. These vectors contain the firefly luciferase gene from Photinus pyralis. In addition, we used the phRL-TK renilla luciferase reporter vector (Promega, Madison, WI) as a control. HuCCT-1 cells were seeded in a suitable tissue culture plate and incubated for 24 h. Each three semiconfluent (70–80%) cells was transfected with three vectors each, pNF-κB-Luc, pE2F-Luc, pCRE-Luc, and simultaneously transfected control vector phRL-TK for all of them, at a ratio of 30:1 for 4 h using SuperFect Transfection Reagents (Qiagen, Valencia, CA) according to the manufacturer’s instructions. The medium was replaced and transfectants were further incubated for 12 h. After incubation, the medium was changed to RPMI 1640 with H. bilis or to RPMI 1640 alone as control. The RPMI 1640 with H. bilis medium was adjusted by approximately 50 MOI (multiplicity of infection). Growth medium was removed from the cultured cells and a sufficient volume of phosphate buffered saline was applied to wash the surface of the culture vessels. One hundred microliters of passive lysis buffer was then dispensed into each culture well. Culture plates were placed on an orbital shaker with gentle shaking at room temperature for 15 min. Lysate samples were cleared for 30 s by centrifugation at 10,000 rpm in a refrigerated microcentrifuge. Firefly and renilla luciferase activity in the samples was measured using a luminometer.
Enzyme-Linked Immunosorbent Assay
HuCC-T1 cells were seeded at a density of 2 × 105 cells into 24-well plates containing culture medium supplemented with 10% FCS. After cells reached subconfluency, live H. bilis was added at approximately 50 MOI. After 24 h of coculture, culture media were collected and centrifuged at 1,500 rpm for 5 min to remove particles, and the supernatants were frozen at −80°C until used for ELISA. The VEGF content in the culture supernatants was determined using an ELISA kit (Becton Dickinson) according to the manufacturer’s instructions.
Angiogenesis Assay
For conditioned media, HuCCT-1 cells were seeded at a final density of 5 × 106 cells into a flask (80 cm2) that contained medium with 10% FCS. After overnight culturing, the medium was changed and H. bilis was added at approximately 50 MOI with 2% FCS medium and then cultured for an additional 24 h. The supernatant was collected and centrifuged at 6,000 rpm for 5 min, then filtered with a 0.22-mm filter to remove particulate matter and bacteria. HUVECs basal medium and filtered bacterial-free medium were mixed at a ratio of 1:1 and used as conditioned medium. To investigate the influence of H. bilis infection on HuCCT-1 cells on tube formation by HUVECs, fibroblasts and HUVECs were cocultured in basal medium or conditioned medium using an angiogenesis kit (Kurabo, Osaka, Japan) according to the manufacturer’s protocols [12, 13]. Briefly, HUVECs and fibroblasts were cocultured in 24-well plates with basal medium or the conditioned medium. Media were changed every 3 days and HUVECs and fibroblasts were cocultured for 11 days. HUVECs were then stained with anti-CD31 antibody to detect endothelial cells according to the manufacturer’s protocols. Tube formation area was measured quantitatively over 15 different fields for each condition using an image analyzer (Kurabo).
Statistical Analysis
Differences between the two groups were evaluated using Student’s t-test. Differences were considered statistically significant if P < 0.05.
Results
NF-κB, E2F, and CRE Activity Induced by H. bilis Infection
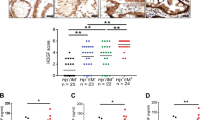
In the control vector and various luciferase expression vectors transfected with the HuCC-T1 cell line, relative luciferase activities were enhanced by H. bilis infection. NF-κB, E2F, and CRE activity was significantly higher than that in the noninfectious stimulation controls. The NF-κB baseline ratio in the HuCC-T1 cell line was approximately 5.15 (range 4.14–6.09). Infection with H. bilis enhanced NF-κB activity to approximately 14.2 (11.29–18.87), which was nearly a three-fold increase over the basal level. The E2F baseline ratio in the HuCC-T1 cell line was approximately 5.64 (4.95–7.11). Infection with H. bilis enhanced E2F activity to approximately 11.9 (9.36–13.44), which was nearly a two-fold increase over the basal level. The CRE baseline ratio in the HuCC-T1 cell line was approximately 4.94 (4.68–5.08). Infection with H. bilis enhanced CRE activity to approximately 8.44 (7.68–9.84), which was nearly a two-fold increase over the basal level (Fig. 1).
Results of dual luciferase reporter assay of NF-κB, E2F, and CRE. Influence of Helicobacter infection on NF-κB, E2F, and CRE activity in HuCC-T1 cell lines. Cell lines were incubated with and without H. bilis for 24 h and the relative luciferase activity was measured by a luminometer. NF-κB, E2F, and CRE activity of H. bilis-infected HuCCT-1 cells was significantly higher in controls (* P < 0.01), and significantly greater NF-κB activity was observed in the H. pylori-infected HuCCT-1 cells compared with the controls (* P < 0.01), which was of the same level as H. bilis-infected HuCCT-1 cells
VEGF Induced by H. bilis Infection
We examined the production of VEGF in the HuCC-T1 cell line cocultured with live H. bilis. The HuCC-T1 cell line produced a constitutively marked amount of VEGF (Fig. 2). The baseline production of VEGF in the HuCC-T1 cell line was approximately 93.6 pg/ml. H. bilis infection enhanced VEGF production to approximately 221 pg/ml, which was nearly a 2.4-fold increase over the basal level (P < 0.01). The increase in VEGF production suggests that H. bilis infection of the HuCC-T1 cell line enhanced NF-κB activity, which leads to VEGF gene transcription.
Result of ELISA of VEGF. Secretion of VEGF into cultured medium by bile duct cancer cell lines determined by ELISA. Cell lines were cultured with and without H. bilis (control). Values are expressed as mean ± SD. Comparisons were performed by Student’s t-test. Results show that secretion of VEGF was significantly higher in the cell line with H. bilis compared with the control (* P < 0.01)
Angiogenesis Induced by H. bilis Infection
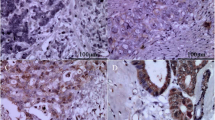
HUVECs cultured in control medium and condition media derived from H. bilis-infected cancer cells were stained with anti-CD31 antibody to examine tube formation. Pictures were taken of five different points per well from three wells, for a total of 15 points. The area of tube formation was measured quantitatively using an image analyzer. The baseline tube formation area for HUVECs was 51,600 pixels, and the tube formation area for the HUVECs in conditioned medium was 68,000 pixels. Thus, tube formation in HUVECs was enhanced by H. bilis-infected medium (P < 0.01) (Fig. 3a–c).
Results of angiogenesis assay. HUVECs cultured with either H. bilis-infected HuCC-T1 medium or noninfected HuCC-T1 medium. After 11 days of culturing, cells were stained with anti-CD31 antibody. Tube formation in cultures of control medium (a) or H. bilis cocultured with HuCCT-1 medium (b) was statistically analyzed using the t-test. The results show that angiogenesis was activated by H. bilis-infected medium (c) (* P < 0.01)
Discussion
In recent years, there has been an increase in the number of reports confirming that H. pylori infection is associated with not only gastric disease but also extragastric disease. For idiopathic thrombocyte purpura, H. pylori eradication treatment is a favorable therapeutic option for patients who are H. pylori-positive [13]. Considering that H. pylori is involved in the pathogenesis and pathophysiology of these autoimmune disorders, it might also trigger autoimmune pancreatitis through induction of autoimmunity and apoptosis [14]. As stated previously, it is probable, although not yet confirmed, that live H. pylori is present in extragastric organs such as the spleen, pancreas, and biliary tracts. On the other hand, H. bilis is bile-tolerant and commonly detected through PCR in patients with cholangio-ductal disease.
In this study, we focused on H. bilis as a virulent organism in humans. Although H. bilis is grown at 37°C in a microaerophilic atmosphere, as for other Helicobacter species, its shape is different from that of H. pylori in that it has a fusiform body with 3–14 multiple bipolar flagella and periplasmic fibers wrapped around the cell. Scanning electron microscopy confirmed the presence of these features (Fig. 4), and the images were similar to the transmission electron microscopic images obtained by Fox et al. [10]. H. bilis is thought to be one cause of hepatitis and colitis in mice [15]. 16S rRNA sequence comparison showed that it had a 97.4% similarity to H. hepaticus and a 93.4% similarity to H. pylori, indicating that H. bilis is more closely related to H. hepaticus [10], which is involved in hepatobiliary malignancies in mice, than to H. pylori. This suggests that H. bilis may have a system that stimulates the malignant potential of targeted cells, which is similar to that of H. hepaticus and H. pylori.
The scanning electron microscopy photo of H. bilis. H. bilis coculture with HuCCT-1 cells. The cells were gently fixed using 2.5% glutalaldehyde for 1 h on ice. After two 10-min washes with phosphate buffered saline, cells were fixed through an ethanol series (50%, 70%, 80%, 85%, 90%, 95%, and 100% for 10 min each) and two 20-min t-butyl alcohol washes. Afterward, the samples were dried under −20°C for 3 h and coated with platinum. Scanning electron microscopy revealed that H. bilis has a fusiform body with multiple bipolar flagella and periplasmic fibers wrapped around the cells
To investigate the effect of H. bilis on bile duct cancer cells, we focused first on NF-κB, one of the key signal transmitters for cancer cell activation. Activation of the NF-κB pathway is involved in the pathogenesis of chronic inflammatory diseases [16], and abnormalities in the NF-κB pathway are frequently seen in a variety of human cancers. NF-κB proteins are localized in the cytoplasm and are associated with a family of inhibitor proteins known as IκB-B.C, which comprise a family of proteins that share a 300-amino acid domain designated as the Rel homology domain [17, 18]. The Rel homology domain mediates DNA binding, dimerization, and nuclear transport of NF-κB proteins. NF-κB is also activated after H. pylori infection in gastric cancer cells [19, 20]. Additionally, it is involved in the upregulation of VEGF mRNA. It has been demonstrated that NF-κB, a critical regulator of genes involved in inflammation, is also required for VEGF gene expression [21]. H. pylori infection also promotes gastric epithelial cell invasion through activation of VEGF expression. These effects appear to be mediated through an NF-κB pathway, since the NF-κB inhibitor significantly attenuates the invasiveness of gastric cancer cells and expression of the VEGF protein [22, 23]. In other transcription factors, VEGF activates CRE-binding protein [24], and CRE mediate the transcription of early growth response of vascular smooth muscle cells [25]. These genes may also play an important role in angiogenesis. The E2F family, whose expression was increased by VEGF [26], plays a crucial role in the control of cell cycle and action of tumor suppressor proteins and is also a target of the transforming proteins of small DNA tumor viruses. This protein and another two members, E2F2 and E2F3, have an additional cyclin binding domain. This protein binds preferentially to retinoblastoma protein pRB in a cell-cycle dependent manner. It can mediate both cell proliferation and p53-dependent/independent apoptosis [27].
In this study, we confirmed that H. bilis infection activates NF-κB in bile duct carcinoma cells, thereby increasing expression of the angiogenic factor VEGF from the cells and elevating their angiogenic potential. Moreover, VEGF may elevate their angiogenic potential via CRE-binding protein, which is activated by H. bilis infection. This is because NF-κB and CRE activation lead to VEGF [28] gene transcription, and VEGF is one of the most important angiogenic factors. Additionally, VEGF may elevate nuclear expression of E2F that leads to bile duct carcinoma cell proliferation. We think that H. bilis may have some malignant potential for bile duct cancer cell lines similar to H. hepaticus for hepatoma of mice. To determine whether H. bilis is definitely a risk factor for bile duct malignancy, it is necessary to culture live H. bilis directly from the bile. This study is the first step in examining the risk of H. bilis infection on bile duct cancer, and it may provide significant insights into the mechanism of development of cholangio-ductal tumor.
References
Uemura N, Okamoto S, Yamamoto S, et al. Helicobacter pylori infection and the development of gastric cancer. N Engl J Med. 2001;345:784–789.
Nakamura S, Matsumoto T, Suekane H, et al. Long-term clinical outcome of Helicobacter pylori eradication for gastric mucosa-associated lymphoid tissue lymphoma with a reference to second-line treatment. Cancer. 2005;104:532–540.
Ward JM, Fox JG, Anver MR, et al. Chronic active hepatitis and associated liver tumors in mice caused by a persistent bacterial infection with a novel Helicobacter species. J Natl Cancer Inst. 1994;86:1222–1227.
Fox JG, Dewhirst FE, Tully JG, et al. Helicobacter hepaticus sp. nov., a microaerophilic bacterium isolated from livers and intestinal mucosal scrapings from mice. J Clin Microbiol. 1994;32:1238–1245.
Pellicano R, Mazzaferro V, Grigioni WF, et al. Helicobacter species sequences in liver samples from patients with and without hepatocellular carcinoma. World J Gasroenterol. 2004;10:598–601.
Silva CP, Pereira-Lima JC, Oliveira AG, et al. Association of the presence of Helicobacter in gallbladder tissue with cholelithiasis and cholecystitis. J Clin Microbiol. 2003;41:5615–5618.
Farshad SH, Alborzi A, Malek Hosseini SA, et al. Identification of Helicobacter pylori DNA in Iranian patients with gallstones. Epidemiol Infect. 2004;132:1185–1189.
Murata H, Tsuji S, Tsujii M, et al. Helicobacter bilis infection in biliary tract cancer. Aliment Pharmacol Ther. 2004;20:90–94.
Matsukura N, Yokomuro S, Yamada S, et al. Association between Helicobacter bilis in bile and biliary tract malignancies: H. bilis in bile from Japanese and Thai patients with benign and malignant diseases in the biliary tract. Jpn J Cancer Res. 2002;93:842–847.
Fox JG, Yan LL, Dewhirst FE, et al. Helicobacter bilis sp. nov., a novel Helicobacter species isolated from bile, livers, and intestines of aged, inbred mice. J Clin Microbiol. 1995;33:445–454.
Maurer KJ, Ihrig MM, Rogers AB, et al. Identification of cholelithogenic enterohepatic Helicobacter species and their role in murine cholesterol gallstone formation. Gastroenterology. 2005;128:1023–1033.
Bishop ET, Bell GT, Bloor S, Broom IJ, Hendry NF, Wheatley DN. An in vitro model of angiogenesis: basic features. Angiogenesis. 1999;3:335–344.
Osugi T, Oshima Y, Fujio Y, et al. Cardiac-specific activation of signal transducer and activator of transcription 3 promotes vascular formation in the heart. J Biol Chem. 2002;277:6676–6681.
Suzuki T, Matsushima M, Masui A, et al. Effect of Helicobacter pylori eradication in patients with chronic idiopathic thrombocytopenic purpura—a randomized controlled trial. Am J Gastroenterol. 2005;100:1265–1270.
Shomer NH, Dangler CA, Schrenzel MD, Fox JG. Helicobacter bilis-induced inflammatory bowel disease in scid mice with defined flora. Infect Immun. 1997;65:4858–4864.
Tak PP, Firestein GS. NF-kappaB: a key role in inflammatory diseases. J Clin Invest. 2001;107:7–11.
Baldwin AS Jr. The NF-kappa B and I kappa B proteins: new discoveries and insights. Annu Rev Immunol. 1996;14:649–683.
Ghosh S, May MJ, Kopp EB. NF-kappa B and Rel proteins: evolutionarily conserved mediators of immune responses. Annu Rev Immunol. 1998;16:225–260.
Kountouras J, Zavos C, Chatzopoulos D. A concept on the role of Helicobacter pylori infection in autoimmune pancreatitis. J Cell Mol Med. 2005;9:196–207.
Aihara M, Tsuchimoto D, Takizawa H, et al. Mechanisms involved in Helicobacter pylori-induced interleukin-8 production by a gastric cancer cell line. MKN45. Infect Immun. 1997;65:3218–3224.
Maeda S, Akanuma M, Mitsuno Y, et al. Distinct mechanism of Helicobacter pylori-mediated NF-kappa B activation between gastric cancer cells and monocytic cells. J Biol Chem. 2001;276:44856–44864.
Shibata A, Nagaya T, Imai T, Funahashi H, Nakao A, Seo H. Inhibition of NF-kappaB activity decreases the VEGF mRNA expression in MDA-MB-231 breast cancer cells. Breast Cancer Res Treat. 2002;73:237–243.
Wu CY, Wang CJ, Tseng CC, et al. Helicobacter pylori promote gastric cancer cells invasion through a NF-kappaB and COX-2-mediated pathway. World J Gastroenterol. 2005;11:3197–3203.
Mayo LD, Kessler KM, Pincheira R, Warren RS, Donner DB. Vascular endothelial cell growth factor activates CRE-binding protein by signaling through the KDR receptor tyrosine kinase. J Biol Chem. 2001;276:25184–25189.
Cui MZ, Laag E, Sun L, Tan M, Zhao G, Xu X. Lysophosphatidic acid induces early growth response gene 1 expression in vascular smooth muscle cells: CRE and SRE mediate the transcription. Arterioscler Thromb Vasc Biol. 2006;26:1029–1035.
Zhu Y, Jin K, Mao XO, Greenberg DA. Vascular endothelial growth factor promotes proliferation of cortical neuron precursors by regulating E2F expression. FASEB J. 2003;17:186–193.
Penzo M, Massa PE, Olivotto E, et al. Sustained NF-kappaB activation produces a short-term cell proliferation block in conjunction with repressing effectors of cell cycle progression controlled by E2F or FoxM1. J Cell Physiol. 2009;218:215–227.
Bancroft CC, Chen Z, Dong G, et al. Coexpression of proangiogenic factors IL-8 and VEGF by human head and neck squamous cell carcinoma involves coactivation by MEK-MAPK and IKK-NF-kappaB signal pathways. Clin Cancer Res. 2001;7:435–442.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Takayama, S., Takahashi, H., Matsuo, Y. et al. Effect of Helicobacter bilis Infection on Human Bile Duct Cancer Cells. Dig Dis Sci 55, 1905–1910 (2010). https://doi.org/10.1007/s10620-009-0946-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-009-0946-6