Abstract
Fluvastatin, the first entirely synthetic statin, has a significant cholesterol-lowing effect comparable with other statins. In addition, it has been shown to inhibit oxidative stress and improve vascular endothelial function. The aim of this study was to clarify the pretreatment effects of fluvastatin on liver function after massive hepatectomy in rats. Six-week-old male Wister rats were divided into two groups: a fluvastatin group (group F), pretreated with oral administration of fluvastatin (20 mg/kg per day) for 2 days before 90% hepatectomy; and a control group (group C), pretreated with vehicle for 2 days before hepatectomy. Animals were sacrificed at 0, 12, 24, 48, and 72 h after hepatectomy. The liver regeneration rate, liver function tests, and hepatic stellate cell activation were examined. The liver regeneration rate in group F was significantly higher at 72 h after hepatectomy (P < 0.05). The serum level of total bilirubin in group F was significantly lower at 48 h after hepatectomy (P < 0.05). Sinusoidal area in group F was maintained histologically. Furthermore, the expression of alpha smooth-muscle actin (α-SMA) protein in the liver was inhibited in group F at 48 h after hepatectomy. This study demonstrated the beneficial effects of fluvastatin in a lethal massive hepatectomy model using rats, with improved hepatic regeneration and microcirculations, by inhibiting the activation of hepatic stellate cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Although massive hepatectomy is sometimes required to achieve a curative resection for advanced hepatic malignancies, most instances of mortality after such surgery are still attributed to hepatic failure with small remnant liver volume [1]. Therefore, a novel strategy is still needed for the treatment of hepatic insufficiency after massive hepatectomy.
Various hypotheses have been reported for the mechanisms of hepatic failure after massive hepatectomy; excessive metabolic loads for each remnant hepatocyte and excessive stress on the hepatic sinusoids with portal overflow [2]. From the microenvironmental viewpoint, reactive oxygen species (ROS) have been reported to have a crucial role after such injury [3]. ROS are evolved during the early posthepatectomy phase, causing initial insults on both parenchymal and nonparenchymal cells, and lead to secondary negative cascades including hepatic hypercytokinemia [3–6]. We previously focused on ROS as the crucial factors in such hepatic injuries, acting via Rho-kinase-mediated pathways [7]. In the study reported here, we focused on the potential role of statins, which are known to deoxidize various enzymes involved in modification of small G proteins such as Rho [8–13]. Although possible anti-inflammatory properties of statins have been reported, no previous reports have evaluated their roles in massive hepatectomy.
Fluvastatin is the first entirely synthetic statin, with the most potent cholesterol reduction property of all the available statins [14, 15]. The aim of the study was to investigate the possible beneficial effects of fluvastatin on hepatic function, including microcirculation and regeneration, using a massive hepatectomy model in rats.
Materials and Methods
Animals
Six-week-old male Wister rats weighing 180–220 g were obtained from Charles River Co., Ltd (Kanagawa, Japan). Throughout the experiment, the animals were maintained behind barriers under controlled conditions and had free access to tap water and diet before and after operation. The University of Tokushima Institutional Animal Care and Use Committee approved all animal protocols, according to the criteria outlined in the “Guide for the Care and Use of Laboratory Animals” prepared by the National Academy for Sciences and published by the National Institutes of Health (NIH).
Experimental Design
Animals were randomly divided into the following two groups: fluvastatin-administrated group (group F; n = 9) and control group (group C; n = 7). In group F, the animals were pretreated with oral doses of fluvastatin 20 mg/kg per day in normal saline (Tanabe Seiyaku Co., Ltd. Osaka, Japan) starting from 2 days before hepatectomy and continuing until the day of hepatectomy, whereas in group C, the animals received vehicle in the same manner.
Surgical procedures were performed under general anesthesia with diethyl ether. Removal of 90% of the hepatic tissue was performed using the method of Higgins and Anderson [16], with minor modifications as described by Kubota et al. [17]. The left, middle, and right lobes were sequentially removed without constricting the inferior vena cava or causing bleeding. The caudate lobe was left intact. All surgical procedures were completed within 20 min. Signs of distress and survival were monitored for up to 1 week. Animals were sacrificed at 12, 24, 48, and 72 h after hepatectomy. Blood samples were obtained from the superior vena cava for biochemical analysis. The intact liver was removed and stored for histological examinations after measurement of its wet weight.
Biochemical Analysis
To evaluate liver injury, the level of serum aspartate aminotransferase (AST), serum alanine aminotransferase (ALT), hyaluronic acid, and total bilirubin were measured using commercially available assay kits (Shikoku Chuken, Inc. Kagawa, Japan).
Histological Examination
Liver tissues were fixed in 10% buffered formalin, embedded in paraffin, cut into sections 4-μm thick, and processed for hematoxylin and eosin (H&E) and immunohistochemical staining. The H&E sections were used to evaluate sinusoidal area. Investigators who were kept blind to the treatment group measured ten areas of sinusoidal area at magnification of ×200 using the NIH image software program (National Institute of Health, MD, USA). The maintenance of sinusoid area was investigated by sinusoidal space rate, which is the area of sinusoid per one view at magnification of ×200. For immunohistochemical evaluations, the sections were incubated overnight with antibodies against proliferating cell nuclear antigen (PCNA, mouse monoclonal) (Santa Cruz, CA, USA) and alpha smooth-muscle actin (α-SMA) diluted 1:100, mouse monoclonal (Abcam, Cambridge, UK) at 4°C. After being washed with phosphate-buffered saline (PBS), bound antibodies were visualized with the Dako Envision system (Dako Chemate EnVision Detection Kit, Peroxidase/DAB, Rabbit/Mouse, Dako Cytomation, Denmark). A normal goat immunoglobulin (Ig)G was used to assess nonspecific reactions. At the magnification of ×200, ten areas of PCNA and α-SMA-positive cells were measured in a blinded fashion for each group.
Statistical Analysis
Data are expressed as mean ± standard deviation (SD). Comparisons in the same group were performed using the paired Student’s t test. Comparisons between groups were conducted using the Mann-Whitney U test. Statistical significance was defined as a P value <0.05.
Results
Liver Regeneration
During the first 48 h of the postoperative period, the intact liver/body-weight ratio was not significantly different between groups. However, it was significantly increased in group F at 72 h after hepatectomy compared with group C (P < 0.05, Fig. 1). The number of PCNA-positive cells in group F was significantly increased over those in group C at 72 h after hepatectomy (Fig. 2).
Hepatic Chemistries
The serum level of AST, ALT, hyaluronic acid, and total bilirubin in the rats are shown in Table 1. The total bilirubin at 48 h after hepatectomy was significantly lower in group F compared with group C (1.9 ± 0.1 vs. 4.9 ± 1.9 mg/dl, P < 0.05). There were no statistically significant differences in the other parameters between the two groups.
Hepatic Sinusoidal Area
Sinusoidal area was maintained in group F compared with group C at 24 h (2.94 ± 1.01 vs. 1.50 ± 0.67%, P < 0.01) and 48 h (0.95 ± 0.41 vs. 0.60 ± 0.24%, P < 0.05) after hepatectomy (Fig. 3). Sinusoidal areas in the both groups were smallest at 48 h after hepatectomy, but at 72 h after hepatectomy, sinusoidal areas in both groups were restored.
The Expression of α-SMA
Alpha SMA-positive cells were significantly decreased in group F compared with group C (2.7 ± 2.6 vs. 17.6 ± 13.5, P < 0.01) at 48 h after hepatectomy (Fig. 4).
Discussion
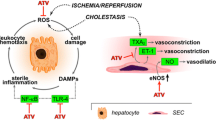
In this study, pretreatment with fluvastatin accelerated liver regeneration and improved cholestasis by inhibiting the activation of the liver stellate cells. Statins are inhibitors of the enzyme hydroxy-methyl-glutaryl-coenzyme-A (HMG-CoA) reductase and are widely used as lipid-lowering agents [12]. In the previous report, HMG-CoA reductase activity increase prior to onset of DNA synthesis or S phase, and has a stimulatory effect on the initiation of liver regeneration [18–20]. Inhibition of HMG-CoA reductase results in decreased farnesyl pyrophosphate, which not only reduces cholesterol levels but also modifies and inactivates small G proteins, including Rho (Fig. 5). Therefore, fluvastatin has been shown to modify posttranslational G-protein-associated phospholipids, resulting in their inactivation, and has been shown to ameliorate ROS production in the liver [12–14]. Although possible anti-inflammatory properties of statins have been reported, no previous reports have evaluated their effects after massive hepatectomy. Therefore, in the study reported here, we investigated the role of fluvastatin, one of the most potent deoxidizer amongst the currently available statins, in an experimental massive hepatectomy model.
The prominent effect of fluvastatin in this study was observed in terms of preserved sinusoidal circulation via the inhibition of hepatic stellate cells, as shown by reduced α-SMA-positive hepatic stellate cells. It has been reported that several factors that improved the microcirculation promote liver regeneration. Wang et al. [21] reported that phosphodiesterase inhibitor, which improves hepatosplanchnic circulation, promotes liver regeneration. Tsujii et al. [22] reported that prostaglandin E2 enhances the proliferation of hepatocytes by increasing intracellular cyclic AMP. Akcan et al. [23] reported that nitric oxide, a flow-dependent factor, is a trigger to initiate the regeneration process. Hepatic stellate cells are located between parenchymal cells and the endothelial lining and have several important functions, such as remodeling of extracellular matrix (ECM) by production of both ECM components and matrix metalloproteinases, production of growth factors and cytokines, and contraction and dilation of the sinusoidal lumen in response to endothelin, angiotensin, thromboxane, and prostaglandins [24–28]. Activation of hepatic stellate cells is mediated by prominent ROS, released by both parenchymal and nonparenchymal cells, in particular by damaged hepatocytes and activated Kupffer cells [24]. It has been reported that the intracellular source of ROS is the intramitochondrial cytochrome P450 system with nicotinamide adenine dinucleotide phosphate and xanthine oxidase, resulting in activation of the extracellular signal-regulated-kinase-signaling pathway [24–28]. Continuing activation of the hepatic stellate cells leads to progressive fibrosis of the liver; fluvastatin, which inhibits activation of hepatic stellate cells, may prevent fibrosis progression.
Among the various factors known to cause hepatic failure after massive hepatectomy, ROS has been reported to play the pivotal role [3, 4]. It is well known that ROS are released by the Kupffer cells via activation by excessive sheer stress and microcirculatory disturbance in the hepatic sinusoids in the intact liver [3–6]. Such ROS cause not only hepatocyte injury but also sinusoidal endothelial cell damage, which further aggravates microcirculatory disturbances. In our previous studies, it was revealed that Rho-kinase, an effector of the small GTPase Rho, plays an important role in ROS production through the nicotinamide adenine dinucleotide phosphate (NADPH) system in the hyperacute phase of hepatic reperfusion [7]. Other studies also showed that Rho-regulated ROS production is involved in the pathogenesis of hepatocellular necrosis and apoptosis [8, 9].
Liver regeneration also might be affected by ROS via indirect or direct effects [29–35]. As an indirect effect, it has been reported that stellate cells activated via the ROS system produce excessive transforming growth factor beta (TGF-β), a potent inhibitory cytokine for liver regeneration [29, 30]. TGF-β has been found to be increased in experimental and human hepatic fibrosis, and TGF-β induces ECM production by hepatic stellate cells. A previous study showed that H2O2, as a major source of ROS, induced transient elevation of p53 and p21 proteins, which inhibit the cell cycle, resulting in arrest of the cell cycle at the G1 phase [34]. Another report showed that ROS induce downregulation of cyclin D expression, which is important for G1-phase progression [35].
As a direct effect, ROS caused acute liver injury and increased transaminase [4, 36]. It has been reported that fluvastatin has anti-inflammatory properties and reduces the serum level of AST and ALT on endotoxin-induced liver injury [37]. Another report showed that statin significantly reduced liver injury associated with enhanced endothelial nitric oxide synthase (eNOS) expression [38]. However, in this study the serum level of AST and ALT was not improved significantly. We suppose that the effect of improving liver injury weaken under excessive stress, such as massive hepatectomy.
In conclusion, this study demonstrated the beneficial effects of fluvastatin via improved hepatic regeneration and microcirculation in a lethal massive hepatectomy model using rats. Fluvastatin may be an effective pharmacological strategy to improve outcomes after massive hepatectomy.
Abbreviations
- α-SMA:
-
Alpha smooth-muscle actin
- ALT:
-
Alanine aminotransferase
- AST:
-
Aspartate aminotransferase
- ECM:
-
Extracellular matrix
- FPP:
-
Farnesyl pyrophosphate
- GGPP:
-
Geranylgeranyl pyrophosphate
- NADPH:
-
Nicotinamide adenine dinucleotide phosphate
- PCNA:
-
Proliferating-cell nuclear antigen
- ROS:
-
Reactive oxygen species
- HMG-CoA:
-
Hydroxy-methyl-glutaryl-coenzyme A
References
Mullen JT, Ribero D, Reddy SK, Donadon M, Zorzi D, Gautam S, Abdalla EK, Curley SA, Capussotti L, Clary BM, Vauthey JN (2007) Hepatic insufficiency and mortality in 1,059 noncirrhotic patients undergoing major hepatectomy. J Am Coll Surg 204:854–862 doi:10.1016/j.jamcollsurg.2006.12.032
Togo S, Kubota T, Matsuo K, Shimizu T, Momiyama N, Takeda K, Tanaka K, Endo I, Sekido H, Shimada H (2004) Mechanism of liver failure after hepatectomy. Nippon Geka Gakkai Zasshi 105:658–663
Schwabe RF, Brenner DA (2006) Mechanisms of Liver Injury. I. TNF-alpha-induced liver injury: role of IKK, JNK, and ROS pathways. Am J Physiol Gastrointest Liver Physiol 290:583–589. doi:10.1152/ajpgi.00422.2005
Taniguchi M, Takeuchi T, Nakatsuka R, Watanabe T, Sato K (2004) Molecular process in acute liver injury and regeneration induced by carbon tetrachloride. Life Sci 75:1539–1549 doi:10.1016/j.lfs.2004.02.030
Choi SS, Sicklick JK, Ma Q, Yang L, Huang J, Qi Y, Chen W, Li YX, Goldschmidt-Clermont PJ, Diehl AM (2006) Sustained Activation of Rac1 in Hepatic stellate cells promotes liver injury and fibrosis in mice. Hepatology 44:1267–1277 doi:10.1002/hep.21375
Zhang W, Wang M, Xie HY, Zhou L, Meng XQ, Shi J, Zheng S (2007) Role of reactive oxygen species in mediating hepatic ischemia-reperfusion injury and its therapeutic applications in liver transplantation. Transplant Proc 39:1332–1337 doi:10.1016/j.transproceed.2006.11.021
Shiotani S, Shimada M, Suehiro T, Soejima Y, Yosizumi T, Shimokawa H, Maehara Y (2007) Involvement of Rho-kinase in cold ischemia-reperfusion injury after liver transplantation in rats. Transplantation 78:555–558
Wei CY, Huang KC, Chou YH, Hsieh PF, Lin KH, Lin WW (2006) The role of Rho-associated kinase in differential regulation by statins of interleukin-1β- and lipopolysaccharide-mediated nuclear factor κB activation and inducible nitric-oxide synthase gene expression in vascular smooth muscle cells. Mol Pharmacol 69:960–967
Kato T, Hashikabe H, Iwata C, Akimoto K, Hattori Y (2004) Statin blocks Rho/Rho-kinase signalling and disrupts the actin cytoskeleton: relationship to enhancement of LPS-mediated nitric oxide synthesis in vascular smooth muscle cells. Biochim Biophys Acta 1689:267–272
Kubota T, Fujisaki K, Itoh Y, Yano T, Sendo T, Oishi R (2004) Apoptotic injury in cultured human hepatocytes induced by HMG-CoA reductase inhibitors. Biochem Pharmacol 67:2175–2186 doi:10.1016/j.bcp.2004.02.037
Fukuyama R, Fujita T, Azuma Y, Hirano A, Nakamuta H, Koida M, Komori T (2004) Statins inhibit osteoblast migration by inhibiting Rac-Akt signaling. Biochem Biophys Res Commun 315:636–642 doi:10.1016/j.bbrc.2004.01.104
Takemoto M, Liao JK (2001) Pleiotropic effect of 3-hydroxy-3-methylalutaryl coenzyme a reductase inhibitors. Arterioscler Thromb Vasc Biol 21:1712–1719 doi:10.1161/hq1101.098486
Endres M, Laufs U (2004) Effect of statins on endothelium and signaling mechanisms. Stroke 35:2708–2711 doi:10.1161/01.STR.0000143319.73503.38
Nakashima A, Ohtawa M, Iwasaki K, Wada M, Kuroda N, Nakashima K (2001) Inhibitory effects of fluvastatin and its metabolites on the formation of several reactive oxygen species. Life Sci 69:1381–1389 doi:10.1016/S0024-3205(01)01223–1
Ikeda M, Abe K, Yamada M, Dansako H, Naka K, Kato N (2006) Different Anti-HCV profiles of statins and their potential for combination therapy with interferon. Hepatology 44:117–125 doi:10.1002/hep.21232
Higgins GM, Anderson RM (1931) Experimental pathology of the liver. I. Restoration of the liver of the white rat following partial surgical removal. Arch Pathol 12:186–202
Kubota T, Takabe K, Yang M, Sekido H, Endo I, Ichikawa Y, Togo S, Shimada H (1997) Minimum sizes for remnant and transplanted livers in rat. J Hepatobiliary Pancreat Surg 4:398–404. doi:10.1007/BF02488972
Field FJ, Mathur SN, LaBrecque DR (1985) Cholesterol metabolism in regenerating liver of the rat. Am J Physiol 249:G679–G684
Trentalance A, Leoni S, Mangiantini MT, Spagnuolo S, Feingold K, Hughes-Fulford M, Siperstein M, Cooper AD, Erickson SK (1984) Regulation of 3-hydroxy-3-methylglutaryl-coenzyme A reductase and cholesterol synthesis and esterification during the first cell cycle of liver regeneration. Biochim Biophys Acta 6:142–151
Zivna H, Zivny P, Palicka V, Simakova E (2002) Influence of high cholesterol diet and pravastatin sodium on the initiation of liver regeneration in rats after partial hepatectomy. Nutrition 18:51–55. doi:10.1016/S0899-9007(01)00678-5
Wang HH, Lautt WW (1998) Evidence of nitric oxide, a flow-dependent factor, being a trigger of liver regeneration in rats. Can J Physiol Pharmacol 76:1072–1079 doi:10.1139/cjpp-76-12-1072
Tsujii H, Okamoto Y, Kikuchi E, Matsumoto M, Nakano H (1993) Prostaglandin E2 and rat liver regeneration. Gastroenterology 105:495–499
Akcan A, Kucuk C, Ok E, Canoz O, Muhtaroglu S, Yilmaz N, Yilmaz Z (2006) The effect of amrinone on liver regeneration in experimental hepatic resection model. J Surg Res 130:66–72 doi:10.1016/j.jss.2005.07.020
Urtasun R, Nieto N (2007) Hepatic stellate cells and oxidative stress. Rev Esp Enferm Dig 99:223–230
Nieto N, Friedman SL, Cederbaum AI (2002) Stimulation and proliferation of primary rat hepatic stellate cells by cytochrome P450 2E1-derived reactive oxygen species. Hepatology 35:62–73 doi:10.1053/jhep.2002.30362
Nieto N, Friedman SL, Greenwel P, Cederbaum AI (1999) CYP2E1-mediated oxidative stress induces collagen type I expression in rat hepatic stellate cells. Hepatology 30:987–996 doi:10.1002/hep.510300433
Duncan RF, Peterson H, Sevanian A (2005) Signal transduction pathways leading to increased eIF4E phosphorylation caused by oxidative stress. Free Radic Biol Med 38:631–643 doi:10.1016/j.freeradbiomed.2004.09.034
Galli A, Svegliati-Baroni G, Ceni E, Milani S, Ridolfi F, Salzano R, Tarocchi M, Grappone C, Pellegrini G, Benedetti A, Surrenti C, Casini A (2005) Oxidative stress stimulates proliferation and invasiveness of hepatic stellate cells via a MMP2-mediated mechanism. Hepatology 41:1074–1084 doi:10.1002/hep.20683
Nakamura T, Sakata R, Ueno T, Sata M, Ueno H (2000) Inhibition of transforming growth factor beta prevents progression of liver fibrosis and enhances hepatocyte regeneration in dimethylnitrosamine-treated rats. Hepatology 32:247–255 doi:10.1053/jhep.2000.9109
Oe S, Lemmer ER, Conner EA, Factor VM, Leveen P, Larsson J, Karlsson S, Thorgeirsson SS (2004) Intact signaling by transforming growth factor beta is not required for termination of liver regeneration in mice. Hepatology 40:1098–1105 doi:10.1002/hep.20426
Fausto N, Campbell JS, Riehle KJ (2006) Liver regeneration. Hepatology 43:S45–S53 doi:10.1002/hep.20969
Horimoto M, Fulop P, Derdak Z, Wands JR, Baffy G (2004) Uncoupling protein-2 deficiency promotes oxidant stress and delays liver regeneration in mice. Hepatology 39:386–392 doi:10.1002/hep.20047
Diehl AM (1999) Effect of ethanol on tumor necrosis factor signaling during liver regeneration. Clin Biochem 32:571–578 doi:10.1016/S0009-9120(99)00057-0
Chen QM, Liu J, Merrett JB (2000) Apoptosis or senescence-like growth arrest: influence of cell-cycle position, p53, p21 and bax in H2O2 response of normal human fibroblasts. Biochem J 347:543–551 doi:10.1042/0264-6021:3470543
Barnouin K, Dubuisson ML, Child ES, Fernandez de Mattos S, Glassford J, Medema RH, Mann DJ, Lam EW (2002) H2O2 induces a transient multi-phase cell cycle arrest in mouse fibroblasts through modulating cyclin D and p21Cip1 expression. J Biol Chem 277:13761–13770 doi:10.1074/jbc.M111123200
Weng D, Lu Y, Wei Y, Liu Y, Shen P (2007) The role of ROS in microcystin-LR-induced hepatocyte apoptosis and liver injury in mice. Toxicology 22:15–23. doi:10.1016/j.tox.2006.12.010
Chen CH, Lee RP, Wu WT, Liao KW, Hsu N, Hsu BG (2007) Fluvastatin ameliorates endotoxin induced multiple organ failure in conscious rats. Resuscitation 74:166–174 doi:10.1016/j.resuscitation.2006.12.002
Harada H, Pavlick KP, Hines IN, Lefer DJ, Hoffman JM, Bharwani S, Wolf RE, Grisham MB (2003) Sexual dimorphism in reduced-size liver ischemia and reperfusion injury in mice: role of endothelial cell nitric oxide synthase. Proc Natl Acad Sci USA 21:739–744. doi:10.1073/pnas.0235680100
Acknowledgments
This study was supported by Grant-in-Aid for Scientific Research (Scientific Research (C) (No. 18591516).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tokunaga, T., Ikegami, T., Yoshizumi, T. et al. Beneficial Effects of Fluvastatin on Liver Microcirculation and Regeneration After Massive Hepatectomy in Rats. Dig Dis Sci 53, 2989–2994 (2008). https://doi.org/10.1007/s10620-008-0241-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-008-0241-y