Abstract
We sought to assess the activity of thiopurine methyltransferase (TPMT) in 14,545 Spanish patients with different diseases amenable to treatment with azathioprine/6-mercaptopurine (6-MP), and to evaluate the proportion of patients with low TPMT activity and therefore a higher risk of myelotoxicity with these drugs. TPMT activity in red blood cells (RBCs) was measured by a radiochemical method. The association between several clinical variables and TPMT activity was assessed by multiple linear regression. We included 14,545 patients: autoimmune hepatitis (n=359 patients), inflammatory bowel disease (n=7,046), multiple sclerosis (n = 814), myasthenia gravis (n=344), pemphigus (n=133), and other diseases (n=5,849). Mean TPMT activity was 20.1 ± 6 U/mL, but differed depending on the disease (P < .001). TPMT distribution was low (<5) in 0.5%; intermediate (5.0–13.7) in 11.9%; or high (≥13.8) in 87.6%. Only when TPMT activity was considered separately in each disease did it reveal a normal distribution. In the multivariate analysis, gender, hematocrit, and treatment with 5-aminosalicylates/steroids/azathioprine/6-MP statistically influenced TPMT activity, although, probably, in a clinically irrelevant manner. This study shows, in a large sample of 14,545 patients, that 0.5% had low TPMT activity, indicating a higher risk of myelotoxicity with azathioprine/6-MP, a figure similar or slightly higher than that reported in other areas. Nevertheless, the trimodal distribution of TPMT activity varied depending on disease, and the proportion of patients with low activity values ranged from 0–0.8%. The drugs prescribed for the treatment of autoimmune diseases, including azathioprine/6-MP, modified TPMT activity, but the magnitude of this effect was very small and the differences found are probably irrelevant from the clinical point of view.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Azathioprine and its metabolite 6-mercaptopurine (6-MP) are purine analogs with immunosuppressive activity. They are prescribed in several autoimmune diseases, such as autoimmune hepatitis [1], inflammatory bowel disease (IBD) [2, 3], or multiple sclerosis [4], among others. The choice of the dose of azathioprine and 6-MP is generally based on patient weight, with the intention to achieve the highest therapeutic efficacy and, at the same time, to reduce the incidence of adverse effects, although this aim is not always possible. Several strategies have been suggested to individualize the thiopurine dose to identify both patients at risk for myelotoxicity as well as patients with subtherapeutic doses and inadequate immunosuppression [5]. These strategies include monitoring changes in the red cell mean corpuscular volume, induction of leukopenia, quantification of 6-thioguanine nucleotides, and the monitoring of thiopurine methyltransferase (TPMT) activity. Quantification of TPMT activity has been considered a promising area, because it may identify unique metabolic profiles in patients at high risk for adverse reaction prior to drug exposure [5].
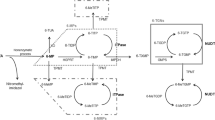
Azathioprine and 6-MP are inactive compounds that must be metabolized to 6-thioguanine nucleotides to exert their cytotoxic and immunosuppressive properties. Azathioprine is a prodrug that is absorbed into the plasma and rapidly converted to 6-MP, via a nonenzymatic process. 6-MP is then metabolized by three competing enzymes: xanthine oxidase, TPMT, and hypoxanthine-guanine phosphoribosyltransferase. Xanthine oxidase metabolizes 6-MP into inactive 6-methylmercaptopurine, and hypoxanthine-guanine phosphoribosyltransferase metabolizes 6-MP into the 6-thioguanine nucleotides, which are believed responsible for the therapeutic activity as well as drug-related leukopenia [6]. Therefore, reduction in TPMT activity predisposes to severe bone marrow suppression because of preferential metabolism of 6-MP to 6-thioguanine nucleotides [7].
TPMT enzymatic activity seems to be the most important metabolic factor for the regulation of 6-thioguanine nucleotides. High concentrations of 6-thioguanine nucleotides are detected in patients with low activity of TPMT, and low concentrations of these metabolites are found in patients with high TMPT activity [8–10]. Marked interindividual variability of azathioprine pharmacokinetics is due partly to a significant genetic polymorphism of the TMPT activity [11]. In this respect, from a genotypic point of view, Weinshilboum and Sladek [12] studied, more than two decades ago, a random sample population of approximately 300 individuals, and found the following trimodal distribution of TPMT activity: 88.6% were homozygous for the high activity allele (TPMTHH), 11.1% were heterozygous (TPMTHL), and only 0.3% were homozygous for the low activity allele (TPMTLL).
TPMT activity has been evaluated in patients with different diseases, and it has been suggested that the aforementioned trimodal distribution may differ depending on the clinical status of the patient [13, 14]. Moreover, among patients with the same disease (e.g., IBD), the frequency with which the low TPMT activity genotype or phenotype is found has been markedly different in several studies [5]. This represents a clinically relevant topic, because it has been assumed that the incidence of hematologic adverse effects in a specific population will depend on the pattern of TPMT activity (specially on the proportion of patients with low TPMT activity) in such a population.
The aim of our study was to assess the activity of TPMT in a large sample of 14,545 Spanish patients with different diseases eligible for treatment with azathioprine or 6-MP, and to evaluate the influence of several variables (including the treatment with these drugs) on TPMT activity; and ii) to evaluate the proportion of patients with low TPMT activity and, therefore, a higher risk of myelotoxicity when treated with azathioprine or 6-MP.
Methods
Patients
TPMT activity in red blood cells (RBCs) was measured in 14,545 patients with autoimmune/inflammatory diseases in a reference laboratory for several Spanish hospitals between 1998 and 2003. Application of TPMT activity determination was addressed to a single laboratory (Departamento de Bioquímica y Biología Molecular de la Universidad de Alcalá), and it was accompanied by a questionnaire where information regarding the following variables was included: reference hospital, age, gender, hematocrit, and treatment for the autoimmune disease (steroids, azathioprine, 6-MP, 5-aminosalycilates). Informed consent was obtained from all patients.
Analysis of TPMT activity
Sample collecting and processing (carried out within a 24-hour period from the extraction) were performed by qualified personal using standardized sampling methods. Samples of venous blood were collected in 5-mL heparinized vacutainer tubes and maintained at 4 °C. The samples were then centrifuged at 800 g for 15 min at 4 °C; the plasma and the buffy coat were discarded and RBCs were washed twice with 0.9% NaCl solution. Two milliliters of packed RBC were resuspended in four volumes of ice-cold water. This step results in the lysis of RBC. The lysate was centrifuged at 13,000 g for 10 min and the supernatant was used immediately for enzyme assays or stored at −85 °C; in this condition, the enzyme remains stable for several weeks. RBC TPMT activity was measured by a radiochemical method as previously described [15]. This procedure is based on the conversion of 6-MP to 6-methylmercaptopurine, using S-adenosyl-l-[methyl-3H]methionine as methyl donor. The assay was performed in a total volume of 150 mL by sequential addition of 5 mL of 6-MP (90 mmol) in dimethyl sulfoxide (DMSO) or 5 mL of DMSO alone, 15 mL of a mixture of dithiothreitol (DTT)/allopurinol in potassium phosphate buffer (150 mmol; pH 7.5), 15 mL of nonradioactive S-adenosyl-l-methionine (SAMe, 250 mmol), 15 mL of radioactive SAMe (50 nmol, final concentration) and finally 100 mL of erythrocyte lysate. DTT and allopurinol final concentrations were 5 mmol and 25 mmol, respectively. The specific activity of S-adenosyl-l-[methyl-3H]methionine was 15 Ci/mmol. The reaction tubes were incubated for 1 hour at 37 °C and the reaction was stopped by adding 200 mL of 0.5 mol borate buffer (pH 10). For the extraction of the reaction product, 2.5 mL of 20% isoamyl alcohol in toluene was added and the tubes were mixed vigorously for 10 seconds followed by centrifugation at 700 g for 5 min. A 1-mL aliquot of the organic phase was placed in a vial with 2 mL of scintillation cocktail and radioactivity was measured in a liquid scintillation counter. Results were corrected for quench and counting efficiency (50%) as well as for partitioning of the reaction product into the organic phase (70%). The enzyme activity was expressed as international units (U/mL RBC, nanomoles of 6-methylmercaptopurine formed per hour per milliliter of packed RBC).
Statistical analysis
For quantitative variables, mean and standard deviation were calculated. For categorical variables, percentages and corresponding 95% confidence intervals (95% CI) were provided. Kolmogorov-Smirnov test was used to evaluate whether TPMT activity followed a normal (Gaussian) distribution. Mean TPMT activity depending on several variables were compared using the Wilcoxon test (when two samples were compared), or the ANOVA test (when more than two samples were compared). A P value < .05 was considered statistically significant. A multiple linear regression analysis was performed. The dependent variable was the TMPT activity, and the independent variables were age (categorized as higher or lower than 40 years, which was the median value), gender (male/female), disease (IBD, autoimmune hepatitis, multiple sclerosis, myasthenia gravis, or pemphigus), hematocrit value (categorized as higher or lower than 39, which was the median value), and treatment with 5-aminosalicylates, steroids, or azathioprine/6-MP. Finally, analysis of the linear regression model’s residuals (the observed value of the dependent value minus the value predicted by the regression equation) was conducted, to evaluate whether the these residuals followed a normal distribution.
Results
Demographic variables
A total of 14,545 patients were included in the study. The mean age was 40 ± 16 (standard deviation) years, and 49% were men. Diseases included in the study (number and respective percentages) were autoimmune hepatitis (359 patients, 2.5%), ulcerative colitis (1,510 patients, 10%), Crohn disease (4,944 patients, 34%), indeterminate colitis (592 patients, 4%), multiple sclerosis (814 patients, 5.6%), myasthenia gravis (344 patients, 2.4%), pemphigus (133 patients, 0.9%), and other diseases with <100 patients included (Beçet disease, scleroderma, systemic lupus erythematosus, polymyositis, polymyalgia, psoriasis, atopic eczema, uveitis, vasculitis, hemolytic anemia, dermatomyositis, lung fibrosis, glomerulonephritis, and chronic myeloid leukemia). Hematocrit mean value was 39.1 ± 5%, and it was higher in males than in females (40.3 versus 38.1, respectively; P < .001). TPMT activity began to be quantified in Spain in 1998, and in that year 244 determinations were applied for (1.7% of the total). The number of applications progressively increased in the following years, up to 2003, when the maximum of 3,407 determinations were reached (24% of the total). Regarding medical treatment at the time of TPMT determination, the percentage of patients receiving each drug was 5-aminosalycilates (4.7%), steroids (26.2), azathioprine or 6-MP (44.8), and infliximab (0.1%).
TPMT activity
Mean TPMT activity was 20.1 ± 6 U/mL RBCs (minimum 0, maximum 46.4). Mean TPMT levels depending on the patients’ disease were IBD (20.4 ± 6), autoimmune hepatitis (21.5 ± 6), multiple sclerosis (18.4 ± 6), myasthenia gravis (20.9 ± 6), and pemphigus (21.1 ± 6). Differences among these values were statistically significant (ANOVA, P < .001). Distribution of TPMT activity in three categories (low, intermediate, and high, based on a classification previously suggested and classically used [16]) is graphically represented in Fig. 1, where it can be observed that 0.5% of the patients had values <5 U/mL RBCs (low levels), 11.9% had values between 5 and 13.7 U/mL RBCs (intermediate levels), and most of the patients (87.6%) had ≥13.8 U/mL RBCs (high levels). The percentage of patients having low, intermediate, and high levels of TPMT activity in each disease group is summarized in Table 1; statistically significant differences were demonstrated when comparing those percentages (P < .001).
Distribution of TPMT activity in our study population, which is graphically represented in Fig. 2, did not follow a normal distribution (P < .001; Kolmogorov-Smirnov Z = 2.87). However, when TPMT activity was considered separately in each disease (autoimmune hepatitis, IBD, multiple sclerosis, myasthenia gravis, and pemphigus), it revealed a normal distribution (Fig. 2). Nevertheless, visual exploration of the graphic in the overall population (Fig. 2, first graphic) showed that the distribution of TPMT values was markedly similar to a Gaussian (normal) one, and it was therefore decided to perform the multiple linear regression analysis. Furthermore, analysis of the linear regression model’s residuals showed that these followed a normal distribution.
As summarized in Fig. 3, differences (P < .001) were demonstrated in TPMT activity in the univariate study depending on gender (male, 20.4; female, 19.9 U/mL) and treatment with azathioprine/6-MP (no treatment, 20.7; treatment, 21.2 U/mL). However, no differences were demonstrated when TPMT activity was compared depending on the remaining variables: age, treatment with 5-aminosalycilates or steroids, and hematocrit value. In the multivariate analysis, the variables associated with TPMT activity were gender, hematocrit, and treatment with 5-aminosalicylates, steroids and azathioprine/6-MP (Table 2).
Discussion
Several strategies have been suggested with the aim of choosing the appropriate azathioprine/6-MP dose, with the intention, on one hand, to identify patients at risk of myelotoxicity and, on the other hand, to detect patients receiving subtherapeutic doses and consequent inadequate immunosuppression [5]. Among these strategies, the monitoring of TPMT activity is considered the most encouraging [5]. Nevertheless, there are conflicting results on the role of TPMT in optimizing therapy, for example, in patients with IBD [5]. Degree of TPMT activity deficit is related to the period of time between azathioprine therapy prescription and hematologic adverse effects presentation. Homozygous patients with low-activity allele present a latent period of only few weeks, whereas in heterozygous patients the time span is longer [5]. Thus, factors other than TPMT deficiency, such as concomitant drugs or environmental factors, could be related with late myelotoxicity appearing in patients treated with azathioprine. In Spain, TPMT activity assessment began to be quantified in 1998, when only 244 determinations were done; this figure has progressively increased through 2003, when 3,407 determinations were done.
Marked interindividual variability of azathioprine pharmacokinetics is due partly to a significant genetic polymorphism of the TMPT activity [11]. A trimodal distribution of TPMT activity has been described [12], where most patients (approximately 90%) are homozygous for the high-activity allele (TPMTHH), approximately only 0.3% are homozygous for the low-activity allele (TPMTLL), and the remaining (approximately 10% of the patients) are heterozygous (TPMTHL). Later, other authors have quantified the activity of this enzyme depending on the genotype of the patient [16], finding the following values: homozygous subjects for the high-activity allele (high levels, >13.8 U/mL RBCs); heterozygous subjects (intermediate levels, between 5 and 13.7 U/mL); and homozygous subjects for the low-activity allele (low levels, <5 U/mL). In our study, mean basal TPMT activity was 20.1 U/mL, with a minimum value of 0 and a maximum value of 46. The analysis of the distribution of TPMT values in these three categories showed that 0.5% of our patients had low levels (<5 U/mL) of TPMT activity, 11.9% had intermediate levels, and most patients (87.6%) had high levels, in accordance with the trimodal distribution.
TPMT activity has been evaluated in patients with quite different diseases, and it has been suggested that the aforementioned trimodal distribution may differ depending on disease [13, 14]. Differences among TPMT values corresponding to the different diseases included in our study were statistically significant, the figures ranging from 18.4 U/mL RBCs in multiple sclerosis to 21.5 in autoimmune hepatitis. Furthermore, the percentage of patients having low, intermediate, and high levels in each disease group was also different; as an example, 0.8% of the patients with autoimmune hepatitis had low TPMT levels, whereas this was the case of no patient with myasthenia gravis or pemphigus.
Although the graphical representation of the distribution of TPMT activity, including all of our study population, seemed to follow a normal distribution (see Fig. 2), statistical testing showed that TPMT distribution was not Gaussian. However, the large sample size (14,545 patients) and the consequent extreme statistical power could explain the fact that very small differences from the clinical point of view may reach statistical significance. However, when TPMT activity was considered separately in each disease (autoimmune hepatitis, IBD, multiple sclerosis, myasthenia gravis, and pemphigus), it revealed a normal distribution. Nevertheless, the graphical representation of TPMT data clearly showed that distribution differed depending on disease. It has been suggested that the unimodal or normal distribution of TPMT activity is more characteristic of some Jewish [17], French [18], or East Asian populations [19]. On the contrary, in other European [20] and North American [21] populations a more evident trimodal distribution has been described.
Two strategies exist to identify patients with TPMT activity deficiency: the quantification of the activity of this enzyme in the erythrocytes (phenotype) and the determination of different cellular DNA mutations (genotype), and strong concordance between both procedures have been reported [5]. It has been suggested that phenotype evaluation (by the study of TPMT erythrocyte activity) could give more information than genotyping as for the metabolic status, which can be altered by environmental factors (e.g., food, treatments, uremia, transfusion) with either induction or inhibition of enzyme activity [21]. In this respect, differences were demonstrated in our patients when comparing TPMT activity depending on gender, although the clinical relevance of the very small differences found seems unclear.
It has been reported that azathioprine/6-MP itself can increase TPMP activity. In our study, the multivariate analysis showed that treatment with these drugs was associated with higher TPMT activity, but the magnitude of this association was very small and the differences found were minimal (20.7 versus 21.2 U/mL RBCs). Again, the large sample size could be responsible for the demonstration of statistically significant differences with, probably, clinically irrelevant differences. On the other hand, other studies could not find any correlation between azathioprine/6-MP treatment and TPMT activity [13, 22, 23]. Furthermore, studies reporting significant rises in TPMT activity after azathioprine have predominantly been in renal [24–27] or cardiac [28] transplantation, or in patients with leukemia [29–31]. These patients have been initiated on other concomitant medications that may also be responsible for TPMT induction in their own right. On the other hand, it has recently been shown that uremia in renal transplant is a significant inducer of TPMT activity [26]. Only one study to date has addressed the issue of TMPT activity in healthy controls following the administration of 6-MP, and reported no induction of TPMT activity [32]. Finally, several pharmacologic studies, performed both in vitro and in vivo, have reported inhibition of this enzyme and an increase of 6-thioguanine nucleotides owing to administration of sulfasalazyne or 5-aminosalicylates, both drugs frequently prescribed in patients with IBD [10, 33–36]. In this respect, treatment with 5-aminosalycilates in our patients was associated, in the multivariate analysis, with higher TPMT activity, but, again, differences (20.9 versus 21.2 U/mL RBCs) are probably irrelevant clinically. Finally, other authors could not demonstrate this relationship between treatment with 5-aminosalycilates and TPMT activity, both in vitro [37] and in vivo [22, 23, 38].
Finally, the question whether TPMT activity monitoring is systematically indicated in all patients who are going to receive azathioprine or 6-MP is still a matter of debate. Although low TPMT activity homozygous patients represent only approximately 0.3% of the general population, heterozygous patients represent at least 10% [12], so more clinical and cost–benefit studies are needed to clarify this issue. TPMT activity determination would be cost effective in all patients if we take into account the great cost treatment of myelotoxicity induced by azathioprine therapy. In this way, two recent studies have demonstrated, using decision analysis models, that the use of pretreatment screening for TPMT in IBD patients commencing azathioprine therapy represents a cost-effective strategy [39, 40].
In summary, this study shows that in a large sample of Spanish patients with different disorders amenable to treatment with purine analogs, 0.5% had low TPMT activity (<5 U/mL RBCs, indicating a higher risk of myelotoxicity when treated with these drugs), a figure similar or slightly higher than that reported in other geographical areas. Nevertheless, the trimodal distribution of TPMT activity varied depending on the disease and the proportion of patients with low activity values ranged from 0.0–0.8%. The knowledge of the TPMT activity distribution in each population seems relevant; the incidence of hematologic adverse effects associated with azathioprine/6-MP treatment probably depends on that distribution. Finally, the drugs prescribed for the treatment of autoimmune diseases, including azathioprine/6-MP, modified TPMT activity, but the magnitude of this effect was very small and the differences found are probably clinically irrelevant.
References
Czaja, AJ (2002) Treatment of autoimmune hepatitis. Semin Liver Dis 22:365–378
Sandborn, W, Sutherland, L, Pearson, D, May, G, Modigliani, R, Prantera, C (2000) Azathioprine or 6-mercaptopurine for inducing remission of Crohn’s disease. Cochrane, Database Syst, Rev CD000545
Pearson, DC, May, GR, Fick, G, Sutherland, LR (2000) Azathioprine for maintaining remission of Crohn’s disease. Cochrane, Database Syst, Rev CD000067
Fernandez, O, Fernandez, V, DeRamon, E (2004) Azathioprine and methotrexate in multiple sclerosis. J Neurol Sci 223:29–34
Gisbert, JP, Gomollon, F, Mate, J, Pajares, JM (2002) Individualized therapy with azathioprine or 6-mercaptopurine by monitoring thiopurine methyl-transferase (TPMT) activity. Rev Clin Esp 202:555–562
Tidd, DM, Paterson, AR (1974) A biochemical mechanism for the delayed cytotoxic reaction of 6- mercaptopurine. Cancer Res 34:738–746
Lennard, L, VanLoon, JA, Weinshilboum, RM (1989) Pharmacogenetics of acute azathioprine toxicity: relationship to thiopurine methyltransferase genetic polymorphism. Clin Pharmacol Ther 46:149–154
Dubinsky, MC, Lamothe, S, Yang, HY, Targan, SR, Sinnett, D, Theoret, Y, et al (2000) Pharmacogenomics and metabolite measurement for 6-mercaptopurine therapy in inflammatory bowel disease. Gastroenterology 118:705–713
Anstey, A, Lennard, L, Mayou, SC, Kirby, JD: Pancytopenia related to azathioprine—an enzyme deficiency caused by a common genetic polymorphism (1992) a review. J R Soc Med 85:752–756
Lowry, PW, Franklin, CL, Weaver, AL, Gennett Pike, M, Mays, DC, Tremaine, WJ, et al. (2001) Measurement of thiopurine methyltransferase activity and azathioprine metabolites in patients with inflammatory bowel disease. Gut 49:665–670
Lennard, L (1999) Therapeutic drug monitoring of antimetabolic cytotoxic drugs. Br J Clin Pharmacol 47:131–143
Weinshilboum, RM, Sladek, SL (1980) Mercaptopurine pharmacogenetics: monogenic inheritance of erythrocyte thiopurine methyltransferase activity. Am J Hum Genet 32:651–662
Menor, C, Fueyo, J, Escribano, O, Pina, MJ, Redondo, P, Cara, C, et al. (2002) Thiopurine methyltransferase activity in a Spanish population sample: decrease of enzymatic activity in multiple sclerosis patients. Mult Scler 8:243–248
Decaux, G, Horsmans, Y, Houssiau, F, Desager, JP (2001) High 6-thioguanine nucleotide levels and low thiopurine methyltransferase activity in patients with lupus erythematosus treated with azathioprine. Am J Ther 8:147–150
Menor, C, Fueyo, JA, Escribano, O, Cara, C, Fernandez-Moreno, MD, Roman, ID, et al. (2001) Determination of thiopurine methyltransferase activity in human erythrocytes by high-performance liquid chromatography: comparison with the radiochemical method. Ther Drug Monit 23:536–541
Snow, JL, Gibson, LE (1995) The role of genetic variation in thiopurine methyltransferase activity and the efficacy and/or side effects of azathioprine therapy in dermatologic patients. Arch Dermatol 131:193–197
Lowenthal, A, Meyerstein, N, Ben-Zvi, Z (2001) Thiopurine methyltransferase activity in the Jewish population of Israel. Eur J Clin Pharmacol 57:43–46
Spire-Vayron de la Moureyre, C, Debuysere, H, Mastain, B, Vinner, E, Marez, D, Lo Guidice, JM, et al. (1998) Genotypic and phenotypic analysis of the polymorphic thiopurine S- methyltransferase gene (TPMT) in a European population. Br J Pharmacol 125:879–887
Park-Hah, JO, Klemetsdal, B, Lysaa, R, Choi, KH, Aarbakke, J (1996) Thiopurine methyltransferase activity in a Korean population sample of children. Clin Pharmacol Ther 60:68–74
Kroplin, T, Weyer, N, Gutsche, S, Iven, H (1998) Thiopurine S-methyltransferase activity in human erythrocytes: a new HPLC method using 6-thioguanine as substrate. Eur J Clin Pharmacol 54:265–271
Szumlanski, CL, Honchel, R, Scott, MC, Weinshilboum, RM (1992) Human liver thiopurine methyltransferase pharmacogenetics: biochemical properties, liver-erythrocyte correlation and presence of isozymes. Pharmacogenetics 2:148–159
Campbell, S, Kingstone, K, Ghosh, S (2002) Relevance of thiopurine methyltransferase activity in inflammatory bowel disease patients maintained on low-dose azathioprine. Aliment Pharmacol Ther 16:389–398
Gisbert, JP, Luna, M, Mate, J, Gonzalez-Guijarro, L, Cara, C, Pajares, JM (2003) Thiopurine methyltransferase activity and myelosuppression in inflammatory bowel disease patients treated with azathioprine and 6-mercaptopurine. Med Clin (Barc) 121:1–5
Mircheva, J, Legendre, C, Soria-Royer, C, Thervet, E, Beaune, P, Kreis, H (1995) Monitoring of azathioprine-induced immunosuppression with thiopurine methyltransferase activity in kidney transplant recipients. Transplantation 60:639–642
Thervet, E, Anglicheau, D, Toledano, N, Houllier, AM, Noel, LH, Kreis, H, et al. (2001) Long-term results of TMPT activity monitoring in azathioprine-treated renal allograft recipients. J Am Soc Nephrol 12:170–176
Weyer, N, Kroplin, T, Fricke, L, Iven, H (2001) Human thiopurine S-methyltransferase activity in uremia and after renal transplantation. Eur J Clin Pharmacol 57:129–136
Chocair, PR, Duley, JA, Simmonds, HA, Cameron, JS (1992) The importance of thiopurine methyltransferase activity for the use of azathioprine in transplant recipients. Transplantation 53:1051–1056
Schutz, E, Gummert, J, Mohr, FW, Armstrong, VW, Oellerich, M (1995) Azathioprine myelotoxicity related to elevated 6-thioguanine nucleotides in heart transplantation. Transplant Proc 27:1298–1300
Lennard, L, Van Loon, JA, Lilleyman, JS, Weinshilboum, RM (1987) Thiopurine pharmacogenetics in leukemia: correlation of erythrocyte thiopurine methyltransferase activity and 6-thioguanine nucleotide concentrations. Clin Pharmacol Ther 41:18–25
Lennard, L, Lilleyman, JS, Van Loon, J, Weinshilboum, RM (1990) Genetic variation in response to 6-mercaptopurine for childhood acute lymphoblastic leukaemia. Lancet 336:225–229
McLeod, HL, Relling, MV, Liu, Q, Pui, CH, Evans, WE (1995) Polymorphic thiopurine methyltransferase in erythrocytes is indicative of activity in leukemic blasts from children with acute lymphoblastic leukemia. Blood 85:1897–1902
Keuzenkamp-Jansen, CW, Leegwater, PA, De Abreu, RA, Lambooy, MA, Bokkerink, JP, Trijbels, JM (1996) Thiopurine methyltransferase: a review and a clinical pilot study. J Chromatogr B Biomed Appl 678:15–22
Szumlanski, CL, Weinshilboum, RM (1995) Sulphasalazine inhibition of thiopurine methyltransferase: possible mechanism for interaction with 6-mercaptopurine and azathioprine. Br J Clin Pharmacol 39:456–459
Lewis, LD, Benin, A, Szumlanski, CL, Otterness, DM, Lennard, L, Weinshilboum, RM, et al. (1997) Olsalazine and 6-mercaptopurine-related bone marrow suppression: a possible drug-drug interaction. Clin Pharmacol Ther 62:464–475
Lowry, PW, Franklin, CL, Weaver, AL, Szumlanski, CL, Mays, DC, Loftus, EV, et al. (2001) Leucopenia resulting from a drug interaction between azathioprine or 6-mercaptopurine and mesalamine, sulphasalazine, or balsalazide. Gut 49:656–664
Lowry, PW, Szumlanski, CL, Weinshilboum, RM, Sandborn, WJ (1999) Balsalazide and azathioprine or 6-mercaptopurine: evidence for a potentially serious drug interaction. Gastroenterology 116:1505–1506
Campbell, S, Ghosh, S (2001) Effective maintenance of inflammatory bowel disease remission by azathioprine does not require concurrent 5-aminosalicylate therapy. Eur J Gastroenterol Hepatol 13:1297–1301
Dubinsky, MC, Yang, H, Hassard, PV, Seidman, EG, Kam, LY, Abreu, MT, et al. (2002) 6-MP metabolite profiles provide abiochemical explanation for 6-MP resistance in patients with inflammatory bowel disease. Gastroenterology 122:904–915
Winter, J, Walker, A, Shapiro, D, Gaffney, D, Spooner, RJ, Mills, PR (2004) Cost-effectiveness of thiopurine methyltransferase genotype screening in patients about to commence azathioprine therapy for treatment of inflammatory bowel disease. Aliment Pharmacol Ther 20:593–599
Dubinsky, MC, Reyes, E, Ofman, J, Chiou, CF, Wade, S, Sandborn, WJ (2005) A cost-effectiveness analysis of alternative disease management strategies in patients with Crohn’s disease treated with azathioprine or 6-mercaptopurine. Am J Gastroenterol 100:2239–2247
Acknowledgment
Supported in part by a Grant from the Instituto de Salud Carlos III (C03/02). TPMT determinations were performed by a project of the “Ministerio de Educación y Cultura” (PM 98-0154), different agreements University-Company (60/2002, 7/2002), and a contract of collaboration with the Cytochrome spin-off (64/2003). They have all been financed by UCB-Celltech Pharma. Patient samples were submitted by hundreds of specialists and hospitals throughout Spain. We especially thank physicians, clinical laboratory specialists, and nurses for their commitment to this program.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gisbert, J.P., Gomollón, F., Cara, C. et al. Thiopurine Methyltransferase Activity in Spain: A Study of 14,545 Patients. Dig Dis Sci 52, 1262–1269 (2007). https://doi.org/10.1007/s10620-006-9119-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-006-9119-z