Abstract
There is a critical need to test how family contextual factors impact outpatient consumer functioning in schizophrenia. This is the first study of two companion studies reported here that tests family factors’ influence on consumer functioning. Ninety-three low income inner-city African American consumer-family dyads were tested to see the possible impact of family factors, based on the EE and family caregiver burden literatures, on consumer psychosocial functioning (work, social, and independent living). The results supported a model wherein greater amounts of family contact had a significant relationship with better consumer psychosocial functioning. Additionally, family dysfunction had a direct negative relationship to consumer psychosocial functioning while family pressures and resources had an indirect negative relationship to consumer psychosocial functioning. Results are in marked contrast to what impacted consumer clinical functioning for the same sample. The findings appear to confirm that family factors differently impact the domains of clinical and psychosocial functioning. These findings are new for understanding the contextual factors that impact consumer functioning, especially psychosocial functioning.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Research demonstrates that African American families generally favour kinship networks, extended family forms, and a strong family orientation (Knowlton 2003; Thornton 1998). Hence, understanding the impact of family factors on consumer functioning for African Americans living with schizophrenia is very important. Nonetheless, little is known about the specific ways that families impact these African American consumers.
The mental health literature concerning consumer and family functioning principally comes from the Expressed Emotion (EE) and caregiver burden literatures. For example, EE is specifically predictive for consumer outcomes such as rehospitalization and relapse although the level of EE must be increased for it to be predictive for African American consumers (Moline et al. 1985; Wuerker et al. 1999). Recent research demonstrates that the perception of family criticalness on the part of the African American consumer is more predictive than EE itself (Koneru and Weisman de Mamani 2007; Rosenfarb et al. 2006). The caregiver burden literature shows that although all families report a sense of burden, African American families report lower levels of burden than whites (Awad and Voruganti 2008; Baronet 1999).
Despite these findings, few efforts have been made to test how family factors such as level of EE and caregiver burden might impact consumer functioning while also testing for how such family factors impact each other (Bogren 1997; Scazufca and Kuipers 1996). No studies, as far as the authors are aware of, have tested numerous family factors and the impact these concurrently have on consumer functioning as a way of clarifying the family’s impact on African American outpatient consumers. The present study is the first of two studies to test the influence of family factors on two different functioning domains: psychosocial and clinical. This study tests a model of the relationships between family factors and the psychosocial functioning of outpatient African American adults living with schizophrenia.
African Americans Living with Schizophrenia and Their Families
In general, African American consumers and their families have been included in fewer clinical protocols while also having fewer clinical resources earmarked for them; this is particularly the case for poorer, urban African-American consumers and their families (McAdoo 1998; NIMH 2008; Williams and Fenton 1999; Workgroup., N. A. M. H. C. B. S. 2000). As noted above, the social networks, extended family forms, and a higher sense of a family-orientation often reported among African-American families (Alston and Turner 1994; Billingsley 1990; Wallace Williams et al. 2003; Williams and Fenton 1999) suggests the importance of clarifying which family factors may play a role in consumer functioning. Indeed, although much of the previous research on family factors on consumer functioning have assumed a deleterious effect (Kymalainen et al. 2006; Leff and Vaughn 1985; Saleebey 1996) research on African American families suggests these same factors can be an informal resource (Guada et al. 2009a, b). A recent study offered preliminary evidence that the influence of the family on psychosocial outcomes was beneficial for African American consumers with schizophrenia (Guada et al. 2009b). No research has tested to see if these factors have the same impact when included in the same study. Identifying these family factors is of critical importance for designing and implementing services specifically targeted to consumers from similar communities.
Consumer Psychosocial Functioning as Outcome
Historically, the concept of consumer functioning was a sort of umbrella term, which included rehospitalization, relapse, psychosocial functioning and symptom severity. Each of these was viewed as different sub-parts of the “consumer functioning” whole (Brekke et al. 2001; Brekke and Long 2000; Phillips et al. 2001). Recent studies have demonstrated, however, that symptom severity is typically only mildly correlated to consumer psychosocial functioning, for example (Brekke and Long 2000; Brekke et al. 1997; Inoue et al. 1997; Phillips et al. 2001). Thus, consumer functioning can be viewed as a set of two distinct but interrelated domains. As previously noted this is the first of two studies wherein the outcome pertains to the consumer psychosocial domain.
The US Department of Health and Human Services, in its supplement Mental Health: Culture, Race, and Ethnicity (Services., U. S. D. o. H. a. H. 2001) identified the critical need to identify the contextual factors, particularly family related, impacting the functioning of consumers from ethnic minority communities with a serious and persistent mental illness (NIMH 2008). However, despite there being a plethora of research about the family’s impact on relapse and rehospitalization, very little has been done in regards to their potential impact on consumer psychosocial functioning (Butzlaff and Hooley 1998; Karno et al. 1987; McFarlane and Cook 2007). Psychosocial functioning is arguably more applicable as an outcome because the vast majority of consumers spend more time in the community than ever before (Geller 2000; Lamb and Bachrach 2001; Mechanic 2008).
Psychosocial functioning is defined here as those areas that require social skills in order to function and cope with the daily demands of the social environment (Brekke and Long 2000; Brekke et al. 1997; Inoue et al. 1997; Phillips et al. 2001). The domains most typically included are work, independent living skills, and interpersonal/family relations (Brekke and Long 2000; Goodman et al. 1993).
Poor psychosocial functioning creates numerous individual, interpersonal, and social problems and it has been increasingly used as an outcome measure. Understanding contextual factors particularly familial factors that may be moderated by ethnicity is critically needed in designing both practice models and mental health policy so as to improve psychosocial functioning of consumers living with schizophrenia (NIMH 2008; Workgroup., N. A. M. H. C. B. S. 2000). The present study takes a “broader view” by concurrently testing family concepts hypothesized to impact consumer functioning and extends the research by using consumer psychosocial functioning as the outcome variable.
Study Hypotheses
The present study selected family factors based on the EE and burden literatures to test their impact on consumer psychosocial functioning for African American adults living with schizophrenia. Thus, for example, family communication style, interpersonal relationships, and level of dysfunction are included based on the EE literature (Anderson et al. 1986; Bebbington and Kuipers 1994; Karno et al. 1987; Leff and Vaughn 1981, 1985; McFarlane et al. 1991). Potential stressors such as resource availability and role demands are included based on the caregiver burden literature and Pearlin’s model of coping with caregiver stressors (Biegel et al. 1994; Cook et al. 1994; Jones et al. 1995; Pearlin et al. 1990; Rivera et al. 1997; Saldana et al. 1999). These findings are from numerous separate studies and the present study offers the opportunity to concurrently include these to test for relationships between family factors while also testing for their effect on consumer psychosocial functioning.
Specific hypothesized structural relationships between variables are based on the literature. For example, based on a model by Pearlin et al. (1997; 1990)—that the resources available to a family can influence its overall functioning—amount of family resources is hypothesized to impact the amount of family dysfunction, specifically, lower resources yield greater dysfunction. It is hypothesized that the amount of family pressures will have a direct negative effect on amount of family resources based on the burden literature that shows more family burden (a kind of family pressure) is related to fewer family resources (Baronet 1999; Li et al. 2007; Magana et al. 2007). In addition, the amount of family dysfunction is hypothesized to have a negative relationship with consumer psychosocial functioning based on EE studies (a kind of family dysfunction) (Barrowclough and Hooley 2003; Breitborde et al. 2007; McFarlane and Cook 2007). Finally, based on the aforementioned study that showed more family contact had an ameliorating effect on consumer psychosocial functioning, (Guada et al. 2009b) the amount of family contact is hypothesized to have a positive direct effect on consumer psychosocial functioning.
Finally, the use of structural equation modeling (SEM) enhances the interpretation of results, and increases our confidence in theoretically derived causal relationships in non-experimental data. SEM allows the use of several scales (observable indicators) to represent latent constructs (variables) while also testing the relationships between the latent constructs. Thus, more complex and multiple relationships are tested at the same time while more accurately modeling error. Such methodology avoids some of the inherent limitations of correlational and regression methods (Kline 2005; Knoke et al. 2002; Tomarken and Waller 2005).
Methods
Sample
The sample came from consumers and their families starting services at a local county mental health facility. The study was approved by the University of Southern California Institutional Review Board, and the Los Angeles County Department of Mental Health. All study participants signed informed consent to participate in the study.
Study subjects lived in South Central Los Angeles, which has a history of being one of the most economically challenged areas in the city with notable disparities in health and mental health care. The US Census Bureau reported that the average household income (in 1999 dollars) was $29,520 (the national average was $42,000 during the same period) with an employment rate of 50% (compared to national average of 64%). Consumer mean monthly income was 1,036.45 (or approximately $12,432 per year) making this a poor sample. The estimated income figures from 1999 figures are provided because families were enrolled and data was collected during the later 1990s and early 2000s. The sample consisted of 94 dyads of African-American consumers and a family member. A family reporter was selected in conference with the family and consumer. Data was collected at baseline before any intervention began.
Measures
Three of the latent variables (Family Pressure, Family Resources, and Family Dysfunction) refer to functioning of the family unit. The fourth (an observable variable) refers to amount of contact between consumer and family. The last latent variable, Consumer Psychosocial Functioning, refers to consumer functioning in the community.
Family Pressure Indicators
The Family Pressure Scale—Ethnic (FPRES-E) is a 64-item scale developed to measure the pressures unique to families from ethnic minority communities (McCubbin et al. 1996). A higher score indicates greater family pressure. The original internal reliability (Chronbach’s alpha) was .92 (McCubbin et al. 1996). The FPRES-E was the strongest predictor of family difficulties in a study with minority families (Native Hawaiian) thus suggesting the validity of the measure (McCubbin et al. 1996). The alpha for this study was .94. The family member representative responded to this scale.
The Financial Well-Being (FWB) subscale of the Family Inventory of Resource Management (FIRM) refers to the family’s ability to meet financial commitments. A higher score indicates greater financial well-being (McCubbin et al. 1996). It was created for use with ethnic minority families (McCubbin et al. 1996; McCubbin et al. 1998). The Chonbach’s alpha for this sample was .85. The FWB was recoded so that a higher score indicates greater financial pressures. The family member representative responded to this scale.
The Burden Assessment Scale (BAS) is a 19-item scale that measures family burden of families with a seriously mentally ill family member (Reinhard et al. 1994). A higher score signifies greater burden. Chronbach’s alpha for initial studies using the BAS were .91 and .89. Data on the validity of the BAS are available in Reinhard et al. (1994). The alpha for this study was .94. The BAS was previously used with African-American samples (Horwitz and Reinhard 1995). The family member representative responded to this scale.
Family Resources Indicators
The Social Support Index (SSI) is a 17-item scale that measures to what degree the family finds support in the community (McCubbin et al. 1996). It uses a 5-point Likert scale ranging from “Strongly Disagree” to “Strongly Agree”. Chronbach’s alpha for initial studies using the SSI was .82 (McCubbin et al. 1996). The alpha for this study was .75. The family member representative responded to this scale.
The Family Member Well-Being Index (FMWB) is an 8-item questionnaire that measures a family member’s health, energy, worry, cheerfulness, etc. (McCubbin et al. 1996). Each item is a 10-point Likert scale ranging from “Not (very much)” to “Very (much)”. The Cronbach’s alpha during development of the scale was .85. Standard scores, means, and standard deviations were tested on numerous ethnic groups including African-American families (McCubbin et al. 1996). The alpha for this study was .74. The family member representative responded to this scale.
Family Dysfunction Indicators
The McMaster Family Assessment Device (MFAD) is a 53-item questionnaire designed to assess families per the McMaster Model of Family Functioning (Epstein et al. 1983). A higher score indicates more dysfunction. Subscales include Problem-solving, Communication, Roles, Affective Responsiveness, Affective Involvement, and Behavior. Please refer to the original paper describing the subscales for further information (Miller et al. 2000).
The validity of the McMaster Family Assessment Device subscales demonstrated both concurrent and discriminate validity (Epstein et al. 1983; Kabacoff et al. 1990). The original Chronbach alpha’s for the six subscales ranged from .72–.92 (Epstein et al. 1983). Reliability was also analyzed with test–retest (Miller et al. 1985) with results ranging from .66 to .76. The alphas for this sample ranged from a high of .80 (Problem Solving) to a low of .40 (Communications), Because the alpha level for Communications was low one item was dropped, which increased its alpha to .53. The ethnic composition of the original samples used in the design of the scale was not listed (Friedmann et al. 1997; Kabacoff et al. 1990; King et al. 1997). The family member representative responded to this scale.
Family Contact
Contact with families is a simple count variable of number of times that the consumer reports having contact with a family member via phone or personal contact in the prior 2 months. The sum of all family (nuclear and extended) contacts was used given the extended family form of the sample (see “Results”). The consumer responded to this scale.
Consumer Psychosocial Functioning Footnote 1
The Role Functioning Scale (RFS) was designed as an assessment tool to rate the psychosocial functioning of seriously mentally ill clients (McPheeters 1984). It is made up of four subscales (Work, Independent Living, Family, and Social), in which raters score subjects on one of seven levels of functioning. A higher level (i.e. score) indicates better functioning. It has shown good reliability and disciminant validity with a sample of African-American clinical and non-clinical women (Goodman et al. 1993). The Chronbach’s alpha for this sample was 0.84. Interrater reliability was established using a protocol detailed in Brekke, et al. (1993). Ratings achieved kappa >.78 for all items (Brekke et al. 1993). Due to potential confounding problems between the Family Contact (FC) and RFS-Family subscale (RFS-F), the RFS-F was not included. The psychosocial outcome reflects social, work, and independent living domains. The consumer responded to this scale.
Analysis
Frequencies, measures of central tendency and dispersion, correlations matrices, analyses for normality and heteroscedicity were used for all indicators. A structural equation modeling (SEM) strategy was employed using AMOS 16.0. The model was tested by analyzing the measurement model and then the structural model using a number of goodness of fit indices. The Root Mean Square Error of Approximation (RMSEA) is a parsimony adjusted index that favors models that are more parsimonious (Kline 2005; Loehlin 1998). The general consensus is that a value of ≤.05 indicates a close approximation, a value of .06–.09 indicates reasonable approximation, and value of ≥.10 indicates poor approximation of error (Kline 2005). The Comparative Fit Index (CFI) is an index that compares the predicted model against a “null” or base model that assumes zero population variances across all observed variables (Kline 2005; Loehlin 1998). Most researchers accept that a value ≥.90 indicates a reasonable fit (Kline 2005). The Non-Normed Fit Index (NNFI), also known as the Tucker-Lewis Index (TLI), is a statistic that corrects for parsimony in that simpler models are favored (similar to the RMSEA) (Bentler and Bonett 1980; Kline 2005). The NNFI is a revision of the original NFI (Normed Fit Index), which tended to underestimate size-fit for smaller samples (Byrne 2001). The NNFI uses an index value from 0–1: the closer the value to 1 the better the fit (Kline 2005; Loehlin 1998).
Results
A total of 93 cases were used for all analyses and a summary of descriptive statistics are provided in Table 1. The majority of cases (n = 90) had information from both a family member and the consumer. In three cases information was only available for the family member (n = 1) or for the consumer (n = 2). Because of the Maximum likelihood estimation (ML) technique these latter cases could be used for analyses (Kline 2005; Loehlin 1998). Only one case from the original 94 cases had no information from either consumer or family member, and was dropped from all analyses. The vast majority of family reporters were women (86.2%) with a mean age of 47 years old (range 18–80). The relationships between consumer and family member were diverse, which suggests the importance of the extended family form for this sample. The average age of the consumer was 42 years old (range 23–64). Consumers lived with a family member on average 45 (SD = 72) days in the previous 6 months before entering the study. Sixty-three percent of consumers lived independently of any family members.
Table 2 summarizes descriptive statistics for each indicator by latent variable. The average number of family contacts was 79 contacts (SD = 111.28) in the prior 2 month period (slightly over once a day). The size of the standard deviation demonstrates that there was wide variation in how often a consumer had contact with family members (range 0–300+). This may be due to the fact that, although the majority of consumers lived independently, the vast majority lived in the same neighborhood as their families (e.g. in same building or on the same block). Other consumers had little to no contact with family members because their families lived in other cities or parts of the state.
Measurement Model Results
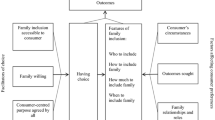
As shown in Fig. 1 the goodness-of-fit indices for the measurement model were: χ2 = 83.501, df = 68, P = .097, RMSEA = .05 (CL: .000–.083), CFI = .95, NNFI = .94. These measurement model indices included a non-significant P value indicating that the predicted and observed covariances were not significantly different from each other. Each latent variable had at least two indicators, and there were no substantial cross-loadings of indicators across latent variables per modification indices used to test for cross-loadings. Factor loadings for the measurement model ranged from a low .45 (McMaster Family Assessment Device—subscale Problem Solving on the Family Dysfunction factor) to a high of .77 (McMaster Family Assessment Device—subscale Affective Involvement on the Family Dysfunction factor).
Measurement model of family variables and consumer psychosocial functioning. χ2 = 83.501, df = 68, P = .097, RMSEA = .05 (CL: .000–.083), CFI = .95, NNFI = .94. Key for indicators 1, Burden Assessment Scale; 2, Family Pressure Scale—Ethnic; 3, Financial Well-Being Scale; 4, Social Support Index; 5, Family Member Well-Being; 6, McMaster Family Assessment Device (MFAD)—Problem Solving; 7, MFAD—Communication; 8, MFAD—Roles; 9, MFAD—Affective Responsiveness; 10, MFAD—Affective Involvement; 11, MFAD—Behavior Control; 12, Role Functioning Scale (RFS)—Work; 13, RFS—Independent Living; 14, RFS—Socialization
The correlations between family factors were all significant: Family Pressure and Family Resources (r = −.77, P = .001), Family Pressure and Family Dysfunction (r = .58, P = .000), and Family Resources and Family Dysfunction (r = −.74, P = .000). Clearly, these correlations are high, which might indicate a problem of colinearity (Kline 2005; Loehlin 1998). Nonetheless, none of the indicators cross-loaded nor were any of the error terms correlated in the measurement model. Hence, while the family latent variables were closely related, they were conceptually distinct enough to remain as separate concepts within the model.
Path (Structural) Model
The structural model was tested for specific relationships across latent family factors. To reiterate, based on a model by Pearlin (Pearlin et al. 1997; 1990)—that the resources available to a family can influence its overall functioning—the family factor Family Resources was modeled as an exogenous variable to Family Dysfunction. In addition, Family Pressures was modeled as an exogenous variable to Family Resources based on the burden literature that shows more family burden (a kind of family pressure) is related to fewer family resources (Baronet 1999; Li et al. 2007; Magana et al. 2007). It was hypothesized that as Family Pressures increased, Family Resources would decrease and amount of Family Dysfunction would increase. The model also included direct paths from Family Dysfunction and Family Contact to Consumer Psychosocial Functioning. It was hypothesized that as Family Dysfunction increased, Consumer Psychosocial Functioning would decrease. At the same time it was hypothesized that as Family Contact increased, Consumer Psychosocial Functioning would likewise increase.
The goodness-of-fit indices for the structural model were: χ2 = 95.292, df = 74, P = .05, RMSEA = .056, RMSEA confidence level (.005–.086), CFI = .93, NNFI = .92. The results demonstrate a reasonable fit although the p-value approached significance. Although the NNFI was not greater than .95, the value of .92 for a smaller sample signifies a reasonable fit (Byrne 2001). The direct paths between all latent variables were significant suggesting a plausible path model for explaining relationships between these variables for this sample (Fig. 2 shows the path estimates).
Discussion
This study offers new information regarding how family factors impact consumer functioning for African American consumers with schizophrenia. The study demonstrates what directly and indirectly impacts overall consumer psychosocial functioning as well as family functioning itself. Each of the hypothesized relationships was significant while the hypothesized model adequately fit the data. Specifically, the relationship between amount of family contact and consumer psychosocial functioning was positive and significant. This replicated a previous finding from a path model that found that amount of family contact had a significant positive relationship to consumer psychosocial functioning (Guada et al. 2009b). Thus, ongoing family contact appears to have a beneficial effect on the consumer’s ability to work, live independently, and to socialize. Ongoing contact with the family is a resource, in and of itself, for these consumers.
In addition, level of family dysfunction had a negative direct effect on psychosocial functioning: the more dysfunction the worse the psychosocial functioning. This is reminiscent of how level of Expressed Emotion (as a specific “kind” of family dysfunction) has a negative impact on a consumer’s level of relapse and re-hospitalization (Barrowclough and Hooley 2003). Hence, two family contextual processes differently impacted consumer psychosocial functioning at the same time. But, these are not necessarily contradictory because even families that have clinical problems can be a resource for a person with schizophrenia living in the community. In fact, the findings demonstrate that fewer family pressures and more family resources are related to improved family functioning, which in turn is related to improved consumer outcomes.
Additionally, the model demonstrated that the amount of family pressures and resources indirectly affected consumer psychosocial functioning by directly affecting the family’s level of functioning. Thus, as the amount of the family’s pressures increased, the family’s resources diminished; as the amount of their resources decreased, the family’s functioning worsened and as the family’s functioning worsened, the consumer’s psychosocial functioning worsened. These findings are reminiscent of findings within the caregiver burden and family treatment literatures. That is, as families experience more pressures and have fewer resources, their ability to adequately function as a family diminishes (NAMI 2003; Wallace Williams et al. 2003).
Thus, the findings suggest that as family pressures decrease, family resources would in turn increase; as family resources increase, the family’s functioning would improve resulting in improved consumer psychosocial. Concurrently, family contact had a significant beneficial impact on consumer functioning. This is a powerful finding since it suggests that the emotional connections between poorer African-American consumers and their families transcend both familial concrete (e.g. financial, discrimination, social supports) and abstract (e.g. sense of burden, sense of well-being) barriers (Wuerker et al. 1999). The study confirms previous research that shows that despite substantial challenges faced by families, they are a major resource for the well-being of consumers. It also provides quantitative evidence that suggests that family functioning is itself imbedded in a context and improvements in this domain are at least indirectly related to consumer outcomes. The study demonstrates the concurrent contextual impact for both consumer and family: consumers embedded in an extended family context that is itself embedded in a surrounding neighborhood context (Barrio 2001; Shurgot and Knight 2004).
Practice Implications
From this sample a clearer picture emerges about the importance of family context for consumer functioning for African American outpatient consumers particularly for functioning in the community. Psychosocial interventions for consumers should focus on the needs of their families as much as on the needs of the consumers. For example, interventions should assess and then assist, as necessary, increasing a family’s own level of social support. Interventions should likewise assist with any concrete pressures (e.g. financial issues or institution-based discrimination) and with decreasing the burden that families experience through psychoeducation, mutual aid groups, respite, and encouraging ongoing contact between consumer & family. The findings suggest that family-focused interventions should concentrate less on changing the family for the consumer’s sake as much as providing education, emotional support, resources and other necessary aids for the family’s sake. Hence, practice interventions targeting families from poorer, African-American populations should include issues around discrimination, financial resources, and increasing social networking, issues not typically included in family-oriented psychoeducation programs (Dixon et al. 2000). Such “family-centric” consumer interventions can both directly and indirectly help the consumer with areas of functioning most important for living in the community (i.e. work, independent living skills, and socialization). Traditional psychoeducation topics are obviously as important for poorer African-American families, but the findings suggest these programs need to include other issues to assist families faced with ongoing pressures and lack of resources. Addressing these issues while helping the overall family’s functioning will also help the consumer’s functioning in the community.
Study Limitations
Cross-sectional studies are limited in establishing causation. Longitudinal analyses are needed to clarify directionality and causality (Kline 2005; Knoke et al. 2002). A longitudinal study offers the advantage of evaluating any changes in the relationships between exogenous and endogenous variables across time. This would offer the opportunity to assess in greater detail how family factors (such as family pressures and overall functioning) change across time and how these changes directly and/or indirectly effect the psychosocial functioning of outpatient consumers with schizophrenia.
The sample size was not ideal for SEM statistical methodology although the sample was larger than what has been seen in previous EE and caregiver burden mental health studies (Baronet 1999; Butzlaff and Hooley 1998; Moline et al. 1985; Weisman et al. 2006; Wuerker et al. 1999). Sample sizes of 100 and more (ideally around 200–300) are recommended to increase power, model specification, and decrease potential technical problems with the analyses (Kline 2005). Thus, the sample size might account for some of the findings between family and consumer functioning variables.
Another potential issue is that there were different reporters across the indicators used for the latent variables. There could be reporter biases that affect the relationships between latent variables (Association, Association and Education 1999; DeVellis 1991; McIver and Carmines 1981). If only a family member, consumer, or an interviewer completed the scales, then relationships between variables may have been different. As previously noted, some studies show that when multiple members of a family report on the same phenomenon there is some divergence in the responses (Bogels and Brechman-Toussant 2006).
Conclusion
The findings are novel for the consumer outcomes literature, because it specifically focused on consumer psychosocial functioning and multiple and concurrent family factors’ impact on it. Likewise, the results offer further, powerful quantitative support that improving family functioning by decreasing the pressures that they face and increasing resources will both directly and indirectly assist outpatient poorer African-American consumers with schizophrenia in the critical areas of work, socialization, and living independently. Future studies will assist in determining whether these relationships are replicated with other African-American samples, whether these findings change over time, and/or are present in the lives of other ethnic and SES groups of consumers and their families. The present study offers a preliminary but vital understanding of the contextual, ecological mechanisms that contribute to psychosocial functioning for adults living with schizophrenia.
Additionally, the study’s results are in marked contrast to those found in the second companion study that tested many of the same family factors’ impact on consumer clinical functioning with the same sample. As will be seen, what impacts a consumer’s ability to live in the community is not what necessarily impacts their symptoms or rate of rehospitalization. Researchers, practitioners, and policy makers need to understand these differences so as to develop interventions that can improve the full spectrum of consumer outcomes.
Notes
In pre-analyses for this study, factors representing consumer clinical functioning and consumer psychosocial functioning were only mildly, albeit non-significantly correlated (r = −.24, P = .06) offering support to treat these as two separate domains and outcomes.
References
Alston, R. J., & Turner, W., L. (1994). A family strengths model of adjustment to disability for African American clients. Journal of Counseling and Development, 7(March/April), 378–383.
American Educational Research Association. (1999). Standards for educational and psychological testing (2nd ed.). Washington, DC: American Educational Research Association.
Anderson, C. M., Reiss, D. J., & Hogarty, G. E. (1986). Schizophrenia and the family. New York, New York: Guilford Press.
Awad, A. G., & Voruganti, L. N. P. (2008). The burden of schizophrenia on caregivers: A review. Pharmacoeconomics, 26(2), 149–162.
Baronet, A.-M. (1999). Factors associated with caregiver burden in mental illness: A critical review of the research literature. Clinical psychology review, 19(7), 819–841.
Barrio, C. (2001). Culture and schizophrenia: A cross-ethnic growh curve analysis. Journal of Nervous and Mental Disease, 189(10), 676–684.
Barrowclough, C., & Hooley, J. M. (2003). Attributions and expressed emotion: A review. Clinical psychology review, 23, 849–880.
Bebbington, P., & Kuipers, L. (1994). The predictive utility of expressed emotion in schizophrenia: An aggregate analysis. Psychological Medicine, 24, 707–718.
Bentler, P. M., & Bonett, D. G. (1980). Significance tests of goodness of fit in the analysis of covariance structures. Psychological Bulletin, 88(3), 588–606.
Biegel, D. E., Milligan, S. E., Putnam, P. L., & Song, L.-Y. (1994). Predictors of burden among lower socioeconomic status caregivers of persons with chronic mental illness. Community Mental Health Journal, 30(5), 473–494.
Billingsley, A. (1990). Understanding African-American family diversity. In Dewart, J. (Ed.), The state of black America. New York: National Urban League, Inc.
Bogels, S. M., & Brechman-Toussant, M. L. (2006). Family issues in child anxiety: Attachment, family functioning, parental rearing and beliefs. Clinical psychology review, 26, 834–856.
Bogren, L. Y. (1997). Expressed emotion, family burden, and quality of life in parents with schizophrenic children. Nordic Journal of Psychiatry, 57, 229–233.
Breitborde, N. J. K., Lopez, S. R., Wickens, T. D., Jenkins, J. H., & Karno, M. (2007). Toward specifying the nature of the relationship between expressed emotion and schizophrenia relapse: The utility of curvilinear models. International Journal of Methods in Psychiatric Research, 16(1), 1–10.
Brekke, J., & Long, J. D. (2000). Community-based psychosocial rehabilitation and prospective change in functional, clinical, and subjective experience variables in schizophrenia. Schizophrenia Bulletin, 26(3), 667–680.
Brekke, J., Levin, S., Wolkon, G., Sobel, G., & Slade, E. (1993). Psychosocial functioning and subjective experience in schizophrenia. Schizophrenia Bulletin, 19, 559–608.
Brekke, J., Raine, A., Ansel, M., Lencz, T., & Bird, L. (1997). Neuropsychological and psychophysiological correlates of psychosocial functioning in schizophrenia. Schizophrenia Bulletin, 23(1), 19–28.
Brekke, J., Kohrt, B., & Green, M. (2001). Neuropsychological functioning as a moderator of the relationship between psychosocial functioning and the subjective experience of self and life in schizophrenia. Schizophrenia Bulletin, 27(4), 697–708.
Butzlaff, R. L., & Hooley, J. M. (1998). Expressed emotion and psychiatric relapse: A meta-analysis. Archives of General Psychiatry, 55(June), 547–552.
Byrne, B. M. (2001). Structural equation modeling with AMOS—Basic concepts, applications, and programming. Mahwah, New Jersey: Lawrence Erlbaum Associates.
Cook, J. A., Lefley, H. P., Pickett, S. A., & Cohler, B. J. (1994). Age and family burden among patients of offspring with severe mental illness. American journal of orthopsychiatry, 64(3), 435–447.
DeVellis, R. F. (1991). Scale development: Theory & applications. Newbury Park, CA: Sage Publications.
Dixon, L., Adams, C., & Lucksted, A. (2000). Update on family psychoeducation for schizophrenia. Schizophrenia Bulletin, 26(1), 5–20.
Epstein, N. B., Baldwin, L. M., & Bishop, D. S. (1983). The McMaster family assessment device. Journal of marital and family therapy, 9(2), 171–180.
Friedmann, M. S., McDermut, W. H., Solomon, D. A., Ryan, C. E., Keitner, G. I., & Miller, I. W. (1997). Family functioning and mental illness: A comparison of psychiatric and nonclinical families. Family Process, 36, 357–367.
Geller, J. L. (2000). The last half-century of psychiatric services reflected in Psychiatric Services. Psychiatric Services, 51, 41–67.
Goodman, S. H., Sewell, D. R., Cooley, E. L., & Leavitt, N. (1993). Assessing levels of adaptive functioning: The role functioning scale. Community Mental Health Journal, 29(2), 119–131.
Guada, J., Brekke, J., Floyd, R., & Barbour, J. (2009a). Assessing the family functioning of inner-city African American families living with schizophrenia with the McMaster Family Assessment Device. Social work in mental health, In press.
Guada, J., Brekke, J., Floyd, R., & Barbour, J. (2009b). A path-analytic assessment of the relationships between perceived criticism and outcomes for African-American consumers with Schizophrenia. Community Mental Health Journal, 45(2), 106–116.
Horwitz, A. V., & Reinhard, S. C. (1995). Ethnic differences in caregiving duties and burden among parents and siblings of persons with severe mental illnesses. Journal of Health and Social Behavior, 36(2), 138–150.
Inoue, S., Tanaka, S., Shimodera, S., & Mino, Y. (1997). Expressed emotion and social function. Psychiatry Research, 72, 33–39.
Jones, S. L., Roth, D., & Jones, P. K. (1995). Effect of demographic and behavioral variables on burden on caregivers of chronic mentally ill persons. Psychiatric Services, 46(2), 141–145.
Kabacoff, R. I., Miller, I. W., Bishop, D. S., Epstein, N. B., & Keitner, G. I. (1990). A psychometric study of the McMaster family assessment device in psychiatric, medical, and nonclinical samples. Journal of family psychology, 3(4), 431–439.
Karno, M., Jenkins, J. H., de la Selva, A., Santana, F., Telles, C., Lopez, S., et al. (1987). Expressed emotion and schizophrenic outcomes among Mexican-American families. The Journal of Nervous and Mental Disease, 175(3), 143–151.
King, C., Hovey, J. D., Brand, E., Wilson, R., & Ghaziuddin, N. (1997). Suicidal adolescents after hospitalization: Parent and family impacts on treatment follow-through. Journal of the American Academy of Child & Adolescent Psychiatry, 36(1), 85–93.
Kline, R. B. (2005). Principles and practice of structural equation modeling (2nd ed.). New York: The Guilford Press.
Knoke, D., Bohrnstedt, G., & Potter Mee, A. (2002). Statistics for social data analysis (4th ed.). Belmont, CA: Wadsworth/Thomas Learning.
Knowlton, A. R. (2003). Informal HIV caregiving in a vulnerable population: Toward a network resource framework. Social Science and Medicine, 56(6), 1307–1320.
Koneru, V. K., & Weisman de Mamani, A. G. (2007). Acculturation and expressed emotion in Caucasian, Latino, and Black relatives of patients with schizophrenia. The Journal of Nervous and Mental Disease, 195(11), 934–938.
Kymalainen, J. A., Weisman, A. G., Rosales, G. A., & Armesto, J. C. (2006). Ethnicity, expressed emotion and communication deviance in family members of patients with schizophrenia. Journal of Nervous and Mental Disorders, 194, 391–396.
Lamb, H. R., & Bachrach, L. L. (2001). Some perspectives on deinstitutionalization. Psychiatric Services, 52, 1039–1045.
Leff, J., & Vaughn, C. (1981). The role of maintenance therapy and relative’s expressed emotion in relapse of schizophrenia: A two-year follow-up. British Journal of Psychiatry, 139, 102–104.
Leff, J., & Vaughn, C. (1985). Expressed emotion in families: Its significance for mental illness. New York: Guilford.
Li, J., Lambert, C. E., & Lambert, V. A. (2007). Predictors of family caregivers’ burden and quality of life when providing care for a family member with schizophrenia in the People’s Republic of China. Nursing and Health Sciences, 9, 192–198.
Loehlin, J. C. (1998). Latent variable models—an introduction to factor, path, and structural analysis (3rd ed.). Mahwah, NJ: Lawrence Erlbaum Associates, Publishers.
Magana, S. M., Ramirez Garcia, J. I., Hernandez, M. G., & Cortez, R. (2007). Psychological distress among Latino family caregivers of adults with schizophrenia: The roles of burden and stigma. Psychiatric Services, 58, 378–384.
McAdoo, H. P. (1998). African-American families: Strengths and realities. In H. I. McCubbin, E. A. Thompson, A. I. Thompson, & J. A. Futrell (Eds.), Resiliency in ethnic minority families: African-American families (Vol. 3, pp. 17–30). Thousand Oaks, CA: Sage Publications.
McCubbin, H. I., Thompson, A. I., & McCubbin, M. A. (1996). Family assessment: Resiliency, coping and adaptation—inventories for research and practice. Madison, Wisconsin: University of Wisconsin Publishers.
McCubbin, H. I., Thompson, E. A., Thompson, A. I., & Futrell, J. A. (1998). Resiliency in ethnic minority families: African-American families (Vol. 3). Thousand Oaks, CA: Sage Publications.
McFarlane, W. R., & Cook, W. L. (2007). Family expressed emotion prior to onset of psychosis. Family Process, 46, 185–197.
McFarlane, W. R., Deakins, S. M., Gingrich, S. L., Dunne, E., Horen, B., & Newmark, M. (1991). Multiple-family psychoeducation group treatment manual. New York, New York: Biosocial Treatment Division New York State Psychiatric Institute.
McIver, J. P., & Carmines, E. G. (1981). Unidimensional scaling. Newbury Park, CA: Sage Publications.
McPheeters, H. L. (1984). Statewide mental health outcome evaluation: A perspective of two southern states. Community Mental Health Journal, 20(1), 44–55.
Mechanic, D. (2008). Mental health and social policy: Beyond managed care (5th ed.). Boston: Allyn & Bacon.
Miller, I. W., Epstein, N. B., Bishop, D. S., & Keitner, G. I. (1985). The McMaster family assessment device: Reliability and validity. Journal of Marital and Family Therapy, 11(4), 345–356.
Miller, I. W., Ryan, C. E., Keitner, G. I., Bishop, D. S., & Epstein, N. B. (2000). The McMaster approach to families: Theory, assessment, treatment and research. Journal of Family Therapy, 22, 168–189.
Moline, R. A., Singh, S., Morris, A., & Meltzer, H. Y. (1985). Family expressed emotion in relapse in schizophrenia in 24 urban American patients. American Journal of Psychiatry, 142(9), 1078–1081.
NAMI. (2003). Family to Family: Recent studies of Family-to-Family. Retrieved 12/22/2006, from http://www.nami.org/Template.cfm?Section=Family-to-Family&template=/ContentManagement/ContentDisplay.cfm&ContentID=36366.
NIMH. (2008). National institute of mental health strategic plan. District of Columbia: National Institute of Mental Healtho. Document Number)
Pearlin, L. I., Mullan, J., Semple, S. J., & Skaff, M. M. (1990). Caregiving and the stress process: An overview of concepts and their measures. The Gerontologist, 30, 538–594.
Pearlin, L. I., Aneshensel, C. S., & LeBlanc, A. J. (1997). The forms and mechanisms of stress proliferation: The case of AIDS caregivers. Journal of Health and Social Behavior, 38(3), 223–236.
Phillips, E. S., Barrio, C., & Brekke, J. (2001). The impact of ethnicity on prospective functional outcomes from community-based psychosocial rehabilitation for persons with schizophrenia. Journal of Community Psychology, 29(6), 657–673.
Reinhard, S. C., Gubman, G. D., Horwitz, A. V., & Minsky, S. (1994). Burden Assessment Scale for families of the seriously mentally ill. Evaluation and Program Planning, 17(3), 261–269.
Rivera, R., Torres, M., & Carre, F. J. (1997). Role burdens: The impact of employment and family responsibilities in the Health status of Latino women. Journal of Health Care for the Poor and Underserved, 8, 99–113.
Rosenfarb, I. S., Bellack, A. S., & Aziz, N. (2006). Family interactions and the course of schizophrenia in African American and White patients. Journal of Abnormal Psychology, 115(1), 112–120.
Saldana, D. H., Dassori, A. M., & Miller, A. L. (1999). When is caregiving a burden? Listening to Mexican American women. Hispanic Journal of Behavioral Sciences, 21(3), 282–301.
Saleebey, D. (1996). The strengths perspective in social work practice: Extentions and cautions. Social Work, 41, 296–305.
Scazufca, M., & Kuipers, E. (1996). Links between expressed emotion and burden of care, in relatives of patients with schizophrenia. British Journal of Psychiatry, 168, 580–587.
Services., U. S. D. o. H. a. H. (2001). Mental health: Culture, race, and ethnicity-a supplement to mental health: A report of the surgeon general. Rockville, MD: US Department of Health and Human Services, Substance Abuse and Mental Health Services Administration, Center for Mental Health Services.
Shurgot, G. S. R., & Knight, B. G. (2004). Preliminary study investigating acculturation, cultural values, and psychological distress in Latino caregivers of dementia patients. Journal of Mental Health and Aging, 10(3), 183–194.
Thornton, M. C. (1998). Indigenous resources and strategies of resistance: Informal caregiving and racial socialization in black communities. In H. I. McCubbin, E. A. Thompson, A. I. Thompson, & J. A. Futrell (Eds.), Resiliency in ethnic minority families: African-American families (Vol. 3, pp. 49–66). Thousand Oaks, CA: Sage Publications.
Tomarken, A. J., & Waller, N. G. (2005). Structural equation modeling: Strengths, limitations, and misconceptions. Annual Review of Clinical Psychology, 1, 31–65.
Wallace Williams, S., Dilworth-Anderson, P., & Goodwin, P. Y. (2003). Caregiver role strain: The contribution of multiple roles and available resources in African-American women. Aging & Mental Health, 7(2), 103–112.
Weisman, A. G., Rosales, G. A., Kymalainen, J. A., & Armesto, J. C. (2006). Ethnicity, expressed emotion, and schizophrenia patients’ perceptions of their family members’ criticism. Journal of Nervous and Mental Disease, 194, 644–649.
Williams, D. R., & Fenton, D. T. (1999). The mental health of African Americans: Findings, questions, and directions. In I. L. Livingston (Ed.), Handbook of black American health—the mosaic of conditions, issues, policies, and prospects (pp. 253–268). Westport, CN: Greenwood Press.
Workgroup., N. A. M. H. C. B. S. (2000). Translating behavioral science into action: Report of the National Advisory Mental Health Council Behavioral Science Group (No. NIH Publication No. 00–4699). Bethesda, MD: National Institutes of Health/National Institute of Mental Healtho. Document Number.
Wuerker, A. K., Haas, G. L., & Bellack, A. (1999). Racial and gender differences in Expressed Emotion and interpersonal control in families of persons with schizophrenia. Family Process, 38(4), 477–496.
Conflict of interest
None for the any authors.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Guada, J., Hoe, M., Floyd, R. et al. How Family Factors Impact Psychosocial Functioning for African American Consumers with Schizophrenia. Community Ment Health J 48, 45–55 (2012). https://doi.org/10.1007/s10597-010-9365-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10597-010-9365-6