Abstract
The purpose of this study was to test a brief instrument to monitor the U.S. public’s attitudes about mental illness. A SAMHSA and CDC-led panel reached consensus through an iterative process to identify generic, multidimensional measures to test using a representative sample of 5,251 adults. Exploratory factor analysis revealed two subscales (Negative Stereotypes [α = 0.66]; Recovery and Outcomes [α = 0.69]). Confirmatory factor analysis supported the convergent validity of the two subscales. Subscale scores differed by sex, race/ethnicity, and experience with mental illness. Inclusion of these brief subscales on existing population-based surveys can help states and others track attitudes about mental illness.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The goals of the President’s New Freedom Commission on Mental Health are to advance the message that mental illness is real, common, and treatable; to eliminate barriers to accessing mental health services; and to reduce public and professional stigma associated with mental illness. Recommendations from the 2001 NIH (National Institutes of Health) sponsored International Conference on Stigma and Global Health called for documenting the burden of stigma, examining social causes and factors that amplify fear and discrimination, and developing and testing interventions to combat stigma across a variety of conditions, such as epilepsy, AIDS, SARS (severe acute respiratory syndrome), and mental illness (Keusch et al. 2006).
Relative to mental illness, stigma is defined as beliefs and attitudes associated with the perception of mental illness as an undesirable characteristic that discredits a person and that may result in social-distancing behaviors and discrimination (Jones et al. 1984; Link and Phelan 2001). Stigma is a barrier to those in need of treatment for mental illness and substance abuse, particularly minority men and women, military personnel, and other vulnerable adults (Ojeda and McGuire 2006; Gary 2005; Wynaden et al. 2005; Segal et al. 2005; Greene-Shortridge et al. 2007; Hoge et al. 2004). Mental disorders like depression, anxiety, and substance abuse and their associated stigma can increase social isolation, limit opportunities for employment, housing, and access to medical care (Smith 2002; Link and Phelan 2001, 2006; Stuart 2006). Stigma can also worsen symptoms and increase risk for coexisting physical disease (Chapman et al. 2005). Persistent structural stigma in the form of insurance barriers and inadequate systems of community support stifles effective efforts to prevent or treat mental illness, and has undesirable social and economic consequences such as the loss of productive workers; progression of poorly treated disease to additional disability, injury, or even death; and heightened care giving costs and interpersonal stress (Keusch et al. 2006; Link and Phelan 2006; Stuart 2005; Druss et al. 2000; Perlick et al. 2007; Schene et al. 1998; Corrigan et al. 2004).
VanBrakel’s (2006) recent review on measuring health-related stigma found that while the consequences of stigma are generally similar across different health conditions and cultures, most instruments developed to assess stigma are condition specific, thus limiting their generalizability and usefulness for tracking trends. Indeed, most research on the stigmatization of people with mental illness relates to people with more severe disorders such as schizophrenia and is presented in vignette form with its own sets of limitations and biases (Link et al. 2004; Kelly and Jorm 2007). Thus, an assessment of public attitudes toward people with mental illness (PWMI) in general, using a brief, generic instrument that could be used by states and communities on local surveillance systems can help them track trends in attitudes and identify local needs for program planning purposes.
In an effort to gauge public attitudes toward PWMI, the Center for Mental Health Services, Substance Abuse and Mental Health Services Administration (SAMHSA), and the Division of Adult and Community Health, National Center for Chronic Disease Prevention and Health Promotion, Centers for Disease Control and Prevention (CDC), collaborated to examine the general public’s perception of PWMI through a representative survey of approximately 5,000 community-dwelling U.S. adults.
Methods
SAMHSA, CDC staff, academic partners, and consumer representatives from SAMSHA with expertise in the areas of mental illness, stigma, and psychometric theory comprised a 19-member panel providing guidance on this project. For the purpose of this paper, this group will be referred to as the Mental Illness Stigma Panel members (MISPM).
Selection of a Stigma Instrument
Numerous scales developed to measure attitudes toward mental illness were reviewed by a SAMHSA contractor and by the MISPM (Taylor and Dear 1981; Cohen and Struening 1962; Link et al. 1987; Angermeyer and Matschinger 2004; Komiya 2000; Bogardus 1925; Bambauer and Prigerson 2006; Scottish Executive 2002; Crisp et al. 2000). The MISPM considered the strengths and weaknesses of a variety of scales and made judgments that were informed by the limitations of the current study. The social distance scales (Bogardus 1925; Link et al. 1987) required a vignette not amenable to the standardized survey used in this study, and would also have limited generalizability (Bogardus 1925; Link et al. 1987; VanBrakel 2006). Studies have shown that people rely on their cognitive schemas when responding to a vignette, and they may respond to the same vignette differently if, for example, the case patient is a man rather than a woman, or vice versa (Scottish Executive 2002; Link et al. 2004). Other possible scales focused on only one disorder and had not been extensively validated in the general population (Komiya 2000; Pyne et al. 2004; Bambauer and Prigerson 2006).
Ultimately, the MISPM selected validated items from the British Omnibus National Survey (ONS), developed by the Royal College of Psychiatrists to measure the stigma of mental illness, as model items for this study (Crisp et al. 2000, 2005).
The ONS is designed to assess the familiarity of people with some of the most common mental illnesses (e.g., severe depression, panic attacks, phobias, schizophrenia, substance abuse, eating disorder), general opinions about people with these specific mental illnesses, and beliefs about likely recovery outcomes for a person with these mental illnesses. As a face-to-face household survey, the ONS used the semantic differential technique to measure attitudes. For example, an ONS interviewer asked a respondent, “Now still thinking of someone with severe depression: I’d like you to choose the point on each of the scales on this card which best describes a person with severe depression. Which point would you choose for item (a)? Dangerous to others … Not dangerous to others”.
For practical reasons with respect to this study’s survey instrument and mode of administration, and for reasons of generalizability noted earlier, no specifications regarding the type of mental illness were made (e.g., a person with dysthymia vs. a person with schizophrenia). Similar to the format used in the Opinions about Mental Illness (OMI) Scale, respondents were expected to self-define the construct of mental illness (Cohen and Struening 1962; Taylor and Dear 1981). Theoretically, respondents’ attitudes can vary depending upon their beliefs and feelings about the cause, nature, treatment, and prognosis of mental illness (Antonak and Livneh 1988). Large-scale studies benefit from such underlying variability. The method of asking about beliefs and attitudes about an illness in general, as opposed to specific diagnoses, was recently used in assessing the U.S. public’s perceptions about people with epilepsy for the purpose of broad surveillance (DiIorio et al. 2004; Kobau et al. 2006). In this case, asking about attitudes toward people with epilepsy in general, rather than about people with specific types of epilepsy (e.g., Benign Rolandic Epilepsy; progressive myoclonic epilepsies; reflex epilepsies; temporal lobe epilepsy) and the multiple types of seizures an individual can have (e.g., absence seizures; atonic seizures; clonic seizures; simple partial seizures; complex partial seizures)—which would be cumbersome for surveillance—demonstrated sufficient variability by demographic characteristics. This suggested that respondents differed in their knowledge, experiences, and opinions relative to epilepsy. This conclusion was supported by the focus groups and cognitive testing undertaken for the epilepsy study, and the final items demonstrated acceptable validity and test–retest reliability in a representative sample of the U.S. population (DiIorio et al. 2004; Kobau et al. 2006).
The MISPM reached consensus on modifications to the ONS through a content validity exercise, and an iterative process. We retained the general ONS response format by providing response options with a positively or negatively phrased anchor for agreement or disagreement. The modified scale met recommendations identified for measuring stigma associated with mental illness (Link et al. 2004). The modified items were proposed for inclusion in Porter Novelli’s 2006 HealthStyles Survey and are shown in Table 1.
Data Collection Instrument
Porter Novelli’s HealthStyles survey, conducted annually in the U.S. since 1995, is designed to assess people’s attitudes and beliefs about chronic and infectious diseases and behaviors (e.g., their attitudes about HIV/AIDS, obtaining a flu shot, and their beliefs about vaccinations); exposure to health information and communication campaigns (e.g., breastfeeding campaign), and self-reported symptoms, diseases and disorders (Pollard 2002). HealthStyles 2006 was based on the results of two surveys mailed to panels of consumers in separate waves, which together comprise the Styles series. The sampling and data collection were conducted by Synovate, Inc. The sampling frame for the Synovate mail panel is purchased from one of the largest credit agencies in the U.S. and includes community-dwelling adults who have ever had utilities, a telephone, a credit card, a loan, a subscription, or similar consumer products registered in their name. Synovate constantly monitors the composition of its panel to identify demographic gaps on their panel (e.g., single men, minorities) and to keep the panel’s composition nationally representative and unbiased. The panel contains approximately 450,000 potential respondents who joined by completing a four-page recruitment mail survey. In return for their participation, respondents were given small incentives (e.g., a 20-min calling card, sweepstakes with a first-place prize of $1,000 and five-second-place prizes of $50). A more detailed explanation of the survey is available elsewhere (Maibach et al. 1996).
The initial survey of the Styles series, ConsumerStyles, was fielded in May through June 2006. Stratified random sampling was used to generate a list of 20,000 (of 450,000) potential respondents for this survey. This sample was stratified by region, household income, population density, age, and household size so as to create a nationally representative sample, and a low income/minority supplement (n = 3,000) was used to ensure that those groups would be adequately represented. In 2006, a total of 13,260 people completed the ConsumerStyles survey, yielding a response rate of 66.3%.Footnote 1 The second wave of the Styles series, HealthStyles, was administered in late June through early August 2006; a total of 6,600 HealthStyles surveys were mailed to households that returned the ConsumerStyles survey. Separate postage-paid return envelopes were provided for the HealthStyles survey. Responses were received from 5,251 HealthStyles participants, yielding a response rate of 79.6%. The data were post-stratified and weighted so that the sample distribution of age, race/ethnicity, sex, household size, and household income matched that of the general population according to the U.S. census. An underlying assumption for the post-stratification weighting is the sameness (homogeneity) of views held by specific groups of the population based on demographic weighting variables. HealthStyles data have been shown to give estimates of risk factors and conditions comparable to those produced by random sampling methodology (Pollard 2002). With the exception of the lowest level of education (i.e., not a high school graduate) being underrepresented, and those at lowest income (i.e., less than $10,000) being slightly overrepresented, comparison of the weighted HealthStyles 2006 sample to the 2005 U.S. Current Population Survey estimates on selected demographic variables, including sex, age, race/ethnicity, education, income, and region, indicates comparable estimates.
Additional Measures
Two items used as indicators of stigma on the 2007 Mental Illness and Stigma module used by about 30 states on their Behavioral Risk Factor Surveillance System (BRFSS) surveys were also included to assess their psychometric properties (Table 1).
Because personal experience can shape attitudes, the following additional questions were included on the HealthStyles survey to examine the associations of attitudes with experience having mental illness or knowing someone with mental illness: (1) “During the past year, have you had (or do you currently have) any of these other health conditions? (“X” all that apply”): (a) Anxiety disorder (e.g., generalized anxiety disorder, obsessive-compulsive disorder, panic disorder, phobia); (b) Dementia (e.g., Alzheimer’s disease); (c) Depression (e.g., major depression, manic-depressive disorder, bipolar disorder, dysthymic disorder); (d) Eating disorder (e.g., anorexia, bulimia, binge eating); (e) Schizophrenia. (2) “Do you personally know anyone who has had any of the following illnesses? (check all that apply)”: (a) Depression (e.g., major depression, manic-depressive disorder, bipolar disorder, dysthymic disorder; (b) Anxiety disorder (e.g., generalized anxiety disorder, obsessive-compulsive disorder, panic disorder, phobia); (c) Dementia (e.g., Alzheimer’s disease); (d) Eating disorder (e.g., anorexia, bulimia, binge eating); (e) Drug addiction; and (f) Alcoholism.
The order of mental illness related questions appeared in the following sections and in the following sequence: Section one of HealthStyles included a section on attitudes, and began by asking respondents to indicate their level of agreement with a number of statements on health-related issues. The attitudinal questions on mental illness were included in this section as individual items interspersed throughout the section. Section two in the survey included a section on “your health” and included questions on self-rated health, and self-reported diseases and disorders (e.g., osteoporosis, asthma, diabetes, skin cancer, high blood pressure, hearing impairment). Immediately following these questions, respondents answered questions on self-reported mental illness. (Additional survey sections focused on health behaviors, nutrition and activity, health risks, and on special populations such as parents and women.) Questions asking respondents whether they knew someone with mental illness appeared toward the end of the survey (Section 10). The latter section targeted all respondents and posed questions on familiarity with a variety of health-related issues.
Analyses
All analyses were conducted with Statistical Package for the Social Sciences (SPSS) (Release 12.0.0, 4 September 2003, and Release 14.0.1, 18 November, 2005). Responses recorded as missing were coded as missing values and excluded from analyses. Data were weighted to account for differences by sex, age, race/ethnicity, household income, and household size. To facilitate comparisons, five items were recoded so that higher scores represented more negative attitudes. Descriptive analyses examining the characteristics of the sample, the distribution of responses by level of agreement, and correlation coefficients among items were conducted using respondents from the entire sample. Initial correlation coefficients at the item level ranged from 0.002 to 0.57, indicating substantially different underlying subdomains and suggesting the need for factor analysis to understand the relationship among items. Following recommendations by Nunnally and Bernstein (1994a) regarding scale length and strength of inter-item correlations, common factor principal axis extraction with varimax rotation was used for exploratory factor analysis (EFA) to explore the underlying relationship among items.
Following preliminary results of the EFA, and given sufficient sample size, we randomly split the sample to conduct exploratory and confirmatory factor analysis (CFA) in two independent samples of respondents. Given sufficient sample size, traditional confirmatory factor analysis was used for cross-validation to test whether the items would load on the same factors as predicted by the EFA model (Devellis 2003). Reliability analyses were conducted to assess inter-item correlations, item-total correlations, and Cronbach’s alpha for each subscale for both the EFA and CFA results (Cronbach 1951). Upon consensus of subscale items, univariate analysis of variance was used to examine subscale scores by selected demographic characteristics. Because no overall goodness-of-fit test exists with principal axis factoring (PAF), we examined individual measures of sampling adequacy and other characteristics of the factor matrices to determine goodness of fit (de Vet et al. 2005; Nunnally and Bernstein 1994b). Pearson correlations were used in this analysis since structural equation modeling tools were not used, and interest was focused on the item relationships rather than on the relationship between latent factors not expected to explain an a-priori full model of stigma (Coenders and Saris 1995).
Results
The final sample of 5,251 adults was generally representative of the U.S. adult population, with the exception of individuals at lower levels of education being slightly underrepresented, and individuals at lower incomes being slightly overrepresented.
Item Analysis
Item means and related estimates for factor analytic studies are seen in Table 2 (de Vet et al. 2005). Responses varied with respect to agreement with individual items tapping into different domains. For example, while only about 4% agreed that a PWMI (person with mental illness) is to blame for his/her condition, 19% agreed that a PWMI is hard to talk with (Table 3). While 70% disagreed that a PWMI could pull himself or herself together if they wanted to, about 30% disagreed that a PWMI can eventually recover (Table 3). With the exception of items on blame, in more than a quarter of instances the level of agreement was neutral (neither agreement nor disagreement; Table 3).
Experience with Mental Illness
Among all respondents, about 12% reported having had anxiety; 12%, depression; almost 4% reported having had an eating disorder, and 1% reported having had schizophrenia. More than one-third of all respondents indicated knowing someone who had anxiety; 30% indicated knowing someone who had dementia; more than one-half reported knowing someone who had depression; almost 20% reported knowing someone who had an eating disorder; almost 13% reported knowing someone who had schizophrenia; 36% reported knowing someone who had a drug addiction, and 55% reported knowing someone who had alcoholism.
Factor Analysis
First, common factor analysis, using principal axis factor extraction with varimax rotation was performed on the entire sample (Nunnally and Bernstein 1994a). Matrix characteristics provided evidence that the data were factorable [e.g., all but one nonredundant residuals were <0.05; Bartlett’s test of spherecity was significant (X 2 = 10,229, df = 55, P < 0.01); anti-image correlations all ≥0.7 with the exception of two items that were close—0.64 (“pull together”) and 0.68 (“blame”); and the Kaiser-Meyer-Olkin measure was (0.732)] (Pett and Lackey 2003a, c).
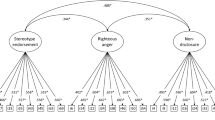
The Kaiser–Guttman rule for selecting factors for which eigenvalues are greater than 1.00, along with an examination of the scree plot, was used to identify factors (Nunnally and Bernstein 1994b; Comrey and Lee 1992; Guttman 1954; Cattell 1966). Three factors emerged that met these two criteria. Items were considered to load on a factor if they had a factor loading of at least 0.3 and differences of 0.2 between the loadings on the two factors. Five items loaded on factor 1, three items loaded on factor 2; and two items loaded on a third factor (Table 4A). The factors explained 41% of the common variance among the items. Despite acceptable goodness-of-fit indices and criteria indicating simple structure, the two-item factor posed a limitation for reliability. However, because the items tapped into a critical domain of stigma related to perceptions of danger, we retained the items, forcing a two-factor solution (Pett and Lackey 2003b).
Given sufficient sample size, we randomly split the sample into two independent samples to run an exploratory factor solution analysis, and a confirmatory analysis for convergent validity. In the forced two-factor solution PAF model, five items loaded on factor 1, and five items loaded on factor 2 (Table 4B). The sympathy item had low factor loadings on both factors. Measures of sampling adequacy were acceptable (KMO = 0.73; Bartlett’s X 2 = 5,262, df = 55, P < 0.01; anti-image correlations were all ≥0.7 with the exception of the two items that tapped into attitudes on blame). Factor 1 was labeled Negative Stereotypes, and factor 2 was labeled Recovery and Outcomes. In the forced two-factor solution, the two items related to blame that previously emerged on a third independent factor in the unforced solution loaded in the factor labeled Negative Stereotypes (Table 4B). Measures of sampling adequacy and goodness-of-fit indices were acceptable, and simple structure was met (Pett and Lackey 2003c). The two factors explained 32% of the common variance among items.
Cronbach’s alpha was 0.69 for the Negative Stereotypes factor, and 0.66 for the Recovery and Outcomes factor, indicating an initial acceptable estimate for internal consistency reliability (Cronbach 1951).
Confirmatory Factor Analysis
Using the second independent sample, the same methodology was applied to test the convergent validity of the EFA models. First, in an unforced common factor analysis, with PAF extraction and varimax rotation, three factors emerged with the same items loading onto three distinct factors with acceptable estimates for sampling adequacy and goodness of fit (Table 4C). This supported the original EFA findings. Again, because two items alone emerged on a third factor, we forced a two-factor solution in the second independent sample. This yielded the same pattern of item loadings as the EFA two-factor solution results, providing support that the two-factor model fit the data using an independent sample (Table 4D).
The reliability coefficient for the CFA sample on factor 1 was 0.70, and it was 0.69 on factor two. These factors explained 32.5% of the common variance among the items.
Scale Scores
Factor scores were obtained by summing the scores for only the items retained in the two-factor solution (Pedhazur and Schmelkin 1991). SPSS Complex Samples was used to obtain more appropriate standard errors for mean scores accounting for the complex survey design (i.e., a more conservative approach). Cases with missing values on an item in either subscale were excluded from analysis. Higher scores reflected more negative attitudes. Subscale scores on the “negative stereotypes” factor differed by sex, race/ethnicity, and experience with mental illness (Table 5). Men had slightly higher scores on stereotypes; Hispanics and adults of another race/ethnicity had slightly more negative attitudes than whites or blacks. Those who knew someone with a mental illness and those who had ever had a mental illness had lower scores (Table 5). While not significantly different from other age groups, there was a trend in the direction of more negative stereotypes in youngest adults.
In terms of recovery and outcomes, men had slightly more negative attitudes than women (significance was borderline). Blacks had slightly lower negative attitudes toward recovery than did whites or Hispanics. There were no differences by geographic region. As was the case with negative stereotypes, those who did not know someone with mental illness had more negative attitudes toward recovery than those who knew someone with mental illness (Table 5). Younger adults had higher, but not significantly higher scores than other age groups.
The correlation coefficient between the two factor scores was 0.09.
Concurrent Validity of BRFSS Items with Factor Subscales
The BRFSS item about treatment (“Treatment can help people with mental illness lead normal lives”) was removed from the Recovery and Outcomes factor to appropriately assess its independent concurrent validity with this factor. The item was moderately correlated (r = 0.6) with that factor, and it was weakly correlated with the Negative Stereotypes factor (r = 0.1). The BRFSS item on sympathy (“People are generally caring and sympathetic to people with mental illness”) was weakly correlated with both factors (r = 0.1).
Discussion
The purpose of this study was to develop and test a brief generic instrument to measure the public’s perceptions toward people with mental illness that could be used on existing public health surveillance systems, such as the BRFSS, or similar population-based surveys. This may allow researchers to routinely monitor stigma by state, in conjunction with a variety of sociodemographic, social, and health-related variables, and would also provide an opportunity to examine historical effects on attitudes. Two factors demonstrated adequate internal consistency reliability, thus meeting the standard criteria for scale development. Our method of using both exploratory and confirmatory analysis supports the validity of the items in this study. The percentages of mental disorders (obtained from self-reports) were within range of other population-based estimates for each respective disorder, providing evidence of the representativeness of the sample (U.S. Dept. of Health and Human Services 1999).
Consistent with its development, the items that comprised the factor related to negative stereotypes capture enduring themes that have influenced negative attitudes about mental illness (Crisp et al. 2000). On a positive note, we found that most people did not strongly agree with negative stereotypes. In some cases, about one-third of the population neither agreed nor disagreed with a statement. These persons’ attitudes may be most amenable to change because they may be more open to new information and the benefits of change (Bandura 1997). This pattern might also reflect the differing beliefs about the cause, course, treatment, and prognosis of mental illness. For example, a recent study examining attitudes toward people living with schizophrenia found that the public felt differently about people with schizophrenia in treatment than it felt about people with schizophrenia not in treatment (NAMI 2008). Finally, this pattern could also reflect response bias or mode effects, as some people with negative views may be reluctant to express them. Other studies examining the attitudes of participants to mailed questionnaires asking about sensitive topics such as interpersonal violence, sexual abuse, other childhood trauma, and injury or suicide survivorship found that participants responded favorably to an opportunity to participate in such studies (Black et al. 2006).
In the original British survey (the British ONS), in which respondents were asked these questions about specific mental illnesses, the most negative views about persons with mental illness being dangerous were expressed about those with schizophrenia, alcoholism, and drug dependence (Crisp et al. 2000), which is similar to U.S. findings (Pescosolido et al. 1999). Untreated physical diseases or disorders, and untreated mental illness can, in some cases, pose serious consequences for people and they warrant intervention. When the media sensationalizes rare, but tragic, events associated with someone having one of these disorders, they amplify fear (Wahl 2003). Less sensational, but more important, are the millions of people who live full, productive lives with these disorders. More media coverage of stories of accomplishment and recovery might contribute to improved attitudes (Wahl 2003).
Public health messages must often strike a balance between raising awareness and promoting risk-prevention practices on the one hand and preventing fear, stigma, and discrimination against subpopulations affected by a particular disorder on the other (Weiss et al. 2006; Person et al. 2004). Strategies for mitigating stigma often require multiple approaches, including primary prevention of disease; providing the public with information to raise awareness and to correct perceptions of risk; offering counseling services for those affected by a disorder; and supporting social policies that promote integration (Weiss et al. 2006).
Findings from the present study suggest that men as a group, and adults who classify themselves as Hispanic or of “other “race/ethnicity might benefit from messages that minimize negative stereotypes about mental illness and its treatment. Men’s scores on negative stereotypes and more negative views toward recovery and outcomes may result from traditional masculine social roles (Moller-Leimkuhler 2002; Tudiver and Talbot 1999). Recent public anti-stigma campaigns, such as Real Men, Real Depression, have attempted to debunk myths surrounding mental illness in men using public figures such as professional football players (National Institute of Mental Health 2007). Given the increased risk of depression, substance abuse, and suicide in men, campaigns focused on improving expectations of positive outcomes related to recovery or to the benefits of treatment may persuade some men to seek help.
Our findings that adults aged 18–24 years were more inclined toward negative stereotypes and more negative about recovery and outcomes merit note because mental illness often has its onset in adolescence or young adulthood. Negative beliefs about the benefits of treatment and recovery may dissuade young adults—who are at high risk for mental illness―from seeking treatment (VanVoorhees et al. 2006). Information about mental illness in SAMHSA’s campaign targeting young adults, “What a Difference a Friend Makes,” may be useful in changing attitudes about the possibility of recovery (U.S. Dept. of Health and Human Services 2007).
Adults classified as Hispanic or of other race/ethnicity held more negative stereotypes than whites or Blacks. Traditional cultural views regarding the symptoms and causes of mental illness that characterize some cultures may help to explain this finding. For example, in a recent study, Hispanic-Americans with lower levels of education often asserted that epilepsy results from sinful behavior (Sirven et al. 2005). A campaign, “La epilepsia es mas comun de lo que piensas” (Epilepsy is more common than you think) is widely disseminated throughout the Hispanic community at multiple levels, using lay community health educators and local media to improve knowledge and attitudes about epilepsy in this population (Epilepsy Foundation 2006). Use of similar community-based outreach strategies may be useful for debunking stereotypes among some racial/ethnic groups.
Blacks had the most positive views about the benefits and expectations associated with treatment and recovery. This is consistent with earlier studies in which African Americans reported more positive attitudes toward seeking mental health services than did whites, and had more positive attitudes about treatment effectiveness (Diala et al. 2001; Anglin et al. 2008). Anglin et al. (2008) found, however, that African Americans believed that mental health problems would improve on their own. Several studies have demonstrated the benefits from supportive social networks among African Americans (Calvert 1997). In this community and others, key opinion leaders may serve as important channels for messages that build on norms regarding recovery and increase skills for seeking and obtaining professional mental health care for those in need of such care.
In the present study, which was restricted to community-dwelling adults, those who knew someone with a mental illness or who ever had a mental illness were less inclined to have negative stereotypes, and had more positive views regarding recovery and outcomes for people with mental illness. Those who are experienced with mental illness may serve as important change agents by disseminating information about recovery throughout community settings.
The quality of the sample in the present study, both in size and representativeness, allowed us to test the measurement properties and validity of our items. The three factors that emerged—stereotypes, beliefs about recovery, and attribution/blame are inclusive of critical domains of stigma (Jones et al. 1984). The differences in the distribution of responses for the two items asking about recovery versus beliefs in treatment highlight the different understandings people may have regarding ambiguous concepts related to “recovery,” “treatment,” and “normal lives.” The high factor loadings of these items, however, indicate that they are tapping into a general construct related to outcomes for people with mental illness. The presence of a third factor related to blame also emerged as a distinct but less robust domain in this study, most likely due to the limited number of items in our survey. Because of the theoretical importance of blame/attribution as a stigma domain (Jones et al. 1984; Corrigan et al. 2002), the further development and testing of a short attribution subscale with these items is recommended for future studies.
The BRFSS item on expectations of treatment exhibited moderate concurrent validity with the Recovery and Outcomes factor. However, it was unsurprising that the psychometric properties of the BRFSS item, “People are generally caring and sympathetic to people with mental illness,” did not have sufficient psychometric properties to be retained in the factor subscales in this study. This item differed substantially from the others by asking respondents to think about what others think rather than to indicate their own thoughts. This difference was underscored by the weak correlation coefficient of this item with the two factor subscales, demonstrating the underlying constructs are unrelated.
The item, “I believe a person with mental illness could pull himself or herself together if he or she wanted” also had acceptable, but weak psychometric properties. These items may tap into empathy, which might also influence social distancing behaviors. If members of the public can be empathetic toward a person with a mental disorder, they may be more likely to offer assistance rather than distancing themselves from the person. Future studies can explore the development of a short subscale using related items to further develop the empathy construct.
There are several limitations to this study. First, we were not able to duplicate the original British ONS, substantially limiting our ability for cross-cultural comparisons between the USA and the UK. Additionally, respondents’ perceptions regarding type of mental illness, its causes, severity, and the level of control obtained from treatment when responding to these questions about mental illness were unknown. However, people in this study did have connections to different types of mental illness because of their own (self-reported) diagnoses or, because of their familiarity with someone else diagnosed with mental illness. This suggests that respondents answered these questions from multiple perspectives. Second, HealthStyles requires fluency in English, ability to understand written questions, and functional capacity, thus this study may have excluded adults who did not speak English, adults with severe limitations, and those with limited education. While the sampling design was designed to be representative, selection bias arising from differences in participants that were not accounted for by the weights applied might have occurred.
This study did not seek to develop and test a full model of stigma associated with mental illness, but rather to validate brief and simple measures that could be used by public health and mental health agencies on existing public health surveillance systems to obtain state-level estimates of stigma and to track changes in attitudes over time following communication campaigns or other interventions that seek to minimize stigma. Many such surveys used for public health surveillance require brief questions that are easily understood and that minimize response burden. Additionally, surveillance is often used to obtain a snapshot of population status and trends while findings often inform more detailed research studies. The use of general questions has been useful for tracking trends in attitudes toward other stigmatizing disorders such as epilepsy and HIV/AIDS (Caveness and Gallup 1980; Herek et al. 2002).
These limitations notwithstanding, there were several strengths of this study. We had a large, representative sample with which we could conduct both exploratory and traditional confirmatory factor analytic analysis (Devellis 2003). This generic, multidimensional, and yet brief instrument demonstrated rigorous convergent validity for potential use to routinely monitor stigma on population surveys. Future studies can develop and test additional short subscales related to blame and empathy for inclusion with these two scales. Furthermore, the BRFSS item on expectations of treatment used on 35 states’ BRFSS surveys demonstrated acceptable concurrent validity with the appropriate subscale on Recovery and Outcomes. Second, we found specific population subgroups, such as men and adults of “other” race/ethnicity with more negative stereotypes and more negative attitudes toward recovery and outcomes. These preliminary findings identify subgroups that might benefit from targeted communication campaigns.
Noting the many factors that can sway attitudes about mental illness (e.g., type of illness; treatment status; sex and age of individual described in a vignette), continued research is warranted to understand the complex dynamics of stigma (VanBrakel 2006). But, inclusion of such brief and generic items on population-based surveys and surveillance systems can help track attitudes about mental illness in U.S. states and communities, and can provide investigators with sociodemographic and health-related covariates with which to further examine stigmatizing attitudes and their associations with current events.
Notes
The response rate for the nationally balanced sample was 66.3%. The response rates for the minority/low income and households with children supplements were 63.5%.
References
Angermeyer, M. C., & Matschinger, H. (2004). Public attitudes to people with depression: Have there been any changes over the last decade? Journal of Affective Disorders, 83, 177–182.
Anglin, D. M., Alberti, P. M., Link, B. G., & Phelan, J. C. (2008). Racial differences in beliefs about the effectiveness and necessity of mental health treatment. American Journal of Community Psychology, e-pub PMID 18612808.
Antonak, R., & Livneh, H. (1988). The measurement of attitudes toward people with disabilities: Methods, psychometrics, and scales (p. 206). Springfield, IL: Charles C. Thomas Publishers.
Bambauer, K. Z., & Prigerson, H. G. (2006). The Stigma Receptivity Scale and its association with mental health service use among bereaved older adults. The Journal of Nervous and Mental Disease, 194(2), 139–141.
Bandura, A. (1997). Self-efficacy: The exercise of control. New York: W.H. Freeman and Company.
Black, M. C., Kresnow, M. J., Simon, T. R., Arias, I., & Shelley, G. (2006). Telephone survey respondents’ reactions to questions regarding interpersonal violence. Violence and Victims, 21(4), 445–459.
Bogardus, E. S. (1925). Measuring social distances. Journal of Applied Sociology, 9, 299–308.
Calvert, W. J. (1997). Protective factors within the family, and their role in fostering resiliency in African–American adolescents. Journal of Cultural Diversity, 4(4), 110–117.
Cattell, R. B. (1966). The scree test for the number of factors. Multivariate Behavior Research, 1, 245–276.
Caveness, W. F., & Gallup, G. H. (1980). A survey of public attitudes toward epilepsy in 1979 with an indication of trends over the past thirty years. Epilepsia, 21, 509–518.
Chapman, D. P., Perry, G. S., & Strine, T. W. (2005). The vital link between chronic disease and depressive disorders. Preventing chronic disease [serial online], Retrieved February 19, 2008, from http://www.cdc.gov/pcd/issues/2005/jan/04_0066.htm.
Coenders, G., & Saris, W. E. (1995). Categorization and measurement quality: The choice between Pearson and Polychoric correlations. In W. E. Saris & A. Munnich (Eds.), The multitrait-multimethod approach to evaluate measurement instruments (pp. 125–144). Budapest: Eotvos University Press.
Cohen, J., & Struening, E. L. (1962). Opinions about mental illness in the personnel of two large mental hospitals. Journal of Abnormal Social Psychology, 64, 349–360.
Comrey, A. L., & Lee, H. B. (1992). A first course in factor analysis. Hillsdale, NJ: Lawrence Erlbaum.
Corrigan, P. W., Markowitz, F. E., & Watson, A. C. (2004). Structural levels of mental illness stigma and discrimination. Schizophrenia Bulletin, 30(3), 481–491.
Corrigan, P. W., Rowan, D., Green, A., Lundin, R., Uphoff-Waswoski, K., White, K., et al. (2002). Challenging two mental illness stigmas: Personal responsibility and dangerousness. Schizophrenia Bulletin, 28(2), 293–309.
Crisp, A. H., Gelder, M., Goddard, E., & Meltzer, H. (2005). Stigmatization of people with mental illnesses: A follow-up study within the Changing Minds campaign of the Royal College of Psychiatrists. World Psychiatry, 4(2), 106–113.
Crisp, A. H., Gelder, M. G., Rix, S., Meltzer, H. I., & Rowlands, O. J. (2000). Stigmatisation of people with mental illness. British Journal of Psychiatry, 1(177), 4–7.
Cronbach, L. J. (1951). Coefficient alpha and the internal structure of tests. Psychometrika, 16, 297–334.
de Vet, H. C., Ader, H. J., Terwee, C. B., & Pouwer, F. (2005). Are factor analytic techniques used appropriately in the validation of health status questionnaires? A systematic review on the quality of factor analysis of the SF-36. Quality of Life Research, 14, 1203–1218.
Devellis, R. (2003). Factor analysis. Scale development: Theory and applications (pp. 102–137). Sage: Thousand Oaks.
Diala, C. C., Muntaner, C., Walrath, C., Nickerson, K., LaVeist, T., & Leaf, P. (2001). Racial/ethnic differences in attitudes toward seeking professional mental health services. American Journal of Public Health, 91(5), 805–807.
DiIorio, C. A., Kobau, R., Holden, E. W., Berkowitz, J. M., Kamin, S. L., Antonak, R. F., et al. (2004). Developing a measure to assess attitudes toward epilepsy in the US population. Epilepsy and Behavior, 5, 965–975.
Druss, B. G., Marcus, S. C., Rosenheck, R. A., Olfson, M., Tanielian, T., & Pincus, H. A. (2000). Understanding disability in mental and general medical conditions. American Journal of Psychiatry, 157(9), 1485–1491.
Epilepsy Foundation. (2006). La epilepsia es mas comun de lo que piensas: Curriculo. Landover, MD: Epilepsy Foundation.
Gary, F. A. (2005). Stigma: Barrier to mental health care among ethnic minorities. Issues in Mental Health Nursing, 26(10), 979–999.
Greene-Shortridge, T. M., Britt, T. W., & Castro, C. A. (2007). The stigma of mental health problems in the military. Military Medicine, 172(2), 157–161.
Guttman, L. (1954). Some necessary conditions for common factor analysis. Psychometrika, 19, 149–161.
Herek, G. M., Captanio, J. P., & Widaman, K. F. (2002). HIV-Related stigma and knowledge in the United States: Prevalence and trends, 1991–1999. American Journal of Public Health, 92(3), 371–377.
Hoge, C. W., Castro, C. A., Messer, S. C., McGurk, D., Cotting, D. I., & Koffman, R. L. (2004). Combat duty in Iraq and Afghanistan, mental health problems, and barriers to care. New England Journal of Medicine, 351(1), 13–22.
Jones, E. E., Farina, A., Hastorf, A. H., Markus, H., Miller, D. T., & Scott, R. A. (1984). The dimensions of stigma: The psychology of marked relationships. New York: W. H. Freeman Company.
Kelly, C. M., & Jorm, A. F. (2007). Stigma and mood disorders. Current Opinions in Psychiatry, 20(1), 13–16.
Keusch, G. T., Wilentz, J., & Kleinman, A. (2006). Stigma and global health: Developing a research agenda. Lancet, 367, 525–527.
Kobau, R., DiIorio, C. A., Anderson, L. A., & Price, P. H. (2006). Further validation and reliability testing of the attitudes and beliefs about living with epilepsy (ABLE) components of the CDC epilepsy program instrument on stigma. Epilepsy and Behavior, 8, 552–559.
Komiya, N. (2000). Emotional openness as a predictor of college students’ attitudes toward seeking psychological help. Journal of Counseling Psychology, 47, 138.
Link, B. G., Cullen, F. T., Frank, J., & Wozniak, J. F. (1987). The social rejection of former mental patients: Understanding why labels matter. American Journal of Sociology, 92, 1461–1500.
Link, B. G., & Phelan, J. C. (2001). Conceptualizing stigma. Annual Review of Sociology, 27, 363–385.
Link, B. G., & Phelan, J. C. (2006). Stigma and its public health implications. Lancet, 367, 528–529.
Link, B. G., Yang, L. H., Phelan, J. C., & Collins, P. Y. (2004). Measuring mental illness stigma. Schizophrenia Bulletin, 30(3), 512–541.
Maibach, E. W., Maxfield, A., Ladin, K., & Slater, M. (1996). Translating health psychology into effective health communication: The American Health Styles audience segmentation project. Journal of Health Psychology, 1, 261–277.
Moller-Leimkuhler, A. M. (2002). Barriers to help-seeking by men: A review of sociocultural and clinical literature with particular reference to depression. Journal of Affective Disorders, 71, 1–9.
National Alliance on Mental Illness. (2008). Schizophrenia: Public attitudes, personal needs. Retrieved September 21, 2008, from http://www.nami.org/sstemplate.cfm?section=SchizophreniaSurvey.
National Institute of Mental Health. (2007). Real men real depression. Retrieved July 3, 2008, from http://menanddepression.nimh.nih.gov/infopage53e5.html?ID=5.
Nunnally, J. C., & Bernstein, I. H. (1994a). Exploratory factor analysis II: Rotation and other topics. In J. C. Nunnally & I. H. Bernstein (Eds.), Psychometric Theory (pp. 491–541). New York: McGraw-Hill.
Nunnally, J. C., & Bernstein, I. H. (1994b). The general model and variance condensation. In J. C. Nunnally & I. H. Bernstein (Eds.), Psychometric theory (pp. 447–490). New York: McGraw-Hill.
Ojeda, V. D., & McGuire, T. G. (2006). Gender and racial/ethnic differences in use of outpatient mental health and substance use services by depressed adults. Psychiatric Quarterly, 77(3), 211–222.
Pedhazur, E. J., & Schmelkin, L. P. (1991). Measurement, design, and analysis: An integrated approach. Hillsdale, NJ: Lawrence Erlbaum.
Perlick, D. A., Rosenheck, R. A., Miklowitz, D. J., Chessick, C., Wolff, N., Kaczynski, R., et al. (2007). Prevalence and correlates of burden among caregivers of patients with bipolar disorder enrolled in the Systematic Treatment Enhancement Program for Bipolar Disorder. Bipolar Disorder, 9(3), 262–273.
Person, B., Sy, F., Holton, K., Govert, B., & Liang, A. (2004). Fear and stigma: The epidemic within the SARS outbreak. Emerging Infectious Diseases, 10(2), 358–363.
Pescosolido, B. A., Monahan, J., Link, B. G., Stueve, A., & Kikuzawa, S. (1999). The public’s view of the competence, dangerousness, and need for legal coercion of persons with mental health problems. American Journal of Public Health, 89, 1339–1345.
Pett, M. A., & Lackey, N. R. (2003a). Extracting the initial factors. In M. A. Pett, N. R. Lackey, & G. Sullivan (Eds.), Making sense of factor analysis: The use of factor analysis for instrument development in health care research (pp. 85–130). Thousand Oaks, CA: Sage.
Pett, M. A., & Lackey, N. R. (2003b). Evaluating and refining the factors. In M. A. Pett, N. R. Lackey, & G. Sullivan (Eds.), Making sense of factor analysis: The use of factor analysis f or instrument development in health care research (pp. 167–206). Thousand Oaks CA: Sage.
Pett, M. A., & Lackey, N. R. (2003c). Assessing the characteristics of matrices. In M. A. Pett, N. R. Lacky, & G. Sullivan (Eds.), Making sense of factor analysis: The use of factor analysis for instrument development in health care research (pp. 51–84). Thousand Oaks, CA: Sage.
Pollard, W. E. (2002). Use of consumer panel survey data for public health communication planning: An evaluation of survey results. In Proceedings of the section on health policy statistics. Alexandria, VA: American Statistical Association.
Pyne, J. M., Kuc, E. J., Schroeder, P. J., Fortney, J. C., Edlund, M., & Sullivan, G. (2004). Relationship between perceived stigma and depression severity. Journal of Nervous and Mental Disease, 192(4), 278–283.
Schene, A. H., Koeter, B., & Van Wijngaarden, M. W. (1998). Family caregiving in schizophrenia: Domains and distress. Schizophrenia Bulletin, 24(4), 609–618.
Scottish Executive (2002). Well? What do you think? A national Scottish survey of public attitudes to mental health, well being, and mental health problems, Scottish Executive. http://www.scotland.gov.uk/publications/2002/12/15967/15279. Accessed 4 Nov 2005.
Segal, D. L., Coolidge, F. L., Mincic, M. S., & O’Riley, A. (2005). Beliefs about mental illness and willingness to seek help: A cross-sectional study. Aging and Mental Health, 9(4), 363–367.
Sirven, J. I., Lopez, R. A., Bazquez, B., & Van Haverbeke, P. (2005). Que es la Epilepsia? Attitudes and knowledge of epilepsy by Spanish-speaking adults in the U.S. Epilepsy and Behavior, 7(2), 259–265.
Smith, M. (2002). Stigma. Advances in Psychiatric Treatment, 8, 317–325.
Stuart, H. (2005). Why stigma matters and why it should be beaten. World Psychiatry, 4(51), 6–7.
Stuart, H. (2006). Mental illness and employment discrimination. Current Opinions in Psychiatry, 19(5), 522–526.
Taylor, S. M., & Dear, M. J. (1981). Scaling community attitudes toward the mentally ill. Schizophrenia Bulletin, 7(2), 225–240.
Tudiver, F., & Talbot, Y. (1999). Why don’t men seek help? Family physicians’ perspectives on help-seeking behavior in men. Journal of Family Practice, 481(1), 47–52.
U.S. Dept. of Health and Human Services. (1999). Mental health: A report of the surgeon general. U.S. Dept. of Health and Human Services, CMHS, NIH, NIMH, U.S. Government Printing Office.
U.S. Dept. of Health and Human Services. (2007). What a difference a friend makes. Substance Abuse and Mental Health Services Administration. Retrieved August 21, 2007, from http://www.whatadifference.samhsa.gov/.
VanBrakel, W. H. (2006). Measuring health-related stigma–a literature review. Psychology, Health & Medicine, 11(3), 307–334.
VanVoorhees, B. W., Fogel, J., Houston, T. K., Cooper, L. A., Wang, N. Y., & Ford, D. E. (2006). Attitudes and illness factors associated with low perceived need for depression treatment among young adults. Social Psychiatry & Psychiatric Epidemiology, 41(9), 746–754.
Wahl, O. F. (2003). News media portrayal of mental illness: Implications for public policy. The American Behavioral Scientist, 46(12), 1594–1600.
Weiss, M. G., Ramakrishna, J., & Somma, D. (2006). Health-related stigma: Rethinking concepts and interventions. Psychology, Health & Medicine, 11(3), 277–287.
Wynaden, D., Chapman, R., Orb, A., McGowan, S., Zeeman, Z., & Yeak, S. (2005). Factors that influence Asian communities’ access to mental health care. International Journal of Mental Health Nursing, 14(2), 88–95.
Acknowledgments
The authors thank Dr. Bill Pollard, CDC; Dr. Deanne Weber, Porter Novelli; Dr. Marc Safran, CDC; Dr. Matthew Zack, CDC; and Dr. Bernice Pescosolido, Indiana University, for their assistance and helpful comments regarding this article.
Disclaimer
The findings and conclusions in this report are those of the author(s) and do not necessarily represent the views of the Centers for Disease Control and Prevention or those of the Substance Abuse and Mental Health Service Administration.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
Members of SAMHSA/CDC Mental Illness Stigma Panel are given before references.
SAMHSA/CDC Mental Illness Stigma Panel Members
SAMHSA/CDC Mental Illness Stigma Panel Members
-
Lynda Anderson, PhD, CDC
-
Richard Antonak, PhD, Vice Provost for Research, University of MA, Boston
-
Daniel Chapman, PhD, CDC
-
Patrick Corrigan, PsychD, Inst. of Psychology, Illinois Institute of Technology
-
Paolo Delvecchio, MSW, SAMHSA
-
Colleen DiIorio, RN, PhD, Dept. of Behavioral Sciences, Emory University
-
Olinda Gonzalez, PhD, SAMHSA
-
Rosemarie Kobau, MPH, CDC
-
Chris Marshall, SAMHSA
-
Mental Health Consumer Representatives (3)
-
David Moriarty, BS, CDC
-
Bernice Pescosolido, PhD, Dept. of Sociology, Indiana University
-
Patricia Price, DO, CDC
-
Carol Schauer, SAMHSA
-
Pamela Tucker, MD, CDC/ATSDR
-
E.Wayne Holden, PhD, RTI International
-
Hatice Zahran, MD, MPH, CDC
Rights and permissions
About this article
Cite this article
Kobau, R., DiIorio, C., Chapman, D. et al. Attitudes About Mental Illness and its Treatment: Validation of a Generic Scale for Public Health Surveillance of Mental Illness Associated Stigma. Community Ment Health J 46, 164–176 (2010). https://doi.org/10.1007/s10597-009-9191-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10597-009-9191-x