Abstract
In prostate cancer metastases to bone, cancer cell-derived cytokines stimulate RANKL expression by cells of the osteoblast lineage, which in turn activates osteoclastic bone resorption. However, it is unclear whether cells of the osteoblast lineage signal back to prostate cancer cells, and if so, whether such direct cross-talk can be targeted therapeutically. Using the human prostate cancer cell line, PC3, we identified two novel signalling pathways acting between cells of the osteoblast lineage and cancer cells. First, exposure to RANKL stimulated the expression and release of IL-6 by PC3 cells in vitro (which is known to promote RANKL expression by osteoblasts). Second, treatment of PC3 cells with IL-6 increased the expression of RANK, the cognate receptor of RANKL, and enhanced the RANKL-induced release of IL-6 by PC3 cells. Third, targeted disruption of IL-6 signaling with tocilizumab, a clinically available antibody against the human IL-6 receptor, inhibited skeletal tumor growth in vivo and reduced serum RANKL levels as well as RANK expression by PC3-derived bone tumors. Similar effects were achieved when RANK expression was knocked down in PC3 cells. In contrast, disruption of IL-6 or RANK/RANKL signalling had no effect on PC3 tumor growth in soft tissues, indicating that these signalling pathways act specifically within the bone microenvironment. In conclusion, prostate cancer cells and cells of the osteoblast lineage communicate via two inter-dependent signaling pathways, which through auto-amplification strongly enhance metastatic prostate cancer growth in bone. Both pathways may be targeted for effective therapeutic intervention.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Prostate cancer has a high propensity to metastasize to the skeleton [1, 2]. We and others have previously demonstrated that the bone microenvironment plays a critical role in supporting cancer cell growth. This is supported by experimental and clinical observations where treatment with anti-resorptive agents (e.g. bisphosphonates) inhibits or even prevents metastatic cancer growth [3–5] while accelerated bone turnover (e.g. through calcium deficiency) stimulates the progression of skeletal secondary tumors [6–8].
The ‘vicious cycle of bone metastasis’, first introduced by Mundy and colleagues in 1997 [9, 10], provides a sound mechanistic model that explains many aspects of the metastatic phenotype in bone. In this model, tumor-derived factors such as PTHrP and other cytokines stimulate RANKL expression in osteoblasts, which leads to the activation of osteoclasts and accelerated bone resorption. This not only generates space for the tumor to grow (by removing existing bone) but also triggers the release of growth factors embedded in the degraded bone matrix. These in turn act on the cancer cells to stimulate further tumor growth. This concept has been extremely useful in explaining the progression of established skeletal metastases. While prostate cancer metastasis to bone usually cause sclerotic lesions on X-ray, histological and biochemical analyses demonstrate that both bone formation and bone resorption are active in such lesions [11].
In patients with metastatic breast or prostate cancer, high circulating levels of interleukin-6 (IL-6) have been associated with disease progression and poor clinical outcomes [12, 13]. Likewise, high IL-6 expression by human prostate cancer cells is a characteristic of a more aggressive phenotype, including an association with hormone refractoriness [14]. IL-6 also appears to have a role in prostate cancer resistance to chemo- or hormonal therapies, which in part act via induction of cell apoptosis [15]. Previous work has demonstrated that in bone metastases, tumor-derived IL-6 can stimulate osteoclast differentiation and osteoclast-mediated bone resorption [16], either through osteoblast activation [17, 18] or through other, indirect mechanisms [19, 20]. Recently, IL-6 has also been shown to promote malignant features in breast and lung cancer cells [21, 22] and to act as a tumor cell attractant in the metastatic process [23]. Previous studies using neuroblastoma or breast cancer cell lines demonstrated that cells of the osteoblast lineage produce cytokines such as IL-6 which can either promote tumor growth or induce bone resorption to allow for further tumor growth in bone [24–27]. Hence, IL-6 may be a therapeutic target, particularly in aggressive and/or androgen-independent prostate cancers [28].
In addition, many tumors express RANK, the cognate receptor of RANKL, and a high concordance between RANK expression by the primary cancer and its skeletal secondaries has been reported [29]. In vitro, RANKL plays an important role in stimulating prostate cancer cell migration [30]. RANKL is produced in bone by cells of the osteoblast lineage, including both osteoblasts and osteocytes, as a regulator of osteoclast differentiation and thus bone remodeling [31]. However, it is unclear whether cells of the osteoblast lineage directly signal back to prostate cancer cells, and if so, whether such direct cross-talk contributes to cancer growth and could therefore be targeted therapeutically.
In the present study, we demonstrate that cells of the osteoblasts lineage communicate directly with prostate cancer cells in bone via two distinct but complementary signaling pathways involving IL-6, RANK and RANKL. As these self-amplifying feed-forward loops significantly enhance tumor growth in bone, their disruption offers therapeutic potential in patients with prostate cancer metastases to bone.
Materials and methods
Antibodies and reagents
Recombinant human cytokines RANKL (Catalog Number: 390-TN/CF), IL-6 (Catalog Number: 206-1L) and anti-RANK monoclonal antibodies (Clone 80707, Catalog Number: 6831) were bought from R&D Systems, Minneapolis, MN. Tocilizumab is a humanized anti-human IL-6R monoclonal antibody which was purchased from (Roche Pharmaceutical Co., Ltd.).
Cell culture
The prostate cancer cell line PC-3 was obtained from ATCC and the cells were cultured in RPMI, supplemented with 10 % fetal calf serum (FCS, JRH Biosciences, KS, USA) and 1 % penicillin–streptomycin solution. All tissue culture media and supplements were supplied by invitrogen (Carlsbad, CA, USA) unless otherwise stated.
Real-time RT-PCR
Human IL-6 mRNA levels were assessed by species-specific primers using real-time RT-PCR. Primers used in this study (GADPH, IL-6, RANK) were as follows: GAPDH, forward-TATGACAAC GAATTTGGCTACAG, reverse-TGATGGTACATGACAAGGTGC; IL-6, forward-CCACACAGACA GCCACTCA, reverse-GCTTGTTCCTCACTACTCTCAAATC; RANK, forward-TCAAGGTGGTGTC TGTCAGG, reverse-CTTTCTGAACCCACTGTGCTC.
IL-6 and RANK mRNA expression
PC3 cells express RANK [5]. To investigate whether RANKL induces IL-6 mRNA expression, PC3 cells were stimulated with recombinant RANKL (R&D Systems, Minneapolis, MN) at concentrations of 25, 50, 100 and 200 ng/mL in RPMI supplemented with 1 % Penicillin/Streptomycin and 0.1 % BSA for 4 h. IL-6 mRNA expression levels were then assessed by real time RT-PCR. Fetal calf serum was removed from the culture media to minimize potential confounding effects of cytokines and growth factors present in the culture medium. To examine the time-course of RANKL-induced IL6 mRNA expression, PC3 cells were stimulated with RANKL (100 ng/mL) using the same media as above for 4, 8 and 24 h, and IL-6 mRNA expression was quantified by real-time RT-PCR.
To determine the effect of IL-6 on RANK expression in PC-3 cells, cells were seeded at a density of 1 × 105 cells/mL in 2 mL supplemented RPMI in a 6-well plate for RNA extraction. Cells were incubated in standard conditions overnight. The medium was then removed and changed to RPMI supplemented with 1 % Penicillin/Streptomycin and 0.1 % BSA, containing IL-6 (12.5, 25, 50 and 100 ng/mL). Cells were incubated for 4 h, and RNA was harvested and RANK expression levels measured.
Biochemical assays
Serum concentrations of tartrate resistant acid phosphatase 5b (TRAcP5b) and the amino-terminal procollagen type I propeptide (PINP) were measured by ELISA [3, 32].
IL-6 pre-treatment and RANKL treatment
Cancer cells (5 × 104 cells/well) were seeded onto 24-well plates in 10 %FCS DMEM. After overnight culture, the cells were pre-treated with IL-6 using concentrations of 12.5, 25, 50, 100 ng/mL for 4 h under serum free conditions (0.1 % BSA RPMI). Cells were then thoroughly washed and treated with RANKL (100 ng/mL). After 4 and 24 h, media were collected for measurement of human IL-6 by ELISA (BD Biosciences Pharmingen).
Co-culture of Kusa O osteoblasts and PC3 cells
Kusa O pre-osteoblasts were differentiated under osteogenic conditions (50 µg/mL ascorbic acid and 10 mM β-glycerophosphate) in a 24-well plate. On day 11 after differentiation, PC3 cells were seeded (5 × 104 cells/well) on top of the Kusa O cells and co-cultured for a further 24, 48 or 72 h. Conditioned media were collected and IL-6 levels assayed by a human (see above) and a mouse-specific IL-6 ELISA (BD Biosciences Pharmingen).
Knock down RANK expression in PC3 cells
RANK expression was silenced in PC3 cells via a lentiviral-based expression system driving the production of short hairpin RNA species (shRNAs, Sigma, USA) according to the manufacturer’s protocol. The clone selected was RANK shRNA (TRCN0000003350) and non-target control (SHC002 V). Puromycin selection (2 μg/mL) was used for 2 weeks.
Growth curves
To assess the in vitro proliferation rate of PC3 non-target and RANK knock-down cells, 5 × 104 cells were seeded in quadruplicate in 2 % FCS RPMI in four twelve-well tissue culture plates at a concentration of 104 cells/well (3.8 cm2) and allowed to adhere overnight. The cells were then counted daily by trypan blue exclusion after trypsinizing until they reached 100 % confluence on day four. Experiments were repeated three times in independent settings to ensure validity of the results.
Mouse model of prostate cancer growth in bone
Male BALB/c nu/nu mice at 4–5 weeks of age (Animal Resources Centre, Canning Vale, WA, Australia) were used for all the animal experiments. All mouse manipulations were performed inside a laminar-flow hood under aseptic conditions whilst maintaining general anesthesia with intra-peritoneal injection of ketamine/xylazine (75/10 mg/kg, unless otherwise noted), in accordance with Animal Welfare Guidelines and approved protocol 2009–2012 by Sydney Local Health District Animal Welfare Committee, Sydney, Australia. Murine xenograft models were used to study prostate cancer cell growth in bone and in subcutaneous tissues. Under anaesthesia, 1 × 105 PC3 cells suspended in 10 μL of phosphate buffered saline (PBS) were injected intra-tibially. The analgesic carprofen (Rimadyl) (5 mg/kg subcutaneously) was administered before inoculation to minimise post-surgical pain. For the follow-up of lytic bone lesions in vivo, mice were anesthetized as above and assessed by digital radiography. Lytic bone areas of the tibiae were measured using interactive image analysis software (ImageJ, NIH, USA) and the size of osteolytic lesions were calculated and the growth of lytic lesions was compared among experimental groups.
The intratibial xenograft murine model used in the current study represents a late step within the metastatic cascade, for which we investigated the growth characteristics of prostate cancer cells within the bone microenvironment.
Intra-skeletal and subcutaneous growth of PC3 during treatment with tocilizumab
Five week-old BALB/c nu/nu male mice (n = 10) were inoculated with 1 × 105 PC3 cells intra-tibially [7, 33]. Mice received tocilizumab (50 mg/kg) via i.p. injection one day prior to tumor cell inoculation and then every 3 days until endpoint. Mice were euthanized on day 30 for analysis by radiography, histology, immunohistochemistry (apoptosis and proliferation) and histomorphometry.
For the subcutaneous model, cells were prepared as above and suspended in a mixture of cold Matrigel and PBS (1:1) at a concentration of 2 × 107 cells/mL. 100 µL of the suspension was implanted subcutaneously at the flank (n = 10). Tumor growth was measured in length and width by calipers every second day from day 6 onwards and tumor volume was determined using the modified ellipsoidal formula [volume = (length × width2)/2] [33]. Following euthanasia on day 69, tumors were removed and weighed.
Growth of RANK knock-down PC3 cells in bone and in subcutaneous soft tissues
Control and RANK knock-down PC3 cells were implanted intra-tibially (105 cells/injection) or subcutaneously (106 cells/injection) into 4 week-old BALB/c nu/nu male mice (n = 10). Intra-tibial tumor growth was monitored using X-ray on days 21, 28 and 35, and bones were analysed by histology and histomorphometry following euthanasia on day 35. The subcutaneous model’s tumor volume was determined as above [33] every second day from day 3 onwards. Following euthanasia on day 69, tumors were removed and weighed.
Histological assessment
Tibiae were fixed for 36 h in 4 % paraformaldehyde buffered with 0.1 M phosphate buffer (pH 7.4) and decalcified in 10 % EDTA at 4 °C for 2 weeks. The tissues were then processed and embedded in paraffin. Five-micron sections were cut from each specimen and stained with haematoxylin and eosin for routine histological examination. Histochemical examination for tartrate-resistant acid phosphatase (TRAcP), as a marker for osteoclasts, was performed by using naphthol AS-MX phosphate (Sigma Chemical Co., St. Louis, MO, USA) as a substrate and fast red violet Luria–Bertani salt (Sigma) as a stain for the reaction product; incubation was performed at room temperature for 30 min [3].
Immunohistochemistry was carried out to evaluate protein expression of human RANK in 5 μm histological sections (monoclonal mouse antibody to human RANK, R&D Systems, Minneapolis, MN, USA; secondary antibodies, Vector Laboratories, Burlingame, CA, USA). By microscopy, positive tumor cells were identified as brown-colored cells. Tumor sections from RANK knock-down experiments and IL-6R antibody treatments were analyzed for mitotic activity on H&E sections or by ki-67 (NeoMarkers) immunohistochemistry. Adjacent sections were stained to identify apoptotic cells using terminal deoxynucleotidyl transferase–mediated dUTP nick end labeling (TUNEL) (In Situ Apoptosis Detection Kit, Millipore), according to the manufacturer’s protocol. The ratio of mitotic cells and apoptotic TUNEL stained cells was determined by counting positive and negative cells in five random fields of non-necrotic areas of tumors in a representative section in each bone specimen (×400 magnification).
Bone histomorphometry
Histomorphometric analysis of the proximal tibial metaphysis was conducted to evaluate bone volume, tumor burden and static measures of bone resorption. Measurements were performed in longitudinal 5 μm sections stained with hematoxylin and eosin (×12.5 magnification) with measurement made interactively using the OsteoMeasure System (Osteometrics, Atlanta, GA, USA). To determine tumor area, one of the most representative sagittal sections with largest tumor area from the proximal tibia was analysed. Osteoclasts were identified as TRAcP positive multinucleated cells associated with tumor bone interfaces. The osteoclast number (×200 magnification) per millimeter of tumor bone interfaces was calculated.
Statistical analysis
All data were presented as the mean ± SE and statistical analysis was conducted using one-way ANOVA, followed with Bonferroni’s adjustment where there were multiple comparisons by means of SPSS 17.0 for Windows (SPSS Inc., Chicago, IL, USA.). Significance was accepted where p < 0.05.
Results
Recombinant and osteoblast-derived RANKL promote IL-6 expression in prostate cancer cells
In vitro, treatment of PC3 cells with recombinant RANKL for 4 h up-regulated IL-6 expression in a concentration-dependent manner, with a maximum effect reached at 100 ng/mL of RANKL (Fig. 1a). Treatment with RANKL at a concentration of 100 ng/mL for 4 and 24 h caused a sustained increase in IL-6 expression levels in PC3 cells (Fig. 1b).
Recombinant and osteoblast-derived RANKL promote IL-6 expression in PC3 prostate cancer cells in vitro. a Treatment with RANKL for 4 h dose-dependently increased IL6 mRNA expression by PC3 cells. b Prolonged treatment with RANKL at maximum effective concentrations (100 ng/mL; see Fig. 1a) resulted in a sustained increase in IL-6 mRNA expression levels in PC3 cells. c Differentiation of murine osteoblast-like Kusa O cells in vitro was associated with a significant rise in RANKL mRNA over time. Maximum levels were reached at day 11 of culture. d Co-culture of PC3 cells with fully differentiated, RANKL-expressing Kusa O cells (harvested on day 11 of culture; see Fig. 1c) progressively stimulated hIL-6 secretion by prostate cancer cells in a time dependent manner. Basal hIL-6 secretion did not change when PC3 cells were cultured alone. e Co-culture of differentiated Kusa O cells with PC3 cells significantly increased mIL-6 production by mouse osteoblast-like cells. Data are mean ± SEM. *denotes significantly different from vehicle-treated group (p < 0.05). All in vitro experiments were repeated three times with similar results obtained. Results shown here are from a representative experiment
As RANKL in bone is primarily derived from cells of the osteoblast lineage [34], we next employed an in vitro co-culture model to investigate whether RANKL generated by osteoblast-like cells increases IL-6 secretion in cancer cells. To this aim, murine Kusa O cells were differentiated for 11 days, at which time they release large amounts of RANKL (Fig. 1c). These cells were then co-cultured with PC3 cells for 72 h. Compared to PC3 cells cultured alone, co-culture with RANKL-secreting osteoblast-like cells increased (human) IL-6 production by PC3 cells more than fourfold (Fig. 1d). Interestingly, the secretion of (murine) IL-6 from Kusa O cells was also increased in the co-culture system (Fig. 1e).
IL-6 induces RANK expression in prostate cancer cells
Treatment of PC3 cells with recombinant IL-6 at 12.5, 25, 50, 100 ng/mL for 4 h dose dependently increased RANK (the cognate receptor for RANKL) mRNA expression levels by prostate cancer cells. As shown in Fig. 2a, IL-6 concentrations of 50 and 100 ng/mL significantly upregulated RANK expression. Together with the above data, this finding suggests that prostate cancer cells may become sensitized to the action of RANKL via an autocrine signalling pathway, through which cancer-derived IL-6 increases RANK expression in the very same cells. To further investigate this possibility, PC3 cells were pre-treated with IL-6 (from 12.5 to 100 ng/mL) for 4 h to enhance RANK expression. Following a thorough wash, cells were then exposed to RANKL (100 ng/mL) for 4 to 24 h. As shown in Figs. 2b and c, the amount of IL-6 released in response to RANKL was significantly greater in cancer cells pre-treated with IL-6. Of note, even concentrations as low as 25 ng/mL IL-6 pretreatment were effective in triggering this response. Thus, while rhRANKL alone has relatively modest effects on IL-6 expression by tumor cells (Figs. 1a, b), pre-exposure of such cells to IL-6 greatly amplifies the effects of RANKL on tumor IL-6 expression.
Treatment with IL-6 sensitizes PC3 prostate cancer cells to the action of o RANKL in vitro. a Treatment of PC3 cells with recombinant IL-6 at 12.5, 25, 50, 100 ng/mL for 4 h dose-dependently increased RANK mRNA expression levels by PC3 cells. b and c PC3 cells were pre-treated with IL-6 at 12.5, 25, 50, 100 ng/mL for 4 h, followed by treatment with RANKL (100 ng/ml) for 4 and 24 h. Pre-treatment of PC3 cells with IL-6 stimulated RANK expression by cancer cells. Exposure to RANKL for 4 (b) and 24 (c) significantly boosted hIL-6 production in pre-treated compared to untreated cells or cells treated with IL-6 only. Data are mean ± SEM. * and ** denote significantly different from controls (*p < 0.05; **p < 0.01). All in vitro experiments were repeated three times with similar results obtained. Results shown here are from a representative experiment
Taken together, the above in vitro data suggest the presence of two signalling pathways that support and amplify direct cross-talk between cancer and bone cells: First, co-culture of RANKL-expressing Kusa O cells with cancer cells directly promotes the release of IL-6 by cancer cells, which in turn enhances RANKL production in osteoblasts and hence osteoclast activity. This direct cross-talk between cancer cells and osteoblasts is amplified through a second autocrine pathway, where tumor-derived IL-6 up-regulates RANK expression within cancer cells, thus sensitizing the tumor to RANKL, further increasing its IL-6 output.
We next examined whether these mechanisms are operational in vivo. Specifically, we asked whether interrupting the putative signalling pathways described above (either by blocking tumor derived IL-6 or by knocking down tumor RANK expression) would affect tumor growth in bone or in soft tissue.
Treatment of mice with anti-IL-6R antibodies reduces PC3 cancer cell growth in bone as well as reducing circulating RANKL levels
It is well established that human IL-6 can activate both the human and murine IL-6R. In contrast, murine IL-6 can only bind and activate the murine IL-6 receptor [35]. To determine the contribution of tumor cell-derived (human) IL-6 on cancer growth in bone, we took advantage of this fact and the high epitope specificity of the anti-human IL-6R antibody, tocilizumab. As the cancer cells introduced into mice are of human origin, any IL-6 produced by these cells will act on both the human and the murine IL-6R, with downstream effects in both human tumor and rodent bone cells. In contrast, murine IL-6 only interacts with the mouse IL-6R and will affect only cells of the murine bone environment. As tocilizumab binds exclusively to the human IL-6 receptor [36] present on the implanted cancer cells, it will only prevent signaling by human, i.e. cancer-derived IL-6. Tocilizumab does not affect signaling by human or mouse IL-6 through the mouse IL-6R on host cells [35].
We first determined whether disrupting the hIL-6 receptor signaling by tocilizumab affects the growth of PC3 cells in bone. To this aim, nude mice were implanted intra-tibially with PC3 cells and then treated with tocilizumab or vehicle. As shown in Fig. 3, 50 mg/kg tocilizumab inhibited PC3 cell growth in bone. Compared to untreated controls, both osteolytic (Figs. 3a, b) and total tumor areas (Figs. 3c, d) were significantly reduced, and cortical bone area and structure were preserved in tocilizumab-treated mice (Fig. 3e). As expected, reduced tumor growth was associated with lower cell proliferation and higher apoptosis rates within the tumor (Figs. 3f–g). Compared to controls, both osteoclast number at the tumor-bone interface and serum TRAcP5b were significantly lower in the tocilizumab-treated group (Figs. 3h–i). Serum RANKL concentrations were significantly higher in animals injected with PC3 cells when compared to non-tumor-bearing mice (p < 0.05). In tocilizumab-treated PC3-bearing animals, RANKL levels were significantly lower cells when compared to untreated controls (29.14 ± 5.43 pg/mL vs. 61.78 ± 13.44 pg/mL, p < 0.05) (Fig. 3j).
Disruption of IL-6R signalling reduces intra-skeletal PC3 cancer cell growth in vivo. a–e Treatment with the human IL-6R antagonist, tocilizumab, reduced tumor growth in mice implanted intra-tibially with PC3 cells. Osteolytic areas as assessed by radiographic (a) and micro-CT (b) analyses as well as histological tumor area (T tumor, BM bone marrow) (c, d) were all significantly smaller in tocilizumab-treated animals than controls. As a result, cortical bone area remained preserved (e) (n = 9). f–g Compared to controls, reduced tumor growth was associated with lower proliferation and higher apoptosis rates in PC3 tumor cells. h–i Compared to controls, osteoclast number at the tumor-bone interface (h), serum TRAcP5b (i) and murine RANKL concentrations (j) were all significantly lower in tocilizumab-treated mice. j Murine RANKL concentrations were significantly higher in animals injected with PC3 cells when compared to non-tumor-bearing mice (*p < 0.05). In tocilizumab-treated PC3-bearing mice, RANKL levels were significantly lower cells when compared to controls (#p < 0.05). k and l When PC3 cells were implanted at subcutaneous sites, treatment with tocilizumab had no effect on tumor growth in vivo (l) with similar tumor masses (k) at endpoint (day 51). Data are mean ± SEM. * and ** denote significantly different from controls (*p < 0.05; **p < 0.01)
Treatment with tocilizumab does not alter tumor growth in subcutaneous PC3 tumors
We next asked whether the IL6-RANKL-RANK signaling pathway is unique to the bone microenvironment or operational in non-skeletal tissues as well. To this aim, we implanted PC3 cells subcutaneously into male nude mice treated with either tocilizumab or PBS. In contrast to the changes seen in bone, tocilizumab had no effect on tumor growth at subcutaneous sites (Figs. 3k, l) with no significant changes in tumor cell proliferation or apoptosis (data not shown). The obvious tissue-dependency of these results strongly suggests that the effect of IL-6 signaling on tumor growth and survival are only operational within the bone microenvironment where there is the potential for reciprocal signaling between cancer and bone cells.
In addition, tocilizumab reduced not only systemically circulating RANKL levels (Fig. 3j) but, relative to controls, also lowered RANK immunoreactive protein levels in PC3-derived bone tumors (Fig. 4a). This in vivo finding is in good keeping with the results of our in vitro experiments, demonstrating that IL-6 induces RANK expression in prostate cancer cells (Fig. 2a). Furthermore, tocilizumab treatment had no effect on RANK expression by PC3 tumor cells implanted subcutaneously (Fig. 4b), indicating the interaction of RANKL-RANK-IL-6 is dependent on the bone environment.
RANK immunohistochemistry staining on PC3 cancer cell growth in vivo. a In vivo, RANK expression in tumor sections obtained from tocilizumab-treated mice was significantly reduced compared to control mice (Scale bar 100 um). b Treatment with tocilizumab had no effect on RANK expression in subcutaneously implanted tumors (Scale bar 100 um)
Knock-down of RANK expression in PC3 cells reduced tumor growth in bone
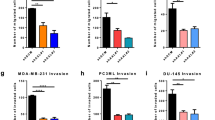
To address the second component of the proposed signalling pathway, we examined whether knock-down of RANK expression in PC3 cancer cells reduced tumor growth in bone and/or subcutaneous tissue. To this aim, RANK expression was effectively knocked down in PC3 cells: Knock-down efficacy was 80 % as assessed by real-time RT-PCR and Western blot (Figs. 5a–b) with no increased IL-6 expression following stimulation of RANK knock-down cells with RANKL (Fig. 5c). While RANK knock-down had no effect on cell growth in vitro (Fig. 5d), in the intra-tibial model, injection with RANK knock-down cells significantly reduced tumor growth in bone compared to NT controls, as reflected by the results of both radiographic (Figs. 5e, f) and histological analyses (Figs. 5g, h). Implantation of PC3 RANK knock-down cells also resulted in significantly reduced osteoclast activity, bone destruction and osteoclast-lined bone surfaces at the bone/tumor interface (Figs. 5i, j). Tumors derived from RANK knock-down cells were characterised by lower mitotic activity (−42 %) and higher rates of apoptosis (+94 %) compared to NT cell-derived tumors (Figs. 5k, l). Serum murine RANKL levels were significantly higher in animals injected with PC3 cells (both RANK knock-down and NT) when compared to non-tumor-bearing mice (p < 0.05). In mice injected with PC3 RANK knock-down cells, RANKL levels were significantly lower when compared to NT controls (24.9 ± 3.11 pg/mL vs. 50.04 ± 7.46 pg/mL, p < 0.05) (Fig. 5m). In contrast, RANK knock-down and control PC3 cells implanted into the subcutaneous soft tissue proliferated at similar rates (Figs. 5n, o).
Knock-down of RANK expression in PC3 prostate cancer cells reduces tumor growth in bone. a–c Knock-down of RANK expression in PC3 cells. Knock-down efficacy was 80 % as assessed by real-time RT-PCR (a) and western blot (b). Compared to controls, treatment of RANK-knock-down cells with RANKL had no effect on IL-6 expression, confirming functional RANK knock-down (c). d Knock-down of RANK expression had no effect on cell growth in vitro. e–j Compared to PC3 control (NT) cells, intra-tibial implantation of PC3 RANK knock-down cells resulted in reduced skeletal tumor growth and cortical bone destruction as assessed by radiography, micro-CT (e and f) and histology (g–j; T tumor, BM bone marrow) (n = 10). k and l, Tumors derived from PC3 RANK knock-down cells were characterized by lower mitotic activity and higher rates of apoptosis compared to NT cell-derived tumors. m Serum murine RANKL levels were significantly higher in animals injected with PC3 cells (both RANK knock-down and NT) when compared to non-tumor-bearing mice (*p < 0.05). In mice injected with PC3 RANK knock-down cells, RANKL levels were significantly lower cells when compared to NT controls (#p < 0.05). n and o PC3 NT and RANK knock-down cells implanted orthotopically into the subcutaneous soft tissues displayed similar growth rates and tumor mass at endpoint (day 69). Data are mean ± SEM. * and ** denote significantly different from controls (*p < 0.05; **p < 0.01)
Discussion
In the current study, we have identified two interdependent and self-amplifying signaling pathways operational within the bone microenvironment to enhance tumor cell cytokine output (Fig. 6). Firstly, in addition to its known effects on osteoclasts, RANKL released by cells of the osteoblast lineage directly stimulates IL-6 expression in cancer cells. In turn, IL-6 promotes RANKL expression in osteoblasts and other cells of the osteoblast lineage, closing a direct feed-forward loop between osteoblasts and tumor cells. Secondly, IL-6 expressed by tumor cells induces, via an autocrine mechanism, expression of RANK on the surface of the tumor cells, thus sensitizing these cells to the action of osteoblast-derived RANKL. We further provide evidence that effective disruption of the direct cross-talk between osteoblasts and tumor cells significantly impacts on cancer cell growth in bone.
Proposed paracrine and autocrine signaling pathways between cancer cells and cells of the osteoblast lineage. The ‘vicious cycle’ of bone metastatic growth as described by Mundy and colleagues (9, 10) is represented by the light blue arrows. From our finding we have proposed two pathways: pathway 1 RANKL produced by cells of the osteoblast lineage binds directly to RANK on cancer cells. This induces IL-6 expression by the tumor, which in turn stimulates RANKL expression by osteoblasts/osteoblast-like cells (9, 18). pathway 2 IL-6 expressed by tumor cells in response to RANKL induces RANK expression by the tumor cell itself, thus sensitizing cancer cells to RANKL. Both signalling pathways are interdependent and, through auto-amplification, act synergistically to boost overall cytokine output within the bone environment. Activation of these mechanisms enhances metastatic tumor growth in bone through direct cross-talk between cancer cells and cells of the osteoblast lineage
RANKL is present at high levels in bone and is derived mainly from cells of the osteoblast lineage (i.e. bone marrow stromal cells, osteoblasts, osteocytes) [31, 34, 37, 38] as well as T cells [39]. Since athymic nude mice lack T cells, it is conceivable that in the setting of our studies, RANKL is mainly derived from cells of the osteoblast lineage [31, 34, 38]. Jones and colleagues demonstrated that RANKL triggers migration of RANK expressing human epithelial cancer cells and melanoma cells [30]. Also, RANK expression by cancer cells appears to correlate with the progression of the primary cancer to skeletal secondaries [29]. However, local RANKL concentrations may also play an important role in cell migration and tissue-specific metastatic cancer cell behaviour as OPG was found to reduce skeletal but not non-skeletal tumor burden in mouse models of malignant melanoma [30]. The interplay of RANKL-RANK-IL-6 from our results further consolidates the role of a direct interaction between osteoblasts and cancer cells within the bone microenvironment.
High circulating levels of IL-6 have been shown to be associated with adverse clinical outcomes in patients with metastatic breast and prostate cancer. For example, survival rates are significantly shorter in cancer patients with persistently high serum IL-6 levels [13, 40–42]. Tocilizumab is a monoclonal anti-human IL-6R antibody recently approved for the treatment of inflammatory autoimmune conditions. Human studies have demonstrated tocilizumab to be effective in the treatment of IL-6-related disorders such as rheumatoid arthritis or Crohn’s disease [43]. Furthermore, targeting the IL-6R may be of clinical benefit in certain malignancies such as multiple myeloma and oral squamous cell carcinoma [44, 45]. However, the use of tocilizumab in human metastatic bone disease has not yet been studied.
We here establish that tocilizumab inhibits prostate cancer growth in murine bone, indicating that tumor-derived IL-6 is critical for tumor growth in bone. Of note, due to its specificity for the human IL-6R, tocilizumab in our experimental setting can only inhibit IL-6 signalling between human (i.e. cancer) cells, while permitting tumor-derived (human) IL-6 to activate the murine IL-6R on host bone cells [35]. We have observed that tocilizumab treatment strongly inhibits tumor growth only within the murine bone environment. This suggests the presence of a biologically relevant autocrine IL-6 signalling pathway in cancer cells dependent on the bone microenvironment. Of note, serum RANKL levels were significantly lower in tumor-bearing mice treated with tocilizumab. This observation provides further evidence that cells of the osteoblast lineage are able to directly communicate with cancer cells via a RANKL/IL-6 dependent pathway, which is distinct from the osteoclast-mediated signaling pathway of the established vicious cycle [9, 10].
Treatment with tocilizumab does not alter tumor growth in subcutaneous PC3 tumors in mice and we believe this may mainly be due to the tissue-dependency within the bone microenvironment where RANKL is produced. However, it is not clear whether tumor growth in soft tissues will be inhibited by tocilizumab in immune-competent mice, in which T cells may produce RANKL to enable the interaction between RANKL and IL-6 from implanted tumor. This needs to be investigated further in future. Furthermore, whether the effects of tocilizumab on tumor growth in patients remains to be investigated. The potential clinical application may be elucidated by further preclinical and clinical trials.
We next demonstrated that IL-6 released by tumor cells induces, via the above mentioned autocrine mechanism, expression of RANK by the cancer itself. This sensitizes the tumor to the action of RANKL expressed by osteoblasts and other cells of the osteoblast lineage. We further established that activation or disruption of IL-6 signaling induces corresponding changes in tumor RANK expression, while knock-down of RANK expression in prostate cancer cells reduces tumor growth in bone. These results provide strong evidence that the cross-talk between metastatic tumor cells and cells of the osteoblast lineage is indeed via RANKL, RANK and IL-6. These results provide possible explanation for clinical findings that high RANK expression in the primary cancer and its skeletal secondaries are correlated with poor clinical prognosis [29].
It is important to note that the additional signaling pathways identified in this study act by amplifying but not replacing components of the classic vicious cycle [9]. The effects of intervention in any of the elements of the new signaling pathways are dependent on the effects on the other elements and our observations are consistent with changes in bone resorption being the critical mediator influencing tumor growth [46–48]. As demonstrated in our study, the lack of activity of any of these treatments in soft tissues emphasizes the importance of the bone specific actions of RANKL, RANK and IL-6. Similarly, the relevance of other elements, such as the release of growth factors by resorptive processes in bone or of pro-resorptive PTHrP [49] by the tumor has been demonstrated by others. Thus, there appears to be strong inter-dependence between the elements of the cycles with bone resorption being the common denominator and final mediator of tumor growth. Whether this or similar interactions exists in other types of cancers remains to be investigated.
In addition, the PC3 xenograft intra-tibial model predominately produces osteolytic changes. Even though osteosclerotic changes are a typical characteristic of human prostate cancer bone metastases, osteolytic changes usually appear first and elevated bone resorption remains a dominant feature of metastatic prostate cancer [50–52]. Also, inhibition of bone resorption with anti-resorptive agents has been shown to slow the progression to metastatic disease in patients with prostate cancer, supporting the crucial role of bone resorption in the growth even of osteosclerotic tumors [53–56]. Therefore, findings from a predominantly osteolytic cancer cell line such as PC3 are of clinical relevance. However, further examination using osteosclerotic models of prostate cancer are required to expand our findings.
In summary, we have identified two self-amplifying signalling pathways which drive prostate cancer growth in bone. These results provide experimental evidence to support therapeutic strategies targetting IL-6 and RANKL signaling in patients with skeletal secondaries from prostate cancer.
References
Coleman RE (2001) Metastatic bone disease: clinical features, pathophysiology and treatment strategies. Cancer Treat Rev 27(3):165–176
Weilbaecher KN, Guise TA, McCauley LK (2011) Cancer to bone: a fatal attraction. Nat Rev Cancer 11(6):411–425
Zheng Y, Zhou H, Brennan K, Blair JM, Modzelewski JR, Seibel MJ, Dunstan CR (2007) Inhibition of bone resorption, rather than direct cytotoxicity, mediates the anti-tumour actions of ibandronate and osteoprotegerin in a murine model of breast cancer bone metastasis. Bone 40(2):471–478
Neudert M, Fischer C, Krempien B, Bauss F, Seibel MJ (2003) Site-specific human breast cancer (MDA-MB-231) metastases in nude rats: model characterisation and in vivo effects of ibandronate on tumour growth. Int J Cancer 107(3):468–477
Armstrong AP, Miller RE, Jones JC, Zhang J, Keller ET, Dougall WC (2008) RANKL acts directly on RANK-expressing prostate tumor cells and mediates migration and expression of tumor metastasis genes. Prostate 68(1):92–104
Price JT, Quinn JM, Sims NA, Vieusseux J, Waldeck K, Docherty SE, Myers D, Nakamura A, Waltham MC, Gillespie MT, Thompson EW (2005) The heat shock protein 90 inhibitor, 17-allylamino-17-demethoxygeldanamycin, enhances osteoclast formation and potentiates bone metastasis of a human breast cancer cell line. Cancer Res 65(11):4929–4938
Zheng Y, Zhou H, Ooi LL, Snir AD, Dunstan CR, Seibel MJ (2011) Vitamin D deficiency promotes prostate cancer growth in bone. Prostate 71(9):1012–1021
Ooi LL, Zheng Y, Zhou H, Trivedi T, Conigrave AD, Seibel MJ, Dunstan CR (2010) Vitamin D deficiency promotes growth of MCF-7 human breast cancer in a rodent model of osteosclerotic bone metastasis. Bone 47(4):795–803
Mundy GR (1997) Mechanisms of bone metastasis. Cancer 80(Suppl 8):1546–1556
Guise TA (2002) The vicious cycle of bone metastases. J Musculoskelet Neuronal Interact 2(6):570–572
Kamiya N, Suzuki H, Yano M, Endo T, Takano M, Komaru A, Kawamura K, Sekita N, Imamoto T, Ichikawa T (2010) Implications of serum bone turnover markers in prostate cancer patients with bone metastasis. Urology 75(6):1446–1451
Michalaki V, Syrigos K, Charles P, Waxman J (2004) Serum levels of IL-6 and TNF-alpha correlate with clinicopathological features and patient survival in patients with prostate cancer. Br J Cancer 90(12):2312–2316
George DJ, Halabi S, Shepard TF, Sanford B, Vogelzang NJ, Small EJ, Kantoff PW (2005) The prognostic significance of plasma interleukin-6 levels in patients with metastatic hormone-refractory prostate cancer: results from cancer and leukemia group B 9480. Clin Cancer Res 11(5):1815–1820
Wegiel B, Bjartell A, Culig Z, Persson JL (2008) Interleukin-6 activates PI3 K/Akt pathway and regulates cyclin A1 to promote prostate cancer cell survival. Int J Cancer 122(7):1521–1529
Domingo-Domenech J, Oliva C, Rovira A, Codony-Servat J, Bosch M, Filella X, Montagut C, Tapia M, Campas C, Dang L, Rolfe M, Ross JS, Gascon P, Albanell J, Mellado B (2006) Interleukin 6, a nuclear factor-kappaB target, predicts resistance to docetaxel in hormone-independent prostate cancer and nuclear factor-kappaB inhibition by PS-1145 enhances docetaxel antitumor activity. Clin Cancer Res 12(18):5578–5586
Hong DS, Angelo LS, Kurzrock R (2007) Interleukin-6 and its receptor in cancer: implications for Translational Therapeutics. Cancer 110(9):1911–1928
De La Mata J, Uy HL, Guise TA, Story B, Boyce BF, Mundy GR, Roodman GD (1995) Interleukin-6 enhances hypercalcemia and bone resorption mediated by parathyroid hormone-related protein in vivo. J Clin Invest 95(6):2846–2852
Suda T, Takahashi N, Udagawa N, Jimi E, Gillespie MT, Martin TJ (1999) Modulation of osteoclast differentiation and function by the new members of the tumor necrosis factor receptor and ligand families. Endocr Rev 20(3):345–357
Franchimont N, Lambert C, Huynen P, Ribbens C, Relic B, Chariot A, Bours V, Piette J, Merville MP, Malaise M (2005) Interleukin-6 receptor shedding is enhanced by interleukin-1beta and tumor necrosis factor alpha and is partially mediated by tumor necrosis factor alpha-converting enzyme in osteoblast-like cells. Arthritis Rheum 52(1):84–93
Kudo O, Sabokbar A, Pocock A, Itonaga I, Fujikawa Y, Athanasou NA (2003) Interleukin-6 and interleukin-11 support human osteoclast formation by a RANKL-independent mechanism. Bone 32(1):1–7
Sansone P, Storci G, Tavolari S, Guarnieri T, Giovannini C, Taffurelli M, Ceccarelli C, Santini D, Paterini P, Marcu KB, Chieco P, Bonafe M (2007) IL-6 triggers malignant features in mammospheres from human ductal breast carcinoma and normal mammary gland. J Clin Invest 117(12):3988–4002
Schafer ZT, Brugge JS (2007) IL-6 involvement in epithelial cancers. J Clin Invest 117(12):3660–3663
Kim MY, Oskarsson T, Acharyya S, Nguyen DX, Zhang XH, Norton L, Massague J (2009) Tumor self-seeding by circulating cancer cells. Cell 139(7):1315–1326
Sohara Y, Shimada H, Minkin C, Erdreich-Epstein A, Nolta JA, DeClerck YA (2005) Bone marrow mesenchymal stem cells provide an alternate pathway of osteoclast activation and bone destruction by cancer cells. Cancer Res 65(4):1129–1135
Ara T, Song L, Shimada H, Keshelava N, Russell HV, Metelitsa LS, Groshen SG, Seeger RC, DeClerck YA (2009) Interleukin-6 in the bone marrow microenvironment promotes the growth and survival of neuroblastoma cells. Cancer Res 69(1):329–337
Bendre MS, Margulies AG, Walser B, Akel NS, Bhattacharrya S, Skinner RA, Swain F, Ramani V, Mohammad KS, Wessner LL, Martinez A, Guise TA, Chirgwin JM, Gaddy D, Suva LJ (2005) Tumor-derived interleukin-8 stimulates osteolysis independent of the receptor activator of nuclear factor-kappaB ligand pathway. Cancer Res 65(23):11001–11009
Bussard KM, Venzon DJ, Mastro AM (2010) Osteoblasts are a major source of inflammatory cytokines in the tumor microenvironment of bone metastatic breast cancer. J Cell Biochem 111(5):1138–1148
Paule B, Terry S, Kheuang L, Soyeux P, Vacherot F, de la Taille A (2007) The NF-kappaB/IL-6 pathway in metastatic androgen-independent prostate cancer: new therapeutic approaches? World J Urol 25(5):477–489
Santini D, Perrone G, Roato I, Godio L, Pantano F, Grasso D, Russo A, Vincenzi B, Fratto ME, Sabbatini R, Della Pepa C, Porta C, Del Conte A, Schiavon G, Berruti A, Tomasino RM, Papotti M, Papapietro N, Muda AO, Denaro V, Tonini G (2011) Expression pattern of receptor activator of NFκB (RANK) in a series of primary solid tumors and related bone metastases. J Cell Physiol 226(3):780–784
Jones DH, Nakashima T, Sanchez OH, Kozieradzki I, Komarova SV, Sarosi I, Morony S, Rubin E, Sarao R, Hojilla CV, Komnenovic V, Kong YY, Schreiber M, Dixon SJ, Sims SM, Khokha R, Wada T, Penninger JM (2006) Regulation of cancer cell migration and bone metastasis by RANKL. Nature 440(7084):692–696
Xiong J, Onal M, Jilka RL, Weinstein RS, Manolagas SC, O’Brien CA (2011) Matrix-embedded cells control osteoclast formation. Nat Med 17(10):1235–1241
Zheng Y, Zhou H, Fong-Yee C, Modzelewski JR, Seibel MJ, Dunstan CR (2008) Bone resorption increases tumour growth in a mouse model of osteosclerotic breast cancer metastasis. Clin Exp Metastasis 25(5):559–567
Zheng Y, Seibel M, Zhou H (2011) Methods in bone biology: cancer and bone. Osteoporosis research: animal models, 1st edn. Springer, New York
Lacey DL, Timms E, Tan HL, Kelley MJ, Dunstan CR, Burgess T, Elliott R, Colombero A, Elliott G, Scully S, Hsu H, Sullivan J, Hawkins N, Davy E, Capparelli C, Eli A, Qian YX, Kaufman S, Sarosi I, Shalhoub V, Senaldi G, Guo J, Delaney J, Boyle WJ (1998) Osteoprotegerin ligand is a cytokine that regulates osteoclast differentiation and activation. Cell 93(2):165–176
Ehlers M, Grotzinger J, deHon FD, Mullberg J, Brakenhoff JP, Liu J, Wollmer A, Rose-John S (1994) Identification of two novel regions of human IL-6 responsible for receptor binding and signal transduction. J Immunol 153(4):1744–1753
Igawa T, Ishii S, Tachibana T, Maeda A, Higuchi Y, Shimaoka S, Moriyama C, Watanabe T, Takubo R, Doi Y, Wakabayashi T, Hayasaka A, Kadono S, Miyazaki T, Haraya K, Sekimori Y, Kojima T, Nabuchi Y, Aso Y, Kawabe Y, Hattori K (2011) Antibody recycling by engineered pH-dependent antigen binding improves the duration of antigen neutralization. Nat Biotechnol 28(11):1203–1207
Axmann R, Böhm C, Krönke G, Zwerina J, Smolen J, Schett G (2009) Inhibition of interleukin-6 receptor directly blocks osteoclast formation in vitro and in vivo. Arthritis Rheum 60(9):2747–2756
Blair JM, Zheng Y, Dunstan CR (2007) RANK ligand. Int J Biochem Cell Biol 39(6):1077–1081
Takayanagi H, Ogasawara K, Hida S, Chiba T, Murata S, Sato K, Takaoka A, Yokochi T, Oda H, Tanaka K, Nakamura K, Taniguchi T (2000) T-cell-mediated regulation of osteoclastogenesis by signalling cross-talk between RANKL and IFN-[gamma]. Nature 408(6812):600–605
Shariat SF, Andrews B, Kattan MW, Kim J, Wheeler TM, Slawin KM (2001) Plasma levels of interleukin-6 and its soluble receptor are associated with prostate cancer progression and metastasis. Urology 58(6):1008–1015
Salgado R, Junius S, Benoy I, Van Dam P, Vermeulen P, Van Marck E, Huget P, Dirix LY (2003) Circulating interleukin-6 predicts survival in patients with metastatic breast cancer. Int J Cancer 103(5):642–646
Ignatoski KM, Friedman J, Escara-Wilke J, Zhang X, Daignault S, Dunn RL, Smith DC, Keller ET (2009) Change in markers of bone metabolism with chemotherapy for advanced prostate cancer: interleukin-6 response is a potential early indicator of response to therapy. J Interferon Cytokine Res 29(2):105–112
Nishimoto N, Kishimoto T (2008) Humanized antihuman IL-6 receptor antibody, tocilizumab. Handb Exp Pharmacol 181:151–160
Shinriki S, Jono H, Ota K, Ueda M, Kudo M, Ota T, Oike Y, Endo M, Ibusuki M, Hiraki A, Nakayama H, Yoshitake Y, Shinohara M, Ando Y (2009) Humanized Anti-Interleukin-6 Receptor Antibody Suppresses Tumor Angiogenesis and In vivo Growth of Human Oral Squamous Cell Carcinoma. Clin Cancer Res 15(17):5426–5434
Sakai A, Oda M, Itagaki M, Yoshida N, Arihiro K, Kimura A (2010) Establishment of an HS23 stromal cell-dependent myeloma cell line: fibronectin and IL-6 are critical. Int J Hematol 92(4):598–608
Guise TA, Mohammad KS, Clines G, Stebbins EG, Wong DH, Higgins LS, Vessella R, Corey E, Padalecki S, Suva L, Chirgwin JM (2006) Basic Mechanisms Responsible for Osteolytic and Osteoblastic Bone Metastases. Clin Cancer Res 12(20):6213s–6216s
Ooi LL, Zheng Y, Stalgis-Bilinski K, Dunstan CR (2011) The bone remodeling environment is a factor in breast cancer bone metastasis. Bone 48(1):66–70
Zheng Y, Zhou H, Dunstan C, Sutherland RL, Seibel M (2013) The role of the bone microenvironment in skeletal metastasis. J Bone Oncol 2(1):47–57
Guise TA, Yin JJ, Thomas RJ, Dallas M, Cui Y, Gillespie MT (2002) Parathyroid hormone-related protein (PTHrP)-(1-139) isoform is efficiently secreted in vitro and enhances breast cancer metastasis to bone in vivo. Bone 30(5):670–676
Zhang J, Dai J, Qi Y, Lin DL, Smith P, Strayhorn C, Mizokami A, Fu Z, Westman J, Keller ET (2001) Osteoprotegerin inhibits prostate cancer-induced osteoclastogenesis and prevents prostate tumor growth in the bone. J Clin Invest 107(10):1235–1244
Brown JE, Cook RJ, Major P, Lipton A, Saad F, Smith M, Lee KA, Zheng M, Hei YJ, Coleman RE (2005) Bone turnover markers as predictors of skeletal complications in prostate cancer, lung cancer, and other solid tumors. J Natl Cancer Inst 97(1):59–69
Berruti A, Tucci M, Mosca A, Tarabuzzi R, Gorzegno G, Terrone C, Vana F, Lamanna G, Tampellini M, Porpiglia F, Angeli A, Scarpa RM, Dogliotti L (2005) Predictive factors for skeletal complications in hormone-refractory prostate cancer patients with metastatic bone disease. Br J Cancer 93(6):633–638
Fizazi K, Carducci M, Smith M, Damiao R, Brown J, Karsh L, Milecki P, Shore N, Rader M, Wang H, Jiang Q, Tadros S, Dansey R, Goessl C (2011) Denosumab versus zoledronic acid for treatment of bone metastases in men with castration-resistant prostate cancer: a randomised, double-blind study. Lancet 377(9768):813–822
Fizazi K, Bosserman L, Gao G, Skacel T, Markus R (2013) Denosumab treatment of prostate cancer with bone metastases and increased urine N-telopeptide levels after therapy with intravenous bisphosphonates: results of a randomized phase II trial. J Urol 189(Suppl 1):S51–S58
Coleman R, Gnant M, Morgan G, Clezardin P (2012) Effects of bone-targeted agents on cancer progression and mortality. J Natl Cancer Inst 104(14):1059–1067
Smith MR, Saad F, Coleman R, Shore N, Fizazi K, Tombal B, Miller K, Sieber P, Karsh L, Damiao R, Tammela TL, Egerdie B, Van Poppel H, Chin J, Morote J, Gomez-Veiga F, Borkowski T, Ye Z, Kupic A, Dansey R, Goessl C (2012) Denosumab and bone-metastasis-free survival in men with castration-resistant prostate cancer: results of a phase 3, randomised, placebo-controlled trial. Lancet 379(9810):39–46
Acknowledgments
This work has been supported in part by the following Grants: Cure Cancer Foundation of Australia (Y.Z), Cancer Institute New South Wales (Y.Z), Cancer Council New South Wales (M.J.S, Y.Z, H.Z, C.R.D), Prostate Cancer Foundation of Australia (PCFA) (M.J.S, Y.Z, H.Z, C.R.D), University of Sydney Cancer Research Fund (M.J.S), National Health and Medical Research Council, Australia (NHMRC) (Y.Z, Early Career Fellowship 596870) and Bundesministerium für Bildung und Forschung (BMBF) and the State of Berlin (K.B. F.B., BCRT-Grant I and II). We thank Dr. Matthew Foley and the staff at the Australian Centre for Microscopy & Microanalysis, The University of Sydney for the facilities as well as scientific and technical assistance.
Conflict of interest
The authors disclose no potential conflicts of interest.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Zheng, Y., Basel, D., Chow, SO. et al. Targeting IL-6 and RANKL signaling inhibits prostate cancer growth in bone. Clin Exp Metastasis 31, 921–933 (2014). https://doi.org/10.1007/s10585-014-9680-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10585-014-9680-3