Abstract
Malignant melanomas are characterized by the ability of early metastatic dissemination to regional lymph nodes and the detection of sentinel lymph node metastases serves as an important prognostic parameter. There is clear evidence that melanoma cells and stromal cells of tumor environment can induce lymphangiogenesis, e.g. growth of lymphatic vessels, and this phenomenon is correlated with lymph node metastases. Vascular endothelial growth factor (VEGF) C represents the most potent and well-recognized lymphangiogenic growth factor secreted in tumor milieu by melanoma cells and tumor-associated macrophages, however the mechanism underlying VEGF-C secretion is not completely understood. We demonstrate that an acidic extracellular pH promotes the expression of VEGF-C in A375P melanoma cells and in melanoma cells isolated from a human spontaneous metastatic lesion, through the NF-κB transcription factor. We also demonstrate that esomeprazole, a proton pump inhibitor which requires acidosis to be activated, is able to prevent VEGF-C expression in acidic melanoma cells by interfering with NF-κB activation. Furthermore, we show that esomeprazole abrogates the enhanced VEGF-C expression in tumor cells grown in a acidic medium and stimulated by IL-1β. On the whole, the present study reveals that acidity may be considered a strong promoter of VEGF-C expression in melanoma cells and provides a new pharmacological target to limit the development of tumor lymphangiogenesis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Dissemination of tumor cells to regional lymph nodes is the first and most common site of metastasis for various solid tumors [1] and the extent of lymph node involvement represents a key determinant for staging and prognosis [2]. Until recently, lymph node colonization by tumor cells is ascribed to a passive process involving tumor cell spread throughout preexisting afferent lymphatic vessels. Now, we know that tumor cells and host inflammatory cells of tumor environment, mainly tumor-associated macrophages, contribute to lymphatic dissemination through de novo formation of lymphatic capillaries, a phenomenon named lymphangiogenesis [3–7]. Among members of vascular endothelial growth factors (VEGF), the VEGF-C is considered the most important lymphangiogenic growth factor, required for embryonic, postnatal lymphatic development and tumor progression, also, VEGF receptor-3 (VEGFR-3) is the determinant receptor of VEGF-C and it represents a marker for lymphatic endothelial cells [8, 9]. Stimulation of VEGF-C/VEGFR-3 axis increases lymph node metastasis [9–11], while VEGFR-3 antagonists are able to inhibit lymphangiogenesis of primary tumor and tumor cells dissemination through lymphatic vessels [12]. Human tumor cells, including human melanoma cells release VEGF-C, that promotes colonization of regional lymph nodes and metastases outgrowth [13]. Lymphatic mapping and sentinel lymph node (SLN) biopsy is the most important prognostic factor for patients with intermediate-thickness melanomas. Recent studies demonstrated that tumor-induced lymphangiogenesis and increased lymph flow precede melanoma metastasis [14]. This discovery suggests that lymphatic vessel growth in sentinel lymph nodes might be considered a premetastatic niche. Furthermore, Hoshida et al. [15] showed that VEGF-C induces hyperplasia of peritumoral lymphatic vessels, increases the flow rate in lymphatic vessels and increases lymph node metastasis. Indeed, several papers are showing that peritumoral lymphatic vessels are functional, and those at the tumor margin play the major role in tumor cells lymphatic dissemination [16]. Although the contribution of lymphatic vessels to tumor progression has been demonstrated and the role of VEFG-C is well defined, the mechanism underlying the induction of VEGF-C in tumor cells remains unclear.
Normal tissues use glycolysis to generate approximately 10 % of the intracellular ATP, while tumor cells use glycolysis to produce more than 50 % of the energy requirement, even when there is enough O2 to support mitochondrial function (aerobic glycolysis) [17]. Indeed, Hypoxia Inducible Factor-α-dependent glycolytic genes are readily induced in tumor cells exposed to mild hypoxia (2–3 % O2), which is low enough to induce HIF1-α activity but high enough to support vigorous oxidative phosphorylation. Moreover, large regions of a tumor are often at a great distance from blood vessels and lymphatic vessels, and this distance causes low levels of O2 tension and nutrients, and increased levels of waste products [18]. Thus, acidosis represents a metabolic hallmark of tumor environment either generated by aerobic glycolysis, anaerobic glycolysis or reduced lymphatic drainage of waste products [19].
Several studies revealed that a reversed pH gradient is present across tumor cells plasma membrane, as the intracellular pH (pHi) ranges from 7.12 to 7.56 and the extracellular pH (pHe) ranges from 6.2 to 6.9 [20]. The maintenance of this gradient is due to the presence of ion transport transmembrane proteins which release protons (H+) and acidify tumor cell extracellular environment [21–23]. Now, we know that tumors with acidic environment are associated with a poorer prognosis [24], resistance to chemotherapy [25], suppression of cytotoxic lymphocytes and natural killer cells tumoricidal activity [26]. Tumor acidity also contributes to tumor cells aggressiveness, by increasing their mutation rate [27], invasiveness into host tissues and secondary organ colonization [28, 29]. The lowest pHe value has been observed near the tumor periphery, where tumor cells are invading normal tissues [30]. These phenomena might be also due to hypoxia, often associated with acidity [31]. However, there is an increased evidence that extracellular acidity per se contributes to malignancy of tumor cells. In addition, acidic environment modifies the expression of VEGF-A, since a transient [32], but not prolonged [33] exposure to acidosis stimulates NF-κB-dependent up-regulation of VEGF-A in human tumor cells. Moreover, 8 h-exposure at pH 5.5 induces in human endometrial carcinoma cells an alternative splicing of VEGF-A (VEGF121) through p38 activation [34].
Here, we show that acidity stimulates VEGF-C expression and secretion in melanoma cells, through NF-κB transcription factor. We also demonstrate that esomeprazole, a proton pump inhibitor (PPI) activated by a low pH, inhibits VEGF-C expression in acidic melanoma cells through the down regulation of NF-κB, either in the absence or in the presence of interleukin-1β (IL-1β), a potent agonist of tumoral VEGF-C. In this study, we used A375P melanoma line and a primary culture of melanoma cells isolated from a human metastatic lesion.
Methods
Materials
Unless specified, all reagents were obtained from Sigma. Antibody were purchased as follows: goat anti-VEGF-C from Abcam, rabbit anti-NFκB, rabbit anti-IkB, anti-rabbit IgG-FITC from Santa Cruz Biotechnology; mouse anti-β-tubulin was from Millipore (05–661); biotinylated secondary antibody streptavidin-horseradish-peroxidase-conjugated-HRP (Universal LSAB™+Kit/HRP, Rabbit/Mouse/Goat) were from DAKO; DAPI staining was from Invitrogen. All products for end point PCR analysis were purchased from Promega. Recombinant human cytokine interleukin-1β (IL-1β) was from PeproTech. siRNA for NF-κB was purchased from Santa Cruz; Lipofectamine 2000 was from Invitrogen; esomeprazole salt (a PPI) was donated from Dr. Stefano Fais (National Institute of Health, Rome). Parthenolide (NF-κB pathway inhibitor) was from Calbiochem (512732).
Cell lines and culture conditions
A375P human melanoma, DU-145 human prostate carcinoma and MCF-7 human breast carcinoma cell lines used in this study were obtained from American Type Culture Collection (ATCC, Rockville, MD); the primary cell culture line SSM2c was obtained from the Laboratory of Tumor Cell Biology, Core Research Laboratory-Istituto Toscano Tumori (CRL-ITT, Florence, Italy) [35]. Cells were cultivated in Dulbecco’s Modified Eagle Medium (DMEM 4500, GIBCO) supplemented with 10 % foetal calf serum (FCS, Boerhinger Mannheim, Germany), at 37 °C in a 10 % CO2 humidified atmosphere. Cells were harvested from subconfluent cultures by incubation with a trypsin–EDTA solution, and propagated every 3 days. Viability of the cells was determined by trypan blue exclusion test. Cultures were periodically monitored for mycoplasma contamination using Chen’s fluorochrome test [36].
Acidic treatment
Low pH medium was obtained by addition of HCl 1 N in DMEM 4500 containing 10 % FCS and pH value was monitored by a pHmeter (Orion PH Meter 520A-1). As pH value was stable (6.6–6.7), acidified medium was added to cultures and the seal caps of flasks were tightly closed. pH of acidified media were verified 2 h later and at the end of the experiment. Cultures were exposed to the acidified medium for 4–24 h. In some experiments 1.5–5 μM parthenolide or 100 μM esomeprazole were added to standard or acidified media. Treatment with 1,000 U/ml IL1-β was performed 2 h before media acidification.
RNA isolation and end point PCR
Total RNA was extracted from cells by using TRI Reagent (Sigma). The amount and purity of RNA were determined spectrophotometrically. cDNA synthesis was obtained by incubating 1 μg of total RNA with 4 U/μl of M-MLV reverse transcriptase. Aliquots of 5 μl of the cDNA mixture were used for PCR amplification. The end-point PCR reactions were carried out in 50 μl of a solution containing specific primers and 0.1 U/μl of GoTaq Polymerase, using a Perkin-Elmer Thermal cycler. The primers were: VEGF-C forward 5′-CCCCACATCTATACACACCTCC-3′, reverse 5′-TCCGGACTCGACCTCTCGGAC-3′; GAPDH forward 5′-ACCACAGTCCATGCCATCAC-3′, reverse 5′-TCCACCACCCTGTTGCTGTA-3′. Aliquots of 10 μl of each PCR mixture were applied to a 2 % agarose gel, electrophoresed and visualized. cDNA products were evaluated on the basis of standard PCR markers.
Real-time quantitative RT-PCR (qPCR)
Quantitative real time PCR (qPCR) was performed using the GoTaq® Probe Systems (Promega). Two microgram of total RNA were used to prepare cDNA using GoScript™ Reverse Transcription System (Promega) according to the manufacturer’s instructions. The qPCR analysis was carried out in triplicate using an Applied Biosystems 7500 Sequence Detector. The primers were designed according to published human cDNA sequences in Genbank database, using the FastPCR software: VEGF-C forward 5′-GAAGGTGAAGGTCGGAGTC-3′ and reverse 5′-GAAGATGGTGATGGGATTTC-3′; VEGFR2 forward 5′-CCAGTCAGAGACCCACGTTT-3′ and reverse 5′-AGTCTTTGCCATCCTGCTGA-3′, VEGFR3 forward 5′-TGGTACCGGCTCAACCTCTC-3′ and reverse 5′-CACGTTTTTGCAGTCCAGCA-3′, and 18S forward 5′-CGCCGCTAGAGGTGAAATTCT-3′ and reverse 5′-CGAACCTCCGACTTTCGTTCT-3′. mRNA was quantified with the ∆∆Ct method as described [37]. mRNA levels were normalized to 18S as an endogenous control.
siRNA transfection
For tumor cell transfections, the siRNA for NFkB was diluted to a final concentration of 20 nM and cells transfected using Lipofectamine 2000 were incubated in standard medium for 24 h before they were exposed to low pH.
Western blotting analysis
Cells, washed twice with ice cold PBS containing 1 mM Na3VO4, were lysed in 100 μl of cell lysis buffer containing: 20 mM Tris–HCl (pH 7.4), 150 mM NaCl, 100 mM HEPES, 1 % Triton X-100, 10 mM glycerophosphate, 100 μM PMSF, 100 mM AEBSF, 5 mM bestatin, 2 mM leupeptin, 1 mM pepstatin A, 80 μM of aprotinin, and 1.5 mM E-64. Supernatants containing equal amounts of protein (65 μg) in Laemmli buffer were separated on 10 % (v/v) SDS–PAGE gel. Fractionated proteins were transferred from the gel to a PVDF nitrocellulose membrane. Blots were stained with Ponceau red to ensure equal loading and complete transfer of proteins and then blocked with 2.5 % (w/v) BSA in T-TBS (0.1 % (v/v) Tween 20 in PBS for 1 h at room temperature. Subsequently, the membrane was probed with rabbit anti-human VEGF-C, rabbit anti-human IkB, or mouse anti-human-β tubulin, diluted 1:1,000 with 2.5 % (w/v) skimmed milk in T-PBS buffer at 4 °C overnight. After washing in T-PBS buffer, the membrane was incubated with a HRP-anti-rabbit (1:16,000) or anti-mouse (1:10,000) secondary antibody, diluted in 2.5 % (w/v) BSA/T-PBS, for 1 h at room temperature. After consecutive washing with T-PBS the immunoreactive bands were visualized by the ECL detection system (GE Healthcare).
Immunofluorescence
Tumor cells were cultured on 25-mm coverslips, fixed for 20 min in 4 % paraformaldehyde and then permeabilized with 0.1 % Triton X-100 solution in PBS. Permeabilized cells were incubated in blocking solution (PBS supplemented with 4 % BSA and 1 % horse serum) and then incubated overnight at 4 °C with anti-NF-κB antibody. Cells were washed and then incubated for 1 h using 1:100 goat anti-rabbit IgG-FITC. Cell nuclei were counterstained with DAPI (1 μg/ml for 30 min). Following two washes in PBS, coverslips were mounted with propylthiogallate on glass slides and the cells were observed with an inverted confocal Nikon Eclipse TE2000 microscope equipped with a ×60S-Fluor oil immersion lens.
Statistical analysis
Densitometric data are expressed as means ± standard errors of the mean (SEM) depicted by vertical bars from representative experiment of at least three independent experiments. Statistical analysis of the data was performed by student’s t test, and p ≤ 0.05 was considered statistically significant.
Results
Expression of VEGF-C in human melanoma cells grown in media at a different pH
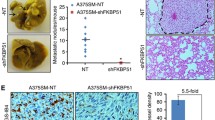
A375P melanoma cells grown in standard culture conditions reach the confluence at the fourth day of growth and pH of media changes from 7.4 to 6.8 (Fig. 1, panel A). We found that mRNA and VEGF-C protein of confluent cells (pH 6.8 medium) are significantly higher than those of cells recovered from sparse cultures (pH 7.2 medium) (Fig. 1, panel B). We also found that VEGF-C expression is enhanced in tumor cells of sparse cultures when they were exposed to media collected from confluent melanoma cell cultures at pH 6.8, (Fig. 1, panel C). To ascertain whether induction of VEGF-C in A375P melanoma cells was related to a low pH, and not to agents released by tumor cells themselves in confluent cultures, we examined whether media collected from sparse cultures acidified to pH 6.6 and media that have not been exposed to cells acidified to pH 6.7 may stimulate VEGF-C expression in melanoma cells. We found that both media stimulate VEFG-C expression in melanoma cells. These results clearly indicate that acidity per se may promote VEGF-C in A375P melanoma cells. Finally, pH response curve (Fig. 1, panel D) shows that change of pH medium from 7.4 to 6.5 promotes VEGF-C expression in a progressive manner and the maximum effect on VEGF-C expression occurs at pH 6.8. pH response curve experiments indicate that acidity does not modify in melanoma cells the very low level of expression of VEGF-C receptor 2 and 3 (data not shown). It is known that VEGF-C binds VEGF-C receptor 3 and induces tyrosine auto-phosphorylation of VEGF-C receptor 2 and 3 leading to angiogenesis and lymphangiogenesis [38].
Change in VEGF-C expression in A375P human melanoma cells grown in an acidic medium. a Growth curve and pH of media in melanoma cell cultures; b VEGF-C mRNA and protein expression of secreted VEGF-C form in sparse (pH 7.2) and confluent (pH 6.7) cell cultures, each band was quantified by densitometric analysis. The corresponding histogram was normalised against GAPDH or β-tubulin, and expressed as the percentage of increment; c VEGF-C mRNA expression in melanoma cells of: (i) sparse cultures grown in an acidic medium collected from confluent cultures, (ii) sparse cultures grown in acidified sparse culture medium, and (iii) sparse cultures grown in acidified medium that have not been exposed to cells (each band was quantified by densitometric analysis, the corresponding histogram was normalised against GAPDH and expressed as the percentage of increment); d quantitative real-time PCR of VEGF-C expression in melanoma cells incubated for 24 h in unexposed media at different pH. Values presented are mean ± SEM of three independent experiments. Asterisk indicates p < 0.05
Low pH stimulates expression of VEGF-C in melanoma cells through NF-κB activity
The up-regulation of VEGF-C expression induced in A375P melanoma cells by an acidic medium was inhibited by the treatment with Parthenolide either at 1.5 or 5 μM (Fig. 2 panel A). The inhibitory effect of Parthenolide, either at 1.5 or 5 μM, was also demonstrated in melanoma cells incubated under normal pH. Moreover, we found that VEGF-C up-regulation was inhibited in A375P melanoma cells transfected with p65 NF-κB siRNA and exposed to an acidic medium (Fig. 2 panel B). These findings suggest that VEGF-C expression of melanoma cells grown under normal and, more effectively, low pH is dependent from NF-κB signaling pathway.
Change in VEGF-C expression in A375P melanoma cells exposed to an acidic medium in the presence of parthenolide (1.5 or 5 μM). a Inhibition by parthenolide of VEGF-C mRNA expression in acidic melanoma cells; b inhibition by siRNA for NF-κB of VEGF-C mRNA expression in acidic melanoma cells. In box of the figure, a representative blot of NF-κB protein expression in A375P melanoma cells grown in acidic medium transfected with siRNA for NF-κB or scramble. mRNA expression was quantified by densitometric analysis, the corresponding histogram was normalised against GAPDH and expressed as the percentage of increment. Values presented are mean ± SEM of three independent experiments. Asterisk indicates p < 0.05
Esomeprazole inhibits VEGF-C expression in acidic human melanoma cells
In order to establish whether a PPI, might be effective to abrogate VEGF-C up-regulation induced by acidity, we choose esomeprazole. Esomeprazole is a common PPI which is protonated and activated in an acidic medium to express its pharmacological effects, among those, the recently described anti-inflammatory special property [39].
For this study, 100 μM esomeprazole was selected in accordance with PPIs plasma level found in human beings after intravenous administration of these drugs. Incubation of human A375P melanoma cells for 24 h in a acidic medium containing 100 μM esomeprazole does not significantly modify their viability (viable cells >95 %) and pH of the medium (data not shown).
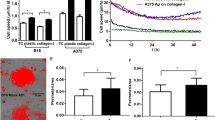
Analysis of intracellular location of NF-κB in melanoma cells grown under a standard or acidic medium, revealed that these cells exposed to a standard pH medium (pH 7.4) express an exclusive labeling in cytoplasm, while cells exposed to a standard medium acidified to pH 6.7, immediately before its use, show nuclear localization of NF-κB/p65 subunit with a peak at 6 h after treatment (Fig. 3, panel A). Interestingly, 100 μM esomeprazole concentration strongly inhibits NF-κB activation in A375P melanoma cells exposed for 6 h to a reduced pH (pH 6.7) (Fig. 3, panel B). Importantly we demonstrate that esomeprazole effectively inhibits VEGF-C expression in acidic melanoma cells (Fig. 3, panel C).
Inhibition by esomeprazole (100 μM) of NF-κB-dependent up-regulation of VEGF-C mRNA expression in acidic A375P melanoma cells. a Double immunofluorescence analysis of NF-kB/p65 nuclear traslocation in melanoma cells exposed to an acidic medium for 4, 6 and 18 h (NF-κB/p65 green, DAPI blue); the columns represent the percentage of cells expressing nuclear NF-kB. b Double immunofluorescence analysis of melanoma cells exposed for 6 h to an acidic medium and treated with esomeprazole (NF-κB/p65 green, DAPI blue), the columns represent the percentage of cells expressing nuclear NF-kB. c Inhibition by esomeprazole of VEGF-C mRNA expression in acidic melanoma cells. d Inhibition by esomeprazole of VEGF-C mRNA expression in acidic melanoma cells treated with IL1-β. mRNA expression was quantified by densitometric analysis, the corresponding histogram was normalised against GAPDH and expressed as the percentage of increment. Values presented are mean ± SEM of at least three independent experiments. Asterisk indicates p < 0.05. (Color figure online)
Inflammatory cytokines, such as TNFα and IL-1β stimulate VEGF-C expression in human vascular endothelial cells mainly through NF-κB activation [40–42], and represent suitable promoters of VEGF-C also in melanoma cells. We found that TNFα and, in a more evident way, IL-1β stimulate VEGF-C mRNA in A375P melanoma cells, and this promotion was inhibited by the NF-κB inhibitor Parthenolide (data not shown). Figure 3, panel D indicates that the IL-1β-stimualted expression of VEGF-C was inhibited in melanoma cells that were incubated with in an acidic medium containing esomeprazole. Esomeprazole, on the other hand, does not abrogate VEGF-C up-regulation induced by IL-1β when tumor cells were incubated in a standard medium (pH 7.4), because esomeprazole activation necessitates an acidic environment. These results indicate that esomeprazole may inhibit VEGF-C expression in A375P melanoma cells stimulated by inflammatory cytokines, only in case acidity takes part to the environmental changes.
Esomeprazole, reduces VEGF-C expression in human melanoma cells freshly isolated from a metastatic human melanoma lesion
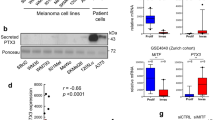
We demonstrated that acidity stimulates VEGF-C expression in human melanoma cells collected from a spontaneous metastatic lesion and esomeprazole blocked it. Also in primary human melanoma, Parthenolide inhibits VEGF-C expression promoted by low pH (Fig. 4, panel A). As we found in A375P melanoma line, we demonstrate that esomeprazole abolishes VEGF-C expression induced by acidity through NF-κB signaling (Fig. 4 panel C, D). Indeed, esomeprazole stimulates, in these primary tumor cells, the expression of the well known inhibitor IKB (Fig. 4 panel B). In addition, esomeprazole, abolishes the up-regulation of VEGF-C expression in tumor cells grown in a acidic medium containing IL-1β. On the whole, esomeprazole exerts an effective anti-VEGF-C activity also in melanoma cells of a primary culture derived from a spontaneous metastatic lesion.
Inhibition of NF-κB-dependent up-regulation of VEGF-C mRNA in acidic primary culture of melanoma. a Inhibition by parthenolide 5 μM of VEGF-C mRNA in melanoma cells grown in an acidic medium. b IκB protein expression in acidic melanoma cells treated with esomeprazole (100 μM) for 24 h; c inhibition by esomeprazole of VEGF-C mRNA of acidic melanoma cells. d Inhibition by esomeprazole of NF-κB-dependent up-regulation of VEGF-C mRNA in melanoma cells treated with IL1β and/or an acidic media for 24 h. mRNA and protein expression were quantified by densitometric analysis, the corresponding histogram was normalised against GAPDH or β-tubulin and expressed as the percentage of increment. Values presented are mean ± SEM of at least three independent experiments. Asterisk indicates p < 0.05
Acidity and VEGF-C expression in breast and prostate carcinoma cells
Figure 5 indicates that the effect of low pH on VEGF-C expression is not limited to melanoma cells, indeed acidified media stimulate VEGF-C expression in some carcinoma cells, e.g. DU145 prostate carcinoma cells and MCF-7 breast carcinoma cells.
VEGF-C expression in breast and prostate carcinoma cells grown in an acidic medium. a Quantitative real time PCR (qPCR) of VEGF-C mRNA of MCF-7 breast carcinoma cells incubated for 24 h at pH 7.4 and 6.7; b qPCR of VEGF-C mRNA of DU145 prostate carcinoma cells incubated for 24 h at pH 7.4, 7.1 and 6.7. Values presented are mean ± SEM of at least two independent experiments. Asterisk indicates p < 0.05
Discussion
Skin malignant melanoma primarily metastasizes to lymph nodes and the detection of sentinel lymph node metastases is considered as an important prognostic parameter [1, 2]. It is well known that melanoma cells can promote growth of lymphatic vessels, mainly at the tumor-stroma interface and the size of peritumoral lymphatic vessels has been indicated as the most important factor that contributes to lymph node metastasis [16]. Some typical structural features of lymphatic vessels, such as a large diameter, a discontinuous layer of basement membrane and absence in small lymphatic vessels of pericytes or vascular smooth muscle cells, make them more accessible for intravasation by tumor cells. Thus the so-called “lymphangiogenic switch” is crucial for tumor cell fate [3, 7]. A potent tumor lymphangiogenesis growth factor is the VEGF-C, which is also indispensable for embryonic lymphangiogenesis [43].
Our results identify for the first time acidity as a positive regulator of mRNA and protein VEGF-C synthesis in melanoma cells and thereby implicate low pH in the control of lymphangiogenesis. The results further suggest that NF-κB signaling plays a role in the up-regulation of VEGF-C in acidic melanoma cells. VEGF-C gene promoter contains conserved putative binding site for NF-κB and no TATA box [41], and different authors [44–46] demonstrated that acidic pH activates NF-κB, which is important to up-regulate IL-8 production in granulocytes [47]. Bellocq et al. [48] have also demonstrated that NF-κB is involved in extracellular pH-mediated up-regulation of inducible nitric oxide synthase.
In order to find a drug to control VEGF-C up-regulation by acidosis, we tested whether esomeprazole, a vacuolar H+-ATPase (V-ATPase) inhibitor, might be effective [47]. We demonstrated that esopremazole, without modifying pH, abrogates NF-κB activation and VEGF-C expression in acidic A375P melanoma cells. In addition, melanoma cells isolated from a spontaneous metastatic lesion express a higher amount of VEGF-C when grown in low pH and esomeprazole abolishes this effect. Esomeprazole, activated by an acidic medium, was also effective to reduce VEGF-C expression in tumor cells exposed to IL-1β. IL-1β has been found to be a strong promoter of melanoma VEGF-C expression through NF-κB pathway. It is known that acidosis and a chronic inflammatory reaction are often associated in tumors. IL-1β stimulation of VEGF-C expression was showed in human lung fibroblasts and vascular endothelial cells [40].
Our findings also indicate that esomeprazole inhibits VEGF-C expression in melanoma cells isolated from a human metastatic lesion. It is possible that during a long-stay in culture, tumor cells may acquire or loose some special characters becoming different from those freshly isolated from a spontaneous tumors. Thus, it is important to confirm every findings using primary cultures to increase their translational significance.
Esomeprazole as vacuolar H+-ATPase (V-ATPase) inhibitor is used extensively to suppress gastric acidity, however V-ATPase is expressed also in the plasma membrane of several tumor cells [49–53], including A375 melanoma cells [54]. De Milito et al. [51] demonstrated that this type of drugs is activated in the mildly acidic extracellular space of tumors, and used at a non-toxic dose, have been shown to suppress the growth of human melanoma in nude mice [55]. Moreover, omeprazole the racemate form, from which the R- and S-isomers (esomeprazole) can be isolated, potentiates the growth-retard effect of cisplatin on human melanomas, probably facilitating the intracellular uptake of the chemotherapeutic drug [56]. Recent studies have elucidated that this type of PPIs can exert anti-inflammatory effects unrelated to the inhibition of gastric acid production [57]. Some non gastric cells, like neutrophils and endothelial cells, express V-type H+-ATPases that may pump proton ions into the extracellular space, where a low extracellular pH stimulates the release of IL-1β by human monocytes [58]. In accordance with our findings, Handa et al. [59] observed that omeprazole and lansoprazole blocked IL-8 production in human umbilical endothelial cells, possibly by interfering with NF-κB pathway. Hashioka et al. [39] proved that these PPIs significantly reduced TNF-α secretion by stimulated monocytic THP-1 cells in a concentration dependent manner.
On the whole, our results identify acidity as a positive regulator of VEGF-C expression and secretion in melanoma cells via NF-κB activation and thereby implicate pH of tumor environment as lymphangiogenesis controller. Indeed, we proved that acidity is also affective in promoting VEGF-C expression in breast and prostate carcinoma cells.
Our data further suggest that esomeprazole abolishes VEGF-C expression when tumor cells are exposed to acidity or both acidity and IL-1β. Thus, we may speculate that to inhibit lymphangiogenesis and interfere with metastatic dissemination through lymphatic vessels, might be considered new therapeutic strategies able to regulate acidity and inflammatory cytokines.
Abbreviations
- HIF1-α:
-
Hypoxia inducible factor-α
- IkB:
-
Inhibitor of kappa B
- IL-1β:
-
Interleukin-1β
- NF-κB:
-
Nuclear factor kappa B
- PPI:
-
Proton pump inhibitor
- SLN:
-
Sentinel lymph node
- siRNA:
-
Short interfering RNA
- VEGF-A:
-
Vascular endothelial growth factor A
- VEGF-C:
-
Vascular endothelial growth factor C
- VEGFR-3:
-
Vascular endothelial growth factor receptor-3
References
Rinderknecht M, Detmar M (2008) Tumor lymphangiogenesis and melanoma metastasis. J Cell Physiol 216:347–354
Dadras SS, Paul T, Bertoncini J, Brown LF, Muzikansky A, Jackson DG et al (2003) Tumor lymphangiogenesis: a novel prognostic indicator for cutaneous melanoma metastasis and survival. Am J Pathol 162:1951–1960
Cao Y (2005) Opinion: emerging mechanisms of tumour lymphangiogenesis and lymphatic metastasis. Nat Rev Cancer 5:735–743
Tammela T, Alitalo K (2010) Lymphangiogenesis: molecular mechanisms and future promise. Cell 140:460–476
Alitalo K, Tammela T, Petrova TV (2005) Lymphangiogenesis in development and human disease. Nature 438:946–953
Plate K (2001) From angiogenesis to lymphangiogenesis. Nat Med 7:151–152
Achen MG, McColl BK, Stacker SA (2005) Focus on lymphangiogenesis in tumor metastasis. Cancer Cell 7:121–127
Karkkainen MJ, Haiko P, Sainio K, Partanen J, Taipale J, Petrova TV et al (2004) Vascular endothelial growth factor C is required for sprouting of the first lymphatic vessels from embryonic veins. Nat Immunol 5:74–80
Su JL, Yen CJ, Chen PS, Chuang SE, Hong CC, Kuo IH et al (2007) The role of the VEGF-C/VEGFR-3 axis in cancer progression. Br J Cancer 96:541–545
Burton JB, Priceman SJ, Sung JL, Brakenhielm E, An DS, Pytowski B et al (2008) Suppression of prostate cancer nodal and systemic metastasis by blockade of the lymphangiogenic axis. Cancer Res 68:7828–7837
He Y, Rajantie I, Pajusola K, Jeltsch M, Holopainen T, Yla-Herttuala S et al (2005) Vascular endothelial cell growth factor receptor 3-mediated activation of lymphatic endothelium is crucial for tumor cell entry and spread via lymphatic vessels. Cancer Res 65:4739–4746
He Y, Kozaki K, Karpanen T, Koshikawa K, Yla-Herttuala S, Takahashi T et al (2002) Suppression of tumor lymphangiogenesis and lymph node metastasis by blocking vascular endothelial growth factor receptor 3 signaling. J Natl Cancer Inst 94:819–825
Skobe M, Hawighorst T, Jackson DG, Prevo R, Janes L, Velasco P et al (2001) Induction of tumor lymphangiogenesis by VEGF-C promotes breast cancer metastasis. Nat Med 7:192–198
Harrell MI, Iritani BM, Ruddell A (2007) Tumor-induced sentinel lymph node lymphangiogenesis and increased lymph flow precede melanoma metastasis. Am J Pathol 170:774–786
Hoshida T, Isaka N, Hagendoorn J, di Tomaso E, Chen YL, Pytowski B, Fukumura D, Padera TP, Jain RK (2006) Imaging steps of lymphatic metastasis reveals that vascular endothelial growth factor-C increases metastasis by increasing delivery of cancer cells to lymph nodes: therapeutic implications. Cancer Res 66:8065–8075
Ji RC (2006) Lymphatic endothelial cells, tumor lymphangiogenesis and metastasis: new insights into intratumoral and peritumoral lymphatics. Cancer Metastasis Rev 25:677–694
Kunkel M, Reichert TE, Benz P, Lehr HA, Jeong JH, Wieand S, Bartenstein P, Wagner W, Whiteside TL (2003) Overexpression of Glut-1 and increased glucose metabolism in tumors are associated with a poor prognosis in patients with oral squamous cell carcinoma. Cancer 97:1015–1024
Helmlinger G, Yuan F, Dellian M, Jain RK (1997) Interstitial pH and pO2 gradients in solid tumors in vivo: high-resolution measurements reveal a lack of correlation. Nat Med 3:177–182
Schornack PA, Gillies RJ (2003) Contributions of cell metabolism and H+ diffusion to the acidic pH of tumors. Neoplasia 5:135–145
Gillies RJ, Raghunand N, Karczmar GS, Bhujwalla ZM (2002) MRI of the tumor microenvironment. J Magn Reson Imaging 16:430–450
Cardone RA, Casavola V, Reshkin SJ (2005) The role of disturbed pH dynamics and the Na+/H+ exchanger in metastasis. Nat Rev Cancer 5:786–795
Hinton A, Bond S, Forgac M (2009) V-ATPase functions in normal and disease processes. Pflugers Arch 457:589–598
Casey JR, Grinstein S, Orlowski J (2010) Sensors and regulators of intracellular pH. Nat Rev Mol Cell Biol 11:50–61
Walenta S, Wetterling M, Lehrke M, Schwickert G, Sundfør K, Rofstad EK, Mueller-Klieser W (2000) High lactate levels predict likelihood of metastases, tumor recurrence, and restricted patient survival in human cervical cancers. Cancer Res 60:916–921
Raghunand N, Mahoney B, van Sluis R, Baggett B, Gillies RJ (2001) Acute metabolic alkalosis enhances response of C3H mouse mammary tumors to the weak base mitoxantrone. Neoplasia 3:227–235
Fischer K, Hoffmann P, Voelkl S, Meidenbauer N, Ammer J, Edinger M et al (2007) Inhibitory effect of tumor cell-derived lactic acid on human T cells. Blood 109:3812–3819
Morita T, Nagaki T, Fukuda I, Okumura K (1992) Clastogenicity of low pH to various cultured mammalian cells. Mutat Res 268:297–305
Rofstad EK, Mathiesen B, Kindem K, Galappathi K (2006) Acidic extracellular pH promotes experimental metastasis of human melanoma cells in athymic nude mice. Cancer Res 66:6699–6707
Moellering RE, Black KC, Krishnamurty C, Baggett BK, Stafford P, Rain M, Gatenby RA, Gillies RJ (2008) Acid treatment of melanoma cells selects for invasive phenotypes. Clin Exp Metastasis 25:411–425
Provent P, Benito M, Hiba B, Farion R, López-Larrubia P, Ballesteros P, Rémy C, Segebarth C, Cerdán S, Coles JA, García-Martín ML (2007) Serial in vivo spectroscopic nuclear magnetic resonance imaging of lactate and extracellular pH in rat gliomas shows redistribution of protons away from sites of glycolysis. Cancer Res 67:7638–7645
Pouysségur J, Dayan F, Mazure NM (2006) Hypoxia signalling in cancer and approaches to enforce tumour regression. Nature 441:437–443
Shi Q, Le X, Wang B, Abbruzzese JL, Xiong Q, He Y et al (2001) Regulation of vascular endothelial growth factor expression by acidosis in human cancer cells. Oncogene 20:3751–3756
Scott PA, Gleadle JM, Bicknell R, Harris AL (1998) Role of the hypoxia sensing system, acidity and reproductive hormones in the variability of vascular endothelial growth factor induction in human breast carcinoma cell lines. Int J Cancer 75:706–712
Elias AP, Dias S (2008) Microenvironment changes (in pH) affect VEGF alternative splicing. Cancer Microenviron 1:131–139
Santini R, Vinci MC, Pandolfi S, Penachioni JY, Montagnani V, Olivito B et al (2012) Hedgehog-GLI signaling drives self-renewal and tumorigenicity of human melanoma-initiating cells. Stem Cells 30:1808–1818
Chen TR (1977) In situ detection of mycoplasma contamination in cell cultures by fluorescent Hoechst 33258 stain. Exp Cell Res 104:255–262
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2[-Delta Delta C(T)] Method. Methods 25(4):402–408
Joukov V, Pajusola K, Kaipainen A, Chilov D, Lahtinen I, Kukk E, Saksela O,Kalkkinen N, Alitalo K. A novel vascular endothelial growth factor, VEGF-C, is a ligand for the Flt4 (VEGFR-3) and KDR (VEGFR-2) receptor tyrosine kinases. EMBO J. 1996 Apr 1;15(7):1751. PubMed PMID: 8612600; PubMed Central PMCID: PMC450088
Hashioka S, Klegeris A, McGeer PL (2009) Proton pump inhibitors exert anti-inflammatory effects and decrease human microglial and monocytic THP-1 cell neurotoxicity. Exp Neurol 217:177–183
Ristimäki A, Narko K, Enholm B, Joukov V, Alitalo K (1998) Proinflammatory cytokines regulate expression of the lymphatic endothelial mitogen vascular endothelial growth factor-C. J Biol Chem 273:8413–8418
Chilov D, Kukk E, Taira S, Jeltsch M, Kaukonen J, Palotie A, Joukov V, Alitalo K (1997) Genomic organization of human and mouse genes for vascular endothelial growth factor C. J Biol Chem 272:25176–25183
Cha HS, Bae EK, Koh JH, Chai JY, Jeon CH, Ahn KS et al (2007) Tumor necrosis factor-alpha induces vascular endothelial growth factor-C expression in rheumatoid synoviocytes. J Rheumatol 34:16–19
Karkkainen MJ, Haiko P, Sainio K, Partanen J, Taipale J, Petrova TV, Jeltsch M, Jackson DG, Talikka M, Rauvala H, Betsholtz C, Alitalo K (2004) Vascular endothelial growth factor C is required for sprouting of the first lymphatic vessels from embryonic veins. Nat Immunol 5:74–80
Watanabe Y, Miura I, Ohgami Y, Fujiwara M (1998) Extracellular presence of IL-8 in the astrocyte-rich cultured cerebellar granule cells under acidosis. Life Sci 63:1037–1046
Shi Q, Abbruzzese JL, Huang S, Fidler IJ, Xiong Q, Xie K (1999) Constitutive and inducible interleukin 8 expression by hypoxia and acidosis renders human pancreatic cancer cells more tumorigenic and metastatic. Clin Cancer Res 5:3711–3721
Xie K (2001) Interleukin-8 and human cancer biology. Cytokine Growth Factor Rev 12:375–391
Xu L, Fidler IJ (2000) Acidic pH-induced elevation in interleukin 8 expression by human ovarian carcinoma cells. Cancer Res 60:4610–4616
Bellocq A, Suberville S, Philippe C, Bertrand F, Perez J, Fouqueray B, Cherqui G, Baud L (1998) Low environmental pH is responsible for the induction of nitric-oxide synthase in macrophages. Evidence for involvement of nuclear factor-kappaB activation. J Biol Chem 273:5086–5092
Sennoune SR, Bakunts K, Martínez GM, Chua-Tuan JL, Kebir Y, Attaya MN, Martínez-Zaguilán R (2004) Vacuolar H+-ATPase in human breast cancer cells with distinct metastatic potential: distribution and functional activity. Am J Physiol Cell Physiol 286:C1443–C1452
Sennoune SR, Martinez-Zaguilan R (2007) Plasmalemmal vacuolar H+-ATPases in angiogenesis, diabetes and cancer. J Bioenerg Biomembr 39:427–433
Fais S, De Milito A, You H, Qin W (2007) Targeting vacuolar H+-ATPases as a new strategy against cancer. Cancer Res 67:10627–10630
Pérez-Sayáns M, García-García A, Reboiras-López MD, Gándara-Vila P (2009) Role of V-ATPases in solid tumors: importance of the subunit C (Review). Int J Oncol 34:1513–1520
Hinton A, Sennoune SR, Bond S, Fang M, Reuveni M, Sahagian GG, Jay D, Martinez-Zaguilan R, Forgac M (2009) Function of a subunit isoforms of the V-ATPase in pH homeostasis and in vitro invasion of MDA-MB231 human breast cancer cells. J Biol Chem 284:16400–16408
Martínez-Zaguilán R, Gillies RJ (1992) A plasma membrane V-type H(+)-ATPase may contribute to elevated intracellular pH (pHin) in some human tumor cells. Ann N Y Acad Sci 671:478–480
De Milito A, Canese R, Marino ML, Borghi M, Iero M, Villa A, Venturi G, Lozupone F, Iessi E, Logozzi M, Della Mina P, Santinami M, Rodolfo M, Podo F, Rivoltini L, Fais S (2010) pH-dependent antitumor activity of proton pump inhibitors against human melanoma is mediated by inhibition of tumor acidity. Int J Cancer 127:207–219
Luciani F, Spada M, De Milito A, Molinari A, Rivoltini L, Montinaro A, Marra M, Lugini L, Logozzi M, Lozupone F, Federici C, Iessi E, Parmiani G, Arancia G, Belardelli F, Fais S (2004) Effect of proton pump inhibitor pretreatment on resistance of solid tumors to cytotoxic drugs. J Natl Cancer Inst 96:1702–1713
Kedika RR, Souza RF, Spechler SJ (2009) Potential anti-inflammatory effects of proton pump inhibitors: a review and discussion of the clinical implications. Dig Dis Sci 54:2312–2317
Jancic CC, Cabrini M, Gabelloni ML, Rodríguez Rodrigues C, Salamone G, Trevani AS, Geffner J (2012) Low extracellular pH stimulates the production of IL-1β by human monocytes. Cytokine 57:258–268
Handa O, Yoshida N, Fujita N, Tanaka Y, Ueda M, Takagi T et al (2006) Molecular mechanisms involved in anti-inflammatory effects of proton pump inhibitors. Inflamm Res 55:476–480
Acknowledgments
We thank Dr Stefano Fais of the Istituto Superiore di Sanità (ISS, Roma) for kindly donation of esomeprazole. This study was financially supported by grants from Istituto Toscano Tumori and Ente Cassa di Risparmio di Firenze.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Peppicelli, S., Bianchini, F., Contena, C. et al. Acidic pH via NF-κB favours VEGF-C expression in human melanoma cells. Clin Exp Metastasis 30, 957–967 (2013). https://doi.org/10.1007/s10585-013-9595-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10585-013-9595-4